Goals of this lecture. Case 2/24/2012. Drug eruptions. The red leg. Pyoderma gangrenosum
|
|
|
- Dustin Harvey
- 5 years ago
- Views:
Transcription
1 Goals of this lecture Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco Drug eruptions Tell the difference between a benign and serious drug eruption Know which drug(s) to stop The red leg Recognize the mimics of cellulitis Pyoderma gangrenosum Avoid a potential disaster Case 46 year old HIV+ man admitted to ICU for r/o sepsis Severely hypotensive IV fluids, norepinephrine Sepsis? antibiotics are started At home has been taking trimethoprim/sulfamethoxazol e for UTI 1
2 Per the drug chart, the most likely culprit is: Day Day -> A vancomycin x x x x B metronidazole x x C ceftriaxone x x x D norepinephrine x x x E omeprazole x x x x F SQ heparin x x x x G trimethoprim/ sulfamethoxazole x x x x x x x 70% Per the drug chart, the most likely culprit is: Day Day -> A vancomycin x x x x B metronidazole x x C ceftriaxone x x x D norepinephrine x x x E omeprazole x x x x F SQ heparin x x x x G trimethoprim/ sulfamethoxazole x x x x x x x A. A B. B 16% C. C D. D E. E 0% 11% 0% 0% 3% Admit day Rash onset Admit day Rash onset F. F G. G A. B. C. D. E. F. G. Drug reactions: 3 things you need to know 1. Type of drug reaction 2. Statistics: Which drugs are most likely to cause that type of reaction? 3. Timing: How long after the drug started did the reaction begin? Drug Eruptions: Degrees of Severity Simple Morbilliform drug eruption Minimal systemic symptoms Complex Drug hypersensitivity reaction Stevens-Johnson syndrome (SJS) Toxic epidermal necrolysis (TEN) Systemic involvement Potentially life threatening 2
3 Common Causes of Cutaneous Drug Eruptions Antibiotics NSAIDs Sulfa Allopurinol Anticonvulsants Morbilliform (Simple) Drug Eruption Begins 5-10 days after drug started Erythematous macules, papules Pruritus No systemic symptoms Risk factors: EBV, HIV infection Treatment: D/C medication diphenhydramine, topical steroids Resolves 7-10 days after drug stopped Gets worse before gets better Simple drug eruption- day 1 Simple drug eruption- day 3 3
4 Simple drug eruption- day 7 Hypersensitivity Reactions Skin eruption associated with systemic symptoms and alteration of internal organs DRESS - Drug reaction w/ eosinophilia and systemic symptoms Begins 2-6 weeks after medication started time to abnormally metabolize the medication Mortality 10-25% Hypersensitivity Reactions Drugs Aromatic anticonvulsants phenobarbital, carbamazepine, phenytoin THESE CROSS-REACT Sulfonamides Lamotrigine Dapsone Allopurinol (HLA-B*5801) NSAIDs Other Abacavir (HLA- B*5701) Nevirapine (HLA-DRB1*0101) Minocycline, metronidazole, azathioprine, gold salts Each class of drug causes a slightly different clinical picture Hypersensitivity Reactions Clinical features Rash Fever (precedes eruption by day or more) Pharyngitis Hepatitis Arthralgias Lymphadenopathy Hematologic abnormalities eosinophilia atypical lymphocytosis Other organs involved myocarditis, interstitial pneumonitis, interstitial nephritis, thyroiditis 4
5 Hypersensitivity Reactions- Treatment Stop the medication Follow CBC with diff, LFT s, BUN/Cr Avoid cross reacting medications!!!! Aromatic anticonvulsants cross react (70%) Phenobarbital, Phenytoin, Carbamazepine Valproic acid and Keppra generally safe Systemic steroids (Prednisone 1.5-2mg/kg) Taper slowly- 1-3 months Allopurinol hypersensitivity may require steroid sparing agent NOT azathioprine (also metabolized by xanthine oxidase) Completely recover, IF the hepatitis resolves Check TSH monthly for 6 months Watch for later cardiac involvement (low EF) Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) Medications Sulfonamides Aromatic anticonvulsants (carbamazapine [HLA-B*1502], phenobarbital, phenytoin) Allopurinol (HLA-B*5801) NSAIDs (esp Oxicams) Nevirapine (HLA-DRB1*0101) Lamotrigine Weaker link: Sertraline, Pantoprazole, Tramadol J Invest Dermatol Jan;128(1):
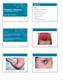
6 Stevens-Johnson (SJS) versus Toxic Epidermal Necrolysis (TEN) Disease BSA SJS < 10% SJS/TEN overlap 10-30% TEN with spots > 30% TEN without spots Sheets of epidermal loss > 10% Stevens-Johnson (SJS) versus Toxic Epidermal Necrolysis (TEN) SJS TEN Atypical targets Mucosal membranes 2 Causes: Drugs Mycoplasma HSV Erythema, bullae Skin pain Mucosal membranes 2 Causes: Drugs Stevens-Johnson Syndrome Stevens-Johnson Syndrome 6
7 Stevens-Johnson Syndrome / Toxic epidermal necrolysis Toxic Epidermal Necrolysis Toxic Epidermal Necrolysis SJS/TEN: Emergency Management Stop all unnecessary medications The major predictor of survival and severity of disease Ophthalmology consult Check for Mycoplasma- 25% of SJS in pediatric patients Treat like a burn patient, but don t overhydrate Monitor fluid and electrolyte status Nutritional support Warm environment Respiratory care Death (up to 25% of patients with more than 30% skin loss, age dependent) 7
