Pioglitazone for Diabetes Prevention in Impaired Glucose Tolerance
|
|
|
- June Anderson
- 5 years ago
- Views:
Transcription
1 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Pioglitazone for Diabetes Prevention in Impaired Glucose Tolerance Ralph A. DeFronzo, M.D., Devjit Tripathy, M.D., Ph.D., Dawn C. Schwenke, Ph.D., MaryAnn Banerji, M.D., George A. Bray, M.D., Thomas A. Buchanan, M.D., Stephen C. Clement, M.D., Robert R. Henry, M.D., Howard N. Hodis, M.D., Abbas E. Kitabchi, M.D., Ph.D., Wendy J. Mack, Ph.D., Sunder Mudaliar, M.D., Robert E. Ratner, M.D., Ken Williams, M.Sc., Frankie B. Stentz, Ph.D., Nicolas Musi, M.D., and Peter D. Reaven, M.D., for the ACT NOW Study A BS TR AC T From the Texas Diabetes Institute and University of Texas Health Science Center (R.A.D., D.T., N.M.) and KenAnCo Biostatistics (K.W.) both in San Antonio; Phoenix Veterans Affairs (VA) Health Care System, Phoenix, AZ (D.C.S., P.D.R.); College of Nursing and Health Innovation, Arizona State University, Phoenix (D.C.S.); SUNY Health Science Center at Brooklyn, Brooklyn, NY (M.B.); Pennington Biomedical Research Center Louisiana State University, Baton Rouge (G.A.B.); University of Southern California Keck School of Medicine, Los Angeles (T.A.B., H.N.H., W.J.M.); Division of Endocrinology and Metabolism, Georgetown University, Washington, DC (S.C.C.); VA San Diego Healthcare System and University of California at San Diego, San Diego (R.R.H., S.M.); University of Tennessee, Division of Endocrinology, Diabetes, and Metabolism, Memphis (A.E.K., F.B.S.); and Medstar Research Institute, Hyattsville, MD (R.E.R.). Address reprint requests to Dr. DeFronzo at the Diabetes Division, University of Texas Health Science Center, 7703 Floyd Curl Dr., San Antonio, TX 78229, or at albarado@ uthscsa.edu. Drs. DeFronzo and Tripathy contributed equally to this article. N Engl J Med 2011;364: Copyright 2011 Massachusetts Medical Society BACKGROUND Impaired glucose tolerance is associated with increased rates of cardiovascular disease and conversion to type 2 diabetes mellitus. Interventions that may prevent or delay such occurrences are of great clinical importance. METHODS We conducted a randomized, double-blind, placebo-controlled study to examine whether pioglitazone can reduce the risk of type 2 diabetes mellitus in adults with impaired glucose tolerance. A total of 602 patients were randomly assigned to receive pioglitazone or placebo. The median follow-up period was 2.4 years. Fasting glucose was measured quarterly, and oral glucose tolerance tests were performed annually. Conversion to diabetes was confirmed on the basis of the results of repeat testing. RESULTS Annual incidence rates for type 2 diabetes mellitus were 2.1% in the pioglitazone group and 7.6% in the placebo group, and the hazard ratio for conversion to diabetes in the pioglitazone group was 0.28 (95% confidence interval, 0.16 to 0.49; ). Conversion to normal glucose tolerance occurred in 48% of the patients in the pioglitazone group and 28% of those in the placebo group (). Treatment with pioglitazone as compared with placebo was associated with significantly reduced levels of fasting glucose (a decrease of 11.7 mg per deciliter vs. 8.1 mg per deciliter [0.7 mmol per liter vs. 0.5 mmol per liter], ), 2-hour glucose (a decrease of 30.5 mg per deciliter vs mg per deciliter [1.6 mmol per liter vs. 0.9 mmol per liter], ), and HbA 1c (a decrease of 4 percentage points vs. an increase of 0.20 percentage points, ). Pioglitazone therapy was also associated with a decrease in diastolic blood pressure (by 2.0 mm Hg vs. mm Hg, P = 3), a reduced rate of carotid intima media thickening (31.5%, P = 47), and a greater increase in the level of high-density lipoprotein cholesterol (by 7.35 mg per deciliter vs. 4.5 mg per deciliter [0.4 mmol per liter vs. 0.3 mmol per liter], P = 08). Weight gain was greater with pioglitazone than with placebo (3.9 kg vs kg, ), and edema was more frequent (12.9% vs. 6.4%, P = 07). CONCLUSIONS As compared with placebo, pioglitazone reduced the risk of conversion of impaired glucose tolerance to type 2 diabetes mellitus by 72% but was associated with significant weight gain and edema. (Funded by Takeda Pharmaceuticals and others; ClinicalTrials.gov number, NCT ) n engl j med 364;12 nejm.org march 24, 2011
2 Pioglitazone for Diabetes Prevention in IGT Type 2 diabetes mellitus affects 21 million Americans, 1 and its prevalence is increasing. 2 Microvascular and macrovascular complications are common in type 2 diabetes mellitus and are related to both the severity and the duration of hyperglycemia. 3 The natural history of type 2 diabetes mellitus has been well defined, 4 starting with a genetic predisposition and progression from normal glucose tolerance with insulin resistance to impaired glucose tolerance and eventually type 2 diabetes mellitus with the superimposition of beta-cell failure. Because hyperglycemia plays a central role in the microvascular and macrovascular complications of diabetes, 3,5,6 it is possible that interventions that prevent or delay hyperglycemia may effectively prevent or delay these long-term complications. Studies have shown that the rate of conversion of impaired glucose tolerance to type 2 diabetes mellitus is reduced with lifestyle modification 7 ; the use of metformin, 7 thiazolidinediones, 8-11 or acarbose 12 ; and bariatric surgery. 13 The greatest reductions in conversion rates have been observed with weight loss, the use of thiazolidinediones, and surgery. Troglitazone was reported to be associated with a 55% decrease in the rate of conversion to diabetes among women with prior gestational diabetes, 11 but this agent is no longer available. In one study, 9 the use of rosiglitazone decreased the risk of diabetes in adults with impaired glucose tolerance by 62%; given concerns about cardiovascular safety, 14 however, the Food and Drug Administration has restricted the use of rosig litazone therapy to patients in whom glycemic control cannot be achieved with other medications and who cannot take pioglitazone. We undertook the present study to examine the effect of pioglitazone on diabetes risk and cardiovascular risk factors in adults with impaired glucose tolerance. Me thods Patients We recruited male and female patients who were 18 years of age or older and had impaired glucose tolerance (defined as a 2-hour glucose level of 140 to 199 mg per deciliter [7.8 to 11.0 mmol per liter] during a single oral glucose-tolerance test) 15 and a body-mass index (BMI, the weight in kilograms divided by the square of the height in meters) of 25 or more. Patients were eligible for enrollment if they had a fasting plasma glucose level between 95 and 125 mg per deciliter (5.3 and 6.9 mmol per liter) and at least one other risk factor for diabetes. 16 The complete list of inclusion and exclusion criteria is provided in Table 1 in the Supplementary Appendix, available with the full text of this article at NEJM.org. The criteria have also been published previously. 16 During the course of recruitment, the glycemic inclusion criteria were modified to include patients with a fasting plasma glucose level between 90 and 125 mg per deciliter (5.0 and 6.9 mmol per liter) if their 2-hour plasma glucose level during the oral glucose-tolerance test was between 170 and 199 mg per deciliter (9.4 and 11.1 mmol per liter) 17 ; the change was made in recognition of the high risk of diabetes in such persons. The first participant was recruited in January 2004, with the screening ultimately including 1827 potentially eligible patients with impaired glucose tolerance (Fig. 1). The enrollment of 602 participants was completed in March Participants were followed until they reached the primary end point of diabetes, withdrew from the study, were lost to follow-up, or completed the end of the study. Study Design The study design and protocol, which have been described previously, 16 are available at NEJM.org. Eight centers participated in the study, which was approved by the institutional review board at each site. Written informed consent was obtained from all participants. The first author designed the study and, along with the coauthors, wrote the first draft and revisions and approved the final version; he also holds the data at the University of Texas Health Science Center in San Antonio. The study was conducted in accordance with the protocol. All authors made the decision to submit the manuscript for publication. All results were transmitted to the Data Coordinating Center in Phoenix, Arizona, where they were recorded and audited and then sent to the Data Analysis Center in San Antonio. Takeda Pharmaceuticals provided financial support for the study but had no access to the data. After eligibility for the study was ascertained, participants underwent randomization according to center and sex and received 30 minutes of dietary instruction consistent with the goals of the Diabetes Prevention Program, 7 which was re- n engl j med 364;12 nejm.org march 24,
