Neovascular glaucoma after central retinal vein occlusion in pre-existing glaucoma
|
|
|
- Caitlin Patterson
- 5 years ago
- Views:
Transcription
1 Chen et al. BMC Ophthalmology 2014, 14:119 RESEARCH ARTICLE Open Access Neovascular glaucoma after central retinal vein occlusion in pre-existing glaucoma Hsi-Fu Chen 1, Min-Chi Chen 3,4, Chi-Chun Lai 2,4, Ling Yeung 1,4, Nan-Kai Wang 2,4, Henry Shen-Lih Chen 2,4, Wan-Chen Ku 1, Shiu-Chen Wu 2,4, Shirley H L Chang 2,4 and Lan-Hsin Chuang 1,4* Abstract Background: To determine the outcome of central retinal vein occlusion (CRVO) in pre-existing glaucoma and the predisposing factors of developing neovascular glaucoma (NVG). Methods: We retrospectively assessed a pre-existing glaucoma CRVO group and a non-glaucoma CRVO group to elucidate the demographics, clinical course and ocular parameters of these two cohorts. Among the pre-existing glaucoma cases, the predisposing factors for the development of NVG were monitored, including the retinal capillary non-perfusion status, intraocular pressure (IOP) and best-corrected visual acuity (BCVA) at presentation. Results: Of 642 CRVO patients reviewed in this 10-year cohort study, 60 (9.3%) had pre-existing glaucoma at a mean follow-up of 30.8 months, including 28 (4.4%) primary open angle glaucoma (POAG), 27 (4.2%) primary angle closure glaucoma (PACG), and 5 (0.8%) normal tension glaucoma (NTG) cases. Although the presence of glaucoma in the CRVO eyes was not significantly associated with the risk of developing NVG, the incidence of developing NVG in pre-existing glaucoma eyes was significantly higher in the group with IOP greater than 20 mmhg at CRVO presentation (P =0.02, Chi-square test) as well as in the ischemic CRVO group compared to the non-ischemic patients (P = 0.005, Fisher s exact test). Overall, 20% of pre-existing glaucoma patients needed glaucoma surgery after a CRVO event, including 11.7% of patients who developed iris neovascularisation (INV) and 8.3% of patients who developed a high IOP without INV. Conclusions: Both the retinal non-perfusion status and uncontrolled IOP contribute to NVG in patients with pre-existing glaucoma after CRVO. Following CRVO, glaucoma surgery is necessary for pre-existing glaucoma cases with intractable elevated IOP with or without INV. Keywords: Neovascular glaucoma, Central retinal vein occlusion with pre-existing glaucoma, Retinal non-perfusion status, Intraocular pressure, Predisposing factors Background Central retinal vein occlusion (CRVO) is a common retinal vascular disease that leads to visual impairment in elderly patients. Previous studies from Western countries have a high incidence of pre-existing primary open angle glaucoma (POAG) in patients with CRVO [1-3]. However, Asian populations differ from Western populations in that the incidence of primary angle closure glaucoma (PACG) is much higher. The incidence of different types of pre-existing glaucoma, intraocular * Correspondence: c571019@cgmh.org.tw 1 Department of Ophthalmology, Chang Gung Memorial Hospital, 222 Mai-Chin Rd, Keelung 204, Taiwan 4 Chang Gung University College of Medicine, Taoyuan, Taiwan Full list of author information is available at the end of the article pressure (IOP) changes and optic neuropathy in CRVO in the Asian population is still unclear. One-third of non-ischemic CRVO may convert to ischemic CRVO [4]. The major complication of ischemic CRVO is neovascular glaucoma (NVG) [4,5]. In CRVO patients with pre-existing glaucoma who have developed NVG, severe corneal oedema and recalcitrant high IOP are typically difficult to manage. Therefore, damage to the optic nerve is difficult to avoid, and any residual vision may be threatened. Thus far, it is still unknown whether pre-existing glaucoma plays a role in the development of NVG in CRVO patients. Regardless of treatment with intravitreal injection of 2014 Chen et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Chen et al. BMC Ophthalmology 2014, 14:119 Page 2 of 6 anti-vascular endothelial growth factor (VEGF) or corticosteroids, conventional panretinal photocoagulation (PRP) can regress retina neovascularisation in CRVO [6]. Because there is a paucity of evidence on this condition, the aim of this cohort study was to determine the profile of pre-existing glaucoma in CRVO in the East Asian population. Additionally, the secondary aims were to explore the predisposing factors and outcomes for the development of NVG in CRVO patients with pre-existing glaucoma. Methods This was a retrospective and comparative long-term cohort study. Patients were enrolled from Jul 1999 to Dec This study was performed in accordance with the Helsinki Declaration of 1975 (1983 revision) and was approved by the Institutional Review Board of the Chang Gung Memorial Hospital, Linkuo, Taiwan. All patients diagnosed with CRVO were identified and followed up monthly within one year, and their clinical data were recorded during a chart review. Demographic characteristics, including gender, age, systemic diseases, the onset of CRVO and preceding eye history, were collected. The general ocular examination, including the best-corrected visual acuity (BVCA), slit-lamp biomicroscope examination, IOP at the first diagnosis of CRVO, indirect ophthalmoscopy, fluorescein angiography findings, or related surgery history, was documented in detail. In this 10-year CRVO cohort study, the study group was consisted of pre-existing glaucoma cases diagnosed with increased IOP, an optic cup/disc ratio larger than 0.5, and glaucomatous visual field changes. NVG was defined as neovascularisation of the iris with an IOP increase 21 mmhg. Optic nerve damage progression was defined as an increasing cup/disc ratio. The type of primary glaucoma, gonioscopy findings, optic cup/disc ratio and visual field data were also recorded. Newly diagnosed participants with CRVO were classified as the control group. We excluded patients who received intravitreous injection of anti-vegf medications or triamcinolone acetonide during the follow-up period. As a proceeding analysis, patients who underwent vitrectomy to clear vitreous haemorrhages, patients who presented with distinct iris neovascularisation or neovascular glaucoma during the first visit or patients with significant diabetic retinopathy observed at short-term follow up (shorter than six