Mesenchymal Stem Cell Therapy for Treatment of Craniofacial Bone Defects: 10 Years of Experience
|
|
|
- Philippa Lawson
- 5 years ago
- Views:
Transcription
1 Regeneration, Reconstruction & Restoration Regeneration Mesenchymal Stem Cell Therapy for Treatment of Craniofacial Bone Defects: 10 Years of Experience Arash Khojasteh a*, Saeed Reza Motamedian b a Department of Oral and Maxillofacial Surgery, Dental Research Center, Research Institute of Dental Sciences, Dental School, Shahid Beheshti University of Medical Sciences, Tehran, Iran; b Department of Orthodontics, Dental School, Shahid Beheshti University of Medical Sciences, Tehran, Iran. *Corresponding author: Arash Khojasteh, Department of Oral and Maxillofacial Surgery, Dental School, Shahid Beheshti University of Medical Science, Daneshjou Boulevard, Evin, Tehran, Iran, P.O arashkhojasteh@sbmu.ac.ir; Tel: Submitted: ; Accepted: ; DOI: /rrr Introduction: Cell delivery in treatment of bone defects has been introduced to promote tissue healing in the recent years. However, no general consensus has been reached regarding the outcome of regenerative medicine for this purpose. The aim of this study was to review our 10 years of experience in application of mesenchymal stem cells (MSCs) in craniofacial bone defects. Applied Methodology: Iliac bone marrow, dental pulp and buccal fat pad were selected to harvest MSCs. Flow cytometric analysis, RT-PCR and differentiation staining including Alizarin red, Oil Red O and Toluidine blue were used to identify MSCs. Four groups of bone substitutes were used for cell delivery: synthetic scaffold [beta-tricalcium phosphate (B-TCP) and hydroxyapatite/tricalcium phosphate (HA/TCP)], xenograft [natural bovine bone mineral (NBBM)], allograft [freeze-dried bone (FDBA), demineralized freeze dried bone] and composite [polycaprolactone/tcp (PCL-TCP), demineralized freeze-dried bone/calcium sulfate]. Rat and rabbit calvaria, dog mandible, rabbit tibia sinus and alveolar cleft defects in human were used as the study models. Histomorphometric and radiomorphological analysis were used to determine new bone formation. Outcomes: Cell-treated groups showed greater new bone formation than cell-free group in all studies. Synthetic scaffolds showed better cell attachment according to scanning electron microscopy (SEM) results. In rat calvarial model, B-TCP loaded with MSCs showed better results than scaffolds carrying platelet rich plasma (PRP). NBBM showed less promising results both in dog mandible and ectopic bone formation in the masseter muscle. FDBA block fixed over a supracrestal defect in dog mandible showed 50% less new bone formation when compared with PCL-TCP as a carrier. Conclusion: More convergence studies with similar protocols of cell cultivation, culture, seeding and delivery should be done in the field of regenerative medicine for better generalizability of results for clinical setting. Keywords: Mesenchymal stem cells; Bone regeneration; Tissue engineering; Craniofacial bone Introduction Bone as a highly differentiated tissue in the body may suffer defects due to congenital diseases, trauma, tumors and senile atrophy. Despite many advances in bone regeneration, reconstruction of large bony defects continues to be beyond the reach. Despite the availability of a plethora of treatment modalities, bone substitutes and various clinical adjuncts, most clinicians and researchers continue to reach the same conclusion. Autogenous bone grafts are still the gold standard to which all other reconstructive procedures are compared. However, autogenous bone grafts have several significant limitations, namely limited availability of competent sites and inherent donor site morbidity (1-4). Over the past few decades, considerable advancements have been made in tissue and bone engineering procedures. Bone engineering procedures apply osteogenic cells, growth factors and scaffolds to promote bone formation. Various osteogenic cells, including mesenchymal stem cells (MSCs) can be used in bone engineering protocols. MSCs have been proven to have proliferation and osteogenic differentiation capacities (5-8). Similarly, previous studies have demonstrated that MSC-based bone augmentation procedures induce higher levels of bone formation compared to acellular treatments (9-12). In addition, co-transplantation of growth factors in these procedures might further promote bone regeneration (13-15). The purpose of this study is to review our 10 years of experience in application of MSCs in craniofacial bone defects.
2 2 Khojasteh & Motamedian Applied Methodology Harvesting the MSCs Iliac bone marrow aspirate Two weeks before regenerative surgery, bone marrow aspirate (10-15 ml) was obtained from the posterior iliac crest. The aspirate was diluted at 1:3 in Dulbecco s modified Eagle s medium (DMEM)/F12 (Gibco, Paisley, UK). On day one, nonadherent cells were discarded and adherent cells were washed with phosphate-buffered saline (PBS) (Gibco, Paisley, UK) and then cultured in DMEM/F12 with antibiotics and 20% autologous serum. Dental pulp Vital third molars of a healthy adult subject indicated for extraction were extracted. Before extraction, the patient was asked to rinse 0.2% chlorhexidine mouthwash (Behsa Co., Tehran, Iran) for one minute. After extraction, the teeth were immersed in saline solution containing antibiotics. The crown of each tooth was cut into several segments and the pulp was exposed. Dental pulp tissue was removed with a barbed broach. Dissected tissue was minced and incubated in 3 mg/ml type I collagenase and 4 mg/ml dispase in PBS (Gibco, Paisley, UK) at 37 C for 30 minutes. Then, the tissue fragments were immersed in α-mem supplemented with 10% fetal bovine serum (FBS) and 1% antibiotics (Gibco, Paisley, UK) and placed in 25 cm2 flasks. Flasks were incubated in humidified atmosphere with 5% CO2 at 37 C. Culture medium was changed twice a week and after reaching the sub-confluent stage, the cells were removed by enzymatic digestion (0.25% trypsin EDTA) and passaged. Third to fourth passage dental pulp stem cells (DPSCs) were subjected to the following experiments. Buccal fat pad Buccal fat pad was harvested from healthy donors via a vestibular incision distal to the maxillary second molar. The fat pad was exposed using blunt dissection while preserving the thin covering membrane; 3-5 ml of the fat was excised and transferred to a laboratory in DMEM. The tissue processing and cultivation of stem cells were done similar to the methods done for dental pulp. Adherent cells were expanded as monolayer cultures in 5% CO 2/ 95% air atmosphere at 37 C; the medium was refreshed every three days. The confluent cells were dissociated with trypsin and sub-cultured in new six-well culture dishes at a plating density of cells/dish. The cells were visible under