Effectiveness of sedation in dacryocystorhinostomy surgery
|
|
|
- Felicity Gilmore
- 5 years ago
- Views:
Transcription
1 Original article Effectiveness of sedation in dacryocystorhinostomy surgery Tuladhar S 1, Adhikari S 1, Bhattarai B K 2 Departments of 1 Ophthalmology and 2 Anesthesiology and Critical Care B P Koirala Institute of Health Sciences, Dharan, Sunsari, Nepal Introduction Abstract Background: Chronic dacryocystitis is a common ophthalmic problem almost always requiring surgery as the only definitive treatment. Aim: To compare the perioperative outcome of external DCR surgery under local anesthesia with and without sedation. Subjects and methods: One hundred consecutive patients with chronic dacryocystitis undergoing dacryocystorhinostomy (DCR) surgery were randomly divided into two groups using computer generated random table. Group A underwent DCR under local anesthesia (LA) without sedation and group B under LA with sedation. The outcome parameters were intra-operative pain, surgeon's comfort, intra-operative complications and duration of surgery. Statistical analysis: SPSS version 11.5 software was used. Chi square test was used to compare the difference between the groups. Results: There were 50 patients in each group. The mean age ± SD of the patients was 34.4±12.12 years (95% CI= years). Sixty-nine percent of them were female. Significantly higher number of patients experienced pain in Group A as compared to Group B (100% vs 50%, P<0.001) Surgeon's discomfort was significantly present in group A as compared to group B (70% vs 10%), (p= ). Blood loss was significantly more in group A than in group B (p=0.017). There was no significant difference in the duration of surgery. The post operative success rate in both the groups was comparable after six months of followup. Conclusion: The use of sedation with LA improves the perioperative outcome of DCR surgery in terms of patient's pain, surgeon's comfort and intra-operative complications. Key words: dacryocystitis, dacryocystorhinostomy, sedation Dacryocystitis is an inflammation of the lacrimal sac secondary to obstruction of the naso-lacrimal duct (NLD). It can be acute or chronic. The definitive Received: Accepted: Correspondence and reprint requests to: Dr Sarita Tuladhar (Dhakal) Department of Ophthalmology B P Koirala Institute of Health Sciences, Dharan, Sunsari, Nepal Phone: Ext 2320 (Office) drtuladharsarita@yahoo.com treatment (Dalgesh et al 1967) of chronic dacryocystitis due to NLD obstruction for duration greater than one year is dacryocystorhinostomy (DCR). The principle of DCR is anastomosing the lacrimal sac to the nasal mucosa of the middle nasal meatus. Toti (1904) first described DCR. The best known technique for DCR was described by Dutemps and Bourget in 1920 (Duffy et al 2000). It can be performed with or without silastic tube intubation. The former has been reported to improve the success rate of the procedure (Duffy et al 25
2 2000; O, Donnell et al 2001). Caldwell et al (1993) described the intra-nasal approach for DCR. Currently endoscopic intra-nasal DCR is available (Massaro et al 1990). Gonnering et al (1991) have described the performance of successful intranasal DCR by using either the argon laser, potassium-titanyl-phosphate: YAG laser, or a CO 2 laser for tissue removal. The overall success rate of external DCR is better than that of the endonasal DCR (Zaman et al 2003). External DCR can be carried out under general anesthesia (GA) or local anesthesia (LA) with or without use of sedation. It is commonly done under LA on outpatients basis (Benger et al 1992; Dresner et al 1991). LA provides anesthesia and excellent hemeostasis for the operation (Fanning, 2000). The commonly used LA in DCR is 2% lignocaine with or without 1:200,000 adrenaline or a mixture of 2% lignocaine and 0.5% bupivacaine in equal parts. The advantage of adding adrenaline to plain lignocaine is that it maintains better homeostasis, prolongs the duration of action of LA and allows the use of higher dose. A number of sedatives can be used in conjunction with LA. The commonly used ones are pethidine (1-2 mg/ kg body weight intramuscularly) and promethazine (1 mg/kg body weight intra-muscularly). Also, midazolam (1-2 mg) or droperidol (0.5 mg) intravenously, along with a modest dosage of alfentanil ( microgram intra-venously), may be given (Fanning, 2000). Ketamine in a dose of mg/kg combined with midazolam may also be given (Fanning, 2000). This combination produces excellent amnesia as well as analgesia. In the past, DCR used to be carried out under GA, but nowadays it is mostly done under LA except in children (<15 years of age). Many studies have compared the outcome of DCR under local anesthesia versus general anesthesia. No published report comparing the outcome of DCR surgery with or without the addition of sedatives is available. This study was carried out to compare the efficacy of DCR surgery under LA with and without sedatives. Subjects and methods One hundred consecutive patients with chronic dacryocystitis undergoing DCR surgery from March 2007 to February 2008 were randomly divided into two groups: A and B, using computer-generated random table. Group A underwent DCR under local anesthesia without sedation and group B with sedation. The drugs used for sedation were pethidine (1 mg/kg) IM with promethazine (0.5mg /kg), which were given IM in the deltoid region half an hour before giving local anesthetics. The local anaesthetic used was 2% lignocaine with adrenaline 1:200,000. The maximum dosage of lignocaine for a healthy adult is 7 mg/kg or 500 mg for a 70 kg person. This corresponds to 25 ml of 2% solution. All patients with NLD obstruction with chronic dacryocystitis and above 15 years of age undergoing DCR surgery were included in the study. The exclusion criteria were failed