Transarterial access through arteriotomy of the femoral artery
|
|
|
- Pamela Johnston
- 5 years ago
- Views:
Transcription
1 TECHNICAL NOTE C.-H. Yeh Y.-M. Wu C.-H. Toh Y.-L. Chen H.-F. Wong A Safe and Efficacious Alternative: Sonographically Guided Internal Jugular Vein Puncture for Intracranial Endovascular Intervention SUMMARY: Transvenous interventions for intracranial vascular lesions are usually performed via venous access of a femoral vein puncture. However, the transjugular route is an alternative with a shorter and less tortuous vascular access for intracranial lesions. Although puncture of the internal jugular vein is generally believed to be too dangerous owing to potential hazardous complications, the safety of the sonographically guided retrograde internal jugular vein puncture technique for intracranial intervention has not been fully evaluated in the English literature. We present our experience with a total of 44 transjugular intervention procedures between April 1999 and June We believe sonographically guided internal jugular vein puncture is a safe and efficacious technique for establishing transvenous access for an intracranial endovascular intervention. ABBREVIATIONS: CCF carotid cavernous fistula; DAVF dural arteriovenous fistula; ECA external carotid artery; GDC Guglielmi detachable coil; ICA internal carotid artery; n-bca n-butyl cyanoacrylate; SVC superior vena cava; VA vertebral artery Transarterial access through arteriotomy of the femoral artery is most commonly used in intracranial endovascular neurointerventions. 1 Through this transarterial route, endovascular procedures are performed for embolization of intracranial vascular lesions and hypervascular tumors. In addition, angioplasty and stent placement for arterial stenosis are also performed in a similar manner. However, some intracranial vascular lesions, including CCF, DAVF, or dural sinus thrombosis, are sometimes preferably managed by a transvenous access. 2,3 The transvenous routes can be established via common femoral vein puncture, internal jugular vein puncture, or direct puncture of abnormally dilated venous sacs. 4 However, puncture of the internal jugular vein for intracranial intervention is generally believed to be dangerous due to the large sheaths used during the procedure, the difficulties in holding adequate pressure against the airway and other soft tissues of the neck during hemostasis, the potential serious complications of expanding cervical hematomas, and the risk of inadvertent carotid artery injury. In our department, we routinely perform a sonographically guided technique in difficult cases of arterial and venous puncture. However, to our knowledge, the safety, efficacy, and potential risk of sonographically guided retrograde internal jugular vein puncture for intracranial intervention has not been fully evaluated in the English literature. In this study, we retrospectively reviewed the consecutive patients who underwent sonographically guided internal jugular vein puncture for an intracranial interventional procedure in our institution during the past 10 years. The safety, efficacy, and potential Received July 12, 2010; accepted after revision September 14. From the Department of Medical Imaging and Intervention, Chang Gung Memorial Hospital, Linkou, and College of Medicine, Chang Gung University, Taoyuan, Taiwan. Please address correspondence to Ho-Fai Wong. MD, Department of Medical College of Medicine, Imaging and Intervention, Chang Gung Memorial Hospital, Linkou, No. 5, Fu Hsing St, Gueishan, Taoyuan 333, Taiwan, R.O.C.; hfwong@adm.cgmh.org. or hfwong@ms4.hinet.net complications of this procedure were collected and analyzed in this study. Technique Patients From April 1999 to June 2010, 44 transjugular intracranial interventions using a sonographically guided internal jugular vein puncture technique were performed in 42 patients at our institution. Two of these patients underwent a second transjugular intervention 2 months and 1.5 years, respectively, after the first procedure. All procedures were performed in accordance with the guidelines of the institutional review board, which approved our retrospective medical chart review and analysis. Procedure Except for 2 procedures of venous sampling, all procedures were performed with the patients under general anesthesia. The site of internal jugular vein puncture was chosen according to the site, location, and venous drainage pattern of the vascular lesion. Patency of the selected Table 1: Patient demographics, coagulation profile, and diagnosis a Demographics Data Mean age (yr) Sex Male 16 Female 26 Coagulation profile Prothrombin time (international normalized ratio) Activated partial thromboplastin time Platelets Diagnosis DAVF, without venous occlusion 11 DAVF, with venous occlusion 5 Venous occlusion 1 CCF 22 DAVF and CCF 1 Cushing syndrome 2 a N 42. INTERVENTIONAL TECHNICAL NOTE AJNR Am J Neuroradiol 33:E7 E12 Jan E7
2 Table 2: Summary of transjugular vein interventional procedures Procedure Data Classification of intervention (n 44) Transvenous embolization 40 Thrombolysis 1 Venous angioplasty and stenting 1 Venous sampling 2 Neck puncture site (n 44) Right internal jugular vein 18 Left internal jugular vein 20 Bilateral internal jugular veins 6 Embolizer used in transvenous embolization (n 40) Microcoil 36 Microcoil and vascular plug 1 Microcoil and n-bca 1 n-bca 2 Concurrent transarterial embolization (n 10) ICA 1 ECA 9 internal jugular vein was confirmed by using real-time sonography with compression and a color Doppler technique. A freehand technique was used in all patients. The selected internal jugular vein was punctured with an 18-ga needle catheter under sonographic guidance. A 6F sheath was introduced into the internal jugular vein by using the Seldinger technique. Right common femoral artery puncture was performed with a conventional method. A 5F or 5.5F catheter was navigated into the feeding artery to obtain the venous roadmap. If needed, complete angiography of bilateral ICAs, ECAs, and VAs was performed to assess the size and location and relationship of feeding arteries and drainage veins of the vascular lesion. Selective catheterization of the dural venous sinus, usually the inferior petrosal sinus or the sigmoid sinus, was performed with a hydrophilic polymer-coated inch angled soft guidewire and a 5F or 5.5F end-hole guiding catheter. A microcatheter with a microwire was navigated coaxially to the optimal location for intervention. Then embolization or other procedures were performed with realtime digital subtraction fluoroscopic mapping. Angiography was performed immediately after completion of the procedure to check the outcome. Patents were generally followed by clinical evaluation. Conventional angiography or MR angiography re-evaluation was performed if clinically indicated. Results Patient Population, Coagulation Profile, and Diagnosis The patient demographics, average of the coagulation profile, and indication for treatment are presented in Table 1. Coagulopathy (prolonged prothrombin time, activated partial thromboplastin time, or decreased platelet count) was found in only 1 patient. Among the 42 patients enrolled, 16 underwent transvenous embolization treatment for DAVFs. Cerebral venous occlusion was present in 5 and absent in 11 of these 16 patients with DAVFs. One patient had a superior sagittal sinus occlusion without a coexistent DAVF. Trans- Fig 1. A 61-year-old woman with a right sigmoid sinus DAVF. A, Right internal carotid artery angiogram in an anteroposterior projection shows early opacification of the right sigmoid sinus and internal jugular vein with retrograde venous drainage through cerebral vein. B and C, After venous sheaths are placed in the bilateral internal jugular veins, trapping of the right sigmoid sinus is performed with a vascular plug (through the right internal jugular vein) and 28 GDCs (through the left internal jugular vein access). D, The fistula is completely obliterated after embolization. E8 Yeh AJNR 33 Jan