3 T h e n e w e ngl a nd j o u r na l o f m e dic i n e 1827 Patients were assessed for eligibility 1225 Were excluded 277 Had FPG out of range 187 Declined to participate 118 Had medical exclusions 12 Had too few risk factors 4 Had behavioral or logistic problems 627 Had OGTT FPG or 2-hr glucose out of range 602 Underwent randomization 303 Were assigned to receive pioglitazone 299 Were assigned to receive placebo 90 Did not have a final visit for the following reasons: 9 Had weight gain 6 Relocated 12 Had work or schedule conflict 18 Had lack of interest 7 Did not give reason 28 Were lost to follow-up 5 Had unrelated illness or adverse events 5 Had other reason 71 Did not have a final visit for the following reasons: 3 Had weight gain 17 Relocated 1 Had work or schedule conflict 9 Had lack of interest 10 Did not give reason 22 Were lost to follow-up 3 Had unrelated illness or adverse events 6 Had other reason 213 Completed study 228 Completed study Figure 1. Enrollment, Randomization, and Follow-up of Study Patients. FPG denotes fasting plasma glucose, and OGTT oral glucose-tolerance test. inforced on follow-up visits. Once enrolled, participants were asked to fast overnight before undergoing an oral glucose-tolerance test at 8 a.m. the next day. Samples were collected every 15 minutes for 2 hours for measurements of glucose, insulin, and C-peptide. 16 Additional baseline assessments included measurements of blood pressure, height, weight, waist circumference, and level of HbA 1c ; a lipid profile; screening blood tests; urinalysis, with calculation of the ratio of microalbumin to creatinine; and electrocardiography. At seven centers, high-resolution B-mode ultrasonography was performed at baseline, 15 to 18 months after baseline, and at the end of the study, to assess the far wall of the right distal common carotid artery (for details, see the Methods section in the Supplementary Appendix). 18,19 Body-fat content was measured with the use of a dual-energy x-ray absorptiometer (DXA) (Hologic). Participants initially received 30 mg of pioglitazone per day or placebo. One month after randomization, the dose of pioglitazone was increased to 45 mg per day. Participants returned at 2, 4, 6, 8, 10, and 12 months during the first year of the study and once every 3 months thereafter. At each visit, weight, blood pressure, and pulse were measured and the extent of edema was graded (with an increase in edema defined as an increase of two grades or more from baseline) (for details, see Table 2 in the Supplementary 1106 n engl j med 364;12 nejm.org march 24, 2011
4 Pioglitazone for Diabetes Prevention in IGT Appendix). Fasting plasma glucose was also measured at each follow-up visit. The levels of HbA 1c, alanine aminotranferase, and aspartate aminotransferase were measured every 6 months, and the oral glucose-tolerance test was repeated annually. All measurements obtained at baseline were repeated at the end of the study. Conversion of Impaired Glucose Tolerance to Diabetes The primary outcome was the development of diabetes 15 (defined as a fasting plasma glucose level 126 mg per deciliter [ 7.9 mmol per liter] or a 2-hour glucose level 200 mg per deciliter [11.1 mmol per liter]); an oral glucose-tolerance test was performed to confirm the diagnosis. If the diagnosis was not confirmed, patients continued with their assigned therapy. Diabetes was not confirmed but was considered to have developed in five patients receiving pioglitazone and five patients receiving placebo. At the final visit, six patients had a single oral glucose-tolerance test with results that met the diagnostic criteria for diabetes; four of the six were started on antidiabetic medication by their physician. Measurements and Calculations Insulin sensitivity was derived from plasma glucose and insulin measurements obtained during the oral glucose-tolerance test (Matsuda index) 20 and from the results of an intravenous glucosetolerance test with frequent sampling. 21 Beta-cell function was calculated as the index of insulin secretion factored by insulin resistance (ΔI / ΔG Matsuda index) during the oral glucosetolerance test, where ΔI /ΔG represents the mean incremental concentrations of plasma insulin and glucose during the 120-minute oral glucose-tolerance test. 22 Beta-cell function was also calculated as the product of insulin secretion and insulin sensitivity (ΔI 0 10 S I ) during the intravenous glucose-tolerance test with frequent sampling. Laboratory methods are described in detail in the Methods section in the Supplementary Appendix. Statistical Analysis The development of diabetes, 15 the primary outcome, was assessed by means of life-table analysis of the time from randomization to incident diabetes. Separate life-table estimated cumulative incidence curves were calculated for the pioglitazone and placebo groups and compared with the use of the log-rank test. 23 The Cox proportional-hazards model was used to estimate the effect of pioglitazone on the primary outcome. 24 Data for patients who were lost to follow-up or who withdrew were censored at the time of the last visit. Statistical tests were two-sided, with an alpha level of 5. Data are reported as means ±SE. We calculated that enrollment of approximately 600 patients was required to achieve 90% power, if treatment with pioglitazone decreased the rate of conversion from impaired glucose tolerance to type 2 diabetes mellitus by 50%. 16 For analyses of secondary outcomes, which included changes in levels of fasting plasma glucose, 2-hour glucose, and HbA 1c, between-group comparisons of changes in repeated or continuous measures were performed with the use of general linear mixed models, with data transformed to logarithms when appropriate. The statistical heterogeneity of treatment effects within subgroups was assessed. No adjustment was made for multiple comparisons, and subgroup analyses were not prespecified. Two approaches were used to assess whether patients who completed the study differed from those who withdrew. The first approach involved a withdrawal-free survival analysis of time to withdrawal, with the final study visit used as the censoring variable. Data for patients who underwent an oral glucose-tolerance test at the end-ofstudy visit were censored at 3 years. All other patients were counted as having withdrawn as of the last study visit. On the basis of this analysis, the hazard ratio for withdrawal in the pioglitazone group as compared with the placebo group was (P = 0.42). In the second approach, missing data (for the two study groups combined) were assessed for each continuous measure with analysis of variance, stratified according to whether the measure was missing at each subsequent visit. Since neither approach produced statistically significant evidence of bias due to missing data, the primary and secondary analyses were performed without data imputation. R esult s Participants The mean age of the 602 study participants was 52.3±0.5 years, and 58% were women (Table 1). The mean BMI was 34.5±0.4. A total of 407 pa- n engl j med 364;12 nejm.org march 24,
5 T h e n e w e ngl a nd j o u r na l o f m e dic i n e Table 1. Baseline Characteristics of the Patients.* Characteristic Pioglitazone (N = 303) Placebo (N = 299) P Value Isolated impaired glucose tolerance no Both impaired glucose tolerance and impaired fasting glucose tolerance no Ratio of women to men % 58/42 58/ Race or ethnic group no Hispanic White Black Other 11 9 Family history of diabetes no. (%) 177 (58.4) 186 (62.2) 0.34 History of gestational diabetes mellitus no. (% of women) 24 (14) 37 (21) 7 Mean age yr 53.0± ± Age group % yr yr yr Height cm 166± ± Mean BMI 33.0± ± BMI group no. (%) <30 79 (26.0) 76 (25.4) (36.0) 100 (33.4) 0.71 > (37.6) 122 (40.8) 0.65 Waist circumference cm Men 110.5± ± Women 103.1± ± HbA 1c % 5.5± ± Fasting plasma glucose mg/dl 105± ± Hr plasma glucose mg/dl 168±1 168± Fasting plasma insulin mu/liter 10.5± ± Lipid levels mg/dl Total cholesterol 169±2 173± LDL cholesterol 104±2 108± HDL cholesterol 40±1 41± Triglycerides 122±3 121± Fasting free fatty acids (μmol/liter) 551±13 528± Blood pressure mm Hg Systolic 127± ± Diastolic 74±0.6 74± * Plus minus values are means ±SE. No intergroup differences were significant. To convert the values for glucose to millimoles per liter, multiply by To convert the values for insulin to picomoles per liter, multiply by To convert the values for cholesterol to millimoles per liter, multiply by To convert the values for triglycerides to millimoles per liter, multiply by BMI denotes body-mass index (the weight in kilograms divided by the square of the height in meters), HDL high-density lipoprotein, and LDL low-density lipoprotein. Race or ethnic group was self-reported n engl j med 364;12 nejm.org march 24, 2011
6 Pioglitazone for Diabetes Prevention in IGT tients had both impaired fasting glucose and impaired glucose tolerance, and 195 had isolated impaired glucose tolerance. Baseline levels of HbA 1c, fasting plasma glucose, and 2-hour glucose were 5.50±4%, 105±0.3 mg per deciliter (5.8±2 mmol per liter), and 168±1 mg per deciliter (9.32±6 mmol per liter), respectively. None of the baseline clinical, anthropometric, or laboratory variables differed significantly between the placebo group and the pioglitazone group (Table 1). Cumulative Hazard Hazard ratio, 0.28 (95% CI, ) Placebo Pioglitazone Follow-up During a median follow-up period of 2.4 years (mean, 2.2), diabetes developed in 50 of the 299 patients in the placebo group (16.7%) and in 15 of the 303 patients in the pioglitazone group (5.0%). The annual average incidence of diabetes, calculated on the basis of person-years, was 7.6% in the placebo group and 2.1% in the pioglitazone group () (Fig. 2). The hazard ratio for development of diabetes in the pioglitazone group was 0.28 (95% confidence interval, 0.16 to 0.49; ). Adjustment for baseline characteristics did not alter the hazard ratio. The number of people who would need to be treated to prevent one case of diabetes was 8 for 2.2 years of the trial and 18 for 1 year. Among the patients who completed the study, 103 of those in the pioglitazone group (48%) and 65 of those in the placebo group (28%) had normal glucose tolerance (). A total of 161 patients did not complete the study (71 in the placebo group and 90 in the pioglitazone group). The median follow-up time for these patients was 7.6 months. Baseline characteristics of the patients who did not complete the study were similar to those of the 441 patients who completed the study (i.e., those who had conversion to type 