Management of non-arteritic anterior ischemic optic neuropathy
|
|
|
- Virginia Bryan
- 5 years ago
- Views:
Transcription
1 Graefes Arch Clin Exp Ophthalmol (2009) 247: DOI /s EDITORIAL Management of non-arteritic anterior ischemic optic neuropathy Sohan Singh Hayreh Received: 5 August 2009 / Accepted: 20 August 2009 / Published online: 30 September 2009 # Springer-Verlag 2009 Introduction Non-arteritic anterior ischemic optic neuropathy (NA-AION) is one of the major causes of seriously impaired vision among the middle-aged and elderly population; in addition, contrary to popular belief, it also occurs in young persons, though less commonly. In spite of it being a common disease, almost all publications on NA-AION contain the following two statements: (1) Pathogenesis of NA-AION is unknown. and (2) There is no known treatment for NA-AION.. Given the current state of our knowledge on NA-AION, neither statement is correct, as will be evident from the following short discussion. (Both pathogenesis and management of NA- AION are discussed at length elsewhere [1, 2]). Management of NA-AION has been highly controversial. Various treatments for NA-AION have been advocated from time to time, but were found to be useless and even, in some cases, harmful. To evaluate the validity of any treatment, there are two essential considerations: (1) it must have a scientific rationale; any treatment without that, irrespective of how aggressively it is advocated and how attractive it may seem, is not going to work in the long run, as was demonstrated by optic nerve sheath decompression in NA-AION, and (2) treatment of a disease must arise from full understanding of its pathogenesis. S. S. Hayreh Department of Ophthalmology and Visual Sciences, College of Medicine, University of Iowa, Iowa City, IA, USA S. S. Hayreh (*) Department of Ophthalmology and Visual Sciences, University Hospitals & Clinics, 200 Hawkins Drive, Iowa City, IA , USA sohan-hayreh@uiowa.edu Pathogenesis of NA-AION Etiologically and pathogenetically, NA-AION is of two types. One, by far the most common, is caused by transient nonperfusion or hypoperfusion of the optic nerve head (ONH) circulation; the second, and rarer type is due to embolic lesions of the arteries/arterioles feeding the ONH. The pathogenesis of NA-AION is discussed at length elsewhere [1, 2]. Briefly, all the available evidence indicates that NA-AION is multifactorial in nature. The risk factors fall into two main categories: 1. Predisposing risk factors: these may be systemic or local in the eye and/or ONH. They make the ONH susceptible to ischemic disorders, but do not necessarily produce NA-AION by themselves. (a). Systemic risk factors: NA-AION patients, compared to the general population, have a significantly higher prevalence of arterial hypertension, nocturnal arterial hypotension, diabetes mellitus, ischemic heart disease and other cardiovascular disorders, hyperlipidemia, atherosclerosis and arteriosclerosis [1, 3 7]. Other associated systemic diseases have also been reported, including sleep apnea [1, 8 10], arterial hypotension due to a variety of causes [11] and malignant arterial hypertension [12], and migraine. (b). Ocular and ONH risk factors: NA-AION is significantly associated with absent or small cup in the optic disc [13, 14], location of the watershed zone of the posterior ciliary arteries in relation to the optic disc [15], and vascular disorders in the nutrient vessels of the ONH [16], optic disc drusen and cataract extraction [17]. Other risk factors include markedly raised intraocular pressure [17], and marked optic disc edema due to any cause
2 1596 Graefes Arch Clin Exp Ophthalmol (2009) 247: [18]. Contrary to the prevalent impression, an absent or small cup is simply a secondary contributing factor, once the process of NA-AION has started, and NOT a primary factor [13, 14, 19]. 2. Precipitating risk factor(s): in a person with predisposing risk factors already present, these risk factors act as the final insult ( last straw ), resulting in ischemia of the ONH and NA-AION. Studies have shown that patients with NA-AION typically complain of discovering visual loss on waking in the morning. In one study, 73% NA- AION patients gave a definite history of discovering the visual loss on waking up in the morning or from a nap, or one the first opportunity in the day to use vision critically [20]. The incidence may actually be much higher than 73%, because many patients were not certain about the time of the day when they discovered the visual loss. Therefore, nocturnal arterial hypotension is the most important factor in this category [20 22]; its role is discussed at length elsewhere [1, 2]. Studies have also shown that arterial hypertensives on oral hypotensive therapy have a significant (p=0.004) association between progressive visual field deterioration in NA-AION and nocturnal hypotension [21, 22]. Serious confounding factors in determining risk factors for NA-AION 1. One of the arguments often put forward by those who believe the pathogenesis of NA-AION is not known is that some patients with NA-AION are perfectly healthy and have no known risk factors. Inability to find a risk factor may be due to several reasons. For example, a totally asymptomatic person, who looks perfectly healthy and feels fine, whose routine physical evaluation does not reveal any systemic, ocular or ONH abnormality may still have risk factors. I have recently found out that fact from an unpleasant personal experience. Recently I had a Holter monitor to record electrocardiogram for a minor reason when I was totally asymptomatic, feeling fine and working perfectly normally. The monitor showed that during the night I was having frequent, recurrent and prolonged periods of complete asystole (with a flat electrocardiogram), some lasting as long as 10 seconds; occasionally the asystoles also occurred during the day. That required urgent pacemaker implantation to prevent me from going into cardiac arrest. The monitoring was done essentially because I am a physician and the cardiologist is my colleague and friend; it would have never been done normally. This clearly shows the fallacy in assuming that a perfectly healthy-looking person does not have any risk factors. 2. In 24-hour ambulatory BP recording in about 800 patients, I often found patients whose blood pressure was ideal during the waking hours, but dropped to very low levels during sleep. Thus, normal blood pressure during the waking hours is no guide to the blood pressure during sleep. 3. Derangement of autoregulation of the ONH blood flow is suspected to play an important role in various types of circulatory disorders of the ONH. Unfortunately, we have no means of evaluating that so far. Thus, the axiom should be that if one does not find any evident risk factor, that does not necessarily mean that person actually has no risk factor. Clearly, a whole host of systemic and local factors, acting in different combinations and to different extents may derange the ONH circulation, with some making the ONH susceptible to ischemia and others acting as the final insult. Nocturnal hypotension seems to be an important precipitating factor in the susceptible patient. Contrary to common misconception, NA-AION is not a thromboembolic disorder in the vast majority of cases. Thus, the pathogenesis of NA-AION is complex but not, as often stated, unknown. Management of NA-AION The main treatments which have been advocated for NA-AION over the recent years are: Optic nerve sheath decompression Sergott et al. [23] in 1989 claimed that optic nerve sheath decompression improved visual function in progressive NA-AION. The procedure gained world-wide favor not only in progressive but also in all types of NA-AION, in spite of the fact that it was pointed out [24] that this procedure had no scientific rationale and may be harmful. A multicenter clinical trial conducted by the United States National Institutes of Health subsequently established that this procedure is not effective and not an appropriate treatment for non-arteritic AION and may be harmful, because 24% of the eyes with optic nerve sheath decompression suffered further visual loss, as compared to only 12% simply left alone [25]. This and another study [26] showed that 41% 43% of cases showed spontaneous visual acuity improvement, without any procedure. Aspirin This has been advocated with the mistaken impression that NA-AION, like stroke, is a thromboembolic disorder which has not been supported by the available studies. For example, two large studies have revealed no long-term benefit from aspirin in reducing the risk of NA- AION in the fellow eye [27, 28], because aspirin has no effect on nocturnal arterial hypotension.
