Glaucoma is a common optic neuropathy characterized by
|
|
|
- Jemimah Ryan
- 5 years ago
- Views:
Transcription
1 Glaucoma The Occlusion Model: Paradigm for Induced Ocular Hypertension in Rats and Mice Rebecca M. Sappington, rian J. Carlson, Samuel D. Crish, and David J. Calkins PURPOSE. Elevated intraocular pressure (IOP) is an important risk factor for glaucoma. nimal models often involve techniques for IOP elevation that are surgically invasive. Here the authors describe a novel and relatively simple method for inducing a highly consistent, modest, and repeatable elevation in IOP for rats and mice. METHODS. IOP was elevated unilaterally by injection of polystyrene microbeads into the anterior chamber to occlude aqueous outflow in rats (2.5 7 L) and mice (1 L). The fellow eye received an equivalent saline injection as internal control. The authors used tonometry to measure microbead-induced IOP elevations. Optic nerves were processed histologically to determine axon loss. RESULTS. For rats, a single injection of microbeads raised IOP by 21% to 34%, depending on volume, for approximately 2 weeks, though they were not tracked to full recovery. IOP in the saline-injected eye was constant. n additional injection (5 L) extended the elevation to 8 weeks. Cumulative pressure exposure for both injections increased linearly. For mice, a single 1- L injection of microbeads elicited a highly regular % elevation in IOP that persisted for more than 3 weeks, with a linear rise in cumulative pressure exposure. For both rats and mice, interanimal variability on a given day was modest, approximately 5% of the mean IOP measurement. Extended elevations (4 5 weeks) induced approximately a % loss of axons in both rats and mice. CONCLUSIONS. These data support a novel and flexible model of modest ocular hypertension with axon loss. The maximal duration of IOP elevation will be further characterized in future studies. (Invest Ophthalmol Vis Sci. 1;51:7 216) DOI: /iovs From the Vanderbilt Eye Institute, Vanderbilt University Medical Center, Nashville, Tennessee. Supported by the Melza M. and Frank Theodore arr Foundation through the Glaucoma Research Foundation Catalyst for a Cure initiative (DJC); National Institutes of Health Grant EY17427 (DJC); a Departmental Unrestricted Grant and a Wasserman ward from Research to Prevent lindness, Inc. (DJC); an merican Health ssistance Foundation National Glaucoma ward (DJC); the Vanderbilt Discovery Science program (DJC); Vanderbilt Vision Research Center National Eye Institute Core Grant (5PEY86 19); and fellowships from Fight for Sight, Inc. (RMS, SDC). Submitted for publication May 4, 9; revised June, ugust 13, and September 22, 9; accepted September 27, 9. Disclosure: R.M. Sappington, None;.J. Carlson, None; S.D. Crish, None; D.J. Calkins, None Corresponding author: David J. Calkins, Department of Ophthalmology and Visual Sciences, The Vanderbilt Eye Institute, Vanderbilt University Medical Center, Ophthalmology Research Lab, 115 Medical Research uilding IV, Nashville, TN ; david.j.calkins@vanderbilt.edu. Glaucoma is a common optic neuropathy characterized by the degeneration of retinal ganglion cells and their axons, which comprise the optic nerve. lthough age is the most significant risk factor for the disease, 1 elevated intraocular pressure (IOP) remains the only modifiable risk factor. 2 In humans, whether open or closed angle, glaucoma is characterized by excavation of the optic disc and defects in the nerve fiber layer that are often accompanied by elevations in IOP. 3 Lowering IOP slows glaucomatous progression, even in patients with IOP in the nominally normal range ( 21 mm Hg). 2 Given the impact of IOP on disease outcome, elevated IOP or ocular hypertension is the predominant feature of most animal models of glaucoma. Rodent species offer convenience as model systems for inducing ocular hypertension because they provide the opportunity to conduct large-scale experimental studies and the potential for genetic manipulations. The three most commonly used models elevate IOP substantially (5% 1% above baseline) by altering aqueous fluid dynamics in the anterior segment. 4,5 These have been applied primarily to rats, most likely because of the technical difficulty of manipulating the significantly smaller mouse eye. 4 6 Their merits and weaknesses have been reviewed extensively elsewhere. 5 riefly, episcleral vein injection of hypertonic saline elevates IOP by altering aqueous outflow through sclerosis. 7,8 This elevation persists as long as days but varies dramatically in magnitude between individual animals. 5,7,9 Laser photocoagulation of either the trabecular meshwork alone or in concert with episcleral veins elevates IOP for far shorter durations: 21 days in the rat 1,11 and 6 weeks in the mouse.,13 For these models, both interanimal variability and variability in the magnitude of elevations are limiting factors, necessitating relatively large numbers of experimental cohorts. 5 In contrast, cauterization of two or three episcleral veins alone elevates IOP by reducing venous outflow, thereby increasing aqueous fluid pressure. 8,14 17 lthough relatively consistent between animals, the potential for ocular ischemia and neovascularization can confound interpretation of this model. 5,9 These most widely used models are limited by the absence of a repeatable internal control in which an equivalent insult in the fellow eye would not result in extended elevated IOP. Such a control would allow the assessment of IOP-induced pathology without confounding factors, such as injury induced by the surgical procedure (e.g., vessel cauterization and sclerosis). lthough the potential for uncontrolled confounds is well recognized, there have been few alternatives. dditional rodent systems for ocular hypertension are also available but have been less extensively used. These include ligation of extraocular veins 18 and intra-aqueous injection of hyaluronic acid. 19 We sought to establish a rodent model of ocular hypertension in which both IOP magnitude and duration could be manipulated relatively simply with minimal confounding factors and with an internal control for each animal. Here we describe a procedure for injecting small volumes of polysty- Investigative Ophthalmology & Visual Science, January 1, Vol. 51, No. 1 Copyright ssociation for Research in Vision and Ophthalmology 7
2 8 Sappington et al. IOVS, January 1, Vol. 51, No. 1 rene microbeads into the anterior chamber to impede aqueous outflow and elevate IOP. This model builds on a limited number of earlier studies using microbeads to elevate IOP in primates, rats, 21 and rabbits. 22 For each animal, one eye is injected with microbeads and other is injected with an equivalent volume of saline. For maximal usefulness as a rodent model, we demonstrate our procedure for use in both rats (2.5- to7- L injections) and mice (1- L injections). We show that IOP after microbead injection is highly consistent both in duration and magnitude with interanimal variability approximately 5% of the mean, whereas saline injection affected IOP very little regardless of volume and duration. Overall, the flexibility and consistency of this model, with a simple internal control, affords the opportunity for specific assessment of IOP-induced pathology. MTERILS ND METHODS nimals This study was conducted in accordance with regulations set forth in the RVO Statement for the Use of nimals in Ophthalmic and Vision Research. nimal protocols were approved by the Institutional nimal Care and Use Committee of the Vanderbilt University Medical Center. Male rown Norway rats aged 3 to 7 months were obtained from Charles River Laboratories (Wilmington, M) and individually housed for the duration of the experiments. Male C57L/6 mice aged 3 to 7 months were obtained from Jackson Laboratories (ar Harbor, ME) and housed in groups for the duration of the experiments. Surgeries For microbead surgeries, one eye was injected with sterile - m polystyrene microbeads, conjugated to lexa Fluor 488 chromophore, ina1 1 6 microbeads/ml solution (Molecular Probes, Eugene, OR), and the other eye was injected with an equivalent volume of sterile physiologic saline (Fisher Scientific, Fair Lawn, NJ). s such, each animal serves as its own control. We selected - m-diameter microbeads based on pilot studies in our laboratory evaluating 5- to - m microbeads alone and in combination (data not shown). efore injections, animals were anesthetized with isoflurane (Minrad Inc., ethlehem, P), which was controlled by a pump that allows continuous administration for up to hours. Pupils were dilated with 1% tropicamide ophthalmic solution (ausch & Lomb, Tampa, FL), and anesthetic drops (.5% proparacaine hydrochloride; ausch & Lomb) were applied to each eye. We pulled micropipettes from borosilicate glass capillaries (1./.75 mm OD/ID with filament; World Precision Instruments, Sarasota, FL) to a final diameter of approximately 1 m on a horizontal electrode puller (model P-97; Sutter Instruments Co., Novato, C). For injections, we used a manual microsyringe pump (DMP; World Precision Instruments) equipped with an injection assembly (MMP-KIT; World Precision Instruments). The glass micropipette fit directly into the injection assembly, which was connected to the microsyringe pump by polyethylene tubing. Mineral oil was used to fill the injection apparatus, and the aqueous-oil interface was visually examined after each injection to confirm injection of the appropriate volume. fter dilation of the iris and protraction of the eye with forceps, a micromanipulator was used to position the micropipette above the anterior chamber approximately 3 mm central to the ora serrata. The slope of the micropipette was closely monitored to avoid contact with the lens and to ensure proper filling of the