Microbial Composition in Peri-implant Health and Disease
|
|
|
- Piers Harper
- 6 years ago
- Views:
Transcription
1 Microbial Composition in Peri-implant Health and Disease Authors Malak Hamzé Saad Fadhel Tutor Py Palmqvist
2 ABSTRACT Although the infectious initiation of peri-implantitis is commonly accepted, differences in microbial composition in peri-implantitis and periodontitis has been the subject of some debate. The presence of periodontal pathogens at sites with peri-implantitis has been documented by many studies. However, other studies have revealed that sites with periimplantitis harbour high levels of microorganisms which have not primarily been associated with periodontitis, such as Candida-, Staphylococcus- and Enterobacteriaceae species. These findings suggest that peri-implantitis may display a flora distinct from that of periodontitis. The aim of the present study was to evaluate the presence of three known periodontal pathogens, Aggregatibacter actinomycetemcomitans (A. actinomycetemcomitans), Porphyromonas gingivalis (P. gingivalis) and Treponema denticola (T. denticola) at healthy and diseased (peri-implantitis) sites. A second aim was to evaluate the presence of Candida-, Staphylococcus- and Enterobacteriaceae-species at the same sites. The hypothesis was that A. actinomycetemcomitans, P. gingivalis, T. denticola, Candida-, Staphylococcus- and Enterobacteriaceae-species would be detected at higher levels in peri-implantitis samples than healthy controls. Samples of peri-implant crevicular fluid (PICF) were obtained from peri-implant pockets in 13 subjects, of which 5 subjects had both healthy and diseased implants, 4 subjects had healthy implants only and the remaining 4 had only diseased implants. Microbial analyses were carried out using Real Time PCR and microbial culture techniques. A. actinomycetemscomitans, P. gingivalis and T. denticola were detected at higher levels at sites with peri-implantitis compared to healthy sites. Furthermore, Klebsiella oxytoca was detected in one peri-implantitis sample whereas Candida- and Staphylococcus species were not detected in any of the samples. Higher counts of periodontal pathogens were detected around implants with peri-implantitis. The suggestion that Candida and Staphylococcus may be present at higher levels in peri-implantitis was not supported by this study as these bacteria could not be detected in any of the samples.
3 INTRODUCTION Dental implants as replacement for missing teeth are common today. Although highly functioning for many patient s implants are vulnerable to infections, so called periimplant diseases, where the two conditions peri-implant mucositis and peri-implantitis are included. Peri-implant mucositis is defined as inflammation in the surrounding mucosa of the dental implant with unaffected supporting bone, clinically seen as bleeding on probing and swelling of the mucosa. In contrast, peri-implantitis includes inflammation in the surrounding mucosa and concomitant peri-implant bone loss. Deep pathological peri-implant pockets and suppuration are common clinical findings associated with peri-implantitis (Lang and Berglundh, 2011). In 2014, dental implants were installed in Sweden. In the same year dental implants were diagnosed with peri-implantitis (Data register of the Swedish Social Insurance Agency). The mean prevalence of peri-implant mucositis and peri-implantitis is 43 % and 22 %, respectively (Jepsen et al., 2015). Peri-implant mucositis is a reversible condition and can be treated efficiently using conservative methods while established peri-implantitis is difficult to manage, but studies have demonstrated that early diagnosis and intervention can improve the outcome of treatment (Salvi et al., 2012; Smeets et al., 2014). Studies have shown that non-surgical treatment of peri-implantitis is ineffective while surgical treatment show better results (Figuero et al., 2014; Smeets et al., 2014). However, surgical treatment demonstrates a success rate of no more than 58 % (Leonhardt et al., 2003). Altogether, this emphasizes the need for more sensitive diagnostic tools as well as adjunctive preventive and intervening treatment strategies for the disease. Determining species associated with peri-implant health and disease has been suggested as a diagnostic tool useful to improve prevention and treatment strategies (Charalampakis et al., 2011). In the oral cavity, dental implants like teeth, are exposed to biofilm formation. Pellicle is formed rapidly and the dental implants are soon colonized by multiple species. Consequently, a supra- and subgingival biofilm is established within weeks to months. In a clinical experimental study by Pontoriero et al. (Pontoriero et al., 1994), the participants were asked to refrain from all oralhygiene practices for 3 weeks. Plaque samples were then gathered and analysed. The study demonstrated a relationship between plaque accumulation and the establishment 3
4 of peri-implant mucositis. A similar study was performed by Zitzmann et al. (Zitzmann et al., 2001). The study concluded that plaque accumulation led to an inflammatory response in the gingiva and the peri-implant mucosa. The inflammation was characterized by an increased inflammatory cell infiltrate including elevated levels of T- and B-cells. Peri-implantitis is a multifactorial disease induced and entertained by an opportunistic infection. The susceptibility for the disease differs among individuals due to many contributing factors, such as genetic disposition, the host s immune system, presence of a virulent flora and environmental factors. Smoking, a history of periodontal disease and poor oral hygiene are known risk factors associated with implant failure and peri-implant disease. Diabetes mellitus and cardiovascular diseases, rough implant surfaces and lack of keratinized mucosa are other factors which have been proposed to increase the risk for disease (Smeets et al., 2014). Peri-implant health is achieved by an equilibrium between the flora colonizing the peri-implant pockets and the host response including the immune system. In a susceptible host, uninterrupted plaque accumulation is followed by increased depth of the peri-implant pockets. A gram-negative flora of anaerobic bacterial species with specific virulence factors increases in this environment at the expense of the less harmful gram positive aerobic flora. When the host s immune response, being either inefficient or excessive, fails to suppress the pathogenic flora the balance maintaining peri-implant health is altered which eventually leads to destruction of the peri-implant tissues (Griffen et al., 1998). Previous microbiological investigations have described the flora associated with periimplant health to be very similar to that of sound periodontal sites. The flora has been demonstrated to consist of mostly gram positive cocci with low proportions of gram negative anaerobic species (Lindhe et al., 2015). Early studies using culture techniques failed to detect species like P. gingivalis and A. actinomycetemcomitans in fully edentulous patients treated with dental implants after complete extraction of teeth due to periodontitis. Consequently, these species were believed to be eradicated when their ecological niches, i.e. the periodontal pockets, were no longer present. This led to the suggestion that periodontal pathogens do not colonize dental implants in fully edentulous patients (Danser et al., 1997). However, this idea was rejected when more sensitive detection methods such as real time PCR 4
5 and DNA-DNA hybridization became available. With these methods, periodontal pathogens such as P. gingivalis, A. actinomycetemcomitans, T. denticola and T. forsythia were detected at low levels at the sulci of newly inserted and healthy implants in fully edentulous patients with a history of severe and aggressive periodontitis (Van Assche et al., 2009). Periodontal pathogens were also identified at the sulci of sound dental implants in patients with partial edentulism (Casado et al., 2011). Hence, the presence of periodontal pathogens at the sulci of dental implants may not always cause disease, owing to the multifactorial nature of periimplant disease. The flora associated with peri-implantitis is mainly composed of gram negative anaerobic rods with high proportions of black-pigmented Bactericides-, Campylobacter- and Fusobacterium species. The presence of periodontal pathogens such as A. actinomycetemcomitans, P. gingivalis, T. denticola, Tanerella. forsythia, Campylobacter gracilis and Campylobacter rectus at sites with periimplantitis has been documented in many studies (Sanz M et al., 1990; Persson et al., 2010). Consequently, it was concluded that peri-implantitis and periodontitis share similar microbial profiles. However, other studies have identified species not primarily associated with periodontal diseases at sites with peri-implantitis. These species include enteric rods (Leonhardt et al., 2003; Renvert et al., 2016), fungal organisms (Leonhardt et al. 1999; Schwarz et al. 2015), Staphylococcus aureus (Persson et al., 2010; Renvert et al., 2016) and human Cytomegalovirus as well as Epstein-Barr virus (Jankovic et al., 2011), thus indicating microbiological differences between periimplantitis and periodontitis. In a culture study by Leonhardt et al. (Leonhardt et al.,1999) it was revealed that diseased implants harboured periodontal pathogens such as, A. actinomycetemcomitans, P. gingivalis, Prevotella intermedia and Prevotella nigrescens in 60 % of the cases. In addition, enteric rods, Candida- and Staphylococcispecies were detected in 55 % of the diseased cases which led to the conclusion that peri-implantitis and periodontitis may share different microbial profiles. In a newly published systematic review 194 microbiological studies were screened of which 47 studies were included in the review. It was concluded that classic periodontal pathogens are often found in the flora of peri-implant disease, however, correlation between studies is difficult due to the use of diifferent detection techniques. For future 5