3 Fig 2. A 63-year-old man with a left indirect CCF. A, Left ICA angiogram in a lateral projection shows early opacification of the cavernous sinus with venous drainage mainly through the left superior ophthalmic vein. B and C, After a 6F sheath is placed into the left internal jugular vein (B), a microcatheter is navigated through the left facial vein, left angular vein, and left superior ophthalmic vein into the left cavernous sinus (C). After 16 GDCs were deployed, the left cavernous sinus was completely occluded without residual fistula. venous embolization of CCFs was performed in 23 patients. One patient with a coexistent CCF and a left jugular bulb DAVF had transvenous embolization for the CCF. Two patients with Cushing syndrome had left internal jugular puncture and right femoral vein puncture simultaneously for venous sampling. Sonographically Guided Internal Jugular Vein Puncture A sonographically guided puncture technique was performed in all 44 procedures. The internal jugular vein sheath was removed immediately after the procedure. After manual compression for 10 minutes, the venotomy wound was simply covered with gauze. No life-threatening complication or inadvertent carotid artery injury occurred. No additional procedure was required for hemostasis of the venotomy wound. No clinically discernible neck hematoma was found. Technique of Transjugular Vein Interventions Details of internal jugular vein puncture, transvenous intervention, and concurrent transarterial intervention are summarized in Table 2. Bilateral internal jugular vein puncture was performed in 6 patients to achieve optimal embolization therapy. In 2 of these 6 patients, a bilateral internal jugular vein approach was necessary for both proximal and distal segment embolization when trapping occluded dural sinuses and associated DAVFs (Fig 1). In the other 4 patients, puncture of the contralateral internal jugular was performed for alternative vascular access after failure of the initially planned transvenous route. Catheterization was performed through the inferior petrosal sinus to the cavernous sinus in 23 patients; through the facial vein, angular vein, and superior ophthalmic vein to the cavernous sinus in 6 patients; to the superior petrosal sinus in 1 patient; through the dural venous sinuses to the superior sagittal sinus in 3 patients; and to the unilateral or contralateral jugular bulb, sigmoid, or transvenous or marginal sinuses in 11 patients. Transvenous embolization performed mainly with electrically detachable coils (GDCs; Boston Scientific, Natick, Massachusetts). One patient with superior sagittal sinus occlusion had mechanical and chemical thrombolysis. Jugular bulb angioplasty and stent placement were performed in 1 patient with jugular bulb occlusion and a DAVF. Concomitant transarterial embolization of feeding arteries with Onyx (ev3, Irvine, California), n-bca, or particles was performed in 9 procedures. Procedure-Related Complications In 1 patient with a right marginal sinus DAVF, herniation and fixation of a microcoil into the internal jugular vein occurred. However, the internal jugular vein remained patent in subsequent follow-up angiography. In 1 patient with left transverse and sigmoid sinus DAVFs, embolization of the left superior petrosal sinus and engorged venous sacs in the left cerebropontine angle was performed to obliterate the extensive fistula and venous drainage. Unfortunately, left temporal intraparenchymal hemorrhage, subdural hemorrhage, and subarachnoid hemorrhage occurred immediately after embolization. This AJNR Am J Neuroradiol 33:E7 E12 Jan E9
4 Fig 3. A 53-year-old man with bilateral indirect CCFs. A and B, Left ICA angiogram in lateral (A) and anteroposterior (B) projections shows early opacification of bilateral cavernous sinuses with venous drainage through the bilateral superior ophthalmic vein. C, After the venous access is established, a microcatheter is navigated through the right facial vein, right superior ophthalmic vein, right cavernous sinus, and left cavernous sinus and into the left superior ophthalmic vein. Then embolization of bilateral superior ophthalmic veins and cavernous sinuses is performed with 31 GDCs. D, No residual fistula is seen on the postembolization angiogram. patient died due to extensive intracranial hemorrhage. In a patient with bilateral CCFs, transarterial embolization of a right-sided fistula with Onyx was performed after optimal transvenous embolization of a left-sided fistula with microcoils. However, regurgitation of Onyx though the residual fistula into the left ICA occurred. The cavernous and clinoid segments of left ICA were completely occluded. Patent collateral perfusion through the anterior communicating artery and left posterior communicating artery was confirmed immediately on right ICA angiography. The patient had only a minor infarct in the left corona radiata and body of the left corpus callosum and recovered smoothly without major neurologic deficits. However, none of these patients had morbidity or mortality associated with the internal jugular vein puncture. Discussion Transvenous endovascular intervention is a well-established technique for many intracranial vascular diseases. Through the venous route, the interventional radiologist can perform embolization of CCFs and DAVFs. 2,5-7 Thrombolysis, embolectomy, and stent placement for dural sinus thrombosis can also be achieved transvenously. 3,8,9 In addition, venous sampling is also performed transvenously for diagnosis of pituitary gland disorders. 10,11 Although femoral vein puncture is the most commonly used venous access, jugular vein puncture and direct puncture of engorged veins in the head and neck are possible alternatives. 5,7 Currently, the internal jugular vein puncture technique is widely used for placement of central venous catheters, tunneled central catheters for hemodialysis, and inferior vena cava filters. 