Postdural Puncture Headache
|
|
|
- John Lamb
- 5 years ago
- Views:
Transcription
1 2015 Annual Meeting and Workshops Postdural Puncture Headache Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University Baltimore, Maryland
2 Disclosures No financial conflicts of interest Off-label discussions (Rx for PDPH): Caffeine Gabapentin Pregabalin Hydrocortisone, dexamethasone Theophylline Sumatriptan Adrenocorticotropic hormone (ATCH) Cosyntropin
3 Overview Pathophysiology Clinical presentation Risk factors Patient-related Needle-related Treatment options Conservative therapy Epidural blood patch
4 Pathophysiology Loss of Cerebrospinal Fluid (CSF) Rate of loss (12 ml/min) > rate of replacement (0.35 ml/min) 150 ml of CSF in brain and spinal cord CSF leakage ICP/traction on cranial structures Blood vessels, meninges, cranial nerves Evidence of CSF loss as main culprit: Direct removal of CSF HA Arch Neurol Psych 1943;49: MRI studies in PDPH patients AA 1997;84:585-90; Brain 2015;138:1492-8
5 Pathophysiology Evidence of CSF loss as main culprit: Removal of 20 ml of CSF HA Arch Neurol Psych 1943;49: HA resolved after intrathecal injection of NaCl HA traction by the sagging brain on pain-sensitive anchoring structures MRI studies in PDPH patients Extradural local static fluid collection in PDPH patients Anesth Analg 1997;84: PDPH rostral distributions of periradicular leaks and epidural collections Brain 2015;138:1492-8
6 Anesth Analg 1997;84:585-90
7 Brain 2015;138:1492-8
8 Brain 2015;138:1492-8
9 Pathophysiology: Other Compensatory cerebral vasodilatation Monro-Kellie hypothesis: cranial homeostasis by maintaining the sum of the volumes of brain, blood and CSF constant Inverse relationship between blood ( 4% of total intracranial volume) and CSF volume ( 10%) CSF will lead to cerebral blood (vasodilatation) to maintain equilibrium and constant intracranial volume Experimental data suggests that an cerebral blood represents cerebral vasodilatation RAPM 2001;26:401-6
10 Pathophysiology: Other Pneumocephalus Anesthesiology 1998;88:76-81 RCT: air vs. saline-lor syringe, 20-G Tuohy No difference: incidence of accidental dural puncture Air = 48/1812 cases (2.6%); Saline = 51/1918 cases (2.7%) However, incidence of PDPH: air > saline PDPH: Air (32/48 = 66.7%) > saline (5/51 = 9.8%) Intrathecal air bubbles detected on CT:» Air = 30/32 patients, Saline = 0/51 patients Exacerbation or co-existence of HA from other etiologies (migraine, tension)
11
12 Clinical Presentation Cardinal feature: postural component of HA Severity varies but PDPH may render the patient bedridden May also have: Neck stiffness (57%), backache (35%), nausea (22%), photophobia, cranial nerve signs, muscle spasms Auditory symptoms (4-12%) Acta Anaesthesiol Scand 1995;39: Ocular symptoms (3-13%) Acta Anaesthesiol Scand 1995;39: Cranial nerves III, IV and VI may result in diplopia and difficulty with accommodation Rarely: visual field defects and nystagmus
13 Clinical Presentation Typical course (without intervention) Onset: onset varies from 1-7 days (median = 2 days) 40-65% within first 24 h; 70-90% within 48 h Severity: varies with needle characteristics Duration: median duration is 5-7 days (no active treatment) PDPH is a diagnosis of exclusion Other etiologies may mimic or co-exist with PDPH May miss some other potentially critical diagnoses Acta Anaesthesiol Scand 1995;39: JAMA 1956;161:586-91
14 Clinical Presentation EBPs for a presumed diagnosis of PDPH; however, patients subsequently were diagnosed with: Meningitis (persistent HA and fever) Obstet Gynecol 1989;74:437-9 Late-onset pre-eclampsia (seizures) BJA 2002;90: Subdural hematoma (seizures) RAPM 2002;27:433-6 Cortical vein thrombosis (confusion, sedation, seizures) Incidence of 1 in 11,000 with onset of HA within 2-3 days postpartum Obstet Gynecol 1997;89:413-8
15 Clinical Presentation Peripartum isolated cortical vein thrombosis 32 y/o with HA 3 days after delivery of her baby Initial dx = PDPH; RX analgesia, caffeine, and fluids Readmitted 2 days after d/c with generalized seizures 1 st MRI intracranial hypotension, received EBP Symptoms worsened; 3 days later visual field defect 2 nd MRI R parietal hematoma with evidence of isolated cortical vein thrombosis Case Rep Med 2013;2013:701264
16 Case Rep Med 2013;2013:701264
17 MRI Findings Cerebellar tonsillar descent and posterior fossa crowding Subdural fluid collections, engorged cerebral venous sinuses, or decreased size of the ventricles Pachymeningeal gadolinium enhancement Nonspecific finding: lower ICP, infectious-inflammatory, neoplastic, or iatrogenic etiologies Neurosurg Rev 2015;38: Headache 2013;53:673-5
18 Headache 2013;53:673-5
19
20 Patient-related Risk Factors Age: PDPH with age Gender: PDPH with female gender? BMI: PDPH with BMI Needle-related factors Needle characteristics Size and shape Needle insertion Bevel orientation: parallel vs. perpendicular Midline vs. paramedian? Continuous intrathecal catheters
21 Age as a Risk Factor Age: PDPH with age Etiology unclear: Elasticity of dura; reactivity of cerebral vessels Narrowed exit routes from the epidural space Differences in pain perception in the elderly (vs. younger) Incidence of PDPH: 22g = 10.8% elderly vs. 27.6% young Anaesthesia 1989;44:571-3 Incidence of PDPH: 25g = 7.8% elderly vs. 12.6% young
22 Gender as a Risk Factor Initial studies: incidence in females JAMA 1956;161: Did not adjust for gender: relatively spinals in paturients Other studies suggest that gender is not a risk factor Multivariate analysis of 1021 spinal anesthetics no association between gender and PDPH AA 1990;70: Cohort study: 2378 spinals with 29-G Quincke: no difference between (1.1%) and (1.5%) Acta Anaesthesiol Scand 1994;38:691-3 Menstrual cycle, hormonal levels do not influence the incidence of PDPH RAPM 1998;23:485-90
23 Gender is a Risk Factor OR= 0.55 (0.44,0.67); p< Anesthesiology 2006;105:613-8
24 BMI as a Risk Factor? PDPH with BMI: epidural pressure in obese IT/EP pressure gradient CSF Intraabd pressure non-csf volume in epidural space Retrospective review of 518 ADP Anesth Analg 2015;121:451-6 PDPH (parturients) = 51% PDPH BMI 31.5 (39%) vs. BMI < 31.5 (56%, p=0.0004) No difference in HA severity or rate of EBP Retrospective review of 125 ADP Int J Obstet Anesth 2014;23:371-5 BMI < 30 (n=65) vs. BMI 30 (n=60) ND in PDPH rate (82% vs. 80%, p=0.83), severity of PDPH (severe 36% vs. 23%, p=0.34), need for EBP (57% vs. 54%, p=0.81)
25 Needle Size as a Risk Factor Needle size = PDPH due to CSF loss/dural hole size CSF loss with 22- vs. 25-G Quincke vs ml/min AA 1989;69: Meta-analysis of 16 RCTs Anesthesiology 1994;81: Incidence of PDPH: less with smaller needles Also, significant reduction in the incidence of severe PDPH with smaller needles No effect of needle size on back pain or failure rate
26 Needle Size as a Risk Factor Needle size in parturients Systematic review of 51 articles CJA 2003;50:460-9 Meta-analysis of PDPH for epidural needles = 52.1% For parturients: 1.5% risk of accidental dural puncture Pooled incidence of PDPH: Husted 18-G = 41.3% Quincke 25-G = 6.3% Sprotte 24-G = 3.5% Whitacre 25-G = 2.2%
27 Needle Shape as a Risk Factor Non-cutting (Whitacre) vs. cutting (Quincke) Meta-analysis of 16 RCTs Anesthesiology 1994;81: Incidence of PDPH significantly less with non-cutting vs. cutting needles Also, significant reduction in the incidence of severe PDPH with non-cutting needles Pencil point needles may cause more trauma and the resulting inflammatory response may close the dural hole faster RAPM 2000;25:
28 Figure 1: Dural lesions produced by 25-G Quincke needles (perpendicular [A] and parallel [B]). Dural surface observed from the epidural space. Reg Anesth Pain Med 2000;25: Figure 2: Dural lesions produced by 25-G Quincke needle observed from subarachnoid space. Note the clean-cut produced in the edges of the lesion
29 Reg Anesth Pain Med 2000;25: Figure 3: Dural lesion produced with a 25-G Whitacre needle seen from the external (epidural) surface. Note the flaps of collagen fibers at the borders of the lesions Figure 4: Dural lesions produced by 25-G Whitacre needles observed from the subarachnoid space. Note the flaps of fibers at the edge of the lesions and the ripple effect around the hole.
