clinical article
|
|
|
- Mitchell Butler
- 5 years ago
- Views:
Transcription
1 clinical article Incidence and predictors of dural venous sinus pressure gradient in idiopathic intracranial hypertension and non-idiopathic intracranial hypertension headache patients: results from 164 cerebral venograms Michael R. Levitt, MD, 1 3 Randall J. Hlubek, MD, 4 Karam Moon, MD, 4 M. Yashar S. Kalani, MD, PhD, 4 Peter Nakaji, MD, 4 Kris A. Smith, MD, 4 Andrew S. Little, MD, 4 Kerry Knievel, DO, 5 Jane W. Chan, MD, 6 Cameron G. McDougall, MD, 4 and Felipe C. Albuquerque, MD 4 Departments of 1 Neurological Surgery, 2 Radiology, and 3 Mechanical Engineering, University of Washington, Seattle, Washington; and Departments of 4 Neurosurgery, 5 Neurology, and 6 Neuro-Ophthalmology, Barrow Neurological Institute, St. Joseph s Hospital and Medical Center, Phoenix, Arizona Objective Cerebral venous pressure gradient (CVPG) from dural venous sinus stenosis is implicated in headache syndromes such as idiopathic intracranial hypertension (IIH). The incidence of CVPG in headache patients has not been reported. Methods The authors reviewed all cerebral venograms with manometry performed for headache between January 2008 and May Patient demographics, headache etiology, intracranial pressure (ICP) measurements, and radiographic and manometric results were recorded. CVPG was defined as a difference 8 mm Hg by venographic manometry. Results One hundred sixty-four venograms were performed in 155 patients. There were no procedural complications. Ninety-six procedures (58.5%) were for patients with IIH. The overall incidence of CVPG was 25.6% (42 of 164 procedures): 35.4% (34 of 96 procedures) in IIH patients and 11.8% (8 of 68 procedures) in non-iih patients. Sixty procedures (36.6%) were performed in patients with preexisting shunts. Seventy-seven patients (49.7%) had procedures preceded by an ICP measurement within 4 weeks of venography, and in 66 (85.7%) of these patients, the ICP had been found to be elevated. CVPG was seen in 8.3% (n = 5) of the procedures in the 60 patients with a preexisting shunt and in 0% (n = 0) of the 11 procedures in the 77 patients with normal ICP (p < for both). Noninvasive imaging (MR venography, CT venography) was assessed prior to venography in 112 (68.3%) of 164 cases, and dural venous sinus abnormalities were demonstrated in 73 (65.2%) of these cases; there was a trend toward CVPG (p = 0.07). Multivariate analysis demonstrated an increased likelihood of CVPG in patients with IIH (OR 4.97, 95% CI ) and a decreased likelihood in patients with a preexisting shunt (OR 0.09, 95% CI ). Conclusions CVPG is uncommon in IIH patients, rare in those with preexisting shunts, and absent in those with normal ICP. Key Words benign intracranial hypertension; headache; idiopathic intracranial hypertension; manometry; pseudotumor cerebri; venography; interventional neurosurgery ABBREVIATIONS BMI = body mass index; CTV = CT venography; CVPG = cerebral venous pressure gradient; ICP = intracranial pressure; IIH = idiopathic intracranial hypertension; MRV = MR venography; NPV = negative predictive value; PPV = positive predictive value. SUBMITTED August 28, ACCEPTED December 10, include when citing Published online March 11, 2016; DOI: / JNS AANS, 2016 J Neurosurg March 11,
2 M. R. Levitt et al. Cerebral venous hypertension has been implicated in the development of headache disorders such as idiopathic intracranial hypertension (IIH), and dural venous sinus stenting has emerged as an alternative to CSF shunting in such patients. 2,15 Noninvasive imaging such as MR venography (MRV) and CT venography (CTV) may show anatomical stenosis or atresia of the venous sinuses in up to 93.1% of IIH patients and 48.9% of chronic daily headache patients but in only 6.8% of controls. 9,11 However, cerebral venography with manometry is the gold standard for determining the cerebral venous pressure gradient (CVPG) across a dural venous sinus stenosis, and this procedure is used to determine which patients are likely to benefit from subsequent dural venous sinus stenting. 1 The prevalence of, and the risk factors for, CVPG in the IIH and non-iih headache populations are not well characterized. Such information could be used to determine which patients are most likely to benefit from venographic manometry and subsequent dural venous sinus stenting. We analyzed a large series of consecutive venograms obtained in both IIH and non-iih headache patients to determine the incidence of CVPG, and developed a predictive model of CVPG risk factors. Methods Patient Population This study was approved by the Institutional Review Board of St. Joseph s Hospital and Medical Center, Phoenix, Arizona. All cerebral venograms with manometry for the indication of headache that were performed at the institution between January 2008 and May 2015 were retrospectively reviewed. Patients were referred for venography and manometry by primary care physicians, neurologists, and neurosurgeons. Other than the diagnosis of headache, there were no specific inclusion criteria for referral, but patients with acute cerebral venous sinus thrombosis and arteriovenous malformations were excluded. In patients with IIH, diagnosis was made on the basis of symptoms referable to intracranial hypertension, intracranial pressure (ICP) 25 cm H 2 O, normal CSF contents, and no structural cause of elevated ICP on neuroimaging. 12 We recorded patient demographic characteristics and body mass index (BMI; calculated as weight in kg/height in m 2 ); headache diagnosis; presence of a preexisting CSF shunt; recent (within 30 days prior to venography) ICP measurement by lumbar puncture, ventricular catheterization, or ICP monitor; and recent (within 3 months prior to venography) noninvasive cerebrovascular imaging by brain MR or CT angiography or venography. Findings of noninvasive imaging were considered abnormal by independent neuroradiological interpretation if a focal stenosis or an atresia was seen. Venography Procedure Cerebral venography was performed under local anesthesia in all patients 18 years or older and under general anesthesia in all pediatric patients (age < 18 years). Standard transfemoral venous access was obtained and a 5-Fr sheath was inserted. A 5-Fr angled catheter (Envoy MPD, DePuy Synthes Co.) was placed over a Glidewire (Terumo Medical Corp.) and navigated into the right jugular bulb, unless significant stenosis necessitated placement in the left jugular bulb. A microcatheter (SL-10 or XT-17, Stryker Neurovascular) and inch microwire (Synchro-2, Boston Scientific Corp.) were navigated into the dural venous sinuses. The microwire was removed, and a standard arterial pressure transducer was calibrated and connected to the microcatheter. Manometry was attempted in the following locations: anterior, middle, and posterior onethird of the superior sagittal sinus; bilateral transverse and sigmoid sinuses; and bilateral jugular bulbs. In patients with dural venous sinus compression from an extrasinus mass, manometry was performed only in the sinus segments proximal and distal to the mass. In patients in whom portions of the venous sinus system were absent, measurements were obtained in all other locations. Cerebral venography of the superior sagittal sinus and bilateral transverse and sigmoid sinuses was also performed through microcatheter injection. All catheters and the femoral sheath were then withdrawn, and hemostasis was obtained by mechanical pressure for 5 to 10 minutes, followed by 2 hours of flat bedrest. Manometry was considered positive when a CVPG of 8 mm Hg or greater was found between any 2 anatomically contiguous segments of the dural venous sinuses (e.g., transverse and sigmoid sinuses). 1 Statistical Analysis Frequencies with percentages and standard deviations with means were used to describe the overall study cohort. Independent-samples t-tests were used to compare mean differences for continuous variables, and chi-square or Fisher exact tests were used for categorical variables. Four patient variables (preexisting CSF shunt, abnormal ICP, abnormal noninvasive imaging findings, and BMI 25) in relation to venographic results were used to obtain diagnostic accuracy, including true and false positive and negative, sensitivity, specificity, and positive and negative predictive value (PPV and NPV, respectively). Multivariate logistic regression was used to identify factors related to CVPG, and receiver operating characteristic analysis was also performed. Cluster analysis was performed to account for the patients who underwent multiple procedures. Statistical significance was defined as p < 0.01; IBM SPSS Statistics for Windows, version 22 (IBM Corp.) and Med- Calc Statistical Software version (MedCalc Software bvba) were used for statistical analyses. Results In total, 164 consecutive venograms were performed in 155 patients; there were no complications related to the procedure. Two patients underwent 3 venogram procedures and 5 patients underwent 2 venogram procedures, with all repeat procedures performed at least 3 months after the initial procedure. Cohort characteristics are shown in Table 1. Recent BMI measurements were available in 117 patients, the majority of whom (78.6% [n = 92]) were overweight (BMI 25) and more than half (53.8% [n = 63]) of whom were obese (BMI 30) at the time of their procedure. The most common headache etiology in the 2 J Neurosurg March 11, 2016
