Evaluation of Diagnostic Fasting in the Investigation of Hypoglycemia in Children Omani Experienc
|
|
|
- Shawn Allen
- 5 years ago
- Views:
Transcription
1 Evaluation of Diagnostic Fasting in the Investigation of Hypoglycemia in Children Omani Experienc Bhasker Bappal, Waad Sharef Mula-Abed Abstract Objectives: To assess the safety and importance of diagnostic fast in the evaluation of hypoglycemia in children in a non-specialist set up. Method: The medical records of 6 patients with hypoglycemia, admitted to Pediatric Unit, Royal Hospital, Muscat, Sultanate of Oman, over a 5 year period, were reviewed. Of these, 96 (8.8%) patients, 5 boys and 44 girls, aged 8 days to 0 years were subjected to diagnostic fast. Results: Of these 96 patients fasted, 77 (80.%) became hypoglycemic (HG group) and 9 (9.8 %) did not develop hypoglycemia on fast (NHG group). In the HG group, 69 (89.6%) patients developed symptomatic hypoglycemia of variable severity and none developed coma or convulsions during fasting. Conclusion: The study has proved that diagnostic fast is Introduction Establishing correct diagnosis is the most important step in the management of hypoglycemia in children. The sample of blood and urine, collected at the time of hypoglycemia may give valuable clue to establish the diagnosis and cause of hypoglycemia. If this window of opportunity is missed, diagnostic fasting may be necessary to unmask the cause of hypoglycemia. The value of focused history and physical examination cannot be underestimated. It is important to find out whether hypoglycemia occurs after a long period of fasting as in fatty acid oxidation defect (FAOD) or soon after a meal as in fructose intolerance. The length of feeding intervals in a baby on demand feeds may also give some information on the duration of fasting tolerance. Similarly, many base-line investigations like blood gases, liver function tests, lactate, creatine kinase, ammonia, uric acid, cholesterol and triglycerides are valuable, but by themselves may not lead to any specific diagnosis. Some of the metabolic and endocrine disorders, no doubt, could be diagnosed without resorting to fasting. Many FAOD could be diagnosed by looking at carnitine profile. However, it may be necessary to induce hypoglycemia by diagnostic fasting and obtain samples of blood and urine for metabolic and hormonal assays. It is important to know that adequate duration of fasting may not always unearth the underlying defect. One should not undertake diagnostic fast lightly as there is an inherent danger of serious complications, if hypoglycemia goes unrecognized during provoked fasting. 3 Therefore, it is important to ensure utmost care, during diagnostic fast. The diagnostic fast is particularly risky in hyperinsulinemic state and in some of the metabolic disorders like fructose, 6 diphosphatase (F., 6DP) deficiency and FAOD. Therefore, many centers do blood TMS before resorting to diagnostic fasting., 4 relatively a safe procedure with considerable amount of diagnostic yield. Key words: Hypoglycemia, fast, ketone utilization defect, succinly Coa transferase deficiency, idiopathic ketotic hypoglycemia, carnitine plamitoyl transferase deficiency. Submitted: 3 March 007 Reviewed: 9 June 007 Accepted: 3 September 007 From the Department of Child Health, Royal Hospital, P.O.Box. 33, Seeb, Muscat, Sultanate of Oman; Department of Chemical Pathology, Royal Hospital, P.O.Box 33, Seeb, Muscat, Sultanat of Oman. Address Correspondence to: Bhasker Bappal, Department of Child Health, Royal Hospital, Muscat, Sultanate of Oman. E mail: bappal@omantel.net.om Objective The objective of the study was to assess the value of diagnostic fast in the evaluation of hypoglycemic disorders in children in a non-specialist set up. Methods The medical records of 6 patients with hypoglycemia, admitted to Pediatric Endocrine and Metabolic Unit, Royal Hospital, Muscat, Sultanate of Oman, over a 5 year period, from Jan. 99-Dec. 005 were reviewed. Of these, 0 (7.%) patients were excluded from the study because of incomplete records, 5 non-availability of records 4 or the diagnosis was made without fasting. 5 The remaining 96 (8.8%) patients were subjected to diagnostic fast as per the Unit protocol. The maximum duration of fasting was based on the age of the child,, usual feeding pattern and fasting tolerance. The duration of fasting was for 8,, 8 and 0 hours for children aged < 6 months, between 6 to months, to years and to 7 years respectively. Children aged < 6 months and those with very short fasting tolerance as in suspected hyperinsulinism and glycogen storage disease are fasted during morning hours. The signs and symptoms of hypoglycemia were closely monitored throughout the fasting period. The frequency of blood glucose (BG) monitoring is individualized depending on the anticipated period of fasting tolerance. If short fasting tolerance is suspected as in hyperinsulinism, the BG was monitored every 5 to 30 minutes after commencing fast. When longer fasting tolerance is anticipated, the BG is monitored 4 to 6 hours after the beginning of fast. The BG was monitored, first every hours, then hourly, when the BG was <3.5 mmol/l and then more frequently, if BG was <3 mmol/l. Hypoglycemia was defined as BG.6 mmol/ L. The patient on diagnostic fast was also considered to have hypoglycemia, if presumed symptoms of hypoglycemia respond to 36
2 dextrose infusion even if BG was >.6 mmol/l. At the end of fasting i.e. when BG.6 mmol/l or end of predetermined duration of fasting, urine and blood samples were collected for the following tests: serum cortisol, growth hormone, C-peptide, insulin, lactate, pyruvate, ammonia, amino acids, free fatty acids, 3 ß.hydroxybutyrate and blood gases. The urine was checked for ketones in all voided samples, during fasting. Blood was also collected for carnitine profile (free, total and acyl-carnitine) if not collected earlier. Fasting was terminated by feeding or by IV 0% dextrose infusion after blood samples collection. Urine sample for organic acids was collected after terminating fasting or immediately after patient recovered from hypoglycemia. Results Of the 96 patients, 7 (7.7%) were from Muscat region and the remaining 79 (8.3%) were referred from different regional hospitals of Oman. There was at least one or more than one documented hypoglycemia in 83 (86.5%) of patients studied. The age group of patients ranged from 8 days to 0 years and there were 5 boys and 44 girls. Table show that 5% of patients were below the age of year,.9% were below the age of years, 48.9% were between to 5 years and only 4.% of patients were in the age group of 5 to 0 years. Table shows that of the 96 patients fasted, 77 (80.%) became hypoglycemic (Hypoglycemic group-hg group) and 9 (9.8 %) did not develop hypoglycemia on fast (Non hypoglycemic group- NHG group). The majority of patients, 69 (89.6%) in HG group developed symptomatic hypoglycemia of variable severity and none in this group developed coma or convulsions during fasting. In 49 (63.6%) patients the BG concentration was between to.6 mmol/l, in 3 (9.9%) the BG was between to < mmol/ L, and in (.6%) the BG dropped around 0.9 mmol/l. The HG group also included 3 (3.9%) patients with BG.6-3. mmol/l, but these were considered to be clinically hypoglycemic because of the hypoglycemic symptoms and prompt recovery following dextrose infusion. Table and the sector diagram also shows the final outcome in the 96 patients fasted. In 77 patients in HG group, specific diagnosis was made in 50 (64.9%) patients; this includes (7.3 %) patients with endocrine diseases and 9 (37.7%) patients with metabolic disorders. In (8.6%), the diagnosis was uncertain and in 5 (6.5%) no diagnosis was established. The specific metabolic conditions diagnosed were: glycogen storage disease in 8 (0.35%), neoglucogenesis defect in (.6%), fatty acid transport defect in 8 (0.35%), FAOD in 6 (6.6%), ketone synthesis defect