T HIS presentation is a study of a consecutive series of 316 penetrating
|
|
|
- Sheena Morrison
- 5 years ago
- Views:
Transcription
1 INTRACRANIAL HEMATOMAS ASSOCIATED WITH PENETRATING WOUNDS OF THE BRAIN* JOSEPH C. BARNETT, M.D.,t AND ARNOLD M. MEIROWSKY, M.D.:~ (Received for publication September 29, 1954) T HIS presentation is a study of a consecutive series of 316 penetrating wounds of the brain with particular reference to the occurrence of intracranial hematomas. The data were made available through the concerted effort of the Medical Officers who were for varying lengths of time associated with an Army Mobile Neurosurgical Unit in Korea3 This unit was attached to a Mobile Army Surgical Hospital, the most forward medical institution offering major surgical facilities. The period represented is from October 13, 1951 through October 31,195~. The report is composed entirely of cases in which operation was performed. By way of definition, any compound wound with entry into the cranial vault and laceration of the meninges, regardless of the severity or extent of cerebral destruction, is considered as a penetrating wound of the brain. This is intended as a broad classification, embracing the through-and-through wounds and other such descriptive terms as tangential wounds of the brain. The conventional and generally accepted terms are used in the classification of the hematomas. The subcortical or intracerebral hematomas in this series refer, in general, to hematomas of the missile canal resulting from laceration of vascular radicles in the path of the missile. When a hematoma was found to occupy the ventricular cavity, out of particular interest, this was classified as an intraventricular hematoma. Direct visualization of the hematoma was the criterion for this diagnosis and in all instances the penetration traversed the ventricular system. It should be stated that an effort was made to differentiate between a hematoma and a few small clots. It is admittedly difficult to conceive that a missile could penetrate the cerebral substance without provoking some small amount of hemorrhage. Of assistance was the impression gained at operation as to the actual degree of space occupancy. As a rule following sufficient exposure, the hematoma forcefully extruded from its confines. On the contrary, with avulsive wounds of the head and brain occasionally large hematomas were found; however, they were not confined and therefore were not considered as intracranial hematomas in this series. A confined hematoma in excess of ~0 cc. was felt to be of clinical significance and was used as a criterion for the diagnosis of hematoma. * Presented at the annual meeting of the Harvey Cushing Society, Hollywood, Florida, April 24, Emory University, Georgia. 811 Bennie Dillon Bldg., Nash~'ille, Tennessee. 34
2 HEMATOMAS WITH PENETRATING WOUNDS OF BRAIN 35 ANALYSIS OF CASES Type of Missile. In ~86 of the 316 cases the injuries were the result of shell fragments. Shell fragments include fragments from mortars, mines, grenades or artillery shell. There were 18 instances in which the offending missile was the result of small arms fire. In the remaining cases the injuries were the result of blasting mishaps or the exact agent causing the injury was unknown. The actual size varied from a few millimeters in diameter to several centimeters. In the instances of tangential or glancing wounds, frequently there were no intracranial metallic fragments, the indriven cranial bone fragments being accountable for the cerebral penetration. Site of Injury. In ~60 cases of the series (8~ per cent), the primary involvement was limited to one cerebral lobe, not taking into consideration involvement below the cortical level. In 44 cases, more than one lobe was involved in the primary injury. This latter group comprised principally the TABLE 1 Incidence of hematomas in 316 cases of penetrating wounds No. of Incidence Site of Hematoma Hematomas (% of series) Epidural 18 3% Subdural 77 21% Intracerebral 87 ~S~ Intraventrieular ~ O. ~% glancing or tangential, the avulsive, and more extensive type of wound. There were 10 eases in the series in which there were two distinct penetrating wounds, and there were ~ instances in which three distinct penetrating wounds were found. Of some interest was the location of these wounds. There were 149 penetrating wounds that primarily involved the frontal lobes; 94 involved the parietal lobes; 75 involved the temporal lobes; ~5 involved the occipital lobes; and 1~ primarily involved the cerebellum. In this series, there seems to be a slight predilection for the left-sided injuries. Fifty-one per cent of the wounds primarily involved the left hemisphere, whereas 39 per cent primarily involved the right hemisphere. Four per cent involved the cerebellum and 6 per cent of the injuries were of a midline nature thus producing bilateral primary involvement. Incidence of Hematomas (Table 1). Of the 316 eases of penetrating wounds, 146 (46.~ per cent) were complicated with confined intracranial hematomas. Thirty-five of these patients presented more than one anatomically significant hematoma at operation. It was noted that the subdural and intracerebral hematomas were frequently associated. Thirty-one of the 35 patients who were found at operation to have more than one anatomically significant hematoma presented an intracerebral as well as a subdural hematoma.
