CLINICAL SCIENCES. also termed perioptic neuritis, is an uncommon
|
|
|
- Nathan Lynch
- 5 years ago
- Views:
Transcription
1 Optic Perineuritis CLINICAL SCIENCES Clinical and Radiographic Features Valerie Purvin, MD; Aki Kawasaki, MD; Daniel M. Jacobson, MD Background: Optic perineuritis is an uncommon variety of orbital inflammatory disease that is distinct from demyelinating optic neuritis. Objective: To describe the clinical and radiographic features of idiopathic optic perineuritis, with particular emphasis on those features that help to distinguish this condition from optic neuritis. Methods: We reviewed the medical records of 14 patients with optic perineuritis who were seen in 2 neuroophthalmology clinics. Results: Patients ranged in age from 24 to years; 5 were older than 50 years. All patients had visual loss, eye pain, or both. The visual acuity was 20/20 or better in 8 of the 15 eyes. The results of visual field testing were normal in 2 eyes, and a paracentral scotoma or an arcuate defect was seen in 7. Magnetic resonance imaging scans demonstrated circumferential enhancement around the optic nerve, sometimes with intraorbital extension. Response to corticosteroids was dramatic; however, 4 patients had a relapse with lowering of the dose. Conclusions: In contrast to those with optic neuritis, patients with optic perineuritis are often older at onset and are more likely to show sparing of central vision. Magnetic resonance imaging scans demonstrate enhancement around, rather than within, the optic nerve. Response to corticosteroids is more dramatic than in patients with optic neuritis, and patients are more likely to experience recurrence after stopping treatment. Arch Ophthalmol. 2001;119: From the Midwest Eye Institute and the Departments of Neurology and Ophthalmology, Indiana University Medical Center, Indianapolis (Drs Purvin and Kawasaki); and the Marshfield Clinic, Marshfield, Wis (Dr Jacobson). OPTIC perineuritis (OPN), also termed perioptic neuritis, is an uncommon inflammatory disorder involving the optic nerve sheath. Historically, the term has been used to describe several different clinical entities. 1 In recent years, OPN has generally been understood to represent a form of idiopathic orbital inflammatory disease, in which the specific target tissue is the optic nerve sheath. 2 While most cases are isolated and idiopathic, OPN occasionally occurs as a manifestation of a specific infectious or inflammatory disorder, such as Wegener granulomatosis or giant cell arteritis. 3 Radiographically, OPN may simulate optic nerve sheath meningioma, 4 but clinically it is more likely to be mistaken for acute demyelinating optic neuritis (ON). In both OPN and ON, patients typically experience acute monocular visual loss, pain with eye movement, and either a normal or a swollen optic disc. The natural history of and response to treatment for these 2 conditions, however, may differ. It is, therefore, important to identify any clinical and radiographic features that might help in distinguishing the 2 expediently. To better characterize the clinical features of OPN, we reviewed the medical records and radiographic studies of 14 affected patients. We paid particular attention to features that might be helpful in distinguishing OPN from ON. RESULTS The 14 patients included 10 women and 4 men, ranging in age from 24 to years (mean, 41 years; median, years) (Table 1). Five patients were older than 50 years at onset. Ocular involvement was monocular when first seen in 13 patients and binocular in 1 (patient 12). Thus, data for 15 eyes were analyzed. All patients had symptoms of visual loss, eye pain, or both. Eight patients had visual loss and eye pain that was commonly exacerbated by eye movement. Pain was absent in 1 patient (patient 2) at onset but developed 3 months later. Pain was not associated with subjective visual loss 1299
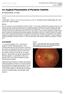
2 PATIENTS AND METHODS The diagnosis of OPN was made in patients who had an acute optic neuropathy and/or disc edema plus either radiographic demonstration of enhancement of the optic nerve sheath or histopathologic evidence of perineural inflammation. We excluded patients with clinical or radiographic evidence of a more widespread orbital process (eg, significant exophthalmos or prominent enlargement or enhancement of extraocular muscles). The presence of subtle orbital abnormalities was not considered an exclusionary factor. Patients were also excluded if they had an established systemic disorder associated with orbital inflammation or if their or a subsequent clinical course evaluation revealed a specific systemic illness as the cause of their optic nerve sheath inflammation. Patients were followed up for a long enough period to ensure that an infectious or neoplastic leptomeningeal process was not present. We analyzed symptoms, optic nerve function (visual acuity, color vision, and visual field), optic disc appearance, and radiographic findings. Response to treatment and long-term course were also studied. All patients underwent laboratory testing to exclude specific systemic inflammatory diseases. In all patients, the complete blood cell count, the erythrocyte sedimentation rate, and the levels of antinuclear antibodies and angiotensin-converting enzyme were determined; a syphilis serologic test was performed; and a chest x-ray film was obtained. All patients underwent magnetic resonance imaging (MRI) of the head and orbits with fat suppression and contrast infusion. In addition, 7 patients underwent testing for antineutrophil cytoplasmic antibodies (including all patients with intracranial extension), 3 were tested for Lyme disease, and 3 underwent a lumbar puncture. A biopsy of the optic nerve lesion was performed in 2 patients. in 5 eyes (patients 1, 4, 9, 12, and 13). Visual loss was variably described as blurring, dimming, splotches, or a spot in vision. Pertinent findings are summarized in Table 1. The visual acuity when first seen was 20/20 or better in 8 (53%) of the 15 eyes. The results of the visual field examination were normal in 2 (13%) of the 15 eyes. Three eyes demonstrated an arcuate defect, and 4 had a paracentral scotoma. A central scotoma or central depression was found in 3 eyes, and only a remaining peripheral island was seen in 2. Disc edema was observed in 10 eyes. Mild motility disturbance was found in 4 eyes (patients 5, 7, 9, and 14). Mild ptosis was seen in 2 patients (patients 6 and 9), and developed later in the course of 2 additional eyes (patients 2 and 14). Magnetic resonance imaging scans demonstrated enhancement around the intraorbital optic nerve in 13 patients. In 1 patient (patient 14), enhancement appeared to involve the full thickness of the optic nerve, and in this patient the diagnosis was based on pathologic examination results. In another patient (patient 8), the MRI scan showed sheath and optic nerve enhancement. There was intracranial extension in 3 patients (patients 2, 8, and 14). None of the scans revealed white matter lesions. All patients had normal laboratory test results, except 1 (patient 7) in whom the fluorescent treponemal antibody absorption test result was weakly positive. In this patient, the results of confirmatory serologic tests (the VDRL test and microhemagglutination treponemal pallidum) and the cerebrospinal fluid fluorescent treponemal antibody absorption test were negative. A biopsy specimen of the optic nerve lesion in 2 patients (patients 2 and 14) showed acute and chronic inflammatory changes without granulomas or vasculitis (Figure 1). All 3 patients with intracranial extension underwent an expanded evaluation for granulomatous disease, including testing for antineutrophil cytoplasmic antibodies (perinuclear antineutrophil cytoplasmic antibody and cytoplasmic antineutrophil cytoplasmic antibody) and chest radiography. The results of these studies were normal. Twelve patients were treated initially with prednisone, typically or 80 mg/d, and 2 were treated initially with indomethacin. All experienced dramatic relief of eye pain, usually within 24 hours of starting treatment, and prompt improvement of vision (within days of initiating corticosteroid therapy). Four patients had a relapse when the corticosteroid dose was reduced, necessitating the use of