Effects of intraduodenal lipid and protein on gut motility and hormone release, glycemia, appetite, and energy intake in lean men 1 3
|
|
|
- Berniece Weaver
- 6 years ago
- Views:
Transcription
1 Effects of intraduodenal lipid and protein on gut motility and hormone release, glycemia, appetite, and energy intake in lean men 1 3 Amy T Ryan, Natalie D Luscombe-Marsh, Alexander A Saies, Tanya J Little, Scott Standfield, Michael Horowitz, and Christine Feinle-Bisset ABSTRACT Background: Intraduodenal lipid modulates gastrointestinal motility and hormone release and suppresses energy intake (EI) more than does intraduodenal glucose. Oral protein is the most satiating macronutrient and modulates postprandial glycemia; the comparative effects of intraduodenal protein and lipid and their combined effects are unclear. Objective: We investigated the effects of intraduodenal protein and lipid, alone or in combination, on antropyloroduodenal motility, gastrointestinal hormone release, glycemia, and EI. Design: Twenty lean men were studied on 5 randomized, doubleblind occasions. Antropyloroduodenal motility, cholecystokinin, glucagon-like peptide-1 (GLP-1), insulin, glucagon, blood glucose, appetite, and nausea were measured during 90-min isocaloric (3 kcal/min) intraduodenal infusions of lipid [pure lipid condition (L3)], protein [pure protein condition (P3)], a 2:1 combination of lipid and protein [2:1 lipid:protein condition (L2P1)], a 1:2 combination of lipid and protein [1:2 lipid:protein condition (L1P2)], or a control. Immediately after the infusion, EI from a buffet lunch was quantified. Results: In comparison with the control, all nutrient infusions suppressed antral and duodenal and stimulated pyloric pressures (P, 0.05). Cholecystokinin and GLP-1 release and pyloric stimulation were lipid-load dependent (r $ 0.39, P, 0.01), insulin and glucagon releases were protein-load dependent (r = 0.83, P, 0.001), and normoglycemia was maintained. L3 but not P3 increased nausea (P, 0.05). Compared with the control, L3 and P3 but not L2P1 or L1P2 suppressed EI (P, 0.05) without major effects on appetite. Conclusions: In lean men, despite differing effects on gut function, intraduodenal lipid and protein produce comparable reductions in energy intake. The effects of lipid may be a result of nausea. Protein also regulates blood glucose by stimulating insulin and glucagon. In contrast, at the loads selected, lipid:protein combinations did not suppress energy intake, suggesting that a threshold load is required to elicit effects. This trial was registered at Australia and New Zealand Clinical Trial Registry ( as Am J Clin Nutr 2013;98: INTRODUCTION An understanding of gastrointestinal sensing of nutrients and its role in the regulation of food intake has major implications for a number of disorders, which are associated with altered gastrointestinal responses to nutrients (1 5). For example, in obese humans, oral and intraduodenal responses to fat are diminished in comparison with lean subjects (1, 2), whereas the satiating effect of oral protein persists (2). Elderly subjects have higher plasma cholecystokinin concentrations, both fasting and in response to intraduodenal lipid, and are less hungry than healthy young subjects (3, 4). In patients with functional dyspepsia, the oral ingestion of a fatty meal or intraduodenal infusion of a triglyceride emulsion induces much greater upper gastrointestinal symptoms than in healthy subjects and compared with carbohydrate (6). The characterization of gastrointestinal effects of nutrients and their relation with the regulation of energy intake, blood glucose, and gastrointestinal symptoms will be an important step to understand the role of dietary nutrients, as well as changes in the diet, for these disorders. In healthy humans, dietary macronutrients modulate gastrointestinal motor and hormone function in a load-dependent manner (7 9). The stimulation of pyloric motility and release of gut hormones, including cholecystokinin (7, 10) and glucagon-like peptide-1 (GLP-1) 4 (7, 8), slow gastric emptying (11), modulate glycemia (12), and suppress energy intake (7 9, 13). Pyloric pressures and plasma cholecystokinin are independent determinants of acute energy intake in healthy individuals in response to intraduodenal lipid and carbohydrate (14). Although intraduodenal whey protein, infused at loads reflecting average gastric emptying of nutrients (0.5 4 kcal/min) suppressed energy intake 1 From the University of Adelaide Discipline of Medicine and National Health and Medical Research Council of Australia Centre of Research Excellence in Translating Nutritional Science to Good Health, University of Adelaide, Adelaide, Australia. 2 Supported by a postgraduate scholarship provided by the Faculty of Health Sciences, University of Adelaide (to ATR), a National Health and Medical Research Council of Australia (NHMRC) New Investigator Project Grant (grant , ; to NDL-M), an NHMRC Career Development Fellowship (grant , ; to TJL), an NHMRC Senior Research Fellowship (grant , ; to CF-B), and an NHMRC Project Grant (grant , ; to CF-B). 3 Address correspondence to C Feinle-Bisset, University of Adelaide Discipline of Medicine, Royal Adelaide Hospital, Adelaide SA 5000, Australia. christine.feinle@adelaide.edu.au. 4 Abbreviations used: BPP, basal pyloric pressure; C, control condition; GIP, glucose-dependent insulinotropic peptide; GLP-1, glucagon-like peptide-1; IPPW, isolated pyloric pressure wave; L-Trp, L-tryptophan; L1P2, 1:2 lipid:protein condition; L2P1, 2:1 lipid:protein condition; L3, pure lipid condition; MI, motility index; N+, subjects who experienced nausea; N2, subjects who did not experience nausea; PW, pressure wave; P3, pure protein condition; VAS, visual analog scale. Received February 27, Accepted for publication May 10, First published online June 26, 2013; doi: /ajcn Am J Clin Nutr 2013;98: Printed in USA. Ó 2013 American Society for Nutrition
2 LIPID, PROTEIN, GUT FUNCTION, AND ENERGY INTAKE 301 (7), its effects on gastrointestinal motility and hormone release seemed weaker than with lipid (9), and thus, effects of whey on energy intake may be mediated by alternative mechanisms. Whey protein also stimulates insulin release and reduces postprandial glycemic excursions in both healthy individuals (15) and type 2 patients with diabetes (16, 17). Although the mechanisms that underlie the effects of protein on glycemia are not fully understood, the effect is at least in part because of the release of the incretin hormones, GLP-1, and glucose-dependent insulinotropic peptide (GIP) and the stimulation of pancreatic b cells by circulating amino acids (15, 18). Furthermore, cholecystokinin (19) and GLP-1 (20) slow gastric emptying, which is a major determinant of postprandial glycemia (12, 21). Therefore, we wanted to compare the effects of intraduodenal lipid and protein and determine whether their combined delivery, which, stimulates the different mechanisms through which they act concurrently, might more potently suppress energy intake while benefiting blood glucose. Thus, we evaluated the effects of isocaloric, intraduodenal infusions of protein and lipid, alone and in combination, on antropyloroduodenal motility, gastrointestinal hormones related to appetite regulation and glycemic control, and energy intake in healthy lean men. We hypothesized that lipid, compared with protein, would more potently 1) stimulate pyloric and suppress antral and duodenal pressures and 2) stimulate cholecystokinin and GLP-1 release, 3) protein, compared with lipid, would more potently stimulate insulin and glucagon release and modulate blood glucose, and 4) combinations of lipid and protein would exert additive effects on these variables. SUBJECTS AND METHODS Subjects Twenty healthy, lean men [mean 6 SEM age: y (range: y); BMI (in kg/m 2 ): (range ); waist circumference: cm) participated in the study (see Supplemental Figure 1 under Supplemental data in the online issue). The number of subjects was based on power calculations on the basis of our previous studies and indicated that n =20 subjects would allow the detection of a 150-kcal difference in energy intake with b = 0.8 and a = 0.05 (9, 22). Participants were recruited from an existing pool of volunteers or through an advertisement in local newspapers. All subjects had been weight stable (#5% of their screening weight) for $3 mo before the study and were unrestrained eaters [score,12 on the eating restraint component of the Three-Factor Eating Questionnaire (23)]. No subject currently smoked, consumed.20 g alcohol/wk, had a history of gastrointestinal symptoms, or was taking medication known to affect energy intake, appetite, or gastrointestinal function. The Royal Adelaide Hospital Research Ethics Committee approved the study protocol (22 October 2009), and all subjects provided written informed consent before their inclusion. Once subjects were enrolled in the study, they were allocated a random sequence of all 5 infusions generated by using the #RAN function in the Microsoft Excel program (Microsoft Corp) by a research officer. Subject and investigators who assessed outcomes (ATR and AAS) were blinded to the random allocation sequence. This trial was registered at Australia and New Zealand Clinical Trial Registry ( anzctr.org.au) as Study outline The study compared the effects of 1) 3-kcal lipid/min [pure lipid condition (L3)], 2) 2-kcal lipid/min + 1-kcal protein/min [2:1 lipid:protein condition (L2P1)], 3) 1-kcal lipid/min + 2-kcal protein/min [1:2 lipid:protein condition (L1P2)], 4) 3-kcal protein/min [pure protein condition (P3)], and 5) a saline control [control condition (C)] infused intraduodenally for 90 min on antropyloroduodenal motility, gastrointestinal hormone release, serum insulin, plasma glucagon, blood glucose, appetite, and energy intakes. Intraduodenal nutrient infusions We used direct intraduodenal infusion of nutrients in our study. During the oral ingestion of meals, the delivery of nutrients to the small intestine (ie, where receptors that sense nutrients and initiate feedback responses are concentrated) is dependent on the rate of gastric emptying. Because there is substantial interindividual and intraindividual variation in rates of gastric emptying (24) and, thus, varying influences from gastric distension (4), the intraduodenal infusion of nutrients bypasses the stomach, while allowing for the delivery of nutrients to the small intestinal lumen at standardized rates that reflect average rates of gastric emptying. In addition, intraduodenal nutrient delivery allowed us to exclude any orosensory influences (including those from taste, smell, and texture) of foods. Although the study paradigm did not directly reflect all influences that occurred during oral the meal ingestion, it enabled us to study the small intestinal contributions in detail, which was the primary focus of this study. Intralipid (a soy-based emulsion consisting primarily of linoleic, oleic, and palmitic acids resembling fatty acids that are common in the diet; 20%, 300 mosmol/l; energy density: 2 kcal/ml; Baxter Healthcare) was used as the lipid source, and whey protein [hydrolyzed whey protein isolate DH17 Ultra (18.5% hydrolysate), MyoPure; Muscle Brand Pty Ltd) was used as the protein source. As a component of dairy products, whey is also common in the diet and has generally been shown to be the most satiating protein source when consumed orally (25, 26). We have used both Intralipid and whey protein extensively in our previous studies to evaluate the role of macronutrients on gastrointestinal function and appetite (7, 9). On the morning of each study day isoosmotic (480 mosm/l) infusion solutions were prepared in 420-mL batches by a research officer who was not involved in either the analysis or interpretation of data. Protein stock solutions were made by dissolving 28 g whey protein hydrolysate powder (to contribute 1 kcal/min of protein for L2P1 infusion) or 56 g whey protein hydrolysate powder (to contribute 2 kcal/min of protein for L1P2 infusion) in distilled water to a volume of 140 or 280 ml, respectively. Solutions of 1.67%, 1.7%, and 1.8% NaCl were prepared by dissolving 6.9, 7.14, or 7.56 g NaCl in 420 ml distilled water, respectively. The L3 solution consisted of ml Intralipid and ml 1.67% NaCl solution. To make up the mixednutrient solutions (L2P1 and L1P2), 105 ml Intralipid and 87.5 ml 1.8% NaCl solution were added to the 1 kcal/min of protein stock solution, and 52.5 ml Intralipid and 175 ml 1.7% NaCl solution were added to the 2 kcal/min of protein stock solution. The P3 solution consisted of 84 g protein hydrolysate powder in 420 ml distilled water, and the C consisted of 420 ml 1.4% NaCl solution (6 g NaCl in 420 ml distilled water). All solutions were
