ORIGINAL ARTICLE. most commonly result. involving the paranasal sinuses, the overlying facial skin, or both. Such defects may result in substantial
|
|
|
- Bathsheba Snow
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Use of Precontoured Positioning Plates and Pericranial Flaps in Midfacial Reconstruction to Optimize Aesthetic and Functional Outcomes Yadranko Ducic, MD, FRCSC; Lance E. Oxford, MD Objectives: To present our experience with reconstruction of midfacial defects using precontoured positioning plates with or without pericranial flaps and to describe our technique in detail. Methods: Thirty-two consecutive patients with midfacial defects subsequent to oncologic resection that were reconstructed primarily with cranial bone grafts and precontoured positioning plates were reviewed for type of defect, functional outcome, complications, and postoperative appearance. Results: Primary reconstruction of all defects in this series was performed. Defects involved the orbital rim, orbital floor, or both in 28 patients (88%), the body of the zygoma in 24 patients (75%), and extended to the skull base in 16 patients (50%). Pericranial flaps were used to cover the bone grafts in 22 patients (69%). Postoperative radiotherapy was performed in 22 patients (69%), preoperative radiotherapy in 5 (16%), and the other 5 (16%) had no radiotherapy. There were no intraoperative complications, and postoperative complications included plate exposure (n=2), ectropion (n=3), and partial bone graft loss or resorption subsequent to completion of radiotherapy (n=2). Postoperatively, appearance was excellent in 24 patients, fair in 6 patients, and poor in 2 patients. Secondary reconstructive procedures were performed in 4 patients (12%). Follow-up ranged from 12 months to 6 years (median, 4.2 years). Conclusions: Precontoured positioning plates with or without pericranial flaps enable precise reconstruction of midfacial defects with precise incorporation of cranial bone grafts. In our series we routinely covered the bone grafts with well-vascularized tissues, leading to a low incidence of complications and excellent aesthetic results. Arch Facial Plast Surg. 2005;7: Author Affiliations: Department of Otolaryngology Head and Neck Surgery, The University of Texas Southwestern Medical Center, Dallas, and the Division of Otolaryngology and Facial Plastic Surgery, John Peter Smith Hospital, Fort Worth, Tex. MIDFACIAL DEFECTS most commonly result after trauma or resection of neoplasms involving the paranasal sinuses, the overlying facial skin, or both. Such defects may result in substantial functional and aesthetic morbidity. Reconstructive goals include obtaining a healed wound, separating the oral cavity from the defect to aid oral intake and speech, supporting orbital contents, and optimizing facial aesthetics. While prostheses are often successful with maxillectomy defects in obturating the palate, especially if sufficient dentition is preserved, 1 the resection of orbital bone and the zygoma compromises support for facial soft tissue and the globe. Reconstruction is more challenging after total maxillectomy if orbital contents are preserved. 2 Numerous methods have been described for reconstructing maxillectomy and midfacial defects, including local or regional flaps, 3 prostheses, bone grafts, titanium mesh, 4,5 and free flaps. 1,6-10 Traditionally, reconstruction of maxillectomy defects involved a dental obturator and skin grafts to the internal mucosal defect. Such reconstruction has the advantage of enabling easy examination to detect tumor recurrence. However, the lack of bony support results in soft tissue contracture that is often exacerbated by postoperative radiotherapy. The advantage of being able to directly survey the defect has been minimized by the improved sensitivity of magnetic resonance imaging and positron emission tomography or computed tomography to detect tumor recurrence after maxillectomy reconstruction. A wide variety of free flaps have been recommended for reconstruction of maxillectomy defects. The rectus abdominis myocutaneous flap is easy to harvest and provides a large volume of tissue to obliterate large palate, orbital exenteration, and skull base defects. 8 However, it is difficult to precisely reconstruct the complex configuration of the malar eminence and orbital rim with soft tissue flaps. Cov- 387
2 Figure 2. Positioning plates have been preadapted to span the proposed area of resection. Note placement of screws well away from the area that will be resected: left nasal bone, zygomatic arch, and right anterior maxilla. Figure 1. Preoperative axial magnetic resonance image demonstrates extensive squamous cell carcinoma of the left maxillary sinus with extension into the skull base. ering bone grafts with such bulky flaps makes ultimate contour results generally mediocre at best. Osteocutaneous free flaps may be used to reconstruct midfacial skeletal defects, but the use of multiple osteotomies to precisely contour the flap may compromise the bony or cutaneous portions of the flap. 2 The use of cranial bone grafts is the traditional method for reconstructing orbital defects. 11 While reconstruction of the facial skeleton may appear straightforward, it is often difficult to recreate the complex 3-dimensional (3-D) anatomy of the zygoma 8 and orbit. What we term precontoured positioning plates are plates precisely contoured to the midfacial skeleton to allow 3-D reconstruction of bony defects with cranial bone grafts. In this article we review the experience of 1 of us (Y.D.) with this method of reconstruction of midfacial defects. METHODS All patients undergoing reconstruction of orbitozygomatic defects with cranial bone grafts and positioning plates were included in this review. A total of 32 patients treated by 1 of us (Y.D.) from September 1997 to September 2003 with this method were reviewed in detail. All patients were followed up for at least 12 months. Patients requiring substantial palatal resection who were thought to be good candidates for successful prosthetic dental obturation were evaluated preoperatively by a maxillofacial prosthodontist, and a surgical obturator was created preoperatively. Medical records were reviewed for location of defect, additional reconstructive procedures performed, and complications. Preoperative and postoperative photographs were reviewed to evaluate aesthetic results. Patients were interviewed and asked to rate their reconstructive result as excellent, fair, or poor. In cases in which the outer frame or contour of the midfacial skeleton was not deformed by neoplasm, 1.3- and 1.7-mm titanium miniplates were bent to conform to the expected defect (Figures 1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11, 12, and 13). Generally, at least 3 such plates were used. Each plate spanned the defect and extended well medially, laterally, or superiorly away from the area of expected resection. A minimum of 3 screws were placed on each end of the plate. The goal was to overlap the areas beneath the precontoured positioning plates to provide a scaffoldlike fingerprint of the anticipated defect. The plates and screws were removed and labeled. With total maxillectomy defects, positioning plates were anchored medially at the superior remnant of the nasomaxillary buttress and over the radix and laterally at the remaining zygomatic arch. If the midfacial skeleton was deformed and unsuitable for use as a template for positioning plates, then plates were contoured on a human skull placed in a sterile plastic bag on a side table. 