light microscopy. The cells were stained with Trypan blue (1:1; v/v) and counted in a counting chamber using a light microscope (Nikon, Tokyo, Japan). Preparation of human serum In human trials, human serum was used for cultivation of the cells. From each donor bone marrow, 20 ml of whole blood was collected in blood bags and quickly transferred into 10-mL vacutainer tubes without anticoagulants (BD, Plymouth, UK), and allowed to clot for 4 hours at 4 C to 8 C. Subsequently, the blood was centrifuged at 1800g at 4 C for 15 minutes. Serum was collected and filtered through a 0.2 mm membrane. Identification of MSCs Flow cytometry analysis Fluorescence-activated cell sorting (FACS) was performed using standard protocols and quantification criteria. The criteria to distinguish positive from negative cells were set individually for each marker. Fluorescein isothiocyanate (FITC) conjugated monoclonal antibodies against CD34 (Miltenyi Biotech, Bergisch Gladbach, Germany), CD44, CD29, CD105 and CD13 (BD Biosciences, San Diego, CA, USA) at a concentration of 2 mg/ml at 4 C were used for 30 minutes. The cells stained with FITClabeled mouse IgG were used as negative controls. The cells were washed twice with PBS and fixed with 1% para-formaldehyde. Analysis was performed on 100,000 cells per sample and the positive expression was defined as the level of fluorescence greater than 99% of the corresponding value for unstained cell sample (11-14). Differentiation Staining Alizarin Red staining (osteogenic differentiation) To induce osteogenic differentiation, cells from third passage were provided with DMEM medium supplemented with 50 mg/ml ascorbic 2-phosphate (Sigma Aldrich, St. Louis, MO, USA), 10 nm dexamethasone (Sigma Aldrich, St. Louis, MO, USA) and 10 mm glycerol phosphate (Sigma Aldrich, St. Louis, MO, USA). After 3 weeks, differentiated cells were fixed for 1 h with 4% formalin and rinsed with PBS (Gibco, Paisley, UK). Mineralization of the extracellular matrix was visualized by staining with 40 mm Alizarin Red S at a ph of 4.2 for 5 minutes. Oil Red staining (adipogenic differentiation) To induce adipose differentiation, third passage confluent cells were treated with a medium containing 100nM dexamethasone (Sigma Aldrich, St. Louis, MO, USA) and 50 mg/ml indomethacin (Sigma Aldrich, St. Louis, MO, USA). After three weeks, the cells were fixed with 4% formalin at room temperature, washed with 70% ethanol and stained with Oil Red solution in 99% isopropanol for 15 minutes. Toluidine blue staining (chondrogenic differentiation) To induce cartilage differentiation, micro-mass culture system was used. For this purpose, third passage cells were
3 Craniofacial regenerative medicine in 10 years 3 Table 1. Gene expression determined by RT-PCR for determination of differentiation potential of MSCs Cell lineage Genes Osteogenic differentiation Osteopontin, Collagen I Chondrogenic differentiation Decorin, Collagen II Adipogenic differentiation LPL, PPARG2 pelleted under 1200 g for 5 minutes and cultured in DMEM supplemented with 10ng/mL transforming growth factor-ß3 (TGFß3; Sigma Aldrich, St. Louis, MO, USA ), 10 ng/ml bone morphogenetic protein-6 (BMP-6; Sigma Aldrich, St. Louis, MO, USA), 50 mg/ml insulin transferrin selenium+ premix (Sigma Aldrich, St. Louis, MO, USA), 1.25 mg bovine serum albumin (BSA; Sigma Aldrich, St. Louis, MO, USA) and 1% FBS (Sigma Aldrich, St. Louis, MO, USA). After three weeks, the pellets were sectioned at 5 μm, stained with toluidine blue for 30 seconds at room temperature and observed under a light microscope. RT-PCR for gene expression The differentiation ability of the cells and some specific gene expressions were also studied by RT-PCR. For this purpose, total RNA was collected from the cells differentiated into bone, cartilage and adipose cells (as detailed above) using RNX- PlusTM solution (CinnaGen Inc., Tehran, Iran). Before the reverse transcription, the RNA samples were digested with DNase I (Fermentas, Waltham, Massachusetts, USA) to remove the contaminating genomic DNA. Standard reversetranscription reaction was performed with 2μg total RNA using Random Hexamer as a primer and Revert Aid TM H Minus First Strand cdna Synthesis Kit (Fermentas, Waltham, Massachusetts, USA) according to the manufacturer instructions. Subsequently, RT-PCR was performed using 2.5 μl cdna, 1X PCR buffer (AMS), 200 μm dntps, 0.2 μm of each primer pair and 1 unit/25 μl reaction Taq DNA polymerase (Fermentas, Waltham, Massachusetts, USA). The primers indicated in Table 1 were used to detect differentiation. Each PCR was performed in triplicate. The products were analyzed on 2% agarose gel and visualized by ethidium bromide staining. Cell Seeding A seeding concentration of cells/ml was cultured on various bone grafts. Each layer of scaffold covering one of 24- well plates was seeded with MSCs in 200 μl of culture medium. The plates were incubated for 1 hour at 37 C allowing cell adhesion; then, half of the samples received 1/500 of standard medium (containing α-mem supplemented with 10% FBS, 1% antibiotic antimycotic solution and 2 mmol/l L- glutamine). We used different incubation times Figure 1. SEM micrograph of bone marrow MSCs attached to allograft scaffold porosities ( 1000) for different types of bone substitutes Including synthetic scaffold [beta-tricalcium phosphate (B-TCP) and hydroxyapatite/tricalcium phosphate (HA/TCP)], xenograft [natural bovine bone mineral (NBBM)], allograft [freeze-dried bone (FDBA), demineralized freeze dried bone] and composite [polycaprolactone/tcp (PCL-TCP), demineralized freeze-dried bone/calcium sulfate ]. The bone substitutes were mixed with cells and incubated for at least 24 hours. We also tested 48 hours to 14 days of incubation in some of our experiments. Cell attachment was assessed by SEM. Scanning Electron Microscopy (SEM) Scaffold surface topography, adherent cell morphology and extracellular matrix culture were assessed using SEM. The seeded scaffolds were rinsed with PBS twice, fixed in 2.5% glutaraldehyde for two hours, and then post-fixed in 1% osmium for another two hours. Then, samples were dehydrated in graded concentrations of alcohol (30, 50, 70, 90, 95, and 100% ethanol). Afterwards, the samples were air dried in a desiccator overnight, sputtered with gold and observed under a SEM (VEGA, TESCAN, Brno-Kohoutovice, Czech Republic) at 10 kv. Images of non-seeded scaffolds were also taken. Moreover, the size of micro- and macro-porosities of each scaffold was measured by Image J 1.46 computer software (Wayne Rasband, NIH, Bethesda, Maryland, U.S.). Application of MSCs Bone substitutes mixed with MSCs were transferred to bone defects in different animal and human models (9-19). Histological and histomorphometric analyses were done after 8-12 weeks according to the study protocols.