3 Graefes Arch Clin Exp Ophthalmol (2009) 247: Levodopa Johnson et al. [29, 30], in a retrospective study of patients with NA-AION, concluded that levodopa appears to be beneficial in the treatment of recent-onset NAION [30]. However, this conclusion was not valid, as discussed in detail elsewhere [31, 32]. First, there is no scientific rationale for the use of levodopa in NA-AION, and second, there were serious statistical problems with their data analysis, because the results of this study were not interpretable in view of the potential confounding and biases that were apparently present. Systemic corticosteroid therapy A recent large, prospective study [33], based on 696 eyes, comparing the visual outcome in treated (364 eyes) versus untreated control (332 eyes) groups, with identical baseline parameters in the two groups, concluded that NA-AION eyes treated during the acute phase with systemic corticosteroids had a significantly higher probability of improvement in visual acuity and visual field than did the untreated group. In eyes with initial visual acuity of 20/70 or worse, seen within 2 weeks of onset, there was visual acuity improvement in 70% in the treated group compared to 41% in the untreated group (odds ratio of improvement: 3.39; 95% CI:1.62, 7.11; p=0.001). Similarly, among those seen within 2 weeks of NA-AION onset with moderate to severe initial visual field defect, there was improvement in 40% of the treated group and 25% of the untreated group (odds ratio: 2.06, 95% CI: 1.24, 3.40; p=0.005). A comparison of treated versus untreated groups also showed that optic disc edema resolved significantly (p=0.0006) faster in the treated group [34]. Use of intravitreal triamcinolone acetonide There have recently been two contradictory small studies on this topic. Jonas et al. [35], in three patients, found that it had no beneficial effect on visual acuity. Kaderli et al. [36], in four eyes, reported visual acuity improvement, but without any improvement in visual fields; however, that study had some notable flaws [37]. Briefly, these include: (a) their study was based on only four eyes, (b) two large natural history studies have shown spontaneous visual acuity improvement in 41% 43% of eyes with NA-AION [25, 26], and (c) more importantly, none of the eyes in the study by Kaderli et al. [36] showed improvement in visual fields and all had altitudinal visual field defects. Studies have shown that in NA-AION and arteritic AION apparent visual acuity improvement without visual field improvement is due to the patient learning to fixate eccentrically, rather than being a genuine visual improvement [26, 38]. In the study by Kaderli et al. [36], eccentric fixation may explain why the visual acuity of the patients apparently improved, while the visual fields did not. Use of intravitreal bevacizumab A case report by Bennett et al. in 2007 [39] claimed visual improvement after an intravitreal injection of bevacizumab (Avastin) 3 weeks after the onset of NA-AION in one eye. The authors claim that bevacizumab a vascular endothelial growth factor (VEGF) inhibitory drug improved visual acuity in the eye by reducing optic disc edema. But it is impossible to judge the effectiveness of a mode of treatment from one eye when 41% 43% of NA-AION eyes show spontaneous visual acuity improvement. In contrast, recently there have been two reports where intravitreal bevacizumab injection actually resulted in the development of NA-AION. Hosseini and Razeghinejad [40] reported a 72-year-old woman who woke up with visual loss 1 week after intravitreal injection of bevacizumab, and was diagnosed to have NA-AION. In this issue of the Journal, Ganssauge et al. [41] report a 51-year-old male who recognized visual field defects 2 weeks after injection with intravitreal of bevacizumab for choroidal neovascularisation, and was diagnosed as having NA-AION. In these two cases, it could be argued that because there was a time lag of 1 week and 2 weeks respectively between the intravitreal injection of bevacizumab and the development of NA-AION, the latter could not be attributed to the former. Since the patient of Ganssauge et al. [41] recognized the visual field defect, the possibility that it was there before and he was unaware cannot be ruled out. I have seen that in some patients with NA-AION. The patient of Hosseini and Razeghinejad [40] woke up with visual loss 1 week after the injection. There is an explanation for the delay between the intravitreal injection and development of visual loss due to NA-AION. In 1981 [42], I reported that asymptomatic optic disc edema is an early sign of NA- AION. More recently, we described the clinical entity of Incipient nonarteritic anterior ischemic optic neuropathy in 55 eyes [19], in which, again, NA-AION patients were seen initially with asymptomatic optic disc edema, and 25% of them later on progressed to classical NAION with median time of progression of 5.8 (interquartile ) weeks from the initial diagnosis.. Thus, contrary to the universal impression, the time of visual loss is not always the time of onset of NA-AION it is only the time when the patient notices it. In these two cases [40, 41], the intravitreal injection most probably started the chain of events. It initially produced Incipient nonarteritic anterior ischemic optic neuropathy ; however, the patients were seen by the ophthalmologist only when they developed and noticed visual loss 1 2 weeks later. The whole subject of intravitreal injection of bevacizumab requires detailed discussion because of the current enthusiasm for the use of anti-vegf drugs in all sorts of disorders in ophthalmology. Naturally the question arises: what is the mechanism of development of NA-AION following intravitreal injection of bevacizumab? The ONH circulation depends upon the perfusion pressure (Perfusion pressure =
4 1598 Graefes Arch Clin Exp Ophthalmol (2009) 247: mean blood pressure minus intraocular pressure) in its capillaries. Following intravitreal injection of anti-vegf drugs, two types of rise of intraocular pressure (IOP) have been reported. 1. Short-term rise of IOP Intravitreal injection increases the volume in the eyeball, thereby resulting in a transient rise of IOP in all eyes. After intravitreal injection of bevacizumab, Kim et al. [43] reported a rise of IOP to 44 mmhg (range, 4 87 mmhg.), Falkenstein et al. [44] a mean IOP of 36. mmhg,, and Hollands et al. [45] an IOP of 25 mmhg or higher at 30 minutes, and one patient required a 1-week course of glaucoma medication to control the IOP. Semoun et al. [46] reported a case of an acute angle-closure glaucoma that occurred immediately after an intravitreal injection of 0.05 ml of bevacizumab. 