DCR, canalicular block and bleeding disorders. Other pathological conditions for exclusion criteria were atrophic rhinitis, rhinosporidosis, deviated nasal septum, hypertrophied turbinates, nasal polyp and malignancies. Similarly, acute dacryocystitis, pyocele, encysted mucocele, post traumatic lid and bony deformity were also excluded. The research proposal was approved by the institutional review board and ethics committee. An informed consent was obtained from all the patients included in the study. The operation was performed in the operation theatre with resuscitation facility, Ambu bag, oxygen supply and drugs required for cardiopulmonary resuscitation, with preparedness for possible problems occurring during the operation due to sedatives. Preoperative blood pressure and pulse were measured. Intra-operatively, at least three readings were taken and postoperative vitals and blood pressure were taken before shifting the patient to the ward. Technique of local anesthesia The delineating incision with a marking pencil was made. The local anesthetic agents were injected subcutaneously, parallel and anterior to the lacrimal crest in the lacrimal sac fossa, superior and posterior to the medial canthal tendon. Steps of external DCR surgery The middle nasal mucosa was packed with sterile ribbon gauge soaked in 2% lignocaine with 1:200,000 adrenaline. A straight vertical incision was made 26
3 medial to the inner canthus, avoiding the angular vein. The anterior lacrimal crest was exposed by blunt dissection. The periosteum was divided from the spine on the anterior lacrimal crest to the fundus of the sac and reflected forwards. The sac was reflected laterally from the lacrimal fossa. The anterior lacrimal crest and the bone from the lacrimal fossa were removed. A probe was introduced into the lacrimal sac through the lower canaliculus and the sac was incised in the 'H' shaped manner to create two flaps. A vertical incision was made in the nasal mucosa to create anterior and posterior flaps. The posterior flaps were excised. The anterior flaps were sutured together and suspended to the overlying muscle with Vicryl 6/0. The medial canthal tendon if divided during surgery was re-sutured to the periostium. The skin incision was closed with interrupted Vicryl sutures. The procedure was done by surgeons with more than 3 years of experience in doing external DCR surgery using the same surgical technique. Postoperative evaluation Syringing was done on the first postoperative day after removal of the nasal pack. Systemic oral antibiotic was given starting from one day before surgery for 7 days and topical for two weeks. A nasal vaso-constrictor drug was given for two weeks. The patients were discharged on the second post-operative day. Measurement of outcomes Pain score of the patients 0 No pain 0-3 Mild pain 4-6 Moderate pain 7-9 Severe pain 10 Maximum pain imaginable On completion of the surgery, the patient was asked to grade the severity of pain experienced during the surgery on a 0-10 numerical rating scale ('o' representing no pain and 10 representing worst pain imaginable). The rated values were categorized for analysis. Surgeon's comfort score during surgery This was also done by the visual analogue scale This is a 0-10 scale where 0 means no discomfort and 10 means maximum discomfort or surgery not possible without second analgesics. The numerical rating of surgeon's discomfort was done as follows. 0 No discomfort 0-3 Minimal discomfort 4-6 Moderate discomfort 7-9 Severe discomfort 10 Surgery not possible In case the patient in group A had unbearable pain and the surgeon's discomfort was so severe that surgery could not be continued, intravenous sedatives were given and surgery continued. Intra-operative complications Hemorrhage-intra-operative blood loss was measured by counting the number of average sized gauge pieces. A fully-soaked-standard sized gauge piece was considered to be equivalent to three to five ml blood loss. Injury to adjacent structures like angular vein, ethmoidal artery, CSF leakage and any other complications, if present, were noted. Duration of surgery The duration of surgery from the beginning of cleaning and draping to the application of the eye pad and bandaging was noted. Post-operative complications, if any, were also noted. Definition of successful surgery: A patent lacrimal passage on syringing and or the patient free of symptom was considered successful surgery. Follow-up The post-operative variables were evaluated on the 1st post-operative day, at 1st week, 6 weeks, 3 months and 6 months. Results Patient characteristics Seventy-two percent of the patients belonged to the age group years. The mean age ± SD of the patients was 34.4±12.12 years (95% CI= years). The mean age in group A was 34.06±12.04 years (95% CI= years) while in group B was 34.74±12.30 years (95% CI= years). Both groups were comparable (p value=0.78). Most of the patients (69%) were female. The female: male ratio in 27
