Missile Injuries of the Anterior Skull Base
|
|
|
- Annabella Amie Townsend
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Missile Injuries of the Anterior Skull Base Harjinder Singh Bhatoe, M.S., M.Ch. 1 ABSTRACT Missile injuries of the anterior skull base usually occur during war or warlike situations. These injuries may be isolated or associated with multiple traumatic injuries. We report 23 such cases managed during military conflicts and peacekeeping operations. All were adult males. Four of these patients sustained bullet injuries; the rest were injured from shrapnel. Eighteen patients had injury to the visual apparatus with permanent blindness. Proptosis was seen in 16, cerebrospinal fluid (CSF) leak from the wound in seven, and CSF orbitorrhea in three patients. Sixteen had irreparable injury to the eye necessitating evisceration/ enucleation, and two had retrobulbar optic nerve injury. Three patients were comatose [Glasgow Coma Scale (GCS) 3/15], and 14 had altered sensorium. Six patients were fully conscious. All were investigated by computed tomography (CT), which revealed injury to the eyeball and skull base, orbital fracture, frontal hematoma, contusion, and pneumocephalus. Seventeen patients underwent emergency surgery, and six patients were initially managed conservatively. Neurosurgical management consisted of making bifrontal flaps, craniotomy/ craniectomy, debridement, and repair of the base with fascia lata. Reconstruction of the orbital rim was required in three cases. All were managed postoperatively with cerebral decongestants and antibiotics in antimeningitic dosages. There was one death in the postoperative period; outcome was good in 16 and moderate in four patients. Twelve patients had retained intracranial splinters; three of these developed recurrent suppurative meningitis. Of the six patients initially managed conservatively, three were subsequently operated for CSF rhinorrhea. Gross communition, dural loss, and injury to the frontal scalp often preclude the use of pericranial repair of the skull base. Fascia lata is extremely useful for reconstruction and repair. Anterior cranial fossa injury probably carries a better prognosis; however, there is increased risk of suppurative complications due to breach of air-filled sinuses by the missile and contamination of the intradural compartment, as compared with supratentorial vault injuries not involving the orbit or paranasal sinuses. Three patients who underwent no operative procedure and remain asymptomatic are under follow-up. Skull Base, volume 14, number 1, Address for correspondence and reprint requests: Harjinder Singh Bhatoe, M.S., M.Ch., Department of Neurosurgery, Army Hospital (R & R), Delhi Cantt , India. hsbhatoe@indiatimes.com. 1 Department of Neurosurgery, Army Hospital (R & R), Delhi, India. Copyright # 2004 by Thieme Medical Publishers, Inc., 333 Seventh Avenue, New York, NY 10001, USA. Tel: +1(212) ,p;2004,14,01,001,008,ftx,en;sbs00368x. 1
2 2 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 14, NUMBER KEYWORDS: Brain abscess, gunshot wound, head injury, meningitis, missile injury, orbitocranial injury Missile injuries of the anterior skull base are an important subgroup of craniocerebral missile injuries. The missile traverses the facio-orbital planes before penetrating the cranium through the anterior skull base. Less commonly, the missile traverses the frontobasal region and exits through the maxillofacial region. In either situation, cerebrospinal fluid (CSF) spaces communicate with potentially infected air-filled mucosa-lined spaces and patients are prone to infection. Although CMIs are well documented, especially in the military medical literature, anterior skull base injuries caused by missiles are seldom reported as a distinct subgroup. 1 We present our experiences with 23 such patients injured during low-intensity military conflicts and peacekeeping operations. CLINICAL MATERIAL AND METHODS Between 1990 and 2002, 157 patients were treated for missile injuries of the brain in three different service hospitals. These injuries were sustained by service personnel during antimilitancy/ peacekeeping/low-intensity military operations undertaken by security forces. Twenty-three (15.4%) sustained injury to the anterior skull base. The injuring missiles were shrapnel in 19 cases (five patients were injured by multiple fragments) and bullets in four cases. The sources of shrapnel were grenades, rockets, and improvised explosive devices. Three patients were injured by 7.62 mm bullets fired from AK-47 rifles, and one patient was injured by a 9 mm bullet fired from carbine(sten). Twelve patients reached a medical unit within 1 hour of injury, and the rest reached medical care within 2 to 6 hours. Until the patients were evacuated to a neurosurgical center (which was possible 6 to 48 hours after injury), they were attended by general surgeons. Assessment Immediately upon arrival in the medical unit, patients airway, breathing, and hemodynamic status was assessed (Table 1). The airway was cleared and oxygenation and hemodynamic stabilization were achieved while the injuries were being assessed. None of these patients had significant thoracic, abdominal, or long bone injuries. However, seven required intubation or tracheostomy due to orofacial swelling. External wounds were small puncture wounds with slight bleeding, gross facial swelling, proptosis, orbitorrhea, and fractures of the maxilla and mandible. Eyeball injuries were managed by an ophthalmic surgeon by evisceration or enucleation. All patients were evaluated with plain radiography of the skull taken in anteroposterior, lateral, and Towne s views (Table 2). Noncontrast computed tomography (CT) was performed in all patients. One patient also underwent carotid angiography. CT showed cerebral contusion, hematoma, missile track, retained intracranial missile, and pneumocephalus besides showing eyeball injury (Figs. 1 5). Neurosurgical Management Seventeen patients underwent emergency neurosurgical procedures for their missile wound. The anterior cranial fossa was exposed through a bicoronal scalp flap and bifrontal craniotomy. The pericranium was preserved so it could be used as a separate Table 1 Initial Glasgow Coma Scale Scores in 23 Patients with Missile Injuries GCS Score No. Patients (%) (65.2%) (21.7%) less than 8 3 (13.1%)
