Laser ablation under real-time magnetic. Robot-Assisted Stereotactic Laser Ablation in Medically Intractable Epilepsy: Operative Technique
|
|
|
- Amberly Waters
- 6 years ago
- Views:
Transcription
1 Operative Technique Robot-Assisted Stereotactic Laser Ablation in Medically Intractable Epilepsy: Operative Technique Jorge Gonzalez-Martinez, MD, PhD* Sumeet Vadera, MD* Jeffrey Mullin, MD, MBA* Rei Enatsu, MD* Andreas V. Alexopoulos, MD, MPH* Ravish Patwardhan, MD William Bingaman, MD* Imad Najm, MD* *Epilepsy Center, Neuroscience Institute Cleveland Clinic, Cleveland, Ohio; Visualase Inc, Houston, Texas Correspondence: Jorge Gonzalez-Martinez, MD, PhD, 9500 Euclid Ave, S6, Cleveland, OH Received, August 13, Accepted, January 2, Published Online, January 19, Copyright 2014 by the Congress of Neurological Surgeons. BACKGROUND: Stereotactic laser ablation offers an advantage over open surgical procedures for treatment of epileptic foci, tumors, and other brain pathology. Robotassisted stereotactic laser ablation could offer an accurate, efficient, minimally invasive, and safe method for placement of an ablation catheter into the target. OBJECTIVE: To determine the feasibility of placement of a stereotactic laser ablation catheter into a brain lesion with the use of robotic assistance, via a safe, accurate, efficient, and minimally invasive manner. METHODS: A laser ablation catheter (Visualase, Inc) was placed by using robotic guidance (ROSA, Medtech Surgical, Inc) under general anesthesia into a localized epileptogenic periventricular heterotopic lesion in a 19-year-old woman with 10-year refractory focal seizure history. The laser applicator (1.65 mm diameter) position was confirmed by using magnetic resonance imaging (MRI). Ablation using the Visualase system was performed under multiplanar imaging with real-time thermal imaging and treatment estimates in each plane. A postablation MRI sequence (T1 postgadolinium contrast injection) was used to immediately confirm the ablation. RESULTS: MRI showed accurate skin entry point and trajectory, with the applicator advanced to the lesion s distal boundary. Ablation was accomplished in less than 3 minutes of heating. The overall procedure, from time of skin incision to end of last ablation, was approximately 90 minutes. After confirmation of proper lesioning by using a T1 contrast-enhanced MRI, the applicator was removed, and the incision was closed using a single stitch. No hemorrhage or other untoward complication was visualized. The patient awoke without any complication, was observed overnight after admitting to a regular floor bed, and was discharged to home the following day. CONCLUSION: This technique, using a combination of Visualase laser ablation, ROSA robot, and intraoperative MRI, facilitated a safe, efficacious, efficient, and minimally invasive approach that could be used for placement of 1 or multiple electrodes in the future. KEY WORDS: Epilepsy, Heterotopia, Lasers, Robotics, Stereotactic techniques, Treatment Operative Neurosurgery 10: , 2014 DOI: /NEU ABBREVIATIONS: EEG, electroencephalography; SEEG, stereoelectroencephalography Laser ablation under real-time magnetic resonance imaging (MRI) guidance for brain pathology is being increasingly used by neurosurgeons. Since the initial cases in France in 2006 targeting metastatic tumors, and subsequent procedures in the United States in 2008 targeting both primary and metastatic brain tumors, surgeons have ablated epileptogenic lesions and radiation necrosis. 1-5 Epileptogenic lesions, including tubers (in tuberous sclerosis), mesial temporal sclerosis (via selective laser amygdalohippocampectomy), as well as focal cortical dysplasias and hamartoma, have been successfully treated. 3,6 The minimally invasive opening (3.2 mm), small diameter of the laser applicator (1.65 mm), and ease of placement with subsequent short ablation time (usually less than 5 minutes) and MRI scanning time (usually less than 90 minutes) have allowed procedures to be performed in a more efficient and safer manner in OPERATIVE NEUROSURGERY VOLUME 10 NUMBER 2 JUNE
2 GONZALEZ-MARTINEZ ET AL comparison with open procedures (where deep lesion access would be contraindicated because of access-related morbidity). A key requirement of laser ablation is accurate and safe placement of the laser fiber within the intended target. The ROSA robot (Medtech Surgical, Inc, Newark, New Jersey) has been increasingly utilized to place single or numerous electrodes or catheters into brain targets. Robot-assisted stereotactic placement of intracerebral devices has been extensively performed with demonstrated accuracy and safety. 7 Additionally, intraoperative MRI allows identification of real-time status of intracranial pathology while maintaining a sterile environment. Based on intraoperative MRI, modification and/or further treatment may be instituted, while maintaining a sterile field and keeping the patient anesthetized. Although not an absolute necessity for performance of the procedure, intraoperative MRI can assist in these notable ways. The combination of these 3 techniques facilitates robot-assisted stereotactic laser placement, with subsequent MRI confirming placement and allowing subsequent treatment confirmation. This is the first operative technique report, to the authors knowledge, describing these 3 modalities. METHODS The patient, a 19-year-old woman, had experienced medically intractable focal partial epilepsy since the age of 9. The epileptogenic zone was localized to the right frontal region by using noninvasive data (semiology, scalp electroencephalography [EEG], MRI, positron emission tomography, and ictal single-photon emission computed tomography) complemented by an invasive evaluation using the stereoelectroencephalography methodology (SEEG). MRI revealed a periventricular heterotopic-appearing lesion that proved to be epileptogenic by intralesional depth electrode ictal recordings. Given her 10-year history of medically refractory epilepsy, treatment options were discussed with the patient, and she elected to proceed with the laser ablation procedure. Working under an institutional review board-approved protocol at the Cleveland Clinic, a preoperative thin-slice MRI with and without contrast was obtained in various sequences (TI, T2, fluid attenuated inversion recovery). The lesion was clearly visualized by using a T1-weighted MRI, suggestive of a hypointense (,1 cm) region adjacent to the right frontal horn and caudate nucleus. This MRI study was uploaded to the ROSA robot and a plan was created whereupon entry point at the right frontal region and target were defined, along with a safe pathway that avoided blood vessels seen on contrasted imaging (Figure 1). The patient was anesthetized in the operative suite, which was adjoining the MRI suite and separated by a retractable wall, with common ceiling tracks for the IMRIS MRI system (IMRIS, Inc, Winnipeg, Manitoba, Canada). Her head was placed in a Leksell frame (Elekta, Inc, Stockholm, Sweden), with left frontal and posterior posts and pins applied; this frame was affixed to the operative bed. The ROSA robot was then moved into position, registered with the patient using surface landmarks (facial features, eg nasion, tip of nose, canthi, etc). The entry point was marked FIGURE 1. Preoperative volumetric T1-weighted with contrast MR images loaded to ROSA software, showing the proposed laser probe trajectory. The entry point at the right frontal region and target were defined, along with a safe pathway that avoided blood vessels. 168 VOLUME 10 NUMBER 2 JUNE
