Associated Variables of Myositis in Systemic Lupus Erythematosus: A Cross-Sectional Study
|
|
|
- Marsha Baker
- 5 years ago
- Views:
Transcription
1 e-issn DOI: /MSM Received: Accepted: Published: Associated Variables of Myositis in Systemic Lupus Erythematosus: A Cross-Sectional Study Authors Contribution: Study Design A Data Collection B Statistical Analysis C Data Interpretation D Manuscript Preparation E Literature Search F Funds Collection G BCDEF EF CD AG Yan Liang Rui-Xue Leng Hai-Feng Pan Dong-Qing Ye Department of Epidemiology and Biostatistics, School of Public Health, Anhui Medical University, Hefei, Anhui, P.R. China Corresponding Author: Dong-Qing Ye, ydq@ahmu.edu.cn Source of support: The National Natural Science Foundation of China ( ) Background: Material/Methods: Results: Conclusions: MeSH Keywords: Full-text PDF: This study aimed to estimate the point prevalence of myositis and identify associated variables of myositis in systemic lupus erythematosus (SLE). Clinical date of patients hospitalized with lupus at the First Affiliated Hospital of Anhui Medical University and Anhui Provincial Hospital were collected. Patients were defined as having myositis if they reported the presence of persistent invalidating muscular weakness combined with increased levels of creatine phosphokinase (CPK) and abnormal electromyography (EMG). The study sample comprised 1701 lupus patients, of which 44 had myositis. Patients with SLE-associated myositis are more likely to have skin rash, alopecia, pericarditis, vasculitis, anti-sm, anti-rnp, anti-dsdna, thrombocytopenia, leukopenia, low C3, low C4, high erythrocyte sedimentation rate (ESR), high D-dimer, and active disease. Multivariate logistic regression found positive associations between leukopenia, alopecia, and active disease with myositis. Negative associations between myositis with the use of corticosteroids or immunosuppressive drugs were revealed in univariate and multivariate analysis. The point prevalence of myositis was 2.6% in SLE patients. The significant association of alopecia, leukopenia, and active disease with myositis suggests that organ damage, hematological abnormality, and high disease activity promote the progression of myositis in lupus patients. Lupus Erythematosus, Systemic Myositis Prevalence Risk Factors
2 Liang Y. et al.: Background Systemic lupus erythematosus (SLE) is a severe autoimmune disease, with multi-organ involvement and diverse clinical manifestations such as lupus nephritis, lupus encephalopathy, and thrombocytopenia [1]. Though not an American College of Rheumatology (ACR) criterion, myositis has traditionally been recognized as a feature in SLE and is considered to be a heterogeneous condition, sometimes less severe than, but sometimes similar to or even worse than, the primary disease [2 4]. In contrast to myalgia, which can affect nearly half of patients with SLE, true myositis is relatively rare and failure to identify these genuine cases probably explains the ill-deserved reputation of lupus myositis. The prevalence of myositis in SLE patients varies widely worldwide. In an African study, the prevalence was 3.4% [2], while in Europe and America the prevalence varies from 4% to 16% [4 10]. The wide variability in the prevalence rates reflects the varying definitions of myositis, the different diagnostic approaches, patient selection criteria, and number of patients involved. Though this condition is not common in SLE patients, myositis usually correlates with SLE activity and patient survival [4]. Thus, the importance of SLE-associated myositis should not be ignored. The non-specific nature of symptoms such as muscle pain, tenderness, and wasting related to myositis could result in a delay in the diagnosis of myositis in SLE patients [2,11]. This indicates a need for appropriate screening methods to detect myositis. In our study, we investigated the prevalence and associated variables of myositis in lupus patients. We believe the results of this study will provide valuable guidance for the prevention and management of this specific problem, as some of the clinical manifestations and laboratory findings of SLE provide helpful clues for earlier diagnosis of myositis. Material and Methods Patient recruitment The protocol for our study was consistent with the provisions of the World Medical Association Declaration of Helsinki, and informed consent was obtained from each subject before enrolment. This study was conducted with the approval of the Ethics Committee of Anhui Medical University. Clinical date of patients hospitalized with lupus at the First Affiliated Hospital of Anhui Medical University and Anhui Provincial Hospital were collected. All patients fulfilled at least 4 of the revised 1997 ACR classification criteria of SLE [12]. Collection of data was carried out from January 2011 to December Myositis Patients were defined as having myositis if they reported the presence of persistent invalidating muscular weakness (of proximal and/or distal mass muscles from upper and lower limbs) combined with increased levels of creatine phosphokinase (CPK) (CPK normal value UI/l) and abnormal electromyography (EMG) (electrical irritability, decrease in the mean duration of motor unit potentials or increase in the percentage of polyphasic motor unit potentials, and rapid firing of the motor unit potentials in relation to the level of activity) at the time of recruitment. Patients with myocardial ischemia at the time of recruitment, which can affect muscle enzyme levels, were excluded. Patients with surgery, trauma, pregnancy, or cancer at the time of recruitment, which might cause musculoskeletal damage, were also excluded. With these criteria, a final sample of 1701 Chinese SLE patients were included in the analyses. Clinical manifestations and laboratory abnormalities Clinical manifestations, including lupus nephritis, skin rash, alopecia, oral ulcers, neuropsychiatric symptoms, arthritis, pleuritis, pericarditis, fever (³38 C), and vasculitis, as well as laboratory abnormalities, including thrombocytopenia (< /L), leukopenia (< /L), autoantibodies, low C3 (<0.85 mg/ml), low C4 (<0.12 mg/ml), high erythrocyte sedimentation rate (ESR) (>20 mm/h), high D-dimer (>0.5 ug/ml), and high fibrinogen (>4.0 mg/ml), were presented at the time of recruitment or within 10 days. Lupus activity, drug use, arterial and venous diseases, hypertension, diabetes mellitus, hypercholesterolemia, and pulmonary arterial hypertension (PAH) SLE disease activity was evaluated by SLE Disease Activity Index (SLEDAI) score [13]. SLEDAI score was calculated based on the clinical manifestations and laboratory abnormalities of SLE patients that presented at the time of recruitment or within 10 days. Active lupus disease was defined as SLEDAI score ³8. Data on use of corticosteroids or immunosuppressive drugs (use in the past month or not) were collected by medical record review. Vascular events were objectively identified: (1) Ischemic heart disease; (2) Ischemic cerebrovascular disease; (3) Ischemic peripheral vascular disease; (4) Deep vein thrombosis; and (5) Pulmonary embolism. For any arterial event, we refer to the occurrence of 1 or more of events 1 3; for any venous event, we refer to the occurrence of 1 or more of events 4 5 [14]. Hypertension was considered to be present if blood pressure was ³140 mm Hg (systolic) or ³90 mm Hg (diastolic) on repeated measurements, or if the patient had been taking antihypertensive medication. Diabetes mellitus was considered to be present if fasting plasma glucose was >7.0 mmoles/liter, or if the patient was currently receiving anti-diabetic therapy. Hypercholesterolemia was considered to be present if a physician recorded the diagnosis in 2544