additional treatment modalities, including intravenous methylprednisolone (2 patients), peribulbar corticosteroids (1 patient), azathioprine (2 patients), and radiation therapy (2 patients). The final visual acuity was 20/25 or better in 12 (80%) of the 15 eyes. Two patients (patients 2 and 14) experienced a poor visual outcome, in each instance associated with a delay in initiating corticosteroid treatment (Table 2). Follow-up intervals ranged from 1 month to 6 years (mean, months; median, months) (Table 2). PATIENT 1 A 26-year-old woman developed right retro-orbital pain exacerbated by eye movement and mild photophobia 2 weeks following an upper respiratory tract infection. The results of an ophthalmologic examination 2 weeks after onset revealed right optic disc edema and subjective color desaturation; otherwise, the test results of optic nerve function were normal. An MRI scan showed enhancement around the right optic nerve (Figure 2). Two weeks later, she began treatment with prednisone, 40 mg/d, which was tapered over 12 days. This brought prompt relief of pain, but the visual acuity declined from 20/20 to 20/40 OD. Eight weeks after the onset of symptoms, she was seen in neuro-ophthalmologic consultation. Her visual acuity was 20/80 OD and 20/20 OS. Goldmann perimetry in the right eye showed an absolute inferior arcuate scotoma plus a smaller superior scotoma (Figure 3). The visual field in the left eye was normal. There was a +2 right relative afferent pupillary defect. The results of external biomicroscopy and ocular motility examinations were normal. The results of a fundus examination revealed moderate hyperemic right optic disc edema and a normal left optic disc (Figure 4). Additional laboratory testing included the determination of the complete blood cell count, the erythrocyte 1300
3 Table 1. Clinical Features When Initially Seen* Patient No./ Sex/Age, y Symptoms Medical History VA in the Involved Eye VF Findings 1/F/26 Pain with EM Preceding URTI 20/20 Inferior arcuate defect 2/M/37 3/M/53 Foggy vision and pain 3 mo later Pain with EM and splotches with exercise None 20/ Inferior paracentral scotoma Remote CRVO 20/20 Superior arcuate defect Optic Disc Findings Other Examination Findings MRI Findings Edema... ONS enhancement and within-orbital fat Normal Mild ptosis and ONS enhancement at decreased upgaze the apex with an later intracranial extension Normal... Thickened ONS with enhancement 4/F/32 Pain on EM Asthma 20/20 Superior paracentral Normal... ONS enhancement scotoma 5/F/31 Pain with EM, None 20/20 Normal Edema Small left ONS enhancement blurring, and diplopia hypertropia 6/F/32 Pain on EM and film over vision None 20/25 Inferior paracentral scotoma Normal Slight ptosis Subtle ONS enhancement 7/F/55 8/F/ 9/F/57 10/M/33 11/F/51 12/M/42 Pain, diplopia, and a spot in vision Decreased vision and pain on EM Pain with EM, slight ptosis, and conjunctival injection Pain with EM and cloudy vision Cloudy vision and eye pain Eye ache in both eyes and mild dimming in the right eye Postoperative DVT HT and osteoarthritis Meniere disease and a preceding febrile illness None, but a preceding URTI 20/300 Central scotoma Normal Mild abduction deficit and right HT 20/40 Small central scotoma ONS enhancement at the apex Moderate edema 1-mm ptosis Enhancement of the optic nerve and orbital fat 20/30 Enlarged blind spot Mild edema Slight abduction deficit, slight ptosis, and mild injection over MR 20/20 Inferior arcuate defect Moderate disc edema None LP Temporal island Mild to moderate edema None 20/20 OD Paracentral Mild edema in and depression in both eyes 20/15 OS the right eye and normal in the left eye 13/F/24 Eye pain Asthma 20/15 Mild central depression 14/F/42 Eye pain for 6 mo and decreased vision in the left eye (left ptosis 3 mo after onset) None CF Temporal island Edema and pallor Mild injection over LR and 0.5-mm exophthalmos ONS and ON enhancement with an intracranial extension ONS enhancement and fat... ONS enhancement... ONS enhancement and fat Mild edema... ONS enhancement and fat Ptosis, eyelid Thickening and edema, enhancement of the ophthalmoparesis, optic nerve with and 2-mm intracranial exophthalmos involvement *VA indicates visual acuity; VF, visual field; MRI, magnetic resonance imaging; EM, eye movement; URTI, upper respiratory tract infection; ONS, optic nerve sheath; CRVO, central retinal vein occlusion; DVT, deep vein thrombosis; HT, hypertension; MR, medial rectus; ON, optic nerve; LR, lateral rectus; LP, light perception; CF, counting fingers; and ellipses, data not applicable. sedimentation rate, and the levels of antinuclear antibodies and angiotensin-converting enzyme and the performance of a syphilis serologic test and chest radiography; the results of all tests were normal or negative. Corticosteroid treatment was reinstituted, starting this time at 80 mg/d and decreasing by 20 mg/wk. The results of reexamination 4 weeks later showed improvement of the visual acuity to 20/20 OD. The visual field was also much improved, showing only mild central depression. Right optic disc edema had resolved, and the disc was mildly pale. PATIENT 2 A 37-year-old previously healthy man experienced foggy vision in his left eye accompanied by a few sparkles of light. He had a sensation of heaviness of the involved eye but no actual eye pain and no discomfort with eye movement. The results of an eye examination 2 weeks after onset showed a visual acuity of 20/ OS, with a 0.9 log unit relative afferent pupil defect and normal optic discs. Goldmann perimetry in the left eye revealed mild central depression and a small scotoma inferior to fixation. Laboratory test results were all normal or negative, and an MRI scan of the head and orbits was interpreted as normal. Reexamination 5 weeks later showed no change in visual acuity, but visual field testing revealed mild additional central depression in the left eye. He received a course of prednisone, 80 mg/d, which was tapered over 4 weeks. Optic nerve function improved; however, 2 months later he experienced abrupt onset of severe left retro-orbital pain with worsening of vision. He did not seek medical attention until 1 month later, at which time an MRI scan demonstrated enhancement around the apical portion of the left optic nerve with extension intracranially (Figure 5). 1301
4 A B M S Figure 1. Patient 14. An excisional biopsy specimen of the left optic nerve of a 42-year-old otherwise healthy woman who experienced progressive painful visual loss in the affected eye over 6 months, unresponsive to corticosteroids. A malignant optic nerve glioma was suspected. A, A low-magnification axial photomicrograph of the optic nerve and sheath complex showing marked thickening of the perioptic meninges (M) and, to a less dramatic extent, the pia mater (white arrow) due to fibrosis and inflammatory infiltration. The infiltrate also extends into the pial septa (black arrow) (hematoxylin-eosin, original magnification 10). B, There is marked expansion of the pial septa (S) by the chronic inflammatory cell infiltrate. The parenchyma of the adjacent optic nerve is slightly infiltrated by lymphocytes (hematoxylin-eosin, original magnification 10). Table 2. Clinical Course* Patient No. Treatment Course 1 Prednisone Low-dose prednisone for 12 d: decreased pain but persistent edema and worse vision; then high-dose prednisone for 4 wk: resolution of disc edema and improved vision; 2 more recurrences again responded to prednisone 2 Prednisone, IV Initial good response to prednisone; mild ptosis and motility disturbance methylprednisolone, 3 mo after onset; lost to follow-up for 1 mo; worse vision responded only RT, and azathioprine modestly to IV corticosteroids; biopsy specimen showed inflammatory cells; stable following RT, taking prednisone and azathioprine 3 Prednisone, IV methylprednisolone, peribulbar corticosteroids, azathioprine, and RT Multiple recurrences with good response to corticosteroids each time; following RT for corticosteroid dependency, stable for 2 y while taking prednisone and azathioprine Final Visual Acuity Follow-up Interval 20/ y CF 2 y 20/25 5 y 4 Prednisone Pain gone in 2 d, and dose tapered over 3 mo 20/20 7 mo 5 Indomethacin Resolved and stable following treatment 20/20 4 mo 6 Indomethacin Improved over 4 wk and no recurrence