4 42 Khojasteh & Motamedian Table 2. Selected studies using mesenchymal stem cells for treatment of craniofacial bone defects
5 Craniofacial regenerative medicine in 10 years 5 Figure 2. SEM micrographs of cultivation of DPSCs after one week over (A) allograft (freeze dried bone allograft) ( 1000); (B) β- TCP ( 1000) (C) xenograft (natural bovine bone mineral) ( 1000) Outcomes The SEM analysis showed lodgment of cells within the pores of the scaffolds (Figure 1). By increasing the time of incubation to seven days, the number of attached cells also increased (20). Synthetic materials showed more attachment that the bovine or human-derived substitutes (Figure 2) (20). The in vivo results of our studies were analyzed based on the type of defect and carrier for MSCs (Table 2). Rat calvarial models Through-and-through 5 mm circular defects were created in rat calvarium. Rat bone marrow mesenchymal stem cells (BMMSCs) delivered by β-tcp or NBBM (Bio-Oss; Geistlich, Wolhusen, Switzerland) were compared with groups receiving PRP-soaked scaffolds. New bone formation was measured histomorphometrically. The maximum bone formation was reported to be 2.53 mm in the β-tcp/msc group six weeks after the surgery (11). Rabbit models Rabbit calvarial model Two studies have been done on 8 mm rabbit calvarial defects.in the first experiment, MSCs were delivered by nano silica gel/hydroxyapatite (nanoha) and new bone formation was measured histologically after six and 12 weeks post-surgery and in another one with the same protocol, MSCs were delivered by FDBA. In each study, there were four groups. Group 1: NanoHA granule; Group 2: Nano-HA+1 ml of autologous plasma rich in growth factors (PRGF); Group 3, Nano-HA+2 ml of culture medium containing 100,000 autogenous MSCs; Group 4, Nano- HA + 2 ml of culture medium containing 100,000 autogenous MSCs +1 ml autologous PRGF. Histomorphometric analysis at six and 12 weeks demonstrated significantly higher bone formation in group 4 (29.45% and 44.55%, respectively). Bone formation in groups 1, 2, and 3 was as follows: 11.35% and 32.53%, 29.10% and 39.74%, and 25.82% and 39.11%, respectively (14). In the second experiment, Nano-HA was replaced by FDBA. Histomorphometric analysis of the sections at six and 12 weeks post-operation demonstrated 14.6% and 20.31% osteogenesis in group 1, 14.35% and 28.44% in group 2, 17.75% and 31.33% in group 3 and 18.94% and 37.21% in group 4, respectively (16). Rabbit tibial model We used rabbit tibia as a study model for delivery of MSCs. Right and left tibiae of each rabbit were prepared, and a 3-mm protruding implant from the tibia was placed in each side. Particulate allogeneic bone/fibrin glue/mscs combination was placed around test implants and particulate bone graft/fibrin glue around controls. Two months postoperatively, the animals were euthanized, and sections were prepared for histological analysis. The mean amount of vertical bone height was higher in the experimental group than the control group (2.09 mm versus 1.03 mm) (21). Dog models Ectopic bone formation For evaluation of ectopic bone formation, a blunt pouch in the masseter muscle of a dog was created, bone marrow derived MSCs were implanted over the HA/TCP (group 1) and NBBM (group 2). The results showed and 23.55% of new bone formation, respectively (19). Mandibular defect in dogs The effectiveness of MSCs in treatment of mandibular defects of
6 6 Khojasteh & Motamedian dogs was studied in three experiments. Six weeks after delivering dog BMMSCs with biphasic scaffold (HA/TCP) or NBBM (Bio- Oss) in a through-and-through 10-mm mandibular defect, new bone formation was reported to be 65.78% and 50.31%, respectively. The use of scaffolds without MSCs was accompanied by significantly lower bone regeneration (44.90% and 36.83%, respectively) (10). In another study we created a mm supracrestal defect in the posterior mandible after extraction of the posterior teeth mimicking severe mandibular atrophy in edentulous patients. PCL-TCP block, which is a composite scaffold was used to carry the cells. The block was fixed with 1.2 mm micro screw (Jeil, Seoul, South Korea) to the underlying bone. Histomorphometric analysis eight weeks after scaffold implantation showed higher amount of lamellar bone in the test side (48.63%) than control side (17.27%) (17). In another study with the same protocol, freeze dried human derived bone block was used to deliver MSCs. Although in this study, MSCs were co-transplanted with recombinant platelet derived growth factor (rh-pdgf) the results showed only 21.52% of new bone formation (22). Human models We studied the application of MSCs in human subjects in three experiments. In the first study, we used HA-TCP loaded with BMMSCs in three cases of unilateral and four cases of bilateral sinus augmentation; dental implants were also placed in six patients, three months post-operatively. MSC-treated patients demonstrated adequate bone augmentation with 41.43% of new bone formation and an average bone height of 12 mm. These findings were based on histomorphometric and radiographic analyses three months after grafting. Radiographs 12 months postoperatively showed a mm bone height increase. Twenty-eight of 30 implants (93%) were reported to be clinically successful at the six-month follow up (9). In the second study, demineralized bone matrix was combined with calcium sulfate (DBM/CaSO4) and BMMSCs for secondary repair of alveolar cleft in two patients. Panoramic radiographs of two cases of grafting of alveolar cleft using MSCs displayed adequate bone fill and union of the segmental arches. Four-month quantitative measurements by tomographic scans showed a bone fill of 34.5% for the first case and 25.6% for the second case (12). In the third trial, we added PRGF to HA/TCP loaded with MSCs to treat alveolar cleft defects in three patients. Cone beam computed tomography showed 52% of new bone formation (13). Discussion The use of cells for treatment of organ disorders is a traditional goal in regenerative medicine. Culturing cells in the lab and then differentiating them to specific cell lines to either produce tissue in the lab or cause tissue healing in situ has always been an ultimate goal for researchers. The problems against tissue formation outside the human body include nutritional supply of the cells and collecting their waste materials. Bioreactors are gradually going to find their place in tissue engineering (22, 23). Diversity among the study protocols such as cell cultivation and differentiation, cell seeding on scaffolds, incubation period and delivery methods can affect the efficacy of regenerative medicine in bone reconstruction. In a recent article we could not detect any common method utilized by tissue engineering studies (7). We performed cell harvesting, culture, differentiation, cell seeding on scaffolds and delivery to sites with the same techniques in our experiments in the past 10 years. Synthetic scaffolds such as TCP showed better results in comparison to NBBM in 6 mm rat calvarial defects when delivering MSCs. The same result was obtained when PRP was added to the scaffold (11). Biphasic synthetic HA/TCP demonstrated better results in regenerating new bone in the dog through and through 10 mm mandibular defect than NBBM (10). HA/TCP also had better cell attachment when compared to NBBM under SEM (11). In two human studies performed for treating alveolar cleft defects, MSCs co-transplanted with HA/TCP caused more bone formation than DBM/CaSO 4 co- transplanted with MSCs (12, 13). FDBA showed less bone formation than nano- HA with silica gel in 8 mm rabbit calvarial defects. FDBA and DFDBA showed the most promising results for cell attachments when investigated under SEM but in vivo studies showed different results. DFDBA loaded with MSCs was used around dental implants in rabbit tibia and revealed 2.1 mm vertical bone growth whereas no new bone formation was noted in the control cell-free group (21). FDBA as a block for treatment of posterior mandibular supracrestal defects in dogs was weaker in inducing new bone formation than PCL- TCP scaffold (26.63% versus 48.63%) (22). In vitro evidence showed proper cell attachment to various scaffolds but in vivo application demonstrated better results when MSCs were delivered by synthetic substitutes (Table 2). Conclusion To the best of our knowledge, bone regenerative potential of cells delivered to the defect site is not comparable to autogenous bone grafting although they can enhance bone healing when applied to bone defects. Future studies with the same protocols of cell cultivation, culture, seeding and delivery should be done in the field of regenerative medicine to reach from bench to bedside. Conflict of Interest: None declared.