3 302 RYAN ET AL administered at a rate of 4 ml/min, delivering 360 ml over 90 min, and nutrient-containing infusions provided a total of 270 kcal. The infusion apparatus was covered at all times, and thus, the investigators who performed the studies (ATR and AAS) and subjects were blinded to the treatment. Protocol Each subject was studied on 5 occasions, each of which was separated by 3 10 d, in a double-blind, randomized, crossover design. Subjects were provided with a standardized meal (beef lasagna; energy content: 519 kcal; McCain Foods) to consume at 1900 the day before each study. Thereafter, subjects were asked to refrain from all solids and liquids and any strenuous physical activity before attending the Department of Medicine at 0830 the next morning. On arrival, a small-diameter (outer diameter: 3.5 mm) manometric catheter (total length: 100 cm; Dentsleeve International, Mui Scientific) was inserted into the stomach through an anesthetized nostril and allowed to pass into the duodenum by peristalsis. The catheter contained 16 side holes spaced at 1.5-cm intervals, with an additional channel used for intraduodenal infusions located cm distal to the end of the sleeve sensor (14.5 cm from the pylorus), and was positioned as described previously (7). Once the manometric catheter was in position (which took between min), fasting motility was monitored until the occurrence of phase III of the interdigestive migrating motor complex. Immediately after cessation of phase III activity, an intravenous cannula was placed in a right forearm vein for blood sampling. At t = 215 min [during motor quiescence (ie, phase I of the migrating motor complex)], a baseline blood sample (14 ml) was taken, and a visual analog scale (VAS) questionnaire (27) to assess appetite perceptions and gastrointestinal symptoms completed by the subject. The baseline measurement of antropyloroduodenal motility also commenced. At t = 0 min, the 90-min intraduodenal infusion of one of the 5 treatments commenced. During the infusion, antropyloroduodenal motility was monitored continuously, and VAS ratings and blood samples were obtained at 15-min intervals. At t = 90 min, the infusion was terminated, and the intraduodenal catheter was removed. Subjects were presented with a standardized cold, buffet-style meal in excess of what they would be expected to consume and instructed to eat freely for #30 min (t = min) until comfortably full (28). The composition of the buffet meal has been described previously (28). After ingestion of the meal, at t = 120 min, a final blood sample was taken, and the VAS was completed, before the intravenous cannula was removed, and the subject was allowed to leave the laboratory. Measurements Antropyloroduodenal motility Antropyloroduodenal pressures were digitized and recorded by using a computer-based system running commercially available software (Flexisoft Version 3; Oakfield Instruments, GS Hebbard) and stored for subsequent analysis. Antropyloroduodenal pressures were analyzed for the number and amplitude of antral, duodenal, and isolated pyloric pressure waves (IPPWs) as well as basal pyloric pressure (BPP) with custom-written software modified to our requirements (A Smout, University Medical Centre, Amsterdam, Netherlands). The definition of pressure waves (PWs), and calculation of BPP have been described previously in detail (7). Plasma cholecystokinin and GLP-1, serum insulin, plasma glucagon, and blood glucose concentrations Venous blood samples (w14 ml) were collected in ice-chilled EDTA-coated tubes. Plasma and serum were separated by centrifugation at 3200 rpm for 15 min at 48C and stored at 2708C for later analysis of cholecystokinin, GLP-1, insulin, and glucagon. Plasma cholecystokinin-8 (pmol/l) was measured by radioimmunoassay after ethanol extraction by using an adaptation of a previous method (29). Standards were prepared by using synthetic sulfated cholecystokinin-8 (Sigma Chemical) and an anti cholecystokinin-8 antibody (C2581, Lot 105H4852; Sigma Chemical). This antibody binds all cholecystokinin peptides containing the sulfated tyrosine residue in position 7, shows a 26% cross-reactivity with unsulfated cholecystokinin-8 and,2% cross-reactivity with human gastrin I, and does not bind to structurally unrelated peptides. Sulfated cholecystokinin I-labeled with Bolton and Hunter reagent (Perkin Elmer) was used as tracer, and samples were incubated for 7 d at 48C. The antibody-bound fraction was separated by the addition of dextran-coated charcoal containing gelatin, and the radioactivity was determined in the supernatant fluid after centrifugation. Intraassay and interassay CVs were 5.8% and 21.1%, respectively. The minimum detectable concentration was 1 pmol/l. Values below the detection limit were treated as 0 (in all hormone assays). Plasma GLP-1 (pmol/l) was determined after ethanol extraction by using a radioimmunoassay kit (GLPIT-36HK; Millipore). The antibody used does not cross-react with glucagon, gastric inhibitory peptide, or other gut or pancreatic peptides, and it measures both GLP-1 (7 36) amide and GLP-1 (9 36) amide. Intraassay and interassay CVs were 6.0% and 8.1%, respectively. The minimum detectable concentration was 3 pmol/l. Serum insulin (mu/l) was measured by ELISA ( ; Mercodia). Intraassay and interassay CVs were 1.6% and 4.6%, respectively. The minimum detectable concentration was 1.0 mu/l. Plasma glucagon (pmol/l) was measured by using a radioimmunoassay kit (GL-32K; Millipore). The antibody used does not cross-react with insulin, proinsulin, C-peptide, somatostatin, or pancreatic polypeptide and has,0.1% cross-reactivity with oxyntomodulin. Intraassay and interassay CVs were 11.2% and 6.7%, respectively. The minimum detectable concentration was 5.7 pmol/l. Venous blood glucose (mmol/l) was measured immediately after collection by the glucose oxidase method by using a portable glucometer (Medisense Precision QID; Abbott Laboratories). The accuracy of this method has been confirmed in our laboratory by using the hexokinase technique (30). Appetite perceptions and gastrointestinal symptoms Perceptions of hunger, prospective consumption, fullness, nausea, and bloating were rated on VAS questionnaires (27). These questionnaires consisted of 100-mm horizontal lines, where 0 mm, which was on the furthest left on the scale, represented the sensation not felt at all, and 100 mm, which was on the furthest right on the scale, represented the sensation felt the greatest possible. Subjects placed vertical marks on each horizontal line to indicate the strength of each sensation felt at that time point.
4 LIPID, PROTEIN, GUT FUNCTION, AND ENERGY INTAKE 303 Energy intake The amount eaten (g) was quantified by weighing the buffet meal before and after consumption. Energy (kcal) and macronutrient (g) intakes and the percentage contribution of energy from fat, carbohydrate, and protein were calculated by using commercially available software (Foodworks, version 3.01; Xyris Software) (28). Total energy intake on each study day was quantified as the sum of energy intake at the buffet and the energy content of the infusion (270 kcal for nutrient infusions; 0 kcal for the saline control). The percentage of compensation in response to each nutrient infusion represented the degree to which subjects compensated for the caloric content of the infusion at the subsequent meal and was calculated by using the following formula (31): Percentage of compensation ¼½ðEI at buffet control EI at buffet after infusant Þ O270 kcalš where EI at buffet control represents energy intake from the ad libitum buffet meal on the control day, and EI at buffet after infusant represents energy intake from the ad libitum buffet meal in response to each infusion. A compensation of 100% represents the full compensation for the caloric load of the infusion. Data and statistical analyses Baseline values for the number and amplitude of antral and duodenal PWs, IPPWs, and BPP, VAS scores, and hormone and blood glucose concentrations were calculated as the mean of values obtained between t = 215 to 0 min. During the 90-min infusion, the number and amplitude of pyloric pressures and BPPs were expressed as mean values over 15-min intervals, and hormone concentrations and VAS scores were expressed as mean values at collection time points. Antral and duodenal motility were expressed as motility indexes (MIs) over 90 min, which were calculated by using the following equation (32): MI ¼ ln½ðsum of amplitudes 3 no: of phasic PWsÞþ1Š Statistical analyses were performed with SPSS software (version 19.0; SPSS Inc, IBM). MIs of antral and duodenal PWs, total number and mean amplitude of IPPWs, mean BPP, AUCs for appetite sensations and hormone concentrations, energy and macronutrient intakes at the buffet meal, and total energy intake (ie, energy intake at the buffet meal plus the energy content of the infusion) were analyzed by 1-factor ANOVA. Post hoc comparisons, adjusted for multiple comparisons by using Bonferroni s correction, were performed when ANOVAs revealed significant effects, and statistical significance was accepted at P, Because 9 of 20 subjects experienced nausea (VAS scores increased by $30 mm for min) during L3 (of these participants, 2 subjects also vomited between 75 and 90 min after commencement of the infusion, and missing data were carried forward to 90 min to allow inclusion in the analysis), but only one subject experienced nausea during the L2P1, one subject experienced nausea during the L1P2, and no subjects experienced nausea during the P3, potential effects of nausea on the response to L3 were evaluated by comparing all outcome variables between subjects who experienced nausea (N+; n = 9) subjects ð1þ ð2þ who did not experience nausea (N2; n = 11) by using an independent-sample t test. Energy intake in response to L3 compared with C was also analyzed separately in N+ and N2 groups. The percentage of compensation was examined by using a 1-sample t test, testing each treatment against a fixed value of 0 (where P represented no compensation of the energy content of the infusant) and against a fixed value of 100 (where P represented perfect compensation or overcompensation for the energy content of the infusant) (31). Relations between loads of protein or lipid with AUCs (calculated by using the trapezoidal rule) for BPP, IPPWs, hormones, blood glucose concentrations, VAS, and energy intake were evaluated by using linear within-subject correlations. Relations of energy intake with mean BPPs, number and amplitude of IPPWs, antral and duodenal MIs, and AUCs for plasma hormones, blood glucose concentrations, and the VAS were evaluated by using linear within-subject correlations (33). Variables with the top-4 ranked r values were included in a multiple regression analysis to establish determinants of energy intake. Significance was accepted at P, 0.05; all data are presented as means 6 SEMs. RESULTS Antropyloroduodenal pressures Baseline values for antral and duodenal MIs, total number and mean amplitude of isolated pyloric PWs, and BPPs did not differ between study days (Table 1). Antral pressures There was an effect of treatment on the antral MI (P, 0.001) (Figure 1A), which reflected a reduction in both the number and amplitude of antral PWs (Table 2). Compared with the C, all nutrient infusions suppressed the antral MI (all P, 0.05), with no difference between any of the nutrient treatments. There was no relation between antral MI with the load of lipid or protein administered. Antral MI during the L3 was slightly greater in N+ than N2 (N+: mm Hg, N2: mm Hg; P, 0.05). IPPWs There was an effect of treatment on the total number of IPPWs (P, 0.001) (Figure 1B, Table 2). Compared with the C, all nutrient infusions increased the number of IPPWs (all P, 0.05) with no difference between any of the nutrient treatments. The number of IPPWs was related directly to the load of lipid (r = 0.39, P, 0.01) administered, so that IPPWs increased with the amount of lipid in the infusion. There was an effect of treatment on the mean amplitude of IPPWs (P, 0.05) (Table 2). All nutrient infusions increased the amplitude of IPPWs compared with the C (all P, 0.05), and L2P1 increased the amplitude of IPPWs compared with the P3 and L1P2 (all P, 0.05). There was no relation between the mean amplitude of IPPWs with the load of lipid or protein administered. There were no differences in the AUC of the number or amplitude of IPPWs during the L3 between N+ and N2 (number: N+, min; N2, min; amplitude: N+: mmhg $ min, N2: mmhg $ min).
