Effect of glycine powder air-polishing as an adjunct in the treatment of peri-implant mucositis: a pilot clinical trial
|
|
|
- Willa Holmes
- 5 years ago
- Views:
Transcription
1 Ying-Jie Ji Zhi-Hui Tang Ren Wang Jie Cao Cai-Fang Cao Li-Jian Jin Effect of glycine powder air-polishing as an adjunct in the treatment of peri-implant mucositis: a pilot clinical trial Authors affiliations: Ying-Jie Ji, Zhi-Hui Tang, Ren Wang, Jie Cao, The Second Dental Center, Peking University School and Hospital of Stomatology, Beijing, China Cai-Fang Cao, Department of Periodontology, Peking University School and Hospital of Stomatology, Beijing, China Li-Jian Jin, Faculty of Dentistry, Periodontology, The University of Hong Kong, Hong Kong SAR, China Corresponding author: Zhi-Hui Tang, DDS 22 South Zhongguancun Street, Haidian District, Beijing , China Tel.: Fax: tang_zhihui@live.cn Key words: air-polishing, mechanical debridement, peri-implant mucositis Abstract Background: Glycine powder air-polishing (GPAP) has the potential to effectively erase biofilms and may improve the treatment efficacy of peri-implant mucositis. This pilot clinical trial evaluated the effect of GPAP as an adjunct in treating peri-implant mucositis. Materials and methods: Twenty-four subjects having at least one implant with peri-implant mucositis were randomly assigned to test (12 subjects with 17 implants) and control (12 subjects with 16 implants) groups. Following baseline assessment, all subjects received oral hygiene instruction and non-surgical debridement. In the test group, the sites with probing depth (PD) 4 mm were additionally treated by GPAP for 5 sec. Clinical parameters were measured at 1-week, 1-month, and 3-month recall visits. Results: At the 3-month visit, the mean reductions in PD at site level were mm and mm in the test and control groups, respectively (P < 0.05), and no significant difference existed between two groups. Mean bleeding score was also significantly reduced in both groups after the intervention. No complications or discomfort were reported during the study. Conclusions: This pilot clinical trial suggests that non-surgical mechanical debridement may effectively control peri-implant mucositis, and adjunctive GPAP treatment seems to have a limited beneficial effect as compared with mechanical debridement alone. However, further clinical trials with a large sample size are needed to confirm this preliminary observation. Date: Accepted 21 December 2012 To cite this article: Ji Y-J, Tang Z-H, Wang R, Cao J, Cao C-F, Jin L-J. Effect of glycine powder air-polishing as an adjunct in the treatment of peri-implant mucositis: a pilot clinical trial. Clin. Oral Impl. Res. 25, 2014, doi: /clr The cause effect relationship between plaque and gingivitis was demonstrated during the 1960s in the experimental gingivitis study (Loe et al. 1965). Thirty years later, a similar study found that 3 weeks of accumulated plaque around implants could also lead to peri-implant mucositis (Pontoriero et al. 1994). Histological studies on soft tissue have shown that inflammatory infiltrations in the mucosa around implants and the gingiva around natural teeth share many features (Berglundh et al. 1992; Ericsson et al. 1992; Trejo et al. 2006). However, if plaque is present for a longer time such as 3 months, the inflammatory infiltration in the peri-implant mucosa would be almost three times greater than in the dentogingival unit (Ericsson et al. 1992; Heitz-Mayfield & Lang 2010). Studies on animal models have also shown bone loss induced by plaque, which are accumulated by ligature (Hurzeler et al. 1995; Marinello et al. 1995; Persson et al. 1996; Isidor 1997). Due to lack of long-term investigation, the relationship between peri-implant mucositis and peri-implantitis remains obscure. However, according to some experts, peri-mucositis, which appears to be a sign of host response to bacterial burden, might be the precursor for peri-implantitis (Heitz-Mayfield et al. 2011; Lang et al. 2011). Therefore, early diagnosis and intervention are of great clinical importance in management of peri-implant infections. Nevertheless, few clinical studies have examined the procedure for treating peri-implant mucositis (Heitz-Mayfield & Lang 2004; Renvert et al. 2008; Maximo et al. 2009; Thone-Muhling et al. 2010; Heitz- Mayfield et al. 2011). Although clinical improvement can be gained through mechanical debridement, there is still quite a high proportion of sites with deep pocket and bleeding tendencies on probing (Ciancio et al. 1995; Strooker et al. 1998; Porras et al. 2002; Lindhe & Meyle 2008; Thone-Muhling et al John Wiley & Sons A/S. Published by Blackwell Publishing Ltd 683
2 2010; Heitz-Mayfield et al. 2011). Adjunctive methods, such as mouth rinse and local antiseptic gel, designed to enhance clinical outcomes have, however, failed to show any additional effect (Ciancio et al. 1995; Strooker et al. 1998; Porras et al. 2002; Lindhe & Meyle 2008; Thone-Muhling et al. 2010; Heitz- Mayfield et al. 2011). Recently, air-polishing devices (APD) have been shown to be a feasible treatment option in periodontal care (Petersilka et al. 2003a,b, c; Moene et al. 2010; Wennstrom et al. 2011). As the initiation of peri-implant mucositis is similarly dependent on the presence of biofilms, APD may potentially be applied in peri-implant cases (Sahrmann et al. 2012). Glycine powder, which is a non-toxic and water-soluble amino acid, has been shown not to change the implant surface profile under scanning electronic microscope (SEM) (Schwarz et al. 2009). Clinical studies have revealed significant improvements in probing depth (PD), bleeding on probing (BOP), and microbiological tests when treating periimplantitis with glycine powder air-polishing (GPAP) (Maximo et al. 2009; Renvert et al. 2011; Sahm et al. 2011). However, it is still argued that GPAP does not show superior results to other methods, such as manual curettes, ultrasonic scalers, and erbium-doped yttrium aluminum garnet (Er: YAG) laser treatment (Maximo et al. 2009; Renvert et al. 2011; Sahm et al. 2011). Nevertheless, no study has been carried out to investigate the effect of APD using glycine powder as an adjunctive method to treat peri-implant mucositis. This pilot clinical trial evaluated the effect of GPAP as an adjunct in the treatment of peri-implant mucositis. Materials and methods The study was a single-blind, randomized, 3-month clinical trial. All the procedures were performed in Beijing, China, from 2010 to The research protocol was approved by the Ethics Committee of Peking University Health Science Center prior to the study. Study population The enrolled subjects were patients who had received implant treatment at least 1 year before at Peking University School & Hospital of Stomatology. Reasons for missing teeth included caries, trauma, congenital missing, or root fracture as previously recorded. The remaining dentition was either periodontally healthy, with gingivitis, or moderate chronic periodontitis (Armitage 1999). Subjects with teeth extracted due to poor periodontal prognosis or who had aggressive or advanced periodontitis were excluded from this study. Participants had to meet the following inclusion criteria: at least one implant site with PD 4 mm and BOP positive; molar or premolar site; no detectable loss of supporting bone as compared with periapical radiographs immediately after restoration. To avoid a range of different implant systems, only one system (ITI â Straumann â, Standard Implant, SLA surface, Waldenburg, Switzerland) was selected. For those with more than one implant, all implants that met the inclusive criteria were analyzed in the study. Subjects who were smokers and who had systemic diseases (e.g., diabetes mellitus and osteoporosis) that might affect the study outcomes were also excluded from the study. Furthermore, those who had received any peri-implant treatment within the last 6 months and those who needed antibiotic treatment were excluded. Clinical measurements and procedures An initial questionnaire containing information about personal particulars, oral habits, and systemic conditions was completed by each participant. Periapical radiographs were taken to detect any loss of supporting bone. Each participant was given an explanation of the study, and a written consent form was obtained before treatment. Then, the implant(s) and the remaining teeth were both checked, and PD, modified plaque index (mpli), and bleeding index (BI) were recorded on a chart. All the examinations were performed by the same trained and calibrated operator (J.Y.J). The following parameters were evaluated at six sites (mesio, medio, disto/buccal, and lingual) of implants using a manual probe ( , PQ-W, Williams, SILVER by Hu-Friedy, Chicago, IL, USA). mpli was graded as follows: (0) no detection of plaque, (1) plaque recognized only by running a probe across a smooth marginal surface of the implant, (2) plaque can be seen at a glance, (3) abundance of soft matter (Mombelli et al. 1987; Mayfield et al. 1998). PD was measured under N force, to the nearest scale (Lindhe & Meyle 2008; Gerber et al. 2009). BI scores were assessed 30 sec after probing: (0) no bleeding, (1) point of bleeding, (2) line of bleeding, (3) drop of bleeding (Renvert et al. 2011). Treatment protocol After baseline examination, the participants were instructed and motivated in oral hygiene practice and then received non-surgical treatment including supra-gingival scaling, root debridement, and polishing according to their periodontal conditions. Before grouping, all the implants were treated by the examiner (J.Y.J.) using ultrasonic scaler with carbon fiber tips (Satelec â P5 ultrasonic scaling machine and PH2L, PH2R tips, Newtron, France). This instrumentation procedure was carried out until the operator felt it was adequate rather than for a defined time. Then, subjects were randomly assigned to the test (GPAP) or control group. Randomization was performed by the toss of a coin (Needleman et al. 2005; Chondros et al. 2009). The allocation was based on subject level, which meant that if there were more than one implant in one individual, all the implants would receive the same treatment modality. The allocation and additional air-polishing procedure were accomplished in an isolated dental room by an operator (C.J.), which was concealed from the examiner (J.Y.J.). Only implants in the test group were further treated by the GPAP (AIR-FLOW master â and AIR-FLOW Perio â, EMS, Nyon, Switzerland). The water and powder were set to medium as a default when the machine was switched on. The outlet of the appliance handpiece was connected to a disposable subgingival nozzle. The nozzle was inserted deep into the pockets with PD 4 mm until resistance was felt, and then the pedal was pressed for 5 sec on each site (Fig. 1). All airpolishing procedures were performed by the same operator (C.J.) who was not involved in clinical examination and data collection, and the study subjects were asked not to discuss their treatment with the examiner until the end of the study. All the treatments, both on implants and natural teeth, were accomplished within the first visit in both groups. During the follow-up visits, oral hygiene instruction (OHI) was reinforced when necessary. PD were re-examined at the 1- and 3-month post-treatment visits. mpli and BI were Fig. 1. Clinical photograph of GPAP usage with a disposable nozzle. 