7 Craniofacial regenerative medicine in 10 years 7 References 1. Lynch SE, Genco RJ, Marx RE. Tissue Engineering, Application in Oral and Maxillofacial Surgery and Periodontics. 2 ed. Chicago: Quintessence; Khojasteh A, Behnia H, Shayesteh YS, Morad G, Alikhasi M. Localized bone augmentation with cortical bone blocks tented over different particulate bone substitutes: a retrospective study. The International journal of oral & maxillofacial implants. 2012;27(6): Hassani A, Khojasteh A, Shamsabad AN. The anterior palate as a donor site in maxillofacial bone grafting: a quantitative anatomic study. Journal of oral and maxillofacial surgery : official journal of the American Association of Oral and Maxillofacial Surgeons. 2005;63(8): Khojasteh A, Behnia H, Naghdi N, Esmaeelinejad M, Alikhassy Z, Stevens M. Effects of different growth factors and carriers on bone regeneration: a systematic review. Oral surgery, oral medicine, oral pathology and oral radiology. 2013;116(6):e Phinney DG, Prockop DJ. Concise review: mesenchymal stem/multipotent stromal cells: the state of transdifferentiation and modes of tissue repair current views. Stem cells. 2007;25(11): Friedenstein AJ, Gorskaja J, Kulagina N. Fibroblast precursors in normal and irradiated mouse hematopoietic organs. Exp Hematol. 1976;4(5): Khojasteh A, Behnia H, Dashti SG, Stevens M. Current trends in mesenchymal stem cell application in bone augmentation: a review of the literature. Journal of oral and maxillofacial surgery : official journal of the American Association of Oral and Maxillofacial Surgeons. 2012;70(4): Mortazavi SH, Khojasteh A, Vaziri H, Khoshzaban A, Roudsari MV, Razavi SHE. The effect of fluoxetine on bone regeneration in rat calvarial bone defects. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(1): Shayesteh YS, Khojasteh A, Soleimani M, Alikhasi M, Khoshzaban A, Ahmadbeigi N. Sinus augmentation using human mesenchymal stem cells loaded into a β-tricalcium phosphate/hydroxyapatite scaffold. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(2): Jafarian M, Eslaminejad MB, Khojasteh A, Abbas FM, Dehghan MM, Hassanizadeh R et al. Marrow-derived mesenchymal stem cells-directed bone regeneration in the dog mandible: a comparison between biphasic calcium phosphate and natural bone mineral. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;105(5):e14-e Khojasteh A, Eslaminejad MB, Nazarian H. Mesenchymal stem cells enhance bone regeneration in rat calvarial critical size defects more than platelete-rich plasma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(3): Behnia H, Khojasteh A, Soleimani M, Tehranchi A, Khoshzaban A, Keshel SH et al. Secondary repair of alveolar clefts using human mesenchymal stem cells. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(2):e1-e Behnia H, Khojasteh A, Soleimani M, Tehranchi A, Atashi A. Repair of alveolar cleft defect with mesenchymal stem cells and platelet derived growth factors: a preliminary report. J Craniomaxillofac Surg. 2012;40(1): Behnia H, Khojasteh A, Kiani MT, Khoshzaban A, Abbas FM, Bashtar M, Dashti SG. Bone regeneration with a combination of nanocrystalline hydroxyapatite silica gel, platelet-rich growth factor, and mesenchymal stem cells: a histologic study in rabbit calvaria. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2013;115(2):e7-e Houshmand B, Behnia H, Khoshzaban A, Morad G, Behrouzi G, Dashti SG. Osteoblastic differentiation of human stem cells derived from bone marrow and periodontal ligament under the effect of enamel matrix derivative and transforming growth factor-beta. The International journal of oral & maxillofacial implants. 2012;28(6):e Behnia H, Khoshzaban A, Zarinfar M, Mashhadi Abbas F, Bahraminasab H, Khojasteh A. Histological Evaluation of Regeneration in Rabbit Calvarial Bone Defects Using Demineralized Bone Matrix, Mesenchymal Stem Cells and Platelet Rich in Growth Factor. J Dent Sch. 2012;30(3): Khojasteh A, Behnia H, Hosseini FS, Dehghan MM, Abbasnia P, Abbas FM. The effect of PCL TCP scaffold loaded with mesenchymal stem cells on vertical bone augmentation in dog mandible: A preliminary report. J Biomed Mater Res B Appl Biomater. 2013;101(5): Khojasteh A, Ghahremani MH, Ostad SN, Eslami M, Motahhary P, Morad G. The Effect of Deproteinized Bovine Bone Mineral on Saos-2 Cell Proliferation. Iran Endod J. 2013;8(3): Eslaminejad MB, Jafarian M, Khojasteh A, Abbas FM, Dehgahn M, Hassanizadeh R. In vivo bone formation by canine mesenchymal stem cells loaded onto HA/TCP scaffolds: qualitative and quantitative analysis. Yakhteh. 2008;10(3): Motamedian SR, Tabatabaei FS, Akhlaghi F, Torshabi M, Gholamin P, Khojasteh A. Response of Dental Pulp Stem Cells to Synthetic, Allograft, and Xenograft Bone Scaffolds. Int J Periodontics Restorative Dent. 21. Khojasteh A, Eslaminejad MB, Nazarian H, Morad G, Dashti SG, Behnia H. Vertical bone augmentation with simultaneous implant placement using particulate mineralized bone and mesenchymal stem cells: a preliminary study in rabbit. J Oral Implantol. 2013;39(1): Khojasteh A, Dashti SG, Dehghan MM, Behnia H, Abbasnia P, Morad G. The osteoregenerative effects of platelet derived growth factor BB cotransplanted with mesenchymal stem cells, loaded on freeze dried mineral bone block: A pilot study in dog mandible. J Biomed Mater Res B Appl Biomater. 2014;102(8): Bijonowski BM, Miller WM, Wertheim JA. Bioreactor design for perfusion-based, highly-vascularized organ regeneration. Current opinion in chemical engineering. 2013;2(1): Please cite this paper as: Khojasteh A, Motamedian SR. Mesenchymal Stem Cell Therapy for Treatment of Craniofacial Bone Defects: 10 Years of Experience. Regen Reconstr Restor. 2016; 1(1): 1-7. DOI: /rrr
Bone Engineering Arash Khojasteh, DMD, OMFS Assistant Professor of Oral and Maxillofacial Surgery Shahid Beheshti University of Medical Sciences
 Bone Engineering Arash Khojasteh, DMD, OMFS Assistant Professor of Oral and Maxillofacial Surgery Shahid Beheshti University of Medical Sciences Tissue Engineering VS Regenerative Medicine Insitu Vs Invitro
Bone Engineering Arash Khojasteh, DMD, OMFS Assistant Professor of Oral and Maxillofacial Surgery Shahid Beheshti University of Medical Sciences Tissue Engineering VS Regenerative Medicine Insitu Vs Invitro
BONE AUGMENTATION AND GRAFTING
 1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
1 A Computer-Guided Bone Block Harvesting Procedure: A Proof-of-Principle Case Report and Technical Notes Effectiveness of Lateral Bone Augmentation on the Alveolar Crest Dimension: A Systematic Review
Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway
 Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway Jieyuan Zhang, Xiaolin Liu, Haiyan Li, Chunyuan Chen, Bin Hu, Xin Niu, Qing
Exosomes/tricalcium phosphate combination scaffolds can enhance bone regeneration by activating the PI3K/Akt signalling pathway Jieyuan Zhang, Xiaolin Liu, Haiyan Li, Chunyuan Chen, Bin Hu, Xin Niu, Qing
PRP Usage in Today's Implantology
 Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
Volume 1, December 2004 www.implant.co.il PRP Usage in Today's Implantology by Dr. R. Shapira Introduction: Treating patients suffering from hematological disorders or using anticoagulant medications always
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary
 SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
SalvinOss Xenograft Bone Graft Material In Vivo Testing Summary Summary of In Vivo Use Of Bioresorbable Xenograft Bone Graft Materials In The Treatment Of One-Walled Intrabony Defects In A Canine Model
Sinus Augmentation Studies Methods and Definition
 FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
FDA approved indications for Infuse Bone Graft in the Maxillofacial Skeleton Alveolar Ridge Augmentation (Buccal Wall Defects) in the Maxilla Maxillary Sinus Floor augmentation Sinus Augmentation Studies
In vitro evaluation of isolation possibility of stem cells from intra oral soft tissue and comparison of them with bone marrow stem cells
 Original Article In vitro evaluation of isolation possibility of stem cells from intra oral soft tissue and comparison of them with bone marrow stem cells P. Torkzaban 1, A. Saffarpour 2, M. Bidgoli 1,
Original Article In vitro evaluation of isolation possibility of stem cells from intra oral soft tissue and comparison of them with bone marrow stem cells P. Torkzaban 1, A. Saffarpour 2, M. Bidgoli 1,
Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS
 Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Page 1 of 5 Issue Date: March 2003, Posted On: 8/1/2005 Multi-Modality Anterior Extraction Site Grafting Increased Predictability for Aesthetics Michael Tischler, DDS The extraction of teeth creates a
Pattern of bone resorption after extraction
 Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
Teeth loss Pattern of bone resorption after extraction 50% in 1st year 2/ 3 in first 3 months Reich KM, Huber CD, Lippnig WR, Um C, Watzek G, Tangl S. (2011, 17). Atrophy of Residual Alveolar Ridge following
More than bone regeneration. A total solution.
 More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
More than bone regeneration. A total solution. More than a dental implant company. A total solution. When it comes to treatment options, your patients want positive results both functionally and esthetically.
