Prospective evaluation of cerebral angiography and computed tomography in cerebral haematoma
|
|
|
- Sara Cannon
- 5 years ago
- Views:
Transcription
1 180 10ournal ofneurology, Neurosurgery, and Psychiatry 1994;57: Neuroradiology, Atkinson Morley's Hospital, London SW20 ONE, UK S F S Halpin J A Britton A Clifton G Hart Neuroradiology, Radcliffe Infirmary, Woodstock Road, Oxford, UK J V Byrne Neurosurgery, Atkinson Morley's Hospital, London SW20 ONE, UK A Moore Correspondence to: Dr S F S Halpin, Neuroradiology, University Hospital of Wales, Health Park, Cardiff CF4 4XW, UK. Received 16 August 1993 and in revised form 17 March Accepted 10 May 1994 Prospective evaluation of cerebral angiography and computed tomography in cerebral haematoma S F S Halpin, J A Britton, J V Byrne, A Clifton, G Hart, A Moore Abstract One hundred and two consecutive patients with cerebral haematoma were prospectively allocated to one of two groups according to their CT on admission. Group 1 patients were thought to have a high probability of an underlying structural lesion and underwent cerebral angiography acutely. If normal, this was repeated at three months. Group 2 patients were thought not to have such a lesion and underwent angiography at three months. Patients older than the mean age of the study population, and hypertensive patients were much less likely to harbour an aneurysm or malformation than younger or normotensive patients (p < 0-01; sensitivity 87-9%, specificity 88.6%). An aneurysm or malformation was the cause of haemorrhage in 12-8% of hypertensive patients, in 309% of patients with haematoma involving the basal ganglia, and 18-2% of those with posterior fossa haemorrhage. Features of CT in isolation give a sensitivity of 77-2% and a specificity of 84-2%. Follow up angiography in group 1 showed an malformation in one of seven patients in whom the original study was normal. These results contrast sharply with data from previous retrospective studies. The decision to investigate a patient with cerebral haematoma should be primarily based on the patient's clinical condition, rather than on the site of haemorrhage. (7 Neurol Neurosurg Psychiatry 1994;57: ) Stroke is caused by spontaneous cerebral haemorrhage in 4% to 119% of patients"2 although rates of up to 40% have been quoted.3 Acute mortality ranges from 18 % to 75%, depending on the size and position of the haematoma and the age and clinical condition of the patient.'45 To prevent recurrence, it is important to identify patients in whom haemorrhage is secondary to an underlying structural lesion, such as an aneurysm, vascular malformation, or tumour. Pathological studies have indicated that primary haemorrhage is most likely to occur in certain sites-in particular the basal ganglia and posterior fossa.6 Factors such as -age, pre-existing systemic hypertension, and haematoma location are commonly employed in selecting patients for angiography. The influence of clinical features and CT on final diagnosis has been described retrospectively,7-" but to our knowledge there has been no prospective angiographic assessment in life of the relative frequency of primary and secondary haemorrhage in patients with cerebral haematoma. Methods All patients presenting consecutively to this hospital between 1989 and 1992 with spontaneous cerebral haematoma were entered into the study. They were assigned to one of two groups after evaluation of their CT on admission by two or three consultant neuroradiologists. If the haematoma was thought likely to be due to an underlying structural cause, angiography was carried out as soon as the patient's condition allowed, and was repeated three months later if negative (group 1). If, however, such a lesion was not suspected, angiography was delayed by three months (group 2). The radiologists were unaware of clinical details other than the patients' ages before assessing the admission CT. Clinical information was recorded for each patient after the CT assessment was made. Patients were declared hypertensive only if there was a documented history of systolic pressures greater than 140 mm Hg or diastolic pressures greater than 90 mm Hg; if there was clinical evidence of longstanding systemic hypertension such as hypertensive retinopathy; or if such hypertension continued from admission to at least two weeks into the post-ictal period. The CT features used to assign patients to each group were the presence or absence of intraventricular or subarachnoid blood, calcification, or prominent vessels, and the site of haemorrhage. Contrast enhancement was not used in the initial assessment. Patients with predominantly subarachnoid haemorrhage were excluded from the study, as were those with a history of trauma. Angiography was carried out via the femoral artery, with selective injections made into -those vessels appropriate to the potential blood supply of the site of the haematoma: most commonly this required ipsilateral internal, and sometimes external, carotid artery injections, and a vertebral arterial study. If an abnormality was found, the examination was extended as clinically appropriate. Full informed consent was obtained from all patients before they were entered into the
2 Prospective evaluation of cerebral angiography and computed tomography in cerebral haematoma study, which was approved by the hospital ethics committee. A X2 test with Yates' correction was used for statistical analysis. Results One hundred and two patients entered the study (62 males, mean age 49-2 y (range 7-71) years and 40 females, mean age 46-4 (range years). Table 1 presents the Table 1 No ofpatients Angiographic findings Diagnosis 11 Aneurysms 31 Arteriovenous malformations 1 Glioma 1 Metastasis 38 No structural lesion found Table 2 Table 3 Patients wrongly asigned to group 2 Patients who did not complete the protocol No of Hypertensivel patients Age other details Site of blood Severe hypertension Basal ganglia 1 30 Eclampsia Frontal/basal 1 60 Haematoma after Basal ganglia streptokinase infusion for mycocardial infarct 1 68 Massive haemorrhagic Middle cerebral infarct territory 1 18 Previously well Basal ganglia 1 12 Previously well Intraventricular 1 35 Dysmorphic facies Frontal 1 65 Overdose of warfarin Frontal (INR 4 2). Atrial fibrillation 1 58 Alcoholic with liver Basal ganglia disease 1 37 Drug abuser with Frontal alcohol cirrhosis 1 70 Previously healthy Basal ganglia 2 45, 58 Bled into tumour Frontal, parietal INR = International normalised ratio. No of Clinical patients Age details Site of blood Finding Hypertensive Basal ganglia AVM or post fossa Normotensive Basal ganglia or AVM parieto-occipital 1 45 NHL with low Basal ganglia/ PCom A platelets on frontal chemotherapy 1 65 History of Temporoparietal MCA DXT for glioma Sylvian 1 