30 Bevel Orientation:? Risk Factor Bevel orientation: parallel vs. perpendicular Theory: longitudinal (parallel) insertion will PDPH as dural fibers more likely be spread than cut thus CSF leakage This assume dural fibers runs longitudinally (controversial) Human dura models: fluid leakage greater when bevel inserted perpendicular vs. parallel 30% lower rate of leakage with parallel vs. perpendicular Anesth Analg 1989;69:457-60
31 Bevel Orientation is a Risk Factor Anesth Analg 1989;69:457-60
32 Bevel Orientation is a Risk Factor OR= 0.29 (0.17,0.50); p< Neurologist 2006;12:224-8
33 Midline vs Paramedian Human dura models: transdural fluid leak when needle inserted at 30 vs. 90 Anesth Analg 1989;69: Little leakage after tangential entry (20- to 25-G Quincke) even at spinal pressures as high as 55 cm H2O Headache 1977;17:64-6 Paramedian: tangential entry will create dural flaps which overlap both entry and exit puncture sites Perpendicular: creation of a tin lid flap which will allow unimpeded transdural outflow of CSF Reg Anesth 1997;22: RCT (n=150) 25-gauge Crawford needle Anesth Pain Med 2011;1:66-9 NS between midline (9.3%) vs. paramedian (10.7%)
34 Reg Anesth 1997;22: Anesth Analg 1989;69:457-60
35 Decreased Risk with IT Catheters? Use of a continuous IT catheters? PDPH Inflammatory response from catheter closure of dural hole 45 C/S pts with dural puncture Acta Anaesthesiol Scand 1994;38: /15 (33%) with EA; 8/17 (47%) with SA; 0/13 (0%) with IT Dural puncture with 16-G Husted needle CJA 1998;45:42-5 IT catheters for hours; no PDPH (n = 3) Spinal drains: 19-G needle used Only a 2.5% [95% CI: %] of patients (15/530) developed PDPH AA 1999;88:388-92
36 Decreased Risk with IT Catheters? 128 witnessed accidental dural punctures 39 EP; 89 IT catheters Acta Anesthesiol Scand 2014;58: PDPH EP = 62% vs. 42% for IT catheters PDPH with EP (vs. IT) OR = 2.2 (95%CI: ) Meta-analysis of 8 studies Internat J Obstet Anesth 2013;22;26-30 EBP with IT catheter (RR = 0.64, 95%CI: , p = 0.001) ND for PDPH with IT (RR = 0.82, 95%CI: , p = 0.06) Meta-analysis of 6 studies (no benefit with IT cath) Br J Anaesth 2010;105: Short-term IT cath (RR = 0.88, 95%CI: , p = 0.32) Long-term IT cath (RR = 0.21, 95%CI: , p = 0.23)
37 Internat J Obstet Anesth 2013;22;26-30
38 Internat J Obstet Anesth 2013;22;26-30
39 Br J Anaesth 2010;105:255-63
40
41 Conservative vs. Invasive Treatment Options Conservative: symptomatic Rx until dural puncture self-seals Invasive: physical attempt to stop leakage of CSF Surveys of management of PDPH Nordic survey (n=153 OB anesth) Acta Anaesth Scand 2011;55: % parturients received EP, EBP = 86% Most common time from Dx to EBP = h N. Am. survey (n = 843 SOAP members) J Clin Anesth 2011;23: After accidental dural puncture (ADP) 75% EP, 25% IT EBP = 81% w/in 24 h after ADP
42 Treatment Options: Conservative Attenuate symptoms until puncture naturally closes Analgesic agents: oral or systemic (NSAIDs, opioids) Hydration: patients may be underhydrated due to nausea Oral fluid intake has not been shown to decrease incidence of PDPH Eur Arch Psychiatr Neurol Sci 1988;237:194-6 Bedrest: will not prevent development of PDPH Lancet 1981;ii: Cochrane Database Syst Rev. 2002;(2):CD001790
43 Treatment Options: Conservative Conservative therapy (%) used by North American OB anesthesiologists after onset of PDPH J Clin Anesth 2011;23:349-60
44 Treatment Options: Conservative Review of RCTs - pharmacologic drugs treating PDPH 13 RCTs (n = 479); unable to perform meta-analysis Caffeine = effective for treating PDPH Pain scores = Gabapentin, hydrocortisone, theophylline Lack of conclusive evidence = sumatriptan, adrenocorticotropic hormone (ATCH), pregabalin, cosyntropin Cochrane Database Syst Rev 2015;CD007887
45 Treatment Options: Caffeine Mechanism of action: cerebral vasoconstriction Caffeine withdrawal cerebral blood flow Psychopharm 2000;147:371-7 May also act through adenosine receptors Neurolog 2001;7: Treatment: IV (500mg caffeine sodium benzoate) or PO 70% efficacy but relief only temporary Ann Pharmacother 1996;30:831-9 May be effective when given prophylactically RAPM 1999;24:51-4 RCT in 60 patients for SA (22-G Quincke) Moderate-severe PDPH less with caffeine Caffeine = 3/30 (10%) vs. Saline = 11/30 (37%), p = 0.03
46 Treatment Options: Steroids Hydrocortisone J Anaesthesiol Clin Pharmacol 2012;28:190-3 RCT (n = 60): hydrocortisone 100mg IV vs placebo At 6 h, VAS with hydrocortisone (6.0 vs. 2.1, p<0.0001) At 24 h, VAS with hydrocortisone (3.8 vs. 1.9, p<0.0001) At 48 h, VAS with hydrocortisone (2.0 vs. 1.1, p<0.0001) Dexamethasone RCT (n = 178); 8 mg IV vs. placebo Acta Anaesthesiol Belg 2011;62:143-6 Intensity of PDPH with dexamethasone RCT (n = 372); 8 mg IV vs. placebo Acta Neurol Belg 2012;112: Severity and incidence of PDPH with dexamethasone
47 Treatment Options: Gabapentanoids Pregabalin J Clin Neurosci 2011;18: RCT; pregabalin (150mg x 3d, then 300mg x 2d) vs. placebo Pregabalin = VAS pain scores and diclofenac requirements Gabapentin Pak J Pharm Sci 2014;27: RCT (n=120); gabapentin 300mg x 2 vs. placebo Gabapentin = VAS pain scores at 24 h Gabapentin vs. ergotamine/caffeine Adv Med Sci 2011;56:25-9 RCT (n=42); Gabapentin = VAS pain vs. ergotamine/caffeine Gabap. vs. pregab. vs. acetaminophen Saudi J Anaesth 2014;8:374-7 RCT (n=90); treatment x 3 days Pain scores = pregabalin < gabapentin < acetaminophen
48 Treatment Options: Others Cosyntropin (ACTH analogue) Anesthesiology 2010;113; RCT (n=90); cosyntropin 1 mg IV vs. saline Cosyntropin = PDPH (33% VS. 69%, P = 0.001), ebp (11% VS. 29%, P = 0.035), time to PDPH development (17.5 h) Mechanism? = aldosterone (salt retention), CSF, morphine Ondansetron J Anesth 2015 (in press) RCT (n = 210): 0.15 mg/kg ondansetron vs. placebo Ondansetron = PDPH (5% vs. 21%, p = 0.001) Mechanism? = venodilation in brain
49 Anesthesiology 2010;113;413-20
50
