Vitamin D: a negative endocrine regulator of the renin angiotensin system and blood pressure
|
|
|
- Allen Houston
- 5 years ago
- Views:
Transcription
1 Journal of Steroid Biochemistry & Molecular Biology (2004) Vitamin D: a negative endocrine regulator of the renin angiotensin system and blood pressure Yan Chun Li a,, Guilin Qiao a, Milan Uskokovic b, Wei Xiang a, Wei Zheng a, Juan Kong a a Department of Medicine, University of Chicago, MC 4076, 5841 S. Maryland Avenue, Chicago, IL 60637, USA b BioXell Inc., Nutley, NJ 07110, USA Abstract The renin angiotensin system (RAS) plays a central role in the regulation of blood pressure, volume and electrolyte homeostasis. Inappropriate activation of the RAS may lead to hypertension. Clinical and epidemiological studies have suggested a correlation between Vitamin D-deficiency and high blood pressure. Our recent studies demonstrate that Vitamin D is a potent endocrine suppressor of renin biosynthesis to regulate the RAS. Mice lacking the Vitamin D receptor (VDR) have elevated production of renin and angiotensin (Ang) II, leading to hypertension, cardiac hypertrophy and increased water intake. These abnormalities can be prevented by treatment with an ACE inhibitor or AT 1 receptor antagonist. Vitamin D repression of renin expression is independent of calcium metabolism, the volume- and salt-sensing mechanisms and the Ang II feedback regulation. In normal mice, Vitamin D-deficiency stimulates renin expression, whereas injection of 1,25-dihydroxyvitamin D 3 [1,25(OH) 2 D 3 ] reduces renin synthesis. In cell cultures, 1,25(OH) 2 D 3 directly suppresses renin gene transcription by a VDR-dependent mechanism. Furthermore, we have found that Gemini compounds have more potent renin-suppressing activity than 1,25(OH) 2 D 3. Collectively, our studies reveal a critical role of the Vitamin D endocrine system in the regulation of blood pressure and volume homeostasis, and suggest that low calcemic Vitamin D analogs may potentially be developed into a new class of anti-hypertensive agents to control renin production and blood pressure Elsevier Ltd. All rights reserved. Keywords: Vitamin D; Vitamin D analogs; Renin; Angiotensin; Hypertension 1. Introduction It is long established that the primary physiological role of the Vitamin D endocrine system is to regulate calcium homeostasis by regulating intestinal and renal calcium transport and bone mineralization [1]. As the most active metabolite of Vitamin D, 1,25-dihydroxyvitamin D 3 [1,25(OH) 2 D 3 ] is responsible for most of the biological actions of the Vitamin D endocrine system, which are mediated by the Vitamin D receptor (VDR), a member of the nuclear receptor superfamily [2]. Since VDR is also widely expressed in tissues not involved in calcium metabolism, it is believed that the Vitamin D endocrine system has additional physiological functions beyond calcium homeostasis. This notion is confirmed by recent studies from many laboratories. For example, studies using genetically mutant mice that lack VDR or 25-hydroxyvitamin D 3 1 -hydroxylase, the rate-limiting enzyme for 1,25(OH) 2 D 3 biosynthesis, show Presented at the 12th Workshop on Vitamin D (Maastricht, The Netherlands, 6 10 July 2003). Corresponding author. Tel.: ; fax: address: cyan@medicine.bsd.uchicago.edu (Y.C. Li). that Vitamin D/VDR regulate not only calcium homeostasis as expected, but also immune responses, reproduction, mammary gland development and hair growth [3 7]. Our recent works demonstrate that 1,25(OH) 2 D 3 also functions as a negative endocrine regulator of the renin angiotensin system (RAS) and thus plays an important role in the regulation of the renocardiovascular functions [8,9]. 2. The renin angiotensin system The RAS is a regulatory cascade that plays an essential role in the regulation of blood pressure, electrolyte and volume homeostasis. Inappropriate stimulation of the RAS has been associated with hypertension. Renin, an aspartyl protease, is the rate-limiting component of the RAS. Its main function is to cleave a 10 amino acid peptide, angiotensin (Ang) I, from angiotensinogen. Ang I is then converted to the octapeptide Ang II by the angiotensin-converting enzyme (ACE), which primarily resides in endothelial cells in blood vessels. Ang II is the central effector of the RAS. Through interacting with Ang II receptors [10] in different tissues, including the brain, heart, kidney, adrenal glands /$ see front matter 2004 Elsevier Ltd. All rights reserved. doi: /j.jsbmb
2 388 Y.C. Li et al. / Journal of Steroid Biochemistry & Molecular Biology (2004) Fig. 1. The renin angiotensin system. ADH, anti-diuretic hormone, also known as vasopressin; ACE, angiotensin-converting enzyme. and peripheral vasculature, Ang II exerts diverse physiological responses that influence the electrolyte and extracellular volume balance and blood pressure (Fig. 1) [11]. In addition, local RAS has been found in tissues such as the kidney, heart and brain, among others [12], the physiological relevance of which remains to be determined. Adding a new level of complexity to the RAS, recently a renin receptor has been reported in the heart, kidney, brain, placenta and liver, which may function to increase the catalytic activity of renin [13], and an ACE homologue, ACE2, has been isolated [14,15] and found to play an essential role in heart functions [16]. Renin is predominantly produced and secreted by special granulated smooth muscle cells located in the afferent glomerular arterioles in the juxtaglomerular (JG) apparatus of the kidney [17]. Secretion of renin from the granulated smooth muscle cells, term JG cells, is controlled by physiological stimuli such as changes in renal vascular perfusion pressure, tubular sodium chloride load, and renal sympathetic nerve activity [11,17]. At the local level, renin secretion is influenced by a large number of bioactive factors such as prostaglandins, nitric oxide, adrenomedullin, Ang II (feedback), endothelin, vasopressin and adenosine [11,17,18]. At the molecular level, recent studies demonstrate that renin biosynthesis is regulated by an array of transcriptional factors [19 23]. These proteins influence renin gene transcription by a positive or negative fashion. 3. Clinical and epidemiological evidence linking Vitamin D-deficiency with hypertension Accumulating evidence from epidemiological and clinical studies in the last decades has suggested a connection between Vitamin D and blood pressure. As ultraviolet (UV) irradiation is essential for the cutaneous production of Vitamin D, circulating Vitamin D levels are greatly influenced by geographic locations, seasonal changes and skin pigmentations. Data obtained from the INTERSALT study centers reveal a linear correlation between the rise in blood pressure or the prevalence of hypertension and the latitudes north or south of the equator [24]. Data from a national survey in China also demonstrate that the prevalence of hypertension and stroke incidence display a high-to-low gradient from the north to the south of the country [25]. Seasonal variations in blood pressure have been reported in temperate climates, with blood pressure higher in the winter (low UV irradiation) than in the summer (high UV irradiation) [26,27]. Dark skin pigmentation, which affects an efficient UV light penetration [28], has also been reported to be associated with higher blood pressure [29,30]. Indeed, UV irradiation has been reported to lower blood pressure in patients with mild essential hypertension [31]. Numerous studies have shown that the serum level of 1,25(OH) 2 D 3 is inversely associated with blood pressure in normotensive and hypertensive subjects [32 34]. More interestingly, such inverse relationship has also been reported between circulating 1,25(OH) 2 D 3 levels and plasma renin activity in patients with essential hypertension [35]. Vitamin D supplement has been reported to be beneficial to the heart. In clinical trials, Vitamin D treatment has been reported to reduce blood pressure in hypertensive or elderly patients [36,37]. In several cases, 1,25(OH) 2 D 3 treatment has been shown to reduce the blood pressure, plasma renin activity, Ang II level and myocardial hypertrophy [38,39]. 