3 MISSILE INJURIES OF THE ANTERIOR SKULL BASE/BHATOE 3 Table 2 Entry Site and Trajectory of Missiles in 23 Patients Entry Site and Trajectory No. Patients Orbitocranial 16 (69.5%) Transethmoidal 3 Maxilloorbitocranial 1 Submandibulofaciocranial 1 Craniofaciosubmandibular 1 Concussive wave 1 flap. Dural tears were defined and margins were retracted by stay sutures. Only the contused brain was debrided and hemostasis was achieved. Metallic splinters were retrieved only if they were visible during debridement. The cranial base was covered with pericranium/ temporalis fascia/ fascia lata after the ethmoid fracture was plugged with bone wax and mashed muscle. Convexity dura was closed watertight. The orbital rim was reconstructed in three cases. No biological adhesives were used in any patient. Postoperatively, all patients were given cerebral decongestants. Antibiotics were administered in antimeningitic dosages for 3 weeks. Prophylactic anticonvulsants (phenytoin) were used in all patients. The patient with the blast injury was treated conservatively for 8 weeks, and CSF rhinorrhea was detected. He underwent evaluation by magnetic Figure 2 Computed tomographic scan shows an orbitocranial hemorrhagic missile track and subarachnoid and intraventricular hemorrhage. resonance imaging (MRI) to locate the site of the CSF leak, which was related to a fracture of the frontal sinus. He underwent transcranial repair of the skull base. Two patients who had only puncture wounds were initially managed conservatively. They underwent evaluation by Iohexol cisternography for CSF rhinorrhea 4 weeks after the injury (Fig. 6) and then underwent transcranial repair through a bifrontal approach. Of the operated patients, three developed postmeningitic hydrocephalus, which required CSF shunting. Postoperatively, there was one death: a soldier who had a Glasgow Coma Scale (GCS) score of 3 on arrival. Two patients with initial GCS scores of 3 and 6, respectively, were severely disabled, and three with initial GCS scores of 10 were moderately disabled. Sixteen patients had good outcomes. No patients developed seizures. No retained intracranial missile has migrated. RESULTS Figure 1 Lateral skull radiograph shows an intracranial splinter, pneumocephalus, and pneumoventriculogram. Postoperatively, one patient whose GCS score was less than 8 with multilobar injury and intraventricular hemorrhage died. Thirteen patients (56.6%)
4 4 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 14, NUMBER Figure 3 Computed tomographic scan shows a tangential injury to the anterior skull base and subarachnoid hemorrhage. recovered well after surgery and were discharged 4 to 6 weeks after injury. Three patients with retained splinters developed meningitis. Overall, the incidence of meningitis was 13.04%. Two (8%) of these patients later developed a brain abscess and one developed hydrocephalus, but no organism was isolated on CSF culture. Meningitis was treated with antimeningitic dosages of Figure 4 Computed tomographic scan of the skull base shows metallic splinters in the right orbit and left parasellar region. Figure 5 Computed tomographic scan shows a retained intracerebral metallic splinter.
5 MISSILE INJURIES OF THE ANTERIOR SKULL BASE/BHATOE 5 retained intracranial splinter, pneumocephalus, and air ventriculogram (see Fig. 1). Iohexol cisternography showed a breach in the ethmoidal region and traction on the ipsilateral ventricle (see Fig. 6). He underwent repair of CSF rhinorrhea through a bifrontal approach. The intracranial splinter could not be retrieved. Since then he has remained asymptomatic. Case 2 Figure 6 Coronal computed tomographic cisternogram shows pneumocephalus, traction on the left ventricular horn, and metallic splinters. antibiotics (penicillin and chloromycetin, cefotaxime, ceftazidime, netromycin, amikacin). One of the patients developed his brain abscess 5 years after his initial injury and after he had suffered three bouts of meningitis. Three patients (13.04%) with hydrocephalus required ventriculoperitoneal shunting. Three patients who did not undergo surgical treatment continue to be under observation and are asymptomatic. However, two lost vision in one eye due to injury to the optic nerve or eyeball. ILLUSTRATIVE CASES Case 1 A 30-year-old soldier sustained a splinter injury to the inner canthus of the right eye in February Cranial CT showed a retained intracranial splinter with no significant cerebral injury or hemorrhage. He therefore was managed conservatively. After 3 months, he was readmitted with headache and CSF rhinorrhea. Skull radiography showed the A 45-year-old soldier sustained a right orbitocranial splinter injury in 1989 while serving with the Indian Peace Keeping Force. He had no focal motor deficit. His right eye had to be enucleated, and limited debridement of the right frontal region was performed. A metallic splinter could not be removed. CT of the brain showed the retained intraparenchymal metallic splinter (see Fig. 5). Over the next 4 years, he suffered from five bouts of pyogenic meningitis, each of which was treated with antibiotics. In 1993 he was admitted with headache and a 2-week history of hemiparesis. CT showed a thick-walled brain abscess associated with vasogenic cerebral edema and the metallic splinter adjacent to the abscess (Fig. 7). The abscess was excised together with the splinter. Pus was sterile for aerobes and anaerobes. Over the next 6 weeks he recovered from the hemiparesis. However, 6 months later, he was readmitted with headache. On this occasion CT showed hydrocephalus. A ventriculoperitoneal shunt was placed and he has remained asymptomatic. DISCUSSION The anterior skull base is the most common region of the skull base injured by a cranial missile. In an autopsy study, this region was injured in 82% of the cases. 2 Injuries in survivors are usually from a lowenergy missile and caused by trauma from direct contact through the missile trajectory. In contrast,