3 ROBOT-ASSISTED STEREOTACTIC LASER ABLATION once a satisfactory registration was achieved, and the robot remained locked in position. After shaving a small region and prepping around the entry site, a cordless power drill was used to both make the scalp incision and the hole in the skull (3.2 mm). The dura was coagulated, opened, and entered, and the robot arm was used to determine both trajectory and depth. Using an aligning rod through the robot trajectory guide, a skull bolt (Visualase, Inc) was placed into the hole and secured in place. The bolt contains a silicone diaphragm allowing loosening for passage and securing of the laser applicator. The 1.65-mm-diameter, 3-mm-length laser-reflecting end was passed through the bone screw and advanced just proximal to the distal end of the target initially, and the 980-nmwavelength laser was placed within the canula and secured. With a sterile field being maintained, the retractable wall between the operative and MRI suites was opened, and the IMRIS MRI was slid into position along the ceiling tracks. After confirmation of the proper laser applicator position (see Figure 2A, B) using intraoperative multiplanar images on MRI (Siemens, Inc, Munich, Germany), correct trajectory was confirmed, and the surgeon elected to advance the canula to the distal end of the lesion (to optimize lesion coverage, with advancement accomplished in approximately 3 minutes). Images were acquired to verify optimal position, and ablation commenced. As a precaution, safety points were designated around the fiber to allow real-time monitoring of heat and to trigger a laser shut-off. If a higher-than-desired (90 C) temperature was reached either close to the laser applicator or in surrounding healthy tissue, the high-limit safety points shut off the laser to protect the cannula. Lowlimit safety points were included if protected cerebral structures reached temperatures of 50 C. The laser was powered at 9 W for approximately 60 seconds. Single planar real-time thermal mapping was superimposed upon MRI, being refreshed every 4 seconds (see Figure 2C-F). The creation of an approximately 1-cm irreversible damage zone lesion was confirmed on both diffusion imaging intraprocedure and on postprocedure gadolinium-enhanced T1-weighted imaging (Figure 2G). The irreversible damage zone was calculated by an Arrhenius rate model of thermal tissue destruction. The MRI was then slid into its original position in its MRI suite, and the laser applicator was removed, with the incision closed with the use of a single stitch (while maintaining sterility throughout the procedure). Figure 3 shows various intraoperative steps in the procedure. RESULTS The procedure, from skin incision to end of ablation, was performed in approximately 90 minutes. The actual laser ablation was performed in less than 3 minutes, with approximately 45 minutes of the procedure s 90 minutes spent acquiring images in the MRI scanner. Approximately 30 additional minutes preoperatively were used to place the patient in the frame and register the robot. Accurate placement of laser applicator (as compared with preplanned trajectories) was achieved by using the robotic guidance and confirmed by the intraoperative MR images. The postablation MRI showed complete ablation of the focal periventricular heterotopic lesion, with approximately a 1-cm ellipsoid lesion being created by the applicator. A gadoliniumenhancing rim (Figure 3) shows the sharp delineation between normal brain and the lesion, with significant drop-off in heat between these areas as planned and described in the Methods section previously. The patient did not experience any neurological or other complications, and awoke immediately following the procedure. Because the postablation scan revealed no bleed, she was transferred to the floor (without intensive care unit or step-down monitoring being required), and was discharged to home the following day after an uncomplicated hospital course. DISCUSSION Laser ablation, whether for superficial or deep lesions of brain, offers a minimally invasive method for accessing tumors, epileptic foci, or other lesioning targets within the brain. The 1.65-mm Visualase laser applicator is placed through a 3.2-mm opening, with the applicator s distal portion able to create a lesion using heat-based ablation. Depending on temperature and duration of time, lesions from approximately 5 mm to 20 mm in width can be created with a single heating episode, and the fiber optic can be retracted within the catheter to create larger lesions. Larger lesions can be ablated with additional trajectories. Using this laser technique, neurosurgeons have treated metastatic and primary brain tumors, using 1 or more applicators when larger tumors were encountered. Laser ablation has also been used by neurosurgeons recently for treatment of symptomatic radiation necrosis, where immediate, significant diminution in edema and symptoms resulted in several patients. 5 In epilepsy, even curved structures such as the hippocampus have been ablated, with 6-month seizure cure results comparable to some 12-month openly performed temporal lobectomy procedures. 3 Difficult-toreach lesions such as hypothalamic hamartoma, where other techniques offer 40% to 60% cure rate, have been treated with over 80% cure rate and a markedly lower complication rate. 3,8 Because laser ablation does not typically cause damage to the corridor through which it enters the lesion, it is advantageous over open procedures. Deep-located epileptogenic zones, frequently associated with focal cortical dysplasias located in depths of sulci, insula, or the interhemispheric fissure, have been difficult to treat because of the damage in the corridor being used for the conventional surgical approach especially when lesions are located in or near eloquent cortical and subcortical structures. In addition, stereotactic radiosurgery use in younger children is questionable owing to the radiation imparted and possible delayed side effects. Hence, stereotactic laser ablation may be preferable for deep lesions for these reasons, as well as for small and well-circumscribed superficial epileptic lesions due to the minimal (several-millimeter) incision created, allowing many procedures to have been done with the patient awake. Proper placement of the laser fiber within the lesion is paramount. One advantage of the robotic system, which uses a similar concept as frameless stereotaxy in its registration of the patient s affixed head to previously acquired MR images, is its accurate targeting of the lesion. Recent studies have shown robot- OPERATIVE NEUROSURGERY VOLUME 10 NUMBER 2 JUNE
4 GONZALEZ-MARTINEZ ET AL FIGURE 2. Intraprocedure ablation superimposed upon T1-weighted images (A-D) with temperature readings (E, F) based on real-time thermal mapping algorithms. G shows postablation contrasted MRI with ring-enhancing lesion in the right periventricular nodule region. assisted trajectories to be safe, accurate, efficient, and comparable to other procedures employing either frame-based stereotaxy or frameless, nonrobotic stereotaxy Another important advantage is the stabilization its arm provides to the drill, allowing an accurate trajectory that leads to the target lesion. This operative technique illustration, utilizing both navigation capabilities of the robot and stabilization, allowed both targeting and placement of the laser fiber to be performed in less than 170 VOLUME 10 NUMBER 2 JUNE
5 ROBOT-ASSISTED STEREOTACTIC LASER ABLATION FIGURE 3. Intra-operative photographs showing robot guiding trajectory (A, B), laser applicator passage into brain through skull bolt (C), robot disconnection and removal after laser probe placement, allowing intraoperative MR imaging procedure (D), and final aspect with dressing applied (E). 45 minutes; this short time duration, coupled with the minimal incision (made with the drill), minimizes infection risk. The Cleveland Clinic Epilepsy Center s experience with the ROSA robot has included accurate placement of multiple intracranial depth electrodes for stereo-eeg lead placement, both efficiently and with minimal complications. Hence, the laser fiber was placed by using this technique. Presumably, future technique could include the placement of numerous depth electrodes into a nonlesional epilepsy patient, with ablation subsequently performed through the same entry hole corresponding to the electrode most proximal to the epileptogenic focus (or interpolated between several such electrodes). Thus the robotic and laser systems are complimentary. Use of the intraoperative MRI has found benefit in neurosurgery, 10 with one of its main attributes being the identification of success while maintaining sterility of the operative field, while the patient remained anesthetized. In our scenario, describing the robotically placed laser applicator, the patient s bed remained in the same position, as the intraoperative MRI was slid into position along ceiling-affixed tracks. This allowed for modification as needed, with only approximately 3 minutes being required to advance the applicator up to 1 cm to reach the distal-most part OPERATIVE NEUROSURGERY VOLUME 10 NUMBER 2 JUNE
