Late-onset secondary pigmentary glaucoma following foldable intraocular lenses implantation in the ciliary sulcus: a long-term follow-up study
|
|
|
- Garey Joseph
- 5 years ago
- Views:
Transcription
1 Chang et al. BMC Ophthalmology 2013, 13:22 RESEARCH ARTICLE Open Access Late-onset secondary pigmentary glaucoma following foldable intraocular lenses implantation in the ciliary sulcus: a long-term follow-up study Shirley HL Chang 1,2, Wei-Chi Wu 1,2 and Shiu-Chen Wu 1,2* Abstract Background: To review the long-term outcomes of eyes with secondary pigmentary glaucoma associated with the implantation of foldable intraocular lenses (IOL) in the ciliary sulcus. Methods: The study retrospectively reviewed a series of cases who developed secondary pigmentary glaucoma after cataract operations. Data were collected from cases that were referred between 2002 and Results: Ten eyes of 10 patients who developed secondary pigmentary glaucoma after foldable IOLs implantation in the sulcus were included in this study. Intraocular pressure (IOP) elevation was present in 2 eyes (20%) within the first 2 weeks following the initial cataract operation. The onset of glaucoma was delayed in the other 8 eyes (80%); the average onset time in these eyes was 21.9 ± 17.1 months after the initial cataract operation. Six eyes (60%) received surgical treatment because of large fluctuations and poor control of IOPs. Only 3 eyes (30%) achieved final visual acuities better than 20/40. Conclusion: Secondary pigmentary glaucoma accompanying the implantation of a foldable IOL in the ciliary sulcus may present as acute IOP elevation during the early postoperative period or, more commonly, late onset of IOP elevation accompanied by advanced glaucomatous optic nerve damage. Despite treatment, the visual prognosis for these patients can be poor. Placing a foldable IOL in the ciliary sulcus could pose a threat to the vision of the patients and long-term follow-up of IOP in these patients is necessary. Keywords: Ciliary sulcus, Foldable intraocular lens, Pigmentary glaucoma Background Secondary pigmentary glaucoma has been reported in patients who have undergone posterior chamber intraocular lens (IOL) implantation during cataract surgery, especially when the IOL was implanted in the ciliary sulcus following rupture of the posterior capsule [1-12]. Secondary pigmentary glaucoma can be identified via pigment deposit on the corneal endothelium and IOL, and by heavy pigmentation of the trabecular meshwork. Mechanical rubbing between the foldable IOL and the posterior region of the iris following the placement of the IOL in the sulcus can contribute to the release of pigments [1-12]. This release may present as either * Correspondence: shiuchen@adm.cgmh.org.tw 1 Department of Ophthalmology, Chang Gung Memorial Hospital, Chang Gung University, No. 5, Fu Shin St., Guei-Shan Hsiang, Taoyuan 333, Taiwan 2 College of Medicine, Chang Gung University, Taoyuan, Taiwan pigment dispersion syndrome accompanied by normal intraocular pressure (IOP) or pigmentary glaucoma accompanied by IOP elevation, glaucomatous optic nerve neuropathy and visual field loss. Because the implantation of a foldable IOL has become a popular choice for lens implantation after phacoemulsification, a significant number of foldable IOLs may have been either inadvertently or intentionally placed in the ciliary sulci of cataract patients following the rupture of the posterior capsule. Most reports regarding the development of secondary pigmentary glaucoma following the implantation of a foldable IOL in the sulcus are either case reports or small case series [3-5,7,10-12]. Only two studies involve a larger number of cases, one of 20 and the other of 30 subjects [8,9]. However, the follow-up periods over which the patients in these studies were monitored are 2013 Chang et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
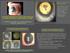
2 Chang et al. BMC Ophthalmology 2013, 13:22 Page 2 of 6 generally short, and most of the patients involved in the aforementioned prior studies are Caucasian. To address these issues, the present study investigates the pattern of IOP elevation and secondary pigmentary glaucoma following the implantation of foldable IOLs in the ciliary sulci of a group of Chinese patients with at least 20 months of follow-up. Both acute-onset and late-onset pigmentary glaucoma following the placement of an IOL in the ciliary sulcus are examined. Methods The present study was designed as a retrospective study. The study reviewed a series of consecutive cases that were referred to the glaucoma clinics at the Department of Ophthalmology at Chang Gung Memorial Hospital in Taoyuan, Taiwan following the development of secondary IOP elevation after the patients underwent cataract operations. Data were collected from cases that were referred between 2002 and The Chang Gung Medical Foundation Institution Review Board approved the study. Cases with secondary IOP elevation following phacoemulsification and foldable IOL implantation in which at least one haptic was placed in the ciliary sulcus were included in the study. All of these cases had open angles and heavy pigmentation on the trabecular meshwork in gonioscopy. Patients who had any history of uveitis, pigment dispersion syndrome, or glaucoma prior to undergoing the cataract operations were excluded. The cornea, iris, lens, and angle status of the fellow eyes were all evaluated by slit-lamp examination and gonioscopy to rule out the diagnosis of primary pigmentary glaucoma. In patients whose gonioscopy showed peripheral anterior synechiae of more than 90 degrees, or who were followed up for fewer than 6 months were also excluded. The main outcome measuresweretheonsetofpigmentaryglaucomaandthe visual results of these cases following medical and surgical glaucoma treatment. External eye photography was performed to record the position of the IOL. Ultrasound biomicroscopy (UBM) was performed to establish the IOL position in the sulcus and to identify any possible contact between the IOL and the iris. Gonioscopy was performed to document both the status and the pigmentation of the angle. Visual field testing was performed to document visual field defects after the onset of glaucoma. The patients records were reviewed to collect the following data: the initial IOPs (defined as IOP at referral) and final IOPs (defined as IOP at last visit); the initial visual acuity (VA) at referral and the final VA at the last visit; any visual field defects; the axial length; the presence or absence of an IOP elevation more than 21 mmhg during the early post-operative period; time of IOP elevation (defined as the time that elapsed between the initial cataract operation and the onset of chronic IOP elevation more than 21 mmhg); the followup period (defined as the time from the referral visit to the last visit); the type of IOL that was used; the presence or absence of vitreous incarceration around the IOL; the decentration of the IOL; the presence of chronic iridocyclitis; the method(s) of IOP control; and the visual outcome. Numerical variables are presented as the means and standard deviations (mean ± SD). Results A total of 10 eyes of 10 patients were enrolled in this study. All of included eyes were referral cases from other clinics or hospitals. All of the included cases were Chinese. The mean age of the patients was 59.6 ± 10.7 years (range: years). Six patients were men, and four patients were women. Two different types of IOLs were used in the patients: 9(90%) one-piece foldable IOLs (Acrysof SA 60AT or SA30AT; Alcon, Fort Worth, Texas, USA), and 1 (10%) silicone IOL (CeeOn 911A, Pharmacia and Upjohn, Kalamazoo, Michigan, USA). At least one haptic of the IOL that was implanted in each eye was placed in the ciliary sulcus. The average time that elapsed between the implantation of the IOL and the onset of IOP elevation was 21.9 ± 17.0 months for all of the cases, and it ranged from 0.5 to 48 months. IOP elevation more than 21 mmhg within the 2 weeks after the initial cataract operation that constituted the early post-operative period was only observed in 2 cases (20%). One of the cases had persistent IOP elevation. The IOP of the other patient was soon put under control by anti-glaucoma medications, and he did not attend follow-up appointments until he experienced a second IOP elevation 4 months later. The other 8 eyes (80%) had delayed glaucoma onset, with the time between the initial cataract operation and the onset of glaucoma ranging between 4 and 48 months. The average period of time between the implantation of the IOL and the onset of glaucoma symptoms in these late-onset cases was 27 ± 15.3 months. Heavy pigmentation was observed in the angles of all of the diseased eyes (Figure 1). Pigment deposit was also observed on the corneal endothelium and the IOLs. Vitreous incarceration around the implanted IOL was found during the examinations of 3 of the 10 eyes (30%), and lens subluxation was noted in 2 eyes (20%). IOL was noted to have different positions at different times during the follow-up period in 1 eye (10%) (Figure 2). Chronic recurrent iridocyclitis was observed in 6 of the eyes (60%) during the follow-up period. UBM showed iris-iol chafing in all of the cases included in the study (Figure 3). The demographic and clinical characteristics of the patients are shown in Table 1.