2. Severe and sustained ocular hypertension Bakri et al. [47] reported sustained ocular hypertension as high as 30, 34, 46, and 50 mmhg in the four patients following 0.5 mg intravitreal ranibizumab for age-related macular degeneration. The elevated IOP persisted across several visits, requiring control with topical glaucoma therapy, and in two cases the addition of a systemic carbonic anhydrase inhibitor. None of the patients had a previous history of glaucoma. Kahook et al. [48] reported six cases of significant and sustained elevation of lop after intravitreal injections of bevacizumab for agerelated macular degeneration, all requiring IOP-Iowering therapy. At the annual meeting of the ARVO in May 2009, there was another report (I do not remember the names of the authors) of four cases with similar persistent elevation of IOP following intravitreal injection of bevacizumab. Jalil et al. [49] reported a case that was found to have an IOP of 56 mmhg 3 days after intravitreal injection of bevacizumab. Similarly, there are many reports showing a substantial rise in IOP a few days or weeks after intravitreal triamcinolone; by contrast, oral steroid therapy for NA-AION did not have that effect on IOP during a short-term treatment [33]. While sustained IOP rise has been recorded by these reports, we do not have information about how common it is after intravitreal ranibizumab, because the usual practice is to monitor IOP only immediately post-injection and not later on. It is possible that it may be more prevalent than reported in the literature. In NA-AION, the ONH already has precarious circulation. Under those circumstances, even a transient high IOP, let alone a prolonged sustained high IOP, has the potential to further compromise the circulation and result in further ONH damage and visual loss. In patients who do not already have NA-AION, the chance of developing NA-AION with this transient or sustained high IOP is limited to those who are susceptible because of the predisposing risk factors discussed above. When treating age-related macular degeneration in those cases, on a risk/benefit ratio, it may be prudent to avoid any immediate or prolonged rise of IOP by taking precautionary measures. For persons who have already had NA-AION in one eye, the risk of the second eye developing NA-AION is much higher than for those who never had NA- AION before. Thus, a high IOP can precipitate development of NA-AION in persons with predisposing risk factors, and can worsen the visual outcome in those with NA-AION. In view of that, intravitreal injections of anti-vegf agents or of triamcinolone have the potential to be harmful in the management of NA-AION a factor not realized in the current enthusiasm for widespread use of anti-vegf agents, particularly a proposed treatment for NA-AION. Moreover, anti-vegf agents on rare occasions have other ocular complications as well as systemic side-effects, e.g., acute elevation of systemic blood pressure, cerebrovascular accidents, myocardial infarctions, and even deaths have been reported in some cases [50]. Conclusion 1. The pathogenesis of NA-AION is highly complex but not unknown. 2. A recent large prospective study has shown that systemic corticosteroid therapy, given according to the regimen described in the original study, results in a significantly higher probability of improvement in visual acuity (p=0.001) and visual field (p=0.005) compared to the untreated group. Therefore, we do now have an effective treatment for NA-AION. 3. Anti-VEGF therapy in treatment of NA-AION has the potential to be harmful. Acknowledgement I am grateful to Ms. Patrician Duffel, our librarian, for her expert help with the bibliography. My wife Shelagh was helpful in the preparation of this manuscript. Conflict of interest References The author has no conflict of interest. 1. Hayreh SS (1996) Acute ischemic disorders of the optic nerve: pathogenesis, clinical manifestations, and management. Ophthalmol Clin North Am 9: Hayreh SS (2009) Ischemic optic neuropathy. Prog Retin Eye Res 28: Repka MX, Savino PJ, Schatz NJ, Sergott RC (1983) Clinical profile and long-term implications of anterior ischemic optic neuropathy. Am J Ophthalmol 96: Guyer DR, Miller NR, Auer CL, Fine SL (1985) The risk of cerebrovascular and cardiovascular disease in patients with anterior ischemic optic neuropathy. Arch Ophthalmol 103: Hayreh SS, Joos KM, Podhajsky PA, Long CR (1994) Systemic diseases associated with nonarteritic anterior ischemic optic neuropathy. Am J Ophthalmol 118:
5 Graefes Arch Clin Exp Ophthalmol (2009) 247: Jacobson DM, Vierkant RA, Belongia EA (1997) Nonarteritic anterior ischemic optic neuropathy. A case-control study of potential risk factors. Arch Ophthalmol 115: Hayreh SS, Zimmerman MB (2008) Nonarteritic anterior ischemic optic neuropathy: clinical characteristics in diabetic patients versus nondiabetic patients. Ophthalmology 115: Mojon DS, Hedges TR 3rd, Ehrenberg B, Karam EZ, Goldblum D, Abou-Chebl A, Gugger M, Mathis J (2002) Association between sleep apnea syndrome and nonarteritic anterior ischemic optic neuropathy. Arch Ophthalmol 120: Palombi K, Renard E, Levy P, Chiquet C, Deschaux C, Romanet JP, Pépin JL (2006) Non-arteritic anterior ischaemic optic neuropathy is nearly systematically associated with obstructive sleep apnoea. Br J Ophthalmol 90: Li J, McGwin G Jr, Vaphiades MS, Owsley C (2007) Non-arteritic anterior ischaemic optic neuropathy and presumed sleep apnoea syndrome screened by the Sleep Apnea scale of the Sleep Disorders Questionnaire (SA-SDQ). Br J Ophthalmol 91: Hayreh SS (1987) Anterior ischemic optic neuropathy. VIII. Clinical features and pathogenesis of post-hemorrhagic amaurosis. Ophthalmology 94: Hayreh SS, Servais GE, Virdi PS (1986) Fundus lesions in malignant hypertension. V. Hypertensive optic neuropathy. Ophthalmology 93: Beck RW, Servais GE, Hayreh SS (1987) Anterior ischemic optic neuropathy. IX. Cup-to-disc ratio and its role in pathogenesis. Ophthalmology 94: Hayreh SS, Zimmerman MB (2008) Nonarteritic anterior ischemic optic neuropathy: refractive error and its relationship to cup/disc ratio. Ophthalmology 115: Hayreh SS (1990) In vivo choroidal circulation and its watershed zones. Eye 4: Hayreh SS (1995) The 1994 Von Sallman Lecture. The optic nerve head circulation in health and disease. Exp Eye Res 61: Hayreh SS (1980) Anterior ischemic optic neuropathy. IV. Occurrence after cataract extraction. Arch Ophthalmol 98: Hayreh SS (1977) Optic disc edema in raised intracranial pressure. VI. Associated visual disturbances and their pathogenesis. Arch Ophthalmol 95: Hayreh SS, Zimmerman MB (2007) Incipient nonarteritic anterior ischemic optic neuropathy. Ophthalmology 114: Hayreh SS, Podhajsky PA, Zimmerman B (1997) Nonarteritic anterior ischemic optic neuropathy: time of onset of visual loss. Am J Ophthalmol 124: Hayreh SS, Zimmerman MB, Podhajsky P, Alward WL (1994) Nocturnal arterial hypotension and its role in optic nerve head and ocular ischemic disorders. Am J Ophthalmol 117: Hayreh SS, Podhajsky P, Zimmerman MB (1999) Role of nocturnal arterial hypotension in optic nerve head ischemic disorders. Ophthalmologica 213: Sergott RC, Cohen MS, Bosley TM, Savino PJ (1989) Optic nerve decompression may improve the progressive form of nonarteritic ischemic optic neuropathy. Arch Ophthalmol 107: Hayreh SS (1990) The role of optic nerve sheath fenestration in management of anterior ischemic optic neuropathy. Arch Ophthalmol 108: The Ischemic Optic Neuropathy Decompression Trial Research Group (1995) Optic nerve decompression surgery for nonarteritic anterior ischemic optic neuropathy (NAION) is not effective and may be harmful. JAMA 273: Hayreh SS, Zimmerman MB (2008) Nonarteritic anterior ischemic optic neuropathy: natural history of visual