6 GONZALEZ-MARTINEZ ET AL of lesion (while still maintaining sterility for the system). While possession of an intraoperative MRI does not preclude a Visualase laser ablation operation from being done, it helped our operation for the reasons cited above. CONCLUSION This case illustrated the feasibility of a unique combination of the robot, laser, and intraoperative MRI. Although we acknowledge that further study is needed, the success of the presently described laser procedure allows the possibility of a future diagnostic-therapeutic combination that offers minimal invasiveness, duration of treatment, and subsequent recovery, without compromising efficacy. Disclosure Dr Patwardhan is a past consultant and present licensor of patented technology, clinically employed, and an equity holder with Visualase, Inc. None of the other authors have a personal, financial, or institutional interest in any of the drugs, materials, or devices described in this article. REFERENCES 1. Carpentier A, Chauvet D, Reina V, et al. MR-guided laser-induced thermal therapy (LITT) for recurrent glioblastomas. Lasers Surg Med. 2012;44(5): Carpentier A, McNichols RJ, Stafford RJ, et al. Laser thermal therapy: real-time MRI-guided and computer-controlled procedures for metastatic brain tumors. Lasers Surg Med. 2011;43(10): Curry DJ, Gowda A, McNichols RJ, Wilfong AA. MR-guided stereotactic laser ablation of epileptogenic foci in children. Epilepsy Behav. 2012;24(4): Rahmathulla G, Recinos PF, Valerio JE, Chao S, Barnett GH. Laser interstitial thermal therapy for focal cerebral radiation necrosis: a case report and literature review. Stereotact Funct Neurosurg. 2012;90(3): Torres-Reveron J, Tomasiewicz HC, Shetty A, Amankulor NM, Chiang VL. Stereotactic laser induced thermotherapy (LITT): a novel treatment for brain lesions regrowing after radiosurgery. J Neurooncol. 2013;113(3): Tovar-Spinoza Z, Carter D, Ferrone D, Eksioglu Y, Huckins S. The use of MRI guided laser-induced thermal ablation for epilepsy. Childs Nerv Syst. 2013;29(11): Cardinale F, Cossu M, Castana L, et al. Stereoelectroencephalography: surgical methodology, safety, and stereotactic application accuracy in 500 procedures. Neurosurgery. 2013;72(3): Pati S, Abla AA, Rekate HL, Ng YT. Repeat surgery for hypothalamic hamartoma in refractory epilepsy. Neurosurg Focus. 2011;30(2):E3. 9. Bekelis K, Radwan T, Desai A, Roberts D. Frameless robotically targeted sterotactic brain biopsy: feasibility, diagnositic yield and safety. J Neurosurg. 2012; 116(5): Hall WA, Truwit CL. Intraoperative MR-guided neurosurgery. J Magn Reson Imaging. 2008;27(2): Nathoo N, Cavuşoglu MC, Vogelbaum MA, Barnett GH. In touch with robotics: neurosurgery for the future. Neurosurgery. 2005;56(3): ; discussion Rizun PR, McBeth PB, Louw DF, Sutherland GR. Robot-assisted neurosurgery. Semin Laparosc Surg. 2004;11(2): Sutherland GR, Lama S, Gan LS, Wolfsberger S, Zareinia K. Merging machines with microsurgery: clinical experience with neuroarm. J Neurosurg. 2013;118(3): Sutherland GR, Latour I, Greer AD. Integrating an image-guided robot with intraoperative MRI: a review of the design and construction of neuroarm. IEEE Eng Med Biol Mag. 2008;27(3): COMMENTS The authors reported on a case of combined use of stereotactic laser ablation, robotic assistance, and intraoperative MRI. This unique and first-time published combination of 3 modern, state-of-the-art techniques, allowed them to ablate an epileptogenic periventricular gray matter nodule in a drug-resistant 19-years-old woman. The procedure was minimally invasive, quick and safe, with only minimal discomfort to the patient who was discharged from the hospital the day after the treatment. Both the robotic assistance and the intraoperative MRI guidance, although not mandatory, increased the probability of being successful and avoiding complications. This report is aimed at describing the surgical technique, and, for this reason, detailed information about the individual clinical frame is not given. Nevertheless, the reader must be warned against the idea that ablating the lesion could certainly lead to seizure freedom. Thus, it must be positively highlighted that the authors performed a long-term Video- SEEG monitoring before indicating the laser ablation. Only once the heterotopic nodule was demonstrated as epileptogenic by the intracerebral recordings, the stereotactic procedure was performed and the lesion ablated. Our group reported 4 of 5 similar cases treated successfully with SEEGguided radiofrequency thermal lesioning. 1 Moreover, the efficacy of laser ablations on other epileptogenic conditions such as hippocampal sclerosis has been reported yet. 2 This evidence led us to be optimistic about the outcome of the reported case, but no information about the result on seizures is given in this report. More clinical studies are needed to consider the immediate neuroradiological outcome as a positive predictor of seizure freedom. If the efficacy of SEEG-laser ablation on seizures will be confirmed by further studies, this new technique will certainly contribute to reducing the invasiveness and decreasing the morbidity of a number of procedures aimed at treating drug-resistant epilepsies. Francesco Cardinale Milan, Italy 1. Cossu M, Fuschillo D, Cardinale F, et al. Stereo-EEG-guided radio-frequency thermocoagulations of epileptogenic grey-matter nodular heterotopy. J Neurol Neurosurg Psychiatry [Epub ahead of print]. 2. Curry DJ, Gowda A, McNichols RJ, Wilfong AA. MR-guided stereotactic laser ablation of epileptogenic foci in children. Epilepsy Behav. 2012;24(4): Epilepsy strikes about 38,000 new patients per year. 1 It is estimated that up to one-third of these patients will be refractory to medical management, necessitating a surgical solution. Yet it is estimated that, nationally, epilepsy surgery centers only operate on 1962 cases a year on average, leaving about 82% of the surgical cases untreated. 1 Englot et al 2 have addressed this treatment gap and among the reasons given for low surgical intervention was patient choice, citing the invasiveness of the surgical intervention as a deterrent. Epilepsy surgery in the future will need to mitigate morbidity, both diagnostically and therapeutically, if we are ever to narrow the treatment gap. The authors submit a welcome article in the development of minimally invasive epilepsy surgery, achieving both invasive diagnostic seizure focus localization and effective surgical treatment in a patient while leaving the cranium intact. The patient did not need extensive hospitalization for recovery of access-related injury. The surgical robot 172 VOLUME 10 NUMBER 2 JUNE
7 ROBOT-ASSISTED STEREOTACTIC LASER ABLATION achieved good accuracy to a subcentimeter target at a 43-mm stereotactic depth. The intraoperative MRI clearly facilitated the safe and effective completion of the surgery as it mitigated the need for patient transport with all the risks of endotrachial tube dislodgement, laser cannula dislodgement, and exposure to unsterile environments. The combination of these minimally invasive and intraoperative guidance techniques can serve as a model for minimally invasive epilepsy surgery in the future. We thank the authors for their contribution and believe that this is a helpful article in the development of ablative epilepsy surgery. We recognize the authors extensive experience in stereoelectroencephalography, and acknowledge that, although this report is a proof-of-principle of the combination of these technologies on a single target, the greater utility of this technological combination will be when multiple targets will need to be treated, such as in tuberous sclerosis and other multifocal epilepsy cases. Sabih Effendi Daniel J. Curry Houston, Texas 1. Schiltz NK, Koroukian SM, Lhatoo SD, Kaiboriboon K. Temporal trends in presurgical evaluations and epilepsy surgery in the U.S. from 1998 to Epilepsy Res. 2013;103(2-3): Englot D, Ouyang D, Garcia P. Epilepsy surgery trends in the United States, Neurology. 2012;78(16): OPERATIVE NEUROSURGERY VOLUME 10 NUMBER 2 JUNE
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT. Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018
 EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
EPILEPSY 2018: UPDATE ON MODERN SURGICAL MANAGEMENT Robert Kellogg, MD Advocate Children s Hospital Park Ridge, IL April 20, 2018 No disclosures OBJECTIVES Brief history of epilepsy surgery Pre-operative