4 Alternatively, a 3-D acrylic model based on the patient s computed tomography scan is used. The model s contour deformity is corrected on a side table with a round burr, followed by placement of positioning plates as mentioned earlier. After resection of the osseous midface, the positioning plates are returned to the predrilled proximal and distal holes on the patient s remaining facial skeleton. Outer table calvarial bone grafts were harvested from the patient s nondominant parietal skull. In patients requiring a craniotomy, grafts were harvested from the inner cortex of the bone flap. The grafts were contoured and secured to the scaffolding provided by the positioning plates. If there was lack of mucosal coverage intraorally, vascularized tissue flaps, most commonly extended pericranial flaps, 12 were routinely used to cover the bone grafts and plates in an effort to decrease the risk of resorption and extrusion. Pericranial flaps were based anteriorly and passed via the nasofrontal region, or laterally and passed into the midface over the zygomatic arch remnant. Temporary dental obturators were secured to the remaining hard palate with titanium screws. RESULTS Our technique enabled primary reconstruction of all defects for which such reconstruction was attempted. Disease requiring resection of the midfacial segment included squamous cell carcinoma (n=19), sinonasal undifferentiated carcinoma (n=4), sarcoma (n=4), adenocarcinoma (n=3), and myxoma (n=2). Defects involved the orbital rim, floor, or both in 28 patients (88%), the body of the zygoma in 24 patients (75%), and extended to the skull base in 16 patients (50%). Pericranial flaps were used to envelop the bone grafts in 22 patients (69%). In addition, 14 temporalis muscle flaps were used. Postoperative radiotherapy was performed in 22 pa- 388
3 Orbit Nose ITF PPS 1 cm Molar Figure 3. Left extended maxillectomy to include the left maxilla, infratemporal fossa (ITF), parapharyngeal space (PPS), orbit, and nasal cavity with attached septum. Figure 5. Pericranial flap has now been passed into the midface and is being retracted through the mouth to demonstrate length. Figure 4. Left laterally based pericranial flap has been harvested (retracted with forceps); temporalis muscle flap is being reflected inferior to the visualized portion of the left auricle. Figure 6. Positioning plates have been re-placed and bone grafts have been placed on the undersurface of the new scaffold. Pericranial flap will now wrap the bone grafts. tients (69%) and was initiated within 8 weeks of resection and reconstruction. Doses in this group ranged from 5500 to 7000 rad (55-70 Gy). Preoperative radiotherapy was used in another 5 patients (16%). There were no intraoperative complications, and postoperative complications included plate exposure in 2 patients, ectropion in 3 patients, and partial bone graft loss or resorption subsequent to completion of radiotherapy in 1 patient each. There was no evidence of complete bone resorption or loss. Postoperative appearance was excellent in 24 patients, fair in 6 patients, and poor in 2 patients, as deemed by the patients themselves. Secondary reconstructive procedures were performed in 4 patients (12%). Follow-up ranged from 12 months to 6 years (median, 4.2 years). COMMENT Midfacial defects present a tremendous challenge for successful reconstruction. Numerous approaches have been described for reconstruction of midfacial and maxillectomy defects, including temporalis muscle flaps 3 ; pectoralis major myocutaneous flaps 13 ; latissimus dorsi, 7 scapular, or parascapular free flaps 9,10 ; and rectus abdominis free flaps. 8 Preoperative evaluation is critical in planning midfacial reconstruction. After maxillectomy, the status of the Figure 7. Pericranial flap has completely wrapped the bone grafts on the oral side. remaining dentition and expected size of the palatal defect determine the likely success of a palatal obturator. We routinely consult a maxillofacial prosthodontist preoperatively. In patients requiring extensive palatal resections who desire dental implants, osteocutaneous free flaps can provide successful dental rehabilitation. Futran et al 1 reported the use of fibula osteocutaneous free flaps in 27 patients with midfacial defects that involved greater than 50% of the maxillary dentition. Osseointegrated implants were placed in 18 patients, and 14 patients were able to tolerate 389
4 A B Figure 8. Patient in Figures 1 through 7. A, Preoperative basal view. B, Postoperative basal view demonstrates adequate maxillary contour. Figure 9. Preoperative coronal computed tomographic scan in a patient with massive odontogenic neoplasm of the right maxilla with involvement of the orbital floor. Figure 11. Postoperative 3-dimensional computed tomographic scan demonstrates adequate restoration of the right midface with positioning plates and bone grafts. Figure 10. After resection of tumor and replacement of positioning plates, bone grafts have been brought into position. They will be covered. a regular diet. Cosmetic results were excellent in patients with inferior maxillary defects. In patients with loss of the orbital rim, the malar prominence, or both, the aesthetic results were fair secondary to flattening of these regions. Secondary procedures to correct ectropion were required in 3 patients. 1 In patients with large midfacial defects the rectus abdominis myocutaneous free flap is a reasonable alternative. Advantages of this flap include ease of harvest with the patient in the supine position, a long pedicle, and a large volume for potentially obliterating orbital exenteration or skull base defects. Browne and Burke 8 reported a series of 12 patients with maxillectomy defects reconstructed with the rectus abdominis free flap. Reconstruction allowed all 9 patients with palatal defects to resume their preoperative diet. When total maxillectomy is combined with orbital exenteration, Cordeiro and Santamaria 14 recommend a rectus myocutaneous free flap with 3 skin islands, for the orbit, lateral nasal wall, and hemipalate. A disadvantage of the flap is the expected atrophy of one third of the flap volume and the inability of this flap to duplicate the patient s premorbid skeletal form