6 investigations, the authors recommended the use of megagenomic teqniques in order to avoid detection bias (Padial- Molina et al., 2016). Methods which are used for microbial detection involve culture techniques, DNA hybridization, polymerase chain reaction (PCR), immunofluorescence and 16S RNA sequencing. The different detection methods all have advantages and disadvantages and analytical results vary depending on the technique used. Hence, comparison of results generated by different techniques in studies may be difficult to make. (Rylev and Kilian., 2008). Hypothesis The hypothesis of the study was that A. actinomyctemcomitans, P. gingivalis and T. denticola would be detected at higher levels around implants with peri-implantitis compared to healthy controls. Secondarily, we hypothesized that Candida-, Enterobacteriaceae- and Staphyloccus- species would also be detected at higher levels around implants with periimplantitis compared to healthy controls. Aim The aim of the present study was to evaluate the presence and detection levels of three known periodontal pathogens, A. actinomycetemcomitans, P. gingivalis and T. denticola at healthy and diseased (peri-implantitis) sites and secondly to evaluate the presence of Candida-, Staphylococcus- and Enterobacteriaceae-species at these sites by cultivation and quantitative polymerase chain reaction (qpcr). MATERIAL AND METHODS Ethical considerations The ethical committee at the institution of Odontology at Umeå University approved this study. The subjects were informed verbally about the content and aim of this study and written consent was given from all the enrolled patients. Patients were given the chance to decline to participate at any time. All patient data was handled with confidentiality and all operators were bound to secrecy. Patient data was coded by the supervisor of the study, senior 6
7 consultant in periodontology Py Palmqvist. Data was handled in a coded manner by the dental students Malak Hamzé and Saad Fadhel and presented in a decoded manner in the report. Only the supervisor had access to the passkey which was store locked at the Department of Periodontology. Literature search Literature search was performed using the electronic PubMed database using a combination of specific mesh-terms such as peri-implantitis, microbiology, microbiota and dental implants. Additionally, hand search was made in the textbook Clinical Periodontology and Implant Dentistry (Lindhe et al., 2008). Statistical Analysis Descriptive data analysis was performed the Microsoft Excel program (Microsoft Corporation, USA Production). Patient sample A total of 13 consecutive adult patients who were transferred to the specialist clinics for Periodontology and Prosthodontics, respectively, in County Council of Västerbotten, Umeå, for treatment of either peri-implantitis or prosthodontic treatment between years 2016 and 2017 were enrolled in the study. The clinical examinations were carried out by three periodontists and one prosthodontist. Only our supervisor PhD Py Palmqvist and the clinicians who treated the patients had access to the uncoded patient data. Questionnaire A questionnaire was delivered to the involved clinicians. The questionnaire was used to ensure that samples of peri-implant crevicular fluid were collected and obtained only from patients with implant sites meeting the inclusion criteria. The questionnaire included clinical data from the patients dental records including radiographic data from the clinical periodontal registration, i.e. peri-implant diagnosis, probing pocket depth (PPD) and bleeding on probing/suppuration (BOP/SUP). Furthermore, the questionnaire contained questions about smoking 7
8 habits, history of periodontitis and presence of systemic disease and medication. However, these anamnestic data were not presented or analysed in this study. Inclusion criteria Patients with at least two implants of which one was diagnosed with periimplantitis and one was healthy were included in the study. However, patients not meeting these inclusion criteria, by demonstrating either diseased or healthy implants but not both, were also included in the study. These patients were included to increase the number of analyzed samples as patients fulfilling these inclusion criteria were lacking in sufficient numbers at the clinic at the time of the study. Implants were considered healthy when demonstrating no BOP/suppuration at any site, a PPD 4 mm in all 4 sites and intact marginal bone level which was determined using intraoral radiographs. The diagnostic criteria for periimplantitis were presence of radiographic marginal bone loss around implants when compared to baseline radiographs one year after implant placement in combination with presence of PPD 4 mm and BOP/SUP. (Lindhe and Meyle, 2008). Exclusion criteria The participants had to be non-smokers and free from systemic diseases. In addition, patients treated with antibiotics for the last 3 months were excluded. However, one unmatched diseased sample did not meet the exclusion criteria for smoking. This sample was included to increase the number of samples. Clinical Investigation The clinical examinations and assessments were carried out by the same four specialists who collected the samples. Peri-implant bone level was evaluated using intraoral radiographs. PPD was measured using a manual periodontal probe (Hu-Friedy PCP-11, Hu-Friedy Mfg. Co., Chicago, USA) at four sites per implant; mesial, distal, buccal and lingual. Values 3 mm were registered. BOP/SUP from the bottom of the peri-implant pocket was registered 30 seconds after probing with an estimated force of 0.25 N (Schwarz et al., 2011). Non- 8
9 bleeding sites were registered as zero (0) and bleeding sites were registered as one (1). Collection of peri-implant fluid Samples of peri-implant crevicular fluid (PICF) were collected with paper points from healthy and diseased sites in 13 subjects, of which 5 subjects fulfilled the inclusions criteria and had both healthy and diseased implants in the same mouth (matched samples). The remaining 8 subjects were unmatched demonstrating either healthy or diseased implants, of which 4 were healthy and 4 were diseased. The dental implants were polished to remove supra-mucosal plaque and the sites were isolated with cotton rolls. Sterile absorbent endodontic paper points were inserted deep into each peri-implant pocket for 30 seconds. The deepest site of each implant was chosen for sampling at implants with peri-implantitis. Two samples were collected from the same site, one for cultivation and one for PCRanalysis. The paper points were inserted into VGMAIII, an anaerobic transport medium (Viable medium of Department of Bacteriology, University of Gothenburg, Anaerobic medium) for cultivation and Eppendorf tubes with 1 ml TE- buffer (Tris EDTA buffer, 10 µm/1µm; ph 8.0) for qpcr analysis. The samples were transported to the Clinical laboratory of Department of Odontology, Medical Faculty, Umeå University for microbiological analyzes. Microbiological Analysis Detection of Candida -, Enterobacteriaceae- and Staphylococcus species by cultivation The samples transported in VGMAIII tubes were incubated at 37 degrees for 2-3 minutes and subsequently diluted 100 times in a salt buffer (Johansson et al., 2014). They were then gently shaken on a Vortex mixer for 1 min. Aliquots of 50 µl of undiluted as well as 100 times diluted samples were spread on Candida- (ChromAgar, Mast Diagnostics, U.K), Enterobacteriaceae- (Violet Red Bile 9