3 36 JOSEPH C. BARNETT AND ARNOLD M. MEIROWSKY There were 13 cases in which there was a clinically significant epidural hematoma. This represents 3 per cent of the series. Of these 13 cases, 5 were complicated by the presence of either an intracerebral or a subdural hematoma. There were 77 cases, ~1 per cent of the series, in which subdural hematomas were found. Of the 77 cases, ~4 were complicated by the presence of either an intracerebral or an epidural hematoma. There were 87 cases in which intracerebral hematomas were present. This represents ~S per cent of the series. Of the 87 cases, 33 were complicated by accompanying subdural or epidural hematomas. There were ~ cases of intraventricular hematoma, s It was noted that some relationship existed between the site of penetration and the likelihood of hematoma (Table ~). Of the wounds primarily TABLE Relationship between location of wound and formation of hematoma Location of Wound No. of Associated Wounds Hematoma Frontal ~ Temporal 75 54% Parietal 94 32% Occipital 25 58% Cerebellum 12 52~ involving the frontal lobes, 3~ per cent were associated with hematomas whereas 54 per cent of wounds primarily involving the temporal lobes were associated with hematomas. Of the wounds involving the parietal lobes, 3~ per cent were associated with hematomas. Fifty-eight per cent of the occipital lobe penetrations and 5~ per cent of the cerebellar wounds were complicated with hematomas. It is of interest to note that frontal and parietal lobe penetrations are less frequently associated with hematoma formation than penetrating wounds elsewhere. Time Factor. Early surgical care for the traumatic neurosurgical patient has been emphasized by many previous writers and observers. 2,4,6,7 In consideration of the time factor in this series of patients, it must be borne in mind that the most reliable data concerning the time of injury were those recorded by the Aidman or the Batallion Surgeon when the patient was first administered medical treatment. There is admittedly a margin of error here, of possibly several hours in some instances, when because of exigencies of battle, the wounded had to await medical treatment. However, when the patient enters the medical evacuation chain, immediate disposition is possible. The helicopter evacuation plan of the seriously injured patient has created a new and now well recognized phase of medical evacuation. 5 Thirty-nine per cent of the patients included in this series were received
4 HEMATOMAS WITH PENETRATING WOUNDS OF BRAIN 37 for definitive neurosurgical care within 3 hours after first medical aid; ~9 per cent were received within 6 hours, and 10 per cent within 8 hours. Thus within a period of 8 hours a total of 78 per cent of the 316 patients were under definitive neurosurgical care. The remaining patients were for the most part from far distant points or were unavoidably detained for tactical reasons. Neurological Findings. Fifty-one per cent of the series on admission showed signs of neurological deficit. Central pareses, paralysis, visual loss, astereognosis, aphasia, marked sensorial change, as well as signs of acute intracranial distress were noted, followed and recorded. Of the 146 patients who were found at operation to have a significant intracranial hematoma 105, or 71 per cent, presented on admission or shortly thereafter conclusive evidence of neurological deficit. This figure compared to the over-all percentage (51 per cent) possibly is of some significance. DISCUSSION There have been many contributions regarding military neurosurgical casualties as to observation and management resulting from World Wars I and II. However, there are remarkably few references to the actual incidence of intracranial hematomas associated with penetrating wounds of the brain. Schorstein 7 in his study of World War II casualties observed that threequarters of the penetrating craniocerebral injuries presenting a small wound of entry were associated with intracranial hematoma. In this series no real effort was made to classify the size of the wounds, feeling that the important factor, as Schorstein stated, was the intracranial confinement of the hematoma; this being in contradistinction to the avulsive type of wound in which cerebral and meningeal bleeding readily escapes from the wound. Matson and Wolkin 3 observed that in instances in which the missile was found located near a cortical surface opposite or within the line of trajectory of the missile, there was likelihood of hematoma formation in the region of the missile. There were 15 instances of this particular situation encountered in the series. In 6 of these 15 a significant hematoma was found in the region of the distantly located missile. It is interesting that statistically this would be comparable to the over-all incidence of hematomas for the series if one were to consider the distant surface injury as a distinct penetrating wound. The time required for the evacuation of the patient to a major surgical facility is important relative to the incidence of hematoma. A total of approximately ~00 cases of penetrating wounds of the Brain were reviewed, these cases antedating the forward location of the neurosurgical team. During the early phase of the Korean conflict, neurosurgical casualties were evacuated to Japan for definitive care. The usual time required for transportation of the patient was from ~4 to 7~ hours. In this group of patients there was a 7 per cent incidence of intracranial hematoma. Some months later when it was possible to offer major surgical facilities within Korea, a neurosurgical team was established at the Evacuation Hospital level. The evacuation time at this level was lessened, usually to 1~ to 36 hours, and