6 6 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 14, NUMBER the orbit or nasal cavity. Although CSF orbitorrhea occurs due to injury of the orbital roof or lateral wall, CSF rhinorrhea is caused by a fracture through the frontal sinus or cribriform plate. However, a missile trajectory through the sinuses, orbit, and skull base may cause the missile to lose its energy before it enters the brain. Hence, although these injuries cause severe maxillofacial injury related to yawing, they often cause less severe brain damage than other trajectories. Only three of the 22 surviving patients (13.63%) had an initial GCS score less than 8, and 14 (66.66%) had a GCS score of 12 or higher. Figure 7 Computed tomographic scan of the patient in Figure 5 obtained 4 years later shows a cerebral abscess and metallic splinter adherent to the abscess wall. missile injuries involving the middle and posterior cranial fossae are from high-energy missiles, and the victims seldom survive. The extent of damage in gunshot wounds is proportional to the amount of kinetic energy of the missile dissipated in the wound. Energy deposited along the missile trajectory shatters the bone and lacerates soft tissues. 3 A missile traversing the face, orbits, PNS, and skull base creates an open, persistent communication between air-filled, mucussecreting cavities and subarachnoid spaces. 4 Skull base fractures involving the frontoethmoidal sinuses may occur without damage to brain due to a blast effect. Such patients may later develop CSF rhinorrhea. High-energy bullets can shatter the skull base without traversing it. 2 Infection is a real threat. The primary threat of infection is from oropharyngeal commensals (staphylococcus) or gram-positive or gram-negative rods contaminating the wound during entry of the missile. 5 Injury to the ocular apparatus causes proptosis and complete permanent loss of vision that often requires enucleation. 1 Maxillofacial and orofacial injury can cause respiratory obstruction and hypoxemia, necessitating immediate intubation or tracheostomy. An external CSF leak can occur through Diagnostic Imaging The initial imaging should be by plain radiography of the skull, which may show retained metallic splinters, pneumocephalus, or, rarely, an air ventriculogram. CT is mandatory for all individuals with a gunshot wound of the brain. Besides defining the extent of brain damage, CT is vital for treatment planning and prognostication 6,7 and three-dimensional imaging with CT may be required to assess the pattern of the fracture and reconstructive procedures. Sequelae of gunshot wounds to the brain may require CT cisternography or MRI for CSF rhinorrhea and carotid angiography to evaluate suspected traumatic aneurysms. 8 Multilobar injuries (especially bilateral), a transventricular trajectory, obliteration of the basal cisterns, and subarachnoid hemorrhage are poor prognostic indicators. When they are combined with the patient s GCS score a fairly accurate prognosis can be reached. 7,9 11 Immediate Surgical Management Most patients with anterior skull base missile injuries require surgical management. These patients are likely to have open wounds associated with extrusion of brain matter and CSF, with or without signs of an expanding intracranial mass lesion. The sensorium may be altered to various degrees and
7 MISSILE INJURIES OF THE ANTERIOR SKULL BASE/BHATOE 7 focal neurological signs may be present. The aims of surgery in these patients are to evacuate the hematoma, to debride the wound, to achieve hemostasis, and to provide tension-free yet watertight dural closure and repair the skull base while sealing the ethmoidal and frontal air sinuses. Gunshot wounds to the brain require adequate exposure. For injuries involving the anterior skull base, a bicoronal scalp flap that provides access to a large flap of pericranium and temporalis fascia is desirable. A bifrontal craniotomy that extends to the skull base is performed preserving as much bone as possible. The orbital rim is wired or reconstructed. The frontal sinuses are sealed and exteriorized. Dura is usually lost, necessitating the use of dural substitutes. Autologous tissues are preferred because a synthetic dural substitute can be undesirable in the presence of contamination. For debridement, a less aggressive, brain-conserving approach is advocated. 