months) were also precluded from this study. During the follow-up period, details regarding the procedures were also recorded for patients who underwent panretinal photocoagulation (PRP) or filtration surgery after CRVO. Data were entered into Excel and were analysed using SPSS software (Statistical Package for Social Sciences). The differences between the non-glaucoma and preexisting glaucoma groups were evaluated using a chisquare test and a 2-sample t-test for categorical and continuous variables, respectively. For the patients with pre-existing glaucoma, the relationships between the development of NVG and ocular parameters were examined using the Fisher s exact test or Wilcoxon rank sum test. Furthermore, the visual and optic nerve changes between the initial and final stages were assessed using the Wilcoxon signed-rank test. In this study, the Snellen visual acuity was converted to the logarithm of the minimum angle of resolution (logmar) units for analysis. A p value of less than 0.05 was considered significant. Results Overall, 642 patients with CRVO were reviewed in this 10-year cohort study. There were 60 eyes from 60 patients who had a history of pre-existing glaucoma before the onset of CRVO. The incidence of pre-existing glaucoma in CRVO was 60/642 (9.3%). Regarding the various types of pre-existing glaucomas, there were 28 primary open angle glaucoma (POAG) cases, 27 primary angle closure glaucoma (PACG) cases and 5 normal tension glaucoma (NTG) cases in this study. A total of 321 patients were excluded from this study due to vitrectomy surgery or intravitreal injections of triamcinolone acetonide or anti-vegf. To compare the characteristics, 60 pre-existing glaucoma cases were categorised as the study group, and 261 non-glaucoma cases were categorised as the control group. The demographics, clinical characteristics and baseline ocular parameters are listed in Table 1. In the preexisting glaucoma group, the age of CRVO onset was significantly older than the control group (57.3 vs years, p<0.001). The prevalence of males was much higher than that of females in both groups. When comparing the ocular parameters, the cup/disc (C/D) ratio was substantially larger in the study group compared to the control group. According to the FAG finding, the proportion of ischemic type CRVO was higher in the pre-existing glaucoma group than in the control group (39.8% VS 45%), although not significantly (p=0.46). Moreover, during CRVO diagnosis, approximately one half (48.3%) of the pre-existing glaucoma participants exhibited a higher increase in the IOP compared to the control group (21.7±9.2 vs. 13.9±4.8 mmhg, p<0.001). However, the vision (BVCA) of both groups at the time of diagnosis was similar. There was no significant difference in the proportion of ischemic type CRVO between the two groups (Table 1). In general, 20.3% (53/261) of the non-pre-existing glaucoma cases and 31.7% (19/60) of the pre-existing glaucoma cases developed NVG. (p=0.06) Furthermore, the incidence of NVG occurred
3 Chen et al. BMC Ophthalmology 2014, 14:119 Page 3 of 6 Table 1 Demographic and ocular characteristics of pre-existing glaucoma in central retinal vein occlusion (CRVO) Non-glaucoma Pre-existing glaucoma p value Case number Gender (female:male) 102: : Age (mean±sd) 57.3± ±14.9 <0.001 Systemic disease DM 71 (27.2%) 14 (23.3%) HTN 131 (50.2%) 29 (48.3%) CRVO onset (months) (mean±sd) 1.6± ± Perfusion status Non-ischemic 157 (60.2%) 33 (55%) Ischemic 104 (39.8%) 27 (45% ) C/D ratio (mean±sd) 0.42± ±0.16 <0.001 IOP at presentation (mmhg) (mean±sd) 13.9± ±9.2 <0.001 BCVA (logmar) (mean±sd) 1.46± ± PRP during follow up 107 (41%) 22 (36.7%) NVG during follow up 53 (20.3%) 19(31.7%) Abbreviations: BCVA best-corrected visual acuity, C/D cup-to-disc, DM diabetes mellitus, HTN hypertension, IOP intraocular pressure, log MAR logarithm of the minimal angle of resolution, and SD standard deviation. p values were calculated using the chi-square test and 2-sample t-test for categorical and continuous variables, respectively. within 6 months for ischemic CRVO was100% (19/19) of cases in the pre-existing glaucoma group and 81.18% (43/53) of cases in the control group (p= 0.05). It is well known that the major complication after the onset of CRVO is the development of NVG, and IOP is typically intractable to medical treatment. To further identify the predisposing factors among the ocular parameters that contribute to the development of NVG in the study group, at the first visit, the IOP, C/D, and retinal nonperfusion status were obtained (Table 2). In the univariate analysis of the development of NVG, there was a significant difference in the mean IOP at the time of presentation between NVG within 0.5 yr and non- NVG within 0.5 yr (29.2±10.1 vs. 19.8±8.29, P=0.007, Wilcoxon rank sum test). Additionally, when the IOP was dichotomised as >20 or 20 mmhg, 10 out of 32 (31.3%) patients with IOP >20 mmhg and 2 out of 28 (7.1%) with IOP 20 mmhg developed NVG within 0.5 yr, respectively (Chi-square test, P=0.020). Considering another fundamental parameter in the pre-existing glaucoma group that is associated with NVG development, a majority (93.3%) of the patients had moderate to severe cupping upon the diagnosis of CRVO. The average C/D upon the presentation of CRVO was 0.72 in the study group. A high incidence of a large C/D ratio was found as 38.3% of the patients in the study group had moderate cupping (0.5 C/D<0.8) and 55% had severe cupping ( 0.8). For pre-existing glaucoma patients, there was a marginal significant difference in the C/D ratio between NVG within 0.5 yr and non-nvg within 0.5 yr [0.78±0.17, (range: ) vs. 0.70±0.16, median 0.75 (range: ) using the Wilcoxon rank sum test (P=0.053)]. During the study period of 30.8 months, C/D increased to subtotal cupping in 37 out of 60 (61.7%) cases, indicating that the RNFL continued to thin, which is a serious consequence after retinal haemorrhage is Table 2 NVG within 0.5 yr after CRVO in pre-existing glaucoma NVG within 0.5 yr Non-NVG within 0.5yr p value C/D ratio at presentation (mean±sd) 0.78± ± Retinal perfusion status 0.005* Non-ischemic 5 28 Ischemic Mean IOP at presentation (mmhg) (mean±sd) 29.2± ± ** IOP > 20 mmhg at presentation IOP 20 mmhg at presentation *** *Fisher s exact test; **Wilcoxon rank sum test; and ***Chi-square test.