5 38 JOSEPH C. BARNETT AND ARNOLD M. MEIROWSKY there was a ~4 per cent incidence of hematoma. These figures compared to the 46 per cent incidence of hematoma in the present series wherein the majority of the patients reached a facility for definitive care within 8 hours would seem significant. This time difference may be of value in the explanation of the somewhat divergent observations of previous authors. 1 The high incidence of confined intracranial hematomas in casualties examined and treated within 8 hours, lends added significance to the availability in a theatre of war of mobile neurosurgical teams at division level. SUMMARY 1. A series of 316 cases of penetrating wounds of the brain, treated by an Army Mobile Neurosurgical Team within 8 hours after injury, have been analyzed with regard to the occurrence of confined intracranial hematomas. 2. The incidence of confined intracranial hematomas was found to be 46.~ per cent. 3. By way of comparison, confined intracranial hematomas were found in ~7 per cent of patients treated 1~-36 hours, and in 7 per cent of patients treated ~4-7~ hours after having been wounded. 4. The high incidence of intracranial hematomas associated with penetrating wounds of the brain necessitates earliest possible definitive neurosurgical treatment. REFERENCES 1. CRAIG, W.M. Neurosurgery in World War II. U.S. Armed Forces med. J., 1952, 3: FINLAYSON, A.I. Penetrating war injuries of brain. Desirability of early definitive surgery. Bull. U.S. Army med. Dept., 1945, 3, No. 87: MATSON, D. D., and WOLKIN, J. Hematomas associated with penetrating wounds of the brain. J. Neurosurg., 1946, 3: MEInOWSKY, A.M. Penetrating craniocerebral trauma. Observations in Korean war. J. Amer. reed. Ass., 1954, 154: MEIROWSKY, A. M., and BARNETT, J.C. Mobile neurosurgical team. Ann. Surg., 1953, 138: MEmOWSKY, A. M., and HARSH, G. R., III. Treatment of penetrating craniocerebral trauma. In: Symposium on Military Medicine, U.S. Army Far East Command, 1951, SCHORSTmN, J. Intracranial haematoma in missile wounds. Brit. J. Surg., 1947, War Surg. Suppl. 1, WANNAMAKER, G.T. Transventricular wounds of the brain. J. Neurosurg., 1954, 11:
Missile Type.$ Eight patients reported injury from metallic fragments and 15 from high velocity missiles. There was no correlation between the
 TANGENTIAL WOUNDS OF SCALP AND SKULL* CAPTAIN PHILIP R. DODGE, M.C., U.S.A.,t AND LT. COL. ARNOLD M. MEIROWSKY, M.C., U.S.A.R. Tokyo Army Hospital, Tokyo, Japan (Received for publication April ~9, 195~)
TANGENTIAL WOUNDS OF SCALP AND SKULL* CAPTAIN PHILIP R. DODGE, M.C., U.S.A.,t AND LT. COL. ARNOLD M. MEIROWSKY, M.C., U.S.A.R. Tokyo Army Hospital, Tokyo, Japan (Received for publication April ~9, 195~)
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
injuries Visual disturbances after missile head Symonds, 1945; Calvert, 1947; Jepson and Whitty, 1947). At University College Hospital,
 Brit. J. Ophthal. (I 972) 56, 905 Visual disturbances after missile head injuries ADELOLA ADELOYE Neurosurgery Unit, University of Ibadan, Nigeria, West Africa Disturbances of vision after head injury,
Brit. J. Ophthal. (I 972) 56, 905 Visual disturbances after missile head injuries ADELOLA ADELOYE Neurosurgery Unit, University of Ibadan, Nigeria, West Africa Disturbances of vision after head injury,
Follow-up study of 103 American soldiers who sustained a brain wound in Vietnam
 Follow-up study of 103 American soldiers who sustained a brain wound in Vietnam MICHAEL E. CAREY, M.D., HAROLD F. YOUNG, M.D., BERKLEY L. RISH, M.D., AND JACOB L. MATHIS, M.D. Divisions of Neurosurgery,
Follow-up study of 103 American soldiers who sustained a brain wound in Vietnam MICHAEL E. CAREY, M.D., HAROLD F. YOUNG, M.D., BERKLEY L. RISH, M.D., AND JACOB L. MATHIS, M.D. Divisions of Neurosurgery,
T HE most adequate method of diagnosing subdural collection of blood
 THE ELECTROENCEPHALOGRAM SUBDURAL HEMATOMA IN LEWIS L. LEVY, M.D., LUDWIG H. SEGERBERG, M.D., RICHARD P. SCHMIDT, M.D., RICHARD C. TURRELL, M.D., AND EPHRAIM ROSEMAN, M.D. Sections of Neurology, Neurosurgery
THE ELECTROENCEPHALOGRAM SUBDURAL HEMATOMA IN LEWIS L. LEVY, M.D., LUDWIG H. SEGERBERG, M.D., RICHARD P. SCHMIDT, M.D., RICHARD C. TURRELL, M.D., AND EPHRAIM ROSEMAN, M.D. Sections of Neurology, Neurosurgery
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Where is the contre-coup? Atypical localization of occipital brain contusion
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Where is the contre-coup? Atypical localization of occipital brain contusion A.I. Cucu, Claudia Florida Costea, R.A. Sascau, B. Dobrovat,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Where is the contre-coup? Atypical localization of occipital brain contusion A.I. Cucu, Claudia Florida Costea, R.A. Sascau, B. Dobrovat,
Infection after depressed fracture of skull. Implications for management of nonmissile injuries
 Implications for management of nonmissile injuries BRYAN JENNETT, M.D., F.R.C.S., AND J. DOUGLAS MILLER, M.D., F.R.C.S. Institute o/ Neurological Sciences, and the University o/glasgow, Glasgow, Scotland
Implications for management of nonmissile injuries BRYAN JENNETT, M.D., F.R.C.S., AND J. DOUGLAS MILLER, M.D., F.R.C.S. Institute o/ Neurological Sciences, and the University o/glasgow, Glasgow, Scotland
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Vascular Malformations of the Brain. William A. Cox, M.D. Forensic Pathologist/Neuropathologist. September 8, 2014
 Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
T HIS report is based on the early phases of treatment of 300 consecutive