15,16 Ablation of atrial fibrillation, 17 transjugular intrahepatic portosystemic shunt, 18 and transvenous hepatic biopsy 19,20 are also reported to be safe via transjugular access. The interventionist can benefit from the internal jugular puncture in many aspects, compared with using the common femoral vein puncture. First, the internal jugular vein is much closer to the intravascular vascular lesion. With the shorter route of catheterization, a shorter guiding catheter can be used. As a result, the available working length of the microcatheter and microwire would be much longer for selective catheterization during the procedure. In addition, with the shorter catheter retained in the patient s body, the risk of iatrogenic thromboembolism would be less during the procedure. Second, several angulations of the guiding catheter are often encountered at the junctions between the SVC and brachiocephalic veins, between the brachiocephalic veins and internal jugular veins, and at the jugular bulbs in a transfemoral route technique. With the transjugular route, the 2 marked angulations at the junctions between the SVC and brachiocephalic veins and between the brachiocephalic veins and internal jugular vein are bypassed. Therefore, less tortuosity of the catheter and, correspondingly, less difficulty of catheterization and embolization would be encountered during the procedure. E10 Yeh AJNR 33 Jan
5 Fig 4. A 54-year-old woman with superior sagittal sinus thrombosis. A and B, Left internal carotid artery angiogram, venous phase, in anteroposterior (A) and lateral (B) projections shows occlusion of superior sagittal sinus, right transverse sinus, right sigmoid sinus, and left transverse sinus (not shown). C, After a 6F guiding catheter is placed into the superior sagittal sinus, angioplasty with a balloon catheter is performed. D, After subsequent 48-hour chemical thrombolysis with urokinase, recanalization of the superior sagittal sinus and left transvenous sinus is confirmed in MR venography 3 days and 6 months later (not shown). In the case presented in Figs 2 and 3, the microcatheter was successfully navigated through the facial vein, angular vein, and superior ophthalmic vein into the cavernous sinus and inferior petrosal sinus. With the benefit of a transjugular vein approach, the tortuosity of the guiding catheter and microcatheter was markedly decreased. Correspondingly, the resistance during advancing the catheter and deploying microcoils was also reduced. Therefore, the procedure can be performed more smoothly with less operation time. Furthermore, the 1-way valves at the junction of internal jugular vein and brachiocephalic vein would impede retrograde catheterization when performing a transfemoral technique, but they are easily bypassed by transjugular routes. Sometimes, endovascular treatments are performed via sonographically guided puncture of pathologically dilated venous sacs or the drainage vein near the vascular lesion. Theoretically, the route of catheterization would be shortest by these vascular accesses. However, due to the relatively smaller caliber and tortuous nature of these venous routes, it can be difficult to place a large-sized vascular sheath, such as the 6F sheath we used in the transjugular vein technique. With the small-sized vascular sheath, the available guiding catheter, guidewire, microcatheter, microwire, and special technique of catheterization (eg, the double-catheter technique and balloon-assisted embolization) are all limited during the procedure. As in the case presented in Fig 4, recannulation of the occluded superior sagittal sinus was performed through left internal jugular vein access. With the benefit of a large-sized (6F) internal jugular vein sheath, a balloon catheter was deployed and inflated without difficulty. In addition, no limitation of trunk or limb movement was required during the subsequent 48-hour chemical thrombolysis. Finally, patients with obesity are not uncommon in the daily practice of interventional neuroradiologists. The marked thick layer of subcutaneous fatty tissue and the deep skin folds around the groin area can make femoral vein puncture time-consuming and sometimes impossible. In these patients, internal jugular vein puncture is another alternative technique. There are also some drawbacks to the internal jugular vein puncture for intracranial interventions. First, internal jugular vein punctures are usually performed antegradely in other procedures (eg, in transjugular hepatic interventions). However, they are uniquely performed retrogradely during intracranial interventions. When one performs the retrograde jugular vein puncture, the conventional landmark guidance technique used in antegrade puncture is not useful. Moreover, retrogradely navigating a guidewire and catheter within a transvenous route would be markedly difficult due to the reversed direction of blood flow and the complex network of venous return in the head and neck regions. Therefore, we routinely use the technique of indirectly obtaining a venous roadmap with a transarterial catheter in the feeding artery to overcome these difficulties. The congenital variation of the head and neck venous net- AJNR Am J Neuroradiol 33:E7 E12 Jan E11
6 work also increases the difficulty of the transjugular technique. For example, the confluence of the facial vein or occipital vein with the internal jugular vein may be located in the middle or lower portion of the neck. They will be bypassed after placement of a vascular sheath with the puncture site in the middle neck according to the conventional landmark guidance technique. Therefore, it is wise to make the site of the internal jugular vein puncture as caudally as possible. As in other transjugular interventions, we are always concerned about the potential inadvertent injury of the carotid artery and venous bleeding due to repeat puncture or penetration of the posterior wall of the jugular vein in patients with coagulopathy. 21 Under ultrasonographic guidance, internal jugular vein puncture can be performed safely and accurately at the optimal venous access site. Therefore, the risk of carotid artery injury, uncontrollable neck bleeding, and neck hematoma are markedly decreased. In this study, transjugular accesses were successfully established in all 44 procedures with sonographic guidance without inadvertent carotid artery injury. No puncture-related morbidity or mortality occurred during any of these procedures. Conclusions Sonographic guidance of internal jugular vein puncture is a useful procedure in establishing a transvenous route for an intracranial endovascular intervention. According to our 10- year experience of intracranial intervention, transvenous accesses were successfully established with sonographic guidance in 44 procedures. No morbidity or mortality associated with the internal jugular vein puncture occurred. Therefore, we believe this technique be a safe and efficacious alternative vascular access for intracranial endovascular interventions. References 1. Kiyosue H, Hori Y, Okahara