Comparison of Goldmann applanation tonometry and dynamic contour tonometry in healthy and glaucomatous eyes
|
|
|
- Milton Owens
- 6 years ago
- Views:
Transcription
1 (2009) 23, & 2009 Macmillan Publishers Limited All rights reserved X/09 $ CLINICAL STUDY Comparison of Goldmann applanation tonometry and dynamic contour tonometry in healthy and glaucomatous eyes P Ceruti, R Morbio, M Marraffa and G Marchini Department of Neurological and Visual Sciences, Clinic, University of Verona, Verona, Italy Correspondence: P Ceruti, Department of Neurological and Visual Sciences, Clinic, Borgo Trento Hospital, University of Verona, Piazzale Stefani 1, Verona 37126, Italy Tel: þ ; Fax: þ pierre77@ libero.it Received: 27 June 2007 Accepted in revised form: 30 December 2007 Published online: 25 January 2008 Abstract Purpose To compare the measurements of intraocular pressure (IOP) with dynamic contour tonometry (DCT) and Goldmann applanation tonometry (GAT) in healthy and glaucomatous eyes and to evaluate the influence of corneal thickness (CCT), corneal curvature (CC), axial length (AL), and age on these tonometric alternatives. Methods Three hundred eyes of 0 healthy subjects, 0 patients with primary open angle glaucoma, and 0 patients with primary angle-closure glaucoma underwent IOP evaluation with DCT and GAT, and measurements of CCT, CC, and AL. Bland Altman plots were used to evaluate the agreement between tonometers. Regression analysis was used to evaluate the influence of ocular structural factors on IOP measurements obtained with both tonometers. Results Bland Altman plots indicated that the 95% limits of agreement between tonometers were 1.4 to 6.6 mmhg. DCT values measured 2.6±1.9 mmhg higher than GAT readings (Po0.001). The mean IOP difference between DCT and GAT (DIOP) was higher in healthy than in glaucomatous eyes and the magnitude of difference increased with increasing CCT. A significant reduction of DIOP with an increase in both CCT (Po0.001) and IOP values (Po0.001) was found. Regression analysis showed no effect of CC, AL, and age on both DCT and GAT readings. In contrast to GAT (Po0.001), DCT measurements were not influenced by CCT (P ¼ 0.43). Conclusions IOP readings obtained by DCT were higher and less affected by CCT than those by GAT. The DIOP was higher in healthy than in glaucomatous eyes and decreased in relation to increased CCT and IOP values. (2009) 23, ; doi:.38/sj.eye.67032; published online 25 January 2008 Keywords: tonometry; Goldmann applanation tonometry; dynamic contour tonometry; corneal thickness; glaucoma Introduction Over the past four decades, the Goldmann applanation tonometry (GAT) has been the gold standard, against which other tonometers have been compared for routine measurements of intraocular pressure (IOP). However, the accuracy of GAT depends on many ocular structural factors, including central corneal thickness (CCT), corneal curvature (CC), and axial length (AL). 1 Measurements of IOP made with applanation tonometry are influenced directly by the CCT. We assume and apply a single value for CCT (520 mm) in applanation tonometry estimates, although there is compelling evidence that CCT varies between individuals, with ethnicity, gender, age, and the presence of pseudoexfoliation of the lens capsule, 2 and has a diurnal variation. 3 Goldmann himself recognized that the tonometer s accuracy was questionable in corneas that were not of average thickness. In recent years, different studies demonstrated that changes in corneal structure and thickness,
2 Comparison of GAT and DAT in healthy and glaucomatous eyes 263 which are both altered by corneal refractive surgery, might be associated with clinically significant underestimates of IOP when measured with GAT Moreover, many cases of normal-tension glaucoma and ocular hypertension have been erroneously diagnosed by underestimation and overestimation of IOP by GAT in patients whose corneas are thinner or thicker than average, respectively Dynamic contour tonometry (DCT), a novel digital nonapplanation contact tonometer, has been proposed as an alternative method for obtaining IOP readings significantly closer to true manometric levels. 16 DCT was designed to be largely independent of structural properties of the cornea and to eliminate most of the systematic errors arising from physiological variables of the eye, which render GAT less accurate. 17 Some recent studies compared the performance of the new device against other tonometers considering either the influence of pachymetry on IOP readings or the impact of refractive surgery as a source of errors in applanation tonometry Only two studies evaluated ocular structural factors other than pachymetry influencing IOP measurements in healthy subjects 31 or African American subjects. 32 In this study, we compared the IOP readings obtained by DCT with those of GAT and analysed the influence of ocular structural factors (CCT, CC, AL) and age on IOP readings in a large group of Caucasian healthy subjects, patients with primary open angle glaucoma (POAG), and patients with primary angle-closure glaucoma (PACG). Moreover, the effect of CCT, CC, AL, IOP, and age on ocular pulse amplitude (OPA) measurements was assessed. Materials and methods One hundred healthy subjects from the hospital staff, 0 patients with POAG, and 0 patients with PACG, all attending their routine clinical appointment at the Glaucoma Service at the Clinic of the University of Verona, contributed 300 eyes that were evaluated in a cross-sectional study. Each participant underwent all the measurements in one randomly selected eye. The Institutional Review Board at the University of Verona approved the study protocol and all study procedures conformed to the Declaration of Helsinki for research involving human subjects. After informed consent was obtained, participants underwent a complete ophthalmic examination including a review of medical history, best-corrected visual acuity assessment, slit-lamp examination, gonioscopy, and fundus biomicroscopy with a þ 78 D lens. The inclusion criteria included best-corrected visual acuity of 0.7 or better and the absence of ocular pathologies other than glaucoma. The exclusion criteria included corneal astigmatism higher than 2 D, corneal diseases, microphthalmos, cataract greater than mild lens opacity (according to the Lens Opacity Classification System III), 33 history of intraocular or refractive surgery, ocular inflammation, and contact lens wear. The patients were classified as glaucomatous if they had IOP higher than 21 mmhg before medications, optic disc with typical glaucomatous findings (cup/disc asymmetry between two eyes X0.2, neuroretinal rim thinning, notching, disk haemorrhage or nerve fibre layer defects), repeatable and reliable abnormal visual field results using the automated perimetry performed with the 24-2 Swedish Interactive Threshold Algorithm (HFA; Carl Zeiss Meditec, Dublin, CA, USA). Reliable visual fields were required to have fixation losses, false-positive results, and false-neive results below 20%. An abnormal visual field was defined as a pattern SD with Po5%, glaucoma hemifield test outside normal limits, or both. The 0 healthy participants were enrolled after a complete ophthalmic examination and a thorough history taking, which confirmed no history of previous ocular surgery and the absence of ocular pathologies. The 0 glaucomatous patients affected by POAG were selected from those who were treated only with topical IOP-lowering medications (b-blockers, carbonic anhydrase inhibitors, prostaglandin analogues, a 2 -agonists) and who did not show peripheral anterior synechiae (PAS) after gonioscopy. The 0 patients with PACG were selected from those who were receiving topical miotic therapy (pilocarpine 2%), alone or in association with other antiglaucoma topical medication, who showed PAS, and who had never undergone previous ocular surgery except for peripheral laser iridotomy. Each participant underwent all the subsequent measurements, which were obtained by the same experienced examiner (PC) in one randomly selected eye, in the following order: biometry, tonometry, and pachymetry. AL and CC were both obtained by optical biometry system (IOL Master; Carl Zeiss AG, Feldbach, Switzerland). IOP was measured first as any manipulation to the eye before tonometry (contact ultrasonic pachymetry) could alter the pressure readings. All measurements with GAT (Haag-Streit International, Köniz, Switzerland) and DCT (Pascal dynamic contour tonometer; Swiss Microtechnology AG, Port, Switzerland) tonometer were taken by the same experienced examiner (PC), who was masked to the readings obtained. A different observer (RM) was used to read and record the IOP readings from both to minimize any potential form of bias. IOP was measured with GAT and DCT tonometer in random order, with a 5-min time interval between readings, to avoid the possibility of IOP fluctuation due to diurnal variations. GAT was assembled on a slit lamp (Haag-Streit International) and calibrated according to the manufacturer s guidelines before each participant underwent tonometry.
