Predictability of the resonance frequency analysis in the survival of dental implants placed in the anterior non-atrophied edentulous mandible
|
|
|
- Godfrey Long
- 6 years ago
- Views:
Transcription
1 Journal section: Oral Surgery Publication Types: Research doi: /medoral Predictability of the resonance frequency analysis in the survival of dental implants placed in the anterior non-atrophied edentulous mandible Raúl González-García 1, Florencio Monje 2, Carlos Moreno-García 2 1 MD, Staff Surgeon. Department of Oral and Maxillofacial Surgery, University Hospital Infanta Cristina, Badajoz, Spain 2 MD, PhD. Oral and Maxillofacial Surgeon, CICOM, Centro de Implantología y Cirugía Oral y Maxilofacial, Badajoz, Spain Correspondence: Calle Los Yébenes 35, 8C 28047, Madrid, Spain raulmaxilo@gmail.com Received: 13/03/2010 Accepted: 02/04/2010 González-García R, Monje F, Moreno-García C. Predictability of the resonance frequency analysis in the survival of dental implants placed in the anterior non-atrophied edentulous mandible. Med Oral Patol Oral Cir Bucal Aug 1;16 (5):e Article Number: Medicina Oral S. L. C.I.F. B pissn eissn: medicina@medicinaoral.com Indexed in: Science Citation Index Expanded Journal Citation Reports Index Medicus, MEDLINE, PubMed Scopus, Embase and Emcare Indice Médico Español Abstract Background: Dental primary implant stability is considered essential in the success of the osseointegration process. The recent advent of the resonance frequency analysis (RFA) seems to effectively measure primary implant stability, although its relationship with implant survival has to be further established. Patients and Methods: Seventy patients with complete mandibular edentulism underwent dental implant rehabilitation by means of the placement of 68 dental implants within the interforaminal region and subsequent placement of an overdenture. Primary implant stability was measured by means of RFA and it was expressed in terms of implant stability quotient (ISQ) on the day of the implant insertion and at the time of the healing abutment placement in a conventional implant two-stage surgical procedure. Results: Overall implant survival rate was 97.1% at the end of the follow-up period. The mean ISQ value for 3.75 and 4.25 mm diameter implants was 78.4 ± 5.46 and ± 5.35 respectively, at the time of the implant placement; and ± 4.34 and ± 6.87 respectively, at the second surgical stage. No statistical differences were observed in relation to changes in mean ISQ value along the healing process. Conclusions: No statistical differences in terms of primary and secondary implant stability measured by RFA exists between 3.75 mm and 4.25 mm diameter implants in the conventional implant two-stage surgical procedure in patients with non-atrophied edentulous mandible being restored with an overdenture. Furthermore, no statistical association between RFA and the implant insertion torque was observed for endosseous dental implant placement at the first surgical stage. Key words: Resonance frequency analysis, endosseous dental implants, anterior mandible, implant survival, primary and secondary implant stability. e664
2 Introduction The use of endosseous dental implants is a very popular alternative for oral rehabilitation, since the introduction of the osseointegration concept by Brånemark in Successful result of the implant insertion procedure depends on factors related to the patient and also to the procedure, including general health status, bio-compatibility of the implanted material, micro- and macroscopic nature of the implant surface, surgical procedure, and quality and quantity of local bone. It is considered that primary implant stability plays a major role in the success of osseointegration (1). It depends on the quality and quantity of bone, the geometry of the implant and the technique for preparation of the implant site (2). Volume and quality of bone are important factors for determining the surgical procedure and the choice of the implant, and are related to the success of implant surgery (3). The resonance frequency analysis (RFA) technique measures implant stability as a function of the complex bone-implant rigidity. Resonance frequency (measured in Hz) is established by the value of the implant stability quotient (ISQ). Implant stability is typically measured between 45 and 85 ISQ, and is mostly determined by bone density at the implant site. RFA has been previously reported to be effective in the detection of implant failure and in the checking of the healing process (4,5). Furthermore, it has been reported the importance of cortical bone in the determination of primary stability, with a positive correlation between RFA and the height of cortical bone in experimental studies with animals (6). Correlation in the patient alive has been studied less extensively. Based upon these previous considerations, the present study analyzes the correlation between primary and secondary stability of endosseous dental implants placed over the anterior mandible of edentulous patients without bone atrophy, and also analyzes implant survival. It also analyzes the influence of the implant diameter in the determination of primary and secondary stability, and its correlation with RFA values. Materials and Methods Sixty-eight endosseous dental implants MG-Osseous (Mozo-Grau S.L, Valladolid, Spain) were used. They were self-screw type Brånemark implants with external hexagon and RBM surface. The object of the study was defined as the number of inserted implants. Two implant diameters 3.75 and 4.25 mm were used in relation to the width of the anterior alveolar crest. The timetable of the study was: 1) inclusion of patients undergoing implant placement due to the absence of teeth in the non-atrophied anterior mandible; 2) insertion of endosseous dental implants in the anterior mandible for an overdenture protocol; 3) measurement of ISQ values by RFA in the first surgical procedure and placement of tapping screws; 4) removal of tapping screws during the second surgical time, measurement of ISQ values and placement of healing abutments (Fig. 1. A,B,C); 5) evaluation of implant survival and statistical analysis of results. During the first surgical stage, drilling sequence was performed according to manufacturer s recommendations: 1) initial drill; 2) 2.0 mm diameter drill; 3) 3.0 mm diameter drill; 4) 3.3 mm diameter drill (last drill for 3.75 mm diameter implants); 5) 3.8 mm diameter drill (last drill for 4.25 mm diameter implants); and 6) drill Fig. 1A. Implant insertion at the first surgical stage. Fig. 1B. Placement of healing abutments at the second surgical stage. Fig. 1C. Panoramic radiography showing implant position at the immediate post-operative time following the first surgical stage. e665