3 Liang Y. et al.: CLINICAL RESEARCH Table 1. Comparison of demographic data between systemic lupus erythematosus patients with myositis and without myositis. Age, median (interquartile range), years 37.0 ( ) 29.5 ( ) Sex, female, n (%) 1516 (91) 38 (86) Disease duration, median (interquartile range), years 2 (0 7) 0 (0 1) <0.001 * Values in bold are statistically significant at p<0.05. Table 2. Comparison of clinical manifestations between systemic lupus erythematosus patients with myositis and without myositis. Lupus nephritis, n (%) 771 (47) 25 (57) Skin rash, n (%) 603 (36) 23 (52) Alopecia, n (%) 145 (9) 12 (27) <0.001 Oral ulcers, n (%) 125 (8) 5 (11) Neuropsychiatric manifestations, n (%) 130 (8) 5 (11) Arthritis, n (%) 244 (15) 7 (16) Pleuritis, n (%) 230 (14) 7 (16) Pericarditis, n (%) 156 (9) 10 (23) Vasculitis, n (%) 155 (6) 12 (27) <0.001 Fever (³38 C), n (%) 214 (13) 9 (20) * Values in bold are statistically significant at p<0.05. the medical record, the patient had ever been prescribed lipid-lowering medication, or the fasting plasma cholesterol level measured was >200 mg/dl. PAH was diagnosed by transthoracic echocardiography (TTE); the criterion is pulmonary arterial systolic pressure (PASP) of >30 mmh at rest. Statistical analysis Continuous variables were summarized as median (interquartile range) and categorical variables as frequency (percentage). Comparison of each variable between different groups was evaluated using the nonparametric Mann-Whitney U test or chi-square test/fisher s exact test. Variables with statistical significance were evaluated by logistic regression analysis; results are presented as odds ratio (OR) along with their 95% confidence intervals. All tests were performed on SPSS Results Patients We studied 1701 patients with SLE, of which 1554 (91.4%) were female. The median (interquartile range) age was 36.0 ( ) years. Forty-four SLE patients in our research had myositis and the prevalence was 2.6%. As shown in Table 1, myositis is more typically observed in younger SLE patients (p=0.032) and in SLE patients with shorter disease duration (p<0.001). There was no difference was in sex distribution between the 2 groups. Clinical characteristics Skin rash, alopecia, pericarditis, and vasculitis were significantly associated with myositis (all p<0.050). The incidence of other clinical characteristics was similar between the patients with myositis and those without myositis (Table 2). Hematologic changes The presence of anti-sm, anti-rnp, anti-dsdna, thrombocytopenia, leukopenia, low C3, low C4, high ESR, and high D-dimer were elevated in the group with myositis (all p<0.050). Rates of fibrinogen and other autoantibodies were comparable between the patients with myositis and those without myositis (Table 3). 2545
4 Liang Y. et al.: Table 3. Comparison of laboratory data between systemic lupus erythematosus patients with myositis and without myositis*. Anti-Sm, n (%) 523 (32) 25 (57) <0.001 Anti-SSA/Ro, n (%) 988 (60) 31 (70) Anti-SSB/La, n (%) 213 (13) 7 (16) Anti-RNP, n (%) 469 (28) 20 (45) Anti-Rib P, n (%) 359 (22) 12 (27) Anti-dsDNA, n (%) 661 (40) 26 (59) Thrombocytopenia, n (%) 368 (22) 17 (39) Leukopenia, n (%) 487 (29) 24 (55) <0.001 Low complement C3, n (%) 1114 (67) 39 (89) Low complement C4, n (%) 809 (49) 35 (80) <0.001 High ESR, n (%) 1182 (71) 38 (86) High D-dimer, n (%) 1257 (76) 42 (95) High fibrinogen, n (%) 592 (36) 11 (25) * All laboratory abnormalities were presented at the time of recruitment or within 10 days. Of the 44 SLE patients with myositis, 18 received drug treatment in the past month; and of the 1657 SLE patients without myositis, 1100 received drug treatment in the past month; ** values in bold are statistically significant at p<0.05. anti-sm anti-smith; anti-rnp anti-ribonucleoprotein; anti-rib P anti-ribosomal RNP; anti-dsdna anti-double-stranded DNA; ESR high erythrocyte sedimentation rate. Table 4. Comparison of disease activity, drug use, arterial and venous diseases, hypertension, diabetes mellitus, hypercholesterolemia and PAH between systemic lupus erythematosus patients with myositis and without myositis. Active lupus disease, n (%) 934 (56) 40 (91) <0.001 Drug use, n (%) 1100 (66) 18 (41) <0.001 Arterial diseases, n (%) 23 (1) 1 (2) Venous diseases, n (%) 9 (1) 0 (0) Hypertension, n (%) 578 (35) 10 (23) Diabetes mellitus, n (%) 290 (18) 9 (20) Hypercholesterolemia, n (%) 50 (3) 0 (0) PAH, n (%) 124 (7) 5 (11) * Values in bold are statistically significant at p<0.05. PAH pulmonary arterial hypertension. Lupus activity, drug use, arterial and venous diseases, hypertension, diabetes mellitus, hypercholesterolemia, and PAH The incidence of active lupus disease was significantly higher in the patients with myositis (p<0.001) and the rate of drug use was significantly lower (p<0.001). The presence of arterial, venous diseases, hypertension, diabetes mellitus, hypercholesterolemia, and PAH were also compared between patients with myositis and without myositis; the results indicate the differences were not significant (Table 4). Independent associated variables for myositis in lupus patients Logistic regression modeling demonstrated that the presence of leukopenia (OR=2.038), alopecia (OR=2.794), and active lupus disease (OR=5.612) were independently associated with 2546
5 Liang Y. et al.: CLINICAL RESEARCH Table 5. Multivariable logistic analysis on risk factors of myositis in patients with systemic lupus erythematosus. Variables p Value OR 95% CI Leukopenia Alopecia Active lupus disease Drug use OR odds ratio; CI confidence intervals. lupus-associated myositis. In contrast, drug use acted as a protective factor in the development of myositis (OR=0.466, p=0.016) (Table 5). Discussion The association of myositis and SLE has been previously explored by several authors [2,15], showing that muscle involvement in SLE patients in the form of diffuse pain or muscular weakness is relatively frequent. A study reported that of 7 SLE patients with myositis, 3 had muscle weakness [15]. Another study of 6 patients who developed overlap syndrome of systemic lupus erythematosus and myositis reported that all patients had symmetrical muscle weakness (proximal muscle weakness in 6 cases and distal muscle weakness in 2 cases) [2]. Similarly, in the present study, the predominant muscular symptoms in the SLE patients with myositis were weakness rather that myalgia; none of the SLE patients with myositis showed dysphagia, dropped head, or symptoms related to a possible muscular involvement of the respiratory system. On the other hand, various histopathological changes have been previously described in the muscles of patients with SLE, including inflammation (myositis), vasculitis, type II fiber atrophy, vessel wall thickening, vacuolar myopathy, neurogenic muscular atrophy, and, rarely, inclusion bodies [2,4,15]. In