Cognitive dysfunction and white matter abnormalities in antiphospholipid syndrome
|
|
|
- Nora Hawkins
- 6 years ago
- Views:
Transcription
1 Pathophysiology 18 (2011) Review Cognitive dysfunction and white matter abnormalities in antiphospholipid syndrome Doruk Erkan a,b,c, Elizabeth Kozora d,e,b, Michael D. Lockshin a,b,c, a The Barbara Volcker Center for Women and Rheumatic Disease, United States b Hospital for Special Surgery, United States c Weill Medical College of Cornell University, United States d Department of Medicine, National Jewish Health, United States e Department of Psychiatry and Neurology, University of Colorado Denver Medical School, United States Received 4 November 2009; received in revised form 28 February 2010; accepted 19 April 2010 Abstract Diagnosis of the antiphospholipid syndrome (APS) requires that a patient have both a clinical event (thrombosis or pregnancy loss) and persistently positive antiphospholipid antibodies (apl). Although stroke and transient ischemic attack are the most common neurologic manifestations of APS, both cognitive dysfunction and magnetic resonance imaging (MRI) white matter hyperintensities can occur in aplpositive patients (with or without APS). Relatively little is known about the cognitive pattern in apl-positive patients; MRI white matter hyperintensities may be related to underlying attentional and executive cognitive impairment. Studies with sophisticated neuroimaging techniques aimed to better understand MRI white matter hyperintensities may eventually facilitate our understanding of cognitive dysfunction in apl-positive patients Elsevier Ireland Ltd. All rights reserved. Keywords: Antiphospholipid syndrome; Cognitive dysfunction; White matter abnormalities Contents 1. Introduction Antiphospholipid syndrome brief overview Etiopathogenesis Clinical manifestations Diagnosis Treatment Cognitive dysfunction and white matter abnormalities in antiphospholipid syndrome Cognitive dysfunction in antiphospholipid syndrome and lupus White matter abnormalities in antiphospholipid syndrome and lupus Conclusion References Corresponding author at: The Barbara Volcker Center for Women and Rheumatic Disease, Hospital for Special Surgery, 535 E 70th Street, New York, NY 10021, United States. Tel.: ; fax: address: LockshinM@hss.edu (M.D. Lockshin) /$ see front matter 2010 Elsevier Ireland Ltd. All rights reserved. doi: /j.pathophys
2 94 D. Erkan et al. / Pathophysiology 18 (2011) Table 1 Revised Sapporo classification criteria for the antiphospholipid syndrome [1]. Clinical criteria 1. Vascular thrombosis One or more clinical episodes of arterial, venous, or small vessel thrombosis, in any tissue or organ. 2. Pregnancy morbidity (a) One or more unexplained deaths of a morphologically normal fetus at or beyond the 10th week of gestation, or (b) One or more premature births of a morphologically normal neonate before the 34th week of gestation because of: eclampsia, severe preeclampsia, or recognized features of placental insufficiency, or (c) Three or more unexplained consecutive spontaneous abortions before the 10th week of gestation, with maternal anatomic or hormonal abnormalities and paternal and maternal chromosomal causes excluded. Laboratory criteria 1. Lupus anticoagulant present in plasma, on 2 or more occasions at least 12 weeks apart, detected according to the guidelines of the International Society on Thrombosis and Hemostasis. 2. Anticardiolipin antibody of IgG and/or IgM isotype in serum or plasma, present in medium or high titer (i.e. >40 GPL or MPL, or >the 99th percentile), on 2 or more occasions, at least 12 weeks apart, measured by a standardized enzyme-linked immunosorbent assay (ELISA). 3. Anti- 2 -glycoprotein-i antibody of IgG and/or IgM isotype in serum or plasma (in titer > the 99th percentile) present on 2 or more occasions, at least 12 weeks apart, measured by a standardized ELISA. Definite APS is present if at least one of the clinical criteria and one of the laboratory criteria are met. Classification of APS should be avoided if less than 12 weeks or more than 5 years separate the positive apl test and the clinical manifestation. In studies of populations of patients who have more than one type of pregnancy morbidity, investigators are strongly encouraged to stratify groups of subjects according to a, b, or c above. 1. Introduction Diagnosis of the antiphospholipid syndrome (APS) requires that a patient have both a clinical event (thrombosis or pregnancy loss) and persistent moderate-to-high titer antiphospholipid antibody (apl), documented by a solid phase serum assay (anticardiolipin [acl] or anti- 2 -glycoprotein-i [ 2 GPI] enzyme-linked immunosorbent assay) and/or by an inhibitor of phospholipid-dependent clotting (lupus anticoagulant [LA] test) (Table 1) [1,2]. Antiphospholipid syndrome can occur as an isolated diagnosis (primary APS) or associated with other systemic rheumatic diseases such as systemic lupus erythematosus (SLE). The presence of apl in the absence of characteristic clinical complications does not indicate APS, and asymptomatic (no history of vascular and pregnancy events) apl-positive patients exist. Although stroke and transient ischemic attack are common neurologic manifestations of APS, other neuropsychiatric syndromes that can occur in apl-positive patients (with or without APS) include (although some controversial) seizures, chorea, migraine, cognitive dysfunction, and white matter hyperintensities [3]. This review article will start with a brief overview of the etiopathogenesis, clinical manifestations, diagnosis, and treatment of APS, which will be followed by a detailed discussion of cognitive dysfunction in apl-positive patients as well as the relationship between cognitive dysfunction and magnetic resonance imaging (MRI) abnormalities (white matter hyperintensities). The detailed description of APS, neurologic manifestations of apl, and management of apl-positive patients can be found elsewhere [4]. 2. Antiphospholipid syndrome brief overview 2.1. Etiopathogenesis Antiphospholipid antibodies exist as a family of autoantibodies directed against phospholipid-binding plasma proteins, most commonly 2 GPI. The binding proteins of interest bind negatively charged phospholipids (cardiolipin, phosphatidylglycerol, phosphatidylserine, phosphatidylinositol), and not necessarily zwitterionic or neutral phospholipids (phosphatidylethanolamine, phosphatidylcholine). Other phospholipid-binding plasma proteins are prothrombin, thrombomodulin, high molecular weight kininogen, low molecular weight kininogen, antithrombin III, protein C, protein S, and annexins I and V [5]. In vivo, the likely relevant phospholipid to which these proteins bind is phosphatidylserine, normally on the inner cell membrane but exteriorized, and therefore made visible, during cell activation and apoptosis. The commonly accepted hypothesis regarding the origin of apl states that an incidental exposure to environmental agents, the antigens of which contain 2 GPI-like peptides, induces apl in susceptible individuals via molecular mimicry. In experimental animal models, passive or active immunization with viral peptides [6], bacterial peptides [7], and heterologous 2 GPI [8] induce polyclonal apl and clinical events associated with APS. 2 -glycoprotein-i polymorphisms influence the generation of apl in individuals but have only a weak relationship to the occurrence of apl-related clinical events [9]. Persons congenitally lacking 2 GPI [10] appear normal. 2 GPI-knock-out mice also appear normal [11]. In humans, although cross-sectional and prospective cohort studies demonstrate that apl can predict future thrombosis, the exact pathogenic mechanism is unknown; several mechanisms are likely involved, as outlined in Table 2. Because high-titer antibody may persist for years in asymptomatic persons and because positive apl tests may precede symptoms for many years, it is likely that vascular injury and/or endothelial cell activation immediately precede thrombosis in persons bearing the antibody. Platelet activation followed by binding of apl to platelet membrane phospholipid-bound annexins may initiate platelet adhesion and thrombosis [12]. Antiphospholipid antibodies may inhibit phospholipid-dependent reactions in the coagulation cascade, for example, fibrinolysis, antithrombin III
3 D. Erkan et al. / Pathophysiology 18 (2011) Table 2 Possible mechanisms of apl-induced thrombosis. 1. Endothelial Cells-aPL interaction a. Endothelial cell damage or activation (via increased expression of adhesion molecules) b. Coexisting anti-endothelial antibodies c. apl-induced monocyte adhesion to endothelial cells d. Increased tissue factor expression 2. Platelet apl interaction a. Platelet activation b. Stimulation of thromboxane production 3. Coagulation system apl interaction a. Inhibition of activation of protein C by the thrombomodulin thrombin complex; b. Inhibition of activation of protein C via its cofactor protein S c. Interaction between apl and substrates of activated protein C such as Factors Va and VIIIa d. Interaction between apl and an annexin V anticoagulant shield 4. Complement activation activity, or protein C and protein S activation [13]. Interaction between apl and an annexin V anticoagulant shield is another proposed but less well accepted mechanism [14]. Recent studies also demonstrate that apl increase tissue factor (a physiologic initiator of coagulation) expression on monocytes [15]. A cluster of 50 upregulated genes may distinguish between apl-positive patients with and without thrombosis [16]. A proposed pathogenesis for apl-mediated thrombosis begins with activation or apoptosis, by unknown (possibly infectious or traumatic) triggers, of platelets, endothelial cells, or trophoblast. The negatively charged phospholipid phosphatidylserine migrates from the inner to the normally electrically neutral outer cell membrane. Circulating 2 GPI then binds to phosphatidylserine. Antiphospholipid antibodies then bind to a 2 GPI dimer, activating complement and through C5a initiating a signaling cascade that induces cell surface tissue factor expression and adhesion molecules. Other components of the innate immune system may also be activated. Platelets aggregate and initiate thrombosis. In addition, antiphospholipid antibodies adversely affect formation of a trophoblast syncytium, placental apoptosis, and trophoblast invasion, all processes required for normal establishment of placental function. In vitro, pathogenic apl induces adhesion molecules and enhance adherence of leukocytes to cultured endothelial cells. In experimental animal models, apl causes fetal resorption (a proxy for recurrent fetal loss) and increase in size and duration of trauma-induced venous and arterial thrombi. Inhibiting complement activation prevents experimental aplinduced fetal death, and C5 knock-out mice carry pregnancies normally despite the presence of apl, implying that a complement-mediated effector mechanism is an absolute requirement for fetal death to occur [17]. In the currently accepted second-hit hypothesis, a second trigger event (such as oral contraceptive use or surgical procedures), which may not be otherwise sufficient to cause thrombosis, is necessary for an asymptomatic apl-positive patient to develop thrombosis. Acquired (oral contraceptive use) and heritable thrombotic risk factors (deficiencies of protein C, protein S, or antithrombin III; mutations of factor V [A506G, factor V Leiden ], prothrombin [G20210A], or methylene tetrahydrofolate reductase [MTHFR C677T, hyperhomocysteinemia]) may increase risk of apl patients Clinical manifestations The clinical manifestations of apl represent a spectrum from asymptomatic to catastrophic APS (multiorgan thromboses). The principal manifestations of APS are venous/arterial thromboses and pregnancy losses. Stroke and transient ischemic attack are the most common presentation of arterial thrombosis whereas deep vein thrombosis, often accompanied by pulmonary embolism, is the most common venous manifestation of APS. Glomerular capillary endothelial cell injury or thrombosis of renal vessels (thrombotic microangiopathy) causes proteinuria without celluria or hypocomplementemia and may lead to severe hypertension and/or renal failure. Many patients have mild thrombocytopenia, livedo reticularis (a lattice like pattern of superficial skin veins), cardiac valve disease (vegetations, valve thickening and dysfunction), or other non-thrombotic manifestations described in several studies but not included in the revised Sapporo criteria [1] due to non-specificity or rarity. These manifestations by themselves do not classify a patient as having APS for clinical studies, but they add information to the diagnosis of individual patients. Some patients develop nonfocal neurologic symptoms such as lack of concentration, forgetfulness, and dizzy spells. Multiple small, hyperintense lesions seen on magnetic resonance imaging (MRI), primarily in the periventricular white matter, do not correlate well with clinical symptoms (Fig. 1) (further discussed in Section 3). Pregnancy losses in patients with apl typically occur after 10 weeks gestation (fetal loss), but early losses also occur (pre-embryonic or embryonic losses) [18]. Antiphospholipid syndrome patients may develop severe, early preeclampsia and HELLP (hemolysis, elevated liver enzymes, low platelets) syndrome. Catastrophic APS is a rare, abrupt, life-threatening complication. It consists of multiple thromboses of medium and small arteries occurring (despite apparently adequate anticoagulation) over a period of days, causing stroke, cardiac, hepatic, adrenal, renal, and intestinal infarction and peripheral gangrene [19] Diagnosis In the presence of characteristic clinical events, APS is diagnosed when patients have persistent apl that include moderate-to-high titer (>40 U) IgG and/or IgM acl, moderate-to-high titer IgG and/or IgM a 2 GPI, and/or positive lupus anticoagulant test [1].