4. Vitamin D as a negative endocrine regulator of the renin angiotensin system The clinical and epidemiological evidence suggests that Vitamin D may regulate blood pressure via regulating the RAS. Based on the inverse relationship between serum 1,25(OH) 2 D 3 levels and plasma renin activity found previously, we speculated that 1,25(OH) 2 D 3 might be a negative endocrine regulator of renin production in vivo. If this hypothesis is correct, disruption of the Vitamin D signaling pathway should lead to a deregulated stimulation of renin synthesis, whereas an increase in serum 1,25(OH) 2 D 3 levels should lead to renin suppression. To test this hypothesis, we examined VDR-null mutant mice, reasoning that renin expression should be increased in these mice due to the lack of VDR-mediated Vitamin D signaling. Indeed, we found that both renin mrna and protein levels in the kidney, as well as the plasma Ang II production, were drastically increased in VDR ( / ) mice, whereas the expression of angiotensinogen in the liver was the same as in wildtype mice. Thus, the increase in plasma Ang II appeared to be mainly due to an increase in renin activity. As a consequence of the aberrant RAS over-stimulation, VDR ( / ) mice developed hypertension, cardiac hypertrophy and an over-drinking behavior. Plasma and urinary aldosterone levels were also increased in VDR ( / ) mice. Cardiac hypertrophy, likely induced by Ang II, was reflected by a higher heart to body weight ratio and increased cardiac myocyte size in the ventricle revealed by histological analyses. Accompanying the cardiac hypertrophy, both cardiac
3 Y.C. Li et al. / Journal of Steroid Biochemistry & Molecular Biology (2004) mrna expression and plasma concentration of atrial natriuretic peptide (ANP) were found to be increased in VDR ( / ) mice, presumably as a compensatory mechanism. The high blood pressure, cardiac hypertrophy and increased water intake seen in VDR ( / ) mice could be corrected by treatment with captopril, an ACE inhibitor, or losartan, an Ang II AT 1 receptor antagonist, confirming that over-stimulation of the RAS is indeed responsible for the abnormalities. Interestingly, captopril or losartan treatment resulted in a drastic up-regulation of renin expression in both wild-type and VDR ( / ) mice. We also showed that renin expression in both wild-type and VDR ( / ) mice was stimulated by dehydration, and suppressed by a high sodium diet. In all cases VDR ( / ) mice still maintained a significantly higher renin expression than wild-type mice. Therefore, despite a high basal renin synthesis, the regulatory mechanisms that control renin production, including the Ang II feedback inhibition and the volume- and salt-sensing mechanisms, are still intact in VDR ( / ) mice. Thus, the sustained renin up-regulation is mediated by other mechanisms. VDR ( / ) mice develop hypocalcemia and secondary hyperparathyroidism [5], which may influence renin production and secretion. To address the contribution of serum calcium or parathyroid hormone (PTH) to renin up-regulation in VDR ( / ) mice, we found that renin up-regulation was already evident in 20-day-old VDR ( / ) mice, before the hypocalcemia developed, and persistent in normocalcemic adult VDR ( / ) mice after their blood calcium was normalized through dietary intervention. The plasma Ang II level remained elevated in the normocalcemic state. On the other hand, renin expression was normal in Gcm2 ( / ) mice [40], even though these mutant mice were as hypocalcemic as VDR ( / ) mice. In addition, renin expression was still elevated in VDR ( / ) mice whose alopecia was rescued by targeted expression of human VDR in the skin [41]. These date strongly suggest that regulation of renin expression by 1,25(OH) 2 D 3 is independent of calcium metabolism or alopecia. However, the contribution of PTH to the renin up-regulation in VDR ( / ) is less certain yet, because serum PTH starts to rise early in life before hypocalcemia develops and can not be completely normalized by dietary treatment, due to the lack of the VDR-mediated Vitamin D inhibition of PTH biosynthesis [42]. We also tested the hypothesis using wild-type mice. We showed that in wild-type mice rendered Vitamin D-deficient by dietary strontium treatment, which inhibits 1,25(OH) 2 D 3 biosynthesis [43], renin expression in the kidney was up-regulated as in VDR ( / ) mice. On the other hand, in wild-type mice receiving several doses of 1,25(OH) 2 D 3 injection renin expression was suppressed. Thus, the inhibitory role of 1,25(OH) 2 D 3 in renin biosynthesis was confirmed in normal mice. We further tested the hypothesis using As4.1 cells, a JG cell-like cell line that was derived from kidney tumors in SV40 T antigen transgenic mice and maintains a high level of renin synthesis [44]. We found that 1,25(OH) 2 D 3 drastically reduced renin mrna expression in As4.1 cells transiently or stably transfected with human VDR cdna. To elucidate the molecular mechanism whereby 1,25(OH) 2 D 3 suppresses renin gene expression, the stably transfected cells were used to analyze the renin gene promoter by luciferase reporter assays. When the cells were transfected with a luciferase reporter plasmid containing a 4.1 kb 5 -flanking sequence of the murine Ren-1c gene, 1,25(OH) 2 D 3 treatment markedly reduced the promoter activity, confirming that 1,25(OH) 2 D 3 directly and negatively regulates renin gene transcription by a VDR-mediated mechanism. Deletion analysis of the Ren-1c gene promoter has identified two short fragments, from 2720 to 2642 and 117 to +1, that are required to mediate the repression by 1,25(OH) 2 D Vitamin D analogs as potential anti-hypertensive agents? Hypertension is a major risk factor for heart attack, stroke, myocardial infarction, congestive heart failure, progressive atherosclerosis and renal failure. As a major pathogenic contributor to hypertension, the RAS has been an important drug target for therapeutic intervention of hypertension, with ACE inhibitors and Ang II receptor antagonists being among the most popular anti-hypertensive drugs [45]. As high-renin hypertension accounts for 10 20% of the patient population with essential hypertension, specific inhibitors for renin production are of significant therapeutic values. Such inhibitors, in theory, can be used alone or in combination