Tetralogy of Fallot Risk factors associated with complete repair
|
|
|
- Tabitha Matilda Fleming
- 5 years ago
- Views:
Transcription
1 British Heart Journal, 1976, 38, Tetralogy of Fallot Risk factors associated with complete repair J. P. Richardson and C. P. Clarke From the Division of Cardiac Surgery, Department of Surgery, Royal Children's Hospital, Melbourne, Australia Ninety-six consecutive total repairs of the tetralogy of Fallot are reviewed. There was an overall hospital mortality of 8&3 per cent and a total incidence of low output cardiac failure of 18-8 per cent, and this was the principal cause of death and the most important source ofpostoperative morbidity. In 49 cases there had been a previous palliative shunt procedure and there was a strikingly lower mortality and a highly significant lower morbidity in this group. Other factors which correlated in a positive fashion with increased mortality and morbidity were chronic hypoxia (as evidenced by polycythaemia), age below 5 years, severe postoperative right ventricular hypertension, and (to a lesser extent) extensive right ventricular outflow tract reconstruction. Data are presented to support the hypothesis that a palliative shunt procedure should be considered in the severely polycythaemic child with a surgically 'unfavourable' right ventricular outflow. This policy carries a low early mortality in our hands (5.4%), and is associated with a low mortality (3-9%) at subsequent repair. This compares with a mortality of 12 8 per cent for primary repair, and the incidence of low output cardiac failure is five times as high in the primary repair as compared to the previously shunted group. The congenital heart defect which is now almost universally known as the tetralogy of Fallot was first recognized as a pathological entity by Nils Stensen in In the succeeding centuries it was known to a number of medical writers but it was not until 1888, after a series of papers by Louis-Etienne Fallot, who in fact called the condition 'Cyanose Cardiaque', that the clinical and pathological features were clearly described and correlated. This author drew attention to four cardinal features of the condition in such a clear and concise fashion that the eponym, 'Fallot's tetralogy', seems to be a fitting memorial. In 1945, Blalock and Taussig first described an operation to palliate the symptoms of the condition, and the first attempt at complete repair of the lesion was made in 1954 by H. W. Scott using whole body hypothermia and circulatory arrest. The subsequent development of safe methods of cardiopulmonary bypass has allowed refinements of surgical techniques such that the operative mortality for complete repair is now about 5 to 10 per cent in Received 17 February most reported series (Malm et al., 1966; Gottsman et al., 1969; Kirklin and Karp, 1970). In an effort to try to recognize factors which correlate with the continuing hospital mortality, we have reviewed the results achieved in a consecutive series of 96 operations conducted during a 4-year period. Subjects and methods During the four-year period ending in 1974, all operations for total repair of the tetralogy of Fallot have been reviewed. The data recorded included age at operation, weight centile using hospital graphs derived from data by Tanner, Whitehouse, and Takaishi (1966), history of a previous shunt procedure, haemoglobin level in g/dl, method of outflow tract reconstruction, the ratio of right ventricular to left ventricular systolic pressure measured at the conclusion of the operation, total cardiopulmonary bypass time, blood loss in the first 6 postoperative hours expressed as ml/kg per hr, mean systolic blood pressure during the first 24 postoperative hours, urine flow during the first 24 postoperative hours expressed as ml/kg per hr,
2 and the subsequent postoperative course in hospital. The two morbidity end-points which were considered were (1) death in hospital and (2) low output cardiac failure. This latter end-point was a clinical diagnosis which was arbitrarily defined by the following features: (1) cool, cyanosed extremities; (2) systolic blood pressure less than 90 mmhg (12 kpa) for the initial 24 hours after operation; (3) urine flow less than 0'7 ml/kg -l hr-' for the whole of the 24-hour period; and/or (4) the necessity for a catecholamine infusion to overcome the clinical signs listed as 1 to 3 above Preoperative and intraoperative observations were correlated with the two morbidity end-points and, in part, with each other. The significance of observed correlations was tested by standard statistical methods (Snedecor and Cochran, 1967). Operative techniques The techniques used during the operation and perfusion were substantially the same for all cases during the period under review. Perfusions were conducted with haemodiluted primes, a bubble oxygenator, a roller pump, and the nasopharyngeal temperature was reduced to 25 C. Intracardiac manoeuvres were carried out with intermittent periods of aortic cross-clamping up to 20 minutes at any one time. The left ventricle or the left atrium was vented. The ventricular septal defect was patched with two-way stretch knitted 'dacron' material. Right ventricular outflow tract patches, when used, were generally of autogenous pericardium, and in a few cases a monocusp valve was TABLE 1 Mortality in 96 consecutive cases of total repair of Fallot's tetralogy Cases Mortality Primary repair 47 6 (12-8%) Previous shunt 49 2 (3 9%) Total 96 8 (8 3%) (0-30>P>020) Tetralogy of Fallot 927 fashioned to provide at least temporary pulmonary valve competence. Right atrial and central arterial pressures were monitored postoperatively in all patients, and left atrial pressure was monitored also on some occasions. Postoperative management was along conventional lines and catecholamine infusion was usually the first drug intervention used if a low cardiac output was diagnosed. Results Influence of prior shunt on results of complete repair The overall results in relation to hospital mortality are shown in Table 1. This shows that the overall mortality for all 96 operations was 8-3 per cent. The mortality was considerably higher in the unshunted as compared with the previously shunted group though the difference on these figures was not statistically significant. The causes of death in the 8 fatal cases are listed in Table 2. The mode of death in all 8 cases was low output cardiac failure as defined above, but in the two previously shunted patients there seemed to be a demonstrable cause for this in that unrecognized obstructive pulmonary vascular disease had supervened in one patient after a Waterston shunt and in the second case the right ventricular outflow tract obstruction had not been relieved. In the remaining 6 cases, all unshunted, there was no such discernible cause for the low output cardiac failure unless one postulates that low pulmonary flow from TABLE 2 Causes of death in 96 consecutive cases of total repair of Fallot's tetralogy Cause of death Cases Low output cardiac failure 6 (all unshunted) Obstructive pulmonary vascular 1 (previous Waterston disease shunt) Unrelieved right ventricular 1 (previous left obsttuction Blalock) Total 8 TAB L E 3 List of previous shunt operations and mortality at subsequent repair Shunt Cases Mortality Right pulmonary artery to aorta (Waterston) 18 1 (5-5%) Left pulmonary artery to aorta (Pott's) 9 0 Left subclavian artery to left pulmonary artery Baock (12-5%) l1(4.5%) Right subclavian artery to right pulmonary artery f 14, 0 f
3 928 Richardson and Clarke early life may result in a left ventricle which is not 'trained' to sustain a normal cardiac output. In any event, for the purpose of this paper, the total mortality in this series in both shunted and unshunted cases was regarded as -the result of low output cardiac failure, and statistical analyses were made on this assumption. Table 3 lists the various types of pulmonary to systemic shunts which required to be taken down at the time of complete repair together with the operative mortality in each group. Though in our experience the technically easiest shunt to take down is a right Blalock, there is no evidence from these figures that one shunt rather than another introduces a significant risk of fatal complications at the time of complete repair. The second analysis was to determine the total incidence of low output cardiac failure in the entire series of 96 operations. The total incidence was regarded as the fatal cases plus those non-fatal cases which met the arbitrary definition of low output TABLE 4 Incidence of low output cardiac failure Cases Cardiac failure Primary repair (31-9%) Previous shunt 49 3 (6-1%) Total (18-8%) (0005>P>0001) 20-15] 41) 0 u 0l0-.0I E z Age in years failure as described above. This analysis is set out in Table 4 and shows clearly that there was 5 times the incidence of this event in the unshunted as opposed to the shunted subset; this difference was highly significant. Influence of patient age on results of complete repair None of the patients in this series was under the age of 2 years. The distribution of patients according to age is illustrated in the bar-graph represented in Fig. 1 and the data are analysed in Table 5. The patients in the shunted group tended to be slightly older, with a median age of 8&3 years as opposed to the unshunted group with a median age of 6-1 years. The mortality and total incidence of low output cardiac failure was 2 to 3 times higher in the patients under the age of 5 years though on the figures available the significance of this difference is not certain. However, our experience suggests that patients over the age of 5 years, especially if they have a prior shunt, have a better postoperative course. Influence of patient's weight (physical development) on results of complete repair The great majority of the patients in this series were much below the appropriate weight in relation to their age. This is illustrated in the bar-graph M Unshunted potients M Shunted patients * Hospital deaths Em Low output failure ib l FJ ni ninn FIG. 1 This bar graph depicts the distribution of the shunted and unshunted patients in the various age groups. The median age of the unshunted patients was 6-1 years compared with 8-3 years in the shunted patients, but this difference did not reach significant levels (0 10 > P > 0 05).
