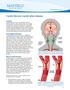
Selective external endarterectomy in patients with ipsilateral symptomatic internal carotid artery occlusion
|
|
|
- Beverly Dixon
- 5 years ago
- Views:
Transcription
1 From the Society for Vascular Surgery Selective external endarterectomy in patients with ipsilateral symptomatic internal carotid artery occlusion Margriet Fokkema, MD, a Boudewijn L. Reichmann, MD, a Anne G. den Hartog, MD, a Catharina J. Klijn, MD, b Marc L. Schermerhorn, MD, c Frans L. Moll, MD, PhD, a and Gert Jan de Borst, MD, PhD, a Utrecht, The Netherlands; and Boston, Mass Background: Selective endarterectomy of external carotid artery (ECA) stenosis has been considered a therapeutic option for patients presenting with symptomatic ipsilateral internal carotid artery (ICA) occlusion to correct cerebral hypoperfusion or eliminate a source of emboli. However, data are scarce, and the long-term benefit of ECA revascularization remains unclear. Our objective was to study the operative results and durability of selective ECA endarterectomy in patients presenting with cerebrovascular symptoms in association with nonacute ipsilateral ICA occlusion. Methods: This was a retrospective analysis of 27 consecutive patients who underwent selective ECA endarterectomy in a single center between 2000 and All patients presented with neurologic symptoms (<6 months of surgery, 78% repeat events) referable to an ipsilateral occlusion of the ICA and concomitant stenosis of the ECA. We assessed the perioperative clinical outcome <30 days and at midterm follow-up (mean, 31.6 months). Patency was defined as freedom of duplex ultrasound detected $50% restenosis. Results: Endarterectomy of the ECA was successful in 26 patients (96.3%) with one ECA found occluded at surgery. No perioperative deaths occurred. In the 30 days after surgery, one patient developed an ipsilateral disabling ischemic stroke (3.7%), and one patient (3.7%) had a myocardial infarction. At follow-up, nine patients had died: one of a fatal ischemic stroke, six of non-vascular-related causes, and two of unknown causes. At 3 years, 83% (standard error, 8%) of patients were free from stroke or death, and 80% (standard error, 8%) of the operated-on arteries were patent. Five patients developed restenosis $50% (n [ 2, asymptomatic) or occlusion (n [ 3, one symptomatic) #3 months, and two other patients developed late asymptomatic restenosis. Conclusions: Selective endarterectomy of the ECA in symptomatic patients with an ipsilateral occlusion of the ICA is a feasible procedure with an acceptable perioperative risk. Most patients remain stroke-free during follow-up and have a low rate of symptomatic restenosis. (J Vasc Surg 2013;58: ) Focal brain region perfusion in patients with symptomatic internal carotid artery (ICA) occlusion depends on the contribution from collateral arteries. 1 In many patients, the ipsilateral external carotid artery (ECA) may form an important collateral route, mainly through the ophthalmic artery. If the ECA contains a flow-limiting high-grade stenosis, revascularization through endarterectomy of this artery may improve cerebral blood flow or eliminate a possible embolic source. 2,3 The recent Carotid Occlusion Surgery Study randomized trial showed no benefit in stroke prevention with extracranial-intracranial (EC-IC) bypass in From the Departments of Vascular Surgery a and Neurology, b University Medical Center Utrecht, Utrecht; and the Department of Vascular and Endovascular Surgery, Beth Israel Deaconess Medical Center, Boston. c Author conflict of interest: Dr Schermerhorn is a consultant for Endologix, Medtronic, and Boston Scientific. Presented as a poster presentation at the 2012 Vascular Annual Meeting of the Society for Vascular Surgery, National Harbor, Md, June 7-9, Additional material for this article may be found online at Reprint requests: Gert Jan de Borst, MD, PhD, UMC Utrecht, Department of Vascular Surgery, G04.129, PO Box 85500, 3508 GA Utrecht, The Netherlands ( g.j.deborst-2@umcutrecht.nl). The editors and reviewers of this article have no relevant financial relationships to disclose per the JVS policy that requires reviewers to decline review of any manuscript for which they may have a conflict of interest /$36.00 Copyright Ó 2013 by the Society for Vascular Surgery. patients with symptomatic occlusion and proven compromised cerebral perfusion compared with the control group receiving best medical treatment. 