52 Presented one Parietal AVM month after haemorrhage 1 23 Normotensive Frontoparietal AVM + IVH 1 66 Normotensive Basal ganglia Cavernous haemangioma Positive angiographic findings in 10 patients whose initial CT did not suggest an underlying structural lesion. AVM = malformation; PCom A = posterior communicating artery aneurysm; NHL = non-hodgkin's lymphoma; DXT = radiotherapy; MCA = middle cerebral artery aneurysm; AVH = intraventricular haemorrhage. Table 4 Influence of blood pressure on angiographic findings A VM Aneurysm Incomplete Primary Tumour Normotensive 28 (50-1) 8 (14 5) 7 (12-7) 10 (18-2) 2 (3 6) Hypertensive 3 (6 4) 3 (6 4) 13 (27 7) 28 (59-6) 0 Number of haemorrhages due to structure and non-structural causes in 47 hypertensive, and 55 normotensive patients. Figures in parentheses are percentages of the subgroup. final diagnoses. Twenty two patients did not complete the full protocol, mostly because they were considered unfit for angiography or to undergo treatment should a causative lesion be found (12 patients). Four patients refused follow up angiography and four died without a postmortem during the study period. Two patients had an obvious tumour on initial CT (one oligodendroglioma and one metastasis); they did not have angiography, and are therefore considered as not having completed the protocol. Table 2 gives details of these 22 patients. Seven haematomas were evacuated before angiography. At operation, three malformations and one aneurysm were discovered; no causative lesion was found in the other three patients at surgery or at angiography three months later. Thirty eight of 44 patients assigned to group 1 completed the protocol. Angiography showed causative malformations in 23 and aneurysms in nine. In one patient, CT showed an underlying tumour. Angiography was not performed and an oligodendroglioma was confirmed by biopsy. In another patient, with known melanoma, the haematoma was in association with several other lesions typical of metastases, and CT follow up confirmed a metastasis at the site of the haematoma. No abnormality was found in six patients, four of whom were aged under 35 and had frontal, frontotemporal, or temporoparietal haematomas. One 52 year old patient had a temporoparietal haematoma in association with subarachnoid blood, and one 48 year old hypertensive patient had a basal ganglia haemorrhage. Four patients in group 1 had an initial angiogram that showed only mass effect, and these patients failed to attend for further angiography. Forty two of 58 patients assigned to group 2 completed the protocol. Angiography showed an malformation in eight and an aneurysm in two. No abnormality was found at delayed angiography in 32. Table 3 presents the data for the 10 patients from group 2 in whom an angiographic structural lesion was found. Table 4 details the findings in patients with normal and raised blood pressure. Forty seven per cent of all patients were hypertensive. There was a highly significant difference between the two (p < 0-001) relative to finding a structural lesion by chance. The influence of age was assessed by separating the patients into two cohorts: those above and those below the mean age of the study population. There was a highly significant difference between the two age groups (p < 0-01). Table 5 details the angiographic findings. There was an even greater discrepancy (p < 0 01) when the results were compared between those who were hypertensive and older than the mean age of the study, and those who were normotensive and below the mean age (table 5). The combination of age and blood pressure in predicting the presence of a structural lesion at angiography gave a sensitivity of 87-9%, and a specificity of
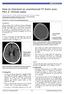
3 1182~~~~~~~~~~~~~~~~~~~~~~~~Halpin, 1182 Britton, Byrne, Clifton, Hart, Moore Table 5 Influence of age and blood pressure on angiographic findings Structural lesion No structural lesion Old patients (n = 39) 12 (30-8) 27 (69-2) Young patients (n = 43) 32 (74-4) 11 (25-6) Old hypertensive patients (n = 35) 4 (11) 31 (89) Young normotensive patients (n = 35) 29 (83) 6 (17) Angiographic findings in patients aged greater than the mean age of the study (old) and patients aged less than this (young) and the findings in hypertensive patients older than 47 and those in normotensive patients younger than 47. Figures in parentheses are the percentage of the subgroup. Table 6 Influence of site of blood on angiographic findings A VM Aneurysnm Inconmplete NVo lesionl Frontal (n = 23) 7 (35) 6 (30) 4 (20) 6 (30) Temporal (n = 34) 14 (41-2) 7 (20-6) 1 (2-9) 12 (35-3) Parietal (n = 3 1) 10 (32-3) 3 (9-7) 4 (12-4) 14 (45-2) Occipital (n = 6) 1 (16-7) 0 1 (16-7) 4 (66-7) Basal ganglia (n = 26) 6 (23-1) 2 (7-8) 10 (38-4) 8 (30-1) Post fossa (n= 11) 2 (18-2) 0 4 (36-4) 5 (45-5) Sylvian (n = 14) 6 (43) 6 (43) 1 (7) 1 (7) Ventricles (n = 3) 2 (66) 0 1 (33) 0 IVH (n =38) 1 1(29) 4 (11) 9 (24) 14 (3637) IVH + SAH (n = 8) 2 (25) 3 (37) 1 (12) 2 (25) IVH-SAH (n =30) 9 (30) 1 (3) 8 (26) 12 (40) SAV-IVH (n I11) 7 (64) 2 (18) 0 2 (18) Angiographic findings when at least part of the haemorrhage occupied the specified site. Figures in parentheses are the percentages for that subgroup. Basal ganglia = any combination of caudate, globus pallidus, putamen, thalamus, internal or external capsule, or insula; IVH= intraventricular haemorrhage; SAH = subarachnoid haemorrhage; post fossa =brainstem and/or cerebellum; sylvian =a haematoma that bridges the sylvian fissure. Figure 1 25 year old patient with sudden onset of right hemiparesis and obtunded consciousness. (A) Non-contrast axial CT scan shows haematoma in the posterior left frontal lobe with some surrounding low density. The patient was allocated to group 1. (B) Late arterial/capillary phase of left internal carotid arteriogram performed the day after the haemorrhage. There is an avascular area (arrows) but no other evidence to suggest an malformnation. (C) Lateral non-contrasted Ti weighted MRI (SE TRITE =600/15). A small focus of high signal was interpreted as representing residual haematoma. An malformation was not demonstrated. (D) Arteriogram performed at three months. There is a small leash of abnormiala vessels high i'n the left frontal lobe with early venous drainage into the sagi'ttal sinus (arrows). c M C 0~~~~~~~ 88&6%, whereas CT evaluation in isolation from clinical data had a sensitivity of 77-2% and a specificity of 84-2% in predicting an underlying lesion by radiology. The location of the haematoma and the presence or absence of free subarachnoid blood or intraventricular blood also influenced the chance of finding a structural lesion at angiography (table 6). Although there was a trend for a haematoma in the frontal or temporal lobe to be associated with an malformation or aneurysm, but for no structural lesion to be found with a parietal or occipital haematoma, this did not reach statistical significance. A haematoma crossing the sylvian fissure is likely linked with a structural cause. The combination of a haematoma with subarachnoid haemorrhage but no intraventricular blood is also linked with a structural cause. Nearly 13% of hypertensive patients had an underlying malformation or aneurysm, (this may be an underestimate, as several hypertensive patients did not complete the protocol). A structural lesion was found in 30-9% of patients with basal ganglia haemorrhage, and 18-2% of those with posterior fossa haemorrhage. Of five pure putamenal haematomas, no cause was found in four, but in one., a venous anomaly was seen on angiography and subsequent MRI showed a cavernous haemangioma..b.. C-1: Rw