5 304 RYAN ET AL TABLE 1 Baseline values for the number and amplitude of antral, pyloric, and duodenal PWs; basal pyloric pressures; and hormone and blood glucose concentrations 1 C P3 L1P2 L2P1 L3 P Antral PWs No NS Amplitude (mm Hg) NS IPPWs No NS Amplitude (mm Hg) NS Mean BPP (mm Hg) NS Duodenal PWs No NS Amplitude (mm Hg) NS Hormone and glucose concentrations Cholecystokinin (pmol/l) NS GLP-1 (pmol/l) NS Serum insulin (mu/l) NS Glucagon (pmol/l) NS Blood glucose (mmol/l) NS 1 All values are means 6 SEs. n = 20. Before 90-min intraduodenal infusions of P3, L3, L2P1, or L1P2 (each at 3 kcal/min) or C. Main treatment effects were determined by using 1-factor ANOVA. BPP, basal pyloric pressure; C, saline control; GLP-1, glucagon-like peptide-1; IPPW, isolated pyloric pressure wave; L1P2, intralipid and whey protein hydrolysate in a 1:2 ratio; L2P1, intralipid and whey protein hydrolysate in a 2:1 ratio; L3, pure lipid; PW, pressure wave; P3, whey protein hydrolysate. BPPs There was an effect of treatment on mean BPPs (P, 0.05); however, the post hoc analysis revealed no significant differences between treatments (Figure 1C, Table 2). There was no relation between BPP and the load of lipid or protein administered. The mean BPP in response to the L3 tended to be greater in N+ than N2 (N+: mm Hg; N2: mm Hg; P = 0.09). FIGURE 1. Means (6SEMs) of the MI for antral pressure waves (A), IPPWs (B), BPPs (C), and the MI for duodenal pressure waves (D) during 90-min, 3-kcal/min intraduodenal infusions of C (open circles), P3 (open triangles), L1P2 (closed triangles), L2P1 (closed squares), or L3 (open squares). n = 20. Treatment effects were determined by using 1-factor ANOVA, and significant differences (P, 0.05) were determined by post hoc comparisons by using Bonferroni correction. A: Treatment effect for MI (over 90 min) of antral pressure waves (P, 0.001): *significantly different from C, P, B: Treatment effect for the total number (over 90 min) of IPPWs (P, 0.001): *significantly different from C, P, C: Treatment effect for mean BPP (over 90 min) (P, 0.05): no significant differences between treatments. D: Treatment effect for MI (over 90 min) of duodenal waves (P, 0.001): *significantly different from C, P, 0.01; # significantly different from L2P1, L1P2, and P3 (P, 0.01). BPP, basal pyloric pressure; C, saline control; IPPW, isolated pyloric pressure wave; L1P2, intralipid and whey protein hydrolysate in a 1:2 ratio; L2P1, intralipid and whey protein hydrolysate in a 2:1 ratio; L3, pure lipid; MI, motility index; P3, whey protein hydrolysate.
6 LIPID, PROTEIN, GUT FUNCTION, AND ENERGY INTAKE 305 TABLE 2 Number, amplitude, and MI of antral and duodenal PWs; number and amplitude of IPPWs; and basal pyloric pressures during 90-min intraduodenal infusions 1 C P3 L1P2 L2P1 L3 P Antral PWs No Amplitude (mm Hg) MI (mm Hg) ,0.001 IPPWs No ,0.001 Amplitude (mm Hg) ,0.05 BPP (mm Hg) ,0.05 Duodenal PWs No Amplitude (mm Hg) MI (mm Hg) , All values are means 6 SEs. n = 20. Intraduodenal infusions were P3, L3, L2P1, or L1P2 (each at 3 kcal/min) or C. Main treatment effects were determined by using 1-factor ANOVA; significant differences were determined by post hoc comparisons by using Bonferroni correction. BPP, basal pyloric pressure; C, saline control; IPPW, isolated pyloric pressure wave; L1P2, intralipid and whey protein hydrolysate in a 1:2 ratio; L2P1, intralipid and whey protein hydrolysate in a 2:1 ratio; L3, pure lipid; MI, motility index; PW, pressure wave; P3, whey protein hydrolysate. 2 Significantly different from C, P, Significantly different from P3, P, Significantly different from L1P2, P, Significantly different from L2P1, P, Duodenal PWs There was an effect of treatment on the duodenal MI (P, 0.001) (Figure 1D), which reflected a reduction in both the number and amplitude of duodenal PWs (Table 2). All nutrients reduced the duodenal MI compared with C (all P, 0.01) and the L3 compared with P3, L1P2, and L2P1 (all P, 0.01). The MI of duodenal PWs was related inversely to the load of lipid (r = 20.54, P, 0.01) administered. The duodenal MI during the L3 was slightly greater in N+ than N2 (N+: mm Hg; N2: mm Hg; P, 0.05). Gut hormone, insulin, glucagon, and blood glucose concentrations Baseline values for plasma cholecystokinin and GLP-1, serum insulin, plasma glucagon, and blood glucose concentrations did not differ between study days (Table 1). Plasma cholecystokinin There was an effect of treatment on the plasma cholecystokinin AUC (P, 0.001) (Figure 2A). Compared with the C, all nutrient infusions increased the plasma cholecystokinin AUC. The L3 also increased the plasma cholecystokinin AUC compared with all other nutrients, the L2P1 compared with L1P2 and P3, and the L1P2 compared with P3 (all P, 0.05). The cholecystokinin AUC (Table 3) was related directly to the load of lipid (r = 0.79, P, 0.001) administered. There was no difference in the cholecystokinin AUC during the L3 between N+ and N2 (N+: pmol $ L 21 $ min; N2: pmol $ L 21 $ min). GLP-1 There was an effect of treatment on the plasma GLP-1 AUC (P, 0.001) (Figure 2B). Compared with the C, all nutrient infusions increased the plasma GLP-1 AUC. The L3 also increased the plasma GLP-1 AUC compared with all other nutrients, the L2P1 compared with L1P2 and P3, and the L1P2 compared with P3 (all P, 0.05). The GLP-1 AUC (Table 3) was related directly to the load of lipid (r = 0.82, P, 0.001) administered. There was no difference in the GLP-1 AUC during the L3 between N+ and N2 (N+: pmol $ L 21 $ min, N2: pmol $ L 21 $ min). Serum insulin There was an effect of treatment on the serum insulin AUC (P, 0.001) (Figure 2C). Compared with the C, all nutrient infusions increased the serum insulin AUC. P3 also increased serum insulin compared with all other nutrients, the L1P2 compared with L2P1 and L3, and the L2P1 compared with L3 (all P, 0.05). The serum insulin AUC (Table 3) was directly related to the load of protein (r = 0.83, P, 0.001) administered. There was no difference in the insulin AUC during the L3 between N+ and N2 (N+: mu $ L 21 $ min; N2: mu $ L 21 $ min). Glucagon There was an effect of treatment on the plasma glucagon AUC (P, 0.001) (Figure 2D). Compared with the C, all nutrient infusions increased the plasma glucagon AUC. P3 also increased the plasma glucagon AUC compared with the L2P1 and L3, the L1P2 compared with L2P1 and L3, and the L2P1 compared with L3 (all P, 0.001). The plasma glucagon AUC (Table 3) was related directly to the load of protein (r = 0.83, P, 0.001) administered. There was no difference in glucagon AUC during L3 between N+ and N2 (N+: pmol $ L 21 $ min; N2: pmol $ L 21 $ min). Blood glucose There was an effect of treatment on blood glucose AUC (P, 0.05) (Figure 2E); however there were no significant differences
7 306 RYAN ET AL FIGURE 2. Mean (6SEM) plasma CCK (A), plasma GLP-1 (B), serum insulin (C), plasma glucagon (D), and blood glucose (E) concentrations during 90-min, 3-kcal/min intraduodenal infusions of C (open circles), P3 (open triangles), L1P2 (closed triangles), L2P1 (closed squares), or L3 (open squares). n = 20. Treatment effect was determined by using 1-factor ANOVA for AUCs of the hormone and glucose profiles, and significant differences (P, 0.05) were determined by post hoc comparisons by using Bonferroni correction. A: Treatment effect (P, 0.001): *significantly different from C, P, 0.05; x significantly different from P3, P, 0.05; + significantly different from L1P2, P, 0.05; # significantly different from L2P1, P, B: Treatment effect (P, 0.001): *significantly different from C, P, 0.05; x significantly different from P3, P, 0.05; + significantly different from L1P2, P, 0.05; # significantly different from L2P1, P, C: Treatment effect (P, 0.001): *significantly different from C, P, 0.05; z significantly different from L3, P, 0.05; # significantly different from L2P1, P, 0.05; + significantly different from L1P2, P, D: Treatment effect (P, 0.001): *significantly different from C, P, 0.001; z significantly different from L3, P, 0.001; # significantly different from L2P1 (P, 0.001). E: Treatment effect (P, 0.05). C, saline control; CCK, cholecystokinin; GLP-1, glucagon-like peptide-1; L1P2, intralipid and whey protein hydrolysate in a 1:2 ratio; L2P1, intralipid and whey protein hydrolysate in a 2:1 ratio; L3, pure lipid; P3, whey protein hydrolysate. between treatments. There was no relation between the blood glucose AUC (Table 3) and load of lipid or protein administered. There was no difference in the blood glucose AUC during the L3 between N+ and N2t (N+: mmol $ L 21 $ min; N2: mmol $ L 21 $ min). Appetite perceptions and gastrointestinal symptoms Hunger There was no difference in baseline hunger ratings between study days. There was a trend for an effect of treatment on the hunger AUC (P = 0.09) (see Supplemental Figure 2A under Supplemental data in the online issue). There was no difference in the hunger AUC during the L3 between N+ and N2 (N+: mm $ min; N2: mm $ min). Prospective consumption There was no difference in baseline prospective consumption ratings between study days. There was an effect of treatment on the prospective consumption AUC (P, 0.05) (see Supplemental Figure 2B under Supplemental data in the online issue); however, there were no significant differences between treatments. The prospective consumption AUC was related weakly to the load of lipid (r = 0.28, P, 0.05) administered. There was no difference in the prospective consumption AUC during the L3 between N+ and N2 (N+: mm $ min; N2: mm $ min). Fullness There was no difference in baseline fullness ratings between study days. There was a trend for an effect of treatment on the