4 96 D. Erkan et al. / Pathophysiology 18 (2011) Treatment Fig. 1. Periventricular hyperintense white matter lesions (magnetic resonance imaging). Lupus anticoagulant test is a functional coagulation assay that measures the ability of apl to inhibit the conversion of prothrombin to thrombin. Guidelines of the International Society on Thrombosis and Hemostasis [20] for diagnosis of LA require: (a) demonstration of a prolonged phospholipiddependent coagulation screening test such as activated partial thromboplastin time (aptt) or dilute Russell viper venom time (drvvt); (b) failure to correct the prolonged screening test by mixing the patient plasma with normal platelet poor plasma, demonstrating the presence of an inhibitor; (c) shortening or correction of the prolonged screening test by the addition of excess phospholipid, demonstrating phospholipid dependency; and (d) exclusion of other coagulopathies. A positive screening coagulation test without confirmatory steps is not a positive LA test. Interpretation of positive tests should take into account the following rules: moderate-to-high titer (>40 U) acl is more strongly associated with clinical events than is low titer; LA is a more specific but less sensitive predictor of thromboses than is Acl [21]; multiple positive apl tests impart a worse prognosis than does any single type of test; and positive apl tests require a repeat test after 12 weeks to exclude transient apl. Antiphospholipid antibody tests developed based on phosphatidylserine, phosphatidylinositol, phosphatidylethanolamine or prothrombin are not well standardized or widely accepted; their clinical and prognostic significance are unknown. Anticoagulation with unfractionated heparin or lowmolecular-weight heparin (LMWH) followed by warfarin is the treatment for APS patients with vascular events. Recent prospective controlled studies conclude that recurrence of thromboses in APS patients can be prevented with moderate intensity warfarin to an international normalized ratio (INR) of [22,23]. Although some APS patients with arterial event may require high intensity (INR 3 4) anticoagulation, in the absence of risk stratified studies the definition of high-risk is currently based on clinical judgment. Most apl-positive patients receive warfarin after ischemic strokes; however, the Antiphospholipid Antibody in Stroke Study (APASS) concluded that for selected apl-positive patients who have neither atrial fibrillation nor high-grade arterial stenosis, aspirin and warfarin therapy (at an INR of 2.2) are equivalent in both efficacy and major bleeding complications [24]. The generalizability of these results is limited as the study group had an average age of 60 years (much higher than the average for APS population), the apl determination was performed only once at the study entry, and the cut-off for assigning a patient to the positive acl group was very low. However, based on APASS results, aspirin is an option for patients with a single low positive apl test who present with stroke. Venous thrombosis in apl-positive patients has a high recurrence rate if anticoagulation is discontinued, and lifelong anticoagulation is usually recommended. It is unknown if patients whose event was triggered by an acquired and reversible thrombotic risk factor can discontinue anticoagulation or switch to aspirin when the trigger factor is eliminated. Normalization of the LA test or acl tests is not an indication to discontinue anticoagulation. Asymptomatic persons serendipitously found to have apl need no preventive therapy. Elimination of reversible thrombosis risk factors (smoking, oral contraceptives) and prophylaxis during high-risk periods (such as surgical interventions or prolonged immobilization) are advised for primary thrombosis prophylaxis in persistently apl-positive individuals. The effectiveness of low-dose aspirin in asymptomatic apl-positive patients has not been demonstrated by controlled studies [25]; high-risk patients determined based on the traditional cardiovascular disease risk factors can be candidates for low-dose prophylactic aspirin therapy. Estrogen and estrogen-containing oral contraceptives are deemed unsafe for APS patients or even for asymptomatic women serendipitously known to bear high-titer antibody. In pregnancy, LMWH and low-dose aspirin combination increases fetal survival rate from 50% to 80% among women who have had a fetal losses and who have unequivocally positive tests for apl. Prophylactic doses of LMWH for women who have had only pregnancy morbidity and full anticoagulant doses for women who have had prior thromboses are used. Treatment begins after confirmation of pregnancy, continues until 48 h before anticipated delivery (to allow epidural
5 D. Erkan et al. / Pathophysiology 18 (2011) anesthesia), and resumes for 8 12 weeks post-partum. No studies unequivocally justify treatment of young women with apl during a first pregnancy, women with only very early losses, or women whose apl titers are low or transient. Nonetheless, it is common to offer such patients low-dose aspirin. Very few studies address the pathogenesis and the treatment of the non-criteria manifestations of apl and currently, there is no evidence that anticoagulation is effective. There is no proven therapy for apl-positive patients with cognitive dysfunction; both mechanistic ( sle-apl-mri-cognitive-dysfunction.asp) and therapeutic (Clinical Trials.gov Identifier: NCT ) studies are underway. Experimental basic science studies (for statins and hydroxychloroquine) and retrospective/cross-sectional clinical studies (for hydroxychloroquine) suggest that these agents may be beneficial in preventing apl-mediated thrombosis [4]. Further controlled clinical trials are needed before recommending these agents in clinical practice; statins are contraindicated during pregnancy. Antiplatelet agents other than aspirin, long-term LMWH treatment, or direct/indirect thrombin inhibitors, empirically used, have not been formally tested in clinical trials. 3. Cognitive dysfunction and white matter abnormalities in antiphospholipid syndrome Cognitive dysfunction with or without white matter hyperintensities impairs quality of life and a better understanding of the nature and pathogenesis of cognitive dysfunction in apl-positive patients is critical to develop rational management approaches. However, only few studies of cognition or neuroimaging in primary APS have been conducted and most of the studies include lupus patients with apl. Similarly, there are relatively few studies of cognition or neuroimaging in the selected group of apl-negative SLE patients without neuropsychiatric syndromes. Furthermore, no studies have directly compared apl-positive patients without SLE with apl-negative SLE patients, and no studies have attempted to correlate the neuroimaging aspects (functional MRI and diffusion tensor imaging [DTI]) to cognitive function in these two patient groups simultaneously. Although, there have been no studies to date that have accurately identified the frequency of neuropsychiatric manifestations in APS, the trajectory of studies in SLE patients with or without apl provide excellent models for the classification of neuropsychiatric manifestations including cognitive dysfunction and neuroimaging abnormalities Cognitive dysfunction in antiphospholipid syndrome and lupus Cognitive difficulties are commonly reported in patients with autoimmune diseases and a better understanding of the nature and pathogenesis of this neurobehavioral manifestation is theoretically and clinically important. To date, SLE has been the most common autoimmune disorder studied, with almost half of these patients demonstrating major psychiatric and neurologic disorders [26]. Cognitive dysfunction is well documented in SLE [27 31] and has been recognized as one of 19 neuropsychiatric symptoms in the revised American College of Rheumatology Criteria for neuropsychiatric lupus [32]. Lupus patients with overt neuropsychiatric manifestations demonstrate severe cognitive and psychological abnormalities with prevalence rates up to 70% [27,31,33 35]. Evenin the absence of overt neuropsychiatric disease, cognitive dysfunction and psychological distress have been identified in 14 54% [36,37]. The most common deficits in SLE occur in attention, learning and recall, verbal and nonverbal fluency, complex psychomotor functions, visuospatial skills and motor dexterity. The presence of cognitive deficits among persons without other neuropsychiatric symptoms suggests the presence of a more subtle process adversely affecting the central nervous system in these SLE patients, and may be useful in our understanding of cognitive functions in APS. Maeshima et al. reported that 72% of 21 SLE patients with apl had abnormal neuropsychological findings in verbal learning and visuoconstructive skills [38]. Denburg et al. reported a significant association positive LA tests and cognitive impairment in patients with SLE [39]. They found LA-positive patients to score significantly lower than LAnegative patients on measures of verbal memory, cognitive flexibility, and psychomotor speed. The impairment was found to be quite significant; LA-positive patients were rated as two to three times more impaired than the LA-negative patients. The same group of investigators also investigated SLE patients who were consistently positive for LA (over three time periods) and reported that these patients had greater cognitive dysfunction than the patients who were persistently negative, a finding likely related to microvascular thrombosis in the LA-positive group [40]. Sanna et al. reported that apl, particularly positive LA test, was statistically more frequent (15.7%) in their SLE patients classified as having a cognitive disorder compared to the SLE patients without cognitive impairment (7.6%) [3]. Leritz et al. reported a significant difference between LA-positive SLE patients (n = 29) and LA-negative SLE patients (n = 27) on measures of attention and visuomotor sequencing [41]. Although these studies support than association between apl and cognitive dysfunction, there are also studies that have not found a relationship between apl and cognitive dysfunction [42 45]. Several studies in primary APS or in asymptomatic aplpositive patients have shown that cognitive deficits may be present independent of any history of known central nervous system involvement. These patients may complain of difficulty with memory, attention, and concentration; or the dysfunction may be subclinical and apparent only with neuropsychological testing. Hanly et al. reported that patients with persistently elevated IgG acl had a significant decline