2 diabetes mellitus during the study or who completed the oral glucosetolerance test at the end of the trial). Reasons for not completing the study included weight gain (in 9 patients in the pioglitazone group and 3 in the placebo group); patients also left for reasons unrelated to the study medication (Fig. 1). The rate of adherence to the study regimen, assessed by means of pill counts, was greater than 80% in both groups. At the end of the study, 64% of the patients in the treatment group were taking pioglitazone at a daily dose of 45 mg and 81% of those in the placebo group were taking the corresponding placebo dose. The major reasons for No. at Risk Placebo Pioglitazone s since Randomization Figure 2. Kaplan Meier Plot of Hazard Ratios for Time to Development of Diabetes. not increasing the dose of pioglitazone from 30 to 45 mg per day or for not maintaining the 45-mg dose were weight gain and edema. Effects of Pioglitazone Protection from diabetes with pioglitazone was of similar magnitude (with no significant heterogeneity) in subgroups defined by sex, age, weight, race or ethnic group, and fasting glucose level, as well as in patients with both impaired glucose tolerance and impaired fasting glucose and those with isolated impaired glucose tolerance (Fig. 3). There was no evidence of heterogeneity of the response according to the baseline level of HbA 1c. Greater reductions in fasting and 2-hour glucose levels were achieved in the pioglitazone group than in the placebo group ( for both comparisons), with a between-group difference of 3.5±1.1 mg per deciliter (0.2±6 mmol per liter) and 14±3 mg per deciliter (0.8±0.17 mmol per liter), respectively, at the end of the study (Fig. 4A and 4B). Levels of HbA 1c differed between the groups throughout the study (), increasing by 0.20±2% in the placebo group, with no change in the pioglitazone group. Body weight, BMI, and body fat increased in the placebo group (96.7±1.2 to 97.3±1.3 kg, 34.5±0.4 to 34.7±0.4, and 39.0±0.7 to 39.3±0.7%, respectively) and in the pioglitazone group (94.9±1.2 to 98.7±1.3 kg, n engl j med 364;12 nejm.org march 24,
7 T h e n e w e ngl a nd j o u r na l o f m e dic i n e Subgroup All Sex Male Female Age <50 yr yr 60 yr Race or ethnic group White Hispanic Black BMI < >35 Waist circumference Men, <100 cm Men, 100 cm Women, <90 cm Women, 90 cm Fasting plasma glucose mg/dl mg/dl mg/dl Glucose test Isolated IGT IFG and IGT Pioglitazone Placebo incidence rate (per 100 person-yr) Hazard Ratio (95% CI) P Value for Heterogeneity Pioglitazone Better Placebo Better Figure 3. Incidence Rates, Hazard Ratios, and Tests for Heterogeneity for All Patients and Selected Subgroups. The figure shows incidence rates per 100 person-years and corresponding hazard ratios and confidence intervals for the effects of pioglitazone as compared with placebo on the conversion of impaired glucose tolerance to diabetes. The x axis is interrupted to allow for better visual presentation. BMI denotes body-mass index (the weight in kilograms divided by the square of the height in meters), IFG impaired fasting glucose, and IGT impaired glucose tolerance. To convert the values for glucose to millimoles per liter, multiply by ±0.4 to 35.5±0.4, and 4±0.8 to 41.9±0.7%, respectively), but the increments were greater with pioglitazone ( for all comparisons). Systolic blood pressure declined slightly in both groups, but the difference in decline between the groups was not significant. Diastolic blood pressure was consistently lower in the pioglitazone group (P = 1). As compared with placebo, pioglitazone reduced levels of both alanine aminotranferase and aspartate aminotransferase (). The change in high-density lipoprotein (HDL) cholesterol was greater with pioglitazone (40±1 to 48±1 mg per deciliter [2.2±6 to 2.7±6 mmol per liter]) than with placebo (41±1 to 45.1±0.7 mg per deciliter [2.3±6 to 2.5±4 mmol per liter]) (P = 08 for the difference between groups). Triglyceride levels declined significantly with pioglitazone (129±7.5 to 110±4.0 mg per deciliter [7.2±0.42 to 6.1±0.22 mmol per liter], P = 07) but not with placebo (124±4.6 to 113±4.0 mg per deciliter [6.9±0.25 to 6.30±0.22 mmol per liter], P = 0.90); the difference between groups was not significant. Neither pioglitazone nor placebo altered levels of low-density lipoprotein cholesterol. Insulin sensitivity as measured with the Matsuda index increased more with pioglitazone than with placebo (4.31±0.24 to 7.65±0.34 vs n engl j med 364;12 nejm.org march 24, 2011
8 Pioglitazone for Diabetes Prevention in IGT A Fasting Plasma Glucose B 2-Hr Plasma Glucose C HbA 1c 0 5 Placebo 10 Pioglitazone D Weight E Systolic Blood Pressure F Diastolic Blood Pressure P= P=1 6.0 G ALT H AST I Carotid Intima Media Thickness P= Figure 4. Effects of Pioglitazone as Compared with Placebo. Over the course of the study, mean percentage changes and standard errors in continuous measures were calculated with the use of a linear, mixed-repeated-measures model fit to all available data for each measure. As compared with placebo, treatment with pioglitazone (dashed lines) had beneficial effects on fasting plasma glucose levels (Panel A), 2-hour plasma glucose levels (Panel B), and HbA 1c levels (Panel C) and on systolic and diastolic blood pressure (Panels E and F, respectively), alanine aminotransferase (ALT) and aspartate aminotransferase (AST) levels (Panels G and H, respectively), and carotid intima media thickness (Panel I). Weight gain was greater with pioglitazone than with placebo (Panel D). (Body-mass index was calculated at each examination with the use of height measured at baseline; as a result, the percentage change in BMI is identical to the percentage change in weight.) A total of 365 patients (placebo group, 186; pioglitazone group, 179) completed the follow-up examination at 15 to 18 months for measurement of carotid intima media thickness, and 336 patients (placebo group, 173; pioglitazone group, 163) completed the final examination for measurement of carotid intima media thickness. P values are shown for the interaction between time and study group, indicating whether the slopes differ significantly over time. 4.31±0.30 to 5.23±0.31, ). Insulin sensitivity as determined with the use of an intravenous glucose-tolerance test with frequent sampling in a subgroup of 191 patients was not altered in either group. The index of insulin secretion factored by insulin resistance, calculated on the basis of the oral glucose-tolerance test (I /ΔG Matsuda index), increased more with pioglitazone than with placebo (3.43±0.12 to 5.44±0.31 vs. 3.81±0.30 to 4.20±0.20, P<05). Similarly, the insulin secretion insulin resistance index, calculated with data from the frequentsampling intravenous glucose-tolerance test, increased more with pioglitazone than with placebo (848±65 to 1186±113 vs. 824±47 to 832±57, P<1). Carotid intima media thickening increased more slowly in the pioglitazone group than in the placebo group throughout the study (Fig. 4I). The differences between groups were 16.4% at the study midpoint and 31.5% at the end of the study (P = 47 for the overall difference between n engl j med 364;12 nejm.org march 24,
9 T h e n e w e ngl a nd j o u r na l o f m e dic i n e groups). The ratio of urinary microalbumin to creatinine was low at baseline; during the study it fell slightly and similarly in the two groups (1.85±0.2 to 1.53±0.2 mg per gram in the pioglitazone group vs. 1.47±0.3 to 1.25±0.3 mg per gram in the placebo group, P = 0.20). Table 2. Number and Type of Adverse Events.* Pioglitazone (N = 303) Placebo (N = 299) Adverse Event no. of events Cancer 3 8 Cardiovascular system Central nervous system 6 5 Death 3 1 Digestive system Edema Elective surgery Endocrine system 1 3 Immune system 2 4 Musculoskeletal system Ophthalmologic system 0 1 Respiratory system 9 6 Reproductive system 4 4 Skin 6 3 Urogenital system 5 3 Weight gain Total * For the comparison of placebo and pioglitazone regarding frequency of edema, cardiovascular events, and total events, P = 07, P = 0.80, and P = 3, respectively. The total number of adverse events excluding edema did not differ significantly between groups (P = 0.52). Edema was defined as an increase above baseline by two or more grades on one or more distinct study visits. Weight gain was defined as a gain of more than 1 kg. Adverse Events Adverse events occurred in 121 patients in the placebo group and 151 patients in the pioglitazone group (P = 3) (Table 2). Edema increased at some point during the trial in 19 patients receiving placebo (6.4%) and 39 patients receiving pioglitazone (12.9%) (P = 07). Events related to the cardiovascular system numbered 23 in the placebo group (7.7%) and 26 in the pioglitazone group (8.6%) (Table 3 in the Supplementary Appendix), with 1 case of congestive heart failure in each group (0.3%). One unexplained sudden death occurred in the placebo group, and three deaths occurred in the pioglitazone group (one unexplained sudden death, one death from biliary carcinoma, and one death from a carcinoid tumor). Nine fractures occurred in 8 of the patients receiving pioglitazone (3%) and eight fractures occurred in 7 of the patients receiving placebo (2.6%) (Table 4 in the Supplementary Appendix). All fractures were associated with trauma. Discussion Although they are considered to have prediabetes, patients in the upper third of the range for impaired glucose tolerance are at or close to the maximum level of insulin resistance and have lost approximately 80% of beta-cell function. 25,26 Histologic studies suggest that the beta-cell mass in patients with impaired fasting glucose is significantly reduced as compared with persons who have normal fasting glucose, 27 and two thirds of the patients in our study had impaired fasting glucose. Moreover, at least 10% of patients with impaired glucose tolerance have background diabetic retinopathy, 28,29 and peripheral neuropathy is common in these patients. 30 Because the characteristic pathophysiological defects of type 2 diabetes mellitus and the microvascular complications of diabetes are already evident in patients with impaired glucose tolerance, it is reasonable to consider interventions at this stage to prevent the development of overt diabetes. Lifestyle interventions effectively reduce the conversion of impaired glucose tolerance to diabetes and remain the primary approach to prevention of type 2 diabetes mellitus. However, many people remain at risk for type 2 diabetes mellitus despite attempts at lifestyle changes. 7,31,32,34 Metformin reduces the risk of conversion to type 2 diabetes mellitus by 31%, without weight gain. 7 Thiazolidinediones also effectively reduce the risk of development of type 2 diabetes mellitus in patients with impaired glucose tolerance In our study, pioglitazone decreased the rate of conversion to diabetes by 72%, a change that was slightly larger than that observed with other thiazolidinediones (52 to 62%) and lifestyle modification (58%). Although subgroup analyses were not prespecified in our study design, pioglitazone reduced the risk of conversion to diabetes in patients with isolated impaired glucose tolerance, in those with both 1112 n engl j med 364;12 nejm.org march 24, 2011