8 SJS/TEN: Treatment Topical Protect exposed skin, prevent secondary infection Aquaphor and Vaseline gauze Systemic- controversial No role for empiric antibiotics Surveillance cultures Treat secondary infection (septicemia) Consider antivirals SJS: high dose corticosteroids mg/kg prednisone (no RCT) TEN: IVIG 0.5-1g/kg/d x 4d Case 83 yo female admitted for slowly increasing LE erythema and poor response to outpatient antibiotics HPI: increasing LE erythema, edema over 3 weeks, somewhat painful PMHx: Sjogren s syndrome, Hashimoto s thyroiditis, Addison s disease 8
9 The red leg Infectious Cellulitis/erysipelas Necrotizing fasciitis Pyomyositis Non-Infectious Vasculitis Pigmented purpuric dermatosis Asteatotic dermatitis Pretibial myxedema Erythema nodosum Contact dermatitis Stasis dermatitis Cellulitis Infection of the dermis Gp A beta hemolytic strep and Staph aureus Rapidly spreading Erythematous, tender plaque, not fluctuant Lower leg Rarely bilateral Patient often toxic WBC, LAD, streaking Treat tinea pedis 9
10 Vasculitis Palpable purpura Degree increases from cephalad to caudad Favors dependent areas (lower legs) May itch, sting, or burn Associated sx: fever, malaise, arthralgias Characteristic skin biopsy Broad differentialconsult dermatology Leukocytoclastic Vasculitis - Etiology Dependent area in hospitalized patient Conditions associated with LCV Idiopathic (45-55%) Infection (15-20%) Inflammatory diseases (15-20%) Medications (10-15%) Malignancy (<5%) Other Hypergammaglobulinemic purpura of Waldenström HIV Cocaine use (p-anca +) 10
11 Leukocytoclastic Vasculitis- Etiology Infection Group A β-hemolytic Streptococcus Tuberculosis Inflammatory diseases Connective tissue disease, inflammatory bowel disease, bowel-associated dermatitis-arthritis syndrome, neutrophilic dermatoses Medications sulfonamides, penicillins, allopurinol, phenytoin, thiazides, quinolones Eosinophils in drug induced vasculitis: 79% systemic, 22% skin only Malignancy Lymphoproliferative (>solid) Pigmented Purpuric Eruption 1-3 cm patch/plaques on the lower leg Confluent tiny papules with hemorrhage Brown-yellow hyperpigmentation due to iron deposition Location: Pretibial Natural history: Chronic Elderly males favored Asymptomatic or pruritic Asteatotic Dermatitis Occurs on the lower legs, the flanks, and the arms Spares the armpits, groin, face First stage: flaking of the skin, pruritic Second stage: cracking of the skin looking like the bed of a dry lake; itchy and stings Third stage: Weepy dermatitis, ITCHY Treatment Moisturize Mid potency topical steroid (TAC) ointment Pretibial Myxedema Bilateral, localized Nonpitting infiltration Nodules and plaques Elephantiasis-like 11
12 Thyroid Dermopathy Pretibial Myxedema Treatment Does not respond to treatment of thyroid disease Intralesional triamcinolone High potency topical steroids under occlusion Compression Erythema Nodosum Reactive condition on the lower legs Females: Males = 3-10:1 Tender, deep, red nodules on the anterior>posterior calves; 1-5 cm Lesions resolve with faint bruise; do not drain! May be associated arthritis/tenosynovitis (ankles, knees); fever 12
13 Triggers of EN Infections: Strep pharyngitis, tuberculosis, systemic fungus (coccidioidomycosis), Yersinia (diarrhea) Sarcoidosis; Behcet s Inflammatory Bowel Disease Pregnancy Medications: OCP s Erythema Nodosum Diagnosis and Treatment Clinical, but biopsy if not responding Treatment: Elevation, bedrest, reduced exercise Support stockings NSAID s or indomethacin SSKI 5-15 gtts TID (this works!!) Look for the trigger Contact Dermatitis Itch >>> pain Patient is non-toxic Erythema and edema can be severe Topical meds and Rhus dermatitis (Poison Oak) are common causes Treat with topical steroids for most cases, but systemic steroids for Rhus dermatitis (2-3 weeks) Contact Dermatitis Leg ulcers are commonly complicated by allergic contact dermatitis Common causes Applied antibiotics (Neomycin, Bacitracin) Topical anesthetics (benzocaine) Other (Vitamin E, topical benadryl) Avoid all topical antibiotics to leg ulcers (except topical metronidazole to prevent odor) 13
14 Stasis Dermatitis/Venous Insufficiency Due to venous hypertension Often bilateral Itchy and/or painful Red, hot, swollen leg No fever, elevated WBC, LAD, streaking Look for: varicosities, edema, venous ulceration, hemosiderin deposition Pinpoint yellow-brown macules and papules = hemosiderin Superimposed contact dermatitis common Stasis Dermatitis/ Venous Insufficiency End stage is permanent sclerosis (sclerotic panniculitis / lipodermatosclerosis) with inverted champagne bottle legs Treat with topical corticosteroids, leg elevation, and compression stockings Stasis Dermatitis/ Venous Insufficiency and Lymphatic Insufficiency As complication of recurrent infection and obesity, edema becomes firm (non-pitting) Skin becomes pebbly, hyperkeratotic and rough (elephantiasis verrucosa nostra = lymphostasis verrucosa cutis) Ulceration in this setting (with lymphatic and venous insufficiency) is significantly harder to heal 14
15 The Red Leg: Key features of the physical exam: Fever Pain Warmth Bilateral Streaking Lymphadenopathy Elevated WBC Cellulitis Yes Yes Yes Almost never Yes Yes Yes Consider another diagnosis No +/- +/- often No No No Case 67M underwent an elective saphenous vein phlebectomy for asymptomatic varicosities 4d post op, he develops erythema around the wound. Ulceration continues to expand despite multiple debridements and broad spectrum antibiotics. Wound cultures are negative 3 weeks later, he is transferred to UCSF and a dermatology consultation is called Tmax 104, WBC 22 15