with ACE inhibitors or Ang II receptor antagonists. Patients with high-renin hypertension generally have higher blood pressure [46] and tend to have a more active sympathetic nervous system [47], thus renin inhibitors may also be used with sympatholytic agents such as the -blockers. In spite of past efforts to develop peptide renin inhibitors [48 50], high toxicity of these compounds made them little use for administration to humans. The finding that 1,25(OH) 2 D 3 suppresses renin biosynthesis has raised the possibility to develop Vitamin D analogs into renin inhibitors for therapeutic purposes. With a large number of low calcemic Vitamin D analogs synthesized, and some of them already approved for clinical uses such as treatment of secondary hyperparathyroidism [51,52], such possibility is not unrealistic. In theory, Vitamin D analogs with equal or better potency but less calcemic effects than 1,25(OH) 2 D 3 are good candidates. To search for such candidates, we have set to screen Vitamin D analog compounds using the As4.1 cells stably transfected with human VDR by Northern blot and luciferase reporter assays. Interestingly, of the nine compounds we first screened, only the two Gemini compounds, which have double side chains at the carbon 20 position [53], displayed renin-suppressing activity equal or better than that of 1,25(OH) 2 D 3, whereas all other Vitamin D
4 390 Y.C. Li et al. / Journal of Steroid Biochemistry & Molecular Biology (2004) Fig. 2. Interaction of the Vitamin D endocrine system and the renin angiotensin system. 1,25(OH) 2 D 3 feedback regulates the production of parathyroid hormone and suppresses renin biosynthesis. The latter may serve to antagonize renin production induced by other physiological factors. Renin is also feedback suppressed by Ang II. Ultraviolet light influences blood pressure via 1,25(OH) 2 D 3. 1,25(OH) 2 D 3, PTH and calcium may also directly affect the cardiovascular functions (dashed lines), as suggested by other studies. PTH, parathyroid hormone. analogs had little or much less inhibitory activity. Continued screening of 11 more Gemini compounds identified six more candidates. The reason why the double-side chain Gemini compounds possess more potent activity in renin inhibition than other Vitamin D analogs or even 1,25(OH) 2 D 3 itself remains to be explored. Animal studies to test the in vivo efficacy of these Gemini compounds are under way in our laboratory. Preliminary data show that the analogs can significantly inhibit renin expression in vivo. 6. Conclusion Studies in the last few years have presented convincing evidence that the Vitamin D endocrine system plays multiple physiological roles. The discovery that 1,25(OH) 2 D 3 suppresses renin gene expression helps explain, at least in part, the inverse relationship between Vitamin D and blood pressure observed previously. Fig. 2 outlines the interaction between the Vitamin D endocrine system and the RAS in the regulation of calcium, electrolytes, volume and blood pressure homeostasis. It is speculated that, under normal physiological conditions, in addition to maintaining the blood calcium concentration, 1,25(OH) 2 D 3 antagonizes other renin-stimulating factors to maintain an appropriate renin level in the body. The counter-balance of 1,25(OH) 2 D 3 may be crucial for preventing the detrimental over-activation of the RAS. Therefore, Vitamin D-deficiency may increase the risk of hypertension, and Vitamin D supplement may be beneficial to the cardiovascular system. Finally, low calcemic Vitamin D analogs may open a new era for the long-sought therapeutic renin inhibitors and potentially offer a new class of anti-hypertensive drugs. Acknowledgements This work was supported by an American Heart Association grant and NIH grants DK59327 and DK62072 (to Y.C. Li). References [1] H.F. DeLuca, The vitamin D story: a collaborative effort of basic science and clinical medicine, FASEB J. 2 (1988) [2] M.R. Haussler, G.K. Whitfield, C.A. Haussler, J.-C. Hsieh, P.D. Thompson, S.H. Selznick, C.E. Dominguez, P.W. Jurutka, The nuclear vitamin D receptor: biological and molecular regulatory properties revealed, J. Bone Miner. Res. 13 (1998) [3] T. Yoshizawa, Y. Handa, Y. Uematsu, S. Takeda, K. Sekine, Y. Yoshihara, T. Kawakami, K. Arioka, H. Sato, Y. Uchiyama, S. Masushige, A. Fukamizu, T. Matsumoto, S. Kato, Mice lacking the vitamin D receptor exhibit impaired bone formation, Nat Genet 16 (1997) [4] D.K. Panda, D. Miao, M.L. Tremblay, J. Sirois, R. Farookhi, G.N. Hendy, D. Goltzman, Targeted ablation of the 25-hydroxyvitamin D 1alpha-hydroxylase enzyme: evidence for skeletal, reproductive, and immune dysfunction, Proc. Natl. Acad. Sci. U.S.A. 98 (2001) [5] Y.C. Li, A.E. Pirro, M. Amling, G. Delling, R. Baron, R. Bronson, M.B. Demay, Targeted ablation of the vitamin D receptor: an animal model of vitamin D-dependent rickets type II with alopecia, Proc. Natl. Acad. Sci. U.S.A. 94 (1997) [6] O. Dardenne, J. Prud homme, A. Arabian, F.H. Glorieux, R. St-Arnaud, Targeted inactivation of the 25-hydroxyvitamin D(3)- 1(alpha)-hydroxylase gene (CYP27B1) creates an animal model of pseudovitamin D-deficiency rickets, Endocrinology 142 (2001) [7] G. Zinser, K. Packman, J. Welsh, Vitamin D(3) receptor ablation alters mammary gland morphogenesis, Development 129 (2002) [8] Y.C. Li, J. Kong, M. Wei, Z.F. Chen, S.Q. Liu, L.P. Cao, 1,25- Dihydroxyvitamin D(3) is a negative endocrine regulator of the renin angiotensin system, J. Clin. Invest. 110 (2002) [9] J. Kong, Y.C. Li, Effect of angiotensin II type I receptor antagonist and angiotensin-converting enzyme inhibitor on vitamin D receptor null mice, Am. J. Physiol. Regul. Integr. Comp. Physiol. 285 (2003) R255 R261. [10] C. Berry, R. Touyz, A.F. Dominiczak, R.C. Webb, D.G. Johns, Angiotensin receptors: signaling, vascular pathophysiology, and interactions with ceramide, Am. J. Physiol. Heart Circ. Physiol. 281 (2001) H2337 H2365. [11] B.J. Ballermann, M.L. Zeidel, M.E. Gunning, B.M. Brenner, Vasoactive peptides and the kidney, in: B.M. Brenner, F.C. Rector (Eds.), The kidney, W.B. Saunders Company, Philadelphia, 1991, pp [12] J.L. Lavoie, C.D. Sigmund, Minireview: overview of the Renin angiotensin system-an endocrine and paracrine system, Endocrinology 144 (2003)