8 TABLE 3 AUCs for plasma cholecystokinin, GLP-1, insulin, glucagon, and blood glucose concentrations during 90-min intraduodenal infusions 1 C P3 L1P2 L2P1 L3 P Cholecystokinin (pmol $ L 21 $ min) , ,0.001 GLP-1 (pmol $ L 21 $ min) , ,0.001 Serum insulin (mu $ L 21 $ min) , ,5, , ,0.001 Glucagon (pmol $ L 21 $ min) ,5, ,5, , ,0.001 Blood glucose (mmol $ L 21 $ min) , All values are means 6 SEs. n = 20. Intraduodenal infusions were P3, L3, L2P1, or L1P2 (each at 3 kcal/min) or C. Main treatment effects were determined by using 1-factor ANOVA; significant differences were determined by post hoc comparisons by using Bonferroni correction. C, saline control; GLP-1, glucagon-like peptide-1; L1P2, intralipid and whey protein hydrolysate in a 1:2 ratio; L2P1, intralipid and whey protein hydrolysate in a 2:1 ratio; L3, pure lipid; P3, whey protein hydrolysate. 2 Significantly different from C, P, Significantly different from P3, P, Significantly different from L1P2, P, Significantly different from L2P1, P, Significantly different from L3, P, LIPID, PROTEIN, GUT FUNCTION, AND ENERGY INTAKE 307 fullness AUC (P = 0.076) (see Supplemental Figure 2C under Supplemental data in the online issue). The fullness AUC was related weakly to the load of lipid (r = 0.28, P, 0.05) administered. There was no difference in the fullness AUC during the L3 between N+ and N2 (N+: mm $ min; N2: mm $ min). Nausea There was no difference in baseline nausea ratings between study days. There was an effect of treatment on the nausea AUC (P, 0.01); nausea was greater during the L3 than C and L1P2 (both P, 0.05) and tended to be greater than during the P3 (P = 0.07) (see Supplemental Figure 2D under Supplemental data in the online issue). The nausea AUC was related weakly to the load of lipid (r = 0.32, P, 0.05) administered. Bloating There was no difference in baseline bloating ratings between study days. There was a trend for an effect of treatment on bloating AUC (P = 0.07) (see Supplemental Figure 2E under Supplemental data in the online issue). The bloating AUC was related weakly to the load of lipid (r = 0.30, P, 0.05) administered. There was no difference in the bloating AUC during the L3 between N+ and N2 (N+: mm 3 min; N2: mm 3 min). Energy and macronutrient intakes There was an effect of treatment on energy intake (kcal) from the buffet meal (P, 0.001) (Table 4). Compared with the C, energy intake was less after the L3 (P, 0.01) and P3 (P, 0.05) and tended to be less after the L2P1 (P = 0.08), with no significant differences between any of the nutrient infusions. There was an effect of treatment on the amount (g) of food consumed at the buffet (P, 0.001), which was less after the P3 and L3 than after the C (both P, 0.01). There was an effect of treatment on intakes (g) of protein and carbohydrate (both P, 0.001) but not fat. Compared with the C, the intake of protein (g) was less after the P3, L3, and L2P1 (all P, 0.05), whereas the intake of carbohydrate (g) was less after the P3 and L3 (both P, 0.05). There was an effect of treatment on the percentage of energy consumed from protein (P, 0.05); however, post hoc comparisons revealed no significant differences between treatments. There was no effect of treatment on the percentage of energy consumed from carbohydrate or fat. Subjects compensated for the caloric content of the P3 (P, 0.01) and L3 (P, 0.01) (P3: %; L3: %; one-sample t test against 0) (P3: P = 0.287; L3: P = 0.975; one-sample t test against 100), with no differences in the percentage of compensation between the L3 and P3. The energy load of L2P1 and L1P2 infusions were not significantly compensated for (L2P1: %; L1P2: %), and the L3 was compensated for better than the L2P1 (P, 0.05). Energy intake in response to the L3 was reduced by w370 kcal in N+ than in N2 (energy intake: N+, kcal, N2, kcal); however, while of physiologic relevance, the result was NS (P = 0.07). In both N+ and N2, energy intake in response to the L3 compared with control was significantly reduced (N+: L3, kcal; C, kcal; P, 0.01; N2: L3, kcal; C, kcal; P, 0.05). The amount of food (g) eaten after the L3 did not differ between N+ and N2 (food intake: N+, g; N2, g). N+ consumed less protein (N+: g; N2:596 6g;P, 0.05) and carbohydrate (N+: g; N2: g; P = 0.05) than did N2. The percentage of total energy consumed as protein (N+: %; N2: 216 1%;P, 0.05) and carbohydrate (N+: %; N2: 486 2%; P, 0.05) was also less in N+ than N2. The percentage of compensation for N+ during the L3 tended to be greater ( %) than for N2 ( %) (P = 0.07). Relations between antropyloroduodenal motility, cholecystokinin, GLP-1, insulin, glucagon, and glucose concentrations and perceptions of appetite and gastrointestinal symptoms with energy intake Energy intake from the buffet was related inversely to fullness (r = 20.37, P, 0.05), nausea (r = 20.59, P, 0.001), and bloating (r = 20.54, P, 0.001) at t = 90 min and related directly to prospective consumption (r = 0.46, P, 0.001) at t =90 min. It was also related inversely to cholecystokinin AUC (r = 20.30, P, 0.05). When nausea, prospective consumption, and cholecystokinin AUCs were included in a multiple regression analysis, nausea was the most significant predictor of energy
9 308 RYAN ET AL TABLE 4 Energy content, weight, and macronutrient distribution (percentage of energy derived from fat, carbohydrate, or protein) of food consumed at a buffet meal and the percentage of compensation in response to 90-min intraduodenal infusions 1 C P3 L1P2 L2P1 L3 P Energy intake Buffet (kcal) ,0.001 Total (kcal) ,0.001 Amount eaten (g) ,0.001 Protein intake g ,0.001 Percentage of energy ,0.05 Carbohydrate intake g ,0.05 Percentage of energy NS Fat intake g NS Percentage of energy NS Percentage of compensation All values are means 6 SEs. n = 20. The buffet meal was consumed immediately after 90-min intraduodenal infusions of P3, L3, L2P1, or L1P2 (each at 3 kcal/min) or C. Main treatment effects were determined by using 1-factor ANOVA; significant differences were determined by post hoc comparisons by using Bonferroni correction. C, saline control; L1P2, intralipid and whey protein hydrolysate in a 1:2 ratio; L2P1, intralipid and whey protein hydrolysate in a 2:1 ratio; L3, pure lipid; P3, whey protein hydrolysate. 2 Significantly different from C, P, Trend for difference compared with C, P, Calculated as the sum of energy intake at the buffet meal and the caloric content of the infusion. 5 Percentage of compensation ([(EI at buffet control EI at buffet after infusant ) O 270 kcal] 3 100) was determined by using a 1-sample t test against a fixed value of 0, which represented the compensation for the energy content of the test infusion, and against a fixed value of 100, which represented perfect compensation for the energy content of the test infusion. 6 Significantly different from fixed value of 0% of compensation (P, 0.05). intake at the buffet (r = 0.48, P, 0.001). No other significant relations were identified. Relations between antropyloroduodenal motility, cholecystokinin, GLP-1, insulin, glucagon, and glucose concentrations The blood glucose AUC was related inversely to the cholecystokinin AUC (r = 20.27, P, 0.05) and glucagon AUC (r = 20.26, P, 0.05). The glucagon AUC was related to the insulin AUC (r = 0.82, P, 0.001). DISCUSSION This study described the effects of isocaloric, intraduodenal infusions of pure lipid and protein and their combinations on antropyloroduodenal motility, cholecystokinin, GLP-1, insulin, glucagon, blood glucose, appetite, and energy intake in healthy lean men. We report that 1) intraduodenal lipid and protein comparably suppressed subsequent energy intake, 2) protein had lesser effects on pyloric pressures and plasma cholecystokinin and GLP-1 than did lipid, 3) protein potently stimulated both insulin and glucagon, thus maintaining normoglycemia, 4) lipid and protein in combination did not have additive effects, and 5) lipid, but not protein, induced nausea. We showed that infusions of lipid and protein, infused at 3 kcal/min, comparably suppressed subsequent energy intake. For lipid, the suppression of energy intake was associated with a potent stimulation of pyloric pressures and gastrointestinal hormone release as well as nausea, in line with our previous findings (9, 14). Compared with lipid, protein also suppressed energy intake, despite weaker effects on cholecystokinin, GLP-1, and gastrointestinal motility, and thus, the suppression of energy intake by protein is likely a result of other mechanisms. Mechanisms that have been suggested include stimulation of insulin release (34), postprandial thermogenesis (35), intestinal gluconeogenesis (36), and direct effects of amino acids, particularly branched-chain amino acids, in regions of the brain, including the hypothalamus (37); however, definitive evidence for a role of these mechanisms remains to be established. Peptide YY has also been suggested as a mediator of the effects of protein on food intake (38); however, this study used unphysiologically high loads of protein, and by using more-moderate amounts, our recent study was unable confirm those findings (2). The suppression of energy intake in the L3 or P3 was not associated with any substantial changes in appetite suppression. This result confirmed our frequent previous observations (7, 39, 40) that, in the absence of gastric distension, intraduodenal nutrients can potently suppress energy intake, with little to no effect on appetite perceptions. Lipid induced nausea in w45% of subjects, in whom energy intake was markedly less than in N2. Thus, nausea contributed, at least in some subjects, to the energy intake suppressant effect of lipid, confirming that nausea affects energy intake in humans (14), possibly by causing a subtle aversion through activation of 5-hydroxytryptamine receptor mechanisms (41). However, nausea was not associated with any major effects on gastrointestinal motility or hormone (particularly cholecystokinin) release and, thus, may have been because of a hypersensitivity to lipid or its digestion products, fatty acids, in the small intestinal
10 LIPID, PROTEIN, GUT FUNCTION, AND ENERGY INTAKE 309 lumen or to cholecystokinin. Changes in the sensitivity to lipid (both hypersensitivity and hyposensitivity) have been shown in various disorders, including functional dyspepsia (42) and obesity (1). We have established that intraduodenal infusions of long-chain triglycerides, glucose, and partially hydrolyzed whey protein dose-dependently modulate antropyloroduodenal motility (7 9), and lipid appears to have the most potent effects (7 9, 22). The current study confirmed that the effects of protein, particularly on pyloric and duodenal pressures, are weaker. Our data also showed major differences in the stimulation of cholecystokinin and GLP-1 release. Although both the L3 and P3 stimulated cholecystokinin and GLP-1 compared with the control, concentrations were much higher during the L3, indicating that lipid is a much more potent stimulus than protein. The potent effects of lipid on gastrointestinal motility and hormone release are a result of the release of fatty acids during fat digestion (43, 44). For example, the entry of kcal fatty acids/min into the small intestine is sufficient to increase plasma cholecystokinin by w7 pmol within 10 min (43), whereas cholecystokinin in response to the P3 only increased by w1 pmol in the first 15 min. Similar differences applied to GLP-1, although the gradual pattern of the rise reflected its release from enteroendocrine L cells located in the distal small intestine. Thus, a marked elevation in plasma GLP-1 in response to the L3 was evident within 30 min, whereas comparable elevations in response to P3 were achieved at 90 min. There is evidence that, like fat, protein digestion to dipeptides or tripeptides and free amino acids enhances gastrointestinal hormone release (45), and because whey protein is considered a fast protein (46), it would be expected that these digestion products would be liberated quickly within the gastrointestinal tract. Amino acids in whey with effects on gastrointestinal motility include arginine, glutamate, glycine, and L-tryptophan (L-Trp). For example, a 20-min intraduodenal infusion of 50 mmol L-Trp/L (w20.4 mg/min) stimulates tonic and phasic pyloric pressures in healthy humans (47). By comparison, our P3 infusion delivered w17 mg L-Trp/min over 90 min, which, thus, may not have reached the required luminal threshold concentration. L-Trp and L-phenylalanine stimulate cholecystokinin (48), and L-Trp, as well as leucine, glutamine, alanine and asparagine (all present in whey) stimulate GLP-1 in human cell lines and in lean, obese, and type 2 diabetic humans (18, 49 52). Thus, the reasons for the relatively weak effects of whey on gastrointestinal function are unclear. We observed a significant stimulation of both insulin and glucagon release by protein than lipid. The slight, but significant, reduction in blood glucose during the P3 at t = 90 min suggested that the glucose-lowering effect of insulin was relatively