line with these findings, the results of muscle biopsy in the present study indicated that inflammation and necrosis were the most common symptoms in the patients with overlap syndrome of SLE and myositis. In addition, less than half of patients showed fibrosis. However, there was no evidence of vasculitis and neuropathy on muscle biopsy. The present study found that myositis is uncommon in lupus patients, with a frequency of 2.6%. This rate was at the lower end of the range of prevalence rates reported from previous studies [2,4 10]. One explanation for the difference may be that all patients recruited in our study were from our Department of Rheumatology. Indeed, some SLE patients, especially those with myositis, have been hospitalized in the Department of Neurology. However, the development of myositis in these patients may not be due to lupus. Thus, the current research is more precise than past research. As expected from previous studies [4], myositis is more common in younger SLE patients and in those with shorter disease duration. There are several potential explanations for this discrepancy. First, the younger SLE patients and/or those with shorter disease duration may have had more active disease, resulting in the development of myositis. Supporting this, in the present study, age and disease duration of SLE patients were negatively associated with SLEDAI scores; moreover, the incidence of active lupus disease was significantly higher in the patients with myositis than in the patients without this feature. Second, it is also possible that the younger SLE patients and/or those with shorter disease duration tended to have more frequent measurements, especially for those with active disease. Therefore, myositis might be more likely to be detected and diagnosed in these patients. The criterion standard for defining myositis is EMG testing [11]. However, this invasive and painful procedure not routinely used in clinical practice. So, at best, identifying risk factors for the development of myositis in SLE may have important implications for the detection and management of this interesting condition. In the present study, logistic regression analysis revealed that alopecia, leukopenia, and active lupus disease were positively associated with myositis. The use of corticosteroids or immunosuppressive drugs was negatively associated with myositis. An association between alopecia and myositis in SLE has been widely reported in the literature [4,16 18]. For instance, a study [4] reviewed the notes on 10 patients with overlap of myositis and SLE and compared their features with 290 patients with SLE without myositis, showing that patients with SLE associated with myositis were more likely to have alopecia. Further, alopecia is usually a reflection of myositis activity. Several studies have shown that after receiving immunosuppressive agents, the hair of myositis patients with alopecia regrew, which coincided with increasing muscle strength [17,18]. These data resonate with our conclusions. In addition, previous studies have reported that patients with SLE-associated myositis were more likely to have other mucocutaneous damage, such as oral ulcers [4,16]. However, these results were not observed in our study. This discrepancy may be due to ethnic or environmental differences between populations. 2547
6 Liang Y. et al.: We proved that leukopenia was an independent risk factor. Although the associations between hematological indices with SLE-associated myositis have been reported in several studies [2 4], this is the first study to reveal that leukopenia was associated with the development of myositis. Future longitudinal investigations are required to determine the exact mechanism of leukopenia in the pathogenesis of SLE-associated myositis. In this study, we revealed that lupus patients with myositis are more likely to have disease flare-ups. We also found that use of corticosteroids or immunosuppressive drugs plays a protective role against the development of SLE-associated myositis, in agreement with previous studies of patients with only myositis [17,18]. However, the protective mechanism of drugs in SLE-associated myositis, either through reducing disease activity or through relieving musculoskeletal pathophysiological change, is not completely understood. The treatments used are basically the same, as many of the treatments used for myositis are applied to autoimmune diseases, including SLE. Corticosteroids were usually used as a first-line therapy. Most SLE patients with myositis seem to respond to corticosteroids at least to some degree and for a period of time. For instance, Maazoun et al. [2] reported that all of their patients with overlap syndrome of systemic lupus erythematosus and myositis had been treated with oral prednisone for 6 weeks, after which the dose was gradually tapered. Over a mean follow-up of 6 years, all patients had full remission of myositis. In the event of either poor response or adverse effects of corticosteroids, a second line of treatment with immunosuppressant may be required. Hashimoto et al. [19] reported that 2 SLE patients with steroid-resistant myositis were successfully treated with methotrexate (MTX); in both cases, steroid-resistant myositis was the main common finding, and this symptom was reduced within a few days, either by 7.5 mg or 5 mg MTX per week. In the present study, all of the 18 SLE patients with myositis who were treated with drugs had received corticosteroid therapy (usually as the initial treatment). If necessary, various immunosuppressants were used. Patients with lupus myositis were more likely to receive methotrexate treatment (often for a simultaneous flare-up of the myositis and their SLE), while cyclophosphamides were only given to those with lupus nephritis. Collectively, these data support treatment of SLE-associated myositis using a corticosteroid such as prednisone, which is then increased or tapered slowly based on the response. For patients who respond poorly to corticosteroids, additional immunosuppressants, such as methotrexate, may be necessary. However, the design of the present study may have introduced bias. Specifically, much of the clinical and laboratory data had to be collected retrospectively, and consequently there were no follow-up data. Therefore, evidence-based data with long-term follow-up that assess the efficacy of corticosteroids and/or immunosuppressants in patients with lupus myositis are required. Given the strong association between vascular events and myositis [20 22], we studied arterial and venous events as well as their traditional risk factors, including hypertension, diabetes and dyslipidemia, as potential correlates of musculoskeletal damage. Neither vascular events nor their traditional risk factors were shown to be associated with myositis. We also compared the presence of PAH between myositis and non-myositis patients, and found that this feature did not make any difference. Treatment for vascular events and PAH have improved over the years, and this could have contributed to lessening their impact on musculoskeletal diseases. We believe this is the first study to investigate possible factors in relation to myositis risk in a cohort of Chinese patient with SLE. However, this study has several