3 Chang et al. BMC Ophthalmology 2013, 13:22 Figure 1 Pigmentation of the angle structure after the implantation of a foldable intraocular lens (IOL) in the ciliary sulcus of one patient. Compared with the angle of the fellow eye (OS), the angle in the eye in which the IOL had been implanted in the sulcus (OD) had much heavier pigmentation. All of the patients had IOPs that were greater than 21 mmhg at the onset of glaucoma. The mean initial IOP was 35.1 ± 7.6 mmhg (range: mmhg). The average range of IOP fluctuation during different visits in these patients was 12.1 ± 7.0 mmhg, with a range from 4 to 21 mmhg. Four eyes (40%) were controlled with medication(s) alone, and, due to large IOP fluctuations (13 ± 5.2 mmhg) and poor control of the IOPs of the 6 remaining eyes (60%), these patients were treated with additional surgical procedures, which included replacing the foldable IOL with a polymethylmethacrylate (PMMA) IOL (3 cases), anterior vitrectomies, or exchange of IOL combined with trabeculectomies that were enhanced with the use of mitomycin C (3 cases). Page 3 of 6 Figure 3 Contact between the intraocular lens (IOL) and the iris demonstrated via ultrasound biomicroscopy (UBM). UBM revealed that the optic of the IOL had direct contact with iris in this case (arrows), in which the IOL tilted because one haptic had been placed in the capsular bag and the other haptic had been placed in the sulcus. After the various treatments, 2 eyes (20%) maintained their initial VAs, 3 eyes (30%) had improved vision, and 5 eyes (50%) had poorer VAs compared with their initial VAs. Only 3 eyes (30%) achieved final VAs better than 20/40. The mean follow-up period was 46.3 ± 21.3 months (range: months). The treatment outcomes and the visual prognoses of the patients are shown in Table 2. The phakic status of the fellow eyes included 5 phakic eyes and 5 pseudophakic eyes. The gonioscopic finding of these fellow eyes all showed an open angle with light Figure 2 Different intraocular lens (IOL) positions examined on different dates following placement in the sulcus. The position of the IOL had shifted between the earlier and later examinations. The locations of both the margin of the IOL (arrows) and the IOL haptic (asterisk) had changed between the 2 examination dates (A and B). The shifting position of the IOL could have caused the dispersion of iris pigment and chronic inflammation of the eye.
4 Chang et al. BMC Ophthalmology 2013, 13:22 Page 4 of 6 Table 1 Demographic and clinical characteristics of 10 patients Eye (R/L) (no.) 5/5 Sex (M/F)(no.) 6/4 Age (year) Average 59.6 ± 10.7 Range Type of IOL(no.) One-piece foldable IOL 9 Silicon IOL 1 IOL subluxation (Yes/No)(no.) 2/8 Chronic iridocyclitis (Yes/No)(no.) 6/4 Time of IOP elevation (months)(no.)* < 2 weeks 2 2 weeks-12 months months 2 >24 months 4 Vitreous incarceration (Yes/No)(no.) 3/7 F female, IOP intraocular pressure, IOL intraocular lens, M male, m months, no. number, R right eye, L left eye. *following cataract surgery in which an IOL was implanted in the ciliary sulcus. pigment. The average IOP of the fellow eyes was 13.0 ± 3.3 mmhg. None of these fellow eyes showed signs of glaucoma. Discussion Our study has shown that secondary pigmentary glaucoma accompanying the implantation of a foldable IOL in the ciliary sulcus may present as an acute IOP elevation during the early postoperative period in a small percentage of patients (20%). Late-onset IOP elevation with glaucomatous optic nerve damage was observed in the majority of the cases (80%). Most previous articles about the development of secondary pigmentary glaucoma following the implantation of an IOL in the ciliary sulcus reported early onset of post-surgical IOP elevation [7,11,12]. Some cases may have had normal IOPs or may have presented with transient IOP elevations during the initial postoperative period and were soon controlled by anti-glaucoma medication. These cases could present as acute IOP elevation with chronic glaucomatous optic nerve damage at a later date. At later stages in our study, large IOP fluctuations even with medical control were noted in 60% of the cases. This observation may be related to changes in the position of the IOL within the sulcus, and surgical interventions are necessary to control the IOPs in the patients. Cases with chronic IOP elevation that is not responsive to treatment with antiglaucoma medications may require the replacement of the IOL, and/or a trabeculectomy with mitomycin C to control the IOP. Anterior vitrectomy might be needed to release the vitreous incarceration of the IOL during the exchange of IOL. Despite the use of various treatments, the visual prognoses for these patients could be poor in an advanced stage of glaucoma. Therefore, the implantation of a foldable IOL in the ciliary sulcus may pose a risk of developing late-onset pigmentary glaucoma, and performing this procedure after the rupture of the posterior capsule during a cataract surgery should be reconsidered. Two previous articles [13,14] that support the use of a single-piece acrylic IOL in the sulcus have been published. However, other studies [7,9,15,16] have reported that this kind of IOL may induce surgical complications ranging from iris chafing and uveitis-glaucoma-hyphema (UGH) syndrome to vitreous hemorrhage. Uy and Chan [8] found evidence of associations between the implantation of sulcus-fixated, single-piece hydrophobic acrylic intraocular lenses and pigment release and secondary Table 2 Treatment outcomes and visual prognoses of patients with pigmentary glaucoma following the implantation of an intraocular lens in the ciliary sulcus Patient no./eye no. Initial IOP (mmhg) Final IOP (mmhg) Initial VA Final VA Management F/U period (months) FC 20/222 IOL exchange + anterior vitrectomy /400 FC Medical treatment /32 20/32 Medical treatment /100 20/50 IOL exchange + anteriorvitrectomy /32 20/200 IOL exchange + anterior vitrectomy + trabeculectomy /22 20/63 IOL exchange /22 20/32 IOL exchange + trabeculectomy /400 20/100 IOL exchange + trabeculectomy FC FC Medical treatment /63 20/285 Medical treatment 76 IOP intraocular pressure, VA visual acuity, Initial IOP IOP at referral, Final IOP IOP in the last visit, Initial VA VA at referral, Final VA VA in the last visit; FC fingers count, F/U follow-up, HM detects hand motion, IOL intraocular lens, m month, mmhg millimeter of mercury, no. number.