anterior chamber. For rats, 2.5- L, 5- L, or 7- L injection volumes (approximately, 5, or 7 microbeads, respectively) were used. For mice, a 1- L injection volume (approximately 1 microbeads) was used. The rate of injection (1 L/s) was controlled by the experimenter and remained constant between subjects. fter injection, antibiotic drops (.5% moxifloxacin hydrochloride ophthalmic solution; lcon, Fort Worth, TX) were placed on each eye, and the animal was allowed to recover for 24 hours before resumption of IOP measurements. IOP Measurements: Rat To avoid the health risks associated with daily administration of anesthesia and the IOP-lowering effect of anesthetic agents, 23 IOP measurements were performed in awake rats. To allow accurate and humane measurement of IOP in awake rats, we used a behavioral training paradigm that began approximately 2 weeks before experiments. ehavioral Training Paradigm. Rats were handled for 1 week before the initiation of training. For the first phase of training, rats were acclimated to the application of anesthetic drops (.5% tetracaine), tactile contact with each eye, and the alert signals of the tonometer (Tono-Pen; Reichert, Inc., Depew, NY). In the second phase of training, generalized tactile contact with each eye was replaced with actual tonometer contact followed by actual tonometer measurements. The latency between initiation of training and full tonometer measurements was between 5 and 1 days. IOP Measurements. The tonometer was used with a protective thin rubber sheath over the exposed metal sensor. IOP for each eye was determined as the mean of to tonometer readings. aseline IOP readings were recorded for two consecutive days before polystyrene microbead/saline injections. The first experimental IOP readings were obtained 24 hours after injection surgery. IOP readings were then obtained daily until termination of the experiment. To avoid irritation of the cornea, saline eye drops were administered daily to each eye at the completion of IOP measurements. IOP was measured for different lengths of time in cohorts of rats so that we could harvest tissue for other purposes. ll IOPs for each animal are reported; no animal was excluded from our analysis because IOP did not remain elevated. For single 2.5- L injections, IOP measurements for individual rats ranged from 3 to 6 days (n 5) to 2 weeks (n 4) after injection. For single 5- L injections, measurements ranged from 6 days (n 7) to 13 days (n 4); for single 7- L injections, measurements were taken for 1 days in four animals. cohort of seven rats had IOP measured daily until day for a single 5- L injection. Finally, a cohort of 11 rats had two 5- L injections; the second occurring 14 to 17 days after the first. IOP was measured in this cohort for 5 to 8 weeks. IOP Measurements: Mouse IOP measurements in mice were performed as previously described with some modification To avoid agitation and because behavioral training proved difficult given the lack of docility, IOP was measured in an anesthetized, rather than an awake, behaving state. s with the rats, the tonometer (Tono-Pen; Reichert, Inc.) was used with the protective sheath over the sensor. riefly, mice were anesthetized with an isoflurane pump before measurement of IOP. IOP for each eye was determined as the mean of tonometer measurements. To avoid irritation of the cornea, hydrating eyedrops were administered daily to each eye at the completion of IOP measurements. Cohorts of mice also had IOPs measured for different lengths of time. s for the rats in our study, all IOPs for each animal are reported with no animal excluded because IOP did not remain elevated. ll mice reported had a single 1- L injection and IOP measurements ranging from 2 weeks (n 1) to 4 weeks (n 5). Tissue Procurement t the conclusion of the experiments, subjects were administered an overdose of pentobarbital ( mg/kg; Hospira, Inc., Lake Forest, IL) and were killed by transcardial perfusion with 4% paraformaldehyde (Sigma, St. Louis, MO). Whole eyes were dissected from the head and postfixed as necessary. Histopathology For assessment of microspheres in the anterior segment, fluorescence in whole mount preparations of anterior segment were examined with a digitally interfaced, upright microscope equipped with four fluorescent cubes (Olympus, Melville, NY) and fluorescent confocal micros-
3 IOVS, January 1, Vol. 51, No. 1 -Induced Elevations in IOP 9 copy (Olympus) at the Vanderbilt University Cell Imaging Core. For quantification of axonal populations in the optic nerve, we followed a protocol as described in recent work. 26 riefly, a 2- to 3-mm section of optic nerve proximal to the globe was isolated, postfixed for 1 hour in 4% paraformaldehyde, and prepared for embedding and semithin sectioning, as previously described. Using 1 oil-immersion and differential interference contrast optics, photomicrographs of each section were collected as a montage with a microscope containing a motorized X-Y-Z stage and a digital charge-coupled device video camera (Provis X7; Olympus). Each montage was contrast- and edgeenhanced using macro-routines written with a software package (ImagePro; Media Cybernetics, Silver Spring, MD). n additional routine was used to identify and count each axon in the montage for which a myelin sheath could be identified. We used this information to calculate the mean local axon density for each section of nerve. Statistical nalysis nalysis was aided by statistical analysis software (Systat ; Systat Software, Inc., Chicago, IL). For comparisons of means for samples meeting normality criteria, standard parametric statistics were used (Student s t-test, NOV F-statistic). For samples failing normality, nonparametric rank statistics were used (Mann-Whitney U test, Kruskal-Wallis H-statistic). For testing whether the slope of a bestfitting regression line differed from zero and whether two slopes differed, we used the Fisher F-ratio calculated from the least-squares regression. For all cases, only the P value for the corresponding test was indicated for simplicity. The use of additional statistics is explained in the text as needed. RESULTS -Induced Elevations in IOP of the Rat Eye fter dilation of the iris, protraction of the eye with forceps and injection (Figures 1), fluorescent microbeads were widely distributed throughout the aqueous regardless of injection volume and could be seen moving with the flow of aqueous (Fig. 1). Within minutes, fewer microbeads were visible, but they were clustered near the trabecular meshwork region of the anterior chamber (Fig. 1C). To determine whether these microbeads were present near aqueous outflow channels, we used fluorescence microscopy to examine histologic preparations from rat eyes. Clusters of microbeads were observed in the connective tissue of the iridocorneal angle of a flat-mount preparation of the anterior segment (Fig. 1D, left). In vertical sections through the anterior segment, microbeads cluster near the iridocorneal angle (Fig. 1D, right). These observations show that microbeads are carried with the aqueous humor toward the trabecular meshwork. To determine how different volumes of microbeads influence IOP in rats, we injected 2.5 L, 5 L, or 7 L saline or microbeads and monitored IOP from 1 to 2 weeks, generally three to five times per week. Figure 2 depicts the daily IOP measurement for individual animals receiving each injection volume. For saline-injected eyes, IOP fluctuated about a consistent baseline value of approximately 21 mm Hg, whereas microbead injection induced an increase of % to 4% (Fig. 2). Figure 2 also demonstrates that for some animals receiving either 2.5 or 5 L injections, microbead injection elicited a rapid (1 day after injection) elevation in IOP that abated by 7% to 8% for 1 to 2 days before recovering. The mean IOP for the saline eyes across animals and days did not depend on injection volume (Fig. 2, mean SD): mm Hg for 2.5- L, mm Hg for 5- L, and mm Hg for 7- L injections (P.34). For these data, each SD was approximately 5% of the mean; hence, the interday variability was modest for each injection volume. The postinjection IOP in microbead-injected eyes averaged across days tended to increase with injection volume (Fig. 2; bracketed period): mm Hg for 2.5- L, mm Hg for 5- L, and mm Hg for 7- L injections. The increase in mean IOP from 2.5 to 5 L and from 2.5 to 7 L were both highly significant (P.1), whereas the elevated IOPs for 5 and 7 L did not differ (P.7). s with the saline eyes, each SD for the postinjection means was modest (4% 6% of the mean), indicating a highly regular elevation in IOP. That the mean IOP increased with injection volume for the microbead eyes but not for the saline-injected eyes suggested that the increase was the result of the number of actual microbeads rather than fluid volume, as calculated (see Materials and Methods). Figure 2 shows that each microbead injection volume was efficacious in elevating IOP above that for the saline eyes, and indeed each postinjection mean elevation was significant (P.1 for each volume). However, it is apparent from Figure 2 that the interanimal variability decreased with increasing injection volume, so that the 2.5- L rats demonstrated the largest spread in IOP between individuals on a given day, whereas the 7- L rats demonstrated the smallest spread in IOP. Thus, in calculating the mean postinjection IOP for the microbead eye across animals for a given day (Fig. 2), the average daily SD decreased from 2.1 for 2.5- L to 1.7 for 5- L to 1.2 for 7- L injections (4%; P.6). These correspond to 8%, 6%, and 4% of the mean postinjection IOP, respectively. This change is apparent in the diminishing magnitude of the error bars with increasing microbead injection volume in Figure 2. For 7 L, certainly the smaller size of the cohort