stronger than the glucose-stimulatory effect of glucagon. Thus, the potential hypoglycemic effect of the insulin response to protein was counteracted by the glucagon response, which was probably mediated by amino acids (50, 52), ensuring that, even after a relatively high protein load, blood glucose concentrations remain in the normoglycemic range. Whey protein has potent insulinotropic effects (18), which are glucose-independent and likely driven by the direct stimulation of pancreatic b cells by insulinogenic (18), particularly branched-chain (50), amino acids and may, thus, reduce postprandial blood glucose in both health and type 2 diabetes (15, 18). Moreover, a recent study showed that, after oral protein consumption, hepatic insulin excretion was reduced, which led to a persistent elevation of serum insulin, in the absence of increased insulin release, even after the termination of feeding (51), which may also be the case for intraduodenal protein. GLP-1 and GIP are the 2 known incretin hormones; however, the release of insulin by GLP-1 is glucose-dependent. Thus, because subjects were euglycemic, GLP-1 should not have had insulinotropic or glucagonostatic effects. We did not evaluate GIP release, but a study showed that lipid and protein both stimulate GIP, and the early GIP release after protein was correlated with the insulin rise (53). At the loads used, the effects of lipid-protein combinations on gut hormones were related directly to the amount of lipid, and the effects on insulin and glucagon were related to the amount of protein, in the infusion, whereas no clear pattern was apparent for effects on motility, and the lipid-protein combinations did not suppress energy intake compared with the control. The reasons for these outcomes are not clear, but if our assumption that critical loads of amino acids and fatty acids, rather than a specific caloric load, within the intestinal lumen are required is correct, it is likely that these thresholds were not reached. It is also possible that, in the combinations, protein and lipid formed complexes, which diminished their effects; however, because combinations displayed intermediate effects between those of the isolated nutrients, particularly on hormones, this outcome seemed unlikely. Thus, additional studies are warranted to define nutrient thresholds for optimal effects on both energy intake and blood glucose control. Several aspects of our study design warrant recognition. Only healthy, lean men were included because they are more sensitive to dietary manipulation than women (54); hence, our findings may not extend to women. In addition, the number of study conditions (n = 5) may have compromised the power of the study to detect significant differences between treatments for some variables. The appetite-suppressive effects of protein have been shown to vary between sources of protein (25, 26), and thus, our results may not apply to alternative sources of protein. In conclusion, despite differing effects on gastrointestinal function, intraduodenal lipid and protein comparably suppress energy intake. Intraduodenal protein also regulates glycemia by stimulating insulin and glucagon. In contrast, at the loads chosen, lipid:protein combinations did not suppress energy intake. Additional research needs to identify effective loads of lipid and protein or their digestion products that offer optimal energy intake suppression and blood glucose control while avoiding adverse effects, thereby offering nutritional benefits for a number of diet-related disorders. We thank Asimina Kallas and Briohny Bartlett for preparing infusions and assisting on study days, and Kylie Lange for statistical support. The authors responsibilities were as follows CF-B: accepted full responsibility for the overall conduct of the study and had primary responsibility for the final content of the manuscript; NDL-M, TJL, MH, and CF-B: designed the research; ATR and AAS: conducted the research, analyzed data, and conducted the statistical analysis; SS: performed the hormone analysis; MH, NDL-M, and TJL: assisted with the interpretation and preparation of the manuscript; ATR and CF-B: wrote the manuscript; and all authors: read and approved the final manuscript. None of the authors had any conflicts of interest to declare. REFERENCES 1. Stewart JE, Seimon RV, Otto B, Keast RS, Clifton PM, Feinle-Bisset C. Marked differences in gustatory and gastrointestinal sensitivity to oleic acid between lean and obese men. Am J Clin Nutr 2011;93:
Review Article. Tanya J Little, Michael Horowitz, and Christine Feinle-Bisset. peptides, including ghrelin, cholecystokinin (CCK), glucagonlike
 Review Article Modulation by high-fat diets of gastrointestinal function and hormones associated with the regulation of energy intake: implications for the pathophysiology of obesity 1 3 Tanya J Little,
Review Article Modulation by high-fat diets of gastrointestinal function and hormones associated with the regulation of energy intake: implications for the pathophysiology of obesity 1 3 Tanya J Little,
Effects of intraduodenal fatty acids on appetite, antropyloroduodenal motility, and plasma CCK and GLP-1 in humans vary with their chain length
 Am J Physiol Regul Integr Comp Physiol 287: R524 R533, 2004. First published May 27, 2004; 10.1152/ajpregu.00039.2004. Effects of intraduodenal fatty acids on appetite, antropyloroduodenal motility, and
Am J Physiol Regul Integr Comp Physiol 287: R524 R533, 2004. First published May 27, 2004; 10.1152/ajpregu.00039.2004. Effects of intraduodenal fatty acids on appetite, antropyloroduodenal motility, and
Initially more rapid small intestinal glucose delivery increases plasma. insulin, GIP and GLP-1, but does not improve overall glycemia in
 Articles in PresS. Am J Physiol Endocrinol Metab (May 10, 2005). doi:10.1152/ajpendo.00099.2005 E-00099-2005.R1 Final accepted version 1 Initially more rapid small intestinal glucose delivery increases
Articles in PresS. Am J Physiol Endocrinol Metab (May 10, 2005). doi:10.1152/ajpendo.00099.2005 E-00099-2005.R1 Final accepted version 1 Initially more rapid small intestinal glucose delivery increases
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function
 Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
The Role of the Free Fatty Acid, Lauric Acid, in Appetite Regulation and its Potential as an Appetite- Suppressant
 The Role of the Free Fatty Acid, Lauric Acid, in Appetite Regulation and its Potential as an Appetite- Suppressant A thesis submitted by Kate Feltrin For the degree of Doctor of Philosophy Discipline of
The Role of the Free Fatty Acid, Lauric Acid, in Appetite Regulation and its Potential as an Appetite- Suppressant A thesis submitted by Kate Feltrin For the degree of Doctor of Philosophy Discipline of
SLENDESTA POTATO EXTRACT PROMOTES SATIETY IN HEALTHY HUMAN SUBJECTS: IOWA STATE UNIVERSITY STUDY Sheila Dana, Michael Louie, Ph.D. and Jiang Hu, Ph.D.
 SLENDESTA POTATO EXTRACT PROMOTES SATIETY IN HEALTHY HUMAN SUBJECTS: IOWA STATE UNIVERSITY STUDY Sheila Dana, Michael Louie, Ph.D. and Jiang Hu, Ph.D. INTRODUCTION KEY CONCLUSIONS Excessive calorie intake
SLENDESTA POTATO EXTRACT PROMOTES SATIETY IN HEALTHY HUMAN SUBJECTS: IOWA STATE UNIVERSITY STUDY Sheila Dana, Michael Louie, Ph.D. and Jiang Hu, Ph.D. INTRODUCTION KEY CONCLUSIONS Excessive calorie intake
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM
 The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
Christine Pelkman, PhD
 Christine Pelkman, PhD Dr. Pelkman is a graduate faculty member in Nutrition, and Director of the Nutrition and Health Research Laboratory at the University of Buffalo. She completed her doctoral and postdoctoral
Christine Pelkman, PhD Dr. Pelkman is a graduate faculty member in Nutrition, and Director of the Nutrition and Health Research Laboratory at the University of Buffalo. She completed her doctoral and postdoctoral
in health and diabetes regulation
 1 Gastric motor function in health and diabetes implications for incretin hormone release and postprandial blood glucose regulation A thesis submitted by Dr Jessica Lee Sing Chang BNutrDiet, BSc(Med),
1 Gastric motor function in health and diabetes implications for incretin hormone release and postprandial blood glucose regulation A thesis submitted by Dr Jessica Lee Sing Chang BNutrDiet, BSc(Med),
Objectives. Define satiety and satiation Summarize the satiety cascade Describe potential dietary interventions aimed at improving satiety
 Foods that Fill Monica Esquivel PhD RDN Assistant Professor, Dietetics Program Director Department of Human Nutrition, Food and Animal Sciences November 8, 2017 Objectives Define satiety and satiation
Foods that Fill Monica Esquivel PhD RDN Assistant Professor, Dietetics Program Director Department of Human Nutrition, Food and Animal Sciences November 8, 2017 Objectives Define satiety and satiation
EFFECTS OF PROTEIN ON GASTROINTESTINAL FUNCTION AND APPETITE REGULATION
 EFFECTS OF PROTEIN ON GASTROINTESTINAL FUNCTION AND APPETITE REGULATION A thesis submitted by Amy T Hutchison for the degree of Doctor of Philosophy Discipline of Medicine School of Medicine University
EFFECTS OF PROTEIN ON GASTROINTESTINAL FUNCTION AND APPETITE REGULATION A thesis submitted by Amy T Hutchison for the degree of Doctor of Philosophy Discipline of Medicine School of Medicine University
Short-term Satiety of High Protein Formula on Obese Subjects: A Pilot Study
 2012 International Conference on Nutrition and Food Sciences IPCBEE vol. 39 (2012) (2012) IACSIT Press, Singapore Short-term Satiety of High Protein Formula on Obese Subjects: A Pilot Study Kamalita Pertiwi
2012 International Conference on Nutrition and Food Sciences IPCBEE vol. 39 (2012) (2012) IACSIT Press, Singapore Short-term Satiety of High Protein Formula on Obese Subjects: A Pilot Study Kamalita Pertiwi
Introduction. The oxytocin/ / vasopressin receptor antagonist, atosiban, delays the gastric emptying of a semisolid meal compared to saline in human
 The oxytocin/ / vasopressin receptor antagonist, atosiban, delays the gastric emptying of a semisolid meal compared to saline in human Bodil Ohlsson, et. al., Sweden BMC Gastroenterology, 2006 Presented
The oxytocin/ / vasopressin receptor antagonist, atosiban, delays the gastric emptying of a semisolid meal compared to saline in human Bodil Ohlsson, et. al., Sweden BMC Gastroenterology, 2006 Presented
Motility Conference Ghrelin
 Motility Conference Ghrelin Emori Bizer, M.D. Division of Gastroenterology/Hepatology November 21, 2007 Ghrelin: Basics Hormone produced by the A-like A endocrine cells in the oxyntic mucosa (stomach body
Motility Conference Ghrelin Emori Bizer, M.D. Division of Gastroenterology/Hepatology November 21, 2007 Ghrelin: Basics Hormone produced by the A-like A endocrine cells in the oxyntic mucosa (stomach body
Gastric emptying and release of incretin hormones after glucose ingestion in humans.
 Gastric emptying and release of incretin hormones after glucose ingestion in humans. J Schirra,, R Arnold, B Göke J Clin Invest. 1996;97(1):92-103. https://doi.org/10.1172/jci118411. Research Article This
Gastric emptying and release of incretin hormones after glucose ingestion in humans. J Schirra,, R Arnold, B Göke J Clin Invest. 1996;97(1):92-103. https://doi.org/10.1172/jci118411. Research Article This
LESSON 3.3 WORKBOOK. How do we decide when and how much to eat?