12 After debridement and hemostasis, CSF leakage from the skull base is addressed. Bone defects are sealed with macerated muscle or bone dust. The anterior skull base is covered with a pericranial fascia lata flap and the dura is closed watertight. A routine closure is performed. Antibiotics are continued postoperatively in addition to cerebral decongestants. Continuous lumbar drainage can be used for 48 to 72 hours to prevent CSF leakage from the wound. Patients with ocular and maxillofacial injuries require definitive surgical management. apparent within a few days to weeks of injury. It can be evaluated with CT cisternography to pinpoint the site of CSF leakage if MRI is precluded by the presence of retained intracranial ferromagnetic splinters. In such patients the anterior skull base is repaired through a bifrontal craniotomy. Retained Intracranial Fragments With the adoption of a less aggressive approach to treatment, it is likely that several patients will have retained intracranial fragments. The risk of suppurative sequelae is high with patients with a missile trajectory though the skull base, particularly when the air sinuses and the orbit have been breached. 12,14,15 These patients may have recurrent meningitis, a cerebral abscess, and hydrocephalus. Prognostic Factors Prognostic factors include the patient s initial postresuscitation GCS score, subarachnoid hemorrhage, multilobar trauma, transventricular wounds, and the extent of the wound. 16 The latter is a function of the velocity of the missile. High-velocity missiles (i.e., rifle bullet wounds) inflict a more severe injury than the low-velocity missiles (e.g., pieces of shrapnel). 2 Delayed Surgical Management Patients with only a puncture wound, minimal contamination, no neurological deficits, and no gross damage as seen on CT (minimal contusion or hemorrhage and no contralateral shift of midline structures) can be managed conservatively and observed over the ensuing months. 12,13 The development of complications like meningitis or brain abscess is treated with appropriate antibiotics. Postmeningitic hydrocephalus may require ventriculoperitoneal shunting. CSF rhinorrhea may become CONCLUSION The anterior skull base is a region of the skull base commonly fractured in cranial missile injuries, and patients with missile injuries of the anterior skull base form a distinct subset of patients with missile injuries of the brain. Missiles traverse the air-filled potentially infected spaces and the visual apparatus may be injured and the upper respiratory passages may be obstructed. Immediate attention to the airway can salvage many of these patients. Management requires a team approach that includes a
8 8 SKULL BASE: AN INTERDISCIPLINARY APPROACH/VOLUME 14, NUMBER maxillofacial surgeon, an ophthalmologist, and a reconstructive surgeon. Evaluation by CT is mandatory. Surgical management is aimed at providing a watertight dura, reduction of intracranial pressure, and control of infection. Outcomes are favorable in survivors. Patients require long-term follow-up to detect sequelae such as meningitis, hydrocephalus, and CSF rhinorrhea. REFERENCES 1. Jankovic S, Buca A, Busic Z, Zuljan I, Primorac D. Orbitocranial injuries: report of 14 cases. Mil Med 1998;163: Betz P, Stiefel D, Hausmann R, Eisenmenger W. Fractures at the base of the skull in gunshots to the head. Forensic Sci Int 1997;86: Swan KG, Swan RC. Principles of ballistics applicable to the treatment of gunshot wounds. Surg Clin North Am 1991;71: Dillon JD Jr, Meirowsky AM. Facio-orbito-cranial missile wounds. Surg Neurol 1975;4: Aarabi B, Taghipour M, Alibii E, Kamgarpour A. Central nervous system infections after military missile wounds. Neurosurgery 1998;42: Shoung HM, Sichez JP, Pertuiset B. The early prognosis of craniocerebral gunshot wounds in civilian practice as an aid to the choice of treatment: a series of 56 cases studied by computed tomography. Acta Neurochir (Wien) 1985; 74: Kaufman HH, Makela ME, Lee KF, et al. Gunshot wounds to the head: a perspective. Neurosurgery 1986;18: Cooper PR. Gunshot wounds of the brain. In: Cooper PR, ed. Head Injury. 3rd ed. Baltimore: Williams & Wilkins; 1993: Levy M. Outcome prediction following penetrating craniocerebral injury in a civilian population: aggressive surgical management in patients with admission Glasgow Coma Scale scores of 6 to 15 Neurosurg Focus 2000; 8:Article Grahm T, Williams FC, Harrington T, et al. Civilian gunshot wounds to the head: a prospective study. Neurosurgery 1990;27: Kennedy F, Gonzalez P, Dang C, et al. The Glasgow Coma Scale and prognosis in gunshot wounds of the brain. J Trauma 1993;35: Brandvold B, Levi L, Feinsod M, et al. Penetrating craniocerebral injuries in the Israeli involvement in the Lebanese conflict, : analysis of a less aggressive surgical approach. J Neurosurg 1990;72: Bhatoe HS, Garg A, Kapoor S, et al. Experiences in the management of splinter injuries of brain in low intensity military conflicts. Asian Arch Crit Care Med 1997;46: Aarabi B. Comparative study of bacteriological contamination between primary and secondary exploration of missile head wounds. Neurosurgery 1987;20: Bhatoe HS. Retained intracranial splinters: a follow-up study in survivors of low intensity military conflicts. Neurol India 2001;49: Splavski B, Vrankovic D, Saric G, et al. Early surgery and other indicators influencing the outcome of war missile skull base injuries. Surg Neurol 1998;50: Commentary The authors have applied the generally accepted principles of skull base surgery to the treatment of missile injuries involving the anterior skull base. We agree with the policy of not removing all intracranial bone and missile fragments if the procedure would carry significant risk to normally functioning brain. They correctly point out that missile injuries of the anterior cranial fossa have better outcomes than injuries further posterior in the skull base. The authors have treated a complicated group of skull base injuries and have achieved quite satisfactory results. Albert L. Rhoton Jr., M.D. 1 Skull Base, volume 14, number 1, Department of Neurological Surgery, College of Medicine, University of Florida, Gainesville, Florida. Copyright # 2004 by Thieme Medical Publishers, Inc., 333 Seventh Avenue, New York, NY 10001, USA. Tel: +1(212) ,p;2004,14,01,008,008,ftx,en;sbs00369x.