outcome. Ophthalmology 115: Beck RW, Hayreh SS, Podhajsky PA, Tan ES, Moke PS (1997) Aspirin therapy in nonarteritic anterior ischemic optic neuropathy. Am J Ophthalmol 123: Newman NJ, Scherer R, Langenberg P, Kelman S, Feldon S, Kaufman D, Dickersin K, Ischemic Optic Neuropathy Decompression Trial Research Group (2002) The fellow eye in NAION: report from the ischemic optic neuropathy decompression trial follow-up study. Am J Ophthalmol 134: Johnson LN, Gould TJ, Krohel GB (1996) Effect of levodopa and carbidopa on recovery of visual function in patients with nonarteritic anterior ischemic optic neuropathy of longer than six months duration. Am J Ophthalmol 121: Johnson LN, Guy ME, Krohel GB, Madsen RW (2000) Levodopa may improve vision loss in recent-onset, nonarteritic anterior ischemic optic neuropathy. Ophthalmology 107: Beck RW (2000) Does Levodopa improve visual function in NAION? Ophthalmology 107: Hayreh SS (2000) Does Levodopa improve visual function in NAION? Ophthalmology 107: Hayreh SS, Zimmerman MB (2008) Non-arteritic anterior ischemic optic neuropathy: role of systemic corticosteroid therapy. Graefes Arch Clin Exp Ophthalmol 246: Hayreh SS, Zimmerman MB (2007) Optic disc edema in nonarteritic anterior ischemic optic neuropathy. Graefes Arch Clin Exp Ophthalmol 245: Jonas JB, Spandau UH, Harder B, Sauder G (2007) Intravitreal triamcinolone acetonide for treatment of acute nonarteritic anterior ischemic optic neuropathy. Graefes Arch Clin Exp Ophthalmol 245: Kaderli B, Avci R, Yucel A, Guler K, Gelisken O (2007) Intravitreal triamcinolone improves recovery of visual acuity in nonarteritic anterior ischemic optic neuropathy. J Neuroophthalmol 27: Hayreh SS (2008) Intravitreal triamcinolone for nonarteritic anterior ischemic optic neuropathy. J Neuroophthalmol 28: Hayreh SS, Zimmerman B, Kardon RH (2002) Visual improvement with corticosteroid therapy in giant cell arteritis. Report of a large study and review of literature. Acta Ophthalmol Scand 80: Bennett JL, Thomas S, Olson JL, Mandava N (2007) Treatment of nonarteritic anterior ischemic optic neuropathy with intravitreal bevacizumab. J Neuroophthalmol 27: Hosseini H, Razeghinejad MR (2009) Anterior ischemic optic neuropathy after intravitreal injection of bevacizumab. J Neuroophthalmol 29: Ganssauge M, Wilhelm H, Bartz-Schmidt K-U, Aisenbrey S (2009) Non-arteritic anterior ischemic optic neuropathy (NA-AION) after intravitreal injection of bevacizumab (Avastin ) for treatment of angioid streaks in pseudoxanthoma elasticum. Graefes Arch Clin Exp Ophthalmol [in press] 42. Hayreh SS (1981) Anterior ischemic optic neuropathy. V. Optic disc edema an early sign. Arch Ophthalmol 99: Kim JE, Mantravadi AV, Hur EY, Covert DJ (2008) Short-term intraocular pressure changes immediately after intravitreal injections of anti-vascular endothelial growth factor agents. Am J Ophthalmol 146: Falkenstein IA, Cheng L, Freeman WR (2007) Changes of intraocular pressure after intravitreal injection of bevacizumab (avastin). Retina 27: Hollands H, Wong J, Bruen R, Campbell RJ, Sharma S, Gale J (2007) Short-term intraocular pressure changes after intravitreal injection of bevacizumab. Can J Ophthalmol 42: Semoun O, Blumen-Ohana E, de Preobrajensky N, Nordmann JP (2009) Glaucome aigu par fermeture de l angle compliquant une injection intravitréenne de bevacizumab. [Acute angle-closure
6 1600 Graefes Arch Clin Exp Ophthalmol (2009) 247: glaucoma complicating an intravitreal injection of bevacizumab]. J Fr Ophtalmol 32: Bakri SJ, McCannel CA, Edwards AO, Moshfeghi DM (2008) Persisent ocular hypertension following intravitreal ranibizumab. Graefes Arch Clin Exp Ophthalmol 246: Kahook MY, Kimura AE, Wong LJ, Ammar DA, Maycotte MA, Mandava N (2009) Sustained elevation in intraocular pressure associated with intravitreal bevacizumab injections. Ophthalmic Surg Lasers Imaging 40: Jalil A, Fenerty C, Charles S (2007) Intravitreal bevacizumab (Avastin) causing acute glaucoma: an unreported complication. Eye 21: Wu L, Martinez-Castellanos MA, Quiroz-Mercado H, Arevalo JF, Berrocal MH, Farah ME, Maia M, Roca JA, Rodriguez FJ, Pan- American Collaborative Retina Study Group (PACORES) (2008) Twelve-month safety of intravitreal injections of bevacizumab (Avastin): results of the Pan-American Collaborative Retina Study Group (PACORES). Graefes Arch Clin Exp Ophthalmol 246:81 87
Neuropathy (NAION) and Avastin. Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013
 Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Frequency of sustained IOP elevation in patients receiving intravitreal injections of anti-vegf agents for exudative age-related macular degeneration
 Frequency of sustained IOP elevation in patients receiving intravitreal injections of anti-vegf agents for exudative age-related Aim Frequency of sustained IOP elevation in patients receiving intravitreal
Frequency of sustained IOP elevation in patients receiving intravitreal injections of anti-vegf agents for exudative age-related Aim Frequency of sustained IOP elevation in patients receiving intravitreal
NIH Public Access Author Manuscript J Neuroophthalmol. Author manuscript; available in PMC 2010 December 1.
 NIH Public Access Author Manuscript Published in final edited form as: J Neuroophthalmol. 2010 June ; 30(2): 193 198. doi:10.1097/wno.0b013e3181e1f71f. Should steroids be offered to patients with nonarteritic
NIH Public Access Author Manuscript Published in final edited form as: J Neuroophthalmol. 2010 June ; 30(2): 193 198. doi:10.1097/wno.0b013e3181e1f71f. Should steroids be offered to patients with nonarteritic
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Obstructive sleep apnea syndrome and non-arteritic anterior ischemic optic neuropathy: a case control study
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Obstructive sleep apnea syndrome and non-arteritic anterior ischemic optic neuropathy: a case
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Obstructive sleep apnea syndrome and non-arteritic anterior ischemic optic neuropathy: a case
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD
 Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Visual outcome of mega-dose intravenous corticosteroid treatment in non-arteritic anterior ischemic optic neuropathy retrospective analysis
 Kinori et al. BMC Ophthalmology 2014, 14:62 RESEARCH ARTICLE Open Access Visual outcome of mega-dose intravenous corticosteroid treatment in non-arteritic anterior ischemic optic neuropathy retrospective
Kinori et al. BMC Ophthalmology 2014, 14:62 RESEARCH ARTICLE Open Access Visual outcome of mega-dose intravenous corticosteroid treatment in non-arteritic anterior ischemic optic neuropathy retrospective
Vascular Disease Ocular Manifestations of Systemic Hypertension
 Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus
 The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
The Prevalence of diabetic optic neuropathy in type 2 diabetes mellitus Received: 25/4/2016 Accepted: 8/12/2016 Introduction Diabetic papillopathy is an atypical form of non-arteritic anterior ischemic
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Association of Retinal Vessel Caliber to Optic Disc and Cup Diameters. Kristine E. Lee, Barbara Eden Kobrin Klein, Ronald Klein, and Stacy M.