 Appetite The psychological desire to eat, driven by feelings of pleasure from the brain. Hunger The biological or physiological need to eat, caused by a release of hormones from the digestive tract. LESSON
Appetite The psychological desire to eat, driven by feelings of pleasure from the brain. Hunger The biological or physiological need to eat, caused by a release of hormones from the digestive tract. LESSON
Role of gastrointestinal factors in hunger and satiety in man
 Proceedings of the Nutrition Society (1992) 51, 7-11 7 Role of gastrointestinal factors in hunger and satiety in man BY N. W. READ Centre for Human Nutrition, University of Shefield, Northern General Hospital,
Proceedings of the Nutrition Society (1992) 51, 7-11 7 Role of gastrointestinal factors in hunger and satiety in man BY N. W. READ Centre for Human Nutrition, University of Shefield, Northern General Hospital,
Human pancreatic exocrine response to nutrients in health and disease
 vi1 REVIEW Human pancreatic exocrine response to nutrients in health and disease J Keller, P Layer... See end of article for authors affiliations... Correspondence to: Dr J Keller, Israelitic Hospital,
vi1 REVIEW Human pancreatic exocrine response to nutrients in health and disease J Keller, P Layer... See end of article for authors affiliations... Correspondence to: Dr J Keller, Israelitic Hospital,
Oat beta glucan: Multiple roles in the gut. A.R. Mackie, B.H. Bajka, B. Kirkhus
 Oat beta glucan: Multiple roles in the gut A.R. Mackie, B.H. Bajka, B. Kirkhus Introduction Food is consumed Food resides in the stomach Chyme is gradually emptied into the duodenum Can oat beta glucan
Oat beta glucan: Multiple roles in the gut A.R. Mackie, B.H. Bajka, B. Kirkhus Introduction Food is consumed Food resides in the stomach Chyme is gradually emptied into the duodenum Can oat beta glucan
Bone Metabolism in Postmenopausal Women Influenced by the Metabolic Syndrome
 Bone Metabolism in Postmenopausal Women Influenced by the Metabolic Syndrome Thomas et al. Nutrition Journal (2015) 14:99 DOI 10.1186/s12937-015-0092-2 RESEARCH Open Access Acute effect of a supplemented
Bone Metabolism in Postmenopausal Women Influenced by the Metabolic Syndrome Thomas et al. Nutrition Journal (2015) 14:99 DOI 10.1186/s12937-015-0092-2 RESEARCH Open Access Acute effect of a supplemented
Recent results of the research into the possible contribution of whey powders in the fight against obesity. David J Baer, PhD
 Recent results of the research into the possible contribution of whey powders in the fight against obesity David J Baer, PhD Beltsville Human Nutrition Research Center Funded by USDA, ARS and the Whey
Recent results of the research into the possible contribution of whey powders in the fight against obesity David J Baer, PhD Beltsville Human Nutrition Research Center Funded by USDA, ARS and the Whey
Megan Lawless. Journal Club. January 20 th, 2011
 Megan Lawless Journal Club January 20 th, 2011 Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1 Proceedings of the National Academy of Sciences September 2007 Abstract
Megan Lawless Journal Club January 20 th, 2011 Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1 Proceedings of the National Academy of Sciences September 2007 Abstract
Appetite, Glycemia and Entero-Insular Hormone Responses Differ Between Oral, Gastric-Remnant and Duodenal Administration of a Mixed Meal Test After
 Appetite, Glycemia and Entero-Insular Hormone Responses Differ Between Oral, Gastric-Remnant and Duodenal Administration of a Mixed Meal Test After Roux-en-Y Gastric Bypass June 2018 How a surgical complication
Appetite, Glycemia and Entero-Insular Hormone Responses Differ Between Oral, Gastric-Remnant and Duodenal Administration of a Mixed Meal Test After Roux-en-Y Gastric Bypass June 2018 How a surgical complication
Gastric Emptying and Release of Incretin Hormones after Glucose Ingestion in Humans
 Gastric Emptying and Release of Incretin Hormones after Glucose Ingestion in Humans Jörg Schirra, Martin Katschinski, Claudia Weidmann, Thomas Schäfer, Uwe Wank, Rudolf Arnold, and Burkhard Göke Clinical
Gastric Emptying and Release of Incretin Hormones after Glucose Ingestion in Humans Jörg Schirra, Martin Katschinski, Claudia Weidmann, Thomas Schäfer, Uwe Wank, Rudolf Arnold, and Burkhard Göke Clinical
Formulation and development of foods for weight management. Paola Vitaglione
 Formulation and development of foods for weight management Paola Vitaglione Weight control and energy balance Weight gain Weight maintenance Weight loss ENERGY IN ENERGY OUT Food intake: Carbohydrates
Formulation and development of foods for weight management Paola Vitaglione Weight control and energy balance Weight gain Weight maintenance Weight loss ENERGY IN ENERGY OUT Food intake: Carbohydrates
Interaction of insulin, glucagon-like peptide 1, gastric inhibitory polypeptide, and appetite in response to intraduodenal carbohydrate 1 3
 Interaction of insulin, glucagon-like peptide 1, gastric inhibitory polypeptide, and appetite in response to intraduodenal carbohydrate 1 3 Jacquelynne H Lavin, Gary A Wittert, Jane Andrews, Bu Yeap, Judith
Interaction of insulin, glucagon-like peptide 1, gastric inhibitory polypeptide, and appetite in response to intraduodenal carbohydrate 1 3 Jacquelynne H Lavin, Gary A Wittert, Jane Andrews, Bu Yeap, Judith
Dietary fiber is defend as the edible parts of plant or analogous carbohydrates
 Chengcheng Jia NUTR 417 Supplement Paper The Soluble Dietary Fiber: Inulin Introduction and Supplement Background: Dietary fiber is defend as the edible parts of plant or analogous carbohydrates that are
Chengcheng Jia NUTR 417 Supplement Paper The Soluble Dietary Fiber: Inulin Introduction and Supplement Background: Dietary fiber is defend as the edible parts of plant or analogous carbohydrates that are
This version is available:
 RADAR Research Archive and Digital Asset Repository Korakianiti, A, Hillier, S and Clegg, M The impact of the cephalic phase on postprandial blood glucose and satiety Korakianiti, A, Hillier, S and Clegg,
RADAR Research Archive and Digital Asset Repository Korakianiti, A, Hillier, S and Clegg, M The impact of the cephalic phase on postprandial blood glucose and satiety Korakianiti, A, Hillier, S and Clegg,
Lecture 3: Digestion and Dieting Physiology
 This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike License. Your use of this material constitutes acceptance of that license and the conditions of use of materials on this
Why would fatty foods aggravate the patient s RUQ pain? What effect does cholecystokinin (CCK) have on gastric emptying?
 CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
CASE 28 A 43-year-old woman presents to the emergency department with the acute onset of abdominal pain. Her pain is located to the right upper quadrant (RUQ) and radiates to the right shoulder. She reports
Gut hormones KHATTAB
 Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
Gut hormones PROF:ABD ALHAFIZ HASSAN KHATTAB Gut as an endocrine gland The talk will cover the following : Historical background. Why this subject is chosen. Gastro-intestinal hormones and their function.
Bariatric Surgery MM /11/2001. HMO; PPO; QUEST 05/01/2012 Section: Surgery Place(s) of Service: Outpatient; Inpatient
 Bariatric Surgery Policy Number: Original Effective Date: MM.06.003 09/11/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 05/01/2012 Section: Surgery Place(s) of Service: Outpatient;
Bariatric Surgery Policy Number: Original Effective Date: MM.06.003 09/11/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 05/01/2012 Section: Surgery Place(s) of Service: Outpatient;
The Small Intestine. The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine.
 The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
The Small Intestine The pyloric sphincter at the bottom of the stomach opens, squirting small amounts of food into your small intestine. approximately six metres (the longest section of your digestive
Lecture 1 - Energy Balance: Concepts, Behaviour, Physiology & the Environment
 PHY3102 THEME 1 (Lectures 1-5) - Nutrition, Digestion and Absorption Lecture 1 - Energy Balance: Concepts, Behaviour, Physiology & the Environment Overview: - Lectures 1 and 2 will introduce the concept
PHY3102 THEME 1 (Lectures 1-5) - Nutrition, Digestion and Absorption Lecture 1 - Energy Balance: Concepts, Behaviour, Physiology & the Environment Overview: - Lectures 1 and 2 will introduce the concept
Digestion: Endocrinology of Appetite
 Digestion: Endocrinology of Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one on one relationship with a qualified health care professional
Digestion: Endocrinology of Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one on one relationship with a qualified health care professional
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
The Effects of Dairy on Subjective Appetite and Post-prandial Glycemia Harvey Anderson University of Toronto
 The Effects of Dairy on Subjective Appetite and Post-prandial Glycemia Harvey Anderson University of Toronto Dairy Research Symposium 2018: Transferring Results for Action February 9, 2018 Château Laurier
The Effects of Dairy on Subjective Appetite and Post-prandial Glycemia Harvey Anderson University of Toronto Dairy Research Symposium 2018: Transferring Results for Action February 9, 2018 Château Laurier
8/27/2012. Mississippi s Big Problem. An Epidemic Now Reaching Our Children. What Can We Do?
 Mississippi s Big Problem. An Epidemic Now Reaching Our Children What Can We Do? Richard D. deshazo, MD Billy S. Guyton Distinguished Professor Professor of Medicine & Pediatrics University of Mississippi
Mississippi s Big Problem. An Epidemic Now Reaching Our Children What Can We Do? Richard D. deshazo, MD Billy S. Guyton Distinguished Professor Professor of Medicine & Pediatrics University of Mississippi
PUBLISHED VERSION Baishideng Publishing Group Co., Limited. All rights reserved.
 PUBLISHED VERSION Deane, Adam Matthew; Besanko, Laura K.; Burgstad, Carly M.; Chapman, Marianne J.; Horowitz, Michael; Fraser, Robert John Lovat Modulation of individual components of gastric motor response
PUBLISHED VERSION Deane, Adam Matthew; Besanko, Laura K.; Burgstad, Carly M.; Chapman, Marianne J.; Horowitz, Michael; Fraser, Robert John Lovat Modulation of individual components of gastric motor response
THE EFFECT OF BREAKFAST CONSUMPTION ON THE ACUTE RESPONSE OF PLASMA ACYLATED-GHRELIN AND GLUCAGON-LIKE PEPTIDE 1 CONCENTRATIONS IN ADULT WOMEN
 THE EFFECT OF BREAKFAST CONSUMPTION ON THE ACUTE RESPONSE OF PLASMA ACYLATED-GHRELIN AND GLUCAGON-LIKE PEPTIDE 1 CONCENTRATIONS IN ADULT WOMEN by Thomas A. Hritz, MS, RD, LDN B.S., University of Pittsburgh,
THE EFFECT OF BREAKFAST CONSUMPTION ON THE ACUTE RESPONSE OF PLASMA ACYLATED-GHRELIN AND GLUCAGON-LIKE PEPTIDE 1 CONCENTRATIONS IN ADULT WOMEN by Thomas A. Hritz, MS, RD, LDN B.S., University of Pittsburgh,
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
Soy Protein. Muscle health benefits: for Sports Nutrition Recovery and during aging. May 9, Mark Cope, PhD
 Soy Protein Muscle health benefits: for Sports Nutrition Recovery and during aging May 9, 2017 Mark Cope, PhD Blending Proteins to Provide Better Muscle Health Importance of Muscle Health The Benefits
Soy Protein Muscle health benefits: for Sports Nutrition Recovery and during aging May 9, 2017 Mark Cope, PhD Blending Proteins to Provide Better Muscle Health Importance of Muscle Health The Benefits
Short-term effects of altering the dietary carbohydrate to fat ratio on circulating leptin and satiety in women
 University of Wollongong Research Online University of Wollongong Thesis Collection 1954-2016 University of Wollongong Thesis Collections 2004 Short-term effects of altering the dietary carbohydrate to
University of Wollongong Research Online University of Wollongong Thesis Collection 1954-2016 University of Wollongong Thesis Collections 2004 Short-term effects of altering the dietary carbohydrate to
Non-nutritive sweeteners: no class effect on the glycemic or appetite responses to ingested glucose
 Europe PMC Funders Group Author Manuscript Published in final edited form as: Eur J Clin Nutr. 2014 May ; 68(5): 629 631. doi:10.1038/ejcn.2014.19. Non-nutritive sweeteners: no class effect on the glycemic
Europe PMC Funders Group Author Manuscript Published in final edited form as: Eur J Clin Nutr. 2014 May ; 68(5): 629 631. doi:10.1038/ejcn.2014.19. Non-nutritive sweeteners: no class effect on the glycemic
Bio& 242 Unit 1 / Lecture 4
 Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Bio& 242 Unit 1 / Lecture 4 system: Gastric hormones GASTRIN: Secretion: By enteroendocrine (G) in gastric pits of the mucosa. Stimulus: Stomach distention and acid ph of chyme causes Gastrin. Action:
Physiology Unit 4 DIGESTIVE PHYSIOLOGY
 Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
Physiology Unit 4 DIGESTIVE PHYSIOLOGY In Physiology Today Functions Motility Ingestion Mastication Deglutition Peristalsis Secretion 7 liters/day! Exocrine/endocrine Digestion Absorption Digestion of
The Role of Protein in Weight Management: A Biochemist s Perspective
 diet and health The Role of Protein in Weight Management: A Biochemist s Perspective Elaine S. Krul Overview Protein, as a macronutrient, functions at a molecular level in the body to impact metabolic
diet and health The Role of Protein in Weight Management: A Biochemist s Perspective Elaine S. Krul Overview Protein, as a macronutrient, functions at a molecular level in the body to impact metabolic
Elizabeth Garrison. Fall A critical Literature Review submitted in partial fulfillment of the requirements for the Senior Research Thesis.