51 Treatment Options: Invasive Epidural blood patch (EBP): considered definitive Rx Immediate relief: mass effect intracranial pressure MRI: mass effect immediately after EBP BJA 1993;71:182-8 Injection of blood into epidural space may result in cerebral vasoconstriction; HA relief RAPM 2001;26:401-6 Long-term relief due to sealant effect of blood over the dural puncture allowing replenishment of lost CSF 6-7 hours after EBP, MRI evaluation demonstrated a thin layer of clot over the dural puncture BJA 1993;71:182-8 Fibroblastic activity over dural puncture seen at 48 hours; collagen deposition seen at 2 weeks AA 1972;51:226-32
52 Epidural Blood Patch Ideal volume, timing of EBL uncertain (15 20 ml) Initial report used only 2 3 ml Anesthesiology 1960;21:565-6 Timing (prophylactic vs. delayed) still controversial Typical reported efficacy of 90-95% may be misleading Anesthesiology 2001;95:334-9 Prospective observational study of 504 EBP for PDPH Complete relief = 75%, incomplete relief = 18%, failure = 7% Failure of EBP was associated with: Needle diameter < 20-G (p < 0.001) Administration of EBP < 4 days (p = 0.037) EBP may be more likely performed in severe PDPH leakage of CSF from large needles
53 incidence of headache is not as high as anticipated when a bloody tap is produced.. (in a patient with PDPH)..Two milliliters of the patient s own blood was injected into the epidural space immediate relief from pain (Dr. Gormley s personal experience who had a postural HA after myelogram) a colleague injected 3 cc. of blood into (Dr. Gormley s) epidural space. headache disappeared with minutes. Anesthesiology 1960;21:565-6
54 Epidural Blood Patch: Prophylactic vs. Therapeutic? Several reviews do not recommend prophylactic EBP over other treatments due to insufficient evidence Cochrane Database Syst Rev 2010;20:CD001791; Anesth Analg 2012;115:133-6 EBP is not a risk-free procedure Some meta-analyses prophylactic EBP may be of benefit 5 non-rct, prophylactic EBP = PDPH (RR = 0.48, 95%CI: 0.23/0.99, p = 0.05) Br J Anaesth 2010;105: RCT, prophylactic EBP = ND in PDPH (RR = 0.25, p = 0.06) 4 RCT (n=173); median quality score = 2 (out of 5) Acta Anaesthesiol Scand 2013;57: Prophylactic EBP = PDPH (RD = -0.48, p = 0.017)
55 Br J Anaesth 2010;105:255-63
56 EBP: How Much Blood to Use? RCT (n=121) 15, 20, 30 ml of blood Anesth Analg 2011 ;113: Partial HA relief = 61%, 73%, 67%, respectively Complete HA relief = 10%, 32%, 26%. Respectively Optimal dose = 20 ml Study of epidural pressure during EBP Internat J Obstet Anesth 2014;23: Injection of blood until mild back pressure or discomfort Mean final volume = 18.9 ± 7.8 ml N. Am. survey (n=843 SOAP members) J Clin Anesth 2011;23:349-60
57 Epidural Blood Patch EBP does not impair subsequent epidural anesthesia 96.6% success in patients with prior EBP AA 1999;89:390-4 Complications (mostly transient): Discomfort (78%) and pain (54%) Anesthesiology 2001;95:334-9 Lower extremity sensory disturbances and weakness (18%), neck discomfort, radicular pain, bradycardia Rare (case reports) but potentially severe Facial nerve paralysis Reg Anesth 1993;18:196-8 Pneumocephalus Ann Emerg Med 1994;23: Meningeal irritation Anesth Analg 1998;87: Permanent paraparesis and cauda equina syndrome (30 ml of blood injected) Anesthesiology 2002;96:1515-7
58 EBP and Infections Concern for the introduction of spreading infection or cancer into the EP/IT space EBP in HIV patients Anesthesiology 1992;76: sero(+), 2 sero(-) received EBP, no adverse neurologic or infectious sequelae in f/u up to 24 months EBP in acute varicella Anesth Analg 2004;99: Asymptomatic 30 d and 1 year after EBP EBP in ALL patient Pain Med 2014;15: Flow cytometry no circulating blasts in peripheral blood No evidence of CNS ALL at 3 months Use of allogenic blood for EBP Int J Obstet Anesth 2005;14:261-2 Postpartum fever concern that blood infected
59 Other Invasive Treatments Epidural Saline (ES): Like EBP, ES is thought to immediately alleviate PDPH by increasing both epidural and lumbar CSF pressures This in turn will increase intracerebral CSF pressures and decrease traction on pain sensitive cranial structures Less effective than EBP, relief is transient Dextran: mechanisms of action presumably similar to ES Fibrin glue: case report of successful treatment after epidural injection of fibrin glue Anesthesiology 1999;91:576-7 Surgical closure: only for the most severe and refractory cases Cephalalgia 2013;33:
60
61 Summary Pathophysiology CSF leakage Clinical presentation PDPH is a diagnosis of exclusion Risk factors Patient-related: age, gender Needle-related: size and shape Treatment options Conservative therapy Epidural blood patch
Post-Dural Puncture Headache. Dr. Jacobs Aurélie Krans Anesthesie 18/03/2016 Kliniek St.-Jan, Brussel
 Post-Dural Puncture Headache Dr. Jacobs Aurélie Krans Anesthesie 18/03/2016 Kliniek St.-Jan, Brussel I - PATHOPHYSIOLOGY August Bier (intrathecal cocaïn1898)! first 2 cases PDPH CSF leak trough dura mater
Post-Dural Puncture Headache Dr. Jacobs Aurélie Krans Anesthesie 18/03/2016 Kliniek St.-Jan, Brussel I - PATHOPHYSIOLOGY August Bier (intrathecal cocaïn1898)! first 2 cases PDPH CSF leak trough dura mater
Postdural puncture headache preventing the impossible, treating the symptoms, evaluating long term effects.
 Postdural puncture headache preventing the impossible, treating the symptoms, evaluating long term effects. Marc Van de Velde, MD, PhD Professor of Anaesthesia, Catholic University Leuven (KUL) Chair Department
Postdural puncture headache preventing the impossible, treating the symptoms, evaluating long term effects. Marc Van de Velde, MD, PhD Professor of Anaesthesia, Catholic University Leuven (KUL) Chair Department
Dural Puncture Headache: How to Prevent It and What to Do When It Happens Kathleen A. Smith, M.D. University of North Carolina, Chapel Hill, NC
 Session: L125 Session: L338 Dural Puncture Headache: How to Prevent It and What to Do When It Happens Kathleen A. Smith, M.D. University of North Carolina, Chapel Hill, NC Disclosures: This presenter has
Session: L125 Session: L338 Dural Puncture Headache: How to Prevent It and What to Do When It Happens Kathleen A. Smith, M.D. University of North Carolina, Chapel Hill, NC Disclosures: This presenter has
Case Discussions Cynthia A. Wong, M.D.