684 Clin. Oral Impl. Res. 25, 2014 / John Wiley & Sons A/S. Published by Blackwell Publishing Ltd
3 recorded at the 1-week, 1-month, and 3-month visits. Adverse events and complaints of discomfort were recorded if any. Intra-examiner reproducibility Five subjects were randomly selected for the assessment of intra-examiner (J.Y.J.) reproducibility. After baseline PD examination, treatment on remaining dentition was carried out, which usually lasted 1 h. Then, before any treatment on the implants, they were probed again for calibration. The weighted kappa analysis was applied, and the reproducibility was 69%. Statistical analysis The statistical analysis was performed with commercially available software (SPSS, version 14.0, SPSS Inc., Chicago, IL, USA). Mean values and standard deviations (mean SD) for the clinical parameters were calculated. Data for both subject level and treated site level were obtained. Fisher s exact test was applied in baseline comparison. At subject level, mean data were calculated using an average of all sites around the implant(s) for each participant. At treated site level, however, only data on deep pockets with PD 4 mm were used and analyzed. Independent and pairwise t-tests were applied. Mixed-effect and longitudinal analysis was also carried out by R (version ) and nparld (version 2.1). The difference with a P-value <0.05 was considered statistically significant. Table 1. Baseline demographics and clinical examination results for subjects in two groups Background GPAP group (N = 12) Control group (N = 12) P-value Mean age (years) Female 50% 67% Periodontal condition Healthy 0 1 (8%) Gingivitis 8 (66.7%) 7 (58.3%) Periodontitis 4 (33.3%) 4 (33.3%) Connected crown Oral hygiene habit Brushing frequency (per day) ID brushing (user) 4 (33%) 6 (50%) Flossing (user) 6 (50%) 7 (58%) Mouth rinse (user) 5 (42%) 3 (25%) Number of subjects with One implant 7 8 Two implants 5 4 Probing depth ( SD) 3.6 (0.47) 3.5 (0.50) Bleeding index (mean SD) 1.4(0.57) 1.5(0.65) Modified plaque index (mean SD) 1.2(0.85) 0.6(0.40) N, number of subjects; connected crown includes connected crown and crown with a pontic; SD, standard deviation; P < 0.05 was bold. Table 2. Probing depth SD at baseline, 1 month, and 3 months in both groups PD (SD) (mm) Baseline 1-month N/n D P-value 1 3-month N/n D P-value 2 GPAP Group S 3.6 (0.47) 3.2 (0.52) (0.48) TS 4.6 (0.50) 3.8 (1.0) < (0.95) <0.001 Control Group S 3.5 (0.50) 3.3 (0.26) (0.38) TS 4.5 (0.55) 3.8 (1.0) < (1.0) <0.001 P-value 3 S TS PD, probing depth; SD, standard deviation; S, subject level; TS, treated site level; N, number of subjects; n, number of treated sites; D, difference between 1 month and baseline; D, difference between 3 months and baseline; P-value 1 and P-value 2 are the results analyzed from 1 month to baseline and 3 months to baseline within one group, respectively; P-value 3 is the result analyzed between two groups at subject level and site level, respectively; P < 0.05 was bold. Results Twelve subjects (17 implants) in the GPAP group and 12 subjects (16 implants) in the control group were enrolled in this study. No subject with more than two implants was included. Data from the 1-week and 1-month follow-ups were missing in one and two subjects, respectively. No complaint of discomfort was reported after any treatment. Baseline demographic characteristics were collected at the first visit and are presented in Table 1. The two groups were evenly distributed in terms of age, sex, periodontal condition, prosthesis pattern, and oral hygiene habits, except for mpli, which was higher in the GPAP group than in the control. Probing depth changes Mean values of PD at subject and site levels are shown in Table 2. At subject level, 1-month and 3-month data in the GPAP group and 3-month data in the control group showed significant PD reductions. The Fig. 2. Probing depth changes in the GPAP group and control group. GPAP Glycine powder air-polishing; S subject level; TS treated site level. 3-month reductions were mm and mm in the GPAP and control group, respectively. No significant difference was found within any visit between the two groups. At treated site level, significant PD reductions were shown at the 1- and 3-month points as compared with the baseline (P-value < 0.001). At the 3-month point, the reductions were mm in the GPAP group and mm in the 2013 John Wiley & Sons A/S. Published by Blackwell Publishing Ltd 685 Clin. Oral Impl. Res. 25, 2014 /
4 Table 3. Modified plaque index levels at baseline, 1-week, 1- and 3-month in both groups mpli (SD) Baseline 1-week N/n P-value * 1-month N/n P-value 3-months N/n P value GPAP Group S 1.2 (0.85) 0.7 (0.62) (0.57) 10 < (0.32) TS 1.4 (1.06) 0.7 (0.81) (0.60) 36 < (0.61) 46 <0.001 Control Group S 0.6 (0.40) 0.5 (0.35) (0.46) (0.38) TS 0.6 (0.68) 0.5 (0.60) (0.65) (0.53) p-value S TS < mpli, modified plaque index; SD, standard deviation; S, subject level; TS, treated site level; N, number of subjects; n, number of treated sites. *,, P-value are the results analyzed from 1-week to baseline, 1-month to baseline and 3-month to baseline, respectively, within one group. P-value is the result analyzed between two groups at subject level and site level respectively; P < 0.05 was bold. control group. No significant difference was detected within the two groups at any visit. Fig. 2 describes the PD changes according to different time points. Plaque index changes Mean values of mpli were calculated from subject data and are presented in Table 3. The GPAP group had higher mpli score than the control group at baseline, which was statistically significant (P = 0.030). Significant mpli improvement was shown at the 1-month visit in the GPAP group as compared with baseline. However, in the control group, mpli was comparable with baseline in all the visits. Plaque index was also analyzed at treated sites. Levels of mpli in the GPAP group were significantly higher than in the control group at baseline. mpli levels in the GPAP group were shown to have reduced significantly at all the follow-up visits. In the control group, however, only data from the 3-month visit showed significant reduction as compared with baseline. Fig. 3 shows the changes in mpli levels according to different visits. Bleeding index changes Mean values of BI were calculated at both subject and site levels, and the outcomes are listed in Table 4. Independent and pairwise comparisons showed that BI levels were significantly reduced only at the 1-week point in both groups. At treated site level, there was a significant reduction in BI at all the visits. Additionally, at the 1-week point, the control group demonstrated a significantly greater BI reduction than the GPAP group (P = 0.013). The changes in BI levels over time course are shown in Fig % and 29.3% of sites turned BOP negative at 3-month point, for the control and GPAP groups, respectively (P = 0.010). Mixed-effect and longitudinal analysis Brunner and Langer models were followed to analyze the repeated measurements over time. There were no significant difference in PD, BI, and mpli between two groups among all visits, and the P-values were 0.74, 0.26, and 0.08, respectively. However, PD, BI and mpli in both groups had significant improvement over time course (P-values < 0.001). Fig. 3. Modified plaque index level changes in the GPAP group and control group. GPAP Glycine powder air-polishing; S subject level; TS treated site level. Discussion As implant insertion to replace missing teeth is increasing from the past decade, attention has been naturally focused on peri-implant supportive care. Reports show that the prevalence of peri-implant mucositis occurs in up to 80% of patients and 50% of implant sites. Peri-implantitis was identified in 28% and 56% of subjects and in 12% and 43% of implant sites in two different studies, respectively (Renvert et al. 2008). Therefore, there is clearly a need to identify an effective method of controlling peri-implant infections. Implants in the anterior region were excluded from this study to avoid esthetic considerations that might affect the results. Unlike previous studies, in which only subjects with good oral hygiene were recruited, in our study no limit in plaque index at baseline was set (Heitz-Mayfield et al. 2011, 2012). Participants improved their levels of oral hygiene during the course of the study. This was thought to be more realistic to clinical practice. In terms of the statistical analysis, data were first analyzed at subject level. Participants background and clinical parameters were compared between the two groups at baseline. Each subject was treated as a unit. However, only deep sites with PD 4mm were treated by GPAP in the test group, and this minor effect might be diluted by shallow pockets. Therefore, site-level analysis was applied as well. Finally, mixed-effect and longitudinal analysis was used to evaluate the effects of GPAP over time. Mechanical debridement with or without GPAP demonstrated significant reduction in PD and BI; therefore, both were effective in reducing peri-implant mucositis. When comparing these two, however, only at the 1-week point, did the control group demonstrate greater BI reduction. Similar results were reported by another study on natural teeth, which showed a higher percentage of BOP positive sites on Day 7 after the GPAP treat- 686 Clin. Oral Impl. Res. 25, 2014 / John Wiley & Sons A/S. Published by Blackwell Publishing Ltd