could contribute to less variability. We then calculated the difference in mean IOP between the saline- and microbead-injected eyes over time by subtracting the data shown in Figure 2. s suggested in Figure 2, the magnitude of this difference (i.e., the IOP elevation) was dependent on injection volume (Fig. 3). For 2.5- L injected animals, the mean difference in postinjection IOP between microbead and saline eyes was mm Hg. For the 5- L injected animals, this difference increased significantly to mm Hg (P.1). For the 7- L injected animals, the difference was mm Hg, which was statistically different from the 2.5- L difference (P.1) but not from the 5- L difference (P.42). For 5 L, the difference in IOP between the saline- and microbead-injected eyes for the postinjection period had a best-fitting regression line whose slope was not different from zero (P.58). The difference curves in Figure 3 demonstrate that after injection, IOP elevation remained relatively stable compared with the saline eye over this short experimental period. s such, the cumulative exposure to elevated IOP should increase roughly linearly with time. 27 To test this directly, we calculated the cumulative area under the difference curves in Figure 3 as a function of time in units of millimeter of mercury per days (Fig. 3). s expected, the cumulative exposure to pressure increased nearly monotonically for each injection volume. To test this, we determined the best-fitting multiparameter sigmoidal function and compared the goodness-of-fit with that of the best-fitting regression line for the 2.5- L and 5- L cumulative pressure data sets, both of which had several more data points than the 7- L set. The best-fitting sigmoids are shown in Figure 3. For the 2.5- L data, the sigmoidal function provided a significantly improved prediction of the data over the bestfitting line (Fisher F ratio 3.7; P.2). In contrast, for the 5- L data, the best-fitting sigmoid approached a straight line and in fact was not different from the regression line (Fisher F ratio.32; P.95). The rate of pressure accumulation for the 5- L injection was also significantly higher than the 2.5- L injection (slope of 7.1 vs. 5.3; P.1).
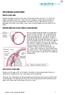
4 21 Sappington et al. IOVS, January 1, Vol. 51, No. 1 C D cornea ciliary body 1µm iris Given that the 5- L injection seemed to yield the most consistent elevation in IOP, we determined next how long a single microbead injection would elevate IOP. Figure 3C demonstrates the mean daily IOP averaged across a cohort of seven 5µm FIGURE 1. Injection of microbeads into the anterior chambers of rats. () injection into the anterior chamber of a rat eye using a glass micropipette (approximately 1- m diameter; arrowhead) with forceps (arrow) to retract the eyelid and stabilize the eye. Low- and highmagnification views included. () Photomicrographs of the anterior segment immediately after injection with 5 L saline (left) or 5 L microbeads (right). s are apparent in the aqueous with no evidence of overt trauma to cornea or iris. (C) -injected eye minutes after 5 L injection (left). s localize in the posterior region of the anterior segment toward the area of aqueous outflow (arrow, magnified in the right). (D) Confocal fluorescence micrograph of flat-mounted anterior chamber from an eye injected with 5 L microbeads (left). Location is near the trabecular meshwork around the iridocorneal angle. In vertical section (right), microbeads are apparent in the iridocorneal angle and cluster near the point of aqueous outflow (arrow). rats followed until day. s earlier, postinjection IOP remained stable to approximately day 13. lthough there appeared to be a slight downward trend, the slope of the bestfitting regression line for this period was not significantly
5 IOVS, January 1, Vol. 51, No. 1 -Induced Elevations in IOP µl 2.5µl 26.9 ± 1.7 FIGURE 2. Injection volume determines magnitude of IOP elevation in rats. () Daily IOP measurements for individual rats receiving a single 2.5 L (n ), 5 L (n 21), or 7 L (n 4) unilateral injection of microbeads (filled circles) and an equivalent volume of saline (open circles) in the opposing eye. IOP is plotted as a function of time, where day is before injection and day 1 is 24 hours after injection. IOP was monitored for 3 to 13 days (2.5- L injections), 6 days to 2 weeks (5 L), or 1 days (7 L). rackets indicate increase in IOP 1 day after injection for 2.5- L and 5- L bead injections, followed by a transient decline. () IOP averaged across the cohort injected once with 2.5 L, 5 L, or 7 L microbeads in the test eye (filled circles) and equivalent volume of saline in the other eye (open circles). rackets indicate postinjection period with corresponding mean SD. 5µl 7µl µl 7µl 28.8 ± ± different from zero (P.17). However, after this point, IOP in the microbead eyes began to decrease, falling by more 2.5 mm Hg by day. This was a significant decline from the postinjection period through day 13 (P.5), indicating that the first sign of IOP recovery from a single 5- L injection can occur at about 2 weeks. Extension of IOP Elevation in the Rat Next we sought to determine whether IOP elevation could be extended by a subsequent injection of 5 L. s earlier, the control eye received an equivalent volume of saline. For each animal in a cohort of 11, IOP from an initial 5- L injection was followed to 13 days, with a second injection given between days 14 and 17. This point was chosen based on the data in Figure 3C, which indicated IOP began to drop approximately 2 weeks after the first injection. IOP was then followed in most of the animals for an additional to 23 days, for a total period of just more than 5 weeks. IOP was followed in a small subset of the animals for nearly 8 weeks. Individual animal IOPs are shown in Figure 4 for the entire experimental period. IOP was highly regular between the two injections (Fig. 4). For the saline eye, mean IOP after the second injection ( mm Hg) was the same as that for the first (21..5 mm Hg; P.89). For the microbead eye, mean IOP after injection for the second injection was also similar to the first: mm Hg versus mm Hg (P.). The slopes of the best-fitting regression lines did not differ for the two postinjection periods for the microbead eyes (P.6), indicating similarity in IOP elevation. In addition, the regression lines for the entire 8-week period for both the saline and the microbead IOPs had slopes that did not differ from zero (P.66). Thus, a second injection of equal volume could extend the IOP elevation by an additional 3 to 6 weeks without a significant change in the magnitude of elevation. The constancy in IOP between the first and second microbead injections is illustrated explicitly in Figure 4C, which shows the difference in daily mean IOP between the microbead- and saline-injected eyes. For the second injection, the postinjection difference was mm Hg compared with mm Hg for the first (P.). Cumulative exposure to elevated IOP in millimeters of mercury per days for the entire injection period increased monotonically (Fig. 4D). The goodness-of-fit for the best-fitting multiparameter sigmoidal function was not significantly improved from that for the best-fitting regression line (Fisher F ratio.42; P.8). The latter had a rate of accumulation of 7.6 mm Hg/d, very close to the rate of 7.1 mm Hg/d for the single 5- L injection shown in Figure 3. These data indicate that though the elevation in IOP afforded by a second 5- L injection was similar in magnitude to that elicited by a single injection, the period of elevation was much longer up to 6 additional weeks. -Induced IOP Elevations in Mouse Eyes Next, we examined whether a 1- L microbead injection could elevate IOP in C57L/6 mice. We chose this volume based on the size difference between the anterior chambers of rats and
6 2 Sappington et al. IOVS, January 1, Vol. 51, No. 1 Test-Control (mmhg) Test-Control (mmhg) Test-Control (mmhg) µl 5µl 7µl mmhg Days C µl 5µl 7µl FIGURE 3. Injection volume and pressure exposure over time in rats. () Difference in mean IOP between microbead- and saline-injected rat eyes (test-control) after a single 2.5- L, 5- L, or 7- L injection plotted against exposure time, where day is before injection and day 1 is 24 hours after injection. () Cumulative exposure to elevated IOP over time (millimeters of mercury per day) calculated from the difference curves in () for a 2.5- L (white circles), 5- L (gray circles), or 7- L (black circles) injection. Lines represent best-fitting multiparameter sigmoidal functions for the 2.5- L and 5- L data. (C) Daily IOP averaged across a cohort of seven rats receiving a single 5- L injection of microbeads (filled circles) and equivalent volume of saline in opposing eye (open circles); measurements taken until day after injection for each animal. Data represent mean SD C mmhg Days Test-Control (mmhg) D FIGURE 4. Second injection of 5 L extends IOP elevation in rats. (, top) Daily IOP measurements for individual rats (n 11) with two 5- L unilateral injections of microbeads (filled circles) and an equivalent volume of saline (open circles) inthe opposing eye. Day is before injection and day 1 is 24 hours after the first injection. Each animal received the second injection 14 to 17 days after the first. Seven of the animals were followed to approximately 5 weeks, and the rest were monitored to nearly 8 weeks. () Mean daily IOP across the cohort for first and second injections. (C) Difference in mean IOP between the microbead and saline eyes (test-control) for the entire experimental period. (D) Cumulative exposure to elevated IOP over time (mm Hg per day) calculated from the difference curves in C for dual 5- L injections. For all panels, the period containing the second injection (14 17 days) is indicated (shaded region).