4 Chen et al. BMC Ophthalmology 2014, 14:119 Page 4 of 6 resolved. Furthermore, the incidence of developing NVG was significantly higher in the pre-existing glaucoma and control group patients with ischemic type CRVO compared to non-ischemic type CRVO.(p=0.005 and p<0.001, Fisher s exact test). Accordingly, panretinal photocoagulation (PRP) was suggested in cases where neovascularisation of the iris occurred at follow-up. Nevertheless, there were 2 PACG cases with an initially normal IOP, which spiked after PRP was performed, and IOP stabilised with additional medication. Seventy-five percent of pre-existing glaucoma patients were regularly using anti-glaucoma agents before the first CRVO event. Among 27 pre-existing PACG patients, 9 patients had received laser iridotomy. Surgical interventions for NVG patients, including filtration surgery and transscleral cyclophotocoagulation, are summarised in Table 3. For patients with end stage glaucoma and poor vision, the type of surgery performed (trabeculectomy with mitomycin C or transscleral cyclophotocoagulation) depended on the physician s preference and patients agreement. An intractable IOP increase without INV was treated with trabeculectomy with or without an antimetabolite agent if useful vision was still present. In this retrospective cohort study, 12 cases (20%) needed surgical intervention to control IOP during the long-term follow up. The two major causes of surgery were uncontrolled IOP in cases that developed NVG (11.7%) and intractable IOP without iris NV (8.3%). It is worth noting that there were some preexisting glaucoma cases that flared up with high IOP without INV, and medical intervention was not sufficient thereafter. Due to the retrospective nature of this study, the exact time point of conversion from the non-ischemic to ischemic type is difficult to detect. For example, a case of NTG with a BCVA of 0.6 with non-ischemic CRVO at presentation converted to ischemic CRVO that was subsequently complicated with NVG. This patient then hesitated PRP, and vision decreased to light sense negative. According to the records, 5 out of 33 non-ischemic cases in the pre-existing glaucoma group (15.1%) developed NVG, and ischemic development was noted as possible for future development during the study period. In general, vision did not significantly improve after conventional glaucoma management up to the 31-month follow-up. In patients with pre-existing glaucoma, vision deteriorated from an initial BCVA log MAR 1.69 (Snellen 0.02) to a final BCVA log MAR1.84 (Snellen 0.014). Because there are three types of pre-existing glaucoma, we analysed the visual outcome based on the mean BCVA and cup disc ratio change (Table 4). As indicated above and in Table 1, the C/D ratio for pre-existing glaucoma cases at CRVO presentation was larger than the control group (0.72 vs. 0.42). When the initial and final ratios were compared, the C/D ratio significantly increased in the overall, POAG, and PACG subgroups. This result demonstrates that the retinal nerve fibre layer defect continued to progress after CRVO, which may be associated with further deterioration of vision for these pre-existing glaucoma cases. Discussion Glaucoma is one of the known risk factors for CRVO [1,2,7,8]. A major complication of CRVO is the development of NVG, which can lead to severe visual impairment. Pre-existing glaucoma is seldom included in CRVO studies in Asian populations where the prevalence of PACG is higher than in the Western countries. Ethnicity may play an important role when evaluating ocular diseases related to glaucoma. In this 10-year cohort study, the incidence of preexisting glaucoma in CRVO was similar to previous studies [7,9]. Recently, Michaelides and Foster also suggested that angle-closure may be associated with retinal vein occlusions in retrospective case series with diverse ethnicity [10]. In contrast, Hayreh et al. concluded that compartment syndrome contradicts the concept of playing a role in RVO [11]. In this study, it is notable that the incidence of PACG was approximately equal to POAG in CRVO. Regarding demographic and ocular parameters, CRVO was more prevalent in the elderly and middle to late stage glaucoma cases with large cupping. Although we do not have exfoliative glaucoma cases in our study, Prata et al. manifested that retinal vascular occlusion in patients with exfoliation syndrome occurs most frequently in the affected or more severely Table 3 The management of various types of pre-existing glaucoma in central retinal vein occlusion (CRVO) POAG PACG NTG Overall incidence Case number Prior use of antiglaucomaagents 26 (92.9%) 16 (26.7%) 3 (60%) 75% Mean deviation (db) Trabe/TSCP for NVG 1/3 (14.3%) 1/2 (11.1%) % Trabe for elevated IOP (w/o INV) 2 (7.1%) 3 (11.1%) 0 8.3% Abbreviations: PACG primary angle closure glaucoma, POAG primary open angle glaucoma, PRP pan-retinal photocoagulation, Trabe trabeculectomy, TSCP transscleralcyclophotocoagulation, and w/o INV without iris neovascularisation.
5 Chen et al. BMC Ophthalmology 2014, 14:119 Page 5 of 6 Table 4 Visual and optic nerve changesin various pre-existing glaucoma types POAG PACG NTG Overall Case number IOP at presentation (mmhg) 24.3± ± ± ±9.2 Baseline BCVA (Snellen) Final BCVA (Snellen) Cup-to-disc ratio Initial (mean±sd) 0.69± ± ± ±0.16 Final (mean±sd) 0.75± ± ± ±0.15 p value Follow-up (months) (mean±sd) 30.1± ± ± ±29.1 Abbreviations: BCVA best-corrected visual acuity, NVG neovascular glaucoma, PACG primary angle closure glaucoma, POAG primary open angle glaucoma, and SD standard deviation. Changes betweenthe initial and final cup-to-disc ratio were examined using the Wilcoxon signed-rank test. affected eye [12]. This is in agreement with the consensus that large cupping in glaucoma patients is vulnerable to CRVO [3,12]. Moreover, the incidence of the ischemic CRVO type in pre-existing glaucoma was similar to that in the non-glaucoma population. Beaumont et al. found that retinal venous occlusion at the optic cup has a higher IOP, C/D ratio and prevalence of POAG [3]. In contrast, Hayreh et al.compared CRVO patients and found that even without glaucoma medication, patients with pre-existing glaucoma had a lower IOP in the lesion eye compared to patients without preexisting glaucoma [13,14]. Cappin et al. found that the IOP was 4 mmhg lower in the CRVO eye compared to the other eye in glaucoma patients. By iris angiography, they also found that the vessel of the iris was relatively dilated in CRVO eyes [15]. However, in the Taiwanese population, 46.7% and 45% of patients in the pre-existing glaucoma group were POAG and PACG, respectively. The IOP at CRVO presentation was higher in the pre-existing glaucoma group (mean: 21.7 mmhg) compared to the non-pre-existing glaucoma group (13.9 mmhg). Because the mean diagnosed time was approximately 1.5 months in this study, it is unknown whether the IOP increase occurred before or after CRVO. The exact mechanism of IOP change after CRVO in different types of glaucoma requires further evaluation. According to an evidence-based study on the natural course of CRVO, the proportion of non-ischemic cases that converted to ischemic cases was as high as 30% in three years [4]. The ischemic type CRVO can lead to NVG in 20% of patients [4]. In our study, for ischemic CRVO, there were more cases with NVG within 6 months in the pre-existing glaucoma group than the control group, but the number of cases was similar after longterm follow up. It is important to understand the other predisposing factors that contribute to the development of NVG in cases with primary glaucoma. We found that in patients with pre-existing glaucoma, the formation of NVG within 0.5 yr was significantly, positively correlated with IOP at presentation and marginally correlated with the C/D ratio at presentation. Due to the retrospective nature of this study, it is difficult to determine the exact IOP changes at the onset of CRVO. However, higher IOP or poor IOP control could theoretically compromise blood perfusion and increase the risk of neovascularisation of the iris. Therefore, it is important to periodically measure the IOP and control IOP after a CRVO event. There was a similar incidence of the conventional management of PRP among the two groups, which suggests that pre-existing glaucoma is not prone to rubeosis iridis. According to the results of this study, the incidence of neovascular glaucoma with increased IOP was lower than the incidence of PRP performed for cases of rubeosis iridis. Although PRP was effective in eliminating ocular neovascularisation in CRVO in this study, Hayreh et al. revealed marked peripheral visual field loss after laser treatment [16]. One of the drawbacks of this retrospective study was the absence of visual field data collected after a CRVO event from; as a result, we could not conclude anything about the change in the visual field. Furthermore, a relatively high proportion (approximately 20%) of preexisting glaucoma patients underwent glaucoma surgery after a CRVO event. This is the first study to address the consequence of two major causes of glaucoma surgery, NVG or persistent elevated IOP without ocular neovascularisation. The pathogenesis of intractable increased IOP without iris neovascularisation after CRVO is not clear. In previous reports, the levels of vascular endothelial growth factor were increased in the aqueous humour of glaucoma cases [17]. After a CRVO event, reduced blood flow in the retinal capillaries leads to hypoxia, upregulation and release of VEGF and ocular neovascularisation. Intractable IOP may be secondary to hypoxic and inflammatory changes after CRVO, all of which aggregated in the pre-existing glaucoma cases even though ocular neovascularisation did not develop.