 Case Discussions Cynthia A. Wong, M.D. Association des Anesthѐsiologistes du Quѐbec April 2014 CASE 1 Maternal Mortality Lewis G (ed). CEMACH 2007. Saving Mothers Lives 2003-2005 Pregnancy Complications
Case Discussions Cynthia A. Wong, M.D. Association des Anesthѐsiologistes du Quѐbec April 2014 CASE 1 Maternal Mortality Lewis G (ed). CEMACH 2007. Saving Mothers Lives 2003-2005 Pregnancy Complications
PDPH: To Patch or Not to Patch
 PDPH: To Patch or Not to Patch Moderators: 1. Kim Strupp, MD FAAP Assistant Professor of Anesthesiology, Children s Hospital Colorado/University of Colorado, Aurora, CO 2. Debnath Chatterjee, MD Associate
PDPH: To Patch or Not to Patch Moderators: 1. Kim Strupp, MD FAAP Assistant Professor of Anesthesiology, Children s Hospital Colorado/University of Colorado, Aurora, CO 2. Debnath Chatterjee, MD Associate
Frank Rosemeier. MD, MRCP(UK), MRCA, DipPEC(SA) Attending Anesthesiologist. JLR Medical Group
 Postdural Puncture Headaches A Contemporary Update Frank Rosemeier MD, MRCP(UK), MRCA, DipPEC(SA) Attending Anesthesiologist JLR Medical Group Maitland, FL Why should we care? Mother want to feel well
Postdural Puncture Headaches A Contemporary Update Frank Rosemeier MD, MRCP(UK), MRCA, DipPEC(SA) Attending Anesthesiologist JLR Medical Group Maitland, FL Why should we care? Mother want to feel well
(แทงข างหล ง...ร าวไปถ งห ว)
 From Back to Head (แทงข างหล ง...ร าวไปถ งห ว) 23 Jul 2018 Natinee Benjangkhaprasert Phonneeya Nimpunyakampong Advisor Lecturer Choopong Luansritisakul 1 Case 62 year-old Thai male Diagnosis: CA Colon
From Back to Head (แทงข างหล ง...ร าวไปถ งห ว) 23 Jul 2018 Natinee Benjangkhaprasert Phonneeya Nimpunyakampong Advisor Lecturer Choopong Luansritisakul 1 Case 62 year-old Thai male Diagnosis: CA Colon
POSTPARTUM MANAGEMENT OF DURAL PUNCTURE
 Document Ref: MAT 0145 WOMEN AND CHILDREN S and CLINICAL SUPPORT SERVICES DIVISION Clinical Guideline POSTPARTUM MANAGEMENT OF DURAL PUNCTURE For use in: (Clinical Area) For use by: (Staff Group) Distributed
Document Ref: MAT 0145 WOMEN AND CHILDREN S and CLINICAL SUPPORT SERVICES DIVISION Clinical Guideline POSTPARTUM MANAGEMENT OF DURAL PUNCTURE For use in: (Clinical Area) For use by: (Staff Group) Distributed
Post-dural puncture headache in pregnant women: What have we learned?
 Rev. Col. Post-dural Anest. 34: puncture 267-272, headche 2006 ARTÍCULO DE REVISIÓN Post-dural puncture headache in pregnant women: What have we learned? Krzysztof M. Kuczkowski, M.D.* ABSTRACT: The obstetric
Rev. Col. Post-dural Anest. 34: puncture 267-272, headche 2006 ARTÍCULO DE REVISIÓN Post-dural puncture headache in pregnant women: What have we learned? Krzysztof M. Kuczkowski, M.D.* ABSTRACT: The obstetric
The spinal headache in pregnant women
 N. J. Obstet. Gynaecol Vol. 1, No. 2, p. 4-9 Nov-Dem 2006 REVIEW The spinal headache in pregnant women Krzysztof M. Kuczkowski Departments of Anesthesiology and Reproductive Medicine, University of California,
N. J. Obstet. Gynaecol Vol. 1, No. 2, p. 4-9 Nov-Dem 2006 REVIEW The spinal headache in pregnant women Krzysztof M. Kuczkowski Departments of Anesthesiology and Reproductive Medicine, University of California,
Post-Dural Puncture Headache(PDPH): an update. Dorel Sandesc
 Post-Dural Puncture Headache(PDPH): an update Dorel Sandesc August Bier 1898: a personal experience of post dural puncture headache Toward the evening I was forced to take to bed and remained there for
Post-Dural Puncture Headache(PDPH): an update Dorel Sandesc August Bier 1898: a personal experience of post dural puncture headache Toward the evening I was forced to take to bed and remained there for
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Complications of Neuraxial Anesthesia An Ounce of Prevention is Worth a Pound of Cure
 Complications of Neuraxial Anesthesia An Ounce of Prevention is Worth a Pound of Cure Brian J Kasson CRNA MHS Faculty/Clinical Instructor Nurse Anesthesia Program Northern Kentucky University Staff Nurse
Complications of Neuraxial Anesthesia An Ounce of Prevention is Worth a Pound of Cure Brian J Kasson CRNA MHS Faculty/Clinical Instructor Nurse Anesthesia Program Northern Kentucky University Staff Nurse
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Effective Epidural Blood Patch Volumes for Postdural Puncture Headache in Taiwanese Women
 ORIGINAL ARTICLE Effective Epidural Blood Patch Volumes for Postdural Puncture Headache in Taiwanese Women Li-Kuei Chen, 1 Chi-Hsiang Huang, 1 Wei-Horng Jean, 2 Cheng-Wei Lu, 2 Chen-Jung Lin, 1 Wei-Zen
ORIGINAL ARTICLE Effective Epidural Blood Patch Volumes for Postdural Puncture Headache in Taiwanese Women Li-Kuei Chen, 1 Chi-Hsiang Huang, 1 Wei-Horng Jean, 2 Cheng-Wei Lu, 2 Chen-Jung Lin, 1 Wei-Zen
Sudden Headache and visual disturbances in a young woman
 Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Spontaneous Intracranial Hypotension Diagnosis and Treatment
 Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Mechanisms of Headache in Intracranial Hypotension
 Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
Mechanisms of Headache in Intracranial Hypotension Stephen D Silberstein, MD Jefferson Headache Center Thomas Jefferson University Hospital Philadelphia, PA Stephen D. Silberstein, MD, FACP Director, Jefferson
EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics
 Appendix 2: Case Report Form EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics Case Report Form Please fill each relevant step carefully Step 1. From Epidural
Appendix 2: Case Report Form EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics Case Report Form Please fill each relevant step carefully Step 1. From Epidural
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics
 Appendix 3: Pre-study Questionnaire EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics All questions in this questionnaire relate to the situation in 2014
Appendix 3: Pre-study Questionnaire EPiMAP Obstetrics European Practices in the Management of Accidental Dural Puncture in Obstetrics All questions in this questionnaire relate to the situation in 2014
PDPH and FOCAL NEUROLOGIC DEFICIT after obstetric regional anesthesia
 PDPH and FOCAL NEUROLOGIC DEFICIT after obstetric regional anesthesia Eva Roofthooft, MD Consultant Anesthetist, Department of Anesthesiology, ZNA Middelheim and Paola Children s Hospital, Antwerp Marc
PDPH and FOCAL NEUROLOGIC DEFICIT after obstetric regional anesthesia Eva Roofthooft, MD Consultant Anesthetist, Department of Anesthesiology, ZNA Middelheim and Paola Children s Hospital, Antwerp Marc
Swiss Association of Obstetric Anesthesia Swiss Association of Anesthesia & Resuscitation Satellite Meeting Interlaken, Switzerland 2007 Lawrence C.