4 Prospective evaluation of cerebral angiography and computed tomography in cerebral haematoma 1183 Figure 2 A 66 year old hypertensive man with sudden onset of hemiparesis. (A) CT shows a small haematoma in the left thalamus. There is patchy low density change in the cerebral white matter seen on this and other axial images suggesting small vessel disease. This patient was allocated to group 2. (B) Early arterial phase lateral left vertebral arteriogram performed three months after ictus. There is an malformation supplied by posterior cerebral arteries with early venous drainage into the vein of Galen. This patient was treated successfully by radiosurgery. A B Seven patients in group 1 had angiography repeated at three months. These studies identified one malformation, and in three patients showed prominent small veins that were attributed to haemorrhage or surgery performed to evacuate the haematoma. Computed tomography showed only intraventricular haemorrhage in three patients, each of whom was normotensive and aged under 40. Two had a choroidal malformation, and in one no angiographic abnormality was found. Further angiography was refused by this child's parents, but subsequent MRI showed no evidence of vascular abnormality. Three incidental aneurysms were detected during angiography in two patients, remote from the site of haemorrhage. These patients have been included in the "non-structural" group. There was only one angiographic complication: a transient dysphasia in a 48 year old ::: :... A B C Figure 3 A 38year old woman admitted after collapse and loss of consciousness. She was thrombocytopaenic after chemotherapy for non-hodgkin's lymphoma. (A) Contiguous axial CT shows haematoma in the right basal ganglia, with a moderate mass effect. The patient was allocated to group 2. Lateral views of vertebral (B) and right carotid (C) arteriograms were taken three months after a craniotomy to evacuate the haematoma. There was an aneurysm at the level of the ophthalmic artery and another at the junction of the right posterior cerebral artery and posterior communicating artery. At surgery the second aneurysm was found to have bled. hypertensive patient with a frontal haematoma. Representative scans and angiograms are shown in figures 1-5. Discussion The first successful evacuation of a cerebral haematoma was carried out in 1888 by McEwan,"2 whose patient made a complete recovery from an upper limb monoplegia. McKissock and coworkers, at this hospital reported in 1959 that the best predictor of outcome after surgery for this condition was the preoperative condition of the patient.'3 14 After successful treatment of acute cerebral haemorrhage, further management depends on the risk of further haemorrhage. How this risk should be assessed becomes critical. Russell's paper in indicated that
5 1184 Figure 4 A 23 year old man found unconscious by friends. Axial CTshows haematoma in the posterior leftfrontal lobe. He was allocated to group 1. Early and delayed angiography showed no lesion. The patient eventually admitted cocaine abuse. Figure 5 A 56 year old woman admitted with sudden onset of headache, double vision, and drowsiness. (A) Axial MRI (SE TRITE = 2500/95). There is a small area of altered signal in the right side of the mid-brain, also shown on CT. This patient was assigned to group 2. (B) Lateral view of vertebral arteriogram in the mid-arterial phase performed three months after ictus. There is a small malformation (arrows) with early venous drainage into the straight sinus. A B *o, :3W.si * qsc',, *: 9 o... gfi :.:: > *:: Xu. ^j$e : ^, ; -. ;..... :. :: ;. : S.i.ds de.: : :.::.:. i... w w XF}..... SR ::. ::... :a}...,.. *.^,*... ;... :::.: :..... : : 6<.r; Halpin, Britton, Byrne, Clifton, Hart, Moore primary haemorrhage was most likely to occur in certain sites-notably the striatum and posterior fossa. It would seem that many physicians have extrapolated this to the false assumption that haemorrhage in the basal ganglia or posterior fossa is almost exclusively due to hypertension. Douglas and Haerer," for example, state that when the diagnosis of hypertensive haemorrhage is obvious, angiography is "ethically unacceptable", whereas others have suggested that angiography should be restricted to patients with haemor- :~n jrhage outside the basal ganglia.'617 This led McCormick and Rosenfield in 1973 to state that "the assumption that hypertension causes most massive brain haemorrhage has become virtual dogma", and "the majority of reports (on this subject) are so poorly controlled and documented as to be of little scientific validity". In their necropsy review of 144 patients who died from massive brain haemorrhage, 36% of patients with hypertension had another cause of haemorrhage, a third having causative malformation or aneurysms; and 19 normotensive and five hypertensive patients had striatal haemorrhage due to a non-hypertensive aetiology.4 Our data confirm the findings of McCormick and Rosenfield: at least 12-8% of our hypertensive patients had an malformation or aneurysm, and at least 31% of patients with basal ganglia haemorrhage and 18% of those with posterior fossa haemorrhage had such a lesion. It is especially important not to ascribe haemorrhage in these sites to non-structural causes as there is evidence that such malformations are more likely to bleed than those in other locations.'8 These assumptions have led to exclusions and omissions from many studies dealing with cerebral haematoma." Weisberg and colleagues have written extensively on the clinical features in those with haematomas in varying sites,'9-21 but few of the patients had angiography. Loes et al9 reviewed the records and radiology of 67 patients referred for angiography after cerebral haemorrhage. In addition to this initial selection, patients with posterior fossa, basal ganglia, or thalamic haemorrhage were excluded, as were patients with bleeding diathesis. Such selection may exclude patients liable to rebleed from structural lesions. In our study three patients had haemorrhage during warfarin treatment, all with an international normalised ratio of greater than 3 5, one of whom was found to have an unsuspected malformation on angiography, and one patient with thrombocytopenia after chemotherapy for non-hodgkin's lymphoma bled from an aneurysm. Tofol et al retrospectively reviewed two groups of patients with non-traumatic intracerebral haemorrhage," 1 1 without significant exclusions. They found a positive angiography rate of 12-8% in hypertensive patients, exactly matching our figure, but concluded that "most hypertensive patients, in particular those with putamenal haemorrhages, do not require arteriography". The sensitivity and specificity of CT in
