Chronic rhinosinusitis (CRS) is a significant health
|
|
|
- Frederick Newman
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE The safety and performance of a maxillary sinus ostium self-dilation device: a pilot study Iain Hathorn, MBChB, FRCSEd (ORL-HNS), Al-Rahim Habib, MSc, Rachelle Dar Santos, BSc, CCRP and Amin Javer, MD, FRCSC Background: Balloon dilation is now commonly used to open sinus ostia while preserving mucosa and minimizing trauma. A new maxillary sinus ostium (MSO) self-dilation device that functions on the principle of osmosis, absorbing a small amount of fluid from the surrounding tissues, can be placed into the MSO under endoscopic visualization and slowly enlarge its outer diameter. The slower dilation may further minimize tissue damage and scarring compared to the currently available balloon dilation systems. The MSO self-dilating expansion device has never been studied before in clinical trials; the purpose of this pilot study is to determine the safety and performance of the device in human subjects. Methods: Twelve chronic rhinosinusitis (CRS) patients presenting with maxillary sinus inflammation requiring FESS were enrolled. The device was inserted into the MSO at the start of surgery and removed after 60 minutes. Endoscopic evaluation for patency was performed immediately after removal, and at 1 week, 1 month, and 3 months. Adverse events were recorded intraoperatively and at each subsequent visit. Results: The device was successfully inserted in 100% of cases attempted (19/19 MSOs, 12 patients). Seventeen (89%) devices remained in the MSO for 60 minutes and dilated to a mean diameter of 4.8 ± 0.5 mm. One patient was withdrawn from the study. No adverse events occurred during insertion or removal of the device. At 3 months postinsertion 14 of 15 MSO dilated (93%) were confirmed patent. Conclusion: Placement of an osmotic self-dilating expansion device in human MSO is safe, achievable and effective at dilating the ostia. C 2014 ARS-AAOA, LLC. Key Words: chronic rhinosinusitis; maxillary sinusitis; dilatation; feasibility studies; balloon; device How to Cite this Article: Hathorn I, Habib A-R, Dar Santos R, Javer A. The safety and performance of a maxillary sinus ostium self-dilation device: a pilot study. Int Forum Allergy Rhinol. 2014;4: Chronic rhinosinusitis (CRS) is a significant health problem. 1, 2 In patients with CRS the maxillary sinus is frequently affected and contributes significantly to the impact of the disease, making it a target for medical and surgical intervention. Treatment of CRS involves medical and surgical treatment or often a combination of the two. The most frequently used surgical approach is functional endoscopic sinus surgery (FESS), which aims to open up the sinus drainage pathways and enhance mucosal St. Paul s Sinus Centre, St. Paul s Hospital, Vancouver, BC, Canada Correspondence to: Iain Hathorn, MBChB, FRCSEd (ORL-HNS), St. Paul s Sinus Centre, St. Paul s Hospital, 1081 Burrard Street, Vancouver, BC V6Z 1Y6, Canada; iainhathorn@hotmail.com Funding sources for the study: SinuSys Corporation. Potential conflict of interest: None provided. Received: 19 December 2013; Revised: 30 March 2014; Accepted: 11 April 2014 DOI: /alr View this article online at wileyonlinelibrary.com. clearance. 3 Surgery can be directed at relieving obstruction and occasionally enlarging the maxillary sinus ostium (MSO), which is routinely performed as part of FESS. FESS is typically performed under general anesthesia and may result in scarring and adhesions postoperatively. It has been suggested that a small middle meatal antrostomy with less tissue removal and preservation of normal structures might be as effective as a large one. 4 This has encouraged alternative approaches to enlarge the sinus ostia including balloon catheter technology. 5 Balloon dilation is now commonly used to open sinus ostia while preserving mucosa and minimizing trauma. It has been shown to be effective for the treatment of obstructed sinus ostia in CRS, 6 8 and may reduce postoperative scarring and stenosis. Balloon technology is constantly developing and is now being used routinely in the office under local anesthesia. 9 There is a new maxillary sinus ostium self-dilation device (Vent-Os TM Sinus Dilation System, SinuSys Corporation, Palo Alto, CA) that functions on the principle of osmosis, 625 International Forum of Allergy & Rhinology, Vol. 4, No. 8, August 2014
2 Hathorn et al. absorbing a small amount of fluid from the surrounding tissues. It can be placed into the maxillary sinus ostium under endoscopic visualization and is able to slowly enlarge its outer diameter under low pressure (42 psi) to a predetermined dimension. Slow, low pressure dilation of the maxillary sinus ostia is expected to minimize tissue damage and potentially reduce scarring. The new self-dilation device has been studied prior to this clinical trial in bench testing, cadaver and animal studies. 10 A total of 13 sheep (26 maxillary sinuses) had a dilation device placed in each of the MSO. Placements were performed under endoscopic visualization with the animals under general anesthesia. The studies showed that the devices were capable of dilating and enlarging the MSO. The diameter of the enlarged ostia measured immediately after removal of the device was very similar to the outer diameter of the device after removal. In 4 animals an endoscopy with measurement of the MSO was performed approximately 2 weeks and 4 weeks after the procedure and showed patency of the MSO with no significant alteration of the diameter. This is the first clinical trial to evaluate the self-dilation device. This pilot study concentrated on the placement, functionality, and removal of the device with the primary objective of assessing the safety and performance of the system for dilation of the MSO. Patients and methods This is a single-center, pilot, open-labeled prospective study. It was conducted with the approval of the University of British Columbia Clinical Research Ethics Board. Patients aged 19 to 75 years inclusive, with a diagnosis of chronic maxillary sinusitis (according to the Canadian Clinical Practice Guidelines for Acute and Chronic Rhinosinusitis) who failed medical management (including topical steroids and antibiotics) and were due to undergo endoscopic sinus surgery were eligible to be enrolled in the study (Fig. 1). The subjects that participated signed a consent form and an endoscopic assessment of the MSO was made preoperatively to assess patency. Preoperative computed tomography (CT) scans were performed in all cases to establish paranasal sinus anatomy and to assess the extent of sinus disease as is standard practice. They had a dilation device placed in 1 or both MSO intraoperatively under direct endoscopic visualization. If other endoscopic sinus surgery was required, it was performed (eg, ethmoidectomy) with the device in situ. Other surgery performed in each case is documented in Table 1. The device was placed at the beginning of surgery with the ethmoid bulla intact and no uncinectomy was performed. The device was left in the MSO for 1 hour to allow it to dilate, after which it was removed using standard endoscopic surgical instruments under direct endoscopic visualization. Standardized photographs and videos were taken immediately after removal to assess the MSO. Patency of the MSO immediately after dilation was recorded. FIGURE 1. Inclusion and exclusion criteria. The outcome measures were as follows: Safety as evidenced by an assessment of the adverse events related to MSO dilation procedure; Efficacy defined by patency of MSO immediately after removal of the dilation device; Reports of sinus related adverse events during the 3 months follow-up period. The subjects were followed-up at 1 week, 1 month, and 3 months after MSO dilation. Postoperatively they were given a 1-week course of oral prednisolone (10 mg OD) and antibiotics (co-amoxiclav), along with regular nasal douches (saline with a single budesonide respule), as is standard practice at our institution following sinus surgery. During the follow-up period if subjects received any other medication, such as topical budesonide spray, this was recorded. At each follow-up visit and preoperatively, rigid nasal endoscopy with a 30-degree and 70-degree endoscope was performed and standard photographs and videos were taken. The patency of the MSO and any adverse events were recorded at each visit. This was a pilot study designed to provide preliminary observations and generate safety and feasibility data to guide future studies. The sample size was selected to meet the goals of this feasibility clinical trial. Descriptive statistics were used for continuous variables and for categorical variables. Device and placement The dilation system is an osmotically driven dilation device and comes packaged with the dilation device preloaded in the distal tip of the cannula of the placement system (Fig. 2). The dilation device was delivered under endoscopic International Forum of Allergy & Rhinology, Vol. 4, No. 8, August