 CSE s for Labor Analgesia PRO! Swiss Association of Obstetric Anesthesia Swiss Association of Anesthesia & Resuscitation Satellite Meeting Interlaken, Switzerland 2007 Lawrence C. Tsen, MD Director of
CSE s for Labor Analgesia PRO! Swiss Association of Obstetric Anesthesia Swiss Association of Anesthesia & Resuscitation Satellite Meeting Interlaken, Switzerland 2007 Lawrence C. Tsen, MD Director of
Continuous Spinal Anaesthesia
 Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
Continuous Spinal Anaesthesia Ph. Biboulet Department of Anesthesiology and Critical Care Medicine, Lapeyronie University Hospital, Montpellier France CSA story : 1906 Dean 1944 Tuohy 1991 CSA revisited
Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital
 Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital Overview Review overall (ERAS and non-eras) data for EA, PVB, TAP Examine
Show Me the Evidence: Epidurals, PVBs, TAP Blocks Christopher L. Wu, MD Professor of Anesthesiology The Johns Hopkins Hospital Overview Review overall (ERAS and non-eras) data for EA, PVB, TAP Examine
Anesthesiology ROUNDS. The Epidural Blood Patch: Beyond the Post-dural Puncture Headache. Anesthesia. Volume 8, Issue 5
 2010 Volume 8, Issue 5 Anesthesiology ROUNDS A PHYSICIAN LEARNING RESOURCE FROM THE UNIVERSITY OF MONTREAL AND McGILL UNIVERSITY FACULTIES OF MEDICINE The Epidural Blood Patch: Beyond the Post-dural Puncture
2010 Volume 8, Issue 5 Anesthesiology ROUNDS A PHYSICIAN LEARNING RESOURCE FROM THE UNIVERSITY OF MONTREAL AND McGILL UNIVERSITY FACULTIES OF MEDICINE The Epidural Blood Patch: Beyond the Post-dural Puncture
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Postpartum headache: diagnosis and management
 : diagnosis and management A Sabharwal MBChB FRCA GM Stocks BSc MB BS FRCA Matrix reference 2B04,3B00 Key points Anaesthetists need to be aware of the differential diagnoses of postpartum headache as they
: diagnosis and management A Sabharwal MBChB FRCA GM Stocks BSc MB BS FRCA Matrix reference 2B04,3B00 Key points Anaesthetists need to be aware of the differential diagnoses of postpartum headache as they
Ventricles, CSF & Meninges. Steven McLoon Department of Neuroscience University of Minnesota
 Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Differential Diagnosis of Orthostatic Headache
 Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Intravenous Cosyntropin Versus Epidural Blood Patch for Treatment of Postdural Puncture Headache
 Pain Medicine 2016; 17: 1337 1342 doi: 10.1093/pm/pnw014 HEADACHE & FACIAL PAIN SECTION Original Research Article Intravenous Cosyntropin Versus Epidural Blood Patch for of Postdural Puncture Headache
Pain Medicine 2016; 17: 1337 1342 doi: 10.1093/pm/pnw014 HEADACHE & FACIAL PAIN SECTION Original Research Article Intravenous Cosyntropin Versus Epidural Blood Patch for of Postdural Puncture Headache
Comparing the effect of pregabalin, gabapentin, and acetaminophen on post-dural puncture headache
 Page 374 ORIGINAL ARTICLE Comparing the effect of pregabalin, gabapentin, and acetaminophen on post-dural puncture headache Alireza Mahoori, Heydar Noroozinia, Ebrahim Hasani, Hadi Saghaleini Department
Page 374 ORIGINAL ARTICLE Comparing the effect of pregabalin, gabapentin, and acetaminophen on post-dural puncture headache Alireza Mahoori, Heydar Noroozinia, Ebrahim Hasani, Hadi Saghaleini Department
CSE Analgesia Represents the Gold Standard for Regional Analgesia in Labour
 CSE Analgesia Represents the Gold Standard for Regional Analgesia in Labour Dr Jason Reidy Nuffield Department of Anaesthetics Oxford University Hospitals CSE analgesia does not represent the gold standard
CSE Analgesia Represents the Gold Standard for Regional Analgesia in Labour Dr Jason Reidy Nuffield Department of Anaesthetics Oxford University Hospitals CSE analgesia does not represent the gold standard
Post-Dural Puncture Headache Following Spinal Anaesthesia: Comparison of 25g Vs 29g Spinal Needles
 Bahrain Medical Bulletin, Vol.24, No.4, December 2002 Post-Dural Puncture Headache Following Spinal Anaesthesia: Comparison of 25g Vs 29g Spinal Needles V.K. Grover, MD, MNAMS* Rajesh Mahajan, MD** Indu
Bahrain Medical Bulletin, Vol.24, No.4, December 2002 Post-Dural Puncture Headache Following Spinal Anaesthesia: Comparison of 25g Vs 29g Spinal Needles V.K. Grover, MD, MNAMS* Rajesh Mahajan, MD** Indu
Spontaneous Intracranial Hypotension Following a Yoga Class: A Case Report
 American Journal of Medical Case Reports, 2015, Vol. 3, No. 10, 314-318 Available online at http://pubs.sciepub.com/ajmcr/3/10/3 Science and Education Publishing DOI:10.12691/ajmcr-3-10-3 Spontaneous Intracranial
American Journal of Medical Case Reports, 2015, Vol. 3, No. 10, 314-318 Available online at http://pubs.sciepub.com/ajmcr/3/10/3 Science and Education Publishing DOI:10.12691/ajmcr-3-10-3 Spontaneous Intracranial
Diagnostic lumbar puncture. Comparative study between 22-gauge pencil point and sharp bevel needle
 J Headache Pain (2005) 6:400 404 DOI 10.1007/s10194-005-0235-5 ORIGINAL Liisa Luostarinen Taina Heinonen Markku Luostarinen Annikki Salmivaara Diagnostic lumbar puncture. Comparative study between 22-gauge
J Headache Pain (2005) 6:400 404 DOI 10.1007/s10194-005-0235-5 ORIGINAL Liisa Luostarinen Taina Heinonen Markku Luostarinen Annikki Salmivaara Diagnostic lumbar puncture. Comparative study between 22-gauge
Low PRESSURE Headaches. What they area and what can you do? Kathleen B. Digre MD University of Utah
 Low PRESSURE Headaches aka Low CSF volume headache: What they area and what can you do? Kathleen B. Digre MD University of Utah Disclosure: I have a part ownership on a patent for thin filmed technology
Low PRESSURE Headaches aka Low CSF volume headache: What they area and what can you do? Kathleen B. Digre MD University of Utah Disclosure: I have a part ownership on a patent for thin filmed technology
LV-EBP: Record-setting large volume epidural blood patch
 LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
LV-EBP: Record-setting large volume epidural blood patch Michael D. Staudt Department of Clinical Neurological Sciences Schulich School of Medicine, Western University London Health Sciences Centre, London,
A 5-Year Audit of Accidental Dural Punctures, Postdural Puncture Headaches, and Failed Regional Anesthetics at a Tertiary-Care Medical Center
 Research Article TheScientificWorldJOURNAL (2009) 9, 715 722 ISSN 1537-744X; DOI 10.1100/tsw.2009.94 A 5-Year Audit of Accidental Dural Punctures, Postdural Puncture Headaches, and Failed Regional Anesthetics
Research Article TheScientificWorldJOURNAL (2009) 9, 715 722 ISSN 1537-744X; DOI 10.1100/tsw.2009.94 A 5-Year Audit of Accidental Dural Punctures, Postdural Puncture Headaches, and Failed Regional Anesthetics
How and why to do an epidural in dogs and cats? Which Indications and which drugs?
 AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
AMVAC/RoSAVA 2014 How and why to do an epidural in dogs and cats? Which Indications and which drugs? Prof. Yves Moens Dipl ECVAA Why do epidurals? A part of a balanced anesthesia A means to provide analgesia
Neurological Complications of the Parturient
 Neurological Complications of the Parturient M. Roseann Diehl, CRNA, DNP, PhDc Associate Professor Professional Practice TCU School of Nurse Anesthesia Fort Worth, Texas Sanford Health, Fargo, ND roseanncannon@gmail.com
Neurological Complications of the Parturient M. Roseann Diehl, CRNA, DNP, PhDc Associate Professor Professional Practice TCU School of Nurse Anesthesia Fort Worth, Texas Sanford Health, Fargo, ND roseanncannon@gmail.com
Insertion of an intrathecal catheter following accidental dural puncture: a meta-analysis
 International Journal of Obstetric Anesthesia (2013) 22, 26 30 0959-289X/$ - see front matter c 2012 Elsevier Ltd. All rights reserved. http://dx.doi.org/10.1016/j.ijoa.2012.10.004 REVIEW ARTICLE Insertion
International Journal of Obstetric Anesthesia (2013) 22, 26 30 0959-289X/$ - see front matter c 2012 Elsevier Ltd. All rights reserved. http://dx.doi.org/10.1016/j.ijoa.2012.10.004 REVIEW ARTICLE Insertion
Marcel Vercauteren. Symptomatology and diagnosis
 Update in Post-Dural Puncture Headache: the do s and don ts? Marcel Vercauteren 183 Post-Dural Puncture Headache (PDPH) is a well-known complication of intended dural puncture (anesthesia, diagnostic),
Update in Post-Dural Puncture Headache: the do s and don ts? Marcel Vercauteren 183 Post-Dural Puncture Headache (PDPH) is a well-known complication of intended dural puncture (anesthesia, diagnostic),
Initiating Labour Analgesia in 2020: Predicting the Future Epidurals, CSEs, Spinal Catheters, Epidrum & Epiphany
 Initiating Labour Analgesia in 2020: Predicting the Future Epidurals, CSEs, Spinal Catheters, Epidrum & Epiphany Kenneth E Nelson, M.D. Associate Professor Wake Forest University, North Carolina, USA Initiating
Initiating Labour Analgesia in 2020: Predicting the Future Epidurals, CSEs, Spinal Catheters, Epidrum & Epiphany Kenneth E Nelson, M.D. Associate Professor Wake Forest University, North Carolina, USA Initiating
Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai. Interventional Options
 10/20/2017 Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai Charles Luoy and Marcel Maya Cedars Sinai Blood Patch Single level Bilevel Targeted Fibrin Glue Interventional Options 1 10/20/2017
10/20/2017 Current & Evolving Percutaneous Treatment Approaches: Cedars-Sinai Charles Luoy and Marcel Maya Cedars Sinai Blood Patch Single level Bilevel Targeted Fibrin Glue Interventional Options 1 10/20/2017
Myelogram and Lumbar Puncture: Pre and Post Procedure Details
 Myelogram and Lumbar Puncture: Pre and Post Procedure Details (Revised October 2011) 1) Patients should be well hydrated. No solid food after midnight but clear liquids in the a.m. 2) Patients who take
Myelogram and Lumbar Puncture: Pre and Post Procedure Details (Revised October 2011) 1) Patients should be well hydrated. No solid food after midnight but clear liquids in the a.m. 2) Patients who take
Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch
 J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
J Neurosurg Spine 9:000 000, 9:483 487, 2008 Occult cervical (C1 2) dural tear causing bilateral recurrent subdural hematomas and repaired with cervical epidural blood patch Case report As o k u m a r
Remembering Donald J. Dalessio, MD The Headache Clinic Featuring the Baylor Scott & White Headache Clinic in Temple, Texas.
