P rimary or mechanical implant
|
|
|
- Baldwin Dennis
- 6 years ago
- Views:
Transcription
1 IMPLANT DENTISTRY / VOLUME 0, NUMBER Effect of Location on Primary Stability and Healing of Dental Implants Alberto Monje, DDS,* Fernando Suarez, DDS,* Carlos Andrés Garaicoa, DDS, Florencio Monje, MD, PhD, Pablo Galindo-Moreno, DDS, PhD, Agustín García-Nogales, PhD,k and Hom-Lay Wang, DDS, MS, PhD P rimary or mechanical implant stability plays the main role in successful osseointegration. 1 The implant stability is determined by the availability of bone to anchor the implants. 2 Likewise, bone quality has shown to be a key factor to foresee predictability in implant therapy. 3 Therefore, a quantitative measurement of bone quality is essential before implant restoration. The assessment of whether to continue with restoration is largely based on the implant stability achieved. Thereupon, implant stability could be considered as the absence of mobility; it represents an essential condition to achieve successful outcomes in implant dentistry. 4,5 Many methods have been proposed to assess initial osseointegration. 6 8 However, most of them are no longer available due to their invasiveness and inaccuracy. 6 In 1996, resonance frequency analysis (RFA) was developed and used implant stability quotient (ISQ) as a quantitative unit to assess *Resident, Graduate Periodontics, Department of Periodontics and Oral Medicine, University of Michigan School of Dentistry, Ann Arbor, MI. Visiting Scholar, Graduate Periodontics, Department of Periodontics and Oral Medicine, University of Michigan School of Dentistry, Ann Arbor, MI. Oral and Maxillofacial Surgeon, CICOM, Center of Implantology, Oral and Maxillofacial Surgery, Badajoz, Spain. Adjunct Professor, Department of Mathematics, University of Extremadura, Badajoz, Spain. kadjunct Professor, Department of Oral Surgery and Implant Dentistry, University of Granada, Granada, Spain. Professor and Director, Department of Periodontics and Oral Medicine, University of Michigan School of Dentistry, Ann Arbor, MI. Reprint requests and correspondence to: Alberto Monje, DDS, Calle Juan Miró s/n, local 16-17, Badajoz, Spain, Phone: , Fax: , amonjec@umich.edu ISSN /13/ Implant Dentistry Volume 0 Number 0 Copyright 2013 by Lippincott Williams & Wilkins DOI: /ID Purpose: To study implant primary stability and bone healing using resonance frequency analysis in different anatomical locations 4 months after placement. Material and Methods: Fifty-six partially edentulous patients restored by dental implants were included. Overall, 214 implants were placed without bone or soft tissue augmentation. All implants were placed with the same drilling protocol and implant insertion torque (35 40 N$cm). Results: The mean implant stability quotient (ISQ) value at baseline for all the locations was 75.4 mm (95% confidence interval, mm). Higher ISQ values were found in the mandible. A significant difference between ISQ values of each location (P, 0.001) was identified. The mean values implant stability. 9 The reading of RFA reflects on the combination of the 3 main factors: (1) stiffness of the implant fixture and its interface with the surrounding tissues, (2) design of the transducer, and (3) total effective length above the bone level. 10 The current version of a RFA device uses a small L-shaped transducer to read the implant stability. This transducer comprises 2 piezoceramic elements: one vibrating by a sinusoidal sign (5 15 Hz), whereas the other serves as a receptor. 11 The ISQ reading ranges from 0 to 100, with the higher number indicating higher stability. Although there is no definitive threshold obtained showed an increase (3.4%) in all the locations, being greater in the posterior lower and upper maxillae (3.8%), whereas for the anterior maxilla, it was the least (1.5%) 4 months after healing. This increase was statistically significant in the posterior upper and lower maxillae (P, 0.001). Conclusion: Higher implant stability was found in mandible compared with maxilla in both periods, immediately after insertion and 4 months later. Therefore, according to ISQ values, restoring implants immediately after insertion or after a healing period of 4 months represents safe time points. (Implant Dentistry 2013;0:1 5) Key Words: implant stability, resonance frequency analysis, osseointegration, implant stability quotient value to differentiate a stable, integrated implant from a failing/failed implant, it has been reported that a successful implant had ISQ ranging from 57 to 82 after 1-year loading. 12 Furthermore, a value less than 50 might indicate a potential risk of implant failure. 11 Therefore, ISQ value at the time of implant placement reports primary or mechanical stability and is determined mostly by the availability of bone surrounding the implant and also by the drilling protocol. However, over the time, the ISQ value reflects the healing process of the bone and thus, the secondary or biological stability achieved
2 2 PRIMARY STABILITY AND BONE HEALING OF IMPLANTS MONJE ET AL Table 1. Mean ISQ Values and CI Obtained at the Baseline Implant Location Mean Value (mm) SE Lower Upper Posterior maxilla 74, ,616 75,797 Anterior maxilla 74, ,055 77,000 Posterior 75, ,662 77,183 mandible Anterior mandible 77, ,133 80,767 by dental implants. 13 Into the bargain, implant macrodesign and microdesign have shown to have an impact on ISQ value. For instance, it has been demonstrated that increasing 0.5 mm in implant width provides 10% to 15% more implant surface and thus greater bone-to-implant interface that achieves higher degree of osseointegration. 14 Therefore, to study appropriately the healing process by RFA, it is required to standardize all these parameters. Henceforth, we aimed to study implant primary stability and bone healing using RFA to study the implants in same width, placed with the drilling protocol, and in different locations 4 months after the placement. Accordingly, the present study provides meaningful data to assess the influence of location on ISQ value and thus about the process of osseointegration. MATERIAL AND METHODS Fifty-six partially edentulous healthy patients requiring oral rehabilitation by dental implants were included in this 95% CI Higher ISQ values were found in the mandible. Nonetheless, there is a significant difference between the ISQ values of each location (P, 0.001). SE indicates standard error. study from November 2009 to September Overall, 214 implants (Nobel Biocare Groovy Implants; Nobel Biocare AB, Göteborg, Sweden) were included in the study, of which, 110 were mm and 104 were mm. All these included implants were placed in native ridges with no necessity of bone or soft tissue augmentation. Depending of the height of the remaining bone were placed either 10 or 11.5 mm implants in length. This study was independently reviewed and approved by the local