limitations. First, myositis is a process that takes place over time, as is the effect of the risk factors we studied. The cross-sectional nature of this study may have limited our ability to fully capture the temporal relationships in the myositis process. In addition, to better correlate SLE-associated myositis with risk factors, it is ideal to collect clinical data at the time of lupus diagnosis. However, in reality it is challenging to obtain these concurrent data. In our study, although a subset of clinical data was obtained at the time of diagnosis, others were obtained at relapse or remission stage. These patients were on medications, including a subset of patients who were on immunosuppressive agents. This is clearly a cofounding variable, and a limitation of our study is that we did not examine these concurrent data. Finally, the generalizability of the findings in the present study may be limited given that lupus patients in our study group were all are Chinese. Further investigation is needed in other ethnic groups. Conclusions This study is the first to discuss the prevalence of myositis in Chinese lupus patients. The significant association of alopecia, leukopenia, and active disease with myositis suggests that organ damage, hematological abnormality, and high disease activity promote the progression of myositis in lupus patients. Declaration of conflicting interests None. 2548
7 Liang Y. et al.: CLINICAL RESEARCH References: 1. Liang Y, Xu WD, Peng H et al: SOCS signaling in autoimmune diseases: Molecular mechanisms and therapeutic implications. Eur J Immunol, 2014; 44: Maazoun F, Frikha F, Snoussi M et al: Systemic lupus erythematosusmyositis overlap syndrome: report of 6 cases. Clin Pract, 2011; 1: e89 3. Record JL, Beukelman T, Cron RQ: High prevalence of myositis in a southeastern United States pediatric systemic lupus erythematosus cohort. Pediatr Rheumatol Online J, 2011; 9: Dayal NA, Isenberg DA: SLE/myositis overlap: Are the manifestations of SLE different in overlapdisease? Lupus, 2002; 11: Estes D, Chlaristian CL: The natural history of systemic lupus erythematosus by prospective analysis. Medicine (Balt), 1971; 50: Feinglass EJ, Arnett FC, Dorsch CA et al: Neuropsychiatric manifestations of systemic lupus erythematosus: diagnosis, clinical spectrum and relationship to other the disease. Medicine (Balt), 1976; 55: Fessel WJ: Systemic lupus in erythematosus in the community. Arch Intern Med, 1974; 134: Tsokos GC, Moutsopolous HM, Steinberg AD: Muscle involvement in systemic lupus erythematosus. JAMA, 1981; 246: Foot RA, Kimbrough SM, Stevens JC: Lupus myositis. Muscle Nerve, 1982; 5: Michet CJ Jr., McKenna CH, Elveback LR et al: Epidemiology of systemic lupus erythematosus and other connective tissue disease in Rochester, Minnesota, 1950 through Mayo Clinic Proc, 1985; 60: Bohan A, Peter JB: Polymyositis and dermatomyositis (first of two parts). N Engl J Med, 1975; 292: Hochberg MC: Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum, 1997; 40: Bombardier C, Gladman DD, Urowitz MB et al: Derivation of the SLEDAI. A disease activity index for lupus patients. The Committee on Prognosis Studies in SLE. Arthritis Rheum, 1992; 35: Lundström E, Gustafsson JT, Jönsen A, Leonard D, Zickert A, Elvin K, et al. HLA-DRB1*04/*13 alleles are associated with vascular disease and antiphospholipid antibodies in systemic lupus erythematosus. Ann Rheum Dis. 2013;72: Jakati S, Rajasekhar L, Uppin M, Challa S: SLE myopathy: A clinicopathological study. Int J Rheum Dis, 2015; 18: Cassano N, Amerio P, D Ovidio R, Vena GA: Hair disorders associated with autoimmune connective tissue diseases. G Ital Dermatol Venereol, 2014; 149: Levine TD: Rituximab in the treatment of dermatomyositis: An open-label pilot study. Arthritis Rheum, 2005; 52: Riley P, Maillard SM, Wedderburn LR et al: Intravenous cyclophosphamide pulse therapy in juvenile dermatomyositis. A review of efficacy and safety. Rheumatology (Oxford), 2004; 43: Hashimoto M, Nonaka S, Furuta E et al: Methotrexate for steroid-resistant systemic lupus erythematosus. Clin Rheumatol, 1994; 13: Van Gelder H, Charles-Schoeman C: The heart in inflammatory myopathies. Rheum Dis Clin North Am, 2014; 40: Tisseverasinghe A, Bernatsky S, Pineau CA: Arterial events in persons with dermatomyositis and polymyositis. J Rheumatol, 2009; 36: Szodoray P, Hajas A, Kardos L et al: Distinct phenotypes in mixed connective tissue disease: subgroups and survival. Lupus, 2012; 21:
Development of SLE among Possible SLE Patients Seen in Consultation: Long-Term Follow-Up. Disclosures. Background. Evidence-Based Medicine.
 Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies
 Original Article Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies Col K Narayanan *, Col V Marwaha +, Col K Shanmuganandan #, Gp Capt S Shankar
Original Article Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies Col K Narayanan *, Col V Marwaha +, Col K Shanmuganandan #, Gp Capt S Shankar
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Mandana Nikpour 1,2, Murray B Urowitz 1*, Dominique Ibanez 1, Paula J Harvey 3 and Dafna D Gladman 1. Abstract
 RESEARCH ARTICLE Open Access Importance of cumulative exposure to elevated cholesterol and blood pressure in development of atherosclerotic coronary artery disease in systemic lupus erythematosus: a prospective
RESEARCH ARTICLE Open Access Importance of cumulative exposure to elevated cholesterol and blood pressure in development of atherosclerotic coronary artery disease in systemic lupus erythematosus: a prospective
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience
 Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Predictors of arthritis in pediatric patients with lupus
 Sule et al. Pediatric Rheumatology (2015) 13:30 DOI 10.1186/s12969-015-0027-7 RESEARCH ARTICLE Open Access Predictors of arthritis in pediatric patients with lupus SD Sule 1*, DG Moodalbail 2, J Burnham
Sule et al. Pediatric Rheumatology (2015) 13:30 DOI 10.1186/s12969-015-0027-7 RESEARCH ARTICLE Open Access Predictors of arthritis in pediatric patients with lupus SD Sule 1*, DG Moodalbail 2, J Burnham
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
Living with Lupus: An Insider s Perspective
 Living with Lupus: An Insider s Perspective Pamela Thorpe, MD, FACP Lupus Foundation of America, Inc. Philadelphia Tri-State Chapter Volunteer May 2014 My Own Story Is it Lupus Yet? The What What is this?
Living with Lupus: An Insider s Perspective Pamela Thorpe, MD, FACP Lupus Foundation of America, Inc. Philadelphia Tri-State Chapter Volunteer May 2014 My Own Story Is it Lupus Yet? The What What is this?
Additional file 2: Details of cohort studies and randomised trials
 Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Observations on the occurrence of exacerbations in clinical course of systemic lupus erythematosus
 112 ORIGINAL Observations on the occurrence of exacerbations in clinical course of systemic lupus erythematosus Reiko Tomioka 1, Kenji Tani 2,KeikoSato 1, Chiyuki Suzuka 1, Yuko Toyoda 1, Jun Kishi 1,
112 ORIGINAL Observations on the occurrence of exacerbations in clinical course of systemic lupus erythematosus Reiko Tomioka 1, Kenji Tani 2,KeikoSato 1, Chiyuki Suzuka 1, Yuko Toyoda 1, Jun Kishi 1,
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study.