4 TABLE 5 Relation of age to mortality and power failure Age (y) No. Mortality Power failure Tetralogy of Fallot 929 Primary repair > (1087%) P> (25 7%) P>0-20 Previous shunt <5 9 (111%) P>020 2 (22.20/) P>0-20 > (25%) 3 (7.50/) Allcases represented in Fig. 2. Half the patients in the unshunted group were below the 10th centile for weight, and a similar proportion in the shunted subset were below the 20th centile. This indicates that the entire group of 96 patients were much less well physically developed than the average population of their age and this difference was highly significant (P < 0-001). However, there was no statistically significant difference in the distribution of the two groups, shunted and unshunted, according to weight centiles, and the mortality and morbidity seemed randomly distributed over the range of centile subgroups as is evident from Table 6. It is concluded that body weight adjusted for age has no predictive value in anticipating hospital morbidity or mortality. Influence of preoperative haemoglobin levels on results of complete repair A raised haemoglobin level in these patients was taken as evidence of chronic hypoxia caused by a reduced or suboptimal pulmonary blood flow. As I S- 0 ll 0 EI z.i Un < (16%) P< (32%) P<O005 fl expected, there tended to be a higher proportion of shunted patients in the groups with normal or near normal haemoglobin levels as is illustrated in Fig. 3, though the difference in observed distribution did not reach significant levels. There was a significantly higher mortality and morbidity in the group with haemoglobin concentrations in excess of 19 g/dl. This is evident in the analysis set out in TABLE 6 Relation of body weight to mortality and low output cardiac failure Weight (centile) All cases Mortality Power failure < 10th 44 6 (13-7%) 9 (20 5%) loth-50th 34 1 (33%) 4 (13-2%) >50th 18 1 (5 6%) 5 (20-2%) NS NS Shunted and unshunted cases appeared randomly distributed between 3 weight/centile subsets. NS=not significant. Percentiles <e ~97 Age/weight percentile subgroups FIG. 2 This bar graph depicts the distribution of shunted and unshunted patients according to weight centiles. There was no significant difference in the distribution of the two groups, but both distributions differed highly significantly from an expected normal population (P < 0 001).
5 930 Richardson and Clarke vw 0 u 43 -o E z Hoemoglobin levels (q/dl) FIG. 3 This bar graph depicts the distribution of shunted and unshunted patients according to haemoglobin levels. The median level in the unshunted group was 17-4g/dl compared with 16-3g/dl in the shunted group, but this difference did not reach significant levels (0-20 >P>0-10). Table 7 and the figures certainly support the thesis that high haemoglobin levels are associated with increased operative risk. Combined influence of major preoperative risk factors on results of complete repair From the analysis thus far it seemed that earlier shunting was associated with a reduced morbidity, whereas a high haemoglobin level was associated TABLE 7 Relation of haemoglobin levels to mortality and low output cardiac failure No. Haemoglobin Mortality Cardiac conc. failure Primary repair 16 <16 g/dl 0 1 (6 3%) g/dl 2 (11-8%) 7 (41-7%) 14 > 19 g/dl 4 (28 6%) 7 (50 0%) P>0-2 P<0-05 Previous shunt (5*9%) 1 (5*9%) 9 1(11-1%) 2(22-2%) NS NS All cases 39 <16 g/dl 0 1 (2.6%) g/dl 3 (8-8%) 8 (23-5%) 23 >19 g/dl 5 (21-7%) 9 (39-1%) P<0-025 P<0 001 TABLE 8 Mortality and morbidity in relation to polycythaemia plus a prior shunt Category Cases Mortality Low output cardiac failure Hb<16g/dl Shunted and > (2 6%) unshunted Hba>16tg/dI 26 2 (7-7%) 3 (11-5%) and shunted f Hba> 16 g/di 32 6 (18-6%) 14 (43 8%) P< P< with an increased risk. By combining these two factors (see Table 8) it was possible to define a low risk group with haemoglobin levels in the normal range, whether or not shunted, a moderate risk group who had raised haemoglobin levels but were previously shunted, and a high risk group who had both high haemoglobin levels and had not had a previous shunt. The observed difference in morbidity in these three clinical groups was highly significant. If each of these three groups was further subdivided into subgroups below and above the age of 5 years (see Table 9), the numbers become too small to achieve statistical significance, but the mortality and morbidity in the younger age subgroups seem to be appreciably higher. Intraoperative correlates of postoperative mortality and morbidity As indicated above, all the operations were conducted along substantially the same lines, and two TABLE 9 Mortality and morbidity in relation to polycythaemia, age, and prior shunting Category Cases Mortality Low output cardiac failure Hb<16 g/dl Age>5 yr Hb < 16 g/dl (12-5%) Age<5 yr Hb> 16 g/dl Shunted 21 1 (5%) 2 (10%) Age>5 yr Hb > 16 g/dl ) Shunted (20%) 1 (20%) Age<5 yr 9 Hb>16g/dl 9 Unshunted (15%) 7 (35%) Age>5 yr J Hb > 16 g/dl 9 Unshunted (25%) 7 (58%) Age<5 yr J
6 intraoperative factors were tested for correlation with the postoperative results. These were: (1) the relation of the right ventricular to the left ventricular systolic pressure at the completion of the operation, and (2) the method of right ventricular outflow tract reconstruction. Relation of ratio of right to left ventricular post repair systolic pressures to results of complete repair At the conclusion of each operation, after cardiopulmonary bypass had been discontinued and when a reasonably stable circulation had been re-established, pressures were recorded in both the right and the left ventricular cavities by needle puncture. A ratio of right to left ventricular systolic pressures below one-third was regarded as indicating a good right ventricular outflow tract reconstruction. If the ratio was between onethird and two-thirds this was generally considered as acceptable but not optimal. If the ratio was in excess of two-thirds this was regarded as unsatisfactory, and on several occasions a further bypass run was conducted in an attempt to allow a more complete relief of the right ventricular outflow tract obstruction. The justification for these attitudes is apparent from perusal of Table 10 which shows quite clearly that there was a statistically significant increase in mortality and morbidity in those cases in which the right ventricular pressure remained high at the end of the repair operation. Shunted and unshunted cases were randomly distributed between the first two groups but as it happened a majority of cases in the third group had previously been shunted. The reason for this was, in part, that this group of patients had been regarded at the time of the original investigation to have a right ventricular outflow tract which was unfavourable for early repair, and hence some of these were shunted as a preliminary procedure hoping that as the child grew older right ventricular outflow tract reconstruction might be technically TABLE 10 Relation of RVp/LVp after repair to mortality and low output cardiac failure RVpILVp Cases Mortality Cardiac failure (29%) 4 (12-6%) (6 0%) 9 (17-7%) (36 4%) 5 (45.5%) 0O005>P> O01>P>005 Shunted and unshunted cases were randomly distributed between first 2 groups but 75 per cent of cases in third group were unshunted. RVp/LVp=ratio of right to left ventricular