3 Maxillary sinus ostium self-dilation device TABLE 1. Subject demographics and characteristics Subject Age (years) Sex Bilateral Lund-Mackay score Side of insertion Additional procedures 1 53 F 1 R, L U(R) 2 53 F 2 L U(R),CB(L) 3 47 M 4 R, L E (R, L), NS 4 69 F 14 R, L U (R), E (R, L), S (L), F (R, L) 5 75 M 4 R, L CB (R, L) 6 41 F 6 R U (L), E (L), F (L) 7 20 M 10 R, L - dislodged U (L), E (R, L), S (R, L), F (R, L) 8 47 M 16 R - removed, L U (R), E (R, L), S (R, L), F (R), CB (L) 9 70 F 9 R, L E (R, L) S (L), F (L), CB (L) M 8 R U (L), E (R, L), F (L), CB (R, L), NS M 8 R U (L), E (R, L), S (R, L), F (L), NS F 6 L U(R) CB = excision of concha bullosa; E = ethmoidectomy; F = frontal sinusotomy; NS = nasal septoplasty; S = sphenoidotomy; U = uncinectomy. FIGURE 2. Vent-Os TM Sinus Dilation System, SinuSys Corp, Palo Alto, CA. guidance via the placement system to the ostium of the maxillary sinus (Fig. 3). All device insertions were conducted intraoperatively under general anesthesia by the senior author (A.R.J.). Once the dilation device was in place, it was released by sliding the slider forward and the placement system was removed. The device then dilated expanding the ostium over a period of time (up to 1 hour) by absorbing a small amount of fluid from the surrounding tissues (Fig. 4). The dilation device was then removed from the ostium. There were 70-degree and 110-degree angled systems available to allow placement of the device. Prior to insertion, the device is approximately 3 mm in diameter and is designed to expand to nearly 5 mm after 60 minutes. Insertion devices were measured before and after each insertion. FIGURE 3. Dilation device placed under endoscopic guidance into the ostium of the maxillary sinus. Results Between May 2012 and January 2013, a total of 14 adults were approached to participate into this prospective, nonrandomized, single-cohort clinical trial. Of those approached, 2 (14%) were excluded as they did not meet the inclusion criteria. The final cohort consisted of 12 individuals with equal distribution of males and females (Table 1). The mean age of the final group was 51.5 ± 17.8 years. Among those included, a total of 19 MSO were evaluated to receive insertion of the experimental device. 627 International Forum of Allergy & Rhinology, Vol. 4, No. 8, August 2014
4 Hathorn et al. FIGURE 4. Osmotic self-dilating expansion device. FIGURE 5. Insertion of device to left maxillary sinus ostium. FIGURE 6. Device in position in left maxillary sinus ostium during FESS. One arm of the device is shown on top of the uncinate holding it in place. FESS = functional endoscopic sinus surgery. This consisted of 10 (53%) right and 9 (47%) left MSO. All MSO were assessed endoscopically prior to surgery but it was not possible to measure the maxillary sinus ostia size due to the presence of the uncinate and inflammation obstructing the MSO. MSO patency was evaluated from the preoperative CT scans. Eleven (58%) MSOs were obstructed and 8 (42%) were narrowed to less than 2.5 mm. All maxillary sinuses had signs and radiographic evidence of maxillary CRS. The device was successfully placed into the MSO in 19 (100%) cases (Figs. 5 and 6). The uncinate process remained intact during the placement of the device in all cases. There were no adverse events reported during placement. The device was straight forward to insert, with a single pass of the placement system sufficient to insert the device in 11 (58%) cases. Placement was successful on a second pass in the remaining 8 (42%) cases. Seventeen (89%) devices remained in situ for the complete 1 hour time period; however, 2 (11%) did not reach the entire time requirement (range, 22 to 40 minutes). In 1 case the device was inadvertently moved during FESS procedure by standard tools and became dislodged. The device was retrieved from the nasal cavity causing no adverse events. In a second case the device was removed by the surgeon to enable better visualization for other FESS procedures. Those devices that did not remain in the MSO for 60 minutes were excluded from further evaluation and an uncinectomy was performed. The insertion devices expanded to a mean of 4.8 ± 0.5 mm. The MSO was observed to remain the same size as the removed device although it was not possible to measure the MSO size accurately due to the intact uncinate. No adverse events were recorded during device removal. MSO patency was evaluated immediately after device removal and at 7, 30, and 90 days (Table 2). After removal of the device, despite the uncinate still being intact, it was possible to visualize most of the MSO endoscopically, unlike the situation preoperatively. Immediately after removal of the device (Fig. 7), 16 of 17 (94%) MSO were visibly patent and 1 of 17 (6%) could not be visualized endoscopically to confirm patency (indeterminate). At 7 days postinsertion, 12 of 15 (80%) MSO were seen to be patent and 3 of 15 (16%) were indeterminate. One individual (2 ostia) was withdrawn from the study by the lead investigator as they were unable to comply with the study followup; they were therefore removed from further study-related evaluation. At 30 days postinsertion, 13 of 15 (87%) MSO were visibly patent, 2 (13%) were indeterminate. At 90 days postinsertion, 14 of 15 (93%) MSO were visibly patent and 1 (7%) was indeterminate (Fig. 8). No MSOs were noted to be nonpatent on endoscopic assessment. There were no specific device related adverse events recorded in the postoperative period. Other adverse events recorded related to FESS, and not specific to device use, included facial pain reported at 7 days among 2 of 11 (18%) subjects and headaches reported by 2 of 11 (18%) individuals at 7 days and 2 (18%) subjects at 30 days. Active bleeding was reported by 3 (27%) individuals at 7 days and 1 (9%) at 30 days postsurgery. One individual (9%) reported a sinus infection at 90 days postsurgery. Topical budesonide to treat postoperative edema was prescribed International Forum of Allergy & Rhinology, Vol. 4, No. 8, August