since 20/20 3 y 7 Prednisone Favorable response to prednisone and stable since 20/25 2 y 8 IV methylprednisolone and prednisone Initial response to brief oral prednisone therapy, but vision worsened when stopped; repeated treatment with a high dose IV brought prompt pain relief and visual recovery; recovery was maintained over a 2-mo taper and since 20/15 6 mo 9 Prednisone Pain gone in a few days, optic nerve function normalized, slowly tapered over 20/ mo a few months, and stable since 10 Prednisone Pain resolved in 2 h, and vision better in 1 wk; unavailable for further 20/15 1 mo follow-up 11 Prednisone Pain resolved in 2 d, and vision improved in 3 d; residual decreased visual 20/50 12 mo acuity and inferior arcuate defect 12 Prednisone Pain resolved in 1 d, and vision improved in 2 d; dose was slowly tapered 20/20 OU 2 mo 13 Prednisone Improved with corticosteroids, which were slowly tapered 20/15 4 mo 14 Prednisone 6-mo progression before diagnosis, excisional biopsy specimen showed fibrosis and inflammation, and stable since NLP 6 y *IV indicates intravenous; RT, radiation therapy; CF, counting fingers; and NLP, no light perception. In retrospect, enhancement around the apical optic nerve could be identified on his initial scan as well. His visual acuity had declined to hand motions OS, with a large dense central scotoma. He enjoyed only a modest response to intravenous methylprednisolone followed by oral prednisone. His vision worsened again 2 months later, at which time he received a course of radiation therapy consisting of 2520 rads (25.2 Gy) in 14 fractions. Recurrence of pain 4 months later was treated with low-dose alternate-day prednisone plus azathioprine. He has been stable for 18 months, since beginning this regimen. COMMENT Optic perineuritis was first described by Edmunds and Lawford 5 in These researchers distinguished between 2 forms of the disorder: exudative and purulent. The exudative form consisted of a localized nonsuppurative pachymeningitis. 1 The purulent form was associ- 1302
5 A R I I I I I I 3 I Figure 3. Patient 1. Goldmann perimetry in the right eye shows an absolute inferior arcuate scotoma and a smaller less dense scotoma in the superior Bjerrum area. The field in the left eye is normal. B R Figure 2. Patient 1. Magnetic resonance imaging scan of the head and orbits, with contrast infusion and fat suppression. A, The axial view shows enhancement around the right intraorbital optic nerve with some streakiness of the surrounding orbital fat. R indicates right side. B, The coronal view confirms that the enhancement is around, rather than within, the optic nerve. ated with leptomeningitis that had extended to involve the subarachnoid space surrounding the optic nerves. In many such cases of OPN, optic nerve function has been said to be normal, an observation consistent with the concept that the inflammatory infiltrate is loosely organized around the optic nerve. More recently, the term OPN has been used to designate a form of orbital inflammatory disease in which the main focus of the inflammatory response is the optic nerve sheath. 6 Other focal forms of orbital inflammatory disease include periscleritis, orbital myositis, and dacryoadenitis. 7 Dutton and Anderson 4 described the clinical, radiographic, and pathologic features of 4 patients with OPN in whom enlargement of the intraorbital optic nerve was thought to represent an optic nerve sheath meningioma. Biopsy specimens, however, demonstrated inflammatory infiltration of the dural sheath in 2 patients and dense perineural fibrous tissue in the other 2. None were associated with a specific inflammatory disorder. Of the 4 patients, 3 differed clinically from patients with optic nerve sheath meningioma in that head and eye pain was prominent. Only 1 of the 4 patients was treated with corticosteroids, which stabilized vision for 6 months until complications led to their discontinuance. A patient with bilateral idiopathic optic nerve sheath inflammation, described by Margo et al, 8 did not experience a beneficial response to corticosteroids. A full-thickness biopsy specimen of the more severely involved optic nerve revealed chronic inflammation of the optic nerve sheath with vasculitic changes and necrobiotic granulomas. Visual loss was attributed in large part to secondary ischemic infarction of the optic nerve, presumably due to circumferential compression of the optic nerve periphery by the mass of the thickened optic nerve sheath. 8 Two similar patients, in whom visual loss was due to vascular occlusion, were described by Winterkorn et al 9 ; however, a biopsy was not performed. The pathologic changes of the optic nerve sheath and the optic nerve that were present in our patients and in those that have been previously described suggest that the clinically defined entity of OPN likely encompasses a spectrum of disorders. Regardless of what unknown process incites the initial inflammatory process in idiopathic cases, the common pathologic reaction consists of marked thickening of the optic nerve sheath due to nonspecific fibrosis. 4 Various stages of predominantly lymphocytic infiltration are usually present. In the case reported by Margo et al, 8 foci of degenerating (necrobiotic) collagen were present in the optic nerve sheath. Of the 4 patients described by Dutton and Anderson, 4 1 showed granulomatous inflammation in the sheath. Visual loss in those patients in whom a biopsy of the optic nerve was performed or in whom the optic nerve was excised correlated with the presence of either optic nerve demyelination 7,10 or infarction. 8 Perivascular lymphocytic infiltration of small optic nerve vessels (vasculitis) has been identified in some patients. 7,11 In most cases of suspected OPN, an optic nerve biopsy is not indicated. The diagnosis is typically based on a combination of clinical and radiographic findings. Neuroimaging in patients with OPN typically shows a characteristic pattern of enhancement around the optic nerve 1303
6 A B Figure 4. Patient 1. Fundus photographs taken 8 weeks after the onset of symptoms show persistent right optic disc edema (A) and a normal left optic disc (B). A B Figure 5. Patient 2. A magnetic resonance imaging scan with contrast infusion obtained 4 months after the onset of visual symptoms. A, The coronal view through the orbital apex shows enhancement around the left optic nerve. There is also mild enlargement and enhancement of extraocular muscles. B, The coronal view more posteriorly demonstrates extension of the inflammatory process intracranially to the anterior cavernous sinus and along the planum sphenoidale. ( tramtrack on axial views and doughnut on coronal views). In addition, MRI scans in some cases show streaky enhancement of orbital fat (Figure 2). These radiographic changes are not found in patients with typical demyelinating ON. In occasional cases of OPN, the substance of the optic nerve also shows enhancement, 12 presumably due to inflammation of intraneural pial septa as well as the nerve sheath. Two of our patients exhibited this finding, with histopathologic correlation demonstrated in 1. In some patients, close inspection may reveal subtle enhancement of extraocular muscles and/or sclera in addition to the characteristic changes in the optic nerve sheath (Figure 5). A careful inspection for these changes may be particularly helpful in cases in which the perineural findings are subtle or indeterminant and particularly in those scans that demonstrate intraneural enhancement. Computed tomographic scanning does not usually provide sufficient spatial resolution to distinguish perineural enhancement from the intraneural enhancement seen in demyelinating ON. Recent advances in MRI, specifically the use of dedicated orbital views with fat suppression and gadolinium, have enabled us to make this distinction. Accordingly, we suspect that the prevalence of this disorder has been underestimated. In the pre-mri era, some cases of OPN may have been diagnosed as being atypical corticosteroid-responsive ON. Based on shared clinical features, patients with OPN are likely to be misdiagnosed initially as having ON. Similar to those with ON, most patients with OPN are women (71% [10 of 14 patients] in our series) and most experience acute monocular visual loss accompanied by eye pain. In patients with both disorders, eye pain is commonly exacerbated by eye movement. Disc edema is often present in patients with both conditions (found in 10 of the 15 eyes in our series). Treatment considerations and prognosis, however, differ for these 2 disorders, particularly regard- 1304