6 98 D. Erkan et al. / Pathophysiology 18 (2011) in psychomotor speed, and persistently elevated IgA acl was related to decline in conceptual reasoning and executive ability [46]. Two studies have examined the cognitive function in primary APS patients compared to controls or other patient groups. Jacobson et al. examined neuropsychological functioning in 27 non-elderly patients with elevated levels (>10 IU) of acl IgG, but without concurrent history of autoimmune disease or any history or report of neurological events [47]. Compared with 27 age- and education-matched controls, there were group differences in domain scores of working memory, executive functions; verbal learning, and memory and visuospatial functioning. The overall frequency of impaired neuropsychological performance was greater among individuals with apl than controls (33% versus 4% respectively), suggesting subtle neurological involvement. Tektonidou et al. examined 39 patients with primary APS, 21 patients with SLE-related APS, and 60 healthy controls using a 3-h neuropsychological battery measuring attention, learning and memory, executive functions and visuospatial skills and depression [48]. In this study, the cut-off limits of apl ELISA positivity are not reported. Results indicated that 42% of the 60 patients with APS (combined primary and SLE-related APS) had cognitive deficits compared with 18% of healthy controls with deficits most common in complex attention and verbal fluency. There was no difference in cognitive performance between patients with primary APS and those with SLE-associated APS (although there was a significant association between cognitive dysfunction and white matter lesions further discussed below). Several studies have investigated the role of apl in relation to dementia or cognitive decline in the aging population. Using a screening tool and standard clinical criteria, one study reported that 56% of elderly APS patients had dementia based on diagnostic criteria [49] (APS patients with dementia were older with a mean age of 68 ± 3 compared to the non-demented APS patients with a mean age of 51 ± 4). Notably, the investigators did not perform standardized cognitive tests but relied on the standard psychiatric definition of dementia. Schmidt et al. found subtle neuropsychological dysfunction in otherwise normal elderly people with increased levels of IgG acl [50]. This correlation with acl IgG titers was significant despite the lack of evidence of any anatomic abnormalities on MRI. De Moorlose et al. evaluated the prevalence of acl in 192 elderly patients [51]; the overall prevalence of acl was 10.9% and decreased by decade in patients years of age from 18% to 10% to 7%, whereas the prevalence of antinuclear antibody (ANA) positivity increased by decade from 22% to 32% to 42%. There was no association between the presence of acl and decreased survival. In contrast, and in keeping with previous findings, Cesbron et al. found a trend towards an increased prevalence of acl by decade in 1042 elderly subjects between the ages of 60 and 99 years [52]. In addition, high acl levels were associated with increased physical disability in this population independent of age, gender, visual or hearing abnormalities, Mini-Mental Status Exam score, or history of cerebro- or cardiovascular disease. It is likely that cognitive dysfunction in these patients is due to multiple mechanisms. The underlying pathophysiology may relate to small vessel ischemic events, or there may be a direct pathogenic role of apl, which has implications in the treatment. Antiphospholipid antibodies may bind to the cells of the central nervous system [53] followed by permeabilization and depolarization of these cells [54]. Animal models corroborate that neuropsychiatric performance is affected by apl independently of the ischemic events [55 57]. In humans, an association has been demonstrated between cognitive dysfunction and both livedo reticularis and white matter lesions on MRI [48]. This finding is suggestive of a microangiopathic mechanism White matter abnormalities in antiphospholipid syndrome and lupus Although relatively few studies have been conducted, neuroimaging abnormalities have been reported in primary APS patients presenting with high levels of overt clinical neurological and psychiatric syndromes. Infarcts and hyperintense white matter foci are the most common abnormalities seen on computerized tomography and MRI in APS patients. However, most neuroimaging studies reported include patients with both APS and lupus. Gomez-Puerta et al. studied a combined lupus/aps group and reported cortical infarcts in 63% of patients, subcortical infarcts in 30%, basal ganglia infarcts in 23% and signs of cerebral atrophy in 37% [58]. Lampropoulos et al. studied 57 patients with APS and/or SLE who have neuropsychiatric symptoms (excluding stroke, epilepsy, or other encephalopathies) [59]. Fourteen patients had APS, 24 were positive for apl but no thrombosis, and 19 had SLE without apl. The frequency of abnormal EEG findings (primarily bitemporal slow activity) of the combined apl and APS groups was 82%, compared to 32% in the SLE group; there was an association between abnormal EEG findings and apl positivity (patients with abnormal EEG findings were more likely to report memory problems; however, no formal cognitive testing was applied). Chapman et al. reported that only half of their demented APS patients had abnormal CT scans and suggested that the demented APS patients with normal CT scans may have had micro-lesions or pathology (not necessarily vascular mediated) that may have been present had MRI or other neuroimaging techniques been used [49]. In contrast, eight of the non-demented subjects with APS showed diffuse slowing and EEG abnormalities. Of those with dementia, six had generalized atrophy and seven of the scans had focal lesions consistent with vascular pathology. Studies using more sophisticated scanning (MRI, DTI) and precise cognitive evaluation (standard neuropsychological testing versus global dementia classification) are new technologies now being studied as better ways to understand cognitive dysfunction in these diseases.
7 D. Erkan et al. / Pathophysiology 18 (2011) As a comparison to APS, neuroimaging abnormalities are also commonly reported in patients with SLE. Studies using cranial MRI reveal diffuse periventricular hyperintensities, infarcts, hemorrhage, cerebral atrophy and small focal lesions [60 64] with reversible and irreversible lesions [65]. Magnetic resonance imaging multiple small hyperintense white matter lesions do not unequivocally imply brain infarction. Jarek et al. reported that only 16% (5 out of 32) of non-npsle patients had MRI abnormalities [66]; subcortical white matter lesions and periventricular hyperintensities were reported most frequently without any evidence of cortical or periventricular atrophy. In a subsequent study by Kozora and Make 20 of the MRI studies previously used in the Jarek study were re-analyzed using quantitative techniques [61]. Cortical atrophy and increased white matter hyperintensities were found in over a third of these patients. In addition, the number of white matter hyperintensities was associated with cognition problems, particularly attention. Gonzalez-Crespo et al. also examined MRI abnormalities in 24 neuropsychiatric SLE patients, 20 non-neuropsychiatric SLE patients, and 10 normal controls similar in age and education [67]. Half of the patients in the non-neuropsychiatric SLE group had well-identified lesions which were described as multiple, small punctate areas of increased signal at periventricular or subcortical white matter of both cerebral hemispheres. A high percentage of the neuropsychiatric SLE group also demonstrated abnormalities, but no differences in number or location of lesions were noted when comparing white matter lesions across the two groups. Subsequent neuroimaging studies in SLE using magnetic resonance spectroscopy (MRS), DTI, and functional MRI (fmri) are under trial to identify the etiology and clinical significance of white matter lesions in this population. These findings may have implications for other autoimmune disorders such as APS. Some studies now suggest that neurometabolite changes associated with white matter damage in the brain may be important mechanisms of cognitive dysfunction in SLE (both non-neuropsychiatric SLE and neuropsychiatric SLE) [68]. In our recent study, increased choline was found in the normal appearing white matter of 60 non-neuropsychiatric SLE patients, and was significantly associated with cognitive dysfunction specific to areas of information processing and executive functioning [69]. Interestingly, no cerebral atrophy or white matter axonal damage was evident. These data confirm and extend our previous observations supporting the role of microstructural white matter changes in the cognitive impairment of nonneuropsychiatric SLE patients. The data also suggest that specific cognitive tests of attention and executive function may be sensitive to myelin damage that develops before axonal injury. In a DTI study in 34 SLE patients, only 59% (20 patients) showed abnormal MRI findings [70]. Atrophy was seen in 15% (3 patients) and non-specific white matter lesions in 75% (15 patients). Quantitative diffusion analysis showed increased diffusion globally, in frontal lobe, and in an internal capsule. Decreased diffusion anisotropy seen