6 Chen et al. BMC Ophthalmology 2014, 14:119 Page 6 of 6 According to an epidemiology study, the severity of diabetic retinopathy and performance of PRP do not correlate with progressive enlargement of cupping [18]. In contrast, this study found that the ischemic change of the retina after CRVO in pre-existing POAG and PACG revealed a retinal nerve fibre layer defect, which progressed throughout the study period. Although with the limitation of the study that different clinicians observed the cupping, this study illustrates the change in the neuroretinal rim in CRVO with pre-existing glaucoma and may partially explain the reason for progressive deteriorated vision in these patients. Generally speaking, vision progressively deteriorated during the long-term follow up in this cohort study. Conclusions The distribution of pre-existing glaucoma in CRVO in the Taiwanese population is different from Western countries. Identifying the profile of pre-existing glaucoma in CRVO is fundamental to further identify effective management strategies. Both the retinal non-perfusion status and uncontrolled IOP contribute to NVG in patients with pre-existing glaucoma after CRVO. Physicians should be aware of the increased IOP after CRVO during follow-up, and glaucoma surgery is necessary for preexisting glaucoma cases with intractable elevated IOP with or without INV. For such underlying glaucoma diseases associated with glaucomatous optic nerve atrophy, prompt beneficial therapy to prevent complications and preserve vision requires further study. Competing interests The authors declare that they have no competing interests. There are no sources of financial support to declare in this paper. Authors contributions HFC, LHC, MCC and CCL conceived of the study, participated in its design and helped to draft the manuscript. MCC and LHC also performed the statistical analysis. LY, NKW, HSLC, WCK, SCW, and SHL C participated in the data collection and analysis. All authors read and approved the final manuscript. 3. Beaumont PE, Kang HK: Cup-to-disc ratio, intraocular pressure, and primary open-angle glaucoma in retinal venous occlusion. Ophthalmology 2002, 109: Central Vein Occlusion Study Group: Natural history and clinical management of central retinal vein occlusion. Arch Ophthalmol 1997, 115: Mclntosh RL, Rogers SL, Lim L, Cheung N, Wang JJ, Mitchell P, Kowalski JW, Nguyen HP, Wong TY: Natural history of central retinal vein occlusion: an evidence-based systematic review. Ophthalmology 2010, 117: The Central Vein Occlusion Study Group: A randomized clinical trial of early panretinal photocoagulation for ischemic central vein occlusion: the Central Vein Occlusion Study Group N report. Ophthalmology 1995, 102: Koizumi H, Daniela C, Ferrara, Claudia B, Richard F, Spaide: Central retinal vein occlusion case control Study. Am J Ophthalmol 2007, 144: Sohan Singh H: Prevalent misconceptions about acute retinal vascularocclusivedisorders. Prog Retin Eye Res 2005, 24: Moisseievl J, Howard D, Yael C, Ayala Lusky SM: Glaucoma and visualoutcome in central retinalveinocclusion. Acta Ophthalmol Scand 1996, 74: Michaelides M, Foster PJ: Retinal vein occlusion and angle closure: a retrospective case series. J Glaucoma 2010, 19: Hayreh SS, Zimmerman MB, Podhajsky PA: Retinal vein occlusion and the optic disk. Retina 2012, 2: Prata TS, Rozenbaum I, de Moraes CG, Lima VC, Liebmann J, Ritch R: Retinal vascular occlusions occur more frequently in the more affected eye in exfoliation syndrome. Eye (Lond) 2010, 24: Sohan Singh H, Bridget Z, Meena B, Patricia P: Intraocular pressure abnormalitiesassociated with central and hemicentral retinal vein occlusion. Ophthalmology 2004, 111: Hayreh SS, March W, Phelps CD: Ocular hypotonyfollowingretinal vein occlusion. Arch Ophthalmol 1978, 96: Cappin JM, Whitelocke R: The iris in central retinal thrombosis. Proc R Soc Med 1974, 67: Hayreh SS, Klugman MR, Podhajsky P, Servais GE, Perkins ES: Argon laser panretinal photocoagulation in ischemic central retinal vein occlusion a 10-year prospective study. Graefes Arch Clin Exp Ophthalmol 1990, 228: Hu DN, Ritch R, Liebmann J, Liu Y, Cheng B, Hu MS: Vascular endothelial growth factor is increased in aqueous humor of glaucomatous eyes. J Glaucoma 2002, 11: Klein BE, Moss SE, Magli YL, Klein R, Hoyer C, Johnson J: Optic disc cupping: prevalence findings from the WESDR. Invest Ophthalmol Vis Sci 1989, 30: doi: / Cite this article as: Chen et al.: Neovascular glaucoma after central retinal vein occlusion in pre-existing glaucoma. BMC Ophthalmology :119. Acknowledgments We do not have anyone or any sources of funding to acknowledge. Author details 1 Department of Ophthalmology, Chang Gung Memorial Hospital, 222 Mai-Chin Rd, Keelung 204, Taiwan. 2 Department of Ophthalmology, Chang Gung Memorial Hospital, Linkuo Medical Center, Taoyuan, Taiwan. 3 Department of Public Health and Biostatistics Consulting Center, School of Medicine, Chang Gung University, Taoyuan, Taiwan. 4 Chang Gung University College of Medicine, Taoyuan, Taiwan. Received: 6 May 2014 Accepted: 24 September 2014 Published: 5 October 2014 References 1. Soni KG, Woodhouse DF: Retinal vascular occlusion as a presenting feature of glaucoma simplex. Br J Ophthalmol 1971, 55: Vadala G, Zanini A, Favero C, Brogliatti B, Boles Carenini B: Evaluation of the clinical course of central retinal vein occlusion in eyes with and without glaucoma. Acta Ophthalmol Scand Suppl 1997, 224: Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective cohort study
 Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Vascular Disease Ocular Manifestations of Systemic Hypertension
 Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Yoshiro Minami 1*, Taiji Nagaoka 2, Akihiro Ishibazawa 1,2 and Akitoshi Yoshida 2
 Minami et al. BMC Ophthalmology (2017) 17:90 DOI 10.1186/s12886-017-0485-4 RESEARCH ARTICLE Open Access Correlation between short- and long-term effects of intravitreal ranibizumab therapy on macular edema
Minami et al. BMC Ophthalmology (2017) 17:90 DOI 10.1186/s12886-017-0485-4 RESEARCH ARTICLE Open Access Correlation between short- and long-term effects of intravitreal ranibizumab therapy on macular edema
