Erik C. Hustak, MD, Mitchell P. Engle, MD, PhD, Ashwin Viswanathan, MD, and Dhanalakshmi Koyyalagunta, MD. Pain Physician 2014; 17:E405-E411
|
|
|
- Jasmin Cannon
- 6 years ago
- Views:
Transcription
1 Pain Physician 2014; 17:E405-E411 ISSN Case Report Lumbar Subarachnoid Hematoma Following an Epidural Blood Patch for Meningeal Puncture Headache Related to the Implantation of an Intrathecal Drug Delivery System Erik C. Hustak, MD, Mitchell P. Engle, MD, PhD, Ashwin Viswanathan, MD, and Dhanalakshmi Koyyalagunta, MD From: University of Texas MD Anderson Cancer Center, Houston, TX. Additional Author information on P. E410 Address Correspondence: Dhanalakshmi Koyyalagunta, MD U.T. MD Anderson Cancer Center Department of Pain Medicine 1515 Holcombe Blvd, Unit 409 Houston, TX Disclaimer: There was no external funding in the preparation of this manuscript. Conflict of interest: Each author certifies that he or she, or a member of his or her immediate family, has no commercial association (i.e., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted manuscript. Persistent meningeal puncture headache (MPH) is a known complication following both intentional and unintentional puncture of the dura mater. We present a case of persistent MPH following implantation of an intrathecal drug delivery system (IDDS). Two separate epidural blood patches (EBP) were performed under radiographic guidance with contrast visualization of the epidural space on postoperative days 16 and 28, respectively. The case was complicated by the development of a symptomatic lumbar subarachnoid hematoma diagnosed on postoperative day 35. The patient subsequently underwent a laminectomy, evacuation of the hematoma, and explanation of the IDDS. This case illustrates a potential unique morbidity associated with the EBP in a patient with an IDDS. The report concludes with a brief review of MPH followed by a discussion of possible mechanisms underlying this complication. Key words: Epidural blood patch, post dural puncture headache, meningeal puncture headache, complications, spinal subarachnoid hematoma, intrathecal drug delivery, implantable pain therapies, ziconotide, tinnitus, pain, pain procedures Pain Physician 2014; 17:E405-E411 Manuscript received: Revised manuscript received: Accepted for publication: Free full manuscript: Meningeal puncture headaches (MPH), traditionally referred to as post-dural puncture headaches, can occur following disruption of the dura and arachnoid mater. Disruption of cerebrospinal fluid (CSF) dynamics secondary to the dural injury is thought to lead to the development of the MPH (1). According to the International Classification of Headache Disorders, a MPH is by definition postural in nature with an exacerbation of symptoms within 15 minutes of assuming an upright position and alleviated within 15 minutes of assuming a recumbent position (2). Many MPHs are initially managed using conservative measures such as fluids, caffeine, recumbent posture, and analgesic therapy. For most patients, symptoms resolve within days to weeks but they occasionally persist for longer periods of time. Often, both the severity and duration of the symptoms encourages the practitioner to explore invasive treatment options such as the epidural blood patch (EBP).
2 Pain Physician: May/June 2014; 17:E405-E411 Conceptually, the EBP originates with Gormley (3) in the 1960s when he noticed that patients with traumatic (bloody) meningeal punctures were less likely to develop a MPH. In 1970, DiGiovanni (4) published his successful utilization of epidural injections of autologous blood for the treatment of MPH. Although multiple other treatment modalities are frequently utilized, the EBP still remains the gold standard for treatment of the MPH. A complex management decision arises when a patient develops a persistent MPH after implantation of an intrathecal drug delivery system (IDSS). Unique factors such as the risk of infecting an implanted medical device, damage to the IDDS catheter, and altered meningeal anatomy need to be considered prior to proceeding with an EBP in this setting. Furthermore, fluoroscopic guidance to ensure both appropriate needle position and contrast spread in the epidural space is essential. We report a case of a MPH following implantation of an IDDS. The patient received 2 EBPs with reasonable pain relief. However, the patient subsequently developed severe back pain with bilateral radiculopathy and was found to have a lumbar subarachnoid hematoma necessitating neurosurgical evacuation and IDDS explantation. Case Report A 46-year-old Caucasian man was referred to the MD Anderson Cancer Pain Management Center with a chief complaint of left groin and lower extremity pain. His pain sequela was the result of treatment he received for adenocarcinoma of the prostate. Specifically, he underwent a robotic assisted radical prostatectomy utilizing a left partial cavernous nerve sparing technique. Fortunately, the patient had no evidence of persistent or recurrent cancer at the time of our consultation. Unfortunately, the pain, described strictly in neuropathic terms, severely limited his ability to enjoy an active lifestyle. The patient failed extensive attempts at medication management with anti-convulsants, tricyclic antidepressants, and opioids. The pain was also refractory to a local anesthetic injection to the prostatic bed performed by the urologist under transrectal ultrasound guidance. After 9 months of suboptimal oral medication management, alternative interventional techniques were proposed including a trial of spinal cord stimulation and/or intrathecal drug delivery. The patient s health insurance company denied a trial of spinal cord stimulation and, ultimately, the patient underwent an intrathecal trial with ziconotide and bupi- vacaine. The single shot intrathecal trial was performed utilizing a 25-gauge pencil point needle at the L3-4 interspace. The dose delivered was 3 mcg of ziconotide and 2 mg of bupivacaine. The patient reported his pain relief as a 100% success. Eventually, he was taken to the operating room and underwent an uncomplicated IDDS implantation with catheter introduction through the L2-L3 inter-laminar space. The catheter tip was advanced to the inferior aspect of the T10 vertebral body. The IDDS was set to deliver 1 mcg of ziconotide and 2 mg of bupivacaine daily. Post-operatively he again reported exceptional pain relief and was discharged home. On postoperative day (POD) 7, the patient reported a mild postural headache along with mild wound tenderness and erythema. He was afebrile and no meningeal signs were appreciated. The patient was provided a prescription for oral antibiotics and instructed to increase his oral intake of fluids. The tenderness and erythema subsequently resolved as did the headache. However, on