CASE REPORT Rhinology, 48, , Orbital and intracranial complications after acute rhinosinusitis*
|
|
|
- Tamsin Fletcher
- 6 years ago
- Views:
Transcription
1 CASE REPORT Rhinology, 48, , 2010 Orbital and intracranial complications after acute rhinosinusitis* Jan Kastner 1, Milos Taudy 1, Jiri Lisy 2, Paul Grabec 3, Jan Betka Department of Otorhinolaryngology and Head and Neck Surgery, University Hospital Motol, 1st Medical Faculty, Charles University, Prague, Czech Republic Department of Imaging Methods, University Hospital Motol, 2nd Medical Faculty, Charles University, Prague, Czech Republic Department of Otorhinolaryngology, General Hospital, 1st Medical Faculty, Charles University, Prague, Czech Republic SUMMARY Background/objectives: Nowadays, intracranial abscess is a rare complication of acute rhinosinusitis. The consequent orbital and intracranial complications of acute rhinosinusitis are rare but must be mutually excluded in complicated rhinosinusitis even when proper surgical and medical treatment tend to efficiently heal the orbital complication. Methods: We report a case of a patient who primarily revealed symptoms of orbitocellulitis as a complication of odontogenous rhinosinusitis. Proper diagnostic and therapeutical measures were undertaken to manage the disease immediately after stationary admission. We strongly rely on a literature review and recommendations on diagnosis and treatment of this possibly lethal complication in the discussion. Results: Two weeks after an inconspicuous healing period, hemiparesis due to formation of an intracranial abscess developed. An emergency situation revealed the unusual character of the clinical situation. In a literature review concerning intracranial complication after acute rhinosinusitis, we demonstrate the complexity of this complication. We indicate the predisposing factors, diagnostic measures and treatment strategy. Conclusion: The possible role of underlying mechanisms of intracranial abscess formation is discussed. The correct indication of imaging methods and accurate evaluation of diminutive symptoms are essential. We recommend performing a complementary CT of the brain or MRI, even when a previous CT scan of the orbit/paranasal sinuses reveals no cerebral pathology, to avoid or minimize the number of future patients with consecutive orbital and intracranial complications of acute rhinosinusitis. Key words: acute rhinosinusitis, intracranial complication, orbitocellulitis, endoscopic drainage, odontogenous INTRODUCTION Rhinosinusitis is clinically defined as inflammation of the nose and paranasal sinuses characterised by two or more symptoms, one of which should be either nasal obstruction or nasal discharge, along with facial pressure and/or loss of smell with positive endoscopic findings and/or CT pathology. In acute rhinosinusitis, the symptoms last less than 12 weeks; clinical ENT examination involves nasal endoscopy. CT scan is not recommended unless the course of disease is very severe, if the patient is immunocompromised, or signs of complications are present (1). Complications of rhinosinusitis might be divided into orbital, osseous and intracranial. Orbital involvement is divided according to the Chandler classification into: preseptal inflammatory oedema (periorbital cellulitis), postseptal orbital cellulitis, subperiosteal abscess, orbital abscess, and other complications (cavernous sinus thrombosis, etc.). Intracranial complications include either phlegmonous inflammation (meningitis, cerebritis) or abscess formation (epidural, subdural, intracerebral), and cavernous sinus thrombosis. Osseous complications are represented by frontal bone osteomyelitis. Their incidence has dramatically decreased when compared to the preantiobiotic era, but it is estimated that in patients affected by acute bacterial rhinosinusitis with intracranial spread, in spite of antibiotic therapy, there is still a high incidence of morbidity, and the mortality rate is between 5% and 10% (2). The spread of infection into the orbit and intracranially follows natural paths or predisposed routes, (i.e. pathogens can pass through the veins or alternatively, they may extend behind sinuses directly *Received for publication: February 15, 2009; accepted: December 8, 2009 DOI: /Rhin09.030
2 458 Kastner et al. through a dehiscence (e.g. in the lamina papyracea) or by eroding the sinus bones) (3,4). Diagnostic imaging should be done urgently, under hospitalization and it should rely on clinical and laboratory (white blood count) examinations, nasal endoscopy, and especially CT scan. Symptomatology of rhinosinusitis may vary, but whenever there is periorbital oedema, a displaced bulb, double- or reduced-vision, ophthalmoplegia or severe frontal headache, frontal swelling, signs of meningitis, focal neurological signs or systemic signs, one must be aware of these complications of rhinosinusitis and perform urgent investigations and intervention. These include a good interdisciplinary co-operation between otorhinolaryngology, ophthalmology, neurology, radiology, and possibly even maxillofacial surgery and paediatrics. The essential treatment of orbital cellulitis, which means a phlegmonous infection posterior to the orbital septum without abscess formation (stage II, according to the Chandler classification), is surgical drainage of the predisposing rhinosinusitis and concurrent parenteral antibiotics. The preferred surgical drainage nowadays is via an endoscopic approach in both children and in adults (5). CASE REPORT A female patient, 30 years old, was sent to the ENT Department of Motol Teaching Hospital, 1st Medical Faculty of Charles University in Prague, from the Ophthalmology Department with suspected unilateral orbitocellulitis. There was an obvious unilateral lid oedema on her left side, slight proptosis and ophthalmoplegia with diplopia, but no visual field loss or vision deterioration. She did not suffer from nasal obstruction, but only minimal nasal discharge and orbital and facial pressure on her left side. The duration of symptoms and ocular signs formation developed over two days. The patient belonged to an average socioeconomic status, with no previous comorbidity, and was not immunocompromised. Nasal endoscopy revealed a yellowish mucus in the middle meatus and mucosal swelling on the left side with no foetor. She was admitted, and blood analysis and CT scans were performed (Figure 1). The patient was subfebrile, with no chills. The white blood count revealed leukocytosis (22 000/ L) and an Figure 1. Coronary (A), axial (B) and sagittal (C) projections in a patient with left-sided odontogenous (black arrow) unilateral acute rhinosinusitis complicated by orbitocellulitis (day 0 preoperatively). Figure 2. Intracranial abscess formation in various planes of coronary (A) and axial (B) projections (day 20 postoperatively). extremely high C-reactive protein (CRP = 315). Parenteral antiobiotics (cefuroxim axetil 750 mg every 8 hours) were administered immediately. CT scans (paranasal sinuses projections: coronary, axial, sagittal) showed a maxillary sinusitis on the left side with the 1 st and 2 nd molar roots protruding into the maxillary sinus with no intraorbital abscess formation, just an effusion of the pre- and postseptal orbital soft tissue components). Stomatology examination was performed; it revealed a presumed