4 Therefore, alternative treatments for patients with symptomatic ICA occlusion are regaining interest and need to be evaluated. Few patients undergo selective endarterectomy of the ECA, and evidence on the benefit of any revascularization in patients with symptomatic ICA occlusion is still debated in the current literature. Most data on revascularization of the ECA come from observational studies based on small case series with heterogeneous patient selection However, most of these studies also included extended procedures such as carotid-subclavian bypass or EC-IC bypass surgery. At present, data on outcomes of purely and selective ipsilateral ECA endarterectomy for patients presenting with a symptomatic ICA occlusion are still limited, and the long-term benefit of selective ECA endarterectomy remains unclear. Therefore, we evaluated all patients within a large tertiary vascular surgery referral center with symptomatic nonacute ICA occlusion who underwent selective ipsilateral ECA endarterectomy and analyzed perioperative and long-term outcome. METHODS Clinical work-up. We used our prospective database on all carotid artery revascularization procedures to search 145
2 146 Fokkema et al July 2013 for consecutive patients undergoing selective revascularization of the ECA between September 2000 and August 2010 in the University Medical Center Utrecht. Patients were eligible if (1) they were scheduled for selective ipsilateral endarterectomy of the ECA (extended to the common carotid artery if necessary), (2) no adjunctive procedures were performed, (3) symptoms were ipsilateral to a nonacute ICA occlusion, (4) procedural details and 30-day outcomes were reported, and (5) follow-up data were available for at least 3 months. The indication for endarterectomy of the ECA was discussed in all patients at a weekly 1- to 2-hour multidisciplinary conference with neurologists, radiologists, and vascular surgeons as part of routine clinical practice. Data collection and follow-up. Patient characteristics and outcomes data were retrieved from electronic medical records. The general practitioner was contacted if there were any uncertainties or if additional information was required (eg, cause of death during follow-up). Imaging data were obtained from our vascular laboratory. Symptoms during regular follow-up were objectified in the outpatient clinic by an experienced independent vascular neurologist (C.K.). Patients with missing imaging data or follow-up of <2 years were contacted to undergo an additional duplex ultrasound (DUS) imaging and a consultation at the neurologist s outpatient clinic. Surgical techniques. All patients underwent surgery under general anesthesia. As a standard of practice in our clinic, cerebral function and perfusion were monitored with electroencephalography and transcranial Doppler during surgery. Findings were used in the same way as with conventional endarterectomy of the ICA. A decrease of <50% of baseline velocity in the ipsilateral middle cerebral artery on transcranial Doppler might lead to shunting as well as focal ipsilateral or bilateral decreases in amplitudes and slowing of electroencephalography waves. The final decision on whether to place a shunt was left to the discretion of the operating surgeon. A board-certified vascular surgeon performed selective endarterectomy of the ECA using the same standardized approach as for longitudinal carotid endarterectomy. The arteriotomy was carried from the CCA into the ECA beyond the distal extent of the stenosis. A standard endarterectomy plane was created and revascularization performed. The orifice of the ICA was oversewn in all cases using 5-0 Prolene suture (Ethicon, Somerville, NJ) to prevent cul-de-sac emboli. In case of persisting irregularities on the ICA origin, additional ICA ligation was performed. A patch angioplasty, consisting of autologous vein, Dacron (DuPont, Wilmington, Del), or bovine pericardium, was applied at the discretion of the operating surgeon. Autologous vein patches were harvested from the distal great saphenous vein at the ankle. Standard postoperative medical management was applied and consisted of antiplatelet drugs combined with a statin. Patients. Eight of the 35 patients initially considered for