3 for smoothing cortical bone (for both implant diameters). Drilling was applied at 1000 rpm, under abundant continuous internal irrigation. Implant insertion torques were 35, 40 and 45 Ncm, in different proportions. Patients inclusion criteria included: 1) complete mandibular edentulism, with adequate preservation of the alveolar mandibular height and width; 2) placement of endosseous dental implants for overdenture fixation in non-atrophied anterior mandible; 3) absence of systemic pathology; 4) absence of smoking habit. Implants were placed following the conventional technique in two steps, with insertion during the first surgical stage and placement of the healing abutments during the second surgical stage, at least 3 months later. RFA was measured by the Ostell Mentor (Integrations Diagnostics AB, Savedalen, Sweden) instrument (7) and quantification was performed by the ISQ value. Measurements were taken twice in the anterior-posterior and lateralmedial vectors during first and second surgical stages. Prosthetic rehabilitation consisted on the placement of a mandibular overdenture option SD-4, with implants in positions A, B, D and E, rigidly fixed with a 10-mm distal cantilevered bar. Statistical package SPSS 13.0 (SPSS Inc., Chicago, IL, US) was used to analyze data. Descriptive statistical analysis for continuous and categorical variables was performed. Student s t test for paired samples was used to compare mean ISQ values between first and second surgical stage. In an attempt to analyze the influence of implant diameter in primary and secondary implant stability measured by RFA, 3.75 mm diameter implants were compared with 4.25 mm diameter implants by the Student s t test for unpaired samples. P value.05 was considered statistically significant. Results Mean age of the whole series was ± 9.71 years. Sixty-eight endosseous dental implants were placed, with an equal distribution among genders (50% placed in male patients and 50% placed in female patients). Fifty 3.75 mm diameter implants (73.5%) and eighteen 4.25 mm diameter implants (26.5%) were inserted. Overall implant success rate was 97.1% at the end of the followup period, with failure of 2 implants, 3.75 and 4.25 mm diameter each. In these cases, a decrease upper than 10 ISQ points was observed in RFA between first and second surgical stages for both implant sizes. Mean insertion torque for the whole series was ± 3.39 Ncm, with 39 (57.4%) implants inserted at 35 Ncm, 22 (32.4%) at 40 Ncm, and 7 (10.3%) at 45 Ncm. Mean ISQ value obtained by the RFA during implant insertion stage was ± 5.50, while mean ISQ value at the second surgical stage for healing abutments connection was ± Mean time between both surgical stages was ± days (range: days). In relation to bone features according to the Lekholm & Zarb classification, bone type I was observed in 78.6% of the inserted implants, bone type II in 14.3%, bone type III in 5.4%, and bone type IV in 1.8%. Considering scores 1 to 4 for bone types I to IV respectively, mean value of the series in relation to bone type was 1.30 ± In the analytic study, significant statistical differences in relation to AFR mean values between the first and second surgical stage were encountered (p=0.031). Mean ISQ value for 3.75 mm diameter implants at the first surgical stage was ± 5.46, and decreased to ± 4.34 at the second surgical stage (measured ± days post-surgery). Mean ISQ value for 4.25 mm diameter implants at the first surgical stage was ± 5.35, and decreased to ± 6.87 at the second surgical stage (measured ± days post-surgery). Following the application of the Student s t test for unpaired data, no significant differences were observed between implant diameters 3.75 mm and 4.25 mm, in relation to primary and secondary implant stability measured by RFA (p=0.11 and p=0.38, respectively). No statistically significant association was either observed between insertion torques and ISQ values during implant insertion at first and second surgical stages. No statistically significant association was either observed between sex and age and ISQ values at the first and second surgical stages. Due to the scarce number of failed implants, and the fact that these implants were of both diameters, analyses of the influence of the ISQ value in the implant success rate was inapplicable, and no parameter was compared with such variable. Although in the present study, both failed implants showed a decrease in ISQ values of 10 and 12 points respectively, a difference equal or major than 10 points between final ISQ value and initial ISQ value did not showed a statistically significant association with implant success rate. Furthermore, 13 (19.11%) endosseous dental implants showed differences equal or major than 10 points between final ISQ value and initial ISQ value, without an observed failure of the osseointegration process in 11 of 13 (84.61%) implants. Discussion The presence of significant higher ISQ values in the anterior site of the mandible than in the posterior site has been previously reported in the literature (8). The width of the implant has also been reported to be an important factor in relation to supported prosthetic loads. As far as the implant is wider, the more decrease of loads is observed due to an increase of the implant surface, as well as the implant length can be decreased. In fact, width has been reported to be more relevant than length, as highest loads concentrate in the coronal zone (7). The fact that each 0.5 mm of implant width increase corres- e666
4 ponds with an increase of 10% to 15% of the implant surface, lead us to study the influence of two implant diameters: 3.75 and 4.25 mm (differing each other 0.5 mm exactly) in the implant stability, measured primarily and secondarily by RFA. In the present study, no significant statistical differences in terms of primary and secondary implant stability were observed between both diameters, although bone type D4 in the Misch classification (7) has been reported to more commonly require wider implants, in contrast to those required by bone type D1 and D2. This disagreement may be attributable to the preponderance of implants over cortical bone in the present series, corresponding to subtypes 1 and 2 of the Lekholm & Zarb classification. In a study about 48 inserted implants in cadaver by Nkenke et al. (9), RFA and histo-morphometric study was performed for every implant. Several items were analyzed: 1) bone-implant contact; 2) trabecular pattern factor (TBPf): it measures the degree of inter-trabecular connectivity, which increases as TBPf decreases; 3) trabecular bone density (bone volume/total volume, BV/TV); and 4) cortical bone height trespassed by the implant. Mean values by RFA (maxilla ± Hz, mandible ± Hz) did not correlate with bone mineral density (maxilla ± mg/cm 3, mandible ± mg/cm 3 ), with BV/TV (maxilla 19.7 ± 8.8%, mandible 34.3 ± 6.0%), and neither with TNPf (maxilla 2.39 ± 1.46 mm-1, mandible ± 3.27 mm-1). However, the authors found a correlation between RFA and bone-implant contact (maxilla 12.6 ± 6.0%, mandible 35.1 ± 5.1%) and between RFA and cortical bone height trespassed by implants (maxilla 2.1 ± 0.7 mm, mandible 5.1 ± 3.7 mm). They concluded that non-invasive measurement of implant stability by RFA had to be improved to allow a more comprehensive prediction of implant site features. In the present series, inclusion of patients without mandibular atrophy is evident by the presence of bone with a mean value of 1.30 ± 0.65 in the Lekholm & Zarb classification, and the fact that 78.6% of the implants were inserted in bone type 1, 14.3% in bone type 2, while only 7.2% in bone types 3 and 4. These results differ slightly from those observed by Misch (7), who reported a distribution of 6%, 66%, 25% and 3% for bone densities D1, D2, D3, and D4, respectively, in the anterior mandible. The presence of a high rate of patients with abundant cortical bone in our series may explain the relative high mean values in the RFA measured in the first and second surgical stages: and 77.09, respectively. In fact, we wanted to test the reported implants only in a selected group of patients with mandibular edentulism without atrophy in the anterior site. Otherwise, this issue can be determinant in the observed high implant success rate. Mean ISQ value at the implant insertion was higher than that for global series (10), which indicates the predictability in terms of primary stability placed in the non-atrophied anterior mandible. Huwiler et al. (11), in a series of 17 implants placed in the patient alive, observed a normal ISQ range