M, et al. Treatment of intracranial dural arteriovenous fistulas: current strategies based on location and hemodynamics, and alternative techniques of transcatheter embolization. Radiographics 2004;24: Klisch J, Huppertz HJ, Spetzger U, et al. Transvenous treatment of carotid cavernous and dural arteriovenous fistulae: results for 31 patients and review of the literature. Neurosurgery 2003;53:836 56, discussion Rahman M, Velat GJ, Hoh BL, et al. Direct thrombolysis for cerebral venous sinus thrombosis. Neurosurg Focus 2009;27:E7 4. Yoshida K, Melake M, Oishi H, et al. Transvenous embolization of dural carotid cavernous fistulas: a series of 44 consecutive patients. AJNR Am J Neuroradiol 2010;31: Ng PP, Higashida RT, Cullen S, et al. Endovascular strategies for carotid cavernous and intracerebral dural arteriovenous fistulas. Neurosurg Focus 2003;15:ECP1 6. Biondi A, Milea D, Cognard C, et al. Cavernous sinus dural fistulae treated by transvenous approach through the facial vein: report of seven cases and review of the literature. AJNR Am J Neuroradiol 2003;24: Berkmen T, Troffkin NA, Wakhloo AK. Transvenous sonographically guided percutaneous access for treatment of an indirect carotid cavernous fistula. AJNR Am J Neuroradiol 2003;24: Masuhr F, Einhaupl K. Treatment of cerebral venous and sinus thrombosis. Front Neurol Neurosci 2008;23: Canhao P, Falcao F, Ferro JM. Thrombolytics for cerebral sinus thrombosis: a systematic review. Cerebrovasc Dis 2003;15: Boscaro M, Arnaldi G. Approach to the patient with possible Cushing s syndrome. J Clin Endocrinol Metab 2009;94: Tomycz ND, Horowitz MB. Inferior petrosal sinus sampling in the diagnosis of sellar neuropathology. Neurosurg Clin N Am 2009;20: Koroglu M, Demir M, Koroglu BK, et al. Percutaneous placement of central venous catheters: comparing the anatomical landmark method with the radiologically guided technique for central venous catheterization through the internal jugular vein in emergent hemodialysis patients. Acta Radiol 2006;47: Docktor BL, Sadler DJ, Gray RR, et al. Radiologic placement of tunneled central catheters: rates of success and of immediate complications in a large series. AJR Am J Roentgenol 1999;173: Pittiruti M, Malerba M, Carriero C, et al. Which is the easiest and safest technique for central venous access? A retrospective survey of more than 5400 cases. J Vasc Access 2000;1: Aziz F, Spate K, Wong J, et al. Changing patterns in the use of inferior vena cava filters: review of a single center experience. J Am Coll Surg 2007;205: Kinney TB. Update on inferior vena cava filters. J Vasc Interv Radiol 2003;14: Lim HE, Pak HN, Tse HF, et al. Catheter ablation of atrial fibrillation via superior approach in patients with interruption of the inferior vena cava. Heart Rhythm 2009;6: Epub 2008 Nov Lorenz JM. Placement of transjugular intrahepatic portosystemic shunts in children. Tech Vasc Interv Radiol 2008;11: Soyer P, Fargeaudou Y, Boudiaf M, et al. Transjugular liver biopsy using ultrasonographic guidance for jugular vein puncture and an automated device for hepatic tissue sampling: a retrospective analysis of 200 consecutive cases. Abdom Imaging 2008;33: Smith TP, Presson TL, Heneghan MA, et al. Transjugular biopsy of the liver in pediatric and adult patients using an 18-gauge automated core biopsy needle: a retrospective review of 410 consecutive procedures. AJR Am J Roentgenol 2003;180: Blaivas M, Adhikari S. An unseen danger: frequency of posterior vessel wall penetration by needles during attempts to place internal jugular vein central catheters using ultrasound guidance. Crit Care Med 2009;37: , quiz 59 E12 Yeh AJNR 33 Jan
Endovascular Treatment of Cavernous Sinus Dural Arteriovenous Fistulas by Direct Puncture of Facial Vein
 J Radiol Sci 2011; 36: 129-134 Endovascular Treatment of Cavernous Sinus Dural Arteriovenous Fistulas by Direct Puncture of Facial Vein Shih-Wei Hsu 1 Yeh-Lin Kuo 1 Min-Hsiung Cheng 2 Department of Diagnostic
J Radiol Sci 2011; 36: 129-134 Endovascular Treatment of Cavernous Sinus Dural Arteriovenous Fistulas by Direct Puncture of Facial Vein Shih-Wei Hsu 1 Yeh-Lin Kuo 1 Min-Hsiung Cheng 2 Department of Diagnostic
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils
 High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
Arterial Map of the Thorax, Abdomen and Pelvis 2017 Edition
 Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
Neuro-Vascular Intervention AAPC Regional Conference Springfield, MA
 Neuro-Vascular Intervention AAPC Regional Conference Springfield, MA October 8, 2010 1 Presented by: David Zielske, MD,CIRCC, CPC H, CCC, CCS, RCC General Recommendations for Physician Dictations State
Neuro-Vascular Intervention AAPC Regional Conference Springfield, MA October 8, 2010 1 Presented by: David Zielske, MD,CIRCC, CPC H, CCC, CCS, RCC General Recommendations for Physician Dictations State
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Intracranial dural arteriovenous fistulas (DAVFs) with retrograde
 ORIGINAL RESEARCH W.J. van Rooij M. Sluzewski G.N. Beute Dural Arteriovenous Fistulas with Cortical Venous Drainage: Incidence, Clinical Presentation, and Treatment BACKGROUND AND PURPOSE: Our purpose
ORIGINAL RESEARCH W.J. van Rooij M. Sluzewski G.N. Beute Dural Arteriovenous Fistulas with Cortical Venous Drainage: Incidence, Clinical Presentation, and Treatment BACKGROUND AND PURPOSE: Our purpose
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Endovascular treatment with transvenous approach for embolization of carotid cavernous fistula
 169 Case Report Endovascular treatment with transvenous approach for embolization of carotid cavernous fistula Benny Young, Agusmanan Bojeng Department of Radiology, University Malaysia Sarawak, Faculty
169 Case Report Endovascular treatment with transvenous approach for embolization of carotid cavernous fistula Benny Young, Agusmanan Bojeng Department of Radiology, University Malaysia Sarawak, Faculty
TEACHING CASE # 5. Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy
 TEACHING CASE # 5 Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy CASE PRESENTATION 22M with right transverse and sigmoid venous sinuses occlusion s/p transvenous
TEACHING CASE # 5 Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy CASE PRESENTATION 22M with right transverse and sigmoid venous sinuses occlusion s/p transvenous
CY2015 Hospital Outpatient: Endovascular Procedure APCs and Complexity Adjustments
 CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
2013 Coding Changes. Diagnostic Radiology. Nuclear Medicine
 2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
2013 Coding Changes The principal coding changes affecting Radiologists in 2013 occur in the Interventional Radiology Section of the AMA/CPT Manual. As in the past, we continue to see the Relative Update
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal
 AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
Irretrievable unraveled coil remaining in the vascular lumen between the cerebral aneurysm and puncture site