5 Y.C. Li et al. / Journal of Steroid Biochemistry & Molecular Biology (2004) [13] G. Nguyen, F. Delarue, C. Burckle, L. Bouzhir, T. Giller, J.D. Sraer, Pivotal role of the renin/prorenin receptor in angiotensin II production and cellular responses to renin, J. Clin. Invest. 109 (2002) [14] M. Donoghue, F. Hsieh, E. Baronas, K. Godbout, M. Gosselin, N. Stagliano, M. Donovan, B. Woolf, K. Robison, R. Jeyaseelan, R.E. Breitbart, S. Acton, A novel angiotensin-converting enzyme-related carboxypeptidase (ACE2) converts angiotensin I to angiotensin 1 9, Circ. Res. 87 (2000) E1 E9. [15] S.R. Tipnis, N.M. Hooper, R. Hyde, E. Karran, G. Christie, A.J. Turner, A human homolog of angiotensin-converting enzyme. Cloning and functional expression as a captopril-insensitive carboxypeptidase, J. Biol. Chem. 275 (2000) [16] M.A. Crackower, R. Sarao, G.Y. Oudit, C. Yagil, I. Kozieradzki, S.E. Scanga, A.J. Oliveira-dos-Santos, J. da Costa, L. Zhang, Y. Pei, J. Scholey, C.M. Ferrario, A.S. Manoukian, M.C. Chappell, P.H. Backx, Y. Yagil, J.M. Penninger, Angiotensin-converting enzyme 2 is an essential regulator of heart function, Nature 417 (2002) [17] E. Hackenthal, M. Paul, D. Ganten, R. Taugner, Morphology, physiology, and molecular biology of renin secretion, Physiol. Rev. 70 (1990) [18] M. Bader, D. Ganten, Regulation of renin: new evidence from cultured cells and genetically modified mice [in process citation], J. Mol. Med. 78 (2000) [19] K. Tamura, Y.E. Chen, M. Horiuchi, Q. Chen, L. Daviet, Z. Yang, M. Lopez-Ilasaca, H. Mu, R.E. Pratt, V.J. Dzau, LXRalpha functions as a camp-responsive transcriptional regulator of gene expression, Proc. Natl. Acad. Sci. U.S.A. 97 (2000) [20] Q. Shi, K.W. Gross, C.D. Sigmund, Retinoic acid-mediated activation of the mouse renin enhancer, J. Biol. Chem. 276 (2001) [21] L. Pan, T.A. Black, Q. Shi, C.A. Jones, N. Petrovic, J. Loudon, C. Kane, C.D. Sigmund, K.W. Gross, Critical roles of a cyclic AMP responsive element and an E-box in regulation of mouse renin gene expression, J. Biol. Chem. 276 (2001) [22] L. Pan, Y. Xie, T.A. Black, C.A. Jones, S.C. Pruitt, K.W. Gross, An Abd-B class HOX.PBX recognition sequence is required for expression from the mouse Ren-1c gene, J. Biol. Chem. 276 (2001) [23] X. Liu, X. Huang, C.D. Sigmund, Identification of a nuclear orphan receptor (Ear2) as a negative regulator of renin gene transcription, Circ. Res. 92 (2003) [24] S.G. Rostand, Ultraviolet light may contribute to geographic and racial blood pressure differences, Hypertension 30 (1997) [25] J. He, M.J. Klag, Z. Wu, P.K. Whelton, Stroke in the People s Republic of China. I. Geographic variations in incidence and risk factors, Stroke 26 (1995) [26] J. Kunes, J. Tremblay, F. Bellavance, P. Hamet, Influence of environmental temperature on the blood pressure of hypertensive patients in Montreal, Am. J. Hypertens. 4 (1991) [27] P.R. Woodhouse, K.T. Khaw, M. Plummer, Seasonal variation of blood pressure and its relationship to ambient temperature in an elderly population, J. Hypertens. 11 (1993) [28] M.F. Holick, Photosynthesis of vitamin D in the skin: effect of environmental and life-style variables, Fed. Proc. 46 (1987) [29] E. Harburg, L. Gleibermann, P. Roeper, M.A. Schork, W.J. Schull, Skin color, ethnicity, and blood pressure I: detroit blacks, Am. J. Public Health 68 (1978) [30] M.J. Klag, P.K. Whelton, J. Coresh, C.E. Grim, L.H. Kuller, The association of skin color with blood pressure in US blacks with low socioeconomic status, JAMA 265 (1991) [31] R. Krause, M. Buhring, W. Hopfenmuller, M.F. Holick, A.M. Sharma, Ultraviolet B and blood pressure, Lancet 352 (1998) [32] E. Kristal-Boneh, P. Froom, G. Harari, J. Ribak, Association of calcitriol and blood pressure in normotensive men, Hypertension 30 (1997) [33] L. Lind, A. Hanni, H. Lithell, A. Hvarfner, O.H. Sorensen, S. Ljunghall, Vitamin D is related to blood pressure and other cardiovascular risk factors in middle-aged men, Am. J. Hypertens. 8 (1995) [34] E.D. Burgess, R.G. Hawkins, M. Watanabe, Interaction of 1,25- dihydroxyvitamin D and plasma renin activity in high renin essential hypertension, Am. J. Hypertens. 3 (1990) [35] L.M. Resnick, F.B. Muller, J.H. Laragh, Calcium-regulating hormones in essential hypertension. Relation to plasma renin activity and sodium metabolism, Ann. Intern. Med. 105 (1986) [36] L. Lind, B. Wengle, L. Wide, S. Ljunghall, Reduction of blood pressure during long-term treatment with active vitamin D (alphacalcidol) is dependent on plasma renin activity and calcium status. A double-blind, placebo-controlled study, Am. J. Hypertens. 2 (1989) [37] M. Pfeifer, B. Begerow, H.W. Minne, D. Nachtigall, C. Hansen, Effects of a short-term vitamin D(3) and calcium supplementation on blood pressure and parathyroid hormone levels in elderly women, J. Clin. Endocrinol. Metab. 86 (2001) [38] Y. Kimura, M. Kawamura, M. Owada, T. Oshima, M. Murooka, T. Fujiwara, K. Hiramori, Effectiveness of 1,25- dihydroxyvitamin D supplementation on blood pressure reduction in a pseudohypoparathyroidism patient with high renin activity, Intern. Med. 38 (1999) [39] C.W. Park, Y.S. Oh, Y.S. Shin, C.M. Kim, Y.S. Kim, S.Y. Kim, E.J. Choi, Y.S. Chang, B.K. Bang, Intravenous calcitriol regresses myocardial hypertrophy in hemodialysis patients with secondary hyperparathyroidism, Am. J. Kidney Dis. 33 (1999) [40] T. Gunther, Z.F. Chen, J. Kim, M. Priemel, J.M. Rueger, M. Amling, J.M. Moseley, T.J. Martin, D.J. Anderson, G. Karsenty, Genetic ablation of parathyroid glands reveals another source of parathyroid hormone, Nature 406 (2000) [41] J. Kong, X.J. Li, D. Gavin, Y. Jiang, Y.C. Li, Targeted expression of human vitamin D receptor in the skin promotes the initiation of postnatal hair follicular cycle and rescue the alopecia in vitamin D receptor null mice, J. Invest. Dermatol. 118 (2002) [42] J. Silver, T. Naveh-many, H. Mayer, H.J. Schmeizer, M.M. Popovtzer, Regulation by vitamin D metabolites of parathyroid hormone gene transcription in vivo in the rat, J. Clin. Invest. 78 (1986) [43] J.L. Omdahl, H.F. DeLuca, Strontium induced rickets: metabolic basis, Science 174 (1971) [44] C.D. Sigmund, K. Okuyama, J. Ingelfinger, C.A. Jones, J.J. Mullins, C. Kane, U. Kim, C.Z. Wu, L. Kenny, Y. Rustum, et al., Isolation and characterization of renin-expressing cell lines from transgenic mice containing a renin-promoter viral oncogene fusion construct, J. Biol. Chem. 265 (1990) [45] P. August, Initial treatment of hypertension, N. Engl. J. Med. 348 (2003) [46] H.R. Brunner, J.H. Laragh, L. Baer, M.A. Newton, F.T. Goodwin, L.R. Krakoff, R.H. Bard, F.R. Buhler, Essential hypertension: renin and aldosterone, heart attack and stroke, N. Engl. J. Med. 286 (1972) [47] M. Esler, S. Julius, A. Zweifler, O. Randall, E. Harburg, H. Gardiner, V. DeQuattro, Mild high-renin essential hypertension. Neurogenic human hypertension? N. Engl. J. Med. 296 (1977) [48] T. Kokubu, E. Ueda, S. Fujimoto, K. Hiwada, A. Kato, Peptide inhibitors of the renin angiotensin system, Nature 217 (1968) [49] K. Poulsen, J. Burton, E. Haber, Purification of hog renin by affinity chromatography using the synthetic competitive inhibitor (d- Leu6)octapeptide, Biochim. Biophys. Acta 400 (1975) [50] J. Burton, R.J. Cody Jr., J.A. Herd, E. Haber, Specific inhibition of renin by an angiotensinogen analog: studies in sodium depletion and renin-dependent hypertension, Proc. Natl. Acad. Sci. U.S.A. 77 (1980) [51] A.J. Brown, A.S. Dusso, E. Slatopolsky, Vitamin D analogues for secondary hyperparathyroidism, Nephrol. Dial Transplant. 17 (Suppl 10) (2002)
6 392 Y.C. Li et al. / Journal of Steroid Biochemistry & Molecular Biology (2004) [52] H.H. Malluche, H. Mawad, N.J. Koszewski, Update on vitamin D and its newer analogues: actions and rationale for treatment in chronic renal failure, Kidney Int. 62 (2002) [53] M.R. Uskokovic, P.S. Manchand, S. Peleg, A.W. Norman, Synthesis and preliminary evaluation of the biological properties of a 1a,25- dihydroxyvitamin D3 analog with two side chains, in: A.W. Norman, R. Bouillon, M. Thomasset (Eds.), Vitamin D: Chemistry, Biology and Clinical Applications of the Steroid Hormone, University of California, Riverside, 1997, pp
NIH Public Access Author Manuscript J Steroid Biochem Mol Biol. Author manuscript; available in PMC 2011 February 10.