10 Pioglitazone for Diabetes Prevention in IGT impaired fasting glucose and impaired glucose tolerance, in both men and women, and in all age and weight groups. The proportion of patients who had a return to normal glucose tolerance was greater with pioglitazone than with placebo. The mean weight gain in patients treated with pioglitazone was 3.6 kg. However, the greater the weight gain, the greater the improvements in betacell function and insulin sensitivity, and thus the greater the reduction in HbA 1c. 26,35,36 The effect of weight gain on cardiovascular risk cannot be ascertained, but in the Prospective Pioglitazone Clinical Trial in Macrovascular Events (PROactive) (ClinicalTrials.gov number, NCT ), 37 a weight gain of 3.6 kg was not associated with an increase in the composite cardiovascular end point. It is not feasible to conduct studies of microvascular outcomes in patients with impaired glucose tolerance because of the large sample and long study duration required. However, if development of diabetic hyperglycemia can be delayed or prevented, it is plausible that the onset of microvascular complications might be slowed. During the course of this study, fasting and 2-hour glucose levels and HbA 1c levels were significantly lower in the pioglitazone group than in the placebo group. The small difference in levels of HbA 1c between the two groups is not surprising, given the low baseline level of HbA 1c in patients with impaired glucose tolerance. However, further glycemic separation between groups over time would presumably have a beneficial effect on microvascular disease. Pioglitazone was associated with lower diastolic blood pressure, higher levels of HDL cholesterol, and reduced rates of carotid intima media thickening, as compared with placebo. Carotid intima media thickening is highly correlated with cardiovascular events, and changes in this measure over time have predictive value beyond that of standard markers of risk. 18,38 Such results suggest that pioglitazone may provide some protection against the development of atherosclerotic cardiovascular disease, which is consistent with reports of reductions in the volume of coronary plaque 39 and in mortality, nonfatal myocardial infarction, and stroke, the secondary end points in the PROactive. 37 Loss to follow-up was relatively high in both study groups (24% in the placebo group and 30% in the pioglitazone group, not a significant difference). Since withdrawal rates and baseline characteristics were similar between groups, biased results seem unlikely. The modest difference in levels of HbA 1c between groups suggests that the reduced progression of carotid intima media thickening with pioglitazone may reflect improvements in other metabolic variables (Fig. 4). Although pioglitazone is a well-documented insulin sensitizer, insulin resistance was reduced according to the Matsuda index of insulin sensitivity measured during the oral glucose-tolerance test but not according to measurement of insulin sensitivity during the frequent-sampling intravenous glucose-tolerance test. These disparate results may partly reflect the greater variation among centers in the results of the intravenous glucose-tolerance test with frequent sampling, which is more difficult to perform. Edema and weight gain were greater with pioglitazone than with placebo, as reported previously, 8,40 and edema largely accounted for the increase in adverse events associated with pioglitazone. Physician-reported congestive heart failure developed in only one patient in each group. Although an increased incidence of fractures has been reported with the use of thiazolidinediones, in this study, the incidence was similar in both groups, and all fractures were related to trauma. In summary, treatment with pioglitazone in patients with impaired glucose tolerance reduced the risk of diabetes, although pioglitazone was associated with significant weight gain and edema. Treatment of 18 participants for 1 year prevented one case of diabetes. Use of pioglitazone improved diastolic blood pressure, HDL cholesterol levels, and serum levels of alanine aminotranferase and aspartate aminotransferase, and it slowed progression of carotid intima media thickening. The influence of these effects on long-term diabetic complications remains to be determined. Supported by Takeda Pharmaceuticals, grants from the General Clinical Research Center (GCRC) at the University of Tennessee Health Science Center (MO1-RR-00221) and the GCRC at the University of Southern California Keck School of Medicine (MO1-RR-00043), and by the Veterans Affairs institutions in Phoenix and San Diego, which contributed their resources and the use of their facilities. Dr. Banerji reports receiving consulting fees from BMS, Novartis, Boehringer Ingelheim, Sanofi-Aventis, Merck, and Roche, and lecture fees from Merck and Sanofi-Aventis; Dr. Buchanan reports receiving consulting fees and lecture fees from Takeda and reports that the University of Southern California Keck n engl j med 364;12 nejm.org march 24,
11 T h e n e w e ngl a nd j o u r na l o f m e dic i n e School of Medicine has received grant support from Takeda; Dr. DeFronzo reports receiving payments for board membership from Amylin, Takeda, ISIS, and Boehringer Ingelheim and reports that the University of Texas Health Science Center at San Antonio has received grant support from Takeda, Amylin, and Eli Lilly; Dr. Henry reports receiving consulting fees, lecture fees, and payment for expert testimony from Takeda; Dr. Musi reports receiving consulting fees from Merck, Daiichi-Sankyo, Takeda, and Novartis; Dr. Ratner reports that the Medstar Research Institute has received consulting fees from Amylin, NovoNordisk, Sanofi-Aventis, and Genentech Roche and grant support from Amylin, NovoNordisk, GlaxoSmithKline, Bayhill, Halozyme, and Integrium; Dr. Reaven reports receiving consulting fees from BMS, lecture fees from Merck, and payment for the development of educational presentations from Amylin; Dr. Reaven reports that the Carl T. Hayden Veterans Affairs Medical Center has received grant support from Amylin; and Dr. Tripathy reports receiving grant support from Takeda Pharmaceuticals. No other potential conflict of interest relevant to this article was reported. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org. We thank our nurses and other technical staff for their expert help, without whom this study would not have been possible; the 602 patients who participated in this study; and Joel Michalek, Ph.D., and Lee Ann Zarzabal, Ph.D., of the Department of Epidemiology and Biostatistics at the University of Texas Health Science Center at San Antonio for help in the initial statistical analyses. References 1. Cowie CC, Rust KF, Byrd-Holt DD, et al. Prevalence of diabetes and impaired fasting glucose in adults in the U.S. population: National Health And Nutrition Examination Survey Diabetes Care 2006;29: Diabetes programme: facts and figures. Geneva: World Health Organization, ( en.) 3. Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ 2000;321: DeFronzo RA. Banting Lecture: from the triumvirate to the ominous octet: a new paradigm for the treatment of type 2 diabetes mellitus. Diabetes 2009;58: Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HA. 10-Year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med 2008;359: Nathan DM, Cleary PA, Backlund JY, et al. Intensive diabetes treatment and cardiovascular disease in patients with type 2 diabetes. N Engl J Med 2005;353: Knowler WC, Barrett-Connor E, Fowler SE, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 2002;346: Xiang AH, Peters RK, Kjos SL, et al. Effect of pioglitazone on pancreatic betacell function and diabetes risk in Hispanic women with prior gestational diabetes. Diabetes 2006;55: Gerstein HC, Yusuf S, Bosch J, et al. Effect of rosiglitazone on the frequency of diabetes in patients with impaired glucose tolerance or impaired fasting glucose: a randomised controlled trial. Lancet 2006;368: [Erratum, Lancet 2006;368:1770.] 