 Technical Note JNET 3:42-46, 2009 Irretrievable unraveled coil remaining in the vascular lumen between the cerebral aneurysm and puncture site Kouhei NII 1) Masanari ONIZUK 1) Yoshirou KNEKO 2) Hiroshi
Technical Note JNET 3:42-46, 2009 Irretrievable unraveled coil remaining in the vascular lumen between the cerebral aneurysm and puncture site Kouhei NII 1) Masanari ONIZUK 1) Yoshirou KNEKO 2) Hiroshi
The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience
 230 Chiriac et al - Superior ophthalmic vein approach The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience A. Chiriac, N. Dobrin 1, Georgiana Ion
230 Chiriac et al - Superior ophthalmic vein approach The superior ophthalmic vein approach for the treatment of carotid-cavernous fistulas: our first experience A. Chiriac, N. Dobrin 1, Georgiana Ion
Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving the Laterocavernous Sinus
 Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique
 Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Untangling Cerebral Dural Arteriovenous Fistulas
 Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Yamaguchi, Susumu; Morikawa, Minoru
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Quadruple coaxial catheter system o arteriovenous fistula Hayashi, Kentaro; Horie, Nobutaka; Yamaguchi, Susumu; Morikawa, Minoru Neurological
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Quadruple coaxial catheter system o arteriovenous fistula Hayashi, Kentaro; Horie, Nobutaka; Yamaguchi, Susumu; Morikawa, Minoru Neurological
Complete Guide for Interventional Radiology
 2015 Complete Guide for Interventional Radiology Contents Introduction... 1 CPT Codes and Descriptions...1 Procedure Codes...2 Chapter 1: The Basics... 5 APC Basics Why Is This Important?...5 CCI Edits
2015 Complete Guide for Interventional Radiology Contents Introduction... 1 CPT Codes and Descriptions...1 Procedure Codes...2 Chapter 1: The Basics... 5 APC Basics Why Is This Important?...5 CCI Edits
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 29, 2018 Mesenteric Arteriogram & Thrombectomy/Thrombolysis
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 29, 2018 Mesenteric Arteriogram & Thrombectomy/Thrombolysis
Complex dural arteriovenous fistulas. Results of combined endovascular and neurosurgical treatment in 16 patients
 J Neurosurg 71:352-358,1989 Complex dural arteriovenous fistulas Results of combined endovascular and neurosurgical treatment in 16 patients STANLEY L. BARNWELL, M.D., PH.D., VAN V. HALBACH, M.D., RANDALL
J Neurosurg 71:352-358,1989 Complex dural arteriovenous fistulas Results of combined endovascular and neurosurgical treatment in 16 patients STANLEY L. BARNWELL, M.D., PH.D., VAN V. HALBACH, M.D., RANDALL
CASE PRESENTATION. Key Words: cerebral venous thrombosis, internal jugular vein stenosis, thrombolysis, stenting (Kaohsiung J Med Sci 2005;21:527 31)
 Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Advanced Neurointerventional Radiology Coding with Case Studies
 Advanced Neurointerventional Radiology Coding with Case Studies Presented by Jeff Majchrzak, BA, RCC, CIRCC Kathy Pride, RHIT, CPC, CCS-P, AHIMA Approved ICD-10-CM/PCS Trainer.. July 16, 2015 1 Disclaimer
Advanced Neurointerventional Radiology Coding with Case Studies Presented by Jeff Majchrzak, BA, RCC, CIRCC Kathy Pride, RHIT, CPC, CCS-P, AHIMA Approved ICD-10-CM/PCS Trainer.. July 16, 2015 1 Disclaimer
Dural arteriovenous fistulas (DAVFs) are acquired abnormal
 ORIGINAL RESEARCH R.G. Nogueira G. Dabus J.D. Rabinov C.J. Eskey C.S. Ogilvy J.A. Hirsch J.C. Pryor Preliminary Experience with Onyx Embolization for the Treatment of Intracranial Dural Arteriovenous Fistulas
ORIGINAL RESEARCH R.G. Nogueira G. Dabus J.D. Rabinov C.J. Eskey C.S. Ogilvy J.A. Hirsch J.C. Pryor Preliminary Experience with Onyx Embolization for the Treatment of Intracranial Dural Arteriovenous Fistulas
Dural arteriovenous fistulas (DAVFs) are relatively
 case report J Neurosurg 122:1208 1213, 2015 Torcular dural arteriovenous fistula treated via stent placement and angioplasty in the affected straight and transverse sinuses: case report Shigeki Takada,
case report J Neurosurg 122:1208 1213, 2015 Torcular dural arteriovenous fistula treated via stent placement and angioplasty in the affected straight and transverse sinuses: case report Shigeki Takada,
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
A Shunt of the Diploic Vein of the Orbital Roof Accompanying a Cavernous Sinus Dural Arteriovenous Fistula: A Case Report
 Journal of Neuroendovascular Therapy 2018; 12: 38 42 Online September 11, 2017 DOI: 10.5797/jnet.cr.2017-0056 A Shunt of the Diploic Vein of the Orbital Roof Accompanying a Cavernous Sinus Dural Arteriovenous
Journal of Neuroendovascular Therapy 2018; 12: 38 42 Online September 11, 2017 DOI: 10.5797/jnet.cr.2017-0056 A Shunt of the Diploic Vein of the Orbital Roof Accompanying a Cavernous Sinus Dural Arteriovenous
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Sinus Venous Thrombosis
 Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Mechanical Thrombectomy of Large Vessel Occlusions Using Stent Retriever Devices
 Mechanical Thrombectomy of Large Vessel Occlusions Using Stent Retriever Devices Joey English MD, PhD Medical Director, Neurointerventional Services California Pacific Medical Center Hospitals, San Francisco,
Mechanical Thrombectomy of Large Vessel Occlusions Using Stent Retriever Devices Joey English MD, PhD Medical Director, Neurointerventional Services California Pacific Medical Center Hospitals, San Francisco,
Interlocking Detachable Coil Occlusion in the Endovascular Treatment of Intracranial Aneurysms: Preliminary Results
 Interlocking Detachable Coil Occlusion in the Endovascular Treatment of Intracranial Aneurysms: Preliminary Results H. Saruhan Cekirge, Isil Saatci, Murat M. Firat, Ferhun Balkanci, and Aytekin Besim PURPOSE:
Interlocking Detachable Coil Occlusion in the Endovascular Treatment of Intracranial Aneurysms: Preliminary Results H. Saruhan Cekirge, Isil Saatci, Murat M. Firat, Ferhun Balkanci, and Aytekin Besim PURPOSE:
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
An Onyx tunnel: reconstructive transvenous balloon-assisted Onyx embolization for dural arteriovenous fistula of the transverse-sigmoid sinus
 TECHNICAL NOTE J Neurosurg 129:922 927, 2018 An Onyx tunnel: reconstructive transvenous balloon-assisted Onyx embolization for dural arteriovenous fistula of the transverse-sigmoid sinus *Mena G. Kerolus,
TECHNICAL NOTE J Neurosurg 129:922 927, 2018 An Onyx tunnel: reconstructive transvenous balloon-assisted Onyx embolization for dural arteriovenous fistula of the transverse-sigmoid sinus *Mena G. Kerolus,
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Ruptured intracranial vertebral confluence
 Endovascular Transluminal Stent-Assisted Coil Embolization of a Vertebral Confluence Aneurysm: Technique Report Michael B. Horowitz, M.D., Elad I. Levy, M.D., Christopher J. Koebbe, M.D., and Charles C.