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
Management of Cerebrospinal Fluid Leaks
 Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
Part 2: Prognosis in Penetrating Brain Injury
 Part 2: Prognosis in Penetrating Brain Injury J Trauma. 2001;51:S44 S86. INTRODUCTION AND METHODOLOGY Part 2 of this document presents early clinical indicators that may be prognostic of outcome among
Part 2: Prognosis in Penetrating Brain Injury J Trauma. 2001;51:S44 S86. INTRODUCTION AND METHODOLOGY Part 2 of this document presents early clinical indicators that may be prognostic of outcome among
T HE primary goal of therapy in fractures
 Treatment of Basal Skull Fractures With and Without Cerebrospinal Fluid Fistulae B. ~TATSON BRAWLEY, M.D.,* AND WILLIAM A. KELLY, M.D. Department of Neurological Surgery, University of Washington School
Treatment of Basal Skull Fractures With and Without Cerebrospinal Fluid Fistulae B. ~TATSON BRAWLEY, M.D.,* AND WILLIAM A. KELLY, M.D. Department of Neurological Surgery, University of Washington School
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
CME Article Clinics in diagnostic imaging (119)
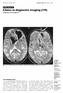 Medical Education Singapore Med.12007,48(11):1055 CME Article Clinics in diagnostic imaging (119) Venkatesh S K, Bhargava V la Ib re, N!47 Fig. I Axial T2 -weighted images of the brain taken at the level
Medical Education Singapore Med.12007,48(11):1055 CME Article Clinics in diagnostic imaging (119) Venkatesh S K, Bhargava V la Ib re, N!47 Fig. I Axial T2 -weighted images of the brain taken at the level
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
injuries Visual disturbances after missile head Symonds, 1945; Calvert, 1947; Jepson and Whitty, 1947). At University College Hospital,
 Brit. J. Ophthal. (I 972) 56, 905 Visual disturbances after missile head injuries ADELOLA ADELOYE Neurosurgery Unit, University of Ibadan, Nigeria, West Africa Disturbances of vision after head injury,
Brit. J. Ophthal. (I 972) 56, 905 Visual disturbances after missile head injuries ADELOLA ADELOYE Neurosurgery Unit, University of Ibadan, Nigeria, West Africa Disturbances of vision after head injury,
T HIS presentation is a study of a consecutive series of 316 penetrating
 INTRACRANIAL HEMATOMAS ASSOCIATED WITH PENETRATING WOUNDS OF THE BRAIN* JOSEPH C. BARNETT, M.D.,t AND ARNOLD M. MEIROWSKY, M.D.:~ (Received for publication September 29, 1954) T HIS presentation is a study
INTRACRANIAL HEMATOMAS ASSOCIATED WITH PENETRATING WOUNDS OF THE BRAIN* JOSEPH C. BARNETT, M.D.,t AND ARNOLD M. MEIROWSKY, M.D.:~ (Received for publication September 29, 1954) T HIS presentation is a study
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Endoscopic Repair of Frontal Sinus Cerebrospinal Fluid Leaks after Firearm Injuries: Report of Two Cases
 e8 Case Report THIEME Endoscopic Repair of Frontal Sinus Cerebrospinal Fluid Leaks after Firearm Injuries: Report of Two Cases Camilo Reyes 1 C. Arturo Solares 2,3 1 Department of Otolaryngology, Universidad
e8 Case Report THIEME Endoscopic Repair of Frontal Sinus Cerebrospinal Fluid Leaks after Firearm Injuries: Report of Two Cases Camilo Reyes 1 C. Arturo Solares 2,3 1 Department of Otolaryngology, Universidad
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature
 Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
PARANASAL SINUS FRACTURES
 Paranasal Sinus Fractures Chapter 23 PARANASAL SINUS FRACTURES MARK GIBBONS, MD, FACS,* and NATHAN SALINAS, MD INTRODUCTION ANATOMY DIAGNOSIS: CLINICAL AND IMAGING STUDIES MANAGEMENT ISSUES AND ALGORITHM
Paranasal Sinus Fractures Chapter 23 PARANASAL SINUS FRACTURES MARK GIBBONS, MD, FACS,* and NATHAN SALINAS, MD INTRODUCTION ANATOMY DIAGNOSIS: CLINICAL AND IMAGING STUDIES MANAGEMENT ISSUES AND ALGORITHM
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Aspiration versus Excision in Management of Intracranial Abscesses
 Med. J. Cairo Univ., Vol. 84, No. 3, December: 229-233, 2016 www.medicaljournalofcairouniversity.net Aspiration versus Excision in Management of Intracranial Abscesses AYMAN T.M. MOHAMED, M.Sc.; AHMED
Med. J. Cairo Univ., Vol. 84, No. 3, December: 229-233, 2016 www.medicaljournalofcairouniversity.net Aspiration versus Excision in Management of Intracranial Abscesses AYMAN T.M. MOHAMED, M.Sc.; AHMED
I N T~, COVRS~, of the postoperative care, at the 36th General Hospital,
 OBSERVATIONS ON EARLY TYPE OF BRAIN ABSCESS FOLLOWING PENETRATING WOUNDS OF THE BRAIN MAJOR J. E. WEBSTER, M.C., A.U.S.,* CAPTAIN R. C. SCHNEIDER, ~.C., A.U.S., A~D LT. COL. J. E. LOFSTRO1V[, M.C., A.U.S.t
OBSERVATIONS ON EARLY TYPE OF BRAIN ABSCESS FOLLOWING PENETRATING WOUNDS OF THE BRAIN MAJOR J. E. WEBSTER, M.C., A.U.S.,* CAPTAIN R. C. SCHNEIDER, ~.C., A.U.S., A~D LT. COL. J. E. LOFSTRO1V[, M.C., A.U.S.t
Open skull fractures with brain fungation: Simple principles for good outcome experience