3 Venography and pressure measurements in IIH and non-iih headache TABLE 1. Cohort characteristics of 164 venogram procedures in 155 headache patients* Characteristic Value Age (yrs) Mean ± Age <18 25 (15%) BMI Mean ± 9.51 BMI (78.6%) Female sex 132 (80.7%) Headache diagnosis Idiopathic intracranial hypertension 96 (58.5%) Congenital hydrocephalus 11 (6.7%) Chiari malformation 10 (6.1%) Extracranial jugular vein compression 8 (4.9%) Tumor or mass compressing sinus 5 (3.0%) Postconcussive 3 (1.8%) Other 31 (18.9%) Preexisting shunt 60 (36.6%) Abnormal ICP ( 25 cm H 2 O) 66 (85.7%) Abnormal findings on noninvasive CV imaging 73 (65.2%) CVPG 42 (25.6%)** CV = cerebrovascular. * Values represent numbers of procedures (%) unless otherwise indicated. Multiple procedures performed in the same patient over time may show different results; however, cluster analysis did not show an effect of repeated measures. Data are thus based on number of procedures. Percentage is from 117 procedures with available and recent BMI measurements. Includes migraines; chronic daily headaches; history of previous sinus thrombosis with persistent headaches despite recanalization, tumor resection, or aneurysm clipping. Percentage is from 77 procedures with preceding ICP measurement. Percentage is from 112 procedures with preceding noninvasive cerebrovascular imaging (MR or CT venography or angiography). ** Percentage is from 164 procedures. 155 patients was IIH (61.9% [n = 96]). The other diagnosis category was composed of heterogeneous headache diagnoses that did not meet IIH criteria, including migraines, chronic daily headaches, history of previous sinus thrombosis with persistent headaches despite recanalization, and history of tumor resection or aneurysm clipping. Sixty (38.7%) of 155 patients had preexisting CSF shunts. Seventy-seven (49.7%) patients underwent ICP measurement within 4 weeks of venography, and 66 (85.7%) of these 77 demonstrated elevated ICP. Noninvasive imaging had been performed within the 3 months preceding the procedure in 112 cases, and 73 (65.2%) of these imaging studies showed dural venous sinus abnormalities such as stenosis or atresia. The overall incidence of CVPG was 25.6% (present in 42 of 164 procedures). The average gradient was 22 ± 16 mm Hg (range 8 81 mm Hg). CVPG was located between the transverse and sigmoid sinuses in all but 2 procedures (in one it was between the anterior and posterior one-third of the superior sagittal sinus and in another it was between the jugular bulb and the extracranial internal jugular vein). Twenty-eight procedures resulted in bilateral CVPG. The average superior sagittal sinus pressure in procedures with and without CVPG was 33.5 mm Hg and 14.6 mm Hg, respectively (p < 0.001). CVPG was found in 34 of 96 procedures (35.4%) in patients with IIH and in 8 of 68 procedures (11.8%) in non- IIH patients; IIH was significantly associated with CVPG on univariate analysis (p < 0.001). No patient with Chiari malformation, posttraumatic headache, or tumor with dural sinus compression had CVPG. Of the 8 procedures in non-iih patients with CVPG, 2 procedures were in 2 patients (ages 2 and 15) with a diagnosis of congenital hydrocephalus, both of whom had ventriculoperitoneal shunts in place. The patient who was 15 years old at the time of the venogram had undergone a lumbar puncture that demonstrated elevated ICP. The 2-year-old patient had symptoms of intermittent shunt malfunction but had not undergone recent ICP measurement. The remaining 6 procedures in which CVPG was identified in the absence of IIH were in patients with the following headache diagnoses: remote history of vestibular schwannoma resection, remote history of meningitis, pulsatile tinnitus, extracranial styloid compression of the jugular vein, remote history of cerebral venous sinus thrombosis (which was radiographically resolved), and chronic headaches not otherwise specified. CVPG was identified during only 8.3% (n = 5) of the procedures in the 60 patients with a preexisting shunt, and in 0% of the 11 procedures in the 77 patients with normal ICP (p < for both). There was a trend toward association between abnormalities on noninvasive imaging and CVPG (p = 0.07). Cross-tabulations of major patient characteristics at the time of the procedure (BMI 25, preexisting shunt, abnormal ICP, abnormal findings on noninvasive cerebrovascular imaging) were performed for the entire sample and for procedures in patients with IIH (Table 2) to determine the predictive accuracy for CVPG. Importantly, abnormal ICP was associated with a 100% NPV, as CVPG was not observed in any procedure in patients with normal ICP. A non-overweight BMI (< 25) was also associated with a high NPV (71.4% for procedures in patients with IIH and 88.0% overall). No factor was an efficient positive predictor of CVPG. Cluster analysis did not reveal any significant effect of the 7 patients who underwent a total of 9 additional procedures. The results of multivariate and receiver operating characteristic analyses are shown in Table 3 and Fig. 1. Because of a substantial overlap between IIH and obesity, BMI was not included in the multivariate analysis. ICP was also excluded because no patient with normal ICP had CVPG, and the analysis was limited to 112 procedures in patients who had prior noninvasive imaging. The diagnosis of IIH was a significant positive predictor of CVPG (OR 4.97, 95% CI ), whereas CVPG was significantly less likely to be found during procedures in patients with preexisting shunts (OR 0.09, 95% CI ). Noninvasive imaging abnormality, age, and sex were not predictors of CVPG. The area under the curve for Fig. 1 was 0.79 (95% CI ). J Neurosurg March 11,
4 M. R. Levitt et al. TABLE 2. Screening characteristics for CVPG in overall cohort and procedures in IIH patients CVPG+ CVPG Sensitivity Specificity PPV NPV Variable True Pos False Neg False Pos True Neg % 95% CI % 95% CI % 95% CI % 95% CI Entire cohort (n = 164) BMI Preexisting shunt Abnormal ICP Abnormal findings on noninvasive CV imaging IIH patients (n = 96) BMI Preexisting shunt Abnormal ICP Abnormal findings on noninvasive CV imaging Neg = negative; pos = positive. TABLE 3. Multivariate analysis of predictors of CVPG in procedures preceded by noninvasive cerebrovascular imaging (n = 112) * p < Variable Odds Ratio 95% CI Age (yrs) Female sex Diagnosis of IIH * Preexisting shunt * Discussion We have reported the overall incidence of CVPG in IIH and non-iih patients in a large cohort of headache patients. A diagnosis of IIH was a significant positive predictor of CVPG. Normal ICP and previous CSF shunting were significant negative predictors, and noninvasive imaging results were not helpful for screening. Headache diagnoses such as Chiari malformation, postconcussive headache, and a tumor compressing the dural venous sinuses were not associated with CVPG, although the sample size for each of these diagnoses was small. The relationship between dural venous sinus stenosis and headache, especially with respect to IIH, and the efficacy of venous stenting have been established in several series and meta-analyses. 1,2,16,18,21 Authors have suggested both causative and reactive relationships between IIH, headache, and dural venous sinus stenosis, but the exact mechanism has not been elucidated. 8,20 Although elevated ICP (and the attendant elevation in cerebral venous pressure) is thought to be a component of both IIH and secondary intracranial hypertension, 13 not all patients with headache, elevated ICP, and elevated cerebral venous pressure demonstrate a CVPG across a focal anatomical location such as the transverse-sigmoid sinus junction. However, most endovascular operators use the presence of a CVPG to determine which patients would benefit from endovascular stenting of the affected dural venous sinus. 1 Thus the overall rate of CVPG, as well as clinical risk factors for CVPG among IIH and non-iih headache patients, would be useful for screening headache patients for possible endovascular intervention. Elevated ICP is a hallmark of IIH that is often, but not always, present in other headache syndromes. 12 While it is possible for elevated ICP to be the result of CVPG, we hypothesize that since no patient in our cohort with normal ICP demonstrated CVPG, elevated ICP is instead the result of dynamic resistance in relation to dural venous sinus stenosis. 4 In this model, elevated ICP precipitates stenosis in certain patients with focal weakness in the dural sinus wall. The elevated cerebral venous pressure upstream from the stenosis prevents the bulk flow resorption of CSF, resulting in a positive feedback loop of increased ICP and further stenosis. Patients without elevated ICP, even in the setting of anatomically narrowed dural venous sinuses, either do not suffer from this positive feedback loop (with the stenosis constituting a normal anatomical variant without physiological consequences in these individuals) or have elevated pressure throughout the entire 4 J Neurosurg March 11, 2016