5 Chang et al. BMC Ophthalmology 2013, 13:22 Page 5 of 6 glaucoma in 20 eyes. They found that 7 eyes [35%] developed pigment release and 3 eyes (15%) developed secondary glaucoma. Chang et al. [9] report the largest case series (30 cases) published to date of patients with chronic complications resulting from sulcal placement of single-piece acrylic IOLs. In addition to pigment dispersion syndrome, they found evidence that complications such as recurrent iridocyclitis with secondary IOP elevation, intraocular hemorrhage, cystoid macular edema (CME), and lens decentration with symptomatic edge glare can occur [9]. However, as the average followup duration in Uy and Chan s study [8] was only 17.2 ± 9.4 months, the incidence could be higher if those patients had been followed up over a longer period. The vision of the patients in our study seems to be much worse than that of patients in previous studies. Only 3 eyes (30%) achieved final VAs of better than 20/40. Chang et al. [9] reported that the mean corrected distance visual acuities of the patients in their study improved postoperatively, resulting in the majority of eyes eventually attaining an acuity of 20/20. Uy and Chan [8] described postoperative best-corrected VAs of 20/40 or better in all of the eyes with pigment release and secondary glaucoma. In light of these findings from other studies, we propose some hypotheses regarding the poor vision of our patients. First, all of our patients were referral cases, and 6 of the eyes (60%) presented with visual acuities that were poorer than 20/40 at the time of referral. The high IOP at referral, corneal edema, lens subluxation and advanced glaucomatous optic nerve damage could be the causes of poor VA at referral. The IOPs of these patients may have fluctuated before they became symptomatic with uncontrolled IOP elevation, and this in turn could have led to advanced glaucomatous optic neuropathy prior to referral. Two eyes had lens subluxation and 6 eyes had chronic iridocyclitis. Finally, fluctuations of the IOPs in these patients were frequently noted despite medical and surgical interventions. All of these factors can lead to poor visual prognoses of our patients. IOP elevation in the patients with sulcal foldable IOL implantation may be resulted from multiple mechanisms, including post-operative inflammation, chronic iridocyclitis, vitreous incarceration and pigment dispersion. Early IOP elevation might mainly result from the inflammation associated with the improper management of surgical complications such as vitreous incarceration. At the later stage, IOP elevation in the patients with sulcal foldable IOL implantation may be resulted from chronic iridocyclitis and pigment dispersion. Iris chafing by the IOL can arise because of the closer contact between the IOL and the iris that results from the sulcal placement of the IOL [2-5,7-12]. In addition, the flexible haptics of a foldable IOL facilitate the rubbing-induced detachment of iris pigments. Finally, the IOL can still be moving around freely as a result of the foldable IOL having a relatively smaller diameter than that of the sulcus (Figure 2). This could subsequently induce a pigment storm resulting in pigment accumulation in the trabecular meshwork that might further compromise the trabecular outflow and give rise to glaucoma. The most common histopathologic finding among the patients in the study by Chang et al. [9] was that of pigment granules on the anterior surface of the IOL, with the greatest accumulation occurring on the haptic of the IOL as well as the peripheral optic and the haptic optic junction. These findings are consistent with the notion of posterior iris chafing caused by the optic and the relatively thick flexible haptics, all of which have squared edges and unpolished side walls. In one study of an experimental pigmentary glaucoma [17] model, researchers demonstrated an acute and substantial lowering of the outflow facility of the trabecular meshwork after pigment particles had been infused into the anterior chamber. During an early stage of the disease, pigment can be phagocytosed by trabecular meshwork cells or migrated away via trabecular endothelial cells with the outflow facility returning to normal [17]. However, in advanced pigmentary glaucoma, the trabecular tissue becomes overwhelmed and there is a loss of endothelial cell migration accompanied by collapse of the trabecular beams and subsequent sclerosis of the tissue [18,19]. This finding is compatible with the clinical course of the lateonset of IOP elevation that was observed in our study. To avoid the complication of secondary pigmentary glaucoma following cataract surgery with vitreous loss, management of the herniated vitreous body using a vitrectomy and choosing and implanting IOL properly are very important. In these cases, the implantation of either a PMMA posterior chamber IOL in sulcus or an anterior chamber IOL can be performed following the vitrectomy. Fixating 3-piece acrylic IOL with suture or capturing the optic within a well-centered capsulorhexisis is another option [9]. As far as we are aware, the present study represents the largest case series to examine pigmentary glaucoma following the implantation of foldable IOLs in the ciliary sulci of an Asian study population. The average followup of the patients is over 3 years. However, the study is still limited by its retrospective nature, variable followup periods, and small number of cases. In addition, no control group was available. Thus, in view of the aforementioned limitations, cause and effect could not be established in this study. Improper management in cases in which there was vitreous loss could also contribute the pigment dispersion in some of our cases. More data are needed to explore both the incidence of secondary pigmentary glaucoma following the implantation of a foldable IOL in the sulcus and the causal relationship between such a procedure and its complications.
6 Chang et al. BMC Ophthalmology 2013, 13:22 Page 6 of 6 Conclusion This study has shown that secondary pigmentary glaucoma following the implantation of a foldable IOL in the ciliary sulcus may present as an acute IOP elevation during the early postoperative period. Or more commonly, it can present as late-onset chronic IOP elevation accompanied by large IOP fluctuations and glaucomatous optic nerve damage during a long-term follow-up period. Surgical interventions are usually needed in these cases. Lateonset of glaucoma symptoms and IOP fluctuation may result in poor visual prognosis despite medical or surgical management. Implantation of a foldable IOL in the ciliary sulcus is therefore not recommended. Because late-onset pressure rise may occur in these patients, long-term follow up for these patients is necessary if such a procedure is to be performed. Informed consent The study was performed with the guidelines required by Chang Gung Medical Foundation Institution Review Board. Abbreviations IOL: Intraocular lenses; IOP: Intraocular pressure; UBM: Ultrasound biomicroscopy; VA: Visual acuity; PMMA: Polymethylmethacrylate; F: Female; M: Male; M: Months; No.: Number; OD: Right eye; OS: Left eye; FC: Finger count; HM: Detect hand motion; F/U: Follow up; mmhg: Millimeter of mercury. Competing interests The authors declare that they have no competing interests. Authors contribution SHLC made substantial intellectual contributions to the conception and design, acquisition of data, and analysis and interpretation of data and revising it critically for important intellectual content and given final approval of the version to be published. WCW was involved in drafting the manuscript, analyzing and interpreting the data and revising it critically for important intellectual content. SCW was involved in revising it critically for important intellectual content and giving final approval of the version to be published. All authors read and approved the final manuscript. 