16 Pyoderma Gangrenosum Rapidly progressive (days) ulcerative process Begins as a small pustule which breaks down forming an ulcer Undermined violaceous border Expands by small peripheral satellite ulcerations which merge with the central larger ulcer Occur anywhere on body Triggered by trauma (pathergy) (surgical debridement, attempts to graft) 16
17 Pyoderma Gangrenosum 50% have no underlying cause Associations (50%): Inflammatory bowel disease (1.5%-5% of IBD patients get PG) Rheumatoid arthritis Seronegative arthritis Hematologic abnormalities (AML) Pyoderma Gangrenosum Workup Skin biopsy for H&E and culture Rheumatoid factor SPEP/UPEP ANCA (ulcers of Wegener granulomatosis can mimic PG) Colonscopy (r/o IBD) Peripheral smear, Bone marrow biopsy (r/o AML) Pyoderma Gangrenosum Treatment AVOID DEBRIDEMENT Refer to dermatology Treatment of underlying disease may not help PG Topical therapy: Superpotent steroids Topical tacrolimus Systemic therapy: Systemic steroids Cyclosporine or Tacrolimus Cellcept Thalidomide TNF-blockers (Remicade) 17
18 A few simple rules to live by: Don t use lotrisone! Never give systemic steroids for psoriasis or atopic dermatitis Only 50% of abnormal nails are due to fungal infections Do an excisional biopsy to diagnose melanoma Cellulitis is almost never bilateral Drug eruptions are usually due to medications started 7-10 prior to onset of the rash 18
Question 1: Per the drug chart, the most likely culprit is:
 Disclosures I have no conflicts of interest to disclose Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco 2
Disclosures I have no conflicts of interest to disclose Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service Department of Dermatology University of California, San Francisco 2
Goals of this talk. Morbilliform. Common Morphologies in the Hospital 11/7/2017. Hospital Based Dermatology: Common and Tough Consult Cases
 Hospital Based Dermatology: Common and Tough Consult Cases Lindy P. Fox MD Associate Professor of Clinical Dermatology Director, Hospital Consultation Service University of California, San Francisco lindy.fox@ucsf.edu
Hospital Based Dermatology: Common and Tough Consult Cases Lindy P. Fox MD Associate Professor of Clinical Dermatology Director, Hospital Consultation Service University of California, San Francisco lindy.fox@ucsf.edu
Disclosures. Outline. Goals of this lecture. Common Dermatologic Disorders: Tips for Diagnosis and Management Part 2 3/26/2014
 Common Dermatologic Disorders: Tips for Diagnosis and Management Part 2 Disclosures I have no conflicts of interest to disclose Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service
Common Dermatologic Disorders: Tips for Diagnosis and Management Part 2 Disclosures I have no conflicts of interest to disclose Lindy P. Fox, MD Associate Professor Director, Hospital Consultation Service
PSEUDO-CELLULITIS - ALL THAT S RED IS NOT INFECTION
 JAN 18 2018 ASP ECHO CLINIC CHARLES KRASNER, M.D. PSEUDO-CELLULITIS - ALL THAT S RED IS NOT INFECTION FIRST HOSPITALIZATION: 62 YEAR OLD MALE ADMITTED WITH DIAGNOSIS OF CELLULITIS Hx of AODM, Morbid Obesity,
JAN 18 2018 ASP ECHO CLINIC CHARLES KRASNER, M.D. PSEUDO-CELLULITIS - ALL THAT S RED IS NOT INFECTION FIRST HOSPITALIZATION: 62 YEAR OLD MALE ADMITTED WITH DIAGNOSIS OF CELLULITIS Hx of AODM, Morbid Obesity,
Cutaneous Drug Reactions
 Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Pediatric Dermatology
 Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Case 1. Debridement Cultures Keflex Silvadene
 The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
9/9/17. Disclosures" Dermatology in Primary Care: Recognition and treatment of common disorders of the skin" A preview" Classic skin infections"
 Disclosures Dermatology in Primary Care: Recognition and treatment of common disorders of the skin I have no conflicts of interest to disclose. I may discuss off-label use of treatments for cutaneous disease.
Disclosures Dermatology in Primary Care: Recognition and treatment of common disorders of the skin I have no conflicts of interest to disclose. I may discuss off-label use of treatments for cutaneous disease.
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa
 More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving
 Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Big rashes in little patients:
 ! Big rashes in little patients: Severe drug eruptions and cutaneous infections!! Marcia Hogeling, MD, FAAD Assistant Clinical Professor Director, Pediatric Dermatology Division of Dermatology David Geffen
! Big rashes in little patients: Severe drug eruptions and cutaneous infections!! Marcia Hogeling, MD, FAAD Assistant Clinical Professor Director, Pediatric Dermatology Division of Dermatology David Geffen
Cellulitis: a practical guide
 Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Bugs and Drugs: What s New in Hypersensitivity Reactions?
 Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Bugs and Drugs: What s New in Hypersensitivity Reactions? Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY
Case 1 History. William Tremaine, M.D. CP
 Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Emergency Dermatology. Emergency Dermatology
 Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
Emergency Dermatology These are rapidly progressive skin conditions and some are potentially lifethreatening. Early recognition is important to implement prompt supportive care and therapy. Some are drug
SJS/TEN spectrum. Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) 10/7/2016
 Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
Jesse Keller MD Assistant Professor Oregon Health & Science University Stevens-Johnson syndrome (SJS) /Toxic Epidermal Necrolysis (TEN) Drug induced dermemergencies that exist on a spectrum Delayed reaction:
Skin Manifestations of Drug Reactions
 Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
CASE REPORT ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX
 ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
ATYPICAL BULLOUS PYODERMA GANGRENOSUM WITH EARLY LESIONS MIMICKING CHICKEN POX Ramesh M 1, Kavya Raju Nayak 2, M.G. Gopal 3, Sharath Kumar B.C 4, Nandini A.S 5 HOW TO CITE THIS ARTICLE: Ramesh M, Kavya
-> Education -> Excellence
 Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Herbal and homeopathic products, often considered natural and non-toxic, can also cause adverse drug reactions.
 Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Melanoma Immunotherapy. Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management
 Melanoma Immunotherapy Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management Mike Buljan, NP UCSF Medical Center Melanoma Oncology Disclosures None Only FDA-approved
Melanoma Immunotherapy Nursing Perspective on Immune-Related Adverse Events: Patient education, Monitoring & Management Mike Buljan, NP UCSF Medical Center Melanoma Oncology Disclosures None Only FDA-approved
Drug allergy and Skin Disorders. Timothy Craig, DO, FACOI Professor of Medicine and Pediatrics Distinguished Educator Penn State University, Hershey
 Drug allergy and Skin Disorders Timothy Craig, DO, FACOI Professor of Medicine and Pediatrics Distinguished Educator Penn State University, Hershey The best screening test for anaphylaxis is? A. histamine
Drug allergy and Skin Disorders Timothy Craig, DO, FACOI Professor of Medicine and Pediatrics Distinguished Educator Penn State University, Hershey The best screening test for anaphylaxis is? A. histamine
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
Skin Manifestations of Systemic Disease. Approach to Dermatalogic Diagnosis 9/6/2016. Go Ahead---Judge a Book by its Cover!
 Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
Go Ahead---Judge a Book by its Cover! Skin Manifestations of Systemic Disease Amelie Hollier, DNP, FNP-BC, FAANP Lafayette, LA President, APEA Objectives Compare diseases of the skin with reactions of
Bacterial Infections in Pediatric Dermatology. Patrick McMahon, MD Children s Hospital of Philadelphia
 Bacterial Infections in Pediatric Dermatology Patrick McMahon, MD Children s Hospital of Philadelphia Fill In The Blank When you see on the skin, you think of a bacterial skin infection SEND SWABS VIRAL
Bacterial Infections in Pediatric Dermatology Patrick McMahon, MD Children s Hospital of Philadelphia Fill In The Blank When you see on the skin, you think of a bacterial skin infection SEND SWABS VIRAL
DERMATOLOGIC EMERGENCIES. Mary Evers D.O., F.A.O.C.D. Georgetown, Texas
 DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
DERMATOLOGIC EMERGENCIES Mary Evers D.O., F.A.O.C.D. Georgetown, Texas SKIN EMERGENCIES??? Subclassifications: Autoimmune (Anaphylaxis, Vasculitis, Pemphigus) Erythroderma (AGEP, DRESS, SJS, TEN) Infectious
10/25/2018. Autoimmunity and how to treat it. Disclosure. Why do we get autoimmunity? James Verbsky MD/PhD Pediatric Rheumatology/Immunology
 Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
GOOD MORNING! AUGUST 5, 2014
 GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
GOOD MORNING! AUGUST 5, 2014 PREP QUESTION During the health supervision visit of a term newborn boy, his mother relates that a cousins child died at age 4 months from sudden infant death syndrome. She
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW
 SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
Objectives. Terminology. Recognize common pediatric dermatologic conditions. Review treatment plans Identify skin manifestations of systemic disease
 Pediatric Visual Dermatological Diagnosis Fernando Vega, M.D. Objectives Recognize common pediatric dermatologic conditions Expand differential diagnosis Review treatment plans Identify skin manifestations
Pediatric Visual Dermatological Diagnosis Fernando Vega, M.D. Objectives Recognize common pediatric dermatologic conditions Expand differential diagnosis Review treatment plans Identify skin manifestations
Concentrate on Descriptors. An Approach to Skin Diseases in the ER
 Concentrate on Descriptors An Approach to Skin Diseases in the ER Toby Maurer, MD University of California, San Francisco Vasculitis-leaky blood vessels Targetoid lesions-round lesions with blue or red
Concentrate on Descriptors An Approach to Skin Diseases in the ER Toby Maurer, MD University of California, San Francisco Vasculitis-leaky blood vessels Targetoid lesions-round lesions with blue or red
Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 17 ISSN 2379-1039 Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis * Amier Ahmad, Md ; Kevin
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 17 ISSN 2379-1039 Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis * Amier Ahmad, Md ; Kevin
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
The skin is the largest organ of the human body. Functions: protection sensation maintain temperature vitamin synthesis
 Dermatology The skin is the largest organ of the human body. Functions: protection sensation maintain temperature vitamin synthesis The image to the left shows an image of skin cells and the proteins which
Dermatology The skin is the largest organ of the human body. Functions: protection sensation maintain temperature vitamin synthesis The image to the left shows an image of skin cells and the proteins which
Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center
 Dermatologic Emergencies Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center Clinical Features of SJS/TEN Initial symptoms Fever, stinging
Dermatologic Emergencies Mark A. Bechtel, MD Clinical Associate Professor Division Director, Dermatology Ohio State University Medical Center Clinical Features of SJS/TEN Initial symptoms Fever, stinging
CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD
 CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD DERMATOLOGY Pathogenesis Immunologic: can involve Type I, II, III, IV hypersensitivity reactions.