10 Agar; Difco Laboratories; Detroit, Michigan, USA), and Staphylococcus (Staphylococcus Medium 110, Becton, Dickinson and Company, Sparks, MD USA) specific plates. The selective plates were incubated for 2-3 days at 37 C before they were examined. Detection of A. actinomycetemcomitans, P. gingivalis and T. deticola and quantification of total number of bacteria by qpcr. Bacterial DNA in the samples which were transported in the TE-buffer were purified by a DNA preparation robot (Diasorin). DNA from standard solutions ( bacterial cells/ml) of A. actinomycetemcomitans and P. gingivalis were purified in the same way. Due to the absence of standard solutions for T. denticola, the samples were studied in a semiquantitative manner. When total number of bacteria in the samples was determined the standard suspension for P. gingivalis was used. The PCR mixture of in total 10µl contained 5µl of Kapa Cyber Green (KK 4601, Kapa Biosystems, Boston USA), 4 µl of template and 1µl of species specific primers (5 µm each). The primers for A. actinomycetemcomitans, P. gingivalis and T. denticola, total number of bacteria, and the PCR programs used are shown in the Appendix. The quantifications were performed by q-pcr Corbett research Rotor-Gene 6000 Rotary Analyze (QIAGEN, Valencia, CA, USA). RESULTS In 5 of the 13 subjects, samples from both healthy and diseased sites could be collected from the same individual, i.e. samples were matched. In 4 of the subjects, only diseased unmatched samples were collected and the remaining 4 were healthy unmatched samples. Matched samples (Subjects 1-5) A. actinomycetemcomitans was detected in 4 out of 5 subjects (2 out of 5 sound implants and 4 out of 5 diseased implants). The diseased implants showed higher detection levels of A. actinomycetemcomitans except in one subject where the opposite was noted. P. gingivalis was detected in 2 out of 5 subjects. In these two subjects, P. gingivalis was detected in samples obtained from both healthy and diseased implants. 10
11 T. denticola was detected in 3 of out 5 subjects. The diseased implants showed higher detection levels of T. denticola compared to healthy implants (Table 1a). Healthy unmatched samples (Subjects 6-9) A. actinomycetemcomitans and P. gingivalis were not detected in any of the 4 subjects. On the other hand, T. denticola were detected in all 4 subjects. It was detected at low levels in all but one of the samples, subject number 6, which revealed a high detection level for T. denticola (Table 1b). Diseased unmatched samples (Subjects 10-13) A. actinomycetemcomitans was detected in 2 out of 4 subjects. P. gingivalis was detected in 1 out of 4 subjects. However, one sample needed to be reanalyzed for P. gingivalis. Unfortunately, re-analysis could not be carried out due to lack of time. Thus, the presence of P. gingivalis could not be evaluated in one of the subjects. T. denticola was detected in 3 out of 4 subjects (Table 1c). Cultivation K. oxytoca, a member of the Enterobacteriaceae family, was detected in one peri-implantitis sample, obtained from subject number 3, whereas Candida- and Staphylococcus-species were not detected in any of the samples. DISCUSSION In the present study, A. actinomycetemcomitans, P. ginigvalis and T. denticola were detected in healthy as well as diseased (peri-implantitis) samples. However, the diseased samples demonstrated higher detection levels of these bacteria. These results are in line with Hultin et al. (Hultin et al., 2002). Hultin et al. used DNA-DNA hybridization for microbial detection and demonstrated that periodontal pathogens such as A. actinomycetemcomitans, P. gingivalis and T. denticola could be detected around both sound and diseased implants. In line with our results, these bacteria were detected more frequently and at higher levels around diseased implants. Since putative pathogens could be found around both healthy and diseased implants, the microbiological composition has not been demonstrated to have a predictive value for peri-implantitis (Casado et al., 2011; Persson and Renvert, 2014). The complex nature of peri-implantitis and the involvement of host and environmental factors makes it hard to predict the long-term health of dental implants solely based on microbial composition. 11
12 In a culture study by Leonhardt et al. (Leonhardt et al., 1999), enteric rods, Candida- and Staphylococcus- species were detected in 55 % of the diseased sites. In our study, Candida- and Staphylococcus-species were not detected in either diseased or healthy sites. Hence, the findings of Leonhardt and coworkers could not be substantiated by our study. However, in line with their results is the detection, in one peri-implantitis sample, of K. oxytoca, which is a member of the Enterobacterceae family. It is possible that we failed to detect Candida and Staphylococcus-species due to the low number of participants in the present study. Furthermore, C. albicans, S. aureus and Enterobacteriaceae species are rarely found in the oral cavity and their presence have been associated with opportunistic infections in immunocompromised patients. A study evaluating their prevalence was carried out by Öhman et al. (Öhman et al., 1995) in a group of 79-year-olds in Gothenburg, Sweden. 100 subjects were included in the study and the majority of the subjects suffered from systemic diseases. The species were detected in few subjects and their presence was correlated to the use of dentures. This might be another possible explanation to why these microbes were not detected in the present study since none of our participants wore dentures. Persson and Renvert (Persson and Renvert, 2014) used DNA- DNA hybridization and demonstrated higher detection levels of a cluster of 7 bacterial species, i.e. T. forsythia, P. gingivalis, Streptococcus mitis, Streptococcus intermedius, S. aureus, Staphylococcus anaerobius and Treponema socranskii, around implants with peri-implantitis compared to healthy controls. The authors suggested a possible association between this cluster of bacteria and the development of peri-implantitis and they highlighted the role of S. aureus and T. forsythia as potential key pathogens since T. forsythia was found in 45% of the diseased sites compared to 15 % of the healthy sites. S. aureus is often found on infected medical devices and is a microbe which is believed to be associated with infections around metallic biomaterials. Hence, its involvement in the development of peri-implantitis has been addressed in studies (Leonhardt et al., 1999). Interestingly, S. aureus, like other Staphylococci, has been shown to have high affinity to titanium surfaces (Harris et al., 2006) and subjects with failing implants have been shown to have less efficient antibodies against S. aureus as well as T. forsythia (Kronström et al., 2001). The present study failed to detect Staphylococcus-species in any of the samples, thus, their possible contribution to implant failure could not be confirmed. 12
13 The discrepancy in the microbial profile of peri-implantitis between studies is in part due to the use of different detection methods. Culture analysis has long been the golden standard for microbial analysis and it has many advantages. However, non-cultivable and dead species are not detected by this method which increases the risk for false negative results. It requires sufficient sample volumes as well as adequate transportation conditions. In contrast, molecular detection methods such as qpcr and DNA-DNA hybridization are less time consuming and more sensitive, allowing the detection of species present at low levels. These methods can detect uncultivable as well as non-vital bacteria. Consequently, microbial data obtained from studies using different detection methods may be very difficult to compare (Padial- Molina et al.,2016). The present study had several limitations and weaknesses. According to the inclusion criteria only matched subjects would be included in the study. However, few patients demonstrated both sound and diseased implants in the same mouth at the time when the study was conducted. Consequently, unmatched subjects with either sound or diseased implants were also included in the study in order to increase the number of participants. Hence, the unmatched samples did not meet the intended inclusion criteria of this study. Anamnestic data such as smoking habits, history of periodontal disease and presence of systemic diseases were not analysed since this study included a small number of participants, which made conclusions difficult to draw. Furthermore, one of the collected unmatched samples did not meet the exclusion criteria regarding smoking habits. This was probably due to inattention to the study protocol by one specialist at the specialist clinic of prosthodontics. This sample was included and analysed because we did not want to further reduce the number of participants. Additionally, clinical assessments may have differed between clinicians and a deviation from the sampling protocol may have occurred. Inter-individual calibration of clinical assessment between the clinicians involved was not performed or evaluated. Other weaknesses were the facts that two samples were lost during the DNA-preparation process and 4 samples were not tested due to lack of time. Finally, collection of samples from only one site per implant may be a weakness as testing multiple sites per implant could contribute to more representative microbial data. 13