10. Knowler WC, Hamman RF, Edelstein SL, et al. Prevention of type 2 diabetes with troglitazone in the Diabetes Prevention Program. Diabetes 2005;54: Buchanan TA, Xiang AH, Peters RK, et al. Preservation of pancreatic beta-cell function and prevention of type 2 diabetes by pharmacological treatment of insulin resistance in high-risk Hispanic women. Diabetes 2002;51: Chiasson JL, Josse RG, Gomis R, Hanefeld M, Karasik A, Laakso M. Acarbose for prevention of type 2 diabetes mellitus: the STOP-NIDDM randomised trial. Lancet 2002;359: Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med 2009;122(3):248. e5-256.e Nissen SE, Wolski K. Effect of rosiglitazone on the risk of myocardial infarction and death from cardiovascular causes. N Engl J Med 2007;356: [Erratum, N Engl J Med 2007;357:100.] 15. American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care 2008;31:Suppl:S55-S DeFronzo RA, Banerji M, Bray GA, et al. Actos Now for the prevention of diabetes (ACT NOW) study. BMC Endocr Disord 2009;9: Edelstein SL, Knowler WC, Bain RP, et al. Predictors of progression from impaired glucose tolerance to NIDDM: an analysis of six prospective studies. Diabetes 1997;46: Hodis HN, Mack WJ, LaBree L, et al. The role of carotid arterial intima-media thickness in predicting clinical coronary events. Ann Intern Med 1998;128: Hodis HN, Mack WJ, Lobo RA, et al. Estrogen in the prevention of atherosclerosis: a randomized, double-blind, placebo-controlled trial. Ann Intern Med 2001; 135: Matsuda M, DeFronzo RA. Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes Care 1999;22: Bergman RN, Phillips LS, Cobelli C. Physiologic evaluation of factors controlling glucose tolerance in man: measurement of insulin sensitivity and beta-cell glucose sensitivity from the response to intravenous glucose. J Clin Invest 1981; 68: Abdul-Ghani MA, Jenkinson CP, Richardson DK, Tripathy D, DeFronzo RA. Insulin secretion and action in subjects with impaired fasting glucose and impaired glucose tolerance: results from the Veterans Administration Genetic Epidemiology Study. Diabetes 2006;55: Kalbfleisch J, Prentice RL. The statistical analysis of failure time data. New York: John Wiley, Lachin JM, Wei LJ. Estimators and tests in the analysis of multiple nonindependent 2 x 2 tables with partially missing observations. Biometrics 1988;44: [Erratum, Biometrics 1988;44:923.] 25. Ferrannini E, Gastaldelli A, Miyazaki Y, Matsuda M, Mari A, DeFronzo RA. Beta-cell function in subjects spanning the range from normal glucose tolerance to overt diabetes: a new analysis. J Clin Endocrinol Metab 2005;90: Gastaldelli A, Ferrannini E, Miyazaki Y, Matsuda M, Mari A, DeFronzo RA. Thiazolidinediones improve beta-cell function in type 2 diabetic patients. Am J Physiol Endocrinol Metab 2007;292:E871-E Butler AE, Janson J, Bonner-Weir S, Ritzel R, Rizza RA, Butler PC. Beta-cell deficit and increased beta-cell apoptosis in humans with type 2 diabetes. Diabetes 2003;52: Diabetes Prevention Program Research Group. The prevalence of retinopathy in impaired glucose tolerance and recent-onset diabetes in the Diabetes Prevention Program. Diabet Med 2007; 24: Cheng YJ, Gregg EW, Geiss LS, et al. Association of A1C and fasting plasma glucose levels with diabetic retinopathy prevalence in the U.S. population: implications for diabetes diagnostic thresholds. Diabetes Care 2009;32: Ziegler D, Rathmann W, Dickhaus T, Meisinger C, Mielck A. Prevalence of polyneuropathy in pre-diabetes and diabetes is associated with abdominal obesity and macroangiopathy: the MONICA/KORA Augsburg Surveys S2 and S3. Diabetes Care 2008;31: Pan XR, Li GW, Hu YH, et al. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance: the Da Qing IGT and Diabetes Study. Diabetes Care 1997;20: Li G, Zhang P, Wang J, et al. The long n engl j med 364;12 nejm.org march 24, 2011
12 Pioglitazone for Diabetes Prevention in IGT term effect of lifestyle interventions to prevent diabetes in the China Da Qing Diabetes Prevention Study: a 20-year follow-up study. Lancet 2008;371: Knowler WC, Fowler SE, Hamman RF, et al. 10-Year follow-up of diabetes incidence and weight loss in the Diabetes Prevention Program Outcomes Study. Lancet 2009;374: [Erratum, Lancet 2009;374:2054.] 34. Lindström J, Ilanne-Parikka P, Peltonen M, et al. Sustained reduction in the incidence of type 2 diabetes by lifestyle intervention: follow-up of the Finnish Diabetes Prevention Study. Lancet 2006;368: Miyazaki Y, Mahankali A, Matsuda M, et al. Improved glycemic control and enhanced insulin sensitivity in type 2 diabetic subjects treated with pioglitazone. Diabetes Care 2001;24: Miyazaki Y, De Filippis E, Bajaj M, et al. Predictors of improved glycemic control with rosiglitazone therapy in type 2 diabetic patients: a practical approach for the primary care physician. Br J Diabetes Vasc Dis 2005;5: Dormandy JA, Charbonnel B, Eckland DJ, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive Study (PROspective pioglitazone Clinical Trial In macrovascular Events): a randomised controlled trial. Lancet 2005;366: Crouse JR III. Thematic review series: patient-oriented research imaging atherosclerosis: state of the art. J Lipid Res 2006;47: Nissen SE, Nicholls SJ, Wolski K, et al. Comparison of pioglitazone vs glimepiride on progression of coronary atherosclerosis in patients with type 2 diabetes: the PERISCOPE randomized controlled trial. JAMA 2008;299: Mazzone T, Meyer PM, Feinstein SB, et al. Effect of pioglitazone compared with glimepiride on carotid intima-media thickness in type 2 diabetes: a randomized trial. JAMA 2006;296: Copyright 2011 Massachusetts Medical Society. n engl j med 364;12 nejm.org march 24,
Diabetes Incidence and Glucose Tolerance after Termination of Pioglitazone Therapy: Results from ACT NOW
 ORIGINAL ARTICLE Diabetes Incidence and Glucose Tolerance after Termination of Pioglitazone Therapy: Results from ACT NOW Devjit Tripathy, Dawn C. Schwenke, MaryAnn Banerji, George A. Bray, Thomas A. Buchanan,
ORIGINAL ARTICLE Diabetes Incidence and Glucose Tolerance after Termination of Pioglitazone Therapy: Results from ACT NOW Devjit Tripathy, Dawn C. Schwenke, MaryAnn Banerji, George A. Bray, Thomas A. Buchanan,
Bariatric Surgery versus Intensive Medical Therapy for Diabetes 3-Year Outcomes
 The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
The new england journal of medicine original article Bariatric Surgery versus Intensive Medical for Diabetes 3-Year Outcomes Philip R. Schauer, M.D., Deepak L. Bhatt, M.D., M.P.H., John P. Kirwan, Ph.D.,
The Burden of the Diabetic Heart
 The Burden of the Diabetic Heart Dr. Ghaida Kaddaha (MBBS, MRCP-UK, FRCP-london) Diabetes Unit Rashid Hospital Dubai U.A.E Risk of CVD in Diabetes Morbidity and mortality from CVD is 2-4 fold higher than
The Burden of the Diabetic Heart Dr. Ghaida Kaddaha (MBBS, MRCP-UK, FRCP-london) Diabetes Unit Rashid Hospital Dubai U.A.E Risk of CVD in Diabetes Morbidity and mortality from CVD is 2-4 fold higher than
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
Approximately 30% of adults in the US have impaired
 ORIGINAL ARTICLE Diabetes Incidence and Glucose Tolerance after Termination of Pioglitazone Therapy: Results from ACT NOW Devjit Tripathy 1, Dawn C. Schwenke 2,3, MaryAnn Banerji 4, George A. Bray 5, Thomas
ORIGINAL ARTICLE Diabetes Incidence and Glucose Tolerance after Termination of Pioglitazone Therapy: Results from ACT NOW Devjit Tripathy 1, Dawn C. Schwenke 2,3, MaryAnn Banerji 4, George A. Bray 5, Thomas
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study
 Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Clinical Trial Synopsis TL-OPI-518, NCT#
 Clinical Trial Synopsis, NCT# 00225264 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl vs Glimepiride
Clinical Trial Synopsis, NCT# 00225264 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl vs Glimepiride
Metabolic Syndrome Update The Metabolic Syndrome: Overview. Global Cardiometabolic Risk
 Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care
 Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy
 Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
Oral Hypoglycemics and Risk of Adverse Cardiac Events: A Summary of the Controversy Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 7, 2012 VanderbiltHeart.com Outline
The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population Years of Age
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population 45 74
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population 45 74
Diabetes Mellitus Type 2 Evidence-Based Drivers
 This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
Diabetes: Staying Two Steps Ahead. The prevalence of diabetes is increasing. What causes Type 2 diabetes?
 Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Why is Earlier and More Aggressive Treatment of T2 Diabetes Better?
 Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Copyright 2017 by Sea Courses Inc.
 Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Eugene Barrett M.D., Ph.D. University of Virginia 6/18/2007. Diagnosis and what is it Glucose Tolerance Categories FPG
 Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Wanner C, Inzucchi SE, Lachin JM, et al. Empagliflozin and
1/28/2014. The Metabolic Syndrome: Early History. Insulin Resistance: Early Diagnosis and Treatment to Prevent Cardiovascular Disease
 : Early Diagnosis and Treatment to Prevent Cardiovascular Disease Henry N. Ginsberg, M.D. Irving Professor of Medicine Columbia University College of Physicans and Surgeons The Metabolic Syndrome: Early
: Early Diagnosis and Treatment to Prevent Cardiovascular Disease Henry N. Ginsberg, M.D. Irving Professor of Medicine Columbia University College of Physicans and Surgeons The Metabolic Syndrome: Early
journal of medicine The new england Rosuvastatin to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Abstract
 The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
The new england journal of medicine established in 1812 november 20, 2008 vol. 359 no. 21 to Prevent Vascular Events in Men and Women with Elevated C-Reactive Protein Paul M Ridker, M.D., Eleanor Danielson,
Why Do We Care About Prediabetes?