5 Venography and pressure measurements in IIH and non-iih headache Fig. 1. Receiver operating characteristic graph of multivariate analysis (see Table 3) of predictors for CVPG. The area under the curve is 0.79 (95% CI ). Figure is available in color online only. venous system (and thus no CVPG). 17 Neither of these types of patients would benefit from focal stenting of the dural venous sinus stenosis, as the former does not have physiologically elevated cerebral venous pressure and the latter has diffusely elevated pressure for which the focal stenosis is not solely responsible. This may explain why patients with a preexisting shunt have a low likelihood of CVPG on both univariate and multivariate analysis, as ICP is likely to be within normal limits in such patients. Indeed, many patients in our cohort who had preexisting shunts presented with worsening headache and (in some cases) elevated ICP suggestive of shunt failure. Thus any patient with concern for headache related to elevated cerebral venous pressure should undergo lumbar puncture or shunt interrogation, and only those with elevated ICP should be screened for CVPG with cerebral venography and manometry. Eight patients without diagnosed IIH had CVPG. It is unclear why the 2 patients with both congenital hydrocephalus and CVPG differed from the 12 other patients with congenital hydrocephalus who did not have CVPG, all of whom had shunts in place. Although pediatric IIH has been reported, 10 both of our pediatric patients had ventriculomegaly on previous cranial imaging, suggesting another etiology that resulted in dural venous incompetence. Another patient with a remote history of extensive dural venous sinus thrombosis (since resolved) likely had secondary intracranial hypertension similar in etiology to IIH, given her bilateral transverse sinus focal stenosis in the location of the resolved sinus thrombosis. Extracranial jugular venous compression has been reported as a distinct headache entity, 7 and its relation to elevated cerebral venous pressure is evidenced by the patient with such compression and CVPG. A communicating hydrocephalus was likely undiagnosed in both the postmeningitic patient and the patient with previous jugular schwannoma resection. Finally, in the 2 remaining non-iih patients with CVPG, presenting symptoms and the absence of neuroimaging findings strongly suggest undiagnosed IIH, although no formal diagnosis was established because these patients were referred from other institutions specifically for venography. Thus patients with IIH-like symptoms may benefit from venography in rare cases, especially when they have elevated ICP. Noninvasive imaging can reveal dural venous sinus abnormalities, although these may represent normal anatomical variants in up to 31% of cases. 3 While there is a good correlation between headache and dural venous sinus abnormalities on noninvasive imaging such as CT venography or MR venography, our results dispute that such imaging should be used as a screening tool to determine whether patients should undergo invasive cerebral venography, as previously suggested. 1 A study of 29 IIH patients and 59 controls demonstrated a correlation of 93% between IIH and dural venous sinus stenosis on MRV, compared with only 7% of asymptomatic controls. 11 Similarly, an MRV study of 724 patients with migraine found bilateral transverse-sigmoid sinus stenosis in 6.7%. 6 Another report of 217 patients who underwent both MRV and lumbar puncture for various neurological indications found that of the 11.1% of patients with elevated ICP, 100% had bilateral transverse-sigmoid sinus stenosis, while the rate of bilateral stenosis in those with normal ICP was 13.4%. 5 These results are similar to those in another study in which 16% of 44 patients with venous sinus stenosis on MRV had normal ICP. 14 However, it is unclear whether symptom severity is specifically related to bilateral (vs unilateral) stenosis. There is a significant association between Chiari malformation and transverse sinus stenosis on MRI, 19 although in our series no patient with Chiari malformation had CVPG. Although previous studies suggest a correlation between noninvasive imaging results and IIH, the rate of CVPG among patients with noninvasive imaging evidence of dural sinus stenosis has not been previously described. Our results suggest that noninvasive imaging may not accurately predict CVPG: the PPV was < 50%, and multivariate analyses failed to demonstrate noninvasive imaging as a significant predictor of CVPG. Indeed, 8 (20.5%) of 39 patients in our cohort with CVPG had anatomically normal venous sinuses on noninvasive imaging. Conversely, patients with normal anatomical variants as well as those with mass lesions extrinsically compressing a dural venous sinus may have alternative or compensatory venous drainage without an elevation in cerebral venous pressures, as was seen in the 5 patients in our cohort with tumors causing compressive venous sinus stenosis, none of whom demonstrated any elevation in venous sinus pressure or CVPG. There was no significant correlation between bilateral stenosis on noninvasive imaging and bilateral CVPG, although our sample size was too small (n = 28) to completely rule out such an association. Importantly, there was a trend (p = 0.07) toward a univariate association between abnormalities on noninvasive imaging J Neurosurg March 11,
6 M. R. Levitt et al. and CVPG. Nevertheless, only 68.3% of the procedures in this study were preceded by noninvasive imaging, so our study may be underpowered to detect a robust association. It remains to be seen whether screening patients as candidates for venography and possible stenting on the basis of noninvasive cerebrovascular imaging results is beneficial. Given our findings, our approach to venography and manometry for headache patients can be summarized as follows. In patients with headache in whom IIH or elevated ICP is suspected, lumbar puncture should be performed. In those patients with elevated ICP without a preexisting CSF shunt, cerebral venography and manometry should be performed to rule out CVPG. Routine noninvasive cerebrovascular imaging may not be predictive of CVPG (although cranial imaging is still recommended to rule out secondary causes of intracranial hypertension), so we do not routinely perform CTV or MRV prior to venography, although such imaging may be shown in future studies to improve patient selection. A high index of suspicion should be in place for IIH patients in particular, whereas patients with normal ICP should not undergo venography unless other compelling clinical factors are present (such as a severe visual field deficit). This study has several limitations. Its retrospective nature introduces a selection bias toward patients with a diagnosis of IIH. The overall incidence of CVPG in the non-iih population should be interpreted with caution, as non-iih referrals were at the discretion of the referring physician, and quantification of headache severity was not routinely performed. However, venographic results from non-iih headache patients have not been previously described, and a proportion of non-iih patients demonstrated CVPG, which may expand the indications for venography. Indeed, the incidence of CVPG in this study may underestimate the rate in headache patients who do not have IIH or a CSF shunt, because 34.8% (23 of 66) of our non-iih headache patients had a preexisting