 Spinal Cerebrospinal Fluid Leak An Under-recognized Cause of Headache More common than expected, why is this type of headache so often misdiagnosed or the diagnosis is delayed? Challenging the One Size
Spinal Cerebrospinal Fluid Leak An Under-recognized Cause of Headache More common than expected, why is this type of headache so often misdiagnosed or the diagnosis is delayed? Challenging the One Size
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology University of Washington, Seattle, WA
 ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
ASA Closed Claims Project: Regional Anesthesia Claims 1990 or later Lorri A. Lee MD Department of Anesthesiology, Seattle, WA OVERVIEW 1. Closed Claims Project 2. Peripheral Nerve Blocks 3. Neuraxial Claims
Combined spinalepidural. epidural analgesia in labour (review) By Neda Taghizadeh
 Combined spinalepidural versus epidural analgesia in labour (review) By Neda Taghizadeh Cochrane review Cochrane collaboration was founded in 1993 and is named after Archie Cochrane (1909-1988), British
Combined spinalepidural versus epidural analgesia in labour (review) By Neda Taghizadeh Cochrane review Cochrane collaboration was founded in 1993 and is named after Archie Cochrane (1909-1988), British
Post dural puncture headache in ceasarean sections A study with 25 gauze quincke needle
 Original article Pravara Med Rev 2011; 3(2) Post dural puncture headache in ceasarean sections A study with 25 gauze quincke needle Zafarullah Beigh *, Mohamad Ommid *, Arun Kumar Gupta **, Shabir Akhoon
Original article Pravara Med Rev 2011; 3(2) Post dural puncture headache in ceasarean sections A study with 25 gauze quincke needle Zafarullah Beigh *, Mohamad Ommid *, Arun Kumar Gupta **, Shabir Akhoon
MANAGEMENT OF ACCIDENTAL DURAL PUNCTURE
 MANAGEMENT OF ACCIDENTAL DURAL PUNCTURE This guideline gives some clinical background information and management suggestions that are appropriate at our hospital when faced with an accidental dural puncture.
MANAGEMENT OF ACCIDENTAL DURAL PUNCTURE This guideline gives some clinical background information and management suggestions that are appropriate at our hospital when faced with an accidental dural puncture.
Lumbar cistern is site of lumbar puncture for removal of CSF sample LC contains cauda equina. Anatomical Review
 Lumbar Puncture Lumbar cistern is site of lumbar puncture for removal of CSF sample LC contains cauda equina Anatomical Review Anatomical review Overview An LP (lumbar puncture) is an invasive diagnostic
Lumbar Puncture Lumbar cistern is site of lumbar puncture for removal of CSF sample LC contains cauda equina Anatomical Review Anatomical review Overview An LP (lumbar puncture) is an invasive diagnostic
While some patients with SIH recover without intervention
 ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
ORIGINAL RESEARCH P.H. Luetmer K.M. Schwartz L.J. Eckel C.H. Hunt R.E. Carter F.E. Diehn When Should I Do Dynamic CT Myelography? Predicting Fast Spinal CSF Leaks in Patients with Spontaneous Intracranial
Introduction to Obstetric Anesthesia
 Introduction to Obstetric Anesthesia Dr A Alberts Department of Anesthesiology and Critical Care 2007 INTRODUCTION During obstetric anesthesia the anesthetist controls the following Maternal Gas exchange,
Introduction to Obstetric Anesthesia Dr A Alberts Department of Anesthesiology and Critical Care 2007 INTRODUCTION During obstetric anesthesia the anesthetist controls the following Maternal Gas exchange,
INTRODUCTION MAIN BODY. Abhijit S. Nair and Basanth Kumar Rayani
 Review Article Korean J Pain 2017 April; Vol. 30, No. 2: 93-97 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2017.30.2.93 Sphenopalatine ganglion block for relieving postdural puncture headache:
Review Article Korean J Pain 2017 April; Vol. 30, No. 2: 93-97 pissn 2005-9159 eissn 2093-0569 https://doi.org/10.3344/kjp.2017.30.2.93 Sphenopalatine ganglion block for relieving postdural puncture headache:
OB Div News March 2009
 OB Div News March 2009 Several articles in this month s review have come from Canadian institutions. In spite of my pride in being Canadian, which was enhanced during the Olympics, this is purely coincidental.
OB Div News March 2009 Several articles in this month s review have come from Canadian institutions. In spite of my pride in being Canadian, which was enhanced during the Olympics, this is purely coincidental.