5 Maxillary sinus ostium self-dilation device TABLE 2. Intraoperative and postoperative patency MSO Intraoperative (after 7-day 30-day 90-day Subject treated device removal) follow-up follow-up follow-up 1A Right Patent Withdraw Withdraw Withdraw 1B Left Patent Withdraw Withdraw Withdraw 2 Left Patent Patent Patent Patent 3A Right Patent No visual No visual No visual 3B Left Patent Patent Patent Patent 4A Right Patent Patent Patent Patent 4B Left Patent Patent Patent Patent 5A Right Patent Patent Patent Patent 5B Left Patent Patent Patent Patent 6 Right Patent Patent Patent Patent 7A Right Patent Patent Patent Patent 7B Left Device dislodged N/A N/A N/A 8A Right Device removed N/A N/A N/A 8B Left Patent Patent Patent Patent 9A Right Patent No visual Patent Patent 9B Left No visual No visual No visual Patent 10 Right Patent Patent Patent Patent 11 Right Patent Patent Patent Patent 12 Left Patent Patent Patent Patent MSO = maxillary sinus ostium; N/A = not applicable. FIGURE 7. Ostia immediately postremoval of device. for 5 (45%) individuals. One subject in the study group underwent revision frontal sinusotomy but there were no revisions of the maxillary sinus related to device use. Therefore, in total, none of 15 (0%) MSOs required revision surgery. Discussion Balloon technology in the sinuses was first introduced in 2005, and developed from the success of balloon use in other specialties. The surrounding mucosa is compressed FIGURE 8. Three months postremoval of dilation device (different patient from Fig. 7). by the balloon and causes microfracture of the circumferential bone. 5, 6 It has been argued that balloon dilation may enhance mucosal preservation, reduce local trauma, and restore the natural sinus drainage pathways resulting in effective relief of symptoms. There have been many studies looking into the feasibility, safety and efficacy of balloon dilation of sinus ostia to treat CRS. Initially, a cadaveric model was used to establish the feasibility and safety of the device. 11 Following this study it was concluded that balloon use was feasible and may cause less mucosal trauma than the standard endoscopic surgical techniques. The first human study involving 10 FESS patients was performed by Brown and Bolger. 12 All planned sinus ostia were successfully dilated (10 maxillary, 5 sphenoid, 3 frontal) with no adverse events reported. The first multicentre trial was the Clinical Evaluation to Confirm Safety and Efficacy of Sinuplasty in the Paranasal Sinuses (CLEAR) study. 6 At 12 weeks, confirmed patency for the maxillary sinus was 84%, 3% nonpatent, and 13% not able to visualize, compared to 93% patent, 0% nonpatent, and 7% unable to visualize in our study. Patient symptom scores in the CLEAR study (20-item Sinonasal Outcomes Test [SNOT-20]) also significantly improved from baseline. This cohort of patients was then followed up at 1 and 2 years. 7, 8 Both studies demonstrated that significant improvements were maintained in Lund-Mackay CT scores and symptom scores (SNOT 20). There are very few comparative studies using balloon technology; however, Plaza et al. 13 published the first randomized controlled clinical trial using balloon dilation of the frontal recess as part of a hybrid procedure in patients with CRS with nasal polyposis (CRSwNP). At 12 months following surgery they demonstrated a statistically significant reduction in Lund-Mackay stage in general and specifically related to the frontal sinus. The patency of the frontal recess seen by office endoscopy was statistically more frequent after balloon treatment (75% vs 63%). The maxillary sinus ostium self-dilation device used in this study has the benefits of a standard balloon, but since 629 International Forum of Allergy & Rhinology, Vol. 4, No. 8, August 2014
6 Hathorn et al. the device dilates slowly and at lower pressure over a set period of time, the mucosal trauma and resulting scarring may potentially be reduced even further. This is the first human study using this device, and it demonstrates that it is feasible to place the dilation device into the MSO under endoscopic guidance (100% successful placement). This compares well with standard balloon dilation studies. The device was easy to insert with successful placement in all cases with at the most 2 passes of the placement system required. Again, in our experience, this compares favorably to balloon devices. The device remained in place the requisite time period to achieve dilation in 89% of MSOs. In 2 MSOs (11%) the device was dislodged or removed to allow better visualization for additional FESS procedures. The device could be placed at the end of FESS in the operating room and removed in recovery, thus alleviating the issues with device displacement during the procedure. The device dilated in all cases when it was successfully placed and remained in situ for the full hour. There were no significant adverse events recorded during device placement or removal. It appears, therefore, that placement of this osmotic self-dilating expansion device in human MSO is safe, achievable and effective at dilating the ostia. At 3 months the sinus ostia appear to remain patent although longer-term follow-up is required. The revision rate of the maxillary sinus was 0% (0/15). This revision rate is lower than that of FESS 14 and that of balloon dilation. 6 8, 15 However, the numbers in this pilot study are small and follow-up relatively short, so it is not possible to determine an accurate revision rate. Further studies will be required to address this. The use of any dilation device has the potential to inadvertently create a false lumen or cannulate an existing accessory ostia. It is unclear what the clinical impact on patient outcomes is in these situations. It is possible that secondary drainage pathways, whether preexisting or created, result in mucus recirculation. However, not all secondary pathways result in recirculation, and not all patients with recirculation are symptomatic. 16 In our study there was no evidence of any false lumens being created or accessory ostia being cannulated. The study has limitations. There was no assessment of patient reported outcomes to assess the effectiveness of the device in improving symptoms. This is mainly due to the fact that as well as the device being placed, other FESS procedures such as ethmoidectomy were performed, and so it would not be possible to attribute any improvement in scores to the device dilating the MSO. Also, although attempts were made to assess and compare the MSO endoscopically preoperatively and postoperatively, there was no measurement of MSO size. This was not possible due to the presence of an intact uncinate. Other studies looking at balloon dilation of the MSO have noted similar problems with measuring ostial size and used patency as their main outcome measure. Establishing MSO patency endoscopically has also been recognized as being difficult in these studies due to increased preservation of tissue using balloon dilation, such as an intact uncinate. 6 Therefore, in our study device size at removal was used as a surrogate for MSO size. The MSO were confirmed either patent or not patent under direct vision endoscopically postoperatively. Again due to the intact uncinate there were MSO that could not be confirmed patent. However, in no cases were the MSO observed to be obstructed. In addition, the follow-up period was only 3 months and therefore was not designed to evaluate long-term outcomes in terms of patency and revision rates. However, the study was designed to address the feasibility of placement and removal of the device, as well as its functionality, with the primary objective of assessing the safety and performance of the system for dilation of the MSO. Further studies are now required to compare the device with other techniques, such as balloon dilation and traditional FESS, and to clearly demonstrate longerterm outcomes and effectiveness now that the safety and feasibility of the device has been established. There are currently ongoing studies designed to assess the longer-term effectiveness of the dilation device. Conclusion Placement of a novel osmotic self-dilating expansion device in human MSO is safe, achievable, and effective at dilating the ostia. Further clinical studies are required to investigate the clinical effectiveness and long-term outcomes of the device, as well as trials looking into its placement under local anesthetic in the office, which are already underway. References 1. Adams PF, Hendershot GE, Marano MA. Centers for Disease Control and Prevention/National Center for Health Statistics. Current estimates from the National Health Interview Survey, Vital Health Stat. 1999;10(200): Blackwell DL, Collins JG, Coles R. Summary health statistics for U.S. adults: National Health Interview Survey, Vital Health Stat. 2002;10(205): Fokkens W, Lund V, Mullol J. European Position Paper on Rhinosinusitis and Nasal Polyps group. European Position Paper on Rhinosinusitis and Nasal Polyps Rhinol Suppl. 