inclusion were excluded because procedures other than surgical ECA endarterectomy were performed, including one stent placement and one EC-IC bypass, five concomitant ipsilateral or contralateral procedures, and one ECA revascularization on the side of a nonoccluded ICA (>70% stenosis). The study included the remaining 27 patients, and their baseline characteristics are summarized in Table I. Patients were a mean age of 64.3 years (range, years), and 19 (70.4%) were men. DUS degree of ECA stenosis $50% was confirmed by a second imaging modality (magnetic resonance angiography or computed tomography angiography). All patients had preoperative neurologic symptoms referable to a nonacute ipsilateral ICA occlusion. The mean time from ICA occlusion (proven on imaging studies) to surgery was 8 months (range, months). Presenting symptoms included ischemic stroke in four (14.8%), hemispheric transient ischemic attack (TIA) in seven (25.9%), or any ocular symptoms in 13 (48.1%), consisting of amaurosis fugax in 11 and the syndrome of chronic ocular ischemia (SCOI, eg, blurred vision and progressive visual loss 22 )in3;inone patient, both were present. Three patients (11.1%) presented with ocular symptoms and hemispheric TIAs. All symptoms were present #6 months before surgery, and 21 patients (77.8%) experienced recurrent events. Six patients underwent ECA surgery because of a single neurologic event in combination with severe cerebrovascular atherosclerosis. The exact indication for ECA endarterectomy is outlined in the Supplementary Table (online only). Bilateral ICA occlusion was present in five patients (18.5%). End points. The primary end point was the development from any major cardiovascular adverse event, including stroke, myocardial infarction (MI), or death. The secondary end point was defined as freedom of presenting symptoms, without the development of any new minor neurologic symptoms (hemispheric TIAs or ocular symptoms, or both). The tertiary end point was patency of the treated ECA. Restenosis was defined as $50% stenosis by DUS criteria 23 (mean peak systolic velocity of the ECA $150 cm/s) or as $50% stenosis on duplex subtraction angiography, computed tomography angiography, or magnetic resonance angiography. Occlusion was defined as a 100% stenosis without blood flow. Lastly, immediate technical success and procedure-related local events, such as infection, bleeding needing reintervention, and permanent or transient cranial nerve injury (CNI) were assessed postoperatively by the operating surgeon. Results were analyzed during the perioperative period (<30 days) and at follow-up at 3 months and thereafter. Survival analyses were performed to demonstrate patency and freedom from stroke or death over time using SPSS 19.0 software (SPSS Inc, Chicago, Ill). RESULTS Perioperative outcome. The operation was technically successful in 26 patients (96.0%). Revascularization could not be performed in one patient because the ECA was occluded at the time of surgery. No patients died. One ipsilateral disabling ischemic stroke (3.7%) occurred 1 day after surgery, most likely caused by hypotension, without occlusion of
3 Volume 58, Number 1 Fokkema et al 147 Table I. Characteristics and preoperative risk factors of 27 patients who underwent external carotid endarterectomy Patient characteristics Table II. Perioperative outcome (<30 days) for 27 patients Outcome No. (%) Major outcome Death 0 (0) Stroke a 1 (3.7) Myocardial infarction 1 (3.7) Procedure-related local events Wound infection 0 (0) Bleeding 1 (3.7) Cranial nerve injury 2 (7.4) Technical success 26 (96.0) Patch used b 18 (66.7) Shunt used 1 (3.7) ICA ligation 7 (25.9) ICA, Internal carotid artery. a Ipsilateral, ischemic. b 16 venous, 1 Dacron, 1 bovine. Median (range) or No. (%) Age, years a 64.3 (48-79) Male sex 19 (70.4) Presenting symptoms b Ischemic stroke 4 (14.8) Hemispheric TIA 7 (25.9) Ocular symptoms (AFX and/or SCOI) 13 (48.1) Hemispheric TIA and ocular symptoms 3 (11.1) Time from ICA occlusion to surgery, months a 8 (0.8-37) Right side treated 16 (59.3) Contralateral ICA occlusion 5 (18.5) Risk factors Current smoker 12 (44.4) Hypertension 15 (55.6) Hypercholesterolemia 22 (81.5) Diabetes mellitus 3 (11.1) Coronary artery disease 10 (37.0) Peripheral artery disease 9 (33.3) GFR, ml/min/1.73 m ( ) Body mass index, kg/m ( ) AFX, Amaurosis