3 264 Comparison of GAT and DAT in healthy and glaucomatous eyes Three consecutive IOP measurements were obtained (paper strips impregnated with fluorescein were used to stain the precorneal tear film) and averaged. Before each reading, the measuring drum was reset to approximately 6 mmhg. If IOP fluctuated during the cardiac pulse cycle, the measurement was recorded in the maximum of the pulsation amplitude (systolic phase). DCT, which automatically provides digital readout values (IOP; OPA, which is the difference between the minimum and maximum values of the pulsatile IOP wave contour during the cardiac cycle; Q-value, the qualitative score of measurement) on a liquid crystal display, was assembled on the same slit lamp and three consecutive reliable IOP readings were obtained and averaged. The corresponding OPA and Q-values were also recorded and the mean of the three readings were calculated for each eye. Particular attention was paid to standardizing the technique of DCT. The DCT tip contacts the cornea in a manner similar to that of GAT, except that correct positioning on the cornea is confirmed by an audible regular flickering signal that changes in pitch with changes in pressure. In our study, the observer (RM) recorded three consecutive readings for each eye only after she was sure that the examiner (PC) had obtained a correct IOP measurement, according to the following criteria: (1) the interrupting coupling procedure, which allows a correct calculation of the values by the device, was never performed before the audible regular flickering signal emitted at least seven consecutive pulsations; (2) the accuracy of each measurement was judged using the qualitative score provided by the device and all IOP readings were recorded only if the Q-value ranged from 1 to 3 (Q ¼ 1, optimum; Q ¼ 2or3, acceptable; Q ¼ 4, questionable; Q ¼ 5 or 6, repetition recommended). Central corneal thickness was measured with an ultrasonic pachymeter (Pachette DGH 500; DGH Technology Inc., Exton, PA, USA) and the probe was placed on the centre of the cornea, over an undilated pupil, after the administration of topical anaesthesia with oxybuprocaine 0.4%. CCT was measured three times consecutively and the mean of the three readings within a range of ±5 mm was calculated for each eye. Statistical analysis was performed with SPSS statistical software (version 13.0; SPSS Science Inc., Chicago, IL, USA) and data were presented as the mean±sd (Po0.05 was considered significant). The comparison between all the IOP measurements by DCT and GAT was performed using the nonparametric Wilcoxon signed ranked test. Furthermore, Bland Altman plots were used to evaluate the agreement between IOP measurements obtained by DCT and GAT. The difference between measurements obtained by DCT and GAT were plotted against their mean. The method of Bland Altman states that 95% range of agreement should be determined and then judged for its range of clinical significance. 34 To examine the possible effects of pachymetry on the tonometer measurements, patients were stratified according to CCT in intervals (CCT p530 mm (n ¼ 94); CCT between 531 and 560 mm (n ¼ 9); CCT 4560 mm (n ¼ 97)) for statistical analysis purposes. To divide the whole sample into three groups with the same number of eyes, the thirty-third (533 mm) and the sixty-sixth (558.7 mm) percentiles were estimated and used as the cutoff values. Then we assessed the IOP measurement of DCT by comparing it to GAT with respect to multiple CCT and various groups of eyes, using the Student s paired t-test. Linear regression analysis was used to evaluate the influence of ocular structural factors (CCT, CC, AL) and age on IOP measurements obtained with both tonometers. Furthermore, the Pearson s bivariate analysis was assessed by correlating the DIOP (which was obtained by calculating the difference (DCT GAT) of the IOP measurements for each patient and then the average of the 300 differences along with the SD) with the range of both CCT and IOP values in the study population. Linear regression analysis was also used to analyse the effect of CCT, CC, AL, IOP, and age on OPA measurements. Results The study included 300 eyes of 300 Caucasian participants from three different groups. All measurements were obtained on 300 randomly selected eyes. The main characteristics of each group are listed in Table 1. The accuracy of the 900 IOP measurements Table 1 Clinical characteristics of the 300 eyes included in the study Sex (M/F) Age (years) CCT (mm) CC (D) AL (mm) OPA (mmhg) DIOP (mmhg) Healthy (n ¼ 0) 48/52 65± ±27.3 ( ) 43.6±1.8 ( ) 23.8±1.6 ( ) 3.02±1.35 þ 3.1±1.4 POAG (n ¼ 0) 46/ ± ±35.6 ( ) 43.4±2 ( ) 24.4±2.1 ( ) 2.97±1.08 þ 2.6±2.3 PACG (n ¼ 0) 38/ ± ±34.4 ( ) 43.7±1.6 ( ) 22.8±1 ( ) 3.87±1.38 þ 2.1±1.9 AL ¼ axial length; CC ¼ corneal curvature; CCT ¼central corneal thickness; OPA ¼ ocular pulse amplitude; DIOP ¼ mean IOP value by DCT mean IOP value by GAT. The data are presented as the mean±sd (range).
4 Comparison of GAT and DAT in healthy and glaucomatous eyes 265 obtained with DCT in our study was high. The mean Q-value in the whole study sample was 1.9±0.7. The examiner achieved a mean optimum value (Q ¼ 1) in 63.4% of measurements and an acceptable value (Q ¼ 2 or 3) in 36.6% of them. The concordance between the two different techniques was high. Mean IOP values obtained by DCT and GAT were strongly correlated in all eyes (r ¼ 0.93, Po0.001). However, IOP readings were significantly higher with DCT than with GAT. The assessment of the whole study population revealed a DIOP of þ 2.6±1.9 mmhg (range ¼ 4.9 to 8.8 mmhg) (Po0.001). IOP values provided by DCT were higher than those by GAT measurements in 273 eyes (91%), lower in 26 eyes (8.7%), and equal in 1 eye (0.3%). Considering each group separately, the results showed a significantly higher DIOP in normal subjects than in patients with PACG (Po0.001), but not with respect to patients with POAG (Table 1). The Bland Altman plot is shown in Figure 1. These plots allow us to investie the existence of any systematic difference between the measurements. The average of the IOP measurements by the two methods is plotted on the x axis and the difference (DCT GAT) on the y axis. The mean difference is the estimated bias and the SD of the differences measures the random fluctuations around this mean. The plot shows that the mean difference (DCT GAT) is positive and that very few points fall outside the boundary limits (95% range of agreement). DCT - GAT (mmhg) SD 6.6 Mean SD AVERAGE of DCT and GAT (mmhg) Figure 1 Bland Altman plot of the agreement between dynamic contour tonometry (DCT) intraocular pressure (IOP) measurements (mmhg) and Goldmann applanation tonometry (GAT) IOP measurements. The difference between the measurements is plotted against the average of the measurements. Solid line: average of the within person differences of DCT GAT. Broken lines: 95% limits of agreement. The analysis of the IOP measurements obtained by DCT and GAT in the subgroup of eyes whose CCT was within 531 and 560 mm revealed a significant difference only between healthy subjects and patients with PACG (P ¼ 0.009). The evaluation of the two tonometers in the subgroup of eyes with thicker corneas (CCT 4560 mm) showed a significant difference either between normal subjects and patients with POAG (P ¼ 0.001) or between normal subjects and patients with PACG (P ¼ 0.03). On the contrary, the comparison of DCT with GAT in the subgroup of eyes with thinner corneas (CCT p530 mm) failed to show any significant difference between healthy and glaucomatous eyes, either with open-angle or angleclosure phenotypes (Table 2). Furthermore, the Pearson s bivariate analysis was assessed by correlating the DIOP with the range of both CCT and IOP values in the study population. The results revealed a significant reduction of DIOP with increasing CCT (Po0.001) (Figure 2). Considering the values recorded in our limited study population, we found an inverse association between DCT and GAT (IOP readings lower with DCT than with GAT) for CCT values above 620 mm either in healthy or in glaucomatous subjects (Figure 3). We also found a significant decrease of DIOP with an increase in IOP value (Po0.001) (Figure 4). The analysis of the data showed an analogous inversion of the performances of both tonometers for IOP values above 24 mmhg. According to this analysis, we estimated that the difference between the two tonometers decreased 0.7 mmhg per -mm increase in CCT and 0.3 mmhg per 1-mmHg increase in IOP value. Linear regression analysis showed no significant effects of CCT (P ¼ 0.43), CC (P ¼ 0.59), AL (P ¼ 0.41), or age (P ¼ 0.57) on DCT readings. On the contrary, IOP values obtained by GAT depended on CCT (P ¼ 0.001) but were not significantly influenced by CC (P ¼ 0.66), AL (P ¼ 0.77), or age (P ¼ 0.34). The OPA values measured by DCT (range ¼ mmhg) were significantly higher in the eyes with PACG than in either normal eyes (Po0.001) or in eyes with POAG (Po0.001) (Table 1). The linear regression analysis revealed that OPA readings were not affected by CCT Table 2 Distribution of the DIOP (mean±sd, mmhg) in the three groups of subjects (healthy, POAG, PACG) considering the CCT subgroup of value (mm, (n ¼ number of eyes)) CCT Healthy POAG PACG p530 (n ¼ 94) þ 3.7±1.5 þ 4.2±1.8 þ 3.5± (n ¼ 9) þ 2.9±1.3 þ 2.3±2.3 þ 2± (n ¼ 97) þ 2.3±0.9 þ 0.7±1.5 þ 1.3±1.6 CCT ¼central corneal thickness; DCT ¼ dynamic contour tonometry; GAT ¼ Goldmann applanation tonometry; DIOP ¼ mean IOP value by DCT mean IOP value by GAT.