5 Table 4. Bleeding index at baseline, 1-week, 1 month, and 3 months in both groups BI (SD) Baseline 1 week N/n P-value 1 1 month N/n P-value 2 3 months N/n P-value 3 GPAP Group S 1.4 (0.57) 0.8 (0.53) (0.91) (0.58) TS 1.7 (0.93) 1.0 (1.0) 46 < (1.2) (0.98) Control Group S 1.5 (0.65) 0.5 (0.25) (0.50) (0.85) TS 1.7 (1.0) 0.5 (0.67) 43 < (0.95) 46 < (1.1) 46 <0.001 P-value 4 S TS BI, bleeding index; GPAP, Glycine powder air-polishing; SD, standard deviation; S, subject level; TS, treated site level; N, number of subjects; n, number of treated sites; P-value 1, P-value 2 and P-value 3 are the results analyzed from 1 week to baseline, 1 month to baseline, and 3 months to baseline, respectively, within one group; P-value 4 is the result analyzed between two groups at subject level and site level, respectively; P < 0.05 was bold. Fig. 4. Bleeding index changes in the GPAP group and control group. GPAP Glycine powder air-polishing; S subject level; TS treated site level. ment as compared with a scaling and root planing (SRP) group (Moene et al. 2010). This might be caused by the damage to the mucosa from high-pressure glycine slurry. One histological study has investigated the trauma from the glycine powder hitting the gingiva when GPAP was used. Biopsies from the gingiva showed that the superficial parakeratinized layer was only slightly detached (Petersilka et al. 2008). However, in the present study, the distance between the slurry and pocket surface was so close that they almost touched, so the damage was more intensive although the nozzle usage would have meant a large decrease in slurry pressure. Interestingly, at 3-month visit, 42.1% and 29.3% of sites turned BOP negative for the control and GPAP groups, respectively, where the peri-mucositis has been completely resolved (P = 0.010). Further study is required to elaborate this point. In a study of anti-infective treatment of peri-implant mucositis, mechanical debridement alone was shown to lead to a 0.63-mm PD reduction after 3 months (Heitz-Mayfield et al. 2011). Porras and his colleagues reported a 0.93-mm PD reduction 3 months after mechanical cleansing and OHI, which was comparable with our study (Porras et al. 2002). In another trial aiming to compare two full-mouth approaches to treating periimplant mucositis, PD reduction reached 0.23 mm in a full-mouth scaling without chlorhexidine (Thone-Muhling et al. 2010). As these are the first data so far using GPAP as an adjunctive treatment in peri-implant mucositis, it is hard to compare them with other studies. Mixed-effect and regression analysis showed deeper PD at baseline led to greater PD reductions. Interestingly, the result also showed that lower BI levels tended to have greater PD reductions after therapy. It should be noted that the effects reported in this study may be mainly due to ultrasonic debridement plus oral hygiene improvement. Although there were significant improvements in PD and BI through treatment, not all the deep pockets and bleeding sites were eliminated. The same outcomes have been reported in other studies (Porras et al. 2002; Thone-Muhling et al. 2010; Heitz-Mayfield et al. 2011). Explanations may be as follows. Firstly, the submucosal margin has a negative effect on PD reduction. A multiple regression analysis carried out in one study found the submucosal margin of restoration at baseline had a negative effect on pocket reduction (Heitz-Mayfield et al. 2011). Unfortunately, information on sub- or supra-mucosal margins was not recorded in this study. However, based on the authors observation, most of the implants had submucosal margins. Secondly, excellent plaque control was not acquired even after three sessions of OHI reinforcements, which was evident in the large amount of visible plaque in several subjects. Thirdly, there may be host response heterogeneity to plaque and treatment provided. Considering the insignificant adjunctive effect of GPAP, it may be possible that mechanical debridement is fairly effective at removing the plaque biofilms in peri-implant mucositis. Hence, in situations with deep pockets, narrow defects, or implant threads exposure where conventional mechanical debridement is hard to eliminate pathogenic biofilms, GPAP may show some additional effects (Sahrmann et al. 2012; Schar et al. 2013). Another possibility is that the power setting in our study was too mild to remove biofilms and hence not enough to show clinically significant improvement. The 5-sec duration for each site was adopted in this study based on previous studies and the recommendation of the manufacturer (Petersilka et al. 2003a,b,c; Sahm et al. 2011). The complication of emphysema was not reported in this trial. It was shown that treating each site with GPAP for 5 sec is safe in peri-implant mucositis. Another concern is 2013 John Wiley & Sons A/S. Published by Blackwell Publishing Ltd 687 Clin. Oral Impl. Res. 25, 2014 /
6 possible GPAP damage to the implant surface. An in vitro study has shown that GPAP would not cause visible changes to either smooth or sand-blasted, large grit, and acidattacked (SLA) surfaces under SEM (Schwarz et al. 2009). In conclusion, within the limitations of the study, this pilot clinical trial suggests that non-surgical mechanical debridement may effectively control peri-implant mucositis and adjunctive GPAP treatment seems to have a limited beneficial effect as compared with mechanical debridement alone. However, further clinical trials with a large sample size are needed to confirm this preliminary observation. Acknowledgements: We are grateful to the colleagues of the program for their support and comments during the preparation of this manuscript. We thank Dr. Li Xueying (Bio-statistic Department of The First Hospital of Peking University) for her help with the data analysis, and the staff of the JianDe United Dental Equipment Co. for providing EMS AIR-FLOW master â and AIR-FLOW Perio â powder. References Armitage, G.C. (1999) Development of a classification system for periodontal diseases and conditions. Annals of Periodontology 4: 1 6. Berglundh, T., Lindhe, J., Marinello, C., Ericsson, I. & Liljenberg, B. (1992) Soft tissue reaction to de novo plaque formation on implants and teeth. An experimental study in the dog. Clinical Oral Implants Research 3: 1 8. Chondros, P., Nikolidakis, D., Christodoulides, N., Rossler, R., Gutknecht, N. & Sculean, A. (2009) Photodynamic therapy as adjunct to non-surgical periodontal treatment in patients on periodontal maintenance: a randomized controlled clinical trial. Lasers in Medical Science 24: Ciancio, S.G., Lauciello, F., Shibly, O., Vitello, M. & Mather, M. (1995) The effect of an antiseptic mouthrinse on implant maintenance: plaque and peri-implant gingival tissues. Journal of Periodontology 66: Ericsson, I., Berglundh, T., Marinello, C., Liljenberg, B. & Lindhe, J. (1992) Long-standing plaque and gingivitis at implants and teeth in the dog. Clinical Oral Implants Research 3: Gerber, J.A., Tan, W.C., Balmer, T.E., Salvi, G.E. & Lang, N.P. (2009) Bleeding on probing and pocket probing depth in relation to probing pressure and mucosal health around oral implants. Clinical Oral Implants Research 20: Heitz-Mayfield, L.J. & Lang, N.P. (2004) Antimicrobial treatment of peri-implant diseases. International Journal of Oral and Maxillofacial Implants 19(Suppl.): Heitz-Mayfield, L.J. & Lang, N.P. (2010) Comparative biology of chronic and aggressive periodontitis vs. Peri-implantitis. Periodontology : Heitz-Mayfield, L.J., Salvi, G.E., Botticelli, D., Mombelli, A., Faddy, M. & Lang, N.P. (2011) Anti-infective treatment of peri-implant mucositis: a randomised controlled clinical trial. Clinical Oral Implants Research 22: Heitz-Mayfield, L.J., Salvi, G.E., Mombelli, A., Faddy, M. & Lang, N.P. (2012) Anti-infective surgical therapy of peri-implantitis. A 12-month prospective clinical study. Clinical Oral Implants Research 23: Hurzeler, M.B., Quinones, C.R., Morrison, E.C. & Caffesse, R.G. (1995) Treatment of peri-implantitis using guided bone regeneration and bone grafts, alone or in combination, in beagle dogs. Part 1: clinical findings and histologic observations. International Journal of Oral and Maxillofacial Implants 10: Isidor, F. (1997) Clinical probing and radiographic assessment in relation to the histologic bone level at oral implants in monkeys. Clinical Oral Implants Research 8: Lang, N.P., Bosshardt, D.D. & Lulic, M. (2011) Do mucositis lesions around implants differ from gingivitis lesions around teeth? Journal of Clinical Periodontology 38(Suppl. 