 NIH Public Access Author Manuscript Published in final edited form as: J Steroid Biochem Mol Biol. 2010 July ; 121(1-2): 445 447. doi:10.1016/j.jsbmb.2010.04.013. 1,25-Dihydroxyvitamin D 3 reduces systolic
NIH Public Access Author Manuscript Published in final edited form as: J Steroid Biochem Mol Biol. 2010 July ; 121(1-2): 445 447. doi:10.1016/j.jsbmb.2010.04.013. 1,25-Dihydroxyvitamin D 3 reduces systolic
A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets
 Diabetologia () 5:77 DOI.7/s5--- SHORT COMMUNICATION A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets Q. Cheng & Y. C.
Diabetologia () 5:77 DOI.7/s5--- SHORT COMMUNICATION A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets Q. Cheng & Y. C.
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D.
 Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
Regulation of Arterial Blood Pressure 2 George D. Ford, Ph.D. OBJECTIVES: 1. Describe the Central Nervous System Ischemic Response. 2. Describe chemical sensitivities of arterial and cardiopulmonary chemoreceptors,
FOCUS ON CARDIOVASCULAR DISEASE
 The Consequences of Vitamin D Deficiency: FOCUS ON CARDIOVASCULAR DISEASE Vitamin D deficiency is a global health problem. With all the medical advances of the century, vitamin D deficiency is still epidemic.
The Consequences of Vitamin D Deficiency: FOCUS ON CARDIOVASCULAR DISEASE Vitamin D deficiency is a global health problem. With all the medical advances of the century, vitamin D deficiency is still epidemic.
Skeletal. Parathyroid hormone-related protein Analyte Information
 Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Skeletal Parathyroid hormone-related protein Analyte Information 1 2012-04-04 Parathyroid hormone related protein (PTHrP) Introduction Parathyroid hormone-related protein (PTHrP) is actually a family of
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Vitamin D & Cardiovascular Disease
 Vitamin D & Cardiovascular Disease Disclosures None Vitamin D Objectives: Discuss the basics of vitamin D metabolism Discuss the role of vitamin D deficiency in the development of coronary disease Review
Vitamin D & Cardiovascular Disease Disclosures None Vitamin D Objectives: Discuss the basics of vitamin D metabolism Discuss the role of vitamin D deficiency in the development of coronary disease Review
Cardiovascular System B L O O D V E S S E L S 2
 Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
Cardiovascular System B L O O D V E S S E L S 2 Blood Pressure Main factors influencing blood pressure: Cardiac output (CO) Peripheral resistance (PR) Blood volume Peripheral resistance is a major factor
The effect of a change in ambient temperature on blood pressure in normotensives
 (2001) 15, 113 117 2001 Nature Publishing Group All rights reserved 0950-9240/01 $15.00 www.nature.com/jhh ORIGINAL ARTICLE The effect of a change in ambient temperature on blood pressure in normotensives
(2001) 15, 113 117 2001 Nature Publishing Group All rights reserved 0950-9240/01 $15.00 www.nature.com/jhh ORIGINAL ARTICLE The effect of a change in ambient temperature on blood pressure in normotensives
This is the author s final accepted version.
 Nicklin, S. A. (2016) A novel mechanism of action for angiotensin-(1-7) via the angiotensin type 1 receptor. Hypertension, 68(6), pp. 1342-1343. (doi:10.1161/hypertensionaha.116.08215) This is the author
Nicklin, S. A. (2016) A novel mechanism of action for angiotensin-(1-7) via the angiotensin type 1 receptor. Hypertension, 68(6), pp. 1342-1343. (doi:10.1161/hypertensionaha.116.08215) This is the author
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Citation for published version (APA): Lely, A. T. (2007). Towards an integrated approach on RAAS-blockade s.n.
 University of Groningen Towards an integrated approach on RAAS-blockade Lely, Anna Titia IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
University of Groningen Towards an integrated approach on RAAS-blockade Lely, Anna Titia IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
THE RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM
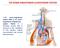 THE RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM The renin angiotensin system (RAS) or the renin angiotensin aldosterone system (RAAS) is a hormone system that is involved in the regulation of the plasma sodium
THE RENIN-ANGIOTENSIN-ALDOSTERONE SYSTEM The renin angiotensin system (RAS) or the renin angiotensin aldosterone system (RAAS) is a hormone system that is involved in the regulation of the plasma sodium
The Endocrine System. I. Overview of the Endocrine System. II. Three Families of Hormones. III. Hormone Receptors. IV. Classes of Hormone Receptor
 The Endocrine System I. Overview of the Endocrine System A. Regulates long term metabolic processes B. Releases hormones from endocrine cells 1. Hormones are chemicals 2. Alter metabolism of cells 3. Release
The Endocrine System I. Overview of the Endocrine System A. Regulates long term metabolic processes B. Releases hormones from endocrine cells 1. Hormones are chemicals 2. Alter metabolism of cells 3. Release
Paul M McKie, Alessandro Cataliotti, Guido Boerrigter, Horng C Chen, Fernando L Martin, and John C Burnett Jr
 Cardiorenal Enhancing and Aldosterone Suppressing Actions of a Novel Designer Natriuretic Peptide in Experimental Hypertension with Ventricular Pressure Overload Paul M McKie, Alessandro Cataliotti, Guido
Cardiorenal Enhancing and Aldosterone Suppressing Actions of a Novel Designer Natriuretic Peptide in Experimental Hypertension with Ventricular Pressure Overload Paul M McKie, Alessandro Cataliotti, Guido
Chapter 16: Endocrine System 1
 Ch 16 Endocrine System Bi 233 Endocrine system Endocrine System: Overview Body s second great controlling system Influences metabolic activities of cells by means of hormones Slow signaling Endocrine glands
Ch 16 Endocrine System Bi 233 Endocrine system Endocrine System: Overview Body s second great controlling system Influences metabolic activities of cells by means of hormones Slow signaling Endocrine glands
Parathyroid hormone (PTH) and 1,25-dihydroxyvitamin D 3
 Parathyroid hormone decreases renal vitamin D receptor expression in vivo Kevin D. Healy, Janeen L. Vanhooke, Jean M. Prahl, and Hector F. DeLuca* Department of Biochemistry, University of Wisconsin, Madison,