fugax; GFR, glomerular filtration rate; ICA, internal carotid artery; SCOI, syndrome of chronic ocular ischemia; TIA, transient ischemic attack. a Data presented as mean (range). b All symptoms ipsilateral of side of ICA occlusion. the ECA. An asymptomatic electrocardiogram-detected MI occurred in another patient (3.7%). Procedure-related local events included transient CNI (hypoglossal nerve) in two patients (7.4%) and bleeding needing re-exploration in one (3.7%; Table II). In seven patients (25.9%), the origin of the occluded ICA was ligated (ICA orifice left in place) during the surgical procedure. A shunt was used preventively in one operation because of bilateral occlusion. The arteriotomy was closed with a patch angioplasty in 18 patients (66.7%), with an ICA transposition flap in two (7.4%), and was closed primarily in seven patients (25.9%). Outcome at 3 months. No new strokes, MIs, or deaths were noted at 3 months, but three patients had minor neurologic symptoms. In one patient who experienced amaurosis and jaw claudication, the ECA proved to be occluded on DUS imaging. Two other patients had recurrent ipsilateral amaurosis (n ¼ 1) and ipsilateral limb shaking TIAs (n ¼ 1). Relief of symptoms was obtained after starting dual-antiplatelet treatment (aspirin combined with clopidogrel) in the first patient and after endarterectomy of the contralateral ECA in the second patient. The cumulative patency rate after 3 months was 80% (standard error [SE], 8%; n ¼ 22; Fig 1). A restenosis $50% was seen in two patients (arteries closed with a patch), and the ECA appeared to be occluded in three other patients (two arteries closed primarily, one with patch). One of these occlusions (3.7%; patient described above) became symptomatic. Midterm outcome. The mean follow-up was 31.6 months (range, 3-78 months). Four patients were lost to follow-up after 3 months. Of these, two patients died, apparently of nonvascular causes, without follow-up >3 months, and one patient refused further follow-up consultation. The patient whose operation failed remained symptom-free and was therefore not further consulted after 3 months. Nine patients died during the course of follow-up; six patients died of nonvascular causes and the cause of death in two patients was unknown (both patients completed follow-up >3 years and were symptom-free). One patient sustained a fatal stroke (territory unknown) after 18 months of follow-up. This patient was known to have severe bilateral disease in both carotid and vertebral arteries, although the treated ECA stayed patent without restenosis (peak systolic velocity, 60 cm/s). At 3 years, 83% (SE, 8%) of patients were free from stroke or death (Fig 2). Three patients had minor neurologic symptoms. One patient had hemispheric TIAs and amaurosis fugax at 20 months; however, the frequency of TIAs decreased, and no progression of ocular symptoms was encountered after stenting of the ipsilateral vertebral artery to optimize cerebral blood flow. The second patient had hemispheric TIAs at 43 months of follow-up. The third patient had recurrent ipsilateral amaurosis fugax at 9 months of follow-up. In this patient, a $50% restenosis of the ECA had already been found at 3 months, but symptoms became apparent at 9 months. Two other new asymptomatic restenoses were identified (arteries closed primarily). At 3 years, 80% (SE, 8%) of arteries were patent (Fig 1). DISCUSSION On the basis of our single-center experience, ECA revascularization through endarterectomy proved to be a feasible procedure with low perioperative morbidity and mortality. Clinical results yielded one early nonfatal stroke and one late fatal stroke. Although three patients experienced early minor neurologic symptoms and three other patients developed late minor symptoms, most patients were relieved from their initial presenting symptoms. Patency at 3 months and 3 years was 80%. The results of this study indicate that external carotid endarterectomy
4 148 Fokkema et al July 2013 Fig 1. Survival analysis shows cumulative proportion of 27 patients with freedom from restenosis or occlusion after undergoing external carotid endarterectomy. SE, Standard error. Fig 2. Survival analysis shows cumulative proportion of 27 patients with freedom from nonfatal stroke or death after undergoing external carotid endarterectomy. SE, Standard error.
