Downloaded by Guangxi University for Nationalities from online.liebertpub.com at 02/20/18. For personal use only. ABSTRACT
|
|
|
- Pearl Marylou Bond
- 6 years ago
- Views:
Transcription
1 TISSUE ENGINEERING Volume 6, Number 4, 2000 Mary Ann Liebert, Inc. Promoted Bone Healing at a Rabbit Skull Gap Between Autologous Bone Fragment and the Surrounding Intact Bone with Biodegradable Microspheres Containing Transforming Growth Factor-b 1 LIU HONG, M.D., 1 YASUHIKO TABATA, Ph.D., 2 SUSUMU MIYAMOTO, M.D., D.Med.Sci., 1 KEISUKE YAMADA, M.D., D.Med.Sci., 1 IKUO AOYAMA, M.S., 1 MAKOTO TAMURA, Ph.D., 3 NOBUO HASHIMOTO, M.D., D.Med.Sci., 1 and YOSHITO IKADA, Ph.D., D.Med.Sci. 2 ABSTRACT This study is a trial to promote repairing of the rabbit skull bone gap between an autologous bone flap and the intact bone with biodegradable gelatin microspheres containing transforming growth factor-b 1 (TGF-b 1). A 10-mm diameter bone defect was prepared in rabbit skulls by drilling out a bone flap of 6 mm in diameter. After a surrounding gap defect of 2 mm was created and treated with 0.5 m g of free TGF-b 1 and gelatin microspheres containing 0.5 m g of free TGF-b1, the circular autologous bone flap was placed in the center. Significant bone healing at the gap defect was observed 3 weeks after implantation of the TGF-b 1-containing gelatin microspheres. The bone mineral density (BMD) was significantly higher than that of other experimental groups. On the contrary, when applied with free TGF-b 1, a fibrous tissue initially infiltrated into the gap defect, resulting in impairing bone healing. The tissue response was similar to that at the defect implanted with empty gelatin microspheres and TGF-b 1-free phosphate-buffered saline solution alone. There was more space in the gap-filling bone in the 16-week view than the 3-week view. It is possible that this was an intermediate step along the way toward normal healing and formation of cancellous bone. We conclude that gelatin microspheres containing TGF-b 1 show promise as an agent to promote bone regeneration of subcritical size defects between surgically positioned autologous bone flaps and surrounding host bone. INTRODUCTION SEVERAL W ORKERS have suggested that the craniofacial skeleton has poor self-regenerative powers beyond the early growing period. This becomes a clinical issue in cases of large defects caused by trauma or tumor resection. 1 Currently, autologous bone grafts have been clinically employed to reconstruct craniofacial 1 Department of Neurosurgery, Medical School, and 2 Institute for Frontier Medical Sciences, Kyoto University, Kyoto, Japan. 3 Kaken Pharmaceutica l Co. Ltd., Kyoto, Japan. 331
2 HONG ET AL. bone defects because of their higher osteoconductive ability and fewer side effects than currently available alloplastic materials. 2 However, the number of autograft sites and the amount of graftable bone found there is limited. It has been demonstrated that fibrous healing doses occur in craniofacial bones if the gap between bone ends exceeds several millimeters, especially if the bone is thin or if soft tissue is interposed. If a material with the ability of enhancing bone formation is obtained, it will achieve bone healing between the bone autografts or the autograft and the surrounding intact bone. As a trial to promote the bone healing, it will be efficient to use osteogenetic growth factors at the bone gap. It is well recognized that there are one or more signaling molecules like growth factors and cytokines that can induce or accelerate bone healing through the desired stages, from woven unorganized through compact lamellar bone. 3 However, it will be impossible to control the timing, concentration, and interaction of the growth factors artificially. Transforming growth factor-b 1 (TGF-b 1) is a multifunctional regulator possessing widespread effects on cellular proliferation, angiogenesis, migration, and immune response. It has been demonstrated that it can cause proliferation of osteoblasts and preosteoblastic cells and exerts an effect on fracture healing and bone regeneration. 4,5 However, the local application of the free TGF-b 1 solution showed the less osteogenic effect in vivo. A promising delivery system is necessary to promote its osteogenetic ability by providing sufficient quantities over the desired time period. We have developed a biodegradable hydrogel system prepared through chemical crosslinking of acidic gelatin with glutaraldehyde and succeeded in releasing biologically active TGF-b 1 based on hydrogel degradation. 6,7 This gelatin hydrogel effectively promoted TGFb 1-induced bone regeneration at a rabbit skull defect at an effective TGF-b 1 dose, in marked contrast to TGF-b 1 in solution. A long-term evaluation study revealed that the regenerated bone had the tissue structure similar to the compact bone that surrounds the diploic space periostally and endostially. 8 In the present study, we prepared microsphere gelatin hydrogel for application to a 2-mm bone defect, and investigated bone formation at the gap defect after application of TGF-b 1 containing gelatin microspheres. Materials MATERIALS AND METHODS Gelatin with an isoelectric point (IEP) of 5.0, prepared through alkaline processing of bovine bone, was kindly supplied from Nitta Gelatin Co. (Osaka, Japan). It is named acidic gelatin on the basis of its low isoelectric point. Human recombinant TGF-b 1 with an IEP of 9.5 was purchased from Sigma Chemical Co., MI. Other chemicals were obtained from Wako Pure Chemical Industries, Ltd. (Osaka, Japan) and used without further purification. Preparation of gelatin microspheres containing TGF-b 1 Gelatin microspheres were prepared through chemical crosslinking of gelatin aqueous solution in an emulsion state, as described previously. 9 Briefly, 10 ml of the mixed gelatin (10 wt%) and glutaradehyde ( wt %) aqueous solution was stirred (420 rpm) (Heidon 600G, Sinto Scientific Co. Tokyo, Japan) in 375 ml of olive oil at 40 C for 10 min to obtain a water-in-oil emulsion. The emulsion temperature was decreased to below 20 C and stirring was continued for 24 h to allow chemical crosslinking of gelatin to proceed. After acetone addition, the crosslinked microspheres were collected by centrifugation (4 C, 3,000 rpm, 5 min) and washed five times by acetone. The washed microspheres were placed in 100 ml of 100 mm glycine aqueous solution containing 0.1 wt% Tween 80, followed by agitating at 37 C for 1 hr to block the residual aldehyde groups of unreacted glutaraldehyde. Then, the resulting microspheres were washed three times with double-distill ed water by centrifugation, freeze-dried, and sterilized with ethylene oxide gas. When calculated from the microsphere volume before and after swelling in 0.05 M phosphate-buffered saline solution (PBS, ph 7.4) for 24 h at 37 C, the water content of microspheres used here was 95 wt%, being the volum e ratio of water in the microspheres to the wet microspheres. At least 100 microspheres were viewed with a light microscope to calculate their volum e. The average diameter or wet microspheres was 100 m m. Next, 8 mg of gelatin microspheres was applied for each skull gap defect, this is the largest amount of 332