in corpus callosum. These diffusion findings were seen also in the patient group with normal MRIs suggesting the diffusion may be sensitive for early changes. Diffusion is known to be particularly sensitive for microstructural changes in white matter. Diffusion anisotropy has been used to assess white matter integrity in amyotrophic lateral scerosis [71] primary lateral sclerosis [72] and multiple sclerosis [73 76]. The changes in diffusion constant could be used in determining acute changes in both gray and white matter, for example in acute stroke. Only one study to date has used at DTI paradigm with APS with lower mean parenchyma diffusivity detected in 30 APS subjects compared to 49 controls. In addition to DTI paradigms, attentional/working memory functions have been examined in SLE patients utilizing fmri. Recently, DiFrancesco et al. examined 10 pediatric onset SLE patients (mean age 17.3 years) using several tasks including the N-back, a measure of working memory [77]. The pattern of abnormal fmri activity suggested that white matter connectivity was disrupted resulting in neuronal network dysfunction. In a recent study, Fitzgibbon et al. also examined working memory, attention and executive function using the N-back in 9 neuropsychiatric SLE patients compared to rheumatoid arthritis and healthy control subjects and report greater frontoparietal activation indicating abnormalities in these particular pathways [78]. Only one study of primary APS patients has investigated neuroimaging abnormalities in relation to cognitive dysfunction and reported a significant correlation between cognitive dysfunction and the presence of white matter lesions on MRI images in APS patients with and without CNS involvement [48]. White matter lesions were identified as ill-defined in hyperintensities on T2 weighted and proton density-fluidattenuated inversion recovery images without prominent hypointensity on T1-weighted images. The lesions were classified according to location (subcortical, periventricular and deep white matter changes) and graded according to size. In 23 APS patients with central nervous system involvement 12 (52%) of the patients had white matter lesions with 100% in the periventricular area primarily punctuate in size. Of the 36 APS patients without central nervous system involvement, 8 (22%) of the patients had white matter lesions with 88% in the periventricular location and primarily punctuate in size. A significant correlation was reported between cognitive deficits and white matter lesions across the two groups. Of the 8 APS patients without central nervous system involvement but white matter lesions, cognitive deficits were identified in 7 of the patients. 4. Conclusion Antiphospholipid syndrome is a systemic autoimmune systemic disease consisting of thromboses, pregnancy losses, and persistent high titer apl. Concomitant prothrombotic risk factors may increase risk for clotting. Differential diagnosis
8 100 D. Erkan et al. / Pathophysiology 18 (2011) is broad, especially in older patients; use of strict diagnostic criteria can help prevent overdiagnosis. Anticoagulation is the primary treatment today, but a future therapeutic approach will likely include immunomodulatory agents with or without antithrombotics. Relatively little is known about the cognitive pattern in these lupus and/or apl-positive patients, and very little information is available regarding specific white matter changes that we believe may be related to underlying attentional and executive cognitive impairment. We believe that understanding the mechanisms of cognitive impairment in lupus and/or apl-positive patients will facilitate early diagnosis and treatment; in addition studies with sophisticated neuroimaging techniques aimed to better understand white matter abnormalities will facilitate our understanding of cognitive dysfunction in APS. References [1] S. Miyakis, M.D. Lockshin, T. Atsumi, D.W. Branch, R.L. Brey, International consensus statement on an update of the classification criteria for definite antiphospholipid syndrome, J. Thromb. Haemost. 4 (2006) [2] W.A. Wilson, A.E. Gharavi, T. Koike, M.D. Lockshin, D.W. Branch, International consensus statement on preliminary classification criteria for definite antiphospholipid syndrome: report of an international workshop, Arthritis Rheum. 42 (1999) [3] G. Sanna, M.L. Bertolaccini, M.J. Cuadrado, H. Liang, M.A. Khamashta, Neuropsychiatric manifestations in systemic lupus erythematosus: prevalence and association with antiphospholipid antibodies, J. Rheumatol. 30 (2003) [4] D. Erkan, M.D. Lockshin, New approaches to the management of Antiphospholipid Syndrome, Nat. Clin. Pract. Rheumatol. 5 (2009) [5] D. Erkan, M.D. Lockshin, What is antiphospholipid syndrome? Curr. Rheumatol. Rep. 6 (2004) [6] A.E. Gharavi, S.S. Pierangeli, E.N. Harris, Origin of antiphospholipid antibodies, Rheum. Dis. Clin. North Am. 27 (2001) [7] M. Blank, I. Krause, M. Fridkin, N. Keller, J. Kopolovic, Bacterial induction of autoantibodies to beta2-glycoprotein-i accounts for the infectious etiology of antiphospholipid syndrome, J. Clin. Invest. 109 (2002) [8] A.E. Gharavi, L.R. Sammaritano, J. Wen, K.B. Elkon, Induction of antiphospholipid antibodies by immunization with beta 2 glycoprotein I (apolipoprotein H), J. Clin. Invest. 90 (1992) [9] M.I. Kamboh, S. Manzi, H. Mehdi, S. Fitzgeral, D.K. Sanghera, Genetic variation in apolipoprotein H (beta2-glycoprotein I) affects the occurrence of antiphospholipid antibodies and apolipoprotein H concentrations in systemic lupus erythematosus, Lupus 8 (1999) [10] L.F. Bancsi, I.K. Van der Linden, R.M. Bertina, B2-glycoprotein I deficiency and the risk of thrombosis, Thromb. Haemost. 67 (1992) [11] Y. Sheng, S.W. Reddel, H. Herzog, Y.X. Wang, T. Brighton, Impaired thrombin generation in beta 2-glycoprotein I null mice, J. Biol. Chem. 276 (2001) [12] J. Nojima, E. Suehisa, H. Kuratsune, T. Machii, T. Koike, Platelet activation induced by combined effects of anticardiolipin and lupus anticoagulant IgG antibodies in patients with systemic lupus erythematosus-possible association with thrombotic and thrombocytopenic complications, Thromb. Haemost. 81 (1999) [13] M.D. Smirnov, D.T. Triplett, P.C. Comp, N.L. Esmon, C.T. Esmon, On the role of phosphatidylethanolamine in the inhibition of activated protein C activity by antiphospholipid antibodies, J. Clin. Invest. 95 (1995) [14] J.H. Rand, X.X. Wu, S. Guller, H.A. Andree, C.J. Lockwood, Antiphospholipid immunoglobulin G antibodies reduce annexin-v levels on syncytiotrophoblast apical membranes and in culture media of placental villi, Am. J. Obstet. Gynecol. 177 (1997) [15] R.A. Roubey, New approaches to prevention of thrombosis in the antiphospholipid syndrome: hopes, trials, and tribulations, Arthritis Rheum. 48 (2003) [16] A. Potti, A. Bild, H.K. Dressman, D.A. Lewis, J.R. Nevins, Gene-expression patterns predict phenotypes of immune-mediated thrombosis, Blood 107 (2006) [17] G. Girardi, J. Berman, P. Redecha, L. Spruce, J.M. Thurman, Complement C5a receptors and neutrophils mediate fetal injury in the antiphospholipid syndrome, J. Clin. Invest. 112 (2003) [18] B.T. Oshiro, R.M. Silver, J.R. Scott, H. Yu, D.W. Branch, Antiphospholipid antibody and fetal death, Obstet. Gynecol. 87 (1996) [19] R.A. Asherson, R. Cervera, P. de Groot, D. Erkan, M.C. Boffa, Catastrophic Antiphospholipid Syndrome (CAPS): International Consensus Statement on Classification Criteria and Treatment Guidelines, Lupus 12 (2003) [20] J.T. Brandt, D.A. Triplett, B. Alving, I. Scharrer, Criteria for the diagnosis of lupus anticoagulants: an update, Thromb. Haemost. 74 (1995) [21] M. Galli, M. Luciani, G. Bertolini, T. Barbui, Lupus anticoagulants are stronger risk factors for thrombosis than anticardiolipin antibodies in the antiphospholipid syndrome: a systematic review of the literature, Blood 101 (2003) [22] M.A. Crowther, J.S. Ginsberg, J. Julian, J. Denburg, J. Hirsch, Comparison of two intensities of warfarin for the prevention of recurrent thrombosis in patients with the antiphospholipid antibody syndrome, N. Engl. J. Med. 349 (2003) [23] G. Finazzi, R. Marchioli, V. Brancaccio, P. Schinco, F. Wisloff, A randomized clinical trial of high-intensity warfarin vs. conventional antithrombotic therapy for the prevention of recurrent thrombosis in patients with the antiphospholipid syndrome (WAPS), J. Thromb. Haemost. 3 (2005) [24] S.R. Levine, R.L. Brey, B.C. Tilley, J.L. Thompson, R.L. Sacco, Antiphospholipid antibodies and subsequent thrombo-occlusive events in patients with ischemic stroke, JAMA 291 (2004) [25] D. Erkan, M.J. Harrison, R. Levy, R.M. Peterson, M. Petri, Aspirin for primary thrombosis prevention in the antiphospholipid syndrome: a randomized, double-blind, placebo-controlled trial in asymptomatic antiphospholipid antibody-positive individuals, Arthritis Rheum. 56 (2007) [26] S.G West, Neuropsychiatric lupus, Rheum. Dis. Clin. North Am. 20 (1994) [27] R.M. Carbotte, S.D. Denburg, J.A. Denburg, Prevalence of cognitive impairment in systemic lupus erythematosus, J. Nerv. Ment. Dis. 174 (1986) [28] J.G. Hanly, N.M. Walsh, J.D. Fisk, B. Eastwood, C. Hong, G. Sherwood, Cognitive impairment and autoantibodies in systemic lupus erythematosus, Br. J. Rheumatol. 32 (1993) [29] B.I. Glanz, D. Slonim, M.B. Urowitz, D.D. Gladman, J. Gough, Pattern of neuropsychologic dysfunction in inactive systemic lupus erythematosus, Neuropsychol. Behav. Neurol. 10 (1997) [30] K.S. Ginsburg, E.A. Wright, M.G. Larson, A.H. Fossel, M. Albert, A controlled study of the prevalence of cognitive dysfunction in randomly selected patients with systemic lupus erythematosus, Arthritis Rheum. 35 (1992) [31] S.D. Denburg, R.M. Carbotte, J.A. Denburg, Cognitive impairment in systemic lupus erythematosus: a neuropsychological study of individual and group deficits, J. Clin. Exp. Neuropsychol. 9 (1987) [32] The American College of Rheumatology Nomenclature and Case Definitions for Neuropsychiatric Lupus Syndromes, Arthritis Rheum. 42 (1999)