2007;(20): Albu S, Tomescu E. Small and large middle meatus antrostomies in the treatment of chronic maxillary sinusitis. Otolaryngol Head Neck Surg. 2004;131: Vaughan WC. Review of balloon sinuplasty. Curr Opin Otolaryngol Head Neck Surg. 2008;16: Bolger WE, Brown CL, Church CA, et al. Safety and outcomes of balloon catheter sinusotomy: a multicenter 24-week analysis in 115 patients. Otolaryngol Head Neck Surg. 2007;137: Kuhn FA, Church CA, Goldberg AN, Levine HL, Sillers MJ, Vaughan WC, Weiss RL. Balloon catheter sinusotomy: one-year follow-up-outcomes and role in functional endoscopic sinus surgery. Otolaryngol Head Neck Surg. 2008;139(3 Suppl 3):S27 S Weiss RL, Church CA, Kuhn FA, Levine HL, Sillers MJ, Vaughan WC. Long-term outcome analysis of balloon catheter sinusotomy: two-year follow-up. Otolaryngol Head Neck Surg. 2008;139(3 Suppl 3):S38 S Stankiewicz J, Tami T, Truitt T, Atkins J, Liepert D, Winegar B. Transantral, endoscopically guided balloon dilatation of the ostiomeatal complex for chronic rhinosinusitis under local anesthesia. Am J Rhinol Allergy. 2009;23: Hester J, Edgren D, Koreck A, Fox J, Mandrusov J. Assessment of the short term patency of the maxillary sinus ostium following dilatation with an osmotic device in a sheep model. Poster presented at: Annual Meeting of the American Rhinologic Society. Poster 2012:P Bolger WE, Vaughan WC. Catheter-based dilation of the sinus ostia: initial safety and feasibility analysis in a cadaver model. Am J Rhinol. 2006;20: Brown CL, Bolger WE. Safety and feasibility of balloon catheter dilation of paranasal sinus ostia: a International Forum of Allergy & Rhinology, Vol. 4, No. 8, August
7 Maxillary sinus ostium self-dilation device preliminary investigation. Ann Otol Rhinol Laryngol. 2006;115: Plaza G, Eisenberg G, Montojo J, Onrubia T, Urbasos M, O Connor C. Balloon dilation of the frontal recess: a randomized clinical trial. Ann Otol Rhinol Laryngol. 2011;120: Hopkins C, Slack R, Lund V, Brown P, Copley L, Browne J. Long-term outcomes from the English national comparative audit of surgery for nasal polyposis and chronic rhinosinusitis. Laryngoscope 2009;119: Levine HL, Sertich AP 2nd, Hoisington DR, Weiss RL, Pritikin J. Multicenter registry of balloon catheter sinusotomy outcomes for 1,036 patients. Ann Otol Rhinol Laryngol. 2008;117: Mann WJ, Tóth M, Gouveris H, Amedee RG. The drainage system of the paranasal sinuses: a review with possible implications for balloon catheter dilation. Am J Rhinol Allergy. 2011;25: International Forum of Allergy & Rhinology, Vol. 4, No. 8, August 2014
Patency of Maxillary Sinus Ostia Following Dilation with a Novel Osmotic Expansion Device
 WHITE PAPER Patency of Maxillary Sinus Ostia Following Dilation with a Novel Osmotic Expansion Device Six-Month Results from a Multi-Center Prospective Study Jerome Hester, MD California Sleep Institute,
WHITE PAPER Patency of Maxillary Sinus Ostia Following Dilation with a Novel Osmotic Expansion Device Six-Month Results from a Multi-Center Prospective Study Jerome Hester, MD California Sleep Institute,
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
Description. Section: Surgery Effective Date: April 15, 2014 Subsection: Surgery Original Policy Date: June 7, 2012 Subject: Page: 1 of 12
 Last Review Status/Date: March 2014 Page: 1 of 12 Description Balloon ostial dilation (also known as balloon sinuplasty ) is proposed as an alternative to traditional endoscopic sinus surgery for patients
Last Review Status/Date: March 2014 Page: 1 of 12 Description Balloon ostial dilation (also known as balloon sinuplasty ) is proposed as an alternative to traditional endoscopic sinus surgery for patients
Topic: Balloon Catheter Dilation for Treatment of Sinusitis Date of Origin: August 8, Section: Surgery Last Reviewed Date: February 2014
 Medical Policy Manual Topic: Balloon Catheter Dilation for Treatment of Sinusitis Date of Origin: August 8, 2006 Section: Surgery Last Reviewed Date: February 2014 Policy No: 153 Effective Date: April
Medical Policy Manual Topic: Balloon Catheter Dilation for Treatment of Sinusitis Date of Origin: August 8, 2006 Section: Surgery Last Reviewed Date: February 2014 Policy No: 153 Effective Date: April
Learner Objectives. Overview. Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation 7/31/2017
 Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System
 WHITE PAPER Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA Introduction Establishment
WHITE PAPER Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA Introduction Establishment
MEDICAL POLICY EFFECTIVE DATE: 04/21/11 REVISED DATE: 06/21/12, 05/23/13, 06/19/14, 06/18/15, 06/16/16, 06/15/17
 MEDICAL POLICY SUBJECT: SINUS OSTIAL DILATION FOR PAGE: 1 OF: 6 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: SINUS OSTIAL DILATION FOR PAGE: 1 OF: 6 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Protocol. Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis
 Protocol Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis Medical Benefit Effective Date: 04/01/15 Next Review Date: 11/19 Preauthorization No Review Dates: 07/07, 07/08, 11/08, 05/09, 01/10,
Protocol Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis Medical Benefit Effective Date: 04/01/15 Next Review Date: 11/19 Preauthorization No Review Dates: 07/07, 07/08, 11/08, 05/09, 01/10,
Description. Section: Surgery Effective Date: April 15, 2017 Subsection: Surgery Original Policy Date: June 7, 2012 Subject: Page: 1 of 13
 Last Review Status/Date: March 2017 Page: 1 of 13 Description Balloon ostial dilation (also known as balloon sinuplasty ) is proposed as an alternative to traditional endoscopic sinus surgery for patients
Last Review Status/Date: March 2017 Page: 1 of 13 Description Balloon ostial dilation (also known as balloon sinuplasty ) is proposed as an alternative to traditional endoscopic sinus surgery for patients
Limitations of balloon sinuplasty in frontal sinus surgery
 Eur Arch Otorhinolaryngol (2011) 268:1463 1467 DOI 10.1007/s00405-011-1626-7 RHINOLOGY Limitations of balloon sinuplasty in frontal sinus surgery S. Heimgartner J. Eckardt D. Simmen H. R. Briner A. Leunig
Eur Arch Otorhinolaryngol (2011) 268:1463 1467 DOI 10.1007/s00405-011-1626-7 RHINOLOGY Limitations of balloon sinuplasty in frontal sinus surgery S. Heimgartner J. Eckardt D. Simmen H. R. Briner A. Leunig
Expand your in-office treatment options for sinusitis. The Vent-Os Sinus Dilation System is simple and cost-effective. Vent-Os. Sinus Dilation System
 Expand your in-office treatment options for sinusitis The Vent-Os Sinus Dilation System is simple and cost-effective Vent-Os Sinus Dilation System Vent-Os Sinus Dilation System A Fast and Effective In-Office
Expand your in-office treatment options for sinusitis The Vent-Os Sinus Dilation System is simple and cost-effective Vent-Os Sinus Dilation System Vent-Os Sinus Dilation System A Fast and Effective In-Office
Medicare Advantage Medical Policy. Title: Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis
 Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis Description/Background CHRONIC RHINOSINUSITIS Chronic rhinosinusitis
Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis Description/Background CHRONIC RHINOSINUSITIS Chronic rhinosinusitis
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Balloon Sinuplasty for Treatment of Chronic Sinusitis Page 1 of 18 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Balloon Sinuplasty for Treatment of Chronic Sinusitis
Balloon Sinuplasty for Treatment of Chronic Sinusitis Page 1 of 18 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Balloon Sinuplasty for Treatment of Chronic Sinusitis
The ORIOS 2 Study: Office-Based Balloon Sinus Dilation A prospective multi-center study of 203 patients
 The ORIOS 2 Study: Office-Based Balloon Sinus Dilation A prospective multi-center study of 203 patients Boris Karanfilov, MD, Ohio Sinus Institute, Dublin, OH 1 Stacey Silvers, MD, Madison ENT & Facial
The ORIOS 2 Study: Office-Based Balloon Sinus Dilation A prospective multi-center study of 203 patients Boris Karanfilov, MD, Ohio Sinus Institute, Dublin, OH 1 Stacey Silvers, MD, Madison ENT & Facial
In-office, multisinus balloon dilation: 1-Year outcomes from a prospective, multicenter, open label trial DO NOT COPY METHODS.