3 PROMOTED BONE HEALING BY TGF-b 1-MICROSPHERES this material that can fit in the defect. TGF-b 1 was impregnated into gelatin microspheres by dropping 12.5 m g/ml of TGF-b 1 solution in PBS (40 m L) onto 8 mg of freeze-dried gelatin microspheres, and the mixture was left at 4 C for 12 h to allow the solution to absorb into the microspheres. TGF-b 1-free empty microspheres were prepared similarly, except that PBS was added. The PBS solution with or without TGFb 1 was completely absorbed into these microspheres because it was less than the amount required for equilibration of the internal versus external microsphere environments. Animal experiments Fifty Japanese white rabbits weighing from 2.0 to 2.5 kg were anesthetized by intravenous administration of sodium pentobarbita l. In addition, lidocaine solution containing 1 wt% epinephrine was injected subcutaneously at the rabbit head for local anesthesia. The 4-cm-long scalp skin cut was prepared at midline head of rabbit. Then the pericranium was cut along the sagittal suture and retracted to expose the bilateral parietal bone of rabbit. Two bone defects of 10 mm in diameter were prepared per rabbit skull, one on each side of the sagittal suture symmetrically by taking out a skull bone flap of 6 mm in diameter with a microdrill. All the procedures were performed with the aid of an operating microscope so as not to injure the underlying dura mater. After the autologous bone flap obtained was placed at the center of skull defect, the 2-mm-width gap defect between the bone flap and the surrounding skull bone was filled with gelatin microspheres containing TGF-b 1 (Fig. 1). There were four kinds of agents applied: group A, gelatin microsphere containing TGF-b 1; group B, PBS solution with TGF-b 1; group C, gelatin microsphere containing without TGF-b 1; and group D, PBS solution without TGF-b 1. The type of agent was randomly selected from either the right or left bone defect of different rabbits. Following implantation, the pericranium and scalp were carefully sutured with 4-0 nylon suture. The rabbits were sacrificed by intravenous administration of an overdose of sodium pentobarbital 3, 6, 9, 12, and 16 weeks after implantation (n 5 10). Five defects were obtained for each group at each time point. The skull bone specimen containing two defects was taken out from each rabbit and fixed in 10 wt% neutralized aqueous solution of formaldehyde for bone assessments. FIG. 1. A photograph of rabbit skull defects (10 mm in diameter) applied with combination of an autologous bone flap (6 mm in diameter) and PBS (right) or gelatin microspheres containing 0.5 m g of TGF-b 1 (left). The bone flap was placed in the center of the skull defect and the 2 mm gap between the bone flap and the surrounding skull bone was implanted with PBS and the gelatin microspheres. 333
4 HONG ET AL. Assessment of bone formation of gap defects Bone formation at the skull gap defect between the bone flap and the surrounding skull bone was assessed first on the basis of plain film X-ray to evaluate qualitatively mineral deposition at the gap defect. The plain film X-ray radiograph of each bone specimen was taken at 46 kv and 2 ma for 15 s. Then, bone mineral density (BMD) at every gap defect was quantitated by dual energy X-ray absorptom etry (DEXA) (model DCS 600, Aloka Co., Tokyo, Japan). The BMD value for each gap defect was obtained by average of BMD values measured at eight sites evenly selected from the gap defect around the bone flap. The region of interest in the absorptometry measurement was adjusted at mm 2. Following the BMD measurement, the skull bone specimens were demineralized in 10 wt% ethylenediamine tetraacetic acid aqueous solution, embedded in paraffin, and cut into 2-m m-thick sections at the center of the skull defect or the nearest site possible. The sections were stained with tartrate-resistant acid phosphatase and eosin to highlight osteoclasts, histologically viewing throughout the trabecular bone newly formed at the gap defect. From the 2-mm-width area located at the gap defect on histological sections, the perimeter length of total trabecular bone surface, the bone surface where active osteoblasts characterized by basophilic cuboided cytoplasm located were recruited (active formation surface), and the bone surface where osteoclasts characterized by red staining irregular multinucleated cell located were recruited (active resorption surface) was measured by use of an image analyzer with a light microscope. The measurement FIG. 2. Soft X-ray photographs of rabbit skull defects 3 weeks after application with an autologous bone flap combined with PBS (A), TGF-b 1-free gelatin microspheres (B), 0.5 m g of free TGF-b 1 (C), and gelatin microspheres containing 0.5 m g of TGF-b 1 (D). Bar 5 1 mm. 334
5 PROMOTED BONE HEALING BY TGF-b 1-MICROSPHERES was performed by a researcher blinded to the individual experiment groups. The fractional active formation surface (FrAFS) and fractional active resorption surface (FrARS) were defined as the perimeter percentage of the active formation surface and the active resorption surface to the total bone surface, respectively. The value of FrAFS and FrARS for each specimen was averaged by two gap defects at one skull defect. Statistical analysis Each defect was considered independent. All the data were statistically analyzed by Scheffe s F test for multiple comparison and statistical significance was accepted at p, Experimental results were expressed as the mean 6 the standard deviation (SD) about the mean. RESULTS Bone formation at the skull gap defect by gelatin microspheres containing TGF-b 1 Figures 2 and 3 show plain film X-ray photographs of skull defects 3 and 16 weeks after implantation with TGF-b 1-containing gelatin microspheres or other agents. The gap defect became radiopaque 3 weeks FIG. 3. Soft X-ray photographs of rabbit skull defects 16 weeks after application with an autologous bone flap combined with PBS (A), TGF-b 1-free gelatin microspheres (B), 0.5 m g of free TGF-b 1 (C), and gelatin microspheres containing 0.5 m g of TGF-b 1 (D). Bar 5 1 mm. 335