9 D. Erkan et al. / Pathophysiology 18 (2011) [33] E. Kozora, L.L. Thompson, C.M. Cullum, A pilot study evaluating neuropsychological and psychological status of patients with systemic lupus erythematosus (SLE), J. Clin. Exp. Neuropsychol. 13 (1991) [34] H. Stein, K. Walters, A. Dillon, M. Schulzer, Systemic lupus erythematosus a medical and social profile, J. Rheumatol. 13 (1986) [35] B.C. Sonies, J.H. Klippel, R.B. Gerber, C.H. Gerber, Cognitive performance in systemic lupus erythematosus, Arthritis Rheum. 25 (1982) S80 (abstract). [36] R.L. Brey, S.L. Holliday, A.R. Saklad, M.G. Navarrete, D. Hermosillo- Romo, Neuropsychiatric syndromes in lupus: prevalence using standardized definitions, Neurology 58 (2002) [37] E. Kozora, L.L. Thompson, S.G. West, B.L. Kotzin, Analysis of cognitive and psychological deficits in systemic lupus erythematosus patients without overt central nervous system disease, Arthritis Rheum. 39 (1996) [38] E. Maeshima, Y. Yamada, S. Yukawa, H. Nomoto, Higher cortical dysfunction, antiphospholipid antibodies, and neuroradiological examinations in systemic lupus erythematosus, Intern. Med. 31 (1992) [39] S.D. Denburg, R.M. Carbotte, J.A. Denburg, Psychological aspects of systemic lupus erythematosus: cognitive function, mood, and selfreport, J. Rheumatol. 24 (1997) [40] S.D. Denburg, Cognitive correlates of antiphospholipid antibody positivity in SLE, Arthritis Rheum. 36 (1993) S103 (abstract). [41] E. Leritz, J. Brandt, M. Minor, F. Reis-Jensen, M. Petri, Subcortical cognitive impairment in patients with systemic lupus erythematosus, J. Int. Neuropsychol. Soc. 6 (2000) [42] S. Carlomagno, S. Migliaresi, L. Ambrosone, M. Sannino, G. Sanges, Cognitive impairment in systemic lupus erythematosus: a follow-up study, J. Neurol. 247 (2000) [43] S.L. Holliday, G. Navarete, A. Escalante, A.R. Saklad, R.L. BreY, Demographic, symptomatic, and serologic predictors of cognitive function in systemic lupus erythematosus: preliminary results from SALUD, J. Int. Neuropsychol. Soc. 6 (2000) (abstract). [44] K. Waterloo, R. Omdal, G. Husby, S.I. Mellgren, Neuropsychological function in systemic lupus erythematosus: a five-year longitudinal study, Rheumatology (Oxford) 41 (2002) [45] K. Waterloo, R. Omdal, H. Sjoholm, W. Koldingsnes, E.A. Jacobsen, Neuropsychological dysfunction in systemic lupus erythematosus is not associated with changes in cerebral blood flow, J. Neurol. 248 (2001) [46] J.G. Hanly, K. Cassell, J.D. Fisk, Cognitive function in systemic lupus erythematosus: results of a 5-year prospective study, Arthritis Rheum. 40 (1997) [47] M.W. Jacobson, L.J. Rapport, P.A. Keenan, R.D. Coleman, G.E. Tietjen, Neuropsychological deficits associated with antiphospholipid antibodies, J. Clin. Exp. Neuropsychol. 21 (1999) [48] M.G. Tektonidou, N. Varsou, G. Kotoulas, A. Antoniou, H.M. Moutsopoulos, Cognitive deficits in patients with antiphospholipid syndrome: association with clinical, laboratory, and brain magnetic resonance imaging findings, Arch. Intern. Med. 166 (2006) [49] J. Chapman, M. Abu-Katash, R. Inzelberg, I. Yust, M.Y. Neufeld, N. Vardinon, Prevalence and clinical features of dementia associated with the antiphospholipid syndrome and circulating anticoagulants, J. Neurol. Sci. 203 (2002) [50] R. Schmidt, A. Auer-Grumbach, F. Fazekas, H. Offenbacher, P. Kapeller, Anticardiolipin antibodies in normal subjects: neuropsychological correlates and MRI findings, Stroke 26 (1995) [51] P. De Moorlose, F. Boehlen, G. Rebe, Prevalence of anticardiolipin and antinuclear antibodies in an elderly hospitalized population and mortality after a 6-year follow-up, Age Aging 26 (1997) (letter). [52] J.Y. Cesbron, P. Amouyel, E. Masy, Anticardiolipin antibodies and physical disability in elderly, Ann. Intern. Med. 126 (1997) 1003 (letter). [53] B. Caront, C. Calderaro, C. Alessandri, C. Conti, F.R. Tinghino, Serum anti-beta2-glycoprotein I antibodies from patients with antiphospholipid antibody syndrome bind central nervous system cells, J. Autoimmun. 11 (1998) [54] J. Chapman, M. Cohen-Armon, Y. Shoenfeld, A.D. Korczyn, Antiphospholipid antibodies permeabilize and depolarize brain synaptoneurosomes, Lupus 8 (1999) [55] A. Katzav, C.G. Pick, A.D. Korczyn, E. Oest, M. Blank, Y. Shoenfeld, J. Chapman, Hyperactivity in a mouse model of the antiphospholipid syndrome, Lupus 10 (2001) [56] L. Ziporen, Y. Shoenfeld, Y. Levy, A.D. Korczyn, Neurological dysfunction and hyperactive behavior associated with antiphospholipid antibodies. A mouse model, J. Clin. Invest. 100 (1997) [57] Y. Shoenfeld, A. Nahum, A.D. Korczyn, M. Dano, R. Rabinowitz, Neuronal-binding antibodies from patients with antiphospholipid syndrome induce cognitive deficits following intrathecal passive transfer, Lupus 12 (2003) [58] J.A. Gomez-Puerta, R. Cervera, L.M. Calvo, B. Gomez-Anson, G. Espinosa, Dementia associated with the antiphospholipid syndrome: clinical and radiological characteristics of 30 patients, Rheumatology (Oxford) 44 (2005) [59] C.E. Lampropoulos, M. Koutroumanidis, P.P. Reynolds, I. Manidakis, G.R. Hughes, Electroencephalography in the assessment of neuropsychiatric manifestations in antiphospholipid syndrome and systemic lupus erythematosus, Arthritis Rheum. 52 (2005) [60] A.M. Aisen, T.O. Gabrielsen, W.J. McCune, MR imaging of systemic lupus erythematosus involving the brain, Am. J. Roentgenol. 144 (1985) [61] E. Kozora, B. Make, Neuropsychological effects of rehabilitation in patients with chronic obstructive pulmonary disease (COPD): a pilot study, in: 1998 American Psychological Association Meeting, San Francisco, CA, [62] O. Ishikawa, K. Ohnishi, Y. Miyachi, H. Ishizaka, Cerebral lesions in systemic lupus erythematosus detected by magnetic resonance imaging. Relationship to anticardiolipin antibody, J. Rheumatol. 21 (1994) [63] R.A. Fields, W.L. Sibbitt, H. Toubbeh, A.D. Bankhurst, Neuropsychiatric lupus erythematosus, cerebral infarctions, and anticardiolipin antibodies, Ann. Rheum. Dis. 49 (1990) [64] C.A. Davie, A. Feinstein, L.D. Kartsounis, G.J. Barker, N.J. McHugh, Proton magnetic resonance spectroscopy of systemic lupus erythematosus involving the central nervous system, J. Neurol. 242 (1995) [65] W.L. Sibbitt, R.R. Sibbitt, W.M. Brooks, Neuroimaging in neuropsychiatric systemic lupus erythematosus, Arthritis Rheum. 42 (1999) [66] M.J. Jarek, S.G. West, M.R. Baker, K.M. Rak, Magnetic resonance imaging in systemic lupus erythematosus patients without a history of neuropsychiatric lupus erythematosus, Arthritis Rheum. 37 (1994) [67] M.R. Gonzalez-Crespo, F.J. Blanco, A. Ramos, E. Ciruelo, I. Mateo, M.A. Lopez-Pino, Magnetic resonance imaging of the brain in systemic lupus erythematosus, Br. J. Rheum. 34 (1995) [68] E. Kozora, D.B. Arciniegas, Brain abnormalities in SLE patients with cognitive impairment, Arthritis Rheum. 54 (2006) S273 (abstract). [69] C.M. Filley, E. Kozora, M.S. Brown, D.E. Miller, S. West, White matter microstructure and cognition in non-neuropsychiatric systemic lupus erythematosus, Cogn. Behav. Neurol. 22 (2009) [70] L. Zhang, M. Harrison, L.A. Heier, R.D. Zimmerman, L. Ravdin, Diffusion changes in patients with systemic lupus erythematosus, Magn. Reson. Imaging 25 (2007) [71] C.M. Ellis, A. Simmons, D.K. Jones, J. Bland, J.M. Dawson, Diffusion tensor MRI assesses corticospinal tract damage in ALS, Neurology 53 (1999) [72] A.M. Ulug, T. Grunewald, M.T. Lin, A.K. Kamal, C.G. Filippi, Diffusion tensor imaging in the diagnosis of primary lateral sclerosis, J. Magn. Reson. Imaging 19 (2004)
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Current View of the Treatment of Antiphospholipid Syndrome
 GROUPE HOSPITALIER PITIE SALPETRIERE Current View of the Treatment of Antiphospholipid Syndrome Pr Zahir AMOURA Department of Internal Medicine French National Reference center for SLE and APS Hôpital
GROUPE HOSPITALIER PITIE SALPETRIERE Current View of the Treatment of Antiphospholipid Syndrome Pr Zahir AMOURA Department of Internal Medicine French National Reference center for SLE and APS Hôpital
ORIGINAL INVESTIGATION. Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings
 ORIGINAL INVESTIGATION Cognitive Deficits in Patients With Antiphospholipid Syndrome Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings Maria G. Tektonidou, MD; Natassa
ORIGINAL INVESTIGATION Cognitive Deficits in Patients With Antiphospholipid Syndrome Association With Clinical, Laboratory, and Brain Magnetic Resonance Imaging Findings Maria G. Tektonidou, MD; Natassa
Rituximab. B Cell Inhibition in APS. Methods. B Cell Inhibition in APS. Disclosure 11/6/2011
 Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Rituximab in Antiphospholipid Syndrome (RITAPS) A Pilot Open-Label Phase II Prospective Trial for Non-Criteria Manifestations of Antiphospholipid Antibodies (NCT: 00537290) Disclosure Research Support:
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Thrombophilia. Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS
 Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Autoimmune Thrombophilia Dr. A Sarrafnejad PhD Dep. Immunology School of public health TUMS Saraf@sina.tums.ac.ir Acquired Thrombophilia HIT PNH Cyckle cell Anemia Myeloproliferative lf Diseases Thrombocytosis
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Lupus Anticoagulants (LA), Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update. Antiphospholipid. Antiphospholipid
 , Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
, Antiphospholipid (APL) Antibodies & APL Syndrome: Review & Update William L. Nichols, MD Mayo Clinic College of Medicine Rochester, Minnesota USA Disclosures & Objectives (Nichols) Disclosures Relevant
Key words: antiphospholipid syndrome, trombosis, pathogenesis
 26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
Situaciones estresantes en el lupus
 Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Antiphospholipid Syndrome ( APS)
 Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Antiphospholipid Syndrome ( APS) Edward John Walter Bowie, MD Mayo Medical School the first to identify APS as an acquired thrombophilia Graham Robert Vivian Hughes MD FRCP Unit Rayne Institute St Thomas