7 IOVS, January 1, Vol. 51, No. 1 -Induced Elevations in IOP 213 FIGURE 5. Single injection of 1 L elevates IOP in mice. () Daily IOP measurements for individual mice (n 6) after a single 1- L unilateral injection of microbeads (filled circles) and an equivalent volume of saline (open circles) in the opposing eye. Eyes were monitored for 23 days after injection without a significant decrease in IOP. Day is before injection and day 1 is 24 hours after injection. Line represents IOP averaged across the cohort (mean SD). () second cohort of mice (n 8) with same injection regimen as in () but with a different experimenter. IOP returned to baseline by day 21. (C) Difference in mean IOP between microbead- and salineinjected mouse eyes (test-control) for the cohorts shown in () and () plotted against exposure time. (D) Cumulative exposure to elevated IOP over time (mm Hg per day) calculated from the difference curves in (C) with bestfitting multiparameter sigmoidal function (solid lines). racket indicates period without additional accumulation for the cohort in () C D Test-Control (mmhg) mmhg Days cohort cohort 5 1 cohort cohort 5 1 mice. In rats, the volume of the anterior chamber is approximately L 28 compared with 7 L in mice. 29 IOP was measured every 1 day to 2 days, as described, for 23 days for one cohort (n 6; Fig. 5) and for 21 days for a second cohort (n 8; Fig. 5). Injections for the second cohort were performed by a less experienced user. For the first cohort (Fig. 5), IOP for the saline eye fluctuated about a baseline value of approximately mm Hg (.3.8 mm Hg). injection induced an increase of approximately % (..8 mm Hg), a significant elevation (P.1). oth sets of measurements were approximately % lower than for rats, some of which could be attributable to our use of isoflurane anesthesia. s seen in rats (Fig. 2), each SD across days for both the saline and the microbead IOPs was approximately 5% of the mean; hence, the interday variability was modest, indicating a highly regular elevation in IOP. The interanimal variability also was modest. In calculating the mean IOP for the microbead eye across animals for a given day, the average daily SD after injection was 1.3 mm Hg (approximately 7.5% of the mean), which was the same for the saline eye. For the second cohort of mice (Fig. 5), the IOP for the saline eye was similar to that for the first cohort: mm Hg. However, the IOP elevation for the microbead eye was significantly lower: mm Hg (P.1). This was due in part to a lesser peak value of approximately 19 mm Hg compared with 21 to 22 mm Hg for the first cohort. However, IOP elevation in the microbead eye also decreased relatively rapidly, returning to the saline eye values by day 21 (P.1). For the first cohort (Fig. 5), the difference in postinjection IOP between microbead and saline eyes was mm Hg and was nearly flat across days (Fig. 5C). The slope of the best-fitting regression line for the postinjection period was not significantly different from zero (P.31). For the second cohort, in contrast, the difference curve was flat only until day 7, at which point it decreased until reaching a value close to by day 21. The best-fitting multiparameter sigmoidal function for the cumulative pressure exposure for the first cohort (Fig. 5) was not significantly different from the best-fitting regression line (P.24; Fig. 5D). For this line, the rate of pressure accumulation was 4.7 mm Hg/d (P.1). For the second cohort (Fig. 5), the sigmoidal function provided a significantly improved representation of the data over the best-fitting line (Fisher F ratio 4.8; P.8). This was apparent especially for latter times for which accumulation did not change (Fig. 5D, bracketed area). Thus, though a single 1- L injection of microbeads in the mouse can elevate IOP above baseline for more than 3 weeks, variability was seen in the duration of IOP elevation between the two cohorts. Pathology in the Optic Nerve Resulting from -Induced IOP Elevation xonal degeneration in the optic nerve is an important hallmark for models of glaucoma involving increased IOP. 4 7 To ascertain whether elevations due to microbead injection similarly induce optic nerve abnormalities, we prepared crosssections through the optic nerves of both rats and mice and quantified mean axon density and number of axons. Figure 6 shows examples of nerves from the saline-injected right eye (left) and microbead-injected left eye (right) for the cohort of rats we monitored until approximately 5 weeks after receiving a second 5- L injection 14 to 17 days after the first (Fig. 4, IOP). The nerve from the microbead eye demonstrates clear axonal disorder, reduction in axon packing, and axonal distension. Figure 6 shows similar examples from the mice receiving a single 1- L injection with elevated IOPs for approximately 4 weeks (Fig. 5). For the rat cohort, average axon density in nerves from the saline/right eyes ( axons/mm 2 ) was the same as naive nerves ( axons/mm 2 ; P.85), whereas axon density in nerves from the microbead/left eyes was 16% lower ( axons/mm 2 ; P.4). For mice, average axon density in the saline nerves ( axons/mm 2 ) did not differ from that of naive nerves ( axons/mm 2 ; P.53), whereas axon density in the microbead nerves was 27% lower ( axons/
8 214 Sappington et al. IOVS, January 1, Vol. 51, No. 1 C 1.2 xon Density xon Counts Naive / 1. Left Eye / Right Eye 1µm * * * * Rat Mouse Rat mm2; P.3). We also calculated the total number of axons in the nerves by multiplying axon density by the cross-sectional nerve area. s with axon density, the average number of axons in rat nerves from saline eyes ( axons) was the same as in naive nerves ( axons; P.53), whereas the number of axons in microbead nerves was % lower ( axons; P.4). Similarly, for mice, the average number of axons in saline nerves was the same as for naive nerves ( axons; P.6), whereas microbead nerves had % less ( axons; P.4). Thus, sustained elevations in IOP induced by microbead injections resulted in modest but measurable thinning of the axon population in the optic nerve. For simplicity, Figure 6C shows axon density and axon number as ratios (left to right eyes) for Mouse FIGURE 6. Optic nerve abnormality resulting from microbead-induced elevations in IOP. () High-magnification light micrographs of cross-sections through rat optic nerve after dual 5- L injections of saline (left) or microbeads (right). Second injection occurred 2 weeks after the first; tissue was harvested 22 days later. IOPs are shown in Figure 4E. Nerve of bead-injected eye shows diminished axon density, enlarged axons (white arrows), and degenerating axon profiles (black arrowheads). () Crosssections through mouse optic nerve after a single 1- L injection of saline (left) or microbeads (right). Tissue was harvested 28 days after injection; IOPs are shown in Figure 5. Nerve from microbead eye shows diminished axon density, glial hypertrophy (black arrows), and degenerating profiles (black arrowheads). Scale applies to all micrographs. (C) Mean axon density and total number of axons for optic nerves from naive, saline-injected (right eye) and microbead-injected (left eye) rats and mice, shown as ratios of left to right eyes. sterisks indicate a significant difference between saline- and microbead-injected nerves for both rat (% decrease, dual 5- L injections) and mice (23% decrease, single 1- L injection). IOPs of rat cohort are shown in Figure 4E; those of the mouse are shown in Figure 5. both rats and mice. For naive samples, the two eyes were identical for all measurements, leading to ratios close to unity (P ⱖ.). DISCUSSION In this study, we describe a means for the induction of modest ocular hypertension in rodents in which both the magnitude and the duration of IOP elevation can be reliably manipulated by the injection of polystyrene microbeads into the anterior chamber (Fig. 1). Our model builds on a limited number of earlier studies using microbeads to elevate IOP in primates, rats,21 and rabbits.22 In our paradigm, microbead injection was