systolic pressures. Tetralogy of Fallot 931 easier. Despite the fact that in general a previous shunt was associated with a low mortality and morbidity it does not seem to protect the patient from the serious prognostic import of a high residual right ventricular pressure. Method of right ventricular outflow tract reconstruction and results of total repair While it is generally recognized that the major obstacle to successful total correction is difficulty with the reconstruction of the right ventricular outflow tract, it has none the less been suggested that a long outflow tract patch across the pulmonary valve ring resulting in pulmonary valve regurgitation is associated with higher mortality and morbidity and, therefore, should be avoided if at all possible (Kirklin and Karp, 1970). Our experience in this regard is set out in Table 11. Our patients were about equally divided into a first group with an intact, unobstructed pulmonary valve, a second group which required pulmonary valvotomy with the inevitable production of some pulmonary valve regurgitation, and a third group which required extensive patch reconstruction of the outflow tract with the patch extending across the pulmonary valve ring and therefore associated with free pulmonary valve regurgitation (except for three isolated cases in which a monocusp valve was constructed from pericardium). As can be seen, there was an increased mortality and morbidity in those patients requiring extensive right ventricular outflow tract reconstruction, but on the basis of these figures the observed difference was not significant. Our experience suggests that it is far more important to achieve more or less complete relief of right ventricular outflow tract obstruction by whatever means is necessary even if this leaves a regurgitant pulmon- TABLE 11 Relation of right ventricular outflow tract reconstruction to mortality and low output cardiac failure Reconstruction Cases Mortality Cardiac failure Infundibulectomy alone 30 1 (3 3%) 3 (10%) Infundibular patch Pulmonary valvotomy 32 2 (6 25%) 7 (21.9%) with PR Patch reconstruction 29 5 (17-4%) 8 (27.6%) across pulmonary valve ringll 1-~~~0 30>P>0-20Ji Shunted and unshunted cases appeared randomly distributed between 4 reconstruction groups. PR=Pulmonary valve regurgitation.
7 932 Richardson and Clarke ary valve. This last feature seems of little importance, in the short term at least, so long as the right ventricular pressure is low. Bypass time Not surprisingly the total cardiopulmonary bypass time in the previously shunted group of patients was slightly longer than in the unshunted patients. The median bypass time for the shunted patients was 101 minutes compared with a median figure of 93 minutes for the unshunted patients, but this difference was not statistically significant from our figures. Postoperative drainage Again, not surprisingly, the postoperative chest drainage during the first 6 hours in the previously shunted group was slightly larger, amounting to a median figure of 2'7 ml/kg-l hr-' compared with a median figure of 1 9 ml/kg-1 hr-' for the unshunted group, but once again this difference was not statistically significant. Discussion Although in the experience of some surgeons a previous systemic to pulmonary artery anastomosis is associated with a higher surgical mortality at the second stage repair (Ehrenhaft, Fisher, and Lawrence, 1963), the general consensus is that a previous shunt does not militate against a good result at the time of complete repair. There have been only a few published reports (Leachman, Hallman, and Cooley, 1965; Ebert and Sabiston, 1967) in which data are supplied to support the thesis that there is a lower incidence of complications in the previously shunted group. Two reasons have been advanced for this lower morbidity. In the first place a previous shunt results in a reduced haemoglobin level, and in the second place it may increase left ventricular size and work potential when this is initially small. Our data could be interpreted to support either or both of these hypotheses. Early complete repair has been advocated (Barratt-Boyes and Neutze, 1973; Rees and Starr, 1973) because of the alleged high mortality from shunting in infancy. However, this has not been our experience. During the period in which we undertook the 96 total repairs which have been reviewed, we also operated on a further 37 infants, under the age of 2, with the tetralogy of Fallot and electively performed shunt operations, with only 2 hospital deaths (5 4%) and no late deaths. Only a few of this group of infants came forward for complete repair during the period under review. The number who died from natural causes without surgical referral is not known. Clearly, the final answer to the question of the best surgical policy to follow in respect of these patients will come when it is possible to follow a whole cohort of infants with this diagnosis from infancy to adult life in centres with varying surgical policies. Only then will we be able truly to appreciate the total attrition from natural causes, from early shunting or early repair, and from early shunting (if indicated) and subsequent repair. In the meantime, we believe our experience justifies a continuing policy (in our unit, at least) of performing a shunt procedure in infants with the tetralogy of Fallot who have significant hypoxic symptoms, especially if the right ventricular outflow tract, as depicted by cineangiography, seems to require an extensive reconstruction. Delayed, elective, total repair can then be undertaken with the expectation of a low operative mortality and morbidity. Finally, our experience also lends strong support to the idea that persistent right ventricular hypertension after repair carries a bad immediate prognosis. References Barratt-Boyes, B. G., and Neutze, J. M. (1973). Primary repair of tetralogy of Fallot in infancy using profound hypothermia with circulatory arrest and limited cardiopulmonary bypass. Annals of Surgery, 178, 406. Blalock, A., and Taussig, H. B. (1945). The surgical treatment of malformations of the heart in which there is pulmonary stenosis or pulmonary atresia. Journal of the American Medical Association, 128, 189. Ebert, P. A., and Sabiston, D. C. (1967). Surgical management of the tetralogy of Fallot. Influence of a previous systemic-pulmonary anastomosis on the results of open correction. Annals of Surgery, 165, 806. Ehrenhaft, J. L., Fisher, J. M., and Lawrence, M. S. (1963). Evaluation of results after correction of tetralogy of Fallot. Journal of Thoracic and Cardiovascular Surgery, 45, 224. Fallot, E. A. L. (1888). Contribution a I'anatomie pathologique de la maladie bleue (cyanose cardiaque). Marseillemddicale, 25, 77. Gotsman, M. S., Beck, W., Barnard, C. N., O'Donovan, T. G., and Schrire, V. (1969). Results of repair of tetralogy of Fallot. Circulation, 40, 803. Kirklin, J. W., and Karp, R. B. (1970). The Tetralogy of Fallot from a Surgical Viewpoint. W. B. Saunders, Philadelphia. Leachman, R. D., Hallman, G. L., and Cooley, D. A. (1965). Relationship between polycythemia and surgical mortality in patients undergoing total correction for tetralogy of Fallot. Circulation, 32, 65. Malm, J. R., Blumenthal, S., Bowman, F. O., Jr., Ellis, K., Jameson, A. G., Jesse, M. J., and Yeoh, C. B. (1966).