 Association of Retinal Vessel Caliber to Optic Disc and Cup Diameters Kristine E. Lee, Barbara Eden Kobrin Klein, Ronald Klein, and Stacy M. Meuer PURPOSE. To investigate whether optic disc size is related
Association of Retinal Vessel Caliber to Optic Disc and Cup Diameters Kristine E. Lee, Barbara Eden Kobrin Klein, Ronald Klein, and Stacy M. Meuer PURPOSE. To investigate whether optic disc size is related
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
In the treatment of neovascular and. Original Research
 Original Research Hellenic J Cardiol 2013; 54: 435-440 Influence of Intravitreal Injection of Bevacizumab on Systemic Blood Pressure Changes in Patients with Exudative Form of Age-Related Macular Degeneration
Original Research Hellenic J Cardiol 2013; 54: 435-440 Influence of Intravitreal Injection of Bevacizumab on Systemic Blood Pressure Changes in Patients with Exudative Form of Age-Related Macular Degeneration
Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization
 Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Original Article Ocular Complications after Intravitreal Bevacizumab Injection in Eyes with Choroidal and Retinal Neovascularization Aimal Khan, P.S Mahar, Azfar Nafees Hanfi, Umair Qidwai Pak J Ophthalmol
Anterior Ischemic Optic Neuropathy in Patients Younger than 50 Years PISIT PREECHAWAT, BEAU B. BRUCE, NANCY J. NEWMAN, AND VALÉRIE BIOUSSE
 Anterior Ischemic Optic Neuropathy in Patients Younger than 50 Years PISIT PREECHAWAT, BEAU B. BRUCE, NANCY J. NEWMAN, AND VALÉRIE BIOUSSE PURPOSE: To characterize anterior ischemic optic neuropathy (AION)
Anterior Ischemic Optic Neuropathy in Patients Younger than 50 Years PISIT PREECHAWAT, BEAU B. BRUCE, NANCY J. NEWMAN, AND VALÉRIE BIOUSSE PURPOSE: To characterize anterior ischemic optic neuropathy (AION)
Effect of Prophylactic Intraocular Pressure Lowering Medication on Intraocular Pressure Spikes After Intravitreal Injections
 CLINICAL SCIENCES Effect of Prophylactic Intraocular Pressure Lowering Medication on Intraocular Pressure Spikes After Intravitreal s Max P. C. Frenkel; Shamim A. Haji, MD; Ronald E. P. Frenkel, MD Objective:
CLINICAL SCIENCES Effect of Prophylactic Intraocular Pressure Lowering Medication on Intraocular Pressure Spikes After Intravitreal s Max P. C. Frenkel; Shamim A. Haji, MD; Ronald E. P. Frenkel, MD Objective:
Is NTG different from POAG?
 Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Case Report A Case of Recurrent Transient Monocular Visual Loss after Receiving Sildenafil
 Case Reports in Ophthalmological Medicine Volume 2011, Article ID 645089, 4 pages doi:10.1155/2011/645089 Case Report A Case of Recurrent Transient Monocular Visual Loss after Receiving Sildenafil Asaad
Case Reports in Ophthalmological Medicine Volume 2011, Article ID 645089, 4 pages doi:10.1155/2011/645089 Case Report A Case of Recurrent Transient Monocular Visual Loss after Receiving Sildenafil Asaad
CLINICAL SCIENCES. Use of Best and Final Visual Acuity Outcomes in Ophthalmological Research
 CLINICAL SCIENCES Use of and Visual Acuity Outcomes in Ophthalmological Research David A. DiLoreto, Jr, MD, PhD; Neil M. Bressler, MD; Susan B. Bressler, MD; Andrew P. Schachat, MD Objective: To evaluate
CLINICAL SCIENCES Use of and Visual Acuity Outcomes in Ophthalmological Research David A. DiLoreto, Jr, MD, PhD; Neil M. Bressler, MD; Susan B. Bressler, MD; Andrew P. Schachat, MD Objective: To evaluate
Ischaemic optic neuropathy: the Singapore scene
 O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic Anterior Ischemic Optic Neuropathy and Optic Neuritis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):289-294 http://dx.doi.org/10.3341/kjo.2016.30.4.289 Original Article Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):289-294 http://dx.doi.org/10.3341/kjo.2016.30.4.289 Original Article Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic
Anterior Ischemic Optic Neuropathy (AION)
 Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
COLOUR DOPPLER IMAGING IN GIANT CELL (TEMPORAL) ARTERITIS: SERIAL EXAMINATION AND COMPARISON WITH NON-ARTERITIC ANTERIOR ISCHAEMIC OPTIC NEUROPATHY
 COLOUR DOPPLER IMAGING IN GIANT CELL (TEMPORAL) ARTERITIS: SERIAL EXAMINATION AND COMPARISON WITH NON-ARTERITIC ANTERIOR ISCHAEMIC OPTIC NEUROPATHY F. D. GHANCHI1, T. H. WILLIAMSON\ c. S. LIM2, Z. BUTT2,
COLOUR DOPPLER IMAGING IN GIANT CELL (TEMPORAL) ARTERITIS: SERIAL EXAMINATION AND COMPARISON WITH NON-ARTERITIC ANTERIOR ISCHAEMIC OPTIC NEUROPATHY F. D. GHANCHI1, T. H. WILLIAMSON\ c. S. LIM2, Z. BUTT2,
Delayed Choroidal Perfusion in Giant Cell Arteritis
 Tournai of Clinical Neuro-ophthalmology 11(4): 221-227,1991. 1991 Raven Press, Ltd., New York Delayed Choroidal Perfusion in Giant Cell Arteritis H. G. Mack, B. Me SC., M.B.B.S., J. O'Day, F.R.A.C.P.,
Tournai of Clinical Neuro-ophthalmology 11(4): 221-227,1991. 1991 Raven Press, Ltd., New York Delayed Choroidal Perfusion in Giant Cell Arteritis H. G. Mack, B. Me SC., M.B.B.S., J. O'Day, F.R.A.C.P.,
Retinal Complications of Obstructive Sleep Apnea A Growing Concern!