4 group A was 3.5:1 while in group B was 3.4:1 (p=>0.05). 62% of the study populations were house wives, 11% students, 10% farmers, 6% labors, 3% businessmen, 3% tailors and 2% service holders. Sixty percent of the study population was from India and 40% from Nepal. Among the Nepalese, 16% were from Sunsari district and the remaining from near-by districts of eastern Nepal. Twenty-two patients in group A and 28 in group B had dacryocystitis in right eye, while 25 in group A and 20 in group B had it in left eye. Three patients in group A and 2 in group B had bilateral disease. Of the total, 5% had bilateral involvement. The mean duration of symptoms in group A was 1.34±0.88 years (95% CI= years) while in group B it was 1.13±0.89 years (95% CI= years). There was no difference in duration of symptoms in the two groups (p=0.24). Changes in vital signs (pulse rate and blood pressure) are given in Table 1. Intra-operative pain In group A, all patients (50) had pain while in group B, 50% (25patients) had pain and 50% (25 patients) did not have pain (p=<0.001). Grading of pain In group A, 2% of patients had maximum pain imaginable, 32% had severe pain, 34% had moderate pain, 32% had mild pain, while in group B, 8% patients had severe pain, 20% had moderate pain and 72% had mild pain (p value <0.001). Surgeon's discomfort In group A, the surgeon had no or minimal discomfort in 15 cases, and moderate discomfort or more in 35 cases; while in group B, the surgeon had no or minimal discomfort in 45 cases and moderate discomfort or more in 5 patients (p value ). Comparison of blood loss In group A, 29 patients had less than 20 ml of blood loss, and 21 patients had > 20 ml while in group B, 40 patients had less than 20 ml of blood loss and 10 patients had > 20 ml (p value 0.017). Table 1 Comparison of pre-operative, intra-operative and post-operative vitals Characteristic Categories Mean ± SD p value Group A Group B Preoperative Systolic BP 120.2± ± vitals (mmhg) Diastolic BP 78.16±8 77.2± (mmhg) Pulse Rate 83.36± ± (per minute) Intra-operative Systolic BP ± ± vitals (mmhg) Diastolic BP 82.72± ± (mmhg) Pulse Rate 88.6± ± (per minute) Postoperative Systolic BP 125.8± ± vitals (mmhg) Diastolic BP 81.28± ± (mmhg) Pulse Rate 86.52± ± (per minute) Table 2 Grading of intra-operative pain Groups Number Mild Moderate Severe Maximum of pain patients imaginable Group A 50 32% 34% 32% 2% Group B 25 72% 20% 8% 0% p-value Table 3 Surgeon's discomfort Groups No or minimal Moderate discomfort discomfort or more Group A Group B 45 5 P value
5 Duration of surgery The duration of surgery in group A was 82.5±6.2 minutes while in group B 77.5±5.9 minutes (p value=0.08). Success rate of surgery (among the followed-up patients) 1st POD: 100% in both groups 7th POD: 94% in group A 96% in group B 6 weeks: 87.9% in group A 90.1% in group B 3 months: 83.3% in group A 88.9% in group B 6 months: 87.5% in group A 92.35% in group B Follow-up rate 7th POD: 100% in both groups. 6 weeks: 66% in group A 66% in group B 3 months: 36% in group A 36% in group B 6 months: 16% in group A 26% in group B Discussion Since tear secretion decreases with age, the actual prevalence of NLD blockade reported in older people may just be an underestimation. Dalgesh et al (1967) in a large series of normal subjects older than 40 years observed the incidence of NLD obstruction in males and females to be 9% and 10% respectively. After 90 years of age, the prevalence was reported to be 35-40%. Other studies have supported this fact. In older age, the lacrimal system loses elasticity and fails to flush the debris which is collected through the complex and this might be one of the reasons for increased prevalence in these age groups. Ali and Ahmad (2002) reported that 70.8% of the patients of chronic dacryocystitis were in the age group years. Similarly, Dresner et al (1991) reported the highest disease prevalence in age group years. According to a study by Zaman et al, 80% of the patients with chronic dacryocystitis were in the age group years (Zaman et al 2003). According to the recent study by Badhu et al (2005) in eastern Nepal, the mean age of patients with chronic dacryocystitis was 27.4±13.7 years (95% CI=26.34 to years). As expected, we also found similar results. The mean age group of our patients was 34.4±12.12 years (95% CI= years). 71% of them belonged to the years group. We couldn't explain the difference in the age of presentation as reported in the literature from the western and neighboring countries. It is likely that some genetic, environmental, hormonal or some unidentified insults may be responsible. Most of the authors have reported that the disease is more common in females. It has been suggested that females have a nasolacrimal duct of smaller length and size. Also, the angulation of the canal where obstruction is more likely is more in females. These anatomical factors might be a reason why this condition is more common in females. The association of chronic dacryocystitis with serious gynecological pathology or hysterectomy due to de-epithelization is reported by Zolli and Stanon. They reasoned it to be due to hormonal imbalance (Zolland et al 1973). The fact that the disease is more prevalent in the younger age group contradicts this hypothesis (Badhu et al 2005). We did not study the socioeconomic status of the patients though some studies report a higher prevalence in patients of a lower socioeconomic class. We studied the occupation, which can be taken as one of the arms of socioeconomic status. Most of our patients were housewives. Since two-third of our study population was female, it is no surprise that housewives were found to be commonly affected. We think it is a chance association rather than a cause effect. A larger sample with involvement of different professions would confirm whether profession has any role in its pathogenesis. The published study from this part of Nepal reported a higher incidence in patients coming from subtropical lowlands with monsoon climate (Badhu et al 2005, 2006). In our study, the majority of the patients were from subtropical lowlands of Nepal and India. While analyzing the nasolacrimal duct involvement, we found that most (95%) of the patients had unilateral involvement. Fifty percent of the patients had it on the right side and 45% on the left side. But as described in the literature, dacryocystitis is more common in the left 29