11): Lindhe, J. & Meyle, J. (2008) Peri-implant diseases: consensus report of the sixth european workshop on periodontology. Journal of Clinical Periodontology 35: Loe, H., Theilade, E. & Jensen, S.B. (1965) Experimental gingivitis in man. Journal of Periodontology 36: Marinello, C.P., Berglundh, T., Ericsson, I., Klinge, B., Glantz, P.O. & Lindhe, J. (1995) Resolution of ligature-induced peri-implantitis lesions in the dog. Journal of Clinical Periodontology 22: Maximo, M.B., de Mendonca, A.C., Renata, S.V., Figueiredo, L.C., Feres, M. & Duarte, P.M. (2009) Short-term clinical and microbiological evaluations of peri-implant diseases before and after mechanical anti-infective therapies. Clinical Oral Implants Research 20: Mayfield, L., Skoglund, A., Nobreus, N. & Attstrom, R. (1998) Clinical and radiographic evaluation, following delivery of fixed reconstructions, at gbr treated titanium fixtures. Clinical Oral Implants Research 9: Moene, R., Decaillet, F., Andersen, E. & Mombelli, A. (2010) Subgingival plaque removal using a new air-polishing device. Journal of Periodontology 81: Mombelli, A., van Oosten, M.A., Schurch, E.J. & Land, N.P. (1987) The microbiota associated with successful or failing osseointegrated titanium implants. Oral Microbiology and Immunology 2: Needleman, I., Moles, D.R. & Worthington, H. (2005) Evidence-based periodontology, systematic reviews and research quality. Periodontology : Persson, L.G., Ericsson, I., Berglundh, T. & Lindhe, J. (1996) Guided bone regeneration in the treatment of periimplantitis. Clinical Oral Implants Research 7: Petersilka, G.J., Bell, M., Haberlein, I., Mehl, A., Hickel, R. & Flemmig, T.F. (2003a) In vitro evaluation of novel low abrasive air polishing powders. Journal of Clinical Periodontology 30: Petersilka, G., Faggion, C.J., Stratmann, U., Gerss, J., Ehmke, B., Haeberlein, I. & Flemmig, T.F. (2008) Effect of glycine powder air-polishing on the gingiva. Journal of Clinical Periodontology 35: Petersilka, G.J., Steinmann, D., Haberlein, I., Heinecke, A. & Flemmig, T.F. (2003c) Subgingival plaque removal in buccal and lingual sites using a novel low abrasive air-polishing powder. Journal of Clinical Periodontology 30: Petersilka, G.J., Tunkel, J., Barakos, K., Heinecke, A., Haberlein, I. & Flemmig, T.F. (2003b) Subgingival plaque removal at interdental sites using a low-abrasive air polishing powder. Journal of Periodontology 74: Pontoriero, R., Tonelli, M.P., Carnevale, G., Mombelli, A., Nyman, S.R. & Lang, N.P. (1994) Experimentally induced peri-implant mucositis. A clinical study in humans. Clinical Oral Implants Research 5: Porras, R., Anderson, G.B., Caffesse, R., Narendran, S. & Trejo, P.M. (2002) Clinical response to 2 different therapeutic regimens to treat peri-implant mucositis. Journal of Periodontology 73: Renvert, S., Lindahl, C., Roos, J.A. & Persson, G.R. (2011) Treatment of peri-implantitis using an er: yag laser or an air-abrasive device: a randomized clinical trial. Journal of Clinical Periodontology 38: Renvert, S., Roos-Jansaker, A.M. & Claffey, N. (2008) Non-surgical treatment of peri-implant mucositis and peri-implantitis: a literature review. Journal of Clinical Periodontology 35: Sahm, N., Becker, J., Santel, T. & Schwarz, F. (2011) Non-surgical treatment of peri-implantitis using an air-abrasive device or mechanical debridement and local application of chlorhexidine: a prospective, randomized, controlled clinical study. Journal of Clinical Periodontology 38: Sahrmann, P., Ronay, V., Sener, B., Jung, R.E., Attin, T. & Schmidlin, P.R. (2012) Cleaning potential of glycine air-flow application in an in vitro peri-implantitis model. Clinical Oral Implants Research, doi: /j x. Schar, D., Ramseier, C.A., Eick, S., Arweiler, N.B., Sculean, A. & Salvi, G.E. (2013) Anti-infective therapy of peri-implantitis with adjunctive local drug delivery or photodynamic therapy: six-month outcomes of a prospective randomized clinical trial. Clinical Oral Implants Research 24: Schwarz, F., Ferrari, D., Popovski, K., Hartig, B. & Becker, J. (2009) Influence of different air-abrasive 688 Clin. Oral Impl. Res. 25, 2014 / John Wiley & Sons A/S. Published by Blackwell Publishing Ltd
7 powders on cell viability at biologically contaminated titanium dental implants surfaces. Journal of Biomedical Materials Research. Part B, Applied Biomaterials 88: Strooker, H., Rohn, S. & Van Winkelhoff, A.J. (1998) Clinical and microbiologic effects of chemical versus mechanical cleansing in professional supportive implant therapy. International Journal of Oral and Maxillofacial Implants 13: Thone-Muhling, M., Swierkot, K., Nonnenmacher, C., Mutters, R., Flores-de-Jacoby, L. & Mengel, R. (2010) Comparison of two full-mouth approaches in the treatment of peri-implant mucositis: a pilot study. Clinical Oral Implants Research 21: Trejo, P.M., Bonaventura, G., Weng, D., Caffesse, R.G., Bragger, U. & Lang, N.P. (2006) Effect of mechanical and antiseptic therapy on peri-implant mucositis: an experimental study in monkeys. Clinical Oral Implants Research 17: Wennstrom, J.L., Dahlen, G. & Ramberg, P. (2011) Subgingival debridement of periodontal pockets by air polishing in comparison with ultrasonic instrumentation during maintenance therapy. Journal of Clinical Periodontology 38: Supporting Information Additional Supporting Information may be found in the online version of this article: Fig. S1. A CONSORT flowchart of the enrollment, allocation, follow-up and analysis John Wiley & Sons A/S. Published by Blackwell Publishing Ltd 689 Clin. Oral Impl. Res. 25, 2014 /
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of
 Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Persson GR, Salvi GE, Heitz-Mayfield LJA et al. Antimicrobial therapy using a local drug delivery system (Arestin) in the treatment of peri-implantitis I: microbiological outcomes. Clin Oral Imp Res 2006;
Please visit the C.E. Pavilion to validate your course attendance Or If There s a Line Go cdapresents.com
 UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
UCLA Innovations 2016 CDA Presents in Anaheim Tara Aghaloo, DDS, MD, PhD Dean Ho, MS, PhD Jay Jayanetti Eric C. Sung, DDS David T. W. Wong, DMD, DMSc Benjamin M. Wu, DDS, PhD Saturday, May 14, 2016 8:00
Case Presentation. Overall Health. Oral Hygiene. Chief Complaint. I hate my upper denture. I can t taste food. I want an implant solution
 Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Case Presentation Medical History Age & Gender 62 years old female Peri-implant Osteitis Overall Health Good Hx of Smoking 5 cigarets per day (Peri-implantitis) Oral Hygiene Fair Systemic Disease Osteoarthritis
Subgingival Air Polishing in Dentistry
 Western Kentucky University TopSCHOLAR Honors College Capstone Experience/Thesis Projects Honors College at WKU 5-7-2015 Subgingival Air Polishing in Dentistry Chelsea T-P. Howell Western Kentucky University,
Western Kentucky University TopSCHOLAR Honors College Capstone Experience/Thesis Projects Honors College at WKU 5-7-2015 Subgingival Air Polishing in Dentistry Chelsea T-P. Howell Western Kentucky University,
Clinpro Glycine Prophy Powder
 Clinpro Glycine Prophy Powder 3M 2016. All Rights Reserved VIDEO 3M 2016. All Rights Reserved 2 Presentation Overview Air Polishing Procedure With Clinpro Glyciene Prophy Powder Use and Efficiency for
Clinpro Glycine Prophy Powder 3M 2016. All Rights Reserved VIDEO 3M 2016. All Rights Reserved 2 Presentation Overview Air Polishing Procedure With Clinpro Glyciene Prophy Powder Use and Efficiency for
Product Information Clinpro Prophy Powder 4 Bottles à 100 g
 Ordering Information Item No. Product Information 671 Clinpro Prophy Powder 4 Bottles à 1 g Clinpro Prophy Powder 12613 Clinpro Prophy Paste 2 à 2 g Cherry Fine 12657 Clinpro Prophy Paste 2 à 2 g Mint
Ordering Information Item No. Product Information 671 Clinpro Prophy Powder 4 Bottles à 1 g Clinpro Prophy Powder 12613 Clinpro Prophy Paste 2 à 2 g Cherry Fine 12657 Clinpro Prophy Paste 2 à 2 g Mint
Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology
 Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Article Periimplant diseases: where are we now? Consensus of the Seventh European Workshop on Periodontology LANG, Niklaus P, BERGLUNDH, Tord, MOMBELLI, Andrea Abstract Peri-implant diseases present in
Frank Schwarz *, Andrea Schmucker and Jürgen Becker
 Schwarz et al. International Journal of Implant Dentistry (2015) 1:22 DOI 10.1186/s40729-015-0023-1 REVIEW Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis
Schwarz et al. International Journal of Implant Dentistry (2015) 1:22 DOI 10.1186/s40729-015-0023-1 REVIEW Efficacy of alternative or adjunctive measures to conventional treatment of peri-implant mucositis
Factors influencing severity of periimplantitis
 Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
Martin Saaby Eva Karring Søren Schou Flemming Isidor Factors influencing severity of periimplantitis Authors affiliations: Martin Saaby, Søren Schou, Section for Oral and Maxillofacial Surgery and Oral
As an increasing number of
 LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
LITERATURE REVIEWS Understanding Peri-implantitis: A Strategic Review Preetinder Singh, MDS* The high survival rate of osseointegrated dental implants is well documented, but it is becoming increasingly
The International Journal of Periodontics & Restorative Dentistry
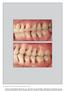 The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
The International Journal of Periodontics & Restorative Dentistry 395 Clinical Case Report on Treatment of Generalized Aggressive Periodontitis: 5-Year Follow-up Kai-Fang Hu, DDS, MD 1 /Ya-Ping Ho, DDS,
Û mectron Air-Polishing
 new! Û perio function Û mectron Air-Polishing 2 Û combi The new multi-talented prophylaxis unit offers several treatment options. The powerful, well controlled ultrasound allows gentle scaling. Over 40
new! Û perio function Û mectron Air-Polishing 2 Û combi The new multi-talented prophylaxis unit offers several treatment options. The powerful, well controlled ultrasound allows gentle scaling. Over 40
photodynamic therapy, surface decontamination
 Dorothee Schär Christoph A. Ramseier Sigrun Eick Nicole B. Arweiler Anton Sculean Giovanni E. Salvi Anti-infective therapy of peri-implantitis with adjunctive local drug delivery or photodynamic therapy:
Dorothee Schär Christoph A. Ramseier Sigrun Eick Nicole B. Arweiler Anton Sculean Giovanni E. Salvi Anti-infective therapy of peri-implantitis with adjunctive local drug delivery or photodynamic therapy:
Department of Oral Surgery, Heinrich Heine University, D Düsseldorf, Germany.