 Retinal Complications of Obstructive Sleep Apnea A Growing Concern! Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl
Retinal Complications of Obstructive Sleep Apnea A Growing Concern! Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England. Retinal Vein Occlusion (RVO) with Macular oedema (MO)
 Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Ischemic optic neuropathies are the most common acute. Ischemic Optic Neuropathies REVIEW ARTICLE
 REVIEW ARTICLE Ischemic Optic Neuropathies Katie Luneau, MD,* Nancy J. Newman, MD,* and Valérie Biousse, MD* Abstract: Anterior ischemic optic neuropathy (AION) is the most common cause of acute optic
REVIEW ARTICLE Ischemic Optic Neuropathies Katie Luneau, MD,* Nancy J. Newman, MD,* and Valérie Biousse, MD* Abstract: Anterior ischemic optic neuropathy (AION) is the most common cause of acute optic
Christopher Kin Ming Orr, M.D. Clinical Assistant Instructor, College of Medicine SUNY Downstate Medical Center
 Christopher Kin Ming Orr, M.D. Clinical Assistant Instructor, College of Medicine SUNY Downstate Medical Center Presentation 52 y/o Caucasian woman presents with painless decreased vision in left eye x
Christopher Kin Ming Orr, M.D. Clinical Assistant Instructor, College of Medicine SUNY Downstate Medical Center Presentation 52 y/o Caucasian woman presents with painless decreased vision in left eye x
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Disorders of the optic nerve represent a relatively common
 The new england journal of medicine Review Article Edward W. Campion, M.D., Editor Ischemic Optic Neuropathies Valérie Biousse, M.D., and Nancy J. Newman, M.D. From the Departments of Ophthalmology (V.B.,
The new england journal of medicine Review Article Edward W. Campion, M.D., Editor Ischemic Optic Neuropathies Valérie Biousse, M.D., and Nancy J. Newman, M.D. From the Departments of Ophthalmology (V.B.,
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Postural effects on intraocular pressure and ocular perfusion pressure in patients with non-arteritic anterior ischemic optic neuropathy
 Yang et al. BMC Ophthalmology (2017) 17:47 DOI 10.1186/s12886-017-0441-3 RESEARCH ARTICLE Open Access Postural effects on intraocular pressure and ocular perfusion pressure in patients with non-arteritic
Yang et al. BMC Ophthalmology (2017) 17:47 DOI 10.1186/s12886-017-0441-3 RESEARCH ARTICLE Open Access Postural effects on intraocular pressure and ocular perfusion pressure in patients with non-arteritic
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
T he extent of damage to the optic nerve caused by nonarteritic
 1274 EXTENDED REPORT Frequency doubling technology perimetry in non-arteritic ischaemic optic neuropathy with altitudinal defects C A Girkin, G McGwin Jr, J DeLeon-Ortega... See end of article for authors
1274 EXTENDED REPORT Frequency doubling technology perimetry in non-arteritic ischaemic optic neuropathy with altitudinal defects C A Girkin, G McGwin Jr, J DeLeon-Ortega... See end of article for authors
A Pilot with Decreased Vision
 A Pilot with Decreased Vision Christopher T. Bird, MD, MS Lt Col, USAF, MC, SFS Clifton M. Nowell, DO, MS Maj, USAF, MC, FS USAF School of Aerospace Medicine WPAFB, OH RAM 2013 1 Disclosure Information
A Pilot with Decreased Vision Christopher T. Bird, MD, MS Lt Col, USAF, MC, SFS Clifton M. Nowell, DO, MS Maj, USAF, MC, FS USAF School of Aerospace Medicine WPAFB, OH RAM 2013 1 Disclosure Information
MEASURING THE SIZE OF A TREATMENT EFFECT: RELATIVE RISK REDUCTION, ABSOLUTE RISK REDUCTION, AND NUMBER NEEDED TO TREAT
 MEASURING THE SIZE OF A TREATMENT EFFECT: RELATIVE RISK REDUCTION, ABSOLUTE RISK REDUCTION, AND NUMBER NEEDED TO TREAT Hussein Hollands, MD, MS (epid) Peter J. Kertes, MD, CM, FRCS(C) 72 The purpose of
MEASURING THE SIZE OF A TREATMENT EFFECT: RELATIVE RISK REDUCTION, ABSOLUTE RISK REDUCTION, AND NUMBER NEEDED TO TREAT Hussein Hollands, MD, MS (epid) Peter J. Kertes, MD, CM, FRCS(C) 72 The purpose of
Aging & Ophthalmology
 Aging & Ophthalmology Pr Jean-Marie Rakic Dr Denis Malaise January 2018 Major ocular diseases 1. Cataract 2. Age-related macular degeneration 3. Ischemic optic neuropathy 4. Horton arteritis 5. Glaucoma
Aging & Ophthalmology Pr Jean-Marie Rakic Dr Denis Malaise January 2018 Major ocular diseases 1. Cataract 2. Age-related macular degeneration 3. Ischemic optic neuropathy 4. Horton arteritis 5. Glaucoma
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Retinopathy of Prematurity. Objectives. Normal Retina Development. ROP Pathogenesis 6/8/2018. Thomas W. Hejkal, MD, PhD Eye Consultants, PC
 Retinopathy of Prematurity Thomas W. Hejkal, MD, PhD Eye Consultants, PC Chair Emeritus Department of Ophthalmology UNMC drhejkal@eyeconsultantspc.com (No commercial interests) Objectives Identify risk
Retinopathy of Prematurity Thomas W. Hejkal, MD, PhD Eye Consultants, PC Chair Emeritus Department of Ophthalmology UNMC drhejkal@eyeconsultantspc.com (No commercial interests) Objectives Identify risk
Retina Conference. Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014
 Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Diabetic maculopathy 11/ An update on. Miss Vasuki Sivagnanavel
 Miss Vasuki Sivagnanavel Consultant Ophthalmologist An update on Diabetic maculopathy Despite advances in the management of diabetes, diabetic retinopathy is already the commonest cause of blindness among
Miss Vasuki Sivagnanavel Consultant Ophthalmologist An update on Diabetic maculopathy Despite advances in the management of diabetes, diabetic retinopathy is already the commonest cause of blindness among
ISCHEMIC OPTIC neuropathy (ION)
 OBSERVATION Ischemic Optic Neuropathy Associated With Internal Carotid Artery Dissection Valérie Biousse, MD; Monique Schaison, MD; Pierre-Jean Touboul, MD; Jacques D Anglejan-Chatillon, MD; Marie-Germaine
OBSERVATION Ischemic Optic Neuropathy Associated With Internal Carotid Artery Dissection Valérie Biousse, MD; Monique Schaison, MD; Pierre-Jean Touboul, MD; Jacques D Anglejan-Chatillon, MD; Marie-Germaine
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Macular edema (ME) is the most common
 MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
MANAGEMENT OF RETINAL VEIN OCCLUSIONS * Peter A. Campochiaro, MD ABSTRACT Macular edema (ME) is the most common cause of reduced vision in patients with retinal vein occlusions (RVOs). The primary cause
Clinical Characteristics of Optic Neuritis in Koreans Greater than 50 Years of Age
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(2):111-115 http://dx.doi.org/10.3341/kjo.2012.26.2.111 Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(2):111-115 http://dx.doi.org/10.3341/kjo.2012.26.2.111 Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than
Sleep Disorders and the Eye. Jasmine Gopwani MBBS FRCS(Ophthalmology) Consultant Neuro-Ophthalmologist
 Sleep Disorders and the Eye Jasmine Gopwani MBBS FRCS(Ophthalmology) Consultant Neuro-Ophthalmologist Introduction - Obstructive sleep apnea - Nocturnal lagophthalmos - Circadian rhythm disorders in blindness
Sleep Disorders and the Eye Jasmine Gopwani MBBS FRCS(Ophthalmology) Consultant Neuro-Ophthalmologist Introduction - Obstructive sleep apnea - Nocturnal lagophthalmos - Circadian rhythm disorders in blindness
Diabetic eye disease. Diabetic retinopathy. Sam S. Dahr, M.D. Retina Center of Oklahoma.