shunt. Finally, incomplete availability of patient characteristics such as ICP measurement and noninvasive cerebrovascular imaging results weakens the power of our statistical analysis and limits the generalizability of our findings. A future study with prospective standardized data collection of these variables is required to refine and validate our preliminary findings. Conclusions CVPG was present in 35.4% (n = 34) of the 96 procedures conducted in 96 IIH patients. Patients with normal ICP did not demonstrate CVPG, and the presence of a preexisting shunt significantly reduced its likelihood. Patients with elevated ICP (especially with IIH) without previous shunting should be routinely considered for venography and manometry to rule out CVPG. Acknowledgments We thank Kristina Chapple, PhD, for her assistance with statistical analysis. References 1. Ahmed RM, Wilkinson M, Parker GD, Thurtell MJ, Macdonald J, McCluskey PJ, et al: Transverse sinus stenting for idiopathic intracranial hypertension: a review of 52 patients and of model predictions. AJNR Am J Neuroradiol 32: , Albuquerque FC, Dashti SR, Hu YC, Newman CB, Teleb M, McDougall CG, et al: Intracranial venous sinus stenting for benign intracranial hypertension: clinical indications, technique, and preliminary results. World Neurosurg 75: , , Ayanzen RH, Bird CR, Keller PJ, McCully FJ, Theobald MR, Heiserman JE: Cerebral MR venography: normal anatomy and potential diagnostic pitfalls. AJNR Am J Neuroradiol 21:74 78, Bateman GA: Arterial inflow and venous outflow in idiopathic intracranial hypertension associated with venous outflow stenoses. J Clin Neurosci 15: , Bono F, Cristiano D, Mastrandrea C, Latorre V, D Asero S, Salvino D, et al: The upper limit of normal CSF opening pressure is related to bilateral transverse sinus stenosis in headache sufferers. Cephalalgia 30: , Bono F, Messina D, Giliberto C, Cristiano D, Broussard G, Fera F, et al: Bilateral transverse sinus stenosis predicts IIH without papilledema in patients with migraine. Neurology 67: , Dashti SR, Nakaji P, Hu YC, Frei DF, Abla AA, Yao T, et al: Styloidogenic jugular venous compression syndrome: diagnosis and treatment: case report. Neurosurgery 70:E795 E799, De Simone R, Ranieri A, Bonavita V: Advancement in idiopathic intracranial hypertension pathogenesis: focus on sinus venous stenosis. Neurol Sci 31 (Suppl 1):S33 S39, De Simone R, Ranieri A, Montella S, Erro R, Fiorillo C, Bonavita V: Sinus venous stenosis-associated IIHWOP is a powerful risk factor for progression and refractoriness of pain in primary headache patients: a review of supporting evidences. Neurol Sci 32 (Suppl 1):S169 S171, Dwyer CM, Prelog K, Owler BK: The role of venous sinus outflow obstruction in pediatric idiopathic intracranial hypertension. J Neurosurg Pediatr 11: , Farb RI, Vanek I, Scott JN, Mikulis DJ, Willinsky RA, Tomlinson G, et al: Idiopathic intracranial hypertension: the prevalence and morphology of sinovenous stenosis. Neurology 60: , Friedman DI, Jacobson DM: Diagnostic criteria for idiopathic intracranial hypertension. Neurology 59: , Karahalios DG, Rekate HL, Khayata MH, Apostolides PJ: Elevated intracranial venous pressure as a universal mechanism in pseudotumor cerebri of varying etiologies. Neurology 46: , Kelly LP, Saindane AM, Bruce BB, Ridha MA, Riggeal BD, Newman NJ, et al: Does bilateral transverse cerebral venous sinus stenosis exist in patients without increased intracranial pressure? Clin Neurol Neurosurg 115: , Lai LT, Danesh-Meyer HV, Kaye AH: Visual outcomes and headache following interventions for idiopathic intracranial hypertension. J Clin Neurosci 21: , Puffer RC, Mustafa W, Lanzino G: Venous sinus stenting for idiopathic intracranial hypertension: a review of the literature. J Neurointerv Surg 5: , Rohr A, Bindeballe J, Riedel C, van Baalen A, Bartsch T, Doerner L, et al: The entire dural sinus tree is compressed in patients with idiopathic intracranial hypertension: a longitudinal, volumetric magnetic resonance imaging study. Neuroradiology 54:25 33, Goodwin CR, Elder BD, Ward A, Orkoulas-Razis D, Kosztowski TA, Hoffberger J, et al: Risk factors for failed transverse sinus stenting in pseudotumor cerebri patients. Clin Neurol Neurosurg 127:75 78, Saindane AM, Bruce BB, Desai NK, Roller LA, Newman NJ, Biousse V: Transverse sinus stenosis in adult patients 6 J Neurosurg March 11, 2016
7 Venography and pressure measurements in IIH and non-iih headache with Chiari malformation type I. AJR Am J Roentgenol 203: , Stevens SA, Previte M, Lakin WD, Thakore NJ, Penar PL, Hamschin B: Idiopathic intracranial hypertension and transverse sinus stenosis: a modelling study. Math Med Biol 24:85 109, Teleb MS, Cziep ME, Lazzaro MA, Gheith A, Asif K, Remler B, et al: Idiopathic intracranial hypertension. A systematic analysis of transverse sinus stenting. Interv Neurol 2: , 2013 Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author Contributions Conception and design: Albuquerque, Levitt. Acquisition of data: Albuquerque, Levitt, Hlubek, Moon, Kalani, McDougall. Analysis and interpretation of data: Albuquerque, Levitt, Hlubek. Drafting the article: Albuquerque, Levitt. Critically revising the article: all authors. Reviewed submitted version of manuscript: all authors. Statistical analysis: Albuquerque, Levitt. Administrative/ technical/material support: Albuquerque, Levitt, Hlubek, Moon. Study supervision: Albuquerque. Correspondence Felipe C. Albuquerque, c/o Neuroscience Publications, Barrow Neurological Institute, St. Joseph s Hospital and Medical Center, 350 W. Thomas Rd., Phoenix, AZ neuropub@ dignityhealth.org. J Neurosurg March 11,
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA)
 Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Prevalence of venous sinus stenosis in Pseudotumor cerebri(ptc) using digital subtraction angiography (DSA) Dr.Mohamed hamdy ibrahim MBBC,MSc,MD, PhD Neurology Degree Kings lake university (USA). Fellow
Khalil Zahra, M.D Neuro-interventional radiology
 Khalil Zahra, M.D Neuro-interventional radiology 1 Disclosure None 2 Outline Etiology and pathogensis Imaging techniques and Features Literature review Treatment modalities Endovascular techniques Long
Khalil Zahra, M.D Neuro-interventional radiology 1 Disclosure None 2 Outline Etiology and pathogensis Imaging techniques and Features Literature review Treatment modalities Endovascular techniques Long
A Case of Stent Placement for Intracranial Hypertension Associated with Venous Sinus Stenosis
 DOI: 10.5797/jnet.cr.2016-0080 A Case of Stent Placement for Intracranial Hypertension Associated with Venous Sinus Stenosis Rei Yamaguchi, Koji Sato, Hiroya Fujimaki, and Ken Asakura Objective: We encountered
DOI: 10.5797/jnet.cr.2016-0080 A Case of Stent Placement for Intracranial Hypertension Associated with Venous Sinus Stenosis Rei Yamaguchi, Koji Sato, Hiroya Fujimaki, and Ken Asakura Objective: We encountered
What do lumbar puncture and jugular venoplasty say about a connection between chronic fatigue syndrome and idiopathic intracranial hypertension?
 The ejournal of the European Society of Minimally Invasive Neurological Therapy What do lumbar puncture and jugular venoplasty say about a connection Nicholas Higgins, John D Pickard, Andrew M Lever Abstract
The ejournal of the European Society of Minimally Invasive Neurological Therapy What do lumbar puncture and jugular venoplasty say about a connection Nicholas Higgins, John D Pickard, Andrew M Lever Abstract
Dural venous sinus angioplasty and stenting for the treatment of idiopathic intracranial hypertension
 1 Department of Interventional Neuroradiology, Oregon Health and Science University, Portland, Oregon, USA 2 School of Medicine, Oregon Health and Science University, Portland, Oregon, USA 3 Department
1 Department of Interventional Neuroradiology, Oregon Health and Science University, Portland, Oregon, USA 2 School of Medicine, Oregon Health and Science University, Portland, Oregon, USA 3 Department
THE SWOLLEN DISC. Valerie Biousse, MD Emory University School of Medicine Atlanta, GA
 THE SWOLLEN DISC Valerie Biousse, MD Emory University School of Medicine Atlanta, GA Updated from: Neuro-Ophthalmology Illustrated. Biousse V, Newman NJ. Thieme, New-York,NY. 2 nd Ed, 2016. Edema of the
THE SWOLLEN DISC Valerie Biousse, MD Emory University School of Medicine Atlanta, GA Updated from: Neuro-Ophthalmology Illustrated. Biousse V, Newman NJ. Thieme, New-York,NY. 2 nd Ed, 2016. Edema of the
Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis.
 Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis. Poster No.: R-0005 Congress: 2015 ASM Type: Scientific Exhibit Authors: A.