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
 Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
Ian Carroll MD, MS https://med.stanford.edu/profiles/ian-carroll CarrollCSFleak@gmail.com SIH and/or POTS? Disclosures No Conflicts of Interest This work is supported by the Considine CSF Leaks Fund Thank
Post-dural Puncture Headache in the Obstetric Patient: Needle Size, Number of Dural Puncture and Timing of Ambulation
 http://www.ijwhr.net Open Access doi 10.15296/ijwhr.2015.34 Original Article Post-dural Puncture Headache in the Obstetric Patient: Needle Size, Number of Dural Puncture and Timing of Ambulation Sousan
http://www.ijwhr.net Open Access doi 10.15296/ijwhr.2015.34 Original Article Post-dural Puncture Headache in the Obstetric Patient: Needle Size, Number of Dural Puncture and Timing of Ambulation Sousan
Obstetrical Anesthesia. Safe Pain Relief for Childbirth
 Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
Obstetrical Anesthesia Safe Pain Relief for Childbirth Introduction Pain relief (analgesia) for labor and delivery is now safer than ever. In the United States approximately two-thirds of all women receive
The Safety of Lumbar Punctures. Samuel Frank, MD
 The Safety of Lumbar Punctures Samuel Frank, MD Risk Factors Modifiable Non-Modifiable Gauge of spinal needle Needle shape Bevel orientation & angle of insertion Stylet replacement Operator experience
The Safety of Lumbar Punctures Samuel Frank, MD Risk Factors Modifiable Non-Modifiable Gauge of spinal needle Needle shape Bevel orientation & angle of insertion Stylet replacement Operator experience
Efficacy of postoperative epidural analgesia Block B M, Liu S S, Rowlingson A J, Cowan A R, Cowan J A, Wu C L
 Efficacy of postoperative epidural analgesia Block B M, Liu S S, Rowlingson A J, Cowan A R, Cowan J A, Wu C L CRD summary This review evaluated the efficacy of post-operative epidural analgesia. The authors
Efficacy of postoperative epidural analgesia Block B M, Liu S S, Rowlingson A J, Cowan A R, Cowan J A, Wu C L CRD summary This review evaluated the efficacy of post-operative epidural analgesia. The authors
Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage
 DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
DOI 10.1186/s40064-016-3775-z CASE STUDY Open Access Diagnosis and treatment of spontaneous intracranial hypotension due to cerebrospinal fluid leakage Yake Zheng 1, Yajun Lian 1*, Chuanjie Wu 1, Chen
Trust Guideline for the Management of Inadvertent Dural Puncture and Post Dural Puncture Headache in Obstetrics
 A clinical guideline recommended for use In: By: For: Key words: Written by: Delivery Suite All Anaesthetic Staff Women in labour who have had an inadvertent dural puncture when having an epidural sited
A clinical guideline recommended for use In: By: For: Key words: Written by: Delivery Suite All Anaesthetic Staff Women in labour who have had an inadvertent dural puncture when having an epidural sited
Ghulam Murtaza, Akhtar Aziz Khan, Nighat Abbas and Sabahat Tariq Department of Anaesthesialogy, Nawabshah Medical College, Sindh
 IntI. Chern. Pharrn. Med. J. Vol. 2(1), pp.163-l74 (2005) FREQUENCY OF POSTDURAL PUNCTURE HEADACHE FOLLOWING SPINAL ANAESTHESIA FOR CAESAREAN SECTION: A COMPARISON BETWEEN 25-G AND 27-G PENCIL POINT SPINAL
IntI. Chern. Pharrn. Med. J. Vol. 2(1), pp.163-l74 (2005) FREQUENCY OF POSTDURAL PUNCTURE HEADACHE FOLLOWING SPINAL ANAESTHESIA FOR CAESAREAN SECTION: A COMPARISON BETWEEN 25-G AND 27-G PENCIL POINT SPINAL
CHANGES IN INTRACRANIAL PRESSURE ASSOCIATED WITH EXTRADURAL ANAESTHESIA
 Br. J. Anaesth. (1986), 58, 676680 CHANGES IN INTRACRANIAL PRESSURE ASSOCIATED WITH EXTRADURAL ANAESTHESIA H. HILT, H.J. GRAMM AND J. LINK Extradural blockade is commonly used in our clinic to provide
Br. J. Anaesth. (1986), 58, 676680 CHANGES IN INTRACRANIAL PRESSURE ASSOCIATED WITH EXTRADURAL ANAESTHESIA H. HILT, H.J. GRAMM AND J. LINK Extradural blockade is commonly used in our clinic to provide
Labor Epidural: Local Anesthetics and Beyond
 Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Eldor Epidural Kit (CSEN 68) Epidural catheter technique
 Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
Eldor Epidural Kit (CSEN 68) Epidural catheter technique Using the epidural needle the epidural space is reached by the loss of resistance technique or the hanging drop technique, while the proximal opening
ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT
 ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT Jeff Gadsden, MD, FRCPC, FANZCA Associate Professor Duke University Department of Anesthesiology Regional Anesthesia and Acute Pain Medicine DISCLOSURES
ENHANCED RECOVERY PROTOCOLS FOR KNEE REPLACEMENT Jeff Gadsden, MD, FRCPC, FANZCA Associate Professor Duke University Department of Anesthesiology Regional Anesthesia and Acute Pain Medicine DISCLOSURES
DURAL PUNCTURE EPIDURAL ANALGESIA IS NOT SUPERIOR TO CONTINUOUS LABOR EPIDURAL ANALGESIA
 DURAL PUNCTURE EPIDURAL ANALGESIA IS NOT SUPERIOR TO CONTINUOUS LABOR EPIDURAL ANALGESIA Deepak Gupta *, Arvind Srirajakalidindi *, Vitaly Soskin ** Abstract Background: Some anesthesiologists consider
DURAL PUNCTURE EPIDURAL ANALGESIA IS NOT SUPERIOR TO CONTINUOUS LABOR EPIDURAL ANALGESIA Deepak Gupta *, Arvind Srirajakalidindi *, Vitaly Soskin ** Abstract Background: Some anesthesiologists consider
Post Caesarean Analgesia An Update. Kim Ekelund MD, PhD, associate professor Rigshospitalet Copenhagen, Denmark
 Post Caesarean Analgesia An Update Kim Ekelund MD, PhD, associate professor Rigshospitalet Copenhagen, Denmark Post caesarean analgesia No Conflicts of Interests Neuraxial opioids Multimodal therapy Plan
Post Caesarean Analgesia An Update Kim Ekelund MD, PhD, associate professor Rigshospitalet Copenhagen, Denmark Post caesarean analgesia No Conflicts of Interests Neuraxial opioids Multimodal therapy Plan
PAAQS Reference Guide
 Q. 1 Patient's Date of Birth (DOB) *Required Enter patient's date of birth PAAQS Reference Guide Q. 2 Starting Anesthesiologist *Required Record the anesthesiologist that started the case Q. 3 Reporting
Q. 1 Patient's Date of Birth (DOB) *Required Enter patient's date of birth PAAQS Reference Guide Q. 2 Starting Anesthesiologist *Required Record the anesthesiologist that started the case Q. 3 Reporting
Current evidence in acute pain management. Jeremy Cashman
 Current evidence in acute pain management Jeremy Cashman Optimal analgesia Best possible pain relief Lowest incidence of side effects Optimal analgesia Best possible pain relief Lowest incidence of side
Current evidence in acute pain management Jeremy Cashman Optimal analgesia Best possible pain relief Lowest incidence of side effects Optimal analgesia Best possible pain relief Lowest incidence of side
Mr David A McDonald Service Improvement Manager Whole System patient Flow Improvement Programme Scottish Government
 Mr David A McDonald Service Improvement Manager Whole System patient Flow Improvement Programme Scottish Government Introduction Brief update Two main topics Use of Gabapentin Local Infiltration Analgesia
Mr David A McDonald Service Improvement Manager Whole System patient Flow Improvement Programme Scottish Government Introduction Brief update Two main topics Use of Gabapentin Local Infiltration Analgesia
Introduction. Eldor Spinal needle A Pencil Point Needle Invented by Prof. Joseph Eldor 1995 Double hole needle
 Eldor Spinal Needle Dr. Neeti Singh, Dr. N. Subedi, Dr. B. Shrestha, S. K. Mahargan, S. Tabdar, B. M. Shrestha and Dr. J. Agrawal KATHMANDU MEDICAL COLLEGE & NARAYANI SUBREGIONAL HOSPITAL Introduction
Eldor Spinal Needle Dr. Neeti Singh, Dr. N. Subedi, Dr. B. Shrestha, S. K. Mahargan, S. Tabdar, B. M. Shrestha and Dr. J. Agrawal KATHMANDU MEDICAL COLLEGE & NARAYANI SUBREGIONAL HOSPITAL Introduction
CSF Leaks. Abnormal communication between the subarachnoid space and the tympanomastoid space or nasal cavity. Presenting symptoms:
 CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
Confirmation with Epidurogram Necessary?
 Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Use of Fluoroscopy for Interlaminar Lumbar Epidural Injection: Is Confirmation with Epidurogram Necessary? Saeid Alemo, MD Department of Neurosurgery,Drexel University College of Medicine, Philadelphia,Pennsylvania
Nerve Blocks & Long Acting Analgesia for Plastic Surgeons. Karol A Gutowski, MD, FACS
 Nerve Blocks & Long Acting Analgesia for Plastic Surgeons Karol A Gutowski, MD, FACS Disclosures None related to this topic Why is Non-Opioid Analgesia Important Opioid epidemic Less opioid use Less PONV
Nerve Blocks & Long Acting Analgesia for Plastic Surgeons Karol A Gutowski, MD, FACS Disclosures None related to this topic Why is Non-Opioid Analgesia Important Opioid epidemic Less opioid use Less PONV
Patients and Methods. This article is featured in This Month in Anesthesiology. Please see this issue of ANESTHESIOLOGY, page 5A.