14 Conclusion The results of this study confirm the findings in several previous studies showing that the periodontal pathogens A. actinomycetemcomitans, P. gingivalis and T. denticola are present at higher levels in diseased peri-implant pockets compared to healthy controls. These pathogens were also detected in clinically healthy peri-implant sites. Furthermore, the study failed to corroborate the findings of previous studies demonstrating presence of Candida- and Staphylococcus-species in peri-implantitis. For future studies, a higher number of participants is recommended and the promotion of megagenomic detection methods in order to avoid detection bias. ACKNOWLEDGMENTS We would like to thank our supervisor, PhD Py Palmqvist for her support and guidance throughout the course of the study and for collecting clinical data and microbial samples together with Martin Ågren, Uday Najim and Peder Willhelmsson at the department of Periodontology and Prosthodontics at Umeå University. We are very grateful to Rolf Claesson for the microbiogical laboratory work at the Clinical Laboratory of Dental School in Umeå. And finally, we would like to express our gratitude to Anders Esberg for helping us with the statistics and making of the graphs. 14
15 REFERENCES Berglundh T, Zitzmann NU, Donati M (2011). Are peri-implantitis lesions different from periodontitis lesions? J Clinl Periodont 38: Casado PL, Otazu IB, Balduino A, de Mello W, Barboza EP, Duarte ME (2011). Identification of periodontal pathogens in healthy periimplant sites. Implant Dent 20: Charalampakis G, Rabe P, Leonhardt A, Dahlén G (2011). A follow-up study of periimplantitis cases after treatment. Periodontol : Danser M.M., van Winkelhoff, A.J, van der Velden, U (1997). Periodontal bacteria colonizing oral mucous membranes in edentulous patients wearing dental implants. J Periodontol 68: Figuero E, Granziani F, Sanz L, Herrera D, Sanz M (2014). Management of peri-implant mucositis and peri-implantitis. Periodontol : Griffen AL, Becker MR, Lyons SR, Moeschberger ML, Leys EJ (1998). Prevalence of Porphyromonas gingivalis and periodontal health status. J Clin Microbiol 36: Harris LG, Mead L, Müller-Oberländer E, Richards RG (2006). Bacteria and cell cytocompatibility studies on coated medicalgradetitaniumsurfaces. J Biomed Mater Res 78: Hultin M, Gustafsson A, Hallström H, Johansson LA, Ekfeldt A, Klinge B (2002). Microbiological findings and host response in patients with peri-implantitis. Clin Oral Implant Res 13: Jankovic, Aleksic, B. Dimitrijevic, Lekovic V, Camargo P, Kenney B (2011). Prevalence of human cytemogalovirus and Epstein- Barr virus in subgingival plaque at peri-implantitis, mucositis and healthy sites. Int J Oral Maxillofac Surg 40: Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks J et al (2015). Primary prevention of peri-implantitis: Managing peri-implant mucositis. J Clin Periodontol 16:
16 Johansson A, Haubek D (2014). Pathogenicity of the highly leukotoxic JP2 clone of Aggregatibacter actinomycetemcomitans and its geographic dissemination and role in aggressive periodontitis. J Oral Microbiol 6: 1. Kronström M, Svenson B, Hellman M, Persson GR (2001). Early implant failures in patients treated with Brånemark System titanium dental implants. Int J Oral Maxillofac Implant 16: Lang, N. P, Berglundh, T (2011). Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology. J Clin Periodontol 38: Leonhardt A, Renvert S, Dahlen G (1999). Microbial findings at failing implants. Clin Oral Implants 10: Leonhardt A, Bergstrom C, Lekholm (2003). Microbiologic diagnostics at titanium implants. Clin Implant Dent Relat Res 5: Leonhardt A, Dahlen G, Renvert S (2003). Five- year clinical, microbiological, and radiological outcome following treatment of peri-implantitis in man. J Periodontol 74: Lindhe J, Lang NP (2015). Clinical Periodontology and Implant Dentistry, 4 th edition, Oxford. Lindhe J, Meyle J (2008). Peri-implant diseses: Consensus report of the sixth European Workshop on Periodontology. J Periodontol 25: Persson G.R, Samuelsson E, Lindahl C, Renvert S (2010). Mechanical non-surgical treatment of peri-implantitis. J Clin Periodontol 37: Persson GR, Renvert S (2014). Cluster of bacteria associated with peri-implantitis. Clin Implant Dent Relat 16: Miguel P.M, Jesus L.M, Francisco O, Pablo G.M, (2014). Microbial profiles and detection technique in Peri-implant diseases: a systematic Review. J Oral Macillofac Res 3: Pontoriero R, Tonelli M.P, Carnevale G, Mombelli A, Nyman S.R, Lang N.P (1994). Experimentally induced peri-implant mucositis. Clin Oral Implants Res 5:
17 Renvert, Cecila W, Rutger G Persson (2016). Cytokine and microbial profiles in relation the clinical outcome following treatment of peri-implnaititis. Clin Oral Implants Res 00: 1-6. Rylev M, Killan M (2008). Prevalence and distribution of principal periodontal pathogens worldwide. J Clin periodontal 35: Salvi GE, Aglietta M, Eick S, Sculean A, Lang NP, Ramseier CA (2012). Reversibility of experimental peri-implant mucositis compared with experimental gingivitis in humans. Clin Oral Implants Res 23: Smeets R, Henningsen A, Jung O, Heiland M, Hammächer C, Stein JM (2014). Definition, Etiology, prevention and treatment of peri-implantitis- a review. Head Face Med 10: 34. Sanz M, Newman MG, Nachnani S, Holt R, Stewart R, Flemmig T (1990). Characterisation of the subgingival microbial flora around endosteal sapphire dental implants in partially edentulous patients. Int J Oral Macillofac Implants 5: Schwarz F, Sahm N, Becker J (2011). Impact of the outcome of guided bone regeneration in dehiscence. Clin Oral Implants Res 23: Schward F, Becker K, Rahn S, Hagewald A, Pfeffer K, Henrich B (2015). Real- time PCR analysis of fungal organisms and bacterial species at peri-implantitis sites. J implant Dent 1: 9. Van Assche, N, Van Essche, Pauwels M, Teughels W, Quirynen M (2009). Do periodontopathogens disappear after full-mouth tooth extraction? J Clin Periodontol 36: Zitzmann N U, Berglundh T, Marinello C.P, Lindhe J (2001). Experimental peri-implant mucositis in man. J Clin Periodontol 28: Ohman S-C, Österberg T, Dahlen G, Landahl S (1995). The prevalence of Staphylococcus aureus, Enterobacteriaceae species, and Candida species and their relation to oral mucosal lesions in a group of 79- years - olds in Göteborg. Acta Odontol Scand 53:
18 Tables Table 1. The amount of T. d in each sample was estimated using C t-values. C t -values are represented by plus signs (+). High C t-values correspond to a low detection levels of bacteria and low C t -values correspond to high detection levels. E.g., + symbolizes a low and ++++ a high detection level of T. d. + = > 29.92; ++ = ; +++ = ; ++++ = Table 1a. Proportion of periodontal pathogens in matched implants with peri-implantitis compared to healthy implants. Subjects Periimplant status Total viable counts per ml A.a TVC/ml (%) 0.5 (1.8 %) 0.2 (0.001 %) 54 (18.6 %) 8.2 (2.0 %) 77 (6.4 %) 410 (7.3 %) P.g TVC/ml (%) 9.s3 (46.5 %) 859 (33.0 %) 282 (65.6 %) 4900 (87.5 %) T.d TVC/ml (%) Nt Nt Nt Nt Table 1b. Proportion of periodontal pathogens in unmatched healthy implants. Subjects Total viable counts per ml 10 3 A.a TVC/ml (%) P.g TVC/ml (%) T.d TVC/ml (%) Table 1c. Proportion of periodontal pathogens in unmatched implants with peri-implantitis. Subject Total viable counts per ml 10 3 A.a TVC/ml (%) P.g TVC/ml (%) T.d TVC/ml (%) (0.2 %) (8.3 %) 9350 (91.7 %) = Healthy implant 1 = Implant with peri-implantitis TVC/ml = Total viable counts per ml = Not detected Nt = Not tested - = Lost sample 18
19 % of total amount of bacteria % of total amount of bacteria Figures Aggregatibacter actinomycetemcomitans Aa; Subject 2 PI; 18,6 Aa; Subject 5 PI; Aa; Subject 4 PI; 7,3 6,4 Aa; Subject 1 H; 1,8 Aa; Subject 1 PI; 0,001 2,0 Figure 1a. Proportion of A. actinomycetemcomitans in matched subjects 1-5. Porphyromonas gingivalis Porphyromonas gingivalis; Subject 3 H; 46,5 33,0 Porphyromonas gingivalis; Subject 5 PI; 87,5 Porphyromonas gingivalis; Subject 5 H; 65,6 Figure 1b. Proportion of P. gingivalis in matched subjects
20 % of total amount of bacteria % of total amount of bacteria Aggregatibacter actinomycetemcomitans Porphyrmonas gingivalis Figure 1c. Proportions of A. actinomycetemcomitans (left) and P. gingivalis (right) in healthy implants (Subjects 6-9) compared to implants with peri-implantitis (subjects 10-13). 20
21 APPENDIX 16S rdna primer pairs for detecting the total number of bacteria and A. actinomycetemcomitans, P. ginigvalis and T. denticola (Kirakodu et al., 2008). Reverse Forward Universal A.a P.g T.d GATTAGATACCCTGG TAGTCCAC TACCTTGTTACGAGC TT CTAGGTATTGCGAAACAT TTG CGTGAAATTAAGCTGGTA ATC AGGCAGCTTGCCATACTT GCG ACTGTTAGCAACTACCG ATCT TAATACCGAATGTGCTATTACAT TCAAAGAAGCATTCCCTCTTCTT CTTTA Cycling setting and annealing temperatures for quantification of bacteria using Corbette Research Rotor Gene 6000 Rotary Analyze (QIAGEN, Valencia, CA, USA) Prime Universal A.a P.g T.d Hold/time 95 /600 sec 95 /600 sec 95 /600 sec 95 /600 sec Cycling/time 95 /10 sec 95 /10 sec 95 /10 sec 95 /10 sec Cycling/time 52 /5 sec 55 /5 sec 60 /5 sec 59 /5 sec Cycling/time 72 /30 sec 72 /10 sec 72 /16 sec 72 /13 sec 21
Quantitative Analysis of Aggregatibacter actinomycetemcomitans and Porphyromonas gingivalis in Adolescents from Ghana
 Quantitative Analysis of Aggregatibacter actinomycetemcomitans and Porphyromonas gingivalis in Adolescents from Ghana Frida Söderqvist and Nina Willdén Tutors: Anders Johansson, Rolf Claesson, Carola Höglund
Quantitative Analysis of Aggregatibacter actinomycetemcomitans and Porphyromonas gingivalis in Adolescents from Ghana Frida Söderqvist and Nina Willdén Tutors: Anders Johansson, Rolf Claesson, Carola Höglund
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Materials and Methods: Literature review and Authors opinion.