ethical committee of the University Hospital Infanta Cristina (Badajoz, Spain). Written consent from each subject was obtained before the treatment. Inclusion and Exclusion Criteria All the patients recruited met the following inclusion criteria: patients had to be between 18 and 85 years of age, with no systemic diseases or conditions known to alter bone metabolism and exhibit adequate oral hygiene. Patients were selected to undergo implant therapy in native bone with Table 2. Mean ISQ Values and CIs Obtained 4 Months After Implant Placement 95% CI Implant Location Mean Value (mm) SE Lower Upper Posterior maxilla 77, ,763 78,306 Anterior maxilla 75, ,662 77,616 Posterior 78, ,916 79,732 mandible Anterior mandible 80, ,447 82,753 Higher values were registered in the mandible, and a significant difference between the ISQ values of each location (P, 0.001) was also identified. SE indicates standard error. proper bone quality, width, and height and thus, no necessity of bone or soft tissue augmentation. Hence, patients whom underwent either socket preservation or bone augmentation at the time of the surgery or previously were excluded. Also, patients were excluded if they were pregnant, smokers, or taking medications known to modify bone metabolism. Implant Placement All implants were placed in proper bone quality, width, and height. Each patient was required to take 500 mg of amoxicillin or 300 mg of clindamycin, if allergic, 1 hour before the surgery. All operations were performed under local anesthesia or under local anesthesia + intravenous sedation. A full-thickness incision was made to release the flaps. Implants were inserted according to manufacturer s protocol. All implants were placed with the same insertion torque (35 40 N$cm). Finally, the facial flap was released to ensure a tension-free closure, and the flaps were sutured with absorbable suture. All patients received postoperative instructions and were given antibiotics and analgesic medications. The sutures were removed after 7 to 10 days. Resonance Frequency Analyses A RFA device (Ostell Mentor; Integration Diagnostics AB, Göteborg, Sweden) was used for the measurement of primary implant stability. Basically, a designated metal rod (Smartpeg; Integration Diagnostics AB) was screwed into the implant screw vent. Then, a probe was placed close to the rod at the midfacial side and the buccal side of the implant. The ISQ was generated and recorded forbothsides.the2measurements were averaged to represent the primary stability of each implant. Statistical Analysis The mean values of scores were calculated and divided into 4 groups according to their locations (anterior/ posterior and upper/lower jaw). For this, a mixed model was applied to compare the ISQ values at baseline and after the healing period in all the locations.
3 IMPLANT DENTISTRY / VOLUME 0, NUMBER RESULTS Fig. 1. Increasing of ISQ values registered at the baseline and 4 months after implant placement. According to this, the increase is statistically significant in the posterior upper and lower maxillae (P, 0.001). PX indicates posterior maxilla; AX, anterior maxilla; PN, posterior mandible; AN, anterior mandible. Table 3. Mean ISQ Value, SD, and CV of All the Locations Implant Location Implants (N) Mean ISQ Value (mm) SD CV, % Posterior maxilla 4 months Baseline Anterior maxilla 4 months Baseline Posterior mandible 4 months Baseline Anterior mandible 4 months Baseline Total 4 months Baseline The mean values obtained showed an increasing in all the locations (3.4%) being greater in the posterior lower and upper maxilla (3.8%), whereas for the anterior maxilla it was slighter (1.5%). SD indicates standard deviation; CV, coefficient of variation. Descriptive Analysis All dental implants were successfully maintained for 4 months. The number of implants placed in the maxilla was 87 (40.65%) and 36 (16.82%) for the posterior and the anterior areas, respectively. A lesser number of implants was analyzed in the mandible, 71 (33.17%) for the posterior, and 20 (9.34%) for the anterior areas. ISQ Values at the Baseline The mean ISQ value at the baseline for all the locations was 75.4 mm (95% confidence interval [CI], mm). The mean values obtained in each location are represented in Table 1. Higher ISQ values were found out in the mandible. Nonetheless, there is a significant difference between the ISQ values of each location (P, 0.001). ISQ Values 4 Months After Implant Placement The mean ISQ value 4 months after implant placement for all the locations was mm (95% CI, mm). The mean values in each location are represented in Table 2. Again, higher values were registered in the mandible, and a significant difference between the ISQ values of each location (P, 0.001) was also identified. Comparison Between Baseline and 4 Months ISQ Values Figure 1 depicts the evolution of the ISQ values registered at both timelines. The mean values obtained showed an increase (3.4%) in all the locations, being greater in the posterior lower and upper maxillae (3.8%), whereas for the anterior maxilla, it was slighter (1.5%). Therefore, the increase is statistically significant in the posterior upper and lower maxillae (P, 0.001) (Table 3). Moreover, the differences observed in the increases in all the locations are statistically significant among them (P, 0.001) (Fig. 2). Fig. 2. Ninety-five percent CI for the increment of ISQ values from the baseline upto 4 months. Hence, the differences observed in the increases in all the locations are statistically significant among them (P, 0.001). PX indicates posterior maxilla; AX, anterior maxilla; PN, posterior mandible; AN, anterior mandible. DISCUSSION Assuming that implant primary stability plays the major role in early osseointegration, 15 factors related to it must be assessed thoroughly to achieve
4 4 PRIMARY STABILITY AND BONE HEALING OF IMPLANTS MONJE ET AL successful implant therapy. Many parameters, such as implant macrodesign and microdesign or drilling protocol, have shown to affect implant primary stability. 16 Nonetheless, the main parameter that determines dramatically the implant stability over the time is the bone quality. According to Misch (1989) bone quality classification, the location defines bone density. Hence, osseointegration varies according to implant position, and thus, in an attempt to not disturb the biological stability process, loading protocol relies on the location. Many studies have investigated the factors (eg, gender, diameter and length of the implants, surface coating, and other factors) that might affect implant stability. 12,17 According to recent publication, excepting implant length all the other factors, such as anatomical locations, implant surface, drilling protocol, measurement period, and implant diameter, have been shown to influence ISQ. 17 Hence, the purpose of this study was to assess, under the same features and conditions, the effect of implant position upon primary stability and to understand how these implants heal up to 4 months. RFA is a valid method to quantify initial implant stability. Primary stability is related to the percentage of bone-toimplant contact and the bone density around the implant. 