6 eye compared to the right eye (Delaney et al 2002). The cause of right preponderance in our study may be due to the small sample size. The mean duration of symptoms was 1.23±0.8 years (95% CI= years).the symptoms of the patients varied from 6 months to 3 years. The duration of the symptoms mentioned in the literature is variable, the maximum reported being 50 years. In our study, there was an increase in intraoperative blood pressure and pulse rate in both the groups. However, the increase in pulse was significantly higher in group A than in group B. The increase in intraoperative and postoperative blood pressure and pulse in group A compared to group B can be explained as the group A patients had more pain compared to group B. In group A, all patients complained of pain, while in group B, 50% of the patients had pain. The severity of pain was more in group A compared to group B. (p value <0.001). In group A, the surgeons rated moderate or more discomfort in 35 cases while in group B, moderate or more discomfort was rated only in 5 cases. Discomfort was significantly higher in group A, compared to group B (p value <0.001). The significant difference in pain and comfort can be explained by the fact that only local anesthesia was given in group A while in group B, local anesthesia with sedatives was given. The amount of blood loss was more in group A compared to group B (p=0.017). The more hemorrhage in group A can be explained by the surgeon's discomfort and the intraoperative pain experienced by the patients. The duration of surgery in both groups was comparable (p value=0.08). This is because the duration of surgery depends on the surgeon's skill. On the 7th POD, 1 patient in group A and 2 patients in group B had wound infection. According to Yazici and Meyer (2002), postoperative wound infection in DCR surgery can be controlled by selective use of antibiotics preoperatively and postoperatively. All the patients were given pre- and post-operative antibiotics in our study. Poor personal hygiene and inadequate cleaning of the wound may be the cause of the wound infection. Success of surgery is defined as patent lacrimal passage on syringing and free of watering. All the patients in both the groups had patent lacrimal passage on syringing on the first postoperative day. After six months, 87.5% of the patients in group A and 92% of the patients in group B had patent syringing. The success of conventional primary external DCR with or without mucosal flap is 85% to 99%. The success rate reported from this part of Nepal is 88.6% (Badhu et al 2005). In our study, the success rate was comparable on the 1st POD, 7th POD and at 6 weeks. But success rate was more in group B than in A after 6 weeks. This is due to the inequality in the follow-up rates in the two groups. Attempts were made to increase the follow-up rate by explaining about the need of post-operative syringing and evaluation. The low follow-up rate may be due to the low socioeconomic condition, transportation difficulties and tendency of the patients not to return for follow-up once their symptoms are relieved. Conclusion The demographic patterns and success rate of DCR surgery are similar to the previous reports from this part of the world. The use of sedatives improves the outcome of DCR surgery in terms of patient's pain, surgeon's comfort and intraoperative complications. References Ali A, Ahmad T A (2002). Dacryocystorhinostomya review of 51 cases. Pak J Ophthalmol 18; 4: Badhu B P, Karki B S, Khanal B, Dulal S, Das H (2006). Microbiological patterns of dacryocystitis. Ophthalmology 113 (12): 2377, p 1-2 Badhu B, Dulal S, Kumar S, S.K.D. Thakur, A. Sood, H. Das (2005). Epidemiology of Chronic Dacryocystitis and Success Rate of External Dacryocystorhinostomy in Nepal. Orbit 24: Benger R (1992). Day-surgery external dacryocystorhinostomy. Aust N Z J Ophthalmol 20: Caldwell GW (1993). Two new operations for obstruction of the nasal duct with preservation of 30
7 the canaliculi and an incidental description of a new lacrimal probe. Med J 57: 581. Dalgesh R, Mannor GE, Milalan AL, Barret L (1967). Idiopathic acquired lacrimal drainage obstruction. Br J Ophthalmol 51: 643 Delaney YM, Khoosabeh R, Lagalla R, Ponte F, Mc Lean CJ et al (2002). External DCR for the treatment of the acquired partial nasolacrimal duct obstruction in adults. Br Journal of Ophthalmology 86: Dresner S C, Klussman K G, Meyer D R et al (1991). Outpatient dacryocystorhinostomy. Ophthalmic Surg 22: Duffy MT, Mass R, Parlak M, Koorneef L, Bosmak S, et al (2000). Advances in lacrimal surgery. Current opin Ophthalmol 11(5): Fanning GL (2000). Local anesthesia for dacryocystorhinostomy. Current Anaesthesia and Critical Care 11: Gonnering RS, Lyon DB, and Fischer JC (1991). Endoscopic laser-assisted lacrimal surgery. Am J Ophthalmol 111: 152. Massaro BM, Gonnering RS, Harris GJ (1990). Endonasal laser DCR. A new approach to nasolacrimal duct obstruction. Arch. Ophthalmol 108:1172. O Donnell B, Shah R, Harris GJ, Rose GE, Puukula P et al (2001). Dacryocystorhinostomy for epiphora in the presence of a patent lacrimal system. Clin Experiment Ophthalmol 29(1): Toti A (1904). Nuovo metodo conservatore di cura radicale delle suppurazioni croniche del sacco lacrimale (dacrio cistorhinostomia). Clin Moderna (Firanze) Yazici B, Meyer DR (2002). Selective antibiotic use to prevent postoperative wound infection after external dacryocystorhinostomy. Ophthal Plast Reconstr Surg 18 (5): Zaman M, Babar TF, Saeed N (2003), A review of 120 cases of dacryocystorhinostomies (Dutemps and Bourguet technique). J Aub Med Coll Abbotabad 15: Zolland S NL, Oguya JH, Pratt LL, Kominek P, Novak V (1973). Cancer of the lacrimal sac. Presentation of five cases and review of the literature. Ann Otol Rhionol 82; 2:
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS
 DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
THE EXTERNAL DACRYOCYSTORHINOSTOMY (DCR)
 Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction
 Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Repeat DCR with Silicone Tube intubation : A Prospective Study.
 Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Dacryocystorh i nostomy in South West England
 Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy
 Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Shreya M. Shah, Mehul A. Shah & Chintan Patel
 Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
Minimally Invasive Technique of Dacryocystorhinostomy
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy
 SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider
 Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice
 10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
To analyse the success rate of external Dacryocystorhinostomy related with anatomical osteotomy size made during surgery
 2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
Comparison of outcome of external DCR and endonasal DCR surgery among the rural population
 Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
International Journal of Pharma and Bio Sciences
 Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Modified endoscopic dacryocystorhinostomy with posterior lacrimal sac flap for nasolacrimal duct obstruction!"#$%&'()*+,-*&'!./0(&
 Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences,
Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences,
Congenital lacrimal fistula
 Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy surgeries, a randomized clinical study
 Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Pediatric Epiphora. Lacrimal drainage system begins to develop at the. Pediatric Ophthalmology. Saurbhi Khurana MD, FICO
 Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
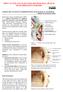 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population
 Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Lacrimal drainage surgery in patients with rare nasal diseases
 (2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
(2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
Syringing And Probing Under Local Anesthesia In Infants
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
A simple and evolutional approach proven to recanalise the nasolacrimal duct obstruction
 See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience
 Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Preoperative Computed Tomography Findings for Patients with Nasolacrimal Duct Obstruction or Stenosis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic Dacryocystitis
 Kuldeep Thakur et al ORIGINAL ARTICLE 10.5005/jp-journals-10013-1314 Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic
Kuldeep Thakur et al ORIGINAL ARTICLE 10.5005/jp-journals-10013-1314 Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic
Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction
 J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Repair of Eyelid Trauma
 Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application
 10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
Nasolacrimal duct obstruction: the relationship with nasal allergy
 Romanian Journal of Rhinology, Vol. 7, No. 27, July - September 2017 DOI: 10.1515/rjr-2017-0018 Original study Nasolacrimal duct obstruction: the relationship with nasal allergy Desiderio Passali 1, Leandro
Romanian Journal of Rhinology, Vol. 7, No. 27, July - September 2017 DOI: 10.1515/rjr-2017-0018 Original study Nasolacrimal duct obstruction: the relationship with nasal allergy Desiderio Passali 1, Leandro
Yunhai Tu, 1 Zhenbin Qian, 2 Jiao Zhang, 1 Wencan Wu, 1 and Tianlin Xiao Introduction. 2. Patients and Methods
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy
 Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Awake regional versus general anesthesia in preterms and ex-preterm infants for herniotomy Department of Anaesthesia University Children s Hospital Zurich Switzerland Epidemiology Herniotomy needed in
Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment of Canalicular Obstruction
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/10.3341/k jo.2017.31.1.1 Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/10.3341/k jo.2017.31.1.1 Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment
ORIGINAL ARTICLE. Intranasal Localization of the Lacrimal Sac
 ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis
 Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Treatment of obstructive epiphora in adults by balloon dacryocystoplasty
 692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici,
692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici,
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION
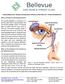 NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
INTERVENTIONAL PROCEDURES PROGRAMME
 Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Philippine Journal of OPHTHALMOLOGY ABSTRACT
 Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 80/ Oct. 05, 2015 Page 14022
 STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
ENDONASAL CARBON-DIOXIDE LASER ASSISTED DACRYOCYS- TORHINOSTOMY VERSES EXTERNAL DACRYOCYSTORHINOSTOMY
 9 Main Article ENDONASAL CARBON-DIOXIDE LASER ASSISTED DACRYOCYS- TORHINOSTOMY VERSES EXTERNAL DACRYOCYSTORHINOSTOMY Ashok Verma, Mazin Al Khabori, Rajiv Zutshi* ABSTRACT: This is a prospective, non- randomized