5 266 Comparison of GAT and DAT in healthy and glaucomatous eyes 8 6 DCT - GAT (mmhg) CCT (μm) Figure 2 Scatterplot of DIOP (mean IOP difference between dynamic contour tonometry (DCT) and Goldmann applanation tonometry (GAT) readings) (mmhg) vs CCT (central corneal thickness) (microns) in 300 eyes (r ¼ 0.492; Po0.001). Solid lines: 95% confidence intervals. Broken line: linear regression line. (P ¼ 0.96), CC (P ¼ 0.19), or age (P ¼ 0.09), while the values were influenced by DIOP (Po0.001) and AL (Po0.001). Discussion In this study on healthy and glaucomatous subjects, 300 eyes from three different groups of Caucasian participants were accurately enrolled to create comparable samples (Table 1). We found a high correlation between DCT and GAT measurements and the agreement analysis revealed wide 95% limits of agreement between instruments (Figure 1). However, IOP readings obtained by DCT were 2.6 mmhg higher than those by GAT. Similar results, in spite of different mean values, have been reported by previous investiions. 16,19 21,23 31,35,36 The DIOP between DCT and GAT readings was higher in healthy than in glaucomatous eyes, either with open-angle or angleclosure phenotypes (Table 1). The same outcome has been found by analysing IOP measurements obtained by DCT and GAT in different groups of subjects with the same CCT value, except for POAG subjects with thinner corneas. Furthermore, the significance of DIOP between healthy and glaucomatous eyes intensified with increasing CCT (Table 2). The explanation of this outcome was unclear. Topical IOP-lowering medications could bias the measurements of DCT on glaucomatous eyes. Both histological changes of collagen (due to an upregulation of matrix metalloproteinases) and modification of the corneal endothelial pump function have been reported after the administration of topical antiglaucoma therapy. 37,38 Drug-induced changes of corneal structural properties, such as hydration and rigidity, could explain the different ability of DCT compared to GAT to measure IOP in glaucomatous compared to healthy eyes. This observation requires further confirmation in healthy eyes subjected to manometry. Several studies showed a significantly lower correlation of CCT with DCT than with GAT. 16,28 31 Correspondingly, the present study indicated that DCT readings were statistically independent of CCT, CC, AL, or age. On the contrary, IOP values obtained by GAT depended on CCT but were not significantly influenced by other ocular structural factors and age. Furthermore, the OPA readings were not influenced by CCT, CC, and age but were affected by DIOP and AL. Larger values of OPA were associated with a decrease in the difference between DCT and GAT and a decrease of AL values. These findings explain why OPA values were found to be higher in the glaucomatous patients with angle-closure phenotype (lowest AL) than either normal subjects (median AL) (Po0.001) or glaucomatous patients with open-angle phenotype (highest AL) (Po0.001). For eyes with low values of OPA, DCT
6 Comparison of GAT and DAT in healthy and glaucomatous eyes 267 a IOP (mmhg) G CCT (μm) b 35 IOP (mmhg) c IOP (mmhg) CCT (μm) CCT (μm) Figure 3 Scattergram showing the correlation between mean IOP readings obtained by dynamic contour tonometry (DCT) and Goldmann applanation tonometry (GAT) (mmhg) with increasing CCT (central corneal thickness) value (microns) in healthy subjects (a), patients with POAG (b), and patients with PACG (c). Solid line: linear function of the data for GAT. Broken line: linear function of the data for DCT. measurements tended to be higher than GAT, whereas for eyes with high values of OPA, GAT measurements tended to be higher than DCT. While DCT provides a digital readout of the OPA, which represents the average of the minimum IOP readings during the cardiac cycle (diastolic phase), GAT readings were obtained during the systolic phase. These findings explain why the differences between DCT and GAT were related to OPA. Similar results, in spite of different study populations, have been reported by previous investiions. 39,40 Moreover, we evaluated the performance of DCT over a wide range of CCT and IOP values recorded in our study population. The DIOP between DCT and GAT measurements decreased with an increase in CCT (Figures 2 and 3) and IOP values (Figure 4). This finding is in agreement with other studies that showed that the difference between the tonometers declined as CCT increased. 36,41 On the contrary, only Barleon et al 35 observed that the difference between the two instruments was greatest in eyes with lower IOP value, gradually lessening as IOP increased. Considering the values recorded in our limited study population, we found an inverse association between DCT and GAT for CCT values above 620 mm and IOP values above 24 mmhg. There is evidence of varying bias, as indicated by the slope of the regression line of the differences between the instruments: for smaller CCT and IOP values, DCT measurements tended to be higher than GAT measurements, whereas for higher CCT (4620 mm) and IOP values (424 mmhg), DCT measurements tended to be lower than GAT measurements, whether in healthy or in glaucomatous subjects. The existence of varying bias indicates that the amount of disagreement between the two instruments is not constant throughout
7 268 Comparison of GAT and DAT in healthy and glaucomatous eyes DCT - GAT (mmhg) IOP (mmhg) Figure 4 Correlation between DIOP (mean IOP difference between dynamic contour tonometry (DCT) and Goldmann applanation tonometry (GAT) readings) (mmhg) with increasing IOP value (mmhg) in 300 eyes (r ¼ 0.469; Po0.001). Solid lines: 95% confidence intervals. Broken line: linear function of the data. the range of measurements, but rather varies with the actual measurement. In our study, the wide and varying 95% limits of agreement between DCT and GAT indicated that, although they are highly correlated, measurements should not be used interchangeably. Our study reveals a good overall correlation between DCT and GAT, but the high correlation of 0.93 masks the important systematic difference between these machines and the agreement between instruments differs in high or low IOP ranges. This difference between IOP values from DCT and GAT could be clinically significant and might alter management decisions in some cases. Acknowledgements Piero Ceruti has full access to all the data in the study and takes responsibility of the integrity of the data and the accuracy of the data analysis. We do not have financial interest in any aspect of this study or sources of support. We do not have any commercial or proprietary interest in the product or company. We did not receive payment as a consultant, reviewer, or evaluator. References 1 Whitacre MM, Stein R. Sources of error with use of Goldmann-type tonometers. Surv Ophthalmol 1993; 38: Inoue K, Okugawa K, Oshika T, Amano S. Morphological study of corneal endothelium and corneal thickness in pseudoexfoliation syndrome. Jpn J Ophthalmol 2003; 47: Whitacre MM, Stein RA, Hassanein K. The effect