6 HONG ET AL. after implantation with the TGF-b 1-containing gelatin microspheres (Fig. 2D). Little gap defect radio-opacity was found in the specimens receiving 0.5 m g of free TGF-b 1. This radiographic appearance was similar to that of gap defect treated with TGF-b 1-free gelatin microspheres and PBS (Fig. 2). The free TGFb 1-induced radio-opaque area tended to increase 16 weeks after implantation, although a radiolucent line remained around the bone flap. The similar time change was observed for defects after application with groups C and D. For the gelatin microspheres containing TGF-b 1, the gap defect remained radio-opaque at 16-week after implantation (Fig. 3). Figure 4 shows the time profile of BMD values at the gap defect of rabbit skulls after application of various agents. The BMD value of gap defects after application with group A was significantly higher than that of other agents 3 weeks after implantation, and reached a maximum level at 6 weeks after implantation, followed by the subsequent gradual decrease. There was little change in the BMD value at the gap defect after application with free TGF-b 1 over the time range studied, which was similar to the time profile of BMD value for empty microspheres and PBS. No significant difference of BMD values at gap 16 weeks after application with all agents. Histological evaluation of bone formation at the gap defect enhanced by gelatin microspheres containing TGF-b 1 Figures 5 and 6 show the histological sections of gap defects 3 and 16 weeks after application of various agents. Significantly, bone formation occurred at the gap defect 3 weeks after receiving the TGF-b 1- containing gelatin microsphere implantation, and the bone flap was connected to the surrounding skull bone. Bone formation enhanced by free TGF-b 1 at the gap defect was hardly noticeable and instead a fibrous tissue was observed at the defect, which was histologically similar to that occurring in groups C and D (Fig. 5). Gelatin microspheres were completely degraded and did not remain at the gap defect 3 weeks after implantation, irrespective of the TGF-b 1 incorporation. The bone tissue regenerated by TGF-b 1-containing gelatin microspheres 16 weeks after implantation turned loose compared with bone tissues 3 weeks after implantation (Fig. 6D). The amount of bone formed 16 weeks after application with groups B, C, FIG. 4. The time course of BMD values at the gap defect of rabbits between the bone flap and the surrounding skull bone after treatment with gelatin microspheres containing 0.5 m g of TGF-b 1 and other agents. (p ) p, 0.05 against the BMD value of defects applied with PBS. ( ) p, 0.05 against the BMD value of defects applied with TGF-b 1-free gelatin microspheres. ( ) p, 0.05 against the BMD value of defects applied with free TGF-b
7 PROMOTED BONE HEALING BY TGF-b 1-MICROSPHERES and D seemed to increase when compared with that 3 weeks after treatment. However, the thickness of the newly formed bone seems thinner than that formed after application with group A, and, the newly formed bone was located near to dura mater. Fibrous tissues were still observed to interpose at the gap defect (Fig. 6A C). Figure 7 shows the time profile of FrAFS and FrARS values for bone newly formed at the gap defect after application with various agents. For all experimental agents, the FrAFS and FrARS values of bone regenerated initially increased to attain a maximum level and thereafter decreased to a similar level. However, the implantation period to attain the maximum levels was shortened by application with the Group A reagent. After an implantation period of 12 weeks, both the FrAFS and FrARS levels became similar, irrespective of the agent of experimental groups. There was no significant difference in the BMD value and the bone area for each experimental group during the whole observation period. DISCUSSION It has been reported that several growth factors such as bone morphogenetic protein, basic fibroblast growth factor, and TGF-b 1 possessed osteogenetic ability, and they were applied to skull defect models to accelerate the bone regeneration TGF-b 1 exists mainly in bone and has been demonstrated to possess an effect on the proliferation of preosteoblastic and osteoblastic cells, including human osteoblasts. A single therapeutic dose of TGF-b 1 also has been shown to promote bone formation at a critical-sized defect. 18,19 We have demonstrated that TGF-b 1 was ionically complexed with acidic gelatin and, as a result, was released in vivo from the gelatin hydrogel during hydrogel biodegradation. In our previous study, application of TGF-b 1 could effectively recruit osteoblasts at defect margin adjacent to dipole and dura mater. FIG. 5. Histological sections of the gap defect of rabbits between the bone flap and the surrounding skull bone 3 weeks after application with PBS (A), TGF-b 1-free gelatin microspheres (B), 0.5 m g of free TGF-b 1 (C), and gelatin microspheres containing 0.5 m g of TGF-b 1 (D). Arrows indicate the edge of gap defect. Bar 5 1 mm. BF, Bone flap; C, connective tissue; DM, dura mater; NB, new bone; HB, host bone. (TRAP and eosin staining; original magnification 3 40.) 337
8 HONG ET AL. FIG. 6. Histological sections of the gap defect of rabbits between the bone flap and the surrounding skull bone 16 weeks after application with PBS (A). TGF-b 1-free gelatin microspheres (B), 0.5 m g of free TGF-b 1 (C), and gelatin microspheres containing 0.5 m g of TGF-b 1 (D). Arrows indicate the edge of gap defect. Bar 5 1 mm. BF, Bone flap; C, connective tissue; DM, dura mater; NB, new bone; HB, host bone. (TRAP and eosin staining; original magnification 3 40.) An application of more than 0.1 m g of TGF-b 1-containing gelatin hydrogels with a suitable biodegradability in a disc type could significantly induce bone formation at a rabbit skull defect in 6 mm diameter 6 weeks after implantation. 8 It appeared that the controlled release of TGF-b 1 not only enhanced osteoblast recruitment into the bone defect but also prolonged osteoblasts in the active state. The present study clearly demonstrated that the TGF-b 1 incorporated in gelatin microspheres could significantly promote bone healing at the skull bone gap between the autograft and the intact bone, which is similar to the result obtained by the TGF-b 1-incorporating gelatin hydrogel of disc type. It enabled bone to connect between the autologous bone flap and the surrounding skull bone within a short time period, whereas free TGF-b 1 was ineffective. This is likely explained in terms of controlled release of TGF-b 1 from gelatin microspheres. It is possible that the controlled release of TGF-b 1 localized at the skull defect enhances recruitment of active osteoblasts, thereby resulting in superior bone formation. Free TGF-b 1 may have been shown to reduce bone regeneration due to shunting of the TGF-b 1 solution out of the site and into the interstitial compartment at large, or to its being rapidly metabolized. The achievement of the balance of resorption and formation at newly formed bone by application of TGF-b 1-containing gelatin microspheres seemed no different with normal bone formation at the defect. It is likely that this microsphere system enables TGF-b 1 to be released over an extended time period at the defect site, resulting in promoting the bone healing at the gap defect between the bone flap and host bone. The self-regenerated bone was observed after 16 weeks, and the BMD values of the gap defect with PBS applied were comparable to those of TGF-b 1-containing gelatin microspheres. However, the thickness of the newly formed bone apparently was thinner than that promoted by TGF-b 1-containing microspheres. The new bone formed near to the dura mater is probably explained by the markedly high-affinity receptors for TGF-b 1 located in the dura mater. 