6 Prospective evaluation of cerebral angiography and computed tomography in cerebral haematoma 1185 predicting an angiographic abnormality seem disappointing in this study when compared with others,7-'0 who have found that CT is accurate in predicting the presence of an underlying structural lesion. These authors have used entry criteria less broad than ours. We included patients with basal ganglia or posterior fossa haemorrhage, tending to place them in group 2 according to available literature, and were proved wrong on several occasions. Hayward and O'Reilly,8 using a first generation CT scanner with a 160 x 160 matrix, reported that CT is 90% accurate in predicting the cause of cerebral haemorrhage, but excluded all patients with posterior fossa haemorrhage, those below the age of 21, and patients on whom angiography was not performed. More recently, in a retrospective study of 149 patients with cerebral haematoma, Laissy et al reported sensitivity and specificity of CT to be 96% and 100% respectively in detecting malformation or aneurysm, using a combination of CT findings, including site of haemorrhage and the presence or absence of intraventricular or subarachnoid haemorrhage.7 Their 149 patients were selected from a total of 452, however, and no information is given as to how patients were selected for angiography. Similar to McCormick et al, they found that neither age nor systemic blood pressure were good predictors of patients with abnormal angiograms. There were fewer aneurysms in our study population compared with other studies.7910 We attributed this to the fact that we excluded patients whose scans predominantly showed subarachnoid haemorrhage. Repeating angiography when an acute study does not show a structural lesion has been advocated by Willinsky et al,22 who state that up to 15% of small malformations were not shown on the first examination, presumably due to a mass effect from haematoma. We discovered one malformation at follow up angiography, which had not been previously apparent, and Laissy et al found three "angiomas" in this manner.7 An alternative approach, used in our group 2, is not to perform angiography acutely in those patients for whom surgery is not contemplated, but to wait until any mass effect had subsided. We discovered an malformation or aneurysm in 10 such patients, none of whom came to harm by the delay in diagnosis. By the same token, 48 patients were saved from having two rather than one angiogram. We would accept, however, that delay in diagnosing and treating an aneurysm may have serious consequences. Like us, Loes et al 9 found an association between location of haematoma and angiographic abnormality, and speculate that the small proportion of structural lesions found with haematoma in the parietal and occipital lobes may be related to the predilection of amyloid angiopathy for these areas.23 This diagnosis may be difficult to make, and its occurrence might contribute to the small numbers of positive angiograms in elderly patients. Of course, there may be many diagnoses hidden within a diagnosis of "primary" haemorrhage: lesions such as cavernous haemangioma and vasculitis, for example, are unlikely to be shown by angiography.'425 Other conditions predisposing to cerebral haemorrhage such as bleeding diatheses, diabetes mellitus, and liver disease4 2$28 should be detectable by clinical and laboratory investigation. A history of drug abuse may be difficult to elicit, but can cause cerebral haemorrhage,29 30 and haemorrhage into a tumour will sometimes not reveal the underlying cause until the haematoma has absorbed.3' 32 In our experience this is unusual, however. Although this study collected consecutive patients prospectively, they were a selected group by referral to our hospital. Therefore patients who were considered too sick to be transferred and those dying before arrival were excluded. Other logistic factors may have biased the series, which might explain the paucity of patients with tumours, as such patients may not have been sent to us. Similarly, elderly patients, in whom the presumed diagnosis was of a non-structural lesion, may not have been referred. Such selection, although unintentional on our part, may have biased our results by increasing the percentage of patients in whom a structural lesion was found. We have no measure of how many patients with cerebral haemorrhage are not referred because the clinician believes they have a "primary" bleed, nor how such a clinician makes this decision. Similarly, we do not know how often the diagnosis of haemorrhage is not made because the patient presenting with a stroke does not have CT. As the mean age of our study group was 46-4 (range 7-71) years, we suspect that many elderly patients who are likely to have amyloid angiopathy were not referred. We used angiography as our gold standard and it is questionable whether MRI or magnetic resonance angiography (MRA) would be preferable. Whereas MRI may throw further light on the cause of haemorrhage within the "primary" group, there is as yet no evidence to suggest that it would be as sensitive as angiography in the detection of malformation.33 Willinsky et al state that very small malformations are, by their nature, occult on MRI." In one of our patients, MRI did not detect a small malformation, but MRA was not performed. A prospective comparison between MRI, MRA, and angiography in patients with cerebral haematoma is currently under assessment at this hospital. In summary, we believe our data support the recommendation that angiography should be considered in all patients with cerebral haematoma, regardless of the site of haemorrhage, or a history of hypertension, and that the clinical condition of the patient should be the deciding factor. We further believe that an angiogram that shows no abnormality apart from mass effect should be repeated after an appropriate interval, especially if the patient is young and normotensive.