between 55 and 74 at the time of implant insertion. They also observed an increase in ISQ values during the week following implant insertion, followed by a decrease during weeks 2 to 4, and a posterior increase to ISQ values obtained during the insertion phase, or even higher. Loss of implant stability occurring one week after implant insertion can be attributable to loss of mechanical stability identified during the early healing period, which has been previously described by Abrahamsson et al. (12). Otherwise, the osseointegration phase by contact osseogenesis, previously documented in animal studies after 2-4 weeks, is represented by the slight increase of ISQ values observed during the late phase of the healing process, from the fourth week. Based on the failure of an implant, which lost stability after 3 weeks with an important decrease of 20 ISQ units, from 68 to 45 in a week, authors conclude that RFA is a specific but not sensitive biomechanic test of implant stability, without predictive value for implant failure, as far as the observed low ISQ value was found once the implant had already lost stability, and also the ISQ value of 45 was marginal and no significant difference was observed with respect to ISQ range of the rest of the series. Interestingly, these results are quite similar to those obtained in the present study, as we could not demonstrate a statistically significant association between loss of ISQ units and failure of implant osseointegration. In fact, an 84.61% of the implants loosing 10 or more ISQ points showed successful osseointegration despite decrease of implant stability values, in contrast to 15.39% that did not osseointegrate. Because of the design of the study and due to the fact that it was performed in patients alive, it was impossible to serially evaluate the evolution of post-operative ISQ values along the weeks that followed implant insertion, and thus final ISQ measurement was performed at the second surgical stage during the placement of healing abutments. Abrahamsson et al. (12), in animal studies, report a gradually increase in ISQ values after an initial decrease, from the 4 th week following implant insertion. The evaluation of mean RFA at the 16 th week (range 12 to 27 weeks) performed in our study showed a decrease of mean ISQ value up to 1.95 units, which was significantly different, although it did not have any clinical influence, as implant osseointegration did not change. Correlation of ISQ values decrease at the 16 th week with bone morphogenesis at the bone-implant interface must be analyzed further in future studies, although high initial ISQ values and the presence of bone type 1 and 2 in a large number of patients could explain results observed in the present study. RFA has showed an important sensibility in monitoring e667
5 implant stability changes. Friberg et al. (1) showed an increase of implant stability for implants in the upper maxilla from insertion to the second surgical stage at the placement of healing abutments, and further increase one year later to the prosthetic load. In a clinical study with bone graft in the maxilla, Rasmusson et al. (13) reported an increase in ISQ values along the time, and recommended the use of small diameter drills for implant insertion, in order to generate high compression forces that allow higher stability, at least initially. Similarly, Glauser et al. (14), in a study using RFA in 81 dental implants for a year, observed a continuous decrease of implant stability that finally failed. They concluded that low ISQ values after 1 to 2 months seem to indicate a higher risk for a future implant failure. This information can be useful to avoid a potential implant failure, unloading implants with a decreasing implant stability diagnosed by RFA. In our series, implant stability in the moment of the healing abutment connection was slightly lower, although final ISQ values were in the rank of implant success previously reported in the literature. Kessler-Liechti et al. (15), in a study over 205 implants, observed a mean ISQ of 64.5 for interforaminal implants that were asymptomatic at any time of the follow-up. These authors, however, did not observe any significant differences in terms of ISQ values at different post-surgical times. Among three methods for the evaluation of implant stability (RFA, Periotest and insertion torque), only RFA has been correlated to bone-implant contact in experimental studies with animals (6,16). However, in the study over maxilla and mandible of human cadaver this correlation was less pronounced, probably because properties of human mandible and maxilla change rapidly in a short period of time. In relation to these results, we did not find a statistically significant association between RFA and insertion torque at the non-atrophied edentulous interforaminal mandible. Two aspects not evaluated in the present study seem to play a major role in the determination of implant stability: bone-implant contact surface and height of alveolar cortical bone. In fact, previous studies have correlated RFA with height of the alveolar cortical bone. Also, recent bibliography in relation to implant failure evaluate peri-implantitis as the loss of vertical bone around an implant more than 4 mm during the first year, and 1.5 mm each following year (16-18). Design of prospective studies that acutely evaluate these parameters may provide important information about the ability to predict implant survival in relation to primary and secondary stability, influenced by bone density, height of alveolar cortical bone and bone-implant contact surface. Conclusions In the present series of edentulous patients with nonatrophied mandible restored by an overdenture, the resonance frequency analysis at the 16 th week from the endosseous dental implant insertion showed a significant decrease of 2 ISQ units, although no significant differences in terms of primary and secondary implant stability among 3.75 and 4.25 mm diameter implants were encountered in the traditional two-step implant rehabilitation procedure. Otherwise, no statistical association between the resonance frequency analysis and the implant insertion torque value at the first surgical stage was encountered. References with links to Crossref - DOI References 1. Friberg B, Jemt T, Lekholm U. Early failures in 4,641 consecutively placed Brånemark dental implants: a study from stage 1 surgery to the connection of completed prostheses. Int J Oral Maxillofac Implants. 1991;6: Sennerby L, Roos J. Surgical determinants of clinical success of osseointegrated oral implants: a review of the literature. Int J Prosthodont. 1998;11: Ekfeldt A, Christiansson U, Eriksson T, Lindén U, Lundqvist S, Rundcrantz T, et al. A retrospective analysis of factors associated with multiple implant failures in maxillae. Clin Oral Implants Res. 2001;12: Sennerby L, Persson LG, Berglundh T, Wennerberg A, Lindhe J. Implant stability during initiation and resolution of experimental periimplantitis: an experimental study in the dog. Clin Implant Dent Relat Res. 2005;7: Brouwers JE, Lobbezoo F, Visscher CM, Wismeijer D, Naeije M. Reliability and validity of the instrumental assessment of implant stability in dry human mandibles. J Oral Rehabil. 2009;36: Meredith N, Book K, Friberg B, Jemt T, Sennerby L. Resonance frequency measurements of implant stability in vivo. A cross-sectional and longitudinal study of resonance frequency measurements on implants in the edentulous and partially dentate maxilla. Clin Oral Implants Res. 1997;8: Capek L, Simunek A, Slezak R, Dzan L. Influence of the orientation of the Osstell transducer during measurement of dental implant stability using resonance frequency analysis: a numerical approach. Med Eng Phys. 2009;31: Boronat López A, Balaguer Martínez J, Lamas Pelayo J, Carrillo García C, Peñarrocha Diago M. Resonance frequency analysis of dental implant stability during the healing period. Med Oral Patol Oral Cir Bucal. 