Parathyroid hormone decreases renal vitamin D receptor expression in vivo Kevin D. Healy, Janeen L. Vanhooke, Jean M. Prahl, and Hector F. DeLuca* Department of Biochemistry, University of Wisconsin, Madison,
Vitamin D. Vitamin functioning as hormone. Todd A Fearer, MD FACP
 Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Endocrine System Hormones (Ch. 45)
 Endocrine System Hormones (Ch. 45) Regulation Why are hormones needed? chemical messages from one body part to another communication needed to coordinate whole body daily homeostasis & regulation of large
Endocrine System Hormones (Ch. 45) Regulation Why are hormones needed? chemical messages from one body part to another communication needed to coordinate whole body daily homeostasis & regulation of large
Role of Minerals in Hypertension
 Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction
 Cardio-Metabolic Franchise Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction Randy L Webb, PhD Rutgers Workshop October 21, 2016 Heart
Cardio-Metabolic Franchise Entresto Development of sacubitril/valsartan (LCZ696) for the treatment of heart failure with reduced ejection fraction Randy L Webb, PhD Rutgers Workshop October 21, 2016 Heart
Circulating renin is synthesized in the renal juxtaglomerular
 Appropriate Regulation of Renin and Blood Pressure in 45-kb Human Renin/Human Angiotensinogen Transgenic Mice Daniel F. Catanzaro, Rong Chen, Yan Yan, Lufei Hu, Jean E. Sealey, John H. Laragh Abstract
Appropriate Regulation of Renin and Blood Pressure in 45-kb Human Renin/Human Angiotensinogen Transgenic Mice Daniel F. Catanzaro, Rong Chen, Yan Yan, Lufei Hu, Jean E. Sealey, John H. Laragh Abstract
Endocrine System Hormones. AP Biology
 Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? u chemical messages from one body part to another u communication needed to coordinate whole body u daily homeostasis & regulation
Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? u chemical messages from one body part to another u communication needed to coordinate whole body u daily homeostasis & regulation
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Vitamin D and Cardiovascular System Merajuddin Shah MD, DM (Cardiology), FICC
 40 Vitamin D and Cardiovascular System Merajuddin Shah MD, DM (Cardiology), FICC Vitamins are organic compounds essential for growth, maintenance of health and body metabolism. As vitamins are not synthesized
40 Vitamin D and Cardiovascular System Merajuddin Shah MD, DM (Cardiology), FICC Vitamins are organic compounds essential for growth, maintenance of health and body metabolism. As vitamins are not synthesized
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Citation for published version (APA): Meems, L. (2015). Vitamin D biology and heart failure: Clinical and experimental studies [Groningen]
![Citation for published version (APA): Meems, L. (2015). Vitamin D biology and heart failure: Clinical and experimental studies [Groningen] Citation for published version (APA): Meems, L. (2015). Vitamin D biology and heart failure: Clinical and experimental studies [Groningen]](/thumbs/89/101183507.jpg) University of Groningen Vitamin D biology and heart failure Meems, Laura IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
University of Groningen Vitamin D biology and heart failure Meems, Laura IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
ΚΑΡΔΙΑΚΗ ΑΝΕΠΑΡΚΕΙΑ ΚΑΙ ΑΝΤΑΓΩΝΙΣΤΕΣ ΑΛΔΟΣΤΕΡΟΝΗΣ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ MD, FESC. E.Α Κ/Δ Γ.Ν.ΚΑΤΕΡΙΝΗΣ
 ΚΑΡΔΙΑΚΗ ΑΝΕΠΑΡΚΕΙΑ ΚΑΙ ΑΝΤΑΓΩΝΙΣΤΕΣ ΑΛΔΟΣΤΕΡΟΝΗΣ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ MD, FESC. E.Α Κ/Δ Γ.Ν.ΚΑΤΕΡΙΝΗΣ Aldosterone is a mineralocorticoid hormone synthesized by the adrenal glands that has several regulatory
ΚΑΡΔΙΑΚΗ ΑΝΕΠΑΡΚΕΙΑ ΚΑΙ ΑΝΤΑΓΩΝΙΣΤΕΣ ΑΛΔΟΣΤΕΡΟΝΗΣ ΣΠΥΡΟΜΗΤΡΟΣ ΓΕΩΡΓΙΟΣ MD, FESC. E.Α Κ/Δ Γ.Ν.ΚΑΤΕΡΙΝΗΣ Aldosterone is a mineralocorticoid hormone synthesized by the adrenal glands that has several regulatory
VITAMIN D AND THE ATHLETE
 VITAMIN D AND THE ATHLETE CONSIDERATIONS FOR THE PRACTITIONER Written by Bruce Hamilton, Qatar Vitamin D is a steroid hormone that has previously been given little attention, partially as a result of its
VITAMIN D AND THE ATHLETE CONSIDERATIONS FOR THE PRACTITIONER Written by Bruce Hamilton, Qatar Vitamin D is a steroid hormone that has previously been given little attention, partially as a result of its
POTASSIUM. The Facts. compiled by the Nestlé Research Center
 POTASSIUM The Facts compiled by the Nestlé Research Center A public health concern? Studies have shown that a diet high in sodium or low in potassium is linked with a higher risk for elevated blood pressure
POTASSIUM The Facts compiled by the Nestlé Research Center A public health concern? Studies have shown that a diet high in sodium or low in potassium is linked with a higher risk for elevated blood pressure
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Doctor of Philosophy
 Regulation of Gene Expression of the 25-Hydroxyvitamin D la-hydroxylase (CYP27BI) Promoter: Study of A Transgenic Mouse Model Ivanka Hendrix School of Molecular and Biomedical Science The University of
Regulation of Gene Expression of the 25-Hydroxyvitamin D la-hydroxylase (CYP27BI) Promoter: Study of A Transgenic Mouse Model Ivanka Hendrix School of Molecular and Biomedical Science The University of
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
BIOL 2458 A&P II CHAPTER 18 SI Both the system and the endocrine system affect all body cells.
 BIOL 2458 A&P II CHAPTER 18 SI 1 1. Both the system and the endocrine system affect all body cells. 2. Affect on target cells by the system is slow. Affect on target cells by the system is fast. INTERCELLULAR
BIOL 2458 A&P II CHAPTER 18 SI 1 1. Both the system and the endocrine system affect all body cells. 2. Affect on target cells by the system is slow. Affect on target cells by the system is fast. INTERCELLULAR
MECHANISM AND MODE OF HORMONE ACTION. Some definitions. Receptor: Properties of receptors. PRESENTED BY MBUNKUR GLORY NKOSI.
 MECHANISM AND MODE OF HORMONE ACTION. PRESENTED BY MBUNKUR GLORY NKOSI. OUTLINE. Introduction Some definitions Hormone secretion, transport, and clearance from the blood. Feedback control of hormone secretion.
MECHANISM AND MODE OF HORMONE ACTION. PRESENTED BY MBUNKUR GLORY NKOSI. OUTLINE. Introduction Some definitions Hormone secretion, transport, and clearance from the blood. Feedback control of hormone secretion.