9 IOVS, January 1, Vol. 51, No. 1 -Induced Elevations in IOP 2 limited to one eye, with the other eye receiving an equivalent volume of saline. This serves as a convenient internal control for the surgical procedure except for the microbeads themselves. Examination of the anterior segment after injection suggests that the microbeads could have been carried by the flow of aqueous humor into the region of the trabecular meshwork, where they congregated (Fig. 1). lthough microbead injection elicited reliable elevations in IOP for both rats and mice, equivalent-volume injections of saline in the fellow eye had little or no lasting effect on IOP. It is reasonable to conclude that elevations in IOP observed in the microbead-injected eye are the result of impeded outflow rather than an increase in general volume of the anterior segment or some other facet of the surgical procedure (i.e., inflammation or corneal wound healing). The relatively small day-to-day variability once IOP is elevated can be explained by simple persistence of the microbeads near the outflow region. This remains to be tested explicitly. We found that the magnitude of IOP elevation in rats, as measured by tonometry, could be controlled by varying the injection volume because larger volumes (i.e., more microbeads) induced a higher elevation. For example, in the rat, a single 2.5- L injection of microbeads elevated IOP on average by mm Hg compared with mm Hg for a 5- L injection (P.1). These increments represented a 21% and a 34% increase, respectively, compared with the saline companion eye (Figs. 2, 3). Increasing the volume to 7 L did not significantly increase IOP compared with 5 L (Fig. 3). The elevation in IOP afforded by a single 5- L injection persisted for approximately 2 weeks, with a statistically linear accumulation of pressure exposure during this period (Figs. 3, C). second 5- L injection elevated IOP up to an additional 6 weeks, with a magnitude and a rate of accumulation of pressure exposure very similar to that of a single injection (Figs. 4C, D). Thus, two 5- L injections can elicit a near constant elevation in IOP for approximately 8 weeks (Fig. 4E). That the period of elevation afforded by a second 5- L injection lasts so much longer probably indicates a cumulative buildup of microbeads in the outflow region that reaches some critical mass. We doubt that this elevation is permanent, but its complete duration remains to be determined in future planned experiments. s well, in this study we did not track IOP from the first injection to full recovery to baseline. Thus, though modest recovery was observed by approximately 2 weeks, the precise duration remains unknown until additional studies are completed. For mice, we found that a single 1- L microbead injection could elicit a mm Hg elevation above IOP for the saline eye, a % increment comparable to that of the rat (Figs 5, C). This elevation could persist for slightly more than 3 weeks, affording a statistically linear accumulation in exposure to increased pressure (Fig. 5D). However, there was significant variability in the durability of this single injection that depended on the experimenter: a second cohort from a relatively newer user demonstrated IOP elevation of lower magnitude and duration (Fig. 5). This might have resulted, for example, from the inadvertent presence of air bubbles in the injection apparatus yielding a slightly smaller injection volume. In this sense, a single 1- L injection for the mouse eye can have an effect similar to that of back-to-back 5- L injections in the larger rat eye, depending on the success of the injection. Even so, similar to the 5- L injection in rats, the interanimal variability was modest: on a given day, IOP varied between animals by approximately 5% of the mean. The % elevation in IOP arising from microbead injection in rodents more closely resembles changes in IOP associated with mild to moderate ocular hypertension in untreated human eyes, which are on average 38% above mm Hg. In contrast, in other heavily used models, the magnitude of IOP elevation is frequently 5% to 1% above that of the fellow eye and is entirely dependent on the success of the surgical procedure. 4,5,1 Combined with its reliability after microbead injection, the less severe magnitude of IOP elevation could prove useful in identifying subtle aspects of the early response in glaucoma. We found that the % elevation in IOP elicited a modest but measurable thinning of the axon population in the optic nerve for both rats and mice after 4 to 5 weeks (Fig. 6). This thinning was concurrent with signs of the typical hallmarks of glaucomatous pathology (gliosis, degenerating profiles, disorganization), which also were modest compared with other models. ecause such incremental changes could present a problem to preclinical testing of neuroprotective interventions, more extensive studies are under way to determine whether nerve abnormalities continue to progress with a more extensive period of IOP elevation. cknowledgments The authors thank Quintus Ngumah at the University of labama irmingham for early advice on technique and the Vanderbilt University Medical Center Cell Imaging Shared Resource core facility for support with confocal imagery. References 1. Coleman L, Miglior S. Risk factors for glaucoma onset and progression. Surv Ophthalmol. 8;53(suppl 1):S3 S1. 2. Kass M, Heuer DK, Higginbotham EJ, et al. The ocular hypertension treatment study a randomized trial determines that topical ocular hypotensive medication delays or prevents the onset of primary open angle glaucoma. rch Ophthalmol. 2;1: Jonas J, udde WM. Diagnosis and pathogenesis of glaucomatous optic neuropathy: morphological aspects. Prog Retinal Eye Res. ;19: Morrison JC. Elevated intraocular pressure and optic nerve injury models in the rat. J Glaucoma. 5;14: Pang IH, Clark F. Rodent models for glaucoma retinopathy and optic neuropathy. J Glaucoma. 7;16: McKinnon SJ, Schlamp CL, Nickells RW. Mouse models of retinal ganglion cell death and glaucoma. Exp Eye Res. 9;88: Morrison JC, Moore CG, Deppmeier LM, et al. rat model of chronic pressure-induced optic nerve damage. Exp Eye Res. 1997; 64: Nissirios N, Chanis R, Johnson E, et al. Comparison of anterior segment structures in two rat glaucoma models: an ultrasound biomicroscopic study. Invest Ophthalmol Vis Sci. 8;49: Goldblum D, Mittag T. Prospects for relevant glaucoma models with retinal ganglion cell damage in the rodent eye. Vision Res. 2;42: Ueda J, Sawaguchi S, Hanyu T, et al. Experimental glaucoma model in the rat induced by laser trabecular photocoagulation after an intracameral injection of India ink. Jpn J Ophthalmol. 1998;42: Levkovitch-Verbin H, Quigley H, Martin KR, et al. Translimbal laser photocoagulation to the trabecular meshwork as a model of glaucoma in rats. Invest Ophthalmol Vis Sci. 2;43: ihara M, Lindsey JD, Weinreb RN. Experimental mouse ocular hypertension: establishment of the model. Invest Ophthalmol Vis Sci. 3;44: Grozdanic SD, etts DM, Sakaguchi DS, et al. Laser-induced mouse model of chronic ocular hypertension. Invest Ophthalmol Vis Sci. 3;44: Sawada, Neufeld H. Confirmation of the rat model of chronic moderately elevated intraocular pressure. Exp Eye Res. 1999;69: ayer U, Danias J, rodie S, et al. Electroretinographic abnormalities in a rat glaucoma model with chronic elevated intraocular pressure. Exp Eye Res. 1;
10 216 Sappington et al. IOVS, January 1, Vol. 51, No Shareef SR, Garcia-Valenzuela E, Salierno, et al. Chronic ocular hypertension following episcleral venous occlusion in rats. Exp Eye Res. 1995;61: Mittag TW, Danias J, Pohorenec G, et al. Retinal damage after 3 to 4 months of elevated intraocular pressure in a rat glaucoma model. Invest Ophthalmol Vis Sci. ;41: Yu S, Tanabe T, Yoshimura N. rat model of glaucoma induced by episcleral vein ligation. Exp Eye Res. 6;83: enozzi J, Nahum LP, Campanelli JL, et al. Effect of hyaluronic acid on intraocular pressure in rats. Invest Ophthalmol Vis Sci. 2; 43: Weber J, Zelenak D. Experimental glaucoma in the primate induced by latex microspheres. J Neurosci Methods. 1;111: Urcola JH, Hernandez M, Vecino E. Three experimental glaucoma models in rats: comparison of the effects of intraocular pressure elevation on retinal ganglion cell size and death. Exp Eye Res. 6;83: Ngumah QC, uchthal SD, Dacheux RF. Longitudinal non-invasive proton NMR spectroscopy measurement of vitreous lactate in a rabbit model of ocular hypertension. Exp Eye Res. 6;83: Jia L, Cepurna WO, Johnson EC, et al. Effect of general anesthetics on IOP in rats with experimental aqueous outflow obstruction. Invest Ophthalmol Vis Sci. ;41: Sappington RM, Sidorova T, Long DJ, Calkins D. TRPV1: contribution to retinal ganglion cell apoptosis and increased intracellular Ca 2 with exposure to hydrostatic pressure. Invest Ophthalmol Vis Sci. 9;5: Sappington RM, Calkins DJ. Contribution of TRPV1 to microgliaderived IL-6 and NF translocation with elevated hydrostatic pressure. Invest Ophthalmol Vis Sci. 8;49: Inman DM, Sappington RM, Horner PJ, Calkins DJ. Quantitative correlation of optic nerve pathology with ocular pressure and corneal thickness in the D/2 mouse model of glaucoma. Invest Ophthalmol Vis Sci. 6;47: McKinnon SJ, Lehman DM, Kerrigan-aumrind L, et al. Caspase activation and amyloid precursor protein cleavage in rat ocular hypertension. Invest Ophthalmol Vis Sci. 2;43: Mermoud, aerveldt G, Minckler DS, Prata J Jr, Rao N. queous humor dynamics in rats. Graefes rch Clin Exp Ophthalmol. 1996;234(suppl 1):S198 S Zhang D, Vetrivel L, Verkman S. quaporin deletion in mice reduces intraocular pressure and aqueous fluid production. J Gen Physiol. 2;119: Sommer, Tielsch JM, Katz J, et al. Relationship between intraocular pressure and primary open angle glaucoma among white and black mericans: the altimore Eye Survey. rch Ophthalmol. 1991;19:
Glaucoma is the second leading cause of blindness worldwide.