Normal Variations and Artifacts in MR Venography that may cause Pitfalls in the Diagnosis of Cerebral Venous Sinus Thrombosis. Poster No.: R-0005 Congress: 2015 ASM Type: Scientific Exhibit Authors: A.
I diopathic intracranial hypertension (IIH) is an uncommon
 1662 PAPER Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting J N P Higgins, C Cousins, B K Owler, N Sarkies, J D Pickard... See end of article for authors affiliations...
1662 PAPER Idiopathic intracranial hypertension: 12 cases treated by venous sinus stenting J N P Higgins, C Cousins, B K Owler, N Sarkies, J D Pickard... See end of article for authors affiliations...
Sometimes symptomatic intracranial venous. Styloidogenic Jugular Venous Compression Syndrome: Diagnosis and Treatment: Case Report CASE REPORT TOPIC
 TOPIC CASE REPORT CASE REPORT Shervin R. Dashti, MD, PhD* Peter Nakaji, MD Yin C. Hu, MD Don F. Frei, MD Adib A. Abla, MD Tom Yao, MD* David Fiorella, MD, PhD *Norton Neuroscience Center, Norton Healthcare,
TOPIC CASE REPORT CASE REPORT Shervin R. Dashti, MD, PhD* Peter Nakaji, MD Yin C. Hu, MD Don F. Frei, MD Adib A. Abla, MD Tom Yao, MD* David Fiorella, MD, PhD *Norton Neuroscience Center, Norton Healthcare,
Intracranial hypertension and headache. Daniel Tibussek, MD
 Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
Intracranial hypertension and headache. Daniel Tibussek, MD none Disclosures Overview Case Clinical presentation of pediatric PTC Nomenclature, Definition What is intracranial hypertension? Diagnostic
Idiopathic intracranial hypertension (IIH) is a relatively
 LITERATURE REVIEW Fifty shades of gradients: does the pressure gradient in venous sinus stenting for idiopathic intracranial hypertension matter? A systematic review Cameron M. McDougall, MD, 1,2 Vin Shen
LITERATURE REVIEW Fifty shades of gradients: does the pressure gradient in venous sinus stenting for idiopathic intracranial hypertension matter? A systematic review Cameron M. McDougall, MD, 1,2 Vin Shen
Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls
 AJNR Am J Neuroradiol 21:74 78, January 2000 Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls R. H. Ayanzen, C. R. Bird, P. J. Keller, F. J. McCully, M. R. Theobald, and J. E. Heiserman
AJNR Am J Neuroradiol 21:74 78, January 2000 Cerebral MR Venography: Normal Anatomy and Potential Diagnostic Pitfalls R. H. Ayanzen, C. R. Bird, P. J. Keller, F. J. McCully, M. R. Theobald, and J. E. Heiserman
IIH, a syndrome of intracranial hypertension without mass
 Published July 28, 2011 as 10.3174/ajnr.A2575 ORIGINAL RESEARCH R.M. Ahmed M. Wilkinson G.D. Parker M.J. Thurtell J. Macdonald P.J. McCluskey R. Allan V. Dunne M. Hanlon B.K. Owler G.M. Halmagyi Transverse
Published July 28, 2011 as 10.3174/ajnr.A2575 ORIGINAL RESEARCH R.M. Ahmed M. Wilkinson G.D. Parker M.J. Thurtell J. Macdonald P.J. McCluskey R. Allan V. Dunne M. Hanlon B.K. Owler G.M. Halmagyi Transverse
T he aetiology of idiopathic intracranial hypertension is
 PAPER MR venography in idiopathic intracranial hypertension: unappreciated and misunderstood J N P Higgins, J H Gillard, B K Owler, K Harkness, J D Pickard... See end of article for authors affiliations...
PAPER MR venography in idiopathic intracranial hypertension: unappreciated and misunderstood J N P Higgins, J H Gillard, B K Owler, K Harkness, J D Pickard... See end of article for authors affiliations...
Idiopathic intracranial hypertension is a syndrome of raised
 ORIGINAL RESEARCH M. Bussière R. Falero D. Nicolle A. Proulx V. Patel D. Pelz Unilateral Transverse Sinus Stenting of Patients with Idiopathic Intracranial Hypertension BACKGROUND AND PURPOSE: The pathophysiology
ORIGINAL RESEARCH M. Bussière R. Falero D. Nicolle A. Proulx V. Patel D. Pelz Unilateral Transverse Sinus Stenting of Patients with Idiopathic Intracranial Hypertension BACKGROUND AND PURPOSE: The pathophysiology
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings. Jonathan A. Micieli, MD Valérie Biousse, MD
 Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Typical idiopathic intracranial hypertension Optic nerve appearance and brain MRI findings Jonathan A. Micieli, MD Valérie Biousse, MD A 24 year old African American woman is referred for bilateral optic
Intracranial pressure in unresponsive chronic migraine
 J Neurol (2014) 261:1365 1373 DOI 10.1007/s00415-014-7355-2 ORIGINAL COMMUNICATION Intracranial pressure in unresponsive chronic migraine Roberto De Simone Angelo Ranieri Silvana Montella Paolo Cappabianca
J Neurol (2014) 261:1365 1373 DOI 10.1007/s00415-014-7355-2 ORIGINAL COMMUNICATION Intracranial pressure in unresponsive chronic migraine Roberto De Simone Angelo Ranieri Silvana Montella Paolo Cappabianca
Idiopathic intracranial hypertension (IIH) is a disease of
 Venous Sinus Stenting in Idiopathic Intracranial Hypertension: Results of a Prospective Trial Marc J. Dinkin, MD, Athos Patsalides, MD, MPH Background: Our goal was to evaluate the safety and efficacy
Venous Sinus Stenting in Idiopathic Intracranial Hypertension: Results of a Prospective Trial Marc J. Dinkin, MD, Athos Patsalides, MD, MPH Background: Our goal was to evaluate the safety and efficacy
MR Venography in the Pediatric Patient
 AJNR Am J Neuroradiol 26:50 55, January 2005 MR Venography in the Pediatric Patient Nancy Rollins, Claro Ison, Timothy Booth, and Jon Chia BACKGROUND AND PURPOSE: Little is known about age-related changes
AJNR Am J Neuroradiol 26:50 55, January 2005 MR Venography in the Pediatric Patient Nancy Rollins, Claro Ison, Timothy Booth, and Jon Chia BACKGROUND AND PURPOSE: Little is known about age-related changes
Literature Review: Neurosurgery
 NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
NANOS 2018 Kona, Hawaii Literature Review: Neurosurgery Neil R. Miller, MD FACS Frank B. Walsh Professor of Neuro-Ophthalmology Professor of Ophthalmology, Neurology & Neurosurgery Johns Hopkins University
National Hospital for Neurology and Neurosurgery
 National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
National Hospital for Neurology and Neurosurgery Venous sinus stents (for the treatment of venous sinus stenosis and idiopathic intracranial hypertension) Lysholm Department of Neuroradiology If you would
Idiopathic hydrocephalus in children and idiopathic intracranial hypertension in adults: two manifestations of the same pathophysiological process?