 Anesthesiology 2001; 95:334 9 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Effectiveness of Epidural Blood Patch in the Management of Post Dural Puncture Headache
Anesthesiology 2001; 95:334 9 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Effectiveness of Epidural Blood Patch in the Management of Post Dural Puncture Headache
Safety and quality of neuraxial analgesia. Ulla Sipiläinen HUCS Jorvi hospital
 Safety and quality of neuraxial analgesia Ulla Sipiläinen 6.10. 2011 HUCS Jorvi hospital Chestnut s Checklist Preparation for neuraxial labor analgesia 1.Communicate (early) with obst provider review parturient
Safety and quality of neuraxial analgesia Ulla Sipiläinen 6.10. 2011 HUCS Jorvi hospital Chestnut s Checklist Preparation for neuraxial labor analgesia 1.Communicate (early) with obst provider review parturient
SEEING KETAMINE IN A NEW LIGHT
 SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
OPUS MEDICAL B.V.B.A. Spoorwegstraat 76 B-3500 Hasselt Belgium Tel.: +32(0)11/ Fax: +32(0)11/
 LOCAL REGIONAL http://www.opusmedical.com Spinal Needles Epidural Needles Sets for Continuous Epidural Anesthesia Needles for Combined Spinal-Epidural Anesthesia Sets for Combined Spinal-Epidural Anesthesia
LOCAL REGIONAL http://www.opusmedical.com Spinal Needles Epidural Needles Sets for Continuous Epidural Anesthesia Needles for Combined Spinal-Epidural Anesthesia Sets for Combined Spinal-Epidural Anesthesia
MANAGEMENT OF THE PARTURIENT WITH COMORBID NEUROLOGICAL DISEASE - PATHWAYS TO SUCCESS
 MANAGEMENT OF THE PARTURIENT WITH COMORBID NEUROLOGICAL DISEASE - PATHWAYS TO SUCCESS LISA LEFFERT, MD CHIEF OBSTETRIC ANESTHESIA DEPARTMENT OF ANESTHESIA, CRITICAL CARE & PAIN MEDICINE MASSACHUSETTS GENERAL
MANAGEMENT OF THE PARTURIENT WITH COMORBID NEUROLOGICAL DISEASE - PATHWAYS TO SUCCESS LISA LEFFERT, MD CHIEF OBSTETRIC ANESTHESIA DEPARTMENT OF ANESTHESIA, CRITICAL CARE & PAIN MEDICINE MASSACHUSETTS GENERAL
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Post-dural puncture headache in young adults: comparison of two small-gauge spinal catheters with different needle design
 BJA Advance Access published February 18, 2005 British Journal of Anaesthesia Page 1 of 5 doi:10.1093/bja/aei100 Post-dural puncture headache in young adults: comparison of two small-gauge spinal catheters
BJA Advance Access published February 18, 2005 British Journal of Anaesthesia Page 1 of 5 doi:10.1093/bja/aei100 Post-dural puncture headache in young adults: comparison of two small-gauge spinal catheters
Coexistence of migraine and idiopathic intracranial hypertension without papilledema
 / GX'~C1~.. Coexistence of migraine and idiopathic intracranial hypertension without papilledema Ninan T. Mathew, MD; K. Ravishankar, MD; and Luis C. Sanin, MD!
/ GX'~C1~.. Coexistence of migraine and idiopathic intracranial hypertension without papilledema Ninan T. Mathew, MD; K. Ravishankar, MD; and Luis C. Sanin, MD!
ERAS: Enhanced Recovery After Surgery. Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University; Baltimore, Maryland
 ERAS: Enhanced Recovery After Surgery Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University; Baltimore, Maryland Overview History and basic principles of ERAS Review published
ERAS: Enhanced Recovery After Surgery Christopher L. Wu, M.D. Professor of Anesthesiology The Johns Hopkins University; Baltimore, Maryland Overview History and basic principles of ERAS Review published
Gastrointestinal and urinary complications in the postoperative period
 The 13 th Annual Perioperative Medicine Summit Fort Lauderdale, Florida Gastrointestinal and urinary complications in the postoperative period Dan Hunt, MD Professor of Medicine Director, Division of Hospital
The 13 th Annual Perioperative Medicine Summit Fort Lauderdale, Florida Gastrointestinal and urinary complications in the postoperative period Dan Hunt, MD Professor of Medicine Director, Division of Hospital
Continuous Wound Infusion and Postoperative Pain Current status?
 Continuous Wound Infusion and Postoperative Pain Current status? Pr Patricia Lavand homme Department of Anesthesiology St Luc Hospital University Catholic of Louvain Medical School Brussels, Belgium Severe
Continuous Wound Infusion and Postoperative Pain Current status? Pr Patricia Lavand homme Department of Anesthesiology St Luc Hospital University Catholic of Louvain Medical School Brussels, Belgium Severe
Analgesia after c delivery - wound infusions, tap blocks and intrathecal opioids; what more can we offer our patients?
 Analgesia after c delivery - wound infusions, tap blocks and intrathecal opioids; what more can we offer our patients? Ashraf S Habib, MBBCh, MSc, MHSc, FRCA Associate Professor of Anesthesiology Interim
Analgesia after c delivery - wound infusions, tap blocks and intrathecal opioids; what more can we offer our patients? Ashraf S Habib, MBBCh, MSc, MHSc, FRCA Associate Professor of Anesthesiology Interim
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
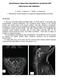 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test
 Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Intraspinal (Neuraxial) Analgesia Community Nurses Competency Test 1 Intraspinal (Neuraxial) Analgesia for Community Nurses Competency Test 1) Name the two major classifications of pain. i. ii. 2) Neuropathic
Grande half-sweet caffeine for post-dural headaches. Iona Berger January 31, 2017
 Grande half-sweet caffeine for post-dural headaches Iona Berger January 31, 2017 1 Objectives o Describe the pathophysiology and signs and symptoms of post-dural headaches o Explain the proposed mechanism
Grande half-sweet caffeine for post-dural headaches Iona Berger January 31, 2017 1 Objectives o Describe the pathophysiology and signs and symptoms of post-dural headaches o Explain the proposed mechanism
Post-dural puncture headache: pathogenesis, prevention and treatment
 British Journal of Anaesthesia 91 (5): 718±29 (2003) DOI: 10.1093/bja/aeg231 Post-dural puncture headache: pathogenesis, prevention and treatment D. K. Turnbull 1 * and D. B. Shepherd 12 1 Academic Anaesthetic
British Journal of Anaesthesia 91 (5): 718±29 (2003) DOI: 10.1093/bja/aeg231 Post-dural puncture headache: pathogenesis, prevention and treatment D. K. Turnbull 1 * and D. B. Shepherd 12 1 Academic Anaesthetic
Erik C. Hustak, MD, Mitchell P. Engle, MD, PhD, Ashwin Viswanathan, MD, and Dhanalakshmi Koyyalagunta, MD. Pain Physician 2014; 17:E405-E411
 Pain Physician 2014; 17:E405-E411 ISSN 2150-1149 Case Report Lumbar Subarachnoid Hematoma Following an Epidural Blood Patch for Meningeal Puncture Headache Related to the Implantation of an Intrathecal
Pain Physician 2014; 17:E405-E411 ISSN 2150-1149 Case Report Lumbar Subarachnoid Hematoma Following an Epidural Blood Patch for Meningeal Puncture Headache Related to the Implantation of an Intrathecal
Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities
 DOI 10.1007/s10072-013-1364-2 BRIEF COMMUNICATION Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities Angelo Franzini G. Messina L. Chiapparini G.
DOI 10.1007/s10072-013-1364-2 BRIEF COMMUNICATION Treatment of spontaneous intracranial hypotension: evolution of the therapeutic and diagnostic modalities Angelo Franzini G. Messina L. Chiapparini G.
01/07/2018 ISCHAEMIC PAIN IN NON-RECONSTRUCTABLE CRITICAL LIMB ISCHAEMIA PRESENTATION OUTLINE
 ISCHAEMIC PAIN IN NON-RECONSTRUCTABLE CRITICAL LIMB ISCHAEMIA Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE A Typical Case Background
ISCHAEMIC PAIN IN NON-RECONSTRUCTABLE CRITICAL LIMB ISCHAEMIA Dr. Áine Ní Laoire The Oxford Advanced Pain & Symptom Management Course Nottingham 27 th June 2018 PRESENTATION OUTLINE A Typical Case Background
MEDICAL POLICY SUBJECT: KETAMINE INFUSION THERAPY FOR THE TREATMENT OF CHRONIC PAIN SYNDROMES POLICY NUMBER: CATEGORY: Technology Assessment
 Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