 In-office, multisinus balloon dilation: 1-Year outcomes from a prospective, multicenter, open label trial James Gould, M.D., 1 Ian Alexander, M.D., 2 Edward Tomkin, D.O., 3 and David Brodner, M.D. 4 ABSTRACT
In-office, multisinus balloon dilation: 1-Year outcomes from a prospective, multicenter, open label trial James Gould, M.D., 1 Ian Alexander, M.D., 2 Edward Tomkin, D.O., 3 and David Brodner, M.D. 4 ABSTRACT
Sinusitis is a highly prevalent condition, affecting approximately
 ORIGINAL ARTICLE Office-based balloon sinus dilation: a prospective, multicenter study of 203 patients Boris Karanfilov, MD 1, Stacey Silvers, MD 2, Raza Pasha, MD 3, Ashley Sikand, MD 4, Alan Shikani,
ORIGINAL ARTICLE Office-based balloon sinus dilation: a prospective, multicenter study of 203 patients Boris Karanfilov, MD 1, Stacey Silvers, MD 2, Raza Pasha, MD 3, Ashley Sikand, MD 4, Alan Shikani,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Balloon Sinuplasty for Treatment of Chronic Sinusitis Page 1 of 17 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Balloon Sinuplasty for Treatment of Chronic Sinusitis
Balloon Sinuplasty for Treatment of Chronic Sinusitis Page 1 of 17 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Balloon Sinuplasty for Treatment of Chronic Sinusitis
Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis
 Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis Policy Number: 7.01.105 Last Review: 3/2018 Origination: 3/2007 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Balloon Ostial Dilation for Treatment of Chronic Rhinosinusitis Policy Number: 7.01.105 Last Review: 3/2018 Origination: 3/2007 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Surgical Management of Sinusitis (What About Balloons?) Relative Indications for Sinus Surgery in Children
 Surgical Management of Sinusitis (What About Balloons?) Andrew N. Goldberg M.D. Andrew H. Murr M.D. Michael J. Cunningham, M.D. Department of Otolaryngology and Communication Enhancement Children s Hospital
Surgical Management of Sinusitis (What About Balloons?) Andrew N. Goldberg M.D. Andrew H. Murr M.D. Michael J. Cunningham, M.D. Department of Otolaryngology and Communication Enhancement Children s Hospital
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
Functional endoscopic sinus surgery (FESS) has been
 Effectiveness of intraoperative mitomycin C in maintaining the patency of a frontal sinusotomy: A preliminary report of a double-blind randomized placebo-controlled trial Kwai-Onn Chan, M.D.,* Mireille
Effectiveness of intraoperative mitomycin C in maintaining the patency of a frontal sinusotomy: A preliminary report of a double-blind randomized placebo-controlled trial Kwai-Onn Chan, M.D.,* Mireille
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery
 Page: 1 of 8 Last Review Status/Date: March 2015 Use Following Endoscopic Sinus Surgery Description Sinus stents are devices that are used postoperatively following endoscopic sinus surgery (ESS). The
Page: 1 of 8 Last Review Status/Date: March 2015 Use Following Endoscopic Sinus Surgery Description Sinus stents are devices that are used postoperatively following endoscopic sinus surgery (ESS). The
Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinonasal Polyposis
 Medical Policy Manual Surgery, Policy No. 198 Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinonasal Polyposis Next Review: August 2019 Last Review:
Medical Policy Manual Surgery, Policy No. 198 Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinonasal Polyposis Next Review: August 2019 Last Review:
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
Allergic fungal rhinosinusitis a new staging system*
 ORIGINAL CONTRIBUTION Rhinology 49: 318-323, 2011 Allergic fungal rhinosinusitis a new staging system* Carl M. Philpott 1,2, Allan Clark 2, Amin R. Javer 1 1 St Paul s Sinus Centre, Vancouver, British
ORIGINAL CONTRIBUTION Rhinology 49: 318-323, 2011 Allergic fungal rhinosinusitis a new staging system* Carl M. Philpott 1,2, Allan Clark 2, Amin R. Javer 1 1 St Paul s Sinus Centre, Vancouver, British
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Balloon Sinuplasty: Indications and Cost-Effectiveness
 Balloon Sinuplasty: Indications and Cost-Effectiveness Marilene B. Wang, MD Professor, Department of Head and Neck Surgery David Geffen School of Medicine at UCLA Chief of Otolaryngology VA Greater Los
Balloon Sinuplasty: Indications and Cost-Effectiveness Marilene B. Wang, MD Professor, Department of Head and Neck Surgery David Geffen School of Medicine at UCLA Chief of Otolaryngology VA Greater Los
EVALUATION OF PATIENT'S OUTCOME AFTER ENDOSCOPIC SINUS SURGERY
 Basrah Journal Of Surgery Bas J Surg, September, 16, 2010 EVALUATION OF PATIENT'S OUTCOME AFTER ENDOSCOPIC SINUS SURGERY Hiwa A Abdulkareem MB.ChB, FICMS, CABS(ENT); Teaching Hospital; University of Sulaimania.
Basrah Journal Of Surgery Bas J Surg, September, 16, 2010 EVALUATION OF PATIENT'S OUTCOME AFTER ENDOSCOPIC SINUS SURGERY Hiwa A Abdulkareem MB.ChB, FICMS, CABS(ENT); Teaching Hospital; University of Sulaimania.