necrotic 1 st molar. On the very day of admission, surgery under general anaesthesia was performed in terms of endoscopic sinus surgery on the left side (partial anterior ethmoidectomy and supraturbinal antrostomy) and necrotic molar extraction. Swabs (inclusive for anaerobic infection) of the maxillary sinus empyema was taken and according to probable odontegenous etiology, parenteral antibiotics were changed from cefuroxim to a combination of clindamycin (600 mg every 8 hours) and gentamycin (240 mg/day for 5 days). However, the swab revealed no positive results after two days of cultivation, therefore the antibiotics combination was consulted with the microbiology center of our hospital. The postoperative healing period was unconspicuous, free of any evident complication. The patient was not febrile or subfebrile from the 1 st postoperative day, the periocular oedema was in regression, and there was only residual crusting in the left nasal cavity with no putrid secretion. The only one residual symptom remaining was a slight pressure located in her left eye. A neurology and ophthalmology check-up were administered, but they revealed no pathology ( fully regular findings ) as well as stomatology check-up. The blood test before discharge displayed normal or almost normal findings (leuk / L, CRP 14) and the patient was released on the 7 th postoperative day, still continuing with peroral antibiotics intake (clindamycin 300mg every 8 hours) for another week. The patient was seen twice more (day 10 and 15 postoperatively) at the out-patient unit for cleaning her left nasal cavity of residual crusting (no nasal discharge or symptoms re-manifestation was recorded) and to review the definite histology (benign nasal/paranasal mucosa). On day 20 postoperatively, she was re-admitted urgently because a hemiparesis on the right side developed. Brain CT
3 Delayed intracranial complication 459 Figure 3. Coronary (A) and axial (B) projections documenting the post endoscopic sinus surgery result (day 21 postoperatively). revealed signs of meningitis (loss of subarachnoidal space and contrast saturation of pial veins) and an intracranial (subdural) abscess formation in the parafalcinic area left, i.e. interhemispheric empyema (Figure 2). Postoperative CT scans (taken on day 21 postoperatively) showed a good result of sinus surgery (Figure 3). Proper neurology, neurosurgery (craniotomy for subdural abscess) and medical measures were undertaken to manage the intracranial complication. The abscess fluid cultivation (for aerobes, anaerobes, fungi) was negative again. Blood culture was negative. No immunodeficiency was found. The patient still suffered from minimal residual neurological sequelae (residual motoric lesion on the right side) three months after hemiparesis manifestation. DISCUSSION Coincidence of orbital and intracranial complication of acute rhinisinusitis has been described very marginally in the literature. Most studies encompass orbital or intracranial complication separately, many include acute and chronic rhinosinusitis together, and the majority focuses on children. An interesting distribution of rhinosinusitis complications is seen upon demographic assessment. Two famous North- American studies on intracranial complications in rhinosinusitis in a predominantly adult, and young adult population and children do not handle orbital co-complications separately (4,6). Only 2 out of 24 patients (8.3%) in Clayman s study suffered from subsequent symptoms associated with intracranial complications typical for orbitocellulitis (ophthalmoplegia and decreased visual acuity) as well (4). Another retrospective study that focused on intracranial complications of rhinosinisutis revealed that in 3 of 15 patients (20%) there was additional subperiosteal abscess formation in the orbit (7). One of the latest North-American studies documented only about 4 cases of intracranial complications among 74 paediatric patients who were admitted for orbital infection (5.4%) (8). Only 1 of 52 patients (1,9%) with orbital cellulitis/orbital abscess subsequently developed an intracranial complication in a large retrospective study from Australia (meningitis) (9). Some studies from Africa have detailed a relatively large number of complications in rhinosinusitis, probably due to the lower availability of antibiotics administered for acute rhinosinusitis. One study from the region of West Africa revealed that orbitocellulitis developed in 47 of 90 (52%) patients admitted for rhinosinusitis. In 10 of 47 (19%) suffering from orbitocellulitis, a subsequent intracranial complication developed (cavernous sinus thrombosis, meningitis, etc.) (10). Another study from South Africa has reported the distribution of complications in 59 patients (children and young adults) with complicated rhinosinusitis: intracranial: 36 patients (61%), orbital: 13 (22%) and both intra-cranial and orbital: 10 patients (17%). There was a mortality of 5% (3 of 59 patients) (11). A large retrospective study concerning rhinogenic intracranial complications has shown that despite advances of modern medicine, a relatively high mortality of 16% is present (35 from 219 patients) with a prevalence of meningitis followed by brain abscess and subdural empyema (12). In a study from the Middle East, 9 of 116 patients (8%) developed an orbital abscess (after predisposing rhinisinusitis and trauma) and an intracranial complication (13). A study from Israel on orbital complications secondary to acute rhinosinusitis in children aged 2 and younger strongly relied on a meticulous multidisciplinary follow-up in a hospital. Surgical intervention was avoided in the majority of cases with proper diagnosis (only 1 from 52 was operated) (14). In Europe, 25 patients with complicated rhinosinusitis were followed up in a German study. The percentage of complications showed 20 (80%) patients with orbital complications, 3 (12%) with intracranial complications, and 2 (8%) with both orbital and intracranial complications (15). Consequently, no matter in what region of the world, there exists a group of patients with co-existing orbital and intracranial complications in rhinosinusitis, or where orbital complications of rhinosinusitis account for predisposing factors for developing intracranial complications (16,17). The neurological symptomatology is often mild or absent. Only one paper has stressed the role of MRI in early detection of intracranial cocomplications (8). All other studies strongly suggested relying on CT scanning, while the study by Herrmann (8) emphasized adjuvant MRI scanning due to some false negative results of CT scans in patients with subsequent intracranial abscess. MRI is advisable in patients with positive symptomatology ( changes in mentation, persistent fever) or indefinite CT findings. Some guidelines for the management of periorbital cellulitis/abscess have been proposed in Europe in the past (18,19). Standard CT scans done immediately for all cases of complicated rhinosinusitis after admission was not fully stressed. But EP³OS 2007 (= European position paper on rhinosinusitis and nasal polyps published by the European Rhinologic Society in 2007) has established that CT scanning is the preferred method of imaging in rhinosinusitis (1). CT scans in adults as well as in children upon admission is considered as conditio sine qua non.