POD 16 the patient reported a severe postural headache with the additional complaint of tinnitus. His tinnitus was thought to be secondary to ziconotide so his dose was decreased to 0.7 mcg per day. Given the severity of his headache and the fact that it fulfilled diagnostic criteria for a MPH, an EBP was performed at L5-S1 interspace, below the level of the lumbar incision using radiographic guidance. An 18-gauge Tuohy needle was utilized and the epidural space was identified using a standard loss of resistance technique. Appropriate needle tip position in the epidural space was confirmed by a lack of CSF return from the Tuohy needle and by radiographic evidence of epidural contrast spread (Fig. 1A). Twenty ml of autologous blood was then collected in a sterile fashion and injected slowly through the needle. After the procedure, the patient reported good headache relief. On POD 23 he reported near complete resolution of his headache. From a functional standpoint, he had returned to work and was pleased with the procedural outcome. On POD 28 the MPH and tinnitus recurred and the patient returned to clinic for a repeat EBP. An EBP was performed at L4-L5 interspace utilizing an identical technique except that after the epidural space was identified, a catheter was advanced just distal to the epidural needle up to the L2-L3 interspace level within the epidural space. Aspiration from the catheter was negative and contrast was again injected, radiographically demonstrating epidural spread (Fig. 1B). Twenty ml of autologous blood was then slowly injected. To- E406
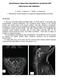
3 Lumbar Subarachnoid Hematoma Following an Epidural Blood Patch Fig. 1. The epidural space was appropriately identified during both epidural blood patches (EBP). A: Epidural contrast spread during the initial EBP performed with an 18 G Touhy needle at the L5-S1 interspace. B: Epidural contrast spread during second EBP performed with an 18 gauge Touhy needle and catheter at the L4-5 interspace. ward the end of this procedure, the patient felt mild pressure behind his eyes. The next day the patient was sent for a neurology consultation for his persistent tinnitus. By the time he was seen, he experienced slight return of MPH symptoms. A magnetic resonance imaging (MRI) scan of his brain was performed and was unremarkable. On POD 34, the patient presented to the MD Anderson emergency department with increasing headache, low back pain, bilateral lower extremity radicular pain, and subjective complaints of urinary retention. A STAT MRI of his lumbosacral spine was obtained which revealed a blood collection within the thecal sac at the L4-L5 level (Fig. 2A-B). A neurosurgical consultation was obtained, and given the patient s subjective assessment that his symptoms were worsening, the decision was made to offer surgical exploration. On POD 35 the patient was taken to the operating room for an L4 and L5 laminectomy, evacuation of a subarachnoid hematoma (Fig. 2C), and explantation of the IDDS. The dura was closed with silk sutures along with application of Duraseal (Fig. 2D; Covidien, Mansfield, MA). No signs of superficial or deep surgical site infections were identified. The patient was discharged home without MPH symptoms. His original lower extremity and groin neuropathic pain complaints subsequently returned and he was again managed pharmacologically with anti-convulsants, tricyclic antidepressants, and opioid therapy. Discussion MPH is a relatively common complication following puncture of the dura mater. The incidence of MPH increases with both increasing needle diameter and with the utilization of cutting tip needles (5). The headache usually begins within hours after dural puncture and is classically described in the occipital and frontal regions. It can be associated with nausea, vomiting, dizziness, photophobia, phonophobia, tinnitus, diplopia, neck stiffness, and scapular pain. Left untreated, most MPH will resolve within 1 2 weeks, however some may persist for several months or longer (6). The mechanism of MPH is classically described as a disruption of CSF homeostasis where CSF is produced by the choroid plexus and absorbed by the arachnoid villa. Following puncture of the dura mater a potential pathway is created allowing the extrusion of CSF through the dural defect resulting in a reduction of CSF in the intracranial space (1). Previous work has demonstrated that dural defects from needles greater than 25 G are capable of producing CSF extrusion greater than CSF production (7). The relationship between MPH and loss of CSF is more complicated than frequently E407
4 Pain Physician: May/June 2014; 17:E405-E411 Fig. 2. Localization and removal of the lumbar subarachnoid hematoma. Magnetic resonance imaging T1 sagittal (A) and axial (B) images showing the subarachnoid hematoma (white arrows) at the L4 and L5 vertebral levels. Surgical evacuation of hematoma (C) and dural repair with silk suture and Duraseal (D). thought and likely depends on other patient characteristics. For instance, some patients develop a MPH with relatively little CSF loss while others do not develop a MPH despite significant CSF loss. The mechanism by which this perturbation in CSF leads to MPH is not entirely clear. The classically described mechanism for the development of the MPH is caudal movement of brain structures after a loss of CSF leading to traction on pain sensitive intracranial structures (dura mater, venous sinuses, bridging veins, cranial nerves, and cervical nerves). However, MRI evidence does not consistently demonstrate this caudal E408
5 Lumbar Subarachnoid Hematoma Following an Epidural Blood Patch movement of the brain is necessary for MPH (1). An additional etiology is that loss of CSF causes a reflexive intracranial vasodilation in order to maintain the same intracranial volume as dictated by the Monroe-Kellie doctrine (1,8). This vasodilation then drives nocicieptive intracranial inputs in ways similar to migraine headache and possibly sensitizes the trigeminocervical complex leading to the full MPH symptomatology (9,10). The treatment of MPH generally starts with conservative management that includes bed rest, hydration, and caffeine therapy. Unfortunately, none of these are exceptionally effective in the treatment of MPH (6). Other pharmacological therapies previously studied include triptans, DDAVP, cosyntropin, hydrocortisone, and gabapentin (8,11). Several recent articles have demonstrated the efficacy of occipital nerve blocks in the treatment MPH, presumably by blocking the trigeminocervical input (9,10,12). Although other treatments may show promise, the EBP still remains the gold standard for the treatment of MPH with good evidence for its efficacy (13). This patient s clinical presentation was slightly atypical in