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
The Antiphospholipid Syndrome
 The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
The Antiphospholipid Syndrome 1 / 6 2 / 6 3 / 6 The Antiphospholipid Syndrome Antiphospholipid antibody syndrome (commonly called antiphospholipid syndrome or APS) is an autoimmune disease present mostly
Daniel Egan, MD April 13, 2012
 Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Daniel Egan, MD April 13, 2012 Aug 2006 (at age 15): Acute unprovoked DVT in left common femoral vein Factor V Leiden heterozygous Positive lupus inhibitor Lovenox BID 2 weeks later: increased clot burden,
Prevalence of antiphospholipid auto antibodies in patients with thrombosis
 EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
EUROPEAN ACADEMIC RESEARCH Vol. IV, Issue 6/ September 2016 ISSN 2286-4822 www.euacademic.org Impact Factor: 3.4546 (UIF) DRJI Value: 5.9 (B+) Prevalence of antiphospholipid auto antibodies in patients
AN INTERESTING CASE OF RESPIRATORY DISTRESS. Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai
 AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
AN INTERESTING CASE OF RESPIRATORY DISTRESS Dr.V.Akila Devi DNB PG Southern Railway Headquarters Hospital Chennai 11 month old female infant 1 st born to parents of NC marriage referred from Kolkatta H/O:
A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating Prophylaxis after Deep Vein Thrombosis- Pulmonary Embolism
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.6.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:274-278 A Case of Antiphospholipid Syndrome Refractory to Secondary Anticoagulating
Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome
 Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Turk J Hematol 2007; 24:69-74 Turkish Society of Hematology RESEARCH ARTICLE Lupus anticoagulant and anticardiolipin antibodies in SLE with secondary Antiphospholipid Antibody Syndrome Shveta Garg, Annamma
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Antiphospholipid antibodies
 CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
CARDIOLOGY PATIENT PAGE CARDIOLOGY PATIENT PAGE Antiphospholipid Antibodies Caron P. Misita, PharmD; Stephan Moll, MD Antiphospholipid antibodies (APLAs) are proteins that may be present in the blood and
Mortality in the Catastrophic Antiphospholipid Syndrome
 ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
ARTHRITIS & RHEUMATISM Vol. 54, No. 8, August 2006, pp 2568 2576 DOI 10.1002/art.22018 2006, American College of Rheumatology Mortality in the Catastrophic Antiphospholipid Syndrome Causes of Death and
T he antiphospholipid syndrome (APS) is a thrombophilic
 1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
1639 EXTENDED REPORT ntiphospholipid antibody tests: spreading the net M L ertolaccini, S Gomez, J F P Pareja, Theodoridou, G Sanna, G R V Hughes, M Khamashta... See end of article for authors affiliations...
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist
 Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Antiphospholipid Antibody Syndrome: Management Issues for the Hematologist Wisconsin Institute of Discovery Karen Rossi/Bristol-Myers Squibb Morey A. Blinder, MD Washington University, St. Louis, MO March
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
Summary of the 11th International Congress on Antiphospholipid Antibodies, Sydney, Australia, November 2004
 Journal of Reproductive Immunology 66 (2005) 85 90 Meeting report Summary of the 11th International Congress on Antiphospholipid Antibodies, Sydney, Australia, November 2004 The 11th International Congress
Journal of Reproductive Immunology 66 (2005) 85 90 Meeting report Summary of the 11th International Congress on Antiphospholipid Antibodies, Sydney, Australia, November 2004 The 11th International Congress
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Mohammadreza Tabatabaei IBTO COAG LAB
 Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Thrombophilia: To test or not to test
 Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Disclosures. Sneddon Syndrome: Untangling the Web. Case Presentation. MRI head w/ and w/o contrast. Further Workup. Further Workup 10/26/2017
 Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Sneddon Syndrome: Untangling the Web Sadhana Murali, MD, PGY-4 University of Wisconsin-Madison WNS Conference October 27-28, 2017 Disclosures I have no relevant financial relationships with any commercial
Thrombophilia. Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC. GASCO Atlanta Sept 8 th, Disclosures. Conflicts of interest: NONE
 LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
Antiphospholipid Antibody Testing: Which Are Most Useful for Diagnosis?
 Rheum Dis Clin N Am 32 (2006) 455 463 Antiphospholipid Antibody Testing: Which Are Most Useful for Diagnosis? Maria Laura Bertolaccini, MD, PhD*, Graham R.V. Hughes, MD, FRCP Lupus Research Unit, The Rayne
Rheum Dis Clin N Am 32 (2006) 455 463 Antiphospholipid Antibody Testing: Which Are Most Useful for Diagnosis? Maria Laura Bertolaccini, MD, PhD*, Graham R.V. Hughes, MD, FRCP Lupus Research Unit, The Rayne
10/24/2013. Heparin-Induced Thrombocytopenia (HIT) Anticoagulation Management in ECMO Therapy:
 Anticoagulation Management in ECMO Therapy: Heparin-Induced (HIT) Michael H. Creer, MD Professor of Pathology Director, Clinical Laboratories, Medical Co- Director, Hematopathology and Chief, Division
Anticoagulation Management in ECMO Therapy: Heparin-Induced (HIT) Michael H. Creer, MD Professor of Pathology Director, Clinical Laboratories, Medical Co- Director, Hematopathology and Chief, Division
All about Antiphospholipid Syndrome. M.B. Agarwal, MD Prof & Head, Dept of Haematology, Bombay Hospital Institute of Medical Sciences, Mumbai, India
 All about Antiphospholipid Syndrome M.B. Agarwal, MD Prof & Head, Dept of Haematology, Bombay Hospital Institute of Medical Sciences, Mumbai, India 1 2 3 4 5 6 Antiphospholipid syndrome A study of 192
All about Antiphospholipid Syndrome M.B. Agarwal, MD Prof & Head, Dept of Haematology, Bombay Hospital Institute of Medical Sciences, Mumbai, India 1 2 3 4 5 6 Antiphospholipid syndrome A study of 192
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Clinical consequences of antiphospholipid antibodies
 Clinical consequences of antiphospholipid antibodies R.H.W.M. Derksen 1*, P.G. de Groot 2,3 1 Department of Rheumatology and Clinical Immunology, Room F02.127, 2 Thrombosis and Haemostasis Laboratory,
Clinical consequences of antiphospholipid antibodies R.H.W.M. Derksen 1*, P.G. de Groot 2,3 1 Department of Rheumatology and Clinical Immunology, Room F02.127, 2 Thrombosis and Haemostasis Laboratory,
Antiphospholipid Syndrome
 Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
Antiphospholipid Syndrome EliA Cardiolipin and EliA β2-glycoprotein I Fully Automated Testing for Antiphospholipid Syndrome (APS) Testing for APS according to classification criteria determination of anti-β2-glycoprotein
CEREBRO VASCULAR ACCIDENTS
 CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
Arterial Ischemic Stroke with Protein S Deficiency in Pakistan
 Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
Anaesthesiologic management of a parturient with a known antiphospholipid syndrome
 Anaesthesiologic management of a parturient with a known antiphospholipid syndrome Pascal Vuilleumier Universitätsklinik für Anästhesie und Schmerztherapie Case presentation: Mrs A. B. 1975 Early monday
Anaesthesiologic management of a parturient with a known antiphospholipid syndrome Pascal Vuilleumier Universitätsklinik für Anästhesie und Schmerztherapie Case presentation: Mrs A. B. 1975 Early monday
HEPARIN-INDUCED THROMBOCYTOPENIA (HIT)
 HEPARIN-INDUCED THROMBOCYTOPENIA (HIT) OBJECTIVE: To assist clinicians with the investigation and management of suspected and documented heparin-induced thrombocytopenia (HIT). BACKGROUND: HIT is a transient,
HEPARIN-INDUCED THROMBOCYTOPENIA (HIT) OBJECTIVE: To assist clinicians with the investigation and management of suspected and documented heparin-induced thrombocytopenia (HIT). BACKGROUND: HIT is a transient,
Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome
 Original Article Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome Paula Gonçalves Perches¹, Daniela Pezzutti Domingues¹, Andréia Latanza Gomes², Augusta
Original Article Evaluation of antiphospholipid antibodies testing for the diagnosis of antiphospholipid syndrome Paula Gonçalves Perches¹, Daniela Pezzutti Domingues¹, Andréia Latanza Gomes², Augusta
Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study
 Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Asian Pacific Journal of Allergy and Immunology ORIGINAL ARTICLE Clinical and immunological characteristics of antiphospholipid syndrome in an Asian population: a retrospective study Kanon Jatuworapruk,
Catastrophic antiphospholipid syndrome: how to diagnose a rare but highly fatal disease
 502919TAB5610.1177/1759720X13502919Therapeutic Advances in Musculoskeletal DiseaseCL Aguiar and D Erkan 2013502919 Therapeutic Advances in Musculoskeletal Disease Review Catastrophic antiphospholipid syndrome:
502919TAB5610.1177/1759720X13502919Therapeutic Advances in Musculoskeletal DiseaseCL Aguiar and D Erkan 2013502919 Therapeutic Advances in Musculoskeletal Disease Review Catastrophic antiphospholipid syndrome:
ANTIPHOSPHOLIPID ANTIBODIES
 CLINICAL REVIEW CLINICIAN S CORNER Management of Antiphospholipid Antibody Syndrome A Systematic Review Wendy Lim, MD Mark A. Crowther, MD John W. Eikelboom, MBBS ANTIPHOSPHOLIPID ANTIBODIES were first
CLINICAL REVIEW CLINICIAN S CORNER Management of Antiphospholipid Antibody Syndrome A Systematic Review Wendy Lim, MD Mark A. Crowther, MD John W. Eikelboom, MBBS ANTIPHOSPHOLIPID ANTIBODIES were first
THROMBOPHILIA SCREENING
 THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
ORIGINAL PAPERS. Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F. Abstract
 ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