in 3 (3.9%) and ketone utilization defect in (.6%). In the patients with uncertain diagnosis, the possibilities considered were: idiopathic ketotic hypoglycemia (IKHG) in 5 (9.5%), Reye syndrome in 3 (3.9%), mitochondrial respiratory chain defect in (.6%), succinyl CoA transferse (SCOT) deficiency in (.3%) and F, 6D deficiency in another (.3%). In the NHG group, there were 9 patients aged.6 to 4 years with a mean of. years. The duration of fasting ranged from 4.5 to 8 hours. There was past history of documented hypoglycemia in 4 patients; 9 had only one episode and 5 of them had or more symptomatic hypoglycemic episodes before referral, and suspected hypoglycemia in 5 patients. In 3 patients, diagnostic fast was interrupted by parents prematurely and in patients, the investigations were incomplete. None in the remaining 4 patients developed hypoglycemia though the duration of fasting was considered to be appropriate for the age. Only (0.5%) patients showed laboratory evidence of metabolic disease. In one patient, the diagnosis was carnitine palmitoyl transferase (CPT-) deficiency based on elevated plasma free carnitine, and in the other patient, the diagnosis of 3.hydroxy. methylglutaryl CoA (HMGCoA) lyase deficiency was made on the basis of the characteristic urine organic acid abnormality on TMS. Discussion The study has revealed that more number of children present with hypoglycemia during the first month of life as compared to the later part of infancy. The metabolic transition that takes place during the first few days of life in a neonate increases the vulnerability to hypoglycemia. The risk of hypoglycemia increases again after the age of one year with maximum number cluster around the age of to 5 years. This may be that toddlers get fed less frequently, thus exposing those with defect in glucose homeostasis to hypoglycemia. Of the 96 patient s fasted as whole, specific endocrine (.9%) and metabolic (30.%) diagnosis was made in 50 (5.%) patients. Whereas, in Morris study that included 38 patients fasted, specific endocrine and metabolic diagnosis was made only in.7% of cases. In the latter study, 57.% patients had hypoglycemia before referral as compared to 8.3% in the present study. It is not surprising, therefore to have more specific diagnosis in our series. The metabolic conditions diagnosed were; glycogen storage disease and defects in gluconeogenesis, fatty acid transport, fatty acid oxidation, ketone body synthesis and ketone body utilization. Morris found IKHG as the main cause of hypoglycemia in children, comprising nearly 3% of the total cases. It is important to recognize that the presence of ketosis in a patient with hypoglycemia is not equivalent to IKHG, as this is a diagnosis of exclusion. 6,7 Ketosis is a normal physiological response to fasting. 37
3 Table. Age Distribution of Patients at Referral Age Group < month to <6 month 6 to < month to < years to <5 years 5 to 0 years No % 0.4% 6.3% 8.3%.9% 48.9% 4 (5%) 7 (75%) Table. Final Diagnosis in Fasted Hypoglycemic (HG) and Non-Hypoglycemic (NHG) Groups. HYPOGLYCEMIC GROUP (N=77, 80. %) DISORDER DIAGNOSIS FREQUENCY % ENDOCRINE SPECIFIC METABOLIC DISEASE a) Hyperinsulinism b) ACTH deficiency c) ACTH resistance d) Hypopitutarism. Glycogen Storage Disease a. GSD- b. GSD-3 c. GSD-0. Neoglucogenesis defect a) Fructose -6 DP Deficiency b) Glycerol kinase 3. Fatty acid transport and oxidation defects (a)fatty acid transport CPT- CPT- (b)fatty acid oxidation defect Long chain hydroxyacyl dehydrogenase Glutaric aciduria- Ehtylmelonic aciduria % 7.3% 0.35%.6% 0.35% 6.6% 4. Ketone synthesis defect Hydroxymethylglutaryl CoA lyase deficiency 3 3.9% 5. Ketone utilization defect -ketothiolase deficiency.6% DIAGNOSIS UNCERTAIN. Idiopathic ketotic hypoglycemia 5 9.5%. Fructose -6 diphosphatase deficiency 3. Succinyl CoA transferse deficiency (SCOT) 4.Mtochondrial Respiratory chain defect 5. Reye syndrome 3 7 9% NO DIAGNOSIS 5 6.4% NON-HYPOGLYCEMIC GROUP (N= 9, 9.8 %) SPECIFIC METABOLIC DIAGNOSIS CPT- Hydroxymethylglutaryl CoA lyase deficiency.% NO DIAGNOSIS % 38
4 It is also a normal compensatory response to fasting in growth hormone, cortisol deficiency and in many metabolic disorders. In contrast, ketosis due to ketolytic disorder is an abnormal biochemical response as the defect is in the utilization of ketones by tissues. 8 The diagnosis of 5 (5.6%) patients with IKHG in our series was based on the absence of laboratory evidence of other diseases known to have ketotosis during hypoglycemia. The diagnosis was supported by the history of intrauterine growth retardation, with or without low plasma alanine, normal lactate and carnitine, suppressed C- peptide and appropriately elevated cortisol. 5 One condition that may be difficult to exclude from IKHG is SCOT deficiency. 9 This is a ketone utilization defect with variable severity and may have intermittent or persistent ketoacidosis. During the episodes of ketosis, BG may be normal, low or high. 0 As in IKHG, no abnormality is found in plasma carnitine, lactate, ammonia and urine organic acids. 0, The possibility of SCOT was considered in one patient who presented with hypoglycemic ketoacidosis at the age of 8 months and had severe recurrent course. The biochemical analysis during ketoacidosis showed elevated plasma nonesterified fatty acids (NEFA), ß.hydroxybutyrate and acetoacetate with profound ketonuria. 8 The patient also developed metabolic acidosis, ketosis and hypoglycemia within hours of fasting. The diagnosis of SCOT could be confirmed by SCOT enzyme activity in skin fibroblasts or by molecular genetics. Among the 5 cases of fatty acid transport and oxidation defect diagnosed in our series, the commonest defect was CPT- deficiency. 8 The CPT- facilitates the transfer of long chain fatty acids through the inner mitochondrial membrane. 7 Of the total 8 patients with CPT- deficiency, 5 presented with fasting hypoglycemia and had features of Reye s syndrome in addition. In 5, the diagnosis was made on the basis of elevated free carnitine. The markedly elevated free carnitine is diagnostic of CPT- deficiency. However, it is not necessary that such patients must always have elevated free carnitine. 8 Two siblings in the present study had clinical and a biochemical finding identical to CPT- deficiency but the plasma free carnitine concentration was within normal. There was one 8- month-old infant with CPT-/translocase deficiency who had two episodes of hypoglycemia before referral. The clinical examination showed no cardiac and skeletal muscle involvement, and serum creatine kinase and free carnitine was normal. Urine TMS showed no dicarboxylic aciduira. The level of C6 and C6: species of long chain acylcarnitine was markedly increased supporting the diagnosis of CPT-/translocase deficiency. The 5 patients with FAOD in this series include with long chain hydroxyacyl dehydrogenase (LCHAD), with glutaric aciduria- (GA-) and with ethylmelonic aciduria (EMA). The patients with LCHAD presented with recurrent hypoglycemic seizures for the first time at the age of 3 and year respectively and both remained well in between the attacks of hypoglycemia. The first patient s family had lost two siblings at an early age from an undiagnosed seizure disorder. The urine organic acids during fasting revealed long chain 3 hydroxy dicarboxylic aciduria (C more than C0 acids) with minimum ketonuria. The free carnitine was low and long chain acylcarnitine was elevated. The 3 patients with GA- reported in the study were referred at the age of 4.5 year, 0 year and 6 month. The first two patients were siblings. All presented with recurrent hypoglycemia associated with lactic acidosis at the age of.5 year, 5 year and 3 month respectively. The first patient also had exercise induced muscle cramps with elevated creatine kinase. The urine organic acids by TMS showed elevated lactate, ethylmelonic acid, short and medium chain glycine conjugates and.hydroxyglutaric acid. All of them responded to pharmacological dose of riboflavin. 