6. Mastropasqua L, Lobefalo L, Gallenga PE: Iris chafing in pseudophakia. Doc Ophthalmol 1994, 87: Micheli T, Cheung LM, Sharma S, et al: Acute haptic-induced pigmentary glaucoma with an AcrySof intraocular lens. J Cataract Refract Surg 2002, 28: Uy HS, Chan PS: Pigment release and secondary glaucoma after implantation of single-piece acrylic intraocular lenses in the ciliary sulcus. Am J Ophthalmol 2006, 142: Chang DF, Masket S, Miller KM, et al: Complications of sulcus placement of single-piece acrylic intraocular lenses: recommendations for backup IOL implantation following posterior capsule rupture. J Cataract Refract Surg 2009, 35: Chang SH, Lim G: Secondary pigmentary glaucoma associated with piggyback intraocular lens implantation. J Cataract Refract Surg 2004, 30: Chang WH, Werner L, Fry LL, et al: Pigmentary dispersion syndrome with a secondary piggyback 3-piece hydrophobic acrylic lens. Case report with clinicopathological correlation. J Cataract Refract Surg 2007, 33: Wintle R, Austin M: Pigment dispersion with elevated intraocular pressure after AcrySof intraocular lens implantation in the ciliary sulcus. J Cataract Refract Surg 2001, 27: Taskapili M, Engin G, Kaya G, et al: Single-piece foldable acrylic intraocular lens implantation in the sulcus in eyes with posterior capsule tear during phacoemulsification. J Cataract Refract Surg 2005, 31: Taskapili M, Gulkilik G, Kocabora MS, et al: Comparison of sulcus implantation of single-piece hydrophilic foldable acrylic and polymethylmethacrylate intraocular lenses in eyes with posterior capsule tear during phacoemulsification surgery. Eur J phthalmol 2007, 17: Toma HS, Dibernardo C, Schein OD, et al: Recurrent vitreous hemorrhage secondary to haptic-induced chafing. Can J Ophthalmol 2007, 42: Masket S: Cataract surgical problem. J Cataract Refract Surg 2007, 33: Epstein DL, Freddo TF, Anderson PJ, et al: Experimental obstruction to aqueous outflow by pigment particles in living monkeys. Invest Ophthalmol Vis Sci 1986, 27: Richardson TM, Hutchinson BT, Grant WM: The outflow tract in pigmentary glaucoma: a light and electron microscopic study. Arch Ophthalmol 1977, 95: Kampik A, Green WR, Quigley HA, et al: Scanning and transmission electron microscopic studies of two cases of pigment dispersion syndrome. Am J Ophthalmol 1981, 91: doi: / Cite this article as: Chang et al.: Late-onset secondary pigmentary glaucoma following foldable intraocular lenses implantation in the ciliary sulcus: a long-term follow-up study. BMC Ophthalmology :22. Acknowledgements We thank Lien-Min Lee for her technical support. None of the authors have any financial support for this submission. Received: 29 December 2012 Accepted: 28 May 2013 Published: 7 June 2013 References 1. Detry-Morel ML, Van AE, Pourjavan S, et al: Anterior segment imaging using optical coherence tomography and ultrasound biomicroscopy in secondary pigmentary glaucoma associated with in-the-bag intraocular lens. J Cataract Refract Surg 2006, 32: Hadid O, Megaw R, Owen R, et al: Secondary pigment dispersion syndrome with single-piece acrylic IOL. J Cataract Refract Surg 2010, 36: LeBoyer RM, Werner L, Snyder ME, et al: Acute haptic-induced ciliary sulcus irritation associated with single-piece AcrySof intraocular lenses. J Cataract Refract Surg 2005, 31: Almond MC, Wu MC, Chen PP: Pigment dispersion and chronic intraocular pressure elevation after sulcus placement of 3-piece acrylic intraocular lens. J Cataract Refract Surg 2009, 35: Iwase T, Tanaka N: Elevated intraocular pressure in secondary piggyback intraocular lens implantation. J Cataract Refract Surg 2005, 31: Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Alastair Porteous * and Laura Crawley
 Porteous and Crawley BMC Ophthalmology 2018, 18(Suppl 1):219 https://doi.org/10.1186/s12886-018-0858-3 CASE REPORT Case report of secondary pigment dispersion glaucoma, recurrent uveitis and cystoid macular
Porteous and Crawley BMC Ophthalmology 2018, 18(Suppl 1):219 https://doi.org/10.1186/s12886-018-0858-3 CASE REPORT Case report of secondary pigment dispersion glaucoma, recurrent uveitis and cystoid macular
2/26/2017. Sameh Galal. M.D, FRCS Glasgow. Lecturer of Ophthalmology Research Institute of Ophthalmology
 Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Sameh Galal M.D, FRCS Glasgow Lecturer of Ophthalmology Research Institute of Ophthalmology No financial interest in the subject presented 1 Managing cataracts in children remains a challenge. Treatment
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015
 Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Structural changes of the anterior chamber following cataract surgery during infancy
 Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study
 ISSN 2231-4261 ORIGINAL ARTICLE Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study 1* 1 1 V. H. Karambelkar, Ankit Sharma, Viraj Pradhan 1 Department of Ophthalmology, Krishna
ISSN 2231-4261 ORIGINAL ARTICLE Subnormal Vision in Uneventful Cataract Surgery after 6 Weeks Hospital Based Study 1* 1 1 V. H. Karambelkar, Ankit Sharma, Viraj Pradhan 1 Department of Ophthalmology, Krishna
Electronic poster presentations
 Electronic poster presentations Cataract Surgery E-00002 Blue-light exposure in an animal model of uveal melanoma B.F. Fernandes, S. Di Cesare, S. Maloney, J.-C. Marshall, W. Dawson, M.N. Burnier, Jr.
Electronic poster presentations Cataract Surgery E-00002 Blue-light exposure in an animal model of uveal melanoma B.F. Fernandes, S. Di Cesare, S. Maloney, J.-C. Marshall, W. Dawson, M.N. Burnier, Jr.
Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support
 European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
European Journal of Ophthalmology / Vol. 17 no. 5, 2007 / pp. 714-719 Intrascleral-fixated intraocular lenses for aphakic correction in the absence of capsular support R.A. AZNABAYEV, I.S. ZAIDULLIN, M.S.H.
Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective cohort study
 Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Pseudophakic angle-closure from a Soemmering ring
 Suwan et al. BMC Ophthalmology (2016) 16:91 DOI 10.1186/s12886-016-0257-6 CASE REPORT Open Access Pseudophakic angle-closure from a Soemmering ring Yanin Suwan *, Bayasgalan Purevdorj, Chaiwat Teekhasaenee,
Suwan et al. BMC Ophthalmology (2016) 16:91 DOI 10.1186/s12886-016-0257-6 CASE REPORT Open Access Pseudophakic angle-closure from a Soemmering ring Yanin Suwan *, Bayasgalan Purevdorj, Chaiwat Teekhasaenee,
Megalocornea is a non-progressive, uniformly
 Case Report 191 Anterior Megalophthalmos Chien-Kuang Tsai, MD; Ing-Chou Lai, MD; Hsi-Kung Kuo, MD; Mei-Chung Teng, MD; Po-Chiung Fang, MD We describe a 36-year-old female who suffered from presenile cataract
Case Report 191 Anterior Megalophthalmos Chien-Kuang Tsai, MD; Ing-Chou Lai, MD; Hsi-Kung Kuo, MD; Mei-Chung Teng, MD; Po-Chiung Fang, MD We describe a 36-year-old female who suffered from presenile cataract
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
Anterior segment imaging
 Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
Article Date: 11/1/2016 Anterior segment imaging AS OCT vs. UBM vs. endoscope; case based approaches BY BENJAMIN BERT, MD, FACS AND BRIAN FRANCIS, MD, MS Currently, numerous imaging modalities are available
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs
 The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
The Anterior Segment & Glaucoma Visual Recognition & Interpretation of Clinical Signs Quiz created by Jane Macnaughton MCOptom & Peter Chapman BSc MCOptom FBDO CET Accreditation C19095 2 CET Points (General)
Clinical Evaluation of the BunnyLens IOL
 Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
Clinical Evaluation of the BunnyLens IOL Introduction: BunnyLens is a foldable Hydrophlic Acrylic IOL with four ear shaped haptic design. The lens design offers many advantages in terms of: 1. Centration
TOXIC ANTERIOR SEGMENT SYNDROME (TASS) WITH SEVERE PIGMENT DISPERSION K. Stephen Sudhakar 1, M. Loganathan 2, R. Panduragan 3, C.
 TOXIC ANTERIOR SEGMENT SYNDROME (TASS) SEVERE PIGMENT DISPERSION K. Stephen Sudhakar 1, M. Loganathan 2, R. Panduragan 3, C. Charanya 4 HOW TO CITE THIS ARTICLE: K. Stephen Sudhakar, M. Loganathan, R.
TOXIC ANTERIOR SEGMENT SYNDROME (TASS) SEVERE PIGMENT DISPERSION K. Stephen Sudhakar 1, M. Loganathan 2, R. Panduragan 3, C. Charanya 4 HOW TO CITE THIS ARTICLE: K. Stephen Sudhakar, M. Loganathan, R.
Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular Lens in Previous Vitrectomized Eyes
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(2):181-185 http://dx.doi.org/10.3341/kjo.2014.28.2.181 Case Report Sutureless Intrascleral Pocket Technique of Transscleral Fixation of Intraocular
Citation BMC Ophthalmology, 2016, v. 16, article no. 64
 Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Title Recurrent acute angle-closure attack due to plateau iris syndrome after cataract extraction with or without argon laser peripheral iridoplasty: a case report Author(s) Choy, NKB; Chan, JCH; Chien,
Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution
 Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
Hirota et al. BMC Ophthalmology 2014, 14:39 RESEARCH ARTICLE Open Access Dehiscence of detached internal limiting membrane in eyes with myopic traction maculopathy with spontaneous resolution Kazunari
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Optometric Postoperative Cataract Surgery Management
 Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Financial Disclosures Optometric Postoperative Cataract Surgery Management David Dinh, OD Oak Cliff Eye Clinic Dallas Eye Consultants March 10, 2015 Comanagement Joint cooperation between two or more specialists
Refractive Dilemma. Challenging Case
 Challenging Case Refractive Dilemma Section Editor: Alireza Baradaran-Rafii, MD Case presentation A 21-year old man was referred to an ophthalmology clinic insisting on getting rid of his glasses which
Challenging Case Refractive Dilemma Section Editor: Alireza Baradaran-Rafii, MD Case presentation A 21-year old man was referred to an ophthalmology clinic insisting on getting rid of his glasses which
Routine OCT and UBM of the anterior segment
 Reprinted from No. 160 december 2012 Volume 17 Routine OCT and UBM of the anterior segment Michel Puech ISSN : 1274-5243 R e p r i n t e d w i t h t h e s u p p o r t o f t h e L a b o r a t o r y Q u
Reprinted from No. 160 december 2012 Volume 17 Routine OCT and UBM of the anterior segment Michel Puech ISSN : 1274-5243 R e p r i n t e d w i t h t h e s u p p o r t o f t h e L a b o r a t o r y Q u
Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure
 ORIGINAL ARTICLE Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure Jimmy S. M. Lai, 1 FRCS, FRCOphth, FHKAM (Ophthalmology), M.Med (Ophthalmology),
ORIGINAL ARTICLE Long-term outcome after cataract extraction in patients with an attack of acute phacomorphic angle closure Jimmy S. M. Lai, 1 FRCS, FRCOphth, FHKAM (Ophthalmology), M.Med (Ophthalmology),
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures
 Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Measure #192: Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures 2012 PHYSICIAN QUALITY REPORTING OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
Understanding Angle Closure
 Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Case Understanding Angle Closure Dominick L. Opitz, OD, FAAO Associate Professor Illinois College of Optometry 56 year old Caucasian Male Primary Eye Exam BCVA: 20/25 OD with+1.25 DS 20/25 OS with +1.75
Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur
 Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur Fathilah Jaais, MRCOphth, Department of Ophthalmology, Faculty of Medicine, University of Malaya, Lembah Pantai, 50603 Kuala
Secondary Intraocular Lens Implantation in University Hospital l, Kuala Lumpur Fathilah Jaais, MRCOphth, Department of Ophthalmology, Faculty of Medicine, University of Malaya, Lembah Pantai, 50603 Kuala
DRAFT CONSENSUS STATEMENT FOR COMMENT October
 DRAFT CONSENSUS STATEMENT FOR COMMENT October 9 2015 This statement was developed as a result of breakout group recommendations from the March 24, 2014 Developing Novel Endpoints for Premium IOLs Workshop
DRAFT CONSENSUS STATEMENT FOR COMMENT October 9 2015 This statement was developed as a result of breakout group recommendations from the March 24, 2014 Developing Novel Endpoints for Premium IOLs Workshop
Nature and Science 2016;14(9)
 Comparison between Implantable Contact Lens (ICL) versus Acry Sof Cachet Phakic Intraocular Lenses in Correction of Moderate to High Myopia Khaled Nada, M. Sc.; Mohammed Attia, M. D and Ashraf El Habbak,
Comparison between Implantable Contact Lens (ICL) versus Acry Sof Cachet Phakic Intraocular Lenses in Correction of Moderate to High Myopia Khaled Nada, M. Sc.; Mohammed Attia, M. D and Ashraf El Habbak,
Corporate Medical Policy
 Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Corporate Medical Policy Optical Coherence Tomography (OCT) Anterior Segment of the Eye File Name: Origination: Last CAP Review: Next CAP Review: Last Review: optical_coherence_tomography_(oct)_anterior_segment_of_the_eye
Pediatric traumatic cataract Presentation and Management. Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017
 Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Pediatric traumatic cataract Presentation and Management Dr. Kavitha Kalaivani Pediatric ophthalmology Sankara Nethralaya Nov 7, 2017 Management of Traumatic Cataract Ocular trauma presents many problems
Cataract Surgery in Patients with Uveitis
 Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
Cataract Surgery in Patients with Uveitis Chris Kalogeropoulos MD, PhD, FEBO Professor of Ophthalmology Faculty of Medicine, University of Ioannina President of Hellenic Society for the Study of Ocular
go the distance NEW AcrySof IQ ReSTOR +2.5 D It s a wide world. Help your patients and everywhere in between.
 NEW AcrySof IQ ReSTOR +2.5 D It s a wide world. Help your patients go the distance and everywhere in between. Now with ACTIVEFOCUS optical design for active-lifestyle patients. Recommend AcrySof IQ ReSTOR
NEW AcrySof IQ ReSTOR +2.5 D It s a wide world. Help your patients go the distance and everywhere in between. Now with ACTIVEFOCUS optical design for active-lifestyle patients. Recommend AcrySof IQ ReSTOR
84 Year Old with Rosacea
 84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
84 Year Old with Rosacea S/p tap and injection of intravitreal vancomycin, ceftazidime, dexamethasone Post-injection day#1 Va HM IOP 14 mmhg Post-injection week#3 BCVA 20/20-3 (plano +0.50 x 180) IOP 23
THE CURRENT TREATMENT OF GLAUCOMA IS DIrected
 Three-Year Follow-up of the Tube Versus Trabeculectomy Study STEVEN J. GEDDE, JOYCE C. SCHIFFMAN, WILLIAM J. FEUER, LEON W. HERNDON, JAMES D. BRANDT, AND DONALD L. BUDENZ, ON BEHALF OF THE TUBE VERSUS
Three-Year Follow-up of the Tube Versus Trabeculectomy Study STEVEN J. GEDDE, JOYCE C. SCHIFFMAN, WILLIAM J. FEUER, LEON W. HERNDON, JAMES D. BRANDT, AND DONALD L. BUDENZ, ON BEHALF OF THE TUBE VERSUS
Case Study. Monocular Malignant Melanoma
 Case Study Monocular Malignant Melanoma Case History A 52 year old Caucasian female presented with a number of naevi on the skin and a right ciliary body malignant melanoma twelve years ago and had an
Case Study Monocular Malignant Melanoma Case History A 52 year old Caucasian female presented with a number of naevi on the skin and a right ciliary body malignant melanoma twelve years ago and had an
CLINICAL SCIENCES. The Effect of Texturing the Intraocular Lens Edge on Postoperative Glare Symptoms
 CLINICAL SCIENCES The Effect of Texturing the Intraocular Lens Edge on Postoperative Glare Symptoms A Randomized, Prospective, Double-Masked Study Will R. Meacock, FRCOphth; David J. Spalton, FRCS, FRCOphth;
CLINICAL SCIENCES The Effect of Texturing the Intraocular Lens Edge on Postoperative Glare Symptoms A Randomized, Prospective, Double-Masked Study Will R. Meacock, FRCOphth; David J. Spalton, FRCS, FRCOphth;
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
CATARACT SURGERY IN UVEITIS. Professor Harminder Singh Dua
 Research Institute of Ophthalmology, Cairo 11 th International Conference, 3-4 February, 2017 CATARACT SURGERY IN UVEITIS Professor Harminder Singh Dua MBBS, DO, DO(Lond), MS, MNAMS, FRCS, FRCOphth., FEBO,
Research Institute of Ophthalmology, Cairo 11 th International Conference, 3-4 February, 2017 CATARACT SURGERY IN UVEITIS Professor Harminder Singh Dua MBBS, DO, DO(Lond), MS, MNAMS, FRCS, FRCOphth., FEBO,
COURSE DESCRIPTION BASIC FUNDAMENTALS
 TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
TACKLING POSTERIOR CAPSULE RUPTURE AND IOL IMPLANTATION: A VIDEO BASED COURSE TUESDAY - 29 th APRIL, 2014: 1.00 PM-2.30 PM, BCEC, ROOM 258 A ; SESSION 29-308 COURSE DESCRIPTION BASIC FUNDAMENTALS Early