The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis. Patients. Vincent Honrubia MD, FACS
 The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis Patients Vincent Honrubia MD, FACS Allyssa Cantu, PA-S Sharon Gelman, MEd, PA-S Rachel Tsai, BS Director,
The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis Patients Vincent Honrubia MD, FACS Allyssa Cantu, PA-S Sharon Gelman, MEd, PA-S Rachel Tsai, BS Director,
BALLOON OSTIAL DILATION FOR TREATMENT OF CHRONIC SINUSITIS
 BALLOON OSTIAL DILATION FOR TREATMENT OF CHRONIC SINUSITIS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services,
BALLOON OSTIAL DILATION FOR TREATMENT OF CHRONIC SINUSITIS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services,
Incidence of accessory ostia in patients with chronic maxillary sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
Sinus Surgery (Functional Endoscopic Sinus Surgery and Balloon Sinuplasty)
 Sinus Surgery (Functional Endoscopic Sinus Surgery and Balloon Sinuplasty) Date of Origin: 10/2015 Last Review Date: 06/28/2017 Effective Date: 07/01/2017 Dates Reviewed: 10/2015, 06/2017 Developed By:
Sinus Surgery (Functional Endoscopic Sinus Surgery and Balloon Sinuplasty) Date of Origin: 10/2015 Last Review Date: 06/28/2017 Effective Date: 07/01/2017 Dates Reviewed: 10/2015, 06/2017 Developed By:
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery
 Last Review Status/Date: March 2014 Page: 1 of 7 Use Following Endoscopic Sinus Surgery Description Sinus stents are devices that are used postoperatively following endoscopic sinus surgery (ESS). The
Last Review Status/Date: March 2014 Page: 1 of 7 Use Following Endoscopic Sinus Surgery Description Sinus stents are devices that are used postoperatively following endoscopic sinus surgery (ESS). The
Topical medications administered by nebulizers are
 ORIGINAL ARTICLE The effect of head position on the distribution of topical nasal medication using the Mucosal Atomization Device: a cadaver study Al-Rahim R. Habib, BSc, Andrew Thamboo, MD, Jamil Manji,
ORIGINAL ARTICLE The effect of head position on the distribution of topical nasal medication using the Mucosal Atomization Device: a cadaver study Al-Rahim R. Habib, BSc, Andrew Thamboo, MD, Jamil Manji,
Steroid-Eluting Ethmoidal Stent Versus Antero- -Posterior Ethmoidectomy: Comparison Of Efficacy And Safety In Allergic Patients
 Steroid-Eluting Ethmoidal Stent Versus Antero- -Posterior Ethmoidectomy: Comparison Of Efficacy And Safety In Allergic Patients Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Steroid-Eluting Ethmoidal Stent Versus Antero- -Posterior Ethmoidectomy: Comparison Of Efficacy And Safety In Allergic Patients Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinus Disease
 Page: 1 of 8 Last Review Status/Date: March 2017 Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and Description Sinus stents are devices used postoperatively following
Page: 1 of 8 Last Review Status/Date: March 2017 Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and Description Sinus stents are devices used postoperatively following
By: Abdulrahman A. Al-Humaizi Rhinology Fellow, F2
 20.03.2017 By: Abdulrahman A. Al-Humaizi Rhinology Fellow, F2 Objectives Introduction Materials and methods Results Discussion Literature Review Conclusion Introduction Topical delivery to the paranasal
20.03.2017 By: Abdulrahman A. Al-Humaizi Rhinology Fellow, F2 Objectives Introduction Materials and methods Results Discussion Literature Review Conclusion Introduction Topical delivery to the paranasal
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Treatment Options for Chronic Sinusitis
 Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision
 THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
An Innovative Treatment Option for Patients with Recurrent Nasal Polyps
 An Innovative Treatment Option for Patients with Recurrent Nasal Polyps Burden of illness and management of Chronic Sinusitis with Nasal Polyps Continuum of care and polyp recurrence Clinical and health
An Innovative Treatment Option for Patients with Recurrent Nasal Polyps Burden of illness and management of Chronic Sinusitis with Nasal Polyps Continuum of care and polyp recurrence Clinical and health
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
Clinical Policy: Balloon Sinus Ostial Dilation for Treatment of Chronic Sinusitis
 Clinical Policy: Balloon Sinus Ostial Dilation for Treatment of Chronic Sinusitis Reference Number: CP.MP.119 Last Review Date: 11/17 See Important Reminder at the end of this policy for important regulatory
Clinical Policy: Balloon Sinus Ostial Dilation for Treatment of Chronic Sinusitis Reference Number: CP.MP.119 Last Review Date: 11/17 See Important Reminder at the end of this policy for important regulatory
MEDICAL POLICY I. POLICY FUNCTIONAL ENDOSCOPIC SINUS SURGERY FOR CHRONIC RHINOSINUSITIS MP POLICY TITLE POLICY NUMBER
 Original Issue Date (Created): 8/1/2018 Most Recent Review Date (Revised): 1/30/2018 Effective Date: 8/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Original Issue Date (Created): 8/1/2018 Most Recent Review Date (Revised): 1/30/2018 Effective Date: 8/1/2018 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER
Unique Journal of Medical and Dental Sciences Available online: Research Article
 ISSN 2347-5579 Unique Journal of Medical and Dental Sciences Available online: www.ujconline.net Research Article STUDY OF ANATOMICAL VARIATIONS OF LATERAL WALL OF NOSE BY ENDOSCOPE Kolvekar VD 1*, Kazi
ISSN 2347-5579 Unique Journal of Medical and Dental Sciences Available online: www.ujconline.net Research Article STUDY OF ANATOMICAL VARIATIONS OF LATERAL WALL OF NOSE BY ENDOSCOPE Kolvekar VD 1*, Kazi
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Modification of the Lund-Kennedy Endoscopic Scoring System Improves Its Reliability and Correlation With Patient-Reported Outcome Measures
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Modification of the Lund-Kennedy Endoscopic Scoring System Improves Its Reliability and Correlation With
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Modification of the Lund-Kennedy Endoscopic Scoring System Improves Its Reliability and Correlation With
DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS. Dr. Ziyad Al-Abduljabbar
 DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS Dr. Ziyad Al-Abduljabbar International Forum of Allergy & Rhinology, Vol. 5, No. 9, September 2015 INTRODUCTION
DURATION OF ORAL ANTIBIOTIC IN THE SETING OF MAXIMAL MEDICAL THERAPY FOR CHRONIC RHINOSINUSITIS Dr. Ziyad Al-Abduljabbar International Forum of Allergy & Rhinology, Vol. 5, No. 9, September 2015 INTRODUCTION
A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis
 Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Chronic rhinosinusitis (CRS) refers to inflammation of
 ORIGINAL ARTICLE The efficacy and safety of an office-based polypectomy with a vacuum-powered microdebrider Eng Cern Gan, MBBS, MRCS (Edin), MMED (ORL), Al-Rahim R. Habib, BSc, Iain Hathorn, MBChB, FRCS
ORIGINAL ARTICLE The efficacy and safety of an office-based polypectomy with a vacuum-powered microdebrider Eng Cern Gan, MBBS, MRCS (Edin), MMED (ORL), Al-Rahim R. Habib, BSc, Iain Hathorn, MBChB, FRCS
Functional Endoscopic Sinus Surgery (FESS)
 Functional Endoscopic Sinus Surgery (FESS) Last Review Date: December 12, 2017 Number: MG.MM.SU.56C2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Functional Endoscopic Sinus Surgery (FESS) Last Review Date: December 12, 2017 Number: MG.MM.SU.56C2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Original Article Comparison of different surgical approaches of functional endoscopic sinus surgery on patients with chronic rhinosinusitis
 Int J Clin Exp Med 2014;7(6):1585-1591 www.ijcem.com /ISSN:1940-5901/IJCEM0000315 Original Article Comparison of different surgical approaches of functional endoscopic sinus surgery on patients with chronic
Int J Clin Exp Med 2014;7(6):1585-1591 www.ijcem.com /ISSN:1940-5901/IJCEM0000315 Original Article Comparison of different surgical approaches of functional endoscopic sinus surgery on patients with chronic
Site of Service: Select Surgical Procedures. Select a hyperlink below to be directed to that section.
 MEDICAL POLICY 7.01.559 Sinus Surgery BCBSA Ref. Policies: 7.01.105, 7.01.155 Effective Date: June 1, 2018 RELATED MEDICAL POLICIES: Last Revised: Sept. 21, 2018 7.01.558 Rhinoplasty Replaces: N/A 11.01.524
MEDICAL POLICY 7.01.559 Sinus Surgery BCBSA Ref. Policies: 7.01.105, 7.01.155 Effective Date: June 1, 2018 RELATED MEDICAL POLICIES: Last Revised: Sept. 21, 2018 7.01.558 Rhinoplasty Replaces: N/A 11.01.524
Site of Service - Select Surgical Procedures. Select a hyperlink below to be directed to that section.