SYSTEM OVERVIEW MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY
 SYSTEM OVERVIEW MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY Software NeuroBlate Fusion Software is the exclusive software intelligence behind the NeuroBlate System. NeuroBlate Fusion allows neurosurgeons
SYSTEM OVERVIEW MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY Software NeuroBlate Fusion Software is the exclusive software intelligence behind the NeuroBlate System. NeuroBlate Fusion allows neurosurgeons
NOW WITH SYSTEM OVERVIEW MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY
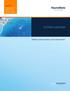 NOW WITH SYSTEM OVERVIEW MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY Mini-Bolt Access Robotically Controlled Probe Driver MRI-Guided Laser Energy PRECISION AND CONFIDENCE DELIVERED THROUGH A MINIMALLY
NOW WITH SYSTEM OVERVIEW MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY Mini-Bolt Access Robotically Controlled Probe Driver MRI-Guided Laser Energy PRECISION AND CONFIDENCE DELIVERED THROUGH A MINIMALLY
A Minimally Invasive Option for Patients Considering Brain Surgery
 PATIENT S GUIDE A Minimally Invasive Option for Patients Considering Brain Surgery MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY Robotically Controlled Probe Driver Precise nature of the NeuroBlate System
PATIENT S GUIDE A Minimally Invasive Option for Patients Considering Brain Surgery MINIMALLY INVASIVE ROBOTIC LASER THERMOTHERAPY Robotically Controlled Probe Driver Precise nature of the NeuroBlate System
The American Approach to Depth Electrode Insertion December 4, 2012
 The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
Multimodal Imaging in Extratemporal Epilepsy Surgery
 Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012
 Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012 Case Hans O. Lűders Epilepsy Center Medical Center, University Hospitals, Cleveland
Stereotactic Electroencephalography (seeg) in the Pre-surgical Investigation of Refractory Focal Epilepsy December 4, 2012 Case Hans O. Lűders Epilepsy Center Medical Center, University Hospitals, Cleveland
Difficult-to-Localize Intractable Focal Epilepsy: An In-Depth Look
 Current Literature In Clinical Science Difficult-to-Localize Intractable Focal Epilepsy: An In-Depth Look Stereoelectroencephalography in the Difficult to Localize Refractory Focal Epilepsy: Early Experience
Current Literature In Clinical Science Difficult-to-Localize Intractable Focal Epilepsy: An In-Depth Look Stereoelectroencephalography in the Difficult to Localize Refractory Focal Epilepsy: Early Experience
Over the last few years, laser interstitial thermotherapy. focus Neurosurg Focus 41 (4):E3, 2016
 neurosurgical focus Neurosurg Focus 41 (4):E3, 2016 The use of custom 3D printed stereotactic frames for laser interstitial thermal ablation: technical note Nicholas J. Brandmeir, MD, James McInerney,
neurosurgical focus Neurosurg Focus 41 (4):E3, 2016 The use of custom 3D printed stereotactic frames for laser interstitial thermal ablation: technical note Nicholas J. Brandmeir, MD, James McInerney,
21 ST CENTURY TECHNOLOGY IN PEDIATRIC NEUROLOGIC DISORDERS PEDIATRIC NEUROLOGIC DISORDERS YOUR LEARNING EXPERIENCE LEARNING OBJECTIVES
 21 ST CENTURY TECHNOLOGY IN PEDIATRIC NEUROLOGIC DISORDERS Saturday, April 30, 2016 11:00 am David J. Siegler, M.D. Board Certified American Board of Psychiatry and Neurology National Board of Physicians
21 ST CENTURY TECHNOLOGY IN PEDIATRIC NEUROLOGIC DISORDERS Saturday, April 30, 2016 11:00 am David J. Siegler, M.D. Board Certified American Board of Psychiatry and Neurology National Board of Physicians
Subject: Magnetoencephalography/Magnetic Source Imaging
 01-95805-16 Original Effective Date: 09/01/01 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Magnetoencephalography/Magnetic Source Imaging THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
01-95805-16 Original Effective Date: 09/01/01 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Magnetoencephalography/Magnetic Source Imaging THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION,
Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology. Tim Lucas, MD, PhD Neurosurgery
 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD, PhD Neurosurgery Timothy.Lucas@uphs.upenn.edu 2016 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD,
Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD, PhD Neurosurgery Timothy.Lucas@uphs.upenn.edu 2016 Laser Interstitial Thermal Therapy (LITT) in Neuro-Oncology Tim Lucas, MD,
Stereotactic Minimally Invasive Brain Repair brings hope for patients with seizure disorders
 Stereotactic Minimally Invasive Brain Repair brings hope for patients with seizure disorders It is well known that, currently, the incidence rate of epilepsy is approximately 20-50/100,000 worldwide. This
Stereotactic Minimally Invasive Brain Repair brings hope for patients with seizure disorders It is well known that, currently, the incidence rate of epilepsy is approximately 20-50/100,000 worldwide. This
Department of Neurosurgery, Children s National Medical Center, Washington, DC
 NEUROSURGICAL FOCUS Neurosurg Focus 45 (3):E8, 2018 Early outcomes of stereoelectroencephalography followed by MR-guided laser interstitial thermal therapy: a paradigm for minimally invasive epilepsy surgery
NEUROSURGICAL FOCUS Neurosurg Focus 45 (3):E8, 2018 Early outcomes of stereoelectroencephalography followed by MR-guided laser interstitial thermal therapy: a paradigm for minimally invasive epilepsy surgery
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective
 Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
Epilepsy Surgery, Imaging, and Intraoperative Neuromonitoring: Surgical Perspective AC Duhaime, M.D. Director, Pediatric Neurosurgery, Massachusetts General Hospital Professor, Neurosurgery, Harvard Medical
The Changing Surgical Landscape in Kids
 The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
The Changing Surgical Landscape in Kids December 7, 2013 Howard L. Weiner, MD NYU Langone Medical Center American Epilepsy Society Annual Meeting Disclosure none American Epilepsy Society 2013 Annual Meeting
9/30/2016. Advances in Epilepsy Surgery. Epidemiology. Epidemiology
 Advances in Epilepsy Surgery George Jallo, M.D. Director, Institute for Brain Protection Sciences Johns Hopkins All Children s Hospital St Petersburg, Florida Epidemiology WHO lists it as the second most
Advances in Epilepsy Surgery George Jallo, M.D. Director, Institute for Brain Protection Sciences Johns Hopkins All Children s Hospital St Petersburg, Florida Epidemiology WHO lists it as the second most
Magnetic Resonance guided Laser Interstitial Thermal Therapy for medically intractable epilepsy
 Magnetic Resonance guided Laser Interstitial Thermal Therapy for medically intractable epilepsy Alexander G. Weil, MD, FRCSC, FAANS, FACS 1,2 1 Division of Pediatric Neurosurgery, Department of Surgery,
Magnetic Resonance guided Laser Interstitial Thermal Therapy for medically intractable epilepsy Alexander G. Weil, MD, FRCSC, FAANS, FACS 1,2 1 Division of Pediatric Neurosurgery, Department of Surgery,
Clinical Policy Title: Laser thermal ablation for epileptic seizures
 Clinical Policy Title: Laser thermal ablation for epileptic seizures Clinical Policy Number: 09.03.01 Effective Date: October 1, 2014 Initial Review Date: June 5, 2014 Most Recent Review Date: June 22,
Clinical Policy Title: Laser thermal ablation for epileptic seizures Clinical Policy Number: 09.03.01 Effective Date: October 1, 2014 Initial Review Date: June 5, 2014 Most Recent Review Date: June 22,
ChosingPhase 2 Electrodes
 ChosingPhase 2 Electrodes ACNS Course ECoG/Invasive EEG Houston, February 4 th, 2015 Stephan Schuele, MD, MPH Comprehensive Epilepsy Center Northwestern Memorial Hospital Northwestern University, Feinberg
ChosingPhase 2 Electrodes ACNS Course ECoG/Invasive EEG Houston, February 4 th, 2015 Stephan Schuele, MD, MPH Comprehensive Epilepsy Center Northwestern Memorial Hospital Northwestern University, Feinberg
The ROSA system (Zimmer Biomet/Medtech Surgical) Applications of a robotic stereotactic arm for pediatric epilepsy and neurooncology surgery
 CLINICAL ARTICLE J Neurosurg Pediatr 20:364 370, 2017 Applications of a robotic stereotactic arm for pediatric epilepsy and neurooncology surgery Brandon A. Miller, MD, PhD, Afshin Salehi, MD, David D.