 outcome Our experience. IAIM, 2015; 2(9): 65-69. Original Research Article Open skull fractures with brain fungation: Simple principles for good outcome Our experience M. V. Vijaya Sekhar 1, K.V. Ramprasad
outcome Our experience. IAIM, 2015; 2(9): 65-69. Original Research Article Open skull fractures with brain fungation: Simple principles for good outcome Our experience M. V. Vijaya Sekhar 1, K.V. Ramprasad
Fleece-Bound Tissue Sealing in Microvascular Decompression
 DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
PA SYLLABUS. Syllabus for students of the FACULTY OF MEDICINE No.2
 Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
TBI are twice as common in males High potential for poor outcome Deaths occur at three points in time after injury
 Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
Head Injury Any trauma to (closed vs. open) Skull Scalp Brain Traumatic brain injury (TBI) High incidence Most common causes Falls Motor vehicle accidents Other causes Firearm- related injuries Assaults
MICHAEL L. LEVY, M.D.
 Neurosurg Focus 8 (1):Article 2, 1999 Outcome prediction following penetrating craniocerebral injury in a civilian population: aggressive surgical management in patients with admission Glasgow Coma Scale
Neurosurg Focus 8 (1):Article 2, 1999 Outcome prediction following penetrating craniocerebral injury in a civilian population: aggressive surgical management in patients with admission Glasgow Coma Scale
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Penetrating Trauma in Pediatric Patients. Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017
 Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Chapter 57: Nursing Management: Acute Intracranial Problems
 Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
Thoracic spine stab injury with pneumocephalus and pneumorrhachiasis: a unique case report and review of literature
 Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Thoracic spine stab injury with pneumocephalus and pneumorrhachiasis: a unique case report and review of literature Rakesh Kumar,
Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Thoracic spine stab injury with pneumocephalus and pneumorrhachiasis: a unique case report and review of literature Rakesh Kumar,
Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D.
 J Neurosurg 48:355-359, 1978 Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D. Department of Radiology, University
J Neurosurg 48:355-359, 1978 Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D. Department of Radiology, University
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
To study the association of CSF leak in fronotbasal skull fractures classified with the Burstein s classification
 International Journal of Advances in Medicine Chhabra RS et al. Int J Adv Med. 2018 Feb;5(1):126-130 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180070
International Journal of Advances in Medicine Chhabra RS et al. Int J Adv Med. 2018 Feb;5(1):126-130 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180070
Department of Neurosurgery, The MD Anderson Cancer Center, Houston, Texas
 J Neurosurg 121:645 652, 2014 AANS, 2014 Predictors of outcome in civilians with gunshot wounds to the head upon presentation Clinical article Loyola V. Gressot, M.D., 1 Roukoz B. Chamoun, M.D., 2 Akash
J Neurosurg 121:645 652, 2014 AANS, 2014 Predictors of outcome in civilians with gunshot wounds to the head upon presentation Clinical article Loyola V. Gressot, M.D., 1 Roukoz B. Chamoun, M.D., 2 Akash
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Infection after depressed fracture of skull. Implications for management of nonmissile injuries
 Implications for management of nonmissile injuries BRYAN JENNETT, M.D., F.R.C.S., AND J. DOUGLAS MILLER, M.D., F.R.C.S. Institute o/ Neurological Sciences, and the University o/glasgow, Glasgow, Scotland
Implications for management of nonmissile injuries BRYAN JENNETT, M.D., F.R.C.S., AND J. DOUGLAS MILLER, M.D., F.R.C.S. Institute o/ Neurological Sciences, and the University o/glasgow, Glasgow, Scotland
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series
 CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Blow-in fracture of both orbital roofs caused by shear strain to the skull. Department of Neurosurgery, Kanto Teishin Hospital, Tokyo, Japan
 J Neurosurg 49:734-738, 1978 Blow-in fracture of both orbital roofs caused by shear strain to the skull Case report OSAMU SATO, M.D., HIROSHI KAMITANI, M.D., AND TAKASHI KOKUNAI, M.D. Department of Neurosurgery,
J Neurosurg 49:734-738, 1978 Blow-in fracture of both orbital roofs caused by shear strain to the skull Case report OSAMU SATO, M.D., HIROSHI KAMITANI, M.D., AND TAKASHI KOKUNAI, M.D. Department of Neurosurgery,
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
Ventricles, CSF & Meninges. Steven McLoon Department of Neuroscience University of Minnesota
 Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
T HE PREVENTION and control of infection in penetrating head wounds