8 Factors that modify hemodynamic results in total correction of tetralogy of Fallot. Journal of Thoracic and Cardiovascular Surgery, 52, 502. Rees, G. M., and Starr, A. (1973). Total correction of Fallot's tetralogy in patients aged less than 1 year. British Heart J'ournal, 35, 898. Scott, H. W., Collins, H. A., and Foster, J. H. (1954). Hypothermia as an adjuvant in cardiovascular surgery. Experimental and clinical observations. American Surgeon, 20, 799. Snedecor, G. W., and Cochran, W. G. (1967). Statistical Methods, 6th ed. Iowa State University Press, Ames, Iowa. Tetralogy of Fallot 933 Stensen, N. (1671). In Bartholin, T., Acta Medica et Philosophica Hafniensia, Vol. 1, p P. Haubold, Hafniae. Tanner, JY M., Whitehouse, R. H., and Takaishi, M. (1966). Standards from birth to maturity for height, weight, height velocity, and weight velocity: British children, Archives of Disease in Childhood, 41, 454 and 613. Address for reprints to J. P. Richardson, Esq., F.R.C.S., Division of Cardiac Surgery, Royal Children's Hospital, Flemington Road, Parkville, Victoria 3052, Australia. Br Heart J: first published as /hrt on 1 September Downloaded from on 16 November 2018 by guest. Protected by
Aorta-to-Right Pulmonary Artery Anastomosis Causing Obstruction of the Right Pulmonary Artery
 Aorta-to-Right Pulmonary Artery Anastomosis Causing Obstruction of the Right Pulmonary Artery Management During Correction of Tetralogy of Fallot William A. Gay, Jr., M.D., and Paul A. Ebert, M.D. ABSTRACT
Aorta-to-Right Pulmonary Artery Anastomosis Causing Obstruction of the Right Pulmonary Artery Management During Correction of Tetralogy of Fallot William A. Gay, Jr., M.D., and Paul A. Ebert, M.D. ABSTRACT
Research Presentation June 23, Nimish Muni Resident Internal Medicine
 Research Presentation June 23, 2009 Nimish Muni Resident Internal Medicine Research Question In adult patients with repaired Tetralogy of Fallot, how does Echocardiography compare to MRI in evaluating
Research Presentation June 23, 2009 Nimish Muni Resident Internal Medicine Research Question In adult patients with repaired Tetralogy of Fallot, how does Echocardiography compare to MRI in evaluating
Indications for the Brock operation in current
 Thorax (1973), 28, 1. Indications for the Brock operation in current treatment of tetralogy of Fallot H. R. MATTHEWS and R. H. R. BELSEY Department of Thoracic Surgery, Frenchay Hospital, Bristol It is
Thorax (1973), 28, 1. Indications for the Brock operation in current treatment of tetralogy of Fallot H. R. MATTHEWS and R. H. R. BELSEY Department of Thoracic Surgery, Frenchay Hospital, Bristol It is
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
Pulmonary Artery: Operative Repair
 Tetralogy of Fallot with a Single Pulmonary Artery: Operative Repair J. Jacques Mistrot, M.D., William F. Bernhard, M.D., Amnon Rosenthal, M.D., and Aldo R. Castaneda, M.D. ABSTRACT Surgical repair was
Tetralogy of Fallot with a Single Pulmonary Artery: Operative Repair J. Jacques Mistrot, M.D., William F. Bernhard, M.D., Amnon Rosenthal, M.D., and Aldo R. Castaneda, M.D. ABSTRACT Surgical repair was
Total Correction of Tetralogy of Fallot
 Brit. Heart J., 1968, 30, 563. Total Correction of Tetralogy of Fallot Review of Ten Years' Experience BERNARD S. GOLDMAN*, WILLIAM T. MUSTARD, AND GEORGE S. TRUSLER From the Department of Surgery, Hospital
Brit. Heart J., 1968, 30, 563. Total Correction of Tetralogy of Fallot Review of Ten Years' Experience BERNARD S. GOLDMAN*, WILLIAM T. MUSTARD, AND GEORGE S. TRUSLER From the Department of Surgery, Hospital
Cardiac surgery relative to population: pattern of cardiac surgery in South Australia,
 Thorax, 1977, 32, 57-577 Cardiac surgery relative to population: pattern of cardiac surgery in South Australia, 1949-751 H. D. SUTHERLAND, D. R. CRADDOCK, J. L. WADDY, AND G. R. NUNN From the Cardio-Thoracic
Thorax, 1977, 32, 57-577 Cardiac surgery relative to population: pattern of cardiac surgery in South Australia, 1949-751 H. D. SUTHERLAND, D. R. CRADDOCK, J. L. WADDY, AND G. R. NUNN From the Cardio-Thoracic
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Congenital heart disease in the neonate: results of
 Archives of Disease in Childhood, 1983, 58, 137-141 Congenital heart disease in the neonate: results of surgical treatment E L BOVE, C BULL, J STARK, M DE LEVAL, F J Thoracic Unit, The Hospitalfor Sick
Archives of Disease in Childhood, 1983, 58, 137-141 Congenital heart disease in the neonate: results of surgical treatment E L BOVE, C BULL, J STARK, M DE LEVAL, F J Thoracic Unit, The Hospitalfor Sick
MRI (AND CT) FOR REPAIRED TETRALOGY OF FALLOT
 MRI (AND CT) FOR REPAIRED TETRALOGY OF FALLOT Linda B Haramati MD, MS Departments of Radiology and Medicine Bronx, New York OUTLINE Pathogenesis Variants Initial surgical treatments Basic MR protocols
MRI (AND CT) FOR REPAIRED TETRALOGY OF FALLOT Linda B Haramati MD, MS Departments of Radiology and Medicine Bronx, New York OUTLINE Pathogenesis Variants Initial surgical treatments Basic MR protocols
Debanding and repair of ventricular septal defect: a new technique for older patients
 Thorax, 1979, 34, 531-53 5 Debanding and repair of ventricular septal defect: a new technique for older patients P LAURIDSEN, A UHRENHOLDT, AND I H RYGG From the Department of Thoracic Surgery R and Cardiovascular
Thorax, 1979, 34, 531-53 5 Debanding and repair of ventricular septal defect: a new technique for older patients P LAURIDSEN, A UHRENHOLDT, AND I H RYGG From the Department of Thoracic Surgery R and Cardiovascular
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Congenital Cardiac Anomalies
 Congenital Cardiac Anomalies One-Stage Repair in Infancy Donald B. Doty, M.D., Ronald M. Lauer, M.D., and J. L. Ehrenhaft, M.D. ABSTRACT A proposed preferred treatment plan consisting of one-stage operative
Congenital Cardiac Anomalies One-Stage Repair in Infancy Donald B. Doty, M.D., Ronald M. Lauer, M.D., and J. L. Ehrenhaft, M.D. ABSTRACT A proposed preferred treatment plan consisting of one-stage operative
Reconstruction of right ventricular outflow with a valved homograft conduit
 Thorax (1974), 29, 617. Reconstruction of right ventricular outflow with a valved homograft conduit D. J. WHEATLEY, S. PRUSTY, and D. N. ROSS Department of Surgery, National Heart Hospital, London WI Wheadey,
Thorax (1974), 29, 617. Reconstruction of right ventricular outflow with a valved homograft conduit D. J. WHEATLEY, S. PRUSTY, and D. N. ROSS Department of Surgery, National Heart Hospital, London WI Wheadey,
The Surgical Treatment of Tetralogy of Fallot
 COLLECTIVE REVIEW The Surgical Treatment of Tetralogy of Fallot H. E. Sinchez, M.D., D.Sc., E. M. Cornish, B.Sc.(Hons), M.B., Ch.B., Feng Chu Shih, M.D., J. de Nobrega, F.R.C.S., J. Hassoulas, M.Med.(Cape
COLLECTIVE REVIEW The Surgical Treatment of Tetralogy of Fallot H. E. Sinchez, M.D., D.Sc., E. M. Cornish, B.Sc.(Hons), M.B., Ch.B., Feng Chu Shih, M.D., J. de Nobrega, F.R.C.S., J. Hassoulas, M.Med.(Cape
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Adult Congenital Heart Disease T S U N ` A M I!