CLINICAL ARTICLE J Neurosurg Pediatr 20:364 370, 2017 Applications of a robotic stereotactic arm for pediatric epilepsy and neurooncology surgery Brandon A. Miller, MD, PhD, Afshin Salehi, MD, David D.
The Surgical Treatment of Epilepsy
 The Surgical Treatment of Epilepsy Jeffrey S. Schweitzer, MD, PhD Kaiser Los Angeles Medical Center Division of Restorative Neurosurgery Ancient craniotomy When Cao started complaining about splitting
The Surgical Treatment of Epilepsy Jeffrey S. Schweitzer, MD, PhD Kaiser Los Angeles Medical Center Division of Restorative Neurosurgery Ancient craniotomy When Cao started complaining about splitting
neuro mate Frameless Gen II stereotactic robot
 neuro mate Frameless Gen II stereotactic robot Table of contents neuro mate Frameless Gen II stereotactic robot 4 System benefits 6 Robotic workflow 7 Applications: SEEG (stereoelectroencephalography)
neuro mate Frameless Gen II stereotactic robot Table of contents neuro mate Frameless Gen II stereotactic robot 4 System benefits 6 Robotic workflow 7 Applications: SEEG (stereoelectroencephalography)
SEEG and the Hippocampus
 THE SIXTH CLEVELAND CLINIC BRAIN MAPPING WORKSHOP September 6-9, 2017 HiMSS Technology Showcase at the Cleveland Convention Center One St. Clair Ave NE Cleveland, OH Limited to just 40 participants THE
THE SIXTH CLEVELAND CLINIC BRAIN MAPPING WORKSHOP September 6-9, 2017 HiMSS Technology Showcase at the Cleveland Convention Center One St. Clair Ave NE Cleveland, OH Limited to just 40 participants THE
EMG, EEG, and Neurophysiology in Clinical Practice
 Mayo School of Continuous Professional Development EMG, EEG, and Neurophysiology in Clinical Practice Matthew T. Hoerth, M.D. Ritz-Carlton, Amelia Island, Florida January 29-February 4, 2017 2016 MFMER
Mayo School of Continuous Professional Development EMG, EEG, and Neurophysiology in Clinical Practice Matthew T. Hoerth, M.D. Ritz-Carlton, Amelia Island, Florida January 29-February 4, 2017 2016 MFMER
Surgical Modalities for Epilepsy Treatment. C.J. Bui, MD, FAANS Ochsner Neuroscience Symposium 2016
 Surgical Modalities for Epilepsy Treatment C.J. Bui, MD, FAANS Ochsner Neuroscience Symposium 2016 Conflict of Interest Nothing to disclose Surgical Modalities Diagnostic Subdural Grids Depth Electrodes
Surgical Modalities for Epilepsy Treatment C.J. Bui, MD, FAANS Ochsner Neuroscience Symposium 2016 Conflict of Interest Nothing to disclose Surgical Modalities Diagnostic Subdural Grids Depth Electrodes
Leksell Gamma Knife Icon. Treatment information
 Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Surgery for Medically Refractory Focal Epilepsy
 Surgery for Medically Refractory Focal Epilepsy Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence
Surgery for Medically Refractory Focal Epilepsy Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence
Research Perspectives in Clinical Neurophysiology
 Research Perspectives in Clinical Neurophysiology A position paper of the EC-IFCN (European Chapter of the International Federation of Clinical Neurophysiology) representing ~ 8000 Clinical Neurophysiologists
Research Perspectives in Clinical Neurophysiology A position paper of the EC-IFCN (European Chapter of the International Federation of Clinical Neurophysiology) representing ~ 8000 Clinical Neurophysiologists
The relevance of somatosensory auras in refractory temporal lobe epilepsies
 BRIEF COMMUNICATION The relevance of somatosensory auras in refractory temporal lobe epilepsies Ghazala Perven, Ruta Yardi, Juan Bulacio, Imad Najm, William Bingaman, Jorge Gonzalez-Martinez, and Lara
BRIEF COMMUNICATION The relevance of somatosensory auras in refractory temporal lobe epilepsies Ghazala Perven, Ruta Yardi, Juan Bulacio, Imad Najm, William Bingaman, Jorge Gonzalez-Martinez, and Lara
focus Neurosurg Focus 41 (4):E10, 2016
 neurosurgical focus Neurosurg Focus 41 (4):E10, 2016 Stereotactic laser ablation for hypothalamic and deep intraventricular lesions Robert T. Buckley, MD, 1 Anthony C. Wang, MD, 1 John W. Miller, MD, PhD,
neurosurgical focus Neurosurg Focus 41 (4):E10, 2016 Stereotactic laser ablation for hypothalamic and deep intraventricular lesions Robert T. Buckley, MD, 1 Anthony C. Wang, MD, 1 John W. Miller, MD, PhD,
Faculty/Presenter Disclosure. Intracranial EEG Recording. Objectives. General Themes. Why invasive recordings? 6/27/2018
 CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure Intracranial EEG Recording Faculty: Dr Richard S McLachlan Relationships with financial sponsors: None currently
CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure Intracranial EEG Recording Faculty: Dr Richard S McLachlan Relationships with financial sponsors: None currently
Epilepsy & Behavior Case Reports
 Epilepsy & Behavior Case Reports 1 (2013) 45 49 Contents lists available at ScienceDirect Epilepsy & Behavior Case Reports journal homepage: www.elsevier.com/locate/ebcr Case Report Partial disconnection
Epilepsy & Behavior Case Reports 1 (2013) 45 49 Contents lists available at ScienceDirect Epilepsy & Behavior Case Reports journal homepage: www.elsevier.com/locate/ebcr Case Report Partial disconnection
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy
 Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy 1. Introduction Epilepsy is a common neurological disorder, which affects about 1 %
Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy 1. Introduction Epilepsy is a common neurological disorder, which affects about 1 %
Essential standard work and patient care techniques: stereoelectroencephalography, stereotactic targeting, and laser interstitial thermal therapy
 Essential standard work and patient care techniques: stereoelectroencephalography, stereotactic targeting, and laser interstitial thermal therapy Jeffrey S. Raskin, Kathryn M. Wagner, Dylan Adams, JoWinsyl
Essential standard work and patient care techniques: stereoelectroencephalography, stereotactic targeting, and laser interstitial thermal therapy Jeffrey S. Raskin, Kathryn M. Wagner, Dylan Adams, JoWinsyl
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting?