20 It is well known that TGF-b 1 is also associated with the formation of fibrous scar tissue. 21 Thus, the prevention of the scalp fibrous tissue infiltrating into the defect and the formation of fibrous scar tissue are the 338
9 PROMOTED BONE HEALING BY TGF-b 1-MICROSPHERES FIG. 7. The time course of FrAFS (s ) and FrARS (d ) values of the bone newly formed at the gap defect of rabbits between the bone flap and the surrounding skull bone after application with various agents. important problems to be resolved for the practical application of TGF-b 1-containing gelatin microspheres as a promising therapeutic agent for promoting the bone healing. ACKNOWLEDGMENT This research was supported by Research for the Future Program Grant No. JSPS-RFTF from the Japan Society for the Promotion of Science. 339
10 HONG ET AL. REFERENCES 1. Schmitz, J.P., and Hollinger, J.O. The critical size defect as an experimental model for craniomandibulo facial nonunions. Clin. Orthop. 205, 299, Habal, M.B. Bone grafting in craniofacial surgery. Clin. Plast. Surg. 21, 349, Lind, M. Growth factor: possible new clinical tools. A review. Acta Orhop. Scand. 67, 407, Bosch, C., Melsen, B., Gibbons, R., and Vargervik, K. Human recombinant transforming growth factor- b 1 in healing of calvarial bone defects. J. Craniofac. Surg. 7, 300, Lind, M., Schumacker, B., Soballe, K., Keller, J., Melsen, F., and Bunger, C. Transforming growth factor-b enhances fracture healing in rabbit tibiae. Acta Orthop. Scand. 64, 553, Yamamoto, M., Tabata, Y., Hong, L., Miyamato, S., Hashimoto, N., and Ikada, Y. Bone regeneration by transforming growth factor b 1 release from a biodegradable hydrogel. J. Cont. Rel. 14, 133, Tabata, Y., and Ikada, Y. Protein release from gelatin matrics. Adv. Drug Deliv. Rev. 31, 287, Hong, L., Tabata, Y., Miyamoto, S., Yamamoto, M., Yamada, K., Hashimoto, N., and Ikada, Y. Bone regeneration at rabbit skull defects treated with transforming growth factor b 1 incorporated in hydrogels with different biodegradabilities. J. Neurosurg. 92, 315, Tabata, Y., Hijikata, S., Muniruzzaman, M.D., and Ikada, Y. Neovascularizati on effect of biodegradable gelatin micropheres incorporating basic fibroblast growth factor. J. Biomater. Sci. Polymer Edn. 10, 79, Linkhart, T.A., Mohan, S., and Baylink, D.J. Growth factors for bone growth and repair: IGF, TGFb and BMP. Bone 19 (Suppl. 1), 1S, Canalis, E. Effect of growth factor on bone cell replication and differentiation. Clin. Orthop. 193, 246, Cook, S.D., Wolfe, M.W., Salkeld, S.L., and Rueger, D.C. Effect of recombinant human osteogenic protein on healing of segmental defects in non-human primates. J. Bone Joint Surg. 77, 734, Takita, H., Tsuruga, E., Ono, I., and Kuboki, Y. Enhancement by bfgf of osteogenesis induced by rhbmp-2 in rats. Eur. J. Oral Sci. 105, 588, Tabata, Y., Yamada, K., Miyamoto, S., Nagata, I., Kikuchi, H., Aoyama, I., Tamura, M., and Ikada, Y. Bone regeneration by basic fibroblast growth factor complexed with biodegradable hydrogels. Biomaterials 19, 807, Yamada, K., Tabata, Y., Yamamoto, K., Miyamoto, S., Nagata, I., Kikuchi, H., and Ikada, Y. Potentiality of bfgf incorporated in biogradable hydrogens for skull bone regeneration. J. Neurosurg. 86, 871, Hong, L., Tabata, Y., Yamamoto, M., Miyamoto, S., Yamada, K., Hashiomoto, N., and Ikada, Y. Comparison of bone regeneration in a rabbit skull defect by recombinant human BMP-2 incorporated in biodegradable hydrogel and in solution. J. Biomater. Sci. Polymer Edn. 9, 1001, Moxham, J.P., Kibblewhite, D.J., Dvorak, M., Perey, B., Tencer, A.F., Bruce, A.G., and Strong, D.M. TGF-b 1 forms functionally normal bone in a segmental sheep tibial diaphyseal defect. J. Otolaryngol. 25, 388, McKinney, L., and Hollinger, J.O. A bone regeneration study: transforming growth factor-b 1 and its delivery. J. Craniofac. Surg. 7, 36, Moxham, J.P., Kibblewhite, D.J., Bruce, A.G., Rigley, T., Gillespy, T 3rd, and Lane, J. Transform ing growth factor-b 1 in a guanidine-extracte d demineralized bone matrix carrier rapidly closes a rabbit critical calvarial defect. J. Otolaryngol. 25, 82, Mehrara, B.J., Steinbrech, D.S., Saadeh, P.B., Gittes, G.K., and Longaker, M.T. Expression of high-affinity receptors for TGF-b during rat cranial suture fusion. Ann. Plast. Surg. 42, 502, Shah, M., Foreman, D.M., and Ferguson, M.W. Neutralisation of TGF-beta 1 and TGF-beta 2 or exogenous addition of TGF-beta 3 to cutaneous rat wounds reduces scarring. J. Cell Sci. 108, 983, Address reprint requests to: Yasuhiko Tabata, Ph.D. Institute for Frontier Medical Sciences Kyoto University 53 Kawara-cho Shogoin Sakyo-ku, Kyoto , Japan yasuhiko@frontier.kyoto- u.ac.jp 340
Tokyo, Japan; and c Department of Biomaterials, Field of Tissue Engineering, Institute for Frontier Medical Sciences, Kyoto University, Kyoto, Japan
 CASE REPORT Easy-to-Use Preservation and Application of Platelet-Rich Plasma in Combination Wound Therapy With a Gelatin Sheet and Freeze-Dried Platelet-Rich Plasma: A Case Report Naoki Morimoto, MD, a
CASE REPORT Easy-to-Use Preservation and Application of Platelet-Rich Plasma in Combination Wound Therapy With a Gelatin Sheet and Freeze-Dried Platelet-Rich Plasma: A Case Report Naoki Morimoto, MD, a
In Vivo Heat-stimulus Triggered Osteogenesis
 In Vivo Heat-stimulus Triggered Osteogenesis Kunihiro Ikuta 1, Hiroshi Urakawa 1, Eiji Kozawa 1, Shunsuke Hamada 1, Naoki Ishiguro 2, Yoshihiro Nishida 1. 1 Nagoya University, Nagoya, Japan, 2 Nagoya Graduated
In Vivo Heat-stimulus Triggered Osteogenesis Kunihiro Ikuta 1, Hiroshi Urakawa 1, Eiji Kozawa 1, Shunsuke Hamada 1, Naoki Ishiguro 2, Yoshihiro Nishida 1. 1 Nagoya University, Nagoya, Japan, 2 Nagoya Graduated
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
Please note: Links to movies, ppt slideshows and any other multimedia files are not available in the pdf version of presentations.