 Adult Congenital Heart Disease T S U N ` A M I! Erwin Oechslin, MD, FRCPC, FESC Director, Congenital Cardiac Centre for Adults University Health Network Peter Munk Cardiac Centre / Toronto General Hospital
Adult Congenital Heart Disease T S U N ` A M I! Erwin Oechslin, MD, FRCPC, FESC Director, Congenital Cardiac Centre for Adults University Health Network Peter Munk Cardiac Centre / Toronto General Hospital
Ostium primum defects with cleft mitral valve
 Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Thorax (1965), 20, 405. VIKING OLOV BJORK From the Department of Thoracic Surgery, University Hospital, Uppsala, Sweden Ostium primum defects are common; by 1955, 37 operated cases had been reported by
Operative Closure of Isolated Defects of the Ventricular Septum: Planned Delay
 Operative Closure of Isolated Defects of the Ventricular Septum: Planned Delay R. Darryl Fisher, M.D., Scott L. Faulkner, M.D., C. Gordon Sell, M.D., Thomas P. Graham, Jr., M.D., and Harvey W. Bender,
Operative Closure of Isolated Defects of the Ventricular Septum: Planned Delay R. Darryl Fisher, M.D., Scott L. Faulkner, M.D., C. Gordon Sell, M.D., Thomas P. Graham, Jr., M.D., and Harvey W. Bender,
The Chest X-ray for Cardiologists
 Mayo Clinic & British Cardiovascular Society at the Royal College of Physicians, London : 21-23-October 2013 Cases-Controversies-Updates 2013 The Chest X-ray for Cardiologists Michael Rubens Royal Brompton
Mayo Clinic & British Cardiovascular Society at the Royal College of Physicians, London : 21-23-October 2013 Cases-Controversies-Updates 2013 The Chest X-ray for Cardiologists Michael Rubens Royal Brompton
Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS
 Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS ABSTRACT Background: The congenital heart disease occurs in 0,8% of live births and they have a wide spectrum
Pattern of Congenital Heart Disease A Hospital-Based Study *Sadiq Mohammed Al-Hamash MBChB, FICMS ABSTRACT Background: The congenital heart disease occurs in 0,8% of live births and they have a wide spectrum
Extreme pulmonary hypertension caused by mitral valve disease
 British Heart Journal, I975, 37, 74-78. Extreme pulmonary hypertension caused by mitral valve disease Natural history and results of surgery C. Ward and B. W. Hancock From the Cardio-Thoracic Unit, Northern
British Heart Journal, I975, 37, 74-78. Extreme pulmonary hypertension caused by mitral valve disease Natural history and results of surgery C. Ward and B. W. Hancock From the Cardio-Thoracic Unit, Northern
Long-term Results of Aortopulmonary Anastomosis for Tetralogy of Fallot
 Long-term Results of Aortopulmonary Anastomosis for Tetralogy of Fallot Morbidity and Mortality, 1946-1969 By ROGER B. COLE, M.D., ALEXANDER J. MUSTER, M.D., DAVID E. FIXLER, AND MILTON H. PAUL, M.D. SUMMARY
Long-term Results of Aortopulmonary Anastomosis for Tetralogy of Fallot Morbidity and Mortality, 1946-1969 By ROGER B. COLE, M.D., ALEXANDER J. MUSTER, M.D., DAVID E. FIXLER, AND MILTON H. PAUL, M.D. SUMMARY
Children with Single Ventricle Physiology: The Possibilities
 Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
The blue baby. Case 4
 Case 4 The blue baby Mrs Smith has brought her baby to A&E because she says he has started turning blue. What are your immediate differential diagnoses? 1 Respiratory causes: Congenital respiratory disorder.
Case 4 The blue baby Mrs Smith has brought her baby to A&E because she says he has started turning blue. What are your immediate differential diagnoses? 1 Respiratory causes: Congenital respiratory disorder.
Since 1954, when Lillehei completed the first successful
 Current Surgical Management of Tetralogy of Fallot Vaughn A. Starnes, MD, Giovanni Battista Luciani, MD, David A. Latter, MD, and Michael 1. Griffin, MD Division of Cardiothoracic Surgery, University of
Current Surgical Management of Tetralogy of Fallot Vaughn A. Starnes, MD, Giovanni Battista Luciani, MD, David A. Latter, MD, and Michael 1. Griffin, MD Division of Cardiothoracic Surgery, University of
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Intra-operative Echocardiography: When to Go Back on Pump
 Intra-operative Echocardiography: When to Go Back on Pump GREGORIO G. ROGELIO, MD., F.P.C.C. OUTLINE A. Indications for Intraoperative Echocardiography B. Role of Intraoperative Echocardiography C. Criteria
Intra-operative Echocardiography: When to Go Back on Pump GREGORIO G. ROGELIO, MD., F.P.C.C. OUTLINE A. Indications for Intraoperative Echocardiography B. Role of Intraoperative Echocardiography C. Criteria
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum
 Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Oximetric detection of intracardiac left-to-right shunts'
 British Heart Journal, 1979, 42, 690-694 Oximetric detection of intracardiac left-to-right shunts' MICHAEL D. FREED, OLLI S. MIETTINEN, AND ALEXANDER S. NADAS From the Department of Cardiology, Children's
British Heart Journal, 1979, 42, 690-694 Oximetric detection of intracardiac left-to-right shunts' MICHAEL D. FREED, OLLI S. MIETTINEN, AND ALEXANDER S. NADAS From the Department of Cardiology, Children's
Pulmonarv Arterv Plication: with Type I Trunms Arteriosus. A New S&gical Procedure for Small Infants
 Pulmonarv Arterv Plication: A New S&gical Procedure for Small Infants with Type I Trunms Arteriosus S. Bert Litwin, M.D., and David Z. Friedberg, M.D. ABSTRACT A new technique is reported for constriction
Pulmonarv Arterv Plication: A New S&gical Procedure for Small Infants with Type I Trunms Arteriosus S. Bert Litwin, M.D., and David Z. Friedberg, M.D. ABSTRACT A new technique is reported for constriction
Surgical management of tricuspid
 Surgical management of tricuspid Thorax (1969), 24, 239. atresia P. B. DEVERALL, J. C. R. LINCOLN, E. ABERDEEN, R. E. BONHAM-CARTER, AND D. J. WATERSTON From the Hospital for Sick Children, Great Ormond
Surgical management of tricuspid Thorax (1969), 24, 239. atresia P. B. DEVERALL, J. C. R. LINCOLN, E. ABERDEEN, R. E. BONHAM-CARTER, AND D. J. WATERSTON From the Hospital for Sick Children, Great Ormond
AMERICAN ACADEMY OF PEDIATRICS 993 THE NATURAL HISTORY OF CERTAIN CONGENITAL CARDIOVASCULAR MALFORMATIONS. Alexander S. Nadas, M.D.