4 460 Kastner et al. When one examines the results of studies on complications of rhinosinusitis, it is evident that orbital complications exceed intracranial complications by up to 20%. We propose performing an additional CT or MRI of the brain in patients admitted with orbital complications of rhinosinusitis despite negative brain pathology on the initial CT of the orbit/paranasal sinuses. Due to the different settings of CT of the orbit and CT of the brain, it was impossible to detect interhemispheric subdural empyema in an atypical location in our patient. The usual microbiological profile seems to be the same in all continents, with a prevalence of Streptococcus, Staphylococcus, anaerobes (e.g. Fusobacterium) present. Fungi is prevalent in immunocompromised individuals. A blood culture seems to be ineffective in the majority of cases. There might be a large number of negative cultures due to antibiotic pretreatment or cultivation failure. Possible future trends in revealing infectious agents are implemented in terms of molecular genetic methods (20). The predominance of complications in patients during the second and third decades of life is thought to be associated with a peak in the vascularity of the bony diploic system (and thus continued growth of the frontal sinus). Understandably, this implies that retrograde septic thrombophlebitis is the most likely route of infection. The direct or hematogenous routes are less common; atypical locations of the intracranial abscess might be found with hematogenous spread. The predominant location of complicated rhinosinusitis is the frontoethmoidal region. The maxillary sinus is predominantly affected in odontogenous rhinosinusitis; conversely, pansinusitis is surprisingly seldomly seen. Management of individual complications has been well established. These consist of medical measures (i.e. stationary treatment, parenteral broad spectrum antibiotics (for anaerobes as well) and surgical drainage of abscesses. Endo scopic sinus surgery is preferred over the external approach in surgical drainage of predisposing rhinosinusitis. A multidisciplinary approach is required in orbital or intracranial abscess formation. Standard treatment does not involve corticosteroids: these are administered only if the patient may benefit from reducing intracranial or intraorbital oedema (21). Intracranial infections still account for serious morbidity and mortality rates. In addition, the postoperative sequelae with residual neurological symptoms often imply disaster for a previously healthy, mostly young, adult population. CONCLUSION The diagnostic and therapeutic management of orbital complications of rhinosinusitis has been fully established. Nevetheless, some patients, especially young adults, suffer from subsequent intracranial complications. A co-existing/consequent intracranial complication affects this group of patients with orbital complications of rhinosinusitis in up 20% of cases according to reviews of the scientific literature. That is probably due to the aggressiveness of the infection or spread via anatomical channels. Proper treatment measures may mask these predisposing factors, and therefore in general, if one of the complications appears, the others must be excluded. We recommend to conclude treatment by performing a CT of the brain or MRI when an orbital complication has occurred following rhinosinusitis despite a negative brain pathology in CT scans of the orbit and paranasal sinuses and/or minimal or absent symptomatology before dismission from inhouse treatment. ACKNOWLEDGEMENTS To Professor Daniel Simmen (ORL-Zentrum, Klinik Hirslanden, Zurich, Switzerland) and to Professor Eduard Zverina (Neurosurgical unit, Dept. of Otorhinolaryngology and Head and Neck Surgery, University Hospital Motol, 1 st Medical Faculty, Charles University, Prague, Czech Republic) for their help, lectures and valuable consultations. Supported by grant GAUK /06 and IGA (Czech Republic). REFERENCES 1. Fokkens WJ, Lund VJ, Mullol J, et al. European Position Paper on Rhinosinusitis and Nasal Polyps Rhinology 2007; 45 suppl 20: Chandler JR, Langenbrunner DJ, Stevens ER. The pathogenesis of orbital complications in acute sinusitis. Laryngoscope 1970; 80: Lang EE, Curran AJ, Patil N, Walsh RM, Rawluk D, Walsh MA. Intracranial complications of acute frontal sinusitis. Clin Otolaryngol 2001; 26: Clayman GL, Adams GL, Paugh DR, Koopmann CF, Jr. Intracranial complications of paranasal sinusitis: a combined institutional review. Laryngoscope 1991; 101: Mortimore S, Wormald PJ. Management of acute complicated sinusitis: a 5-year review. Otolaryngol Head Neck Surg 1999; 121: Lerner DN, Choi SS, Zalzal GH, Johnson DL.Intracranial complications of sinusitis in childhood.ann Otol Rhinol Laryngol 1995; 104: Gallagher RM, Gross CW, Phillips, CD. Suppurative Intracranial Complications of Sinusitis Laryngoscope 1998; 108: Herrmann BW, Forsen JW. Simultaneous intracranial and orbital complications of acute rhinosinusitis in children. Int J Pediatr Otorhinolaryngol 2004; 68: Ferguson MP, McNab AA. Current treatment and outcome in orbital cellulitis. Aust N Z J Ophthalmol 1999; 27: Nwaorgu OGB, Awobem JF, Onakoya PA, Awobem AA. Orbital cellulitis complicating sinusitis: a 15-year review. Nigerian J Surg Res 2004; 6: Tshifularo M, Monama GM. Complications of inflammatory sinusitis in children: institutional review. SA Fam Pract 2006; 48: Singh B, Van Dellen J, Ramjettan S, Maharaj TJ. Sinogenic intracranial complications. J Laryngol Otol. 1995; 109: Chaudhry IA, Shamsi FA, Elzaridi E, Al-Rashed W, Al-Amri A, Al-Anezi F, Arat YO, Holck DE.Outcome of treated orbital cellulitis in a tertiary eye care center in the middle East. Ophthalmology 2007; 114:
5 Delayed intracranial complication Eviatar E, Gavriel H, Pitaro K, Vaiman M, Goldman M, Kessler A. Conservative treatment in rhinosinusitis orbital complications in children aged 2 years and younger. Rhinology. 2008; 46: Eufinger H, Machtens E. Purulent pansinusitis, orbital cellulitis and rhinogenic intracranial complications. J Craniomaxillofac Surg 2001; 29: Reynolds DJ, Kodsi SR, Rubin SE, Rodgers IR. Intracranial infection associated with preseptal and orbital cellulitis in the pediatric patient. J AAPOS 2003; 7: Brijlal Meena MK, Sharma P. Epidural empyema secondary to orbital cellulitis: a case report. Eur J Ophthalmol 2007; 17: Jones NS, Walker JL, Bassi S, Jones T, Punt J. The intracranial complications of rhinosinusitis: can they be prevented? Laryngoscope 2002; 112: Howe L, Jones NS. Guidelines for the management of periorbital cellulitis/abscess. Clin Otolaryngol Allied Sci 2004; 29: Gosepath J, Brieger J, Vlachtsis K, Mann WJ. Fungal DNA is present in tissue specimens of patients with chronic rhinosinusitis. Am J Rhinol 2004; 18: Yen MT, Yen KG. Effect of corticosteroids in the acute management of pediatric orbital cellulitis with subperiosteal abscess. Ophthal Plast Reconstr Surg 2005; 21: Jan Kastner Dept. of Otorhinolaryngology and Head and Neck Surgery University Hospital Motol, 1st Medical Faculty Charles University V Uvalu Prague Czech Republic Tel: Fax: jkastner@ .cz, jkastner@uni-mainz.de
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Orbital Complications of Acute Sinusitis: Evaluation, Management and Outcome Havle Abhay *,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Orbital Complications of Acute Sinusitis: Evaluation, Management and Outcome Havle Abhay *,
Introduction. Ophthalmic manifestations can result from a myriad of Non Sinogenic and Sinogenic Disease :
 Ophthalmic Manifestations of Paranasal Sinus Disease; A Clinical Grading System Surayie Al Dousary, MD Associate Professor Director Rhinology Research Chair & Fatma Al Anazy, MD Associate Professor Rhinology
Ophthalmic Manifestations of Paranasal Sinus Disease; A Clinical Grading System Surayie Al Dousary, MD Associate Professor Director Rhinology Research Chair & Fatma Al Anazy, MD Associate Professor Rhinology
Inflammation of the paranasal sinuses is a common
 Case Report 5 Concomitant ilateral Orbital and rain bscesses-unusual Complications of Pediatric Rhinosinusitis Shiang-Fu Huang, MD; Ta-Jen Lee, MD; Kuang-Lin Lin, MD Rhinosinusitis is a common medical
Case Report 5 Concomitant ilateral Orbital and rain bscesses-unusual Complications of Pediatric Rhinosinusitis Shiang-Fu Huang, MD; Ta-Jen Lee, MD; Kuang-Lin Lin, MD Rhinosinusitis is a common medical
Sinusitis & its complication. MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University
 Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
A descriptive study of the patients with orbital complication of acute and chronic sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
ORIGINAL ARTICLE. Group Chandler Maloney. First Inflammatory oedema Preseptal cellulitis. Second Orbital Cellulitis Subperiosteal abscess
 ORBITAL MANIFESTATIONS OF SINUS DISEASE T. Jyothirmayi 1, V. Meenakshi 2, M. Deepika 3 HOW TO CITE THIS ARTICLE: T. Jyothirmayi, V. Meenakshi, M. Deepika. Orbital Manifestations of Sinus Disease. Journal
ORBITAL MANIFESTATIONS OF SINUS DISEASE T. Jyothirmayi 1, V. Meenakshi 2, M. Deepika 3 HOW TO CITE THIS ARTICLE: T. Jyothirmayi, V. Meenakshi, M. Deepika. Orbital Manifestations of Sinus Disease. Journal
Chronic Rhinosinusitis-Treatment
 Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Chronic Rhinosinusitis-Treatment INFECTION INFLAMMATION Predisposing Factors Anatomical variations Allergic rhinitis Acute sinusitis Immune deficiency Rhinosinusitis Non-allergic rhinitis Chronic sinusitis
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
ORIGINAL ARTICLE. Intracranial Complications of Sinusitis in Children and Adolescents and Their Outcomes. of sinusitis are uncommon
 ORIGINAL ARTICLE Intracranial s of Sinusitis in Children and Adolescents and Their Outcomes John A. Germiller, MD, PhD; Daniel L. Monin, MD; Anthony M. Sparano, MD; Lawrence W. C. Tom, MD Objective: To
ORIGINAL ARTICLE Intracranial s of Sinusitis in Children and Adolescents and Their Outcomes John A. Germiller, MD, PhD; Daniel L. Monin, MD; Anthony M. Sparano, MD; Lawrence W. C. Tom, MD Objective: To
Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications: A Case-Control Study
 The Scientific World Journal Volume 2013, Article ID 453297, 5 pages http://dx.doi.org/10.1155/2013/453297 Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications:
The Scientific World Journal Volume 2013, Article ID 453297, 5 pages http://dx.doi.org/10.1155/2013/453297 Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications:
Orbital Complications of Sinogenic Origin: A Case Study of 20 Patients
 World Articles of Ear, Nose and Throat ---------------------Page 1 Orbital Complications of Sinogenic Origin: A Case Study of 20 Patients Authors: Shrinivas Shripatrao Chavan*, Sunil D.Deshmukh**, Vasant
World Articles of Ear, Nose and Throat ---------------------Page 1 Orbital Complications of Sinogenic Origin: A Case Study of 20 Patients Authors: Shrinivas Shripatrao Chavan*, Sunil D.Deshmukh**, Vasant
This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy.