CUTANEOUS DRUG REACTIONS OR I WOULDN T HAVE SEEN IT, IF I HADN T BELIEVED IT Edmund J. Rosser Jr., DVM, DACVD DERMATOLOGY Pathogenesis Immunologic: can involve Type I, II, III, IV hypersensitivity reactions.
ExtraintestinalManifestations of IBD
 ExtraintestinalManifestations of IBD Hyun Kim, M.D. San Diego Digestive Disease Consultants Associate Professor, UCSD School of Medicine Why Other Organs Involved in IBD? Organ Involvement Bones, Joints
ExtraintestinalManifestations of IBD Hyun Kim, M.D. San Diego Digestive Disease Consultants Associate Professor, UCSD School of Medicine Why Other Organs Involved in IBD? Organ Involvement Bones, Joints
Cutanous Manifestation of Lupus Erythematosus. Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university
 Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
Cutanous Manifestation of Lupus Erythematosus Presented By: Dr. Naif S. Al Shahrani Salman Bin Abdaziz university A 50-year old lady, who is otherwise healthy, presented to the dermatology clinic with
DERMATOLOGY FOR THE INTERNIST. Emilie Chow, MD 8/2017
 DERMATOLOGY FOR THE INTERNIST Emilie Chow, MD 8/2017 GOALS ALL SLIDES ARE FOCUSED ON CLINICAL CASES IN THE FORM OF QUESTIONS AND MKSAP COVERED TOPICS USING POLLEV.COM Reference for material is MKSAP 17
DERMATOLOGY FOR THE INTERNIST Emilie Chow, MD 8/2017 GOALS ALL SLIDES ARE FOCUSED ON CLINICAL CASES IN THE FORM OF QUESTIONS AND MKSAP COVERED TOPICS USING POLLEV.COM Reference for material is MKSAP 17
PHLEBOLOGY AND DERMATOLOGY COMPETITIVE OR COMPLEMENTARY?
 PHLEBOLOGY AND DERMATOLOGY COMPETITIVE OR COMPLEMENTARY? Dr Inga Vanhandenhove AZ Monica - Antwerp Disclosure Speaker name:... X Inga Vanhandenhove I have the following potential conflicts of interest
PHLEBOLOGY AND DERMATOLOGY COMPETITIVE OR COMPLEMENTARY? Dr Inga Vanhandenhove AZ Monica - Antwerp Disclosure Speaker name:... X Inga Vanhandenhove I have the following potential conflicts of interest
Cutaneous Adverse Drug Reactions in Domestic Animals. Katherine Doerr, DVM, Dip. ACVD. Veterinary Dermatology Center
 Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
Cutaneous Adverse Drug Reactions in Domestic Animals Katherine Doerr, DVM, Dip. ACVD Veterinary Dermatology Center Maitland, Rockledge, Waterford Lakes, FL Not highly studied in veterinary medicine Unknown
A. Erythema multiforme and related diseases
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Erythema, Erythroderma (Exfoliative Dermatitis) Erythema is caused by telangiectasia or hyperemia in the papillary and reticular
Skin lesions & Abrasions
 Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
Skin lesions & Abrasions What Are Skin Lesions? A skin lesion is a part of the skin that has an abnormal growth or appearance compared to the skin around it Types of Skin Lesions Two types of skin lesions
COMMON SKIN INFECTIONS. Sports Medicine
 COMMON SKIN INFECTIONS Sports Medicine IMPETIGO IS A SUPERFICIAL BACTERIAL INFECTION CAUSED BY: STREPTOCOCCI OR STAPHYLOCOCCUS AUREUS BOULOUS IMPETIGO IMPETIGO COMES IN TWO FORMS: BOULOUS OR NON- BOULOUS
COMMON SKIN INFECTIONS Sports Medicine IMPETIGO IS A SUPERFICIAL BACTERIAL INFECTION CAUSED BY: STREPTOCOCCI OR STAPHYLOCOCCUS AUREUS BOULOUS IMPETIGO IMPETIGO COMES IN TWO FORMS: BOULOUS OR NON- BOULOUS
Dermatology Pearls for Inpatient Medicine. Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University
 Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
Dermatology Pearls for Inpatient Medicine Dr Peter J Green MD FRCPC Professor, Division of Dermatology Dalhousie University Objectives 1. Review spectrum of cutaneous manifestations seen with inpatient
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123
 BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
Bacterial Infections. Ron Rapini MD Chernosky Chair Dept Dermatology Professor of Pathology Univ of Texas and MD Anderson Cancer Cntr Houston, Texas
 Bacterial Infections Ron Rapini MD Chernosky Chair Dept Dermatology Professor of Pathology Univ of Texas and MD Anderson Cancer Cntr Houston, Texas Conflict of interest statement: Book royalties- Elsevier
Bacterial Infections Ron Rapini MD Chernosky Chair Dept Dermatology Professor of Pathology Univ of Texas and MD Anderson Cancer Cntr Houston, Texas Conflict of interest statement: Book royalties- Elsevier
Hammer Toe. Photo Diagnosis. Case 1. Illustrated quizzes on problems seen in everyday practice. Questions. Answers
 Illustrated quizzes on problems seen in everyday practice Hammer Toe Case 1 This 48-year-old gentleman has a long history of Rheumatoid arthritis, for which he has been on Methotrexate 10 mg weekly for
Illustrated quizzes on problems seen in everyday practice Hammer Toe Case 1 This 48-year-old gentleman has a long history of Rheumatoid arthritis, for which he has been on Methotrexate 10 mg weekly for
Antibiotic Stewardship for Skin and Soft Tissue Infection and Respiratory Tract Infections