 OBSERVATIONS ON INFECTION IN PENETRATING WOUNDS OF THE HEAD MAJOR STUART N. ROWE, M.C., A.U.S., AND MAJOR OSCAR A. TURNER, M.C., A.U.S. (Received for publication April 19, 1945) T HE PREVENTION and control
OBSERVATIONS ON INFECTION IN PENETRATING WOUNDS OF THE HEAD MAJOR STUART N. ROWE, M.C., A.U.S., AND MAJOR OSCAR A. TURNER, M.C., A.U.S. (Received for publication April 19, 1945) T HE PREVENTION and control
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
CSF Leaks. Abnormal communication between the subarachnoid space and the tympanomastoid space or nasal cavity. Presenting symptoms:
 CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
Original Article Management of Cranial Air Gun Pellet Injuries
 Egyptian Journal of Neurosurgery Volume 31 / No. 1 / January March 01 7-3 Original Article Management of Cranial Air Gun Pellet Injuries 1 Ashraf Shaker Zidan*, Ashraf Ahamed Zaher and 3 Adel Elbadrawy
Egyptian Journal of Neurosurgery Volume 31 / No. 1 / January March 01 7-3 Original Article Management of Cranial Air Gun Pellet Injuries 1 Ashraf Shaker Zidan*, Ashraf Ahamed Zaher and 3 Adel Elbadrawy
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Use of tissue adhesive in the surgical treatment of cerebrospinal fluid leaks. Experience with isobutyl 2-cyanoacrylate in 12 cases
 Use of tissue adhesive in the surgical treatment of cerebrospinal fluid leaks Experience with isobutyl 2-cyanoacrylate in 12 cases JOHN A. MAXWELL, M.D., AND STEPHEN I. COLDWARE, M.D. Division of Neurological
Use of tissue adhesive in the surgical treatment of cerebrospinal fluid leaks Experience with isobutyl 2-cyanoacrylate in 12 cases JOHN A. MAXWELL, M.D., AND STEPHEN I. COLDWARE, M.D. Division of Neurological
MAXILLOFACIAL TRAUMA. The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital
 MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
Transcranial resection of tumors of the paranasal sinuses and nasal cavity
 J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
J Neurosurg 71:10-15, 1989 Transcranial resection of tumors of the paranasal sinuses and nasal cavity J. BoB BLACKLOCK, M.D., RANDAL S. WEBER, M.D., YA-YEN LEE, M.D., AND HELMUTH GOEPFERT~ M.D. Section
Neurosurgery (Orthopaedic PGY-1) Goals. Objectives
 Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Neurosurgery (Orthopaedic PGY-1) Length: 1 month of PGY-1 (Orthopaedic Designated Residents) or 1 month of PGY-2, -3, or -4 year Location: The Queen's Medical Center Primary Supervisor: William Obana,
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Neurosurgical Techniques
 Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Neurosurgical Techniques EBEN ALEXANDER, JR., M.D., EDITOR Supratentorial Skull Flaps GuY L. ODOM, M.D., AND BARNES WOODHALL,!V[.D. Department of Surgery, Division of Neurosurgery, Duke University Medical
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
FRONTAL SINUS FRACTURES February 1995
 TITLE: FRONTAL SINUS FRACTURES SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds DATE: February 22, 1995 RESIDENT PHYSICIAN: Kelly D. Sweeney, M.D. FACULTY: Brian P. Driscoll, M.D. SERIES EDITOR: Francis
TITLE: FRONTAL SINUS FRACTURES SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds DATE: February 22, 1995 RESIDENT PHYSICIAN: Kelly D. Sweeney, M.D. FACULTY: Brian P. Driscoll, M.D. SERIES EDITOR: Francis
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
ISPUB.COM. GSW To The Face: "Hunting Camp" C Perry, B Phillips CASE REPORT
 ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
Evaluation of Craniocerebral Trauma Using Computed Tomography
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 57-62 Evaluation of Craniocerebral Trauma Using Computed Tomography
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 57-62 Evaluation of Craniocerebral Trauma Using Computed Tomography
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Moath Darweesh. Zaid Emad. Anas Abu -Humaidan
 3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
3 Moath Darweesh Zaid Emad Anas Abu -Humaidan Introduction: First two lectures we talked about acute and chronic meningitis, which is considered an emergency situation. If you remember, CSF examination
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488
 National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. Railway accidents injured pedal cyclist
 Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Leptomeningeal Cyst of the Orbital Roof in an Adult: Case Report and Literature Review
 CASE REPORT Leptomeningeal Cyst of the Orbital Roof in an Adult: Case Report and Literature Review Jeremy D. Meier, M.D., 1 Arthur B. Dublin, M.D., M.B.A., F.A.C.R., 2 and E. Bradley Strong, M.D. 1 ABSTRACT
CASE REPORT Leptomeningeal Cyst of the Orbital Roof in an Adult: Case Report and Literature Review Jeremy D. Meier, M.D., 1 Arthur B. Dublin, M.D., M.B.A., F.A.C.R., 2 and E. Bradley Strong, M.D. 1 ABSTRACT
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Vertex epidural hematomas caused by injury of the superior sagittal sinus