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alginate, tooth-shaped, for constructs, encapsulated pulp cells in, 589 590 Antibiotic paste, triple, change in root length and width
Index Note: Page numbers of article titles are in boldface type. A Alginate, tooth-shaped, for constructs, encapsulated pulp cells in, 589 590 Antibiotic paste, triple, change in root length and width
Chemicals in Surgical Periodontal Therapy
 Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
Chemicals in Surgical Periodontal Therapy von Alexandrina L. Dumitrescu 1. Auflage Chemicals in Surgical Periodontal Therapy Dumitrescu schnell und portofrei erhältlich bei beck-shop.de DIE FACHBUCHHANDLUNG
( ) 2009;28(2):89-94
 ( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
( ) 2009;28(2):89-94 Osseointegration is important in the functional aspect, however, esthetics is also important, especially in the maxillary anterior region. An adequate surgical technique is necessary
REFERENCES for PLATELET RICH PLASMA (PRP)
 REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
REFERENCES for PLATELET RICH PLASMA (PRP) Daif ET. Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral
Dental Implants: A Predictable Solution for Tooth Loss. Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor
 Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Dental Implants: A Predictable Solution for Tooth Loss Reena Talwar, DDS PhD FRCD(C) Oral & Maxillofacial Surgeon Associate Clinical Professor What are Dental Implants? Titanium posts used to replace missing
Posterior mandible and vertical augmentation
 CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
CASE REPORT Bilateral Vertical Ridge Augmentation With Block Grafts and Guided Bone Regeneration in the Posterior Mandible: A Case Report Maria A. Peñarrocha* Jose A. Vina Laura Maestre David Peñarrocha-Oltra
Procedure Manual and Catalog
 Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Procedure Manual and Catalog TM Why SynthoGraft? SynthoGraft offers a unique structure which provides stability, while its micro-porosity allows for rapid vascularization and subsequent resorption. Although
Versatile grafting Solutions
 Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
Versatile grafting Solutions A Canadian company serving Canadian dentists since 1997 Here s why your colleagues are calling us for their bone regeneration needs Founded in 1997 Citagenix has been providing
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute.
 chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
chronos Bone Void Filler. Beta-Tricalcium Phosphate ( β-tcp) bone graft substitute. Osteoconductive Resorbable Synthetic chronos Bone Void Filler chronos granules and preforms are synthetic, porous, osteoconductive,
botiss dental bone & tissue regeneration biomaterials collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
dental bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 botiss regeneration system maxresorb flexbone* collacone.. max
botiss biomaterials bone & tissue regeneration collacone max Innovative composite matrix socket preservation form-fitting resorbable composite
 bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
bone & tissue regeneration botiss biomaterials socket preservation Innovative composite matrix form-fitting resorbable composite 1 Socket preservation safeguarding your sockets collacone.. max flexbone*
Mesenchymal Stem Cells Reshape and Provoke Proliferation of Articular. State Key Laboratory of Bioreactor Engineering, East China University of
 Mesenchymal Stem Cells Reshape and Provoke Proliferation of Articular Chondrocytes by Paracrine Secretion Lei Xu, Yuxi Wu, Zhimiao Xiong, Yan Zhou, Zhaoyang Ye *, Wen-Song Tan * State Key Laboratory of
Mesenchymal Stem Cells Reshape and Provoke Proliferation of Articular Chondrocytes by Paracrine Secretion Lei Xu, Yuxi Wu, Zhimiao Xiong, Yan Zhou, Zhaoyang Ye *, Wen-Song Tan * State Key Laboratory of
The anatomic limitations of the. Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD*
 CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
CASE REPORT Implant Installation With Simultaneous Ridge Augmentation. Report of Three Cases Jun-Beom Park, DDS, MSD, PhD* The anatomic limitations of the residual alveolar bone may cause problems for
2.79J/3.96J/BE.441/HST522J DENTAL TISSUE REPLACEMENT AND REGENERATION
 Massachusetts Institute of Technology Harvard Medical School Brigham and Women s/massachusetts General Hosp. VA Boston Healthcare System 2.79J/3.96J/BE.441/HST522J DENTAL TISSUE REPLACEMENT AND REGENERATION
Massachusetts Institute of Technology Harvard Medical School Brigham and Women s/massachusetts General Hosp. VA Boston Healthcare System 2.79J/3.96J/BE.441/HST522J DENTAL TISSUE REPLACEMENT AND REGENERATION
The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up
 643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
643 The Use of Freeze-Dried Bone Allograft as an Alternative to Autogenous Bone Graft in the Atrophic Maxilla: A 3-Year Clinical Follow-up Marco Aurélio Bianchini, DDS, MSc, PhD 1 André R. Buttendorf,
Biomaterials Line. MIS Corporation. All Rights Reserved.
 7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
7. Biomaterials Line MIS Corporation. All Rights Reserved. 6. MIS s Quality System complies with international quality standards: ISO 13485: 2003 - Quality Management System for Medical Devices, ISO 9001:
A WIDE RANGE OF REGENERATIVE SOLUTIONS
 A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
A WIDE RANGE OF REGENERATIVE SOLUTIONS INDICATIONS: 1/ SOCKET AND RIDGE PRESERVATION 2/ FILLING OF EXTRACTION SOCKETS Biomaterials offers portfolio of regenerative materials for implantology, aimed at
An Owner's Guide to Natural Healing. Autologous Conditioned Plasma (ACP)
 An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
An Owner's Guide to Natural Healing Autologous Conditioned Plasma (ACP) Healing after an injury involves a well-orchestrated and complex series of events where proteins in the blood have primary roles,
Clinical UM Guideline
 Clinical UM Guideline Subject: Biological Materials to Aid in Soft and Hard Tissue Grafting Guideline #: 03-401 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This
Clinical UM Guideline Subject: Biological Materials to Aid in Soft and Hard Tissue Grafting Guideline #: 03-401 Current Effective Date: 03/24/2017 Status: New Last Review Date: 02/08/2017 Description This
SUPPLEMENTAL MATERIAL. Supplementary Methods
 SUPPLEMENTAL MATERIAL Supplementary Methods Culture of cardiomyocytes, fibroblasts and cardiac microvascular endothelial cells The isolation and culturing of neonatal rat ventricular cardiomyocytes was
SUPPLEMENTAL MATERIAL Supplementary Methods Culture of cardiomyocytes, fibroblasts and cardiac microvascular endothelial cells The isolation and culturing of neonatal rat ventricular cardiomyocytes was
The growing science of hard-tissue engineering
 RESEARCH Vertical Bone Augmentation With Simultaneous Implant Placement Using Particulate Mineralized Bone and Mesenchymal Stem Cells: A Preliminary Study in Rabbit Arash Khojasteh, DMD, MS 1 Mohamadreza
RESEARCH Vertical Bone Augmentation With Simultaneous Implant Placement Using Particulate Mineralized Bone and Mesenchymal Stem Cells: A Preliminary Study in Rabbit Arash Khojasteh, DMD, MS 1 Mohamadreza
INTERNATIONAL MEDICAL COLLEGE
 INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
INTERNATIONAL MEDICAL COLLEGE Joint Degree Master Program: Implantology and Dental Surgery (M.Sc.) Specialized Modules: List of individual modules Specialized Module 1 Basic principles of implantology
Inion BioRestore. Bone Graft Substitute. Product Overview
 Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
Inion BioRestore Bone Graft Substitute Product Overview Inion BioRestore Introduction Inion BioRestore is a synthetic bone graft substitute, which remodels into bone and is easy to use. Inion BioRestore
REASONS TO USE R.T.R.