 Antibiotic Stewardship for Skin and Soft Tissue Infection and Respiratory Tract Infections Ghinwa Dumyati, MD Professor of Medicine Center for Community Health and Infectious Diseases Division University
Antibiotic Stewardship for Skin and Soft Tissue Infection and Respiratory Tract Infections Ghinwa Dumyati, MD Professor of Medicine Center for Community Health and Infectious Diseases Division University
Dermergency! An Approach to Identification and Management of Life-Threatening Rashes
 Dermergency! An Approach to Identification and Management of Life-Threatening Rashes Gabby Anderson, PharmD PGY2 Emergency Medicine Pharmacy Resident anderson.gabrielle@mayo.edu Pharmacy Grand Rounds January
Dermergency! An Approach to Identification and Management of Life-Threatening Rashes Gabby Anderson, PharmD PGY2 Emergency Medicine Pharmacy Resident anderson.gabrielle@mayo.edu Pharmacy Grand Rounds January
الركودي الجلد التهاب= Stasis dermatitis
 1 / 10 Stasis dermatitis Stasis dermatitis is a common inflammatory skin disease that occurs on the lower extremities in patients with chronic venous insufficiency with venous hypertension. Stasis dermatitis
1 / 10 Stasis dermatitis Stasis dermatitis is a common inflammatory skin disease that occurs on the lower extremities in patients with chronic venous insufficiency with venous hypertension. Stasis dermatitis
DERMATOLOGICAL EMERGENCIES. DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE
 DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
DERMATOLOGICAL EMERGENCIES DR. Ian Hoyle MBBS DIP IMC RCS (Ed), DA (UK),FRACGP,FACRRM,DIP DERM(Wales) TASMANIAN SKIN AND BODY CENTRE Dermatological Emergencies INFECTIONS ERYTHRODERMA DRUG ERUPTIONS STEVENS-JOHNSON
Right type of lesions for topicals. Onychomycosis. Common Diseases and Infections of the SKIN. Toby Maurer, MD University of California, San Francisco
 Common Diseases and Infections of the SKIN Toby Maurer, MD University of California, San Francisco Onychomycosis Topical treatment use for the right type of lesions Naftin gel for small superficial lesions
Common Diseases and Infections of the SKIN Toby Maurer, MD University of California, San Francisco Onychomycosis Topical treatment use for the right type of lesions Naftin gel for small superficial lesions
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Drug Allergy: A Rash ionale for Treatment
 Drug Allergy: A Rash ionale for Treatment Heather A. Powell, PharmD, BCPS Assistant Professor of Clinical Sciences Roosevelt University College of Pharmacy Jordan O. Powell, PharmD Clinical Pharmacist
Drug Allergy: A Rash ionale for Treatment Heather A. Powell, PharmD, BCPS Assistant Professor of Clinical Sciences Roosevelt University College of Pharmacy Jordan O. Powell, PharmD Clinical Pharmacist
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
=ﻰﻤاﻤﺤﻠا ﺔﻴﻘﻠﺤﻠا ﺔذﺒاﻨﻠا
 1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
1 / 15 Erythema Annulare Centrifugum and Other Figurate Erythemas The figurate erythemas include a variety of eruptions characterized by annular and polycyclic lesions. Classification of this group has
D.R.E.S.S. Syndrome An update. David H. Peng MD MPH Department of Dermatology Keck School of Medicine of USC
 D.R.E.S.S. Syndrome An update David H. Peng MD MPH Department of Dermatology Keck School of Medicine of USC I have no disclosures I will be discussing off label uses for medications Maculopapular Morbilliform
D.R.E.S.S. Syndrome An update David H. Peng MD MPH Department of Dermatology Keck School of Medicine of USC I have no disclosures I will be discussing off label uses for medications Maculopapular Morbilliform
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Disclaimer. This is a broad survey and cannot cover all differential diagnoses or each condition in thorough detail
 Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
THE TIP OF THE ICEBERG SAMER BOLIS, DO PGY-3 LEHIGH VALLEY HEALTH NETWORK, ALLENTOWN PA
 THE TIP OF THE ICEBERG SAMER BOLIS, DO PGY-3 LEHIGH VALLEY HEALTH NETWORK, ALLENTOWN PA Case The patient is a 48 year-old female, who recently returned from a trip to Puerto Rico. She presents to the ED
THE TIP OF THE ICEBERG SAMER BOLIS, DO PGY-3 LEHIGH VALLEY HEALTH NETWORK, ALLENTOWN PA Case The patient is a 48 year-old female, who recently returned from a trip to Puerto Rico. She presents to the ED
CPC. Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand
 CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
CPC Chutika Srisuttiyakorn, M.D. Kobkul Aunhachoke, M.D. Phramongkutklao Hospital Bangkok, Thailand A 53 year-old woman with fever, facial swelling and rashes on face, trunk and upper extremities for 3
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Eczema. By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University
 Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Venous Insufficiency Ulcers. Patient Assessment: Superficial varicosities. Evidence of healed ulcers. Dermatitis. Normal ABI.
 Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
Venous Insufficiency Ulcers Patient Assessment: Superficial varicosities Evidence of healed ulcers Dermatitis Normal ABI Edema Eczematous skin changes 1. Scaling 2. Pruritus 3. Erythema 4. Vesicles Lipodermatosclerosis
What's New in Oncodermatopathology: Immunotherapy Reactions
 What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature
 Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature Sarah M. Persing, MPH, a and Donald Laub Jr, MD, FACS a,b a University of Vermont College of Medicine, Burlington;
Superficial Granulomatous Pyoderma of the Face: A Case Report and Review of the Literature Sarah M. Persing, MPH, a and Donald Laub Jr, MD, FACS a,b a University of Vermont College of Medicine, Burlington;
Annual Rheumatology & Therapeutics Review for Organizations & Societies
 Annual Rheumatology & Therapeutics Review for Organizations & Societies Update on Granulomatosis with Polyangiitis (Wegener s) Philip Seo, MD, MHS Director, Johns Hopkins Vasculitis Center Director, Johns
Annual Rheumatology & Therapeutics Review for Organizations & Societies Update on Granulomatosis with Polyangiitis (Wegener s) Philip Seo, MD, MHS Director, Johns Hopkins Vasculitis Center Director, Johns
Personalized Medical Care:Recognition, Management, and Maybe Prevention of Cutaneous Hypersensitivity Reactions
 Personalized Medical Care:Recognition, Management, and Maybe Prevention of Cutaneous Hypersensitivity Reactions Bernard A. Cohen, M.D. Johns Hopkins Children s Center Baltimore, Maryland (NO disclosures)
Personalized Medical Care:Recognition, Management, and Maybe Prevention of Cutaneous Hypersensitivity Reactions Bernard A. Cohen, M.D. Johns Hopkins Children s Center Baltimore, Maryland (NO disclosures)
Case 1. Background. Presenting Symptoms. Schecter Case1 Differential Diagnosis of TB 1
 TB or Not TB? Case 1 Gisela Schecter, M.D., M.P.H. California Department of Public Health Background 26 year old African American male Born and raised in Bay Area of California Convicted of cocaine trafficking
TB or Not TB? Case 1 Gisela Schecter, M.D., M.P.H. California Department of Public Health Background 26 year old African American male Born and raised in Bay Area of California Convicted of cocaine trafficking
Rayos Prior Authorization Program Summary
 Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Midwifery Management Process for Common Health Problems
 StudentL 1 Lower Limb Cellulitis University of Washington School of Nursing Nurse- Midwifery Education Program NCLIN 512 Fall 2012 Midwifery Management Process for Common Health Problems 1. Common Health
StudentL 1 Lower Limb Cellulitis University of Washington School of Nursing Nurse- Midwifery Education Program NCLIN 512 Fall 2012 Midwifery Management Process for Common Health Problems 1. Common Health
Cellulitis and Soft Tissue Infections. Sally Williams MD
 Cellulitis and Soft Tissue Infections Sally Williams MD Cellulitis: A very common infection 25 cases per 1000 patient years More common in men, obese patients 60% occurs in the lower extremities 74% handled
Cellulitis and Soft Tissue Infections Sally Williams MD Cellulitis: A very common infection 25 cases per 1000 patient years More common in men, obese patients 60% occurs in the lower extremities 74% handled
Management of Pyoderma Gangrenosum Mentoring in IBD XVII
 Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
The World of Dermatology
 The World of Dermatology, F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates, LTD Objectives Cite the advances in management
The World of Dermatology, F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates, LTD Objectives Cite the advances in management
Granulomatosis and Polyangiitis Presenting as Superficial Granulomatous Pyoderma
 Case Report Granulomatosis and Polyangiitis Presenting as Superficial Granulomatous Pyoderma Sophia Zhang 1*, Ellen Roh 2, Timothy Patton 3 1 University of Pittsburgh School of Medicine, 3550 Terrace St,
Case Report Granulomatosis and Polyangiitis Presenting as Superficial Granulomatous Pyoderma Sophia Zhang 1*, Ellen Roh 2, Timothy Patton 3 1 University of Pittsburgh School of Medicine, 3550 Terrace St,
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level
 Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Diagnosis and Management of Common and Infective Skin Diseases in Children at primary care level Dr Ng Su Yuen Paediatrician and Paediatric Dermatologist Hospital Pulau Pinang Outline Common inflammatory
Contents. Part I Genodermatoses
 Contents Part I Genodermatoses 1 Hyperkeratotic Palms and Soles with Periorificial Keratosis............... 3 2 Indurated, Dark, Hairy Plaques, with Arthritis and Deafness.............. 9 3 Cleft Palate,
Contents Part I Genodermatoses 1 Hyperkeratotic Palms and Soles with Periorificial Keratosis............... 3 2 Indurated, Dark, Hairy Plaques, with Arthritis and Deafness.............. 9 3 Cleft Palate,
Significance. Outline and Objectives. S007 Systemic Therapies for Medical Oncology
 S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Rashes Not To Be Missed In Children
 May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