2008;13:E Nkenke E, Hahn M, Lell M, Wiltfang J, Schultze-Mosgau S, Stech B, et al. Anatomic site evaluation of the zygomatic bone for dental implant placement. Clin Oral Implants Res. 2003;14: Boronat-López A, Peñarrocha-Diago M, Martínez-Cortissoz O, Mínguez-Martínez I. Resonance frequency analysis after the placement of 133 dental implants. Med Oral Patol Oral Cir Bucal. 2006;11:E Huwiler MA, Pjetursson BE, Bosshardt DD, Salvi GE, Lang NP. Resonance frequency analysis in relation to jawbone characteristics and during early healing of implant installation. Clin Oral Implants Res. 2007;18: Abrahamsson I, Berglundh T, Linder E, Lang NP, Lindhe J. Early bone formation adjacent to rough and turned endosseous implant surfaces. An experimental study in the dog. Clin Oral Implants Res. 2004;15: Rasmusson L, Meredith N, Cho IH, Sennerby L. The influence of simultaneous versus delayed placement on the stability of titanium implants in onlay bone grafts. A histologic and biomechanic study in the rabbit. Int J Oral Maxillofac Surg. 1999;28: e668
6 14. Glauser R, Sennerby L, Meredith N, Rée A, Lundgren A, Gottlow J, et al. Resonance frequency analysis of implants subjected to immediate or early functional occlusal loading. Successful vs. failing implants. Clin Oral Implants Res. 2004;15: Kessler-Liechti G, Zix J, Mericske-Stern R. Stability measurements of 1-stage implants in the edentulous mandible by means of resonance frequency analysis. Int J Oral Maxillofac Implants. 2008;23: Huang HM, Lee SY, Yeh CY, Lin CT. Resonance frequency assessment of dental implant stability with various bone qualities: a numerical approach. Clin Oral Implants Res. 2002;13: Ko CC, Douglas WH, DeLong R, Rohrer MD, Swift JQ, Hodges JS, et al. Effects of implant healing time on crestal bone loss of a controlled-load dental implant. J Dent Res. 2003;82: Huang HM, Tsai CM, Chang CC, Lin CT, Lee SY. Evaluation of loading conditions on fatigue-failed implants by fracture surface analysis. Int J Oral Maxillofac Implants. 2005;20: e669
P rimary or mechanical implant
 IMPLANT DENTISTRY / VOLUME 0, NUMBER 0 2013 1 Effect of Location on Primary Stability and Healing of Dental Implants Alberto Monje, DDS,* Fernando Suarez, DDS,* Carlos Andrés Garaicoa, DDS, Florencio Monje,
IMPLANT DENTISTRY / VOLUME 0, NUMBER 0 2013 1 Effect of Location on Primary Stability and Healing of Dental Implants Alberto Monje, DDS,* Fernando Suarez, DDS,* Carlos Andrés Garaicoa, DDS, Florencio Monje,
Comparison of implant primary stability between maxillary edentulous ridges receiving intramembranous origin block grafts
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.18732 http://dx.doi.org/doi:10.4317/medoral.18732 Comparison of implant primary stability between maxillary edentulous ridges
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.18732 http://dx.doi.org/doi:10.4317/medoral.18732 Comparison of implant primary stability between maxillary edentulous ridges
Hiron Andreaza da Cunha, MS 1 /Carlos Eduardo Francischone, DMD 2 /Hugo Nary Filho, DDS 3 / Rubelisa Cândido Gomes de Oliveira, BDS 4
 A Comparison Between Cutting Torque and Resonance Frequency in the Assessment of Primary Stability and Final Torque Capacity of and TiUnite Single-Tooth Implants Under Immediate Loading Hiron Andreaza
A Comparison Between Cutting Torque and Resonance Frequency in the Assessment of Primary Stability and Final Torque Capacity of and TiUnite Single-Tooth Implants Under Immediate Loading Hiron Andreaza
Narrow-diameter implants in premolar and molar areas
 2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
2 Long-term follow-up of 2.5mm NDIs supporting a fixed prosthesis Narrow-diameter implants in premolar and molar areas EDUARDO ANITUA, DDS, MD, PHD¹,² A narrow-diameter implant (NDI) is an implant with
Endosseous dental implants initially showed very
 Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Five-mm-Diameter Implants without a Smooth Surface Collar: Report on 98 Consecutive Placements Franck Renouard, DDS*/Jean-Pierre Arnoux, DDS**/David P. Sarment, DDS*** In recent years, indications for
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. Department of Periodontology, School of Dental Medicine, University of Bern,
Resonance frequency analysis-reliability in third generation instruments: Osstell mentor
 Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.17861 http://dx.doi.org/doi:10.4317/medoral.17861 Resonance frequency analysis-reliability in third generation instruments:
Journal section: Periodontology Publication Types: Research doi:10.4317/medoral.17861 http://dx.doi.org/doi:10.4317/medoral.17861 Resonance frequency analysis-reliability in third generation instruments:
Etiology, risk factors and management of implant fractures
 Journal section: Oral Surgery Publication Types: Review doi:10.4317/medoral.15.e504 Etiology, risk factors and management of implant fractures Arturo Sánchez-Pérez 1, Mª José Moya-Villaescusa 1, Alfonso
Journal section: Oral Surgery Publication Types: Review doi:10.4317/medoral.15.e504 Etiology, risk factors and management of implant fractures Arturo Sánchez-Pérez 1, Mª José Moya-Villaescusa 1, Alfonso
It is of interest to develop and evaluate
 RESEARCH Validation of Resonance Frequency Analysis by Comparing Implant Stability Quotient Values With Histomorphometric Data Ashish Thomas Kunnekel, MDS 1 * K. Chandrasekharan Nair, MDS 2 E. Munirathnam
RESEARCH Validation of Resonance Frequency Analysis by Comparing Implant Stability Quotient Values With Histomorphometric Data Ashish Thomas Kunnekel, MDS 1 * K. Chandrasekharan Nair, MDS 2 E. Munirathnam
Osseointegrated dental implant treatment generally
 Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Placement of Dental Implants Without Flap Surgery: A Clinical Report Bader H. Al-Ansari, BDS, MScD*/Robert R. Morris, DMD** Traditionally, the procedure of implant placement requires a surgical periosteal
Case study 2. A Retrospective Multi-Center Study on the Spiral Implant
 Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Case study 2 A Retrospective Multi-Center Study on the Spiral Implant Benny Karmon DMD, Jerry Kohen DMD, Ariel Lor DMD, Yiftach Gratciany DMD, Zvi Laster DMD, Gideon Hallel DMD MPA, Tsvia Karmon A Retrospective
Dental Research Journal
 Dental Research Journal Original Article The effect of shape, length and diameter of implants on primary stability based on resonance frequency analysis Hamidreza Barikani, Shadab Rashtak, Soolmaz Akbari,
Dental Research Journal Original Article The effect of shape, length and diameter of implants on primary stability based on resonance frequency analysis Hamidreza Barikani, Shadab Rashtak, Soolmaz Akbari,
The Brånemark osseointegration method, using titanium dental implants (fixtures)
 Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
Early Failures in 4,641 Consecutively Placed Brånemark Dental Implants: A Study From Stage 1 Surgery to the Connection of Completed Prostheses Bertil Friberg, DDS/Torsten Jemt, DDS, PhD/Ulf Lekholm, DDS,
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel
 PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
PALATAL POSITIONING OF IMPLANTS IN SEVERELY RESORBED POSTERIOR MAXILLAE F. Atamni, M.Atamni, M.Atamna, Private Practice Tel-aviv Israel Abstract: Objectives: To evaluate an alternative treatment for rehabilitation
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis.
 Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. Atieh MA, Ibrahim HM, Atieh AH. J Periodontol. 2010 Oct;81(10):1350-66. BACKGROUND: Platform
Immediately restored dental implants for partial-arch applications. A literature update
 Immediately restored dental for partialarch applications. A literature update Celia Carrillo García 1, Araceli Boronat López 1, Miguel Peñarrocha Diago 2 (1) Master of Oral Surgery and Implantology (2)
Immediately restored dental for partialarch applications. A literature update Celia Carrillo García 1, Araceli Boronat López 1, Miguel Peñarrocha Diago 2 (1) Master of Oral Surgery and Implantology (2)
Resonance Frequency Analysis Measurements of Implants at Placement Surgery
 Resonance Frequency Analysis Measurements of Implants at Placement Surgery Pär-Olov Östman, DDS a /Mats Hellman, DDS a /Inger Wendelhag, PhD b /Lars Sennerby, DDS, PhD c Purpose: The knowledge of what
Resonance Frequency Analysis Measurements of Implants at Placement Surgery Pär-Olov Östman, DDS a /Mats Hellman, DDS a /Inger Wendelhag, PhD b /Lars Sennerby, DDS, PhD c Purpose: The knowledge of what
Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent
 Journal section: Oral Surgery Publication Types: Research doi:0.7/medoral..e Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent Oscar Arias-Irimia, Cristina Barona-Dorado,
Journal section: Oral Surgery Publication Types: Research doi:0.7/medoral..e Pre-operative evaluation of the volume of bone graft in sinus lifts by means of CompuDent Oscar Arias-Irimia, Cristina Barona-Dorado,
BIOMECHANICS AND OVERDENTURES
 Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Proceedings of the 6th International Conference on Mechanics and Materials in Design, Editors: J.F. Silva Gomes & S.A. Meguid, P.Delgada/Azores, 26-30 July 2015 PAPER REF: 5734 BIOMECHANICS AND OVERDENTURES
Young-Jin Park, DDS,* and Sung-Am Cho, DDS, MS, PhD
 J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
J Oral Maxillofac Surg 68:1338-1344, 2010 Retrospective Chart Analysis on Survival Rate of Fixtures Installed at the Tuberosity Bone for Cases With Missing Unilateral Upper Molars: A Study of 7 Cases Young-Jin
A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2011.3.4.190 A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis In-Ho Kang,
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2011.3.4.190 A comparative study on the initial stability of different implants placed above the bone level using resonance frequency analysis In-Ho Kang,
Enhancing implant stability with osseodensification a case report with 2-year follow-up
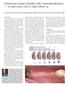 Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
Enhancing implant stability with osseodensification a case report with 2-year follow-up Dr. Salah Huwais discusses how osseodensification facilitates ridge expansion with enhanced implant stability Introduction
EFFECT OF IMPLANT DESIGN ON INITIAL STABILITY
 CLINICAL EFFECT OF IMPLANT DESIGN ON INITIAL STABILITY OF TAPERED IMPLANTS Linus Chong, DDS, MS; Ahmed Khocht, DDS, MSD; Jon B. Suzuki, DDS, PhD; John Gaughan, PhD Implant design is one of the parameters
CLINICAL EFFECT OF IMPLANT DESIGN ON INITIAL STABILITY OF TAPERED IMPLANTS Linus Chong, DDS, MS; Ahmed Khocht, DDS, MSD; Jon B. Suzuki, DDS, PhD; John Gaughan, PhD Implant design is one of the parameters
The International Journal of Periodontics & Restorative Dentistry
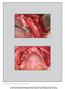 The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
The International Journal of Periodontics & Restorative Dentistry 141 Screw Spreading: Technical Considerations and Case Report Renato Sussumu Nishioka, DDS, PhD, MSc* Alberto Noriyuki Kojima, DDS, PhD,
During the last 30 years, endosseous oral
 Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
Influence of Variations in Implant Diameters: A 3- to 5-Year Retrospective Clinical Report Carl-Johan Ivanoff, DDS*/Kerstin Gröndahl, DDS, PhD**/Lars Sennerby, DDS, PhD***/ Christina Bergström, MSc****/Ulf
The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges
 Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Case Study 48 The Use of Alpha-Bio Tec's Narrow NeO Implants with Cone Connection for Restoration of Limited Width Ridges Dr. Amir Gazmawe DMD, Specialist in Prosthodontics, Israel Dr. Amir Gazmawe graduated
Harsukh Educational Charitable Society International Journal of Community Health and Medical Research
 Harsukh Educational Charitable Society International Journal of Community Health and Medical Research Journal home page:www.ijchmr.com doi: 10.21276/ijchmr ISSN E: 2457-0117 ISSN P:2581-5040 Index Copernicus
Harsukh Educational Charitable Society International Journal of Community Health and Medical Research Journal home page:www.ijchmr.com doi: 10.21276/ijchmr ISSN E: 2457-0117 ISSN P:2581-5040 Index Copernicus
DEVELOPMENT OF PREDICTABLE STABILITY TEST FOR ASSESSMENT OF OPTIMUM LOADING TIME IN DENTAL IMPLANT
 ORIGINAL ARTICLE DOI:10.4047/jkap.2008.46.6.628 DEVELOPMENT OF PREDICTABLE STABILITY TEST FOR ASSESSMENT OF OPTIMUM LOADING TIME IN DENTAL IMPLANT Seong-Kyun Kim 1, DDS, PhD, Seong-Joo Heo 2, DDS, PhD,
ORIGINAL ARTICLE DOI:10.4047/jkap.2008.46.6.628 DEVELOPMENT OF PREDICTABLE STABILITY TEST FOR ASSESSMENT OF OPTIMUM LOADING TIME IN DENTAL IMPLANT Seong-Kyun Kim 1, DDS, PhD, Seong-Joo Heo 2, DDS, PhD,
Annals of Dental Research
 P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
P a g e 1 ADR 7 (1), 1-6, 2017 Journal Homepage: www.hgpub.com/ojs2/index.php/adr Direct Sinus Lift with Putty Alloplastic Bone Substitute for Simultaneous Implant Placement A Case Report Chander Prakash*,
A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE
 J Korean Acad Prosthodont : Volume 44, Number 3, 2006 A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE Jong-Hyuk Lee 1,2, D.D.S., M.S.D., Jae-Ho Yang 1, D.D.S.,
J Korean Acad Prosthodont : Volume 44, Number 3, 2006 A STUDY ON THE CORRELATION BETWEEN IMPLANT STABILITY VALUES AND INITIAL INSERTION TORQUE Jong-Hyuk Lee 1,2, D.D.S., M.S.D., Jae-Ho Yang 1, D.D.S.,
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Prosthetic Options in Implant Dentistry. Hakimeh Siadat, DDS, MSc Associate Professor
 Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Prosthetic Options in Dentistry Hakimeh Siadat, DDS, MSc Associate Professor Dental Research Center, Department of Prosthodontics & Dental s Faculty of Dentistry, Tehran University of Medical Sciences
Influence of the prosthetic arm length (palatal position) of zygomatic implants upon patient satisfaction
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21033 http://dx.doi.org/doi:10.4317/medoral.21033 Influence of the prosthetic arm length (palatal position) of zygomatic implants
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21033 http://dx.doi.org/doi:10.4317/medoral.21033 Influence of the prosthetic arm length (palatal position) of zygomatic implants
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Local alveolar bone quality and quantity,
 RESEARCH Use of Osteotomes for Implant Bed Preparation Effect on Material Properties of Bone and Primary Implant Stability Tim Krafft, PD Dr Dr Friedrich Graef, Dr Werner Winter, Dr-Ing Manfred Wichmann,
RESEARCH Use of Osteotomes for Implant Bed Preparation Effect on Material Properties of Bone and Primary Implant Stability Tim Krafft, PD Dr Dr Friedrich Graef, Dr Werner Winter, Dr-Ing Manfred Wichmann,
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
ABSTRACT INTRODUCTION
 ABSTRACT Purpose: Evaluation of stress distribution maxilla under parafunctional loading on short dental implant using 3-dimensional (3D) finite element models. Material and method: 3D maxillary and mandibular
ABSTRACT Purpose: Evaluation of stress distribution maxilla under parafunctional loading on short dental implant using 3-dimensional (3D) finite element models. Material and method: 3D maxillary and mandibular
In vitro comparison of primary stability of two implant designs in D3 bone
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21714 http://dx.doi.org/doi:10.4317/medoral.21714 In vitro comparison of primary stability of two implant designs in D3 bone