of corneal thickness on applanation tonometry. Am J Ophthalmol 1993; 115: Zadok D, Tran DB, Twa M, Carpenter M, Schanzlin DJ. Pneumotonometry versus Goldmann tonomerty after laser in situ keratomileusis for myopia. J Cataract Refract Surg 1999; 25: Mardelli PG, Piebenga LW, Whitacre MM, Siegmund KD. The effect of excimer laser photorefractive keratectomy on intraocular pressure measurements using the Goldmann applanation tonometer. Ophthalmology 1997; 4: Park HJ, Uhm KB, Hong C. Reduction in intraocular pressure after laser in situ keratomileusis. J Cataract Refract Surg 2001; 27: Rashad KM, Bahnassy AA. Changes in intraocular pressure after laser in situ keratomileusis. J Refract Surg 2001; 17: Duch S, Serra A, Castanera J, Abos R, Quintana M. Tonometry after laser in situ keratomileusis treatment. J Glaucoma 2001; : Fournier AV, Podtetenev M, Lemire J, Thompson P, Duchesne R, Perreault C et al. Intraocular pressure change measured by Goldmann tonometry after laser in situ keratomileusis. J Cataract Refract Surg 1998; 24: Abbasoğlu ÖE, Bowman RW, Cavanagh HD, Cavanagh HD, McCulley JP. Reliability of intraocular pressure measurements after myopic excimer photorefractive keratectomy. Ophthalmology 1998; 5: Garzozi HJ, Chung HS, Yang Y, Kagemann L, Harris A. Intraocular pressure and photorefractive keratectomy; a
8 Comparison of GAT and DAT in healthy and glaucomatous eyes 269 comparison of three different tonometers. Cornea 2001; 20: Shah S, Chatterjee A, Mathai M, Kelly SP, Kwartz J, Henson D et al. Relationship between corneal thickness and measured intraocular pressure in a general ophthalmology clinic. Ophthalmology 1999; 6: Morad Y, Sharon E, Hefetz L, Nemet P. Corneal thickness and curvature in normal-tension glaucoma. Am J Ophthalmol 1998; 76: Copt RP, Thomas R, Mermoud A. Corneal thickness in ocular hypertension, primary open-angle glaucoma, and normal tension glaucoma. Arch Ophthalmol 1999; 117: Brandt JD, Beiser JA, Kass MA, Gordon MO. Central corneal thickness in the Ocular Hypertension Treatment Study (OHTS). Ophthalmology 2001; 8: Kniestedt C, Michelle N, Stamper RL. Dynamic contour tonometry: a comparative study on human cadaver eyes. Arch Ophthalmol 2004; 122: Kanngiesser HE, Robert YCE. Dynamic contour tonometry [ARVO abstract]. Invest Ophthalmol Vis Sci 2002; 43: E-Abstract Burvenich H, Burvenich E, Vincent C. Dynamic contour tonometry (DCT) versus non-contact tonometry (NCT): a comparison study. Bull Soc Belge Ophthalmol 2005; 298: Schneider E, Grehn F. Intraocular pressure measurementfcomparison of dynamic contour tonometry and goldmann applanation tonometry. J Glaucoma 2006; 15: Ku JK, Danesh-Meyer HV, Craig JP, Gamble GD, McGhee CN. Comparison of intraocular pressure measured by Pascal dynamic contour tonometry and Goldmann applanation tonometry. 2006; 20: Pache M, Wilmsmeyer S, Lautebach S, Funk J. Dynamic contour tonometry versus Goldmann applanation tonometry. A comparative study. Graefes Arch Clin Exp Ophthalmol 2005; 243: Hoffmann C, Bachmann LM, Thiel MA. Intraocular pressure using dynamic contour tonometry and contact lens tonometry. BMC Ophthalmol 2004; 4: Kniestedt C, Lin S, Choe J, Nee M, Bostrom A, Stürmer J et al. Correlation between intraocular pressure, central corneal thickness, stage of glaucoma, and demographic patient data: prospective analysis of biophysical parameters in tertiary glaucoma practice population. J Glaucoma 2006; 15: Kotecha A, White ET, Shewry JM, Garway-Heath DF. The relative effects of corneal thickness and age on Goldmann applanation tonometry and dynamic contour tonometry. Br J Ophthalmol 2005; 89: Kniestedt C, Lin S, Choe J, Bostrom A, Nee M, Stamper RL. Clinical comparison of contour and applanation tonometry and their relationship to pachymetry. Arch Ophthalmol 2005; 123: Doyle A, Lachkar Y. Comparison of dynamic contour tonometry with goldmann applanation tonometry over a wide range of central corneal thickness. J Glaucoma 2005; 14: Kniestedt C, Kanngiesser H, Stamper RL. Assessment of Pascal dynamic contour tonometer in monitoring IOP after LASIK. J Cataract Refract Surg 2005; 31: Duba I, Wirthlin AC. Dynamic contour tonometry for post-lasik intraocular pressure measurements. Klin Monastbl Augenheilkd 2004; 221: Siganos DS, Papastergiou GI, Moedas C. Assessment of the Pascal dynamic contour tonometer in monitoring intraocular pressure in unoperated eyes and eyes after LASIK. J Cataract Refract Surg 2004; 30: Kaufmann C, Bachmann LM, Thiel MA. Intraocular pressure measurements using dynamic contour tonometry after laser in situ keratomileusis. Invest Ophthalmol Vis Sci 2003; 44: Kaufmann C, Bachmann LM, Thiel MA. Comparison of dynamic contour tonometry with goldmann applanation tonometry. Invest Ophthalmol Vis Sci 2004; 45: Medeiros FA, Sample PA, Weinreb RN. Comparison of dynamic contour tonometry and Goldmann applanation tonometry in Africa American Subjects. Ophthalmology 2007; 114: Chylack LT, Wolfe JK, Singer DM, Leske MC, Bullimore MA, Bailey IL et al. The lens opacities classification system III. Arch Ophthalmol 1993; 33: Bland JM, Altman DG. Measuring agreement in method comparison studies. Stat Methods Med Res 1999; 8: Barleon L, Hoffmann EM, Berres M, Pfeiffer N, Grus FH. Comparison of dynamic contour tonometry and Goldmann applanation tonometry in glaucoma patients and healthy subjects. Am J Ophthalmol 2006; 142: Francis BA, Hsieh A, Lai MY, Chopra V, Pena F, Azen S et al. Effects of corneal thickness, corneal curvature and intraocular pressure level on Goldmann applanation tonometry and dynamic contour tonometry. Ophthalmology 2007; 114: Viestenz A, Martus P, Schlotzer-Schrehardt U, Langenbucher A, Mardin CY. Impact of prostaglandin- F(2alpha)-analogues and carbonic anhydrase inhibitors on central corneal thicknessfa cross-sectional study on 403 eyes. Klin Monatsnl Augenheilkd 2004; 221: Kaminski S, Hommer A, Koyuncu D, Biowski R, Barisani T, Baumgartner I. Influence of dorzolamide on corneal thickness, endothelial cell count and corneal sensibility. Acta Ophthalmol Scand 1998; 76: Punjabi OS, Ho HK, Kniestedt C, Bostrom AG, Stamper RL, Lin SC. Intraocular pressure and ocular pulse amplitude comparisons in different types of glaucoma using dynamic contour tonometry. Curr Res 2006; 31: Kaufmann C, Bachmann LM, Robert YC, Thiel MA. Ocular pulse amplitude in healthy subjects as measured by dynamic contour tonometry. Arch Ophthalmol 2006; 124: Pache M, Wilmsmeyer S, Lautebach S, Funk J. Dynamic contour tonometry versus Goldmnann applanation tonometry: a comparative study. Graefes Arch Clin Exp Ophthalmol 2005; 243:
INTRODUCTION S. HERDENER, D. HAFIZOVIC, M. PACHE, S. LAUTEBACH, J. FUNK. University Eye Hospital, Freiburg - Germany
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
Dina H. Erickson, O.D., a Denise Goodwin, O.D., a Michael Rollins, O.D., b Amber Belaustegui, O.D., c and Chad Anderson a
 Optometry (2009) 80, 169-174 Comparison of dynamic contour tonometry and Goldmann applanation tonometry and their relationship to corneal properties, refractive error, and ocular pulse amplitude Dina H.