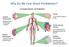 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Supplementary Online Content
 Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
In the past 6 years, several randomized controlled
 Perspectives in Diabetes (How) Can We Prevent Type 2 Diabetes? Thomas A. Buchanan In the past 6 years, several randomized controlled trials have been conducted to test the impact of behavioral and pharmacological
Perspectives in Diabetes (How) Can We Prevent Type 2 Diabetes? Thomas A. Buchanan In the past 6 years, several randomized controlled trials have been conducted to test the impact of behavioral and pharmacological
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schauer PR, Kashyap SR, Wolski K, et al. Bariatric surgery
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schauer PR, Kashyap SR, Wolski K, et al. Bariatric surgery
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
Diabetes Care Publish Ahead of Print, published online February 25, 2011
 Pathophysiology/Complications O R I G I N A L A R T I C L E Diabetes Care Publish Ahead of Print, published online February 25, 2011 The Relationship Between b-cell Function and Glycated Hemoglobin Results
Pathophysiology/Complications O R I G I N A L A R T I C L E Diabetes Care Publish Ahead of Print, published online February 25, 2011 The Relationship Between b-cell Function and Glycated Hemoglobin Results
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
American Academy of Insurance Medicine
 American Academy of Insurance Medicine October 2012 Dr. Alison Moy Liberty Mutual Dr. John Kirkpatrick Thrivent Financial for Lutherans 1 59 year old male, diagnosed with T2DM six months ago Nonsmoker
American Academy of Insurance Medicine October 2012 Dr. Alison Moy Liberty Mutual Dr. John Kirkpatrick Thrivent Financial for Lutherans 1 59 year old male, diagnosed with T2DM six months ago Nonsmoker
Cardiovascular Complications of Diabetes
 VBWG Cardiovascular Complications of Diabetes Nicola Abate, M.D., F.N.L.A. Professor and Chief Division of Endocrinology and Metabolism The University of Texas Medical Branch Galveston, Texas Coronary
VBWG Cardiovascular Complications of Diabetes Nicola Abate, M.D., F.N.L.A. Professor and Chief Division of Endocrinology and Metabolism The University of Texas Medical Branch Galveston, Texas Coronary
Discussion points. The cardiometabolic connection. Cardiometabolic Risk Management in the Primary Care Setting
 Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Session #5 Cardiometabolic Risk Management in the Primary Care Setting Sonja Reichert, MD MSc FCFP FACPM Betty Harvey, RNEC BScN MScN Amanda Mikalachki, RN BScN CDE S Discussion points Whom should we be
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Glycemic control a matter of life and death
 Glycemic control a matter of life and death Linda Garcia Mellbin MD PhD Specialist in Cardiology & Internal medicine Dep of Cardiology Karolinska University Hospital /Karolinska Institutet Mortality (%)
Glycemic control a matter of life and death Linda Garcia Mellbin MD PhD Specialist in Cardiology & Internal medicine Dep of Cardiology Karolinska University Hospital /Karolinska Institutet Mortality (%)
Cedars Sinai Diabetes. Michael A. Weber
 Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Glucose and CV disease
 Glucose and CV disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic,
Glucose and CV disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic,
Clinical Trial Synopsis TL-OPI-525, NCT#
 Clinical Trial Synopsis, NCT#00762736 Title of Study: A Phase II, Double-Blind, Randomized, Placebo-Controlled, Proof-of-Concept Study of the Efficacy, Safety, and Tolerability of Pioglitazone HCl (ACTOS
Clinical Trial Synopsis, NCT#00762736 Title of Study: A Phase II, Double-Blind, Randomized, Placebo-Controlled, Proof-of-Concept Study of the Efficacy, Safety, and Tolerability of Pioglitazone HCl (ACTOS
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS
 FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS
 IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
IMPROVED DIAGNOSIS OF TYPE 2 DIABETES AND TAILORING MEDICATIONS Dr Bidhu Mohapatra, MBBS, MD, FRACP Consultant Physician Endocrinology and General Medicine Introduction 382 million people affected by diabetes
Clinical Trial Synopsis TL-OPI-516, NCT#
 Clinical Trial Synopsis, NCT#00225277 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl Versus
Clinical Trial Synopsis, NCT#00225277 Title of Study: A Double-Blind, Randomized, Comparator-Controlled Study in Subjects With Type 2 Diabetes Mellitus Comparing the Effects of Pioglitazone HCl Versus
Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset Type 2 Diabetes
 ORIGINAL ARTICLE korean j intern med 2012;27:66-71 pissn 1226-3303 eissn 2005-6648 Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset
ORIGINAL ARTICLE korean j intern med 2012;27:66-71 pissn 1226-3303 eissn 2005-6648 Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset
What s New. in Clinical Research
 What s New in Clinical Research This new department features articles discussing recent developments in drug therapy, as well as review articles on specific drug therapies or disease states. Articles will
What s New in Clinical Research This new department features articles discussing recent developments in drug therapy, as well as review articles on specific drug therapies or disease states. Articles will
Diabetes and Cardiovascular Risks in the Polycystic Ovary Syndrome
 Diabetes and Cardiovascular Risks in the Polycystic Ovary Syndrome John E. Nestler, M.D. William Branch Porter Professor of Medicine Chair, Department of Internal Medicine Virginia Commonwealth University
Diabetes and Cardiovascular Risks in the Polycystic Ovary Syndrome John E. Nestler, M.D. William Branch Porter Professor of Medicine Chair, Department of Internal Medicine Virginia Commonwealth University
Diabetes Overview. How Food is Digested
 Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Goals for Medical Treatment in Obesity and Prediabetes: Improving Outcomes
 Goals for Medical Treatment in Obesity and Prediabetes: Improving Outcomes Leigh Perreault, MD Associate Professor of Medicine Endocrinology, Metabolism and Diabetes University of Colorado Anschutz Medical
Goals for Medical Treatment in Obesity and Prediabetes: Improving Outcomes Leigh Perreault, MD Associate Professor of Medicine Endocrinology, Metabolism and Diabetes University of Colorado Anschutz Medical
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Serra AL, Poster D, Kistler AD, et al. Sirolimus and kidney
The promise of the thiazolidinediones in the management of type 2 diabetes-associated cardiovascular disease
 The promise of the thiazolidinediones in the management of type 2 diabetes-associated cardiovascular disease Steve Smith, Group Director Scientific Affairs, Diabetes & Metabolism GlaxoSmithKline R & D
The promise of the thiazolidinediones in the management of type 2 diabetes-associated cardiovascular disease Steve Smith, Group Director Scientific Affairs, Diabetes & Metabolism GlaxoSmithKline R & D
A Fork in the Road: Navigating Through New Terrain
 A Fork in the Road: Navigating Through New Terrain Carol Hatch Wysham, MD Clinical Associate Professor of Medicine University of Washington School of Medicine Section Head, Rockwood Center for Diabetes
A Fork in the Road: Navigating Through New Terrain Carol Hatch Wysham, MD Clinical Associate Professor of Medicine University of Washington School of Medicine Section Head, Rockwood Center for Diabetes
TYPE 2 DIABETES MELLITUS (T2DM) is a heterogeneous
 0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(6):2846 2851 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032044 Pharmacological Treatment
0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(6):2846 2851 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032044 Pharmacological Treatment
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus. Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre
 Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Diabetes: Definition Pathophysiology Treatment Goals. By Scott Magee, MD, FACE
 Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes
 Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
Obesity, Insulin Resistance, Metabolic Syndrome, and the Natural History of Type 2 Diabetes Genetics, environment, and lifestyle (obesity, inactivity, poor diet) Impaired fasting glucose Decreased β-cell
T he prevalence of type 2 diabetes
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
Ischemic Heart and Cerebrovascular Disease. Harold E. Lebovitz, MD, FACE Kathmandu November 2010
 Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Ischemic Heart and Cerebrovascular Disease Harold E. Lebovitz, MD, FACE Kathmandu November 2010 Relationships Between Diabetes and Ischemic Heart Disease Risk of Cardiovascular Disease in Different Categories
Implementing Type 2 Diabetes Prevention Programmes
 Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
Implementing Type 2 Diabetes Prevention Programmes Jaakko Tuomilehto Department of Public Health University of Helsinki Helsinki, Finland FIN-D2D Survey 2004 Prevalence of previously diagnosed and screen-detected
Update on Cardiovascular Outcome Trials in Diabetes. Rury R. Holman, FMedSci NIHR Senior Investigator 11 th February 2013
 Update on Cardiovascular Outcome Trials in Diabetes Rury R. Holman, FMedSci NIHR Senior Investigator 11 th February 2013 Residual Vascular Risk in People with Diabetes 2 Analyses based on 530,083 participants