 AMERICAN ACADEMY OF PEDIATRICS 993 tnicular overload is the major problem and left ventricular failure occurs. Since for many years the importance of hepatomegaly in the diagnosis of cardiac failure has
AMERICAN ACADEMY OF PEDIATRICS 993 tnicular overload is the major problem and left ventricular failure occurs. Since for many years the importance of hepatomegaly in the diagnosis of cardiac failure has
after Repair of Tetralogy of Fallot
 Chronic Congestive Heart Failure after Repair of Tetralogy of Fallot ALBERT P. ROCCHINI, M.D., AMNON ROSENTHAL, M.D., MICHAEL FREED, M.D., ALDO R. CASTANEDA, M.D., AND ALEXANDER S. NADAS, M.D. SUMMARY
Chronic Congestive Heart Failure after Repair of Tetralogy of Fallot ALBERT P. ROCCHINI, M.D., AMNON ROSENTHAL, M.D., MICHAEL FREED, M.D., ALDO R. CASTANEDA, M.D., AND ALEXANDER S. NADAS, M.D. SUMMARY
PATENT DUCTUS ARTERIOSUS (PDA)
 PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
PATENT DUCTUS ARTERIOSUS (PDA) It is a channel that connect the pulmonary artery with the descending aorta (isthumus part). It results from the persistence of patency of the fetal ductus arteriosus after
A teenager with tetralogy of fallot becomes a soccer player
 ISSN 1507-6164 DOI: 10.12659/AJCR.889440 Received: 2013.06.06 Accepted: 2013.07.10 Published: 2013.09.23 A teenager with tetralogy of fallot becomes a soccer player Authors Contribution: Study Design A
ISSN 1507-6164 DOI: 10.12659/AJCR.889440 Received: 2013.06.06 Accepted: 2013.07.10 Published: 2013.09.23 A teenager with tetralogy of fallot becomes a soccer player Authors Contribution: Study Design A
Congenital heart disease: When to act and what to do?
 Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Inter-surgeon variability in long-term outcomes after transatrial repair of tetralogy of Fallot: 25 years experience with 675 patients.
 Inter-surgeon variability in long-term outcomes after transatrial repair of tetralogy of Fallot: 25 years experience with 675 patients. Y d'udekem, JC Galati, IE Konstantinov, MMH Cheung, CP Brizard Royal
Inter-surgeon variability in long-term outcomes after transatrial repair of tetralogy of Fallot: 25 years experience with 675 patients. Y d'udekem, JC Galati, IE Konstantinov, MMH Cheung, CP Brizard Royal
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Total Correction of Tetralogy of Fallot in Infancy
 Total Correction of Tetralogy of Fallot in Infancy Postoperative Hemodynamic Evaluation By CECILLE 0. SUNDERLAND, M.D., RUrTH G. MATARAZZO, PH.D., MARTIN H. LEES, M.D., VicroR D. MENASHE, M.D., LAWRENCE
Total Correction of Tetralogy of Fallot in Infancy Postoperative Hemodynamic Evaluation By CECILLE 0. SUNDERLAND, M.D., RUrTH G. MATARAZZO, PH.D., MARTIN H. LEES, M.D., VicroR D. MENASHE, M.D., LAWRENCE
Anomalous muscle bundle of the right ventricle
 British Heart Journal, 1978, 40, 1040-1045 Anomalous muscle bundle of the right ventricle Its recognition and surgical treatment M. D. LI, J. C. COLES, AND A. C. McDONALD From the Department of Paediatrics,
British Heart Journal, 1978, 40, 1040-1045 Anomalous muscle bundle of the right ventricle Its recognition and surgical treatment M. D. LI, J. C. COLES, AND A. C. McDONALD From the Department of Paediatrics,
Atrioventricular Valve Dysplasia
 Atrioventricular Valve Dysplasia How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job
Atrioventricular Valve Dysplasia How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job
Common Defects With Expected Adult Survival:
 Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Aortography in Fallot's Tetralogy and Variants
 Brit. Heart J., 1969, 31, 146. Aortography in Fallot's Tetralogy and Variants SIMON REES AND JANE SOMERVILLE From The Institute of Cardiology and National Heart Hospital, London W.J In patients with Fallot's
Brit. Heart J., 1969, 31, 146. Aortography in Fallot's Tetralogy and Variants SIMON REES AND JANE SOMERVILLE From The Institute of Cardiology and National Heart Hospital, London W.J In patients with Fallot's
The Rastelli procedure has been traditionally used for repair
 En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
HISTORY. Question: What type of heart disease is suggested by this history? CHIEF COMPLAINT: Decreasing exercise tolerance.
 HISTORY 15-year-old male. CHIEF COMPLAINT: Decreasing exercise tolerance. PRESENT ILLNESS: A heart murmur was noted in childhood, but subsequent medical care was sporadic. Easy fatigability and slight
HISTORY 15-year-old male. CHIEF COMPLAINT: Decreasing exercise tolerance. PRESENT ILLNESS: A heart murmur was noted in childhood, but subsequent medical care was sporadic. Easy fatigability and slight
The need for right ventricular outflow tract reconstruction
 Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
CASE REPORT. Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea. G. A. Lopez, M.D., and A. R. C. Dobell, M.D.
 CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
CASE REPORT Mycotic Aneurysm of Ascending Aorta Due to Sarcina Lutea G. A. Lopez, M.D., and A. R. C. Dobell, M.D. ABSTRACT A patient developed a mycotic aneurysm of the aortic suture line after aortic
Pulmonary valve echo motion in pulmonary
 British HeartJournal, I975, 37, ii84-ii90. Pulmonary valve echo motion in pulmonary regurgitation' Arthur E. Weyman, James C. Dillon, Harvey Feigenbaum, and Sonia Chang From the Department of Medicine,
British HeartJournal, I975, 37, ii84-ii90. Pulmonary valve echo motion in pulmonary regurgitation' Arthur E. Weyman, James C. Dillon, Harvey Feigenbaum, and Sonia Chang From the Department of Medicine,
14 Valvular Stenosis
 14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
14 Valvular Stenosis 14-1. Valvular Stenosis unicuspid valve FIGUE 14-1. This photograph shows severe valvular stenosis as it occurs in a newborn. There is a unicuspid, horseshoe-shaped leaflet with a
THE SURGICAL MANAGEMENT OF
 POSTGRAD. MED. J. (I961), 37, 659 THE SURGICAL MANAGEMENT OF FALLOT'S TETRALOGY FALLOT'S tetralogy is a condition of cyanotic congenital heart disease associated with pulmonary stenosis and a ventricular
POSTGRAD. MED. J. (I961), 37, 659 THE SURGICAL MANAGEMENT OF FALLOT'S TETRALOGY FALLOT'S tetralogy is a condition of cyanotic congenital heart disease associated with pulmonary stenosis and a ventricular
of Cavopulmonary Anastomosis
 Takedown and Reconstruction of Cavopulmonary Anastomosis John Rohmer, M.D., Jan M. Quaegebeur, and A. Gerard Brom, M.D. M.D., ABSTRACT Takedown and reconstruction of a previous Glenn anastomosis at the
Takedown and Reconstruction of Cavopulmonary Anastomosis John Rohmer, M.D., Jan M. Quaegebeur, and A. Gerard Brom, M.D. M.D., ABSTRACT Takedown and reconstruction of a previous Glenn anastomosis at the
3 Aortopulmonary Window
 0 0 0 0 0 Aortopulmonary Window Introduction Communications between the ascending aorta and pulmonary artery constitute a spectrum of malformations which is collectively designated aortopulmonary window,
0 0 0 0 0 Aortopulmonary Window Introduction Communications between the ascending aorta and pulmonary artery constitute a spectrum of malformations which is collectively designated aortopulmonary window,
The pulmonary valve is the most common heart valve
 Biologic versus Mechanical Valve Replacement of the Pulmonary Valve After Multiple Reconstructions of the RVOT Tract S. Adil Husain, MD, and John Brown, MD Indiana University School of Medicine, Department
Biologic versus Mechanical Valve Replacement of the Pulmonary Valve After Multiple Reconstructions of the RVOT Tract S. Adil Husain, MD, and John Brown, MD Indiana University School of Medicine, Department
Hemodynamic assessment after palliative surgery
 THERAPY AND PREVENTION CONGENITAL HEART DISEASE Hemodynamic assessment after palliative surgery for hypoplastic left heart syndrome PETER LANG, M.D., AND WILLIAM I. NORWOOD, M.D., PH.D. ABSTRACT Ten patients
THERAPY AND PREVENTION CONGENITAL HEART DISEASE Hemodynamic assessment after palliative surgery for hypoplastic left heart syndrome PETER LANG, M.D., AND WILLIAM I. NORWOOD, M.D., PH.D. ABSTRACT Ten patients
Total Anomalous Pulmonary Venous Return
 Total Anomalous Pulmonary Venous Return Correlation of Hemodynamic Observations and Surgical Mortality in 58 Cases Robert D. Leachman, M.D., Denton A. Cooley, M.D., Grady L. Hallman, M.D., James W. Simpson,
Total Anomalous Pulmonary Venous Return Correlation of Hemodynamic Observations and Surgical Mortality in 58 Cases Robert D. Leachman, M.D., Denton A. Cooley, M.D., Grady L. Hallman, M.D., James W. Simpson,
A New Radiopaque Surgical Suture* Juro WADA, M.D. and Masahiro ENDO, M.D.