Optometry (2009) 80, 169-174 Comparison of dynamic contour tonometry and Goldmann applanation tonometry and their relationship to corneal properties, refractive error, and ocular pulse amplitude Dina H.
True IOP No Doubt Facts and Figures Figures. Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland
 True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and Julian Garcia-Sanchez METHODS
 Ocular Response Analyzer versus Goldmann Applanation Tonometry for Intraocular Pressure Measurements Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and
Ocular Response Analyzer versus Goldmann Applanation Tonometry for Intraocular Pressure Measurements Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and
Central corneal thickness determined with optical coherence tomography in various types of glaucoma
 Br J Ophthalmol 2000;84:1233 1237 1233 Department of Ophthalmology, Ludwig-Maximilians- University, Munich, Germany M Bechmann M J Thiel B Roesen S Ullrich M W Ulbig K Ludwig Correspondence to: Martin
Br J Ophthalmol 2000;84:1233 1237 1233 Department of Ophthalmology, Ludwig-Maximilians- University, Munich, Germany M Bechmann M J Thiel B Roesen S Ullrich M W Ulbig K Ludwig Correspondence to: Martin
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Laser in situ keratomileusis (LASIK) has
 Changes in Intraocular Pressure After Laser in situ Keratomileusis Khaled M. Rashad, MD; Ahmed A. Bahnassy, MSc, PhD ABSTRACT PURPOSE: To evaluate changes in intraocular pressure (IOP) measurements by
Changes in Intraocular Pressure After Laser in situ Keratomileusis Khaled M. Rashad, MD; Ahmed A. Bahnassy, MSc, PhD ABSTRACT PURPOSE: To evaluate changes in intraocular pressure (IOP) measurements by
Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry
 European Journal of Ophthalmology / Vol. 19 no. 6, 2009 / pp. 936-941 Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry BANU ONCEL,
European Journal of Ophthalmology / Vol. 19 no. 6, 2009 / pp. 936-941 Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry BANU ONCEL,
Central corneal thickness among glaucoma patients attending Menelik II Hospital, Addis Ababa, Ethiopia
 Original article Central corneal thickness among glaucoma patients attending Menelik II Hospital, Addis Ababa, Ethiopia Zelalem Gizachew 1, Abiy Mulugeta 1* Abstract Background: Glaucoma is one of the
Original article Central corneal thickness among glaucoma patients attending Menelik II Hospital, Addis Ababa, Ethiopia Zelalem Gizachew 1, Abiy Mulugeta 1* Abstract Background: Glaucoma is one of the
Central corneal thickness and vascular risk factors in normal tension glaucoma
 Central corneal thickness and vascular risk factors in normal tension glaucoma Aoife Doyle, Ahmed Bensaid and Yves Lachkar L Institut du Glaucome, Fondation Hoˆpital St. Joseph, Paris, France ABSTRACT.
Central corneal thickness and vascular risk factors in normal tension glaucoma Aoife Doyle, Ahmed Bensaid and Yves Lachkar L Institut du Glaucome, Fondation Hoˆpital St. Joseph, Paris, France ABSTRACT.
Correlating central corneal thickness and intraocular pressure in ocular hypertension and glaucoma
 VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer
 518 EXTENDED REPORT Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer P Gunvant, M Baskaran, L Vijaya, I S Joseph, R J Watkins,
518 EXTENDED REPORT Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer P Gunvant, M Baskaran, L Vijaya, I S Joseph, R J Watkins,
Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India
 Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
The Association of Central corneal thickness with Intra-ocular Pressure and Refractive Error in a Nigerian Population
 Peer Reviewed, Open Access, Free Published Quarterly Mangalore, South India ISSN 0972-5997 Volume 6, Issue 3; Jul-Sep 2007 Original Article The Association of Central corneal thickness with Intra-ocular
Peer Reviewed, Open Access, Free Published Quarterly Mangalore, South India ISSN 0972-5997 Volume 6, Issue 3; Jul-Sep 2007 Original Article The Association of Central corneal thickness with Intra-ocular
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
CLINICAL SCIENCES. Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry
 CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
Comparison between Pascal dynamic contour tonometer and Goldmann applanation tonometer after different types of refractive surgery
 DOI 10.1007/s00417-010-1431-9 REFRACTIVE SURGERY Comparison between Pascal dynamic contour tonometer and Goldmann applanation tonometer after different types of refractive surgery Antonios P. Aristeidou
DOI 10.1007/s00417-010-1431-9 REFRACTIVE SURGERY Comparison between Pascal dynamic contour tonometer and Goldmann applanation tonometer after different types of refractive surgery Antonios P. Aristeidou
Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria
 Original Research Article Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria Nkanga DG 1,2, Ibanga AA 1,2, Nkanga ED 2, Etim BA
Original Research Article Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria Nkanga DG 1,2, Ibanga AA 1,2, Nkanga ED 2, Etim BA
CLINICAL SCIENCES. Clinical Significance of Central Corneal Thickness in the Management of Glaucoma
 CLINICAL SCIENCES Clinical Significance of Central Corneal Thickness in the Management of Glaucoma Carolyn Y. Shih, MD; Joshua S. Graff Zivin, PhD; Stephen L. Trokel, MD; James C. Tsai, MD Objective: To
CLINICAL SCIENCES Clinical Significance of Central Corneal Thickness in the Management of Glaucoma Carolyn Y. Shih, MD; Joshua S. Graff Zivin, PhD; Stephen L. Trokel, MD; James C. Tsai, MD Objective: To
Morphological Study of Corneal Endothelium and Corneal Thickness in Pseudoexfoliation Syndrome
 LABORATORY INVESTIGATIONS Morphological Study of Corneal Endothelium and Corneal Thickness in Pseudoexfoliation Syndrome Kenji Inoue*,, Kazuko Okugawa*,, Tetsuro Oshika and Shiro Amano *Department of Ophthalmology,
LABORATORY INVESTIGATIONS Morphological Study of Corneal Endothelium and Corneal Thickness in Pseudoexfoliation Syndrome Kenji Inoue*,, Kazuko Okugawa*,, Tetsuro Oshika and Shiro Amano *Department of Ophthalmology,
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
Clinical Profile of Primary Open Angle Glaucoma Suspects.