that his postural MPH symptoms started one week following meningeal puncture. Furthermore, after originally responding to conservative treatments he eventually developed tinnitus. Cranial nerve symptomatology, including tinnitus, is occasionally reported with MPH. Ravi (14) reported a case of isolated tinnitus following intrathecal catheter placement in a parturient which was treated successfully with an EBP. However, the tinnitus in our case was confounded by his ziconotide infusion with its established central nervous system side effects, including auditory hallucinations. Expert opinion recommends low dosing with gradual titration in order to decrease ziconotide toxicity (3). Although our patient s ziconotide infusion was decreased, his auditory symptoms continued. The exact etiology of the tinnitus could have been secondary to the ziconotide despite the reduction in dose as the therapeutic window is variable between patients. However, given the overall clinical picture, we felt that the patient s symptoms could also be secondary to meningeal puncture pathology. Literature on performing an EBP in the context of an IDDS is quite scarce (15,16). In addition to the common risks associated with an EBP, this circumstance must also take into account additional complications such as infection of an implantable device, damage to the IDDS catheter, rostral spread of the IDDS drug, and a known path for tracking of blood and contaminants into the CSF (17). Subarachnoid hematomas can occur despite appropriate precautions. In this case, the development of a lumbar subarachnoid hemorrhage resulted in the need to remove the IDDS. In order to enhance the safety of the EBPs performed in the context of an IDDS, we confirmed epidural localization utilizing radiographic guidance along with contrast confirmation of injectate location. Despite these efforts in conjunction with the observation of negative CSF flow from the Tuohy needle (both EBPs) and negative aspiration of CSF via a catheter (second EBP), the patient developed a lumbar subarachnoid hematoma. In retrospect, it may have been justified to consider alternative imaging of the spine in an effort to evaluate the precise location of the dural defect. Indium radionucleotide scans, computed tomography (CT) with intrathecal contrast, or MRI with intrathecal gadolinium have all been utilized to detect CSF leaks (8,18). Understanding the location of the dural defect may allow a more targeted EBP or even deposition of epidural fibrin glue (6). Spinal subarachnoid hematoma is exceedingly rare, as the term was recently coined in 1984 and the distinction between subarachnoid hematoma and hemorrhage is often confused in the literature (5,13). The mechanisms underlying the formation of a spaceoccupying lesion, hematoma, is not well understood. Subarachnoid hemorrhages rarely form a hematoma as a result of CSF dynamics diluting any small amount of blood present (13). The literature proposes several factors predisposing to hematoma formation including vascular trauma in the context of coagulopathy associated with spinal anesthesia and epidural procedures (5,7,13). Introduction of blood in excess of CSF flow in the subarachnoid space can lead to hematoma formation (9). The etiology of the spinal subarachnoid hematoma in our case is not entirely clear. He did not have any known coagulopathy. Although we did not aspirate on the Tuohy needle during the first EBP in order to prevent further meningeal punctures, others have reported inadvertent intrathecal hematoma following this technique (19). In addition, inadvertent intrathecal delivery of autologous blood despite negative aspiration on an intrathecal catheter has also been reported (20). It remains unknown to the authors whether the hematoma developed as a result of introduction of autologous blood during the EBP or if the hematoma was secondary to vascular trauma from any one of the procedures along this patient s neuroaxis. Reasonable hypotheses in this case include unrecognized needle or E409
6 Pain Physician: May/June 2014; 17:E405-E411 catheter migration through the dura mater during the EBP, new or old dural punctures which served as tracks for blood to flow into the intrathecal space, or disruption of the normal meningeal architecture such that conditions were favorable for the subarchnoid flow of blood along the implanted catheter. Spinal subarachnoid hematomas in the absence of neurological deficits may often resolve nonoperatively with frequent neurological monitoring and symptomatic treatment with non-steroidal anti-inflammatory drugs (NSAIDS) and steroids (5,7,13). The decision to proceed with surgical evacuation of the subarachnoid hematoma in this case was based upon several factors. First, the patient s subjective complaints of urinary dysfunction were of concern. Second, it was felt that operative intervention was needed to help seal the dural leak that was refractory to multiple EBPs. Indeed, the dural leak was confirmed and sealed intraoperatively by the neurosurgeon. Furthermore, the MPH symptoms resolved shortly after the operation suggesting that the etiology of the patient s symptoms were a result of the dural leak. However, the subarachnoid hematoma itself could have also contributed to headache complaints (7). The final impetus for surgical evacuation and IDDS explantation was secondary to the patient s request for explant. He became distraught over the MPH symptoms and did not feel comfortable continuing with IDDS treatment. Ironically, after nearly a year removed from IDDS explant and continuation of the previous suboptimal pharmacologic regimen, the patient s insurance eventually approved spinal cord stimulation. The patient is currently doing well with an implanted neurostimulation system and minimal anti-convulsant, tricyclic antidepressants, or opioid medications. Conclusion Although the EBP is considered the gold standard treatment for MPH, the clinical decision to perform this procedure following implantation of an IDDS is complex. Our patient presented relatively late after IDDS implantation with a severe MPH. Despite appropriate clinical steps to prevent inadvertent intrathecal injection, the patient developed a subarachnoid hematoma necessitating neurosurgical laminectomy, hematoma evacuation, dural repair, and IDDS explantation. Given this potential clinical outcome, in addition to the risk of infecting an implanted IDDS, interventional physicians should consider exhausting less invasive techniques prior to proceeding with an EBP in a patient with an IDDS. Author Affiliations Dr. Hustak is a Fellow in the Department of Pain Medicine, University of Texas MD Anderson Cancer Center, Houston, TX. Dr. Engle is an Assistant Professor in the Department of Pain Medicine, University of Texas MD Anderson Cancer