5 A B Figure 12. Patient in Figures 9 through 11. A, Preoperative basal view. B, Postoperative basal view demonstrates adequate midface projection. A B Figure 13. Patient in Figures 9 through 12. A, Preoperative frontal view. B, Postoperative frontal view demonstrates adequate midfacial width and symmetry. With midfacial defects involving the body of the zygoma and the orbital rim, it can be challenging to obtain excellent aesthetic outcomes. In a series of 14 patients with primary reconstruction of total maxillectomy defects with preservation of orbital contents, Cordeiro and Santamaria 14 reported that the malar eminence can never be reconstructed well with soft tissue flaps alone. Nonvascularized bone grafts from the calvarium, ribs, and iliac crest were used for orbital floor reconstruction. Reconstruction of the malar eminence was performed secondarily with a free bone graft from the zygomatic remnant to the maxilla adjacent to the nasal spine. Soft tissue reconstruction to obturate the palatal defect was performed with a myocutaneous rectus abdominis free flap in 12 patients and with a pedicled temporalis muscle flap in 2 patients. They did not experience any infections or resorption of the free bone grafts. The most common complication was lower eyelid ectropion in 76.9% of patients. 2 Lee et al 15 also believe that cranial bone grafts provide superior reconstruction of the orbital rim and floor compared with free soft tissue flaps. They reported reconstruction of the orbital rim and floor after maxillectomy with a vascularized outer calvarial bone pedicled on the superficial temporal artery. They think that the natural curvature of outer calvarial bone is well suited for reconstruction of orbital bony defects. Ectropion occurred in 1 patient, and enophthalmos in 2 patients. 15 Successful reconstruction of orbital rim defects after orbital exenteration with free flaps was reported by Chepeha et al. 6 For defects involving less than 30% of the bony orbital rim, reconstruction was performed with osseocutaneous radial forearm free flaps. With more extensive orbital rim defects and defects involving cheek skin or the bony malar eminence, scapular free flaps were used. 6 Cordeiro et al 2 have cautioned that using an osteocutaneous free flap to reconstruct both the orbital floor and maxillary buttress may lead to compromise of the bony and cutaneous portions of a flap. In our series, we were able to obtain excellent aesthetic outcomes using positioning plates with cranial bone grafts for primary reconstruction of the zygoma and orbital rims. Fashioning the plates on the midface before resection allows accurate 3-D reconstruction of these complex regions. Precise reconstruction of the 391
6 orbitozygomatic regions is critical for providing support for facial and orbital soft tissues. We believe that the use of precontoured positioning plates is invaluable in this regard and will naturally lead to improved outcomes compared with simple eyeballing. The scaffold they provide will ensure restoration of the premorbid osseous skeleton. Cranial bone grafts are a well-accepted method for reconstruction of facial bony defects. Free membranous calvarial bone has been shown to have lower rates of resorption compared with endochondral bone grafts from the ilium or ribs. 16 We agree with Pollice and Frodel 17 that covering bone grafts with well-vascularized tissue may decrease the risks for resorption and extrusion. In their series of 6 patients with secondary reconstruction of maxillectomy defects, a pedicled temporoparietal flap was routinely used with cranial bone grafts. 17 Covering the bone grafts with a vascularized radial forearm free flap is another option. Our preference is to use extended pericranial flaps to envelop free bone grafts and positioning plates. Pericranial flaps provide supple, thin tissue that may be pedicled centrally or laterally to reach midfacial reconstructions. 12 Pedicled temporalis muscle flaps are also useful with maxillectomy reconstruction to provide well-vascularized tissue on the internal surface of the bone grafts, specifically in orbital floor graft coverage. The donor site aesthetic morbidity may be well managed with primary hydroxyapatite cranioplasty and secondary lipotransfer to the temporal fossa. The temporalis muscle is useful for obliterating the maxillectomy defect, and it may be primarily skin grafted or allowed to mucosalize. We found a low incidence of complications with our technique of orbitozygomatic reconstruction. The most common complication was ectropion, which was similarly found in other series of midfacial reconstructions and occurred in as many as 79% of patients in 1 review. 2,15,17 Although most of our patients received external beam radiotherapy, the incidence of resorption or extrusion was low. We attribute this to good soft tissue coverage of all grafts. In fact, none of our patients experienced intraoral or mucosal extrusion. Both incidences of extrusion and partial resorption occurred underneath the nasal dorsal skin portion of the reconstruction on average 3.5 years after radiotherapy and were repaired with simple local soft tissue flaps. CONCLUSIONS The use of precontoured positioning plates with cranial bone grafts to repair orbitozygomatic defects is a reliable technique for precise reconstruction of the midfacial skeleton. This technique allows restoration of the 3-D structural support for facial and orbital soft tissues. We recommend enveloping the bone grafts with vascularized tissue such as pericranial flaps, which may be brought into the midface to promote graft viability and decrease resorption and extrusion. Accepted for Publication: April 26, Correspondence: Yadranko Ducic, MD, FRCS(C), Division of Otolaryngology and Facial Plastic Surgery, John Peter Smith Hospital, 1500 S Main St, Suite 303, Fort Worth, TX (yducic@sbcglobal.net). REFERENCES 1. Futran ND, Wadsworth JT, Villaret D, Farwell DG. Midface reconstruction with the fibula free flap. Arch Otolaryngol Head Neck Surg. 2002;128: Cordeiro PG, Santamaria E, Kraus DH, Strong EW, Shah JP. Reconstruction of total maxillectomy defects with preservation of the orbital contents. Plast Reconstr Surg. 1998;102: Koranda FC, McMahon MF, Jernstrom VR. The temporalis muscle flap for intraoral reconstruction. Arch Otolaryngol Head Neck Surg. 1987;113: Ducic Y. Three-dimensional alloplastic orbital reconstruction in skull base surgery. Laryngoscope. 2001;111: Schubert W, Gear AJL, Lee C, et al. Incorporation of titanium mesh in orbital and midface reconstruction. Plast Reconstr Surg. 2002;110: Chepeha DB, Wang SJ, Marentette LJ, et al. Restoration of the orbital aesthetic subunit in complex midface defects. Laryngoscope. 2004;114: Coleman JJ. Microvascular approach to function and appearance of large orbital maxillary defects. Am J Surg. 1989;158: Browne JD, Burke AJC. Benefits of routine maxillectomy and orbital reconstruction with the rectus abdominis free flap. Otolaryngol Head Neck Surg. 1999; 121: Sullivan MJ, Carroll WR, Baker SR, Crompton R, Smith-Wheelock M. The free scapular flap for head and neck reconstruction. Am J Otolaryngol. 