18 Furthermore, RFA was shown to correlate with the amount of cortical bone height. 19,20 Thereupon, implant positioned in the lower maxilla should obtain higher ISQ values. Guler et al 17 reported no significant difference in ISQ values between the maxilla and the mandible. However, the posterior maxilla was generally related with lower values, whereas in the mandible, higher values were obtained. On the other hand, Balleri et al 12 found out that although there was significant difference between maxilla and mandible, it was not between the anterior and posterior areas. Similarly, Ersanli et al 20a showed higher primary implant stability of implants placed in the mandible. 17 Accordingly, the results of this study agrees with previous studies, 12,21 25 where implant primary stability was found to be higher in the mandible due to the bone quality of the healthy patients included. Timing of assessment has been considered another important factor to consider. The ISQ values are thought to be higher during baseline due to the primary stability but tend to decrease as soon as healing process and bone remodeling starts. It reaches its peak at 4 weeks, and it increases until it reaches osseointegration at 6 months. 17 Therefore, it has been stated that RFA values had a higher sensitivity and an optimal specificity at 8 weeks when compared with baseline. 17 According to the results obtained in this study, ISQ values change throughout the healing period after implant placement. Four months after the insertion, mean ISQ values of the 214 implants evaluated increased to an average of 2.54 mm (from to mm), presenting the highest increase in the posterior mandible (2.9%), and the lowest increase in the anterior maxilla (1.11%). This is in agreement with several published reports. 17,26,27 In addition, some studies showed that there is a slightly decrease of ISQ value within the first 3 4 weeks, 22,26 with the lowest at 3 weeks. 28 CONCLUSION Within the limitations of this study, it can be concluded that higher implant stability is found in mandible compared with maxilla in both periods, immediately after insertion and 4 months later. In addition, higher increase in implant stability over the study period is found in mandible. Thus, the results of this study indicated that restoring implants either immediately after insertion or after a healing period of 4 months represents safe time points due to their high stability in nonatrophied ridges. DISCLOSURE The authors claim to have no financial interests, either directly or indirectly, in the products or information listed in the article. ACKNOWLEDGMENTS The authors thank FEDICOM Foundation (Foundation for the Study of Implantology, Oral and Maxillofacial Surgery), Badajoz, Spain, for financial support. They also thank Ms. Mamen Monje-Gil and Ms. Purificación Barragán, Center of Implantology, Oral and Maxillofacial Surgery (CICOM), Badajoz, Spain, for their valuable helping to collect and organize the data included in this study. A. García- Nogales was supported by the Spanish Ministerio de Ciencia e Innovación under the project MTM and the Junta de Extremadura Autonomous Government under the grant GR REFERENCES 1. Misch CE, Hoar J, Beck G, et al. A bone quality-based implant system: A preliminary report of stage I and stage II. Implant Dent. 1998;7: Bayarchimeg D, Namgoong H, Kim BK, et al. Evaluation of the correlation between insertion torque and primary stability of dental implants using a block bone test. J Periodontal Implant Sci. 2013;43: Molly L. Bone density and primary stability in implant therapy. Clin Oral Implants Res. 2006;17(suppl 2): Schroeder A, Pohler O, Sutter F. Tissue reaction to an implant of a titanium hollow cylinder with a titanium surface spray layer [in German]. SSO Schweiz Monatsschr Zahnheilkd. 1976;86: Brånemark PI. Rehabilitation with intra-osseous anchorage of dental prosthesis [in Swedish]. Tandlakartidningen. 1972;844: Huang HM, Lee SY, Yeh CY, et al. Resonance frequency assessment of dental implant stability with various bone qualities: A numerical approach. Clin Oral Implants Res. 2002;13: Lachmann S, Jäger B, Axmann D, et al. Resonance frequency analysis and damping capacity assessment. Part I: An in vitro study on measurement reliability and a method of comparison in the determination of primary dental implant stability. Clin Oral Implants Res. 2006;17: Lachmann S, Laval JY, Jäger B, et al. Resonance frequency analysis and damping capacity assessment. Part 2: Peri-implant bone loss follow-up. An in vitro study with the Periotest and Osstell instruments. Clin Oral Implants Res. 2006; 17: Meredith N, Alleyne D, Cawley P. Quantitative determination of the stability of the implant-tissue interface using resonance frequency analysis. Clin Oral Implants Res. 1996;7: Chan HL, El-Kholy K, Fu JH, et al. Implant primary stability determined by resonance frequency analysis in surgically
5 IMPLANT DENTISTRY / VOLUME 0, NUMBER created defects: A pilot cadaver study. Implant Dent. 2010;19: Atsumi M, Park SH, Wang HL. Methods used to assess implant stability: Current status. Int J Oral Maxillofac Implants. 2007; 22: Balleri P, Cozzolino A, Ghelli L, et al. Stability measurements of osseointegrated implants using Osstell in partially edentulous jaws after 1 year of loading: A pilot study. Clin Implant Dent Relat Res. 2002;4: Gapski R, Wang HL, Mascarenhas P, et al. Critical review of immediate implant loading. Clin Oral Implants Res. 2003;14: Capek L, Simunek A, Slezak R, et al. Influence of the orientation of the Osstell transducer during measurement of dental implant stability using resonance frequency analysis: A numerical approach. Med Eng Phys. 2009;31: Anil S, Al Dosari A. Impact of bone quality and implant type on the primary stability: an experimental study using bovine bone. JOralImplant2013. doi: /AAID-JOI-D Abuhussein H, Pagni G, Rebaudi A, et al. The effect of thread pattern upon implant osseointegration. Clin Oral Implants Res. 2010;21: Guler AU, Sumer M, Duran I, et al. Resonance frequency analysis of 208 Straumann dental implants during the healing period. J Oral Implantol. 2013;39: Meredith N. Assessment of implant stability as a prognostic determinant. Int J Prosthodont. 1998;11: Nkenke E, Hahn M, Lell M, et al. Anatomic site evaluation of the zygomatic bone for dental implant placement. Clin Oral Implants Res. 2003;14: Monje A, Monje F, Suarez F, et al. Comparison of implant primary stability between maxillary edentulous ridges receiving intramembranous origin block grafts. Med Oral Patol Oral Cir Bucal. 