Update on Cardiovascular Outcome Trials in Diabetes Rury R. Holman, FMedSci NIHR Senior Investigator 11 th February 2013 Residual Vascular Risk in People with Diabetes 2 Analyses based on 530,083 participants
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The Metabolic Syndrome: Is It A Valid Concept? YES
 The Metabolic Syndrome: Is It A Valid Concept? YES Congress on Diabetes and Cardiometabolic Health Boston, MA April 23, 2013 Edward S Horton, MD Joslin Diabetes Center Harvard Medical School Boston, MA
The Metabolic Syndrome: Is It A Valid Concept? YES Congress on Diabetes and Cardiometabolic Health Boston, MA April 23, 2013 Edward S Horton, MD Joslin Diabetes Center Harvard Medical School Boston, MA
DIABETES AND METABOLIC SYNDROME
 TRIALS NUMBER OF PARTICIPANTS NUMBER OF WOMEN PERCENTAGE OF WOMEN MEAN AGE MEAN - (YEARS) TRIALS WITH ANALYSIS BY GENDER N, (%) 48,508 20,091 41.4% 61.1 4.3 4/7 (57.1%) HR PROactive (Dormandy et al 61
TRIALS NUMBER OF PARTICIPANTS NUMBER OF WOMEN PERCENTAGE OF WOMEN MEAN AGE MEAN - (YEARS) TRIALS WITH ANALYSIS BY GENDER N, (%) 48,508 20,091 41.4% 61.1 4.3 4/7 (57.1%) HR PROactive (Dormandy et al 61
Update on CVD and Microvascular Complications in T2D
 Update on CVD and Microvascular Complications in T2D Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine
Update on CVD and Microvascular Complications in T2D Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine
The American Diabetes Association estimates
 DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
Effects of Intensive Blood-Pressure Control in Type 2 Diabetes Mellitus
 original article Effects of Blood-Pressure Control in Type 2 Diabetes Mellitus The ACCORD Study Group* ABSTRACT Background There is no evidence from randomized trials to support a strategy of lowering
original article Effects of Blood-Pressure Control in Type 2 Diabetes Mellitus The ACCORD Study Group* ABSTRACT Background There is no evidence from randomized trials to support a strategy of lowering
Glucose Challenge Test as a Predictor of Type 2 Diabetes
 Georgia State University ScholarWorks @ Georgia State University Public Health Theses School of Public Health Fall 1-8-2016 Glucose Challenge Test as a Predictor of Type 2 Diabetes Rahsaan Overton Follow
Georgia State University ScholarWorks @ Georgia State University Public Health Theses School of Public Health Fall 1-8-2016 Glucose Challenge Test as a Predictor of Type 2 Diabetes Rahsaan Overton Follow
Prevention of diabetes in the modern era of affluent society and economic constraints
 Prevention of diabetes in the modern era of affluent society and economic constraints KONSTANTINOS MAKRILAKIS, MD, MPH, PhD ASSOCIATE PROFESSOR IN INTERNAL MEDICINE NATIONAL AND KAPODISTRIAN UNIVERSITY
Prevention of diabetes in the modern era of affluent society and economic constraints KONSTANTINOS MAKRILAKIS, MD, MPH, PhD ASSOCIATE PROFESSOR IN INTERNAL MEDICINE NATIONAL AND KAPODISTRIAN UNIVERSITY
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and
 This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
This article appeared in a journal published by Elsevier. The attached copy is furnished to the author for internal non-commercial research and education use, including for instruction at the authors institution
Diabetes Mellitus: Implications of New Clinical Trials and New Medications
 Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Flaws, Bias, Misinterpretation and Fraud in Randomized Clinical Trials
 Flaws, Bias, Misinterpretation and Fraud in Randomized Clinical Trials Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical companies
Flaws, Bias, Misinterpretation and Fraud in Randomized Clinical Trials Steven E. Nissen MD Chairman, Department of Cardiovascular Medicine Cleveland Clinic Disclosure Consulting: Many pharmaceutical companies
Insulin sensitivity, and b-cell function in relation to hemoglobin A1C
 Nutrition, Metabolism & Cardiovascular Diseases (2014) 24, 27e33 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/nmcd Insulin sensitivity, and b-cell function in relation
Nutrition, Metabolism & Cardiovascular Diseases (2014) 24, 27e33 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/nmcd Insulin sensitivity, and b-cell function in relation
Diabetes. Health Care Disparities: Medical Evidence. A Constellation of Complications. Every 24 hours.
 Health Care Disparities: Medical Evidence Diabetes Effects 2.8 Million People in US 7% of the US Population Sixth Leading Cause of Death Kenneth J. Steier, DO, MBA, MPH, MHA, MGH Dean of Clinical Education
Health Care Disparities: Medical Evidence Diabetes Effects 2.8 Million People in US 7% of the US Population Sixth Leading Cause of Death Kenneth J. Steier, DO, MBA, MPH, MHA, MGH Dean of Clinical Education
Diabete: terapia nei pazienti a rischio cardiovascolare
 Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Diabete: terapia nei pazienti a rischio cardiovascolare Giorgio Sesti Università Magna Graecia di Catanzaro Cardiovascular mortality in relation to diabetes mellitus and a prior MI: A Danish Population
Association between Raised Blood Pressure and Dysglycemia in Hong Kong Chinese
 Diabetes Care Publish Ahead of Print, published online June 12, 2008 Raised Blood Pressure and Dysglycemia Association between Raised Blood Pressure and Dysglycemia in Hong Kong Chinese Bernard My Cheung,
Diabetes Care Publish Ahead of Print, published online June 12, 2008 Raised Blood Pressure and Dysglycemia Association between Raised Blood Pressure and Dysglycemia in Hong Kong Chinese Bernard My Cheung,
Journal of the American College of Cardiology Vol. 48, No. 2, by the American College of Cardiology Foundation ISSN /06/$32.
 Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.03.043
Journal of the American College of Cardiology Vol. 48, No. 2, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.03.043
Meta-analysis: analysis:
 1 Diabetes and TZDs: Risk Factors for Fracture Ann Schwartz, PhD Dept. of Epidemiology and Biostatistics University of California San Francisco July 2010 Osteoporosis CME Presenter Disclosure Information
1 Diabetes and TZDs: Risk Factors for Fracture Ann Schwartz, PhD Dept. of Epidemiology and Biostatistics University of California San Francisco July 2010 Osteoporosis CME Presenter Disclosure Information
The Diabetes Link to Heart Disease
 The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
The Diabetes Link to Heart Disease Anthony Abe DeSantis, MD September 18, 2015 University of WA Division of Metabolism, Endocrinology and Nutrition Oswald Toosweet Case #1 68 yo M with T2DM Diagnosed DM
Basal Insulin and Cardiovascular and Other Outcomes in Dysglycemia
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Basal Insulin and Cardiovascular and Other Outcomes in Dysglycemia The ORIGIN Trial Investigators* A bs tr ac t Background The provision
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Basal Insulin and Cardiovascular and Other Outcomes in Dysglycemia The ORIGIN Trial Investigators* A bs tr ac t Background The provision
A46-yr-old female is referred to you for an abnormal fasting
 SPECIAL FEATURE Approach to the Patient Approach to the Patient with Prediabetes Vanita R. Aroda and Robert Ratner Med Star Clinical Research Center, Washington, D.C. 20003 Prediabetes consists of impaired
SPECIAL FEATURE Approach to the Patient Approach to the Patient with Prediabetes Vanita R. Aroda and Robert Ratner Med Star Clinical Research Center, Washington, D.C. 20003 Prediabetes consists of impaired
Choosing a Diabetes Strategy Where to Start and Where to Go
 Choosing a Diabetes Strategy Where to Start and Where to Go Erin Keely, MD, FRCPC; and Sharon Brez, RN, BScN, MA(Ed), CDE As presented at the University of Ottawa's 52nd Annual Refresher Course for Family
Choosing a Diabetes Strategy Where to Start and Where to Go Erin Keely, MD, FRCPC; and Sharon Brez, RN, BScN, MA(Ed), CDE As presented at the University of Ottawa's 52nd Annual Refresher Course for Family
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes
 A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
A factorial randomized trial of blood pressure lowering and intensive glucose control in 11,140 patients with type 2 diabetes Hypotheses: Among individuals with type 2 diabetes, the risks of major microvascular
Total risk management of Cardiovascular diseases Nobuhiro Yamada
 Nobuhiro Yamada The worldwide burden of cardiovascular diseases (WHO) To prevent cardiovascular diseases Beyond LDL Multiple risk factors With common molecular basis The Current Burden of CVD CVD is responsible
Nobuhiro Yamada The worldwide burden of cardiovascular diseases (WHO) To prevent cardiovascular diseases Beyond LDL Multiple risk factors With common molecular basis The Current Burden of CVD CVD is responsible
Strategies for the prevention of type 2 diabetes and cardiovascular disease
 European Heart Journal Supplements (2005) 7 (Supplement D), D18 D22 doi:10.1093/eurheartj/sui025 Strategies for the prevention of type 2 diabetes and cardiovascular disease Jaakko Tuomilehto 1,2,3 *, Jaana
European Heart Journal Supplements (2005) 7 (Supplement D), D18 D22 doi:10.1093/eurheartj/sui025 Strategies for the prevention of type 2 diabetes and cardiovascular disease Jaakko Tuomilehto 1,2,3 *, Jaana
Type 2 Diabetes in Adolescents
 Type 2 Diabetes in Adolescents Disclosures Paid consultant, Eli Lilly, Inc, Pediatric Type 2 Diabetes Clinical Trials Outline The burden of diabetes Treatment and Prevention Youth Diabetes Prevention Clinic