 High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
Approximately 70% of childhood SURGICAL TREATMENTS FOR PEDIATRIC EPILEPSY PROCEEDINGS. Ronald P. Lesser, MD KEY POINTS
 ASIM May p153-158 5/14/01 9:19 AM Page 153 SURGICAL TREATMENTS FOR PEDIATRIC EPILEPSY Ronald P. Lesser, MD KEY POINTS Most children with epilepsy refractory to drugs can improve with surgery Temporal lobe
ASIM May p153-158 5/14/01 9:19 AM Page 153 SURGICAL TREATMENTS FOR PEDIATRIC EPILEPSY Ronald P. Lesser, MD KEY POINTS Most children with epilepsy refractory to drugs can improve with surgery Temporal lobe
Comparison of Neuronavigation and Frame-Based Stereotactic Systems in Implanting Epileptic Depth Electrodes
 DOI: 10.5137/1019-5149.JTN.11400-14.2 Received: 08.05.2014 / Accepted: 31.07.2014 Published Online: 24.02.2016 Original Investigation Comparison of Neuronavigation and Frame-Based Stereotactic Systems
DOI: 10.5137/1019-5149.JTN.11400-14.2 Received: 08.05.2014 / Accepted: 31.07.2014 Published Online: 24.02.2016 Original Investigation Comparison of Neuronavigation and Frame-Based Stereotactic Systems
Radiofrequency Ablation (RFA) / Microwave Ablation (MWA) of Lung Tumors
 Scan for mobile link. Radiofrequency Ablation (RFA) / Microwave Ablation (MWA) of Lung Tumors Radiofrequency ablation (RFA) and microwave ablation (MWA) are treatments that use image guidance to place
Scan for mobile link. Radiofrequency Ablation (RFA) / Microwave Ablation (MWA) of Lung Tumors Radiofrequency ablation (RFA) and microwave ablation (MWA) are treatments that use image guidance to place
neuro mate stereotactic robot
 neuro mate stereotactic robot Table of contents neuro mate stereotactic robot 4 System benefits 6 Robotic workflow 7 Applications: SEEG (stereoelectroencephalography) 8 Applications: DBS (deep brain stimulation)
neuro mate stereotactic robot Table of contents neuro mate stereotactic robot 4 System benefits 6 Robotic workflow 7 Applications: SEEG (stereoelectroencephalography) 8 Applications: DBS (deep brain stimulation)
Final rapport Bourse Foundation St-Luc
 Final rapport Bourse Foundation St-Luc Dear Dr.Vanoverschelde, During my stay at the Cleveland clinic I was able to perfection my knowledge and skills in treatment of refractory epilepsy. On educational
Final rapport Bourse Foundation St-Luc Dear Dr.Vanoverschelde, During my stay at the Cleveland clinic I was able to perfection my knowledge and skills in treatment of refractory epilepsy. On educational
epilepsy center About Epilepsy Surgery
 epilepsy center About Epilepsy Surgery Epilepsy Surgery Advances in Epilepsy Surgery Are You a Candidate for Surgery? If anticonvulsant medications have failed to control your epilepsy, or you are experiencing
epilepsy center About Epilepsy Surgery Epilepsy Surgery Advances in Epilepsy Surgery Are You a Candidate for Surgery? If anticonvulsant medications have failed to control your epilepsy, or you are experiencing
EPILEPSY. New Ideas about an Old Disease. Gregory D. Cascino, MD
 EPILEPSY New Ideas about an Old Disease Gregory D. Cascino, MD Disclosure Research-Educational Grants Neuro Pace, Inc. American Epilepsy Society American Academy of Neurology Neurology (Associate Editor)
EPILEPSY New Ideas about an Old Disease Gregory D. Cascino, MD Disclosure Research-Educational Grants Neuro Pace, Inc. American Epilepsy Society American Academy of Neurology Neurology (Associate Editor)
Epilepsy Currents and Pearls. Eniko Nagy-Wilde, MD Medical Director of Epilepsy and Clinical Neurophysiology Sutter Medical Center, Sacramento
 Epilepsy Currents and Pearls Eniko Nagy-Wilde, MD Medical Director of Epilepsy and Clinical Neurophysiology Sutter Medical Center, Sacramento No disclosures Presenter Disclosure Information Learning Objectives
Epilepsy Currents and Pearls Eniko Nagy-Wilde, MD Medical Director of Epilepsy and Clinical Neurophysiology Sutter Medical Center, Sacramento No disclosures Presenter Disclosure Information Learning Objectives
Introduction of FIREFLY Technology
 Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Introduction of FIREFLY Technology FIREFLY Technology is a unique, patent-pending, pre-surgical planning and intra - operative navigation technology that is focused on spinal applications and is derived
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Case reports functional imaging in epilepsy
 Seizure 2001; 10: 157 161 doi:10.1053/seiz.2001.0552, available online at http://www.idealibrary.com on Case reports functional imaging in epilepsy MARK P. RICHARDSON Medical Research Council Fellow, Institute
Seizure 2001; 10: 157 161 doi:10.1053/seiz.2001.0552, available online at http://www.idealibrary.com on Case reports functional imaging in epilepsy MARK P. RICHARDSON Medical Research Council Fellow, Institute
radiofrequency thermocoagulation
 Clinical commentary Epileptic Disord 2009; 11 (4): 333-8 Hypothalamic hamartoma causing gelastic seizures treated with stereotactic radiofrequency thermocoagulation Wei Wang 1,2,3,4, Weimin Wang 4, Xiaofei
Clinical commentary Epileptic Disord 2009; 11 (4): 333-8 Hypothalamic hamartoma causing gelastic seizures treated with stereotactic radiofrequency thermocoagulation Wei Wang 1,2,3,4, Weimin Wang 4, Xiaofei
Epilepsy & Functional Neurosurgery
 Epilepsy & Functional Neurosurgery An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Epilepsy Neurosurgery What is a seizure? continuous
Epilepsy & Functional Neurosurgery An Introduction The LSU-Shreveport Department of Neurosurgery Presenting Authors: Neurosurgery Residents & Faculty Epilepsy Neurosurgery What is a seizure? continuous
Stereotactic Diffusion Tensor Tractography For Gamma Knife Stereotactic Radiosurgery
 Disclosures The authors of this study declare that they have no commercial or other interests in the presentation of this study. This study does not contain any use of offlabel devices or treatments. Stereotactic
Disclosures The authors of this study declare that they have no commercial or other interests in the presentation of this study. This study does not contain any use of offlabel devices or treatments. Stereotactic
Evaluation for Epilepsy Surgery
 Evaluation for Epilepsy Surgery What is pre-surgery evaluation? Surgery is one of the therapies to treat epilepsy. In order to decide if surgery will be helpful for you, your doctor needs to evaluate the
Evaluation for Epilepsy Surgery What is pre-surgery evaluation? Surgery is one of the therapies to treat epilepsy. In order to decide if surgery will be helpful for you, your doctor needs to evaluate the
Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity
 Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity December 10, 2013 Joyce Y. Wu, MD Associate Professor Division of Pediatric Neurology David Geffen School of Medicine
Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity December 10, 2013 Joyce Y. Wu, MD Associate Professor Division of Pediatric Neurology David Geffen School of Medicine
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Visualization strategies for major white matter tracts identified by diffusion tensor imaging for intraoperative use
 International Congress Series 1281 (2005) 793 797 www.ics-elsevier.com Visualization strategies for major white matter tracts identified by diffusion tensor imaging for intraoperative use Ch. Nimsky a,b,
International Congress Series 1281 (2005) 793 797 www.ics-elsevier.com Visualization strategies for major white matter tracts identified by diffusion tensor imaging for intraoperative use Ch. Nimsky a,b,
Epilepsy Research: SLATE
 Epilepsy Research: SLATE Jason M. Schwalb, MD, FAANS, FACS Clinical Associate Professor of Neurosurgery Surgical Director, Movement Disorder & Comprehensive Epilepsy Centers Research Scientist, Center
Epilepsy Research: SLATE Jason M. Schwalb, MD, FAANS, FACS Clinical Associate Professor of Neurosurgery Surgical Director, Movement Disorder & Comprehensive Epilepsy Centers Research Scientist, Center
A physiological connectome of the human brain based on intracranial electrical stimulation in patients with epilepsy
 A physiological connectome of the human brain based on intracranial electrical stimulation in patients with epilepsy Cristian Donos 1 Mihai Maliia 2, Ioana Mindruta 2,3, Jean Ciurea 4, Andrei Barborica
A physiological connectome of the human brain based on intracranial electrical stimulation in patients with epilepsy Cristian Donos 1 Mihai Maliia 2, Ioana Mindruta 2,3, Jean Ciurea 4, Andrei Barborica
Clinical Policy Title: Magnetoencephalography and magnetic source imaging
 Clinical Policy Title: Magnetoencephalography and magnetic source imaging Clinical Policy Number: 09.01.07 Effective Date: January 1, 2015 Initial Review Date: July 16, 2014 Most Recent Review Date: July
Clinical Policy Title: Magnetoencephalography and magnetic source imaging Clinical Policy Number: 09.01.07 Effective Date: January 1, 2015 Initial Review Date: July 16, 2014 Most Recent Review Date: July
Advances in Clinical Neuroimaging
 Advances in Clinical Neuroimaging Joseph I. Tracy 1, PhD, ABPP/CN; Gaelle Doucet 2, PhD; Xaiosong He 2, PhD; Dorian Pustina 2, PhD; Karol Osipowicz 2, PhD 1 Department of Radiology, Thomas Jefferson University,
Advances in Clinical Neuroimaging Joseph I. Tracy 1, PhD, ABPP/CN; Gaelle Doucet 2, PhD; Xaiosong He 2, PhD; Dorian Pustina 2, PhD; Karol Osipowicz 2, PhD 1 Department of Radiology, Thomas Jefferson University,
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
PRESURGICAL EVALUATION. ISLAND OF COS Hippocrates: On the Sacred Disease. Disclosure Research-Educational Grants. Patients with seizure disorders
 PRESURGICAL EVALUATION Patients with seizure disorders Gregory D. Cascino, MD Mayo Clinic Disclosure Research-Educational Grants Mayo Foundation Neuro Pace, Inc. American Epilepsy Society American Academy
PRESURGICAL EVALUATION Patients with seizure disorders Gregory D. Cascino, MD Mayo Clinic Disclosure Research-Educational Grants Mayo Foundation Neuro Pace, Inc. American Epilepsy Society American Academy
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
A Patient s Guide to SRS
 A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
A Patient s Guide to SRS Stereotactic Radiosurgery 230 Nebraska St. Sioux City, IA 51101 NOTES 230 Nebraska St. Sioux City, IA 51101 Contents page Introduction 1 SRS and how it works 2 The technology involved
Emerging surgical therapies in the treatment of pediatric epilepsy
 Pediatric Epilepsy Column (Review Article) Emerging surgical therapies in the treatment of pediatric epilepsy Michael Karsy 1, Jian Guan 1, Katrina Ducis 1,2, Robert J. Bollo 1,3 1 Department of Neurosurgery,
Pediatric Epilepsy Column (Review Article) Emerging surgical therapies in the treatment of pediatric epilepsy Michael Karsy 1, Jian Guan 1, Katrina Ducis 1,2, Robert J. Bollo 1,3 1 Department of Neurosurgery,
Femur Condylar Plate System Procedural Steps.