 1. Title Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study. 2. Background Systemic Lupus Erythematosus (SLE) is a chronic, autoimmune and
1. Title Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study. 2. Background Systemic Lupus Erythematosus (SLE) is a chronic, autoimmune and
Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December Reference : NHSCB/A3C/1b
 Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December 2012 Reference : NHSCB/A3C/1b NHS Commissioning Board Clinical Commissioning Policy Statement: Rituximab
Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December 2012 Reference : NHSCB/A3C/1b NHS Commissioning Board Clinical Commissioning Policy Statement: Rituximab
Lupus as a risk factor for cardiovascular disease
 Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Disclosures. Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies. None
 Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
Rheumatological Approaches to Differential Diagnosis, Physical Examination, and Interpretation of Studies Sarah Goglin MD Assistant Professor of Medicine Division of Rheumatology Disclosures None 1 [footer
UNFOLDING NATURE S ORIGAMI: MEDICAL TREATMENT OF TAKAYASU ARTERITIS AND GIANT CELL ARTERITIS
 UNFOLDING NATURE S ORIGAMI: MEDICAL TREATMENT OF TAKAYASU ARTERITIS AND GIANT CELL ARTERITIS CanVasc meeting Montreal Nov 22 2012 Patrick Liang Service de rhumatologie Centre Hospitalier Universitaire
UNFOLDING NATURE S ORIGAMI: MEDICAL TREATMENT OF TAKAYASU ARTERITIS AND GIANT CELL ARTERITIS CanVasc meeting Montreal Nov 22 2012 Patrick Liang Service de rhumatologie Centre Hospitalier Universitaire
Supplementary material
 Supplementary material Table S1: Dubois Guidelines for Diagnosis of DrugInduced Lupus 1. Continuous treatment with a known lupusinducing drug for 1month and usually much longer 2. Presenting symptoms:
Supplementary material Table S1: Dubois Guidelines for Diagnosis of DrugInduced Lupus 1. Continuous treatment with a known lupusinducing drug for 1month and usually much longer 2. Presenting symptoms:
Benlysta (belimumab) Prior Authorization Criteria Program Summary
 Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Original Article. Abstract
 Original Article Diagnostic accuracy of antinuclear antibodies and anti-double stranded DNA antibodies in patients of systemic lupus erythematosus presenting with dermatological features Attiya Tareen*,
Original Article Diagnostic accuracy of antinuclear antibodies and anti-double stranded DNA antibodies in patients of systemic lupus erythematosus presenting with dermatological features Attiya Tareen*,
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Noninfectious Causes of Fever in 128 Patients with Systemic Lupus Erythematosus
 Iran J Public Health, Vol. 48, No.1, Jan 2019, pp.62-68 Original Article Noninfectious Causes of Fever in 128 Patients with Systemic Lupus Erythematosus Feng GUO 1, Jianmei CHEN 1, Yu XIE 1, *Xueping ZHOU
Iran J Public Health, Vol. 48, No.1, Jan 2019, pp.62-68 Original Article Noninfectious Causes of Fever in 128 Patients with Systemic Lupus Erythematosus Feng GUO 1, Jianmei CHEN 1, Yu XIE 1, *Xueping ZHOU
SCLERODERMA OVERLAP SYNDROME: A CASE REPORT Diwakar K. Singh 1, Nataraju H. V 2
 SCLERODERMA OVERLAP SYNDROME: A Diwakar K. Singh 1, Nataraju H. V 2 HOW TO CITE THIS ARTICLE: Diwakar K. Singh, Nataraju H. V. Scleroderma Overlap Syndrome: A Case Report. Journal of Evolution of Medical
SCLERODERMA OVERLAP SYNDROME: A Diwakar K. Singh 1, Nataraju H. V 2 HOW TO CITE THIS ARTICLE: Diwakar K. Singh, Nataraju H. V. Scleroderma Overlap Syndrome: A Case Report. Journal of Evolution of Medical
Lupus. Fast facts. What is lupus? What causes lupus? Who gets lupus?
 Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z
 Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
What your autoantibodies tell us about your disease. Mark Gourley, MD
 What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
What your autoantibodies tell us about your disease Mark Gourley, MD The Importance of the Immune System Defends us against foreign invaders Self (cancer) and Nonself (virus, bacteria, etc.) But, if the
Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis
 THE EGYPTIAN JOURNAL OF IMMUNOLOGY Vol. 23 (1), 2016 Page: 00-00 Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis 1
THE EGYPTIAN JOURNAL OF IMMUNOLOGY Vol. 23 (1), 2016 Page: 00-00 Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis 1
Risk factors for damage in childhood-onset systemic lupus erythematosus in Asians: a case control study
 Sit and Chan Pediatric Rheumatology (2018) 16:56 https://doi.org/10.1186/s12969-018-0271-8 RESEARCH ARTICLE Open Access Risk factors for damage in childhood-onset systemic lupus erythematosus in Asians:
Sit and Chan Pediatric Rheumatology (2018) 16:56 https://doi.org/10.1186/s12969-018-0271-8 RESEARCH ARTICLE Open Access Risk factors for damage in childhood-onset systemic lupus erythematosus in Asians:
UPDATES ON PEDIATRIC SLE
 UPDATES ON PEDIATRIC SLE BY ANGELA MIGOWA, PEDIATRIC RHEUMATOLOGIST/SENIOR INSTRUCTOR AKUHN MBCHB-UON, MMED-AKUHN,PEDIATRIC RHEUMATOLOGY- MCGILL UNIVERSITY HEALTH CENTRE ROSA PARKS OBJECTIVES RECOGNIZE
UPDATES ON PEDIATRIC SLE BY ANGELA MIGOWA, PEDIATRIC RHEUMATOLOGIST/SENIOR INSTRUCTOR AKUHN MBCHB-UON, MMED-AKUHN,PEDIATRIC RHEUMATOLOGY- MCGILL UNIVERSITY HEALTH CENTRE ROSA PARKS OBJECTIVES RECOGNIZE
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab
 (2016) 25, 346 354 http://lup.sagepub.com PAPER Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab DA Roth 1, A Thompson 2, Y Tang 2*, AE
(2016) 25, 346 354 http://lup.sagepub.com PAPER Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab DA Roth 1, A Thompson 2, Y Tang 2*, AE
The many faces of myositis. Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands
 The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS
 Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Clinical Laboratory. [None
 Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
Clinical Laboratory Procedure Result Units Ref Interval Accession Collected Received Double-Stranded DNA (dsdna) Ab IgG ELISA Detected * [None 18-289-900151 Detected] Double-Stranded DNA (dsdna) Ab IgG
ONE of the following:
 Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
.,Dr Ali Alkazzaz Babylon collage of medicine 2016
 .,Dr Ali Alkazzaz Babylon collage of medicine 2016 Lupus history Lupus is the Latin word for wolf 1 st used medically in the 10 th century Described clinically in the 19 th century Butterfly rash in 1845
.,Dr Ali Alkazzaz Babylon collage of medicine 2016 Lupus history Lupus is the Latin word for wolf 1 st used medically in the 10 th century Described clinically in the 19 th century Butterfly rash in 1845
Essential Rheumatology. Dr Ellen Bruce Consultant Rheumatologist CMFT
 Essential Rheumatology Dr Ellen Bruce Consultant Rheumatologist CMFT Saving the best for last! Apparently people recall best the first and last thing they re told. Far too difficult to include everything.
Essential Rheumatology Dr Ellen Bruce Consultant Rheumatologist CMFT Saving the best for last! Apparently people recall best the first and last thing they re told. Far too difficult to include everything.
New Evidence reports on presentations given at EULAR Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis
 New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience
 Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Serum CA125 elevation is independently associated with serositis in SLE patients
 Serum CA125 elevation is independently associated with serositis in SLE patients Z. Yang, Y. Liang, C. Li, R. Zhong Department of Laboratory Diagnostics, Changzheng Hospital, Second Military Medical University,
Serum CA125 elevation is independently associated with serositis in SLE patients Z. Yang, Y. Liang, C. Li, R. Zhong Department of Laboratory Diagnostics, Changzheng Hospital, Second Military Medical University,
Tools to Aid in the Accurate Diagnosis of. Connective Tissue Disease
 Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Connective Tissue Disease Tools to Aid in the Accurate Diagnosis of Connective Tissue Disease Connective Tissue Disease High quality assays and novel tests Inova offers a complete array of assay methods,
Title: BILAG-2004 Index captures SLE disease activity better than SLEDAI Dr Chee-Seng Yee MRCP(UK) University of Birmingham, Birmingham, UK
 ARD Online First, published on May 22, 2007 as 10.1136/ard.2007.070847 Title: BILAG-2004 Index captures SLE disease activity better than SLEDAI-2000 Authors: Dr Chee-Seng Yee MRCP(UK) University of Birmingham,
ARD Online First, published on May 22, 2007 as 10.1136/ard.2007.070847 Title: BILAG-2004 Index captures SLE disease activity better than SLEDAI-2000 Authors: Dr Chee-Seng Yee MRCP(UK) University of Birmingham,
RHEUMATOLOGY OVERVIEW. Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center
 RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
Mortality in idiopathic inflammatory myopathies
 Mortality in idiopathic inflammatory myopathies I.E. Lundberg 1, C.J. Forbess 2 1 Rheumatology Unit, Department of Medicine at Karolinska University Hospital in Solna, Karolinska Institutet, Stockholm,
Mortality in idiopathic inflammatory myopathies I.E. Lundberg 1, C.J. Forbess 2 1 Rheumatology Unit, Department of Medicine at Karolinska University Hospital in Solna, Karolinska Institutet, Stockholm,
2/23/18. Disclosures. Rheumatic Diseases of Childhood. Making Room for Rheumatology. I have nothing to disclose. James J.
 Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Making Room for Rheumatology James J. Nocton, MD Disclosures I have nothing to disclose Rheumatic Diseases of Childhood Juvenile Idiopathic Arthritis (JIA) Systemic Lupus Erythematosus (SLE) Juvenile Dermatomyositis
Vasculitis. Edward Dwyer, M.D. Division of Rheumatology. Vasculitis
 Edward Dwyer, M.D. Division of Rheumatology VASCULITIS is a primary inflammatory disease process of the vasculature Determinants of the Clinical Manifestations of : Target organ involved Size of vessel
Edward Dwyer, M.D. Division of Rheumatology VASCULITIS is a primary inflammatory disease process of the vasculature Determinants of the Clinical Manifestations of : Target organ involved Size of vessel
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital
 Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Market Access CTR Summary
 Market Access CTR Summary Study No.: BEL114246 Title: Efficacy of Belimumab Treatment in a Subpopulation of Systemic Lupus Erythematosus (SLE) Patients: A Pooled Analysis of the HGS1006-C1056 (BLISS-52)
Market Access CTR Summary Study No.: BEL114246 Title: Efficacy of Belimumab Treatment in a Subpopulation of Systemic Lupus Erythematosus (SLE) Patients: A Pooled Analysis of the HGS1006-C1056 (BLISS-52)
Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:814-821 Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy Na Ri Kim 1, Eon Jeong Nam 1, Jong
ORIGINAL ARTICLE Korean J Intern Med 2014;29:814-821 Complex repetitive discharge on electromyography as a risk factor for malignancy in idiopathic inflammatory myopathy Na Ri Kim 1, Eon Jeong Nam 1, Jong
Switching Treatment Between Mycophenolate Mofetil and Azathioprine in Lupus Patients: Indications and Outcomes
 Arthritis Care & Research Vol. 66, No. 12, December 2014, pp 1905 1909 DOI 10.1002/acr.22364 2014, American College of Rheumatology ORIGINAL ARTICLE Switching Treatment Between Mycophenolate Mofetil and
Arthritis Care & Research Vol. 66, No. 12, December 2014, pp 1905 1909 DOI 10.1002/acr.22364 2014, American College of Rheumatology ORIGINAL ARTICLE Switching Treatment Between Mycophenolate Mofetil and
Idiopathic inflammatory myopathies
 Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Advanced oxidation protein products as a biomarker of cutaneous lupus erythematosus complicated by nephritis: a case-control study
 Advanced oxidation protein products as a biomarker of cutaneous lupus erythematosus complicated by nephritis: a case-control study Z. Xie 1 *, M. Zhang 2 *, B. Zhao 1, Q. Wang 1, J. Li 1, Y.Y. Liu 1, Y.H.
Advanced oxidation protein products as a biomarker of cutaneous lupus erythematosus complicated by nephritis: a case-control study Z. Xie 1 *, M. Zhang 2 *, B. Zhao 1, Q. Wang 1, J. Li 1, Y.Y. Liu 1, Y.H.
Systemic Lupus Erythematosus
 Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Reporting Autoimmune Diseases in Hematopoietic Stem Cell Transplantation
 Reporting Autoimmune Diseases in Hematopoietic Stem Cell Transplantation Marcelo C. Pasquini, MD, MSc HVD05_1.ppt Outline Review of autoimmune diseases (AID). Role of transplantation for AID Data collection:
Reporting Autoimmune Diseases in Hematopoietic Stem Cell Transplantation Marcelo C. Pasquini, MD, MSc HVD05_1.ppt Outline Review of autoimmune diseases (AID). Role of transplantation for AID Data collection:
Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology, SDM Medical College, Dharwad, Karnataka, India.
 JOURNAL OF CASE REPORTS 2015;5(1):147-151 A Rare Case of Juvenile Dermatomyositis Vikram Haridas 1,2, Kiran Haridas 1 1,2 Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology,
JOURNAL OF CASE REPORTS 2015;5(1):147-151 A Rare Case of Juvenile Dermatomyositis Vikram Haridas 1,2, Kiran Haridas 1 1,2 Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology,
Test Name Results Units Bio. Ref. Interval
 LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
LL - LL-ROHINI (NATIONAL REFERENCE 135091593 Age 25 Years Gender Male 30/8/2017 91600AM 30/8/2017 93946AM 31/8/2017 84826AM Ref By Final COLLAGEN DISEASES ANTIBODY ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF),
Late onset systemic lupus erythematosus in southern Chinese. Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p.
 Title Late onset systemic lupus erythematosus in southern Chinese Author(s) Ho, CTK; Mok, CC; Lau, CS; Wong, RWS Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p. 437-440 Issued Date 1998
Title Late onset systemic lupus erythematosus in southern Chinese Author(s) Ho, CTK; Mok, CC; Lau, CS; Wong, RWS Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p. 437-440 Issued Date 1998
Comparison between ESR and C-Reactive Protein(CRP) as a Marker of Disease activity in Patients with Rheumatoid Arthritis
 Original Article Comparison between ESR and C-Reactive Protein(CRP) as a Marker of Disease activity in Patients with Rheumatoid Arthritis Ali M.E. Yousef 1, Fatemah A. Elshabacy 2, Sherry K. Abdelrahman
Original Article Comparison between ESR and C-Reactive Protein(CRP) as a Marker of Disease activity in Patients with Rheumatoid Arthritis Ali M.E. Yousef 1, Fatemah A. Elshabacy 2, Sherry K. Abdelrahman
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. J. María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Demystifying. Systemic Lupus Erythematosus: Signs and Symptoms for Early Recognition. Teaching Fellows in Lupus Project
 Demystifying Systemic Lupus Erythematosus: Signs and Symptoms for Early Recognition Teaching Fellows in Lupus Project Introduction: Why are we here? Lupus can take 4-6 years and 3 providers before diagnosis*
Demystifying Systemic Lupus Erythematosus: Signs and Symptoms for Early Recognition Teaching Fellows in Lupus Project Introduction: Why are we here? Lupus can take 4-6 years and 3 providers before diagnosis*
Ischemic Stroke in Critically Ill Patients with Malignancy
 Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Case 1: History of J.H. Outside Evaluation. Outside Labs. Question #1
 Case 1: History of J.H. 64 yo man seen at UCSF 6-256 25-07. 9 months ago onset progressive weakness of arms and legs, with muscle atrophy in arms. 4 months ago red scaly rash on face, back of hands and
Case 1: History of J.H. 64 yo man seen at UCSF 6-256 25-07. 9 months ago onset progressive weakness of arms and legs, with muscle atrophy in arms. 4 months ago red scaly rash on face, back of hands and
Systemic lupus erythematosus in 50 year olds
 Postgrad Med J (1992) 68, 440-444 The Fellowship of Postgraduate Medicine, 1992 Systemic lupus erythematosus in 50 year olds I. Domenech, 0. Aydintug, R. Cervera, M. Khamashta, A. Jedryka-Goral, J.L. Vianna
Postgrad Med J (1992) 68, 440-444 The Fellowship of Postgraduate Medicine, 1992 Systemic lupus erythematosus in 50 year olds I. Domenech, 0. Aydintug, R. Cervera, M. Khamashta, A. Jedryka-Goral, J.L. Vianna
PS + MPs PS - MPs 37% 36% 64% 64%
 Supplementary Figure 1. Amount and distribution of phosphatidylserine negative (PS - ) and phosphatidylserine positive (PS + ) MPs in 280 SLE patients and 280 controls. Circles are proportional to the
Supplementary Figure 1. Amount and distribution of phosphatidylserine negative (PS - ) and phosphatidylserine positive (PS + ) MPs in 280 SLE patients and 280 controls. Circles are proportional to the
Test Name Results Units Bio. Ref. Interval
 135091662 Age 45 Years Gender Male 29/8/2017 120000AM 29/8/2017 100215AM 29/8/2017 110825AM Ref By Final RHEUMATOID AUTOIMMUNE COMREHENSIVE ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF), SERUM ----- 20-60
135091662 Age 45 Years Gender Male 29/8/2017 120000AM 29/8/2017 100215AM 29/8/2017 110825AM Ref By Final RHEUMATOID AUTOIMMUNE COMREHENSIVE ANEL ANTI NUCLEAR ANTIBODY / FACTOR (ANA/ANF), SERUM ----- 20-60
Muscle Pathology Surgical Pathology Unknown Conference. November, 2008 Philip Boyer, M.D., Ph.D.
 Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
Muscle Pathology Surgical Pathology Unknown Conference November, 2008 Philip Boyer, M.D., Ph.D. Etiologic Approach to Differential Diagnosis Symptoms / Signs / Imaging / Biopsy / CSF Analysis Normal Abnormal
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. José María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. José María Pego Reigosa ABSTRACT NUMBER: 2754 Comparison of Individually Tailored vs Systematic Rituximab Regimens to Maintain ANCA-Associated Vasculitis Remissions:
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. José María Pego Reigosa ABSTRACT NUMBER: 2754 Comparison of Individually Tailored vs Systematic Rituximab Regimens to Maintain ANCA-Associated Vasculitis Remissions:
ANCA associated vasculitis in China
 ANCA associated vasculitis in China Min Chen Renal Division, Peking University First Hospital, Beijing 100034, P. R. China 1 General introduction of AAV in China Disease spectrum and ANCA type Clinical
ANCA associated vasculitis in China Min Chen Renal Division, Peking University First Hospital, Beijing 100034, P. R. China 1 General introduction of AAV in China Disease spectrum and ANCA type Clinical
HIGH ANTI-DSDNA CONTENT IN SLE IMMUNE COMPLEXES IS ASSOCIATED WITH CLINICAL REMISSION FOLLOWING BELIMUMAB TREATMENT
 HIGH ANTI-DSDNA CONTENT IN SLE IMMUNE COMPLEXES IS ASSOCIATED WITH CLINICAL REMISSION FOLLOWING BELIMUMAB TREATMENT A. Sohrabian 1, I. Parodis 2, N. Carlströmer-Berthén 1, C. Sjöwall 3, A. Jönsen 4, A.
HIGH ANTI-DSDNA CONTENT IN SLE IMMUNE COMPLEXES IS ASSOCIATED WITH CLINICAL REMISSION FOLLOWING BELIMUMAB TREATMENT A. Sohrabian 1, I. Parodis 2, N. Carlströmer-Berthén 1, C. Sjöwall 3, A. Jönsen 4, A.
Situaciones estresantes en el lupus
 Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Lupus The Clinical Perspective
 Lupus The Clinical Perspective Anca D. Askanase, M.D., M.P.H. Associate Professor of Medicine Director Lupus Center Columbia University Medical Center New York-Presbyterian Hospital Systemic Lupus Erythematosus
Lupus The Clinical Perspective Anca D. Askanase, M.D., M.P.H. Associate Professor of Medicine Director Lupus Center Columbia University Medical Center New York-Presbyterian Hospital Systemic Lupus Erythematosus
Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations
 08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
08/30/10 09/26/10 Systemic lupus erythematosus (SLE): Pleuropulmonary Manifestations Camila Downey S. Universidad de Chile, School of Medicine, Year VII Harvard University, School of Medicine Sept 17,
Erythrocyte-bound C4d in combination with complement and autoantibody status for the monitoring of SLE
 To cite: Merrill JT, Petri MA, Buyon J, et al. Erythrocytebound C4d in combination with complement and autoantibody status for the monitoring of SLE. Lupus Science & Medicine 2018;5:e000263. doi:10.1136/
To cite: Merrill JT, Petri MA, Buyon J, et al. Erythrocytebound C4d in combination with complement and autoantibody status for the monitoring of SLE. Lupus Science & Medicine 2018;5:e000263. doi:10.1136/
2.0 Synopsis. Adalimumab (HUMIRA ) W Clinical Study Report R&D/15/0629. Individual Study Table Referring to Part of Dossier: Volume:
 2.0 Synopsis AbbVie Inc. Name of Study Drug: Adalimumab / HUMIRA Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only)
2.0 Synopsis AbbVie Inc. Name of Study Drug: Adalimumab / HUMIRA Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only)
Association of anti-mcv autoantibodies with SLE (Systemic Lupus Erythematosus) overlapping with various syndromes
 International Journal of Medicine and Medical Sciences Vol. () pp. 21-214, June 211 Available online http://www.academicjournals.org/ijmms ISSN 2-972 211 Academic Journals Full Length Research Paper Association
International Journal of Medicine and Medical Sciences Vol. () pp. 21-214, June 211 Available online http://www.academicjournals.org/ijmms ISSN 2-972 211 Academic Journals Full Length Research Paper Association
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
4/16/2018. Demystifying weakness: how to approach refractory myositis. Objectives. Disclosures. Off-label uses for medications will be discussed
 Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
Undifferentiated Connective Tissue Disease and Overlap Syndromes. Mark S. Box, MD
 Undifferentiated Connective Tissue Disease and Overlap Syndromes Mark S. Box, MD Overlap Syndromes As many as 25% of patients with rheumatic diseases with systemic symptoms cannot be definitely diagnosed
Undifferentiated Connective Tissue Disease and Overlap Syndromes Mark S. Box, MD Overlap Syndromes As many as 25% of patients with rheumatic diseases with systemic symptoms cannot be definitely diagnosed
Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis
 New Evidence reports on presentations given at ACR/ARHP 2010 Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis Report on ACR/ARHP 2010 presentations
New Evidence reports on presentations given at ACR/ARHP 2010 Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis Report on ACR/ARHP 2010 presentations
DRAFT FOR POC BOARD Clinical Commissioning Policy Proposition: Rituximab in Connective Tissue Disease associated Interstitial Lung Disease (adults)
 Clinical Commissioning Policy Proposition: Rituximab in Connective Tissue Disease associated Interstitial Lung Disease (adults) Reference: NHS England A/14/X01 CHECK Information Reader Box (IRB) to be
Clinical Commissioning Policy Proposition: Rituximab in Connective Tissue Disease associated Interstitial Lung Disease (adults) Reference: NHS England A/14/X01 CHECK Information Reader Box (IRB) to be
IMPACT OF LONG TERM-STEROID TREATMENT PRESCRIBED FOR SYSTEMIC AND AUTOIMMUNE DISEASES ON THE DEVELOPMENT OF ATHEROSCLEROSIS.