 See the corresponding editorial in this issue, pp 435 438. J Neurosurg (6 Suppl Pediatrics) 107:439 444, 2007 Idiopathic hydrocephalus in children and idiopathic intracranial hypertension in adults: two
See the corresponding editorial in this issue, pp 435 438. J Neurosurg (6 Suppl Pediatrics) 107:439 444, 2007 Idiopathic hydrocephalus in children and idiopathic intracranial hypertension in adults: two
UNIVERSITY OF NAPLES FEDERICO II
 UNIVERSITY OF NAPLES FEDERICO II DEPARTMENT OF NEUROSCIENCES, REPRODUCTIVE SCIENCES AND ODONTOSTOMATOLOGY PhD Program in Neuroscience XXVII Prof. Lucio Annunziato PhD Thesis THE ROLE OF RAISED INTRACRANIAL
UNIVERSITY OF NAPLES FEDERICO II DEPARTMENT OF NEUROSCIENCES, REPRODUCTIVE SCIENCES AND ODONTOSTOMATOLOGY PhD Program in Neuroscience XXVII Prof. Lucio Annunziato PhD Thesis THE ROLE OF RAISED INTRACRANIAL
CASE PRESENTATION. Key Words: cerebral venous thrombosis, internal jugular vein stenosis, thrombolysis, stenting (Kaohsiung J Med Sci 2005;21:527 31)
 Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Treatment of cerebral venous thrombosis SUCCESSFUL TREATMENT OF CEREBRAL VENOUS THROMBOSIS ASSOCIATED WITH BILATERAL INTERNAL JUGULAR VEIN STENOSIS USING DIRECT THROMBOLYSIS AND STENTING: A CASE REPORT
Clinical trial registration no.: NCT (clinicaltrials.gov) https://thejns.org/doi/abs/ / jns161301
 CLINICAL ARTICLE J Neurosurg 128:120 125, 2018 Analysis of saccular aneurysms in the Barrow Ruptured Aneurysm Trial Robert F. Spetzler, MD, 1 Joseph M. Zabramski, MD, 1 Cameron G. McDougall, MD, 1 Felipe
CLINICAL ARTICLE J Neurosurg 128:120 125, 2018 Analysis of saccular aneurysms in the Barrow Ruptured Aneurysm Trial Robert F. Spetzler, MD, 1 Joseph M. Zabramski, MD, 1 Cameron G. McDougall, MD, 1 Felipe
TEACHING CASE # 5. Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy
 TEACHING CASE # 5 Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy CASE PRESENTATION 22M with right transverse and sigmoid venous sinuses occlusion s/p transvenous
TEACHING CASE # 5 Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy CASE PRESENTATION 22M with right transverse and sigmoid venous sinuses occlusion s/p transvenous
Magnetic resonance imaging in pseudotumor cerebri
 Magnetic resonance imaging in pseudotumor cerebri Poster No.: C-1004 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit J. Saad 1, F. Marrakchi 2, F. Harbi 1 ; 1 Nejran/SA, 2 Ksour Essaf/TN
Magnetic resonance imaging in pseudotumor cerebri Poster No.: C-1004 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit J. Saad 1, F. Marrakchi 2, F. Harbi 1 ; 1 Nejran/SA, 2 Ksour Essaf/TN
Untangling Cerebral Dural Arteriovenous Fistulas
 Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Untangling Cerebral Dural Arteriovenous Fistulas Bradley A. Gross, MD Assistant Professor, Dept of Neurosurgery, University of Pittsburgh September 2017 davfs Definition Clinical Presentation Natural History
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Management of Pseudo Tumor Cerebri by Frequent Tapping VS lumboperitoneal Shunt
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (5), Page 4556-4560 Management of Pseudo Tumor Cerebri by Frequent Tapping VS lumboperitoneal Shunt Ali K. Ali, Maamoun M. Abo Shousha, Mohammed
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (5), Page 4556-4560 Management of Pseudo Tumor Cerebri by Frequent Tapping VS lumboperitoneal Shunt Ali K. Ali, Maamoun M. Abo Shousha, Mohammed
Idiopathic intracranial hypertension, or pseudotumor cerebri, is
 ORIGINAL RESEARCH BRAIN MRI Evidence of Impaired CSF Homeostasis in Obesity- Associated Idiopathic Intracranial Hypertension N. Alperin, S. Ranganathan, A.M. Bagci, D.J. Adams, B. Ertl-Wagner, E. Saraf-Lavi,
ORIGINAL RESEARCH BRAIN MRI Evidence of Impaired CSF Homeostasis in Obesity- Associated Idiopathic Intracranial Hypertension N. Alperin, S. Ranganathan, A.M. Bagci, D.J. Adams, B. Ertl-Wagner, E. Saraf-Lavi,
Sinus Venous Thrombosis
 Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
1. Introduction. Correspondence should be addressed to Robert M. Starke;
 e Scientific World Journal Volume 2015, Article ID 140408, 8 pages http://dx.doi.org/10.1155/2015/140408 Review Article Endovascular Treatment of Venous Sinus Stenosis in Idiopathic Intracranial Hypertension:
e Scientific World Journal Volume 2015, Article ID 140408, 8 pages http://dx.doi.org/10.1155/2015/140408 Review Article Endovascular Treatment of Venous Sinus Stenosis in Idiopathic Intracranial Hypertension:
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Pseudotumor cerebri comorbid with meningioma: A review and case series
 SNI: Unique Case Observations OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Ather Enam, M.D., Aga Khan University, Karachi, Sindh, Pakistan Case Report Pseudotumor
SNI: Unique Case Observations OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Ather Enam, M.D., Aga Khan University, Karachi, Sindh, Pakistan Case Report Pseudotumor
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis
 Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis Poster No.: C-3377 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit
Optimized phase contrast MRV technique outperforms timeof-flight in the diagnosis of cerebral venous thrombosis Poster No.: C-3377 Congress: ECR 2010 Type: Topic: Authors: Keywords: DOI: Scientific Exhibit
The headache profile of idiopathic intracranial hypertension
 The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
The headache profile of idiopathic intracranial hypertension Michael Wall CEPHALALGIA Wall M. The headache profile of idiopathic intracranial hypertension. Cephalalgia 1990;10:331-5. Oslo. ISSN 0333-1024
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and
 Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series
 CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
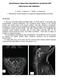 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Michelle L. Ischayek D.O. Emergency Medicine Resident Aria Health
 Michelle L. Ischayek D.O. Emergency Medicine Resident Aria Health History 15 year old African female with CC of Headache. Onset: 2 weeks ago Location: Frontal Character: Sharp & Throbbing Radiation: None
Michelle L. Ischayek D.O. Emergency Medicine Resident Aria Health History 15 year old African female with CC of Headache. Onset: 2 weeks ago Location: Frontal Character: Sharp & Throbbing Radiation: None
Methods. Yahya Paksoy, Bülent Oğuz Genç, and Emine Genç. AJNR Am J Neuroradiol 24: , August 2003
 AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
AJNR Am J Neuroradiol 24:1364 1368, August 2003 Retrograde Flow in the Left Inferior Petrosal Sinus and Blood Steal of the Cavernous Sinus Associated with Central Vein Stenosis: MR Angiographic Findings
ACR Appropriateness Criteria Suspected Lower Extremity Deep Vein Thrombosis EVIDENCE TABLE
 . Fowkes FJ, Price JF, Fowkes FG. Incidence of diagnosed deep vein thrombosis in the general population: systematic review. Eur J Vasc Endovasc Surg 003; 5():-5.. Hamper UM, DeJong MR, Scoutt LM. Ultrasound
. Fowkes FJ, Price JF, Fowkes FG. Incidence of diagnosed deep vein thrombosis in the general population: systematic review. Eur J Vasc Endovasc Surg 003; 5():-5.. Hamper UM, DeJong MR, Scoutt LM. Ultrasound
Department of Neurosurgery, Showa University School of Medicine; and 2 Tokyo Midtown Medical Center, Tokyo, Japan
 CLINICAL ARTICLE Detection rates and sites of unruptured intracranial aneurysms according to sex and age: an analysis of MR angiography based brain examinations of 4070 healthy Japanese adults Yohichi
CLINICAL ARTICLE Detection rates and sites of unruptured intracranial aneurysms according to sex and age: an analysis of MR angiography based brain examinations of 4070 healthy Japanese adults Yohichi
IIH, previously known as pseudotumor cerebri, is a syndrome
 ORIGINAL RESEARCH A.H. Aiken J.A. Hoots A.M. Saindane P.A. Hudgins Incidence of Cerebellar Tonsillar Ectopia in Idiopathic Intracranial Hypertension: A Mimic of the Chiari I Malformation BACKGROUND AND