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
The Urinary System and Homeostasis *
 OpenStax-CNX module: m46446 1 The Urinary System and Homeostasis * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section,
OpenStax-CNX module: m46446 1 The Urinary System and Homeostasis * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of this section,
Therapeutic golas in the treatment of CKD-MBD
 Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Therapeutic golas in the treatment of CKD-MBD Hemodialysis clinic Clinical University Center Sarajevo Bantao, 04-08.10.2017, Sarajevo Abbvie Satellite symposium 06.10.2017 Chronic Kidney Disease Mineral
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
K K MK-4 MK-4 1,25-D3
 22 5 13 D 25-Hydroxyvitamin D Gla K K D K D K K K -4MK-4 MK-4 MK-4 steriod and xenobiotic receptorsxr MK-4 SXR MK-4 K MK-4 D 1,25-D3 D 1 CYP27B1CYP27B1-KO D CYP27B1-KO D D CYP27B1-KO Ca 1,25-D3 D Vitamin
22 5 13 D 25-Hydroxyvitamin D Gla K K D K D K K K -4MK-4 MK-4 MK-4 steriod and xenobiotic receptorsxr MK-4 SXR MK-4 K MK-4 D 1,25-D3 D 1 CYP27B1CYP27B1-KO D CYP27B1-KO D D CYP27B1-KO Ca 1,25-D3 D Vitamin
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Aldosterone synthase inhibitors. John McMurray BHF Cardiovascular Research Centre University of Glasgow
 Aldosterone synthase inhibitors John McMurray BHF Cardiovascular Research Centre University of Glasgow Inhibition of aldosterone synthesis is hypothesized to be of benefit to patients with cardiovascular
Aldosterone synthase inhibitors John McMurray BHF Cardiovascular Research Centre University of Glasgow Inhibition of aldosterone synthesis is hypothesized to be of benefit to patients with cardiovascular
OMICS Journals are welcoming Submissions
 OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
OMICS Journals are welcoming Submissions OMICS International welcomes submissions that are original and technically so as to serve both the developing world and developed countries in the best possible
Endocrine System Hormones
 Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? chemical messages from one body part to another communication needed to coordinate whole body homeostasis & regulation metabolism
Endocrine System Hormones 2007-2008 Regulation Why are hormones needed? chemical messages from one body part to another communication needed to coordinate whole body homeostasis & regulation metabolism
Vitamin D in Cattle: Calcium and Beyond. Corwin D. Nelson, Ph.D. Assistant Professor of Physiology Department of Animal Sciences
 OH HO OH Vitamin D in Cattle: Calcium and Beyond Corwin D. Nelson, Ph.D. Assistant Professor of Physiology Department of Animal Sciences Seminar Outline 1. Basics of vitamin D metabolism and genomic actions
OH HO OH Vitamin D in Cattle: Calcium and Beyond Corwin D. Nelson, Ph.D. Assistant Professor of Physiology Department of Animal Sciences Seminar Outline 1. Basics of vitamin D metabolism and genomic actions
Data Alert #2... Bi o l o g y Work i n g Gro u p. Subject: HOPE: New validation for the importance of tissue ACE inhibition
 Vascular Bi o l o g y Work i n g Gro u p c/o Medical Education Consultants, In c. 25 Sy l van Road South, We s t p o rt, CT 06880 Chairman: Carl J. Pepine, MD Professor and Chief Division of Cardiovascular
Vascular Bi o l o g y Work i n g Gro u p c/o Medical Education Consultants, In c. 25 Sy l van Road South, We s t p o rt, CT 06880 Chairman: Carl J. Pepine, MD Professor and Chief Division of Cardiovascular
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
J Jpn Coll Angiol, 2009, 49:
 Online publication October 6, 2009 48 2 20 J Jpn Coll Angiol, 2009, 49: 293 297 atrial natriuretic peptide, brain natriuretic peptide, guanylyl cyclase-a receptor, cardiac remodeling, cardiac hypertrophy
Online publication October 6, 2009 48 2 20 J Jpn Coll Angiol, 2009, 49: 293 297 atrial natriuretic peptide, brain natriuretic peptide, guanylyl cyclase-a receptor, cardiac remodeling, cardiac hypertrophy
Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic
![Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic Heart Failure. Acute. Plasma [NE] (pg/ml) 24 Hours. Chronic](/thumbs/90/103241154.jpg) Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Heart Failure Heart failure is the inability of the heart to deliver sufficient blood to the tissues to ensure adequate oxygen supply. Clinically it is characterized by signs of volume overload or symptoms
Diuretic Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Cardiorenal Syndrome Prof. Dr. Bülent ALTUN Hacettepe University Faculty of Medicine Department of Internal Medicine Division of Nephrology
 Cardiorenal Syndrome Prof. Dr. Bülent ALTUN Hacettepe University Faculty of Medicine Department of Internal Medicine Division of Nephrology Heart and Kidney The kidney yin dominates water, The heart yang
Cardiorenal Syndrome Prof. Dr. Bülent ALTUN Hacettepe University Faculty of Medicine Department of Internal Medicine Division of Nephrology Heart and Kidney The kidney yin dominates water, The heart yang
UCLA Nutrition Bytes. Title. Permalink. Journal ISSN. Author. Publication Date. Calcium and Hypertension. https://escholarship.org/uc/item/68b658ss
 UCLA Nutrition Bytes Title Calcium and Hypertension Permalink https://escholarship.org/uc/item/68b658ss Journal Nutrition Bytes, 4(2) ISSN 1548-601X Author Martinez, Christina Publication Date 1998-01-01
UCLA Nutrition Bytes Title Calcium and Hypertension Permalink https://escholarship.org/uc/item/68b658ss Journal Nutrition Bytes, 4(2) ISSN 1548-601X Author Martinez, Christina Publication Date 1998-01-01
Hormones. Introduction to Endocrine Disorders. Hormone actions. Modulation of hormone levels. Modulation of hormone levels
 Introduction to Endocrine Disorders Hormones Self-regulating system (homeostasis) Affect: Growth Metabolism Reproduction Fluid and electrolyte balance Hormone actions Endocrine gland Hormone synthesis
Introduction to Endocrine Disorders Hormones Self-regulating system (homeostasis) Affect: Growth Metabolism Reproduction Fluid and electrolyte balance Hormone actions Endocrine gland Hormone synthesis
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Hormonal Control of Osmoregulatory Functions *
 OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
Relationship between renal injury and the antagonistic roles of angiotensin-converting enzyme (ACE) and ACE2
 Relationship between renal injury and the antagonistic roles of angiotensin-converting enzyme (ACE) and ACE2 C. Ma, H. Xin, X.-Y. Jiang, Y.-X. Wang and Y.-S. Zhang Key Laboratory of Animal Physiology and
Relationship between renal injury and the antagonistic roles of angiotensin-converting enzyme (ACE) and ACE2 C. Ma, H. Xin, X.-Y. Jiang, Y.-X. Wang and Y.-S. Zhang Key Laboratory of Animal Physiology and
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB
 COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
COMPLETE INHIBITION OF RENAL RESERVE IN CHRONIC RENAL FAILURE BY A COMBINATION OF ACEI AND ARB CG Musso ¹, J Reynaldi¹, N Imperiali ¹, L Algranati ¹, DG Oreopoulos ² Nephrology Department Hospital Italiano
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Pharmacology - Problem Drill 11: Vasoactive Agents
 Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Pharmacology - Problem Drill 11: Vasoactive Agents Question No. 1 of 10 1. Vascular smooth muscle contraction is triggered by a rise in. Question #01 (A) Luminal calcium (B) Extracellular calcium (C) Intracellular
Effect of Sodium Loading and Depletion on Cyclic Nucleotides in Plasma and Aorta. Interaction between Prostacyclin and Cyclic Nucleotides