Start with ME. LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. TECNIS TORIC 1-PIECE IOL
 LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. Start with ME. TECNIS TORIC 1-PIECE IOL INDICATIONS: The TECNIS Toric 1-Piece Posterior Chamber Lens is indicated for the visual correction
LEAVE A LEGACY OF EXCELLENT OUTCOMES FOR PATIENTS WITH ASTIGMATISM. Start with ME. TECNIS TORIC 1-PIECE IOL INDICATIONS: The TECNIS Toric 1-Piece Posterior Chamber Lens is indicated for the visual correction
Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 622-626 Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal S.M. EL-BAHA, A. EI-SAMADONI, H.F. IDRIS,
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 622-626 Intraoperative biometry for intraocular lens (IOL) power calculation at silicone oil removal S.M. EL-BAHA, A. EI-SAMADONI, H.F. IDRIS,
and done ONE CYPASS MICRO-STENT IS ALL IT TAKES TO DELIVER ON THE PROMISE OF MIGS SAFE, CONSISTENT, LONG-TERM IOP CONTROL
 FOR THE REDUCTION OF IOP IN MILD TO MODERATE PRIMARY OPEN-ANGLE GLAUCOMA AT THE TIME OF CATARACT SURGERY and done ONE CYPASS MICRO-STENT IS ALL IT TAKES TO DELIVER ON THE PROMISE OF MIGS SAFE, CONSISTENT,
FOR THE REDUCTION OF IOP IN MILD TO MODERATE PRIMARY OPEN-ANGLE GLAUCOMA AT THE TIME OF CATARACT SURGERY and done ONE CYPASS MICRO-STENT IS ALL IT TAKES TO DELIVER ON THE PROMISE OF MIGS SAFE, CONSISTENT,
LENS INDUCED GLAUCOMA
 LENS INDUCED GLAUCOMA PRESENTER P SHILPA RAVI 2 ND YEAR PG DEPT OF OPHTHALMOLOGY LENS INDUCED GLAUCOMA It is a form of secondary glaucoma where intraocular pressure is raised due to disorder in crystalline
LENS INDUCED GLAUCOMA PRESENTER P SHILPA RAVI 2 ND YEAR PG DEPT OF OPHTHALMOLOGY LENS INDUCED GLAUCOMA It is a form of secondary glaucoma where intraocular pressure is raised due to disorder in crystalline
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #192 (NQF 0564): Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures National Quality Strategy Domain: Patient Safety 2016 PQRS OPTIONS FOR
Measure #192 (NQF 0564): Cataracts: Complications within 30 Days Following Cataract Surgery Requiring Additional Surgical Procedures National Quality Strategy Domain: Patient Safety 2016 PQRS OPTIONS FOR
Objectives. Tubes, Ties and Videotape: Financial Disclosure. Five Year TVT Results IOP Similar
 Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Tubes, Ties and Videotape: Surgical Video of Glaucoma Implants and Financial Disclosure I have no financial interests or relationships to disclose. Herbert P. Fechter MD, PE Eye Physicians and Surgeons
Comparison of the Long-term Clinical Results of Hydrophilic and Hydrophobic Acrylic Intraocular Lenses
 Korean J Ophthalmol Vol. 19:29-33, 2005 Comparison of the Long-term Clinical Results of Hydrophilic and Hydrophobic Acrylic Intraocular Lenses Youngwoo Suh, MD 1, Chunghoon Oh, MD 2, Hyo-Myung Kim, MD,
Korean J Ophthalmol Vol. 19:29-33, 2005 Comparison of the Long-term Clinical Results of Hydrophilic and Hydrophobic Acrylic Intraocular Lenses Youngwoo Suh, MD 1, Chunghoon Oh, MD 2, Hyo-Myung Kim, MD,
Sulcoflex Trifocal Supplementary IOL. When expectations and outcomes align. An elegant solution for the correction of presbyopia MADE IN UK
 Sulcoflex Trifocal Supplementary IOL When expectations and outcomes align An elegant solution for the correction of presbyopia MADE IN UK We ve been innovating IOLs longer than anyone else. Rayner manufactured
Sulcoflex Trifocal Supplementary IOL When expectations and outcomes align An elegant solution for the correction of presbyopia MADE IN UK We ve been innovating IOLs longer than anyone else. Rayner manufactured
A Study to Compare The Efficacy of 0.5% Timolol Eye Drops Versus 0.2% Brimonidine Eye Drops in Management of Rise In Iop Following Nd-Yag Capsulotomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. II (Sep. 2017), PP 71-76 www.iosrjournals.org A Study to Compare The Efficacy of 0.5%
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. II (Sep. 2017), PP 71-76 www.iosrjournals.org A Study to Compare The Efficacy of 0.5%
3/16/2018. Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim. Prof. of Ophthalmology Al-Azhar University
 Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
Ultrasound Biomicroscopy in Glaucoma By Ahmed Salah Abdel Rehim Prof. of Ophthalmology Al-Azhar University 1 Ultrasound biomicroscopy (UBM) is a recent technique to visualize anterior segment with the
Original Article. Address for Correspondance Dr. Charu Mithal Upgraded Dept. of Ophthalmology, LLRM Medical College Meerut.
 Original Article EVALUATION OF THE VISUAL OUTCOME AND COMPLICATION OF SECONDARY IMPLANTATION OF OPEN-LOOP ANTERIOR CHAMBER, SULCUS FIXATED POSTERIOR CHAMBER AND SCLERAL FIXATED POSTERIOR CHAMBER INTRAOCULAR
Original Article EVALUATION OF THE VISUAL OUTCOME AND COMPLICATION OF SECONDARY IMPLANTATION OF OPEN-LOOP ANTERIOR CHAMBER, SULCUS FIXATED POSTERIOR CHAMBER AND SCLERAL FIXATED POSTERIOR CHAMBER INTRAOCULAR
New supplementary intraocular lens for refractive enhancement in pseudophakic patients
 ARTICLE New supplementary intraocular lens for refractive enhancement in pseudophakic patients Günal Kahraman, MD, Michael Amon, MD PURPOSE: To assess the efficacy and safety of implanting a secondary
ARTICLE New supplementary intraocular lens for refractive enhancement in pseudophakic patients Günal Kahraman, MD, Michael Amon, MD PURPOSE: To assess the efficacy and safety of implanting a secondary
Incidence of Early Onset Glaucoma after Infant Cataract Extraction With and Without
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 Title: Incidence of Early Onset Glaucoma after Infant Cataract Extraction With and Without Intraocular Lens Implantation Authors: Inez B.Y. Wong, FRCSEd(Ophth),
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 Title: Incidence of Early Onset Glaucoma after Infant Cataract Extraction With and Without Intraocular Lens Implantation Authors: Inez B.Y. Wong, FRCSEd(Ophth),
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
 European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
European Journal of Ophthalmology / Vol. 13 no. 4, 2003 / pp. 377-382 The evaluation of retinal nerve fiber layer in pigment dispersion syndrome and pigmentary glaucoma using scanning laser polarimetry
Clinical and functional features of the eyes with phakic lenses before and after bilensectomy
 Clinical and functional features of the eyes with phakic lenses before and after bilensectomy D.O. Marshava Multiprofile clinics L/J Kutaisi (Georgia) E-mail: marshava-david@mail.ru Key words: cataract,
Clinical and functional features of the eyes with phakic lenses before and after bilensectomy D.O. Marshava Multiprofile clinics L/J Kutaisi (Georgia) E-mail: marshava-david@mail.ru Key words: cataract,
Issue 15 The following key clinical peer reviewed journals will be reviewed: MONTHLY RESEARCH UPDATE 151(3) American Journal of Ophthalmology 129(5)
 Welcome to Bausch and Lomb s monthly research update. With our background in clinical ophthalmic research, mainly of the anterior eye, Bausch and Lomb have asked us to produce an independent report of
Welcome to Bausch and Lomb s monthly research update. With our background in clinical ophthalmic research, mainly of the anterior eye, Bausch and Lomb have asked us to produce an independent report of
Every week, the John A. Moran Eye Center at the
 Analyzing Explanted IOLs A review of the pathological processes that affect pseudophakic patients postoperative vision. BY LILIANA WERNER, MD, PHD Every week, the John A. Moran Eye Center at the University
Analyzing Explanted IOLs A review of the pathological processes that affect pseudophakic patients postoperative vision. BY LILIANA WERNER, MD, PHD Every week, the John A. Moran Eye Center at the University
Disorders of the. blood-aqueous barrier after. phacoemulsification in diabetic patients CLINICAL STUDY. Y Liu, L Luo, M He and X Liu
 (2004) 18, 900 904 & 2004 Nature Publishing Group All rights reserved 0950-222X/04 $30.00 www.nature.com/eye CLINICAL STUDY Disorders of the blood-aqueous barrier after phacoemulsification in diabetic
(2004) 18, 900 904 & 2004 Nature Publishing Group All rights reserved 0950-222X/04 $30.00 www.nature.com/eye CLINICAL STUDY Disorders of the blood-aqueous barrier after phacoemulsification in diabetic
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
2/6/2018. Andrew Siedlecki, M.D.