Center. Dr. Viswanathan is an Assistant Professor in the Department of Neurosurgery, University of Texas MD Anderson Cancer Center, Houston, TX. Dr. Koyyalagunta is a Professor in the Department of Pain Medicine, University of Texas MD Anderson Cancer Center, Houston, TX. References 1. Grant R, Condon B, Hart I, Teasdale GM. Changes in intracranial CSF volume after lumbar puncture and their relationship to post-lp headache. J Neurol Neurosurg Psychiatry 1991; 54: The International Classification of Headache Disorders: 2nd edition. Cephalalgia 2004; 24: Williams JA, Day M, Heavner JE. Ziconotide: An update and review. Expert Opin Pharmacother 2008; 9: DiGiovanni AJ, Dunbar BS. Epidural injections of autologous blood for postlumbar-puncture headache. Anesth Analg 1970; 49: Domenicucci M, Ramieri A, Paolini S, Russo N, Occhiogrosso G, Di Biasi C, Delfini R. Spinal subarachnoid hematomas: Our experience and literature review. Acta Neurochir (Wien) 2005; 147: ; discussion Freeman ED, Hoelzer BC, Eldrige JS, Moeschler SM. Fibrin glue to treat spinal fluid leaks associated with intrathecal drug systems. Pain Pract 2013; EPub ahead of print. Nov.20, Kreppel D, Antoniadis G, Seeling W. Spinal hematoma: A literature survey with meta-analysis of 613 patients. Neurosurg Rev 2003; 26: Schievink WI. Novel neuroimaging modalities in the evaluation of spontaneous cerebrospinal fluid leaks. Curr Neurol Neurosci Rep 2013; 13: Brem SS, Hafler DA, Van Uitert RL, Ruff RL, Reichert WH. Spinal subarachnoid hematoma: A hazard of lumbar puncture resulting in reversible paraplegia. N Engl J Med 1981; 304: Akin Takmaz S, Unal Kantekin C, Kaymak C, Basar H. Treatment of postdural puncture headache with bilateral greater occipital nerve block. Headache 2010; 50: Wagner Y, Storr F, Cope S. Gabapentin in the treatment of post-dural puncture headache: A case series. Anaesth Intensive Care 2012; 40: Matute E, Bonilla S, Girones A, Planas A. Bilateral greater occipital nerve block for post-dural puncture headache. Anaesthesia 2008; 63: Koyama S, Tomimatsu T, Kanagawa T, Sawada K, Tsutsui T, Kimura T, Chang E410
7 Lumbar Subarachnoid Hematoma Following an Epidural Blood Patch YS, Wasada K, Imai S, Murata Y. Spinal subarachnoid hematoma following spinal anesthesia in a patient with HELLP syndrome. Int J Obstet Anesth 2010; 19: Ravi R. Isolated tinnitus following placement of an intrathecal catheter for accidental dural puncture. Int J Obstet Anesth 2006; 15: Hardy PA. Extradural blood patch of a cerebrospinal fluid cutaneous fistula in the presence of an intrathecal drug delivery system. Anesthesiology 1994; 81: Huch K, Kunz U, Kluger P, Puhl W. Epidural blood patch under fluoroscopic control: Non-surgical treatment of lumbar cerebrospinal fluid fistula following implantation of an intrathecal pump system. Spinal Cord 1999; 37: Engle MP, Vinh BP, Harun N, Koyyalagunta D. Infectious complications related to intrathecal drug delivery system and spinal cord stimulator system implantations at a comprehensive cancer pain center. Pain Physician 2013; 16: Vanopdenbosch LJ, Dedeken P, Casselman JW, Vlaminck SA. MRI with intrathecal gadolinium to detect a CSF leak: A prospective open-label cohort study. J Neurol Neurosurg Psychiatry 2011; 82: Kalina P, Craigo P, Weingarten T. Intrathecal injection of epidural blood patch: A case report and review of the literature. Emerg Radiol 2004; 11: Aldrete JA, Brown TL. Intrathecal hematoma and arachnoiditis after prophylactic blood patch through a catheter. Anesth Analg 1997; 84: E411
8
Post-Dural Puncture Headache. Dr. Jacobs Aurélie Krans Anesthesie 18/03/2016 Kliniek St.-Jan, Brussel
 Post-Dural Puncture Headache Dr. Jacobs Aurélie Krans Anesthesie 18/03/2016 Kliniek St.-Jan, Brussel I - PATHOPHYSIOLOGY August Bier (intrathecal cocaïn1898)! first 2 cases PDPH CSF leak trough dura mater
Post-Dural Puncture Headache Dr. Jacobs Aurélie Krans Anesthesie 18/03/2016 Kliniek St.-Jan, Brussel I - PATHOPHYSIOLOGY August Bier (intrathecal cocaïn1898)! first 2 cases PDPH CSF leak trough dura mater
Postdural puncture headache preventing the impossible, treating the symptoms, evaluating long term effects.
 Postdural puncture headache preventing the impossible, treating the symptoms, evaluating long term effects. Marc Van de Velde, MD, PhD Professor of Anaesthesia, Catholic University Leuven (KUL) Chair Department
Postdural puncture headache preventing the impossible, treating the symptoms, evaluating long term effects. Marc Van de Velde, MD, PhD Professor of Anaesthesia, Catholic University Leuven (KUL) Chair Department
Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch
 J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
Dural Puncture Headache: How to Prevent It and What to Do When It Happens Kathleen A. Smith, M.D. University of North Carolina, Chapel Hill, NC
 Session: L125 Session: L338 Dural Puncture Headache: How to Prevent It and What to Do When It Happens Kathleen A. Smith, M.D. University of North Carolina, Chapel Hill, NC Disclosures: This presenter has
Session: L125 Session: L338 Dural Puncture Headache: How to Prevent It and What to Do When It Happens Kathleen A. Smith, M.D. University of North Carolina, Chapel Hill, NC Disclosures: This presenter has
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
POSTPARTUM MANAGEMENT OF DURAL PUNCTURE
 Document Ref: MAT 0145 WOMEN AND CHILDREN S and CLINICAL SUPPORT SERVICES DIVISION Clinical Guideline POSTPARTUM MANAGEMENT OF DURAL PUNCTURE For use in: (Clinical Area) For use by: (Staff Group) Distributed
Document Ref: MAT 0145 WOMEN AND CHILDREN S and CLINICAL SUPPORT SERVICES DIVISION Clinical Guideline POSTPARTUM MANAGEMENT OF DURAL PUNCTURE For use in: (Clinical Area) For use by: (Staff Group) Distributed
Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage
 DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
 Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
LV-EBP: Record-setting large volume epidural blood patch
 LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
Sudden Headache and visual disturbances in a young woman
 Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics
 Appendix 2: Case Report Form EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics Case Report Form Please fill each relevant step carefully Step 1. From Epidural
Appendix 2: Case Report Form EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics Case Report Form Please fill each relevant step carefully Step 1. From Epidural
Spontaneous Intracranial Hypotension Diagnosis and Treatment
 Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Frank Rosemeier. MD, MRCP(UK), MRCA, DipPEC(SA) Attending Anesthesiologist. JLR Medical Group
 Postdural Puncture Headaches A Contemporary Update Frank Rosemeier MD, MRCP(UK), MRCA, DipPEC(SA) Attending Anesthesiologist JLR Medical Group Maitland, FL Why should we care? Mother want to feel well