ORIGINAL PAPERS Adv Clin Exp Med 2014, 23, 5, 729 733 ISSN 1899 5276 Copyright by Wroclaw Medical University Marek Cieśla 1, B D, Ewa Wypasek 1, 2, B D 1, 2, A, E, F, Anetta Undas IgA Antiphospholipid
Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time
 Clin. Lab. 2009;55:XXX-XXX Copyright ORIGINAL ARTICLE Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time HORATIU OLTEANU 2, KATHARINE. A. DOWNES 1, JIGAR
Clin. Lab. 2009;55:XXX-XXX Copyright ORIGINAL ARTICLE Warfarin Does Not Interfere with Lupus Anticoagulant Detection by Dilute Russell s Viper Venom Time HORATIU OLTEANU 2, KATHARINE. A. DOWNES 1, JIGAR
Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome
 Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome L. Stojanovich 1, M. Kontic 2, D. Smiljanic 3, A. Djokovic 1, B. Stamenkovic 4 D. Marisavljevic
Association between non-thrombotic neurological and cardiac manifestations in patients with antiphospholipid syndrome L. Stojanovich 1, M. Kontic 2, D. Smiljanic 3, A. Djokovic 1, B. Stamenkovic 4 D. Marisavljevic
Patient with Musculo-skeletal Complaints - Summary
 Patient with Musculo-skeletal Complaints - Summary 1. Soft Tissue Rheumatism or Arthritis 2. Arthritis Monoarticular Polyarticular - :- (Asymmetrical) (Symetrical) :- -Crystals, Gout - Infective acute
Patient with Musculo-skeletal Complaints - Summary 1. Soft Tissue Rheumatism or Arthritis 2. Arthritis Monoarticular Polyarticular - :- (Asymmetrical) (Symetrical) :- -Crystals, Gout - Infective acute
Mabel Labrada, MD Miami VA Medical Center
 Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Mabel Labrada, MD Miami VA Medical Center *1-Treatment for acute DVT with underlying malignancy is for 3 months. *2-Treatment of provoked acute proximal DVT can be stopped after 3months of treatment and
Central nervous system involvement in the antiphospholipid (Hughes) syndrome
 Rheumatology 2003;42:200 213 doi:10.1093/rheumatology/keg080, available online at www.rheumatology.oupjournals.org Review Central nervous system involvement in the antiphospholipid (Hughes) syndrome G.
Rheumatology 2003;42:200 213 doi:10.1093/rheumatology/keg080, available online at www.rheumatology.oupjournals.org Review Central nervous system involvement in the antiphospholipid (Hughes) syndrome G.
PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE
 Autoimmune Disorders in Gynecology/Obstetrics PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE Abstract The spectrum
Autoimmune Disorders in Gynecology/Obstetrics PD Dr. med. habil. Michaela Jaksch, Consultant Laboratory Medicine, Medical Director, Freiburg Medical Laboratory ME LLC, Dubai, UAE Abstract The spectrum
Sang Hyuk Park, 1,2 Seongsoo Jang, 3 Chan-Jeoung Park, 3 and Hyun-Sook Chi Introduction
 BioMed Research International Volume 2016, Article ID 2641526, 6 pages http://dx.doi.org/10.1155/2016/2641526 Research Article Clinical Application of Revised Laboratory Classification Criteria for Antiphospholipid
BioMed Research International Volume 2016, Article ID 2641526, 6 pages http://dx.doi.org/10.1155/2016/2641526 Research Article Clinical Application of Revised Laboratory Classification Criteria for Antiphospholipid
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
The antiphospholipid syndrome: still an enigma
 CHALLENGING SCENARIOS IN THROMBOSIS The antiphospholipid syndrome: still an enigma Shruti Chaturvedi 1 and Keith R. McCrae 2 1 Division of Hematology, Vanderbilt University Medical Center, Nashville, TN;
CHALLENGING SCENARIOS IN THROMBOSIS The antiphospholipid syndrome: still an enigma Shruti Chaturvedi 1 and Keith R. McCrae 2 1 Division of Hematology, Vanderbilt University Medical Center, Nashville, TN;
Thyroid disease and haemostasis: a relationship with clinical implications? Squizzato, A.
 UvA-DARE (Digital Academic Repository) Thyroid disease and haemostasis: a relationship with clinical implications? Squizzato, A. Link to publication Citation for published version (APA): Squizzato, A.
UvA-DARE (Digital Academic Repository) Thyroid disease and haemostasis: a relationship with clinical implications? Squizzato, A. Link to publication Citation for published version (APA): Squizzato, A.
TECHNICAL SERIES. Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss. ...Setting trends TULIP DIAGNOSTICS (P) LTD.
 For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
For the use of Registered Medical Practioners and Laboratories only TECHNICAL SERIES Lupus Anticoagulants: Basic Concepts and Laboratory Diagnosiss TULIP DIAGNOSTICS (P) LTD. Gitanjali, Tulip Block, Dr.
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
Review Article. Catastrophic Antiphospholipid Syndrome. Introduction. Etiopathogenesis. Man-Chi Leung and Woon-Leung Ng
 Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Review Article Catastrophic Antiphospholipid Syndrome Man-Chi Leung and Woon-Leung Ng Abstract: Keywords: The catastrophic antiphospholipid syndrome is a potentially life threatening rheumatological condition
Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수
 Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수 Thrombophilia A hereditary or acquired disorder predisposing to thrombosis Questions Why should we test? Who should we test For what disorders?
Genetic Tests for the Better Outcome of VTE? 서울대학교병원혈액종양내과윤성수 Thrombophilia A hereditary or acquired disorder predisposing to thrombosis Questions Why should we test? Who should we test For what disorders?
Antiphospholipid antibody syndrome an overview
 Antiphospholipid antibody syndrome an overview C Sridevi, DNB (Medicine) DNB (Cardiology) MNAMS* P Krishnam Raju, MD DM (Cardiology)* INTRODUCTION Antiphospholipid antibody syndrome (APLAS) was first described
Antiphospholipid antibody syndrome an overview C Sridevi, DNB (Medicine) DNB (Cardiology) MNAMS* P Krishnam Raju, MD DM (Cardiology)* INTRODUCTION Antiphospholipid antibody syndrome (APLAS) was first described
Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus
 J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid Antibody
 Journal of Rheumatic Diseases Vol. 22, No. 2, April, 2015 http://dx.doi.org/10.4078/jrd.2015.22.2.106 Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid
Journal of Rheumatic Diseases Vol. 22, No. 2, April, 2015 http://dx.doi.org/10.4078/jrd.2015.22.2.106 Case Report A Case of Massive Pulmonary Embolism in Systemic Lupus Erythematosus without Antiphospholipid
Hemostasis. PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures
 Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
DWI assessment of ischemic changes in the fetal brain
 DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
Interactive Case Vignette: DOACs (Direct Oral Anti-Coagulants) vs. Warfarin for APLA (Anti-Phospholipid Antibody Syndrome)
 Interactive Case Vignette: DOACs (Direct Oral Anti-Coagulants) vs. Warfarin for APLA (Anti-Phospholipid Antibody Syndrome) Ara Metjian, MD Duke Debates Benign Hematologic Highlights April 22, 2017 Disclaimer
Interactive Case Vignette: DOACs (Direct Oral Anti-Coagulants) vs. Warfarin for APLA (Anti-Phospholipid Antibody Syndrome) Ara Metjian, MD Duke Debates Benign Hematologic Highlights April 22, 2017 Disclaimer
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients. David Liff MD Oklahoma Heart Institute Vascular Center
 DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
DVT Pathophysiology and Prophylaxis in Medically Hospitalized Patients David Liff MD Oklahoma Heart Institute Vascular Center Overview Pathophysiology of DVT Epidemiology and risk factors for DVT in the
Supplemental Figures and Legends
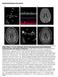 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Approach to Thrombosis
 Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
Approach to Thrombosis Theera Ruchutrakool, M.D. Division of Hematology Department of Medicine Siriraj Hospital Faculty of Medicine Mahidol University Approach to Thrombosis Thrombosis: thrombus formation
PROGNOSIS AND SURVIVAL
 CANCER ASSOCIATED THROMBOSIS PROGNOSIS AND SURVIVAL Since French internist Armand Trousseau reported the occurrence of mysterious thrombotic disorders in cancer patients in the mid-19th century, the link
CANCER ASSOCIATED THROMBOSIS PROGNOSIS AND SURVIVAL Since French internist Armand Trousseau reported the occurrence of mysterious thrombotic disorders in cancer patients in the mid-19th century, the link
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience
 Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
THROMBOSIS PRODUCT HIGHLIGHTS
 PRODUCT HIGHLIGHTS AESKU.DIAGNOSTICS has extensive experience and know-how in the Anti-Phospholipid Syndrome (APS) field and offers the most comprehensive panel of anti-phospholipid tests, employing highly
PRODUCT HIGHLIGHTS AESKU.DIAGNOSTICS has extensive experience and know-how in the Anti-Phospholipid Syndrome (APS) field and offers the most comprehensive panel of anti-phospholipid tests, employing highly
REVIEW ARTICLE. Antiphospholipid syndrome
 REVIEW ARTICLE 336 Antiphospholipid syndrome Sanjay C Keswani BSc MRCP Naresh Chauhan MRCP 1 J R Soc Med 2002;95:336 342 The antiphospholipid syndrome (APS) is characterized by thrombosis, recurrent fetal
REVIEW ARTICLE 336 Antiphospholipid syndrome Sanjay C Keswani BSc MRCP Naresh Chauhan MRCP 1 J R Soc Med 2002;95:336 342 The antiphospholipid syndrome (APS) is characterized by thrombosis, recurrent fetal
DOACs in SPECIAL POPULATIONS
 DOACs in SPECIAL POPULATIONS Ann K Wittkowsky PharmD, CACP, FASHP, FCCP Clinical Professor University of Washington School of Pharmacy Director, Anticoagulation Services UWMedicine Department of Pharmacy
DOACs in SPECIAL POPULATIONS Ann K Wittkowsky PharmD, CACP, FASHP, FCCP Clinical Professor University of Washington School of Pharmacy Director, Anticoagulation Services UWMedicine Department of Pharmacy
Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu VK*; Singh H
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 4 ISSN 2379-1039 Catastrophic antiphospholipid syndrome: A rare but serious complication of antiphospholipid antibody syndrome Sandhu
Primary Care practice clinics within the Edmonton Southside Primary Care Network.