 This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/92131/
This is a repository copy of The microbial causes of complicated Acute Bacterial Rhinosinusitis and implications for empirical antimicrobial therapy. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/92131/
Clinical Manifestations of Intracranial Complication Associated With Paranasal Sinus Infection
 Clinical Manifestations of Intracranial Complication Associated With Paranasal Sinus Infection Byoung-Ki Kim, M.D., Hwa-Young Lee. M.D., Hee-Jung Song, M.D., Tae-Hong Kim*,.M,D., Moon-Gu Han, M,D., Gun-Sei
Clinical Manifestations of Intracranial Complication Associated With Paranasal Sinus Infection Byoung-Ki Kim, M.D., Hwa-Young Lee. M.D., Hee-Jung Song, M.D., Tae-Hong Kim*,.M,D., Moon-Gu Han, M,D., Gun-Sei
PERIORBITAL SWELLING - COMPLICATION FROM ADJACENT STRUCTURES CASE REPORTS AND REVIEW OF LITERATURE
 VOLUME 26, NO. 3 JUNE 1985 PERIORBITAL SWELLING - COMPLICATION FROM ADJACENT STRUCTURES CASE REPORTS AND REVIEW OF LITERATURE K Sukumaran S Chandran N Janakarajah P K Garg Department of Ophthalmology Faculty
VOLUME 26, NO. 3 JUNE 1985 PERIORBITAL SWELLING - COMPLICATION FROM ADJACENT STRUCTURES CASE REPORTS AND REVIEW OF LITERATURE K Sukumaran S Chandran N Janakarajah P K Garg Department of Ophthalmology Faculty
Bilateral Diplopia and Abducent Nerve Palsy Secondary to Odontogenic Sinusitis: An Unusual Presentation
 Bahrain Medical Bulletin, Vol. 36, No. 4, December 2014 Bilateral Diplopia and Abducent Nerve Palsy Secondary to Odontogenic Sinusitis: An Unusual Presentation Samer Malas, MD* Hiba Al-Reefy, MB, BCh,
Bahrain Medical Bulletin, Vol. 36, No. 4, December 2014 Bilateral Diplopia and Abducent Nerve Palsy Secondary to Odontogenic Sinusitis: An Unusual Presentation Samer Malas, MD* Hiba Al-Reefy, MB, BCh,
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Management of Children with Preseptal and Orbital Cellulitis
 Management of Children with Preseptal and Orbital Cellulitis Trust Ref: B24/2017 1. Introduction Periorbital infections are infections involving the soft tissues surrounding the globe of the eye. Chandler
Management of Children with Preseptal and Orbital Cellulitis Trust Ref: B24/2017 1. Introduction Periorbital infections are infections involving the soft tissues surrounding the globe of the eye. Chandler
Emergency Ocular Motility Disorders Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Emergency Ocular Motility Disorders Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Emergency Ocular Motility Disorders Cranial nerves palsies (oculomotor, Trochlear & abducent) Orbital
Emergency Ocular Motility Disorders Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Emergency Ocular Motility Disorders Cranial nerves palsies (oculomotor, Trochlear & abducent) Orbital
Characteristics of Superior Orbital Subperiosteal Abscesses in Children
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Characteristics of Superior Orbital Subperiosteal Abscesses in Children Lourdes Quintanilla-Dieck, MD; Sivakumar
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Characteristics of Superior Orbital Subperiosteal Abscesses in Children Lourdes Quintanilla-Dieck, MD; Sivakumar
ISPUB.COM. An Orbital Cellulitis Demanding Multispeciality Management. N Ezhilvathani, Thiagarajan, T Cherian INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 An Orbital Cellulitis Demanding Multispeciality Management N Ezhilvathani, Thiagarajan, T Cherian Citation N Ezhilvathani,
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 An Orbital Cellulitis Demanding Multispeciality Management N Ezhilvathani, Thiagarajan, T Cherian Citation N Ezhilvathani,
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
Vascular and Parameningeal Infections of the Head and Neck
 Vascular and Parameningeal Infections of the Head and Neck Kevin B. Laupland, MD, MSc, FRCPC Associate Professor Departments of Medicine, Critical Care Medicine, Pathology and Laboratory Medicine, and
Vascular and Parameningeal Infections of the Head and Neck Kevin B. Laupland, MD, MSc, FRCPC Associate Professor Departments of Medicine, Critical Care Medicine, Pathology and Laboratory Medicine, and
Moath Darweesh. Zaid Emad. Anas Abu -Humaidan
 3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
Complications of acute rhinosinusitis in The Netherlands
 Family Practice 2012; 29:147 153 doi:10.1093/fampra/cmr062 Advance Access published on 5 September 2011 Ó The Author 2011. Published by Oxford University Press. All rights reserved. For permissions, please
Family Practice 2012; 29:147 153 doi:10.1093/fampra/cmr062 Advance Access published on 5 September 2011 Ó The Author 2011. Published by Oxford University Press. All rights reserved. For permissions, please
Provider Led Entity. CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018
 Provider Led Entity CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018 Appropriateness of advanced imaging procedures* in patients with rhinosinusitis and the following clinical presentations or diagnoses:
Provider Led Entity CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018 Appropriateness of advanced imaging procedures* in patients with rhinosinusitis and the following clinical presentations or diagnoses:
Limitations of balloon sinuplasty in frontal sinus surgery
 Eur Arch Otorhinolaryngol (2011) 268:1463 1467 DOI 10.1007/s00405-011-1626-7 RHINOLOGY Limitations of balloon sinuplasty in frontal sinus surgery S. Heimgartner J. Eckardt D. Simmen H. R. Briner A. Leunig
Eur Arch Otorhinolaryngol (2011) 268:1463 1467 DOI 10.1007/s00405-011-1626-7 RHINOLOGY Limitations of balloon sinuplasty in frontal sinus surgery S. Heimgartner J. Eckardt D. Simmen H. R. Briner A. Leunig
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST
 www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
www.manchesterchildrensent.com ACUTE PAEDIATRIC EAR PRESENTATIONS PROF IAIN BRUCE PAEDIATRIC OTOLARYNGOLOGIST & ADULT OTOLOGIST A CHILD WITH EARACHE UNCOMPLICATED AOM ACUTE OTITIS MEDIA Acute otitis media
The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults
 The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults *Kolo ES Department of Otorhinolaryngology, Bayero University Kano/Aminu Kano Teaching Hospital, Kano, Nigeria
The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults *Kolo ES Department of Otorhinolaryngology, Bayero University Kano/Aminu Kano Teaching Hospital, Kano, Nigeria
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum
 Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
SINUSITIS/RHINOSINUSITIS
 1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
1. Medical Condition TUEC Guidelines SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which is the inflammation
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum
 Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Kathleen R. Fink, MD Virginia Mason Medical Center. 6 th Nordic Emergency Radiology Course 2017
 Kathleen R. Fink, MD Virginia Mason Medical Center 6 th Nordic Emergency Radiology Course 2017 Disclosure My spouse has a financial relationship with a commercial organization that may have a direct or
Kathleen R. Fink, MD Virginia Mason Medical Center 6 th Nordic Emergency Radiology Course 2017 Disclosure My spouse has a financial relationship with a commercial organization that may have a direct or
PRESEPTAL AND ORBITAL CELLULITIS IN CHILDREN- CLINICAL GUIDELINE V3.0
 PRESEPTAL AND ORBITAL CELLULITIS IN CHILDREN- CLINICAL GUIDELINE V3.0 Page 1 of 8 1. Aim/Purpose of this Guideline 1.1. This guideline applies to medical and nursing staff caring for a child with Preseptal
PRESEPTAL AND ORBITAL CELLULITIS IN CHILDREN- CLINICAL GUIDELINE V3.0 Page 1 of 8 1. Aim/Purpose of this Guideline 1.1. This guideline applies to medical and nursing staff caring for a child with Preseptal
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
Allergic Fungal Rhinosinusitis
 Allergic Fungal Rhinosinusitis My Published Experience 1999-2018 Prof. Surayie H Al Dousary Professor of Rhinology Rhinology research Chair Director KSU Rhinology fellowship Program Director KSU Rhinology
Allergic Fungal Rhinosinusitis My Published Experience 1999-2018 Prof. Surayie H Al Dousary Professor of Rhinology Rhinology research Chair Director KSU Rhinology fellowship Program Director KSU Rhinology
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488
 National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Grand Round. Subdural empyema and other suppurative complications of paranasal sinusitis * *
 Subdural empyema and other suppurative complications of paranasal sinusitis Melissa K Osborn, James P Steinberg Lancet Infect Dis 2007; 7: 62 67 Division of Infectious Diseases, Department of Medicine,
Subdural empyema and other suppurative complications of paranasal sinusitis Melissa K Osborn, James P Steinberg Lancet Infect Dis 2007; 7: 62 67 Division of Infectious Diseases, Department of Medicine,
ACUTE MASTOIDITIS IN CHILDREN: SUSCEPTIBILITY FACTORS AND MANAGEMENT
 & ACUTE MASTOIDITIS IN CHILDREN: SUSCEPTIBILITY FACTORS AND MANAGEMENT Slobodan Spremo*, Biljana Udovčić Clinic for Otorhinolaryngology, Clinic Center in Banja Luka, Zdrave Korde 1, 78000 Banja Luka, Bosnia
& ACUTE MASTOIDITIS IN CHILDREN: SUSCEPTIBILITY FACTORS AND MANAGEMENT Slobodan Spremo*, Biljana Udovčić Clinic for Otorhinolaryngology, Clinic Center in Banja Luka, Zdrave Korde 1, 78000 Banja Luka, Bosnia
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis
 Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Acute Otitis Media, Acute Bacterial Sinusitis, and Acute Bacterial Rhinosinusitis This guideline, developed by Larry Simmons, MD, in collaboration with the ANGELS team, on October 3, 2013, is a significantly
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017
 Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Characteristics of Patients Treated for Orbital Cellulitis: An Analysis of Inpatient Data
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Characteristics of Patients Treated for Orbital Cellulitis: An Analysis of Inpatient Data Emily Marchiano,
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Characteristics of Patients Treated for Orbital Cellulitis: An Analysis of Inpatient Data Emily Marchiano,