Postdural Puncture Headaches A Contemporary Update Frank Rosemeier MD, MRCP(UK), MRCA, DipPEC(SA) Attending Anesthesiologist JLR Medical Group Maitland, FL Why should we care? Mother want to feel well
Postdural Puncture Headache
 2015 Annual Meeting and Workshops Postdural Puncture Headache Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University Baltimore, Maryland Disclosures No financial conflicts of
2015 Annual Meeting and Workshops Postdural Puncture Headache Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University Baltimore, Maryland Disclosures No financial conflicts of
Effective Epidural Blood Patch Volumes for Postdural Puncture Headache in Taiwanese Women
 ORIGINAL ARTICLE Effective Epidural Blood Patch Volumes for Postdural Puncture Headache in Taiwanese Women Li-Kuei Chen, 1 Chi-Hsiang Huang, 1 Wei-Horng Jean, 2 Cheng-Wei Lu, 2 Chen-Jung Lin, 1 Wei-Zen
ORIGINAL ARTICLE Effective Epidural Blood Patch Volumes for Postdural Puncture Headache in Taiwanese Women Li-Kuei Chen, 1 Chi-Hsiang Huang, 1 Wei-Horng Jean, 2 Cheng-Wei Lu, 2 Chen-Jung Lin, 1 Wei-Zen
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury
 Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Incidental durotomy during spine surgery occurs in. Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks
 J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
Post-Dural Puncture Headache(PDPH): an update. Dorel Sandesc
 Post-Dural Puncture Headache(PDPH): an update Dorel Sandesc August Bier 1898: a personal experience of post dural puncture headache Toward the evening I was forced to take to bed and remained there for
Post-Dural Puncture Headache(PDPH): an update Dorel Sandesc August Bier 1898: a personal experience of post dural puncture headache Toward the evening I was forced to take to bed and remained there for
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
While some patients with SIH recover without intervention
 ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Obstetrical Anesthesia. Safe Pain Relief for Childbirth
 Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
PDPH: To Patch or Not to Patch
 PDPH: To Patch or Not to Patch Moderators: 1. Kim Strupp, MD FAAP Assistant Professor of Anesthesiology, Children s Hospital Colorado/University of Colorado, Aurora, CO 2. Debnath Chatterjee, MD Associate
PDPH: To Patch or Not to Patch Moderators: 1. Kim Strupp, MD FAAP Assistant Professor of Anesthesiology, Children s Hospital Colorado/University of Colorado, Aurora, CO 2. Debnath Chatterjee, MD Associate
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Intradural Spinal Vein Enlargement in Craniospinal Hypotension
 AJNR Am J Neuroradiol 26:34 38, January 2005 Case Report Intradural Spinal Vein Enlargement in Craniospinal Hypotension M. Todd Burtis, John L. Ulmer, Glenn A. Miller, Alexandru C. Barboli, Scott A. Koss,
AJNR Am J Neuroradiol 26:34 38, January 2005 Case Report Intradural Spinal Vein Enlargement in Craniospinal Hypotension M. Todd Burtis, John L. Ulmer, Glenn A. Miller, Alexandru C. Barboli, Scott A. Koss,
EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics
 Appendix 3: Pre-study Questionnaire EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics All questions in this questionnaire relate to the situation in 2014
Appendix 3: Pre-study Questionnaire EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics All questions in this questionnaire relate to the situation in 2014
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai. Interventional Options
 10/20/2017 Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai Charles Luoy and Marcel Maya Cedars Sinai Blood Patch Single level Bilevel Targeted Fibrin Glue Interventional Options 1 10/20/2017
10/20/2017 Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai Charles Luoy and Marcel Maya Cedars Sinai Blood Patch Single level Bilevel Targeted Fibrin Glue Interventional Options 1 10/20/2017
Remembering Donald J. Dalessio, MD The Headache Clinic Featuring the Baylor Scott & White Headache Clinic in Temple, Texas.
 Spinal Cerebrospinal Fluid Leak An Under-recognized Cause of Headache More common than expected, why is this type of headache so often misdiagnosed or the diagnosis is delayed? Challenging the One Size
Spinal Cerebrospinal Fluid Leak An Under-recognized Cause of Headache More common than expected, why is this type of headache so often misdiagnosed or the diagnosis is delayed? Challenging the One Size
Continuous Spinal Anaesthesia
 Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
Regional Anesthesia. Fatiş Altındaş Dept. of Anesthesiology
 Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Regional Anesthesia Fatiş Altındaş Dept. of Anesthesiology Regional anesthesia - Definition Renders a specific area of the body, e.g. foot, arm, lower extremities insensating to stimulus of surgery or
Eldor Epidural Kit (CSEN 68) Epidural catheter technique
 Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
How and why to do an epidural in dogs and cats? Which Indications and which drugs?
 AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
Author Information. Case Information
 Author Information Full Names: Jonathan M. Hagedorn, MD Susan M. Moeschler, MD Affiliation: Mayo Clinic, Rochester, MN Email Contacts: jonhagedornmd@yahoo.com Moeschler.susan@mayo.edu Case Information
Author Information Full Names: Jonathan M. Hagedorn, MD Susan M. Moeschler, MD Affiliation: Mayo Clinic, Rochester, MN Email Contacts: jonhagedornmd@yahoo.com Moeschler.susan@mayo.edu Case Information
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Transforaminal epidural blood patch for intractable spontaneous cerebrospinal fluid leak: a case report
 Fujiwara et al. JA Clinical Reports (2017) 3:2 DOI 10.1186/s40981-016-0073-2 CASE REPORT Transforaminal epidural blood patch for intractable spontaneous cerebrospinal fluid leak: a case report Open Access
Fujiwara et al. JA Clinical Reports (2017) 3:2 DOI 10.1186/s40981-016-0073-2 CASE REPORT Transforaminal epidural blood patch for intractable spontaneous cerebrospinal fluid leak: a case report Open Access
Postoperative Paraplegia after Nonvascular Thoracic Surgery. K Popat, T Ngyugen, A Kowalski, M Daley, J Arens, D Thakar
 ISPUB.COM The Internet Journal of Anesthesiology Volume 8 Number 1 Postoperative Paraplegia after Nonvascular Thoracic Surgery K Popat, T Ngyugen, A Kowalski, M Daley, J Arens, D Thakar Citation K Popat,
ISPUB.COM The Internet Journal of Anesthesiology Volume 8 Number 1 Postoperative Paraplegia after Nonvascular Thoracic Surgery K Popat, T Ngyugen, A Kowalski, M Daley, J Arens, D Thakar Citation K Popat,
National Hospital for Neurology and Neurosurgery
 National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
Case Discussions Cynthia A. Wong, M.D.