 Lasers Surg Med. 2007 Jun;39(5):428-40 Immunohistochemical characterization of periodontal wound healing following nonsurgical treatment with fluorescence controlled Er:YAG laser radiation in dogs. Schwarz
Lasers Surg Med. 2007 Jun;39(5):428-40 Immunohistochemical characterization of periodontal wound healing following nonsurgical treatment with fluorescence controlled Er:YAG laser radiation in dogs. Schwarz
Perio Reports Vol. 26 No. 1. Polishing. January page 2. page 1
 Polishing page 1 Perio Reports Vol. 26 No. 1 page 2 January 2014 20% Register Now & Save off tuition Don t Miss These Keynote Speakers Dr. Michael Abernathy Mark Dilatush and Howie Horrocks Dr. Howard
Polishing page 1 Perio Reports Vol. 26 No. 1 page 2 January 2014 20% Register Now & Save off tuition Don t Miss These Keynote Speakers Dr. Michael Abernathy Mark Dilatush and Howie Horrocks Dr. Howard
Primary prevention of periimplantitis: peri-implant mucositis S152
 J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
J Clin Periodontol 2015; 42 (Suppl. 16): S152 S157 doi: 10.1111/jcpe.12369 Primary prevention of periimplantitis: Managing peri-implant mucositis Jepsen S, Berglundh T, Genco R, Aass AM, Demirel K, Derks
Biofilm Removal With Air Polishing & Subgingival Air Polishing
 Earn 2 CE credits This course was written for dentists, dental hygienists, and assistants. Biofilm Removal With Air Polishing & Subgingival Air Polishing A Peer-Reviewed Publication Written by Karen Davis,
Earn 2 CE credits This course was written for dentists, dental hygienists, and assistants. Biofilm Removal With Air Polishing & Subgingival Air Polishing A Peer-Reviewed Publication Written by Karen Davis,
Illustrations by Carole Fumat.
 www.acteongroup.com To visualize our channel: www.youtube.com/user/acteonsatelec (1) Mombelli A, et al. The epidemiology of peri-implantitis. Clinical Oral Implants Research 23 (Oct 2012): 67-76 (2) European
www.acteongroup.com To visualize our channel: www.youtube.com/user/acteonsatelec (1) Mombelli A, et al. The epidemiology of peri-implantitis. Clinical Oral Implants Research 23 (Oct 2012): 67-76 (2) European
Interest in and studies on osseointegration
 CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
CASE REPORT A Two-Stage Surgical Approach to the Treatment of Severe Peri-Implant Defect: A 30-Month Clinical Follow- Up Report Jong-Eun Kim, DDS, MSD 1 Ha-Young Kim, DDS, MSD 1 Jung-Bo Huh, DDS, MSD,
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment
 The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
The use of the LiteTouch Er:YAG laser in peri-implantitis treatment Authors_Prof. Tzi Kang Peng, Taiwan & Prof. Georgi Tomov, Bulgaria _Introduction With oral implantology experience its Renaissance, the
Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports
 0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
0 Class II Furcations Treated by Guided Tissue Regeneration in Humans: Case Reports R.G. Caffesse, B.A. Smith/ B. Duff, E.C. Morrison, D. Merrill/ and W. Becker In the cases reported here, the response
Straumann SmartOne. Stage 4 Af terc are and maintenance. Step 2 Maintenance visit
 Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Stage 4 Af terc are and maintenance Step 2 Maintenance visit Overview Assessment and treatment planning Step 1 Patient's expectations, history and examination Step 2 Treatment planning Step 3 Consultation
Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93.
 Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Julia Collins Den 1200 Journal #4 1. Demographics Patient is J.S. age 29, Heavy/II 2. Assessment Patient had no significant findings in medical history. Her vital signs were 130/99, pulse 93. Patient does
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Abstract Purpose: Materials and methods Results:
 Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
Evaluation of peri-implant tissue response according to the presence of keratinized mucosa Bum-Soo Kim 1, Young-Kyun Kim 1, Pil-Young Yun 1, Yang-Jin Lee 2, Hyo-Jeong Lee 3, Su-Gwan Kim 4 1Department of
What You Should Know About Dental Implants: The Process of Care Applies
 Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Learn how the process of care model can apply to dental implants and empower decisions for providing quality care for clients. Starting with assessing the need for implants, the process covers documentation,
Key words: Peri- implant Mucositis, Peri- implantitis, Peri- implant Diseases, Treatment
 PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
PERIODONTOLOGY 2000 Management of peri- implant mucositis and peri- implantitis Elena Figuero 1, Filippo Graziani 2, Ignacio Sanz 1, David Herrera 1,3, Mariano Sanz 1,3 1. Section of Graduate Periodontology,
The International Journal of Periodontics & Restorative Dentistry
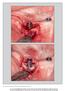 The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
The International Journal of Periodontics & Restorative Dentistry 729 Resective Treatment of Peri-implantitis: Clinical and Radiographic Outcomes After 2 Years Emmanuel Englezos, DDS, MSc 1 Jan Cosyn,
Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters
 Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters REVIEWED PAPER Most patients visiting dental surgeries suffer from various types of periodontopathies. Since
Impact of Photodynamic Therapy Applied by FotoSan on Periodontal Tissues Clinical Parameters REVIEWED PAPER Most patients visiting dental surgeries suffer from various types of periodontopathies. Since
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera
 Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Cause related therapy: Professional mechanical plaque control Zsuzsanna Papp Prof. István Gera Periodontal Clinic, Semmelweis University, Budapest 2017.02.14. Complex periodontal therapy Systemic phase
Periodontal Regeneration
 Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
Periodontal Regeneration Regeneration The most ideal treatment Attempts to recreate the tissues destroyed by periodontitis Cement, bone and ligament Reduces the risk for recession and sensitivity (could
PERIODONTAL CASE PRESENTATION - 1
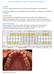 PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
PERIODONTAL CASE PRESENTATION - 1 Overview A 32 year-old patient presented with generalized aggressive periodontitis. Treatment included non-surgical therapy with adjunctive antibiotics and surgical treatment.