 MRI - CT - histology comparison of bone healing in rabbit calvarial critical sized defects using bioactive glass scaffolds with adipose derived stem cells and VEGF or adipose tissue extract Poster No.:
MRI - CT - histology comparison of bone healing in rabbit calvarial critical sized defects using bioactive glass scaffolds with adipose derived stem cells and VEGF or adipose tissue extract Poster No.:
An Owner's Guide to Natural Healing. Autologous Conditioned Plasma (ACP)
 An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier. MEDLINEUNITE Bioactive Bone Graft
 Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
Bioactive Glass Biphasic β-tcp & HA Granules Alkylene Oxide Polymer Carrier Principles of Bone Healing Reparative Phase Healing Cascade 1. Cellular infiltration and migration to site (fibroblasts, macrophages,
FORMATION OF BONE. Intramembranous Ossification. Bone-Lec-10-Prof.Dr.Adnan Albideri
 FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
FORMATION OF BONE All bones are of mesodermal origin. The process of bone formation is called ossification. We have seen that formation of most bones is preceded by the formation of a cartilaginous model,
Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2, Patrick Smith, M.D. 2, and Larry S. Matthews, M.D. 2
 Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Skeletal Radiol (1986) 15:27-31 Skeletal Radiology Computed tomography and plain radiography in experimental fracture healing Ethan M. Braunstein, M.D. 1, Steven A. Goldstein, Ph.D. 2, Janet Ku, M.S. 2,
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Product Information. MIS Corporation. All Rights Reserved.
 Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
Product Information MIS Corporation. All Rights Reserved. MIS Warranty: MIS exercises great care and effort in maintaining the superior quality of its products. All MIS products are guaranteed to be free
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
Tobacco and Bone Health
 Tobacco and Bone Health Prof. Dr. Alok Chandra Agrawal MS Orthopaedics, DNB Orthopaedics, PhD Orthopaedics MAMS All India Institute of Medical Sciences Raipur CG Cigarette smoking is commonly identified
Tobacco and Bone Health Prof. Dr. Alok Chandra Agrawal MS Orthopaedics, DNB Orthopaedics, PhD Orthopaedics MAMS All India Institute of Medical Sciences Raipur CG Cigarette smoking is commonly identified
BONE TISSUE. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
BONE TISSUE Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology BONE FUNCTION Support Protection (protect internal organs) Movement (provide leverage system for skeletal muscles, tendons, ligaments
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis
 Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Anabolic Therapy With Teriparatide Indications Beyond Osteoporosis Andreas Panagopoulos MD, PhD Upper Limb & Sports Medicine Orthopaedic Surgeon Assistant Professor, University of Patras Outline Teriparatide
Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study
 Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Journal of Orthopaedic Surgery 2010;18(1):63-7 Radiological and histological analysis of synthetic bone grafts in recurring giant cell tumour of bone: a retrospective study Hiroyuki Hattori, Hiroaki Matsuoka,
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft
 Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
Single-Stage Full-Thickness Scalp Reconstruction Using Acellular Dermal Matrix and Skin Graft Yoon S. Chun, MD, a and Kapil Verma, BA b a Division of Plastic and Reconstructive Surgery, Department of Surgery,
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Calcium Phosphate Cement
 Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
Calcium Phosphate Cement Fast-Setting Bone Graft and AutoGraft Extender. * Ossilix is a high performance next generation calcium phosphate cement indicated for filling bony defects in cancellous bone.
BEGO BIOMATERIALS When the result counts
 BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
Slow release of bone morphogenetic protein 2 from a gelatin sponge to promote regeneration of tracheal cartilage in a canine model
 General Thoracic Surgery Slow release of bone morphogenetic protein 2 from a gelatin sponge to promote regeneration of tracheal cartilage in a canine model Taku Okamoto, MD a Yasumichi Yamamoto, MD a Masashi
General Thoracic Surgery Slow release of bone morphogenetic protein 2 from a gelatin sponge to promote regeneration of tracheal cartilage in a canine model Taku Okamoto, MD a Yasumichi Yamamoto, MD a Masashi
Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats
 Journal of Biomaterials Science (2010) DOI:10.1163/092050610X540477 brill.nl/jbs Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats Yanjun Ge, Hailan Feng and Lei
Journal of Biomaterials Science (2010) DOI:10.1163/092050610X540477 brill.nl/jbs Application of a Novel Resorbable Membrane in the Treatment of Calvarial Defects in Rats Yanjun Ge, Hailan Feng and Lei
Gelatin Sheet Incorporating Basic Fibroblast Growth Factor Enhances Healing of Devascularized Sternum in Diabetic Rats
 Gelatin Sheet Incorporating Basic Fibroblast Growth Factor Enhances Healing of Devascularized Sternum in Diabetic Rats Atsushi Iwakura, MD; Yasuhiko Tabata, PhD; Nobushige Tamura, MD; Kazuhiko Doi, MD;
Gelatin Sheet Incorporating Basic Fibroblast Growth Factor Enhances Healing of Devascularized Sternum in Diabetic Rats Atsushi Iwakura, MD; Yasuhiko Tabata, PhD; Nobushige Tamura, MD; Kazuhiko Doi, MD;
o~ r;'c' - OSTEOARTHRITIS
 Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Osteoarthritis and Cartilage (2001) 9, Supplement A, S102-S108 2001 OsteoArthritis Research Society International doi:10.1053/joca.2001.0451, available online at http://www.idealibrary.com on IDE~l Osteoarthritis
Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway
 Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway Jieyuan Zhang, Xiaolin Liu, Haiyan Li, Chunyuan Chen, Bin Hu, Xin Niu, Qing
Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway Jieyuan Zhang, Xiaolin Liu, Haiyan Li, Chunyuan Chen, Bin Hu, Xin Niu, Qing
Biology. Dr. Khalida Ibrahim
 Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
Biology Dr. Khalida Ibrahim BONE TISSUE Bone tissue is a specialized form of connective tissue and is the main element of the skeletal tissues. It is composed of cells and an extracellular matrix in which
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
Title. CitationJournal of hard tissue biology, 22(3): Issue Date Doc URL. Type. File Information. Skull
 Title Bone Augmentation Using Novel Unidirectional Porous Skull Author(s)Kashiwazaki, Haruhiko; Harada, Naoki; Akazawa, Toshi CitationJournal of hard tissue biology, 22(3): 337-341 Issue Date 2013-07 Doc
Title Bone Augmentation Using Novel Unidirectional Porous Skull Author(s)Kashiwazaki, Haruhiko; Harada, Naoki; Akazawa, Toshi CitationJournal of hard tissue biology, 22(3): 337-341 Issue Date 2013-07 Doc
Synthetic and absorbable autograft substitute with osteoinduction
 putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
putty Synthetic and absorbable autograft substitute with osteoinduction Quality made in Germany Synthetic and absorbable autograft substitute with osteoinduction Information on the synthetic bone grafting
Repair of large segmental bone defects in rabbits using BMP and FGF composite xenogeneic bone
 Repair of large segmental bone defects in rabbits using BMP and FGF composite xenogeneic bone X. Li 1 *, Z. Lin 2 *, Y. Duan 2, X. Shu 2, A. Jin 2, S. Min 2 and W. Yi 1 1 Department of Spinal Surgery,
Repair of large segmental bone defects in rabbits using BMP and FGF composite xenogeneic bone X. Li 1 *, Z. Lin 2 *, Y. Duan 2, X. Shu 2, A. Jin 2, S. Min 2 and W. Yi 1 1 Department of Spinal Surgery,
Pre op Failed endodontic treatment with sinus involvement.