 Haffajee AD, Bogren A, Hasturk H et al. Subgingival microbiota of chronic periodontitis subjects from different geographic locations. J Clin Periodontol 2004; 31:996-1002. Purpose: To compare the subgingival
Haffajee AD, Bogren A, Hasturk H et al. Subgingival microbiota of chronic periodontitis subjects from different geographic locations. J Clin Periodontol 2004; 31:996-1002. Purpose: To compare the subgingival
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study
 Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
FACULTY OF HEALTH SCIENCES INSTITUTE OF CLINICAL DENTISTRY
 Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Professor Gottfried Schmalz Editor-in-Chief Clinical Oral Investigations Universität Regensburg Fakultät für Medizin Poliklinik für Zahnerhatungskunde und Parodontologie Frans-Josef-Strauss-Allee 11 93053
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions
 Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Original Article An Investigation of Antibiotic Resistance of Aggregatibacter Actinomycetemcomitans and Porphyromonas Gingivalis in Peri-implantitis Lesions Z. Kadkhoda 1, S. Torabi 2, A. Aliramezani 3.
Journal of Periodontology & Implant Dentistry. Research Article
 Journal of Periodontology & Implant Dentistry Research Article Assessment of Aggregatibacter actinomycetemcomitans and Prevotella intermedia Counts around Healthy Implants, Diseased Implants and Sound
Journal of Periodontology & Implant Dentistry Research Article Assessment of Aggregatibacter actinomycetemcomitans and Prevotella intermedia Counts around Healthy Implants, Diseased Implants and Sound
JSS Medical and Dental College and Hospital, JSS University, Mysore, India *Author for Correspondence
 CLINICAL, MICROBIOLOGICAL AND MOLECULAR STUDY OF PORPHYROMONAS GINGIVALIS IN PATIENTS WITH CHRONIC PERIODONTITIS *Mayuri Vajawat 1, Vijay Kumar 2, K.G. Rajeshwari 3 and P.C. Deepika 4 1&4 Department of
CLINICAL, MICROBIOLOGICAL AND MOLECULAR STUDY OF PORPHYROMONAS GINGIVALIS IN PATIENTS WITH CHRONIC PERIODONTITIS *Mayuri Vajawat 1, Vijay Kumar 2, K.G. Rajeshwari 3 and P.C. Deepika 4 1&4 Department of
The Microbial Etiology and Pathogenesis of Peri-Implantitis
 The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
The Microbial Etiology and Pathogenesis of Peri-Implantitis Liqaa Shallal Farhan Department of Maxillofacial Surgery, College of Dentistry, University of Anbar, Iraq Abstract Patients with moderate Perimplantitis
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
Detection of predominant subgingival periopathogens around submerged and non submerged hydroxy apatite implants
 [Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
[Downloaded free from http://www.jdionline.org on Sunday, January 26, 2014, IP: 201.22.186.203] Click here to download free Android application for this journa ORIGINAL ARTICLE Detection of predominant
Microbiota and Oral Disease Prof. Dennis Cvitkovitch
 1 Professor Dennis Cvitkovitch Faculty of Dentistry Dental Research Institute University of Toronto The human microbiome We are a composite species: eukaryotic, bacterial, archeal Every human harbors over
1 Professor Dennis Cvitkovitch Faculty of Dentistry Dental Research Institute University of Toronto The human microbiome We are a composite species: eukaryotic, bacterial, archeal Every human harbors over
Volume 2 Issue
 Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Polyspecies biofilm formation involved in overdenture peri-implantitis
 Romanian Biotechnological Letters Vol., No. x, Copyright 2016 University of Bucharest Printed in Romania. All rights reserved ORIGINAL PAPER Polyspecies biofilm formation involved in overdenture peri-implantitis
Romanian Biotechnological Letters Vol., No. x, Copyright 2016 University of Bucharest Printed in Romania. All rights reserved ORIGINAL PAPER Polyspecies biofilm formation involved in overdenture peri-implantitis
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up
 Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Original article The impact of smoking and previous periodontal disease on peri-implant microbiota and health: a retrospective study up to 7-year follow-up Alessandro Quaranta, DDS, PhD 1 Bartolomeo Assenza,
Microbiota Around Root-Form Endosseous Implants: A Review of the Literature
 Microbiota Around Root-Form Endosseous Implants: A Review of the Literature Kees Heydenrijk, DDS, PhD 1 /Henny J. A. Meijer, DDS, PhD 2 /Wil A. van der Reijden, PhD 1 / Gerry M. Raghoebar, MD, DDS, PhD
Microbiota Around Root-Form Endosseous Implants: A Review of the Literature Kees Heydenrijk, DDS, PhD 1 /Henny J. A. Meijer, DDS, PhD 2 /Wil A. van der Reijden, PhD 1 / Gerry M. Raghoebar, MD, DDS, PhD
Peri-implantitis Review
 1 2 Aro n J. Saf f er D DS M S Di pl omate o f th e Ame ric an Bo ard of P eri od o n tol og y A quarterly review of the latest publications related to the study of Peri-implant inflammation and bone loss
1 2 Aro n J. Saf f er D DS M S Di pl omate o f th e Ame ric an Bo ard of P eri od o n tol og y A quarterly review of the latest publications related to the study of Peri-implant inflammation and bone loss
The International Journal of Periodontics & Restorative Dentistry
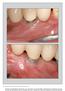 The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
The International Journal of Periodontics & Restorative Dentistry 91 Matrix Metalloproteinase-8 Levels in Peri-implant Sulcus Fluid Adjacent to Titanium and Zirconium Nitride Surfaces Richard Meissen,
International Journal of Pharma and Bio Sciences PERIODONTAL PATHOGENS AMONG PRE PUBERTAL, PUBERTAL AND POST PUBERTAL GIRLS, IN CHENNAI, INDIA.
 Research Article Microbiology International Journal of Pharma and Bio Sciences ISSN 0975-6299 PERIODONTAL PATHOGENS AMONG PRE PUBERTAL, PUBERTAL AND POST PUBERTAL GIRLS, IN CHENNAI, INDIA. KANAKAM ELIZABETH
Research Article Microbiology International Journal of Pharma and Bio Sciences ISSN 0975-6299 PERIODONTAL PATHOGENS AMONG PRE PUBERTAL, PUBERTAL AND POST PUBERTAL GIRLS, IN CHENNAI, INDIA. KANAKAM ELIZABETH
Journal of Dentistry, Tehran University of Medical Sciences
 Comparison of Systemic Ciprofloxacin in Elimination of A.a from Active Sites with Combination of Metronidzole and Amoxicillin in Patients with Aggressive Periodontitis: A Randomized Double Blind Controlled
Comparison of Systemic Ciprofloxacin in Elimination of A.a from Active Sites with Combination of Metronidzole and Amoxicillin in Patients with Aggressive Periodontitis: A Randomized Double Blind Controlled
Microbial Complexes Detected in the Second/Third Molar Region in Patients With Asymptomatic Third Molars
 J Oral Maxillofac Surg 60:1234-1240, 2002 Microbial Complexes Detected in the Second/Third Molar Region in Patients With Asymptomatic Third Molars Raymond P. White, Jr, DDS, PhD,* Phoebus N. Madianos,
J Oral Maxillofac Surg 60:1234-1240, 2002 Microbial Complexes Detected in the Second/Third Molar Region in Patients With Asymptomatic Third Molars Raymond P. White, Jr, DDS, PhD,* Phoebus N. Madianos,
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
What s new for the clinician? Summaries of and excerpts from recently published papers
 http://dx.doi.org/10.17159/2519-0105/2017/v72no8a8 < 387 What s new for the clinician? Summaries of and excerpts from recently published papers SADJ September 2017, Vol 72 no 8 p387- p391 Compiled and
http://dx.doi.org/10.17159/2519-0105/2017/v72no8a8 < 387 What s new for the clinician? Summaries of and excerpts from recently published papers SADJ September 2017, Vol 72 no 8 p387- p391 Compiled and
Microbiologic and Clinical Findings of Implants in Healthy Condition and with Peri-Implantitis
 Microbiologic and Clinical Findings of Implants in Healthy Condition and with Peri-Implantitis Luigi Canullo, DDS, PhD 1 /David Peñarrocha-Oltra, DDS, MSc, PhD 2 / Ugo Covani, MD, DDS, PhD 3 /Paulo Henrique
Microbiologic and Clinical Findings of Implants in Healthy Condition and with Peri-Implantitis Luigi Canullo, DDS, PhD 1 /David Peñarrocha-Oltra, DDS, MSc, PhD 2 / Ugo Covani, MD, DDS, PhD 3 /Paulo Henrique
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Parodontitis versus Peri-Implantitis: Klinische und mikrobiologische Diagnose?