7 1186 Halpin, Britton, Byrne, Clifton, Hart, Moore 1 Waltimo 0, Kaste M, Aho K, Kotila M. Outcome of stroke in the Espoo-Kauniainen area, Finland. Ann Clin Res 1980;12: Tsemetis SA. Surgical mangement of intracerebral haematomas. Neurosurgery 1985;16: Jellinger K. Intracranial aneurysms: pathology and aetiology. In: Pia HW, ed. Intracranial aneurysms. Berlin: Springer, 1979: McCormick WF, Rosenfield DB. Massive brain haemorrhage: a review of 144 cases and an examination of their causes. Stroke 1973;4: Sahs AL, Perrett GE, Locksley HB. Intracranial aneurysms and subarachnoid haemorrhage: a cooperative study. Philadelphia: Lippincott and Co, Russell DS in discussion: The pathology of spontaneous intracranial haemorrhage. Proceedings of the Royal Society of Medicine 1953;47: Laissy JP, Normand G, Monroe M, Duchateau C, Alibert A, Thiebot J. Spontaneous intracerebral haematomas from various causes. Predictive value of CT compared with Angiography. Neuroradiology 1991 ;33: Hayward RS, O'Reilly GVA. Intracerebral Haemorrhage. Accuracy of computerised axial scanning in predicting the underlying pathology. Lancet 1976;i: Loes DJ, Smoker WRK, Biller J, Cornell SH. Non traumatic lobar intracerebral haemorrhage: CT/Angiographic correlation. American Journal of Neuroradiology 1987;8: Toffol GJ, Biller J, Adams HP, Smoker WR. The predicted value of arteriography in nontraumatic intracerebral haemorrhage Stroke 1986;17: Tofol GJ, Biller J, Adams HP Jr. Nontraumatic intracerebral haemorrhage in young adults. Arch Neurol 1987;44: MacEwan W. An address on the surgery of the brain and spinal cord. BMg 1888;2: McKissock W, Richardson A, Walsh I. Primary intracerebral haemorrhage: results of the surgical treatment of 214 consecutive cases. Lancet 1959;ii: McKissock W, Richardson A, Taylor J. Primary intracerebral haemorrhage: a controlled trial of surgical and conservative treatment in 180 unselected cases, Lancet 1961;ii: Douglas MA, Haerer AF. Long term prognosis of hypertensive intracerebral haemorrhage. Stroke 1982;13: Papo I, Janny P, Caruselli G, Colnet G, Luongo A. Intracranial time pressure course in primary intracerebral haemorrhage. Neurosurgery 1979;4: Ojeman RG, Mohr JP. Hypertensive brain haemorrhage. Clin Neurosurg 1976;23: Willinsky R, Lasjaunias P, Terbrugge K, Pruvost P. Malformations arterioveineuses cerebrales. Analyse de l'angio-archictecture chez des patients ayant presente un accident hemorragigue. J Neuroradiol 1988;15: Weisberg LA. Subcortical lobar intracerebral haemorrhage: clinical computed tomographic correlations. J Neurol Neurosurg Psychiatry 1985;48: Weisberg LA, Stazio A, Shamsnia M, Elliott D. Nontraumatic temporal subcortical haemorrhage, clinical computed tomographic analysis. Neuroradiology 1990;32: Weisberg LA. CT in intracranial haemorrhage. Arch Neurol 1979;36: Willinsky R, Lasjaunias P, Comoy J, Provost P. Cerebral micro malformations. Review of 13 cases. Acta Neurochir (Wien) 1988;91: Vinters HV, Gilbert HJ. Cerebral amyloid angiopathy II, the distribution of amyloid vascular changes. Stroke 1983;14: Bitoh S, Hasegawa H, Fujiwara M, Sakurai M. Angiographically occult vascular malformations causing intracranial haemorrhage. Surg Neurol 1982;17: Edwards KR. Haemorrhagic complications of cerebral arteritis. Surg Neurol 1988;17: Ojeman RG, Heros RC. Spontaneous brain haemorrhage. Stroke 1983;14: Almaani WS, Awidi AS. Spontaneous intracranial bleeding in haemorrhagic diathesis. Surg Neurol 1982;17: Ruscadella J, Peiro A. Prognostic factors in intraparenchymatous haematoma with ventricular haemorrhage. Neuroradiology 1986;28: Yu YJ, Cooper DR, Wellenstein DE, Block B. Cerebral angiitis and intracerebral haemorrhage associated with metamphetamine abuse. J Neurosurg 1983;58: Bessen HA. Intracranial haemorrhage associated with phenylcyclidine abuse. JAMA 1982;248: Scott M. Spontaneous intracerebral haematoma caused by cerebral neoplasms. _J Neurosurg 1975;42: Gildersleeve N, Koo AH, McDonald CJ. Metastatic tumour presenting as intracerebral haemorrhage. Radiology 1977;124: Willinsky RA, Fitzgerald M, Terbrugge K, Montanera W, Wallace M. Delayed angiography in the investigation of intracerebral haematomas caused by small malformations. Neurology 1993;35: J Neurol Neurosurg Psychiatry: first published as /jnnp on 1 October Downloaded from on 6 November 2018 by guest. Protected by copyright.
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Diagnostic Cerebral Angiography in Spontaneous Intracranial Haemorrhage: A Guide for Developing Countries
 Original Article Diagnostic Cerebral Angiography in Spontaneous Intracranial Haemorrhage: A Guide for Developing Countries Ishak Abu Bakar, Ibrahim Lutfi Shuaib, Abdul Rahman Mohd Ariff, Nyi Nyi Naing
Original Article Diagnostic Cerebral Angiography in Spontaneous Intracranial Haemorrhage: A Guide for Developing Countries Ishak Abu Bakar, Ibrahim Lutfi Shuaib, Abdul Rahman Mohd Ariff, Nyi Nyi Naing
Brain Arteriovenous Malformations Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos
 Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Epilepsy after two different neurosurgical approaches
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Spontaneous ICH accounts for 10% 15% of cases
 J Neurosurg 117:761 766, 2012 Computed tomography angiography: improving diagnostic yield and cost effectiveness in the initial evaluation of spontaneous nonsubarachnoid intracerebral hemorrhage Clinical
J Neurosurg 117:761 766, 2012 Computed tomography angiography: improving diagnostic yield and cost effectiveness in the initial evaluation of spontaneous nonsubarachnoid intracerebral hemorrhage Clinical
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Short Communications. Alcoholic Intracerebral Hemorrhage
 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid
CT angiography and its role in the investigation of intracranial haemorrhage
 CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
CT angiography and its role in the investigation of intracranial haemorrhage RD Magazine, 39, 458, 29-30 Dr M Igra Radiology SPR Leeds General Infirmary Dr I Djoukhadar Research fellow Wolfson Molecular
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Clinical and neuroradiological investigations do not disclose
 Value of Repeat Angiography in Patients With Spontaneous Subcortical Hemorrhage Akihiko Hino, MD; Masahito Fujimoto, MD; Tarumi Yamaki, MD; Yoshihiro Iwamoto, MD; Tetsuya Katsumori, MD Background and Purpose
Value of Repeat Angiography in Patients With Spontaneous Subcortical Hemorrhage Akihiko Hino, MD; Masahito Fujimoto, MD; Tarumi Yamaki, MD; Yoshihiro Iwamoto, MD; Tetsuya Katsumori, MD Background and Purpose
Methods. Treatment options for intracranial arteriovenous malformations
 AJNR Am J Neuroradiol 25:1139 1143, August 2004 Complete Obliteration of Intracranial Arteriovenous Malformation with Endovascular Cyanoacrylate Embolization: Initial Success and Rate of Permanent Cure
AJNR Am J Neuroradiol 25:1139 1143, August 2004 Complete Obliteration of Intracranial Arteriovenous Malformation with Endovascular Cyanoacrylate Embolization: Initial Success and Rate of Permanent Cure
Computerised axial tomography in patients with severe migraine: a preliminary report
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 990-994 Computerised axial tomography in patients with severe migraine: a preliminary report G. D. HUNGERFORD', G. H. du BOULAY2, AND K. J.