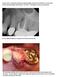 Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Case #1 of 10 consecutive extraction sockets grafted with Socket Graft Putty, covered with Socket Seal and sealed with Periacryl. I D # HEU This patient is a 66 year old female. Pre op Failed endodontic
Ankle and subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
THE NEXT FRONTIER OF BONE REGENERATION
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature swiss made SmartBone is new composite bone substitute specifically developed for bone regeneration in oral and maxillofacial reconstructive
Department of Orthopaedic Surgery NHO, Utsunomiya National Hospital, 2160, Shimo-Okamoto, Utsunomiya City Tochigi, Japan
 Send Orders of Reprints at reprints@benthamscience.org 98 The Open Biomedical Engineering Journal, 2012, 6, 98-103 Open Access Use of an Injectable Complex of!-tricalcium Phosphate Granules, Hyaluronate,
Send Orders of Reprints at reprints@benthamscience.org 98 The Open Biomedical Engineering Journal, 2012, 6, 98-103 Open Access Use of an Injectable Complex of!-tricalcium Phosphate Granules, Hyaluronate,
B&B DENTAL. implant company
 B&B DENTAL implant company Histological analysis of a Novocor Plus implant inserted in sheep bone FACULTY OF NORMAL HUMAN ANATOMY of the UNIVERSITY OF MODENA and PARMA (1990) Micro x-ray of a thick section
B&B DENTAL implant company Histological analysis of a Novocor Plus implant inserted in sheep bone FACULTY OF NORMAL HUMAN ANATOMY of the UNIVERSITY OF MODENA and PARMA (1990) Micro x-ray of a thick section
Promoting Fracture Healing Through Systemic or Local Administration of Allogeneic Mesenchymal Stem Cells
 Promoting Fracture Healing Through Systemic or Local Administration of Allogeneic Mesenchymal Stem Cells Gang Li Dept. of Orthopaedics and Traumatology School of Biomedical Sciences, The Chinese University
Promoting Fracture Healing Through Systemic or Local Administration of Allogeneic Mesenchymal Stem Cells Gang Li Dept. of Orthopaedics and Traumatology School of Biomedical Sciences, The Chinese University
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2
 RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
RECONSTRUCTION OF SCALP DEFECTS: AN INSTITUTIONAL EXPERIENCE Sathyanarayana B. C 1, Somashekar Srinivas 2 HOW TO CITE THIS ARTICLE: Sathyanarayana B. C, Somashekar Srinivas. Reconstruction of Scalp Defects:
synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D.
 C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
C E L L P L E X TCP synthetic CANCELLOUS BONE technical monograph Presented by Barbara Blum, Ph.D. TECHNICAL MONOGRAPH CELLPLEX TCP SYNTHETIC CANCELLOUS BONE CELLPLEX TCP synthetic CANCELLOUS BONE introduction
In Vivo Evaluation of BioSphere Bioactive Bone Graft Putty: Improved Bone Formation
 In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
In Vivo Evaluation of BioSphere Bioactive Bone Graft : Improved Bone Formation ABSTRACT BioSphere is a novel bone graft product that was developed using spherical particles of bioactive glass with a narrow,
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
ULTRASONIC DEVICE IN BONE CUTTING
 Acta orthop. scand. 52, 5-10, 1981 ULTRASONIC DEVICE IN BONE CUTTING A Histological and Scanning Electron Microscopical Study H. ARO*, H. KALLIONIEMI**, A. J. AHO* & P. KELLOKUMPU-LEHTINEN*** *Department
Acta orthop. scand. 52, 5-10, 1981 ULTRASONIC DEVICE IN BONE CUTTING A Histological and Scanning Electron Microscopical Study H. ARO*, H. KALLIONIEMI**, A. J. AHO* & P. KELLOKUMPU-LEHTINEN*** *Department
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration.
 Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Paracrine Effect of Mesenchymal Stem Cells derived from Human Adipose tissue in Bone Regeneration. By Linero I., Chaparro O., 2014 Suzana Tufegdzic 1 Background 2 Background Stem Cells: undifferentiated
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Micro-CT evaluation on osteoconductivity of DCPD-coated β-tcp granule using experimental rats
 Journal of Physics: Conference Series PAPER OPEN ACCESS Micro-CT evaluation on osteoconductivity of DCPD-coated β-tcp granule using experimental rats To cite this article: Khairul Anuar Shariff et al 2018
Journal of Physics: Conference Series PAPER OPEN ACCESS Micro-CT evaluation on osteoconductivity of DCPD-coated β-tcp granule using experimental rats To cite this article: Khairul Anuar Shariff et al 2018
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Elastic Skeleton of Intracranial Cerebral Aneurysms in Rats
 1722 Elastic Skeleton of Intracranial Cerebral Aneurysms in Rats Naohiro Yamazoe, MD, Nobuo Hashimoto, MD, Haruhiko Kikuchi, MD, and Fumitada Hazama, MD In an attempt to clarify the developmental mechanism
1722 Elastic Skeleton of Intracranial Cerebral Aneurysms in Rats Naohiro Yamazoe, MD, Nobuo Hashimoto, MD, Haruhiko Kikuchi, MD, and Fumitada Hazama, MD In an attempt to clarify the developmental mechanism
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
Regeneration Bone Grafting & Soft Tissue Management OSTEON TM II Table of Contents Bone Graft Material OSTEON TM II Collagen 04 OSTEON TM Collagen 06 OSTEON TM II 08 OSTEON TM 12 ORTHOPEDIC OSTEON TM 14
RapidSorb Resorbable Tacks. Resorbable Fixation System.
 RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS
 GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS Based Upon the Published Source: Martin GJ, Jr., Boden SD, Titus L, Scarborough NL. New formulations of demineralized bone matrix
GRAFTON DEMINERALIZED BONE: FIBER TECHNOLOGY AND PERFORMANCE IMPLICATIONS Based Upon the Published Source: Martin GJ, Jr., Boden SD, Titus L, Scarborough NL. New formulations of demineralized bone matrix
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Bone Void Filler. Callos. The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE
 Callos Bone Void Filler The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE Callos Calcium Phosphate Cement Callos is a high performance next generation calcium phosphate cement indicated
Callos Bone Void Filler The Next Generation in Calcium Phosphate Cement A COLSON ASSOCIATE Callos Calcium Phosphate Cement Callos is a high performance next generation calcium phosphate cement indicated
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Enhancement of fracture healing-current trends
 Enhancement of fracture healing-current trends DR. CHETAN PRADHAN MS, F.ASIF (Swiss) CONSULTANT ORTHOPAEDIC SURGEON SANCHETI HOSPITAL, PUNE. Iliac crest : the gold standard Osteogenicity : ability to form
Enhancement of fracture healing-current trends DR. CHETAN PRADHAN MS, F.ASIF (Swiss) CONSULTANT ORTHOPAEDIC SURGEON SANCHETI HOSPITAL, PUNE. Iliac crest : the gold standard Osteogenicity : ability to form
Središnja medicinska knjižnica.