Periodontitis & Implants
 Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
Objectives Periodontitis & Implants Dr Simon Hinckfuss D.C.D (Melb), Cert.Perio, MS (Minn, USA) Diplomat of the American Board of Periodontology Diagnose common types of periodontal disease Describe the
COMPARISON OF HAND AND ULTRASONIC INSTRUMENTATION ON PERIODONTAL PARAMETERS IN GHANAIAN PATIENTS WITH MODERATE CHRONIC PERIODONTITIS
 March 216 Vol. 5, No. 1 PostgraduateMedical Journal of Ghana COMPARISON OF AND INSTRUMENTATION ON PERIODONTAL PARAMETERS IN GHANAIAN PATIENTS WITH MODERATE CHRONIC PERIODONTITIS Abstract Vasco E, Kwamin
March 216 Vol. 5, No. 1 PostgraduateMedical Journal of Ghana COMPARISON OF AND INSTRUMENTATION ON PERIODONTAL PARAMETERS IN GHANAIAN PATIENTS WITH MODERATE CHRONIC PERIODONTITIS Abstract Vasco E, Kwamin
Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report
 Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Bull Tokyo Dent Coll (2014) 55(4): 217 224 Case Report Periodontal Therapy for Severe Chronic Periodontitis with Periodontal Regeneration and Different Types of Prosthesis: A 2-year Follow-up Report Takashi
Effect of air-polishing with glycine and bicarbonate powders on a. nanocomposite used in dental restoration: an in vitro study
 Effect of air-polishing with glycine and bicarbonate powders on a nanocomposite used in dental restoration: an in vitro study Luca Giacomelli 1,*, M.S., PhD, Marco Salerno 2, M.S., PhD, Giacomo Derchi
Effect of air-polishing with glycine and bicarbonate powders on a nanocomposite used in dental restoration: an in vitro study Luca Giacomelli 1,*, M.S., PhD, Marco Salerno 2, M.S., PhD, Giacomo Derchi
Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study
 Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Clin Oral Invest (2017) 21:717 724 DOI 10.1007/s00784-016-1941-x ORIGINAL ARTICLE Bacterial colonization of the peri-implant sulcus in dentate patients: a prospective observational study M. A. Stokman
Antimicrobial Treatment of Peri-implant Diseases
 Antimicrobial Treatment of Peri-implant Diseases Lisa J. A. Heitz-Mayfield, BDS, MDSc, Odont Dr 1 /Niklaus P. Lang, DDS, MS, PhD 2 Purpose: To review the literature on the treatment of peri-implant diseases.
Antimicrobial Treatment of Peri-implant Diseases Lisa J. A. Heitz-Mayfield, BDS, MDSc, Odont Dr 1 /Niklaus P. Lang, DDS, MS, PhD 2 Purpose: To review the literature on the treatment of peri-implant diseases.
Location of unaccessible implant surface areas during debridement in simulated peri-implantitis therapy
 Steiger-Ronay et al. BMC Oral Health (2017) 17:137 DOI 10.1186/s12903-017-0428-8 RESEARCH ARTICLE Open Access Location of unaccessible implant surface areas during debridement in simulated peri-implantitis
Steiger-Ronay et al. BMC Oral Health (2017) 17:137 DOI 10.1186/s12903-017-0428-8 RESEARCH ARTICLE Open Access Location of unaccessible implant surface areas during debridement in simulated peri-implantitis
Mechanical Non Surgical Therapy: An Indispensable Tool
 IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
IOSR Journal of Dental and Medical Sciences (JDMS) ISSN: 2279-0853, ISBN: 2279-0861. Volume 1, Issue 4 (Sep-Oct. 2012), PP 36-41 Mechanical Non Surgical Therapy: An Indispensable Tool 1 Ashu Bhardwaj,
VOLUME 66. No.6. DECEMBER 2017
 VOLUME 66. No.6. DECEMBER 2017 PUBBLICAZIONE PERIODICA BIMESTRALE - POSTE ITALIANE S.P.A. - SPED. IN A.P.D.L. 353/2003 (CONV. IN L. 27/02/2004 N 46) ART. I, COMMA I, DCB/CN - ISSN 0026-4970 TAXE PERçUE
VOLUME 66. No.6. DECEMBER 2017 PUBBLICAZIONE PERIODICA BIMESTRALE - POSTE ITALIANE S.P.A. - SPED. IN A.P.D.L. 353/2003 (CONV. IN L. 27/02/2004 N 46) ART. I, COMMA I, DCB/CN - ISSN 0026-4970 TAXE PERçUE
An In Vitro Study of the Treatment of Implant Surfaces With Different Instruments
 An In Vitro Study of the Treatment of Implant Surfaces With Different Instruments Reiner Mengel, Dr med dent, DDS*/Christian-Eiben Buns, Dr med dent, DDS*/ Claudia Mengel, Dr med dent, DDS*/ Lavin Flores-de-Jacoby,
An In Vitro Study of the Treatment of Implant Surfaces With Different Instruments Reiner Mengel, Dr med dent, DDS*/Christian-Eiben Buns, Dr med dent, DDS*/ Claudia Mengel, Dr med dent, DDS*/ Lavin Flores-de-Jacoby,
Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report
 C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
C A S E R E P O R T Replacement of a congenitally missing lateral incisor in the maxillary anterior aesthetic zone using a narrow diameter implant: A case report Rhoodie Garrana 1 and Govindrau Mohangi
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester
 Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Periodontal Treatment Protocol Department of Orthodontics and Restorative Dentistry, Glenfield Hospital, Leicester 1. Periodontal Assessment Signs of perio disease: - Gingivae become red/purple - Gingivae
Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic case report.
 European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
European International Journal of Science and Technology Vol. 6 No. 5 July 2017 Treatment of dental recessions in the esthetic zone by gingival and osseous recontouring. A multidisciplinary perio-prosthodontic
Linking Research to Clinical Practice
 Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Is Non Surgical Periodontal Therapy Cost Effective? Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information
Purpose: To assess the long term survival of sites treated by GTR.
 Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
Cortellini P, Tonetti M. Long-term tooth survival following regenerative treatment of intrabony defects. J Periodontol 2004; 75:672-8. (28 Refs) Purpose: To assess the long term survival of sites treated
PREVENTIVE DENTISTRY. Straumann Next Generation Dentistry Prevent. Restore. Enhance.
 PREVENTIVE DENTISTRY Prevent. Restore. Enhance. 2 Next Generation Dentistry: Take a holistic approach with innovative solutions that enable preventive dentistry. If given the option, we all prefer prevention
PREVENTIVE DENTISTRY Prevent. Restore. Enhance. 2 Next Generation Dentistry: Take a holistic approach with innovative solutions that enable preventive dentistry. If given the option, we all prefer prevention
 HVE (Suction-evacuation) Suggestions for ultrasonics and glycine/air polishing HVE is a critical part of infection control when using these treatment modalities. The goal is to aspirate the plume before
HVE (Suction-evacuation) Suggestions for ultrasonics and glycine/air polishing HVE is a critical part of infection control when using these treatment modalities. The goal is to aspirate the plume before
Dental Water Jet. By: Jennifer Buffington, Lindsay Hunt, Ruth Gardner
 Dental Water Jet By: Jennifer Buffington, Lindsay Hunt, Ruth Gardner What is a Dental Water Jet? A home, dental self-care device that uses a stream of pulsating water to irrigate the subgingival sulcus
Dental Water Jet By: Jennifer Buffington, Lindsay Hunt, Ruth Gardner What is a Dental Water Jet? A home, dental self-care device that uses a stream of pulsating water to irrigate the subgingival sulcus
Implantology without Periodontology is like Yin without Yang.
 Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Implantology without Periodontology is like Yin without Yang. NIWOP: The systematic and evidence-based workflow #niwop wh.com No Implantology without Periodontology NIWOP 1 Pretreatment Optimal periodontal
Home care. Home care. Core Values for Treating Patients in Practice. Professional care. BSP Roadshows 2008/9
 3. Periodontal Treatment BSP Roadshows 2008/9 Core Values for Treating Patients in Practice 3. Periodontal Treatment Phil Ower www.periocourses.co.uk Why is it so important? Oral hygiene methods what s
3. Periodontal Treatment BSP Roadshows 2008/9 Core Values for Treating Patients in Practice 3. Periodontal Treatment Phil Ower www.periocourses.co.uk Why is it so important? Oral hygiene methods what s
Confidence for you comfort for your patient
 Clinpro Glycine Prophy Powder For supra- and subgingival cleaning Clinpro Glycine Prophy Powder with TCP For added sensitivity relief Confidence for you comfort for your patient f TCP functionalized Tri-Calcium
Clinpro Glycine Prophy Powder For supra- and subgingival cleaning Clinpro Glycine Prophy Powder with TCP For added sensitivity relief Confidence for you comfort for your patient f TCP functionalized Tri-Calcium
Clinical Management of an Unusual Case of Gingival Enlargement
 Clinical Management of an Unusual Case of Gingival Enlargement Abstract Aim: The purpose of this article is to report a case of conditioned gingival enlargement managed by nonsurgical periodontal therapy.
Clinical Management of an Unusual Case of Gingival Enlargement Abstract Aim: The purpose of this article is to report a case of conditioned gingival enlargement managed by nonsurgical periodontal therapy.
Effect of glycine powder air-polishing on the gingiva
 J Clin Periodontol 2008 doi: 10.1111/j.1600-051X.2007.01195.x Effect of glycine powder air-polishing on the gingiva Petersilka G, Faggion Jr. CM, Stratmann U, Gerss J, Ehmke B, Haeberlein I, Flemmig TF.
J Clin Periodontol 2008 doi: 10.1111/j.1600-051X.2007.01195.x Effect of glycine powder air-polishing on the gingiva Petersilka G, Faggion Jr. CM, Stratmann U, Gerss J, Ehmke B, Haeberlein I, Flemmig TF.