 Femur Condylar Plate System Procedural Steps www.carbo-fix.com 1 Table of Contents Introduction..3 Instrumentation Set... 8 Procedural Steps:...... 12 Ordering Information 19 2 Introduction The CarboFix
Femur Condylar Plate System Procedural Steps www.carbo-fix.com 1 Table of Contents Introduction..3 Instrumentation Set... 8 Procedural Steps:...... 12 Ordering Information 19 2 Introduction The CarboFix
Accuracy of intracranial electrode placement for stereoelectroencephalography: A systematic review and meta-analysis
 CRITICAL REVIEW AND INVITED COMMENTARY Accuracy of intracranial electrode placement for stereoelectroencephalography: A systematic review and meta-analysis *Vejay N. Vakharia, Rachel Sparks, Aidan G. O
CRITICAL REVIEW AND INVITED COMMENTARY Accuracy of intracranial electrode placement for stereoelectroencephalography: A systematic review and meta-analysis *Vejay N. Vakharia, Rachel Sparks, Aidan G. O
Catheter-directed Thrombolysis
 Scan for mobile link. Catheter-directed Thrombolysis Catheter-directed thrombolysis treats vascular blockages and improves blood flow by dissolving abnormal blood clots. A blood clot, or thrombus, can
Scan for mobile link. Catheter-directed Thrombolysis Catheter-directed thrombolysis treats vascular blockages and improves blood flow by dissolving abnormal blood clots. A blood clot, or thrombus, can
System. Humeral Nail. Surgical Technique
 System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
System Humeral Nail Surgical Technique Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL
Deep Brain Stimulation (DBS)
 Patient & Family Guide 2016 Deep Brain Stimulation (DBS) www.nshealth.ca Deep Brain Stimulation (DBS) Deep brain stimulation (DBS) is used to help control stiffness or uncontrollable movements. Your neurosurgeon
Patient & Family Guide 2016 Deep Brain Stimulation (DBS) www.nshealth.ca Deep Brain Stimulation (DBS) Deep brain stimulation (DBS) is used to help control stiffness or uncontrollable movements. Your neurosurgeon
3. PATIENT POSITIONING & FRACTURE REDUCTION 3 8. DISTAL GUIDED LOCKING FOR PROXIMAL NAIL PROXIMAL LOCKING FOR LONG NAIL 13
 Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
Contents IMPLANT FEATURES 2 1. INDICATIONS 3 2. PRE-OPERATIVE PLANNING 3 3. PATIENT POSITIONING & FRACTURE REDUCTION 3 4. INCISION 4 5. ENTRY POINT 4-6 6. PROXIMAL NAIL INSERTION 6-7 7. PROXIMAL LOCKING
UNPRECEDENTED BENEFITS TRANSFORMATIVE RESULTS. In clinical studies, patients reported an immediate, significant reduction of tremor.
 UNPRECEDENTED BENEFITS TREMOR IMPROVEMENT In clinical studies, patients reported an immediate, significant reduction of tremor. * NON-INVASIVE Focused ultrasound is capable of penetrating the skull without
UNPRECEDENTED BENEFITS TREMOR IMPROVEMENT In clinical studies, patients reported an immediate, significant reduction of tremor. * NON-INVASIVE Focused ultrasound is capable of penetrating the skull without
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Computational Medical Imaging Analysis Chapter 7: Biomedical Applications
 Computational Medical Imaging Analysis Chapter 7: Biomedical Applications Jun Zhang Laboratory for Computational Medical Imaging & Data Analysis Department of Computer Science University of Kentucky Lexington,
Computational Medical Imaging Analysis Chapter 7: Biomedical Applications Jun Zhang Laboratory for Computational Medical Imaging & Data Analysis Department of Computer Science University of Kentucky Lexington,
How do we evaluate patients before epilepsy surgery?