2013;18:e449 e a. Ersanli S, Karabuda C, Beck F, Leblebicioglu B. Resonance frequency analysis of one-stage dental implant stability during the osseointegration period. JPriodontol 2005;76: Balshi SF, Allen FD, Wolfinger GJ, et al. A resonance frequency analysis assessment of maxillary and mandibular immediately loaded implants. Int J Oral Maxillofac Implants. 2005;20: Barewal RM, Oates TW, Meredith N, et al. Resonance frequency measurement of implant stability in vivo on implants with a sandblasted and acid-etched surface. Int J Oral Maxillofac Implants. 2003; 18: Becker W, Sennerby L, Bedrossian E, et al. Implant stability measurements for implants placed at the time of extraction: A cohort, prospective clinical trial. J Periodontol. 2005;76: Ostman PO, Hellman M, Sennerby L. Direct implant loading in the edentulous maxilla using a bone densityadapted surgical protocol and primary implant stability criteria for inclusion. Clin Implant Dent Relat Res. 2005;7(suppl 1): S60 S Sjöström M, Lundgren S, Nilson H, et al. Monitoring of implant stability in grafted bone using resonance frequency analysis. A clinical study from implant placement to 6 months of loading. Int J Oral Maxillofac Surg. 2005;34: Crismani AG, Bernhart T, Schwarz K, et al. Ninety percent success in palatal implants loaded 1 week after placement: A clinical evaluation by resonance frequency analysis. Clin Oral Implants Res. 2006;17: Sim CP, Lang NP. Factors influencing resonance frequency analysis assessed by Osstell mentor during implant tissue integration: I. Instrument positioning, bone structure, implant length. Clin Oral Implants Res. 2010; 21: Han J, Lulic M, Lang NP. Factors influencing resonance frequency analysis assessed by Osstell mentor during implant tissue integration: II. Implant surface modifications and implant diameter. Clin Oral Implants Res. 2010;21:
Comparison of implant primary stability between maxillary edentulous ridges receiving intramembranous origin block grafts
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.18732 http://dx.doi.org/doi:10.4317/medoral.18732 Comparison of implant primary stability between maxillary edentulous ridges
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.18732 http://dx.doi.org/doi:10.4317/medoral.18732 Comparison of implant primary stability between maxillary edentulous ridges
Predictability of the resonance frequency analysis in the survival of dental implants placed in the anterior non-atrophied edentulous mandible
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.16982 http://dx.doi.org/doi:10.4317/medoral.16982 Predictability of the resonance frequency analysis in the survival of dental
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.16982 http://dx.doi.org/doi:10.4317/medoral.16982 Predictability of the resonance frequency analysis in the survival of dental
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
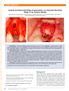 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Hiron Andreaza da Cunha, MS 1 /Carlos Eduardo Francischone, DMD 2 /Hugo Nary Filho, DDS 3 / Rubelisa Cândido Gomes de Oliveira, BDS 4
 A Comparison Between Cutting Torque and Resonance Frequency in the Assessment of Primary Stability and Final Torque Capacity of and TiUnite Single-Tooth Implants Under Immediate Loading Hiron Andreaza
A Comparison Between Cutting Torque and Resonance Frequency in the Assessment of Primary Stability and Final Torque Capacity of and TiUnite Single-Tooth Implants Under Immediate Loading Hiron Andreaza
Dental Research Journal
 Dental Research Journal Original Article The effect of shape, length and diameter of implants on primary stability based on resonance frequency analysis Hamidreza Barikani, Shadab Rashtak, Soolmaz Akbari,
Dental Research Journal Original Article The effect of shape, length and diameter of implants on primary stability based on resonance frequency analysis Hamidreza Barikani, Shadab Rashtak, Soolmaz Akbari,
DEVELOPMENT OF PREDICTABLE STABILITY TEST FOR ASSESSMENT OF OPTIMUM LOADING TIME IN DENTAL IMPLANT
 ORIGINAL ARTICLE DOI:10.4047/jkap.2008.46.6.628 DEVELOPMENT OF PREDICTABLE STABILITY TEST FOR ASSESSMENT OF OPTIMUM LOADING TIME IN DENTAL IMPLANT Seong-Kyun Kim 1, DDS, PhD, Seong-Joo Heo 2, DDS, PhD,
ORIGINAL ARTICLE DOI:10.4047/jkap.2008.46.6.628 DEVELOPMENT OF PREDICTABLE STABILITY TEST FOR ASSESSMENT OF OPTIMUM LOADING TIME IN DENTAL IMPLANT Seong-Kyun Kim 1, DDS, PhD, Seong-Joo Heo 2, DDS, PhD,
EFFECT OF IMPLANT DESIGN ON INITIAL STABILITY
 CLINICAL EFFECT OF IMPLANT DESIGN ON INITIAL STABILITY OF TAPERED IMPLANTS Linus Chong, DDS, MS; Ahmed Khocht, DDS, MSD; Jon B. Suzuki, DDS, PhD; John Gaughan, PhD Implant design is one of the parameters
CLINICAL EFFECT OF IMPLANT DESIGN ON INITIAL STABILITY OF TAPERED IMPLANTS Linus Chong, DDS, MS; Ahmed Khocht, DDS, MSD; Jon B. Suzuki, DDS, PhD; John Gaughan, PhD Implant design is one of the parameters
MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION
 Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
Case Report International Journal of Dental and Health Sciences Volume 02, Issue 06 MANAGEMENT OF ATROPHIC ANTERIOR MAXILLA USING RIDGE SPLIT TECHNIQUE, IMMEDIATE IMPLANTATION AND TEMPORIZATION Rakshith
The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study
 26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
It is of interest to develop and evaluate
 RESEARCH Validation of Resonance Frequency Analysis by Comparing Implant Stability Quotient Values With Histomorphometric Data Ashish Thomas Kunnekel, MDS 1 * K. Chandrasekharan Nair, MDS 2 E. Munirathnam
RESEARCH Validation of Resonance Frequency Analysis by Comparing Implant Stability Quotient Values With Histomorphometric Data Ashish Thomas Kunnekel, MDS 1 * K. Chandrasekharan Nair, MDS 2 E. Munirathnam
Annals of Dental Research
 P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
10 Years of XiVE Implantology Unlimited
 10 Years of XiVE Implantology Unlimited Implantology Unlimited is obligate for XiVE and every limit gives always a push to surrender new challenges: Primary stability in low bone quality? No problem with
10 Years of XiVE Implantology Unlimited Implantology Unlimited is obligate for XiVE and every limit gives always a push to surrender new challenges: Primary stability in low bone quality? No problem with
Assessment of Implant Stability of Two-piece Zirconium Dioxide Implants using the Resonance Frequency Analysis: A Pilot Study
 IJEDS Assessment of Implant Stability of Two-piece Zirconium Dioxide Implants using 10.5005/jp-journals-10029-1103 the Resonance Frequency Analysis RESEARCH ARTICLE Assessment of Implant Stability of Two-piece
IJEDS Assessment of Implant Stability of Two-piece Zirconium Dioxide Implants using 10.5005/jp-journals-10029-1103 the Resonance Frequency Analysis RESEARCH ARTICLE Assessment of Implant Stability of Two-piece
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S.
 THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
THE USE OF TEMPORARY ANCHORAGE DEVICES FOR MOLAR INTRUSION & TREATMENT OF ANTERIOR OPEN BITE By Eduardo Nicolaievsky D.D.S. Skeletal anchorage, the concept of using the facial skeleton to control tooth
STABILITY OF IMPLANTS AND NATURAL TEETH MONTHS OF FUNCTION AS DETERMINED BY THE PERIOTEST OVER 60 CLINICAL
 CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
CLINICAL STABILITY OF IMPLANTS AND NATURAL TEETH AS DETERMINED BY THE PERIOTEST OVER 60 MONTHS OF FUNCTION Sheldon Winkler, DDS Harold F. Morris, DDS, MS J. Robert Spray, DDS KEY WORDS Implant Natural
A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2011.3.4.190 A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis In-Ho Kang,
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2011.3.4.190 A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis In-Ho Kang,
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
e153 Resident, Department of Periodontics and Oral Medicine, University of Michigan School of Dentistry, Ann Arbor, Michigan, USA.
 e153 Comparison of Microstructures Between Block Grafts from the Mandibular Ramus and Calvarium for Horizontal Bone Augmentation of the Maxilla: A Case Series Study Alberto Monje, DDS 1 /Florencio Monje,
e153 Comparison of Microstructures Between Block Grafts from the Mandibular Ramus and Calvarium for Horizontal Bone Augmentation of the Maxilla: A Case Series Study Alberto Monje, DDS 1 /Florencio Monje,
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE
 J Korean Acad Prosthodont : Volume 44, Number 3, 2006 A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE Jong-Hyuk Lee 1,2, D.D.S., M.S.D., Jae-Ho Yang 1, D.D.S.,
J Korean Acad Prosthodont : Volume 44, Number 3, 2006 A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE Jong-Hyuk Lee 1,2, D.D.S., M.S.D., Jae-Ho Yang 1, D.D.S.,
Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis
 CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
CASE REPORT Rehabilitation of atrophic partially edentulous mandible using ridge split technique and implant supported removable prosthesis Dr Ashish Yadav 1, Dr Aratee Gupta 2, Dr Archana Singh 3, 1,3-
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Identification of Stability Changes for Immediately Placed Dental Implants
 Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
Enhancing implant stability with osseodensification a case report with 2-year follow-up
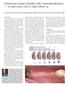 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Resonance Frequency Analysis Measurements of Implants at Placement Surgery
 Resonance Frequency Analysis Measurements of Implants at Placement Surgery Pär-Olov Östman, DDS a /Mats Hellman, DDS a /Inger Wendelhag, PhD b /Lars Sennerby, DDS, PhD c Purpose: The knowledge of what
Resonance Frequency Analysis Measurements of Implants at Placement Surgery Pär-Olov Östman, DDS a /Mats Hellman, DDS a /Inger Wendelhag, PhD b /Lars Sennerby, DDS, PhD c Purpose: The knowledge of what
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Implant stability, whether immediately following surgery
 RESEARCH The Evaluation of the Reliability of Periotest for Implant Stability s: An In Vitro Study Hakan Bilhan, PhD, DDS 1 Altug Cilingir, PhD, DDS 2 Canan Bural, PhD, DDS 3 Caglar Bilmenoglu, PhD, DDS
RESEARCH The Evaluation of the Reliability of Periotest for Implant Stability s: An In Vitro Study Hakan Bilhan, PhD, DDS 1 Altug Cilingir, PhD, DDS 2 Canan Bural, PhD, DDS 3 Caglar Bilmenoglu, PhD, DDS
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
Pressure Necrosis And Osseointegration: An Editorial White Paper*
 Pressure Necrosis And Osseointegration: An Editorial White Paper* Alan Meltzer, DMD, MScD; Harold Baumgarten, DMD; Tiziano Testori, MD, DDS; Paolo Trisi, DDS, PhD Published by Pressure Necrosis And Osseointegration:
Pressure Necrosis And Osseointegration: An Editorial White Paper* Alan Meltzer, DMD, MScD; Harold Baumgarten, DMD; Tiziano Testori, MD, DDS; Paolo Trisi, DDS, PhD Published by Pressure Necrosis And Osseointegration:
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols
 Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Group 3 Consensus Statements Consensus Statements and Recommended Clinical Procedures Regarding Loading Protocols Hans-Peter Weber, DMD, Dr Med Dent 1 /Dean Morton, BDS, MS 2 /German O. Gallucci, DMD,
Osstell ISQ. The objective way to measure implant stability.