Practice patterns regarding noninvasive rhinosinusitis in the immunosuppressed patient population
 Practice patterns regarding noninvasive rhinosinusitis in the immunosuppressed patient population Zara M. Patel, Emory University Journal Title: Allergy & Rhinology Volume: Volume 4, Number 3 Publisher:
Practice patterns regarding noninvasive rhinosinusitis in the immunosuppressed patient population Zara M. Patel, Emory University Journal Title: Allergy & Rhinology Volume: Volume 4, Number 3 Publisher:
Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities
 Romanian Journal of Rhinology, Volume 8, No. 29, January-March 2018 ORIGINAL STUDY DOI: 10.2478/rjr-2018-0003 Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities Emilia
Romanian Journal of Rhinology, Volume 8, No. 29, January-March 2018 ORIGINAL STUDY DOI: 10.2478/rjr-2018-0003 Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities Emilia
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Sinusitis/Rhinosinusitis SINUSITIS/RHINOSINUSITIS
 1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
1. Medical Condition SINUSITIS/RHINOSINUSITIS Sinusitis refers to inflammation of the sinuses only while the more clinically relevant term should be Rhinosinusitis which refers to inflammation of both
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases
 Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
European position paper on Rhinosinusitis & Nnasal Polyps 2012 (summary)
 Rhinology Chair Weekly Activity European position paper on Rhinosinusitis & Nnasal Polyps 2012 (summary) Mohammed s. Al-Ahmari 12/02/2012 www.rhinologychair.org conference@rhinologychair.org Rhinology
Rhinology Chair Weekly Activity European position paper on Rhinosinusitis & Nnasal Polyps 2012 (summary) Mohammed s. Al-Ahmari 12/02/2012 www.rhinologychair.org conference@rhinologychair.org Rhinology
Incidence of accessory ostia in patients with chronic maxillary sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
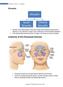 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus surgery
 Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
AMSER Case of the Month July 2018 Complicated Headache with Fever
 AMSER Case of the Month July 2018 Complicated Headache with Fever Benjamin Park, MS IV Dr. Karen Xie Department of Radiology University of Illinois College of Medicine at Chicago Patient Presentation CC:
AMSER Case of the Month July 2018 Complicated Headache with Fever Benjamin Park, MS IV Dr. Karen Xie Department of Radiology University of Illinois College of Medicine at Chicago Patient Presentation CC:
Index. K Keratectomy, 213
 Index A Acute bacterial rhinosinusitis (ABRS), 76, 78 Acute rhinosinusitis (ARS), 77 83 diagnostic symptoms, 75 direct and indirect costs, 75 pathophysiology, 76, 77 sinonasal inflammationin, 75 treatment
Index A Acute bacterial rhinosinusitis (ABRS), 76, 78 Acute rhinosinusitis (ARS), 77 83 diagnostic symptoms, 75 direct and indirect costs, 75 pathophysiology, 76, 77 sinonasal inflammationin, 75 treatment
Orbital and Ocular Adnexal Disorders with Red Eyes
 Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Orbital and Ocular Adnexal Disorders with Red Eyes Jason Lee Associate Consultant Department of Ophthalmology and Visual Sciences Practical Ophthalmology for the Family Physician 21 Jan 2017 No financial
Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A. Case Report
 ISSN: 2250-0359 Volume 5 Issue 3 2015 Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A Case Report Roshan Kumar Verma Naresh K panda PGIMER, Chandigarh, India ABSTRACT
ISSN: 2250-0359 Volume 5 Issue 3 2015 Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A Case Report Roshan Kumar Verma Naresh K panda PGIMER, Chandigarh, India ABSTRACT
Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre
 Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
Original Article DOI: 10.17354/ijss/2016/130 Incidence of Odontogenic Sinusitis Experience in a Tertiary Care Centre B G Prakash 1, Suhasini Biyyapu 2 1 Professor, Department of ENT, JSS Medical College,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,350 108,000 1.7 M Open access books available International authors and editors Downloads Our
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
ISSN X (Print) Research Article. *Corresponding author Dr.V. Krishna Chaitanya
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Document Title: Selected E.N.T. Emergencies Related to Sepsis. Author(s): Jim Holliman (Uniformed Services University), MD, FACEP, 2012
 Project: Ghana Emergency Medicine Collaborative Document Title: Selected E.N.T. Emergencies Related to Sepsis Author(s): Jim Holliman (Uniformed Services University), MD, FACEP, 2012 License: Unless otherwise
Project: Ghana Emergency Medicine Collaborative Document Title: Selected E.N.T. Emergencies Related to Sepsis Author(s): Jim Holliman (Uniformed Services University), MD, FACEP, 2012 License: Unless otherwise
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
A Study of Anatomical Variations in Patients with Chronic Rhinosinusitis.