Principles of Periodontal Instrumentation. Periodontology I - 4th year 23/2/2012 Dr. Murad Shaqman
 Principles of Periodontal Instrumentation Periodontology I - 4th year 23/2/2012 Dr. Murad Shaqman Outline Classification of periodontal instruments General principles of instrumentation Principles of scaling
Principles of Periodontal Instrumentation Periodontology I - 4th year 23/2/2012 Dr. Murad Shaqman Outline Classification of periodontal instruments General principles of instrumentation Principles of scaling
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta
 Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Mario Roccuzzo Luca Bonino Paola Dalmasso Marco Aglietta Long-term results of a three arms prospective cohort study on implants in periodontally compromised patients: 10-year data around sandblasted and
Ucer, C; Wright, S; Scher E; West, N; Retzepi, M; Simpson, S; Slade, K; Donos, N
 ADI GUIDELINES On Peri-implant Monitoring and Maintenance Ucer, C; Wright, S; Scher E; West, N; Retzepi, M; Simpson, S; Slade, K; Donos, N Scope of the Problem: During the last two decades implant treatment
ADI GUIDELINES On Peri-implant Monitoring and Maintenance Ucer, C; Wright, S; Scher E; West, N; Retzepi, M; Simpson, S; Slade, K; Donos, N Scope of the Problem: During the last two decades implant treatment
The majority of the early research concerning
 Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Gingival Recession Around Implants: A 1-Year Longitudinal Prospective Study Paula N. Small, DDS, MPH 1 /Dennis P. Tarnow, DDS 2 A longitudinal study was performed, which measured the soft tissue around
Correlations between clinical parameters in implant maintenance patients: analysis among healthy and history-of-periodontitis groups
 Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
Seki et al. International Journal of Implant Dentistry (2017) 3:45 DOI 10.1186/s40729-017-0108-0 International Journal of Implant Dentistry RESEARCH Correlations between clinical parameters in implant
ABSTRACT INTRODUCTION. Research Article. Eon-Jeong Park, Eun-Young Kwon Jeomil Choi, Ji-Young Joo. , Hyun-Joo Kim. , Ju-Youn Lee
 J Periodontal Implant Sci. 218 Oct;48(5):295-34 https://doi.org/151/jpis.218.48.5.295 pissn 293-2278 eissn 293-2286 Research Article Clinical and microbiological effects of the supplementary use of an
J Periodontal Implant Sci. 218 Oct;48(5):295-34 https://doi.org/151/jpis.218.48.5.295 pissn 293-2278 eissn 293-2286 Research Article Clinical and microbiological effects of the supplementary use of an
effect of surgical debridement vs. non-surgical debridement for the treatment of chronic periodontitis.
 J Clin Periodontol 2002; 29(Suppl. 3): 92 102 Copyright # Blackwell Munksgaard 2002 Printed in Denmark. All rights reserved ISSN 1600-2865 Review article A systematic review of the effect of surgical debridement
J Clin Periodontol 2002; 29(Suppl. 3): 92 102 Copyright # Blackwell Munksgaard 2002 Printed in Denmark. All rights reserved ISSN 1600-2865 Review article A systematic review of the effect of surgical debridement
Anti-Cardiolipin Antibodies Detection in Sera of Chronic Periodontitis Patients
 P-01 Anti-Cardiolipin Antibodies Detection in Sera of Chronic Periodontitis Patients NOOR RASHIDAH S 1, HASLINA T 2, WAN MAJDIAH WM 3, ZAINUDDIN SLA 2 1 Periodontic Clinic, Klinik Pergigian Datuk Kumbar,
P-01 Anti-Cardiolipin Antibodies Detection in Sera of Chronic Periodontitis Patients NOOR RASHIDAH S 1, HASLINA T 2, WAN MAJDIAH WM 3, ZAINUDDIN SLA 2 1 Periodontic Clinic, Klinik Pergigian Datuk Kumbar,
Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report
 Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Bull Tokyo Dent Coll (2013) 54(4): 243 250 Case Report Longitudinal Supportive Periodontal Therapy for Severe Chronic Periodontitis with Furcation Involvement: A 12-year Follow-up Report Akiyo Komiya-Ito,
Porous titanium granules in the treatment of peri-implant osseous defects a 7-year follow-up study
 Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Andersen et al. International Journal of Implant Dentistry (2017) 3:50 DOI 10.1186/s40729-017-0106-2 International Journal of Implant Dentistry SHORT REPORT Open Access Porous titanium granules in the
Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
 ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
ull Tokyo Dent Coll (2017) 58(3): 177 186 Case Report doi:10.2209/tdcpublication.2016-0039 Periodontist-Dental Hygienist Collaboration in Periodontal Care for Chronic Periodontitis: An 11-year Case Report
Sample Competency Forms
 Sample Competency Forms The competency and assessment forms and grading criteria included in this packet are suggestions only. Utilize and/or modify as it fits with your institution s practices. Procedures
Sample Competency Forms The competency and assessment forms and grading criteria included in this packet are suggestions only. Utilize and/or modify as it fits with your institution s practices. Procedures
Treatment Concepts for PERI-IMPLANTITIS
 Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Treatment Concepts for PERI-IMPLANTITIS CONTENT Definition, diagnosis and prevalence 3 Risk factors and preventive measures 5 Latest evidence on the treatment of peri-implantitis 6 Clinical Cases Regenerative
Periodontal Maintenance
 Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
Periodontal Maintenance Friday, February 20, 2015 1:06 PM Periodontal disease control always begins with patient education - Plaque control, diet, smoking cessation, impact that systemic health has on
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter
 THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
THE PERIODONTAL ASPECT OF IMPLANT THERAPY Prof. Dr. Windisch Péter Periodontal aspects of implant therapy 1) Comprehensive perioprosthodontic treatment by utilizing implants on perio-patients. 2) Anatomical
Peri-implant marginal bone loss: What is the current concensus? an academic controversy or a clinical challenge?
 Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Peri-implant marginal bone loss; What is the current concensus? Bjorn.Klinge@mah.se Peri-implant marginal bone loss: an academic controversy or a clinical challenge? Björn Klinge Eur J Oral Implantol 2012;5
Multidisciplinary treatment planning for patients with severe periodontal disease
 Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Clinical Multidisciplinary treatment planning for patients with severe periodontal disease Josselin Lethuillier, 1 Sébastien Felenc, 2 Philippe Bousquet 3 Abstract Periodontally compromised patients usually
Periodontal Treatment Guide
 Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Periodontal Treatment Guide Teamwork for treating periodontal disease The treatment of patients with periodontal disease should involve the application of standard procedures based on commonly accepted
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy
 Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Consensus Statements and Recommended Clinical Procedures Regarding Risk Factors in Implant Therapy David L. Cochran, DDS, MS, PhD, MMSci 1 /Søren Schou, DDS, PhD, Dr Odont 2 / Lisa J. A. Heitz-Mayfield,
Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014
 Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014 Tooth Replacement treatment options and benefits Identify Existing Patients
Optimal Peri- Implant Maintenance Science, Systems, and Success! Susan S. Wingrove RDH, BS RDH UnderOneRoof Chicago, IL 2014 Tooth Replacement treatment options and benefits Identify Existing Patients
Effect of thread size on the implant neck area: preliminary results at 1 year of function
 Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Young-Il Kang* Dong-Won Lee* Kwang-Ho Park Ik-Sang Moon Effect of thread size on the implant neck area: preliminary results at 1 year of function Authors affiliations: Young-Il Kang*, Dong-Won Lee*, Ik-Sang
Volume 2 Issue
 Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
Volume 2 Issue 2 2017 Page 333 to 340 Research Article Oral Health and Dentistry ISSN: 2573-4989 The Anti-Inflammatory Actions of an Intra-Oral Adhesive Patch Containing Botanical Extracts Exert Inhibitory
PERI-IMPLANTITIS A PROBLEM.
 PERI-IMPLANTITIS A PROBLEM. Infections around implants are stubborn. What can help? What doesn t? How can infections be prevented? Geistlich News 02 2014 5 Illustration: Büro Haeberli How prevalent is
PERI-IMPLANTITIS A PROBLEM. Infections around implants are stubborn. What can help? What doesn t? How can infections be prevented? Geistlich News 02 2014 5 Illustration: Büro Haeberli How prevalent is
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature
 The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
The Efficacy of Supportive Peri-Implant Therapies in Preventing Peri-Implantitis and Implant Loss: a Systematic Review of the Literature Ausra Ramanauskaite 1, Tellervo Tervonen 2,3 1 Department of Dental
Antimicrobial Treatment for Advanced Periodontal Disease
 Antimicrobial Treatment for Advanced Periodontal Disease James S. Kohner, DDS DISCLOSURES December 15, 2011 Editor's Note: This author's case report is based on the work of Jorgen Slots, DDS, DMD, PhD,
Antimicrobial Treatment for Advanced Periodontal Disease James S. Kohner, DDS DISCLOSURES December 15, 2011 Editor's Note: This author's case report is based on the work of Jorgen Slots, DDS, DMD, PhD,
Consensus Report Tissue augmentation and esthetics (Working Group 3)
 B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
B. Klinge Thomas F. Flemmig Consensus Report Tissue augmentation and esthetics (Working Group 3) Members of working group: Matteo Chiapasco Jan-Eirik Ellingsen Ronald Jung Friedrich Neukam Isabella Rocchietta
Effects of KTP Laser Irradiation, Diode Laser, and LED on Tooth Bleaching: A Comparative Study.