 Translimbal Laser Photocoagulation to the Trabecular Meshwork as a Model of Glaucoma in Rats Hana Levkovitch-Verbin, Harry A. Quigley, Keith R. G. Martin, Danielle Valenta, Lisa A. Baumrind, and Mary Ellen
Translimbal Laser Photocoagulation to the Trabecular Meshwork as a Model of Glaucoma in Rats Hana Levkovitch-Verbin, Harry A. Quigley, Keith R. G. Martin, Danielle Valenta, Lisa A. Baumrind, and Mary Ellen
Glaucoma Drops Control Intraocular Pressure and Protect Optic Nerves in a Rat Model of Glaucoma
 Glaucoma Drops Control Intraocular Pressure and Protect Optic Nerves in a Rat Model of Glaucoma John C. Morrison, 1^ Kristina B. Nylander, 1 Andreas K. Lauer, 1 William. Cepurna, 1 and Elaine Johnson l
Glaucoma Drops Control Intraocular Pressure and Protect Optic Nerves in a Rat Model of Glaucoma John C. Morrison, 1^ Kristina B. Nylander, 1 Andreas K. Lauer, 1 William. Cepurna, 1 and Elaine Johnson l
Retinal Nerve Fiber Analysis: the Role It Plays in Assessing Glaucoma Grace Martin, CPOT
 Retinal Nerve Fiber Analysis: the Role It Plays in Assessing Glaucoma Grace Martin, CPOT Every day, patients experiencing visual difficulties are seen in the optometric practice. This can range from a
Retinal Nerve Fiber Analysis: the Role It Plays in Assessing Glaucoma Grace Martin, CPOT Every day, patients experiencing visual difficulties are seen in the optometric practice. This can range from a
MATERIALS AND METHODS
 Glaucoma A Novel Method for the Induction of Experimental Glaucoma Using Magnetic Microspheres Paulina A. Samsel, 1 Lilian Kisiswa, 1 Jonathan T. Erichsen, 1 Stephen D. Cross, 1 and James E. Morgan 1,2
Glaucoma A Novel Method for the Induction of Experimental Glaucoma Using Magnetic Microspheres Paulina A. Samsel, 1 Lilian Kisiswa, 1 Jonathan T. Erichsen, 1 Stephen D. Cross, 1 and James E. Morgan 1,2
CLASS-y Laser Treats Glaucoma
 Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
1/31/2018. Course Objectives. Diagnostic Testing. Optic Nerve Damage ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY TECHNICIAN: -SDP
 ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
Written by Administrator Wednesday, 13 January :27 - Last Updated Thursday, 21 January :34
 angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
angle closure glaucoma A type of glaucoma caused by a sudden and severe rise in eye pressure. Occurs when the pupil enlarges too much or too quickly, and the outer edge of the iris blocks the eye s drainage
Experimental Glaucoma Model in the Rat Induced by Laser Trabecular Photocoagulation After an Intracameral Injection of India Ink
 LABORATORY INVESTIGATIONS Experimental Glaucoma Model in the Rat Induced by Laser Trabecular Photocoagulation After an Intracameral Injection of India Ink Jun Ueda,* Shoichi Sawaguchi,* Takako Hanyu,*
LABORATORY INVESTIGATIONS Experimental Glaucoma Model in the Rat Induced by Laser Trabecular Photocoagulation After an Intracameral Injection of India Ink Jun Ueda,* Shoichi Sawaguchi,* Takako Hanyu,*
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
SAFE, PERMANENT EYE-COLOR CHANGE
 SAFE, PERMANENT EYE-COLOR CHANGE Prepared by Gregg Homer JSD (PhD) February 1, 2012 THE PIGMENTARY GLAUCOMA ISSUE Glaucoma Defined Glaucoma is currently defined as a disturbance of the structural or functional
SAFE, PERMANENT EYE-COLOR CHANGE Prepared by Gregg Homer JSD (PhD) February 1, 2012 THE PIGMENTARY GLAUCOMA ISSUE Glaucoma Defined Glaucoma is currently defined as a disturbance of the structural or functional
Preclinical Models of Ocular Glaucoma at CBI
 Preclinical Models of Ocular Glaucoma at CBI Comparative Biosciences, Inc. 786 Lucerne Drive Sunnyvale, CA 94085 Telephone: 408.738.9260 www.compbio.com Premier Preclinical Contract Research Organization
Preclinical Models of Ocular Glaucoma at CBI Comparative Biosciences, Inc. 786 Lucerne Drive Sunnyvale, CA 94085 Telephone: 408.738.9260 www.compbio.com Premier Preclinical Contract Research Organization
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
WORLD GLAUCOMA WEEK What is Glaucoma? Can I develop glaucoma if I have increased eye pressure?
 WORLD GLAUCOMA WEEK What is Glaucoma? Glaucoma is a group of diseases that damage the optic nerve and can result in gradual vision loss and blindness. However, with early detection and treatment, you can
WORLD GLAUCOMA WEEK What is Glaucoma? Glaucoma is a group of diseases that damage the optic nerve and can result in gradual vision loss and blindness. However, with early detection and treatment, you can
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Radiation Pretreatment Does Not Protect the Rat Optic Nerve From Elevated Intraocular Pressure Induced Injury
 Glaucoma Radiation Pretreatment Does Not Protect the Rat Optic Nerve From Elevated Intraocular Pressure Induced Injury Elaine C. Johnson, 1 William O. Cepurna, 1 Dongseok Choi, 1,2 Tiffany E. Choe, 1 and
Glaucoma Radiation Pretreatment Does Not Protect the Rat Optic Nerve From Elevated Intraocular Pressure Induced Injury Elaine C. Johnson, 1 William O. Cepurna, 1 Dongseok Choi, 1,2 Tiffany E. Choe, 1 and
Training Checking Vision Tonometry
 Training 101-2 Checking Vision Tonometry Checking Vision The classic example of an eye chart is the Snellen eye chart, in general they show 11 rows of capital letters. The top row contains one letter (usually
Training 101-2 Checking Vision Tonometry Checking Vision The classic example of an eye chart is the Snellen eye chart, in general they show 11 rows of capital letters. The top row contains one letter (usually
Intraoperative Gonioscopy: A Key to Angle Surgery
 Intraoperative Gonioscopy: A Key to Angle Surgery Shakeel Shareef, MD Associate Professor Flaum Eye Institute Univ. of Rochester School of Med. Rochester, NY Phaco vs. MIGS PHACO MIGS Viewing Full corneal
Intraoperative Gonioscopy: A Key to Angle Surgery Shakeel Shareef, MD Associate Professor Flaum Eye Institute Univ. of Rochester School of Med. Rochester, NY Phaco vs. MIGS PHACO MIGS Viewing Full corneal
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
relative s privacy, do not identify your relative by full name in any assignment.