 Case Discussions Cynthia A. Wong, M.D. Association des Anesthѐsiologistes du Quѐbec April 2014 CASE 1 Maternal Mortality Lewis G (ed). CEMACH 2007. Saving Mothers Lives 2003-2005 Pregnancy Complications
Case Discussions Cynthia A. Wong, M.D. Association des Anesthѐsiologistes du Quѐbec April 2014 CASE 1 Maternal Mortality Lewis G (ed). CEMACH 2007. Saving Mothers Lives 2003-2005 Pregnancy Complications
Introduction to Obstetric Anesthesia
 Introduction to Obstetric Anesthesia Dr A Alberts Department of Anesthesiology and Critical Care 2007 INTRODUCTION During obstetric anesthesia the anesthetist controls the following Maternal Gas exchange,
Introduction to Obstetric Anesthesia Dr A Alberts Department of Anesthesiology and Critical Care 2007 INTRODUCTION During obstetric anesthesia the anesthetist controls the following Maternal Gas exchange,
Intrathecal Baclofen for CNS Spasticity
 Intrathecal Baclofen for CNS Spasticity Last Review Date: October 13, 2017 Number: MG.MM.ME.31bC7 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary
Intrathecal Baclofen for CNS Spasticity Last Review Date: October 13, 2017 Number: MG.MM.ME.31bC7 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary
Lumbar CSF Drains for Thoracic Aortic Surgery
 Lumbar CSF Drains for Thoracic Aortic Surgery John C. Klick, MD CASE CAG Why do them? Open descending thoracic aortic aneurysm repair (still the gold standard) has an incidence of postoperative paraplegia
Lumbar CSF Drains for Thoracic Aortic Surgery John C. Klick, MD CASE CAG Why do them? Open descending thoracic aortic aneurysm repair (still the gold standard) has an incidence of postoperative paraplegia
Trust Guideline for the Management of Inadvertent Dural Puncture and Post Dural Puncture Headache in Obstetrics
 A clinical guideline recommended for use In: By: For: Key words: Written by: Delivery Suite All Anaesthetic Staff Women in labour who have had an inadvertent dural puncture when having an epidural sited
A clinical guideline recommended for use In: By: For: Key words: Written by: Delivery Suite All Anaesthetic Staff Women in labour who have had an inadvertent dural puncture when having an epidural sited
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Mechanisms of Headache in Intracranial Hypotension
 Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
Epidural Steroid Injection
 Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Epidural Steroid Injection Epidural steroid injections (ESI) are performed to place anti-inflammatory medication (steroid) and local anesthetic in the epidural space to target irritated nerves and relieve
Drainage of an acute spinal epidural hematoma that developed without risk factors in the thoracic spine using epidural needle -A case report-
 Anesth Pain Med 2017; 12: 266-270 https://doi.org/10.17085/apm.2017.12.3.266 Case Report http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2017.12.3.266&domain=pdf&date_stamp=2017-07-25 pissn 1975-5171
Anesth Pain Med 2017; 12: 266-270 https://doi.org/10.17085/apm.2017.12.3.266 Case Report http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2017.12.3.266&domain=pdf&date_stamp=2017-07-25 pissn 1975-5171
Two Cases of Secondary Intracranial Hypotension
 online ML Comm CASE REPORT J Korean Neurotraumatol Soc 2011;7:103-107 ISSN 1738-8708 Two Cases of Secondary Intracranial Hypotension Yong-Sang Kim, MD, Byung Moon Cho, MD, Sung-Min Cho, MD, Se-Hyuck Park,
online ML Comm CASE REPORT J Korean Neurotraumatol Soc 2011;7:103-107 ISSN 1738-8708 Two Cases of Secondary Intracranial Hypotension Yong-Sang Kim, MD, Byung Moon Cho, MD, Sung-Min Cho, MD, Se-Hyuck Park,
Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities
 DOI 10.1007/s10072-013-1364-2 BRIEF COMMUNICATION Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities Angelo Franzini G. Messina L. Chiapparini G.
DOI 10.1007/s10072-013-1364-2 BRIEF COMMUNICATION Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities Angelo Franzini G. Messina L. Chiapparini G.
A Patient s Guide to Pain Management: Pain Pumps
 A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Pain Management: Pain Pumps 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Management of Symptomatic Sacral Perineural Cysts
 Management of Symptomatic Sacral Perineural Cysts Jianqiang Xu 1, Yongdong Sun 1, Xin Huang 1, Wenzhong Luan 2 * 1 Department of Neurosurgery, General Hospital of Fengfeng Group, Handan, China, 2 Department
Management of Symptomatic Sacral Perineural Cysts Jianqiang Xu 1, Yongdong Sun 1, Xin Huang 1, Wenzhong Luan 2 * 1 Department of Neurosurgery, General Hospital of Fengfeng Group, Handan, China, 2 Department
Epidural Blood Patch for the Treatment of Spontaneous and Iatrogenic Orthostatic Headache
 Pain Physician 2016; 19:E1115-E1122 ISSN 2150-1149 Retrospective Evaluation Epidural Blood Patch for the Treatment of Spontaneous and Iatrogenic Orthostatic Headache Yun So, MD, Jung Min Park, MD, Pil-moo
Pain Physician 2016; 19:E1115-E1122 ISSN 2150-1149 Retrospective Evaluation Epidural Blood Patch for the Treatment of Spontaneous and Iatrogenic Orthostatic Headache Yun So, MD, Jung Min Park, MD, Pil-moo
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain
 Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
Beth Israel Deaconess Medical Center Department of Anesthesia, Critical Care, and Pain Medicine Rotation: Interventional Pain Goals GOALS AND OBJECTIVES The ACGME recognizes that interventional pain medicine
PSEUDO-SUBARACHNOID HEMORRHAGE AFTER INADVERTENT DURAL PUNCTURE DURING CERVICAL EPIDURAL STEROID INJECTION
 PSEUDO-SUBARACHNOID HEMORRHAGE AFTER INADVERTENT DURAL PUNCTURE DURING CERVICAL EPIDURAL STEROID INJECTION HAI NGUYEN, DO, MPH Anesthesiology Resident (University of Kansas Wichita) JOEL CAVAZOS, MD Pain
PSEUDO-SUBARACHNOID HEMORRHAGE AFTER INADVERTENT DURAL PUNCTURE DURING CERVICAL EPIDURAL STEROID INJECTION HAI NGUYEN, DO, MPH Anesthesiology Resident (University of Kansas Wichita) JOEL CAVAZOS, MD Pain
Dr P.W.Buczkowski. Consultant in Anaesthesia & Pain Medicine. Royal Derby Hospital
 Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
Dr P.W.Buczkowski Consultant in Anaesthesia & Pain Medicine Royal Derby Hospital INTERVENTIONAL PAIN MANAGEMENT III Neuroaxial Drug Delivery KYIV May 2010 Dr J Azzopardi MD FRCA FFPMANZCA FFPMRCA Consultant
INJECTION PROCEDURES
 INJECTION PROCEDURES GENERAL CONSIDERATIONS AND PREPARATION FOR THE INJECTION In general, injection procedures for the spine and some other parts of the body entail the use of live x- ray known as flouroscopy
INJECTION PROCEDURES GENERAL CONSIDERATIONS AND PREPARATION FOR THE INJECTION In general, injection procedures for the spine and some other parts of the body entail the use of live x- ray known as flouroscopy
POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY
 Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Spontaneous intracranial hypotension complicated with cerebral venous thrombosis and subdural effusion: a case report
 Case Report Spontaneous intracranial hypotension complicated with cerebral venous thrombosis and subdural effusion: a case report Murali Krishna Menon 1, Thara Prathap 2, Muhammed Jasim Abdul Jalal 3 1
Case Report Spontaneous intracranial hypotension complicated with cerebral venous thrombosis and subdural effusion: a case report Murali Krishna Menon 1, Thara Prathap 2, Muhammed Jasim Abdul Jalal 3 1
Complications of Neuraxial Anesthesia An Ounce of Prevention is Worth a Pound of Cure
 Complications of Neuraxial Anesthesia An Ounce of Prevention is Worth a Pound of Cure Brian J Kasson CRNA MHS Faculty/Clinical Instructor Nurse Anesthesia Program Northern Kentucky University Staff Nurse
Complications of Neuraxial Anesthesia An Ounce of Prevention is Worth a Pound of Cure Brian J Kasson CRNA MHS Faculty/Clinical Instructor Nurse Anesthesia Program Northern Kentucky University Staff Nurse
Post-dural puncture headache in pregnant women: What have we learned?