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.21714 http://dx.doi.org/doi:10.4317/medoral.21714 In vitro comparison of primary stability of two implant designs in D3 bone
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae
 Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
Survival Analysis of Endosseous Implants in Grafted and Nongrafted Edentulous Maxillae Jonas P. Becktor, DDS 1 /Sten Isaksson, MD, DDS, PhD 2 /Lars Sennerby, DDS, PhD 3 Purpose: The aim of this study was
The influence of platform switching on the biomechanical aspects of the implant-abutment system. A three dimensional finite element study
 Journal section: Biomaterials and bioengineering in dentistry Publication Types: Research doi:10.4317/medoral.17243 http://dx.doi.org/doi:10.4317/medoral.17243 The influence of platform switching on the
Journal section: Biomaterials and bioengineering in dentistry Publication Types: Research doi:10.4317/medoral.17243 http://dx.doi.org/doi:10.4317/medoral.17243 The influence of platform switching on the
G03: Complications 12/7/2013 8:00AM 4:30PM
 American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
American Association of Oral and Maxillofacial Surgeons 2013 Dental Implant Conference December 5 7, 2013 Sheraton Chicago Hotel & Towers G03: Complications 12/7/2013 8:00AM 4:30PM Prosthetic Complications
Implant stability, whether immediately following surgery
 RESEARCH The Evaluation of the Reliability of Periotest for Implant Stability s: An In Vitro Study Hakan Bilhan, PhD, DDS 1 Altug Cilingir, PhD, DDS 2 Canan Bural, PhD, DDS 3 Caglar Bilmenoglu, PhD, DDS
RESEARCH The Evaluation of the Reliability of Periotest for Implant Stability s: An In Vitro Study Hakan Bilhan, PhD, DDS 1 Altug Cilingir, PhD, DDS 2 Canan Bural, PhD, DDS 3 Caglar Bilmenoglu, PhD, DDS
Retreatment: Fractured Implants Due To Biomechanical Overload
 Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Glenn J. Wolfinger, DMD, FACP Retreatment: Fractured Implants Due To Biomechanical Overload Thomas J. Balshi, DDS, FACP he strength of osseointegration, T the biologic and biomechanical union of bone to
Implant osseointegration and successful restoration
 Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Prosthodontic Complications in a Prospective Clinical Trial of Single-stage Implants at 36 Months Jacqueline P. Duncan, DMD, MDSc 1 /Elena Nazarova, DMD, PhD 2 /Theodora Vogiatzi, DDS 1 / Thomas D. Taylor,
Brånemark System Facts & Figures
 Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
Brånemark System Facts & Figures Brånemark System is synonymous with the revolution in dental care by the introduction of safe and effective implants. Professor Brånemark, its inventor, always put the
The surgical placement of dental implants has
 Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
Flapless Implant Surgery: A 10-year Clinical Retrospective Analysis Luis Dominguez Campelo, DDS 1 /Jose R. Dominguez Camara, MD, DDS 2 Purpose: This article is a retrospective clinical analysis of implants
The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study
 26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
26 News No.26 January 2011 The Use Of 6mm Long Implants In Cases With Limited Bone Height: A Preliminary 6-Month Clinical Study Make it Simple 2 The Use Of 6mm Long Implants In Cases With Limited Bone
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation
 The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
The Self-tapping and ICE 3i Implants: A Prospective 3-Year Multicenter Evaluation Mithridade Davarpanah, MD, DDS 1 /Henry Martinez, DDS 2 /Jean-François Tecucianu, MD, DDS 3 / Gil Alcoforado, DDS 4 /Daniel
Architecture and microenvironment
 RESEARCH Comparison of Delayed Implant Placement vs Immediate Implant Placement Using Resonance Frequency Analysis: A Pilot Study on Rabbits Ashish T. Kunnekel, MDS 1 * Mohit T. Dudani, MDS 2 Chandrasekharan
RESEARCH Comparison of Delayed Implant Placement vs Immediate Implant Placement Using Resonance Frequency Analysis: A Pilot Study on Rabbits Ashish T. Kunnekel, MDS 1 * Mohit T. Dudani, MDS 2 Chandrasekharan
Ilser Turkyilmaz Lars Sennerby Celal Tumer Muhittin Yenigul Mehmet Avci
 Ilser Turkyilmaz Lars Sennerby Celal Tumer Muhittin Yenigul Mehmet Avci Stability and marginal bone level measurements of unsplinted implants used for mandibular overdentures: a 1-year randomized prospective
Ilser Turkyilmaz Lars Sennerby Celal Tumer Muhittin Yenigul Mehmet Avci Stability and marginal bone level measurements of unsplinted implants used for mandibular overdentures: a 1-year randomized prospective
Implant stability is considered one of the most important
 Development of Implant Stability During Early Healing of Immediately Loaded Implants Antonin Simunek, MD, PhD 1 /Dana Kopecka, MD, PhD 2 /Tomas Brazda, MD 2 / Jakub Strnad, PhD 3 /Lukas Capek, PhD 4 /Radovan
Development of Implant Stability During Early Healing of Immediately Loaded Implants Antonin Simunek, MD, PhD 1 /Dana Kopecka, MD, PhD 2 /Tomas Brazda, MD 2 / Jakub Strnad, PhD 3 /Lukas Capek, PhD 4 /Radovan
Comparison of Implant Stability Using Resonance Frequency Analysis: Osteotome Versus Conventional Drilling
 Original Article Comparison of Implant Stability Using Resonance Frequency Analysis: Osteotome Versus Conventional Drilling Rokhsareh Sadeghi 1, Amir Reza Rokn 2, Asghar Miremadi 3 1 Assistant Professor,
Original Article Comparison of Implant Stability Using Resonance Frequency Analysis: Osteotome Versus Conventional Drilling Rokhsareh Sadeghi 1, Amir Reza Rokn 2, Asghar Miremadi 3 1 Assistant Professor,
scientific compendium
 scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
scientific compendium Zimmer Tapered Screw-Vent Implant Success Stories in Stability and Survival Rates Zimmer Tapered Screw-Vent Implant Scientific Compendium table of contents CLINICAL & PRE-CLINICAL
Resonance Frequency Measurement of Implant Stability In Vivo on Implants with a Sandblasted and Acid-Etched Surface
 Resonance Frequency Measurement of Implant Stability In Vivo on Implants with a Sandblasted and Acid-Etched Surface Reva M. Barewal, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 /Neil Meredith, BDS, MSc, PhD
Resonance Frequency Measurement of Implant Stability In Vivo on Implants with a Sandblasted and Acid-Etched Surface Reva M. Barewal, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 /Neil Meredith, BDS, MSc, PhD
Areview of recent studies concerning molar. Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report
 Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
Single Molar Replacement with a Progressive Thread Design Implant System: A Retrospective Clinical Report George E. Romanos, Dr med dent 1 /Georg H. Nentwig, Prof Dr med dent 2 Many clinical studies have
There are many longitudinal investigations
 A 3-Arm Study of Early Loading of Rough-Surfaced Implants in the Completely Edentulous Maxilla and in the Edentulous Posterior Maxilla and Mandible: Results After 1 Year of Loading Thomas Nordin, DDS 1
A 3-Arm Study of Early Loading of Rough-Surfaced Implants in the Completely Edentulous Maxilla and in the Edentulous Posterior Maxilla and Mandible: Results After 1 Year of Loading Thomas Nordin, DDS 1
External Hexagon Hybrid Implants. External Hexagon Hybrid Implants. Versatility.
 External Hexagon Hybrid Implants Versatility. www.pibranemark.com HEX-S Solid Enhanced Macrogeometry Easy, Safe and Simplified installation (!). Special Conical Drills have the same geometry of Hybrid
External Hexagon Hybrid Implants Versatility. www.pibranemark.com HEX-S Solid Enhanced Macrogeometry Easy, Safe and Simplified installation (!). Special Conical Drills have the same geometry of Hybrid
NobelActive Inventor s perspective on this new direction for implants
 NobelActive Inventor s perspective on this new direction for implants Nobel Biocare launches a unique new implant with revolutionary features due to the advanced design of its implant body NobelActive.
NobelActive Inventor s perspective on this new direction for implants Nobel Biocare launches a unique new implant with revolutionary features due to the advanced design of its implant body NobelActive.
Radiological assessment of peri-implant bone loss: a 12-month retrospective study.