 How do we evaluate patients before epilepsy surgery? Yotin Chinvarun, MD Chaiyos Khongkhatithum, MD How do we evaluate patients before epilepsy surgery? Chaiyos Khongkhatithum, MD Division of Neurology
How do we evaluate patients before epilepsy surgery? Yotin Chinvarun, MD Chaiyos Khongkhatithum, MD How do we evaluate patients before epilepsy surgery? Chaiyos Khongkhatithum, MD Division of Neurology
Spike voltage topography in temporal lobe epilepsy
 Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 5-17-2016 Spike voltage topography in temporal lobe epilepsy Ali Akbar Asadi-Pooya Thomas
Thomas Jefferson University Jefferson Digital Commons Department of Neurology Faculty Papers Department of Neurology 5-17-2016 Spike voltage topography in temporal lobe epilepsy Ali Akbar Asadi-Pooya Thomas
Approximately one-third of newly diagnosed epilepsy
 clinical article J Neurosurg 122:526 531, 2015 Intraoperative computed tomography for intracranial electrode implantation surgery in medically refractory epilepsy Darrin J. Lee, MD, PhD, 1 Marike Zwienenberg-Lee,
clinical article J Neurosurg 122:526 531, 2015 Intraoperative computed tomography for intracranial electrode implantation surgery in medically refractory epilepsy Darrin J. Lee, MD, PhD, 1 Marike Zwienenberg-Lee,
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE
 CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
CAREFULLY READ ALL INSTRUCTIONS PRIOR TO USE INDICATIONS FOR USE The LATERA Absorbable Nasal Implant is indicated for supporting upper and lower lateral nasal cartilage. CAUTION: Federal law restricts
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
INNOVATIONS AND SAFETY
 INNOVATIONS AND SAFETY IN EPILEPSY SURGERY 31.08.2018-01.09.2018 Austria Trend Hotel Savoyen Rennweg 16, 1030, Vienna, Austria Organizing Committee Christian Dorfer Medical University of Vienna, Department
INNOVATIONS AND SAFETY IN EPILEPSY SURGERY 31.08.2018-01.09.2018 Austria Trend Hotel Savoyen Rennweg 16, 1030, Vienna, Austria Organizing Committee Christian Dorfer Medical University of Vienna, Department
Advanced Imaging Techniques MRI, PET, SPECT, ESI-MSI, DTI December 8, 2013
 Advanced Imaging Techniques MRI, PET, SPECT, ESI-MSI, DTI December 8, 2013 Robert C. Knowlton, MD, MSPH University of California San Francisco Seizure Disorders Surgical Program American Epilepsy Society
Advanced Imaging Techniques MRI, PET, SPECT, ESI-MSI, DTI December 8, 2013 Robert C. Knowlton, MD, MSPH University of California San Francisco Seizure Disorders Surgical Program American Epilepsy Society
1. POLICY: Magnetic Resonance Image Guided High Intensity Focused Ultrasound (MRgFUS) for Essential Tremor
 Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Retired Date: Page 1 of 10 1. POLICY: Magnetic Resonance Image (MRgFUS) for Essential Tremor 2. RESPONSIBLE PARTIES: Medical Management Administration, Utilization Management, Integrated Care Management,
Hamartomas and epilepsy: clinical and imaging characteristics
 Seizure 2003; 12: 307 311 doi:10.1016/s1059 1311(02)00272-8 Hamartomas and epilepsy: clinical and imaging characteristics B. DIEHL, R. PRAYSON, I. NAJM & P. RUGGIERI Departments of Neurology, Pathology
Seizure 2003; 12: 307 311 doi:10.1016/s1059 1311(02)00272-8 Hamartomas and epilepsy: clinical and imaging characteristics B. DIEHL, R. PRAYSON, I. NAJM & P. RUGGIERI Departments of Neurology, Pathology
Candidates for Epilepsy Surgery. Presurgical Evaluation. Presurgical Evaluation. Presurgical Evaluation. Presurgical Evaluation 8/27/2017
 PresurgicalEpilepsy Eval: A multidisciplinary approach to intractable epilepsy Tayard Desudchit MD Faculty Of Medicine Chulalongkorn U. Candidates for Epilepsy Surgery Persistent seizures despite appropriate
PresurgicalEpilepsy Eval: A multidisciplinary approach to intractable epilepsy Tayard Desudchit MD Faculty Of Medicine Chulalongkorn U. Candidates for Epilepsy Surgery Persistent seizures despite appropriate
Radiofrequency Ablation of Liver Tumors
 Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Intracranial Studies Of Human Epilepsy In A Surgical Setting
 Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Magnetic Resonance Imaging-Guided Laser Interstitial Thermal Therapy for Treatment of Drug-Resistant Epilepsy
 Neurotherapeutics (2017) 14:176 181 DOI 10.1007/s13311-016-0498-3 CURRENT PERSPECTIVES Magnetic Resonance Imaging-Guided Laser Interstitial Thermal Therapy for Treatment of Drug-Resistant Epilepsy Joon
Neurotherapeutics (2017) 14:176 181 DOI 10.1007/s13311-016-0498-3 CURRENT PERSPECTIVES Magnetic Resonance Imaging-Guided Laser Interstitial Thermal Therapy for Treatment of Drug-Resistant Epilepsy Joon
X-Ray Guided Robotic Radiosurgery for Solid Tumors
 X-Ray Guided Robotic Radiosurgery for Solid Tumors Mohan Bodduluri Accuray Incorporated 570 Del Rey Avenue Sunnyvale, CA 94085 USA and J. M. McCarthy Department of Mechanical and Aerospace Engineering
X-Ray Guided Robotic Radiosurgery for Solid Tumors Mohan Bodduluri Accuray Incorporated 570 Del Rey Avenue Sunnyvale, CA 94085 USA and J. M. McCarthy Department of Mechanical and Aerospace Engineering
EEG Wave of the Future: The Video-EEG and fmri Suite?
 Current Literature In Clinical Science EEG Wave of the Future: The Video-EEG and fmri Suite? Mapping Preictal and Ictal Haemodynamic Networks Using Video-Electroencephalography and Functional Imaging.
Current Literature In Clinical Science EEG Wave of the Future: The Video-EEG and fmri Suite? Mapping Preictal and Ictal Haemodynamic Networks Using Video-Electroencephalography and Functional Imaging.
Step by step description - Use of Bonopty Bone Biopsy System, 12 gauge
 Step by step description - Use of Bonopty Bone Biopsy System, 12 gauge Before use, please read the Instructions For Use which accompany the product for indications, contraindications, warnings and precautions.
Step by step description - Use of Bonopty Bone Biopsy System, 12 gauge Before use, please read the Instructions For Use which accompany the product for indications, contraindications, warnings and precautions.
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES. Mr. Johnson. Seizures at 29 Years of Age. Dileep Nair, MD Juan Bulacio, MD
 Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Knee Surgical Technique
 Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Knee Surgical Technique COMPASS Universal Hinge by Jimmy Tucker, M.D. Orthopaedic Surgeon Director, Arkansas Sports Medicine, P.A. Little Rock, Arkansas Table of contents Design features 3 Indications
Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri)
 1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
Introduction. Case. Case Report. Jin-gyu Choi 1, Si-hoon Lee 2, Young-Min Shon 2,3, Byung-chul Son 1,3
 96 Journal of Epilepsy Research Vol. 5, No. 2, 2015 Long-Term Migration of a Deep Brain Stimulation (DBS) Lead in the Third Ventricle Caused by Cerebral Atrophy in a Patient with Anterior Thalamic Nucleus
96 Journal of Epilepsy Research Vol. 5, No. 2, 2015 Long-Term Migration of a Deep Brain Stimulation (DBS) Lead in the Third Ventricle Caused by Cerebral Atrophy in a Patient with Anterior Thalamic Nucleus
Laser interstitial thermal therapy: A first line treatment for seizures due to hypothalamic hamartoma?
 HYPOTHALAMIC HAMARTOMAS AND EPILEPSY Laser interstitial thermal therapy: A first line treatment for seizures due to hypothalamic hamartoma? Victor X. Du, Shashank V. Gandhi, Harold L. Rekate, and Ashesh
HYPOTHALAMIC HAMARTOMAS AND EPILEPSY Laser interstitial thermal therapy: A first line treatment for seizures due to hypothalamic hamartoma? Victor X. Du, Shashank V. Gandhi, Harold L. Rekate, and Ashesh
Imaging of Pediatric Epilepsy MRI. Epilepsy: Nonacute Situation
 Imaging of Pediatric Epilepsy Epilepsy: Nonacute Situation MR is the study of choice Tailor MR study to suspected epileptogenic zone Temporal lobe Extratemporal A. James Barkovich, MD University of California
Imaging of Pediatric Epilepsy Epilepsy: Nonacute Situation MR is the study of choice Tailor MR study to suspected epileptogenic zone Temporal lobe Extratemporal A. James Barkovich, MD University of California
Magnetoencephalography/Magnetic Source Imaging
 6.01.21 Magnetoencephalography/Magnetic Source Imaging Section 6.0 Radiology Subsection Effective Date February 27, 2015 Original Policy Date June 1, 2004 Next Review Date February 2016 Description Magnetoencephalography
6.01.21 Magnetoencephalography/Magnetic Source Imaging Section 6.0 Radiology Subsection Effective Date February 27, 2015 Original Policy Date June 1, 2004 Next Review Date February 2016 Description Magnetoencephalography
Safety and efficacy of stereoelectroencephalography in pediatric focal epilepsy: a single-center experience
 CLINICAL ARTICLE J Neurosurg Pediatr 22:444 452, 2018 Safety and efficacy of stereoelectroencephalography in pediatric focal epilepsy: a single-center experience *Hannah E. Goldstein, MD, 1 Brett E. Youngerman,
CLINICAL ARTICLE J Neurosurg Pediatr 22:444 452, 2018 Safety and efficacy of stereoelectroencephalography in pediatric focal epilepsy: a single-center experience *Hannah E. Goldstein, MD, 1 Brett E. Youngerman,