 3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
3 REASONS TO USE R.T.R. AFTER EACH EXTRACTION Fully resorbable ß-TCP material RTR 3raisons 120x280.indd 1 16/06/15 10:52 1AVOID SPONTANEOUS RIDGE RESORPTION After tooth extraction, spontaneous healing
Scientific & Clinical Evidence Jason membrane
 Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Scientific & Clinical Evidence Jason membrane Pericardium GBR/GTR Membrane Facts - CE since 2009 - so far no serious clinical complication or objection - approx. 250.000 successful clinical treatments
Redefining Regeneration
 Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Redefining Regeneration Taking Volume to the MAX One Product, One Treatment, Real VOLUME Buccal Bone Loss Socket Preservation Lateral / Vertical Augmentation Grafting Material Scaffold Barrier (4-6 months)
Clinical UM Guideline
 Clinical UM Guideline Subject: Bone Grafts for Dental and Oral Surgical Services Guideline #: 04-201 Current Effective Date: 03/24/2017 Status: Revised Last Review Date: 02/08/2017 Description This document
Clinical UM Guideline Subject: Bone Grafts for Dental and Oral Surgical Services Guideline #: 04-201 Current Effective Date: 03/24/2017 Status: Revised Last Review Date: 02/08/2017 Description This document
THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS. Collagenated heterologous cortico-cancellous bone mix + TSV Gel GTO I N S P I R E D B Y N A T U R E
 GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
GTO THE NEW STANDARD OF EXCELLENCE IN BIOMATERIALS Collagenated heterologous cortico-cancellous bone mix + TSV Gel R E G E N E R A T I O N S C I E N C E I N S P I R E D B Y N A T U R E A unique biotechnology
Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs
 Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Current Applied Physics 5 (2005) 507 511 www.elsevier.com/locate/cap Evaluation of different grafting materials in three-wall intra-bony defects around dental implants in beagle dogs Ui-Won Jung a, Hee-Il
Innovative Range of Regenerative Solutions
 TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
TM Innovative Range of Regenerative Solutions MIS Implant Technologies Ltd. All rights reserved. Optimal volumes and quality of hard and soft tissue are required to satisfy the goals of oral rehabilitation
Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI Procedure. Subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
OSTEOAMP Allogeneic Morphogenetic Proteins Subtalar Nonunions OSTEOAMP Case Report SUBTALAR NONUNIONS Dr. Jason George DeVries and Dr. Brandon M. Scharer Orthopedic & Sports Medicine, Bay Care Clinic,
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
BEGO BIOMATERIALS When the result counts
 BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
BEGO BIOMATERIALS When the result counts Partners in Progress INTRO Challenge what exists get the right answers We practise systematic thinking with a passion and we are never satisfied with the status
Bone Grafting for Socket Preservation
 Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Bone Grafting for Socket Preservation Dr. Karl R. Koerner Normal extraction facial bone loss. Excessive force. Commonly the thickness of facial bone. Hussain, A. et al. Ridge preservation comparing a nonresorbable
Maxillary sinus augmentation without any graft material- A case Report
 A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
A CASE REPORT ISSN: 2321-4988 D.Shiva kumar et al. /JPR:BioMedRx: An International Journal 2013,1(8), Available online through www.jpronline.info Maxillary sinus augmentation without any graft material-
Ankle and subtalar arthrodesis
 OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
OSTEOAMP Allogeneic Morphogenetic Proteins Ankle Nonunions OSTEOAMP Case Report ANKLE NONUNIONS Dr. Jason George DeVries Orthopedic & Sports Medicine, Bay Care Clinic, 501 N. 10th Street, Manitowoc, WI
The body wants to heal
 58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
58 A promising new particulate graft material: a case study The body wants to heal DR PETER J.M. FAIRBAIRN, DETROIT MERCY, MI, USA, AND LONDON, ENGLAND, AND DR MINAS LEVENTIS, ATHENS, GREECE The notion
Protein-Mediated Anti-Adhesion Surface against Oral Bacteria
 Electronic Supplementary Material (ESI) for Nanoscale. This journal is The Royal Society of Chemistry 2018 Supporting Information Protein-Mediated Anti-Adhesion Surface against Oral Bacteria Xi Liu a,b,
Electronic Supplementary Material (ESI) for Nanoscale. This journal is The Royal Society of Chemistry 2018 Supporting Information Protein-Mediated Anti-Adhesion Surface against Oral Bacteria Xi Liu a,b,
Cartilage Engineering From Autologous Fat For Oro-Facial Deformity Reconstruction - Focus On The Nose
 Cartilage Engineering From Autologous Fat For Oro-Facial Deformity Reconstruction - Focus On The Nose 12-month progress report submitted to AOMS Mr Atheer Ujam PhD student Primary supervisor: Professor
Cartilage Engineering From Autologous Fat For Oro-Facial Deformity Reconstruction - Focus On The Nose 12-month progress report submitted to AOMS Mr Atheer Ujam PhD student Primary supervisor: Professor
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
Vertical and Horizontal Augmentation Using Guided Bone Regeneration. Ph.D. Thesis. Dr. med. dent. et univ. Istvan Urban
 Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Vertical and Horizontal Augmentation Using Guided Bone Regeneration Ph.D. Thesis Dr. med. dent. et univ. Istvan Urban Supervisor: Prof. Dr. Katalin Nagy, DDS, PhD Faculty of Dentistry, University of Szeged
Gladstone Institutes, University of California (UCSF), San Francisco, USA
 Fluorescence-linked Antigen Quantification (FLAQ) Assay for Fast Quantification of HIV-1 p24 Gag Marianne Gesner, Mekhala Maiti, Robert Grant and Marielle Cavrois * Gladstone Institutes, University of
Fluorescence-linked Antigen Quantification (FLAQ) Assay for Fast Quantification of HIV-1 p24 Gag Marianne Gesner, Mekhala Maiti, Robert Grant and Marielle Cavrois * Gladstone Institutes, University of
Years of research and advancement in
 Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Immediate Implants with Guided Bone Regeneration Using Titanium Mesh and Alloplast in an Infected Site: A Case Report Mahesh et al Dr. Lanka Mahesh 1 Dr. Ajay Bibra 2 Dr. Vishal Gupta 3 Abstract Years
Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla
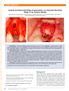 CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
CASE REPORT Vertical and Horizontal Ridge Augmentation of a Severely Resorbed Ridge in the Anterior Maxilla Alberto Monje,* Florencio Monje, Fernando Suarez,* Raúl González-García, Laura Villanueva-Alcojol,
Alpha-Bio's GRAFT complete portfolio bone substitutes resorbable membranes best combination of quality & value with efficient, easy-to-use products
 Alpha-Bio Tec, a world leader in advanced implantology solutions, is proud to present its growing biomaterials product line: Alpha-Bio's GRAFT, which has taken a leading position in the global dental biomaterials
Alpha-Bio Tec, a world leader in advanced implantology solutions, is proud to present its growing biomaterials product line: Alpha-Bio's GRAFT, which has taken a leading position in the global dental biomaterials
Case Study. Case # 1 Author: Dr. Suheil Boutros (USA) 2013 Zimmer Dental, Inc. All rights reserved. 6557, Rev. 03/13.
 Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Placement of a Zimmer Trabecular Metal Dental Implant with Simultaneous Ridge Augmentation and Immediate Non-Functional Loading Following Tooth Extraction and Orthodontic Treatment for Implant Site Development
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation. Sanju P. Jose
 Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Evaluation of a Combination Allograft Material Compared to DFDBA in Alveolar Ridge Preservation by Sanju P. Jose B.S., University of Maryland Baltimore County, 2008 D.D.S., University of Maryland School
Repair of human periodontal bone defects by autologous grafting stem cells derived from inflammatory dental pulp tissues
 Li et al. Stem Cell Research & Therapy (2016) 7:141 DOI 10.1186/s13287-016-0404-2 RESEARCH Open Access Repair of human periodontal bone defects by autologous grafting stem cells derived from inflammatory
Li et al. Stem Cell Research & Therapy (2016) 7:141 DOI 10.1186/s13287-016-0404-2 RESEARCH Open Access Repair of human periodontal bone defects by autologous grafting stem cells derived from inflammatory
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report
 Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
Alveolar Ridge Augmentation with Titanium Mesh and Particulate Allograft A Case Report Dr. Pratibha Borasi, Dr. Praneeta Kamble Department of Periodontics, Nair Hospital Dental College, Mumbai, Maharashtra,
THE NEXT FRONTIER OF BONE REGENERATION. where Technology meets Nature
 THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
THE NEXT FRONTIER OF BONE REGENERATION where Technology meets Nature SmartBone is a new hybrid bioactive bone substitute specifically developed for bone regeneration in reconstructive surgery. SmartBone
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT
 ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
ALVEOLAR RIDGE AUGMENTATION UTILIZING PLATELET RICH FIBRIN IN COMBINATION WITH DEMINERALIZED FREEZE-DRIED BONE ALLOGRAFT A CASE REPORT * Mishal Piyush Shah 1 and Sheela Kumar Gujjari 2 1 Department of
L6 GLUT4myc Cell Growth Protocol
 L6 GLUT4myc Cell Growth Protocol Background: Parental L6 cells selected for high fusion (2, 3) were stably transfected with a rat GLUT4 cdna carrying a myc epitope (recognized by the commercially available
L6 GLUT4myc Cell Growth Protocol Background: Parental L6 cells selected for high fusion (2, 3) were stably transfected with a rat GLUT4 cdna carrying a myc epitope (recognized by the commercially available
ab Adipogenesis Assay Kit (Cell-Based)
 ab133102 Adipogenesis Assay Kit (Cell-Based) Instructions for Use For the study of induction and inhibition of adipogenesis in adherent cells. This product is for research use only and is not intended
ab133102 Adipogenesis Assay Kit (Cell-Based) Instructions for Use For the study of induction and inhibition of adipogenesis in adherent cells. This product is for research use only and is not intended
Contemporary Implant Dentistry
 Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Contemporary Implant Dentistry C H A P T ER 1 4 O F C O N T E M P OR A R Y O R A L A N D M A X I L L OFA C IA L S U R G E RY B Y : D R A R A S H K H O J A S T EH Dental implant is suitable for: completely
Management of a complex case
 2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
2 Soft- and hard-tissue reconstruction of a severely deficient site prior to implant placement: a case report Management of a complex case Younes Khosroshahy, DDS, MFDS RCS (Eng), Dip Imp Dent RCSEd, Blue
Oral Health and Dentistry
 Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Page 107 to 118 Volume 1 Issue 2 2017 Case Report Oral Health and Dentistry ISSN: 2573-4989 Full Mouth Implants Rehabilitation of a Patient with Ectodermal Dysplasia After 3-Ds Ridge Augmentation and Bilateral
Complications of postoperative swelling of the maxillary sinus membrane after sinus floor augmentation
 Complications of postoperative swelling of the maxillary sinus membrane after sinus floor augmentation Abstract Objective The aim of this article was to investigate postoperative swelling of the maxillary
Complications of postoperative swelling of the maxillary sinus membrane after sinus floor augmentation Abstract Objective The aim of this article was to investigate postoperative swelling of the maxillary
RELIABLE WHEN IT COUNTS. The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4
 RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
RELIABLE WHEN IT COUNTS 1 RELIABLE WHEN IT COUNTS RESISTANT TO EXPOSURE The unique collagenase-resistant membrane protects bone graft and supports treatment success even when exposed 4 RELIABLE BARRIER
Developments in bone grafting in veterinary orthopaedics part one
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Developments in bone grafting in veterinary orthopaedics part one Author : John Innes, Peter Myint Categories : Vets Date
Symbios Xenograft Granules Porcine Bone Graft Material
 Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Symbios Xenograft Granules Porcine Bone Graft Material 32671122-USX-1607_Symbios Highlight Brochure.indd 1 2016-09-27 12:12 Symbios Xenograft Granules Porcine bone graft material Symbios Xenograft Granules
Cerasorb M DENTAL. O:\Zulassung\Cerasorb Dental Kanada 2013\Texte\Cerasorb M Dental final IFU docx
 Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Cerasorb M DENTAL Resorbable, pure-phase beta-tricalcium phosphate matrix with interconnecting porosity for bone regeneration for use in dental and maxillofacial surgery DESCRIPTION: Cerasorb M DENTAL
Guided Tissue and Bone Regeneration
 Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Guided Tissue and Bone Regeneration One toolbox for your needs! Tefguide 9000 742 401 12x24 mm pc 1 Osgide 9000 701 520 15 x 20 mm pc 1 Osbone 9000 800 255 250-1000 μm 0.25 cc 5 Product Specifications
Protocol for Gene Transfection & Western Blotting
 The schedule and the manual of basic techniques for cell culture Advanced Protocol for Gene Transfection & Western Blotting Schedule Day 1 26/07/2008 Transfection Day 3 28/07/2008 Cell lysis Immunoprecipitation
The schedule and the manual of basic techniques for cell culture Advanced Protocol for Gene Transfection & Western Blotting Schedule Day 1 26/07/2008 Transfection Day 3 28/07/2008 Cell lysis Immunoprecipitation
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the
 In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the art materials science with concepts from the life sciences.
In the last decade of the 20 th century, special emphasis was put on an emerging field of science: Tissue engineering,which combines the state of the art materials science with concepts from the life sciences.
Department of Oral and Maxillofacial Surgery, Loma Linda University, Loma Linda, CA 92354, USA 2
 Plastic Surgery International Volume 2011, Article ID 165824, 7 pages doi:10.1155/2011/165824 Review Article Reconstruction of Mandibular Defects Using Bone Morphogenic Protein: Can Growth Factors Replace
Plastic Surgery International Volume 2011, Article ID 165824, 7 pages doi:10.1155/2011/165824 Review Article Reconstruction of Mandibular Defects Using Bone Morphogenic Protein: Can Growth Factors Replace
Application of mesenchymal stem cells in bone regenerative procedures in oral implantology. A literature review
 Journal section: Implantology Publication Types: Review doi:10.4317/jced.51186 http://dx.doi.org/10.4317/jced.51186 Application of mesenchymal stem cells in bone regenerative procedures in oral implantology.
Journal section: Implantology Publication Types: Review doi:10.4317/jced.51186 http://dx.doi.org/10.4317/jced.51186 Application of mesenchymal stem cells in bone regenerative procedures in oral implantology.