 Overview Do you or a family member have glaucoma? Do you wonder what this diagnosis means? Glaucoma affects tens of millions of people worldwide. Despite its prevalence, many people lack accurate information
Overview Do you or a family member have glaucoma? Do you wonder what this diagnosis means? Glaucoma affects tens of millions of people worldwide. Despite its prevalence, many people lack accurate information
Speaker Disclosure Statement. " Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose.
 Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Speaker Disclosure Statement Dr. Tim Maillet and Dr. Vladimir Kozousek have no conflicts of interest to disclose. Diabetes Morbidity Diabetes doubles the risk of stroke. Diabetes quadruples the risk of
Ganglion Cell Death in Rat Retina by Persistent Intraocular Pressure Elevation
 Korean J Ophthalmol Vol. 18:15-22, 2004 Ganglion Cell Death in Rat Retina by Persistent Intraocular Pressure Elevation Do Hyun Kim, MD, Hwa Sun Kim, MS, Myung Douk Ahn, MD, Myung Hoon Chun, MD* Department
Korean J Ophthalmol Vol. 18:15-22, 2004 Ganglion Cell Death in Rat Retina by Persistent Intraocular Pressure Elevation Do Hyun Kim, MD, Hwa Sun Kim, MS, Myung Douk Ahn, MD, Myung Hoon Chun, MD* Department
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs
 The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature of
 1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
Noninvasive Measurement of Rodent Intraocular Pressure with a Rebound Tonometer
 Noninvasive Measurement of Rodent Intraocular Pressure with a Rebound Tonometer Wan-Heng Wang, J. Cameron Millar, Iok-Hou Pang, Martin B. Wax, and Abbot F. Clark PURPOSE. The present study evaluated the
Noninvasive Measurement of Rodent Intraocular Pressure with a Rebound Tonometer Wan-Heng Wang, J. Cameron Millar, Iok-Hou Pang, Martin B. Wax, and Abbot F. Clark PURPOSE. The present study evaluated the
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
GLAUCOMA. An Overview
 GLAUCOMA An Overview Compiled by Campbell M Gold (2004) CMG Archives http://campbellmgold.com --()-- IMPORTANT The health information contained herein is not meant as a substitute for advice from your
GLAUCOMA An Overview Compiled by Campbell M Gold (2004) CMG Archives http://campbellmgold.com --()-- IMPORTANT The health information contained herein is not meant as a substitute for advice from your
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Apoptosis in Retinal Ganglion Cell Decrease in Human Glaucomatous Eyes
 ELSEVIER Apoptosis in Retinal Ganglion Cell Decrease in Human Glaucomatous Eyes Shigekuni Okisaka, Akira Murakami, Atsushi Mizukawa and Junji Ito Department of Ophthalmology, National Defense Medical College,
ELSEVIER Apoptosis in Retinal Ganglion Cell Decrease in Human Glaucomatous Eyes Shigekuni Okisaka, Akira Murakami, Atsushi Mizukawa and Junji Ito Department of Ophthalmology, National Defense Medical College,
Corporate Medical Policy
 Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Glaucoma What You Should Know
 Glaucoma What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research that leads
Glaucoma What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research that leads
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Vision Research & Clinical Trials Havener Eye Institute Jenna Rajczyk Demarcus Williams 13 April 2018
 Vision Research & Clinical Trials Havener Eye Institute Jenna Rajczyk Demarcus Williams 13 April 2018 Our Journey to Clinical Research Types of Research Animal Behavioral Basic/Fundamental Translational
Vision Research & Clinical Trials Havener Eye Institute Jenna Rajczyk Demarcus Williams 13 April 2018 Our Journey to Clinical Research Types of Research Animal Behavioral Basic/Fundamental Translational
Understanding Angle Closure
 Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Around The Globe in 60 Minutes
 Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
 European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
THE EYE: RETINA AND GLOBE
 Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Vision I. Steven McLoon Department of Neuroscience University of Minnesota
 Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
Vision I Steven McLoon Department of Neuroscience University of Minnesota 1 Eye Cornea Sclera Conjunctiva 2 Eye The conjunctiva lines the inner surface of the eyelids and outer surface of the sclera. 3
Elevated intraocular pressure (IOP) is a major risk factor for
 Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Micro-Invasive Glaucoma Surgery (Aqueous Stents)
 Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Glaucoma. How is Glaucoma Diagnosed? Glaucoma Testing
 Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
T.opically applied corticoids were shown to produce in man an increase in intraocular pressure, a reduction in outflow facility,
 Aqueous outflow facility in monkeys and the effect of topical corticoids Mansour F. Armaly The ocular effects of topically applied dexamethasone 21-phosphate and subconjunctivally administered methylprednisolone
Aqueous outflow facility in monkeys and the effect of topical corticoids Mansour F. Armaly The ocular effects of topically applied dexamethasone 21-phosphate and subconjunctivally administered methylprednisolone
3/16/2018. Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim. Prof. of Ophthalmology Al-Azhar University
 Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation
 Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care
 The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
A LITTLE ANATOMY. three layers of eye: 1. outer: corneosclera. 2. middle - uvea. anterior - iris,ciliary body. posterior - choroid
 GLAUCOMA A LITTLE ANATOMY three layers of eye: 1. outer: corneosclera 2. middle - uvea anterior - iris,ciliary body posterior - choroid connection at the pars plana between post and ant uvea 3. retina
GLAUCOMA A LITTLE ANATOMY three layers of eye: 1. outer: corneosclera 2. middle - uvea anterior - iris,ciliary body posterior - choroid connection at the pars plana between post and ant uvea 3. retina
Diabetic Retinopathy Screening Program in the Cree Region of James Bay of Quebec
 RUIS McGILL VIRTUAL HEALTH AND SOCIAL SERVICES CENTRE (CvSSS) SIMPLIFYING TELEHEALTH! Diabetic Retinopathy Screening Program in the Cree Region of James Bay of Quebec Nurse and Imager Training Prepared
RUIS McGILL VIRTUAL HEALTH AND SOCIAL SERVICES CENTRE (CvSSS) SIMPLIFYING TELEHEALTH! Diabetic Retinopathy Screening Program in the Cree Region of James Bay of Quebec Nurse and Imager Training Prepared
Intraocular Pressure Reconstitution and Maintenance for Cadaveric Porcine Eyes in Simulated Wet-Lab Experience
 Intraocular Pressure Reconstitution and Maintenance for Cadaveric Porcine Eyes in Simulated Wet-Lab Experience Francesca Marie Giliberti, MD Julia Marie Parisi Fullerton, MD Virginia Commonwealth University
Intraocular Pressure Reconstitution and Maintenance for Cadaveric Porcine Eyes in Simulated Wet-Lab Experience Francesca Marie Giliberti, MD Julia Marie Parisi Fullerton, MD Virginia Commonwealth University
Ophthalmology. Glaucoma
 Ophthalmology Glaucoma The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems ranging
Ophthalmology Glaucoma The Ophthalmology service offers the latest and most comprehensive eye care for patients. With a dedicated team of eye surgeons and consultants, we treat vision problems ranging
3/31/2019. Role of IOP. Role of IOP. Role of IOP. Role of IOP. Evaluation of glaucoma has changed Why hasn t treatment?