 MEDICAL POLICY 7.01.559 Sinus Surgery BCBSA Ref. Policies: 7.01.105, 7.01.155 Effective Date: June 1, 2018* RELATED MEDICAL POLICIES: Last Revised: May 1, 2018 7.01.558 Rhinoplasty Replaces: N/A 11.01.524
MEDICAL POLICY 7.01.559 Sinus Surgery BCBSA Ref. Policies: 7.01.105, 7.01.155 Effective Date: June 1, 2018* RELATED MEDICAL POLICIES: Last Revised: May 1, 2018 7.01.558 Rhinoplasty Replaces: N/A 11.01.524
BALLOON SINUS OSTIAL DILATION
 BALLOON SINUS OSTIAL DILATION UnitedHealthcare Oxford Clinical Policy Policy Number: ENT 021.6 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
BALLOON SINUS OSTIAL DILATION UnitedHealthcare Oxford Clinical Policy Policy Number: ENT 021.6 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
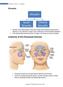 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
A double-blind randomised controlled trial of gloved versus ungloved merocel middle meatal spacers for endoscopic sinus surgery*
 ORIGINAL CONTRIBUTION A double-blind randomised controlled trial of gloved versus ungloved merocel middle meatal spacers for endoscopic sinus surgery* Elaheh Akbari 1, Carl M. Philpott 1, Avi J. Ostry
ORIGINAL CONTRIBUTION A double-blind randomised controlled trial of gloved versus ungloved merocel middle meatal spacers for endoscopic sinus surgery* Elaheh Akbari 1, Carl M. Philpott 1, Avi J. Ostry
ISSN X (Print) Research Article. *Corresponding author Dr.V. Krishna Chaitanya
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
BALLOON SINUS OSTIAL DILATION
 UnitedHealthcare of California (HMO) UnitedHealthcare Benefits Plan of California (EPO/POS) UnitedHealthcare of Oklahoma, Inc. UnitedHealthcare of Oregon, Inc. UnitedHealthcare Benefits of Texas, Inc.
UnitedHealthcare of California (HMO) UnitedHealthcare Benefits Plan of California (EPO/POS) UnitedHealthcare of Oklahoma, Inc. UnitedHealthcare of Oregon, Inc. UnitedHealthcare Benefits of Texas, Inc.
REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT
 CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
Corporate Medical Policy
 Corporate Medical Policy Surgical Treatment of Sinus Disease Description of Procedure or Service Sinusitis refers to infection or inflammation of the sinuses, which are small openings in the bones of the
Corporate Medical Policy Surgical Treatment of Sinus Disease Description of Procedure or Service Sinusitis refers to infection or inflammation of the sinuses, which are small openings in the bones of the
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
Disclaimers. Topical Therapy. The Problem. Topical Therapy for Chronic Rhinosinusitis No Disclosures
 Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Topical Therapy for Chronic Rhinosinusitis No Disclosures Disclaimers Off-label use of multiple steroid and antibiotic medications Large talk, limited time Steven D. Pletcher MD University of California,
Imaging Anatomy in Revision Sinus Surgery
 Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
ARTICLE. Revision Endoscopie Sinus Surgery: The St. Paul's Sinus Centre Experience
 ARTICLE Revision Endoscopie Sinus Surgery: The St. Paul's Sinus Centre Experience Brad Mechor, MD, FRCSC and Amin R. Javer, MD, FRCSC ABSTRACT Objective: To determine the most common findings in patients
ARTICLE Revision Endoscopie Sinus Surgery: The St. Paul's Sinus Centre Experience Brad Mechor, MD, FRCSC and Amin R. Javer, MD, FRCSC ABSTRACT Objective: To determine the most common findings in patients
Sinusitis: Medical and Surgical Management. R. Jonathan Lara, DO, FAOCO. Sonoran Ear Nose & Throat
 Sinusitis: Medical and Surgical Management R. Jonathan Lara, DO, FAOCO Sonoran Ear Nose & Throat 27 th Annual Southwestern Conference on Medicine April 26, 2018 What are sinuses? Air filled cavities of
Sinusitis: Medical and Surgical Management R. Jonathan Lara, DO, FAOCO Sonoran Ear Nose & Throat 27 th Annual Southwestern Conference on Medicine April 26, 2018 What are sinuses? Air filled cavities of
The Association Of Maxillary Accessory Ostia With Chronic Rhinosinusitis What is essential; ventilation or drainage. Ahmed Hussien MD.
 The Association Of Maxillary Accessory Ostia With Chronic Rhinosinusitis What is essential; ventilation or drainage. Ahmed Hussien MD. ENT Department Benha Faculty of Medicine, Benha University, Egypt.
The Association Of Maxillary Accessory Ostia With Chronic Rhinosinusitis What is essential; ventilation or drainage. Ahmed Hussien MD. ENT Department Benha Faculty of Medicine, Benha University, Egypt.
PATIENT SELECTION AND MANAGEMENT OF IN-OFFICE BALLOON SINUS DILATION UNDER LOCAL ANESTHESIA IN ADOLESCENT PATIENTS
 WHITE PAPER PATIENT SELECTION AND MANAGEMENT OF IN-OFFICE BALLOON SINUS DILATION UNDER LOCAL ANESTHESIA IN ADOLESCENT PATIENTS Jeffrey S. Rosenbloom, MD Jeffrey Holland, AAS, CRC Alamo ENT Associates,
WHITE PAPER PATIENT SELECTION AND MANAGEMENT OF IN-OFFICE BALLOON SINUS DILATION UNDER LOCAL ANESTHESIA IN ADOLESCENT PATIENTS Jeffrey S. Rosenbloom, MD Jeffrey Holland, AAS, CRC Alamo ENT Associates,
Canine Fossa Puncture for Severe Maxillary Disease in Unilateral Chronic Sinusitis With Nasal Polyp
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Canine Fossa Puncture for Severe Maxillary Disease in Unilateral Chronic Sinusitis With Nasal Polyp Jang
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Canine Fossa Puncture for Severe Maxillary Disease in Unilateral Chronic Sinusitis With Nasal Polyp Jang
Delivering Innovation. Where It s Needed. August 2018
 Delivering Innovation. Where It s Needed. August 2018 Forward-Looking Statements Certain statements in this presentation constitute forward-looking statements within the meaning of the Securities Act of
Delivering Innovation. Where It s Needed. August 2018 Forward-Looking Statements Certain statements in this presentation constitute forward-looking statements within the meaning of the Securities Act of
Endoscopic Frontal Sinusotomy Preventing Recurrence or a Route to Revision?
 The Laryngoscope VC 2010 The American Laryngological, Rhinological and Otological Society, Inc. Endoscopic Frontal Sinusotomy Preventing Recurrence or a Route to Revision? Carl M. Philpott, FRCS(ORL-HNS,
The Laryngoscope VC 2010 The American Laryngological, Rhinological and Otological Society, Inc. Endoscopic Frontal Sinusotomy Preventing Recurrence or a Route to Revision? Carl M. Philpott, FRCS(ORL-HNS,
MP Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinus Disease. Related Policies None
 Medical Policy MP 7.01.134 Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinus BCBSA Ref. Policy: 7.01.134 Last Review: 02/26/2018 Effective Date:
Medical Policy MP 7.01.134 Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinus BCBSA Ref. Policy: 7.01.134 Last Review: 02/26/2018 Effective Date:
A Study of Anatomical Variations in Patients with Chronic Rhinosinusitis.