 DOI: 10.21276/aimdr.2018.4.2.OT3 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Clinical Profile of Primary Open Angle Glaucoma Suspects. Pradnya Abhinav Mohan 1 1 Fellow Phaco-surgery, Department
DOI: 10.21276/aimdr.2018.4.2.OT3 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Clinical Profile of Primary Open Angle Glaucoma Suspects. Pradnya Abhinav Mohan 1 1 Fellow Phaco-surgery, Department
An Ultra-High-Speed Scheimpflug Camera for Evaluation of Corneal Deformation Response and Its Impact on IOP Measurement
 Glaucoma An Ultra-High-Speed Scheimpflug Camera for Evaluation of Corneal Deformation Response and Its Impact on IOP Measurement Christopher Kai-Shun Leung, 1 Cong Ye, 1 and Robert N. Weinreb 2 1 Department
Glaucoma An Ultra-High-Speed Scheimpflug Camera for Evaluation of Corneal Deformation Response and Its Impact on IOP Measurement Christopher Kai-Shun Leung, 1 Cong Ye, 1 and Robert N. Weinreb 2 1 Department
Changes in Central Corneal Thickness over Time
 Changes in Central Corneal Thickness over Time The Ocular Hypertension Treatment Study James D. Brandt, MD, 1 Mae O. Gordon, PhD, 2 Julia A. Beiser, MS, 2 Shan C. Lin, MD, 3 Monica Y. Alexander, MD, 4
Changes in Central Corneal Thickness over Time The Ocular Hypertension Treatment Study James D. Brandt, MD, 1 Mae O. Gordon, PhD, 2 Julia A. Beiser, MS, 2 Shan C. Lin, MD, 3 Monica Y. Alexander, MD, 4
Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure
 Ophthalmology, Article ID 461681, 5 pages http://dx.doi.org/1.1155/214/461681 Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure Yuta Sakaue,
Ophthalmology, Article ID 461681, 5 pages http://dx.doi.org/1.1155/214/461681 Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure Yuta Sakaue,
Elevated intraocular pressure (IOP) is the most important. The Effect of Trabeculectomy on Ocular Pulse Amplitude. Glaucoma
 Glaucoma The Effect of Trabeculectomy on Ocular Pulse Amplitude Christophe Breusegem, 1 Steffen Fieuws, 2 Thierry Zeyen, 1 and Ingeborg Stalmans 1 PURPOSE. To investigate whether trabeculectomy, besides
Glaucoma The Effect of Trabeculectomy on Ocular Pulse Amplitude Christophe Breusegem, 1 Steffen Fieuws, 2 Thierry Zeyen, 1 and Ingeborg Stalmans 1 PURPOSE. To investigate whether trabeculectomy, besides
Central Corneal Thickness in Primary Angle Closure and Open Angle Glaucoma
 Original Article Central Corneal Thickness in Primary Angle Closure and Open Angle Glaucoma Sasan Moghimi 1,2, MD; Hamidreza Torabi 1, MD; Hesam Hashemian 1, MD; Heydar Amini 1, MD; Shan Lin 2, MD 1 Department
Original Article Central Corneal Thickness in Primary Angle Closure and Open Angle Glaucoma Sasan Moghimi 1,2, MD; Hamidreza Torabi 1, MD; Hesam Hashemian 1, MD; Heydar Amini 1, MD; Shan Lin 2, MD 1 Department
Refractive corneal surgery (RCS) using a laser, such as. Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery.
 Glaucoma Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery Yoon Jeon Kim, 1 Sung-Cheol Yun, 2 Jung Hwa Na, 3 Hung Won Tchah, 1 Jong Jin Jung, 3 and Kyung Rim Sung 1 PURPOSE. To
Glaucoma Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery Yoon Jeon Kim, 1 Sung-Cheol Yun, 2 Jung Hwa Na, 3 Hung Won Tchah, 1 Jong Jin Jung, 3 and Kyung Rim Sung 1 PURPOSE. To
Analysis of differences in intraocular pressure evaluation performed with contact and non-contact devices
 Lanza et al. BMC Ophthalmology (2018) 18:233 https://doi.org/10.1186/s12886-018-0900-5 RESEARCH ARTICLE Open Access Analysis of differences in intraocular pressure evaluation performed with contact and
Lanza et al. BMC Ophthalmology (2018) 18:233 https://doi.org/10.1186/s12886-018-0900-5 RESEARCH ARTICLE Open Access Analysis of differences in intraocular pressure evaluation performed with contact and
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
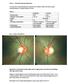 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev S.K., Dr. Med. Sc., Prof.; Lazar Yu.M., Cand. Med. Sc.; Tatarina Yu.A., Junior Research Fellow
 Changes in corneoscleral rigidity and corneal thickness at various target intraocular pressures in patients with stabilized primary open-angle glaucoma Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev
Changes in corneoscleral rigidity and corneal thickness at various target intraocular pressures in patients with stabilized primary open-angle glaucoma Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev
Diabetes, Hyperglycemia, and Central Corneal Thickness
 Diabetes, Hyperglycemia, and Central Corneal Thickness The Singapore Malay Eye Study Daniel H. W. Su, MMed(Ophth), FRCS(Ed), 1 Tien Y. Wong, PhD, FRCS(Ed), 1,2,3 Wan-Ling Wong, BSc, 1 Seang-Mei Saw, PhD,
Diabetes, Hyperglycemia, and Central Corneal Thickness The Singapore Malay Eye Study Daniel H. W. Su, MMed(Ophth), FRCS(Ed), 1 Tien Y. Wong, PhD, FRCS(Ed), 1,2,3 Wan-Ling Wong, BSc, 1 Seang-Mei Saw, PhD,
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (8), Page
 The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (8), Page 1371-1376 Relationship Between Corneal Astigmatism and Intraocular Pressure Abdulrahman E. Algarni 1, Mohammad Abahussin 2, Nuha
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (8), Page 1371-1376 Relationship Between Corneal Astigmatism and Intraocular Pressure Abdulrahman E. Algarni 1, Mohammad Abahussin 2, Nuha
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial
 Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements
 Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
Original article Comparative evaluation of time domain and spectral domain optical coherence tomography in retinal nerve fiber layer thickness measurements Dewang Angmo, 1 Shibal Bhartiya, 1 Sanjay K Mishra,
CLINICAL SCIENCES. Comparison of Ocular Response Analyzer Parameters in Chinese Subjects With Primary Angle-Closure and Primary Open-Angle Glaucoma
 CLINICAL SCIENCES Comparison of Ocular Response Analyzer Parameters in Chinese Subjects With Primary Angle-Closure and Primary Open-Angle Glaucoma Arun Narayanaswamy, DNB; Daniel H. Su, FRCS(Edin); Mani
CLINICAL SCIENCES Comparison of Ocular Response Analyzer Parameters in Chinese Subjects With Primary Angle-Closure and Primary Open-Angle Glaucoma Arun Narayanaswamy, DNB; Daniel H. Su, FRCS(Edin); Mani
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
CLINICAL SCIENCES. Ocular Pulse Amplitude in Healthy Subjects as Measured by Dynamic Contour Tonometry
 CLINICAL SCIENCES Ocular Pulse Amplitude in Healthy Subjects as Measured by Dynamic Contour Tonometry Claude Kaufmann, MD; Lucas M. Bachmann, MD, PhD; Yves C. Robert, MD; Michael A. Thiel, MD, PhD Objectives:
CLINICAL SCIENCES Ocular Pulse Amplitude in Healthy Subjects as Measured by Dynamic Contour Tonometry Claude Kaufmann, MD; Lucas M. Bachmann, MD, PhD; Yves C. Robert, MD; Michael A. Thiel, MD, PhD Objectives:
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
NIIOS. Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece VASILIS S.
 Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece Goldman applanation tonometry is still the gold standard for measuring IOP, but its accuracy is
Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece Goldman applanation tonometry is still the gold standard for measuring IOP, but its accuracy is
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Central corneal thickness and normal tension glaucoma: A cross-sectional study
 Optometry (2006) 77, 134-140 Central corneal thickness and normal tension glaucoma: A cross-sectional study Michael Sullivan-Mee, O.D., a Kathy D. Halverson, O.D., a Mollie C. Saxon, O.D., a Glenn B. Saxon,
Optometry (2006) 77, 134-140 Central corneal thickness and normal tension glaucoma: A cross-sectional study Michael Sullivan-Mee, O.D., a Kathy D. Halverson, O.D., a Mollie C. Saxon, O.D., a Glenn B. Saxon,
Kobe University Repository : Kernel
 Kobe University Repository : Kernel タイトル Title 著者 Author(s) 掲載誌 巻号 ページ Citation 刊行日 Issue date 資源タイプ Resource Type 版区分 Resource Version 権利 Rights DOI JaLCDOI URL Agreement of Rebound Tonometer in Measuring
Kobe University Repository : Kernel タイトル Title 著者 Author(s) 掲載誌 巻号 ページ Citation 刊行日 Issue date 資源タイプ Resource Type 版区分 Resource Version 権利 Rights DOI JaLCDOI URL Agreement of Rebound Tonometer in Measuring
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Comparison of Central Corneal Thickness Measurements with Pentacam, Orbscan II, and Ultrasound Pachymeter
 Comparison of Central Corneal Thickness Measurements with Pentacam, Orbscan II, and Ultrasound Pachymeter Abbas-Ali Yekta, PhD 1 Hassan Hashemi, MD 2,3 Mehdi KhabazKhoob, MSc 3 Asghar Dostdar, MSc 4 Shiva
Comparison of Central Corneal Thickness Measurements with Pentacam, Orbscan II, and Ultrasound Pachymeter Abbas-Ali Yekta, PhD 1 Hassan Hashemi, MD 2,3 Mehdi KhabazKhoob, MSc 3 Asghar Dostdar, MSc 4 Shiva
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
1 Birmingham and Midland Eye Centre, City Hospital, Birmingham, 2 Ophthalmic Research Group, Life and Health Sciences, Aston
 Accuracy of Goldmann, Ocular Response Analyser, Pascal and TonoPen XL Tonometry in Keratoconic and Normal Eyes Susan P Mollan MB CHB MRCOphth 1, James S Wolffsohn BSc PhD PgDip MCOptom 2, Maged Nessim
Accuracy of Goldmann, Ocular Response Analyser, Pascal and TonoPen XL Tonometry in Keratoconic and Normal Eyes Susan P Mollan MB CHB MRCOphth 1, James S Wolffsohn BSc PhD PgDip MCOptom 2, Maged Nessim
Clinical Study Differences between Goldmann Applanation Tonometry and Dynamic Contour Tonometry following Trabeculectomy
 Ophthalmology Volume 2010, Article ID 357387, 5 pages doi:10.1155/2010/357387 Clinical Study Differences between Goldmann Applanation Tonometry and Dynamic Contour Tonometry following Trabeculectomy Efstathios
Ophthalmology Volume 2010, Article ID 357387, 5 pages doi:10.1155/2010/357387 Clinical Study Differences between Goldmann Applanation Tonometry and Dynamic Contour Tonometry following Trabeculectomy Efstathios
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Assessing the Relationship between Central Corneal Thickness and Retinal Nerve Fiber Layer Thickness in Healthy Subjects
 1 1 1 1 1 1 Assessing the Relationship between Central Corneal Thickness and Retinal Nerve Fiber Layer Thickness in Healthy Subjects Authors: Tarkan Mumcuoglu, 1* Kelly A Townsend, 1* Gadi Wollstein, 1
1 1 1 1 1 1 Assessing the Relationship between Central Corneal Thickness and Retinal Nerve Fiber Layer Thickness in Healthy Subjects Authors: Tarkan Mumcuoglu, 1* Kelly A Townsend, 1* Gadi Wollstein, 1
Accuracy and Repeatability of a New Portable Ultrasound Pachymeter
 Accuracy and Repeatability of a New Portable Ultrasound Pachymeter Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of Physics (Optometry), School
Accuracy and Repeatability of a New Portable Ultrasound Pachymeter Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of Physics (Optometry), School
A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT) Retinal Nerve Fiber Layer Measurements Based on Time Domain OCT Measurements
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(5):369-377 http://dx.doi.org/10.3341/kjo.2012.26.5.369 Original Article A Formula to Predict Spectral Domain Optical Coherence Tomography (OCT)
INTRODUCTION MIKLOS SCHNEIDER 1, GABOR BORGULYA 2, ANDRAS SERES 1, ZOLTAN Z. NAGY 1, JANOS NEMETH 1
 European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 180-187 Central corneal thickness measurements with optical coherence tomography and ultrasound pachymetry in healthy subjects and in patients
European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 180-187 Central corneal thickness measurements with optical coherence tomography and ultrasound pachymetry in healthy subjects and in patients
Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma
 SCIENTIFIC REPORT Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma P Fogagnolo, L Rossetti, F Mazzolani, N Orzalesi... Br J Ophthalmol ;9:. doi: 1.113/bjo.5.795
SCIENTIFIC REPORT Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma P Fogagnolo, L Rossetti, F Mazzolani, N Orzalesi... Br J Ophthalmol ;9:. doi: 1.113/bjo.5.795
Investigation of the relationship between central corneal thickness and retinal nerve fiber layer thickness in ocular hypertension
 Acta Medica Anatolia Volume 2 Issue 1 2014 Investigation of the relationship between central corneal thickness and retinal nerve fiber layer thickness in ocular hypertension Remzi Mısır 1, Sinan Sarıcaoğlu
Acta Medica Anatolia Volume 2 Issue 1 2014 Investigation of the relationship between central corneal thickness and retinal nerve fiber layer thickness in ocular hypertension Remzi Mısır 1, Sinan Sarıcaoğlu
Interest in central corneal thickness (CCT) and glaucoma was. Central Corneal Thickness and Glaucoma in East Asian People.
 Glaucoma Central Corneal Thickness and Glaucoma in East Asian People Alexander C. Day, 1,2 David Machin, 3 Tin Aung, 4 Gus Gazzard, 2 Rahat Husain, 4 Paul T. K. Chew, 5 Peng T. Khaw, 1,2,6 Steve K. L.
Glaucoma Central Corneal Thickness and Glaucoma in East Asian People Alexander C. Day, 1,2 David Machin, 3 Tin Aung, 4 Gus Gazzard, 2 Rahat Husain, 4 Paul T. K. Chew, 5 Peng T. Khaw, 1,2,6 Steve K. L.
THE TAMILNADU DR.M.G.R. MEDICAL UNIVERSITY CHENNAI, TAMILNADU
 A STUDY ON COMPARISON OF CENTRAL CORNEAL THICKNESS IN NORMALS, PRIMARY OPEN ANGLE GLAUCOMA AND OCULAR HYPERTENSIVES DISSERTATION SUBMITTED FOR MASTER OF SURGERY DEGREE BRANCH III - OPHTHALMOLOGY APRIL
A STUDY ON COMPARISON OF CENTRAL CORNEAL THICKNESS IN NORMALS, PRIMARY OPEN ANGLE GLAUCOMA AND OCULAR HYPERTENSIVES DISSERTATION SUBMITTED FOR MASTER OF SURGERY DEGREE BRANCH III - OPHTHALMOLOGY APRIL
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
STANDARD AUTOMATED PERIMETRY IS A GENERALLY
 Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Central Cornea Thickness in Glaucoma and Non- Glaucoma African Population
 Ophthalmology Research: An International Journal 6(4): 1-8, 2016; Article no.or.31121 ISSN: 2321-7227 SCIENCEDOMAIN international www.sciencedomain.org Central Cornea Thickness in Glaucoma and Non- Glaucoma
Ophthalmology Research: An International Journal 6(4): 1-8, 2016; Article no.or.31121 ISSN: 2321-7227 SCIENCEDOMAIN international www.sciencedomain.org Central Cornea Thickness in Glaucoma and Non- Glaucoma
PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY
 ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
Based on the studies by Goldmann and Schmidt 1 and Ehlers. Central Corneal Thickness Correlated with Glaucoma Damage and Rate of Progression
 Central Corneal Thickness Correlated with Glaucoma Damage and Rate of Progression Jost B. Jonas, 1,2 Andrea Stroux, 3,4 Isabel Velten, 1 Anselm Juenemann, 1 Peter Martus, 3 and Wido M. Budde 1,2 PURPOSE.
Central Corneal Thickness Correlated with Glaucoma Damage and Rate of Progression Jost B. Jonas, 1,2 Andrea Stroux, 3,4 Isabel Velten, 1 Anselm Juenemann, 1 Peter Martus, 3 and Wido M. Budde 1,2 PURPOSE.