7 ing the future development of multiple sclerosis. Based on our data, we found several features to be helpful in distinguishing OPN from ON (Table 3). The age distribution of patients with OPN is broader, and the average age is older than in patients with ON. Our patients age ranged from 24 to years (mean, 41 years). The average age of patients with ON is years; only 15% of cases occur in individuals older than 50 years. 13 In contrast, 5 (36%) of our 14 patients were older than 50 years. The tempo and pattern of visual loss also differed in our patients compared with those with ON. In contrast to visual loss in patients with ON, which usually occurs over several days, visual loss in many of our patients with OPN progressed for several weeks before they were correctly diagnosed and treatment was initiated. Although occasional patients with ON demonstrate sparing of central vision, we found this to be a common pattern in patients with OPN. The visual acuity was 20/20 in 8 (53%) of the 15 eyes. The results of visual field testing were normal in 3 eyes; a paracentral scotoma was seen in 4, and an arcuate defect was seen in 3. Thus, 10 of the 15 eyes demonstrated sparing of central vision. In contrast, in a study of 103 patients with ON, Perkin and Rose 13 found only 4.2% to have central sparing. In keeping with their tendency to spare central vision, the degree of dyschromatopsia was less than typically seen in patients with ON. Mild motility disturbance, due to extraocular muscle inflammation, is occasionally a helpful feature. Four of the 14 patients had abnormal ocular motility, based either on eliciting a history of diplopia or on examination findings. One of these 4 and an additional patient exhibited mild ptosis in the involved eye, and 2 others developed mild ptosis later in their course. These are not typical features of ON (unless there is associated brainstem involvement due to multifocal demyelinating disease), and their presence in a patient suspected of having ON should suggest the alternative diagnosis of OPN. Finally, the response to treatment may help in differentiating OPN from ON. Of our 14 patients with OPN, 12 were treated with corticosteroids, and all demonstrated dramatic relief of pain on initiating treatment, typically within hours and all within a day. Visual loss also showed prompt recovery. Relapse following discontinuation of treatment, however, was common. These features, particularly the recurrence of pain and/or visual loss on corticosteroid tapering, should suggest a diagnosis of OPN rather than ON. Specific inflammatory and neoplastic entities, such as sarcoidosis, lymphoma, leptomeningeal carcinomatosis, and some fungal infiltrations, may demonstrate a similar response to treatment. These disorders, however, soon declare themselves by demonstrating recurrence and progression with or without continued corticosteroid treatment. The prognosis for visual outcome in patients with OPN is generally excellent. This is greatly influenced, however, by the interval between the onset of visual loss and the initiation of treatment. In 2 patients with a poor visual outcome, treatment was delayed by a month or more. Table 3. Features That Distinguish Optic Neuritis From Optic Perineuritis Feature Optic Neuritis Optic Perineuritis Age at onset Usually young adults (only 15% are 50 y) Broader range (36% are 50 y) Visual loss Usually central Often paracentral or arcuate Time course Progression over days Progression over weeks Natural history Spontaneous recovery Progressive visual loss Response to corticosteroid treatment Variable; uncommon relapse after stopping Prompt and dramatic; common relapse after brief treatment Magnetic resonance imaging scan findings Optic nerve enhancement with or without white matter lesions Perineural enhancement and streaky fat with or without extraocular muscle enhancement The other factor that influences prognosis is the frequency of recurrent attacks. Initiating treatment with higher doses of corticosteroids (eg, prednisone, 80 mg/d) and more prolonged treatment at this level appear to lessen the likelihood of recurrent attacks. The possibility of OPN should be considered in all patients in whom ON is diagnosed. Magnetic resonance imaging is particularly important in patients with clinical findings that are atypical for demyelinating ON. Specifically, these would include age older than 45 years, sparing of central vision, visual loss progressing for longer than 2 weeks, persistence of disc edema, recurrence of pain, and visual loss after discontinuing corticosteroid therapy. Patients in whom pain is particularly severe or is out of proportion to visual loss might also be considered in this category. Careful scrutiny, in terms of history and physical examination, for evidence of orbital involvement (diplopia, subtle ptosis, and chemosis) may also help to identify these patients. It is important to accurately distinguish between OPN and ON for 2 reasons. First, the prognosis is different in these disorders. Patients with ON are at high risk of developing multiple sclerosis and should be counseled accordingly. Patients with OPN, in contrast, are not at increased risk for demyelinating disease but are likely to experience a recurrence of visual loss in the future. Second, treatment considerations differ for the 2 entities. Corticosteroids have not been shown to influence the visual outcome in patients with ON and, therefore, many patients with ON are managed expectantly (ie, without treatment). Patients with OPN, however, will continue to lose vision, in some cases irreversibly, unless treated with corticosteroids or other antiinflammatory agents. Furthermore, the dosage and route of administration differ. The recommended regimen for OPN (oral prednisone, 80 mg/d) is contraindicated in patients with ON because of the association of this treatment with recurrences of ON. On the other hand, the rather short (2-week) course of corticosteroid treatment used in patients with ON is not long enough to achieve lasting remission in most patients with OPN. 1305
8 Accepted for publication February 1, Corresponding author and reprints: Valerie A. Purvin, MD, Midwest Eye Institute, 201 Pennsylvania Pkwy, Indianapolis, IN ( REFERENCES 1. Miller NR, Newman NJ. Walsh and Hoyt s Clinical Neuro-ophthalmology. 5th ed. Baltimore, Md: Williams & Wilkins; Kennerdell JS, Dresner SC. The nonspecific orbital inflammatory syndromes. Surv Ophthalmol. 1984;29: Nassani S, Cocito L, Arcuri T, Favale E. Orbital pseudotumor as a presenting sign of temporal arteritis. Clin Exp Rheumatol. 1995;13: Dutton JJ, Anderson RL. Idiopathic inflammatory perioptic neuritis simulating optic nerve sheath meningioma. Am J Ophthalmol. 1985;100: Edmunds W, Lawford JB. Examination of optic nerve from cases of amblyopia in diabetes. Trans Ophthalmol Soc U K. 1883;3: Rootman J. Diseases of the Orbit. Philadelphia, Pa: JB Lippincott Co; Rush JA, Kennerdell JS, Donin JF. Acute periscleritis: a variant of idiopathic orbital inflammation. Orbit. 1982;4: Margo CE, Levy MH, Beck RW. Bilateral idiopathic inflammation of the optic nerve sheaths. Ophthalmology. 1989;96: Winterkorn JMS, Odel JG, Behrens MM, Hilal S. Large optic nerve with central retinal artery and vein occlusions from optic neuritis/perineuritis rather than tumor. J Neuroophthalmol. 1994;14: Hykin PG, Spalton DJ. Bilateral perineuritis of the optic nerves. J Neurol Neurosurg Psychiatry. 1991;54: Zhang TL, Shao SF, Zhang T, et al. Idiopathic inflammation of optic nerve simulating optic nerve sheath meningioma: CT demonstration. J Comput Assist Tomogr. 1987;11: Fay AM, Kane SA, Kazim M, et al. Magnetic resonance imaging of optic perineuritis. J Neuroophthalmol. 1997;17: Perkin GD, Rose FC. Optic Neuritis and Its Differential Diagnosis. New York, NY: Oxford University Press Inc; 1979:22. ARCHIVES Web Quiz Winner Congratulations to the winner of our May quiz, Noemi Lois, MD, PhD, Retina Service, Ophthalmology Department, Aberdeen Royal Infirmary, Aberdeen, Scotland. The correct answer to our May challenge was juxtafoveal retinal pigment epithelial hamartoma. For a complete discussion of this case, see the Clinicopathologic Reports, Case Reports, and Small Case Series section in the June ARCHIVES (Holz FG, Alexandridis E, Völcker HE, Dithmar S, Grossniklaus HE. Spontaneous incomplete avulsion of juxtafoveal retinal pigment epithelial hamartoma. Arch Ophthalmol. 2001;119: ). Be sure to visit the Archives of Ophthalmology World Wide Web site ( and try your hand at our Clinical Challenge Interactive Quiz. We invite visitors to make a diagnosis based on selected information from a case report or other feature scheduled to be published in the following month s print edition of the ARCHIVES. The first visitor to our Web editors with the correct answer will be recognized in the print journal and on our Web site and will also receive a free copy of the book The Art of JAMA II. 1306
Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in a Young Patient
 Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Neuro-Ocular Grand Rounds
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
CHIASMAL NEURITIS IS A
 CLINICAL SCIENCES Idiopathic Chiasmal Neuritis Clinical Features and Prognosis Aki Kawasaki, MD; Valerie A. Purvin, MD Objectives: To describe the clinical features of idiopathic chiasmal neuritis in a
CLINICAL SCIENCES Idiopathic Chiasmal Neuritis Clinical Features and Prognosis Aki Kawasaki, MD; Valerie A. Purvin, MD Objectives: To describe the clinical features of idiopathic chiasmal neuritis in a
Role Of Various Factors In The Treatment Of Optic Neuritis----A Study Abstract Aim: Materials & Methods Discussion: Conclusion: Key words
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 9 Ver. X (September). 2016), PP 51-57 www.iosrjournals.org Role Of Various Factors In The Treatment
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Alan G. Kabat, OD, FAAO (901)
 THE SWOLLEN OPTIC DISC: EMERGENCY OR ANOMALY? Alan G. Kabat, OD, FAAO (901) 252-3691 Memphis, Tennessee alan.kabat@alankabat.com Course description: The swollen disc presents a diagnostic dilemma. While
THE SWOLLEN OPTIC DISC: EMERGENCY OR ANOMALY? Alan G. Kabat, OD, FAAO (901) 252-3691 Memphis, Tennessee alan.kabat@alankabat.com Course description: The swollen disc presents a diagnostic dilemma. While
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland
 Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Neuro-Ocular Grand Rounds Anthony B. Litwak,OD, FAAO VA Medical Center Baltimore, Maryland Dr. Litwak is on the speaker and advisory boards for Alcon and Zeiss Meditek COMMON OPTIC NEUROPATHIES THAT CAN
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Neuro-ophthalmologyophthalmology. Marek Michalec, MD.
 Neuro-ophthalmologyophthalmology Marek Michalec, MD. Neuro-ophthalmology Study integrating ophthalmology and neurology Disorders affecting parts of CNS devoted to vision or eye: Afferent system (visual
Neuro-ophthalmologyophthalmology Marek Michalec, MD. Neuro-ophthalmology Study integrating ophthalmology and neurology Disorders affecting parts of CNS devoted to vision or eye: Afferent system (visual
Clinical Characteristics of Optic Neuritis in Koreans Greater than 50 Years of Age
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(2):111-115 http://dx.doi.org/10.3341/kjo.2012.26.2.111 Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(2):111-115 http://dx.doi.org/10.3341/kjo.2012.26.2.111 Original Article Clinical Characteristics of Optic Neuritis in Koreans Greater than
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome
 A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome medicine2.missouri.edu/jahm/patient-presenting-ptosis-ophthalmoplegia-decreased-periorbital-sensations-facial-drooptolosa-hunt-syndrome/
A Patient Presenting with Ptosis, Ophthalmoplegia, and Decreased Periorbital Sensations and Facial Droop in Tolosa-Hunt Syndrome medicine2.missouri.edu/jahm/patient-presenting-ptosis-ophthalmoplegia-decreased-periorbital-sensations-facial-drooptolosa-hunt-syndrome/
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD
 Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Sequential non-arteritic anterior ischemic optic neuropathy (NAION) Jonathan A. Micieli, MD Valérie Biousse, MD A 68 year old white woman had a new onset of floaters in her right eye and was found to have
Neuro-Ophthalmic Masqueraders
 Neuro-Ophthalmic Masqueraders Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Mayo Clinic Health System in Albert Lea Denise Goodwin, OD, FAAO Pacific University College of Optometry Please silence all mobile
Neuro-Ophthalmic Masqueraders Leonid Skorin, Jr., OD, DO, MS, FAAO, FAOCO Mayo Clinic Health System in Albert Lea Denise Goodwin, OD, FAAO Pacific University College of Optometry Please silence all mobile
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
Index Note: Page numbers of article titles are in boldface type. A Acetazolamide, in idiopathic intracranial hypertension, 49 52, 60 Angiography, computed tomography, in cranial nerve palsy, 103 107 digital
In some patients with pituitary macroadenoma, visual acuity
 ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
ORIGINAL RESEARCH A.M. Tokumaru I. Sakata H. Terada S. Kosuda H. Nawashiro M. Yoshii Optic Nerve Hyperintensity on T2-Weighted Images among Patients with Pituitary Macroadenoma: Correlation with Visual
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings. Jonathan A. Micieli, MD Valérie Biousse, MD
 Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
Learn Connect Succeed. JCAHPO Regional Meetings 2015
 Learn Connect Succeed JCAHPO Regional Meetings 2015 OPTIC NEUROPATHY AS EASY AS 1,2,3,4 OPTIC NERVE ANATOMY M. Tariq Bhatti, MD Departments of Ophthalmology and Neurology Duke Eye Center and Duke University
Learn Connect Succeed JCAHPO Regional Meetings 2015 OPTIC NEUROPATHY AS EASY AS 1,2,3,4 OPTIC NERVE ANATOMY M. Tariq Bhatti, MD Departments of Ophthalmology and Neurology Duke Eye Center and Duke University
Temporal arteritis. Occurrence of ocular complications 7 years after diagnosis. University of Edinburgh, and Royal Infirmary of Edinburgh
 Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Neuro Ocular Grand Rounds Anthony B. Litwak, OD, FAAO VA Medical Center Baltimore, MD
 Neuro Ocular Grand Rounds Anthony B. Litwak, OD, FAAO VA Medical Center Baltimore, MD 58 YOWM! C/O I think there is something wrong with my vision, but I m not sure what it is.! +PMH for HTN, atrial fibrillation,
Neuro Ocular Grand Rounds Anthony B. Litwak, OD, FAAO VA Medical Center Baltimore, MD 58 YOWM! C/O I think there is something wrong with my vision, but I m not sure what it is.! +PMH for HTN, atrial fibrillation,
IMAGE OF THE MOMENT PRACTICAL NEUROLOGY
 178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
178 PRACTICAL NEUROLOGY IMAGE OF THE MOMENT Gawn G. McIlwaine*, James H. Vallance* and Christian J. Lueck *Princess Alexandra Eye Pavilion, Chalmers Street, Edinburgh UK; The Canberra Hospital, P.O. Box
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Optic Nerve Disorders: Structure and Function and Causes
 Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
Optic Nerve Disorders: Structure and Function and Causes Using Visual Fields, OCT and B-scan Ultrasound to Diagnose and Follow Optic Nerve Visual Losses Ohio Ophthalmological Society and Ophthalmic Tech
THE SWOLLEN DISC. Valerie Biousse, MD Emory University School of Medicine Atlanta, GA
 THE SWOLLEN DISC Valerie Biousse, MD Emory University School of Medicine Atlanta, GA Updated from: Neuro-Ophthalmology Illustrated. Biousse V, Newman NJ. Thieme, New-York,NY. 2 nd Ed, 2016. Edema of the
THE SWOLLEN DISC Valerie Biousse, MD Emory University School of Medicine Atlanta, GA Updated from: Neuro-Ophthalmology Illustrated. Biousse V, Newman NJ. Thieme, New-York,NY. 2 nd Ed, 2016. Edema of the
CHRONIC RETROBULBAR AND CHIASMAL NEURITIS*t
 Brit. J. Ophthal. (1967) 51, 698 CHRONIC RETROBULBAR AND CHIASMAL NEURITIS*t BY From the Department of Medicine, University of Bristol, and the United Bristol Hospitals AcuTE retrobulbar neuritis is a
Brit. J. Ophthal. (1967) 51, 698 CHRONIC RETROBULBAR AND CHIASMAL NEURITIS*t BY From the Department of Medicine, University of Bristol, and the United Bristol Hospitals AcuTE retrobulbar neuritis is a