 Osstell ISQ. The objective way to measure implant stability. www.osstell.com Three reasons why you need Osstell ISQ. Dr Tiziano Testori, Private Practice, Como, Italy: I use the Osstell meter as a quality-assurance
Osstell ISQ. The objective way to measure implant stability. www.osstell.com Three reasons why you need Osstell ISQ. Dr Tiziano Testori, Private Practice, Como, Italy: I use the Osstell meter as a quality-assurance
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
TOPICS. T O P I C S Day 1. Implant Locations. Implant Placement in the Posterior Maxilla. Anatomy and risk factors Option 1: Short implants
 T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
In 1981, Dr. Albrektsson, a member of
 Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space
 Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Case Report Immediate Loading with Flapless Implant Surgery for Rehabilitation of Single Bound Edentulous Space Nidhi Bhatia 1, Shweta Bali 2, Meenu Taneja Bhasin 3, Priyanka Aggarwal 4, Vaibhav Joshi
Resonance frequency analysis-reliability in third generation instruments: Osstell mentor
 Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.17861 http://dx.doi.org/doi:10.4317/medoral.17861 Resonance frequency analysis-reliability in third generation instruments:
Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.17861 http://dx.doi.org/doi:10.4317/medoral.17861 Resonance frequency analysis-reliability in third generation instruments:
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
BONE CHARACTERISTICS AND IMPLANT STABILITY
 REVIEWS BONE CHARACTERISTICS AND IMPLANT STABILITY Elitsa Sabeva 1, Stefan Peev 1, Mariya Miteva 1, Milena Georgieva 2 1 Department of Periodontology and Dental Implantology, Faculty of Dental Medicine,
REVIEWS BONE CHARACTERISTICS AND IMPLANT STABILITY Elitsa Sabeva 1, Stefan Peev 1, Mariya Miteva 1, Milena Georgieva 2 1 Department of Periodontology and Dental Implantology, Faculty of Dental Medicine,
The influence of radiotherapy on osseointegration
 Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Experience with Osseointegrated Implants Placed in Irradiated Tissues in Japan and the United States Atsushi Niimi, DDS, DMSc*/Minoru Ueda, DDS, PhD**/ Eugene E. Keller, DDS, PhD***/Philip Worthington,
Enhanced Implant Stability with a Chemically Modified SLA Surface: A Randomized Pilot Study
 Enhanced Implant Stability with a Chemically Modified SLA Surface: A Randomized Pilot Study Thomas W. Oates, DMD, PhD 1 /Pilar Valderrama, DDS, MS 2 /Mark Bischof, Dr Med Dent 3 / Rabah Nedir, Dr Med Dent
Enhanced Implant Stability with a Chemically Modified SLA Surface: A Randomized Pilot Study Thomas W. Oates, DMD, PhD 1 /Pilar Valderrama, DDS, MS 2 /Mark Bischof, Dr Med Dent 3 / Rabah Nedir, Dr Med Dent
Maxillary Sinus Lateral Wall Thickness and Their Morphologic Patterns in the Atrophic Posterior Maxilla
 Maxillary Sinus Lateral Wall Thickness and Their Morphologic Patterns in the Atrophic Posterior Maxilla Alberto Monje, D.D.S.*, Andrés Catena PhD Florencio Monje, MD, PhD, Raúl Gonzalez-García MD, PhD,
Maxillary Sinus Lateral Wall Thickness and Their Morphologic Patterns in the Atrophic Posterior Maxilla Alberto Monje, D.D.S.*, Andrés Catena PhD Florencio Monje, MD, PhD, Raúl Gonzalez-García MD, PhD,
Implant stability is considered one of the most important
 Development of Implant Stability During Early Healing of Immediately Loaded Implants Antonin Simunek, MD, PhD 1 /Dana Kopecka, MD, PhD 2 /Tomas Brazda, MD 2 / Jakub Strnad, PhD 3 /Lukas Capek, PhD 4 /Radovan
Development of Implant Stability During Early Healing of Immediately Loaded Implants Antonin Simunek, MD, PhD 1 /Dana Kopecka, MD, PhD 2 /Tomas Brazda, MD 2 / Jakub Strnad, PhD 3 /Lukas Capek, PhD 4 /Radovan
Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report
 Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
Research & Reviews: Journal of Dental Sciences Rehabilitating a Compromised Site for Restoring Form, Function and Esthetics- A Case Report Priyanka Prakash* Division of Periodontology, Department of Dental
NobelActive Inventor s perspective on this new direction for implants
 NobelActive Inventor s perspective on this new direction for implants Nobel Biocare launches a unique new implant with revolutionary features due to the advanced design of its implant body NobelActive.
NobelActive Inventor s perspective on this new direction for implants Nobel Biocare launches a unique new implant with revolutionary features due to the advanced design of its implant body NobelActive.
BONE SPREADING TECHNIQUE A CASE REPORT. simultaneous implant placement and is an alternative Summer s osteotome both clinical use as well as the
 BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
 Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Neenu M Varghese et al Case Report 10.5005/jp-journals-10012-1148 A Novel Technique for the Management of a Maxillary Anterior Alveolar Defect with an Implant-retained Fixed Prosthesis: A Clinical Report
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
I have always enjoyed Dr. Steigmann s lecture because it is practical, insightful and supported with sound rationale
 March 19-24, 2018 1 Introduction I have always enjoyed Dr. Steigmann s lecture because it is practical, insightful and supported with sound rationale Prof. Hom Lay Wang Dr. Marius Steigmann Dr. Steigmann
March 19-24, 2018 1 Introduction I have always enjoyed Dr. Steigmann s lecture because it is practical, insightful and supported with sound rationale Prof. Hom Lay Wang Dr. Marius Steigmann Dr. Steigmann
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Primary implant stability has been identified as a major
 CLINICAL Osstell Resonance Frequency Measurement Values as a Prognostic Factor in Implant Dentistry Tim Krafft, PD, Dr. med. DMD 1 Friedrich Graef, Dr. rer. nat. 2 Matthias Karl, PD, DMD 3 * Resonance
CLINICAL Osstell Resonance Frequency Measurement Values as a Prognostic Factor in Implant Dentistry Tim Krafft, PD, Dr. med. DMD 1 Friedrich Graef, Dr. rer. nat. 2 Matthias Karl, PD, DMD 3 * Resonance
Open Access The Effect of Flapless and Full-thickness Flap Techniques on Implant Stability During the Healing Period
 Send Orders for Reprints to reprints@benthamscience.ae The Open Dentistry Journal, 2015, 9, 243-249 243 Open Access The Effect of Flapless and Full-thickness Flap Techniques on Implant Stability During
Send Orders for Reprints to reprints@benthamscience.ae The Open Dentistry Journal, 2015, 9, 243-249 243 Open Access The Effect of Flapless and Full-thickness Flap Techniques on Implant Stability During
Flapless Dental Implantation using Cortex Implants
 Flapless Dental Implantation using Cortex Implants By Dr. Meir Mamraev DMD LLB W e P r o v e I t E v e r y D a y The following case study discusses the flapless implant surgery approach using the Cortex
Flapless Dental Implantation using Cortex Implants By Dr. Meir Mamraev DMD LLB W e P r o v e I t E v e r y D a y The following case study discusses the flapless implant surgery approach using the Cortex
MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT
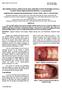 ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
ISSN: 0976-2876 (Print) ISSN: 2250-0138 (Online) MULTIDIRECTIONAL APPROACH OF ORAL REHABILITATION WITH IMPLANTS IN A PATIENT WITH LIMITED MOUTH OPENING: A CASE REPORT ROMESH SONI a, HARAKH CHAND BARANWAL
EFFECTIVE DATE: 04/24/14 REVISED DATE: 04/23/15, 04/28/16, 06/22/17, 06/28/18 POLICY NUMBER: CATEGORY: Dental
 MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
MEDICAL POLICY SUBJECT: DENTAL IMPLANTS PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an Essential
The International Journal of Periodontics & Restorative Dentistry
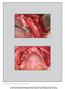 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