9 Main Article ENDONASAL CARBON-DIOXIDE LASER ASSISTED DACRYOCYS- TORHINOSTOMY VERSES EXTERNAL DACRYOCYSTORHINOSTOMY Ashok Verma, Mazin Al Khabori, Rajiv Zutshi* ABSTRACT: This is a prospective, non- randomized
Effects of Nasopore Packing on Dacryocystorhinostomy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):73-80 http://dx.doi.org/10.3341/kjo.2013.27.2.73 Effects of Nasopore Packing on Dacryocystorhinostomy Original Article Sun Young Jang 1,
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):73-80 http://dx.doi.org/10.3341/kjo.2013.27.2.73 Effects of Nasopore Packing on Dacryocystorhinostomy Original Article Sun Young Jang 1,
Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy
 Original Article Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy Khawaja Khalid Shoaib, Salahuddin Ahmad, Muhammad Manzoor, Sabihuddin Ahmed, Iftikhar Aslam Syed Nadeem ul Haq Pak
Original Article Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy Khawaja Khalid Shoaib, Salahuddin Ahmad, Muhammad Manzoor, Sabihuddin Ahmed, Iftikhar Aslam Syed Nadeem ul Haq Pak
Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy
 Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study
 ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
Regional nerve block of the upper eyelid in oculoplastic surg e r y
 E u ropean Journal of Ophthalmology / Vol. 16 no. 4, 2006 / pp. 5 0 9-5 1 3 Regional nerve block of the upper eyelid in oculoplastic surg e r y A.R. ISMAIL, T. ANTHONY, D.J. MORDANT, H. MacLEAN Portsmouth
E u ropean Journal of Ophthalmology / Vol. 16 no. 4, 2006 / pp. 5 0 9-5 1 3 Regional nerve block of the upper eyelid in oculoplastic surg e r y A.R. ISMAIL, T. ANTHONY, D.J. MORDANT, H. MacLEAN Portsmouth
Comparison of preoperative infraorbital block with periincisional infiltration for postoperative pain relief in cleft lip surgeries
 Original Article Comparison of preoperative infraorbital block with periincisional infiltration for postoperative pain relief in cleft lip surgeries V. Gaonkar, Swati R. Daftary Department of Anaesthesia,
Original Article Comparison of preoperative infraorbital block with periincisional infiltration for postoperative pain relief in cleft lip surgeries V. Gaonkar, Swati R. Daftary Department of Anaesthesia,
Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study
 10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
Management of epiphora and lacrimal obstruction in adults
 Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Original Article Bicanalicular intubation procedure for acquired punctual stenosis
 Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Watery Eye. Watering of the eye (epiphora) Causes of overproduction of tears
 Watery Eye Watery Eye Tears are formed by the lacrimal gland, which lies beneath the outer part of the upper lid, and by cells in the conjunctival surface of the eye. Watering of the eye (epiphora) This
Watery Eye Watery Eye Tears are formed by the lacrimal gland, which lies beneath the outer part of the upper lid, and by cells in the conjunctival surface of the eye. Watering of the eye (epiphora) This
Endonasal dacryocystorhinostomy was first. Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study. Main Article
 Main Article Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study Sudip Kumar Das, 1 Chiranjib Das, 1 Amit Bikram Maiti, 2 Ruma Guha, 3 Subhendu Chowdhury 1 ABSTRACT Introduction Over last
Main Article Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study Sudip Kumar Das, 1 Chiranjib Das, 1 Amit Bikram Maiti, 2 Ruma Guha, 3 Subhendu Chowdhury 1 ABSTRACT Introduction Over last
INFORMATION REGARDING YOUR NASAL SURGERY
 INFORMATION REGARDING YOUR NASAL SURGERY This document contains information about the following aspects of nasal surgery: Pre-op information: How to prepare for surgery. Procedure: Wat is done during surgery.
INFORMATION REGARDING YOUR NASAL SURGERY This document contains information about the following aspects of nasal surgery: Pre-op information: How to prepare for surgery. Procedure: Wat is done during surgery.
The modified endoscopic pre-lacrimal approach: how I do it
 Specialty Techniques Page 1 of 6 The modified endoscopic pre-lacrimal approach: how I do it Leslie T. Koh 1, Rataphol C. Dhepnorrarat 2 1 Department of Otolaryngology-Head & Neck Surgery, Changi General
Specialty Techniques Page 1 of 6 The modified endoscopic pre-lacrimal approach: how I do it Leslie T. Koh 1, Rataphol C. Dhepnorrarat 2 1 Department of Otolaryngology-Head & Neck Surgery, Changi General
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Dr. Najah طب بغداد. Lecture: 14
 2015 2016 The lacrimal apparatus The lacrimal system consists of: Lecture: 14 Dr. Najah طب بغداد 1- Secretory portion: Comprises the following: a- The lacrimal gland: Which is divided into palpebral (Aqueoussecretion)
2015 2016 The lacrimal apparatus The lacrimal system consists of: Lecture: 14 Dr. Najah طب بغداد 1- Secretory portion: Comprises the following: a- The lacrimal gland: Which is divided into palpebral (Aqueoussecretion)
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
PUBLISHED VERSION.
 PUBLISHED VERSION Shay Keren, Gad Dotan, Leah Leibovitch, Dinesh Selva, and Igal Leibovitch Indocyanine green assisted removal of orbital lacrimal duct cysts in children Ophthalmology, 2015; 2015:130215-1-130215-5