5 Volume 58, Number 1 Fokkema et al 149 Table III. Overview of the literature on ECA revascularization; outcome per study a Study author, Age, mean year No. b years ECA revascularization seca Other 30-day stroke/death FU, mean years Relieve/ improve of Sx, % Stroke/death/ vascular death Restenosis (Sx)/ occlusion (Sx) UMCU, / /9/1 c 4(0)/1(1) Paty, d 0 0/1 1.8 NA 0/6/4 0(0)/2(0) Karkos, / /1/1 0(0)/0(0) AbuRahma, e / /5/5 NA Harris, f 0 0/ /0/0 1(1)/0(0) Rush, f 0 0/ /6/5 3(NA)/1(NA) Boontje, (50-79) 11 g 0 0/ /5/0 NA Nicholls, NA 4 0 0/0 NA 100 1/1/1 NA Floriani, h 62 6 d 0 0/ /1/1 0(0)/0(0) Sterpetti, f 0 1/ /NA/NA 8(4)/1(1) i Friedman, d 7 d 0/ /3/2 NA Nicolosi, d 0 0/ /5/1 c NA Belkin, /0 NA 80 0/0/0 NA Santiani, j d 1 0/ /2/2 NA Gertler, k /7 NA 90 l 7/NA/8 m NA Street, n / /0/0 NA/(NA)/1(1) Fisher, n 13 o / /0/0 2(2)/0(0) Rogers, n 14 NA 14 d 0 0/0 NA NA 0/0/0 NA ECA, External carotid artery; FU, follow-up; ICA, internal carotid artery; NA, not available; seca, selective external carotid artery endarterectomy, unless otherwise indicated; Sx, symptoms; TIA, transient ischemic attack. 3 and 5 and 1 subclavian or common carotid artery-eca bypass, results not included in outcome. a Data reported as number of patients unless indicated otherwise. b All patients presenting symptomatic with ipsilateral ICA occlusion, unless otherwise indicated. c Two unknown causes of death. d Some patients had adjunctive bypasses (n ¼ 3, 3, 6, 1, 2, and 9, respectively). e All patients had bilateral occlusion. f Bilateral procedure (n ¼ 1, 2, and 3, respectively). g Three patients underwent cul-de-sac removal alone, without ECA endarterectomy. h Four of six patients had a 100% ICA stenoses. i Data available for 16 patients. j One patient had contralateral TIA. k Collective review of 23 articles. l Outcome not specified for 19%. m Data available for 196 patients. n Articles published <1978 not included in article by Gertler et al. o Two asymptomatic patients. should be considered as a treatment option for patients who most often present with repeat symptoms referable to a nonacute ICA occlusion and severe external carotid stenosis. However, the net benefit will be limited in patients with poor life expectancy and severe generalized cardiovascular disease. Symptomatic ICA occlusion has a significant annual risk of stroke of 2.4% to 6%, with the highest risk in the first 1.5 years after presentation (8%) Occlusion of the ICA may result in a hemodynamic stroke, a type of ischemic stroke that is caused by hypoperfusion rather than by embolism or local vasculopathy. 27 Neurologic symptoms may arise if the collateral pathways (via the contralateral intracranial flow via the circle of Willis, the ipsilateral ECA, or the posterior circulation) are diminished. 28 Optimization of cerebral blood flow can be considered to relieve cerebrovascular symptoms and to prevent stroke and subsequent death. 29 Few treatment options are available for these patients, with secondary preventive medication being the standard of care. Currently, no type of revascularization has been shown of proven benefit. 2,4 Earlier cohort studies, most of which were published before 1990, showed the 30-day safety of endarterectomy of the ECA in patients with established ipsilateral ICA occlusion. In a literature review that included most series published before 1987, 195 ECA endarterectomies and 23 ECA bypasses were described in symptomatic patients with ipsilateral ICA occlusion. 17 The overall 30-day neurologic complication rate was 5%, and the perioperative mortality rate was 3%. Many patients in these series received ECA surgery preceding EC-IC bypass surgery or combined with adjunctive carotid-subclavian surgery, and would thus be exposed to higher operative risk than those undergoing ECA endarterectomy alone. 30 A subsequent literature overview 1 year later of 192 selective ECA endarterectomy procedures reported that selective ECA endarterectomy alone carried a low risk, with a perioperative neurologic deficit rate of 1.6% and a mortality rate of 0%. 12