FDBA(Freeze Dried Bone Allograft) SureOss Cortical Bone - Powder / Chip. OsteOss Cortical with Cancellous Bone - Powder / Chip
 PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
PERIODONTAL Bone & Skin Allograft Products FDBA(Freeze Dried Bone Allograft) SureOss - Powder / Chip OsteOss Cortical with - Powder / Chip DFDBA(Demineralized Freeze Dried Bone Allograft) SureOss -D Demineralized
Clinical Report The Use of Autogenous Bone Grafting With Platelet-Rich Plasma for Alveolar Ridge Reconstruction: A Clinical Report
 The Use of Autogenous Bone Grafting With Platelet-Rich Plasma for Alveolar Ridge Reconstruction: A Ziv Simon, DMD, MSc, and Joseph Friedlich, DDS Abstract Implant dentistry has become an effective and
The Use of Autogenous Bone Grafting With Platelet-Rich Plasma for Alveolar Ridge Reconstruction: A Ziv Simon, DMD, MSc, and Joseph Friedlich, DDS Abstract Implant dentistry has become an effective and
ctive Bone Bonding Bone Regeneration Osteostimulation*
 www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
www.bonalive.com ctive Bone Bonding Bone Regeneration Osteostimulation* A revolution in bone grafting Osteoconductive bone graft substitute with osteostimulative* properties *non-osteoinductive Before
Does Hyperbaric Oxygen Therapy Improve Bone Regeneration With Mesenchymal Stem Cells
 Does Hyperbaric Oxygen Therapy Improve Bone Regeneration With Mesenchymal Stem Cells Johannes Schneppendahl, MD 1, Jan Grassmann, MD 1, Marcel Betsch, M.D. 2, Michael Wild, MD, PhD 3, Mohssen Hakimi, MD,
Does Hyperbaric Oxygen Therapy Improve Bone Regeneration With Mesenchymal Stem Cells Johannes Schneppendahl, MD 1, Jan Grassmann, MD 1, Marcel Betsch, M.D. 2, Michael Wild, MD, PhD 3, Mohssen Hakimi, MD,
Bone marrow-derived mesenchymal stem cells improve diabetes-induced cognitive impairment by
 Nakano et al. Supplementary information 1. Supplementary Figure 2. Methods 3. References Bone marrow-derived mesenchymal stem cells improve diabetes-induced cognitive impairment by exosome transfer into
Nakano et al. Supplementary information 1. Supplementary Figure 2. Methods 3. References Bone marrow-derived mesenchymal stem cells improve diabetes-induced cognitive impairment by exosome transfer into
Surgical Therapy. Tuesday, April 2, 13. Alessan"o Geminiani, DDS, MS
 Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Surgical Therapy Alessan"o Geminiani, DDS, MS Periodontal Flap: a surgical procedure in which incisions are made in the gingiva or mucosa to allow for separation of the epithelium and connective tissues
Puros Cancellous Particulate Allograft & Puros Block Allograft
 Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
Puros Cancellous Particulate Allograft & Puros Block Allograft Puros Cancellous Particulate Allograft The Natural Choice For Healthy 1 Bone Growth. 1. Proven, Predictable Regeneration Acts as an osteoconductive
The Original remains unique.
 The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
The Original remains unique. Geistlich leading regeneration 2A, 2B Geistlich is the world leader in regenerative dentistry. We transform natural biomaterials into safe and reliable treatment methods that
Product Catalog. Dental Bone & Tissue Regeneration
 Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
Product Catalog Dental Bone & Tissue Regeneration Bone graft regeneration Guided bone substitutes regeneration Osteogenesis Controlled resorption rate Angiogenesis Long term volume stability Remodeling
Socket preservation in the daily practice: A clinical case report
 Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
Clinical Socket preservation in the daily practice: A clinical case report Rabih Abi Nader 1 and Carine Tabarani 2 Abstract Soft tissue contour depends on the underlying bone anatomy. Following tooth extraction,
SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT
 MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
MAVEN CASE REPORT SOCKET WHETHER TO PRESERVE IT NOW OR TO CREATE LATER? - A CASE REPORT Dr. Parthasarathi Biswas 1, Dr. Debajyoti Mondal 1, Dr. B Praveena Devi 1, Dr. Indrasri Das 2, Dr. Somen Bagchi 3,
easy-graft TM CRYSTAL
 1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
1 easy-graft TM CRYSTAL Overview 2 Advantages easy-graft : principle & application Material & studies Indications easy-graft CRYSTAL & CLASSIC Advantages of easy-graft CRYSTAL 3 Easy handling: Injectable
ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report
 ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report Yaqian Chen, Qingqing Wu, Yi Man State Key Laboratory of Oral Diseases, West China
ß-tricalcium phosphate used with onlay graft for horizontal bone augmentation yielded preferable result: a case report Yaqian Chen, Qingqing Wu, Yi Man State Key Laboratory of Oral Diseases, West China
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS
 rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
rhpdgf-bb/β-tcp TECHNOLOGY OVERVIEW AUGMENT Bone Graft THE FIRST AND ONLY PROVEN ALTERNATIVE TO AUTOGRAFT IN ANKLE AND HINDFOOT ARTHRODESIS AUGMENT Bone Graft T HE F I R S T A ND O N LY PROV EN A LT ERN
Supplemental Experimental Procedures
 Cell Stem Cell, Volume 2 Supplemental Data A Temporal Switch from Notch to Wnt Signaling in Muscle Stem Cells Is Necessary for Normal Adult Myogenesis Andrew S. Brack, Irina M. Conboy, Michael J. Conboy,
Cell Stem Cell, Volume 2 Supplemental Data A Temporal Switch from Notch to Wnt Signaling in Muscle Stem Cells Is Necessary for Normal Adult Myogenesis Andrew S. Brack, Irina M. Conboy, Michael J. Conboy,
Supplementary data Supplementary Figure 1 Supplementary Figure 2
 Supplementary data Supplementary Figure 1 SPHK1 sirna increases RANKL-induced osteoclastogenesis in RAW264.7 cell culture. (A) RAW264.7 cells were transfected with oligocassettes containing SPHK1 sirna
Supplementary data Supplementary Figure 1 SPHK1 sirna increases RANKL-induced osteoclastogenesis in RAW264.7 cell culture. (A) RAW264.7 cells were transfected with oligocassettes containing SPHK1 sirna
BioVin Collagen Membrane
 BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
BioVin Collagen Membrane Resorbable cross-linked collagen membrane BioVin Bovine Bone Bovine Bone Substitute OToss Synthetic Bone Synthetic Resorbable Biphasic Calcium Phosphate OToss Synthetic Bone Inject
Ridge Augmentation. Selection of Applicable Abstracts and Posters. Using Titanium-Reinforced PTFE Membranes
 Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Ridge Augmentation Selection of Applicable Abstracts and Posters Using Titanium-Reinforced PTFE Membranes Gultekin BA, Cansiz E, Borahan MO. Clinical and 3-Dimensional Radiographic Evaluation of Autogenous
Instructions for Use. APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests
 3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
3URGXFW,QIRUPDWLRQ Sigma TACS Annexin V Apoptosis Detection Kits Instructions for Use APO-AB Annexin V-Biotin Apoptosis Detection Kit 100 tests For Research Use Only. Not for use in diagnostic procedures.
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH
 PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH PRO-STIM Injectable Inductive Graft TECHNICAL MONOGRAPH Headline Contents Headline Appendix 4 5 7 8 13 14 Clinical Benefits Self-Forming Porous Scaffold
Mouse primary keratinocytes preparation
 Mouse primary keratinocytes preparation 1. Fill a 150 X 25 mm petri dish with ice. Put newborn mice (2 3 days old) in the petri dish and insert it in an ice bucket. Leave the mice in the ice bucket for
Mouse primary keratinocytes preparation 1. Fill a 150 X 25 mm petri dish with ice. Put newborn mice (2 3 days old) in the petri dish and insert it in an ice bucket. Leave the mice in the ice bucket for
In vitro Growth and Characterization of Stem Cells from Human Dental Pulp of Deciduous Versus Permanent Teeth
 Original Article In vitro Growth and Characterization of Stem Cells from Human Dental Pulp of Deciduous Versus Permanent Teeth MR. Baghaban Eslaminejad 1, S. Vahabi 2, M. Shariati 3, H. Nazarian 1 1 Associate
Original Article In vitro Growth and Characterization of Stem Cells from Human Dental Pulp of Deciduous Versus Permanent Teeth MR. Baghaban Eslaminejad 1, S. Vahabi 2, M. Shariati 3, H. Nazarian 1 1 Associate
Gene Activation for Excellent Bone Remodeling
 Osteostimulative bone regeneration granules Gene Activation for Excellent Bone Remodeling Injectable Putty Granules BIOMATERIALS STIMULATING THE BONE REGENERATION Noraker has been involved in biomaterial
Osteostimulative bone regeneration granules Gene Activation for Excellent Bone Remodeling Injectable Putty Granules BIOMATERIALS STIMULATING THE BONE REGENERATION Noraker has been involved in biomaterial