 SPINAL CORD INJURIES A REVIEW OF THE EARLY TREATMENT IN 300 CONSECUTIVE CASES DURING THE KOREAN CONFLICT MAJOR GORDON T. WANNAMAKER, M.C., U.S.A.* Section of Neurological Surgery, Tokyo Army Hospital,
SPINAL CORD INJURIES A REVIEW OF THE EARLY TREATMENT IN 300 CONSECUTIVE CASES DURING THE KOREAN CONFLICT MAJOR GORDON T. WANNAMAKER, M.C., U.S.A.* Section of Neurological Surgery, Tokyo Army Hospital,
Chronic Subdural Hematoma Following Maxillofacial Fracture: Report of 2 Cases
 Shimane J. Med. Sci., Vol.35 pp.15-19, 2018 Chronic Subdural Hematoma Following Maxillofacial Fracture: Report of 2 Cases Takashi KOIKE 1,2, Takahiro KANNO 2, Masaaki KARINO 2, Aya YOSHINO 2, Joji SEKINE
Shimane J. Med. Sci., Vol.35 pp.15-19, 2018 Chronic Subdural Hematoma Following Maxillofacial Fracture: Report of 2 Cases Takashi KOIKE 1,2, Takahiro KANNO 2, Masaaki KARINO 2, Aya YOSHINO 2, Joji SEKINE
I N T~, COVRS~, of the postoperative care, at the 36th General Hospital,
 OBSERVATIONS ON EARLY TYPE OF BRAIN ABSCESS FOLLOWING PENETRATING WOUNDS OF THE BRAIN MAJOR J. E. WEBSTER, M.C., A.U.S.,* CAPTAIN R. C. SCHNEIDER, ~.C., A.U.S., A~D LT. COL. J. E. LOFSTRO1V[, M.C., A.U.S.t
OBSERVATIONS ON EARLY TYPE OF BRAIN ABSCESS FOLLOWING PENETRATING WOUNDS OF THE BRAIN MAJOR J. E. WEBSTER, M.C., A.U.S.,* CAPTAIN R. C. SCHNEIDER, ~.C., A.U.S., A~D LT. COL. J. E. LOFSTRO1V[, M.C., A.U.S.t
ORIGINAL ARTICLE. Temporal Lobe Injury in Temporal Bone Fractures. imaging (MRI) to evaluate lesions of the temporal
 ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
Part 2: Prognosis in Penetrating Brain Injury
 Part 2: Prognosis in Penetrating Brain Injury J Trauma. 2001;51:S44 S86. INTRODUCTION AND METHODOLOGY Part 2 of this document presents early clinical indicators that may be prognostic of outcome among
Part 2: Prognosis in Penetrating Brain Injury J Trauma. 2001;51:S44 S86. INTRODUCTION AND METHODOLOGY Part 2 of this document presents early clinical indicators that may be prognostic of outcome among
T HE purpose of this presentation is to
 INCIDENCE OF POSTTRAUMATIC EPILEPSY IN KOREAN VETERANS AS COMPARED WITH THOSE FROM WORLD WAR I AND WORLD WAR II* WILLIAM F. CAVENESS, M.D.t A. EARL WALKER, M.D.,:~ AND PETER B. ASCROFT, M.S., F.R.C.S.w
INCIDENCE OF POSTTRAUMATIC EPILEPSY IN KOREAN VETERANS AS COMPARED WITH THOSE FROM WORLD WAR I AND WORLD WAR II* WILLIAM F. CAVENESS, M.D.t A. EARL WALKER, M.D.,:~ AND PETER B. ASCROFT, M.S., F.R.C.S.w
Management of Cerebrospinal Fluid Leaks
 Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
HIROSHI NAKAGUCHI, M.D., PH.D., TAKEO TANISHIMA, M.D., PH.D., Clinical Material and Methods
 J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
Cognitive Rehabilitation
 Last Review Date: March 10, 2017 Number: MG.MM.ME.58Cv2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: March 10, 2017 Number: MG.MM.ME.58Cv2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature
 Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
TBI are twice as common in males High potential for poor outcome Deaths occur at three points in time after injury
 Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Medical Review Guidelines Magnetic Resonance Angiography
 Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Gunshot Wounds of the Abdomen: Association of Surface Wounds with Internal Injuries
 Gunshot Wounds of the Abdomen: Association of Surface Wounds with Internal Injuries Abstract Ashfaq A. Razzaq ( Department of Surgery, Jinnah Post-graduate Medical Center, Karachi. ) Objective: To evaluate
Gunshot Wounds of the Abdomen: Association of Surface Wounds with Internal Injuries Abstract Ashfaq A. Razzaq ( Department of Surgery, Jinnah Post-graduate Medical Center, Karachi. ) Objective: To evaluate
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Extradural hematoma (EDH) accounts for 2% of all head injuries (1). In
 CASE REPORT Conservative management of extradural hematoma: A report of sixty-two cases A. Rahim H. Zwayed 1, Brandon Lucke-Wold 2 Zwayed ARH, Lucke-wold B. Conservative management of extradural hematoma:
CASE REPORT Conservative management of extradural hematoma: A report of sixty-two cases A. Rahim H. Zwayed 1, Brandon Lucke-Wold 2 Zwayed ARH, Lucke-wold B. Conservative management of extradural hematoma:
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG)
 USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
USASOC Neurocognitive Testing and Post Injury Evaluation and Treatment Clinical Practice Guideline (CPG) Note: The intent of this CPG is to serve as general guidance for medics and medical officers. It
Penetrating Trauma in Pediatric Patients. Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017
 Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
10/6/2017. Notice. Traumatic Brain Injury & Head Trauma
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Epilepsy after two different neurosurgical approaches
 Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Journal ofneurology, Neurosurgery, and Psychiatry, 1976, 39, 1052-1056 Epilepsy after two different neurosurgical approaches to the treatment of ruptured intracranial aneurysm R. J. CABRAL, T. T. KING,
Aspiration versus Excision in Management of Intracranial Abscesses
 Med. J. Cairo Univ., Vol. 84, No. 3, December: 229-233, 2016 www.medicaljournalofcairouniversity.net Aspiration versus Excision in Management of Intracranial Abscesses AYMAN T.M. MOHAMED, M.Sc.; AHMED
Med. J. Cairo Univ., Vol. 84, No. 3, December: 229-233, 2016 www.medicaljournalofcairouniversity.net Aspiration versus Excision in Management of Intracranial Abscesses AYMAN T.M. MOHAMED, M.Sc.; AHMED
MICHAEL L. LEVY, M.D.