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
4/06/2013. Medication Observation POAG. Proportion. Native American 0.1% 0.4%
 Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC)
 Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
Dada T et al Original article Evaluation of retinal nerve fiber layer thickness parameters in myopic population using scanning laser polarimetry (GDxVCC) Dada T1, Aggarwal A1, Bali SJ2, Sharma A1, Shah
Intraocular pressure (IOP) is of fundamental importance in
 Glaucoma Effect of Corneal Stiffening on Goldmann Applanation Tonometry and Tono-Pen Measurements in Canine Eyes Junhua Tang, 1 Xueliang Pan, 2 Paul A. Weber, 3 and Jun Liu 1,3 PURPOSE. To experimentally
Glaucoma Effect of Corneal Stiffening on Goldmann Applanation Tonometry and Tono-Pen Measurements in Canine Eyes Junhua Tang, 1 Xueliang Pan, 2 Paul A. Weber, 3 and Jun Liu 1,3 PURPOSE. To experimentally
Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach
 ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
The changes in corneal biomechanical parameters after phototherapeutic keratectomy in eyes with granular corneal dystrophy
 (2009) 23, 1790 179 & 2009 Macmillan Publishers Limited All rights reserved 090-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY The changes in corneal biomechanical parameters after phototherapeutic keratectomy
(2009) 23, 1790 179 & 2009 Macmillan Publishers Limited All rights reserved 090-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY The changes in corneal biomechanical parameters after phototherapeutic keratectomy
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
CLINICAL SCIENCES. tonometry (GAT) has become the gold standard against which other tonometers
 CLINICAL SCIENCES Dynamic Contour Tonometry A Comparative Study on Human Cadaver Eyes Christoph Kniestedt, MD; Michelle Nee, MD; Robert L. Stamper, MD Objective: To compare intraocular pressure measurements
CLINICAL SCIENCES Dynamic Contour Tonometry A Comparative Study on Human Cadaver Eyes Christoph Kniestedt, MD; Michelle Nee, MD; Robert L. Stamper, MD Objective: To compare intraocular pressure measurements
Comparison of a New Non-Contact Tonometer with Goldmann Applanation
 Eye (1989) 3, 332-337 Comparison of a New Non-Contact Tonometer with Goldmann Applanation M. J. MOSELEY, N. M. EVANS and A. R. FIELDER Leicester Summary A comparison of a new non-contact tonometer (Keeler
Eye (1989) 3, 332-337 Comparison of a New Non-Contact Tonometer with Goldmann Applanation M. J. MOSELEY, N. M. EVANS and A. R. FIELDER Leicester Summary A comparison of a new non-contact tonometer (Keeler
LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS. Darshana Soma
 LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS Darshana Soma A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, in partial
LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS Darshana Soma A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, in partial
Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure Glaucoma
 Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
RETINAL NERVE FIBER LAYER
 CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
CLINICAL SCIENCES The Effect of Scan Diameter on Retinal Nerve Fiber Layer Thickness Measurement Using Stratus Optic Coherence Tomography Giacomo Savini, MD; Piero Barboni, MD; Michele Carbonelli, MD;
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma
 Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Present relevant clinical findings of four landmark glaucoma trials OHTS, EMGT, CNTGS and CIGTS.
 Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Comparison of Intraocular Pressure Measurements by the Ocular Response Analyzer and Goldmann Applanation Tonometer after Penetrating Keratoplasty
 Comparison of Intraocular Pressure Measurements by the Ocular Response Analyzer and Goldmann Applanation Tonometer after Penetrating Keratoplasty in Keratoconic Patients Sepehr Feizi, MD 1 Mohammad Pakravan,
Comparison of Intraocular Pressure Measurements by the Ocular Response Analyzer and Goldmann Applanation Tonometer after Penetrating Keratoplasty in Keratoconic Patients Sepehr Feizi, MD 1 Mohammad Pakravan,
C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma
 접수번호 : 2008-099 Korean Journal of Ophthalmology 2009;23:193-197 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.193 C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma Jaewan
접수번호 : 2008-099 Korean Journal of Ophthalmology 2009;23:193-197 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.3.193 C-reactive Protein and Lipid Profiles in Korean Patients With Normal Tension Glaucoma Jaewan
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Retinal Nerve Fiber Layer and Central Corneal Thickness in Patients with Exfoliation Syndrome
 Retinal Nerve Fiber Layer and Central Corneal Thickness in Patients with Exfoliation Syndrome Rana Sorkhabi, MD 1 Mohammad Bagher Rahbani, MD 2 Mohammad Hosein Ahoor, MD 2 Vahide Manoochehri, MD 3 Abstract
Retinal Nerve Fiber Layer and Central Corneal Thickness in Patients with Exfoliation Syndrome Rana Sorkhabi, MD 1 Mohammad Bagher Rahbani, MD 2 Mohammad Hosein Ahoor, MD 2 Vahide Manoochehri, MD 3 Abstract
A comparison of HRT II and GDx imaging for glaucoma detection in a primary care eye clinic setting
 (2007) 21, 1050 1055 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye CLINICAL STUDY A comparison of HRT II and GDx imaging for glaucoma detection in a primary
(2007) 21, 1050 1055 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye CLINICAL STUDY A comparison of HRT II and GDx imaging for glaucoma detection in a primary
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Correspondence should be addressed to Fusako Fujimura;
 BioMed Research International Volume 2013, Article ID 370592, 5 pages http://dx.doi.org/10.1155/2013/370592 Research Article Repeatability and Reproducibility of Measurements Using a NT-530P Noncontact
BioMed Research International Volume 2013, Article ID 370592, 5 pages http://dx.doi.org/10.1155/2013/370592 Research Article Repeatability and Reproducibility of Measurements Using a NT-530P Noncontact
Elevated intraocular pressure (IOP) is a major risk factor for
 Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Clinical Guidance and Monitoring for Change. Cecilia Fenerty MD FRCOphth Manchester Royal Eye Hospital
 Clinical Guidance and Monitoring for Change Cecilia Fenerty MD FRCOphth Manchester Royal Eye Hospital Glaucoma Referral Criteria 2000 Original referral scheme Simple criteria based on IOP/Disc/Field Solitary
Clinical Guidance and Monitoring for Change Cecilia Fenerty MD FRCOphth Manchester Royal Eye Hospital Glaucoma Referral Criteria 2000 Original referral scheme Simple criteria based on IOP/Disc/Field Solitary
Discrimination between normal and glaucomatous eyes with visual field and scanning laser polarimetry measurements
 586 Glaucoma Service, Department of Ophthalmology, University of Campinas, Campinas, Brazil R Lauande-Pimentel R A Carvalho H C Oliveira D C Gonçalves L M Silva V P Costa Glaucoma Service, Department of
586 Glaucoma Service, Department of Ophthalmology, University of Campinas, Campinas, Brazil R Lauande-Pimentel R A Carvalho H C Oliveira D C Gonçalves L M Silva V P Costa Glaucoma Service, Department of
Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification
 Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
The Ocular Response Analyzer (ORA; Reichert Ophthalmic
 Glaucoma Lack of Association Between Corneal Hysteresis and Corneal Resistance Factor With Glaucoma Severity in Primary Angle Closure Glaucoma Monisha E. Nongpiur, 1,2 Owen Png, 2 Jestin W. Chiew, 3 Kenric
Glaucoma Lack of Association Between Corneal Hysteresis and Corneal Resistance Factor With Glaucoma Severity in Primary Angle Closure Glaucoma Monisha E. Nongpiur, 1,2 Owen Png, 2 Jestin W. Chiew, 3 Kenric
Make a more confident glaucoma risk assessment with Corneal Hysteresis, a superior predictor of glaucoma progression.
 Make a more confident glaucoma risk assessment with Corneal Hysteresis, a superior predictor of glaucoma progression. Advancing Eye Care. American Innovation. Reichert Ocular Response Analyzer G3. Make
Make a more confident glaucoma risk assessment with Corneal Hysteresis, a superior predictor of glaucoma progression. Advancing Eye Care. American Innovation. Reichert Ocular Response Analyzer G3. Make
S Morishita, T Tanabe, S Yu, M Hangai, T Ojima, H Aikawa, N Yoshimura. Clinical science
 Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
Department of Ophthalmology and Visual Sciences, Kyoto University Graduate School of Medicine, Kyoto, Japan Correspondence to: Dr T Tanabe, Department of Ophthalmology, The Tazuke Kofukai Medical Institute,