 A New Radiopaque Surgical Suture* Juro WADA, M.D. and Masahiro ENDO, M.D. SUMMARY We have developed a new X-ray visible suture. It is a polyester suture containing platinum wires. The radiopaque suture
A New Radiopaque Surgical Suture* Juro WADA, M.D. and Masahiro ENDO, M.D. SUMMARY We have developed a new X-ray visible suture. It is a polyester suture containing platinum wires. The radiopaque suture
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
CONGENITAL HEART DISEASE (CHD)
 CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
CONGENITAL HEART DISEASE (CHD) DEFINITION It is the result of a structural or functional abnormality of the cardiovascular system at birth GENERAL FEATURES OF CHD Structural defects due to specific disturbance
Management of Infants with Large Ventricular Septa1 Defects
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 15 * NUMBER * FEBRUARY 1973 Management of Infants with Large Ventricular
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 15 * NUMBER * FEBRUARY 1973 Management of Infants with Large Ventricular
and scope of open-heart surgery
 Posigrad. med. J. (October 1967) 43, 668-676. The technique IN this paper the various methods of carrying out open-heart surgery are described, and the clinical results that are currently being obtained
Posigrad. med. J. (October 1967) 43, 668-676. The technique IN this paper the various methods of carrying out open-heart surgery are described, and the clinical results that are currently being obtained
Septal Defects. How does the heart work?
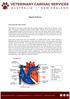 Septal Defects How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right side
Septal Defects How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right side
Conduit Reconstruction of Right Ventricular Outflow Tract
 Conduit Reconstruction of Right Ventricular Outflow Tract Experience with 17 Patients E. Ross Kyger, 111, M.D., Luigi Chiariello, M.D., Grady L. Hallman, M.D., and Denton A. Cooley, M.D. ABSTRACT Evaluation
Conduit Reconstruction of Right Ventricular Outflow Tract Experience with 17 Patients E. Ross Kyger, 111, M.D., Luigi Chiariello, M.D., Grady L. Hallman, M.D., and Denton A. Cooley, M.D. ABSTRACT Evaluation
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT
 LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency
 Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Results of Mitral Valve Replacement, with Special Reference to the Functional Tricuspid Insufficiency Ken-ichi ASANO, M.D., Masahiko WASHIO, M.D., and Shoji EGUCHI, M.D. SUMMARY (1) Surgical results of
Outline. Congenital Heart Disease. Special Considerations for Special Populations: Congenital Heart Disease
 Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Myocardial Ischemia in Infants
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 8 NUMBER 5 NOVEMBER 1969. * Myocardial Ischemia in Infants Its Role in Three
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 8 NUMBER 5 NOVEMBER 1969. * Myocardial Ischemia in Infants Its Role in Three
Cardiac anaesthesia. Simon May
 Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Cardiac anaesthesia Simon May Contents Cardiac: Principles of peri-operative management for cardiac surgery Cardiopulmonary bypass, cardioplegia and off pump cardiac surgery Cardiac disease and its implications
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Surgical implications of right aortic arch with isolation of left subclavian artery'
 British Heart journal, I975, 37, 93I-936. Surgical implications of right aortic arch with isolation of left subclavian artery' L. Rodriguez,2 T. Izukawa, C. A. F. MoEs, G. A. Trusler, and W. G. Williams
British Heart journal, I975, 37, 93I-936. Surgical implications of right aortic arch with isolation of left subclavian artery' L. Rodriguez,2 T. Izukawa, C. A. F. MoEs, G. A. Trusler, and W. G. Williams
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Indication and Technique of Total Correction of Tetralogy of Fallot in 228 Patients
 Indication and Technique of Total Correction of Tetralogy of Fallot in 228 Patients Qingyu Wu, MD Department of Cardiac Surgery, Cardiovascular Institute and Fu Wai Hospital, Chinese Academy of Medical
Indication and Technique of Total Correction of Tetralogy of Fallot in 228 Patients Qingyu Wu, MD Department of Cardiac Surgery, Cardiovascular Institute and Fu Wai Hospital, Chinese Academy of Medical
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
Systemic-Pulmonary Shunts in Neonates and Infants Using Microporous Expanded Polytetrduoroethylene: Immediate and Late Results
 Systemic-Pulmonary Shunts in Neonates and Infants Using Microporous Expanded Polytetrduoroethylene: Immediate and Late Results James S. Donahoo, M.D., Timothy J. Gardner, M.D., Kenneth Zahka, M.D., and
Systemic-Pulmonary Shunts in Neonates and Infants Using Microporous Expanded Polytetrduoroethylene: Immediate and Late Results James S. Donahoo, M.D., Timothy J. Gardner, M.D., Kenneth Zahka, M.D., and
T who has survived first-stage palliative surgical management
 Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
Surgical Treatment for Atrioventricular Septal Defect. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
PULMONARY ARTERY STENTING AFfER TOTAL SURGICAL CORRECTION OF RIGHT VENTRICULAR OUTFLOW TRACT OBSTRUCTIVE LESIONS
 Articles 5 PULMONARY ARTERY STENTING AFfER TOTAL SURGICAL CORRECTION OF RIGHT VENTRICULAR OUTFLOW TRACT OBSTRUCTIVE LESIONS SAMEH ARAB, MD; ERIC ROSENTHAL, MD, MRCP; SHAKEEL QURESHI, MB, MRCP; MICHAEL
Articles 5 PULMONARY ARTERY STENTING AFfER TOTAL SURGICAL CORRECTION OF RIGHT VENTRICULAR OUTFLOW TRACT OBSTRUCTIVE LESIONS SAMEH ARAB, MD; ERIC ROSENTHAL, MD, MRCP; SHAKEEL QURESHI, MB, MRCP; MICHAEL
Long-term results of complete correction with homograft reconstruction in pulmonary
 British HeartJournal, I972, 34, 29-36. Long-term results of complete correction with homograft reconstruction in pulmonary outflow tract atresial Jane Somerville (House Surgeon to the Thoracic Surgical
British HeartJournal, I972, 34, 29-36. Long-term results of complete correction with homograft reconstruction in pulmonary outflow tract atresial Jane Somerville (House Surgeon to the Thoracic Surgical
Candice Silversides, MD Toronto Congenital Cardiac Centre for Adults University of Toronto Toronto, Canada
 PVR Following Repair of TOF Now? When? Candice Silversides, MD Toronto Congenital Cardiac Centre for Adults University of Toronto Toronto, Canada Late Complications after TOF repair Repair will be necessary