 Neurosurg Focus 8 (1):Article 2, 1999 Outcome prediction following penetrating craniocerebral injury in a civilian population: aggressive surgical management in patients with admission Glasgow Coma Scale
Neurosurg Focus 8 (1):Article 2, 1999 Outcome prediction following penetrating craniocerebral injury in a civilian population: aggressive surgical management in patients with admission Glasgow Coma Scale
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
IDENTIFYING TARGET POPULATIONS & DESIGNING CLINICAL TRIALS FOR ANTIEPILEPTOGENESIS. Ettore Beghi Istituto Mario Negri, Milano ITALY
 IDENTIFYING TARGET POPULATIONS & DESIGNING CLINICAL TRIALS FOR ANTIEPILEPTOGENESIS Ettore Beghi Istituto Mario Negri, Milano ITALY OUTLINE Definitions & background risks in epilepsy End-points Target populations
IDENTIFYING TARGET POPULATIONS & DESIGNING CLINICAL TRIALS FOR ANTIEPILEPTOGENESIS Ettore Beghi Istituto Mario Negri, Milano ITALY OUTLINE Definitions & background risks in epilepsy End-points Target populations
Retired Brigadier of the Croatian Army (HV), War Commander of the Surgical Team of the Croatian Ministry of Internal Affairs (MUP) Special Police 2
 Acta Chir Croat 0; 9: 9-5 Ozljede glave Running head: Head injuries Josip Husar, Israel Oserohwovo Introduction The prognosis of brain injuries is good in patients who respond to simple commands, are not
Acta Chir Croat 0; 9: 9-5 Ozljede glave Running head: Head injuries Josip Husar, Israel Oserohwovo Introduction The prognosis of brain injuries is good in patients who respond to simple commands, are not
I N individuals who have sustained antenor polar brain injury, the differentiation
 VOL. 122, No. 3 FRONTAL EPIDURAL HEMATOMA* THE ANGIOGRAPHIC DIAGNOSIS WITH A NEW FINDING By DAVID DEE, JR., M.D.,f MERLIN E. WOESNER, M.D., and ISAAC SANDERS, M.D. LOS ANGELES, CALIFORNIA I N individuals
VOL. 122, No. 3 FRONTAL EPIDURAL HEMATOMA* THE ANGIOGRAPHIC DIAGNOSIS WITH A NEW FINDING By DAVID DEE, JR., M.D.,f MERLIN E. WOESNER, M.D., and ISAAC SANDERS, M.D. LOS ANGELES, CALIFORNIA I N individuals
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
A rare complication of chronic subdural hematoma evacuation: brain stem hemorrhage: a case report
 DOI: 10.2478/romneu-2018-0057 Article A rare complication of chronic subdural hematoma evacuation: brain stem hemorrhage: a case report Ghassen Gader, Mouna Rkhami, Maher Ben Salem, Mohamed Badri, Kamel
DOI: 10.2478/romneu-2018-0057 Article A rare complication of chronic subdural hematoma evacuation: brain stem hemorrhage: a case report Ghassen Gader, Mouna Rkhami, Maher Ben Salem, Mohamed Badri, Kamel
Sample page. Radiology. Cross Coder. Essential links from CPT codes to ICD-10-CM and HCPCS
 Cross Coder 2018 Radiology Essential links from CPT codes to ICD-10-CM and HCPCS POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com. Contents Introduction...
Cross Coder 2018 Radiology Essential links from CPT codes to ICD-10-CM and HCPCS POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com. Contents Introduction...