PUBLISHED VERSION Shay Keren, Gad Dotan, Leah Leibovitch, Dinesh Selva, and Igal Leibovitch Indocyanine green assisted removal of orbital lacrimal duct cysts in children Ophthalmology, 2015; 2015:130215-1-130215-5
Stent technique for endoscopic dacryocystorhinostomy Our expertise
 Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Comparative Study Of Probing Done with and without Endoscopic Assistance
 Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
FACTORS AFFECTING THE SUCCESS RATE OF EXTERNAL DACRYOCYSTORHINOSTOMY AT B. P. KOIRALA INSTITUTE OF HEALTH SCIENCES, DHARAN, NEPAL
 FACTORS AFFECTING THE SUCCESS RATE OF EXTERNAL DACRYOCYSTORHINOSTOMY AT B. P. KOIRALA INSTITUTE OF HEALTH SCIENCES, DHARAN, NEPAL 1* 1 2 Pokharel SM, Chaudhary SK, Chaurasiya BD Affiliation 1. Assistant
FACTORS AFFECTING THE SUCCESS RATE OF EXTERNAL DACRYOCYSTORHINOSTOMY AT B. P. KOIRALA INSTITUTE OF HEALTH SCIENCES, DHARAN, NEPAL 1* 1 2 Pokharel SM, Chaudhary SK, Chaurasiya BD Affiliation 1. Assistant
A study of comparison between the efficacy of endoscopic septoplasty and traditional septoplasty
 International Surgery Journal Yadav PK et al. Int Surg J. 2016 Aug;3(3):1134-1140 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20162190
International Surgery Journal Yadav PK et al. Int Surg J. 2016 Aug;3(3):1134-1140 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20162190
Original Article External dacryocystorhinostomy outcomes in patients with a history of dacryocystitis
 Original Article External dacryocystorhinostomy outcomes in patients with a history of dacryocystitis Daniel R. Lefebvre, MD, a,b Sonya Dhar, MD, c,d Irene Lee, MD, e Felicia Allard, MD, f and Suzanne
Original Article External dacryocystorhinostomy outcomes in patients with a history of dacryocystitis Daniel R. Lefebvre, MD, a,b Sonya Dhar, MD, c,d Irene Lee, MD, e Felicia Allard, MD, f and Suzanne
Keywords: Dexmedetomidine, fentanyl, tympanoplasty, monitored anaesthesia care. INTRODUCTION:
 13 Original article A COMPARATIVE OBSERVATIONAL STUDY BETWEEN DEXMEDETOMIDINE V/S COMBINATION OF MIDAZOLAM- FENTANYL FOR TYMPANOPLASTY SURGERY UNDER MONITORED ANESTHESIA CARE Dr. Parul Pachotiya (Professor
13 Original article A COMPARATIVE OBSERVATIONAL STUDY BETWEEN DEXMEDETOMIDINE V/S COMBINATION OF MIDAZOLAM- FENTANYL FOR TYMPANOPLASTY SURGERY UNDER MONITORED ANESTHESIA CARE Dr. Parul Pachotiya (Professor
A randomized placebo controlled trial of Mitomycin - C in surgical outcome of primary endoscopic dacryocystorhinostomy
 Al Am een J Med Sci 2013; 6(3):231-236 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G A randomized placebo controlled trial of Mitomycin - C in
Al Am een J Med Sci 2013; 6(3):231-236 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G A randomized placebo controlled trial of Mitomycin - C in
Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy with and without Silicon Tube Intubation
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach
 Bahrain Medical Bulletin, Vol. 22, No. 1, March 2000 Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach Basel T Baarah, MD* Wael Abu-Laban, MD**
Bahrain Medical Bulletin, Vol. 22, No. 1, March 2000 Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach Basel T Baarah, MD* Wael Abu-Laban, MD**
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
A new method for identifying the cut ends in canalicular laceration
 www.nature.com/scientificreports OPEN ecei e : 23 une 201 ccepte : 25 anuar 2017 u is e : 24 e ruar 2017 A new method for identifying the cut ends in canalicular laceration Wenyan Peng 1, Yandong Wang
www.nature.com/scientificreports OPEN ecei e : 23 une 201 ccepte : 25 anuar 2017 u is e : 24 e ruar 2017 A new method for identifying the cut ends in canalicular laceration Wenyan Peng 1, Yandong Wang
Nasal Polyps. Multimedia Health Education. Disclaimer
 Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of Nasal Polyps must be made in conjunction with your Physician or
Disclaimer This movie is an educational resource only and should not be used to manage your health. All decisions about the management of Nasal Polyps must be made in conjunction with your Physician or
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Value of nasal endoscopy and probing in the diagnosis and management of children with congenital epiphora
 314 Department of Ophthalmology, Ninewells Hospital, Dundee DD1 9SY, UK C J MacEwen JDHYoung C W Barras Department of Otolaryngology B Ram P S White Correspondence to: Dr MacEwen c.j.macewen@dundee.ac.uk
314 Department of Ophthalmology, Ninewells Hospital, Dundee DD1 9SY, UK C J MacEwen JDHYoung C W Barras Department of Otolaryngology B Ram P S White Correspondence to: Dr MacEwen c.j.macewen@dundee.ac.uk
Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy
 Eur J Ophthalmol 2012; 00 ( 00) : 000-000 DOI: 10.5301/ejo.5000157 ORIGINAL ARTICLE Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy Juan
Eur J Ophthalmol 2012; 00 ( 00) : 000-000 DOI: 10.5301/ejo.5000157 ORIGINAL ARTICLE Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy Juan
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Balloon Dacryoplasty: Indications, Techniques and Outcomes
 INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
Controlled Trial of Wound Infiltration with Bupivacaine for Post Operative Pain Relief after Caesarean Section