 A summary of Richard Mattes research since 2005: Effects of food form, feeding patterns, and specific nutrients on appetite, satiety, and metabolic responses in humans Elizabeth Garrison Fall 2011 A critical
A summary of Richard Mattes research since 2005: Effects of food form, feeding patterns, and specific nutrients on appetite, satiety, and metabolic responses in humans Elizabeth Garrison Fall 2011 A critical
EAT TO LIVE: THE ROLE OF THE PANCREAS. Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008
 EAT TO LIVE: THE ROLE OF THE PANCREAS Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008 THE ROLE OF THE PANCREAS Exocrine pancreas Endocrine pancreas THE ROLE OF THE PANCREAS EXOCRINE
EAT TO LIVE: THE ROLE OF THE PANCREAS Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008 THE ROLE OF THE PANCREAS Exocrine pancreas Endocrine pancreas THE ROLE OF THE PANCREAS EXOCRINE
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE. CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010
 Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Practical Strategies for the Clinical Use of Incretin Mimetics CME/CE Robert R. Henry, MD Authors and Disclosures CME/CE Released: 09/15/2009; Valid for credit through 09/15/2010 Introduction Type 2 diabetes
Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, ,
 IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
IDP Biological Systems Gastrointestinal System Section Coordinator: Jerome W. Breslin, PhD, Assistant Professor of Physiology, MEB 7208, 504-568-2669, jbresl@lsuhsc.edu Overall Learning Objectives 1. Characterize
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption),
 Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Normal Fuel Metabolism Five phases of fuel homeostasis have been described A. Phase I is the fed state (0 to 3.9 hours after meal/food consumption), in which blood glucose predominantly originates from
Asma Karameh. -Shatha Al-Jaberi محمد خطاطبة -
 -2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
-2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
Developing nations vs. developed nations Availability of food contributes to overweight and obesity
 KNH 406 1 Developing nations vs. developed nations Availability of food contributes to overweight and obesity Intake Measured in kilojoules (kj) or kilocalories (kcal) - food energy Determined by bomb
KNH 406 1 Developing nations vs. developed nations Availability of food contributes to overweight and obesity Intake Measured in kilojoules (kj) or kilocalories (kcal) - food energy Determined by bomb
Comparative effects of small intestinal glucose on blood pressure, heart rate, and noradrenaline responses in obese and healthy subjects
 ORIGINAL RESEARCH Physiological Reports ISSN 251-817X Comparative effects of small intestinal glucose on blood pressure, heart rate, and noradrenaline responses in obese and healthy subjects Laurence G.
ORIGINAL RESEARCH Physiological Reports ISSN 251-817X Comparative effects of small intestinal glucose on blood pressure, heart rate, and noradrenaline responses in obese and healthy subjects Laurence G.
MIREIA LORENZO-FIGUERAS
 EFFECTS OF HIGH-FAT vs. HIGH-CARBOHYDRATE DIETS ON PROXIMAL GASTRIC RELAXATION, GASTRIC EMPTYING, ph OF GASTRIC CONTENTS AND PLASMA CHOLECYSTOKININ IN THE HORSE By MIREIA LORENZO-FIGUERAS A DISSERTATION
EFFECTS OF HIGH-FAT vs. HIGH-CARBOHYDRATE DIETS ON PROXIMAL GASTRIC RELAXATION, GASTRIC EMPTYING, ph OF GASTRIC CONTENTS AND PLASMA CHOLECYSTOKININ IN THE HORSE By MIREIA LORENZO-FIGUERAS A DISSERTATION
Digestive System Module 4: The Stomach *
 OpenStax-CNX module: m49286 1 Digestive System Module 4: The * Donna Browne Based on The by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0
OpenStax-CNX module: m49286 1 Digestive System Module 4: The * Donna Browne Based on The by OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 4.0
The Science of Protein. The Continued Exploration of the Impact of High-Quality Protein on Optimal Health
 The Science of Protein The Continued Exploration of the Impact of High-Quality Protein on Optimal Health 1 The Following Will Be Discussed 1. What is Protein? 2. Evolution of Protein Research 3. Protein
The Science of Protein The Continued Exploration of the Impact of High-Quality Protein on Optimal Health 1 The Following Will Be Discussed 1. What is Protein? 2. Evolution of Protein Research 3. Protein
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
Chapter 20 The Digestive System Exam Study Questions
 Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
Chapter 20 The Digestive System Exam Study Questions 20.1 Overview of GI Processes 1. Describe the functions of digestive system. 2. List and define the four GI Processes: 20.2 Functional Anatomy of the
STUDY OVERVIEW KEY TAKEAWAYS
 Avocado fruit on postprandial markers of cardio-metabolic risk: A randomized controlled dose response trial in overweight and obese men and women Britt Burton-Freeman, Eunyoung Park, Indika Edirisinghe
Avocado fruit on postprandial markers of cardio-metabolic risk: A randomized controlled dose response trial in overweight and obese men and women Britt Burton-Freeman, Eunyoung Park, Indika Edirisinghe
Role of the proximal and distal stomach in mixed solid and liquid meal emptying
 Gut, 1991,32,615-619 Departments of Nuclear Medicine, Medicine, and Gastroenterology, Royal Adelaide Hospital, Adelaide, South Australia P J Collins M Horowitz B E Chatterton R Heddle J Dent Subdepartment
Gut, 1991,32,615-619 Departments of Nuclear Medicine, Medicine, and Gastroenterology, Royal Adelaide Hospital, Adelaide, South Australia P J Collins M Horowitz B E Chatterton R Heddle J Dent Subdepartment
Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences
 Supplemental Data Dual stable-isotope experiment Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences across the forearm, adjusted for forearm blood flow (FBF) (1).
Supplemental Data Dual stable-isotope experiment Skeletal muscle metabolism was studied by measuring arterio-venous concentration differences across the forearm, adjusted for forearm blood flow (FBF) (1).
The Role of Protein in Weight Management: A Biochemist s Perspective
 The Role of Protein in Weight Management: A Biochemist s Perspective Elaine S. Krul, PhD Global Nutrition Solae LLC, St. Louis, MO American Meat Science Association Reciprocal Meat Conference, June 18,
The Role of Protein in Weight Management: A Biochemist s Perspective Elaine S. Krul, PhD Global Nutrition Solae LLC, St. Louis, MO American Meat Science Association Reciprocal Meat Conference, June 18,
MEDICAL POLICY: Enteral and Parenteral Nutrition
 POLICY: PG0114 ORIGINAL EFFECTIVE: 02/15/07 LAST REVIEW: 08/14/18 MEDICAL POLICY: Enteral and Parenteral Nutrition GUIDELINES This policy does not certify benefits or authorization of benefits, which is
POLICY: PG0114 ORIGINAL EFFECTIVE: 02/15/07 LAST REVIEW: 08/14/18 MEDICAL POLICY: Enteral and Parenteral Nutrition GUIDELINES This policy does not certify benefits or authorization of benefits, which is
Ertugliflozin (Steglatro ) 5 mg daily. May increase to 15 mg daily. Take in the morning +/- food. < 60: Do not initiate; discontinue therapy
 Sodium-glucose Cotransporter-2 (SGLT2) s Inhibit SGLT in proximal renal tubules, reducing reabsorption of filtered glucose from tubular lumen Lowers renal threshold for glucose à increase urinary excretion
Sodium-glucose Cotransporter-2 (SGLT2) s Inhibit SGLT in proximal renal tubules, reducing reabsorption of filtered glucose from tubular lumen Lowers renal threshold for glucose à increase urinary excretion
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
Cross-Matches for Bioequivalence Evaluation Division using Needle Free Jet Injector (Comfort-In) and conventional Pen type syringe.
 Cross-Matches for Bioequivalence Evaluation Division using Needle Free Jet Injector (Comfort-In) and conventional Pen type syringe. Dr. EunJig, Lee http://www.yuhs.or.kr/en/hospitals/severance/clinic_dept/endo_dept/phy_directory/docprofile.asp?sno=1734
Cross-Matches for Bioequivalence Evaluation Division using Needle Free Jet Injector (Comfort-In) and conventional Pen type syringe. Dr. EunJig, Lee http://www.yuhs.or.kr/en/hospitals/severance/clinic_dept/endo_dept/phy_directory/docprofile.asp?sno=1734
Chapter 12. Ingestive Behavior
 Chapter 12 Ingestive Behavior Drinking a. fluid compartments b. osmometric thirst c. volumetric thirst Eating a. energy sources b. starting a meal c. stopping a meal d. eating disordersd Drinking a. fluid
Chapter 12 Ingestive Behavior Drinking a. fluid compartments b. osmometric thirst c. volumetric thirst Eating a. energy sources b. starting a meal c. stopping a meal d. eating disordersd Drinking a. fluid
Short Bowel Syndrome: Medical management
 Short Bowel Syndrome: Medical management La Sindrome dell'intestino Corto in età pediatrica Brescia 18 marzo 2011 Jon A.Vanderhoof, M.D. Division of Pediatric GI Harvard Medical School Children s Hospital,
Short Bowel Syndrome: Medical management La Sindrome dell'intestino Corto in età pediatrica Brescia 18 marzo 2011 Jon A.Vanderhoof, M.D. Division of Pediatric GI Harvard Medical School Children s Hospital,
The role of proteins and amino acids in food intake and satiety
 The role of proteins and amino acids in food intake and satiety Daniel TOME AGROPARISTECH Departement of Life Sciences and Health INRA, UMR914 Nutrition physiology and ingestive behavior, Paris, France
The role of proteins and amino acids in food intake and satiety Daniel TOME AGROPARISTECH Departement of Life Sciences and Health INRA, UMR914 Nutrition physiology and ingestive behavior, Paris, France
POSTPRANDIAL hypotension, defined as a fall in
 Journal of Gerontology: MEDICAL SCIENCES 2005, Vol. 60A, No. 7, 940 946 Copyright 2005 by The Gerontological Society of America Intraduodenal Guar Attenuates the Fall in Blood Pressure Induced by Glucose
Journal of Gerontology: MEDICAL SCIENCES 2005, Vol. 60A, No. 7, 940 946 Copyright 2005 by The Gerontological Society of America Intraduodenal Guar Attenuates the Fall in Blood Pressure Induced by Glucose
University of Buea. Faculty of Health Sciences. Programme in Medicine
 Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
Faculty of Health Sciences University of Buea Wednesday, 28 th January 2009 Time: 8 00-10 00 Programme in Medicine MED 303 (Gastrointestinal Physiology) EXAMS (2008-2009) Identify the letter of the choice
PHARMACOLOGY AND THERAPEUTICS. novel mechanism by which exenatide can attenuate postprandial glycemia.