 1 IMPACT OF LONG TERM-STEROID TREATMENT PRESCRIBED FOR SYSTEMIC AND AUTOIMMUNE DISEASES ON THE DEVELOPMENT OF ATHEROSCLEROSIS. A NETWORK ORGANIZED BY THE EUROPEAN FEDERATION OF INTERNAL MEDICINE Coordination:
1 IMPACT OF LONG TERM-STEROID TREATMENT PRESCRIBED FOR SYSTEMIC AND AUTOIMMUNE DISEASES ON THE DEVELOPMENT OF ATHEROSCLEROSIS. A NETWORK ORGANIZED BY THE EUROPEAN FEDERATION OF INTERNAL MEDICINE Coordination:
The Power of the ANA. April 2018 Emily Littlejohn, DO MPH
 Emergent Rheumatologic Diseases and Disorders for Primary Care. The Power of the ANA April 2018 Emily Littlejohn, DO MPH Question 1: the ANA test is: A) A screening test with high specificity to diagnose
Emergent Rheumatologic Diseases and Disorders for Primary Care. The Power of the ANA April 2018 Emily Littlejohn, DO MPH Question 1: the ANA test is: A) A screening test with high specificity to diagnose
Lupus and Your Kidneys. Michael P. Madaio, MD Professor of Medicine Chairman of Medicine Medical College of Georgia Augusta, Georgia
 Lupus and Your Kidneys Michael P. Madaio, MD Professor of Medicine Chairman of Medicine Medical College of Georgia Augusta, Georgia Kidney Inflammation and Abnormal Function as a Result of Lupus (Lupus
Lupus and Your Kidneys Michael P. Madaio, MD Professor of Medicine Chairman of Medicine Medical College of Georgia Augusta, Georgia Kidney Inflammation and Abnormal Function as a Result of Lupus (Lupus
Case # 2 3/27/2017. Disclosure of Relevant Financial Relationships. Clinical history. Clinical history. Laboratory findings
 Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus
 Original papers Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus Martyna Tomczyk-Socha 1, B E, Hanna Sikorska-Szaflik 2, B E, Marek Frankowski 3, B D, Karolina
Original papers Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus Martyna Tomczyk-Socha 1, B E, Hanna Sikorska-Szaflik 2, B E, Marek Frankowski 3, B D, Karolina
Systemic lupus erythematosusassociated optic neuritis: clinical experience and literature review
 Systemic lupus erythematosusassociated optic neuritis: clinical experience and literature review Yen-Ching Lin, 1,2,3 An-Guor Wang 2,3 and May-Yung Yen 2,3 1 Department of Ophthalmology, Suao Veterans
Systemic lupus erythematosusassociated optic neuritis: clinical experience and literature review Yen-Ching Lin, 1,2,3 An-Guor Wang 2,3 and May-Yung Yen 2,3 1 Department of Ophthalmology, Suao Veterans
Autoimmune diseases. SLIDE 3: Introduction to autoimmune diseases Chronic
 SLIDE 3: Introduction to autoimmune diseases Chronic Autoimmune diseases Sometimes relapsing : and remitting. which means that they present as attacks Progressive damage Epitope spreading more and more
SLIDE 3: Introduction to autoimmune diseases Chronic Autoimmune diseases Sometimes relapsing : and remitting. which means that they present as attacks Progressive damage Epitope spreading more and more
Supplemental Figures and Legends
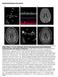 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Research. Prevalence of lower-extremity amputation among patients with diabetes mellitus: Is height a factor? Methods
 Research Prevalence of lower-extremity amputation among patients with diabetes mellitus: Is height a factor? Chin-Hsiao Tseng An abridged version of this article appeared in the Jan. 31, 2006, issue of
Research Prevalence of lower-extremity amputation among patients with diabetes mellitus: Is height a factor? Chin-Hsiao Tseng An abridged version of this article appeared in the Jan. 31, 2006, issue of
Is it Autoimmune or NOT! Presented to AONP! October 2015!
 Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
Systemic lupus erythematosus in a male patient
 IOP Conference Series: Earth and Environmental Science PAPER OPEN ACCESS Systemic lupus erythematosus in a male patient To cite this article: H Sibarani and Z Zubir 2018 IOP Conf. Ser.: Earth Environ.
IOP Conference Series: Earth and Environmental Science PAPER OPEN ACCESS Systemic lupus erythematosus in a male patient To cite this article: H Sibarani and Z Zubir 2018 IOP Conf. Ser.: Earth Environ.
Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory myositis
 Rheumatology 26;45:874 879 Advance Access publication 31 January 26 Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory
Rheumatology 26;45:874 879 Advance Access publication 31 January 26 Two simple, reliable and valid tests of proximal muscle function, and their application to the management of idiopathic inflammatory
Definition Chronic autoimmune disease The body s immune system starts attacking itself Can affect most organs and tissues in the body Brain, lungs, he
 LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
CME for Family Medicine Specialists. Evelyn Sutton, MD, FRCPC, FACP November 17, 2018
 CME for Family Medicine Specialists Evelyn Sutton, MD, FRCPC, FACP November 17, 2018 Disclosures Received $ from Advisory Board Consultant: Amgen, Abvie, Pfizer, Actelion, Lilly, Grants: Arthritis Society,
CME for Family Medicine Specialists Evelyn Sutton, MD, FRCPC, FACP November 17, 2018 Disclosures Received $ from Advisory Board Consultant: Amgen, Abvie, Pfizer, Actelion, Lilly, Grants: Arthritis Society,
Circulating 20S Proteasome Levels in Patients with Mixed Connective Tissue Disease and Systemic Lupus Erythematosus
 CLINICAL AND VACCINE IMMUNOLOGY, Sept. 2008, p. 1489 1493 Vol. 15, No. 9 1556-6811/08/$08.00 0 doi:10.1128/cvi.00187-08 Copyright 2008, American Society for Microbiology. All Rights Reserved. Circulating
CLINICAL AND VACCINE IMMUNOLOGY, Sept. 2008, p. 1489 1493 Vol. 15, No. 9 1556-6811/08/$08.00 0 doi:10.1128/cvi.00187-08 Copyright 2008, American Society for Microbiology. All Rights Reserved. Circulating
Test Name Results Units Bio. Ref. Interval
 135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
135091660 Age 44 Years Gender Male 29/8/2017 120000AM 29/8/2017 100219AM 29/8/2017 105510AM Ref By Final EXTRACTABLENUCLEAR ANTIGENS (ENA), QUANTITATIVE ROFILE CENTROMERE ANTIBODY, SERUM 20-30 Weak ositive