 Bahrain Medical Bulletin, Vol.23, No.2, June 2001 Controlled Trial of Wound Infiltration with Bupivacaine for Post Operative Pain Relief after Caesarean Section Omar Momani, MD, MBBS, JBA* Objective: The
Bahrain Medical Bulletin, Vol.23, No.2, June 2001 Controlled Trial of Wound Infiltration with Bupivacaine for Post Operative Pain Relief after Caesarean Section Omar Momani, MD, MBBS, JBA* Objective: The
Commen Nose Diseases
 Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
Commen Nose Diseases Symptoms List: Nasal obstruction. Nasal discharge: Anterior (Rhinorrhea). Posterior (Postnasal discharge). Epistaxis. Hyposmia and Anosmia. Headache. Snoring. Nasal Obstruction Definition:
Proboscis lateralis: report of two cases
 The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 74/Dec 29, 2014 Page 15535
 RANDOMISED CLINICAL TRIAL TO COMPARE THE EFFECT OF PRETREATMENT OF KETAMINE AND LIGNOCAINE ON PROPOFOL INJECTION PAIN Hanumanthappa V. Airani 1, Bhagyashree Amingad 2, Chandra Kumar B. M 3 HOW TO CITE
RANDOMISED CLINICAL TRIAL TO COMPARE THE EFFECT OF PRETREATMENT OF KETAMINE AND LIGNOCAINE ON PROPOFOL INJECTION PAIN Hanumanthappa V. Airani 1, Bhagyashree Amingad 2, Chandra Kumar B. M 3 HOW TO CITE
Management of Extensive Maxillofacial Trauma With Bony Foreign Body Within the Orbit From a Chainsaw Injury
 Management of Extensive Maxillofacial Trauma With Bony Foreign Body Within the Orbit From a Chainsaw Injury Randall O. Craft, MD, a Kyle R. Eberlin, MD, a Michael H. Stella, MD, b and Edward J. Caterson,
Management of Extensive Maxillofacial Trauma With Bony Foreign Body Within the Orbit From a Chainsaw Injury Randall O. Craft, MD, a Kyle R. Eberlin, MD, a Michael H. Stella, MD, b and Edward J. Caterson,
A ptosis repair of aponeurotic defects by the posterior approach
 British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 586-590 A ptosis repair of aponeurotic defects by the posterior approach J. R. 0. COLLIN From the Department of Clinical Ophthalmology, Moorfields Eye Hospital,
Patient profile, indications, complications and Evaluation of Septoplasty outcome in a Base Hospital in Sri Lanka
 Patient profile, indications, complications and Evaluation of Septoplasty outcome in a Base Hospital in Sri Lanka Rubasinghe M.S., De Silva M.D.K., Wanasinghe W.M.S.C.L., De Livera R.J.K., Wimalaratna
Patient profile, indications, complications and Evaluation of Septoplasty outcome in a Base Hospital in Sri Lanka Rubasinghe M.S., De Silva M.D.K., Wanasinghe W.M.S.C.L., De Livera R.J.K., Wimalaratna
Lower Eyelid Malposition
 Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Effects of analgesia methods on serum IL-6 and IL-10 levels after cesarean delivery
 Effects of analgesia methods on serum IL-6 and IL-10 levels after cesarean delivery Z.-M. Xing*, Z.-Q. Zhang*, W.-S. Zhang and Y.-F. Liu Anesthesia Department, No. 1 People s Hospital of Shunde, Foshan,
Effects of analgesia methods on serum IL-6 and IL-10 levels after cesarean delivery Z.-M. Xing*, Z.-Q. Zhang*, W.-S. Zhang and Y.-F. Liu Anesthesia Department, No. 1 People s Hospital of Shunde, Foshan,
The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR)
 International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubric (ICO-OSCAR) The International Council of Ophthalmology s Ophthalmology Surgical Competency Assessment Rubrics
A new method using xenogeneicacellular dermal matrix in the reconstruction of lacrimal drainage
 A new method using xenogeneicacellular dermal matrix in the reconstruction of lacrimal drainage Li Chen, 1,2,3 Bo Gong, 2,3,4 Zhengzheng Wu, 1,2,3 Jacquelyn Jetton, 5 Rong Chen, 2,3,4 Chao Qu 1,2,3 1 Department
A new method using xenogeneicacellular dermal matrix in the reconstruction of lacrimal drainage Li Chen, 1,2,3 Bo Gong, 2,3,4 Zhengzheng Wu, 1,2,3 Jacquelyn Jetton, 5 Rong Chen, 2,3,4 Chao Qu 1,2,3 1 Department
A Prospective comparative study of Local anaesthesia & Spinal anaesthesia for Lichtenstein hernioplasty in a tertiary care hospital
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. VII (Nov. 2015), PP 47-51 www.iosrjournals.org A Prospective comparative study of Local
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. VII (Nov. 2015), PP 47-51 www.iosrjournals.org A Prospective comparative study of Local
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Surgical Correction of Crow s Feet Deformity With Radiofrequency Current
 INTERNATIONAL CONTRIBUTION Oculoplastic Surgery Surgical Correction of Crow s Feet Deformity With Radiofrequency Current Min-Hee Ryu, MD; David Kahng, MD; and Yongho Shin, MD, PhD Aesthetic Surgery Journal
INTERNATIONAL CONTRIBUTION Oculoplastic Surgery Surgical Correction of Crow s Feet Deformity With Radiofrequency Current Min-Hee Ryu, MD; David Kahng, MD; and Yongho Shin, MD, PhD Aesthetic Surgery Journal
POLYTHENE TUBES IN CANALICULUS SURGERY*
 Brit. J. Ophthal. (1963) 47, 203. POLYTHENE TUBES IN CANALICULUS SURGERY* BY T. P. GRIFFITHt From the Corneo-Plastic Unit and Regional Eye Bank, Queen Victoria Hospital, East Grinstead, Sussex CANALICULUS
Brit. J. Ophthal. (1963) 47, 203. POLYTHENE TUBES IN CANALICULUS SURGERY* BY T. P. GRIFFITHt From the Corneo-Plastic Unit and Regional Eye Bank, Queen Victoria Hospital, East Grinstead, Sussex CANALICULUS
Morphological and morphometrical study of the nasal opening of nasolacrimal duct in man
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