3 The one patient with EMA described here presented with recurrent hypoketotic hypoglycemia from the age of.5 years. Investigations showed mild elevation of liver enzymes and serum lactate with low free carnitine. Urine organic acid by TMS revealed elevated EMA. This patient was developmentally normal and had no neurological or vascular abnormalities. The urine could also be positive for ethylmelonic acid in GA-, SCAD and mitochondrial disorders. 7 The clinical features described resemble mild form of GA-. EMA has considerable phenotypic variability and may or may not be associated with skeletal myopathy, cardiomyopathy, vasculopathy 8, 4, 5 and neurological manifestations. There were 3 patients presented with mitochondrial HMGCoA lyase deficiency. This is a ketone body synthetic defect, which is considered to be the commonest organic aciduria in Saudi Arabia. 6 The presentation in the first two patients aged 4 year and year resembled Reye s encephalopathy and the other aged 0 months presented with recurrent hypoglycemic seizures. The urine TMS in all, revealed 3.hydroxy.3.methylglutaric acid, 3.methylglutaric acid and hydroxyisovaleric acid. The 0 month old baby showed developmental delay on follow up. The patients with ketothiolase deficiency described are siblings. The mitochondrial acetoacetyl CoA thiolase (ß ketothiolase) like SCOT is a ketone utilization defect. But unlike SCOT, this condition is easily diagnosed because of the presence of specific metabolites in urine by TMS. The patients present with severe intermittent ketoacidosis. 7 In both patients, the symptoms started at around the age of.5 years. They presented with recurrent episodes of hypoglycemia and ketoacidosis. During diagnostic fast there was marked ketosis with a fall in BG to < 3 mmol/l. Urine organic acid revealed hyperketonuria, dicarboxylic aciduria, 3 hydroxy carboxylic acid, tiglylglycine and metabolites of isoleucine. 39
5 One patient with hepatic F., 6DP deficiency had the first episode of hypoglycemia with severe lactic acidemia on day of life and made uneventful recovery. 8 He remained asymptomatic till the age of 8 months, thereafter; he had 3 more similar episodes. Diagnostic fast at the age of 4 months resulted in hypoglycemia, metabolic acidosis, lactic acidemia and elevated liver enzymes. No abnormality was found in serum carnitine and organic acids. The deficiency of F, 6DP was confirmed by the absence of enzyme activity (zero activity) in leucocytes study. The patient with glycerol kinase deficiency (GKD), presented at the age of 7 days with hypoglycemia had the classical clinical and hormonal abnormalities of congenital adrenal hypoplasia. On follow up, he developed features of Duchene s muscular dystrophy. This is an X- linked, over-lap syndrome with congenital adrenal hypoplasia and Duchene muscular dystrophy as the main manifestations. 9 Glycerol contributes up to 0% of glucose generation by gluconeogenesis during fasting. 0 During diagnostic fast he developed hypoglycemia and blood showed elevated triglyceride and urine showed elevated glycerol. The study included 8 patients with glycogen storage disease (GSD). The patient with GSD-0 is discussed further as this diagnostic possibility is not usually entertained. A 4 year old boy presented with recurrent episodes of early morning lethargy with or without convulsions from the age of.5 year. He was earlier investigated elsewhere and was being treated with anticonvulsants. Clinically, there was no hepatomegaly, the rest of systemic examination was normal and his basal investigations, including plasma carnitine showed no abnormalities. At the end of 4.5 hours of diagnostic fasting, BG was < mmol/l, urine showed excess ketones and serum lactate was within the normal range. The post prandial BG ranged from 8 to 3 mmol/l with concomitant increase in lactate levels to 4 to 6 mmol/l. This constellation of clinical and biochemical findings are consistent with the diagnosis of GSD-0. The diagnosis could be confirmed by the assay of glycogen synthetase enzyme in hepatic tissue. Mutation analysis of the GYS gene (p.) is a non-invasive method for establishing the diagnosis. Conclusion In this study of highly selected group of patients with documented hypoglycemia upon diagnostic fast, hypoglycemia was provoked in 4/5 th of patients and in more than /3 rd of patients a definite cause for the hypoglycemia was established. The metabolic disorders constituted the commonest cause of hypoglycemia in almost half of the children. The final confirmation of diagnosis depends on demonstrating the specific enzymatic defects or mutational defects of the genes governing the three metabolic pathways' of glucose homeostasis. This facility is generally not accessible for pediatricians from the developing countries. The cases discussed with the background of clinical features, results of metabolic-endocrine investigations and diagnostic fast, gives ample evidence that diagnostic fast is a valuable procedure both in terms of establishing the diagnosis and in guiding management in a non-specialist pediatric set-up, and it is a fairly safe procedure, if adequate safety precautions are taken. References. Morris AA, Thekekara A, Wilks Z, Clayton PT, Leonard JV, A. Evaluation of fasts for investigating hypoglycaemia or suspected metabolic disease. Arc Dis Child 996; 75:5-9.. Bonnefont JP, Specola NB, Vassault A, Lombes A, Ogier H, de Klerk JB et al. The fasting test in paediatrics: application to the diagnosis of pathological hypo and hyperketotic states. Eur J Pediatr 990; 50: Gregersen N, Lauritzen R, Rasmussen K. Suberylglycine excretion in theurine from a patient with dicarboxylic aciduria. Clin Chim Acta 976; 70: Van Hove JL, Zhang W, Kahler SG, Roe CR, Chen YT, Terada N et al. Medium chain acyl-coa dehydrogenase (MCAD) deficiency: diagnosis by acylcarnitine analysis in blood. Am J Hum Genet 993; 5: Ansley-Green A, Solteiz G. In: Hypoglyccemia in infancy and childhood. A clinical approach to the child with hypoglycemia. Churchil Livingstone: London, 985. p Stanley CA. Praising ketotic hypoglycemia. Arch Dis Child 006; 9: Roe CR, Ding J. Mitochondrial fatty acid oxidation disorders. In: Sciver CR, Beaudet AL, Sly WS, Valle D, ed. The metabolic and molecular basis of inherited disease. 8 th Ed. New York: McGrow-Hill Medical Publishing, 00; : Pagliara AS, Karl IE, DeVio DC, Feigin RD, Kipins DM.Hypoalaninemia: a concomittent of ketotic hypoglycemia. J Clin Invest 97; 5: Tildon JT, Cornblath M. Succinly CoA: 3 Ketoacid CoA Transferase deficiency: A cause of Ketoacidosis in infancy. J Clin Invest 97; 5: Berry GT, Fukao T, Mitchell GA, Mazur A, Ciafre M, Gibson J et al. Neonatal Hypoglycemia in severe Succinyl CoA deficiency. J Inherit Metab Dis 00; 4: Longo N, Fukao T, Singh R, Pasquali M, Barrios RG, Kondo N et al. Succinyl CoA:3-ketoacid transferase (SCOT) deficiency in a new patient homozygous for an R7X mutation. J Inherit Metab Dis 004; 7: Stanley CA, Sunaryo F, Hale DE, Bonnefont JP, Demaugre F, Saudubray JM. Elevated plasma carnitine in the hepatic form of carnitine palmitoyltransferase- deficiency. J Inherit Metab Dis 99; 5: Gregersen, N, Wintzensen H, Christensen SKE, Christensen MF, Brandt NJ, Rasmussen K. C(6)-C(0)-dicarboxylic aciduria: Investigations of a patient with riboflavin responsive multiple acyl-coa dehydrogenation defects. Pediatr Res 98; 6: Birkebaek NH, Simonsen H, Gregersen N. Hypoglycaemia and elevated urine ethylmalonic acid in a child homozygous for the short-chain acyl-coa dehydrogenase 65G > A gene variation. Acta Paediatr 00; 9: Ozand PT, Rashed M, Millington DS, Sakati N, Hazzaa S, Rahbeeni Z et al. Ethymelonic aciduria: an organic acidemia with CNS involvement and vasculopathy. Brain Dev 994; 6:-. 6. Mitchell GA, Ozand PT, Robert MF, Asmarina L, Roberts J. HMG CoA lyase deficiency: identification of five causal point mutations in codons 4 and 4, including a frequent Saudi Arabian mutation, R4Q. Am J Hum Genet 998; 6: Przyrembel H, Wendel U, Becker K, Bremer HJ, Bruinvis L, Ketting D et al. Glutaric aciduria type II: report on a previously undescribed metabolic disorder Clin Chim Acta 976; 66:
6 8. Baker L, Winegrad AI. Fasting hypoglycaemia and metabolic acidosis associated with deficiency of hepatic fructose-, 6-diphosphatase activity Lancet 970; : Sehgal A, Stack J. Complex glycerol kinase deficiency: An X-linked disorder associated with adrenal hypoplasia congenita. Indian J Pediatr 005; 7: Dietze G, Wicklmayr M, Hepp KD, Bogner W, Mehnert H, Czempiel H et al. On gluconeogenesis of human liver. Accelerated hepatic glucose formation induced by increased precursor supply. Diabetologia 976; : Weinstein DA, Correia CE, Saunders AC, Wolfsdorf JI. Hepatic glycogen synthase deficiency: an infrequently recognized cause of ketotic hypoglycemia Mol Genet Metab 006; 87:
Fatty Acid Oxidation Disorders- an update. Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London
 Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
Fatty Acid Oxidation Disorders- an update Fiona Carragher Biochemical Sciences, GSTS Pathology St Thomas Hospital, London An update. Overview of metabolism Clinical presentation and outcome Diagnostic
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children
 National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
National Metabolic Biochemistry Network Guidelines for the investigation of hypoglycaemia in infants and children Aim To provide guidance on the biochemical investigation of hypoglycaemia in infants and
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital
 e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
e-learning Fatty Acid Oxidation Defects Camilla Reed and Dr Simon Olpin Sheffield Children s Hospital Fatty Acids Fatty acids are a major source of energy and body fat is an energy dense material. They
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis)
 Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
Newborn Screen & Development Facts about the genetic diseases new since March 2006 (Excluding Cystic Fibrosis) 1) Argininosuccinic acidemia (ASA) a) Incidence: ~1 in 70,000 b) Deficiency in an enzyme of
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA
 NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
NEONATAL HYPOGLYCEMIA HEATHER MCKNIGHT-MENCI, MSN, CRNP CHILDREN S HOSPITAL OF PHILADELPHIA WHAT IS NEONATAL HYPOGLYCEMIA? Glucose concentration low enough to cause signs and symptoms of impaired brain
Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when
 CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
CPT2 Deficiency Carnitine palmitoyl transferase 2 deficiency (CPT2) is a rare inherited disorder that occurs when the last step in the entry of fats into sac-like bodies called mitochondria is blocked.
Fatty acid oxidation. Naomi Rankin
 Fatty acid oxidation Naomi Rankin Fatty acid oxidation Provides energy to muscles from lipid stores, spares glucose for the brain Lipolysis of triglycerides results in FFA, mainly C16 and C18 FA oxidation
Fatty acid oxidation Naomi Rankin Fatty acid oxidation Provides energy to muscles from lipid stores, spares glucose for the brain Lipolysis of triglycerides results in FFA, mainly C16 and C18 FA oxidation
ANATOMY OF A METABOLIC CRISIS: FAOD-style. Mark S. Korson, MD Tufts Medical Center Boston, MA
 ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
ANATOMY OF A METABOLIC CRISIS: FAOD-style Mark S. Korson, MD Tufts Medical Center Boston, MA NORMAL PHYSIOLOGY Anabolic Eating well Calories eaten > body s needs BRAIN uses GLUCOSE MUSCLE uses GLUCOSE
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Mitochondrial Fatty Acid Oxidation Deficiencies Prof. Niels Gregersen
 Mitochondrial Fatty Acid Oxidation Deficiencies Research Unit for Molecular Medicine Clinical Institute Aarhus University Hospital and Faculty of Health Sciences Aarhus University, Aarhus, Denmark 1 Menu
Mitochondrial Fatty Acid Oxidation Deficiencies Research Unit for Molecular Medicine Clinical Institute Aarhus University Hospital and Faculty of Health Sciences Aarhus University, Aarhus, Denmark 1 Menu
Fatty Acid Beta-Oxidation Disorders: A Brief Review
 Mini Review Received: July 12, 2015 Accepted: November 12, 2015 Published online: March 11, 2016 Fatty Acid Beta-Oxidation Disorders: A Brief Review Vijay A. Vishwanath Division of Pediatric Neurology,
Mini Review Received: July 12, 2015 Accepted: November 12, 2015 Published online: March 11, 2016 Fatty Acid Beta-Oxidation Disorders: A Brief Review Vijay A. Vishwanath Division of Pediatric Neurology,
Not Your Typical Case of Ketotic Hypoglycemia
 Not Your Typical Case of Ketotic Hypoglycemia Linda Steinkrauss, RN, MSN, CPNP Objectives By the end of this session, attendees should be able to: 1. Discuss the difference between idiopathic ketotic hypoglycemia
Not Your Typical Case of Ketotic Hypoglycemia Linda Steinkrauss, RN, MSN, CPNP Objectives By the end of this session, attendees should be able to: 1. Discuss the difference between idiopathic ketotic hypoglycemia
INBORN ERRORS OF METABOLISM (IEM) IAP UG Teaching slides
 INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
INBORN ERRORS OF METABOLISM (IEM) 1 OBJECTIVES What are IEMs? Categories When to suspect? History and clinical pointers Metabolic presentation Differential diagnosis Emergency and long term management
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Inborn Errors of Metabolism. Metabolic Pathway. Digestion and Fasting. How is Expanded Newborn Screening Different? MS/MS. The body is a factory.
 Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
Inborn Errors of Metabolism The body is a factory. Inborn errors of metabolism are rare genetic disorders in which the body cannot properly turn food into energy. The disorders are usually caused by defects
VLCAD At a Glance. Before VLCAD was included on the newborn screening test, three types of VLCAD were recognized by the severity of the condition:
 VLCAD At a Glance VLCAD is one of several *Fatty Acid Oxidation Disorders (FAOD) in which there is an inability to break down certain fats, caused by an enzyme deficiency. This results in a decreased ability
VLCAD At a Glance VLCAD is one of several *Fatty Acid Oxidation Disorders (FAOD) in which there is an inability to break down certain fats, caused by an enzyme deficiency. This results in a decreased ability
LILY FOUNDATION. An Introduction to Ketogenic Diets. Susan Wood. Matthew s Friends. Registered Dietitian Adults & Paediatrics
 LILY FOUNDATION An Introduction to Ketogenic Diets Susan Wood Registered Dietitian Adults & Paediatrics Matthew s Friends What is a ketogenic diet? A MEDICAL treatment. Mimics fasting metabolism Alters
LILY FOUNDATION An Introduction to Ketogenic Diets Susan Wood Registered Dietitian Adults & Paediatrics Matthew s Friends What is a ketogenic diet? A MEDICAL treatment. Mimics fasting metabolism Alters
Manipulation of the Nutrient Sensors (AMPK/TOR) with Anaplerotic Diet Therapy (Triheptanoin) An Alternative to Diet Restriction
 Manipulation of the Nutrient Sensors (AMPK/TOR) with Anaplerotic Diet Therapy (Triheptanoin) An Alternative to Diet Restriction CharlesR.Roe,MD Institute of Metabolic Disease Baylor University Medical
Manipulation of the Nutrient Sensors (AMPK/TOR) with Anaplerotic Diet Therapy (Triheptanoin) An Alternative to Diet Restriction CharlesR.Roe,MD Institute of Metabolic Disease Baylor University Medical
Newborn Screening in Manitoba. Information for Health Care Providers
 Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Newborn Screening in Manitoba Information for Health Care Providers Newborn screening: a healthy start leads to a healthier life Health care professionals have provided newborn screening for phenylketonuria
Introduction to Organic Acidemias. Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.
 Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
Introduction to Organic Acidemias Hilary Vernon, MD PhD Assistant Professor of Genetic Medicine Johns Hopkins University 7.25.2014 A Brief Historical Overview Garrod, Archibald E. 1902. The Incidence of
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES
 3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
3 HYDROXY 3 METHYLGLUTARYL CoA (3 HMG CoA) LYASE DEFICIENCY RECOMMENDATIONS ON EMERGENCY MANAGEMENT OF METABOLIC DISEASES Patient s name: Date of birth: Please read carefully. Meticulous and prompt treatment
Neonatal Hypoglycaemia
 Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
Neonatal Hypoglycaemia Dr Shubha Srinivasan Paediatric Endocrinologist The Children s Hospital at Westmead Hypoglycaemia and the Brain CSF glucose is 2/3 that of plasma Intracerebral glucose 1/3 that of
The laboratory investigation of lactic acidaemia. J Bonham/T Laing
 The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
The laboratory investigation of lactic acidaemia J Bonham/T Laing Reference range Typical ranges for blood lactate are: Newborn 0.3-2.2 mmol/l Nielsen J et al1 1994 1-12mo 0.9-1.8 mmol/l Bonnefont et al
Hyperglycaemia. Clinical presentation. Definition of hyperglycaemia. Approach to the problem
 Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
Hyperglycaemia 1 Clinical presentation Hyperglycaemia is usually picked up incidentally on routine blood glucose assessment or in response to finding glycosuria. It may be noted as part of the workup of
The spectrum and outcome of the. neonates with inborn errors of. metabolism at a tertiary care hospital
 The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
The spectrum and outcome of the neonates with inborn errors of metabolism at a tertiary care hospital Dr. Sevim Ünal Neonatology Division, Ankara Children s Hematology Oncology Research Hospital, Ankara,
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Patient Demographics 5/12/2016
 Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
Beyond the Naked Eye: A Case Presentation on a Rare Form of Congenital Hyperinsulinism (HI) Pediatric Endocrine Nursing Society May 14, 2016 Enyo Dzata, MSN, CRNP Congenital Hyperinsulinism Center Division
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review -
 Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Guideline for the diagnosis and management of isovaleryl-coa-dehydrogenase deficiency (isovaleric acidemia) - a systematic review - Guideline development group International interdisciplinary guideline
Overview. o Limitations o Normal regulation of blood glucose o Definition o Symptoms o Clinical forms o Pathophysiology o Treatment.
 Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Pål R. Njølstad MD PhD KG Jebsen Center for Diabetes Research University of Bergen, Norway Depertment of Pediatrics Haukeland University Hospital Broad Institute of Harvard & MIT Cambridge, MA, USA Hypoglycemia
Inborn Errors of Metabolism (IEM)
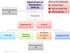 Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Clinical Presentation Inborn Errors of Metabolism (IEM) Click on the following: - Clinical Pearl - link to movie clip - link to picture Investigations Blood Work Urine No Acidosis NH 4 + Metabolic Acidosis
Urea Cycle Defects. Dr Mick Henderson. Biochemical Genetics Leeds Teaching Hospitals Trust. MetBioNet IEM Introductory Training
 Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
Urea Cycle Defects Dr Mick Henderson Biochemical Genetics Leeds Teaching Hospitals Trust The Urea Cycle The urea cycle enables toxic ammonia molecules to be converted to the readily excreted and non toxic
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE
 THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
THE ED APPROACH OF THE CHILD WITH SUSPECTED METABOLIC DISEASE Dr. Nadeem Qureshi M.D, FAAP, FCCM Associate Professor Pediatrics School of Medicine. St Louis University Attending Physician Pediatric Emergency
Module : Clinical correlates of disorders of metabolism Block 3, Week 2
 Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
Module : Clinical correlates of disorders of metabolism Block 3, Week 2 Department of Paediatrics and Child Health University of Pretoria Tutor : Prof DF Wittenberg : dwittenb@medic.up.ac.za Aim of this
BRIEF REPORT. Provocative Tests
 Brief Report FASTING HYPOKETOTIC COMA IN A CHILD WITH DEFICIENCY OF MITOCHONDRIAL 3- METHYLGLUTARYL-COA SYNTHASE GEOFFREY N. THOMPSON, M.D., PH.D., BETTY Y.L. HSU, PH.D., JAMES J. PITT, B.SC., EILEEN TREACY,
Brief Report FASTING HYPOKETOTIC COMA IN A CHILD WITH DEFICIENCY OF MITOCHONDRIAL 3- METHYLGLUTARYL-COA SYNTHASE GEOFFREY N. THOMPSON, M.D., PH.D., BETTY Y.L. HSU, PH.D., JAMES J. PITT, B.SC., EILEEN TREACY,
Muscle Metabolism. Dr. Nabil Bashir
 Muscle Metabolism Dr. Nabil Bashir Learning objectives Understand how skeletal muscles derive energy at rest, moderate exercise, and strong exercise. Recognize the difference between aerobic and anaerobic
Muscle Metabolism Dr. Nabil Bashir Learning objectives Understand how skeletal muscles derive energy at rest, moderate exercise, and strong exercise. Recognize the difference between aerobic and anaerobic
Neonatal Hypoglycemia
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Neonatal Hypoglycemia. These podcasts are designed to give medical students an overview of key topics in pediatrics.