Endovascular Transluminal Stent-Assisted Coil Embolization of a Vertebral Confluence Aneurysm: Technique Report Michael B. Horowitz, M.D., Elad I. Levy, M.D., Christopher J. Koebbe, M.D., and Charles C.
Thrombectomy, open, arteriovenous fistula without revision, autogenous or nonautogenous dialysis graft (separate procedure)
 Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Hospital Outpatient 2019 Edition All Reimbursement Amounts are Listed at ational Unadjusted Medicare Rates and Do ot Include the 2%
Dialysis Vascular Access Coverage, Coding and Reimbursement Overview Hospital Outpatient 2019 Edition All Reimbursement Amounts are Listed at ational Unadjusted Medicare Rates and Do ot Include the 2%
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Borden type3 superior sagittal sinus dural arteriovenous fistula, angiographic features and endovascular treatment.
 Borden type3 superior sagittal sinus dural arteriovenous fistula, angiographic features and endovascular treatment. Poster No.: C-1939 Congress: ECR 2013 Type: Scientific Exhibit Authors: T. Dotsu 1, H.
Borden type3 superior sagittal sinus dural arteriovenous fistula, angiographic features and endovascular treatment. Poster No.: C-1939 Congress: ECR 2013 Type: Scientific Exhibit Authors: T. Dotsu 1, H.
Straub Endovascular System &
 Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Basics of Interventional Radiology Coding 2018
 Basics of Interventional Radiology Coding 2018 Prepared and Published By: MedLearn Publishing A Division of MedLearn Media, Inc. 445 Minnesota Street, Suite 514 St. Paul, MN 55101 1-800-252-1578 medlearnmedia.com
Basics of Interventional Radiology Coding 2018 Prepared and Published By: MedLearn Publishing A Division of MedLearn Media, Inc. 445 Minnesota Street, Suite 514 St. Paul, MN 55101 1-800-252-1578 medlearnmedia.com
Cordis EXOSEAL Vascular Closure Device
 to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device A Guide to Good Access and Closure Transfemoral Access Closure Pocket Guide LinkedIn page Follow us on CORDIS EMEA
to receive our latest news and key activities. Cordis EXOSEAL Vascular Closure Device A Guide to Good Access and Closure Transfemoral Access Closure Pocket Guide LinkedIn page Follow us on CORDIS EMEA
Basics of Interventional Radiology Coding 2017
 Basics of Interventional Radiology Coding 2017 Prepared and Published By: MedLearn Publishing A Division of Panacea Healthcare Solutions, Inc. 287 East Sixth Street, Suite 400 St. Paul, MN 55101 1-800-252-1578
Basics of Interventional Radiology Coding 2017 Prepared and Published By: MedLearn Publishing A Division of Panacea Healthcare Solutions, Inc. 287 East Sixth Street, Suite 400 St. Paul, MN 55101 1-800-252-1578
As with any intervention, selection of an appropriate
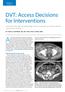 DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Rheolytic Thrombectomy of the Occluded Internal Carotid Artery in the Setting of Acute Ischemic Stroke
 AJNR Am J Neuroradiol 22:526 530, March 2001 Rheolytic Thrombectomy of the Occluded Internal Carotid Artery in the Setting of Acute Ischemic Stroke Richard J. Bellon, Christopher M. Putman, Ronald F. Budzik,
AJNR Am J Neuroradiol 22:526 530, March 2001 Rheolytic Thrombectomy of the Occluded Internal Carotid Artery in the Setting of Acute Ischemic Stroke Richard J. Bellon, Christopher M. Putman, Ronald F. Budzik,
Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report
 122 Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report Wen-Sou Lin 1, Hung-Wen Kao 2, Chun-Jen Hsueh 2, Chun-An Cheng 3 Abstract- Purpose: Cerebral
122 Intrasinus Thrombolysis by Mechanical and Urokinase for Severe Cerebral Venous Sinus Thrombosis : A Case Report Wen-Sou Lin 1, Hung-Wen Kao 2, Chun-Jen Hsueh 2, Chun-An Cheng 3 Abstract- Purpose: Cerebral
Vascular Access: Management of Complications. Chris Burrell, South West Cardiothoracic Centre, Plymouth
 Vascular Access: Management of Complications Chris Burrell, South West Cardiothoracic Centre, Plymouth Alternative Vascular Access Sites Femoral Axillary Brachial Radial Ulnar Femoral v Radial Vascular
Vascular Access: Management of Complications Chris Burrell, South West Cardiothoracic Centre, Plymouth Alternative Vascular Access Sites Femoral Axillary Brachial Radial Ulnar Femoral v Radial Vascular
Transfemoral Venous Embolization of Vein of Galen Malformations
 643 Transfemoral Venous Embolization of Vein of Galen Malformations Christopher F. Dowd 1 Van V. Halbach 1 2 Stanley L. Barnwell 1 2 Randall T. Higashida 1 2 MichaelS. B. Edwards 2 3 Grant B. Hieshima
643 Transfemoral Venous Embolization of Vein of Galen Malformations Christopher F. Dowd 1 Van V. Halbach 1 2 Stanley L. Barnwell 1 2 Randall T. Higashida 1 2 MichaelS. B. Edwards 2 3 Grant B. Hieshima
Permanent central venous catheters: complications and strategies using different accesses.