 DOI: 10.2127/aimdr.201..2.EN1 Original Article ISSN (O):239-222; ISSN (P):239-21 A Study of Anatomical Variations in Patients with Chronic Rhinosinusitis. Smruti Swain 1 1 Associate Professor, Department
DOI: 10.2127/aimdr.201..2.EN1 Original Article ISSN (O):239-222; ISSN (P):239-21 A Study of Anatomical Variations in Patients with Chronic Rhinosinusitis. Smruti Swain 1 1 Associate Professor, Department
European position paper on Rhinosinusitis & Nnasal Polyps 2012 (summary)
 Rhinology Chair Weekly Activity European position paper on Rhinosinusitis & Nnasal Polyps 2012 (summary) Mohammed s. Al-Ahmari 12/02/2012 www.rhinologychair.org conference@rhinologychair.org Rhinology
Rhinology Chair Weekly Activity European position paper on Rhinosinusitis & Nnasal Polyps 2012 (summary) Mohammed s. Al-Ahmari 12/02/2012 www.rhinologychair.org conference@rhinologychair.org Rhinology
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Eosinophilic Rhinosinusitis is Not a Disease of Ostiomeatal Occlusion
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Eosinophilic Rhinosinusitis is Not a Disease of Ostiomeatal Occlusion Kornkiat Snidvongs, MD; David Chin,
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Eosinophilic Rhinosinusitis is Not a Disease of Ostiomeatal Occlusion Kornkiat Snidvongs, MD; David Chin,
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Evaluation of Modified FESS in Management of chronic rhinosinusitis
 Evaluation of Modified FESS in Management of chronic rhinosinusitis Mohamed A. El-Begermy, M.D.; Ossama H. Abdel-Latif, M.D.; Mohamed Albeltagy, M.D.* Department of Otolaryngology, Ain Shams University,
Evaluation of Modified FESS in Management of chronic rhinosinusitis Mohamed A. El-Begermy, M.D.; Ossama H. Abdel-Latif, M.D.; Mohamed Albeltagy, M.D.* Department of Otolaryngology, Ain Shams University,
Richard J. Harvey 26 Wall of the Maxillary Sinus Christos C. Georgalas and Wytske J. Fokkens 27 Pterygopalatine Space...
 Contents............................................................ viii Preface......................................................................... xi Acknowledgments.............................................................
Contents............................................................ viii Preface......................................................................... xi Acknowledgments.............................................................
OSTEITIS IN CRS. Rhinology Chair Meeting presented by Amal Binhazza a
 OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
Pediatric Endoscopic Sinus Surgery in a Tertiary Government Hospital: Patient Profile and Surgical Indications
 Philippine Journal Of Otolaryngology-Head And Neck Surgery Vol. 4 No. January June ichael Joseph C. David, D Gil. Vicente, D, Antonio H. Chua, D, Jose R. Reyes emorial edical Center St. Luke s edical Center
Philippine Journal Of Otolaryngology-Head And Neck Surgery Vol. 4 No. January June ichael Joseph C. David, D Gil. Vicente, D, Antonio H. Chua, D, Jose R. Reyes emorial edical Center St. Luke s edical Center
ISSN: Volume 4 Issue Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary. sinusitis
 ISSN: 2250-0359 Volume 4 Issue 3 2014 Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary sinusitis Thulasidas P ¹ Venkatraman V ² ¹ Sinus and Nose Hospital, Chennai, India,
ISSN: 2250-0359 Volume 4 Issue 3 2014 Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary sinusitis Thulasidas P ¹ Venkatraman V ² ¹ Sinus and Nose Hospital, Chennai, India,
STUDY OF CORRELATION BETWEEN NASAL ENDOSCOPY AND RHINOGENIC HEADACHE Santhosha Kumar B 1, Manjunath Rao S. V 2
 STUDY OF CORRELATION BETWEEN NASAL ENDOSCOPY AND RHINOGENIC HEADACHE Santhosha Kumar B 1, Manjunath Rao S. V 2 HOW TO CITE THIS ARTICLE: Santhosha Kumar B, Manjunath Rao S. V. Study of Correlation between
STUDY OF CORRELATION BETWEEN NASAL ENDOSCOPY AND RHINOGENIC HEADACHE Santhosha Kumar B 1, Manjunath Rao S. V 2 HOW TO CITE THIS ARTICLE: Santhosha Kumar B, Manjunath Rao S. V. Study of Correlation between
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): July 30, 2013 Most Recent Review Date (Revised): May 20, 2014 Effective Date: August 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): July 30, 2013 Most Recent Review Date (Revised): May 20, 2014 Effective Date: August 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
Advances in the Surgical Management of Chronic Rhinosinusitis
 Rhinitis and Sinusitis dvances in the Surgical Management of Chronic Rhinosinusitis Erin D. Wright, MDCM, MEd, FRCSC; Saul Frenkiel, MDCM, FRCSC bstract The surgical management of chronic rhinosinusitis
Rhinitis and Sinusitis dvances in the Surgical Management of Chronic Rhinosinusitis Erin D. Wright, MDCM, MEd, FRCSC; Saul Frenkiel, MDCM, FRCSC bstract The surgical management of chronic rhinosinusitis
Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery
 ORIGINAL ARTICLE Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery R L A Raja Ahmad, MS (ORL)*, B S Gendeh, MS (ORL)** Department of Otolaryngology-Head & Neck Surgery, Kulliyyah
ORIGINAL ARTICLE Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery R L A Raja Ahmad, MS (ORL)*, B S Gendeh, MS (ORL)** Department of Otolaryngology-Head & Neck Surgery, Kulliyyah
ORIGINAL ARTICLE. Toru Kikawada, MD; Takeo Nonoda, MD; Mariko Matsumoto, MD; Mikino Kikura, MD; Keiko Kikawada, MD
 ORIGINAL ARTILE Treatment of Intractable iseased Tissue in the Maxillary Sinus After Endoscopic Sinus Surgery With High-Pressure Water Jet and Preservation of the Periosteum Toru Kikawada, M; Takeo Nonoda,
ORIGINAL ARTILE Treatment of Intractable iseased Tissue in the Maxillary Sinus After Endoscopic Sinus Surgery With High-Pressure Water Jet and Preservation of the Periosteum Toru Kikawada, M; Takeo Nonoda,
FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)
 FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS) Protocol: SUR055 Effective Date: June 1, 2018 Table of Contents Page COMMERCIAL, MEDICAID AND MEDICARE COVERAGE RATIONALE... 1 DEFINITIONS... 2 DESCRIPTION OF
FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS) Protocol: SUR055 Effective Date: June 1, 2018 Table of Contents Page COMMERCIAL, MEDICAID AND MEDICARE COVERAGE RATIONALE... 1 DEFINITIONS... 2 DESCRIPTION OF
Protocol. Implantable Sinus Stents for Postoperative Use Following Endoscopic Sinus Surgery and for Recurrent Sinus Disease
 (701134) Medical Benefit Effective Date: 04/01/17 Next Review Date: 01/19 Preauthorization No Review Dates: 01/13, 01/14, 01/15, 01/16, 01/17, 01/18 This protocol considers this test or procedure investigational.
(701134) Medical Benefit Effective Date: 04/01/17 Next Review Date: 01/19 Preauthorization No Review Dates: 01/13, 01/14, 01/15, 01/16, 01/17, 01/18 This protocol considers this test or procedure investigational.
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
The advent of high-resolution computerized tomography
 An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients Jonathan Y. Ting,
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients Jonathan Y. Ting,