 INR Monitoring and Warfarin Dose Adjustment Last Review: November 2016 Intervention(s) and/or Procedure: Registered Nurses (RNs) adjust warfarin dosage according to individual patient International Normalized
INR Monitoring and Warfarin Dose Adjustment Last Review: November 2016 Intervention(s) and/or Procedure: Registered Nurses (RNs) adjust warfarin dosage according to individual patient International Normalized
Dental Management Considerations for Patients on Antithrombotic Therapy
 Dental Management Considerations for Patients on Antithrombotic Therapy Warfarin and Antiplatelet Joel J. Napeñas DDS FDSRCS(Ed) Program Director General Practice Residency Program Department of Oral Medicine
Dental Management Considerations for Patients on Antithrombotic Therapy Warfarin and Antiplatelet Joel J. Napeñas DDS FDSRCS(Ed) Program Director General Practice Residency Program Department of Oral Medicine
Chapter 1 Introduction
 Chapter 1 Introduction There are several disorders which carry an increased risk of thrombosis, clots that interfere with normal circulation, including: venous thromboembolism (VTE), comprising both deep
Chapter 1 Introduction There are several disorders which carry an increased risk of thrombosis, clots that interfere with normal circulation, including: venous thromboembolism (VTE), comprising both deep
Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome
 ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
ARD Online First, published on March 18, 2005 as 10.1136/ard.2004.032813 1 Close Association between valvular heart disease and central nervous system manifestations in the antiphospholipid syndrome Category:
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Available Online at CODEN: IJRSFP (USA) Vol. 9, Issue, 3(L), pp , March, 2018.
 ISSN: 0976-3031 Available Online at http://www.recentscientific.com CODEN: IJRSFP (USA) International Journal of Recent Scientific Research Vol. 9, Issue, 3(L), pp. 25504-25508, March, 2018 Research Article
ISSN: 0976-3031 Available Online at http://www.recentscientific.com CODEN: IJRSFP (USA) International Journal of Recent Scientific Research Vol. 9, Issue, 3(L), pp. 25504-25508, March, 2018 Research Article
Updates in Diagnosis & Management of VTE
 Updates in Diagnosis & Management of VTE TRACY MINICHIELLO, MD CHIEF, ANTICOAGULATION& THROMBOSIS SERVICE-SAN FRANCISCO VAMC PROFESSOR OF MEDICINE UNIVERSITY OF CALIFORNIA, SAN FRANCISCO Financial Disclosures-NONE
Updates in Diagnosis & Management of VTE TRACY MINICHIELLO, MD CHIEF, ANTICOAGULATION& THROMBOSIS SERVICE-SAN FRANCISCO VAMC PROFESSOR OF MEDICINE UNIVERSITY OF CALIFORNIA, SAN FRANCISCO Financial Disclosures-NONE
Keywords: apl, Hughes syndrome, pregnancy loss, prothrombin, thrombosis. Introduction
 Journal of Thrombosis and Haemostasis, 10: 2512 2518 DOI: 10.1111/jth.12014 ORIGINAL ARTICLE Clinical accuracy for diagnosis of antiphospholipid syndrome in systemic lupus erythematosus: evaluation of
Journal of Thrombosis and Haemostasis, 10: 2512 2518 DOI: 10.1111/jth.12014 ORIGINAL ARTICLE Clinical accuracy for diagnosis of antiphospholipid syndrome in systemic lupus erythematosus: evaluation of
Thrombosis and emboli. Peter Nagy
 Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Thrombosis and emboli Peter Nagy A thrombus is any solid object developing from the blood in vivo within the vascular system or heart. Thrombosis is hemostasis in the wrong place. Major components, forms:
Menopausal Hormone Therapy & Haemostasis
 Menopausal Hormone Therapy & Haemostasis The Haematologist Perspective Dr. Batia Roth-Yelinek Coagulation unit Hadassah MC Menopausal Hormone Therapy & Hemostasis Hemostatic mechanism Mechanism of estrogen
Menopausal Hormone Therapy & Haemostasis The Haematologist Perspective Dr. Batia Roth-Yelinek Coagulation unit Hadassah MC Menopausal Hormone Therapy & Hemostasis Hemostatic mechanism Mechanism of estrogen
FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK
 07 June, 2018 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK Document Filetype: PDF 365.11 KB 0 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK I recently had a MRI last week with
07 June, 2018 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK Document Filetype: PDF 365.11 KB 0 FILE / PERIVENTRICULAR MICROVASCULAR ISCHEMIC CHANGES EBOOK I recently had a MRI last week with
Antiphospholipid antibodies and thrombosis: strength of association
 (2003) 4, 180 186 & 2003 The European Hematology Association All rights reserved 1466-4680/03 $25.00 www.nature.com/thj REVIEW Antiphospholipid antibodies and thrombosis: strength of association Monica
(2003) 4, 180 186 & 2003 The European Hematology Association All rights reserved 1466-4680/03 $25.00 www.nature.com/thj REVIEW Antiphospholipid antibodies and thrombosis: strength of association Monica
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
DEBATE: PFO MANAGEMENT TO CLOSE OR NOT TO CLOSE. Matthew Starr, MD Stroke Attending
 DEBATE: PFO MANAGEMENT TO CLOSE OR NOT TO CLOSE Matthew Starr, MD Stroke Attending DISCLOSURES None DEBATE Should PFO be closed? * * Sometimes yes THE CASE AGAINST PFO CLOSURE 1. Did the PFO cause the
DEBATE: PFO MANAGEMENT TO CLOSE OR NOT TO CLOSE Matthew Starr, MD Stroke Attending DISCLOSURES None DEBATE Should PFO be closed? * * Sometimes yes THE CASE AGAINST PFO CLOSURE 1. Did the PFO cause the
Antiphospholipid syndrome: treatment controversies
 REVIEW Antiphospholipid syndrome: treatment controversies Guillermo Ruiz- Irastorza & Munther A Khamashta Author for correspondence St Thomas Hospital, Lupus Research Unit, The Rayne Institute, London,
REVIEW Antiphospholipid syndrome: treatment controversies Guillermo Ruiz- Irastorza & Munther A Khamashta Author for correspondence St Thomas Hospital, Lupus Research Unit, The Rayne Institute, London,
Schematic Of Heparin Induced Thrombocytopenia Platelet Count
 Schematic Of Heparin Induced Thrombocytopenia Platelet Count Normal IgG and IgG2 differentially inhibit HIT antibody-dependent platelet activation that platelet counts were lower in FcγRIIA 131RR patients
Schematic Of Heparin Induced Thrombocytopenia Platelet Count Normal IgG and IgG2 differentially inhibit HIT antibody-dependent platelet activation that platelet counts were lower in FcγRIIA 131RR patients
The Perioperative Management of Heparin Induced Thrombocytopenia. Chaitan K. Narsule, M.D. March 5, 2008
 The Perioperative Management of Heparin Induced Thrombocytopenia Chaitan K. Narsule, M.D. March 5, 2008 Overview Case Presentation Incidence of HIT Pathophysiology Clinical Presentation Laboratory Diagnosis
The Perioperative Management of Heparin Induced Thrombocytopenia Chaitan K. Narsule, M.D. March 5, 2008 Overview Case Presentation Incidence of HIT Pathophysiology Clinical Presentation Laboratory Diagnosis
Life Science Journal 2016;13(11) Predictors of MRI Brain Changes in Systemic Lupus Erythematosus Patients
 Predictors of MRI Brain Changes in Systemic Lupus Erythematosus Patients Yasser El Miedany 1, Sami M Bahlas 2, Yasser M Bawazir 3, Ibtisam M Jali 4 1 Honorary senior clinical lecturer, King's college London,
Predictors of MRI Brain Changes in Systemic Lupus Erythematosus Patients Yasser El Miedany 1, Sami M Bahlas 2, Yasser M Bawazir 3, Ibtisam M Jali 4 1 Honorary senior clinical lecturer, King's college London,
Guidelines. 704 q 2000 Blackwell Science Ltd GUIDELINES ON THE INVESTIGATION AND MANAGEMENT OF THE ANTIPHOSPHOLIPID SYNDROME
 British Journal of Haematology 2000, 109, 704±715 Guidelines GUIDELINES ON THE INVESTIGATION AND MANAGEMENT OF THE ANTIPHOSPHOLIPID SYNDROME In 1991, the Haemostasis and Thrombosis Task Force of the British
British Journal of Haematology 2000, 109, 704±715 Guidelines GUIDELINES ON THE INVESTIGATION AND MANAGEMENT OF THE ANTIPHOSPHOLIPID SYNDROME In 1991, the Haemostasis and Thrombosis Task Force of the British
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