 Rev. Col. Post-dural Anest. 34: puncture 267-272, headche 2006 ARTÍCULO DE REVISIÓN Post-dural puncture headache in pregnant women: What have we learned? Krzysztof M. Kuczkowski, M.D.* ABSTRACT: The obstetric
Rev. Col. Post-dural Anest. 34: puncture 267-272, headche 2006 ARTÍCULO DE REVISIÓN Post-dural puncture headache in pregnant women: What have we learned? Krzysztof M. Kuczkowski, M.D.* ABSTRACT: The obstetric
Open Discectomy. North American Spine Society Public Education Series
 Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
Open Discectomy North American Spine Society Public Education Series What Is Open Discectomy? Open discectomy is the most common surgical treatment for ruptured or herniated discs of the lumbar spine.
SURGICAL REMOVAL OF A LOOPED AND KNOTTED EPIDURAL CATHETER IN A POSTPARTUM PATIENT
 SURGICAL REMOVAL OF A LOOPED AND KNOTTED EPIDURAL CATHETER IN A POSTPARTUM PATIENT - A Case Report - O. AL-KAYED *, F. AL-BOUTI **, AND M.O. ABABNEH *** Summary We report a case of unsuccessful removal
SURGICAL REMOVAL OF A LOOPED AND KNOTTED EPIDURAL CATHETER IN A POSTPARTUM PATIENT - A Case Report - O. AL-KAYED *, F. AL-BOUTI **, AND M.O. ABABNEH *** Summary We report a case of unsuccessful removal
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Intrathecal Opioid Therapy for Management of Chronic Pain
 Intrathecal Opioid Therapy for Management of Chronic Pain Date of Origin: 01/2000 Last Review Date: 09/27/2017 Effective Date: 09/27/2017 Dates Reviewed: 11/2002, 12/2003, 12/2004, 12/2005, 12/2006, 12/2007,
Intrathecal Opioid Therapy for Management of Chronic Pain Date of Origin: 01/2000 Last Review Date: 09/27/2017 Effective Date: 09/27/2017 Dates Reviewed: 11/2002, 12/2003, 12/2004, 12/2005, 12/2006, 12/2007,
Differential Diagnosis of Orthostatic Headache
 Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Spontaneous Intracranial Hypotension Following a Yoga Class: A Case Report
 American Journal of Medical Case Reports, 2015, Vol. 3, No. 10, 314-318 Available online at http://pubs.sciepub.com/ajmcr/3/10/3 Science and Education Publishing DOI:10.12691/ajmcr-3-10-3 Spontaneous Intracranial
American Journal of Medical Case Reports, 2015, Vol. 3, No. 10, 314-318 Available online at http://pubs.sciepub.com/ajmcr/3/10/3 Science and Education Publishing DOI:10.12691/ajmcr-3-10-3 Spontaneous Intracranial
Lumbar Puncture. Practical Skills Teaching. Year 3 Medical Students MB BCh
 Lumbar Puncture Practical Skills Teaching Year 3 Medical Students MB BCh 2012-2013 Contents Introduction to workshop... 3 Overall Session Aim... 4 Intended learning objectives... 4 Workshop Structure Guidance
Lumbar Puncture Practical Skills Teaching Year 3 Medical Students MB BCh 2012-2013 Contents Introduction to workshop... 3 Overall Session Aim... 4 Intended learning objectives... 4 Workshop Structure Guidance
(แทงข างหล ง...ร าวไปถ งห ว)
 From Back to Head (แทงข างหล ง...ร าวไปถ งห ว) 23 Jul 2018 Natinee Benjangkhaprasert Phonneeya Nimpunyakampong Advisor Lecturer Choopong Luansritisakul 1 Case 62 year-old Thai male Diagnosis: CA Colon
From Back to Head (แทงข างหล ง...ร าวไปถ งห ว) 23 Jul 2018 Natinee Benjangkhaprasert Phonneeya Nimpunyakampong Advisor Lecturer Choopong Luansritisakul 1 Case 62 year-old Thai male Diagnosis: CA Colon
16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces
 16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces Moderators: Kendra Grim, MD, Robert T. Wilder, MD, PhD Institution:
16 year old with Disabling Chest Wall Pain after Thoracoscopic Talc Pleurodesis for Treatment of Recurrent Spontaneous Pneumothoraces Moderators: Kendra Grim, MD, Robert T. Wilder, MD, PhD Institution:
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 1 Dumbbell Shaped Thoracic Spine Cavernous Hemangioma: A Case Report and Review of the Literature J Gonzalez-Cruz, A Nanda Citation J Gonzalez-Cruz,
The spinal headache in pregnant women
 N. J. Obstet. Gynaecol Vol. 1, No. 2, p. 4-9 Nov-Dem 2006 REVIEW The spinal headache in pregnant women Krzysztof M. Kuczkowski Departments of Anesthesiology and Reproductive Medicine, University of California,
N. J. Obstet. Gynaecol Vol. 1, No. 2, p. 4-9 Nov-Dem 2006 REVIEW The spinal headache in pregnant women Krzysztof M. Kuczkowski Departments of Anesthesiology and Reproductive Medicine, University of California,
Efficacy of epidural blood patch with fibrin glue additive in refractory headache due to intracranial hypotension: preliminary report
 DOI 0.86/s40064-06-975- RESEARCH Efficacy of epidural blood patch with fibrin glue additive in refractory due to intracranial hypotension: preliminary report Justin Elwood *, Misha Dewan 2, Jolene Smith
DOI 0.86/s40064-06-975- RESEARCH Efficacy of epidural blood patch with fibrin glue additive in refractory due to intracranial hypotension: preliminary report Justin Elwood *, Misha Dewan 2, Jolene Smith
UCSD DEPARTMENT OF ANESTHESIOLOGY
 UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
Pure cervical radiculopathy due to spontaneous spinal epidural haematoma (SSEH): report of a case solved conservatively
 Eur Spine J (2006) 15 (Suppl. 5): S569 S573 DOI 10.1007/s00586-005-0023-6 CASE REPORT Carlos Villas Alvaro Silva Matı as Alfonso Pure cervical radiculopathy due to spontaneous spinal epidural haematoma