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA
 UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
UK NATIONAL METABOLIC BIOCHEMISTRY NETWORK GUIDELINES FOR THE INVESTIGATION OF HYPERAMMONAEMIA Hyperammonaemia results from defective catabolism of amino acids to urea. Recognition and treatment of hyperammonaemia,
Roles of Lipids. principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular
 Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Roles of Lipids principal form of stored energy major constituents of cell membranes vitamins messengers intra and extracellular = Oxidation of fatty acids Central energy-yielding pathway in animals. O
Metabolic Disorders. Chapter Thomson - Wadsworth
 Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Metabolic Disorders Chapter 28 1 Metabolic Disorders Inborn errors of metabolism group of diseases that affect a wide variety of metabolic processes; defective processing or transport of amino acids, fatty
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center
 Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
Spectrum of Inborn Errors of Metabolism in Jordan: Five Years Experience at King Hussein Medical Center Kefah Al-Qa qa MD*, Wajdi Amayreh MD*, Ali Al-Hawamdeh MD* ABSTRACT Objective: To describe the different
23.1 Lipid Metabolism in Animals. Chapter 23. Micelles Lipid Metabolism in. Animals. Overview of Digestion Lipid Metabolism in
 Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition
 Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Suspected Metabolic Disease in the Newborn Period Acute Management "What do I do?" Barbara Marriage, PhD RD Abbott Nutrition Introduction Review clinical findings that may be suspicious of a metabolic
Part III => METABOLISM and ENERGY. 3.4 Lipid Catabolism 3.4a Fatty Acid Degradation 3.4b Ketone Bodies
 Part III => METABOLISM and ENERGY 3.4 Lipid Catabolism 3.4a Fatty Acid Degradation 3.4b Ketone Bodies Section 3.4a: Fatty Acid Degradation Synopsis 3.4a - Triglycerides (or fats) in the diet or adipose
Part III => METABOLISM and ENERGY 3.4 Lipid Catabolism 3.4a Fatty Acid Degradation 3.4b Ketone Bodies Section 3.4a: Fatty Acid Degradation Synopsis 3.4a - Triglycerides (or fats) in the diet or adipose
Presentation and investigation of mitochondrial disease in children
 Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Presentation and investigation of mitochondrial disease in children Andrew Morris Willink Unit, Manchester Mitochondrial function Carbohydrate Fat Respiratory chain Energy Mitochondria are the product
Paediatric Hypoglycaemia and the Laboratory. AACB Webinar, 8 th April 2015 Tina Yen
 Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
Paediatric Hypoglycaemia and the Laboratory AACB Webinar, 8 th April 2015 Tina Yen Synopsis Definition and classification Newborn and Neonatal Hypoglycaemia Transient Persistant Hypoglycaemia in infants
KETOGENIC DIET ISMAIL HALAHLEH, MSC. نقیب اخصاي یي التغذیة الفلسطینیین
 KETOGENIC DIET ISMAIL HALAHLEH, MSC. نقیب اخصاي یي التغذیة الفلسطینیین INTRODUCTION WHAT IS KETOGENIC DIET???? KETOGENIC DIET The ketogenic diet (KD) is a diet that is high in fat, low in carbohydrate,
KETOGENIC DIET ISMAIL HALAHLEH, MSC. نقیب اخصاي یي التغذیة الفلسطینیین INTRODUCTION WHAT IS KETOGENIC DIET???? KETOGENIC DIET The ketogenic diet (KD) is a diet that is high in fat, low in carbohydrate,
Positive Newborn Screens: What do you do next?
 Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Positive Newborn Screens: What do you do next? James B. Gibson, MD, Ph.D. Biochemical Geneticist at Specially for Children Clinical Associate Professor of Pediatrics UTHSCSA Carla R. Scott, MD Pediatric
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015
 Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
Routine Newborn Screening, Testing the Newborn Inherited Metabolic Disorders Update August 2015 Metabolic birth defects can cause physical problems, mental retardation and, in some cases, death. It is
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری
 بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
بنام خدا هیپوگلیسمی درنوزادان و گاالکتوزمی دکتر انتظاری Serum glucose< 35 mg/dl 1-3 hr of life < 40 mg/dl 3-24 hr < 45 mg/dl after 24 hr 10% NL newborns can t maintain BS>30 if delayed feeding >3-6 hrs
How MS/MS Revolutionized Newborn Screening
 How MS/MS Revolutionized Newborn Screening David S Millington, PhD Medical Research Professor of Pediatrics Director, Biochemical Genetics Laboratory Duke University Medical Center NEWBORN SCREENING IN
How MS/MS Revolutionized Newborn Screening David S Millington, PhD Medical Research Professor of Pediatrics Director, Biochemical Genetics Laboratory Duke University Medical Center NEWBORN SCREENING IN
Basal Ganglia Involvement in Mitochondrial Acetoacetyl-CoA Thiolase deficiency (T2).
 Basal Ganglia Involvement in Mitochondrial Acetoacetyl-CoA Thiolase deficiency (T2). Stéphanie Paquay Robert Debré Hospital Reference Center For Metabolic Diseases Paris, France Mitochondrial Acetoacetyl-CoA
Basal Ganglia Involvement in Mitochondrial Acetoacetyl-CoA Thiolase deficiency (T2). Stéphanie Paquay Robert Debré Hospital Reference Center For Metabolic Diseases Paris, France Mitochondrial Acetoacetyl-CoA
My Experiences and Understanding of VLCAD Deficiency and its Treatment Charles R. Roe, MD June 26, 2011 (Now retired)
 My Experiences and Understanding of VLCAD Deficiency and its Treatment Charles R. Roe, MD June 26, 2011 (Now retired) This disorder is characterized by the deficiency of the VLCAD enzyme that is required
My Experiences and Understanding of VLCAD Deficiency and its Treatment Charles R. Roe, MD June 26, 2011 (Now retired) This disorder is characterized by the deficiency of the VLCAD enzyme that is required
Disorders of Mitochondrial Fatty Acid Oxidation and Ketone Body Handling
 14 Disorders of Mitochondrial Fatty Acid Oxidation and Ketone Body Handling Marinus Duran 14.1 Introduction Long-chain (C 16 C 20 ) fatty acids, which are stored in adipose tissue, can be b-oxidised for
14 Disorders of Mitochondrial Fatty Acid Oxidation and Ketone Body Handling Marinus Duran 14.1 Introduction Long-chain (C 16 C 20 ) fatty acids, which are stored in adipose tissue, can be b-oxidised for
Controversies in Neonatal Hypoglycemia PAC / LAC CONFERENCE, JUNE 1 ST 2017
 Controversies in Neonatal Hypoglycemia PRIYA JEGATHEESAN, MD PAC / LAC CONFERENCE, JUNE 1 ST 2017 Disclosure I have no conflicts of interest to disclose Objectives Review Recommendations from different
Controversies in Neonatal Hypoglycemia PRIYA JEGATHEESAN, MD PAC / LAC CONFERENCE, JUNE 1 ST 2017 Disclosure I have no conflicts of interest to disclose Objectives Review Recommendations from different
ACUTE & CHRONIC ETHANOL EFFECTS An Overview
 ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
ACUTE & CHRONIC ETHANOL EFFECTS An Overview University of Papua New Guinea School of Medicine & Health Sciences, Division of Basic Medical Sciences Clinical Biochemistry: PBL Seminar MBBS Yr 4 VJ Temple
3-Hydroxy-3-methylglutaric Aciduria: Response to Carnitine Therapy and Fat and Leucine Restriction
 J. Inher. Metab. Dis. 10 (1987) 142-146 3-Hydroxy-3-methylglutaric Aciduria: Response to Carnitine Therapy and Fat and Leucine Restriction M. DASOUKI 1, D. BUCHANAN 1, N. MERCER 2, K. M. GIBSON 3 and J.
J. Inher. Metab. Dis. 10 (1987) 142-146 3-Hydroxy-3-methylglutaric Aciduria: Response to Carnitine Therapy and Fat and Leucine Restriction M. DASOUKI 1, D. BUCHANAN 1, N. MERCER 2, K. M. GIBSON 3 and J.