 DOI: 10.2127/aimdr.201..2.EN1 Original Article ISSN (O):239-222; ISSN (P):239-21 A Study of Anatomical Variations in Patients with Chronic Rhinosinusitis. Smruti Swain 1 1 Associate Professor, Department
DOI: 10.2127/aimdr.201..2.EN1 Original Article ISSN (O):239-222; ISSN (P):239-21 A Study of Anatomical Variations in Patients with Chronic Rhinosinusitis. Smruti Swain 1 1 Associate Professor, Department
Orbital complications of ENT diseases
 International Journal of Otorhinolaryngology and Head and Neck Surgery Kumar A et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jan;4(1):210-216 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Kumar A et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jan;4(1):210-216 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
Pediatric Endoscopic Sinus Surgery in a Tertiary Government Hospital: Patient Profile and Surgical Indications
 Philippine Journal Of Otolaryngology-Head And Neck Surgery Vol. 4 No. January June ichael Joseph C. David, D Gil. Vicente, D, Antonio H. Chua, D, Jose R. Reyes emorial edical Center St. Luke s edical Center
Philippine Journal Of Otolaryngology-Head And Neck Surgery Vol. 4 No. January June ichael Joseph C. David, D Gil. Vicente, D, Antonio H. Chua, D, Jose R. Reyes emorial edical Center St. Luke s edical Center
PA PROGRAMA ANALITICĂ
 RED: 0 DATA: 0..03 MINISTRY OF HEALTH OF THE REPUBLIC OF MOLDOVA STATE MEDICAL AND PHARMACEUTICAL UNIVERSITY NICOLAE TESTEMIŢANU Approved at the Medicine Faculty Council meeting Minutes Nr. of a Dean of
RED: 0 DATA: 0..03 MINISTRY OF HEALTH OF THE REPUBLIC OF MOLDOVA STATE MEDICAL AND PHARMACEUTICAL UNIVERSITY NICOLAE TESTEMIŢANU Approved at the Medicine Faculty Council meeting Minutes Nr. of a Dean of
Destructive Giant Maxillary Sinus Mucocele: A Case Report
 Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Unique Journal of Medical and Dental Sciences Available online: Research Article
 ISSN 2347-5579 Unique Journal of Medical and Dental Sciences Available online: www.ujconline.net Research Article STUDY OF ANATOMICAL VARIATIONS OF LATERAL WALL OF NOSE BY ENDOSCOPE Kolvekar VD 1*, Kazi
ISSN 2347-5579 Unique Journal of Medical and Dental Sciences Available online: www.ujconline.net Research Article STUDY OF ANATOMICAL VARIATIONS OF LATERAL WALL OF NOSE BY ENDOSCOPE Kolvekar VD 1*, Kazi
ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS
 From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision
 THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
Histopathology of Nasal Masses
 ORIGINAL ARTICLE Histopathology of Nasal Masses 1 Hemant Chopra, 2 Kapil Dua, 3 Neha Chopra, 4 Vikrant Mittal AIJCR Histopathology of Nasal Masses 1 Professor and Head, Dayanand Medical College, Ludhiana,
ORIGINAL ARTICLE Histopathology of Nasal Masses 1 Hemant Chopra, 2 Kapil Dua, 3 Neha Chopra, 4 Vikrant Mittal AIJCR Histopathology of Nasal Masses 1 Professor and Head, Dayanand Medical College, Ludhiana,
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
ORIGINAL ARTICLE. Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis
 ORIGINAL ARTICLE Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis John M. DelGaudio, MD; Ron E. Swain Jr, MD; Todd T. Kingdom, MD; Susan Muller, DMD; Patricia A. Hudgins, MD Objective:
ORIGINAL ARTICLE Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis John M. DelGaudio, MD; Ron E. Swain Jr, MD; Todd T. Kingdom, MD; Susan Muller, DMD; Patricia A. Hudgins, MD Objective:
Cavernous sinus thrombosis: Departmental guidelines
 Michele Long Division of Otorhinolaryngology Faculty of Health Sciences Tygerberg Campus, University of Stellenbosch Cavernous sinus thrombosis: Departmental guidelines Anatomy- cavernous sinus 2cm in
Michele Long Division of Otorhinolaryngology Faculty of Health Sciences Tygerberg Campus, University of Stellenbosch Cavernous sinus thrombosis: Departmental guidelines Anatomy- cavernous sinus 2cm in
CNS Complications of Frontal Sinus Disease
 Chapter CNS Complications of Frontal Sinus Disease Core Messages (Overview) Although less common since the advent of antibiotics, CNS complications of frontal sinusitis still occur and warrant a high index
Chapter CNS Complications of Frontal Sinus Disease Core Messages (Overview) Although less common since the advent of antibiotics, CNS complications of frontal sinusitis still occur and warrant a high index
ORIGINAL ARTICLE RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS.
 RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
Concepts in Rhinosinusitis. Nick Jones University of Nottingham
 Concepts in Rhinosinusitis Nick Jones University of Nottingham Definition of rhinosinusitis Very broad and is based on clinical symptoms, CT and endoscopy NOT on pathology Definition of rhinosinusitis
Concepts in Rhinosinusitis Nick Jones University of Nottingham Definition of rhinosinusitis Very broad and is based on clinical symptoms, CT and endoscopy NOT on pathology Definition of rhinosinusitis
Institutional repositories
 PUBLISHED VERSION Khong, Jwu Jin; Malhotra, Raman; Selva-Nayagam, Dinesh Niranjan; Wormald, Peter-John Efficacy of endoscopic sinus surgery for paranasal sinus mucocele including modified endoscopic Lothrop
PUBLISHED VERSION Khong, Jwu Jin; Malhotra, Raman; Selva-Nayagam, Dinesh Niranjan; Wormald, Peter-John Efficacy of endoscopic sinus surgery for paranasal sinus mucocele including modified endoscopic Lothrop
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