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
The Rorschach Test in Clinical Diagnosis
 The Rorschach Test in Clinical Diagnosis Sol L. Garfield University of Connecticut Originally published in JCLP, 3, 375 381 (1947). 2000 John Wiley & Sons, Inc. J Clin Psychol 56: 387 393, 2000. Introduction
The Rorschach Test in Clinical Diagnosis Sol L. Garfield University of Connecticut Originally published in JCLP, 3, 375 381 (1947). 2000 John Wiley & Sons, Inc. J Clin Psychol 56: 387 393, 2000. Introduction
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Anton-Babinski syndrome as a rare complication of chronic bilateral subdural hematomas
 DOI: 10.2478/romneu-2018-0050 Article Anton-Babinski syndrome as a rare complication of chronic bilateral subdural hematomas D. Adam, D. Iftimie, Cristiana Moisescu, Gina Burduşa ROMANIA Romanian Neurosurgery
DOI: 10.2478/romneu-2018-0050 Article Anton-Babinski syndrome as a rare complication of chronic bilateral subdural hematomas D. Adam, D. Iftimie, Cristiana Moisescu, Gina Burduşa ROMANIA Romanian Neurosurgery
2/20/2019 BRAIN DISSECTION CODING AND DOCUMENTATION OBJECTIVES INTRODUCTION
 BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Emergency Department Stroke Registry Indicator Specifications 2018 Report Year (07/01/2017 to 06/30/2018 Discharge Dates)
 2018 Report Year (07/01/2017 to 06/30/2018 Discharge Dates) Summary of Changes I62.9 added to hemorrhagic stroke ICD-10-CM diagnosis code list (table 3) Measure Description Methodology Rationale Measurement
2018 Report Year (07/01/2017 to 06/30/2018 Discharge Dates) Summary of Changes I62.9 added to hemorrhagic stroke ICD-10-CM diagnosis code list (table 3) Measure Description Methodology Rationale Measurement
ASSOCIATED INJURIES IN TRAUMATIC PARAPLEGIA AND TETRAPLEGIA. Department of Surgical Neurology, Western General Hospital, Edinburgh, Scotland
 PAPERS READ AT THE 1967 SCIENTIFIC MEETING 215 However, in order to diminish her spasticity she continued at her home treatment of mobilisation by a physiotherapist. During one of the treatments, the right
PAPERS READ AT THE 1967 SCIENTIFIC MEETING 215 However, in order to diminish her spasticity she continued at her home treatment of mobilisation by a physiotherapist. During one of the treatments, the right
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
T HIS study is an attempt to aggregate the etiological factors affecting eye
 THE DIAGNOSTIC SIGNIFICANCE OF RESTRICTED OCULAR MOTILITY IN CHILDREN ROBERT G. MURRAY, M.D. Division of Ophthalmology, Department of Surgery, University of North Carolina School of Medicine, Chapel Hill,
THE DIAGNOSTIC SIGNIFICANCE OF RESTRICTED OCULAR MOTILITY IN CHILDREN ROBERT G. MURRAY, M.D. Division of Ophthalmology, Department of Surgery, University of North Carolina School of Medicine, Chapel Hill,
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
recommendations of the Royal College of
 Archives of Emergency Medicine, 1993, 10, 138-144 Skull X-ray after head injury: the recommendations of the Royal College of Surgeons Working Party Report in practice R. E. MACLAREN, H. I. GHOORAHOO &
Archives of Emergency Medicine, 1993, 10, 138-144 Skull X-ray after head injury: the recommendations of the Royal College of Surgeons Working Party Report in practice R. E. MACLAREN, H. I. GHOORAHOO &
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
CHEAT SHEETS ARE THEY REALLY SAVING YOU ANYTHING? Preparing for the Transition to ICD-10
 CHEAT SHEETS ARE THEY REALLY SAVING YOU ANYTHING? Preparing for the Transition to ICD-10 The Use of Cheat Sheets Do not use cheat sheets!! Where s my cheat sheet? What does it look like? Turning a blind
CHEAT SHEETS ARE THEY REALLY SAVING YOU ANYTHING? Preparing for the Transition to ICD-10 The Use of Cheat Sheets Do not use cheat sheets!! Where s my cheat sheet? What does it look like? Turning a blind
Radiology Corner. Keyhole Fracture of the Skull
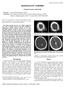 Radiology Corner Keyhole Fracture of the Skull Guarantor: 2LT Aaron M. Jackson, USA 1 Contributors: 2LT Aaron M. Jackson, USA 1 ; 2nd LT. Brett K. Searcey, USAF 1 ; James G. Smirniotopoulos, M.D. 1 ; Col
Radiology Corner Keyhole Fracture of the Skull Guarantor: 2LT Aaron M. Jackson, USA 1 Contributors: 2LT Aaron M. Jackson, USA 1 ; 2nd LT. Brett K. Searcey, USAF 1 ; James G. Smirniotopoulos, M.D. 1 ; Col
Functional Neuroanatomy and Traumatic Brain Injury The Frontal Lobes
 Functional Neuroanatomy and Traumatic Brain Injury The Frontal Lobes Jessica Matthes, Ph.D., ABN Barrow TBI Symposium March 23, 2019 jessica.matthes@dignityhealth.org Outline TBI Mechanisms of Injury Types
Functional Neuroanatomy and Traumatic Brain Injury The Frontal Lobes Jessica Matthes, Ph.D., ABN Barrow TBI Symposium March 23, 2019 jessica.matthes@dignityhealth.org Outline TBI Mechanisms of Injury Types
Head Trauma Inservice (October)
 John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
John Tramell - Head Trauma Inservice, October 2005.doc Page 1 Head Trauma Inservice (October) Head trauma is the leading cause of death in trauma patients. Having a basic understanding of the anatomy and
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
USE OF NEAR INFRARED SPECTROSCOPY TO IDENTIFY TRAUMATIC INTRACRANIAL HEMATOMAS
 JOURNAL OF BIOMEDICAL OPTICS 2(1), 31 41 (JANUARY 1997) USE OF NEAR INFRARED SPECTROSCOPY TO IDENTIFY TRAUMATIC INTRACRANIAL HEMATOMAS Claudia S. Robertson, Shankar P. Gopinath, and Britton Chance* Baylor
JOURNAL OF BIOMEDICAL OPTICS 2(1), 31 41 (JANUARY 1997) USE OF NEAR INFRARED SPECTROSCOPY TO IDENTIFY TRAUMATIC INTRACRANIAL HEMATOMAS Claudia S. Robertson, Shankar P. Gopinath, and Britton Chance* Baylor
INJURY / DISEASE RELATED EVENTS
 InjType = Type of injury InjCause = Cause of injury InjPlace = Place of injury InjIntent = Intent of injury 1. CDE Variable InjType = Type of injury InjCause = Cause of injury InjPlace = Place of injury
InjType = Type of injury InjCause = Cause of injury InjPlace = Place of injury InjIntent = Intent of injury 1. CDE Variable InjType = Type of injury InjCause = Cause of injury InjPlace = Place of injury
T HE PREVENTION and control of infection in penetrating head wounds
 OBSERVATIONS ON INFECTION IN PENETRATING WOUNDS OF THE HEAD MAJOR STUART N. ROWE, M.C., A.U.S., AND MAJOR OSCAR A. TURNER, M.C., A.U.S. (Received for publication April 19, 1945) T HE PREVENTION and control
OBSERVATIONS ON INFECTION IN PENETRATING WOUNDS OF THE HEAD MAJOR STUART N. ROWE, M.C., A.U.S., AND MAJOR OSCAR A. TURNER, M.C., A.U.S. (Received for publication April 19, 1945) T HE PREVENTION and control
BRAIN ABSCESS: ASPIRATION, DRAINAGE, OR EXCISION? BY 0. V. JOOMA,* J. B. PENNYBACKER, and G. K. TUTTON
 J. NeuroL Neurosurg. Psychiat., 1951, 14, 308. BRAIN ABSCESS: ASPIRATION, DRAINAGE, OR EXCISION? BY 0. V. JOOMA,* J. B. PENNYBACKER, and G. K. TUTTON From the Nuffield Department of Surgery, RadcliiOe
J. NeuroL Neurosurg. Psychiat., 1951, 14, 308. BRAIN ABSCESS: ASPIRATION, DRAINAGE, OR EXCISION? BY 0. V. JOOMA,* J. B. PENNYBACKER, and G. K. TUTTON From the Nuffield Department of Surgery, RadcliiOe
Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D.