 Andrew Siedlecki, M.D. Siedlecki Cataract and Vision Care Optimization- Improved Uncorrected VA Reduced Spectacle Dependency Minimize Complications Fast Rehabilitation Provide Options for Patients Optometrists
Andrew Siedlecki, M.D. Siedlecki Cataract and Vision Care Optimization- Improved Uncorrected VA Reduced Spectacle Dependency Minimize Complications Fast Rehabilitation Provide Options for Patients Optometrists
Late Intraocular Lens Subluxation in Patients with Uveitis
 Late Intraocular Lens Subluxation in Patients with Uveitis LR Steeples, NP Jones Manchester Royal Eye Hospital Introduction Late in-the-bag IOL subluxation is an unusual complication of phacoemulsification
Late Intraocular Lens Subluxation in Patients with Uveitis LR Steeples, NP Jones Manchester Royal Eye Hospital Introduction Late in-the-bag IOL subluxation is an unusual complication of phacoemulsification
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Title. with prior vitrectomy. Author(s) Takashi. Issue Date Wichtig Editore.
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Spontaneous dislocation of in-the-b with prior vitrectomy Matsumoto, Makiko; Yamada, Koki; Ue Azusa; Tsuiki, Eiko; Kumagami, Take Takashi European
DNB QUESTIONS 2014 PAPER 1. b) What are the Clinical Conditions in Which Nystagmus is Seen? c) Management of Nystagmus.
 DNB QUESTIONS 2014 PAPER 1 1. a) How Will you investigate a case of Nystagmus? b) What are the Clinical Conditions in Which Nystagmus is Seen? c) Management of Nystagmus. 2. a) What is the Principle of
DNB QUESTIONS 2014 PAPER 1 1. a) How Will you investigate a case of Nystagmus? b) What are the Clinical Conditions in Which Nystagmus is Seen? c) Management of Nystagmus. 2. a) What is the Principle of
Gonioscopy and Slit Lamp Exam for the Glaucoma Suspect. Disclosure GONIOSCOPY: Gonioscopy Why?? What should I look for? GONIOSCOPY
 Gonioscopy and Slit Lamp Exam for the Glaucoma Suspect Disclosure Michael Chaglasian has the following disclosures:» 1. Advisory Board: Alcon, Allergan, Bausch+Lomb, Carl Zeiss Meditec, Merck, Sucampo»
Gonioscopy and Slit Lamp Exam for the Glaucoma Suspect Disclosure Michael Chaglasian has the following disclosures:» 1. Advisory Board: Alcon, Allergan, Bausch+Lomb, Carl Zeiss Meditec, Merck, Sucampo»
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA
 EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
EFFICACY AND SAFETY OF CANALOPLASTY IN SAUDI PATIENTS WITH UNCONTROLLED OPEN ANGLE GLAUCOMA DR.FAISAL ALMOBARAK ASSISTANT PROFESSOR AND CONSULTANT DEPARTMENT OF OPHTHALMOLOGY COLLEGE OF MEDICINE AND KING
Uveitis Glaucoma Hyphaema Syndrome. General review
 Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:11-17 REVIEW Uveitis Glaucoma Hyphaema Syndrome. General review Zemba Mihail, Camburu Georgiana *Ophthalmology Department,
Romanian Journal of Ophthalmology, Volume 61, Issue 1, January-March 2017. pp:11-17 REVIEW Uveitis Glaucoma Hyphaema Syndrome. General review Zemba Mihail, Camburu Georgiana *Ophthalmology Department,
TRABECULECTOMY THE BEST AND WORST CANDIDATES
 TRABECULECTOMY THE BEST AND WORST CANDIDATES MICHAEL F. OATS, MD OPHTHALMIC CONSULTANTS OF BOSTON ASCRS 2014 FINANCIAL DISCLOSURES None TRABECULECTOMY Performed for over 100 years Most commonly performed
TRABECULECTOMY THE BEST AND WORST CANDIDATES MICHAEL F. OATS, MD OPHTHALMIC CONSULTANTS OF BOSTON ASCRS 2014 FINANCIAL DISCLOSURES None TRABECULECTOMY Performed for over 100 years Most commonly performed
Srishti Raj, Gunjan Joshi, Manpreet Kaur, Faisal Thattaruthody, Sushmita Kaushik, Surinder S. Pandav
 Clinical and Experimental Vision and Eye Research (2018), 1, 16 20 ORIGINAL ARTICLE Role of laser peripheral iridotomy and treatment outcomes in patients of pigment dispersion syndrome, pigmentary ocular
Clinical and Experimental Vision and Eye Research (2018), 1, 16 20 ORIGINAL ARTICLE Role of laser peripheral iridotomy and treatment outcomes in patients of pigment dispersion syndrome, pigmentary ocular
Clinical study of traumatic cataract and its management
 Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Clinical study of traumatic cataract and its management Original article Manjula Mangane, M.R. Pujari, Chethan N. Murthy Department of Ophthalmology, Basaweshwar Teaching and General Hospital, Gulbarga,
Predictability and accuracy of IOL formulas in high myopia
 ARTICLE Predictability and accuracy of IOL formulas in high myopia Mohamed Yasser Sayed Saif, MD 1 ; Mohamed Othman Abdel Khalek, MD 1 ; Ahmed Tamer Sayed Saif, MD 2 ; Passant Sayed Saif, MD 3 ; Sherif
ARTICLE Predictability and accuracy of IOL formulas in high myopia Mohamed Yasser Sayed Saif, MD 1 ; Mohamed Othman Abdel Khalek, MD 1 ; Ahmed Tamer Sayed Saif, MD 2 ; Passant Sayed Saif, MD 3 ; Sherif
5/18/2014. Fundamentals of Gonioscopy Workshop Aaron McNulty, OD, FAAO Walt Whitley, OD, MBA, FAAO
 1 Fundamentals of Gonioscopy Workshop Aaron McNulty, OD, FAAO Walt Whitley, OD, MBA, FAAO 2 3 4 5 6 Optometry s Meeting 2014 The Most Valuable Glaucoma Tool Glaucoma Diagnosis Gonioscopy Central corneal
1 Fundamentals of Gonioscopy Workshop Aaron McNulty, OD, FAAO Walt Whitley, OD, MBA, FAAO 2 3 4 5 6 Optometry s Meeting 2014 The Most Valuable Glaucoma Tool Glaucoma Diagnosis Gonioscopy Central corneal
Nate Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Assistant Dean, Clinical Care Services Director of CE Chief of Specialty Care Clinics
 Nate Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Assistant Dean, Clinical Care Services Director of CE Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic lighthiz@nsuok.edu YAG
Nate Lighthizer, O.D., F.A.A.O. Assistant Professor, NSUOCO Assistant Dean, Clinical Care Services Director of CE Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic lighthiz@nsuok.edu YAG
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
ASCRS 2016 Instructional Course Mastering Femtosecond Laser Assisted Phacoemulsification. An Evidence-Based Review
 ASCRS 2016 Instructional Course 07-410 Mastering Femtosecond Laser Assisted Phacoemulsification An Evidence-Based Review TIMOTHY V ROBERTS MBBS (NSW), MMed (Syd), FRANZCO, FRACS, GAICD Vision Eye Institute,
ASCRS 2016 Instructional Course 07-410 Mastering Femtosecond Laser Assisted Phacoemulsification An Evidence-Based Review TIMOTHY V ROBERTS MBBS (NSW), MMed (Syd), FRANZCO, FRACS, GAICD Vision Eye Institute,
WGA. The Global Glaucoma Network
 The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
The Global Glaucoma Network Fort Lauderdale April 30, 2005 Indications for Surgery 1. The decision for surgery should consider the risk/benefit ratio. Note: Although a lower IOP is generally considered
Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens without conjunctival dissection in managing lens complications
 Yeung et al. BMC Ophthalmology (2018) 18:108 https://doi.org/10.1186/s12886-018-0776-4 RESEARCH ARTICLE Open Access Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens
Yeung et al. BMC Ophthalmology (2018) 18:108 https://doi.org/10.1186/s12886-018-0776-4 RESEARCH ARTICLE Open Access Combined 23-gauge transconjunctival vitrectomy and scleral fixation of intraocular lens
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Cataract Surgery in 2017 DARBY D. MILLER, MD MPH CORNEA, CATARACT AND REFRACTIVE SURGERY ASSISTANT PROFESSOR OF OPHTHALMOLOGY MAYO CLINIC FLORIDA Natural