PVR Following Repair of TOF Now? When? Candice Silversides, MD Toronto Congenital Cardiac Centre for Adults University of Toronto Toronto, Canada Late Complications after TOF repair Repair will be necessary
Surgical Treatment for Double Outlet Right Ventricle. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
Experience with counterpulsation in
 British Heart J7ournal, 1977, 39, 198-202 Experience with counterpulsation in cardiac surgical patients G. H. SMITH AND W. E. MORGAN From Sheffield Cardiothoracic Unit, Northern General Hospital, Sheffield
British Heart J7ournal, 1977, 39, 198-202 Experience with counterpulsation in cardiac surgical patients G. H. SMITH AND W. E. MORGAN From Sheffield Cardiothoracic Unit, Northern General Hospital, Sheffield
Adults with Congenital Heart Disease. Michael E. McConnell MD, Wendy Book MD Teresa Lyle RN NNP
 Adults with Congenital Heart Disease Michael E. McConnell MD, Wendy Book MD Teresa Lyle RN NNP Outline History of CHD Statistics Specific lesions (TOF, TGA, Single ventricle) Erythrocytosis Pregnancy History
Adults with Congenital Heart Disease Michael E. McConnell MD, Wendy Book MD Teresa Lyle RN NNP Outline History of CHD Statistics Specific lesions (TOF, TGA, Single ventricle) Erythrocytosis Pregnancy History
Recent technical advances and increasing experience
 Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Pediatric Open Heart Operations Without Diagnostic Cardiac Catheterization Jean-Pierre Pfammatter, MD, Pascal A. Berdat, MD, Thierry P. Carrel, MD, and Franco P. Stocker, MD Division of Pediatric Cardiology,
Patent ductus arteriosus PDA
 Patent ductus arteriosus PDA Is connecting between the aortic end just distal to the origin of the LT sub clavian artery& the pulmonary artery at its bifurcation. Female/male ratio is 2:1 and it is more
Patent ductus arteriosus PDA Is connecting between the aortic end just distal to the origin of the LT sub clavian artery& the pulmonary artery at its bifurcation. Female/male ratio is 2:1 and it is more
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS Pediatric Cardiology
 Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Cardiovascular Pathophysiology: Right to Left Shunts aka Cyanotic Lesions Ismee A. Williams, MD, MS iib6@columbia.edu Pediatric Cardiology Learning Objectives To discuss the hemodynamic significance of
Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course
 Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
Pediatr Cardiol (2017) 38:264 270 DOI 10.1007/s00246-016-1508-2 ORIGINAL ARTICLE Surgical Repair of Ventricular Septal Defect; Contemporary Results and Risk Factors for a Complicated Course Maartje Schipper
Supplemental Table 1. ICD-9 Codes for Diagnoses and Procedures
 Supplemental Table 1. ICD-9 Codes for Diagnoses and Procedures ICD-9 Code Description Heart Failure 402.01 Malignant hypertensive heart disease with heart failure 402.11 Benign hypertensive heart disease
Supplemental Table 1. ICD-9 Codes for Diagnoses and Procedures ICD-9 Code Description Heart Failure 402.01 Malignant hypertensive heart disease with heart failure 402.11 Benign hypertensive heart disease
Tetralogy of Fallot (TOF) with absent pulmonary valve
 Repair of Tetralogy of Fallot with Absent Pulmonary Valve Syndrome Karl F. Welke, MD, and Ross M. Ungerleider, MD, MBA Tetralogy of Fallot (TOF) with absent pulmonary valve syndrome (APVS) occurs in 5%
Repair of Tetralogy of Fallot with Absent Pulmonary Valve Syndrome Karl F. Welke, MD, and Ross M. Ungerleider, MD, MBA Tetralogy of Fallot (TOF) with absent pulmonary valve syndrome (APVS) occurs in 5%
Surgical options for tetralogy of Fallot
 Surgical options for tetralogy of Fallot Serban Stoica FRCS(CTh) MD ACHD study day, 19 September 2017 Anatomy Physiology Children Adults Complications Follow up Anatomy Etienne Fallot (1850-1911) VSD Overriding
Surgical options for tetralogy of Fallot Serban Stoica FRCS(CTh) MD ACHD study day, 19 September 2017 Anatomy Physiology Children Adults Complications Follow up Anatomy Etienne Fallot (1850-1911) VSD Overriding
Management of a Patient after the Bidirectional Glenn
 Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
describes 28 years of experience in the surgical management of tetralogy of Fallot with subarterial VSD at Tenri Hospital in Japan.
 EARLY AND LATE RESULTS OF REPAIR OF TETRALOGY OF FALLOT WITH SUBARTERIAL VENTRICULAR SEPTAL DEFECT A comparative evaluation of tetralogy with perimembranous ventricular septal defect Between November 1966
EARLY AND LATE RESULTS OF REPAIR OF TETRALOGY OF FALLOT WITH SUBARTERIAL VENTRICULAR SEPTAL DEFECT A comparative evaluation of tetralogy with perimembranous ventricular septal defect Between November 1966
Serial Cardiac Catheterizations and Exercise Hemodynamics after Correction of Tetralogy of Fallot
 Serial Cardiac Catheterizations and Exercise Hemodynamics after Correction of Tetralogy of Fallot Average Follow-Up 13 Months and 7 Years after Operation By J. DAvm BmSTOW, M.D., FRANK E. KLOSTER, M.D.,
Serial Cardiac Catheterizations and Exercise Hemodynamics after Correction of Tetralogy of Fallot Average Follow-Up 13 Months and 7 Years after Operation By J. DAvm BmSTOW, M.D., FRANK E. KLOSTER, M.D.,
The Double Switch Using Bidirectional Glenn and Hemi-Mustard. Frank Hanley
 The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
10/10/2018. Disclosures. Introduction (II) Introduction (I) The authors have no disclosures
 PERFUSION METHODS AND MODIFICATIONS TO THE CARDIOPULMONARY BYPASS CIRCUIT FOR MIDLINE UNIFOCALIZATION PROCEDURES Tristan D. Margetson CCP, FPP, Justin Sleasman, CCP, FPP, Sami Kollmann, CCP, Patrick J.
PERFUSION METHODS AND MODIFICATIONS TO THE CARDIOPULMONARY BYPASS CIRCUIT FOR MIDLINE UNIFOCALIZATION PROCEDURES Tristan D. Margetson CCP, FPP, Justin Sleasman, CCP, FPP, Sami Kollmann, CCP, Patrick J.
CARDIOVASCULAR SURGERY
 Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Congenital Heart Disease: Cyanotic Lesions. Amitesh Aggarwal
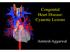 Congenital Heart Disease: Cyanotic Lesions Amitesh Aggarwal 12 y/o male admitted because of dyspnea and cyanosis Patient has been cyanotic since few months after birth Has episodes of tachypnea and worsening
Congenital Heart Disease: Cyanotic Lesions Amitesh Aggarwal 12 y/o male admitted because of dyspnea and cyanosis Patient has been cyanotic since few months after birth Has episodes of tachypnea and worsening