May 2016 Rashes Not To Be Missed In Children Dr Chan Yuin Chew Dermatologist Dermatology Associates Gleneagles Medical Centre Scope of presentation Focus on rashes May lead to significant morbidity if
Commonly Coded Conditions in Dermatology
 Commonly Coded Conditions in Dermatology No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or mechanically, including photocopying,
Commonly Coded Conditions in Dermatology No part of this presentation may be reproduced or transmitted in any form or by any means (graphically, electronically, or mechanically, including photocopying,
Wound Assessment Report
 Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Wound Assessment Report Single Assessment, Single Wound Mary Taylor Assessment Patient ID MT4367147 Date of Birth 1939-4-18 Left Foot, Sole: Wound A Image taken 16-45-43 Area 1.7cm2 Perimeter 48mm Maximum
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
PRIMARY CUTANEOUS NEUTROPHILIC DISORDERS
 PRIMARY CUTANEOUS NEUTROPHILIC DISORDERS Victoria J. Hogarth, 1 *Bláithín Moriarty 2 1. Department of Dermatology, King s College Hospital NHS Foundation Trust, London, UK 2. St John s Institute of Dermatology,
PRIMARY CUTANEOUS NEUTROPHILIC DISORDERS Victoria J. Hogarth, 1 *Bláithín Moriarty 2 1. Department of Dermatology, King s College Hospital NHS Foundation Trust, London, UK 2. St John s Institute of Dermatology,
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
MEK/BRAF inhibitors and the implications on patients and health care providers
 MEK/BRAF inhibitors and the implications on patients and health care providers Tara McKeown NP Paediatric Neuro Oncology Hospital for Sick Children Adjunct Lecturer, Lawrence S. Bloomberg, Faculty of Nursing,
MEK/BRAF inhibitors and the implications on patients and health care providers Tara McKeown NP Paediatric Neuro Oncology Hospital for Sick Children Adjunct Lecturer, Lawrence S. Bloomberg, Faculty of Nursing,
Jess Dreicer, MD Internal Medicine, PGY-3
 Jess Dreicer, MD Internal Medicine, PGY-3 Problem List Myelodysplastic syndrome Problem List Myelodysplastic syndrome Giant cell arteritis Treatments Prednisone 60 mg -6 weeks Problem List Myelodysplastic
Jess Dreicer, MD Internal Medicine, PGY-3 Problem List Myelodysplastic syndrome Problem List Myelodysplastic syndrome Giant cell arteritis Treatments Prednisone 60 mg -6 weeks Problem List Myelodysplastic
Jeopardy. What s the rash? $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400
 Jeopardy Antibodies & more antibodies Aching joints What s the rash? Potpourri Image Challenge $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400 $500 $500
Jeopardy Antibodies & more antibodies Aching joints What s the rash? Potpourri Image Challenge $100 $100 $100 $100 $100 $200 $200 $200 $200 $200 $300 $300 $300 $300 $300 $400 $400 $400 $400 $400 $500 $500
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Common Cutaneous Signs of Medical Illnesses
 Common Cutaneous Signs of Medical Illnesses DR COLIN THENG MBBS, MMED (FAM. MED), MRCP(UK), FAMS SENIOR CONSULTANT DERMATOLOGIST THE SKIN SPECIALISTS & LASER CLINIC MOUNT ALVERNIA MEDICAL CENTRE D, #07-61
Common Cutaneous Signs of Medical Illnesses DR COLIN THENG MBBS, MMED (FAM. MED), MRCP(UK), FAMS SENIOR CONSULTANT DERMATOLOGIST THE SKIN SPECIALISTS & LASER CLINIC MOUNT ALVERNIA MEDICAL CENTRE D, #07-61
HIV-Dermatology Concepts in 2011
 HIV-Dermatology Concepts in 2011 Toby Maurer, MD Dept of Dermatology University of California, San Francisco Skin disease that is catalyst for HIV testing and indication for starting EARLY antiretrovirals
HIV-Dermatology Concepts in 2011 Toby Maurer, MD Dept of Dermatology University of California, San Francisco Skin disease that is catalyst for HIV testing and indication for starting EARLY antiretrovirals
When is Limb Edema Not Heart Failure
 When is Limb Edema Not Heart Failure An Approach to the Swollen Leg Greg Harding M.D. Vascular Surgeon Faculty/Presenter Disclosure Faculty: Greg Harding M.D. Relationships with commercial interests: None
When is Limb Edema Not Heart Failure An Approach to the Swollen Leg Greg Harding M.D. Vascular Surgeon Faculty/Presenter Disclosure Faculty: Greg Harding M.D. Relationships with commercial interests: None
2019 update on pyoderma gangrenosum
 2019 update on pyoderma gangrenosum Kanade Shinkai, MD PhD University of California, San Francisco F106: Updates in neutrophilic and pustular dermatoses I have no conflicts of interest to disclose. I will
2019 update on pyoderma gangrenosum Kanade Shinkai, MD PhD University of California, San Francisco F106: Updates in neutrophilic and pustular dermatoses I have no conflicts of interest to disclose. I will
Distinguishing cellulitis from its mimics
 REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will distinguish cellulitis from its mimics Emily C. Keller, MD Department of Dermatology, Cleveland Clinic Kenneth J. Tomecki, MD Vice Chairman, Department
REVIEW CME CREDIT EDUCATIONAL OBJECTIVE: Readers will distinguish cellulitis from its mimics Emily C. Keller, MD Department of Dermatology, Cleveland Clinic Kenneth J. Tomecki, MD Vice Chairman, Department
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