Retreatment: Fractured Implants Due To Biomechanical Overload
 Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Implant Placement in Maxillary Anterior Region Along with Soft and Hard Tissue Grafting- A Case Report.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 10 Ver. XII (October. 2016), PP 68-73 www.iosrjournals.org Implant Placement in Maxillary Anterior
Practical Advanced Periodontal Surgery
 Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Practical Advanced Periodontal Surgery Serge Dibart Blackwell Munksgaard Chapter 8 Papillary Construction After Dental Implant Therapy Peyman Shahidi, DOS, MScD, Serge Dibart, DMD, and Yun Po Zhang, PhD,
Specialty Dentistry. Dentistry has nine specialty fields recognized by the American Dental Association
 Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
Specialty Dentistry Dentistry has nine specialty fields recognized by the American Dental Association Dental Public Health Endodontics Oral and Maxillofacial Pathology Oral and Maxillofacial Radiology
WORKSHOP ON THE STATE OF THE SCIENCE OF IMPLANT DENTISTRY. Chicago August 2006
 WORKSHOP ON THE STATE OF THE SCIENCE OF IMPLANT DENTISTRY. Chicago August 2006 Group 1. What Is the Effect on Outcomes of Time to Loading of a Fixed or Removable Prosthesis Placed on Implant(s)? How does
WORKSHOP ON THE STATE OF THE SCIENCE OF IMPLANT DENTISTRY. Chicago August 2006 Group 1. What Is the Effect on Outcomes of Time to Loading of a Fixed or Removable Prosthesis Placed on Implant(s)? How does
Resonance Frequency Measurement of Implant Stability In Vivo on Implants with a Sandblasted and Acid-Etched Surface
 Resonance Frequency Measurement of Implant Stability In Vivo on Implants with a Sandblasted and Acid-Etched Surface Reva M. Barewal, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 /Neil Meredith, BDS, MSc, PhD
Resonance Frequency Measurement of Implant Stability In Vivo on Implants with a Sandblasted and Acid-Etched Surface Reva M. Barewal, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 /Neil Meredith, BDS, MSc, PhD
Revisions for CDT 2016
 Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
Revisions for CDT 2016 This document was developed from preliminary actions of the Code Maintenance Committee (CMC). This document has been compared to the CMC meeting notes and the ASCII file. This document
scientific compendium
 scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
More than a fixed rehabilitation.
 More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have elaborate expectations
More than a fixed rehabilitation. A reason to smile. In combination with: Patient expectations drive dental treatments for fixed edentulous immediate restorations. Patients today have elaborate expectations
Tapered Screw-Vent Implant System
 Tapered Screw-Vent Implant System The implant of choice brings flexibility to your practice. 1 clinical results and secondary stability Tapered Screw-Vent Implant Celebrates 11 Years of Quality Celebrating
Tapered Screw-Vent Implant System The implant of choice brings flexibility to your practice. 1 clinical results and secondary stability Tapered Screw-Vent Implant Celebrates 11 Years of Quality Celebrating
Basic information on the. Straumann Pro Arch TL. Straumann Pro Arch TL
 Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Basic information on the Straumann Pro Arch TL Straumann Pro Arch TL Contents 1. Introduction 2 1.1 Discover more treatment options with the 4 mm Short Implant 2 2. Technical information 3 3. Step-by-step
Esthetic management of multiple missing anterior teeth A Case report
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 1 Ver. II (Jan. 2014), PP 97-101 Esthetic management of multiple missing anterior teeth A
Analysis of 472 Brånemark System TiUnite Implants: A Retrospective Study
 Kobe J. Med. Sci., Vol. 55, No. 3, pp. E73-E81, 2009 Analysis of 472 Brånemark System TiUnite Implants: A Retrospective Study YASUYUKI SHIBUYA*, MASAKI KOBAYASHI, JUNICHIRO TAKEUCHI, TOMOKO ASAI, MAHO
Kobe J. Med. Sci., Vol. 55, No. 3, pp. E73-E81, 2009 Analysis of 472 Brånemark System TiUnite Implants: A Retrospective Study YASUYUKI SHIBUYA*, MASAKI KOBAYASHI, JUNICHIRO TAKEUCHI, TOMOKO ASAI, MAHO
Featured Patient Case #1: Complete Mouth Reconstruction with Hybrid Restorations
 Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Philip L. Fava II, DMD, MDSc Robert A. Levine, DDS, FCPP, FISPPS 9880 Bustleton Ave, Suite 211 Philadelphia, PA 19115 PADentalImplants.com 215-677-8686 Featured Patient Case #1: Complete Mouth Reconstruction
Zygomatic Implants Using the Sinus Slot Technique: Clinical Report of a Patient Series
 Zygomatic Implants Using the Sinus Slot Technique: Clinical Report of a Patient Series Miguel Peñarrocha, MD, DDS, PhD 1 /Roberto Uribe, DDS, MDS 2 /Berta García, DDS, MDS 3 /Eva Martí, DDS 4 Purpose:
Zygomatic Implants Using the Sinus Slot Technique: Clinical Report of a Patient Series Miguel Peñarrocha, MD, DDS, PhD 1 /Roberto Uribe, DDS, MDS 2 /Berta García, DDS, MDS 3 /Eva Martí, DDS 4 Purpose:
Clinical evaluation of osseointegration using resonance frequency analysis
 Review Article Clinical evaluation of osseointegration using resonance frequency analysis Parth Satwalekar, Sandeep Nalla, Ramaswamy Reddy, Sheeba Glory Chowdary SVS Institute of Dental Sciences, Mahabubnagar,
Review Article Clinical evaluation of osseointegration using resonance frequency analysis Parth Satwalekar, Sandeep Nalla, Ramaswamy Reddy, Sheeba Glory Chowdary SVS Institute of Dental Sciences, Mahabubnagar,
Guided surgery as a way to simplify surgical implant treatment in complex cases
 52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
52 STARGET 1 I 12 StraUMaNN CareS r ry vincenzo MiriSOLA Di TOrreSANTO AND LUCA COrDArO Guided surgery as a way to simplify surgical implant treatment in complex cases Background A 41-year-old woman with
International Journal of Applied Dental Sciences 2018; 4(1): Dr. Renu gupta, Dr. RP Luthra, Suhani Kukreja
 2018; 4(1): 213-218 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(1): 213-218 2018 IJADS www.oraljournal.com Received: 06-11-2017 Accepted: 07-12-2017 Dr. Renu gupta Professor and head, Department
2018; 4(1): 213-218 ISSN Print: 2394-7489 ISSN Online: 2394-7497 IJADS 2018; 4(1): 213-218 2018 IJADS www.oraljournal.com Received: 06-11-2017 Accepted: 07-12-2017 Dr. Renu gupta Professor and head, Department
Endosseous cylindric implants are well accepted
 Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Soft Tissue Exposure of Endosseous Implants Between Stage I and Stage II Surgery as a Potential Indicator of Early Crestal Bone Loss Joseph A. Toljanic, DDS*/Mark L. Banakis, DDS**/Leslee A. K. Willes,
Jie Han Martina Lulic Niklaus P. Lang
 Jie Han Martina Lulic Niklaus P. Lang Factors influencing resonance frequency analysis assessed by Osstellt mentor during implant tissue integration: II. Implant surface modifications and implant diameter
Jie Han Martina Lulic Niklaus P. Lang Factors influencing resonance frequency analysis assessed by Osstellt mentor during implant tissue integration: II. Implant surface modifications and implant diameter
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report
 Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
Surgery All at Once : Socket preservation and immediate placement of an implant in an infected site in the anterior region a Case Report W.P. van der Schoor*, A.R.M. van der Schoor Tooth extraction followed
Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study
 Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Original Article Evaluation of implant stability and crestal bone loss around the implant prior to prosthetic loading: A six month study P. Singh, H. G. Garge*, V. S. Parmar, M. Viswambaran*, M. M. Goswami*
Non-osseointegrated. What type of mini-implants? 3/27/2008. Require a tight fit to be effective Stability depends on the quality and.