 Diabetes Volume 65, January 2016 269 Sony S. Thazhath, 1,2 Chinmay S. Marathe, 1,2 Tongzhi Wu, 1,2 Jessica Chang, 1,2 Joan Khoo, 1,2 Paul Kuo, 1,2,3 Helen L. Checklin, 1,2 Michelle J. Bound, 1,2 Rachael
Diabetes Volume 65, January 2016 269 Sony S. Thazhath, 1,2 Chinmay S. Marathe, 1,2 Tongzhi Wu, 1,2 Jessica Chang, 1,2 Joan Khoo, 1,2 Paul Kuo, 1,2,3 Helen L. Checklin, 1,2 Michelle J. Bound, 1,2 Rachael
SPHINCTER OF ODDI DYSFUNCTION (SOD)
 SPHINCTER OF ODDI DYSFUNCTION (SOD) Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice
SPHINCTER OF ODDI DYSFUNCTION (SOD) Sphincter of Oddi dysfunction refers to structural or functional disorders involving the biliary sphincter that may result in impedance of bile and pancreatic juice
Index. Page references in bold refer to figures and page references in italic refer to tables.
 Page references in bold refer to figures and page references in italic refer to tables. Adrenaline, high-fat response in post-obese 142 Alcohol absorption 11-12 balance equation 17 and obesity 10-11 thermogenesis
Page references in bold refer to figures and page references in italic refer to tables. Adrenaline, high-fat response in post-obese 142 Alcohol absorption 11-12 balance equation 17 and obesity 10-11 thermogenesis
Gastric and Small Intestinal Determinants of. Postprandial Blood Pressure and Glycaemia
 Gastric and Small Intestinal Determinants of Postprandial Blood Pressure and Glycaemia Thesis by Laurence Trahair B HSc (Hons), B Med Rad (Nuc Med) For the Degree of Doctor of Philosophy Discipline of
Gastric and Small Intestinal Determinants of Postprandial Blood Pressure and Glycaemia Thesis by Laurence Trahair B HSc (Hons), B Med Rad (Nuc Med) For the Degree of Doctor of Philosophy Discipline of
EVects of glucagon-like peptide-1(7-36)amide on antro-pyloro-duodenal motility in the interdigestive state and with duodenal lipid perfusion in humans
 Gut ;: 31 Clinical Research Unit for Gastrointestinal Endocrinology and Department of Gastroenterology and Endocrinology, Philipps-University, Marburg, Germany J Schirra P Houck U Wank R Arnold M Katschinski
Gut ;: 31 Clinical Research Unit for Gastrointestinal Endocrinology and Department of Gastroenterology and Endocrinology, Philipps-University, Marburg, Germany J Schirra P Houck U Wank R Arnold M Katschinski
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation. Introduction. Predisposing factor. Introduction.
 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Physiology 12. Overview. The Gastrointestinal Tract. Germann Ch 19
 Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Physiology 12 The Gastrointestinal Tract Germann Ch 19 Overview 1 Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Glossary. acute PEM protein-energy malnutrition caused by recent severe food restriction; characterized in children by thinness for height (wasting).
 Glossary Protein acidosis above-normal acidity in the blood and body fluids. acids compounds that release hydrogen ions in a solution. acute PEM protein-energy malnutrition caused by recent severe food
Glossary Protein acidosis above-normal acidity in the blood and body fluids. acids compounds that release hydrogen ions in a solution. acute PEM protein-energy malnutrition caused by recent severe food
British Journal of Nutrition
 (211), 15, 1644 1651 q The Authors 211 doi:1.117/s7114515489 Comparative effects of glucose and xylose on blood pressure, gastric emptying and incretin hormones in healthy older subjects Lora Vanis 1,2,
(211), 15, 1644 1651 q The Authors 211 doi:1.117/s7114515489 Comparative effects of glucose and xylose on blood pressure, gastric emptying and incretin hormones in healthy older subjects Lora Vanis 1,2,
Targeted Nutrition Therapy Nutrition Masters Course
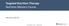 Targeted Nutrition Therapy Nutrition Masters Course Nilima Desai, MPH, RD Learning Objectives Review clinical studies on innovative, targeted nutrition therapies for: o Blood glucose management o Dyslipidemia
Targeted Nutrition Therapy Nutrition Masters Course Nilima Desai, MPH, RD Learning Objectives Review clinical studies on innovative, targeted nutrition therapies for: o Blood glucose management o Dyslipidemia
Gastrointestinal mediation of glucose homeostasis and postprandial cardiovascular risk
 Gastrointestinal mediation of glucose homeostasis and postprandial cardiovascular risk A thesis submitted by Dr Sony Sebastian Thazhath MBBS, MD For the degree of Doctor of Philosophy Discipline of Medicine
Gastrointestinal mediation of glucose homeostasis and postprandial cardiovascular risk A thesis submitted by Dr Sony Sebastian Thazhath MBBS, MD For the degree of Doctor of Philosophy Discipline of Medicine
British Journal of Nutrition
 (2009), 101, 1094 1102 q The Authors 2008 doi:10.1017/s0007114508042372 Reproducibility of energy intake, gastric emptying, blood glucose, plasma insulin and cholecystokinin responses in healthy young
(2009), 101, 1094 1102 q The Authors 2008 doi:10.1017/s0007114508042372 Reproducibility of energy intake, gastric emptying, blood glucose, plasma insulin and cholecystokinin responses in healthy young
Parenteral and Enteral Nutrition
 Parenteral and Enteral Nutrition Audis Bethea, Pharm.D. Assistant Professor Therapeutics I December 5 & 9, 2003 Parenteral Nutrition Definition process of supplying nutrients via the intravenous route
Parenteral and Enteral Nutrition Audis Bethea, Pharm.D. Assistant Professor Therapeutics I December 5 & 9, 2003 Parenteral Nutrition Definition process of supplying nutrients via the intravenous route
Nutrition Support Calculations Brianne Squires
 Nutrition Support Calculations Brianne Squires 1. Determine the following for Ensure at 68 ml/hour (Note: when working with volumes of formula for enteral formula, it is expressed in total volume/ml not
Nutrition Support Calculations Brianne Squires 1. Determine the following for Ensure at 68 ml/hour (Note: when working with volumes of formula for enteral formula, it is expressed in total volume/ml not
Effects of Glucagon-like Peptide-1-(7-36)amide (GLP-1) on Gastric Motor Function in Health and Diabetes: Potential Mechanism of Action
 Effects of Glucagon-like Peptide-1-(7-36)amide (GLP-1) on Gastric Motor Function in Health and Diabetes: Potential Mechanism of Action Doctoral thesis submitted to the Autonomous University of Barcelona
Effects of Glucagon-like Peptide-1-(7-36)amide (GLP-1) on Gastric Motor Function in Health and Diabetes: Potential Mechanism of Action Doctoral thesis submitted to the Autonomous University of Barcelona
Overview. Physiology 1. The Gastrointestinal Tract. Guyton section XI
 Overview Physiology 1 The Gastrointestinal Tract Guyton section XI Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Overview Physiology 1 The Gastrointestinal Tract Guyton section XI Basic functions of the GI tract Digestion Secretion Absorption Motility Basic functions of the GI tract Digestion: : Dissolving and breaking
Home Total Parenteral Nutrition for Adults
 Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
Home Total Parenteral Nutrition for Adults Policy Number: Original Effective Date: MM.08.007 05/21/1999 Line(s) of Business: Current Effective Date: PPO, HMO, QUEST Integration 05/27/2016 Section: Home
PARENTERAL NUTRITION THERAPY
 UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
UnitedHealthcare Benefits of Texas, Inc. 1. UnitedHealthcare of Oklahoma, Inc. 2. UnitedHealthcare of Oregon, Inc. UnitedHealthcare of Washington, Inc. UnitedHealthcare West BENEFIT INTERPRETATION POLICY
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Drugs used in Diabetes. Dr Andrew Smith
 Drugs used in Diabetes Dr Andrew Smith Plan Introduction Insulin Sensitising Drugs: Metformin Glitazones Insulin Secretagogues: Sulphonylureas Meglitinides Others: Acarbose Incretins Amylin Analogues Damaglifozin
Drugs used in Diabetes Dr Andrew Smith Plan Introduction Insulin Sensitising Drugs: Metformin Glitazones Insulin Secretagogues: Sulphonylureas Meglitinides Others: Acarbose Incretins Amylin Analogues Damaglifozin
Substrates in clinical nutrition Ilze Jagmane
 Substrates in clinical nutrition Ilze Jagmane Latvian Society of Parenteral and Enteral Nutrition September, 2013 Introduction Food contains one or more of the following nutrients: Water Carbohydrate Lipids
Substrates in clinical nutrition Ilze Jagmane Latvian Society of Parenteral and Enteral Nutrition September, 2013 Introduction Food contains one or more of the following nutrients: Water Carbohydrate Lipids
EVALUATION OF A SATIETY HORMONE IN PIGS WITH DIVERGENT GENETIC POTENTIAL FOR FEED INTAKE AND GROWTH
 EVALUATION OF A SATIETY HORMONE IN PIGS WITH DIVERGENT GENETIC POTENTIAL FOR FEED INTAKE AND GROWTH A.C. Clutter 1, R. Jiang 2, J.P. McCann 3 and D.S. Buchanan 4 Story in Brief Experiments were designed
EVALUATION OF A SATIETY HORMONE IN PIGS WITH DIVERGENT GENETIC POTENTIAL FOR FEED INTAKE AND GROWTH A.C. Clutter 1, R. Jiang 2, J.P. McCann 3 and D.S. Buchanan 4 Story in Brief Experiments were designed
Follow this and additional works at: Part of the Human Ecology Commons
 Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2012 Comparison of the Effects of Two Oat-based Cereals on Appetite and Satiety, and the Effect of a Fat Emulsion of Appetite,
Louisiana State University LSU Digital Commons LSU Master's Theses Graduate School 2012 Comparison of the Effects of Two Oat-based Cereals on Appetite and Satiety, and the Effect of a Fat Emulsion of Appetite,
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc
 Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
Effect of changing lipid formulation in Parenteral Nutrition in the Newborn Experimental Pathology BSc Word count: 6939 0 CONTENTS Abstract...2 Acknowledgements...3 Introduction...4 Materials and Methods...11
(*) (*) Ingestion, digestion, absorption, and elimination. Uptake of nutrients by body cells (intestine)
 Human Digestive System Food is pushed along the digestive tract by peristalsis the rhythmic waves of contraction of smooth muscles in the wall of the canal Accessory glands. Main stages of food processing
Human Digestive System Food is pushed along the digestive tract by peristalsis the rhythmic waves of contraction of smooth muscles in the wall of the canal Accessory glands. Main stages of food processing