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Neovascular glaucoma (NVG) is the end result of. Clinical Experience in the Management of Neovascular Glaucoma. Original Article METHODS
 Original Article J Chin Med Assoc 2004;67:131-135 Tung-Mei Kuang Catherine Jui-Ling Liu Ching-Kuang Chou Wen-Ming Hsu Department of Ophthalmology, Taipei Veterans General Hospital and National Yang-Ming
Original Article J Chin Med Assoc 2004;67:131-135 Tung-Mei Kuang Catherine Jui-Ling Liu Ching-Kuang Chou Wen-Ming Hsu Department of Ophthalmology, Taipei Veterans General Hospital and National Yang-Ming
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Prevalence Of Primary Open Angle Glaucoma in Diabetic Patients
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. III (June. 2017), PP 147-151 www.iosrjournals.org Prevalence Of Primary Open Angle Glaucoma
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. III (June. 2017), PP 147-151 www.iosrjournals.org Prevalence Of Primary Open Angle Glaucoma
NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION
 October 2006 E AST AFRICAN MEDICAL JOURNAL 559 East African Medical Journal Vol. 83 No. 10 October 2006 NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION: A.O. Ashaye, FWACS, MSc, Department of Ophthalmology,
October 2006 E AST AFRICAN MEDICAL JOURNAL 559 East African Medical Journal Vol. 83 No. 10 October 2006 NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION: A.O. Ashaye, FWACS, MSc, Department of Ophthalmology,
MANAGEMENT OF NEOVASCULAR GLAUCOMA
 MSO EXPRESS: ISSUE 3 MANAGEMENT OF NEOVASCULAR GLAUCOMA Associate Professor Dr. Norlina Mohd Ramli, Dr. Ng Ker Hsin Associate Professor Dr. Norlina Mohd Ramli MBBS (UK) MRCOphth (UK) MS Ophthal (Mal) Fellowship
MSO EXPRESS: ISSUE 3 MANAGEMENT OF NEOVASCULAR GLAUCOMA Associate Professor Dr. Norlina Mohd Ramli, Dr. Ng Ker Hsin Associate Professor Dr. Norlina Mohd Ramli MBBS (UK) MRCOphth (UK) MS Ophthal (Mal) Fellowship
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
EFFECTIVENESS OF RADIAL OPTIC NEUROTOMY FOR ISCHEMIC CENTRAL RETINAL VEIN OCCLUSION ABSTRACT
 ORIGINAL ARTICLE EFFECTIVENESS OF RADIAL OPTIC NEUROTOMY FOR ISCHEMIC CENTRAL RETINAL VEIN OCCLUSION Mir Ali Shah 1, Faisal Nawaz 2, Adnan Alam 3, Bilal Khan 4 1-4 Department of Ophthalmology, Lady Reading
ORIGINAL ARTICLE EFFECTIVENESS OF RADIAL OPTIC NEUROTOMY FOR ISCHEMIC CENTRAL RETINAL VEIN OCCLUSION Mir Ali Shah 1, Faisal Nawaz 2, Adnan Alam 3, Bilal Khan 4 1-4 Department of Ophthalmology, Lady Reading
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Clinical Study Evaluation of Peripapillary Nerve Fiber Layer after Dexamethasone Implantation (Ozurdex) in Branch Retinal Vein Occlusions
 Ophthalmology Volume 2016, Article ID 2050796, 4 pages http://dx.doi.org/10.1155/2016/2050796 Clinical Study Evaluation of Peripapillary Nerve Fiber Layer after Dexamethasone Implantation (Ozurdex) in
Ophthalmology Volume 2016, Article ID 2050796, 4 pages http://dx.doi.org/10.1155/2016/2050796 Clinical Study Evaluation of Peripapillary Nerve Fiber Layer after Dexamethasone Implantation (Ozurdex) in
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus
 The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England. Retinal Vein Occlusion (RVO) with Macular oedema (MO)
 Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
 Research Article http://www.alliedacademies.org/clinical-ophthalmology-and-vision-science/ A 2-year retrospective study of the treatment of retinal vein occlusion with dexamethasone 0.7 mg intravitreal
Research Article http://www.alliedacademies.org/clinical-ophthalmology-and-vision-science/ A 2-year retrospective study of the treatment of retinal vein occlusion with dexamethasone 0.7 mg intravitreal
Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic Syndrome
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Hindawi Publishing Corporation Journal of Ophthalmology Volume 215, Article ID 62372, 5 pages http://dx.doi.org/1.1155/215/62372 Clinical Study Choroidal Thickness in Eyes with Unilateral Ocular Ischemic
Intravitreal Bevacizumab (IVB) In The Management of Recalcitrant Neovascular Glaucoma (NVG)
 March 2008 Sonia Rani John et al. - IVB in NVG 33 ORIGINAL ARTICLE Intravitreal Bevacizumab (IVB) In The Management of Recalcitrant Neovascular Glaucoma (NVG) Dr. Sonia Rani John DNB, Dr. Meena Chakrabarti
March 2008 Sonia Rani John et al. - IVB in NVG 33 ORIGINAL ARTICLE Intravitreal Bevacizumab (IVB) In The Management of Recalcitrant Neovascular Glaucoma (NVG) Dr. Sonia Rani John DNB, Dr. Meena Chakrabarti
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
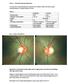 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Development and classification of rubeosis iridis
 British Journal of Ophthalmology, 1979, 63, 150-156 Development and classification of rubeosis iridis in diabetic eye disease LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki,
British Journal of Ophthalmology, 1979, 63, 150-156 Development and classification of rubeosis iridis in diabetic eye disease LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki,
Incidence and Clinical Features of Neovascularization of the Iris following Acute Central Retinal Artery Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(5):352-359 http://dx.doi.org/10.3341/kjo.2016.30.5.352 Original Article Incidence and Clinical Features of Neovascularization of the Iris following
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(5):352-359 http://dx.doi.org/10.3341/kjo.2016.30.5.352 Original Article Incidence and Clinical Features of Neovascularization of the Iris following
Study of the Effect of Injection Bevacizumab through Various Routes in Neovascular Glaucoma
 JOCGP Original Article Study of the Effect of Injection Bevacizumab through Various 10.5005/jp-journals-10008-1200 Routes in Neovascular Glaucoma Study of the Effect of Injection Bevacizumab through Various
JOCGP Original Article Study of the Effect of Injection Bevacizumab through Various 10.5005/jp-journals-10008-1200 Routes in Neovascular Glaucoma Study of the Effect of Injection Bevacizumab through Various
Glaucoma Burden in a Public Sector Hospital
 Original Article Glaucoma Burden in a Public Sector Hospital P.S Mahar, M Aamir Shahzad Pak J Ophthalmol 28, Vol. 24 No. 3...............................................................................