 Non-osseointegrated What type of mini-implants? Require a tight fit to be effective Stability depends on the quality and quantity of cortical and trabecular bone. Osseointegrated Non-osseointegrated AbsoAnchor
Non-osseointegrated What type of mini-implants? Require a tight fit to be effective Stability depends on the quality and quantity of cortical and trabecular bone. Osseointegrated Non-osseointegrated AbsoAnchor
Measurement of the Maxilla and Zygoma as an Aid in Installing Zygomatic Implants
 J Oral Maxillofac Surg 59:1193-1198, 2001 Measurement of the Maxilla and Zygoma as an Aid in Installing Zygomatic Implants Yuki Uchida, DDS, PhD,* Masaaki Goto, DDS, PhD, Takeshi Katsuki DDS, PhD, and
J Oral Maxillofac Surg 59:1193-1198, 2001 Measurement of the Maxilla and Zygoma as an Aid in Installing Zygomatic Implants Yuki Uchida, DDS, PhD,* Masaaki Goto, DDS, PhD, Takeshi Katsuki DDS, PhD, and
Clinical Perspectives
 Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Clinical Perspectives Inside This Issue: Revised Drilling Guidelines For Parallel Walled Implants Case Presentation By: Pär-Olov Östman, DDS, PhD, MD Volume 8, Issue 1 Recommended Drilling Guidelines For
Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique
 e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
e116 Pouch Roll Technique for Implant Soft Tissue Augmentation: A Variation of the Modified Roll Technique Sang-Hoon Park, DDS, MS* Hom-Lay Wang, DDS, MSD, PhD** This paper presents three cases of peri-implant
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
PLACEMENT OF DENTAL IMPANT IN POSTERIOR MAXILLARY RIDGE USING INDIRECT SINUS LIFT TECHNIQUE WITHOUT GRAFT: A CASE REPORT
 CSE REPORT PLCEMENT OF DENTL IMPNT IN POSTERIOR MXILLRY RIDGE USING INDIRECT SINUS LIFT TECHNIQUE WITHOUT GRFT: CSE REPORT S.P.S Sooch 1, Puja 2, Seema ggarwal 3 (e) ISSN Online: 2321-9599 (p) ISSN Print:
CSE REPORT PLCEMENT OF DENTL IMPNT IN POSTERIOR MXILLRY RIDGE USING INDIRECT SINUS LIFT TECHNIQUE WITHOUT GRFT: CSE REPORT S.P.S Sooch 1, Puja 2, Seema ggarwal 3 (e) ISSN Online: 2321-9599 (p) ISSN Print:
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure
 Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
Placement of Posterior Mandibular and Maxillary Implants in Patients with Severe Bone Deficiency: A Clinical Report of Procedure Leonard Krekmanov, DDS, PhD 1 The purpose of this investigation was to modify
MALO CLINIC PROTOCOL IMMEDIATE-FUNCTION CONCEPT UPPER AND LOWER JAW REHABILITATION: A CLINICAL REPORT
 MALO CLINIC PROTOCOL IMMEDIATE-FUNCTION CONCEPT UPPER AND LOWER JAW REHABILITATION: A CLINICAL REPORT PURPOSE Rehabilitation case with an implant-supported rehabilitation with immediate function implants.
MALO CLINIC PROTOCOL IMMEDIATE-FUNCTION CONCEPT UPPER AND LOWER JAW REHABILITATION: A CLINICAL REPORT PURPOSE Rehabilitation case with an implant-supported rehabilitation with immediate function implants.
While the protocol for direct bone-to-implant
 Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
Immediate Functional Loading of Brånemark System Implants in Edentulous Mandibles: Clinical Report of the Results of Developmental and Simplified Protocols Glenn J. Wolfinger, DMD 1 / Thomas J. Balshi,
The Implant Stability Quotient Whitebook. The relationship between reliable diagnostics and safe, successful dental implant procedures 1 st edition
 The Implant Stability Quotient Whitebook The relationship between reliable diagnostics and safe, successful dental implant procedures 1 st edition Executive summary 4 Foreword by Professor Lars Sennerby,
The Implant Stability Quotient Whitebook The relationship between reliable diagnostics and safe, successful dental implant procedures 1 st edition Executive summary 4 Foreword by Professor Lars Sennerby,
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Mini implants for Stabilization of partial dentures
 Systematically to the goal Mini implants for Stabilization of partial dentures Winfried Walzer Prostheses are still considered by many to be aesthetically pleasing, cost-effective, but often associated
Systematically to the goal Mini implants for Stabilization of partial dentures Winfried Walzer Prostheses are still considered by many to be aesthetically pleasing, cost-effective, but often associated
Immediate function or immediate
 Immediate function with dental implants Immediate function or immediate loading is defined as the placement of a dental implant fixture, abutment and functional (provisional) restoration all at stage one
Immediate function with dental implants Immediate function or immediate loading is defined as the placement of a dental implant fixture, abutment and functional (provisional) restoration all at stage one