IDIOPATHIC INTRACRANIAL HYPERTENSION
 IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy
 Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
Results of Transmedial-Canthal Ethmoidal Decompression for Severe Dysthyroid Optic Neuropathy Kenji Ohtsuka and Yasushi Nakamura Department of Ophthalmology, Sapporo Medical University School of Medicine,
MRI Imaging of Neuromyelitis Optica
 July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
July 2009 MRI Imaging of Neuromyelitis Optica Jenna Nolan, Harvard Medical School Year III Gillian Lieberman, MD Our Patient: Initial Presentation J.H. is a 29 year-old woman who presents with acute vision
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Supplementary Online Content
 Supplementary Online Content Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA
Supplementary Online Content Park KH, Kim YK, Woo SJ, et al. Iatrogenic occlusion of the ophthalmic artery after cosmetic facial filler injections: a national survey by the Korean Retina Society. JAMA
New Insights on Optic Neuritis in Young People
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Case Study New Insights on Optic Neuritis in Young People Sergio Carmona 1, Sandra Barbosa 1 and Maria Laura Ortube 2 * 1 Department of Neuro-ophthalmology, Hospital
THE OPTIC CHIASM MAY BE DAMAGED BY A VARIETY
 Clinical Features Associated With Lesions Other Than Pituitary Adenoma in Patients With an Optic Chiasmal Syndrome LUIS J. MEJICO, MD, NEIL R. MILLER, MD, AND LI MING DONG, PHD PURPOSE: Pituitary adenomas
Clinical Features Associated With Lesions Other Than Pituitary Adenoma in Patients With an Optic Chiasmal Syndrome LUIS J. MEJICO, MD, NEIL R. MILLER, MD, AND LI MING DONG, PHD PURPOSE: Pituitary adenomas
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Idiopathic sclerosing inflammation of the orbit is a
 Case Report 758 Bilateral Idiopathic Sclerosing Inflammation of the Orbit: Report of Three Cases Chun-Hsi Liu, MD; Lih Ma 1, MD; Wan-Jen Ku, MD; Ling-Yuh Kao 1, MD; Yueh-Ju Tsai 1, MD We report 3 cases
Case Report 758 Bilateral Idiopathic Sclerosing Inflammation of the Orbit: Report of Three Cases Chun-Hsi Liu, MD; Lih Ma 1, MD; Wan-Jen Ku, MD; Ling-Yuh Kao 1, MD; Yueh-Ju Tsai 1, MD We report 3 cases
Ischaemic optic neuropathy: the Singapore scene
 O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
O r i g i n a l A r t i c l e Singapore Med J 2007; 48 (4) : 281 Ischaemic optic neuropathy: the Singapore scene Cullen J F, Por Y M Abstract The commonest cause of an optic neuropathy in Singapore is
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Frosted branch angiitis with undiagnosed Hodgkin lymphoma
 European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 310-313 SHORT COMMUNICTIONS & CSE REPORTS Frosted branch angiitis with undiagnosed Hodgkin lymphoma MINH-TRI HU 1, PIERRE LISE 1, LURENCE DE
European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 310-313 SHORT COMMUNICTIONS & CSE REPORTS Frosted branch angiitis with undiagnosed Hodgkin lymphoma MINH-TRI HU 1, PIERRE LISE 1, LURENCE DE
Five steps: Overview
 Optic atrophy is not a diagnosis Andrew G. Lee, MD Professor of Ophthalmology, Neurology and Neurosurgery, Weill Cornell Medical College Chair, Department of Ophthalmology, Houston Methodist Hospital,
Optic atrophy is not a diagnosis Andrew G. Lee, MD Professor of Ophthalmology, Neurology and Neurosurgery, Weill Cornell Medical College Chair, Department of Ophthalmology, Houston Methodist Hospital,
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
! Women greater than men (4:1)» Typical of other autoimmune diseases
 1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
1 2 3 4 : Overview and Diagnosis Suzanne K. Freitag, M.D. Director, Ophthalmic Plastic Surgery Massachusetts Eye and Ear Infirmary Harvard Medical School! I have no financial disclosures. Learning Objectives!
Clinically isolated syndromes (CIS) may
 RECOGNIZING AND MANAGING THE CLINICALLY ISOLATED SYNDROME* Steven L. Galetta, MD ABSTRACT Clinically isolated demyelinating syndromes, such as optic neuritis, transverse myelitis, and brain-stem disorders,
RECOGNIZING AND MANAGING THE CLINICALLY ISOLATED SYNDROME* Steven L. Galetta, MD ABSTRACT Clinically isolated demyelinating syndromes, such as optic neuritis, transverse myelitis, and brain-stem disorders,
Kimura s Disease of the Orbit Successfully Treated with Radiotherapy Alone: A Case Report
 Published online: March 13, 2014 1663 2699/14/0051 0087$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: March 13, 2014 1663 2699/14/0051 0087$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
NANOS Patient Brochure
 NANOS Patient Brochure Transient Visual Loss Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and
NANOS Patient Brochure Transient Visual Loss Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and
Band atrophy of the optic nerve: A report on different anatomical locations in three patients
 Saudi Journal of Ophthalmology (2013) 27, 65 69 Case Report Band atrophy of the optic nerve: A report on different anatomical locations in three patients Alberto Gálvez-Ruiz, MD a,b, ; Nawal Arishi, MD
Saudi Journal of Ophthalmology (2013) 27, 65 69 Case Report Band atrophy of the optic nerve: A report on different anatomical locations in three patients Alberto Gálvez-Ruiz, MD a,b, ; Nawal Arishi, MD
Case Presentation VASCULITIS. Case Presentation. Case Presentation. Vasculitis
 Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Orbital Tumors - A Clinico Pathological Study
 Orbital Tumors - A Clinico Pathological Study Radha. J. DO, Ani Sreedhar. MS. Little Flower Hospital, Angamaly, Kerala ORIGINAL ARTICLES Abstract: Aim. To study the clinical and histopathological profiles
Orbital Tumors - A Clinico Pathological Study Radha. J. DO, Ani Sreedhar. MS. Little Flower Hospital, Angamaly, Kerala ORIGINAL ARTICLES Abstract: Aim. To study the clinical and histopathological profiles
Clinical prospective study of visual function in patients with acute optic neuritis
 Journal of the Formosan Medical Association (2013) 112, 87e92 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical prospective study of visual function
Journal of the Formosan Medical Association (2013) 112, 87e92 Available online at www.sciencedirect.com journal homepage: www.jfma-online.com ORIGINAL ARTICLE Clinical prospective study of visual function
COPYRIGHT 2012 THE TRANSVERSE MYELITIS ASSOCIATION. ALL RIGHTS RESERVED
 The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
The Transverse Myelitis Association...advocating for those with acute disseminated encephalomyelitis, neuromyelitis optica, optic neuritis and transverse myelitis ACUTE DISSEMINATED ENCEPHALOMYELITIS (ADEM)
Evaluation of ONH Pallor in Glaucoma Patients and Suspects. Leticia Rousso, O.D. Joseph Sowka, O.D
 Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Traumatic Partial Optic Nerve Avulsion with Globe luxation. Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine
 Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
Traumatic Partial Optic Nerve Avulsion with Globe luxation Presented by: Mostafa ElManhaly Resident in Alexandria Faculty Of Medicine A 23 year old male patient presented to the emergency department in
VASCULITIS. Case Presentation. Case Presentation
 VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Chief Complaint. History. History of Similar Episodes. A 10 Year-Old Boy With Headache
 A 10 Year-Old Boy With Headache Chief Complaint Recent Advances in Neurology 2013 10 year-old boy presented with his fifth lifetime bout of left-sided head pain followed by diplopia. Amy A. Gelfand, MD
A 10 Year-Old Boy With Headache Chief Complaint Recent Advances in Neurology 2013 10 year-old boy presented with his fifth lifetime bout of left-sided head pain followed by diplopia. Amy A. Gelfand, MD
3/16/2018. Optic Nerve Examination. Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Anterior Ischemic Optic Neuropathy (AION)
 Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
Anterior Ischemic Optic Neuropathy (AION) Your doctor thinks you have suffered an episode of anterior ischemic optic neuropathy (AION). This is the most common cause of sudden decreased vision in patients
OPTIC NEUROPATHIES Optic Neuritis vs AION. Jacqueline M.S. Winterkorn, Ph.D., M.D.