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology
 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES Discipline of Biochemistry and Molecular Biology 1 PBL SEMINAR ACUTE & CHRONIC ETHANOL EFFECTS An Overview Sites
OVERVIEW M ET AB OL IS M OF FR EE FA TT Y AC ID S
 LIPOLYSIS LIPOLYSIS OVERVIEW CATABOLISM OF FREE FATTY ACIDS Nonesterified fatty acids Source:- (a) breakdown of TAG in adipose tissue (b) action of Lipoprotein lipase on plasma TAG Combined with Albumin
LIPOLYSIS LIPOLYSIS OVERVIEW CATABOLISM OF FREE FATTY ACIDS Nonesterified fatty acids Source:- (a) breakdown of TAG in adipose tissue (b) action of Lipoprotein lipase on plasma TAG Combined with Albumin
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona
 BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
BIOTIN (BIOTINIDASE) DEFICIENCY Marc E. Tischler, PhD; University of Arizona BIOTIN (BIOTINIDASE) DEFICIENCY biotin in the body is recycled by its removal from carboxylase enzymes to which it is attached
number Done by Corrected by Doctor Faisal Al-Khatib
 number 22 Done by Baraa Ayed Corrected by Yaseen Fatayer Doctor Faisal Al-Khatib 1 P a g e Today we are going to cover these concepts: Oxidation of odd number fatty acids Oxidation of very long fatty acids
number 22 Done by Baraa Ayed Corrected by Yaseen Fatayer Doctor Faisal Al-Khatib 1 P a g e Today we are going to cover these concepts: Oxidation of odd number fatty acids Oxidation of very long fatty acids
Using the Organic Acids Test Part 3 Dr. Jeff Moss
 Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part III Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Using organic acids to resolve chief complaints and improve quality of life in chronically ill patients Part III Jeffrey Moss, DDS, CNS, DACBN jeffmoss@mossnutrition.com 413-530-08580858 (cell) 1 Summer
Lipid metabolism. Degradation and biosynthesis of fatty acids Ketone bodies
 Lipid metabolism Degradation and biosynthesis of fatty acids Ketone bodies Fatty acids (FA) primary fuel molecules in the fat category main use is for long-term energy storage high level of energy storage:
Lipid metabolism Degradation and biosynthesis of fatty acids Ketone bodies Fatty acids (FA) primary fuel molecules in the fat category main use is for long-term energy storage high level of energy storage:
Alvaro Serrano Russi MD University of Iowa Hospitals and Clinics
 Retrospective Analysis of the Region 4 Post Analytical Tool and Confirmatory Testing for Long Chain Fatty Acid Oxidation Disorders Screened in the State of Iowa Alvaro Serrano Russi MD University of Iowa
Retrospective Analysis of the Region 4 Post Analytical Tool and Confirmatory Testing for Long Chain Fatty Acid Oxidation Disorders Screened in the State of Iowa Alvaro Serrano Russi MD University of Iowa
Metabolic Changes in ASD. Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius
 Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Metabolic Changes in ASD Norma J. Arciniegas, MD Simón E. Carlo, MD Instituto Filius 12 patients 3 Autism: Ages 3/3/3.7 3 PDD: Ages 3/3/6 3 Asperger: Ages 6/7/15.1 3 Speech delay and Sensory Problems (SHL):
Staff at the Nottingham Children s Hospital. Guidelines process; paediatric endocrinology team
 Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
Hypoglycaemia Title of Guideline Contact Name and Job Title (author) Hypoglycaemia in infants and children: aetiology, investigation and treatment Dr. Hoong-Wei Gan ST6 Paediatric Endocrinology & Diabetes
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting
 Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
Work-Up and Initial Management of Common Metabolic Emergencies in the Inpatient Setting Kristin Lindstrom, MD Division of Genetics and Metabolism Phoenix Children s Hospital AzAAP Pediatrics in the Red
The breakdown of fats to provide energy occurs in segregated membrane-bound compartments
 CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
CPT1a deficiency The breakdown of fats to provide energy occurs in segregated membrane-bound compartments of the cell known as mitochondria. Carnitine palmitoyltransferase Ia (CPT1a) is a protein that
SCAD and GA-II: Truths and Confusions
 SCAD and GA-II: Truths and Confusions Bill Rhead* Medical College of Wisconsin *MD, PhD GA-II Severe GA-II is as bad as: SCAD + MCAD + COMBINED! VLCAD + IVA + GA-I Severe GA-II is always fatal Mild
SCAD and GA-II: Truths and Confusions Bill Rhead* Medical College of Wisconsin *MD, PhD GA-II Severe GA-II is as bad as: SCAD + MCAD + COMBINED! VLCAD + IVA + GA-I Severe GA-II is always fatal Mild
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine
 Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Lynne A. Wolfe, MS, ACNP, PNP, BC Department of Genetics Yale School of Medicine Harvey Levy, MD Mark Korson, MD Piero Rinaldo, MD, PhD Larry Sweetman, PhD K. Michael Gibson, PhD Charlie Roe, MD Jerry
Hypoglycaemia of the neonate. Dr. L.G. Lloyd Dept. Paediatrics
 Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Hypoglycaemia of the neonate Dr. L.G. Lloyd Dept. Paediatrics Why is glucose important? It provides 60-70% of energy needs Utilization obligatory by red blood cells, brain and kidney as major source of
Fatty acid oxidation. doc. Ing. Zenóbia Chavková, CSc.
 Fatty acid oxidation doc. Ing. Zenóbia Chavková, CSc. Physiological functions of fatty acids 1. Structural components of cell membranes (phospholipids and sphingolipids) 2. Energy storage (triacylglycerols)
Fatty acid oxidation doc. Ing. Zenóbia Chavková, CSc. Physiological functions of fatty acids 1. Structural components of cell membranes (phospholipids and sphingolipids) 2. Energy storage (triacylglycerols)
TITLE: NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA. Eilish O Connell, Clinical Education Facilitator, NCIMD
 NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
NO. OF PAGES: Page 1 of 17 SUPERCEDES: N/A NURSING GUIDELINES FOR THE MANAGEMENT OF CHILDREN WITH METHYLMALONIC ACIDURIA NAME/ Eilish O Connell, Clinical Education Facilitator, NCIMD SIGNATURE: DATE: NAME/
Metabolic Muscle Disease
 Metabolic Muscle Disease Dr. Simon Olpin Consultant Clinical Scientist in Inherited Metabolic Disease Department of Clinical Chemistry Sheffield Children s Hospital Clinical Diagnosis of Muscle Disease
Metabolic Muscle Disease Dr. Simon Olpin Consultant Clinical Scientist in Inherited Metabolic Disease Department of Clinical Chemistry Sheffield Children s Hospital Clinical Diagnosis of Muscle Disease
Isovaleric Acidemia: Quick reference guide
 Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
Isovaleric Acidemia: Quick reference guide Introduction Isovaleric acidemia (IVA) is an inborn error of the leucine pathway caused by defects of the isovaleryl-oadehydrogenase (IV). The clinical presentation
4/23/2015. Linda Steinkrauss, MSN, PNP. No conflicts of interest
 Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Linda Steinkrauss, MSN, PNP No conflicts of interest 1 5 year old African-American female presented to our Endocrinology Clinic with hypoglycemia Abnormal chromosomes Duplication of 11q13.5-11p14.1 affecting
Tala Saleh. Razi Kittaneh ... Nayef Karadsheh
 Tala Saleh Razi Kittaneh... Nayef Karadsheh β-oxidation of Fatty Acids The oxidation of fatty acids occurs in 3 steps: Step 1: Activation of the Fatty acid FA + HS-CoA + ATP FA-CoA + AMP + PPi - The fatty
Tala Saleh Razi Kittaneh... Nayef Karadsheh β-oxidation of Fatty Acids The oxidation of fatty acids occurs in 3 steps: Step 1: Activation of the Fatty acid FA + HS-CoA + ATP FA-CoA + AMP + PPi - The fatty
Inborn Errors of Metabolism in the Emergency Department. Will Davies June 2014
 Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Inborn Errors of Metabolism in the Emergency Department Will Davies June 2014 Inborn Errors of Metabolism in the Emergency Department Overview Although individually rare, altogether they are 1:1000-2500
Most common is the congenital adrenogenital syndrome (AGS) or congenital adrenal hyperplasia (CAH) due to 21-hydroxylase deficiency.
 Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Newborn Screening Examination parameters: TSH-neonatal (hypothyreosis), 17-OH progesterone (AGS), galactose (galactosemia), galactose-uridyl transferase (galacto semia), biotinidase (biotinidase ), phenylalanine
Biol 219 Lec 7 Fall 2016
 Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Cellular Respiration: Harvesting Energy to form ATP Cellular Respiration and Metabolism Glucose ATP Pyruvate Lactate Acetyl CoA NAD + Introducing The Players primary substrate for cellular respiration
Title: Assessing Recommendations Related To Timeliness of Newborn Screening
 Title: Assessing Recommendations Related To Timeliness of Newborn Screening Purpose: In January 2014, the Secretary s Discretionary Advisory Committee on Heritable Diseases on Newborns and Children (Committee)
Title: Assessing Recommendations Related To Timeliness of Newborn Screening Purpose: In January 2014, the Secretary s Discretionary Advisory Committee on Heritable Diseases on Newborns and Children (Committee)
Glycogen Storage Disease Type III also known as Cori or Forbe s Disease/Debrancher Enzyme Deficiency
 Glycogen Storage Disease Type III also known as Cori or Forbe s Disease/Debrancher Enzyme Deficiency What is GSDIII? Glycogen Storage Disease type 3 is an inherited condition caused by a defect in a gene
Glycogen Storage Disease Type III also known as Cori or Forbe s Disease/Debrancher Enzyme Deficiency What is GSDIII? Glycogen Storage Disease type 3 is an inherited condition caused by a defect in a gene
Biochemistry: A Short Course
 Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Tymoczko Berg Stryer Biochemistry: A Short Course Second Edition CHAPTER 27 Fatty Acid Degradation Dietary Lipid (Triacylglycerol) Metabolism - In the small intestine, fat particles are coated with bile
Metabolic diseases of the liver
 Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Metabolic diseases of the liver Central role in metabolism Causes and mechanisms of dysfunction Clinical patterns of metabolic disease Clinical approach to problem-solving Specific disorders Liver s central
Lipid Metabolism. Remember fats?? Triacylglycerols - major form of energy storage in animals
 Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Remember fats?? Triacylglycerols - major form of energy storage in animals Your energy reserves: ~0.5% carbs (glycogen + glucose) ~15% protein (muscle, last resort) ~85% fat Why use fat for energy? 1 gram
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism
 Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Newborn Screening & Methods for Diagnosing Inborn Errors of Metabolism Patricia Jones, PhD DABCC FACB UT Southwestern Medical Center Children s Medical Center Dallas, Texas Learning Objectives Justify
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD
 Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Genética e Hígado: Cómo contribuye la genética en el algoritmo diagnóstico de la enfermedad hepática pediátrica? Nicholas Ah Mew, MD April 24, 2017 SAP 2017 Buenos Aires Genetic disorders are rare why
Post mortem investigation of Inherited Metabolic Disease - the last opportunity for a diagnosis -
 Post mortem investigation of Inherited Metabolic Disease - the last opportunity for a diagnosis - Dr Simon Olpin Lead Clinical Scientist in Inherited Metabolic Disease Sheffield Children s Hospital SIDS/SUDI
Post mortem investigation of Inherited Metabolic Disease - the last opportunity for a diagnosis - Dr Simon Olpin Lead Clinical Scientist in Inherited Metabolic Disease Sheffield Children s Hospital SIDS/SUDI
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS
 PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
PROTEIN METABOLISM: SPECIFIC WAYS OF AMINO ACIDS CATABOLISM AND SYNTHESIS SPECIFIC WAYS OF AMINO ACID CATABOLISM After removing of amino group the carbon skeletons of amino acids are transformed into metabolic
Chapter 24 Lecture Outline
 Chapter 24 Lecture Outline Carbohydrate Lipid and Protein! Metabolism! In the catabolism of carbohydrates, glycolysis converts glucose into pyruvate, which is then metabolized into acetyl CoA. Prepared
Chapter 24 Lecture Outline Carbohydrate Lipid and Protein! Metabolism! In the catabolism of carbohydrates, glycolysis converts glucose into pyruvate, which is then metabolized into acetyl CoA. Prepared
Introduction. Overview
 Carnitine palmitoyltransferase 1A deficiency Michael J Bennett PhD FRCPath ( Dr. Bennett of The Children's Hospital of Philadelphia and the University of Pennsylvania has no relevant financial relationships
Carnitine palmitoyltransferase 1A deficiency Michael J Bennett PhD FRCPath ( Dr. Bennett of The Children's Hospital of Philadelphia and the University of Pennsylvania has no relevant financial relationships
CARE OF THE NEWBORN HYPOGLYCAEMIA
 CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
CARE OF THE NEWBORN HYPOGLYCAEMIA Background Definition A true blood glucose of less than 2.6 mmol/l venous sample. Neonatal hypoglycaemia is commonly defined as a true blood glucose of less than 2.6 mmol/l
Fatty Acid Oxidation Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial, ethical, legal, and social
Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia
 Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
Neonatal Nursing Education Brief: Evidence-Based Update: Using Glucose Gel to Treat Neonatal Hypoglycemia http://www.seattlechildrens.org/healthcare-professionals/education/continuing-medicalnursing-education/neonatal-nursing-education-briefs/
The Arctic Variant of CPT-1A
 The Arctic Variant of CPT-1A Matthew Hirschfeld, MD/PhD Department of Pediatric Hospital Medicine Alaska Native Medical Center Anchorage, AK Background CPT-1 = carnitine palmitoyltransferase type 1 Expressed
The Arctic Variant of CPT-1A Matthew Hirschfeld, MD/PhD Department of Pediatric Hospital Medicine Alaska Native Medical Center Anchorage, AK Background CPT-1 = carnitine palmitoyltransferase type 1 Expressed
Robert Barski. Biochemical Genetics St James s University Hospital, Leeds. MetBioNet IEM Introductory Training
 Robert Barski Biochemical Genetics St James s University Hospital, Leeds Lactate is produced as the fate of anaerobic metabolism of pyruvate. It is an important intermediary metabolite especially with
Robert Barski Biochemical Genetics St James s University Hospital, Leeds Lactate is produced as the fate of anaerobic metabolism of pyruvate. It is an important intermediary metabolite especially with
MetBioNet Best Practice Guidelines. Investigation of an inherited metabolic cause of cardiomyopathy
 Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Introduction MetBioNet Best Practice Guidelines Investigation of an inherited metabolic cause of Inborn errors of metabolism (IEM) account for at least 5% of cases of. In some disorders, is the major cause
Medium-chain acyl-coa dehydrogenase deficiency
 Medium-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Medium-chain acyl-coa dehydrogenase MCAD
Medium-chain acyl-coa dehydrogenase deficiency Introductory information Written by: V. Prietsch & P. Burgard Reviewed & Revised for North America by: S. van Calcar Medium-chain acyl-coa dehydrogenase MCAD
Fatty Acid Oxidation Disorders Organic Acid Disorders
 Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial,
Genetic Fact Sheets for Parents Fatty Acid Oxidation Disorders Organic Acid Disorders Screening, Technology, and Research in Genetics is a multi-state project to improve information about the financial,
DIAGNOSIS OF FATTY ACID OXIDATION DISORDERS BY MASS SPECTROMETRY
 DIAGNOSIS OF FATTY ACID OXIDATION DISORDERS BY MASS SPECTROMETRY Eric Law Chemical Pathology, PWH 15 January 2010 Outline of talk Basic of mitochondrial fatty acid oxidation (FAO) Laboratory investigations
DIAGNOSIS OF FATTY ACID OXIDATION DISORDERS BY MASS SPECTROMETRY Eric Law Chemical Pathology, PWH 15 January 2010 Outline of talk Basic of mitochondrial fatty acid oxidation (FAO) Laboratory investigations
Genomics & Modern Health Care Caring for the Special Children & Adults of Isolated Populations. Propionic Acidemia
 Genomics & Modern Health Care Caring for the Special Children & Adults of Isolated Populations Propionic Acidemia D. Holmes Morton MD Pediatrician, Clinic for Special Children Strasburg, Pennsylvania 17579
Genomics & Modern Health Care Caring for the Special Children & Adults of Isolated Populations Propionic Acidemia D. Holmes Morton MD Pediatrician, Clinic for Special Children Strasburg, Pennsylvania 17579