 Parodontitis versus Peri-Implantitis: Klinische und mikrobiologische Diagnose? Arndt Güntsch & Bernd W. Sigusch Parodontologie Nachrichten 1/2010 Literaturverzeichnis (1) Berglundh T, Lindhe J, Marinello
Parodontitis versus Peri-Implantitis: Klinische und mikrobiologische Diagnose? Arndt Güntsch & Bernd W. Sigusch Parodontologie Nachrichten 1/2010 Literaturverzeichnis (1) Berglundh T, Lindhe J, Marinello
Rare case of generalised aggressive periodontitis in the primary dentition
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Rare case of generalised aggressive periodontitis in the primary dentition
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2014 Rare case of generalised aggressive periodontitis in the primary dentition
Materials & Methods SRP alone vs. SRP+lasers in treatment of periodontitis 1. Study Design
 Gordon J. Christensen Clinicians Report January 2015, Volume 8 Issue 1: Addendum Materials & Methods SRP alone vs. SRP+lasers in treatment of periodontitis 1. Study Design The aim of this study was to
Gordon J. Christensen Clinicians Report January 2015, Volume 8 Issue 1: Addendum Materials & Methods SRP alone vs. SRP+lasers in treatment of periodontitis 1. Study Design The aim of this study was to
Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters
 Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters REVIEWED PAPER Most patients visiting dental surgeries suffer from various types of periodontopathies. Since
Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters REVIEWED PAPER Most patients visiting dental surgeries suffer from various types of periodontopathies. Since
Quantification of Subgingival Microflora in a Peri Implantitis Patient Using RTPCR - A Case Report
 Journal of Periodontology & Implant Dentistry Case Report Quantification of Subgingival Microflora in a Peri Implantitis Patient Using RTPCR - A Case Report Ponnudurai Samuel Ganna Prakash * Ramalingm
Journal of Periodontology & Implant Dentistry Case Report Quantification of Subgingival Microflora in a Peri Implantitis Patient Using RTPCR - A Case Report Ponnudurai Samuel Ganna Prakash * Ramalingm
Rate of cultivable subgingival periodontopathogenic bacteria in chronic periodontitis
 157 Journal of Oral Science, Vol. 46, No. 3, 157-161, 2004 Original Rate of cultivable subgingival periodontopathogenic bacteria in chronic periodontitis Mohammad Hossein Salari and Zainab Kadkhoda Department
157 Journal of Oral Science, Vol. 46, No. 3, 157-161, 2004 Original Rate of cultivable subgingival periodontopathogenic bacteria in chronic periodontitis Mohammad Hossein Salari and Zainab Kadkhoda Department
Received 18 June 2004; returned 6 August 2004; revised 1 December 2004; accepted 8 December 2004
 Journal of Antimicrobial Chemotherapy (2005) 55, 347 351 doi:10.1093/jac/dki013 Advance Access publication 4 February 2005 Concentrations and in vivo antibacterial activity of spiramycin and metronidazole
Journal of Antimicrobial Chemotherapy (2005) 55, 347 351 doi:10.1093/jac/dki013 Advance Access publication 4 February 2005 Concentrations and in vivo antibacterial activity of spiramycin and metronidazole
Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series
 Rima Jaiswal et al Case Report 10.5005/jp-journals-10012-1146 Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series 1 Rima Jaiswal, 2 S Mahantesha, 3 S Ashwini ABSTRACT Introduction:
Rima Jaiswal et al Case Report 10.5005/jp-journals-10012-1146 Reclaiming the Lost Bastion for Successful Implant Therapy: A Case Series 1 Rima Jaiswal, 2 S Mahantesha, 3 S Ashwini ABSTRACT Introduction:
Dent Clin N Am 49 (2005) Peri-implantitis
 Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Dent Clin N Am 49 (2005) 661 676 Peri-implantitis Bjo rn Klinge, DDS, Odont Dr a, *, Margareta Hultin, DDS, Odont Dr a, Tord Berglundh, DDS, Odont Dr b a Karolinska Institutet, Institute of Odontology,
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Actinobacteria, 307 308 Actinomycetes, 307 308 Actinomycosis, in oral cavity, 288 290 Aggregatibacter, 308 309 Amoxicillin, in odontogenic infections,
Note: Page numbers of article titles are in boldface type. A Actinobacteria, 307 308 Actinomycetes, 307 308 Actinomycosis, in oral cavity, 288 290 Aggregatibacter, 308 309 Amoxicillin, in odontogenic infections,
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y
 Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Periodontal conditions in patients Title dental implant treatment. Ito, T; Yasuda, M; Norizuki, Y; Sas Author(s) S; Furuya, Y; Kato, T; Yajima, Y Journal Bulletin of Tokyo Dental College, 5 URL http://hdl.handle.net/10130/2329
Dynamics of initial subgingival colonization of pristine peri-implant pockets
 Marc Quirynen Roel Vogels Wouter Peeters Daniel van Steenberghe Ignace Naert Anne Haffajee Dynamics of initial subgingival colonization of pristine peri-implant pockets Authors affiliations: Marc Quirynen,
Marc Quirynen Roel Vogels Wouter Peeters Daniel van Steenberghe Ignace Naert Anne Haffajee Dynamics of initial subgingival colonization of pristine peri-implant pockets Authors affiliations: Marc Quirynen,
Periodontal Microbiology (Dental Plaque)
 Periodontal Microbiology (Dental Plaque) Dental plaque Dental plaque is soft deposits that form the biofilm adhering to the tooth surface of other hard surface in the oral cavity, including removable and
Periodontal Microbiology (Dental Plaque) Dental plaque Dental plaque is soft deposits that form the biofilm adhering to the tooth surface of other hard surface in the oral cavity, including removable and
ARESTIN (minocycline hcl) subgingival powder
 ARESTIN (minocycline hcl) subgingival powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
ARESTIN (minocycline hcl) subgingival powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This
2017 WORLD WORKSHOP. Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March DOI: /jcpe.12957
 Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Received: 20 December 2017 Revised: 6 February 2018 Accepted: 1 March 2018 DOI: 10.1111/jcpe.12957 2017 WORLD WORKSHOP Peri implant diseases and conditions: Consensus report of workgroup 4 of the 2017
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen
![Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen Citation for published version (APA): de Waal, Y. C. M. (2015). Peri-implant infections [Groningen]: University of Groningen](/thumbs/82/86452679.jpg) University of Groningen Peri-implant infections de Waal, Yvonne IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Peri-implant infections de Waal, Yvonne IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Microbial and Genetic Testing in the Treatment of Periodontal Disease
 Microbial and Genetic Testing in the Treatment of Periodontal Disease Mr P.Renton-Harper Specialist in Periodontics prh@perio.co.uk www.perio.co.uk Periodontal Disease A bacterial infection in a susceptible
Microbial and Genetic Testing in the Treatment of Periodontal Disease Mr P.Renton-Harper Specialist in Periodontics prh@perio.co.uk www.perio.co.uk Periodontal Disease A bacterial infection in a susceptible
Mechanical Non Surgical Therapy: An Indispensable Tool
 IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
- BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis
 Journal of Periodontology & Implant Dentistry Research Article - BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis Rosaiah
Journal of Periodontology & Implant Dentistry Research Article - BANA Hydrolysis as a Comparative Tool in the Evaluation of Amoxicillin and Azithromycin in the Treatment of Chronic Periodontitis Rosaiah
Detection of Herpes Simplex Virus in Chronic Generalized Periodontitis via Polymerase Chain Reaction: A Pilot Study
 Journal of Periodontology & Implant Dentistry Research Article Detection of Herpes Simplex Virus in Chronic Generalized Periodontitis via Polymerase Chain Reaction: A Pilot Study Thomas George Veliyaveetil
Journal of Periodontology & Implant Dentistry Research Article Detection of Herpes Simplex Virus in Chronic Generalized Periodontitis via Polymerase Chain Reaction: A Pilot Study Thomas George Veliyaveetil
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis
 Journal of Dental Research, Dental Clinics, Dental Prospects Original Article Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis Zeinab
Journal of Dental Research, Dental Clinics, Dental Prospects Original Article Antimicrobial effect of chlorhexidine on Aggregatibacter actinomycetemcomitans biofilms associated with peri-implantitis Zeinab
Peri implantitis. Frank Schwarz 1* Jan Derks 2* Alberto Monje 3,4 Hom Lay Wang 4. Abstract 2017 WORLD WORKSHOP
 Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1111/jcpe.12954 2017 WORLD WORKSHOP Peri implantitis Frank Schwarz 1* Jan Derks 2* Alberto Monje 3,4 Hom Lay Wang 4
Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1111/jcpe.12954 2017 WORLD WORKSHOP Peri implantitis Frank Schwarz 1* Jan Derks 2* Alberto Monje 3,4 Hom Lay Wang 4
Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease?