Original Article Glaucoma Burden in a Public Sector Hospital P.S Mahar, M Aamir Shahzad Pak J Ophthalmol 28, Vol. 24 No. 3...............................................................................
Research Article Prognostic Factor Analysis of Intraocular Pressure with Neovascular Glaucoma
 Journal of Ophthalmology Volume 216, Article ID 125895, 9 pages http://dx.doi.org/1.1155/216/125895 Research Article Prognostic Factor Analysis of Intraocular Pressure with Neovascular Glaucoma Satoko
Journal of Ophthalmology Volume 216, Article ID 125895, 9 pages http://dx.doi.org/1.1155/216/125895 Research Article Prognostic Factor Analysis of Intraocular Pressure with Neovascular Glaucoma Satoko
GONIOSCOPIC FINDINGS IN PATIENTS WITH ACUTE CENTRAL/HEMICENTRAL RETINAL VEIN OCCLUSIONS
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 2 SURGERY ORIGINAL PAPERS GONIOSCOPIC FINDINGS IN PATIENTS WITH ACUTE CENTRAL/HEMICENTRAL RETINAL VEIN OCCLUSIONS D. Călugăru 1, M. Călugăru 2 University
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 2 SURGERY ORIGINAL PAPERS GONIOSCOPIC FINDINGS IN PATIENTS WITH ACUTE CENTRAL/HEMICENTRAL RETINAL VEIN OCCLUSIONS D. Călugăru 1, M. Călugăru 2 University
Clinical Features of Ocular Ischemic Syndrome and Risk Factors for Neovascular Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 2017 Jun 26. [Epub ahead of print] https://doi.org/10.3341/kjo.2016.0067 Original Article Clinical Features of Ocular Ischemic Syndrome and Risk Factors for Neovascular
pissn: 1011-8942 eissn: 2092-9382 2017 Jun 26. [Epub ahead of print] https://doi.org/10.3341/kjo.2016.0067 Original Article Clinical Features of Ocular Ischemic Syndrome and Risk Factors for Neovascular
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Disc Hemorrhages in Patients with both Normal Tension Glaucoma and Branch Retinal Vein Occlusion in Different Eyes
 Korean Journal of Ophthalmology 21(4):222-227, 2007 DOI : 10.3341/kjo.2007.21.4.222 Disc Hemorrhages in Patients with both Normal Tension Glaucoma and Branch Retinal Vein Occlusion in Different Eyes Young
Korean Journal of Ophthalmology 21(4):222-227, 2007 DOI : 10.3341/kjo.2007.21.4.222 Disc Hemorrhages in Patients with both Normal Tension Glaucoma and Branch Retinal Vein Occlusion in Different Eyes Young
Efficacy and Safety of Intracameral Bevacizumab for Treatment of Neovascular Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):538-547 https://doi.org/10.3341/kjo.2017.0017 Original Article Efficacy and Safety of Intracameral Bevacizumab for Treatment of Neovascular
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(6):538-547 https://doi.org/10.3341/kjo.2017.0017 Original Article Efficacy and Safety of Intracameral Bevacizumab for Treatment of Neovascular
Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage
 Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Retinal vein occlusion (RVO) is a vascular disease
 INTRAVITREAL RANIBIZUMAB FOR RETINAL VEIN OCCLUSION THROUGH 1 YEAR IN CLINICAL PRACTICE TROELS BRYNSKOV, MD,* HENRIK KEMP, MD,* TORBEN L. SØRENSEN, MD, DMSC* Purpose: To evaluate the efficacy and safety
INTRAVITREAL RANIBIZUMAB FOR RETINAL VEIN OCCLUSION THROUGH 1 YEAR IN CLINICAL PRACTICE TROELS BRYNSKOV, MD,* HENRIK KEMP, MD,* TORBEN L. SØRENSEN, MD, DMSC* Purpose: To evaluate the efficacy and safety
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
Anterior chamber depth and angle-closure glaucoma after central retinal vein occlusion
 Wu et al. BMC Ophthalmology (2016) 16:68 DOI 10.1186/s12886-016-0256-7 RESEARCH ARTICLE Anterior chamber depth and angle-closure glaucoma after central retinal vein occlusion Shiu-Chen Wu 1,2, Yung-Sung
Wu et al. BMC Ophthalmology (2016) 16:68 DOI 10.1186/s12886-016-0256-7 RESEARCH ARTICLE Anterior chamber depth and angle-closure glaucoma after central retinal vein occlusion Shiu-Chen Wu 1,2, Yung-Sung
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Clinical Study Effect of Preoperative Intravitreal Bevacizumab on the Surgical Outcome of Neovascular Glaucoma at Different Stages
 Hindawi Ophthalmology Volume 2017, Article ID 7672485, 7 pages https://doi.org/10.1155/2017/7672485 Clinical Study Effect of Preoperative Intravitreal Bevacizumab on the Surgical Outcome of Neovascular
Hindawi Ophthalmology Volume 2017, Article ID 7672485, 7 pages https://doi.org/10.1155/2017/7672485 Clinical Study Effect of Preoperative Intravitreal Bevacizumab on the Surgical Outcome of Neovascular
Christina L. Ryu, 1 Adrian Elfersy, 1 Uday Desai, 1 Thomas Hessburg, 1 Paul Edwards, 1 and Hua Gao 1,2. 1. Introduction
 Ophthalmology, Article ID 317694, 6 pages http://dx.doi.org/10.1155/2014/317694 Research Article The Effect of Antivascular Endothelial Growth Factor Therapy on the Development of Neovascular Glaucoma
Ophthalmology, Article ID 317694, 6 pages http://dx.doi.org/10.1155/2014/317694 Research Article The Effect of Antivascular Endothelial Growth Factor Therapy on the Development of Neovascular Glaucoma
Diabetic and the Eye: An Introduction
 Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Variability of IOP following laser photocoagulation used in the treatment of diabetic retinopathy
 International Surgery Journal Agarwal S et al. Int Surg J. 2017 Oct;4(10):3433-3440 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174511
International Surgery Journal Agarwal S et al. Int Surg J. 2017 Oct;4(10):3433-3440 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20174511
Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(4):238-242 DOI: 10.3341/kjo.2011.25.4.238 Evaluation of Changes of Macular Thickness in Diabetic Retinopathy after Cataract Surgery Original
New vessel formation in retinal branch vein occlusion
 Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Neuropathy (NAION) and Avastin. Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013
 Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Efficacy of panretinal laser in ischemic central retinal vein occlusion: A systematic review
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 17: 901-910, 2019 Efficacy of panretinal laser in ischemic central retinal vein occlusion: A systematic review CHENGFANG LI 1, RONGRONG WANG 2, GUOJUN LIU 1, ZHEN
EXPERIMENTAL AND THERAPEUTIC MEDICINE 17: 901-910, 2019 Efficacy of panretinal laser in ischemic central retinal vein occlusion: A systematic review CHENGFANG LI 1, RONGRONG WANG 2, GUOJUN LIU 1, ZHEN