 : Photomed Laser Surg. 2007 Apr;25(2):91-5 Effects of KTP Laser Irradiation, Diode Laser, and LED on Tooth Bleaching: A Comparative Study. Zhang C, Wang X, Kinoshita J, Zhao B, Toko T, Kimura Y, Matsumoto
: Photomed Laser Surg. 2007 Apr;25(2):91-5 Effects of KTP Laser Irradiation, Diode Laser, and LED on Tooth Bleaching: A Comparative Study. Zhang C, Wang X, Kinoshita J, Zhao B, Toko T, Kimura Y, Matsumoto
The Oral ATP- A Photo Tour
 The Oral ATP- A Photo Tour The Patient: Jax Goodman 1.5 year old, neutered male Labrador Retriever cross, 65 pounds Indication for oral examination: preventative therapy Stage 1: Assessment A. Initial
The Oral ATP- A Photo Tour The Patient: Jax Goodman 1.5 year old, neutered male Labrador Retriever cross, 65 pounds Indication for oral examination: preventative therapy Stage 1: Assessment A. Initial
Clinical outcomes following surgical treatment of peri-implantitis at grafted and non-grafted implant sites: a retrospective analysis
 Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Ramanauskaite et al. International Journal of Implant Dentistry (2018) 4:27 https://doi.org/10.1186/s40729-018-0135-5 International Journal of Implant Dentistry RESEARCH Clinical outcomes following surgical
Periodontal Case Report
 Periodontal Case Report By Dan AlAhmed 431200041 Saleha AlZahrani 431200123 Raghad AlSaawy 431200297 Afnan AlAssiri 431200687 Mawadh Demyati 431200824 Hend Jaddoh 431201247 Alaa AlDoss 431201808 Rawan
Periodontal Case Report By Dan AlAhmed 431200041 Saleha AlZahrani 431200123 Raghad AlSaawy 431200297 Afnan AlAssiri 431200687 Mawadh Demyati 431200824 Hend Jaddoh 431201247 Alaa AlDoss 431201808 Rawan
The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series
 CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
CLINICAL AND RESEARCH REPORT The Treatment of Gingival Recession Associated with Deep Corono-Radicular Abrasions (CEJ step) a Case Series Giovanpaolo Pini-Prato, Carlo Baldi, Roberto Rotundo, Debora Franceschi,
BioFilm Eraser. Advantages
 BioFilm Eraser Perio-Mate is used in the treatment of periodontal pockets and peri-implantitis. Avoiding injury to the soft tissues and root surfaces inside delicate periodontal pockets during cleaning
BioFilm Eraser Perio-Mate is used in the treatment of periodontal pockets and peri-implantitis. Avoiding injury to the soft tissues and root surfaces inside delicate periodontal pockets during cleaning
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys
 The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
The Influence of Controlled Occlusal Overload on Peri-implant Tissue. Part 3: A Histologic Study in Monkeys Takashi Miyata, DDS, DDSc 1 /Yukinao Kobayashi, DDS 2 /Hisao Araki, DDS, DDSc 3 / Takaichi Ohto,
GOALS FOR THE PERIODONTAL PATIENT
 1 Goals for the Periodontal Patient: 1. Modify Risk Factors a. Overall goal is total health. b. Research shows that oral health is related to total health c. #1 preventable risk fact is tobacco use d.
1 Goals for the Periodontal Patient: 1. Modify Risk Factors a. Overall goal is total health. b. Research shows that oral health is related to total health c. #1 preventable risk fact is tobacco use d.
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis
 Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Risk of Implant Failure and Marginal Bone Loss in Subjects with a History of Periodontitis: A Systematic Review and Meta-Analysis Syarida H. Safii, DDS [Correction added after online publication 1 June
Why implants need even better care than natural teeth.
 Why implants need even better care than natural teeth. ± How to increase the lifespan of your implant. BETTER ORAL HEALTH FOR ALL Expert advisory board Hugo Roberto Lewgoy, DDS, MSc, PhD., Department of
Why implants need even better care than natural teeth. ± How to increase the lifespan of your implant. BETTER ORAL HEALTH FOR ALL Expert advisory board Hugo Roberto Lewgoy, DDS, MSc, PhD., Department of
Show biofilm the red card
 Show biofilm the red card BIOFILM-ERASER 1 A NEW APPLICATION Effective treatment for periodontal and peri-implant inflammation Periodontitis and peri-implantitis are bacterial inflammations with similar
Show biofilm the red card BIOFILM-ERASER 1 A NEW APPLICATION Effective treatment for periodontal and peri-implant inflammation Periodontitis and peri-implantitis are bacterial inflammations with similar
POWER AIR-FLOW HANDY 3.0 DEVICES
 POWER AIR-FLOW HANDY 3.0 DEVICES THE BETTER WAY FOR BIOFILM MANAGEMENT Introducing AIR-FLOW THERAPY AIR-FLOW Therapy is completely different than other air polishing systems. This advanced technology offers
POWER AIR-FLOW HANDY 3.0 DEVICES THE BETTER WAY FOR BIOFILM MANAGEMENT Introducing AIR-FLOW THERAPY AIR-FLOW Therapy is completely different than other air polishing systems. This advanced technology offers
CLINICAL APPLICATION GUIDE DIAGNOSTIC INSTRUMENTS & PERIODONTAL SCALERS/ CURETTES
 CLINICAL APPLICATION GUIDE DIAGNOSTIC INSTRUMENTS & PERIODONTAL SCALERS/ CURETTES DIAGNOSTIC INSTRUMENTATION EXPLORERS Explorers are used to examine tooth surfaces for calculus, decalcified and carious
CLINICAL APPLICATION GUIDE DIAGNOSTIC INSTRUMENTS & PERIODONTAL SCALERS/ CURETTES DIAGNOSTIC INSTRUMENTATION EXPLORERS Explorers are used to examine tooth surfaces for calculus, decalcified and carious
Linking Research to Clinical Practice
 Prevention of Root Caries Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information to clinical dental
Prevention of Root Caries Denise M. Bowen, RDH, MS Linking Research to Clinical Practice The purpose of Linking Research to Clinical Practice is to present evidence based information to clinical dental
Peri-implantitis susceptibility as it relates to periodontal therapy and supportive care
 Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal
Bjarni E. Pjetursson Christoph Helbling Hans-Peter Weber Giedre Matuliene Giovanni E. Salvi Urs Brägger Kurt Schmidlin Marcel Zwahlen Niklaus P. Lang Peri-implantitis susceptibility as it relates to periodontal
Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study
 R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
R. Burkhardt N. P. Lang Role of flap tension in primary wound closure of mucoperiosteal flaps: a prospective cohort study Authors affiliation: R. Burkhardt, N. P. Lang, The University of Hong Kong, Hong
The International Journal of Periodontics & Restorative Dentistry
 The International Journal of Periodontics & Restorative Dentistry 485 Bacterial Biofilm Morphology on a Failing Implant with an Oxidized Surface: A Scanning Electron Microscope Study Massimo Simion, MD,
The International Journal of Periodontics & Restorative Dentistry 485 Bacterial Biofilm Morphology on a Failing Implant with an Oxidized Surface: A Scanning Electron Microscope Study Massimo Simion, MD,
EFFECTIVENESS OF ORAL HYGIENE INSTRUCTION MEDIA ON PERIODONTAL HEALTH AMONG HEARING IMPAIRED CHILDREN
 EFFECTIVENESS OF ORAL HYGIENE INSTRUCTION MEDIA ON PERIODONTAL HEALTH AMONG HEARING IMPAIRED CHILDREN Malee Arunakul, Yosvimol Kuphasuk 2 and Romcharee Boonyathanasit 3 Department of Pediatric Dentistry,
EFFECTIVENESS OF ORAL HYGIENE INSTRUCTION MEDIA ON PERIODONTAL HEALTH AMONG HEARING IMPAIRED CHILDREN Malee Arunakul, Yosvimol Kuphasuk 2 and Romcharee Boonyathanasit 3 Department of Pediatric Dentistry,
Faculty of Dentistry PERIODONTICS 1429 /1430
 Faculty of Dentistry ORAL BASIC AND CLINICAL SCIENCES DEPARTMENT Course Portfolio PERIODONTICS Course Number PERIO 401 O.B.C.S 445 1429 /1430 2008/ 2009 Course Syllabus CONTENTS: 1- INSTRUCTOR INFORMATION
Faculty of Dentistry ORAL BASIC AND CLINICAL SCIENCES DEPARTMENT Course Portfolio PERIODONTICS Course Number PERIO 401 O.B.C.S 445 1429 /1430 2008/ 2009 Course Syllabus CONTENTS: 1- INSTRUCTOR INFORMATION