 Endocrinol. Japon. 1982, 29 (2), 245-250 Effect of Sodium Loading and Depletion on Cyclic Nucleotides in Plasma and Aorta. Interaction between Prostacyclin and Cyclic Nucleotides MANABU YOSHIMURA, TERUO
Endocrinol. Japon. 1982, 29 (2), 245-250 Effect of Sodium Loading and Depletion on Cyclic Nucleotides in Plasma and Aorta. Interaction between Prostacyclin and Cyclic Nucleotides MANABU YOSHIMURA, TERUO
The effect of vitamin D on calcium and phosphate homeostasis
 Plasma 25-Hydroxyvitamin D Levels and Risk of Incident Hypertension Among Young Women John P. Forman, Gary C. Curhan, Eric N. Taylor Abstract Numerous cross-sectional studies demonstrate an inverse association
Plasma 25-Hydroxyvitamin D Levels and Risk of Incident Hypertension Among Young Women John P. Forman, Gary C. Curhan, Eric N. Taylor Abstract Numerous cross-sectional studies demonstrate an inverse association
Vitamin D physiology
 Progress in Biophysics and Molecular Biology 92 (2006) 4 8 Review Vitamin D physiology P. Lips www.elsevier.com/locate/pbiomolbio Department of Endocrinology, VU University Medical Center, P.O. Box 7057,
Progress in Biophysics and Molecular Biology 92 (2006) 4 8 Review Vitamin D physiology P. Lips www.elsevier.com/locate/pbiomolbio Department of Endocrinology, VU University Medical Center, P.O. Box 7057,
Mineralocorticoids. Introduction
 Mineralocorticoids Introduction concepts to remember: a) water, glucose, mineral metabolism; b) adrenal in stress and blood pressure 15 Renin - angiotensin (RAS) and kallikrein kinin (KKS) systems: synthesis,
Mineralocorticoids Introduction concepts to remember: a) water, glucose, mineral metabolism; b) adrenal in stress and blood pressure 15 Renin - angiotensin (RAS) and kallikrein kinin (KKS) systems: synthesis,
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
INTERNATIONAL JOURNAL OF INSTITUTIONAL PHARMACY AND LIFE SCIENCES
 International Journal of Institutional Pharmacy and Life Sciences 5(3): May-June 2015 INTERNATIONAL JOURNAL OF INSTITUTIONAL PHARMACY AND LIFE SCIENCES Life Sciences Research Article!!! Received: 06-05-2015;
International Journal of Institutional Pharmacy and Life Sciences 5(3): May-June 2015 INTERNATIONAL JOURNAL OF INSTITUTIONAL PHARMACY AND LIFE SCIENCES Life Sciences Research Article!!! Received: 06-05-2015;
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Klotho: renal and extra-renal effects
 Klotho: renal and extra-renal effects Juan F. Navarro-González, MD, PhD, FASN Nephrology Service and Research Division University Hospital Nuestra Señora de Candalaria Santa Cruz de Tenerife. Spain Klotho:
Klotho: renal and extra-renal effects Juan F. Navarro-González, MD, PhD, FASN Nephrology Service and Research Division University Hospital Nuestra Señora de Candalaria Santa Cruz de Tenerife. Spain Klotho:
Chapter 11 Lecture Outline
 Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 11 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Ch45: Endocrine System
 Ch45: Endocrine System Endocrine System Homeostasis is the tendency to maintain a stable internal environment. Function = with hormones to maintain homeostasis Works with nervous system Anatomy Location:
Ch45: Endocrine System Endocrine System Homeostasis is the tendency to maintain a stable internal environment. Function = with hormones to maintain homeostasis Works with nervous system Anatomy Location:
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Close to site of release (at synapse); binds to receptors in
 Chapter 18: The Endocrine System Chemical Messengers 1. Neural 2. Endocrine 3. Neuroendocrine 4. Paracrine 5. Autocrine Endocrine System --Endocrine and nervous systems work together --Endocrine vs. Nervous
Chapter 18: The Endocrine System Chemical Messengers 1. Neural 2. Endocrine 3. Neuroendocrine 4. Paracrine 5. Autocrine Endocrine System --Endocrine and nervous systems work together --Endocrine vs. Nervous
2) Storehouse for the hormones produced by the hypothalamus of the brain. 2)
 AP 2 Exam Chapter 16 Endocrie Due Wed. night 4/22 or Thurs. morning 4/23 Name: Matching; match the labeled organ with the most appropriate response or identification. Figure 16.1 Using Figure 16.1, match
AP 2 Exam Chapter 16 Endocrie Due Wed. night 4/22 or Thurs. morning 4/23 Name: Matching; match the labeled organ with the most appropriate response or identification. Figure 16.1 Using Figure 16.1, match
Vitamin D status and parathyroid hormone levels in relation to blood pressure: a population-based study in older men and women
 Original Article doi: 10.1111/j.1365-2796.2007.01778.x Vitamin D status and parathyroid hormone levels in relation to blood pressure: a population-based study in older men and women M. B. Snijder 1,2,
Original Article doi: 10.1111/j.1365-2796.2007.01778.x Vitamin D status and parathyroid hormone levels in relation to blood pressure: a population-based study in older men and women M. B. Snijder 1,2,
Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system
 Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system Basic Elements of cell signaling: Signal or signaling molecule (ligand, first messenger) o Small molecules (epinephrine,
Cell Biology Lecture 9 Notes Basic Principles of cell signaling and GPCR system Basic Elements of cell signaling: Signal or signaling molecule (ligand, first messenger) o Small molecules (epinephrine,
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
ENDOCRINE SYSTEM CLASS NOTES
 ENDOCRINE SYSTEM CLASS NOTES The endocrine system is a collection of glands that secrete hormones directly into the circulatory system to be carried toward a distant target organ. These hormones will be
ENDOCRINE SYSTEM CLASS NOTES The endocrine system is a collection of glands that secrete hormones directly into the circulatory system to be carried toward a distant target organ. These hormones will be
ESPEN Congress Prague 2007
 ESPEN Congress Prague 2007 Key papers in the field of nutrition Dietitian Geila S Rozen Key Papers in the field of Nutrition ESPEN 2007 Prague Geila S Rozen Clinical Nutrition Dep. Rambam health campus
ESPEN Congress Prague 2007 Key papers in the field of nutrition Dietitian Geila S Rozen Key Papers in the field of Nutrition ESPEN 2007 Prague Geila S Rozen Clinical Nutrition Dep. Rambam health campus
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Vitamin D and Cardiovascular Disease
 Vitamin D and Cardiovascular Disease Carrie W. Nemerovski, Pharm.D., Michael P. Dorsch, Pharm.D., Robert U. Simpson, Ph.D., Henry G. Bone, M.D., Keith D. Aaronson, M.D., and Barry E. Bleske, Pharm.D.,
Vitamin D and Cardiovascular Disease Carrie W. Nemerovski, Pharm.D., Michael P. Dorsch, Pharm.D., Robert U. Simpson, Ph.D., Henry G. Bone, M.D., Keith D. Aaronson, M.D., and Barry E. Bleske, Pharm.D.,
Ch45: Endocrine System
 Ch45: Endocrine System Endocrine System Homeostasis is the tendency to maintain a stable internal environment. Function = coordinate and control the body with hormones to maintain homeostasis Works with
Ch45: Endocrine System Endocrine System Homeostasis is the tendency to maintain a stable internal environment. Function = coordinate and control the body with hormones to maintain homeostasis Works with
The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome
 CRC IRB Proposal Matthew Champion PGY-1 8/29/12 The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome Study Purpose
CRC IRB Proposal Matthew Champion PGY-1 8/29/12 The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome Study Purpose
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