Eur Spine J (2006) 15 (Suppl. 5): S569 S573 DOI 10.1007/s00586-005-0023-6 CASE REPORT Carlos Villas Alvaro Silva Matı as Alfonso Pure cervical radiculopathy due to spontaneous spinal epidural haematoma
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Idiopathic Spinal Subarachnoid Hemorrhage: A Case Report and Review of the Literature
 THIEME GLOBAL SPINE JOURNAL Case Report e59 Idiopathic Spinal Subarachnoid Hemorrhage: A Case Report and Review of the Literature Justin M. Moore 1 Rondhir Jithoo 1 Peter Hwang 1 1 Department of Neurosurgery,
THIEME GLOBAL SPINE JOURNAL Case Report e59 Idiopathic Spinal Subarachnoid Hemorrhage: A Case Report and Review of the Literature Justin M. Moore 1 Rondhir Jithoo 1 Peter Hwang 1 1 Department of Neurosurgery,
A 5-Year Audit of Accidental Dural Punctures, Postdural Puncture Headaches, and Failed Regional Anesthetics at a Tertiary-Care Medical Center
 Research Article TheScientificWorldJOURNAL (2009) 9, 715 722 ISSN 1537-744X; DOI 10.1100/tsw.2009.94 A 5-Year Audit of Accidental Dural Punctures, Postdural Puncture Headaches, and Failed Regional Anesthetics
Research Article TheScientificWorldJOURNAL (2009) 9, 715 722 ISSN 1537-744X; DOI 10.1100/tsw.2009.94 A 5-Year Audit of Accidental Dural Punctures, Postdural Puncture Headaches, and Failed Regional Anesthetics
Myelogram and Lumbar Puncture: Pre and Post Procedure Details
 Myelogram and Lumbar Puncture: Pre and Post Procedure Details (Revised October 2011) 1) Patients should be well hydrated. No solid food after midnight but clear liquids in the a.m. 2) Patients who take
Myelogram and Lumbar Puncture: Pre and Post Procedure Details (Revised October 2011) 1) Patients should be well hydrated. No solid food after midnight but clear liquids in the a.m. 2) Patients who take
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Intracranial Hypotension Concurrent Presented with Pseudo-Subarachnoid Hemorrhage and Transverse Sinus Thrombosis: A Case Report
 NNQ Intracranial Hypotension Concurrent Presented with Pseudo-Subarachnoid Hemorrhage and Transverse Sinus Thrombosis: A Case Report Chieh-Yang Cheng 1, Che-Chuan Wang 1, Tai-Yuan Chen 2, Jinn-Rung Kuo
NNQ Intracranial Hypotension Concurrent Presented with Pseudo-Subarachnoid Hemorrhage and Transverse Sinus Thrombosis: A Case Report Chieh-Yang Cheng 1, Che-Chuan Wang 1, Tai-Yuan Chen 2, Jinn-Rung Kuo
REGIONAL/LOCAL ANESTHESIA and OBESITY
 REGIONAL/LOCAL ANESTHESIA and OBESITY Jay B. Brodsky, MD Stanford University School of Medicine Jbrodsky@stanford.edu Potential Advantages Regional compared to General Anesthesia Minimal intra-operative
REGIONAL/LOCAL ANESTHESIA and OBESITY Jay B. Brodsky, MD Stanford University School of Medicine Jbrodsky@stanford.edu Potential Advantages Regional compared to General Anesthesia Minimal intra-operative
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
STANDARDIZED PROCEDURE NEONATAL LUMBAR PUNCTURE (Neonatal)
 I. Definition The lumbar puncture is used to sample the cerebral spinal fluid (CSF) to determine if an infection exists, to diagnose certain disease states, or (with order of Attending/Fellow) to drain
I. Definition The lumbar puncture is used to sample the cerebral spinal fluid (CSF) to determine if an infection exists, to diagnose certain disease states, or (with order of Attending/Fellow) to drain
Low PRESSURE Headaches. What they area and what can you do? Kathleen B. Digre MD University of Utah
 Low PRESSURE Headaches aka Low CSF volume headache: What they area and what can you do? Kathleen B. Digre MD University of Utah Disclosure: I have a part ownership on a patent for thin filmed technology
Low PRESSURE Headaches aka Low CSF volume headache: What they area and what can you do? Kathleen B. Digre MD University of Utah Disclosure: I have a part ownership on a patent for thin filmed technology
NANOS Patient Brochure
 NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
8/28/18. Anesthetic considerations for patients with implanted devices for treating chronic pain and more. Objectives:
 Anesthetic considerations for patients with implanted devices for treating chronic pain and more Alaa Abd-Elsayed, MD, MPH Medical Director, UW Pain Services Medical Director, Pain Clinic Section Head,
Anesthetic considerations for patients with implanted devices for treating chronic pain and more Alaa Abd-Elsayed, MD, MPH Medical Director, UW Pain Services Medical Director, Pain Clinic Section Head,
Myelography in Cancer Patients: Modified Technique
 617 Myelography in Cancer Patients: Modified Technique Ya-Yan Lee' J. Peter Glass 2 Sidney Wallace' Because of the frequency of multiple sites of involvement, a thorough evaluation of the entire spinal
617 Myelography in Cancer Patients: Modified Technique Ya-Yan Lee' J. Peter Glass 2 Sidney Wallace' Because of the frequency of multiple sites of involvement, a thorough evaluation of the entire spinal
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES
 REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
REVIEW QUESTIONS ON VERTEBRAE, SPINAL CORD, SPINAL NERVES 1. A 28-year-old-women presented to the hospital emergency room with intense lower back spasms in the context of coughing during an upper respiratory
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