Type 2 Diabetes in Adolescents Disclosures Paid consultant, Eli Lilly, Inc, Pediatric Type 2 Diabetes Clinical Trials Outline The burden of diabetes Treatment and Prevention Youth Diabetes Prevention Clinic
Comparative Effectiveness and Safety of Diabetes Medications for Adults with Type 2 Diabetes
 Draft Comparative Effectiveness Review Comparative Effectiveness and Safety of Diabetes Medications for Adults with Type Diabetes Prepared for: Agency for Healthcare Research and Quality U.S. Department
Draft Comparative Effectiveness Review Comparative Effectiveness and Safety of Diabetes Medications for Adults with Type Diabetes Prepared for: Agency for Healthcare Research and Quality U.S. Department
Non alcoholic fatty liver disease and atherosclerosis Raul Santos, MD
 Non alcoholic fatty liver disease and atherosclerosis Raul Santos, MD Sao Paulo Medical School Hospital Sao Paulo, Brazil Disclosure Honoraria received for consult and/or speaker : Astra Zeneca, Amgen,
Non alcoholic fatty liver disease and atherosclerosis Raul Santos, MD Sao Paulo Medical School Hospital Sao Paulo, Brazil Disclosure Honoraria received for consult and/or speaker : Astra Zeneca, Amgen,
Glucose Control and Prevention of Cardiovascular Disease
 Glucose Control and Prevention of Cardiovascular Disease Dr Peter A Senior BMedSci MBBS PhD FRCP(E) Associate Professor, Director Division of Endocrinology, University of Alberta Diabetes Update+, March
Glucose Control and Prevention of Cardiovascular Disease Dr Peter A Senior BMedSci MBBS PhD FRCP(E) Associate Professor, Director Division of Endocrinology, University of Alberta Diabetes Update+, March
ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES
 ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES Pr. Michel KOMAJDA Institute of Cardiology - IHU ICAN Pitie Salpetriere Hospital - University Pierre and Marie Curie, Paris (France) DEFINITION A
ESC GUIDELINES ON DIABETES AND CARDIOVASCULAR DISEASES Pr. Michel KOMAJDA Institute of Cardiology - IHU ICAN Pitie Salpetriere Hospital - University Pierre and Marie Curie, Paris (France) DEFINITION A
Long-Term Effects of Intensive Glucose Lowering on Cardiovascular Outcomes
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Long-Term Effects of Glucose Lowering on Cardiovascular Outcomes The ACCORD Study Group* A bs tr ac t The members of the writing group
T h e n e w e ngl a nd j o u r na l o f m e dic i n e original article Long-Term Effects of Glucose Lowering on Cardiovascular Outcomes The ACCORD Study Group* A bs tr ac t The members of the writing group
Old oral antidiabetic agents in the armamentarium of diabetes mellitus treatment: Safety and efficacy
 Old oral antidiabetic agents in the armamentarium of diabetes mellitus treatment: Safety and efficacy Melpomeni Peppa Assistant Professor of Endocrinology 2 nd Dept of Internal Medicine-Propaedeutic, Athens
Old oral antidiabetic agents in the armamentarium of diabetes mellitus treatment: Safety and efficacy Melpomeni Peppa Assistant Professor of Endocrinology 2 nd Dept of Internal Medicine-Propaedeutic, Athens
The term impaired glucose tolerance
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Risk of Progression to Type 2 Diabetes Based on Relationship Between Postload Plasma Glucose and Fasting Plasma Glucose MUHAMMAD A. ABDUL-GHANI,
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Risk of Progression to Type 2 Diabetes Based on Relationship Between Postload Plasma Glucose and Fasting Plasma Glucose MUHAMMAD A. ABDUL-GHANI,
See accompanying articles, pp. 5, 8, 9, 17, 24, 31, and 44.
 Diabetes Care Volume 37, January 2014 39 Update on Cardiovascular Outcomes at 30 Years of the Diabetes Control and Complications Trial/Epidemiology Complications Study John M. Lachin, 1 Trevor J. Orchard,
Diabetes Care Volume 37, January 2014 39 Update on Cardiovascular Outcomes at 30 Years of the Diabetes Control and Complications Trial/Epidemiology Complications Study John M. Lachin, 1 Trevor J. Orchard,
Application of New Cholesterol Guidelines to a Population-Based Sample
 The new england journal of medicine original article Application of New Cholesterol to a Population-Based Sample Michael J. Pencina, Ph.D., Ann Marie Navar-Boggan, M.D., Ph.D., Ralph B. D Agostino, Sr.,
The new england journal of medicine original article Application of New Cholesterol to a Population-Based Sample Michael J. Pencina, Ph.D., Ann Marie Navar-Boggan, M.D., Ph.D., Ralph B. D Agostino, Sr.,
Early Intervention to Prevent and Treat Type 2 Diabetes
 endocrinology Board Review Manual Statement of Editorial Purpose The Hospital Physician Endocrinology Board Review Manual is a study guide for fellows and practicing physicians preparing for board examinations
endocrinology Board Review Manual Statement of Editorial Purpose The Hospital Physician Endocrinology Board Review Manual is a study guide for fellows and practicing physicians preparing for board examinations
CONTROLLO GLICEMICO E RISCHIO CARDIOVASCOLARE. AGOSTINO CONSOLI DMSI - Università d Annunzio CHIETI ITALY. sul Paziente ad alto rischio CV*
 CONTROLLO GLICEMICO E RISCHIO CARDIOVASCOLARE AGOSTINO CONSOLI DMSI - Università d Annunzio CHIETI ITALY sul Paziente ad alto rischio CV* Does reducing hyperglycemia protect against cardiovascular risk?
CONTROLLO GLICEMICO E RISCHIO CARDIOVASCOLARE AGOSTINO CONSOLI DMSI - Università d Annunzio CHIETI ITALY sul Paziente ad alto rischio CV* Does reducing hyperglycemia protect against cardiovascular risk?
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden
 Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Optimizing risk assessment of total cardiovascular risk What are the tools? Lars Rydén Professor Karolinska Institutet Stockholm, Sweden Cardiovascular Disease Prevention (CVD) Three Strategies for CVD
Prevention of diabetes and its associated
 Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Identifying Individuals at High Risk for Diabetes The Atherosclerosis Risk in Communities study MARIA INÊS SCHMIDT,
Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Identifying Individuals at High Risk for Diabetes The Atherosclerosis Risk in Communities study MARIA INÊS SCHMIDT,
LATE BREAKING STUDIES IN DM AND CAD. Will this change the guidelines?
 LATE BREAKING STUDIES IN DM AND CAD Will this change the guidelines? Objectives 1. Discuss current guidelines for prevention of CHD in diabetes. 2. Discuss the FDA Guidance for Industry regarding evaluating
LATE BREAKING STUDIES IN DM AND CAD Will this change the guidelines? Objectives 1. Discuss current guidelines for prevention of CHD in diabetes. 2. Discuss the FDA Guidance for Industry regarding evaluating
Predictability of 1-h postload plasma glucose concentration: A 10-year retrospective cohort study
 Predictability of 1-h postload plasma glucose concentration: A 10-year retrospective cohort study Lifen Kuang, Zhimin Huang, Zhenzhen Hong, Ailing Chen, Yanbing Li* ORIGINAL ARTICLE Department of Endocrinology
Predictability of 1-h postload plasma glucose concentration: A 10-year retrospective cohort study Lifen Kuang, Zhimin Huang, Zhenzhen Hong, Ailing Chen, Yanbing Li* ORIGINAL ARTICLE Department of Endocrinology
How to Reduce CVD Complications in Diabetes?
 How to Reduce CVD Complications in Diabetes? Chaicharn Deerochanawong M.D. Diabetes and Endocrinology Unit Department of Medicine Rajavithi Hospital, Ministry of Public Health Framingham Heart Study 30-Year
How to Reduce CVD Complications in Diabetes? Chaicharn Deerochanawong M.D. Diabetes and Endocrinology Unit Department of Medicine Rajavithi Hospital, Ministry of Public Health Framingham Heart Study 30-Year
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes!
 Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Prediabetes: You Can Help Your Patients Exit the Express Lane to Diabetes! Jaini Patel, PharmD, BCACP Assistant Professor of Pharmacy Practice Midwestern University Chicago College of Pharmacy Kathleen
Effects of Medical Therapies on Retinopathy Progression in Type 2 Diabetes
 The new england journal of medicine original article Effects of Medical Therapies on Retinopathy Progression in Type 2 Diabetes The ACCORD Study Group and ACCORD Eye Study Group* Abstract Background We
The new england journal of medicine original article Effects of Medical Therapies on Retinopathy Progression in Type 2 Diabetes The ACCORD Study Group and ACCORD Eye Study Group* Abstract Background We
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Individual Study Table Referring to Item of the Submission: Volume: Page:
 2.0 Synopsis Name of Company: Abbott Laboratories Name of Study Drug: Meridia Name of Active Ingredient: Sibutramine hydrochloride monohydrate Individual Study Table Referring to Item of the Submission:
2.0 Synopsis Name of Company: Abbott Laboratories Name of Study Drug: Meridia Name of Active Ingredient: Sibutramine hydrochloride monohydrate Individual Study Table Referring to Item of the Submission:
Welcome and Introduction
 Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Diabetes new challenges, new agents, new order
 Diabetes new challenges, new agents, new order Ken Earle St Georges University Hospitals NHS Foundation Trust Overview Cardiovascular disease unmet needs Treating evident and residual risk Integrating
Diabetes new challenges, new agents, new order Ken Earle St Georges University Hospitals NHS Foundation Trust Overview Cardiovascular disease unmet needs Treating evident and residual risk Integrating