 OPTIC NEUROPATHIES Optic Neuritis vs AION Jacqueline M.S. Winterkorn, Ph.D., M.D. OPTIC NEUROPATHIES Inflammatory Optic Neuritis Ischemic Optic Neuropathy Compressive Optic Neuropathy Traumatic Optic
OPTIC NEUROPATHIES Optic Neuritis vs AION Jacqueline M.S. Winterkorn, Ph.D., M.D. OPTIC NEUROPATHIES Inflammatory Optic Neuritis Ischemic Optic Neuropathy Compressive Optic Neuropathy Traumatic Optic
Fundus Autofluorescence. Jonathan A. Micieli, MD Valérie Biousse, MD
 Fundus Autofluorescence Jonathan A. Micieli, MD Valérie Biousse, MD The retinal pigment epithelium (RPE) has many important functions including phagocytosis of the photoreceptor outer segments Cone Rod
Fundus Autofluorescence Jonathan A. Micieli, MD Valérie Biousse, MD The retinal pigment epithelium (RPE) has many important functions including phagocytosis of the photoreceptor outer segments Cone Rod
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
Difficult Diagnosis: Case History. 7 months prior, she happened to have undergone a C-spine MRI after a car accident
 Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Relevant Disclosures: None Difficult Diagnosis: Recent Advances in Neurology 2013 Jeffrey M. Gelfand, MD Assistant Professor UCSF Neuroinflammation and MS Center UCSF Department of Neurology Case History
Topical Diagnosis of Chiasmal and Retrochiasmal Disorders
 Topical Diagnosis of Chiasmal and Retrochiasmal Disorders Leonard A. Levin CHAPTER 12 TOPICAL DIAGNOSIS OF OPTIC CHIASMAL LESIONS Visual Field Defects Etiologies of the Optic Chiasmal Syndrome Masqueraders
Topical Diagnosis of Chiasmal and Retrochiasmal Disorders Leonard A. Levin CHAPTER 12 TOPICAL DIAGNOSIS OF OPTIC CHIASMAL LESIONS Visual Field Defects Etiologies of the Optic Chiasmal Syndrome Masqueraders
OPHTHALMIC PATHOLOGY SPECIALTY CONFERENCE
 DISCLOSURE STATEMENT OPHTHALMIC PATHOLOGY SPECIALTY CONFERENCE No financial disclosures No off-label usage Diva Regina Salomão, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic College of
DISCLOSURE STATEMENT OPHTHALMIC PATHOLOGY SPECIALTY CONFERENCE No financial disclosures No off-label usage Diva Regina Salomão, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic College of
Jacqueline Theis, O.D., F.A.A.O.
 Neuro-Ophthalmological Emergencies Presenting in Primary Care Optometry Describes the symptoms, signs, and management of neuro-ophthalmological emergencies. Signs/Symptoms to be Concerned about (especially
Neuro-Ophthalmological Emergencies Presenting in Primary Care Optometry Describes the symptoms, signs, and management of neuro-ophthalmological emergencies. Signs/Symptoms to be Concerned about (especially
Bilateral central and centrocaecal scotomata due
 British Journal of Ophthalmology, 1984, 68, 336-342 Bilateral central and centrocaecal scotomata due to mass lesions ISAAC GUTMAN,* MYLES BEHRENS, AND JEFFREY ODEL* From the Department of Ophthalmology,
British Journal of Ophthalmology, 1984, 68, 336-342 Bilateral central and centrocaecal scotomata due to mass lesions ISAAC GUTMAN,* MYLES BEHRENS, AND JEFFREY ODEL* From the Department of Ophthalmology,
SUMMARY OF RANDOMIZED CONTROLLED TRIALS COMPARING DIFFERENT ORBITAL RADIOTHERAPY REGIMENTS AND ORBITAL RADIOTHERAPY TO PLACEBO OR CORTICOSTEROIDS
 TABLE e4. SUMMARY OF RANDOMIZED CONTROLLED TRIALS COMPARING DIFFERENT ORBITAL RADIOTHERAPY REGIMENTS AND ORBITAL RADIOTHERAPY TO PLACEBO OR CORTICOSTEROIDS Study Treatment Groups Primary Outcome Measure
TABLE e4. SUMMARY OF RANDOMIZED CONTROLLED TRIALS COMPARING DIFFERENT ORBITAL RADIOTHERAPY REGIMENTS AND ORBITAL RADIOTHERAPY TO PLACEBO OR CORTICOSTEROIDS Study Treatment Groups Primary Outcome Measure
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Patient with Daily Headache NTERNATIONAL CLASSIFICATION HEADACHE DISORDERS. R. Allan Purdy, MD, FRCPC,FACP. Professor of Medicine (Neurology)
 Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
A trial of corticotrophin gelatin injection in
 Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 869-873 A trial of corticotrophin gelatin injection in acute optic neuritis A. N. BOWDEN, P. M. A. BOWDEN, A. I. FRIEDMANN, G. D. PERKIN, AND
Journal of Neurology, Neurosurgery, and Psychiatry, 1974, 37, 869-873 A trial of corticotrophin gelatin injection in acute optic neuritis A. N. BOWDEN, P. M. A. BOWDEN, A. I. FRIEDMANN, G. D. PERKIN, AND
Visual pathways in the chiasm
 Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Passive ocular proptosis
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 1198-1202 Passive ocular proptosis BRIAN P. O'NEILL From the Department of Neurology, University of Michigan Medical Center, and the Neurology
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 1198-1202 Passive ocular proptosis BRIAN P. O'NEILL From the Department of Neurology, University of Michigan Medical Center, and the Neurology
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
Neuro-imaging for the Ophthalmologist. Karl C. Golnik, MD, MEd University of Cincinnati & The Cincinnati Eye Institute
 Neuro-imaging for the Ophthalmologist Karl C. Golnik, MD, MEd University of Cincinnati & The Cincinnati Eye Institute Neuro-ophthalmology is that subspecialty where the diagnosis is made upon reinterpretation
Neuro-imaging for the Ophthalmologist Karl C. Golnik, MD, MEd University of Cincinnati & The Cincinnati Eye Institute Neuro-ophthalmology is that subspecialty where the diagnosis is made upon reinterpretation
Primary optic nerve meningioma
 Primary optic nerve meningioma British Journal of Ophthalmology, 1980, 64, 553-558 J. E. WRIGHT, N. B. CALL,* AND S. LIARICOSt From the Orbital Clinic, Moorfields Eye Hospital, City Road, London ECJ V
Primary optic nerve meningioma British Journal of Ophthalmology, 1980, 64, 553-558 J. E. WRIGHT, N. B. CALL,* AND S. LIARICOSt From the Orbital Clinic, Moorfields Eye Hospital, City Road, London ECJ V
Pit-like changes of the optic nerve head
 Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Objectives. Unexplained Vision Loss: Where Do I Go From Here. History. History. Drug Induced Vision Loss
 Objectives Unexplained Vision Loss: Where Do I Go From Here Denise Goodwin, OD, FAAO Coordinator, Neuro-ophthalmic Disease Clinic Pacific University College of Optometry goodwin@pacificu.edu Know the importance
Objectives Unexplained Vision Loss: Where Do I Go From Here Denise Goodwin, OD, FAAO Coordinator, Neuro-ophthalmic Disease Clinic Pacific University College of Optometry goodwin@pacificu.edu Know the importance
E, Ixperimental allergic encephalomyelitis
 Experimental allergic optic neuritis in guinea pigs: preliminary report Narsing A. Rao, Mark O. M. Tso," and Lorenz E. Zimmerman An experimental model for acute allergic optic neuritis was produced in
Experimental allergic optic neuritis in guinea pigs: preliminary report Narsing A. Rao, Mark O. M. Tso," and Lorenz E. Zimmerman An experimental model for acute allergic optic neuritis was produced in
OCT : retinal layers. Extraocular muscles. History. Central vs Peripheral vision. History: Temporal course. Optical Coherence Tomography (OCT)
 Optical Coherence Tomography (OCT) OCT : retinal layers 7 Central vs Peripheral vision Extraocular muscles RPE E Peripheral Vision: Rods (95 million) 30% Ganglion cells Central Vision: Cones (5 million)
Optical Coherence Tomography (OCT) OCT : retinal layers 7 Central vs Peripheral vision Extraocular muscles RPE E Peripheral Vision: Rods (95 million) 30% Ganglion cells Central Vision: Cones (5 million)
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI
 Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
Helpful Information for evaluation of new neurological symptoms in patients receiving TYSABRI This information is provided as an educational resource for healthcare providers and should be considered current
MRI Dynamic Color Mapping: a new quantitative technique for imaging soft tissue motion in the orbit
 MRI DYNAMIC COLOR MAPPING: A NEW QUANTITATIVE TECHNIQUE FOR IMAGING SOFT TISSUE MOTION IN THE ORBIT 79 6 MRI Dynamic Color Mapping: a new quantitative technique for imaging soft tissue motion in the orbit
MRI DYNAMIC COLOR MAPPING: A NEW QUANTITATIVE TECHNIQUE FOR IMAGING SOFT TISSUE MOTION IN THE ORBIT 79 6 MRI Dynamic Color Mapping: a new quantitative technique for imaging soft tissue motion in the orbit
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Radiation-induced Brachial Plexopathy: MR Imaging
 Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Radiation-induced Brachial Plexopathy 85 Chapter 5 Radiation-induced Brachial Plexopathy: MR Imaging Neurological symptoms and signs of brachial plexopathy may develop in patients who have had radiation
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Meningiomas account for approximately 4% of all
 Intraorbital Meningiomas A Pathologic Review Using Current World Health Organization Criteria Deepali Jain, MD; Katayoon B. Ebrahimi, MD; Neil R. Miller, MD; Charles G. Eberhart, MD, PhD N Context. Meningiomas
Intraorbital Meningiomas A Pathologic Review Using Current World Health Organization Criteria Deepali Jain, MD; Katayoon B. Ebrahimi, MD; Neil R. Miller, MD; Charles G. Eberhart, MD, PhD N Context. Meningiomas
Review Article Orbital IgG4-Related Disease: Clinical Features and Diagnosis
 International Scholarly Research Network Volume 2012, Article ID 412896, 5 pages doi:10.5402/2012/412896 Review Article Orbital IgG4-Related Disease: Clinical Features and Diagnosis Toshinobu Kubota 1
International Scholarly Research Network Volume 2012, Article ID 412896, 5 pages doi:10.5402/2012/412896 Review Article Orbital IgG4-Related Disease: Clinical Features and Diagnosis Toshinobu Kubota 1
Recurrent transient visual loss in a middle aged woman
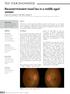 Recurrent transient visual loss in a middle aged woman Chow SY, Draman N, Teh WM, Azhany Y Chow SY, Draman N, Teh WM, et al. Recurrent transient visual loss in a middle aged woman. Malays Fam Physician.
Recurrent transient visual loss in a middle aged woman Chow SY, Draman N, Teh WM, Azhany Y Chow SY, Draman N, Teh WM, et al. Recurrent transient visual loss in a middle aged woman. Malays Fam Physician.
N EOPLASMS of the optic nerves occur
 Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
Tumors of the optic nerve and optic chiasm COLLINS. MAcCARTY~ M.D., ALLEN S. BOYD, JR., M.D., AND DONALD S. CHILDS, JR,, M.D. Departments of Neurologic Surgery and Therapeutic Radiology, Mayo Clinic and
NANOS Patient Brochure
 NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
Neuropathy (NAION) and Avastin. Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013
 Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Non Arteritic Ischemic Optic Neuropathy (NAION) and Avastin Shalom Kelman, MD Clinical Assembly of the AOCOO-HNS Foundation May 9, 2013 Anterior Ischemic Optic Neuropathy Acute, painless, visual loss,
Taking a close look at optic-nerve meningioma
 VOL. 29 NO. 4 PHILIPPINE JOURNAL OF Ophthalmology OCTOBER REVIEW - DECEMBBR 2004 Anthony C. Arnold, MD Jules Stein Eye Institute Department of Ophthalmology University of California, Los Angeles Taking
VOL. 29 NO. 4 PHILIPPINE JOURNAL OF Ophthalmology OCTOBER REVIEW - DECEMBBR 2004 Anthony C. Arnold, MD Jules Stein Eye Institute Department of Ophthalmology University of California, Los Angeles Taking
Case Report IgG4-Related Disease Presenting as Isolated Scleritis
 Hindawi Case Reports in Ophthalmological Medicine Volume 2017, Article ID 4876587, 4 pages https://doi.org/10.1155/2017/4876587 Case Report IgG4-Related Disease Presenting as Isolated Scleritis Eran Berkowitz,
Hindawi Case Reports in Ophthalmological Medicine Volume 2017, Article ID 4876587, 4 pages https://doi.org/10.1155/2017/4876587 Case Report IgG4-Related Disease Presenting as Isolated Scleritis Eran Berkowitz,