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Sequential pharmacological therapies in the management of macular oedema secondary to retinal vein occlusion
 Northern (NHS) Treatment Advisory Group Sequential pharmacological therapies in the management of macular oedema secondary to retinal vein occlusion Author: Paul Madill Specialty Registrar in Public Health
Northern (NHS) Treatment Advisory Group Sequential pharmacological therapies in the management of macular oedema secondary to retinal vein occlusion Author: Paul Madill Specialty Registrar in Public Health
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Natural Short-term Course of Recurrent Macular Edema Following Intravitreal Bevacizumab Therapy in Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):95-101 https://doi.org/10.3341/kjo.2017.31.2.95 Original Article Natural Short-term Course of Recurrent Macular Edema Following Intravitreal
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):95-101 https://doi.org/10.3341/kjo.2017.31.2.95 Original Article Natural Short-term Course of Recurrent Macular Edema Following Intravitreal
Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization
 Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution
 Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
From Outdated to Updated: A Review of Important Clinical Trials in Ocular Disease from 2014
 From Outdated to Updated: A Review of Important Clinical Trials in Ocular Disease from 2014 1. This course is designed to review the important ophthalmic literature that was released between October 2013
From Outdated to Updated: A Review of Important Clinical Trials in Ocular Disease from 2014 1. This course is designed to review the important ophthalmic literature that was released between October 2013
ORIGINAL ARTICLE RISK FACTORS FOR DEVELOPMENT OF ANGLE CLOSURE GLAUCOMA IN EYES WITH SHALLOW ANTERIOR CHAMBER
 RISK FACTORS FOR DEVELOPMENT OF ANGLE CLOSURE GLAUCOMA IN EYES WITH SHALLOW ANTERIOR CHAMBER Sundeep 1, Niveditha H 2, Pooja Patil 3, N V V Himamshu 4, Vinutha B V 5, Liji P 6, M S Smitha Gowda 7, Nivedhitha
RISK FACTORS FOR DEVELOPMENT OF ANGLE CLOSURE GLAUCOMA IN EYES WITH SHALLOW ANTERIOR CHAMBER Sundeep 1, Niveditha H 2, Pooja Patil 3, N V V Himamshu 4, Vinutha B V 5, Liji P 6, M S Smitha Gowda 7, Nivedhitha
Understanding Angle Closure
 Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY
 ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
Progression of diabetic retinopathy after cataract extraction
 BritishlournalofOphthalmology, 1991,75,547-551 Ophthalmology Department, Kaplan Hospital, Rehovot, affiliated with the Hebrew University-Hadassah Medical School, Jerusalem, Israel A Pollock S Dotan M Oliver
BritishlournalofOphthalmology, 1991,75,547-551 Ophthalmology Department, Kaplan Hospital, Rehovot, affiliated with the Hebrew University-Hadassah Medical School, Jerusalem, Israel A Pollock S Dotan M Oliver
Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after Pattern Scanning Laser Photocoagulation in Patients with Diabetic Retinopathy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(3):220-225 http://dx.doi.org/10.3341/kjo.2014.28.3.220 Original Article Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(3):220-225 http://dx.doi.org/10.3341/kjo.2014.28.3.220 Original Article Changes in Peripapillary Retinal Nerve Fiber Layer Thickness after
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Health Technology Appraisal. Aflibercept for treating diabetic macular oedema.
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Aflibercept for treating diabetic macular oedema Final scope Final remit/appraisal objective To appraise the clinical and cost
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Aflibercept for treating diabetic macular oedema Final scope Final remit/appraisal objective To appraise the clinical and cost
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
A retrospective nonrandomized study was conducted at 3
 Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Optic Disc Cupping: Four Year Follow-up from the WESDR
 Investigative Ophthalmology & Visual Science, Vol. 30, o., February 989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Four Year Follow-up from the WER Barbara E. K.
Investigative Ophthalmology & Visual Science, Vol. 30, o., February 989 Copyright Association for Research in Vision and Ophthalmology Optic Disc Cupping: Four Year Follow-up from the WER Barbara E. K.
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
Citation BMC Ophthalmology, 2016, v. 16, article no. 64
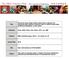 Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
4/27/2010 INTRODUCTION TO RETINAL VASCULAR DISEASE VENOUS/VENULAR CENTRAL RETINAL VEIN OBSTRUCTION / CRVO ADDITIONAL FEATURES /COMPLICATIONS
 INTRODUCTION TO RETINAL VASCULAR DISEASE VENOUS/VENULAR Leo Semes, OD Professor, UAB Optometry 2 CENTRAL RETINAL VEIN OBSTRUCTION CENTRAL RETINAL VEIN OBSTRUCTION / OCCLUSION (CRVO) obstruction of the
INTRODUCTION TO RETINAL VASCULAR DISEASE VENOUS/VENULAR Leo Semes, OD Professor, UAB Optometry 2 CENTRAL RETINAL VEIN OBSTRUCTION CENTRAL RETINAL VEIN OBSTRUCTION / OCCLUSION (CRVO) obstruction of the
Comparison of Ranibizumab and Bevacizumab for Macular Edema Associated with Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(3):209-216 https://doi.org/10.3341/kjo.2015.0158 Original Article Comparison of Ranibizumab and Bevacizumab for Macular Edema Associated with
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(3):209-216 https://doi.org/10.3341/kjo.2015.0158 Original Article Comparison of Ranibizumab and Bevacizumab for Macular Edema Associated with
Bevacizumab (Avastin ) for neovascular glaucoma secondary to ischaemic central retinal vein occlusion
 Bevacizumab (Avastin ) for neovascular glaucoma secondary to ischaemic central retinal vein occlusion Author: William Horsley Lead Pharmacist for April 2011 2011 Summary Neovascular glaucoma is an acutely
Bevacizumab (Avastin ) for neovascular glaucoma secondary to ischaemic central retinal vein occlusion Author: William Horsley Lead Pharmacist for April 2011 2011 Summary Neovascular glaucoma is an acutely
Case Follow Up. Sepi Jooniani PGY-1
 Case Follow Up Sepi Jooniani PGY-1 Triage 54 year old M Pt presents to prelim states noticed today he had reddness to eyes, states worse in R eye. Pt denies any pain or itching. No further complaints.