 Glaucoma Update ROLE FOR RHOPRESSA Gregory D. Searcy, M.D. 1857: German ophthalmologist Albrecht Van Graefe concluded all glaucomatous optic disc excavation is associated with high IOP based on the only
Glaucoma Update ROLE FOR RHOPRESSA Gregory D. Searcy, M.D. 1857: German ophthalmologist Albrecht Van Graefe concluded all glaucomatous optic disc excavation is associated with high IOP based on the only
XUE HUI Department of Histology& Embryology, Basic Medicine College of Jilin University
 SENSE ORGAN XUE HUI Department of Histology& Embryology, Basic Medicine College of Jilin University EYE fibrous globe lens photosensitive cells a system of cells and nerves concentric layers the sclera
SENSE ORGAN XUE HUI Department of Histology& Embryology, Basic Medicine College of Jilin University EYE fibrous globe lens photosensitive cells a system of cells and nerves concentric layers the sclera
Closed Angle Glaucoma Or Narrow Angle Glaucoma. What s is a closed angle type of glaucoma,
 Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Building a Major Ophthalmic Pharmaceutical Company. Aerie Pharmaceuticals, Inc. Company Overview June 2-3, 2015
 Building a Major Ophthalmic Pharmaceutical Company Aerie Pharmaceuticals, Inc. Company Overview June 2-3, 2015 1 Important Information Any discussion of the potential use or expected success of our product
Building a Major Ophthalmic Pharmaceutical Company Aerie Pharmaceuticals, Inc. Company Overview June 2-3, 2015 1 Important Information Any discussion of the potential use or expected success of our product
Chronicity. Narrow Minded. Course Outline. Acute angle closure. Subacute angle closure. Classification of Angle Closure 5/19/2014
 Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Eye Fluids. Dr. Mohamed Saad Daoud
 Eye Fluids 1 Reference Books: Text Book of Medical physiology (Guyton and Hall) Eleventh edition 2 Fluid System of the Eye (Intraocular Fluid) The eye is filled with intraocular fluid, which maintains
Eye Fluids 1 Reference Books: Text Book of Medical physiology (Guyton and Hall) Eleventh edition 2 Fluid System of the Eye (Intraocular Fluid) The eye is filled with intraocular fluid, which maintains
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
N W KNOW. What You Need to Know. What You Know About Glaucoma Could Save Your Sight
 What You Need to Know is the second leading cause of blindness around the world, so it is important to understand its significance and treatment options. While glaucoma is not curable, there are several
What You Need to Know is the second leading cause of blindness around the world, so it is important to understand its significance and treatment options. While glaucoma is not curable, there are several
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
The Pathology and Pathogenesis of Acute Glaucoma in Dogs. Richard R Dubielzig
 The Pathology and Pathogenesis of Acute Glaucoma in Dogs Richard R Dubielzig Overview of Glaucoma Intraocular Pressure too High to Support a Healthy Optic Nerve Terminology used in the classification of
The Pathology and Pathogenesis of Acute Glaucoma in Dogs Richard R Dubielzig Overview of Glaucoma Intraocular Pressure too High to Support a Healthy Optic Nerve Terminology used in the classification of
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma.
 Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Method for comparing visual field defects to local RNFL and RGC damage seen on frequency domain OCT in patients with glaucoma. Donald C. Hood 1,2,* and Ali S. Raza 1 1 Department of Psychology, Columbia
Endocyclophotodestruction in Glaucoma Patients Undergoing Combined Surgery of Pars Plana Vitrectomy and Phacoemulsification
 e-issn 643-370 DOI: 0.269/MSM.89097 Received: 204.04.23 Accepted: 204.0.29 Published: 204.0. Endocyclophotodestruction in Glaucoma Patients Undergoing Combined Surgery of Pars Plana Vitrectomy and Phacoemulsification
e-issn 643-370 DOI: 0.269/MSM.89097 Received: 204.04.23 Accepted: 204.0.29 Published: 204.0. Endocyclophotodestruction in Glaucoma Patients Undergoing Combined Surgery of Pars Plana Vitrectomy and Phacoemulsification
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Uveal Melanoma. Protocol applies to malignant melanoma of the uvea.
 Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Aqueous humor drains from the anterior chamber predominantly
 Influence of Molecular Weight on Intracameral Dextran Movement to the Posterior Segment of the Mouse Eye Antje S. Bernd, Makoto Aihara, James D. Lindsey, and Robert N. Weinreb PURPOSE. Uveoscleral outflow
Influence of Molecular Weight on Intracameral Dextran Movement to the Posterior Segment of the Mouse Eye Antje S. Bernd, Makoto Aihara, James D. Lindsey, and Robert N. Weinreb PURPOSE. Uveoscleral outflow
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015
 Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY
 ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Glaucoma. Glaucoma. Glaucoma. Trevor Arnold, MS, DVM, DACVO
 Glaucoma Trevor Arnold, MS, DVM, DACVO Glaucoma Physiology of Aqueous Humor Produced in the ciliary body Flows out the iridocorneal angle and ciliary cleft High intraocular pressures are caused by a decreased
Glaucoma Trevor Arnold, MS, DVM, DACVO Glaucoma Physiology of Aqueous Humor Produced in the ciliary body Flows out the iridocorneal angle and ciliary cleft High intraocular pressures are caused by a decreased
Micro-Invasive Glaucoma Surgery (Aqueous Stents)
 Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS. Darshana Soma
 LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS Darshana Soma A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, in partial
LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS Darshana Soma A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, in partial
Meet Libby. Corneal Dysgenesis, Degeneration, and Dystrophies Definitions. Dr. Victor Malinovsky
 Meet Libby Corneal Dysgenesis, Degeneration, and Dystrophies 2006 Dr. Victor Malinovsky Definitions Dysgenesis: (congenital anomalies) A development disorder that results in a congenital malformation of
Meet Libby Corneal Dysgenesis, Degeneration, and Dystrophies 2006 Dr. Victor Malinovsky Definitions Dysgenesis: (congenital anomalies) A development disorder that results in a congenital malformation of
Evolution of the Definition of Primary Open-Angle Glaucoma
 OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
Ocular hypertension is present in approximately 8%
 ORIGINAL STUDY The Probability of Glaucoma From Ocular Hypertension Determined by Ophthalmologists in Comparison to a Risk Calculator Steven L. Mansberger, MD, MPH and George A. Cioffi, MD Objective: To
ORIGINAL STUDY The Probability of Glaucoma From Ocular Hypertension Determined by Ophthalmologists in Comparison to a Risk Calculator Steven L. Mansberger, MD, MPH and George A. Cioffi, MD Objective: To
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Frequently Asked Questions about General Ophthalmology:
 1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
1. Normal Eye Structure The eye is a slightly asymmetrical globe, about an inch in diameter. The parts of the eye include: Cornea (a clear dome over the iris), Iris (the pigmented part); Pupil (the black
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
OPHTHALMOLOGY AND ULTRASOUND
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk OPHTHALMOLOGY AND ULTRASOUND Author : JAMES OLIVER Categories : Vets Date : April 28, 2008 JAMES OLIVER discusses why ultrasound
Vet Times The website for the veterinary profession https://www.vettimes.co.uk OPHTHALMOLOGY AND ULTRASOUND Author : JAMES OLIVER Categories : Vets Date : April 28, 2008 JAMES OLIVER discusses why ultrasound
Glaucoma Intraocular Pressure What Will I Notice?
 Glaucoma Glaucoma is the name given to a group of eye conditions in which the optic nerve at the back of the eye is slowly damaged. The diagnosis of glaucoma is made when your optometrist or ophthalmologist
Glaucoma Glaucoma is the name given to a group of eye conditions in which the optic nerve at the back of the eye is slowly damaged. The diagnosis of glaucoma is made when your optometrist or ophthalmologist
Vanderbilt Eye Institute Clinical Trials
 April, 2010 Vanderbilt Eye Institute Clinical Trials Ophthalmology Actively Recruiting Studies For information on our clinical trials and other studies, please contact: Sandy Owings, COA, CCRP Clinic Director
April, 2010 Vanderbilt Eye Institute Clinical Trials Ophthalmology Actively Recruiting Studies For information on our clinical trials and other studies, please contact: Sandy Owings, COA, CCRP Clinic Director