 Formosan Journal of Surgery (2012) 45, 20e24 Available online at www.sciencedirect.com journal homepage: www.e-fjs.com CASE REPORT Vertex epidural hematomas caused by injury of the superior sagittal sinus
Formosan Journal of Surgery (2012) 45, 20e24 Available online at www.sciencedirect.com journal homepage: www.e-fjs.com CASE REPORT Vertex epidural hematomas caused by injury of the superior sagittal sinus
Medical Science An International Journal
 Medical CASE REPORT Science, Vol. 20, No. 81, September 1, 2016 CASE REPORT ISSN 2321 7359 EISSN 2321 7367 Medical Science An International Journal Growing skull fracture Case report & technical aspects
Medical CASE REPORT Science, Vol. 20, No. 81, September 1, 2016 CASE REPORT ISSN 2321 7359 EISSN 2321 7367 Medical Science An International Journal Growing skull fracture Case report & technical aspects
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Trauma is the leading cause of death in the first four decades of life, with head injury being
 Correspondence to: Mr PJ Hutchinson, Academic Department of Neurosurgery, University of Cambridge, Box 167, Addenbrooke s Hospital, Cambridge CB2 2QQ, UK: p.hutch@which.net ACUTE HEAD INJURY FOR THE NEUROLOGIST
Correspondence to: Mr PJ Hutchinson, Academic Department of Neurosurgery, University of Cambridge, Box 167, Addenbrooke s Hospital, Cambridge CB2 2QQ, UK: p.hutch@which.net ACUTE HEAD INJURY FOR THE NEUROLOGIST
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
SURGICAL MANAGEMENT OF DEPRESSED CRANIAL FRACTURES
 CHAPTER 7 M. Ross Bullock, M.D., Ph.D. Virginia Commonwealth University Medical Center, Richmond, Virginia Randall Chesnut, M.D. University of Washington School of Medicine, Harborview Medical Center,
CHAPTER 7 M. Ross Bullock, M.D., Ph.D. Virginia Commonwealth University Medical Center, Richmond, Virginia Randall Chesnut, M.D. University of Washington School of Medicine, Harborview Medical Center,
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
MANAGEMENT OF CSF. Steven D. Schaefer, MD, FACS. Department of Otolaryngology New York Eye and Ear Infirmary
 MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
Subdural Empyema: A Case Report from Southern Zambia and a Review of the Literature
 CASE REPORT Subdural Empyema: A Case Report from Southern Zambia and a Review of the Literature G Musa, A Gots Department of Surgery, Livingstone Central Hospital, P. O. Box 60091, Livingstone, Zambia
CASE REPORT Subdural Empyema: A Case Report from Southern Zambia and a Review of the Literature G Musa, A Gots Department of Surgery, Livingstone Central Hospital, P. O. Box 60091, Livingstone, Zambia
Sinusitis & its complication. MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University
 Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Coding Companion for Neurosurgery/Neurology. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Neurosurgery/Neurology A comprehensive illustrated guide to coding and reimbursement 2011 Contents Getting Started with Coding Companion...i Skin...1 Repair...5 General Musculoskeletal...27
Coding Companion for Neurosurgery/Neurology A comprehensive illustrated guide to coding and reimbursement 2011 Contents Getting Started with Coding Companion...i Skin...1 Repair...5 General Musculoskeletal...27
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
Rerupture of intracranial aneurysms: a clinicoanatomic study
 J Neurosurg 67:29-33, 1987 Rerupture of intracranial aneurysms: a clinicoanatomic study ALBERT HIJDRA, M.D., MARINUS VERMEULEN, M.D., JAN VAN GIJN, M.D., AND HANS VAN CREVEL, M.D. Departments ~[ Neurology.
J Neurosurg 67:29-33, 1987 Rerupture of intracranial aneurysms: a clinicoanatomic study ALBERT HIJDRA, M.D., MARINUS VERMEULEN, M.D., JAN VAN GIJN, M.D., AND HANS VAN CREVEL, M.D. Departments ~[ Neurology.
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes
 Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
ISPUB.COM. An Orbital Cellulitis Demanding Multispeciality Management. N Ezhilvathani, Thiagarajan, T Cherian INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 An Orbital Cellulitis Demanding Multispeciality Management N Ezhilvathani, Thiagarajan, T Cherian Citation N Ezhilvathani,
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 An Orbital Cellulitis Demanding Multispeciality Management N Ezhilvathani, Thiagarajan, T Cherian Citation N Ezhilvathani,
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Atypical Gunshot Injury to the Ear: A Case Report
 International Journal of Otolaryngology and Head & Neck Surgery, 2015, 4, 73-76 Published Online March 2015 in SciRes. http://www.scirp.org/journal/ijohns http://dx.doi.org/10.4236/ijohns.2015.42013 Atypical
International Journal of Otolaryngology and Head & Neck Surgery, 2015, 4, 73-76 Published Online March 2015 in SciRes. http://www.scirp.org/journal/ijohns http://dx.doi.org/10.4236/ijohns.2015.42013 Atypical