 J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
J Neurosurg 72:224-230, 1990 Effect of clot removal on cerebral vasospasm TETSUJI INAGAWA, M.D., MITSUO YAMAMOTO, M.D., AND KAZUKO KAMIYA, M.D. Department of Neurosurgery, Shimane Prefectural Central Hospital,
1 MS Lesions in T2-Weighted Images
 1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
1 MS Lesions in T2-Weighted Images M.A. Sahraian, E.-W. Radue 1.1 Introduction Multiple hyperintense lesions on T2- and PDweighted sequences are the characteristic magnetic resonance imaging (MRI) appearance
Missile Injuries of the Anterior Skull Base
 ORIGINAL ARTICLE Missile Injuries of the Anterior Skull Base Harjinder Singh Bhatoe, M.S., M.Ch. 1 ABSTRACT Missile injuries of the anterior skull base usually occur during war or warlike situations. These
ORIGINAL ARTICLE Missile Injuries of the Anterior Skull Base Harjinder Singh Bhatoe, M.S., M.Ch. 1 ABSTRACT Missile injuries of the anterior skull base usually occur during war or warlike situations. These
Primary Repair of Compound Skull Fractures by Replacement of Bone Fragments*
 1. Neurosurg. / Volume 30 / lune, 1969 Primary Repair of Compound Skull Fractures by Replacement of Bone Fragments* FRED C. KRISS, M.D., JAMES A. TAKEN, M.D., AND EDGAR A. KAHN, M.D. Department o] Surgery,
1. Neurosurg. / Volume 30 / lune, 1969 Primary Repair of Compound Skull Fractures by Replacement of Bone Fragments* FRED C. KRISS, M.D., JAMES A. TAKEN, M.D., AND EDGAR A. KAHN, M.D. Department o] Surgery,
BATLS Battlefield Advanced Trauma Life Support
 J R Army Med Corps 2002; 148: 151-158 BATLS Battlefield Advanced Trauma Life Support CHAPTER 8 HEAD INJURIES Aim 0801. On successfully completing this topic you will be able to: Discuss general management
J R Army Med Corps 2002; 148: 151-158 BATLS Battlefield Advanced Trauma Life Support CHAPTER 8 HEAD INJURIES Aim 0801. On successfully completing this topic you will be able to: Discuss general management
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
APPENDIX D HISTORICAL DATA. Section I. ARMY MEDICAL DEPARTMENT EXPERIENCE FACTORS
 APPENDIX D HISTORICAL DATA Section I. ARMY MEDICAL DEPARTMENT EXPERIENCE FACTORS D-1. Table D-1 depicts the total AMEDD centage distribution of total casualties within percentages by type of casualties
APPENDIX D HISTORICAL DATA Section I. ARMY MEDICAL DEPARTMENT EXPERIENCE FACTORS D-1. Table D-1 depicts the total AMEDD centage distribution of total casualties within percentages by type of casualties
3.02 Understand the functions and disorders of the nervous system Understand the functions and disorders of the nervous system
 3.02 Understand the functions and disorders of the nervous system 1 3.02 Essential Questions What are the functions of the nervous system? What are some disorders of the nervous system? How are nervous
3.02 Understand the functions and disorders of the nervous system 1 3.02 Essential Questions What are the functions of the nervous system? What are some disorders of the nervous system? How are nervous
Louisiana State University Health Sciences Center
 Louisiana State University Health Sciences Center Department of Neurosurgery Student Clerkship Guide 2017 2018 Introduction Welcome to LSUHSC New Orleans neurosurgery rotation. Our department is dedicated
Louisiana State University Health Sciences Center Department of Neurosurgery Student Clerkship Guide 2017 2018 Introduction Welcome to LSUHSC New Orleans neurosurgery rotation. Our department is dedicated
Learning Objectives.