 C L I N I C A L Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease? Johan Hartshorne 1 A critical appraisal of a systematic review: A. Monje, L. Aranda, K.T. Diaz,
C L I N I C A L Is peri-implant maintenance therapy (PIMT) important for preventing peri-implant disease? Johan Hartshorne 1 A critical appraisal of a systematic review: A. Monje, L. Aranda, K.T. Diaz,
Short-term evaluation of dental implants in a diabetic population: an in vivo study
 ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.3.134 Short-term evaluation of dental implants in a diabetic population: an in vivo study Athiban Inbarajan*, MDS, Padmanabhan Thallam Veeravalli,
ORIGINAL ARTICLE http://dx.doi.org/10.4047/jap.2012.4.3.134 Short-term evaluation of dental implants in a diabetic population: an in vivo study Athiban Inbarajan*, MDS, Padmanabhan Thallam Veeravalli,
actinomycetemcornitans and
 Periodontology 2000, Vol. 20, 1999, 341-362 Printed in Denmark. All rights reserved Copyright 8 Munksgaard 1999 PERIODONTOLOGY 2000 ISSN 0906-6713 Ecological considerations in the treatment of Actinobacillus
Periodontology 2000, Vol. 20, 1999, 341-362 Printed in Denmark. All rights reserved Copyright 8 Munksgaard 1999 PERIODONTOLOGY 2000 ISSN 0906-6713 Ecological considerations in the treatment of Actinobacillus
Porous titanium granules in the treatment of peri-implant osseous defects a 7-year follow-up study
 Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
The notable success of dental implants. Relationship Between Smoking and Bleeding on Probing RESEARCH
 RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
RESEARCH Relationship Between Smoking and Bleeding on Probing João Gustavo Oliveira de Souza 1 Marco Aurélio Bianchini, PhD, MSc 2 Cimara Fortes Ferreira, PhD, MSc 3 * The objective of this study was to
Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study
 G. Charalampakis Å. Leonhardt P. Rabe G. Dahlén Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study Authors affiliations: G. Charalampakis, G. Dahlén,
G. Charalampakis Å. Leonhardt P. Rabe G. Dahlén Clinical and microbiological characteristics of peri-implantitis cases: a retrospective multicentre study Authors affiliations: G. Charalampakis, G. Dahlén,
The International Journal of Periodontics & Restorative Dentistry
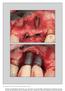 The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
The International Journal of Periodontics & Restorative Dentistry 699 A Classification System for Peri-implant Diseases and Conditions Hector L. Sarmiento, DMD, MSc 1 Michael R. Norton, BDS, FDS, RCS(Ed)
Detection of Periodontal Markers in Chronic Periodontitis
 110 The Open Dentistry Journal, 2011, 5, 110-115 Detection of Periodontal Markers in Chronic Periodontitis Open Access Åsa Leonhardt 1, *, Anette Carlén 2, Lisbeth Bengtsson 2 and Gunnar Dahlén 2 1 Student
110 The Open Dentistry Journal, 2011, 5, 110-115 Detection of Periodontal Markers in Chronic Periodontitis Open Access Åsa Leonhardt 1, *, Anette Carlén 2, Lisbeth Bengtsson 2 and Gunnar Dahlén 2 1 Student
Bacterial Analysis of Peri-implantitis and Chronic Periodontitis in Iranian Subjects
 ORIGINAL REPORT Bacterial Analysis of Peri-implantitis and Chronic Periodontitis in Iranian Subjects Ahmad Reza Ebadian 1, Mahdi Kadkhodazadeh 1, Parisa Zarnegarnia 2, and Gunnar Dahlén 3 1 Department
ORIGINAL REPORT Bacterial Analysis of Peri-implantitis and Chronic Periodontitis in Iranian Subjects Ahmad Reza Ebadian 1, Mahdi Kadkhodazadeh 1, Parisa Zarnegarnia 2, and Gunnar Dahlén 3 1 Department
Maintenance in the Periodontally Compromised Patient. Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club
 Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
Maintenance in the Periodontally Compromised Patient Dr. Van Vagianos January 22, 2009 Charlotte Dental Hygiene Study Club Periodontal Maintenance for Natural Teeth and Implants What is Periodontal Maintenance?
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature
 The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
Effect of Systemically Administered Azithromycin in Early Onset Aggressive Periodontitis
 CLINICAL AND RESEARCH REPORTS Effect of Systemically Administered Azithromycin in Early Onset Aggressive Periodontitis Takeo Fujii, Pao-Li Wang, Yoichiro Hosokawa, Shinichi Shirai, Atsumu Tamura, Kazuhiro
CLINICAL AND RESEARCH REPORTS Effect of Systemically Administered Azithromycin in Early Onset Aggressive Periodontitis Takeo Fujii, Pao-Li Wang, Yoichiro Hosokawa, Shinichi Shirai, Atsumu Tamura, Kazuhiro
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Linking Research to Clinical Practice
 Probiotics and Oral Health Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information to clinical dental
Probiotics and Oral Health Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information to clinical dental
A retrospective study on separate single-tooth implant restorations to replace two or more consecutive. maxillary posterior teeth up to 6 years.
 Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Original Article A retrospective study on separate single-tooth implant restorations to replace two or more consecutive maxillary posterior teeth up to 6 years follow up Myat Nyan Department of Prosthodontics,
Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care
 Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal
Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal
Peri-implantitis. Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
 Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1002/JPER.16-0350 2017 WORLD WORKSHOP Peri-implantitis Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
Received: 6 June 2016 Revised: 14 September 2017 Accepted: 24 September 2017 DOI: 10.1002/JPER.16-0350 2017 WORLD WORKSHOP Peri-implantitis Frank Schwarz 1 Jan Derks 2 Alberto Monje 3,4 Hom-Lay Wang 4
Interrelationship between Periodontitis and Peri-Implantitis: Myth or Reality?
 REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
REVIEW ARTICLE Rashmi Paramashivaiah 1, *, Prabhuji M.L.V 2 1 Reader, 2 Professor& HOD, Krishnadevaraya College of Dental Sciences, Bangalore-562157 *Corresponding Author: Email: rashparams2005@yahoo.co.in
Periodontal Microbiology. Dr. Csifó-Nagy Boróka Department of Periodontology Semmelweis University
 Periodontal Microbiology Dr. Csifó-Nagy Boróka Department of Periodontology Semmelweis University 2016 Topics introduction, historical perspective pathogens of destructive periodontal diseases microbial
Periodontal Microbiology Dr. Csifó-Nagy Boróka Department of Periodontology Semmelweis University 2016 Topics introduction, historical perspective pathogens of destructive periodontal diseases microbial
Periodontitis & Implants
 Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
A STUDY OF PERIODONTAL DISEASE IN CHILDREN AND ADOLESCENTS WITH TYPE 1 DIABETES SUMARRY
 A STUDY OF PERIODONTAL DISEASE IN CHILDREN AND ADOLESCENTS WITH TYPE 1 DIABETES SUMARRY INTRODUCTION Marginal periodontium is the seat of acute and chronic diseases that pose a particular problem in general
A STUDY OF PERIODONTAL DISEASE IN CHILDREN AND ADOLESCENTS WITH TYPE 1 DIABETES SUMARRY INTRODUCTION Marginal periodontium is the seat of acute and chronic diseases that pose a particular problem in general
The International Journal of Periodontics & Restorative Dentistry
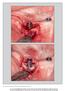 The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS
 THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS Adriana Monea, Lecturer, DMD, PhD Department of Odontology and Periodontology Faculty of Dental Medicine, UMF Tîrgu-Mureş, Romania
THE EFFICIENCY OF INITIAL PHASE TREATMENT IN CHRONIC MARGINAL PERIODONTITIS Adriana Monea, Lecturer, DMD, PhD Department of Odontology and Periodontology Faculty of Dental Medicine, UMF Tîrgu-Mureş, Romania
Transmission of periodontopathic ba Title natural teeth to implants. Okuda, K; Sato, T; Ishihara, K
 Transmission of periodontopathic ba Title natural teeth to implants. Author(s) Aoki, M; Takanashi, K; Matsukubo, T Alternative Okuda, K; Sato, T; Ishihara, K Clinical implant dentistry and rela Journal
Transmission of periodontopathic ba Title natural teeth to implants. Author(s) Aoki, M; Takanashi, K; Matsukubo, T Alternative Okuda, K; Sato, T; Ishihara, K Clinical implant dentistry and rela Journal
THE AMERICAN ACADEMY OF PERIODONTOLOGY
 THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
THE AMERICAN ACADEMY OF PERIODONTOLOGY Suite 800 737 North Michigan Avenue Chicago, Illinois 60611-2690 www.perio.org 2005 The American Academy of Periodontology PDW PERIODONTAL DISEASES what you need
NEW 12-MONTH CLINICAL STUDY RESULTS
 NEW 12-MONTH CLINICAL STUDY RESULTS March 30, 2015 Dear Oxyfresh Professional: We are thrilled to share with you the exciting results of a NEW 12-month, double blind clinical study published in the International
NEW 12-MONTH CLINICAL STUDY RESULTS March 30, 2015 Dear Oxyfresh Professional: We are thrilled to share with you the exciting results of a NEW 12-month, double blind clinical study published in the International
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
Periodontal (Gum) Disease
 Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Periodontal (Gum) Disease If you have been told you have periodontal (gum) disease, you re not alone. An estimated 80 percent of American adults currently have some form of the disease. Periodontal diseases
Periodontopathic Bacteria: A Microbiological View
 ISSN: 2319-7706 Volume 3 Number 10 (2014) pp. 873-877 http://www.ijcmas.com Review Article Periodontopathic Bacteria: A Microbiological View Bhadoria Kiran 1 *, Jana A.M 2 and Shrivastav Archana 1 1 Department
ISSN: 2319-7706 Volume 3 Number 10 (2014) pp. 873-877 http://www.ijcmas.com Review Article Periodontopathic Bacteria: A Microbiological View Bhadoria Kiran 1 *, Jana A.M 2 and Shrivastav Archana 1 1 Department
Subgingival microbiota of chronic periodontitis subjects from different geographic locations
 J Clin Periodontol 2004; 31: 996 1002 doi: 10.1111/j.1600-051X.2004.00597.x Copyright r Blackwell Munksgaard 2004 Printed in Denmark. All rights reserved Subgingival microbiota of chronic periodontitis
J Clin Periodontol 2004; 31: 996 1002 doi: 10.1111/j.1600-051X.2004.00597.x Copyright r Blackwell Munksgaard 2004 Printed in Denmark. All rights reserved Subgingival microbiota of chronic periodontitis
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta
 Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Periodontal infections Sanz, Mariano; van Winkelhoff, Arie Jan; Working Grp 1 Seventh European Wor
 University of Groningen Periodontal infections Sanz, Mariano; van Winkelhoff, Arie Jan; Working Grp 1 Seventh European Wor Published in: Journal of Clinical Periodontology DOI: 10.1111/j.1600-051X.2010.01681.x
University of Groningen Periodontal infections Sanz, Mariano; van Winkelhoff, Arie Jan; Working Grp 1 Seventh European Wor Published in: Journal of Clinical Periodontology DOI: 10.1111/j.1600-051X.2010.01681.x
Diabetes and Periodontal Disease. Brianne Neelis & Katie Torres. Literature Review 1 11/4/08
 1 Diabetes and Periodontal Disease Brianne Neelis & Katie Torres Literature Review 1 11/4/08 2 Introduction Diabetes is a cardiovascular condition that effects an estimated 20 million people in the United
1 Diabetes and Periodontal Disease Brianne Neelis & Katie Torres Literature Review 1 11/4/08 2 Introduction Diabetes is a cardiovascular condition that effects an estimated 20 million people in the United
Committee and study is carried out for one month i.e, from December 2015 January 2016.
 Association between Gram-Negative Enteric Rods, Porphyromonas gingivalis and Changes in Clinical Parameters in Chronic Periodontitis: An Observational Study Bhavya.B 1, Ashwini.S 2, Shruthi.K.R 3 Department
Association between Gram-Negative Enteric Rods, Porphyromonas gingivalis and Changes in Clinical Parameters in Chronic Periodontitis: An Observational Study Bhavya.B 1, Ashwini.S 2, Shruthi.K.R 3 Department
Interest in and studies on osseointegration
 CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
Home care. Home care. Core Values for Treating Patients in Practice. Professional care. BSP Roadshows 2008/9
 3. Periodontal Treatment BSP Roadshows 2008/9 Core Values for Treating Patients in Practice 3. Periodontal Treatment Phil Ower www.periocourses.co.uk Why is it so important? Oral hygiene methods what s
3. Periodontal Treatment BSP Roadshows 2008/9 Core Values for Treating Patients in Practice 3. Periodontal Treatment Phil Ower www.periocourses.co.uk Why is it so important? Oral hygiene methods what s
Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS
 Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS Guidelines for use of antibiotics in periodontal therapy 1. The clinical
Systemic antibiotics Vs Local antibiotics in the Treatment of Periodontal Diseases BY: ABRAHEEM JAMAL ABRAHEEM & AYOUB NAGIBB BURWEISS Guidelines for use of antibiotics in periodontal therapy 1. The clinical
THE EFFECT OF THE DIRECT COMPOSITE VENEERS RESTORATIONS ON THE MICROBIAL STATUS OF ORAL CAVITY
 THE EFFECT OF THE DIRECT COMPOSITE VENEERS RESTORATIONS ON THE MICROBIAL STATUS OF ORAL CAVITY Iamze Taboridze, Associate Professor Rusudan Ivanishvili, PhD student Grigol Robakidze University, Tbilisi,
THE EFFECT OF THE DIRECT COMPOSITE VENEERS RESTORATIONS ON THE MICROBIAL STATUS OF ORAL CAVITY Iamze Taboridze, Associate Professor Rusudan Ivanishvili, PhD student Grigol Robakidze University, Tbilisi,
Oral Health Applications for Probiotics
 Oral Health Applications for Probiotics Andrew McBain Biofilm Research Group Manchester Pharmacy School University of Manchester Overview Oral microbiology introduction Dental probiotics and replacement
Oral Health Applications for Probiotics Andrew McBain Biofilm Research Group Manchester Pharmacy School University of Manchester Overview Oral microbiology introduction Dental probiotics and replacement
TRANSMISSION OF PORPHYROMONAS GINGIVALIS FROM CAREGIVERS TO CHILDREN
 DOI: 10.5272/jimab.2012182.157 Journal of IMAB - Annual Proceeding (Scientific Papers) 2012, vol. 18, book 2 TRANSMISSION OF PORPHYROMONAS GINGIVALIS FROM CAREGIVERS TO CHILDREN Marieta D. Belcheva 1,
DOI: 10.5272/jimab.2012182.157 Journal of IMAB - Annual Proceeding (Scientific Papers) 2012, vol. 18, book 2 TRANSMISSION OF PORPHYROMONAS GINGIVALIS FROM CAREGIVERS TO CHILDREN Marieta D. Belcheva 1,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study
 Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Influence of Patient Age on the Success Rate of Dental Implants Supporting an Overdenture in an Edentulous Mandible: A 3-year Prospective Study Henny J. A. Meijer, DDS, PhD 1 /Rutger H. K. Batenburg, DDS,
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition. By: Kimberly Hawrylyshyn
 Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Staging and Grading of Periodontitis: Framework and Proposal of a New Classification and Case Definition By: Kimberly Hawrylyshyn Background Periodontitis is a microbe induced inflammatory disease that
Clinical outcomes following surgical treatment of peri-implantitis at grafted and non-grafted implant sites: a retrospective analysis
 Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Outcome of dental implants in patients with a history of periodontitis
 Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
Joint Degree Master Program of the International Medical College and the Universities Dresden, Essen, Saarland, Leipzig, Szeged and Bangkok Scientific director: Univ.-Prof. Dr. med. Dr. med. dent. Dr.