Learn Connect Succeed JCAHPO Regional Meetings 2017 Cataract Surgery in 2017 DARBY D. MILLER, MD MPH CORNEA, CATARACT AND REFRACTIVE SURGERY ASSISTANT PROFESSOR OF OPHTHALMOLOGY MAYO CLINIC FLORIDA Natural
Postoperative refraction changes in phacoemulsification cataract surgery with implantation of different types of intraocular lens
 371-376 Iwase:Shoja 7-04-2008 16:57 Pagina 371 European Journal of Ophthalmology / Vol. 18 no. 3, 2008 / pp. 371-376 Postoperative refraction changes in phacoemulsification cataract surgery with implantation
371-376 Iwase:Shoja 7-04-2008 16:57 Pagina 371 European Journal of Ophthalmology / Vol. 18 no. 3, 2008 / pp. 371-376 Postoperative refraction changes in phacoemulsification cataract surgery with implantation
JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES
 JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES BILATERAL ACUTE TRANSILLUMINATION OF THE IRIS Kavitha Avadhani 1, MD, MS, Jay Kalliath 1, MS, FRCS 1 Department of Ophthalmology, NMC Speciality Hospital,
JOURNAL OF OPHTHALMOLOGY AND RELATED SCIENCES BILATERAL ACUTE TRANSILLUMINATION OF THE IRIS Kavitha Avadhani 1, MD, MS, Jay Kalliath 1, MS, FRCS 1 Department of Ophthalmology, NMC Speciality Hospital,
When optical coherence tomography (OCT)
 Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Capsule fixation device for cataract surgery
 European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
European Journal of Ophthalmology / Vol. 19 no. 1, 2009 / pp. 143-146 SHORT COMMUNICATIONS & CASE REPORTS Capsule fixation device for cataract surgery N.M. SERGIENKO 1, Y.N. KONDRATENKO 1, A.K. YAKIMOV
PRESENTED By DR. FAISAL ALMOBARAK, MD
 PRESENTED By DR. FAISAL ALMOBARAK, MD Early FAC associated with hypotony is an important complication after glaucoma filtering procedures, especially trabeculectomy. The reported incidence after trabeculectomy
PRESENTED By DR. FAISAL ALMOBARAK, MD Early FAC associated with hypotony is an important complication after glaucoma filtering procedures, especially trabeculectomy. The reported incidence after trabeculectomy
The Visian ICL Advantages
 The Visian ICL Advantages Many vision correction procedures promise an improved level of vision, but few vision correction alternatives offer the quality and features found with the Visian ICL. These include:
The Visian ICL Advantages Many vision correction procedures promise an improved level of vision, but few vision correction alternatives offer the quality and features found with the Visian ICL. These include:
Cases CFEH. CFEH Facebook Case #4
 CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment surgeon can make
 Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Posterior Segment Complications and Management of Retained Lens Material Jay M. Stewart, MD Cataract surgery is the leading cause of malpractice claims (OMIC) Complicated CE/IOL: Choices the anterior segment
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk cases
 European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
European Journal of Ophthalmology / Vol. 14 no. 4, 2004 / pp. 325-329 Choroidal detachment following retinal detachment surgery: An analysis and a new hypothesis to minimize its occurrence in high-risk
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation
 Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Transient Intraocular Pressure Elevation after Trabeculotomy and its Occurrence with Phacoemulsification and Intraocular Lens Implantation Masaru Inatani*, Hidenobu Tanihara, Takahito Muto*, Megumi Honjo*,
Disclosure: Samuel Masket MD
 Pseudophakic Dysphotopsia Disclosure: Samuel Masket MD Consultant Fees Alcon Laboratories Consultant Fees PowerVision Consultant Fees Ocular Theraputix Consultant Fees WaveTec Royalties Haag-Streit Research
Pseudophakic Dysphotopsia Disclosure: Samuel Masket MD Consultant Fees Alcon Laboratories Consultant Fees PowerVision Consultant Fees Ocular Theraputix Consultant Fees WaveTec Royalties Haag-Streit Research
Chronicity. Narrow Minded. Course Outline. Acute angle closure. Subacute angle closure. Classification of Angle Closure 5/19/2014
 Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Chronicity Narrow Minded The management of narrow angles in the optometric practice Acute Subacute Chronic Aaron McNulty, OD, FAAO Course Outline Classification of Angle Closure Evaluation of narrow angles
Learn Connect Succeed. JCAHPO Regional Meetings 2015
 Learn Connect Succeed JCAHPO Regional Meetings 2015 Pediatric Cataracts: Complicated Cases and Controversies M. Edward Wilson, M.D. N. Edgar Miles Professor of Ophthalmology and Pediatrics Storm Eye Institute
Learn Connect Succeed JCAHPO Regional Meetings 2015 Pediatric Cataracts: Complicated Cases and Controversies M. Edward Wilson, M.D. N. Edgar Miles Professor of Ophthalmology and Pediatrics Storm Eye Institute
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: Continuous curvilinear capsulorhexis, phacoemulsification and in-the-bag placement of
 SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM INTRODUCTION
SPONTANEOUS, LATE, IN-THE-BAG IOL DISLOCATION: ETIOLOGY, RISK FACTORS, PREVENTION, AND MANAGEMENT Session: 21-205 ASCRS San Francisco 2013 Date/Time: April 21, 2013 from 10:00 AM to 11:30 AM INTRODUCTION
Paediatric cataract pathogenesis and management
 Paediatric cataract pathogenesis and management Dr. Kavitha Kalaivani. N Paediatric ophthalmology Sankara Nethralaya February 28-2017 Incidence... 1 to 13 per 10 000 live births 1 200,000 children blind
Paediatric cataract pathogenesis and management Dr. Kavitha Kalaivani. N Paediatric ophthalmology Sankara Nethralaya February 28-2017 Incidence... 1 to 13 per 10 000 live births 1 200,000 children blind
Secondary Glaucomas. Mr Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO Consultant Ophthalmologist, Glaucoma Service, Moorfields Eye Hospital
 Secondary Glaucomas Mr Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO Consultant Ophthalmologist, Glaucoma Service, Moorfields Eye Hospital Introduction: What is glaucoma? Glaucoma is the name given
Secondary Glaucomas Mr Nick Strouthidis MBBS MD PhD FRCS FRCOphth FRANZCO Consultant Ophthalmologist, Glaucoma Service, Moorfields Eye Hospital Introduction: What is glaucoma? Glaucoma is the name given
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
The Effect of Phacoemulsification with Posterior Chamber Intraocular Lens Implantation on Intraocular Pressure and Anterior Chamber Depth
 The Effect of Phacoemulsification with Posterior Chamber Intraocular Lens Implantation on Intraocular Pressure and Anterior Chamber Depth Mohammad Javad Mohamadi, MD 1 Reza Soltani Moghadam, MD 1 Hasan
The Effect of Phacoemulsification with Posterior Chamber Intraocular Lens Implantation on Intraocular Pressure and Anterior Chamber Depth Mohammad Javad Mohamadi, MD 1 Reza Soltani Moghadam, MD 1 Hasan
SAFE, PERMANENT EYE-COLOR CHANGE
 SAFE, PERMANENT EYE-COLOR CHANGE Prepared by Gregg Homer JSD (PhD) February 1, 2012 THE PIGMENTARY GLAUCOMA ISSUE Glaucoma Defined Glaucoma is currently defined as a disturbance of the structural or functional
SAFE, PERMANENT EYE-COLOR CHANGE Prepared by Gregg Homer JSD (PhD) February 1, 2012 THE PIGMENTARY GLAUCOMA ISSUE Glaucoma Defined Glaucoma is currently defined as a disturbance of the structural or functional