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 990-994 Computerised axial tomography in patients with severe migraine: a preliminary report G. D. HUNGERFORD', G. H. du BOULAY2, AND K. J.
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes
 Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Hypertensive Haemorrhagic Stroke. Dr Philip Lam Thuon Mine
 Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
The three main subtypes of stroke
 Neurology 55 Spontaneous intracerebral haemorrhage in the elderly Spontaneous Intracerebral Haemorrhage (ICH) is defined as bleeding into the brain parenchyma without accompanying trauma. This condition
Neurology 55 Spontaneous intracerebral haemorrhage in the elderly Spontaneous Intracerebral Haemorrhage (ICH) is defined as bleeding into the brain parenchyma without accompanying trauma. This condition
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
I ntracranial haemorrhage is the main cause of morbidity and
 294 PAPER Concurrent arterial aneurysms in brain arteriovenous malformations with haemorrhagic presentation C Stapf, J P Mohr, J Pile-Spellman, R R Sciacca, A Hartmann, H C Schumacher, H Mast... See end
294 PAPER Concurrent arterial aneurysms in brain arteriovenous malformations with haemorrhagic presentation C Stapf, J P Mohr, J Pile-Spellman, R R Sciacca, A Hartmann, H C Schumacher, H Mast... See end
Stroke & the Emergency Department. Dr. Barry Moynihan, March 2 nd, 2012
 Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
ATTENDING PHYSICIAN'S STATEMENT STROKE / BRAIN ANEURYSM SURGERY OR CEREBRAL SHUNT INSERTION / CAROTID ARTERY SURGERY
 ATTENDING PHYSICIAN'S STATEMENT STROKE / BRAIN ANEURYSM SURGERY OR CEREBRAL SHUNT INSERTION / CAROTID ARTERY SURGERY A) Patient s Particulars Name of Patient Gender NRIC/FIN or Passport No. Date of Birth
ATTENDING PHYSICIAN'S STATEMENT STROKE / BRAIN ANEURYSM SURGERY OR CEREBRAL SHUNT INSERTION / CAROTID ARTERY SURGERY A) Patient s Particulars Name of Patient Gender NRIC/FIN or Passport No. Date of Birth
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
Stroke in the ED. Dr. William Whiteley. Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian
 Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective
 Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
7 TI - Epidemiology of intracerebral hemorrhage.
 1 TI - Multiple postoperative intracerebral haematomas remote from the site of craniotomy. AU - Rapana A, et al. SO - Br J Neurosurg. 1998 Aug;1():-8. Review. IDS - PMID: 1000 UI: 991958 TI - Cerebral
1 TI - Multiple postoperative intracerebral haematomas remote from the site of craniotomy. AU - Rapana A, et al. SO - Br J Neurosurg. 1998 Aug;1():-8. Review. IDS - PMID: 1000 UI: 991958 TI - Cerebral
Original Research Article
 MAGNETIC RESONANCE IMAGING IN MIDDLE CEREBRAL ARTERY INFARCT AND ITS CORRELATION WITH FUNCTIONAL RECOVERY Neethu Tressa Jose 1, Rajan Padinharoot 2, Vadakooth Raman Rajendran 3, Geetha Panarkandy 4 1Junior
MAGNETIC RESONANCE IMAGING IN MIDDLE CEREBRAL ARTERY INFARCT AND ITS CORRELATION WITH FUNCTIONAL RECOVERY Neethu Tressa Jose 1, Rajan Padinharoot 2, Vadakooth Raman Rajendran 3, Geetha Panarkandy 4 1Junior
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Spontaneous Intracerebral Hemorrhage and Liver Dysfunction
 85 Spontaneous Intracerebral Hemorrhage and Liver Dysfunction Hiroshi Niizuma, MD, Jiro Suzuki, MD, Tsutomu Yonemitsu, MD, and Taisuke Otsuki, MD We evaluated liver function and coagulation parameters
85 Spontaneous Intracerebral Hemorrhage and Liver Dysfunction Hiroshi Niizuma, MD, Jiro Suzuki, MD, Tsutomu Yonemitsu, MD, and Taisuke Otsuki, MD We evaluated liver function and coagulation parameters
NEURORADIOLOGY Part I
 NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
NEURORADIOLOGY Part I Vörös Erika University of Szeged Department of Radiology SZEGED BRAIN IMAGING METHODS Plain film radiography Ultrasonography (US) Computer tomography (CT) Magnetic resonance imaging
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
The significance of traumatic haematoma in the
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Primary pontine haemorrhage: clinical and computed tomographic correlations
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:346-352 Primary pontine haemorrhage: clinical and computed tomographic correlations LEON A WESBERG From the Department of Neurology and Psychiatry
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:346-352 Primary pontine haemorrhage: clinical and computed tomographic correlations LEON A WESBERG From the Department of Neurology and Psychiatry
 www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
North Oaks Trauma Symposium Friday, November 3, 2017
 Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Malignant melanoma and the central nervous system A guide for classification based on the clinical findings
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 526-530 Malignant melanoma and the central nervous system A guide for classification based on the clinical findings R. D. HAYWARD From the Department
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 526-530 Malignant melanoma and the central nervous system A guide for classification based on the clinical findings R. D. HAYWARD From the Department
Specialised Services Policy: CP22. Stereotactic Radiosurgery
 Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER
 CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
Lothian Audit of the Treatment of Cerebral Haemorrhage (LATCH)
 1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
Medical Review Guidelines Magnetic Resonance Angiography
 Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
Cerebrovascular diseases-2
 Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD.
 Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
Cerebral pathology in subarachnoid haemorrhage
 J. Neurol. Neurosurg. Psychiat., 196, 6, 55 pathology in subarachnoid haemorrhage BARBARA SMITH1 From Maida Vale Hospital for Nervous Diseases Subarachnoid haemorrhage due to ruptured intracranial aneurysm
J. Neurol. Neurosurg. Psychiat., 196, 6, 55 pathology in subarachnoid haemorrhage BARBARA SMITH1 From Maida Vale Hospital for Nervous Diseases Subarachnoid haemorrhage due to ruptured intracranial aneurysm
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
T HE blood supply of cerebral arteriovenous malformations is often extensive
 NOVEMBER, 1974 ROENTGENOGRAPHIC ANALYSIS OF ARTERIOVENOUS MALFORMATIONS OF THE OCCIPITAL LOBE* By B. TODD TROOST, M.D.,t and THOMAS H. NEWTON, M.D4 T HE blood supply of cerebral arteriovenous malformations
NOVEMBER, 1974 ROENTGENOGRAPHIC ANALYSIS OF ARTERIOVENOUS MALFORMATIONS OF THE OCCIPITAL LOBE* By B. TODD TROOST, M.D.,t and THOMAS H. NEWTON, M.D4 T HE blood supply of cerebral arteriovenous malformations
Ruptured cerebral aneurysms: early and late prognosis with surgical treatment
 J Neurosurg 59:6-15, 1983 Ruptured cerebral aneurysms: early and late prognosis with surgical treatment A personal series, 1958-1980 REGINALD H. SHEr HARD, M.D., F.R.C.S. Trent Regional Department of Neurosurgery,
J Neurosurg 59:6-15, 1983 Ruptured cerebral aneurysms: early and late prognosis with surgical treatment A personal series, 1958-1980 REGINALD H. SHEr HARD, M.D., F.R.C.S. Trent Regional Department of Neurosurgery,
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Intracranial dural arteriovenous fistulas (DAVFs) with retrograde
 ORIGINAL RESEARCH W.J. van Rooij M. Sluzewski G.N. Beute Dural Arteriovenous Fistulas with Cortical Venous Drainage: Incidence, Clinical Presentation, and Treatment BACKGROUND AND PURPOSE: Our purpose
ORIGINAL RESEARCH W.J. van Rooij M. Sluzewski G.N. Beute Dural Arteriovenous Fistulas with Cortical Venous Drainage: Incidence, Clinical Presentation, and Treatment BACKGROUND AND PURPOSE: Our purpose
Summary of some of the landmark articles:
 Summary of some of the landmark articles: The significance of unruptured intracranial saccular aneurysms: Weibers et al Mayo clinic. 1987 1. 131 patients with 161 aneurysms were followed up at until death,
Summary of some of the landmark articles: The significance of unruptured intracranial saccular aneurysms: Weibers et al Mayo clinic. 1987 1. 131 patients with 161 aneurysms were followed up at until death,
Nontraumatic ICH accounts for 10% 15% of cases of acute
 ORIGINAL RESEARCH J.E. Delgado Almandoz P.W. Schaefer J.N. Goldstein J. Rosand M.H. Lev R.G. González J.M. Romero Practical Scoring System for the Identification of Patients with Intracerebral Hemorrhage
ORIGINAL RESEARCH J.E. Delgado Almandoz P.W. Schaefer J.N. Goldstein J. Rosand M.H. Lev R.G. González J.M. Romero Practical Scoring System for the Identification of Patients with Intracerebral Hemorrhage
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Retrospective analytical six months study of vascular abnormalities of brain
 International Journal of Advances in Medicine http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20160185 Retrospective analytical
International Journal of Advances in Medicine http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20160185 Retrospective analytical
Case 9511 Hypertensive microangiopathy
 Case 9511 Hypertensive microangiopathy Schepers S, Barthels C Section: Neuroradiology Published: 2011, Nov. 3 Patient: 67 year(s), male Authors' Institution Department of Radiology, Jessa ziekenhuis campus
Case 9511 Hypertensive microangiopathy Schepers S, Barthels C Section: Neuroradiology Published: 2011, Nov. 3 Patient: 67 year(s), male Authors' Institution Department of Radiology, Jessa ziekenhuis campus
Vascular Pattern in Tumours
 Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Vascular Pattern in Tumours To cite this article: (1957) Vascular Pattern in Tumours, Acta Radiologica,
Acta Radiologica ISSN: 0001-6926 (Print) (Online) Journal homepage: https://www.tandfonline.com/loi/iaro20 Vascular Pattern in Tumours To cite this article: (1957) Vascular Pattern in Tumours, Acta Radiologica,
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Review Article Differentiating between Hemorrhagic Infarct and Parenchymal Intracerebral Hemorrhage
 Hindawi Publishing Corporation Radiology Research and Practice Volume 2012, Article ID 475497, 11 pages doi:10.1155/2012/475497 Review Article Differentiating between Hemorrhagic Infarct and Parenchymal
Hindawi Publishing Corporation Radiology Research and Practice Volume 2012, Article ID 475497, 11 pages doi:10.1155/2012/475497 Review Article Differentiating between Hemorrhagic Infarct and Parenchymal
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
Role of Computed Tomography in Evaluation of Cerebrovascular Accidents.
 DOI: 10.21276/aimdr.2017.3.2.RD10 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Role of Computed Tomography in Evaluation of Cerebrovascular Accidents. Rishikant Sinha 1, Ahmad Rizwan Karim 2
DOI: 10.21276/aimdr.2017.3.2.RD10 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Role of Computed Tomography in Evaluation of Cerebrovascular Accidents. Rishikant Sinha 1, Ahmad Rizwan Karim 2
Radiographic and statistical analysis of Brain Arteriovenous Malformations.
 Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Radiographic and statistical analysis of Brain Arteriovenous Malformations. Poster No.: C-0996 Congress: ECR 2017 Type: Educational Exhibit Authors: C. E. Rodriguez 1, A. Lopez Moreno 1, D. Sánchez Paré
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS
 Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council
 American Society of Neuroradiology What Is a Stroke? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
American Society of Neuroradiology What Is a Stroke? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Ruptured Cerebral Aneurysm of the Anterior Circulation
 Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
Original Articles * Division of Neurosurgery Department of Surgery Ruptured Cerebral Aneurysm of the Anterior Circulation Management and Microsurgical Treatment Ossama Al-Mefty, MD* ABSTRACT Based on the
VASCULAR MALFORMATIONS. Owen Samuels, MD Adam Webb, MD Emory University
 VASCULAR MALFORMATIONS Owen Samuels, MD Adam Webb, MD Emory University Introduction Brain and spinal cord vascular malformations can be separated into five main categories: 1) Arteriovenous malformation,
VASCULAR MALFORMATIONS Owen Samuels, MD Adam Webb, MD Emory University Introduction Brain and spinal cord vascular malformations can be separated into five main categories: 1) Arteriovenous malformation,
Intracerebral haematoma complicating ruptured cerebral berry aneurysm
 J. Neurol. Neurosurg. Psychiat., 196, 5, 378 Intracerebral haematoma complicating ruptured cerebral berry aneurysm M. R. CROMPTON From the Neurosurgical Department of St. George's Hospital at Atkinson
J. Neurol. Neurosurg. Psychiat., 196, 5, 378 Intracerebral haematoma complicating ruptured cerebral berry aneurysm M. R. CROMPTON From the Neurosurgical Department of St. George's Hospital at Atkinson
ORIGINAL ARTICLE COMPUTED TOMOGRAPHY EVALUATION OF SPONTANEOUS INTRACRANIAL HAEMORRHAGE
 Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 4, pp 647-652, April, 2015 ORIGINAL ARTICLE
Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 4, pp 647-652, April, 2015 ORIGINAL ARTICLE
Uncommon Symptomatic Cerebral Vascular Malformations
 Uncommon Symptomatic Cerebral Vascular Malformations Mauro Bergui and Gianni Boris Bradac Summary: We describe three cases of unusual vascular malformations in which the most relevant angiographic findings
Uncommon Symptomatic Cerebral Vascular Malformations Mauro Bergui and Gianni Boris Bradac Summary: We describe three cases of unusual vascular malformations in which the most relevant angiographic findings
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Overview of imaging modalities for cerebral aneurysms
 Overview of imaging modalities for cerebral aneurysms Soroush Zaghi BIDMC PCE: Radiology August 2008 (Images from BIDMC, PACS.) Our Patient: Presentation Our patient is a 57 y/o woman who reports blowing
Overview of imaging modalities for cerebral aneurysms Soroush Zaghi BIDMC PCE: Radiology August 2008 (Images from BIDMC, PACS.) Our Patient: Presentation Our patient is a 57 y/o woman who reports blowing
Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage
 Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage Hussam A. Yacoub MD Lehigh Valley Health
Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage Hussam A. Yacoub MD Lehigh Valley Health
Angiographically occult arteriovenous malformations
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 1057-1064 Angiographically occult arteriovenous malformations of the brain B. A. BELL, B. E. KENDALL, AND L. SYMON From the National Hospital
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 1057-1064 Angiographically occult arteriovenous malformations of the brain B. A. BELL, B. E. KENDALL, AND L. SYMON From the National Hospital
What You Should Know About Cerebral Aneurysms
 American Society of Neuroradiology American Society of Interventional & Therapeutic Neuroradiology What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Intervention Committee
American Society of Neuroradiology American Society of Interventional & Therapeutic Neuroradiology What You Should Know About Cerebral Aneurysms From the Cerebrovascular Imaging and Intervention Committee
Angioarchitecture of Brain Arteriovenous Malformations and the Risk of Bleeding: An Analysis of Patients in Northeastern Malaysia
 Brief Communication Angioarchitecture of Brain Arteriovenous Malformations and the Risk of Bleeding: An Analysis of Patients in Northeastern Malaysia Shibani KanDai 1, Mohd Shafie abdullah 1, Nyi Nyi naing
Brief Communication Angioarchitecture of Brain Arteriovenous Malformations and the Risk of Bleeding: An Analysis of Patients in Northeastern Malaysia Shibani KanDai 1, Mohd Shafie abdullah 1, Nyi Nyi naing
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Treatment of Unruptured Vertebral Artery Dissecting Aneurysms
 33 Treatment of Unruptured Vertebral Artery Dissecting Aneurysms Isao NAITO, M.D., Shin TAKATAMA, M.D., Naoko MIYAMOTO, M.D., Hidetoshi SHIMAGUCHI, M.D., and Tomoyuki IWAI, M.D. Department of Neurosurgery,
33 Treatment of Unruptured Vertebral Artery Dissecting Aneurysms Isao NAITO, M.D., Shin TAKATAMA, M.D., Naoko MIYAMOTO, M.D., Hidetoshi SHIMAGUCHI, M.D., and Tomoyuki IWAI, M.D. Department of Neurosurgery,
Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital
 ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
ISPUB.COM The Internet Journal of Neurosurgery Volume 9 Number 2 Epidemiology And Treatment Of Cerebral Aneurysms At An Australian Tertiary Level Hospital A Granger, R Laherty Citation A Granger, R Laherty.
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Patient with vertigo, dizziness and depression
 Clinical Case - Test Yourself Neuro/Head and Neck Radiology Patient with vertigo, dizziness and depression Michael Mantatzis, Paraskevi Argyropoulou, Panos Prassopoulos Radiology Department, Democritus
Clinical Case - Test Yourself Neuro/Head and Neck Radiology Patient with vertigo, dizziness and depression Michael Mantatzis, Paraskevi Argyropoulou, Panos Prassopoulos Radiology Department, Democritus
DOWNLOAD PDF RADIOSURGERY FOR CAVERNOUS MALFORMATIONS IN BASAL GANGLIA, THALAMUS AND BRAINSTEM KIDA, Y
 Chapter 1 : Stereotactic radiosurgery for cavernous malformations â Mayo Clinic Most of the lesions were located in the brainstem, followed by the lobar region, cerebellum, thalamus, and basal ganglia
Chapter 1 : Stereotactic radiosurgery for cavernous malformations â Mayo Clinic Most of the lesions were located in the brainstem, followed by the lobar region, cerebellum, thalamus, and basal ganglia
Attending Physician Statement- Stroke
 Instruction to doctor: This patient is insured with us against the happening of certain contingent events associated with his health A claim has been submitted in connection with Stroke / Intracranial
Instruction to doctor: This patient is insured with us against the happening of certain contingent events associated with his health A claim has been submitted in connection with Stroke / Intracranial