Case Follow Up Sepi Jooniani PGY-1 Triage 54 year old M Pt presents to prelim states noticed today he had reddness to eyes, states worse in R eye. Pt denies any pain or itching. No further complaints.
Macular edema (ME) is the most common
 MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care
 The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Prevalence, pattern and risk factors of retinal vein occlusion in an elderly population in Nepal: the Bhaktapur retina study
 Thapa et al. BMC Ophthalmology (2017) 17:162 DOI 10.1186/s12886-017-0552-x RESEARCH ARTICLE Prevalence, pattern and risk factors of retinal vein occlusion in an elderly population in Nepal: the Bhaktapur
Thapa et al. BMC Ophthalmology (2017) 17:162 DOI 10.1186/s12886-017-0552-x RESEARCH ARTICLE Prevalence, pattern and risk factors of retinal vein occlusion in an elderly population in Nepal: the Bhaktapur
Dexamethasone Intravitreal Implant Rescue Treatment for Bevacizumab Refractory Macular Edema Secondary to Branch Retinal Vein Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):108-114 https://doi.org/10.3341/kjo.2017.31.2.108 Original Article Dexamethasone Intravitreal Implant Rescue Treatment for Bevacizumab Refractory
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(2):108-114 https://doi.org/10.3341/kjo.2017.31.2.108 Original Article Dexamethasone Intravitreal Implant Rescue Treatment for Bevacizumab Refractory
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion
 AOP*** 1 Original Article Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion Rasha I Ali1, Kapil G Kapoor 1,2, Adeel N Khan 1, Syed K Gibran 1 Purpose: To
AOP*** 1 Original Article Efficacy of combined intravitreal bevacizumab and triamcinolone for branch retinal vein occlusion Rasha I Ali1, Kapil G Kapoor 1,2, Adeel N Khan 1, Syed K Gibran 1 Purpose: To
FRANZCO, MD, MBBS. Royal Darwin Hospital
 Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Prognosis for rubeosis iridis following central
 British Journal of Ophthalmology, 1979, 63, 735-743 Prognosis for rubeosis iridis following central retinal vein occlusion STEPHEN H. SINCLAIR AND EVANGELOS S. GRAGOUDAS From the Eye Research Institute
British Journal of Ophthalmology, 1979, 63, 735-743 Prognosis for rubeosis iridis following central retinal vein occlusion STEPHEN H. SINCLAIR AND EVANGELOS S. GRAGOUDAS From the Eye Research Institute
ABSTRACT INTRODUCTION
 DOI 10.1007/s40123-017-0114-6 ORIGINAL RESEARCH Real-World Cost Savings Demonstrated by Switching Patients with Refractory Diabetic Macular Edema to Intravitreal Fluocinolone Acetonide (Iluvien): A Retrospective
DOI 10.1007/s40123-017-0114-6 ORIGINAL RESEARCH Real-World Cost Savings Demonstrated by Switching Patients with Refractory Diabetic Macular Edema to Intravitreal Fluocinolone Acetonide (Iluvien): A Retrospective
Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure
 ORIGINAL ARTICLE Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure Jimmy S. M. Lai, 1 FRCS, FRCOphth, FHKAM (Ophthalmology), M.Med (Ophthalmology),
ORIGINAL ARTICLE Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure Jimmy S. M. Lai, 1 FRCS, FRCOphth, FHKAM (Ophthalmology), M.Med (Ophthalmology),
GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 3 SURGERY ORIGINAL PAPERS GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES Nicoleta Anton Apreutesei¹, D. Chiselita²*, O. I. Motas ¹ University of Medicine
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 3 SURGERY ORIGINAL PAPERS GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES Nicoleta Anton Apreutesei¹, D. Chiselita²*, O. I. Motas ¹ University of Medicine
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Andrew J. Barkmeier, MD; Benjamin P. Nicholson, MA; Levent Akduman, MD
 c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
Efficacy and safety of Pro Re Nata regimen without loading dose ranibizumab injections in retinal vein occlusion
 Open Access Original Article Efficacy and safety of Pro Re Nata regimen without loading dose ranibizumab injections in retinal vein occlusion Erkan Unsal 1, Kadir Eltutar 2, Pınar Sultan 3, Hulya Gungel
Open Access Original Article Efficacy and safety of Pro Re Nata regimen without loading dose ranibizumab injections in retinal vein occlusion Erkan Unsal 1, Kadir Eltutar 2, Pınar Sultan 3, Hulya Gungel
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
NIH Public Access Author Manuscript Int Ophthalmol Clin. Author manuscript; available in PMC 2012 July 1.
 NIH Public Access Author Manuscript Published in final edited form as: Int Ophthalmol Clin. 2011 ; 51(3): 27 36. doi:10.1097/iio.0b013e31821e5960. Medical and Surgical Treatment of Neovascular Glaucoma
NIH Public Access Author Manuscript Published in final edited form as: Int Ophthalmol Clin. 2011 ; 51(3): 27 36. doi:10.1097/iio.0b013e31821e5960. Medical and Surgical Treatment of Neovascular Glaucoma
Diabetic Retinopatathy
 Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Electrodiagnostics Alphabet Soup
 Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic What is electrodiagnostics testing? Visual Pathway Basic Understanding VEP
Nathan Lighthizer, O.D., F.A.A.O Assistant Professor, NSUOCO Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic What is electrodiagnostics testing? Visual Pathway Basic Understanding VEP
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs
 The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
Research Article Long-Term Outcome after Vitrectomy for Macular Edema with Retinal Vein Occlusion Dividing into the Occlusion Site
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2014, Article ID 198782, 6 pages http://dx.doi.org/10.1155/2014/198782 Research Article Long-Term Outcome after Vitrectomy for Macular Edema
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2014, Article ID 198782, 6 pages http://dx.doi.org/10.1155/2014/198782 Research Article Long-Term Outcome after Vitrectomy for Macular Edema