 Diabetic eye disease Sam S. Dahr, M.D. Retina Center of Oklahoma www.rcoklahoma.com Downloaded from: The Retina (on 28 May 2007 12:48 AM) 2007 Elsevier Diabetic retinopathy Downloaded from: The Retina
Diabetic eye disease Sam S. Dahr, M.D. Retina Center of Oklahoma www.rcoklahoma.com Downloaded from: The Retina (on 28 May 2007 12:48 AM) 2007 Elsevier Diabetic retinopathy Downloaded from: The Retina
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Ophthalmology Unit Referral Guidelines
 Ophthalmology Unit Referral Guidelines Austin Health Ophthalmology Unit holds sub-specialty sessions to discuss and plan the treatment of patients with specific ocular conditions. General including cataract
Ophthalmology Unit Referral Guidelines Austin Health Ophthalmology Unit holds sub-specialty sessions to discuss and plan the treatment of patients with specific ocular conditions. General including cataract
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery
 The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
The Case: A 64 yo man with chronic back pain has elective multilevel lumbar spinal surgery The Case: Upon awakening from anesthesia, he is blind in both eyes After Non-Ocular Surgeries Nancy J. Newman,
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Incidence and Clinical Features of Neovascularization of the Iris following Acute Central Retinal Artery Occlusion
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(5):352-359 http://dx.doi.org/10.3341/kjo.2016.30.5.352 Original Article Incidence and Clinical Features of Neovascularization of the Iris following
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(5):352-359 http://dx.doi.org/10.3341/kjo.2016.30.5.352 Original Article Incidence and Clinical Features of Neovascularization of the Iris following
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
Diabetic Retinopathy Screening Program in the Cree Region of James Bay of Quebec
 RUIS McGILL VIRTUAL HEALTH AND SOCIAL SERVICES CENTRE (CvSSS) SIMPLIFYING TELEHEALTH! Diabetic Retinopathy Screening Program in the Cree Region of James Bay of Quebec Nurse and Imager Training Prepared
RUIS McGILL VIRTUAL HEALTH AND SOCIAL SERVICES CENTRE (CvSSS) SIMPLIFYING TELEHEALTH! Diabetic Retinopathy Screening Program in the Cree Region of James Bay of Quebec Nurse and Imager Training Prepared
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
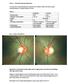 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Patient with Daily Headache NTERNATIONAL CLASSIFICATION HEADACHE DISORDERS. R. Allan Purdy, MD, FRCPC,FACP. Professor of Medicine (Neurology)
 Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Anterior Ischemic Optic Neuropathy
 UNIVERSITY OF ZAGREB SCHOOL OF MEDICINE Laurent Martini Anterior Ischemic Optic Neuropathy GRADUATE THESIS Zagreb, 2016. This graduate thesis was made at the department of Neuro-ophthalmology of KBC Retro,
UNIVERSITY OF ZAGREB SCHOOL OF MEDICINE Laurent Martini Anterior Ischemic Optic Neuropathy GRADUATE THESIS Zagreb, 2016. This graduate thesis was made at the department of Neuro-ophthalmology of KBC Retro,
mg
 24 11 2 40 mg 23 12 19 24 10 26 4 24 10 16 40 mg 23 12 19 1 40 mg 4 6 24 10 16 40 mg 23 12 19 1 4 ml 10 mg/ml 0.5 4 mg 0.05 0.4 ml 40 mg/ml 1 1mL 4mg 40 mg/ml 0.1 ml 2 . 1 40 mg 24 9 6 23 12 19 1 40 mg
24 11 2 40 mg 23 12 19 24 10 26 4 24 10 16 40 mg 23 12 19 1 40 mg 4 6 24 10 16 40 mg 23 12 19 1 4 ml 10 mg/ml 0.5 4 mg 0.05 0.4 ml 40 mg/ml 1 1mL 4mg 40 mg/ml 0.1 ml 2 . 1 40 mg 24 9 6 23 12 19 1 40 mg
Anti VEGF Agents in Retinal Disorders Current Scenario
 Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Retina Anti VEGF Agents in Retinal Disorders Current Scenario Charu Gupta MS Charu Gupta MS, Cyrus M. Shroff MD Shroff Eye Centre, New Delhi T is a group of proteins involved in the regulation of angiogenesis,
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD
 Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington
 Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Cataract and Diabetic macular edema: What should I do?