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.3.e430 Radiological assessment of peri-implant bone loss: a 12-month retrospective study. AJ. Flichy-Fernández 1, J. Ata-Ali 2,
Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.3.e430 Radiological assessment of peri-implant bone loss: a 12-month retrospective study. AJ. Flichy-Fernández 1, J. Ata-Ali 2,
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Immediate implant placement in the Title central incisor region: a case repo. Journal Journal of prosthodontic research,
 Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Immediate implant placement in the Title central incisor region: a case repo Author(s) Sekine, H; Taguchi, T; Yamagami, M; Alternative Takanashi, T; Furuya, K Journal Journal of prosthodontic research,
Implant treatment in patients with severely
 Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
Rehabilitation of Patients with Severely Resorbed Maxillae by Means of Implants With or Without Bone Grafts: A 3- to 5-Year Follow-up Clinical Report Göran Widmark, LDS, Odont Dr 1 /Bernt Andersson, LDS,
Components Of Implant Protective Occlusion A Review
 ISPUB.COM The Internet Journal of Dental Science Volume 7 Number 2 Components Of Implant Protective Occlusion A Review E Prashanti, K Sumanth, J Reddy Citation E Prashanti, K Sumanth, J Reddy. Components
ISPUB.COM The Internet Journal of Dental Science Volume 7 Number 2 Components Of Implant Protective Occlusion A Review E Prashanti, K Sumanth, J Reddy Citation E Prashanti, K Sumanth, J Reddy. Components
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note
 Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
Bone Reduction Surgical Guide for the Novum Implant Procedure: Technical Note Stephen M. Parel, DDS 1 /Steven L. Ruff, CDT 2 /R. Gilbert Triplett, DDS, PhD 3 /Sterling R. Schow, DMD 4 The Novum System
The use of endosseous implants is currently a routine
 Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
Evaluation of 31 Zygomatic Implants and 74 Regular Dental Implants Used in 16 Patients for Prosthetic Reconstruction of the Atrophic Maxilla with Cross-Arch Fixed Bridges Jonas P. Becktor, DDS;* Sten Isaksson,
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible
 A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
A Long-term Retrospective Analysis of Survival Rates of Implants in the Mandible Thomas J. Balshi, DDS, PhD, FACP 1 /Glenn J. Wolfinger, DMD, FACP 2 / Brett E. Stein 3 /Stephen F. Balshi, MBE 4 Purpose:
SCD Case Study. Implant-supported overdentures
 SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
SCD Case Study Implant-supported overdentures An implant-retained overdenture may be indicated in patients with changed anatomy, neuromuscular disorders, significant gag reflex or considerable ridge resorption
Case study 25. Implantology Solutions for Atrophic Maxilla Using Short Implants. Dr. Ariel Labanca Mitre
 Case study 25 Implantology Solutions for Atrophic Maxilla Using Short Implants Dr. Ariel Labanca Mitre Oral Implantology Specialist Prosthodontics Specialist Implantology Solutions for Atrophic Maxilla
Case study 25 Implantology Solutions for Atrophic Maxilla Using Short Implants Dr. Ariel Labanca Mitre Oral Implantology Specialist Prosthodontics Specialist Implantology Solutions for Atrophic Maxilla
NobelActive Product overview
 NobelActive Product overview High primary stability even in demanding situations NobelActive s expanding tapered implant body condenses bone gradually while the apex with drilling blades enables a smaller
NobelActive Product overview High primary stability even in demanding situations NobelActive s expanding tapered implant body condenses bone gradually while the apex with drilling blades enables a smaller
Validating innovation.
 Validating innovation. NobelActive TM technical and clinical story 2 NobelActive technical and clinical story Developing NobelActive. NobelActive origins The life cycle of NobelActive began following years
Validating innovation. NobelActive TM technical and clinical story 2 NobelActive technical and clinical story Developing NobelActive. NobelActive origins The life cycle of NobelActive began following years
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH
 JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
JOURNAL OF CLINICAL AND DIAGNOSTIC RESEARCH How to cite this article: DESHPANDE S S, SARIN S P, PARKHEDKAR R D.PLATFORM SWITCHING OF DENTAL IMPLANTS: PANACEA FOR CRESTAL BONE LOSS?. Journal of Clinical
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
NobelReplace Conical Connection Product overview
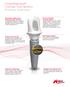 NobelReplace Conical Connection Product overview High primary stability, even in compromised bone situations1 The tapered implant body is designed for high primary stability and is ideal for Immediate
NobelReplace Conical Connection Product overview High primary stability, even in compromised bone situations1 The tapered implant body is designed for high primary stability and is ideal for Immediate
Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants
 Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Flapless Surgery Case Study 48 Flapless, Immediate Implantation & Immediate Loading with Socket Preservation in the Esthetic Area Using the Alpha-Bio Tec's NeO Implants Dr. Gadi Schneider DMD, Specialist
Pressure Necrosis And Osseointegration: An Editorial White Paper*
 Pressure Necrosis And Osseointegration: An Editorial White Paper* Alan Meltzer, DMD, MScD; Harold Baumgarten, DMD; Tiziano Testori, MD, DDS; Paolo Trisi, DDS, PhD Published by Pressure Necrosis And Osseointegration:
Pressure Necrosis And Osseointegration: An Editorial White Paper* Alan Meltzer, DMD, MScD; Harold Baumgarten, DMD; Tiziano Testori, MD, DDS; Paolo Trisi, DDS, PhD Published by Pressure Necrosis And Osseointegration:
CHAPTER 1. General Introduction
 CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
CHAPTER 1 General Introduction Chapter 1 The loss of remaining natural teeth and provision of artificial removable dentition is a major and irreversible procedure for the patient. The main limitations
Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate Loading Protocol: An In-Vivo Study
 J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
J Indian Prosthodont Soc (Apr-June 2013) 13(2):113 121 DOI 10.1007/s13191-012-0240-8 ORIGINAL ARTICLE Comparative Evaluation of Bone in Mandibular Implant Retained Overdentures Using Delayed and Immediate
Mechanical and technical risks in implant therapy.
 Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Mechanical and technical risks in implant therapy. Salvi GE, Brägger U. Int J Oral Maxillofac Implants. 2009;24 Suppl:69-85. To systematically appraise the impact of mechanical/technical risk factors on
Enhanced Implant Stability with a Chemically Modified SLA Surface: A Randomized Pilot Study
 Enhanced Implant Stability with a Chemically Modified SLA Surface: A Randomized Pilot Study Thomas W. Oates, DMD, PhD 1 /Pilar Valderrama, DDS, MS 2 /Mark Bischof, Dr Med Dent 3 / Rabah Nedir, Dr Med Dent
Enhanced Implant Stability with a Chemically Modified SLA Surface: A Randomized Pilot Study Thomas W. Oates, DMD, PhD 1 /Pilar Valderrama, DDS, MS 2 /Mark Bischof, Dr Med Dent 3 / Rabah Nedir, Dr Med Dent
Keywords: Biomechanics, Biostatistics, Maxilla, Maxillary sinus, Sinus floor augmentation.