ORIGINAL RESEARCH A.H. Aiken J.A. Hoots A.M. Saindane P.A. Hudgins Incidence of Cerebellar Tonsillar Ectopia in Idiopathic Intracranial Hypertension: A Mimic of the Chiari I Malformation BACKGROUND AND
Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 2 Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses N Barua, M Bradley, N Patel Citation N Barua, M Bradley,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 2 Hemorrhagic infarction due to transverse sinus thrombosis mimicking cerebral abscesses N Barua, M Bradley, N Patel Citation N Barua, M Bradley,
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
Transverse Sinus Stenosis in Adult Patients With Chiari Malformation Type 1
 Neuroradiology/Head and Neck Imaging Original Research Saindane et al. Transverse Sinus Stenosis on MRI Neuroradiology/Head and Neck Imaging Original Research Amit M. Saindane 1 Beau B. Bruce 2,3,4 Nilesh
Neuroradiology/Head and Neck Imaging Original Research Saindane et al. Transverse Sinus Stenosis on MRI Neuroradiology/Head and Neck Imaging Original Research Amit M. Saindane 1 Beau B. Bruce 2,3,4 Nilesh
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
What is IIH? Idiopathic Intracranial Hypertension (IIH)
 What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
What is IIH? Idiopathic Intracranial Hypertension (IIH) What is Idiopathic Intracranial Hypertension? Idiopathic intracranial hypertension (IIH), also known as benign intracranial hypertension or pseudotumour
NEURO QUIZ 45 EHLERS DANLOS SYNDROME
 NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
NEURO QUIZ 45 EHLERS DANLOS SYNDROME Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D START 1. Regarding
A.J. Hauer Intracranial dural arteriovenous fistulae
 A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
Brain Imaging in Pediatric Pseudotumor Cerebri Syndrome
 Review Article 49 Brain Imaging in Pediatric Pseudotumor Cerebri Syndrome Emanuele David 1,2 Kshitij Mankad 3 1 Department of Radiology, Anatomopathology and Oncology, Sapienza University of Rome, Rome,
Review Article 49 Brain Imaging in Pediatric Pseudotumor Cerebri Syndrome Emanuele David 1,2 Kshitij Mankad 3 1 Department of Radiology, Anatomopathology and Oncology, Sapienza University of Rome, Rome,
an idiopathic intracranial hypertension without papilledema
 Neurol Sci (2010) 31:411 415 DOI 10.1007/s10072-010-0229-1 REVIEW ARTICLE Is idiopathic intracranial hypertension without papilledema a risk factor for migraine progression? Roberto De Simone Angelo Ranieri
Neurol Sci (2010) 31:411 415 DOI 10.1007/s10072-010-0229-1 REVIEW ARTICLE Is idiopathic intracranial hypertension without papilledema a risk factor for migraine progression? Roberto De Simone Angelo Ranieri
Risk of Spaceflight-Induced Intracranial Hypertension / Vision Alterations
 Risk of Spaceflight-Induced Intracranial Hypertension / Vision Alterations Michael A. Williams The Sandra and Malcolm Berman Brain & Spine Institute, Baltimore, MD Adult Hydrocephalus Center Disclosures
Risk of Spaceflight-Induced Intracranial Hypertension / Vision Alterations Michael A. Williams The Sandra and Malcolm Berman Brain & Spine Institute, Baltimore, MD Adult Hydrocephalus Center Disclosures
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
NIH Public Access Author Manuscript J Am Coll Radiol. Author manuscript; available in PMC 2013 June 24.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Radiol. 2010 January ; 7(1): 73 76. doi:10.1016/j.jacr.2009.06.015. Cerebral Aneurysms Janet C. Miller, DPhil, Joshua A.
NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Radiol. 2010 January ; 7(1): 73 76. doi:10.1016/j.jacr.2009.06.015. Cerebral Aneurysms Janet C. Miller, DPhil, Joshua A.
Endovascular Treatment for Idiopathic Intracranial Hypertension Improves Clinical Symptoms and Signs
 THIEME Original Article Artigo Original 1 Endovascular Treatment for Idiopathic Intracranial Hypertension Improves Clinical Symptoms and Signs Tratamento endovascular para hipertensão intracraniana idiopática
THIEME Original Article Artigo Original 1 Endovascular Treatment for Idiopathic Intracranial Hypertension Improves Clinical Symptoms and Signs Tratamento endovascular para hipertensão intracraniana idiopática
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
11/10/2017. Headache and Increased Pressure: A tale of 2 cases. Kathleen Digre MD University of Utah TWO CASES. 23 yo medical practice manager
 Headache and Increased Pressure: A tale of 2 cases Kathleen Digre MD University of Utah TWO CASES 23 yo medical practice manager September 2016 began developing intense frontal headaches first intermittent
Headache and Increased Pressure: A tale of 2 cases Kathleen Digre MD University of Utah TWO CASES 23 yo medical practice manager September 2016 began developing intense frontal headaches first intermittent
Endoscopic Optic Nerve Sheath Fenestration for Treatment of Papilledema Secondary to Intracranial Venous Hypertension: Report of Two Cases
 Case Report Endoscopic Optic Nerve Sheath Fenestration for Treatment of Papilledema Secondary to Intracranial Venous Hypertension: Report of Two Cases Wuttipong Tirakotai MD, MSc, Dr.med*, Patcharapim
Case Report Endoscopic Optic Nerve Sheath Fenestration for Treatment of Papilledema Secondary to Intracranial Venous Hypertension: Report of Two Cases Wuttipong Tirakotai MD, MSc, Dr.med*, Patcharapim
Clinician s Guide To Ordering NeuroImaging Studies
 Clinician s Guide To Ordering NeuroImaging Studies MRI CT South Jersey Radiology Associates The purpose of this general guide is to assist you in choosing the appropriate imaging test to best help your
Clinician s Guide To Ordering NeuroImaging Studies MRI CT South Jersey Radiology Associates The purpose of this general guide is to assist you in choosing the appropriate imaging test to best help your
Advanced Vascular Imaging: Pulsatile Tinnitus. Disclosures. Pulsatile Tinnitus: Differential Diagnosis. Pulsatile Tinnitus
 Advanced Vascular Imaging: Pulsatile Tinnitus Patrick Turski MD, Zach Clark MD, Tabby Kennedy MD The Objectives of this presentation are to: Review the differential diagnosis of pulsatile tinnitus Discuss
Advanced Vascular Imaging: Pulsatile Tinnitus Patrick Turski MD, Zach Clark MD, Tabby Kennedy MD The Objectives of this presentation are to: Review the differential diagnosis of pulsatile tinnitus Discuss
Vascular and Parameningeal Infections of the Head and Neck
 Vascular and Parameningeal Infections of the Head and Neck Kevin B. Laupland, MD, MSc, FRCPC Associate Professor Departments of Medicine, Critical Care Medicine, Pathology and Laboratory Medicine, and
Vascular and Parameningeal Infections of the Head and Neck Kevin B. Laupland, MD, MSc, FRCPC Associate Professor Departments of Medicine, Critical Care Medicine, Pathology and Laboratory Medicine, and
Headache in an Italian pediatric emergency department
 J Headache Pain (2008) 9:83 87 DOI 10.1007/s10194-008-0014-1 ORIGINAL Headache in an Italian pediatric emergency department Paola Scagni Æ Rosaura Pagliero Received: 2 October 2007 / Revised: 3 January
J Headache Pain (2008) 9:83 87 DOI 10.1007/s10194-008-0014-1 ORIGINAL Headache in an Italian pediatric emergency department Paola Scagni Æ Rosaura Pagliero Received: 2 October 2007 / Revised: 3 January
IDIOPATHIC INTRACRANIAL HYPERTENSION
 IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
IDIOPATHIC INTRACRANIAL HYPERTENSION ASSESSMENT OF VISUAL FUNCTION AND PROGNOSIS FOR VISUAL OUTCOME Doctor of Philosophy thesis Anglia Ruskin University, Cambridge Fiona J. Rowe Department of Orthoptics,
7/5/2016. Neonatal high-output cardiac failure. Case 1 POSTNATAL STRATEGIES FOR CEREBRAL ATERIOVENOUS MALFORMATIONS
 John Deveikis, M.D. POSTNATAL STRATEGIES FOR CEREBRAL ATERIOVENOUS MALFORMATIONS JULY, 2016 Neonatal high-output cardiac failure Tachypnea, tachycardia, hypotension, failure to thrive When congenital heart
John Deveikis, M.D. POSTNATAL STRATEGIES FOR CEREBRAL ATERIOVENOUS MALFORMATIONS JULY, 2016 Neonatal high-output cardiac failure Tachypnea, tachycardia, hypotension, failure to thrive When congenital heart