 Cataract and Diabetic macular edema: What should I do? Irini Chatziralli Ophthalmic Surgeon, University Scholar 2 nd Department of Ophthalmology, University of Athens (Director: Prof P. Theodossiadis)
Cataract and Diabetic macular edema: What should I do? Irini Chatziralli Ophthalmic Surgeon, University Scholar 2 nd Department of Ophthalmology, University of Athens (Director: Prof P. Theodossiadis)
Central Retinal Vein Occlusion
 Central Retinal Vein Occlusion Sohan Singh Hayreh, MD, MS, PhD, DSc, FRCS, FRCOphth Professor Emeritus of Ophthalmology Ocular Vascular Clinic Department of Ophthalmology and Visual Sciences The University
Central Retinal Vein Occlusion Sohan Singh Hayreh, MD, MS, PhD, DSc, FRCS, FRCOphth Professor Emeritus of Ophthalmology Ocular Vascular Clinic Department of Ophthalmology and Visual Sciences The University
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Evolution of the Definition of Primary Open-Angle Glaucoma
 OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
A retrospective nonrandomized study was conducted at 3
 Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Department of Ophthalmology, Kangbuk Samsung Hospital, Sungkyunkwan University College of Medicine 1, Seoul, Korea Hangil Eye Hospital 2, Incheon, Korea Seoul National University Bundang Hospital 3, Seongnam,
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema V Swetha E Jeganathan 1,2 * and Karen Madill 3 1 Department of Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Report Inherent Challenges in Managing Long Standing Refractory Diabetic Macular Edema V Swetha E Jeganathan 1,2 * and Karen Madill 3 1 Department of Ophthalmology,
Sudden Vision Loss. Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists
 Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
Rapid Visual Loss. Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist
 Rapid Visual Loss Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist Outline Pathophysiology Differential diagnosis. Patient scenarios in community practice:
Rapid Visual Loss Dr Michael Johnson PhD FCOptom DipOrth DipGlauc DipTp(IP) Independent Prescribing Optometrist Outline Pathophysiology Differential diagnosis. Patient scenarios in community practice:
EFFECTIVENESS OF RADIAL OPTIC NEUROTOMY FOR ISCHEMIC CENTRAL RETINAL VEIN OCCLUSION ABSTRACT
 ORIGINAL ARTICLE EFFECTIVENESS OF RADIAL OPTIC NEUROTOMY FOR ISCHEMIC CENTRAL RETINAL VEIN OCCLUSION Mir Ali Shah 1, Faisal Nawaz 2, Adnan Alam 3, Bilal Khan 4 1-4 Department of Ophthalmology, Lady Reading
ORIGINAL ARTICLE EFFECTIVENESS OF RADIAL OPTIC NEUROTOMY FOR ISCHEMIC CENTRAL RETINAL VEIN OCCLUSION Mir Ali Shah 1, Faisal Nawaz 2, Adnan Alam 3, Bilal Khan 4 1-4 Department of Ophthalmology, Lady Reading
Closed Angle Glaucoma Or Narrow Angle Glaucoma. What s is a closed angle type of glaucoma,
 Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
From Outdated to Updated: A Review of Important Clinical Trials in Ocular Disease from 2014
 From Outdated to Updated: A Review of Important Clinical Trials in Ocular Disease from 2014 1. This course is designed to review the important ophthalmic literature that was released between October 2013
From Outdated to Updated: A Review of Important Clinical Trials in Ocular Disease from 2014 1. This course is designed to review the important ophthalmic literature that was released between October 2013
11/30/2009. Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil
 Normal Ocular Anatomy Glaucoma Dr Sunil Deokule, MD Asst. Prof and Glaucoma Specialist University of Kentucky Definition Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil Optic
Normal Ocular Anatomy Glaucoma Dr Sunil Deokule, MD Asst. Prof and Glaucoma Specialist University of Kentucky Definition Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil Optic
I have nothing to disclose but I
 OPTIC NEUROPATHIES Robert L. Tomsak MD PhD Professor of Ophthalmology and Neurology Wayne State t University it Sh School of Mdii Medicine I have nothing to disclose but I wish I did. dd Road map for this
OPTIC NEUROPATHIES Robert L. Tomsak MD PhD Professor of Ophthalmology and Neurology Wayne State t University it Sh School of Mdii Medicine I have nothing to disclose but I wish I did. dd Road map for this
Common Causes of Vision Loss
 Common Causes of Vision Loss Learning Objectives To identify the most common causes of vision loss in the United States To differentiate the most common forms of agerelated macular degeneration and diabetic
Common Causes of Vision Loss Learning Objectives To identify the most common causes of vision loss in the United States To differentiate the most common forms of agerelated macular degeneration and diabetic
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
VMA at the macula resulting in VMT
 Ocriplasmina for pharmacologic treatment in VMT Teresio Avitabile 1 Introduction PVD is a normal, physiologic process that occurs with aging; however, in some cases, PVD is incomplete Incomplete PVD localized
Ocriplasmina for pharmacologic treatment in VMT Teresio Avitabile 1 Introduction PVD is a normal, physiologic process that occurs with aging; however, in some cases, PVD is incomplete Incomplete PVD localized
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Grand Rounds. Eddie Apenbrinck M.D. University of Louisville School of Medicine Department of Ophthalmology & Visual Sciences 6/20/2014
 Grand Rounds Eddie Apenbrinck M.D. University of Louisville School of Medicine Department of Ophthalmology & Visual Sciences 6/20/2014 Subjective CC: sudden painless loss of vision OD HPI: 75 year old
Grand Rounds Eddie Apenbrinck M.D. University of Louisville School of Medicine Department of Ophthalmology & Visual Sciences 6/20/2014 Subjective CC: sudden painless loss of vision OD HPI: 75 year old
Treatment of central retinal artery occlusions
 Treatment of central retinal artery occlusions Jeffrey N. Weiss Retina Associates of South Florida, Margate, Florida, USA To the Editor: As a practicing retinal specialist for the last 28 years, I read
Treatment of central retinal artery occlusions Jeffrey N. Weiss Retina Associates of South Florida, Margate, Florida, USA To the Editor: As a practicing retinal specialist for the last 28 years, I read
Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema
 Original Article Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema Karen Joyce G. Castro, MD, Marie Joan V. Loy, MD International Eye Institute St. Luke s Medical Center
Original Article Clinical Outcomes After Intravitreal Bevacizumab Injection for Diabetic Macular Edema Karen Joyce G. Castro, MD, Marie Joan V. Loy, MD International Eye Institute St. Luke s Medical Center
ILUVIEN IN DIABETIC MACULAR ODEMA
 1 ILUVIEN IN DIABETIC MACULAR ODEMA Marie Tsaloumas Consultant Ophthalmic Surgeon Queen Elizabeth Hospital, Birmingham bars conference 2104 1 2 Declaration of interest I have sat on Advisory boards for
1 ILUVIEN IN DIABETIC MACULAR ODEMA Marie Tsaloumas Consultant Ophthalmic Surgeon Queen Elizabeth Hospital, Birmingham bars conference 2104 1 2 Declaration of interest I have sat on Advisory boards for
Question 1: Comment on the optic nerve appearance of each eye.
 Case 2 - Right Optic Nerve Head Drusen (ONHD) A 41 year old female was referred by her optometrist for a workup for unilateral optic disc drusen, OCT, and visual field changes. The patient was otherwise
Case 2 - Right Optic Nerve Head Drusen (ONHD) A 41 year old female was referred by her optometrist for a workup for unilateral optic disc drusen, OCT, and visual field changes. The patient was otherwise
Christina L. Ryu, 1 Adrian Elfersy, 1 Uday Desai, 1 Thomas Hessburg, 1 Paul Edwards, 1 and Hua Gao 1,2. 1. Introduction
 Ophthalmology, Article ID 317694, 6 pages http://dx.doi.org/10.1155/2014/317694 Research Article The Effect of Antivascular Endothelial Growth Factor Therapy on the Development of Neovascular Glaucoma
Ophthalmology, Article ID 317694, 6 pages http://dx.doi.org/10.1155/2014/317694 Research Article The Effect of Antivascular Endothelial Growth Factor Therapy on the Development of Neovascular Glaucoma
EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA
 Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Basrah Journal Of Surgery EFFICACY OF INTRAVITREAL TRIAMCINOLONE ACETONIDE FOR THE TREATMENT OF DIABETIC MACULAR EDEMA Salah Zuhair Abed Al-Asadi MB,ChB, FICMS, Lecturer, Department of Surgery, College
Anatomical results and complications after silicone oil removal
 Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
Romanian Journal of Ophthalmology, Volume 61, Issue 4, October-December 2017. pp:261-266 GENERAL ARTICLE Anatomical results and complications after silicone oil removal Brănişteanu Daniel Constantin* **,
10/27/2013. Optic Red Herrings
 Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