 Središnja medicinska knjižnica Pećina, M., Vukičević, S. (2007) Biological aspects of bone, cartilage and tendon regeneration. International Orthopaedics, 31 (6). pp. 719-720. The original publication
Središnja medicinska knjižnica Pećina, M., Vukičević, S. (2007) Biological aspects of bone, cartilage and tendon regeneration. International Orthopaedics, 31 (6). pp. 719-720. The original publication
A gift you do not want. Motion Avascularity Gap Infection. Prognostic Issues. BMA & BMP: Alternative to Autologous BG? 11/21/2016.
 BMA & BMP: Alternative to Autologous BG? Frank A. Liporace, MD Associate Professor Dept. of Orthopaedics Director Orthopaedic Trauma Research New York University / Hospital for Joint Diseases, NY, NY Chairman
BMA & BMP: Alternative to Autologous BG? Frank A. Liporace, MD Associate Professor Dept. of Orthopaedics Director Orthopaedic Trauma Research New York University / Hospital for Joint Diseases, NY, NY Chairman
Maryland AGD AE and Socket Grafting 2015
 The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
The Goodacre Study 5 year retrospective study looked at Crown & Bridge Caries Single crowns 1% FPD abutments 17% Periodontal Involvement Single crowns
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Comparison of Three Fat Graft Preparation Methods: Gravity Separation, Centrifugation, and the Cytori Puregraft System
 PUREGRAFT Comparison of Three Fat Graft Preparation Methods: Gravity Separation, Centrifugation, and the Cytori Puregraft System John K. Fraser Ph.D., Min Zhu M.D., Douglas M. Arm Ph.D., Johnson C. Yu
PUREGRAFT Comparison of Three Fat Graft Preparation Methods: Gravity Separation, Centrifugation, and the Cytori Puregraft System John K. Fraser Ph.D., Min Zhu M.D., Douglas M. Arm Ph.D., Johnson C. Yu
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
ADVANCED BONE GRAFT SYSTEM OVERVIEW
 ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
ADVANCED BONE GRAFT SYSTEM OVERVIEW NANOSS BIOACTIVE ADVANCED BONE GRAFT Table Of Contents INTRODUCTION System Overview... 1 NANOSS BIOACTIVE COMPONENTS Comparison of nanoss Bioactive and Human Bone...
Bones. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
 Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Bones Osteocytes : Are responsible for maintenance of bones Present in lacunae, and send processes. Unable to divide. The division of bones anatomically is : long, short, irregular, flat and sesamoid.
Sinus Augmentation Studies Methods and Definition
 FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
Peggers Super Summaries Basic Sciences Bone
 Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
Bone Overview & Turnover BONES Function o Support o Protection o Assisting movement o Storage of minerals o Production of red blood cells from marrow Types o Cancellous o Compact with Haversian systems
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
CRANIAL RECONSTRUCTION SOLUTIONS
 CRANIAL RECONSTRUCTION SOLUTIONS CRANIAL RECONSTRUCTION SOLUTIONS Your partner of CHOiCE at depuy Synthes CMF, we are dedicated to providing solutions for your individual patient needs. We do this through
CRANIAL RECONSTRUCTION SOLUTIONS CRANIAL RECONSTRUCTION SOLUTIONS Your partner of CHOiCE at depuy Synthes CMF, we are dedicated to providing solutions for your individual patient needs. We do this through
Dr. Heba Kalbouneh. Saba Alfayoumi. Heba Kalbouneh
 11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
11 Dr. Heba Kalbouneh Saba Alfayoumi Heba Kalbouneh 2- Bone Bone tissue is also classified into primary bone and secondary bone. In the beginning, the first bone that is deposited by the osteoblasts is
ctive Bone Bonding Bone Regeneration Osteostimulation*
 www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
THE WOUND SOLUTION. (Freeze dried Acellular Dermal Matrix) (Cryopreserved Acellular Dermal Matrix)
 (Freeze dried Acellular Dermal Matrix) (Cryopreserved Acellular Dermal Matrix) What is / CGCryoDerm?? /CGCryoDerm are processed by the CGBio co. and is available through Daewoong Bio. /CGCryoDerm are an
(Freeze dried Acellular Dermal Matrix) (Cryopreserved Acellular Dermal Matrix) What is / CGCryoDerm?? /CGCryoDerm are processed by the CGBio co. and is available through Daewoong Bio. /CGCryoDerm are an
ORIGINAL ARTICLE. Clinical and Histological Results of Septoplasty With a Resorbable Implant
 Clinical and Histological Results of Septoplasty With a Resorbable Implant Miriam Boenisch, MD; Antal Mink, MD, PhD ORIGINAL ARTICLE Background: The use of a resorbable implant connected with septal cartilage
Clinical and Histological Results of Septoplasty With a Resorbable Implant Miriam Boenisch, MD; Antal Mink, MD, PhD ORIGINAL ARTICLE Background: The use of a resorbable implant connected with septal cartilage
Comparative Animal Study of OssiMend and Healos 13,14
 Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
Comparative Animal Study of OssiMend and Healos 13,14 Objective This study was conducted to evaluate the use of OssiMend as compared with Healos in combination with autologous bone marrow as a bone grafting
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
Pathophysiology of fracture healing
 Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
Pathophysiology of fracture healing Bone anatomy and biomechanics Fracture patterns Bone healing and blood supply Influence of implants 1 What is the structure of bone? 2 Bone structure Four levels: Chemical
SYNTHECEL Dura Repair. Assurance and Versatility for Dura Reconstruction.
 SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
OssiMend Bone Graft Matrix
 OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
OssiMend All-Natural Mineral-Collagen Bone Grafting Matrix Anorganic bone mineral and type I collagen Highly purified, biocompatible matrix Osteoconductive Osteoinductive and Osteogenic in conjunction
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS
 rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
Biologics in ACL: What s the Data?
 Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
Biologics in ACL: What s the Data? Jo A. Hannafin, M.D., Ph.D. Professor of Orthopaedic Surgery, Weill Cornell Medical College Attending Orthopaedic Surgeon and Senior Scientist Sports Medicine and Shoulder
HEALICOIL REGENESORB Suture Anchor V1 07/14
 HEALICOIL REGENESORB Suture Anchor 02438 V1 07/14 Criteria for the Ideal Bioabsorbable Implant 1. Provides adequate initial fixation strength to heal the soft tissues to bone 2. Maintains satisfactory
HEALICOIL REGENESORB Suture Anchor 02438 V1 07/14 Criteria for the Ideal Bioabsorbable Implant 1. Provides adequate initial fixation strength to heal the soft tissues to bone 2. Maintains satisfactory
The advantages of atelo-collagenated, lyophilized (non-heated), bovine bone graft composite. Dr. med. Sami Watad
 The advantages of atelo-collagenated, lyophilized (non-heated), bovine bone graft composite Dr. med. Sami Watad it s a term that describes the physicochemical deletion of the antigenic terminal peptide
The advantages of atelo-collagenated, lyophilized (non-heated), bovine bone graft composite Dr. med. Sami Watad it s a term that describes the physicochemical deletion of the antigenic terminal peptide
BIOACTIVE SYNTHETIC GRAFT
 B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
B U I L D S T R O N G B O N E F A S T Putty Particulate Morsels A BIOACTIVE SYNTHETIC BONE FOR FASTER HEALING NovaBone is a 100% bioactive synthetic material composed from elements that occur naturally
CONFORM FlEX. Demineralized cancellous bone
 CONFORM FlEX Demineralized cancellous bone TABlE OF CONTENTS introduction 2 FEATURES AND BENEFiTS 4 PROCESSiNg AND PACKAgiNg information 5 MUSCUlOSKElETAl TRANSPlANT FOUNDATiON (MTF) 6 ORDERiNg information
CONFORM FlEX Demineralized cancellous bone TABlE OF CONTENTS introduction 2 FEATURES AND BENEFiTS 4 PROCESSiNg AND PACKAgiNg information 5 MUSCUlOSKElETAl TRANSPlANT FOUNDATiON (MTF) 6 ORDERiNg information
Regeneration Bone Grafting & Soft Tissue Management
 Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Regeneration Bone Grafting & Soft Tissue Management Human Histology OSTEON II 26.5 months Regeneration Products information Table of contents Bone Graft Material OSTEON II OSTEON OSTEON II Collagen OSTEON
Author Index. Aiache, A.E. 12. Colon, G.A. 1, 35. Deluca, L Greenwald, D.P. 156 Greenwald, J.A. 144 Gittes, G.K. 144
 Author Index Aiache, A.E. 12 Colon, G.A. 1, 35 Deluca, L. 156 Greenwald, D.P. 156 Greenwald, J.A. 144 Gittes, G.K. 144 Habal, M.B. IX, 38 Huber, P.W. 141 Lineaweaver, W. 163 Longaker, M.T. 144 Luria, L.W.
Author Index Aiache, A.E. 12 Colon, G.A. 1, 35 Deluca, L. 156 Greenwald, D.P. 156 Greenwald, J.A. 144 Gittes, G.K. 144 Habal, M.B. IX, 38 Huber, P.W. 141 Lineaweaver, W. 163 Longaker, M.T. 144 Luria, L.W.
Inion GTR Biodegradable Membrane System
 Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Inion GTR Biodegradable Membrane System The concept of GTR/GBR Intended use The Inion GTR Biodegradable Membrane System is intended to be used as a barrier membrane in dental guided tissue regeneration
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR
 Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Resorbable bilayer synthetic membrane Biomimetic tissue-engineered matrix for GBR and GTR Patented Jet-Spraying technology: Full barrier effect during 4 weeks, and complete resorption in 6 months PATENTED
Blood. Hematopoietic Tissue
 Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
Blood Hematopoietic Tissue Is a type of connective tissue in which its cells are suspended in a circulating fluid. Erythrocytes+ leukocytes + platelets (thrombocytes) =formed elements of blood. These formed
VMIC 2017 The Veterinary Medicine International Conference 2017 Volume 2017
 The Veterinary Medicine International Conference 2017 Volume 2017 Conference Paper Immunogenicity of Bone Graft Using Xenograft Freeze-Dried Cortical, Allograft Freeze-Dried Cortical New Zealand White
The Veterinary Medicine International Conference 2017 Volume 2017 Conference Paper Immunogenicity of Bone Graft Using Xenograft Freeze-Dried Cortical, Allograft Freeze-Dried Cortical New Zealand White
Horizontal bone augmentation by means of guided bone regeneration
 Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Periodontology 2000, Vol. 66, 2014, 13 40 2014 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd Printed in Singapore. All rights reserved PERIODONTOLOGY 2000 Horizontal bone augmentation by means
Abstract. Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University
 Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
Bone marrow injection in patients with delayed union and non-union of long Firas T. Ismaeel, Dept. of Surgery, College of Medicine, Tikrit University Abstract In the process of bone formation and healing
Focus on: IMPLANT TESTING ISO
 Focus on: IMPLANT TESTING ISO 10993-6 Implantation Assess the local pathological effects on living tissue, at both the gross level and microscopic level, Sample of a material or final product that is surgically
Focus on: IMPLANT TESTING ISO 10993-6 Implantation Assess the local pathological effects on living tissue, at both the gross level and microscopic level, Sample of a material or final product that is surgically
THE BUILDING BLOCKS OF BONE FUSION. Medline Demineralized Bone Allografts Safe and Effective Grafting Options
 THE BUILDING BLOCKS OF BONE FUSION. Medline Demineralized Bone Allografts Safe and Effective Grafting Options 2 MEDLINE BUILD ON QUALITY. Successful bone fusion and osteogenesis depend on a number of factors
THE BUILDING BLOCKS OF BONE FUSION. Medline Demineralized Bone Allografts Safe and Effective Grafting Options 2 MEDLINE BUILD ON QUALITY. Successful bone fusion and osteogenesis depend on a number of factors
Using Animal Models to Help Solve Clinical Problems
 Using Animal Models to Help Solve Clinical Problems -Overview -Epidemiology -Improving the Standards for Initial Wound Care -Use of dual purpose bone grafts -Developing a more relevant animal model Research
Using Animal Models to Help Solve Clinical Problems -Overview -Epidemiology -Improving the Standards for Initial Wound Care -Use of dual purpose bone grafts -Developing a more relevant animal model Research
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model
 Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
Joint and Epiphyseal Progenitor Cells Revitalize Tendon Graft and Form Mineralized Insertion Sites in Murine ACL Reconstruction Model Yusuke Hagiwara 1,2, Nathaniel A. Dyment 3, Douglas J. Adams 3, Shinro
BONE REMODELLING. Tim Arnett. University College London. Department of Anatomy and Developmental Biology
 BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
BONE REMODELLING Tim Arnett Department of Anatomy and Developmental Biology University College London The skeleton, out of sight and often out of mind, is a formidable mass of tissue occupying about 9%
The treatment of destructive periodontal disease, due to specific periodontopathic
 1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
1 1 INTRODUCTION The treatment of destructive periodontal disease, due to specific periodontopathic bacteria, aims at the regeneration of a periodontal attachment composed of new cementum, alveolar bone
ORS 2015 Annual Meeting (Orthopedic Research Society)
 ORS 2015 Annual Meeting (Orthopedic Research Society) Poster No: 1045 CERAMENT Bone Void Filler Impregnated with Gentamicin Increases Bone Formation and Decreases the Rate of Detectable Infection after
ORS 2015 Annual Meeting (Orthopedic Research Society) Poster No: 1045 CERAMENT Bone Void Filler Impregnated with Gentamicin Increases Bone Formation and Decreases the Rate of Detectable Infection after