 Emilie O Neill, class of 2016 Learning Objectives 1. Describe the types of deficits that occur with lesions in association areas including: prosopagnosia, neglect, aphasias, agnosia, apraxia 2. Discuss
Emilie O Neill, class of 2016 Learning Objectives 1. Describe the types of deficits that occur with lesions in association areas including: prosopagnosia, neglect, aphasias, agnosia, apraxia 2. Discuss
Only 30% to 40% of acute subdural hematoma (SDH)
 Contralateral Acute Epidural Hematoma After Decompressive Surgery of Acute Subdural Hematoma: Clinical Features and Outcome Thung-Ming Su, MD, Tsung-Han Lee, MD, Wu-Fu Chen, MD, Tao-Chen Lee, MD, and Ching-Hsiao
Contralateral Acute Epidural Hematoma After Decompressive Surgery of Acute Subdural Hematoma: Clinical Features and Outcome Thung-Ming Su, MD, Tsung-Han Lee, MD, Wu-Fu Chen, MD, Tao-Chen Lee, MD, and Ching-Hsiao
Neurotrauma. Béla Faludi Dept.. of Neurology University of PécsP
 Neurotrauma Béla Faludi Dept.. of Neurology University of PécsP Emergency!!! Why here? Opened cranial injury visible: neurosurgery Closed injuries sometimes diagnosed by neurologist Masking situation:
Neurotrauma Béla Faludi Dept.. of Neurology University of PécsP Emergency!!! Why here? Opened cranial injury visible: neurosurgery Closed injuries sometimes diagnosed by neurologist Masking situation:
T HE primary goal of therapy in fractures
 Treatment of Basal Skull Fractures With and Without Cerebrospinal Fluid Fistulae B. ~TATSON BRAWLEY, M.D.,* AND WILLIAM A. KELLY, M.D. Department of Neurological Surgery, University of Washington School
Treatment of Basal Skull Fractures With and Without Cerebrospinal Fluid Fistulae B. ~TATSON BRAWLEY, M.D.,* AND WILLIAM A. KELLY, M.D. Department of Neurological Surgery, University of Washington School
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN
 Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
P1: OTA/XYZ P2: ABC c01 BLBK231-Ginsberg December 23, :43 Printer Name: Yet to Come. Part 1. The Neurological Approach COPYRIGHTED MATERIAL
 Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
Part 1 The Neurological Approach COPYRIGHTED MATERIAL 1 2 Chapter 1 Neurological history-taking The diagnosis and management of diseases of the nervous system have been revolutionized in recent years by
Moath Darweesh. Zaid Emad. Anas Abu -Humaidan
 3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
INDIANA HEALTH COVERAGE PROGRAMS
 INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
INDIANA HEALTH COVERAGE PROGRAMS PROVIDER CODE TABLES Note: Due to possible changes in Indiana Health Coverage Programs (IHCP) policy or national coding updates, inclusion of a code on the code tables
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES
 PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
PROPOSAL FOR MULTI-INSTITUTIONAL IMPLEMENTATION OF THE BRAIN INJURY GUIDELINES INTRODUCTION: Traumatic Brain Injury (TBI) is an important clinical entity in acute care surgery without well-defined guidelines
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Head Injury: Classification Most Severe to Least Severe
 Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Contributors T A B L E O F C O N T E N T S
 JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Emergency Life-Saving Cranial Procedures by Non-Neurosurgeons in Deployed Setting (CPG ID:68) This CPG applies to military non-neurosurgeons
JOINT TRAUMA SYS TEM CLINICAL PRACTIC E GUIDELINE (JTS CPG ) Emergency Life-Saving Cranial Procedures by Non-Neurosurgeons in Deployed Setting (CPG ID:68) This CPG applies to military non-neurosurgeons
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
External guide for safe orthogonal approach
 External guide for safe orthogonal approach Poster No.: C-0768 Congress: ECR 2017 Type: Scientific Exhibit Authors: M. SEOL, J. CHOI, H. KIM ; Jeonju, Jeonrabukdo/KR, Jeonju/ KR Keywords: Ischaemia / Infarction,
External guide for safe orthogonal approach Poster No.: C-0768 Congress: ECR 2017 Type: Scientific Exhibit Authors: M. SEOL, J. CHOI, H. KIM ; Jeonju, Jeonrabukdo/KR, Jeonju/ KR Keywords: Ischaemia / Infarction,
Atypical Gunshot Injury to the Ear: A Case Report
 International Journal of Otolaryngology and Head & Neck Surgery, 2015, 4, 73-76 Published Online March 2015 in SciRes. http://www.scirp.org/journal/ijohns http://dx.doi.org/10.4236/ijohns.2015.42013 Atypical
International Journal of Otolaryngology and Head & Neck Surgery, 2015, 4, 73-76 Published Online March 2015 in SciRes. http://www.scirp.org/journal/ijohns http://dx.doi.org/10.4236/ijohns.2015.42013 Atypical
Andrzej Żyluk 1, Agnieszka Mazur 1, Bernard Piotuch 1, Krzysztof Safranow 2
 POLSKI PRZEGLĄD CHIRURGICZNY 2013, 85, 12, 699 705 10.2478/pjs-2013-0107 Analysis of the reliability of clinical examination in predicting traumatic cerebral lesions and skull fractures in patients with
POLSKI PRZEGLĄD CHIRURGICZNY 2013, 85, 12, 699 705 10.2478/pjs-2013-0107 Analysis of the reliability of clinical examination in predicting traumatic cerebral lesions and skull fractures in patients with