1990;11: Chandrasekhar B, Lorant JA, Terz JJ. Parascapular free flaps for head and neck reconstruction. Am J Surg. 1990;160: Ilankovan V, Jackson IT. Experience in the use of calvarial bone grafts in orbital reconstruction. Br J Oral Maxillofac Surg. 1992;30: Smith JE, Ducic Y. The versatile extended pericranial flap for closure of skull base defects. Otolaryngol Head Neck Surg. 2004;130: Sasaki CT, Ariyan S, Spencer D, Buckwalter J. Pectoralis major myocutaneous reconstruction of the anterior skull base. Laryngoscope. 1985;95: Cordeiro PG, Santamaria E. A classification system and algorithm for reconstruction of maxillectomy and midfacial defects. Plast Reconstr Surg. 2000; 105: Lee HB, Hong JP, Kim KT, Chung YK, Tark KC, Bong JP. Orbital floor and infraorbital rim reconstruction after total maxillectomy using a vascularized calvarial bone flap. Plast Reconstr Surg. 1999;104: Zins JE, Whitaker LA. Membranous versus endochondral bone: implications for craniofacial reconstruction. Plast Reconstr Surg. 1983;72: Pollice PA, Frodel JL Jr. Secondary reconstruction of upper midface and orbit after total maxillectomy. Arch Otolaryngol Head Neck Surg. 1998;124:
Maxillary Reconstruction with the Free Fibula Flap
 Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Maxillary Reconstruction with the Free Fibula Flap Xin Peng, D.D.S., Ph.D., Chi Mao, D.D.S., Ph.D., Guang-yan Yu, D.D.S., Ph.D., Chuan-bin Guo, D.D.S., Ph.D., Min-xian Huang, D.D.S., and Yi Zhang, D.D.S.,
Vascularized Rib for Facial Reconstruction
 Vascularized Rib for Facial Reconstruction Steven P. Davison, M.D., D.D.S., James H. Boehmler, M.D., Jason C. Ganz, M.D., and Bruce Davidson, M.D. Washington, D.C. The reconstruction of maxillectomy defects
Vascularized Rib for Facial Reconstruction Steven P. Davison, M.D., D.D.S., James H. Boehmler, M.D., Jason C. Ganz, M.D., and Bruce Davidson, M.D. Washington, D.C. The reconstruction of maxillectomy defects
 This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
This article was published in an Elsevier journal. The attached copy is furnished to the author for non-commercial research and education use, including for instruction at the author s institution, sharing
The nose, forming a prominent aesthetic highlight
 Nasal reconstruction in surgery of the anterior skull base YADRANKO DUCIC, MD, FACS, AND ALLISON T. PONTIUS, MD, Dallas and Fort Worth, Texas From the Department of Otolaryngology Head and Neck Surgery,
Nasal reconstruction in surgery of the anterior skull base YADRANKO DUCIC, MD, FACS, AND ALLISON T. PONTIUS, MD, Dallas and Fort Worth, Texas From the Department of Otolaryngology Head and Neck Surgery,
A Study of Classification Systems for Maxillectomy Defects
 A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
A Study of Classification Systems for Maxillectomy Defects Zubair Durrani FFDRCS, FRCS, FRCS (OMFS)* Syed Ghazanfar Hassan FFDRCS** Shomaila Ameer Alam BDS*** * Associate Professor & Consultant Oral and
Accepted 13 March 2008 Published online 18 July 2008 in Wiley InterScience ( DOI: /hed.20874
 ORIGINAL ARTICLE ZYGOMATICOMAXILLARY BUTTRESS RECONSTRUCTION OF MIDFACE DEFECTS WITH THE OSTEOCUTANEOUS RADIAL FOREARM FREE FLAP Patricio Andrades, MD, Eben L. Rosenthal, MD, William R. Carroll, MD, Christopher
ORIGINAL ARTICLE ZYGOMATICOMAXILLARY BUTTRESS RECONSTRUCTION OF MIDFACE DEFECTS WITH THE OSTEOCUTANEOUS RADIAL FOREARM FREE FLAP Patricio Andrades, MD, Eben L. Rosenthal, MD, William R. Carroll, MD, Christopher
Three-Dimensional Alloplastic Orbital Reconstruction in Skull Base Surgery
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. HowIDoIt A Targeted Problem and Its Solution Three-Dimensional
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. HowIDoIt A Targeted Problem and Its Solution Three-Dimensional
There has been a resurgence in the description CME. Vascularized Calvarial Bone Flaps and Midface Reconstruction
 CME Vascularized Calvarial Bone Flaps and Midface Reconstruction Steven P. Davison, M.D., D.D.S. Ali N. Mesbahi, M.D. Mark W. Clemens, M.D. Catherine A. Picken, M.D. Washington, D.C. Learning Objectives:
CME Vascularized Calvarial Bone Flaps and Midface Reconstruction Steven P. Davison, M.D., D.D.S. Ali N. Mesbahi, M.D. Mark W. Clemens, M.D. Catherine A. Picken, M.D. Washington, D.C. Learning Objectives:
ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS
 ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS Jesse E. Smith, MD, 1,2 Yadranko Ducic, MD, FRCS(C), 1,2,3 Robert T. Adelson, MD 4 1 Department of Otolaryngology-Head and
ORIGINAL ARTICLE TEMPORALIS MUSCLE FLAP FOR RECONSTRUCTION OF SKULL BASE DEFECTS Jesse E. Smith, MD, 1,2 Yadranko Ducic, MD, FRCS(C), 1,2,3 Robert T. Adelson, MD 4 1 Department of Otolaryngology-Head and
Interesting Case Series. Scalp Reconstruction With Free Latissimus Dorsi Muscle
 Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
Interesting Case Series Scalp Reconstruction With Free Latissimus Dorsi Muscle Danielle H. Rochlin, BA, Justin M. Broyles, MD, and Justin M. Sacks, MD Department of Plastic and Reconstructive Surgery,
BUILDING A. Achieving total reconstruction in a single operation. 70 OCTOBER 2016 // dentaltown.com
 BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
BUILDING A MANDI Achieving total reconstruction in a single operation by Dr. Fayette C. Williams Fayette C. Williams, DDS, MD, FACS, is clinical faculty at John Peter Smith Hospital in Fort Worth, Texas,
Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases
 J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
J Oral Maxillofac Surg 58:1104-1108, 2000 Nasolabial Flap Reconstruction of Oral Cavity Defects: A Report of 18 Cases Yadranko Ducic, MD, FRCS (C),* and Mark Burye, DDS Purpose: This article describes
Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis CASE REPORT
 Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis Peter J. Taub, MD* James P. Bradley, MD* Henry K. Kawamoto, MD, DDS* Los Angeles, California Pittsburgh,
Closure of an Oronasal Fistula in an Irradiated Palate by Tissue and Bone Distraction Osteogenesis Peter J. Taub, MD* James P. Bradley, MD* Henry K. Kawamoto, MD, DDS* Los Angeles, California Pittsburgh,
Young-Hoon Joo, MD; Kwang-Jae Cho, MD; Jun-Ook Park, MD; Min-Sik Kim, MD
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Usefulness of the Anterolateral Thigh Flap With Vascularized Fascia Lata for Reconstruction of Orbital Floor
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Usefulness of the Anterolateral Thigh Flap With Vascularized Fascia Lata for Reconstruction of Orbital Floor
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
Screw hole-positioning guide and plate-positioning guide: A novel method to assist mandibular reconstruction
 Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Journal of Dental Sciences (2012) 7, 301e305 Available online at www.sciencedirect.com journal homepage: www.e-jds.com CASE REPORT Screw hole-positioning guide and plate-positioning guide: A novel method
Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System.
 Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Case Report Reconstruction of a Maxillary Oncologic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF and the MatrixMIDFACE Plating System. Reconstruction of a Maxillary Oncologic Defect
Maxillary reconstruction using the scapular tip free flap: A radiologic comparison of 3D morphology
 ORIGINAL ARTICLE Maxillary reconstruction using the scapular tip free flap: A radiologic comparison of 3D morphology Nitin A. Pagedar, MD, 1 Ralph W. Gilbert, MD, 2 * Harley Chan, PhD, 3 Michael J. Daly,
ORIGINAL ARTICLE Maxillary reconstruction using the scapular tip free flap: A radiologic comparison of 3D morphology Nitin A. Pagedar, MD, 1 Ralph W. Gilbert, MD, 2 * Harley Chan, PhD, 3 Michael J. Daly,
JPRAS Open 6 (2015) 5e10. Contents lists available at ScienceDirect. JPRAS Open. journal homepage:
 JPRAS Open 6 (2015) 5e10 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report Intraosseous hemangioma of the zygomatic bone Junji
JPRAS Open 6 (2015) 5e10 Contents lists available at ScienceDirect JPRAS Open journal homepage: http://www.journals.elsevier.com/ jpras-open Case report Intraosseous hemangioma of the zygomatic bone Junji
 www.oralradiologists.com CONE BEAM CT REPORT CASE XXXX Patient information Patient Name: - Referring Doctor: - Patient DOB: - Scan Date: [Start date] Reason for Exam: Maxillary facial pain Doctor Notes:
www.oralradiologists.com CONE BEAM CT REPORT CASE XXXX Patient information Patient Name: - Referring Doctor: - Patient DOB: - Scan Date: [Start date] Reason for Exam: Maxillary facial pain Doctor Notes:
Review Article Microsurgical Reconstruction of Large, Locally Advanced Cutaneous Malignancy of the Head and Neck
 Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID 415219, 5 pages doi:10.1155/2011/415219 Review Article Microsurgical Reconstruction of Large, Locally Advanced
Hindawi Publishing Corporation International Journal of Surgical Oncology Volume 2011, Article ID 415219, 5 pages doi:10.1155/2011/415219 Review Article Microsurgical Reconstruction of Large, Locally Advanced
The maxilla is the pivotal structure of the midface,
 ORIGINAL ARTICLE MICROVASCULAR FREE FLAP RECONSTRUCTION VERSUS PALATAL OBTURATION FOR MAXILLECTOMY DEFECTS Mauricio A. Moreno, MD, 1,2 Roman J. Skoracki, MD, 1 Ehab Y. Hanna, MD, 2 Matthew M. Hanasono,
ORIGINAL ARTICLE MICROVASCULAR FREE FLAP RECONSTRUCTION VERSUS PALATAL OBTURATION FOR MAXILLECTOMY DEFECTS Mauricio A. Moreno, MD, 1,2 Roman J. Skoracki, MD, 1 Ehab Y. Hanna, MD, 2 Matthew M. Hanasono,
Temporalis Muscle Flap In Midfacial Region Defects
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 7 Number 1 S Yadav, V Dhupar, A Dhupar, F Akkara Citation S Yadav, V Dhupar, A Dhupar, F Akkara.. The Internet Journal of Plastic Surgery. 2009
ISPUB.COM The Internet Journal of Plastic Surgery Volume 7 Number 1 S Yadav, V Dhupar, A Dhupar, F Akkara Citation S Yadav, V Dhupar, A Dhupar, F Akkara.. The Internet Journal of Plastic Surgery. 2009
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI
 Anatomy of the Maxillary Sinus Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor & Consultant Oral&Maxillofacial Surgeon Anatomy of the Maxillary Sinus Diseases of Sinuses 1) Inflammatory:
Anatomy of the Maxillary Sinus Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor & Consultant Oral&Maxillofacial Surgeon Anatomy of the Maxillary Sinus Diseases of Sinuses 1) Inflammatory:
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects
 Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
Open Access Original Article DOI: 10.7759/cureus.2356 Fascia Lata Free Flap Reconstruction of Limited Hard Palate Defects Rhorie P. Kerr 1, Andrea Hanick 1, Michael A. Fritz 1 1. Head and Neck Institute,
The majority of high-energy maxillary defects CRANIOFACIAL
 CRANIOFACIAL Microsurgical Reconstruction of Posttraumatic High-Energy Maxillary Defects: Establishing the Effectiveness of Early Reconstruction Eduardo D. Rodriguez, M.D., D.D.S. Mark Martin, M.D., D.M.D.
CRANIOFACIAL Microsurgical Reconstruction of Posttraumatic High-Energy Maxillary Defects: Establishing the Effectiveness of Early Reconstruction Eduardo D. Rodriguez, M.D., D.D.S. Mark Martin, M.D., D.M.D.
Prophylactic Midface Lift in Midfacial Trauma
 Rapid Communication 347 Ryan Brown, MD 1 Kirk Lozada, MD 2 Sameep Kadakia, MD 2 Eli Gordin, MD 3 Yadranko Ducic, MD 4 1 Department of Otolaryngology, Kaiser Permanente, Denver, Colorado 2 Department of
Rapid Communication 347 Ryan Brown, MD 1 Kirk Lozada, MD 2 Sameep Kadakia, MD 2 Eli Gordin, MD 3 Yadranko Ducic, MD 4 1 Department of Otolaryngology, Kaiser Permanente, Denver, Colorado 2 Department of
Titanium Mesh and Hydroxyapatite Cement Cranioplasty: A Report of 20 Cases
 J Oral Maxillofac Surg 60:272-276, 2002 Titanium Mesh and Hydroxyapatite Cement Cranioplasty: A Report of 20 Cases Yadranko Ducic, MD, FRCS(C)* Purpose: This article describes the use of titanium mesh
J Oral Maxillofac Surg 60:272-276, 2002 Titanium Mesh and Hydroxyapatite Cement Cranioplasty: A Report of 20 Cases Yadranko Ducic, MD, FRCS(C)* Purpose: This article describes the use of titanium mesh
Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap.
 Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Case Report Reconstruction of a Mandibular Osteoradionecrotic Defect with a Fibula Osteocutaneous Flap. Using Synthes ProPlan CMF, Patient Specific Plate Contouring (PSPC) and the MatrixMANDIBLE Plating
Aggressive maxillofacial disassembly in skull base surgery
 Otolaryngology Head and Neck Surgery (2006) 135, 303-311 ORIGINAL RESEARCH Aggressive maxillofacial disassembly in skull base surgery Vladimir Zuzukin, MD, and Yadranko Ducic, MD, FRCS(C), Fort Worth,
Otolaryngology Head and Neck Surgery (2006) 135, 303-311 ORIGINAL RESEARCH Aggressive maxillofacial disassembly in skull base surgery Vladimir Zuzukin, MD, and Yadranko Ducic, MD, FRCS(C), Fort Worth,
ORIGINAL ARTICLE. Reconstruction of the Frontal Sinus and Frontofacial Skeleton With Hydroxyapatite Cement
 ORIGINAL ARTICLE Reconstruction of the Frontal Sinus and Frontofacial Skeleton With Hydroxyapatite Cement Craig D. Friedman, MD; Peter D. Costantino, MD; C. H. Snyderman, MD; Lawrence C. Chow, PhD; Shozo
ORIGINAL ARTICLE Reconstruction of the Frontal Sinus and Frontofacial Skeleton With Hydroxyapatite Cement Craig D. Friedman, MD; Peter D. Costantino, MD; C. H. Snyderman, MD; Lawrence C. Chow, PhD; Shozo
MALIGNANT TUMOURS OF THE JAWS
 MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
MALIGNANT TUMOURS OF THE JAWS MALIGNANT TUMOURS OF THE JAWS Squamous cell carcinoma Osteogenic sarcoma Chondrosarcoma Fibrosarcoma Malignant lymphomas (incl. Burkitt s) Multiple myeloma Ameloblastoma Secondary
MEDPOR. Plastic surgery
 MEDPOR Plastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports in reconstructive,
MEDPOR Plastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports in reconstructive,
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps
 CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
CASE REPORT Reconstruction and Characterization of Composite Mandibular Defects Requiring Double Skin Paddle Fibular Free Flaps Austin M. Badeau, BA, a and Frederic W.-B. Deleyiannis, MD, MPhil, MPH b
Malignant tumours of the maxillary complex: an 18-year review
 British Journal of Plastic Surgery (1998), 51,584-588 9 1998 The British Association of Plastic Surgeons I BRITISH JOURNAL OF PLASTIC SURGERY Malignant tumours of the maxillary complex: an 18-year review
British Journal of Plastic Surgery (1998), 51,584-588 9 1998 The British Association of Plastic Surgeons I BRITISH JOURNAL OF PLASTIC SURGERY Malignant tumours of the maxillary complex: an 18-year review
Extended Bilaminar Forehead Flap With Cantilevered Bone Grafts for Reconstruction of Full-Thickness Nasal Defects
 J Oral Maxillofac Surg 63:566 570, 2005 Extended Bilaminar Forehead Flap With Cantilevered Bone Grafts for Reconstruction of Full-Thickness Nasal Defects Jason K. Potter, DDS, MD,* Yadranko Ducic, MD,
J Oral Maxillofac Surg 63:566 570, 2005 Extended Bilaminar Forehead Flap With Cantilevered Bone Grafts for Reconstruction of Full-Thickness Nasal Defects Jason K. Potter, DDS, MD,* Yadranko Ducic, MD,
OSTEOMYOCUTANEOUS PERONEAL ARTERY PERFORATOR FLAP FOR RECONSTRUCTION OF COMPOSITE MAXILLARY DEFECTS
 OSTEOMYOCUTANEOUS PERONEAL ARTERY PERFORATOR FLAP FOR RECONSTRUCTION OF COMPOSITE MAXILLARY DEFECTS Sukru Yazar, MD, 1 Ming-Huei Cheng, MD, 1 Fu-Chan Wei, MD, FACS, 1 Sheng-Po Hao, MD, FACS, 2 Kai-Ping
OSTEOMYOCUTANEOUS PERONEAL ARTERY PERFORATOR FLAP FOR RECONSTRUCTION OF COMPOSITE MAXILLARY DEFECTS Sukru Yazar, MD, 1 Ming-Huei Cheng, MD, 1 Fu-Chan Wei, MD, FACS, 1 Sheng-Po Hao, MD, FACS, 2 Kai-Ping
Scapular Flap for Maxillectomy Defect Reconstruction and Preliminary Results Using Three-Dimensional Modeling
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Scapular Flap for Maxillectomy Defect Reconstruction and Preliminary Results Using Three-Dimensional Modeling
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Scapular Flap for Maxillectomy Defect Reconstruction and Preliminary Results Using Three-Dimensional Modeling
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY INFERIOR MAXILLECTOMY Tumours of the hard palate and superior alveolus may be resected by inferior maxillectomy (Figure 1). A Le Fort
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
ISSN: Volume 4 Issue Faciomaxillary prosthesis in rehabilitation. After maxillectomy. A clinical study
 ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
ISSN: 2250-0359 Volume 4 Issue 4 2014 Faciomaxillary prosthesis in rehabilitation After maxillectomy A clinical study Prasad c Parimala V Vijjaykanth M Sivakumar P Department of Dental Surgery Govt. Stanley
Extending the traditional resection limits of squamous cell carcinoma of the anterior skull base
 Otolaryngology Head and Neck Surgery (2007) 137, 899-905 ORIGINAL RESEARCH SKULL BASE SURGERY Extending the traditional resection limits of squamous cell carcinoma of the anterior skull base Yadranko Ducic,
Otolaryngology Head and Neck Surgery (2007) 137, 899-905 ORIGINAL RESEARCH SKULL BASE SURGERY Extending the traditional resection limits of squamous cell carcinoma of the anterior skull base Yadranko Ducic,
Wei-Liang Chen, DDS, MD, MBA, Jian-Tao Ye, DDS, MD, Zhao-Hui Yang, DDS, MD, Zhi-Quan Huang, DDS, MD, Da-Ming Zhang, DDS, MS, Ke Wang, DDS, MS
 ORIGINAL ARTICLE REVERSE FACIAL ARTERY SUBMENTAL ARTERY MANDIBULAR OSTEOMUSCULAR FLAP FOR THE RECONSTRUCTION OF MAXILLARY DEFECTS FOLLOWING THE REMOVAL OF BENIGN TUMORS Wei-Liang Chen, DDS, MD, MBA, Jian-Tao
ORIGINAL ARTICLE REVERSE FACIAL ARTERY SUBMENTAL ARTERY MANDIBULAR OSTEOMUSCULAR FLAP FOR THE RECONSTRUCTION OF MAXILLARY DEFECTS FOLLOWING THE REMOVAL OF BENIGN TUMORS Wei-Liang Chen, DDS, MD, MBA, Jian-Tao
By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S.
 THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
A review of the advantages of the anterolateral thigh flap in head and neck reconstruction
 The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
The British Association of Plastic Surgeons (2004) 57, 603 609 A review of the advantages of the anterolateral thigh flap in head and neck reconstruction Jagdeep S. Chana, Fu-chan Wei* Department of Plastic
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty
 CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
CASE REPORT An Innovative Solution to Complex Inguinal Defect: Deepithelialized SIEA Flap With Mini Abdominoplasty Augustine Reid Wilson, MS, Justin Daggett, MD, Michael Harrington, MD, MPH, and Deniz
Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report
 220 Nasal septal reconstruction Case Report Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report Yakup Cil1* Diyarbakır Military Hospital, Department of Plastic Surgery 21000 Diyarbakır, Turkey
220 Nasal septal reconstruction Case Report Fibular Bone Graft for Nasal Septal Reconstruction: A Case Report Yakup Cil1* Diyarbakır Military Hospital, Department of Plastic Surgery 21000 Diyarbakır, Turkey
A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery
 ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
ONCOLOGY LETTERS 14: 7049-7054, 2017 A novel classification system for the evaluation and reconstruction of oral defects following oncological surgery WEI WEI LIU, CHU YI ZHANG, JIAN YIN LI, MING FANG
T. Rapis, S.N. Zanakis, I.F. Letsa, A.P. Karamanos CLINICAL CASE. Summary. Introduction
 Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Journal of BUON 8: 397-401, 2003 2003 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Basal cell carcinoma of the posterior neck, reconstructed with lower trapezius island musculocutaneous
Learning Objectives. Head and Neck Cancer: Post-Treatment Changes. Neck Dissection Classification * Radical neck dissection. Radical Neck Dissection
 Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
Head and Neck Cancer: Post-Treatment Changes Daniel W. Williams III, MD Learning Objectives In patients treated for H/N Cancer: Describe the various types of neck dissections Explain reconstruction techniques
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Case Report Mid Facial Degloving Procedure: Managing A Case of Multiple Mid Face Fractures with Significant External Deformity
 55 Bangladesh J Otorhinolaryngol 2015; 21(1): 51-56 Case Report Mid Facial Degloving Procedure: Managing A Case of Multiple Mid Face Fractures with Significant External Deformity Akhil Chndra Biswas 1,
55 Bangladesh J Otorhinolaryngol 2015; 21(1): 51-56 Case Report Mid Facial Degloving Procedure: Managing A Case of Multiple Mid Face Fractures with Significant External Deformity Akhil Chndra Biswas 1,
ORIGINAL ARTICLE. The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited. decades, the range of reconstructive
 ORIGINAL ARTICLE The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited Eric M. Genden, MD; Bryant B. Lee, MD; Mark L. Urken, MD Background: Although a host of local
ORIGINAL ARTICLE The Palatal Island Flap for Reconstruction of Palatal and Retromolar Trigone Defects Revisited Eric M. Genden, MD; Bryant B. Lee, MD; Mark L. Urken, MD Background: Although a host of local
Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC
 Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Downloaded from Reconstruction of the Breast after Cancer An Overview of Procedures and Options by Karen M. Horton, MD, MSc, FRCSC What is Breast Reconstruction? Reconstruction of the breast involves recreating
Free-Flap Reconstruction of Skull Base and Orbital Defects
 72 Free-Flap Reconstruction of Skull Base and Orbital Defects Weitao Wang, MD 1 Aurora Vincent, MD 2 Mofiyinfolu Sokoya, MD 3 Scott Kohlert, MD 3 Sameep Kadakia, MD 4 Yadranko Ducic, MD, FRCS(C), FACS
72 Free-Flap Reconstruction of Skull Base and Orbital Defects Weitao Wang, MD 1 Aurora Vincent, MD 2 Mofiyinfolu Sokoya, MD 3 Scott Kohlert, MD 3 Sameep Kadakia, MD 4 Yadranko Ducic, MD, FRCS(C), FACS
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Subciliary versus Subtarsal Approaches to Orbitozygomatic Fractures
 CME Subciliary versus Subtarsal Approaches to Orbitozygomatic Fractures Rod J. Rohrich, M.D., Jeffrey E. Janis, M.D., and William P. Adams, Jr., M.D. Dallas, Texas Learning Objectives: After studying this
CME Subciliary versus Subtarsal Approaches to Orbitozygomatic Fractures Rod J. Rohrich, M.D., Jeffrey E. Janis, M.D., and William P. Adams, Jr., M.D. Dallas, Texas Learning Objectives: After studying this
Primary closure of the deltopectoral flap-donor site without skin grafting
 Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Primary closure of the deltopectoral flap-donor site without skin grafting Received: 4/3/2013 Accepted: 14/5/2013 Introduction Reliable and simultaneous reconstruction of head-and-neck defects has been
Clinical Study Use of the Anterolateral Thigh in Cranio-Orbitofacial Reconstruction
 Hindawi Publishing Corporation Plastic Surgery International Volume 2011, Article ID 941742, 6 pages doi:10.1155/2011/941742 Clinical Study Use of the Anterolateral Thigh in Cranio-Orbitofacial Reconstruction
Hindawi Publishing Corporation Plastic Surgery International Volume 2011, Article ID 941742, 6 pages doi:10.1155/2011/941742 Clinical Study Use of the Anterolateral Thigh in Cranio-Orbitofacial Reconstruction
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Chapter 7: Skeletal System: Gross Anatomy
 Chapter 7: Skeletal System: Gross Anatomy I. General Considerations A. How many bones in an average adult skeleton? B. Anatomic features of bones are based on II. Axial Skeleton A. Skull 1. Functionally
Chapter 7: Skeletal System: Gross Anatomy I. General Considerations A. How many bones in an average adult skeleton? B. Anatomic features of bones are based on II. Axial Skeleton A. Skull 1. Functionally
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL
 What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
What is Hemifacial Microsomia? By Pravin K. Patel, MD and Bruce S. Bauer, MD Children s Memorial Hospital, Chicago, IL 773-880-4094 Early in the child s embryonic development the structures destined to
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Reconstruction of large mandibular defects
 Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Immediate Reconstruction of a Large Mandibular Defect of Locally Invasive Benign Lesions (A New Method) Gholamreza Shirani, OMFS, DDS, MS,* Mahnaz Arshad, DDS, 1 Farnoush Mohammadi, OMFS, DDS, MS* Tehran,
Jaw resection JAMES S BROWN. Contents. Resection of the mandible and maxilla. General principles. Applied anatomy
 39 Jaw resection JAMES S BROWN Contents Resection of the mandible and maxilla 391 General principles 391 Applied anatomy 391 Mandible 391 Maxilla 392 Mandibular resection for oral squamous cell carcinoma
39 Jaw resection JAMES S BROWN Contents Resection of the mandible and maxilla 391 General principles 391 Applied anatomy 391 Mandible 391 Maxilla 392 Mandibular resection for oral squamous cell carcinoma
Technique Guide. Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones.
 Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Technique Guide Midface Distractor System. For the temporary stabilization and gradual lengthening of the cranial or midfacial bones. Table of Contents Introduction Midface Distractor System 2 Indications
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
MEDPOR. Oculoplastic surgery
 MEDPOR Oculoplastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
MEDPOR Oculoplastic surgery MEDPOR biomaterial MEDPOR has been a trusted name in the industry since 1985, with hundreds of thousands of procedures performed, and hundreds of published clinical reports
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section. REVIEW SHEET Exercise 10 Axial Skeleton
 ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
ORIGINAL ARTICLE. A Novel Technique for Malar Eminence Evaluation Using 3-Dimensional Computed Tomography
 ORIGINAL ARTICLE A Novel Technique for Malar Eminence Evaluation Using 3-Dimensional Computed Tomography Sami P. Moubayed, MD; Frederick Duong, MD; Christian Ahmarani, MD, FRCSC; Akram Rahal, MD, FRCSC
ORIGINAL ARTICLE A Novel Technique for Malar Eminence Evaluation Using 3-Dimensional Computed Tomography Sami P. Moubayed, MD; Frederick Duong, MD; Christian Ahmarani, MD, FRCSC; Akram Rahal, MD, FRCSC
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY BUCCINATOR MYOMUCOSAL FLAP The Buccinator Myomucosal Flap is an axial flap, based on the facial and/or buccal arteries. It is a flexible
ALTHOUGH FIRST described
 The Cervicodeltopectoral Flap for Single-Stage Resurfacing of Anterolateral Defects of the Face and Neck Yadranko Ducic, MD, FRCSC; Jesse E. Smith, MD SURGICAL TECHNIQUE Objective: To evaluate prospectively
The Cervicodeltopectoral Flap for Single-Stage Resurfacing of Anterolateral Defects of the Face and Neck Yadranko Ducic, MD, FRCSC; Jesse E. Smith, MD SURGICAL TECHNIQUE Objective: To evaluate prospectively
ORIGINAL ARTICLE. some of the most difficult challenges in
 Temporoparietal Fascial Flap in Orbital Reconstruction Amy Lai, MD; Mack L. Cheney, MD ORIGINAL ARTICLE Objective: To evaluate the success of the temporoparietal fascial flap (TPFF) in the primary or secondary
Temporoparietal Fascial Flap in Orbital Reconstruction Amy Lai, MD; Mack L. Cheney, MD ORIGINAL ARTICLE Objective: To evaluate the success of the temporoparietal fascial flap (TPFF) in the primary or secondary
Endoscopic assisted harvest of the pedicled pectoralis major muscle flap
 British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
British Journal of Plastic Surgery (2005) 58, 170 174 Endoscopic assisted harvest of the pedicled pectoralis major muscle flap Arif Turkmen*, A. Graeme B. Perks Plastic Surgery Department, Nottingham City
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Disclosures. The Expanding Role of Microvascular Reconstruction. Overview. Things they are a Changing. Surgical Advisory Board, Genentech Corp
 Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Disclosures Surgical Advisory Board, Genentech Corp The Expanding Role of Microvascular Reconstruction P. Daniel Knott, MD FACS Associate Professor Director, Facial Plastic and Reconstructive Surgery UCSF
Maxillary and Periorbital Fractures January 2004
 TITLE: Maxillary and Periorbital Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 7, 2004 RESIDENT PHYSICIAN: Gordon Shields, MD FACULTY ADVISOR: Francis B. Quinn,
TITLE: Maxillary and Periorbital Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 7, 2004 RESIDENT PHYSICIAN: Gordon Shields, MD FACULTY ADVISOR: Francis B. Quinn,
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY
 Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Nagoya J. Med. Sci. 56. 69-79,1993 THREE-DIMENSIONAL COMPUTED TOMOGRAPIDC ANALYSIS FOR PLACEMENT OF MAXILLOFACIAL IMPLANTS AFTER MAXILLECTOMY MINORU VEDA, YOSHIHIRO SAWAKI, and TOSHIO KANEDA Department
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2
 RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY
 MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
MEDICAL UNIVERSITY OF VARNA FACULTY OF DENTAL MEDICINE DEPARTMENT OF ORAL AND MAXILLOFACIAL SURGERY AND SID SYLLABUS OF ORAL AND MAXILLOFACIAL SURGERY (State examination) ACADEMIC YEAR 2015 2016 1. Asepsis
Technique Guide. SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction.
 Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Maxillofacial Injuries Practical Tips
 Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Cranium Facial bones. Sternum Rib
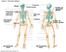 Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Nasolabial flap reconstruction in oral cancer
 Singh et al. World Journal of Surgical Oncology 2012, 10:227 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Nasolabial flap reconstruction in oral cancer Seema Singh, Rajesh Kumar Singh and Manoj
Singh et al. World Journal of Surgical Oncology 2012, 10:227 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Nasolabial flap reconstruction in oral cancer Seema Singh, Rajesh Kumar Singh and Manoj
Implant Preparation. Page 1
 Why SU-POR? SU-POR Surgical Implants are manufactured from a linear high-density polyethylene. SU-POR Surgical Implants allow for tissue ingrowth because of the interconnecting open pore structure. The
Why SU-POR? SU-POR Surgical Implants are manufactured from a linear high-density polyethylene. SU-POR Surgical Implants allow for tissue ingrowth because of the interconnecting open pore structure. The
A longitudinal study of angular artery island flap, used for reconstruction of facial defects
 A longitudinal study of angular artery island flap, used for reconstruction of facial defects KEYWORDS: mid and upper facial defect, angular artery island flap, ipsilateral or contralateral, local flap,
A longitudinal study of angular artery island flap, used for reconstruction of facial defects KEYWORDS: mid and upper facial defect, angular artery island flap, ipsilateral or contralateral, local flap,
ORIGINAL ARTICLE. Le Fort I Osteotomy and Skull Base Tumors. Tyler M. Lewark, MD; Gregory C. Allen, MD; Khalid Chowdhury, MD, FRCSC; Kenny H.
 Le Fort I Osteotomy and Skull Base Tumors A Pediatric Experience ORIGINAL ARTICLE Tyler M. Lewark, MD; Gregory C. Allen, MD; Khalid Chowdhury, MD, FRCSC; Kenny H. Chan, MD Background: The Le Fort I maxillary
Le Fort I Osteotomy and Skull Base Tumors A Pediatric Experience ORIGINAL ARTICLE Tyler M. Lewark, MD; Gregory C. Allen, MD; Khalid Chowdhury, MD, FRCSC; Kenny H. Chan, MD Background: The Le Fort I maxillary
Despite the apparent recent evolution and modification
 Extended orbitozygomatic approach to the skull base to improve access to the cavernous sinus and optic chiasm ALLISON TERESA PONTIUS, MD, and YADRANKO DUCIC, MD, FRCS(C), FACS, Dallas and Fort Worth, Texas
Extended orbitozygomatic approach to the skull base to improve access to the cavernous sinus and optic chiasm ALLISON TERESA PONTIUS, MD, and YADRANKO DUCIC, MD, FRCS(C), FACS, Dallas and Fort Worth, Texas
Skeletal system. Prof. Abdulameer Al-Nuaimi. E. mail:
 Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PARAMEDIAN FOREHEAD FLAP NASAL RECONSTRUCTION SURGICAL TECHNIQUE Brian Cervenka, Travis Tollefson, Patrik Pipkorn The paramedian forehead
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PARAMEDIAN FOREHEAD FLAP NASAL RECONSTRUCTION SURGICAL TECHNIQUE Brian Cervenka, Travis Tollefson, Patrik Pipkorn The paramedian forehead
Hydroxyapatite Cement to Repair Skull Base Defects: Radiologic Appearance
 Hydroxyapatite Cement to Repair Skull Base Defects: Radiologic Appearance Jane L. Weissman, Carl H. Snyderman, and Barry E. Hirsch PURPOSE: To describe the radiologic appearance of hydroxyapatite cement
Hydroxyapatite Cement to Repair Skull Base Defects: Radiologic Appearance Jane L. Weissman, Carl H. Snyderman, and Barry E. Hirsch PURPOSE: To describe the radiologic appearance of hydroxyapatite cement