 Research Article Journal of Periodontal J Periodontal Implant Sci 2013;43:58-63 http://dx.doi.org/10.5051/jpis.2013.43.2.58 Peri-implant bone length changes and survival rates of implants penetrating the
Research Article Journal of Periodontal J Periodontal Implant Sci 2013;43:58-63 http://dx.doi.org/10.5051/jpis.2013.43.2.58 Peri-implant bone length changes and survival rates of implants penetrating the
The success rate for osseointegration of
 RESEARCH CLINICAL EVALUATION OF THE NOBELACTIVE IMPLANT SYSTEM: ACASE SERIES OF 107 CONSECUTIVELY PLACED IMPLANTS AND A REVIEW OF THE IMPLANT FEATURES Tassos Irinakis, DDS, MSc; Colin Wiebe, DDS, MSc The
RESEARCH CLINICAL EVALUATION OF THE NOBELACTIVE IMPLANT SYSTEM: ACASE SERIES OF 107 CONSECUTIVELY PLACED IMPLANTS AND A REVIEW OF THE IMPLANT FEATURES Tassos Irinakis, DDS, MSc; Colin Wiebe, DDS, MSc The
In 1981, Dr. Albrektsson, a member of
 Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
Osseodensification facilitates ridge expansion with enhanced implant stability in the maxilla: part II case report with 2-year follow-up Drs. Ann Marie Hofbauer and Salah Huwais offer another case study
TOPICS. T O P I C S Day 1. Implant Locations. Implant Placement in the Posterior Maxilla. Anatomy and risk factors Option 1: Short implants
 T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
T O P I C S Day 1 Factors influencing the long-term stability of dental implants Surgical procedures in posterior sites: Standard implant placement with or without flap elevation Surgical procedures in
Long-term success of osseointegrated implants
 Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
Against All Odds A No Bone Solution Long-term success of osseointegrated implants depends on the length of the implants used and the quality and quantity of bone surrounding these implants. As surgical
BONE SPREADING TECHNIQUE A CASE REPORT. simultaneous implant placement and is an alternative Summer s osteotome both clinical use as well as the
 BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
BONE SPREADING TECHNIQUE A CASE REPORT AUTHORS: Renato Sussumu Nishioka, DDS, PhD*, João Carlos Paixão** ABSTRACT: Bone spreading technique (BST) is horizontal augmentation with minimal trauma for simultaneous
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re. Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T
 Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Dental Implant Treatment with Diffe Title for Sinus Floor Elevation-A Case Re Sekine, H; Taguchi, T; Seta, S; Tak Author(s) T; Kakizawa, T Journal Bulletin of Tokyo Dental College, 4 URL http://hdl.handle.net/10130/200
Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months
 Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months Jonas P. Becktor, DDS, PhD 1 / Sten Isaksson, MD, DDS, PhD 2
Endosseous Implants and Bone Augmentation in the Partially Dentate Maxilla: An Analysis of 17 Patients with a Follow-up of 29 to 101 Months Jonas P. Becktor, DDS, PhD 1 / Sten Isaksson, MD, DDS, PhD 2
High Crown to Implant Ratio as Stress Factor in Short Implants Therapy
 10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
10.1515/bjdm-2016-0015 BALKAN JOURNAL OF DENTAL MEDICINE ISSN 2335-0245 STOMATOLOGICAL SOCIETY High Crown to Implant Ratio as Stress Factor in Short Implants Therapy SUMMARY Background/Aim: The purpose
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Identification of Stability Changes for Immediately Placed Dental Implants
 Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
Identification of Stability Changes for Immediately Placed Dental Implants Jason D. West, DDS, MS 1 /Thomas W. Oates, DMD, PhD 2 Purpose: To evaluate the changes in stability of immediately placed implants
CHAPTER. 1. Uncontrolled systemic disease 2. Retrognathic jaw relationship
 CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
CHAPTER 7 Immediate Implant Supported Restoration of the Edentulous Arch Stephen G. Alfano and Robert M. Laughlin Department of Oral and Maxillofacial Surgery, Naval Medical Center San Diego, San Diego,
The severely resorbed edentulous maxilla presents
 Rehabilitation of Severely Resorbed Maxillae with Zygomatic Implants: An Evaluation of Implant Stability, Tissue Conditions, and Patients Opinion Before and After Treatment Payam Farzad, DDS, MSc 1 /Lars
Rehabilitation of Severely Resorbed Maxillae with Zygomatic Implants: An Evaluation of Implant Stability, Tissue Conditions, and Patients Opinion Before and After Treatment Payam Farzad, DDS, MSc 1 /Lars
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants
 The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
The Importance of Implant Surface Characteristics in the Replacement of Failed Implants Ghada Alsaadi, DDS, MSc 1 /Marc Quirynen, DDS, PhD 2 /Daniel van Steenberghe, MD, PhD, Dr hc 3 Purpose: The purpose
Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report
 Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
Case report AODMR Use of Implant Retained Overdenture in Atrophic Mandible - A Case Report Sheren Fatima 1, Rajarshi Basu 2, Neelkamal Hallur 3, Aaisha Siddiqua 4, Syed Zakaullah 4, Sumaiyya 2, Chaitanya
RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
 Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
Case Report International Journal of Dental and Health Sciences Volume 02,Issue 01 RESTORATION OF A FULLY EDENTULOUS PATIENT UTILIZING SIMPLE TECHNIQUES FOR IMPRESSION AND FABRICATION OF A HYBRID BRIDGE
A. Dental implants placed on bone subjected to vertical alveolar distraction. show the same performance as those placed on primitive bone
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.18545 http://dx.doi.org/doi:10.4317/medoral.18545 Dental implants placed on bone subjected to vertical alveolar distraction
Journal section: Oral Surgery Publication Types: Research doi:10.4317/medoral.18545 http://dx.doi.org/doi:10.4317/medoral.18545 Dental implants placed on bone subjected to vertical alveolar distraction
Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation
 IJopRD K Harshakumar et al CASE REPORT 10.5005/jp-journals-10019-1179 Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation 1 K Harshakumar, 2 Nimisha
IJopRD K Harshakumar et al CASE REPORT 10.5005/jp-journals-10019-1179 Rehabilitation of a Patient with Completely Edentulous Maxillary Arch using All on 4 Concept of Implantation 1 K Harshakumar, 2 Nimisha
Effect of the lack of primary stability in the survival of dental implants
 Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.54441 http://dx.doi.org/10.4317/jced.54441 Effect of the lack of primary stability in the survival of dental implants Carlos Cobo-Vázquez
Journal section: Oral Surgery Publication Types: Research doi:10.4317/jced.54441 http://dx.doi.org/10.4317/jced.54441 Effect of the lack of primary stability in the survival of dental implants Carlos Cobo-Vázquez
10 Years of XiVE Implantology Unlimited
 10 Years of XiVE Implantology Unlimited Implantology Unlimited is obligate for XiVE and every limit gives always a push to surrender new challenges: Primary stability in low bone quality? No problem with
10 Years of XiVE Implantology Unlimited Implantology Unlimited is obligate for XiVE and every limit gives always a push to surrender new challenges: Primary stability in low bone quality? No problem with
THE CORRELATION BETWEEN BONE DENSITY AND IMPLANT STABILITY Youssef M 1 BDS, Shaaban A M 2 PhD, Eldibany R 2 PhD.
 THE CORRELATION BETWEEN BONE DENSITY AND IMPLANT STABILITY Youssef M 1 BDS, Shaaban A M 2 PhD, Eldibany R 2 PhD. Abstract: Introduction: Long-term studies have documented the successful treatment of edentulous
THE CORRELATION BETWEEN BONE DENSITY AND IMPLANT STABILITY Youssef M 1 BDS, Shaaban A M 2 PhD, Eldibany R 2 PhD. Abstract: Introduction: Long-term studies have documented the successful treatment of edentulous