Over the last few decades, endoscopic third ventriculostomy
 clinical article J Neurosurg Pediatr 17:734 738, 2016 Long-term follow-up of endoscopic third ventriculostomy performed in the pediatric population Matthew G. Stovell, MBBS, 1 Rasheed Zakaria, MA, BMBCh,
clinical article J Neurosurg Pediatr 17:734 738, 2016 Long-term follow-up of endoscopic third ventriculostomy performed in the pediatric population Matthew G. Stovell, MBBS, 1 Rasheed Zakaria, MA, BMBCh,
Stroke & Neurovascular Center of New Jersey. Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center
 Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Transverse-Sigmoid Sinus Dural Arteriovenous Malformations
 Transverse-Sigmoid Sinus Dural Arteriovenous Malformations Kenan I. Amautovic, M.D., and Ali F. Krisht, M.D. '-...--- Learning Objectives: After reading this article, the participant should: 1. Have an
Transverse-Sigmoid Sinus Dural Arteriovenous Malformations Kenan I. Amautovic, M.D., and Ali F. Krisht, M.D. '-...--- Learning Objectives: After reading this article, the participant should: 1. Have an
Neuro-Vascular Intervention AAPC Regional Conference Springfield, MA
 Neuro-Vascular Intervention AAPC Regional Conference Springfield, MA October 8, 2010 1 Presented by: David Zielske, MD,CIRCC, CPC H, CCC, CCS, RCC General Recommendations for Physician Dictations State
Neuro-Vascular Intervention AAPC Regional Conference Springfield, MA October 8, 2010 1 Presented by: David Zielske, MD,CIRCC, CPC H, CCC, CCS, RCC General Recommendations for Physician Dictations State
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis
 Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis Michael P. Spearman, Charles A. Jungreis, Joseph J. Wehner, Peter C. Gerszten, and William C. Welch Summary: We present two cases of acute thrombosis
Endovascular Thrombolysis in Deep Cerebral Venous Thrombosis Michael P. Spearman, Charles A. Jungreis, Joseph J. Wehner, Peter C. Gerszten, and William C. Welch Summary: We present two cases of acute thrombosis
Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction. Erin H. Murphy, MD Rane Center
 Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction Erin H. Murphy, MD Rane Center Disclosure Speaker name: Erin H. Murphy... I have the following potential conflicts
Complete Evaluation of the Chronic Venous Patient: Recognizing deep venous obstruction Erin H. Murphy, MD Rane Center Disclosure Speaker name: Erin H. Murphy... I have the following potential conflicts
Cases of visual impairment caused by cerebral venous sinus occlusion-induced intracranial hypertension in the absence of headache
 Zhao et al. BMC Neurology (2018) 18:159 https://doi.org/10.1186/s12883-018-1156-7 CASE REPORT Open Access Cases of visual impairment caused by cerebral venous sinus occlusion-induced intracranial hypertension
Zhao et al. BMC Neurology (2018) 18:159 https://doi.org/10.1186/s12883-018-1156-7 CASE REPORT Open Access Cases of visual impairment caused by cerebral venous sinus occlusion-induced intracranial hypertension
Research Article Predictions of the Length of Lumbar Puncture Needles
 Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Idiopathic Intracranial Hypertension
 Idiopathic Intracranial Hypertension Dr. Mar'n Su+onBrown MD. FRCPC Neuro-Ophthalmology, Neurology Div of Neurology, Island Health Clinical Assistant Professor, Div of Neurology, UBC Stroke Rapid Assessment
Idiopathic Intracranial Hypertension Dr. Mar'n Su+onBrown MD. FRCPC Neuro-Ophthalmology, Neurology Div of Neurology, Island Health Clinical Assistant Professor, Div of Neurology, UBC Stroke Rapid Assessment
Neuroradiology. of Stroke and Headaches
 Neuroradiology of Stroke and Headaches Learning Objec:ves 1. Iden:fy T1 and T2 sequences 2. Recall the normal anatomy of the intracranial circula:on 3. Apply appropriate CT and MR imaging of the brain
Neuroradiology of Stroke and Headaches Learning Objec:ves 1. Iden:fy T1 and T2 sequences 2. Recall the normal anatomy of the intracranial circula:on 3. Apply appropriate CT and MR imaging of the brain
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
BMB Disclosures. Papilledema can be a. Neurological Emergency, Causing Preventable Blindness
 Reasonable Doubt: Can High Intracranial Pressure Occur Without Papilledema? 15 February 2013 Jonathan C. Horton hortonj@vision.ucsf.edu http://www.ucsf.edu/hortonlab BMB Disclosures Financial Disclosures
Reasonable Doubt: Can High Intracranial Pressure Occur Without Papilledema? 15 February 2013 Jonathan C. Horton hortonj@vision.ucsf.edu http://www.ucsf.edu/hortonlab BMB Disclosures Financial Disclosures
Patient referral for elective coronary angiography: challenging the current strategy
 Patient referral for elective coronary angiography: challenging the current strategy M. Santos, A. Ferreira, A. P. Sousa, J. Brito, R. Calé, L. Raposo, P. Gonçalves, R. Teles, M. Almeida, M. Mendes Cardiology
Patient referral for elective coronary angiography: challenging the current strategy M. Santos, A. Ferreira, A. P. Sousa, J. Brito, R. Calé, L. Raposo, P. Gonçalves, R. Teles, M. Almeida, M. Mendes Cardiology
Clinical Study Endoscopic Third Ventriculostomy in Previously Shunted Children
 Minimally Invasive Surgery Volume 2013, Article ID 584567, 4 pages http://dx.doi.org/10.1155/2013/584567 Clinical Study Endoscopic Third Ventriculostomy in Previously Shunted Children Eva Brichtova, 1
Minimally Invasive Surgery Volume 2013, Article ID 584567, 4 pages http://dx.doi.org/10.1155/2013/584567 Clinical Study Endoscopic Third Ventriculostomy in Previously Shunted Children Eva Brichtova, 1
Management of Cerebral Aneurysms in Polycystic Kidney Disease. Dr H Stockley Consultant Neuroradiologist Greater Manchester Neuroscience Centre
 Management of Cerebral Aneurysms in Polycystic Kidney Disease Dr H Stockley Consultant Neuroradiologist Greater Manchester Neuroscience Centre What is a cerebral aneurysm? Developmental degenerative arterial
Management of Cerebral Aneurysms in Polycystic Kidney Disease Dr H Stockley Consultant Neuroradiologist Greater Manchester Neuroscience Centre What is a cerebral aneurysm? Developmental degenerative arterial
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
NANOS Patient Brochure
 NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
NANOS Patient Brochure Pseudotumor Cerebri Copyright 2016. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for
Life after ARUBA: Management of Unruptured Brain Arteriovenous Malformations (AVMs)
 Life after ARUBA: Management of Unruptured Brain Arteriovenous Malformations (AVMs) Eric L. Zager, MD University of Pennsylvania Department of Neurosurgery No Disclosures Brain AVMs Incidence ~1 in 100,000
Life after ARUBA: Management of Unruptured Brain Arteriovenous Malformations (AVMs) Eric L. Zager, MD University of Pennsylvania Department of Neurosurgery No Disclosures Brain AVMs Incidence ~1 in 100,000
Orbital phlebography in idiopathic intracranial hypertension and chronic tension-type headache
 Original Article Orbital phlebography in idiopathic intracranial hypertension and chronic tension-type headache Acta Radiologica Short Reports 0(0) 1 7! The Foundation Acta Radiologica 2013 Reprints and
Original Article Orbital phlebography in idiopathic intracranial hypertension and chronic tension-type headache Acta Radiologica Short Reports 0(0) 1 7! The Foundation Acta Radiologica 2013 Reprints and
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Selective disconnection of cortical venous reflux as treatment for cranial dural arteriovenous fistulas
 J Neurosurg 101:31 35, 2004 Selective disconnection of cortical venous reflux as treatment for cranial dural arteriovenous fistulas J. MARC C. VAN DIJK, M.D., PH.D., KAREL G. TERBRUGGE, M.D., ROBERT A.
J Neurosurg 101:31 35, 2004 Selective disconnection of cortical venous reflux as treatment for cranial dural arteriovenous fistulas J. MARC C. VAN DIJK, M.D., PH.D., KAREL G. TERBRUGGE, M.D., ROBERT A.
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents
 Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