 Permanent central venous catheters: complications and strategies using different accesses. Poster No.: C-1038 Congress: ECR 2015 Type: Educational Exhibit Authors: M. D. Ferrer-Puchol, R. Ramiro, E. Garcia-Oliver,
Permanent central venous catheters: complications and strategies using different accesses. Poster No.: C-1038 Congress: ECR 2015 Type: Educational Exhibit Authors: M. D. Ferrer-Puchol, R. Ramiro, E. Garcia-Oliver,
Differences between CS-DAVF and TCCF to reveal and redefine CS-DAVF
 Pan et al. Chinese Neurosurgical Journal (2018) 4:26 https://doi.org/10.1186/s41016-018-0121-z CHINESE MEDICAL ASSOCIATION COMMENTARY Differences between CS-DAVF and TCCF to reveal and redefine CS-DAVF
Pan et al. Chinese Neurosurgical Journal (2018) 4:26 https://doi.org/10.1186/s41016-018-0121-z CHINESE MEDICAL ASSOCIATION COMMENTARY Differences between CS-DAVF and TCCF to reveal and redefine CS-DAVF
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
UNMH Radiology Clinical Privileges. Name: Effective Dates: From To
 All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective April 28, 2017: Initial Privileges (initial appointment) Renewal of Privileges (reappointment)
All new applicants must meet the following requirements as approved by the UNMH Board of Trustees, effective April 28, 2017: Initial Privileges (initial appointment) Renewal of Privileges (reappointment)
Fluoroscopy-guided Combined (Surgical/Endovascular) Treatment of Dural Arteriovenous Fistula
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.2.106 Case Report Fluoroscopy-guided Combined (Surgical/Endovascular) Treatment
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.2.106 Case Report Fluoroscopy-guided Combined (Surgical/Endovascular) Treatment
The current optimized approach for patients with a ruptured
 ORIGINAL RESEARCH I. Oran C. Cinar Continuous Intra-Arterial Infusion of Nimodipine During Embolization of Cerebral Aneurysms Associated With Vasospasm BACKGROUND AND PURPOSE: Despite rigorous efforts,
ORIGINAL RESEARCH I. Oran C. Cinar Continuous Intra-Arterial Infusion of Nimodipine During Embolization of Cerebral Aneurysms Associated With Vasospasm BACKGROUND AND PURPOSE: Despite rigorous efforts,
A.J. Hauer Intracranial dural arteriovenous fistulae
 A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS
 Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
Arterial Access for Diagnosis and Intervention T-Woei Tan, MD, FACS Assistant Professor of Surgery Vascular Endovascular Surgery Louisiana State University Health - Shreveport Disclosures None Objective
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
BACKGROUND AND PURPOSE:
 AJNR Am J Neuroradiol 26:1715 1722, August 2005 Dural Sinus Compartment in Dural Arteriovenous Shunts: A New Angioarchitectural Feature Allowing Superselective Transvenous Dural Sinus Occlusion Treatment
AJNR Am J Neuroradiol 26:1715 1722, August 2005 Dural Sinus Compartment in Dural Arteriovenous Shunts: A New Angioarchitectural Feature Allowing Superselective Transvenous Dural Sinus Occlusion Treatment
9/7/2018. Disclosures. CV and Limb Events in PAD. Challenges to Revascularization. Challenges. Answering the Challenge
 Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Disclosures State-of-the-Art Endovascular Lower Extremity Revascularization Promotional Speaker Jansen Pharmaceutical Promotional Speaker Amgen Pharmaceutical C. Michael Brown, MD, FACC al Cardiology Associate
Endovascular treatment for pseudoocclusion of the internal carotid artery
 Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Endovascular treatment for pseudoocclusion of the internal carotid artery Daqiao Guo, Xiao Tang, Weiguo Fu Institute of Vascular Surgery, Fudan University, Department of Vascular Surgery, Zhongshan Hospital
Diverter Stent Insertion
 Open Access Journal of Neuroscience and Neurological Disorders Case Report Direct Carotid Puncture for Flow ISSN 2639-3220 Diverter Stent Insertion Bhogal P 1 *, Phillips TJ 2 and Makalanda HLD 1 1 Department
Open Access Journal of Neuroscience and Neurological Disorders Case Report Direct Carotid Puncture for Flow ISSN 2639-3220 Diverter Stent Insertion Bhogal P 1 *, Phillips TJ 2 and Makalanda HLD 1 1 Department
Recanalization Techniques: Sharp Needle Recanalization. Recanalization Techniques: Sharp Needle Recanalization
 Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
BILLING BULLETIN. Re: Interventional Cardiology. Bulletin #: 1. Date Issued: November 10, Background
 BILLING BULLETIN Re: Interventional Cardiology Bulletin #: 1 Date Issued: November 10, 2016 Background This Billing Bulletin provides billing guidance when submitting claims to Manitoba Health, Seniors
BILLING BULLETIN Re: Interventional Cardiology Bulletin #: 1 Date Issued: November 10, 2016 Background This Billing Bulletin provides billing guidance when submitting claims to Manitoba Health, Seniors
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1
 Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Endovascular Treatment for Spontaneous Vertebral Arteriovenous Fistula in Neurofibromatosis Type 1: A Case Report
 Endovascular Treatment for Spontaneous Vertebral Arteriovenous Fistula in Neurofibromatosis Type 1: A Case Report Case Report Yon Kwon Ihn, MD 1, Won Sang Jung, MD 1, Bum-Soo Kim, MD 1 We report the case
Endovascular Treatment for Spontaneous Vertebral Arteriovenous Fistula in Neurofibromatosis Type 1: A Case Report Case Report Yon Kwon Ihn, MD 1, Won Sang Jung, MD 1, Bum-Soo Kim, MD 1 We report the case
Transarterial Occlusion of Solitary Intracerebral Arteriovenous Fistulas
 747 Transarterial Occlusion of Solitary Intracerebral Arteriovenous Fistulas Van V. Halbach 1 2 Randall T. Higashida 1 2 Grant B. Hieshima 1 2 Carl W. Hardin 1 Christopher F. Dowd 1 Stanley L. Barnwell
747 Transarterial Occlusion of Solitary Intracerebral Arteriovenous Fistulas Van V. Halbach 1 2 Randall T. Higashida 1 2 Grant B. Hieshima 1 2 Carl W. Hardin 1 Christopher F. Dowd 1 Stanley L. Barnwell
ADDITIONS. The following codes have been added.
 ADDITIONS The following codes have been added. 99446 Interprofessional telephone/internet assessment and management service provided by treating/requesting physician or other qualified health care professional;
ADDITIONS The following codes have been added. 99446 Interprofessional telephone/internet assessment and management service provided by treating/requesting physician or other qualified health care professional;
Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
 CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
CLINICAL IMAGES Ochsner Journal 17:311 316, 2017 Ó Academic Division of Ochsner Clinic Foundation Transjugular Intrahepatic Portosystemic Shunt Reduction for Management of Recurrent Hepatic Encephalopathy
Case #1. Case #1- Possible codes. Unraveling the -59 modifier. Principles of Interventional. CASE 1: Simple angioplasty
 Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Naviga&ng the Road Map of Vascular Families
 Naviga&ng the Road Map of Vascular Families AAPC Regional Conference Chicago, IL October 26, 2012 Presented by: David Dunn, MD, FACS CIRCC, CCVTC, CPC- H, CCC, CCS, RCC Na&onal Coding Standards Sources
Naviga&ng the Road Map of Vascular Families AAPC Regional Conference Chicago, IL October 26, 2012 Presented by: David Dunn, MD, FACS CIRCC, CCVTC, CPC- H, CCC, CCS, RCC Na&onal Coding Standards Sources
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges VASCULAR AND INTERVENTIONAL RADIOLOGY
 MIDLAND MEMORIAL HOSPITAL Delineation of Privileges VASCULAR AND INTERVENTIONAL RADIOLOGY Physician Name: Vascular and Interventional Radiology Core Privileges Qualifications Your home for healthcare Minimum
MIDLAND MEMORIAL HOSPITAL Delineation of Privileges VASCULAR AND INTERVENTIONAL RADIOLOGY Physician Name: Vascular and Interventional Radiology Core Privileges Qualifications Your home for healthcare Minimum
IMAGES. in PAEDIATRIC CARDIOLOGY
 IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
IMAGES in PAEDIATRIC CARDIOLOGY Images Paediatr Cardiol. 2005 Jan-Mar; 7(1): 12 17. PMCID: PMC3232568 Stent implantation for coarctation facilitated by the anterograde trans-septal approach N Sreeram and
DAVFs are defined as abnormal communications between
 ORIGINAL RESEARCH E. Lekkhong S. Pongpech K. ter Brugge P. Jiarakongmun R. Willinsky S. Geibprasert T. Krings Transvenous Embolization of Intracranial Dural Arteriovenous Shunts through Occluded Venous
ORIGINAL RESEARCH E. Lekkhong S. Pongpech K. ter Brugge P. Jiarakongmun R. Willinsky S. Geibprasert T. Krings Transvenous Embolization of Intracranial Dural Arteriovenous Shunts through Occluded Venous
Vascular injury from an arterial closure device
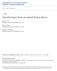 Washington University School of Medicine Digital Commons@Becker Open Access Publications 1-1-2007 Vascular injury from an arterial closure device Jeffrey P. C. Lin Brian G. Rubin William D. Middleton Follow
Washington University School of Medicine Digital Commons@Becker Open Access Publications 1-1-2007 Vascular injury from an arterial closure device Jeffrey P. C. Lin Brian G. Rubin William D. Middleton Follow
SDAVFs are rare acquired vascular lesions predominantly
 CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
Case Report. Case Report
 AJNR Am J Neuroradiol 25:333 337, February 2004 Case Report Stent-Coil Treatment of a Distal Internal Carotid Artery Dissecting Pseudoaneurysm on a Redundant Loop by Use of a Flexible, Dedicated Nitinol
AJNR Am J Neuroradiol 25:333 337, February 2004 Case Report Stent-Coil Treatment of a Distal Internal Carotid Artery Dissecting Pseudoaneurysm on a Redundant Loop by Use of a Flexible, Dedicated Nitinol
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
Obliterative hepatocavopathy ultrasound and cavography findings
 doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
doi:10.2478/v10019-008-0020-6 case report Obliterative hepatocavopathy ultrasound and cavography findings Ramazan Kutlu Department of Radiology, Inonu University School of Medicine, Malatya, Turkey ackgound.
Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting
 How To Treat Resistant Central Venous Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting Dafsah A Juzar T. Santoso National Heart Center, Harapan Kita, & Medistra Hospital
How To Treat Resistant Central Venous Occlusion: A New Technique Antegrade wiring i with retrograde ballooning and stenting Dafsah A Juzar T. Santoso National Heart Center, Harapan Kita, & Medistra Hospital
INTRAHEPATIC PSS: AN INTERVENTIONALIST S PERSPECTIVE
 INTRAHEPATIC PSS: AN INTERVENTIONALIST S PERSPECTIVE Matthew W. Beal, DVM, DACVECC College of Veterinary Medicine, Michigan State University, East Lansing, MI Key Points: Percutaneous transjugular coil
INTRAHEPATIC PSS: AN INTERVENTIONALIST S PERSPECTIVE Matthew W. Beal, DVM, DACVECC College of Veterinary Medicine, Michigan State University, East Lansing, MI Key Points: Percutaneous transjugular coil
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 22, 2018 Paracentesis & Transjugular Liver Biopsy
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 22, 2018 Paracentesis & Transjugular Liver Biopsy
Combining endovascular and neurosurgical treatments of high-risk dural arteriovenous fistulas in the lateral sinus and the confluence of the sinuses
 J Neurosurg 90:289 299, 1999 Combining endovascular and neurosurgical treatments of high-risk dural arteriovenous fistulas in the lateral sinus and the confluence of the sinuses KATSUYA GOTO, M.D., PH.D.,
J Neurosurg 90:289 299, 1999 Combining endovascular and neurosurgical treatments of high-risk dural arteriovenous fistulas in the lateral sinus and the confluence of the sinuses KATSUYA GOTO, M.D., PH.D.,
Balloon-assisted guide catheter positioning to overcome extreme cervical carotid tortuosity: technique and case experience
 Department of Neurosurgery, Stony Brook University Medical Center, Cerebrovascular Center, Stony Brook, New York, USA Correspondence to Dr D Fiorella, Department of Neurological Surgery, Stony Brook University
Department of Neurosurgery, Stony Brook University Medical Center, Cerebrovascular Center, Stony Brook, New York, USA Correspondence to Dr D Fiorella, Department of Neurological Surgery, Stony Brook University
2019 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule
 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
 Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Management of Endoleaks. Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09
 Management of Endoleaks Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09 Endoleak Failure to totally exclude the abdominal aortic aneurysm (AAA) from continued perfusion and pressurization
Management of Endoleaks Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09 Endoleak Failure to totally exclude the abdominal aortic aneurysm (AAA) from continued perfusion and pressurization
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Rescue Balloon Reposition of the Protruding Coil Loops during Endovascular Treatment of An Anterior Communicating Artery Aneurysm: A Case Report
 Case Report Rescue Balloon Reposition of the Protruding Coil Loops during Endovascular Treatment of An Anterior Communicating Artery Aneurysm: A Case Report Hong Gee Roh, MD 1, Hyun-Seung Kang, MD 2, Pyoung
Case Report Rescue Balloon Reposition of the Protruding Coil Loops during Endovascular Treatment of An Anterior Communicating Artery Aneurysm: A Case Report Hong Gee Roh, MD 1, Hyun-Seung Kang, MD 2, Pyoung
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
2018 Endovascular Reimbursement Coding Fact Sheet
 The information contained in this document is provided for informational purposes only and represents no statement, promise, or guarantee by Cordis Corporation concerning levels of reimbursement, payment,
The information contained in this document is provided for informational purposes only and represents no statement, promise, or guarantee by Cordis Corporation concerning levels of reimbursement, payment,