6 150 Fokkema et al July 2013 After 1988, only a few additional reports on isolated ECA endarterectomy were published. The most recent and largest single-center series involved 57 patients. 5 Although three patients had adjunctive bypasses and the eversion technique was used in 73%, the results were comparable to our study. The 30-day complications included one death, one MI, one neck hematoma, and one asymptomatic occlusion. At 3 years, stroke-free survival was 86% (SE, 7.8%), which was consistent with the 83% (SE, 8%) in the current series. An updated summary of the available literature is reported in Table III. Although these studies were not generalizable, the overall complication risk with ECA surgery was acceptably low and seems to outweigh the annual stroke risk as identified in patients with ICA occlusion without revascularization. Despite 50 years of experience with extracranial surgical techniques, the exact indications and outcome of selective ECA endarterectomy remain poorly defined. 6 There seems to be no role for ECA revascularization in asymptomatic patients with ICA occlusion or in patients presenting with a major stroke at time of occlusion of the ICA without further neurologic or ocular symptoms. 2,7 In patients without recurrent symptoms and major stroke, sufficient collateral pathways are expected to compensate for the absent ipsilateral ICA flow. None of the four patients in our cohort who presented with a single stroke experienced further neurologic events, despite occlusion or restenosis in two of these. Currently, advanced imaging techniques, such as selective arterial spin-labeled MRI, are available to aid patient selection. Selective arterial spin-labeled perfusion MRI was recently introduced as a method to assess the contribution of the individual arteries to the perfusion of the brain. 31 If the brain region supplied by the ECA contains diminished flow, ECA endarterectomy is more likely to provide benefit. 1 Although we were not able to use these new imaging techniques, they might be of help to select future patients who will benefit most from surgical intervention and to objectively determine the change in cerebral perfusion after intervention. Surgical techniques for ECA endarterectomy have been widely discussed in the literature. 11,12,19 ECA endarterectomy seems neither more risky nor more technically demanding than ICA endarterectomy. 9 Patch (venous or prosthetic) closure or closure with a part of the ICA and obliteration of the ICA stump was associated with improved patency outcome in other series. 9,12 Nine of the arteries in our series were closed primarily, most likely because the ECA had a sufficiently large lumen. Our numbers were too small to relate method of closure with patency at follow-up. Although patch ruptures have been reported as a complication, none was seen in patients with venous patches obtained from the ankle. Patients with bilateral ICA occlusion seem to have a comparable risk for subsequent ischemic stroke as patients with unilateral occlusion. 32 The risk of surgery in patients with bilateral occlusion is expected to be higher, but endarterectomy of the ECA has demonstrated low operative risk and resulted in increased cerebral perfusion and relief of symptoms. 7,17 Four of five patients in our cohort with bilateral occlusion did clinically well, and three of the five ECAs stayed patent during follow-up. Also in patients with bilateral occlusion, compensation through collateral branches other than the ECA have likely developed over time to supply adequate flow and prevent further symptoms. This study was limited by the use of retrospective data and the low incidence of selective ECA endarterectomy in a highly selected population. For example, we were not able to differentiate patients who were operated on for a hemodynamic problem from patients who were treated to eliminate a source of emboli because preoperative studies investigating flow could not be obtained. Also, the reasons for some technical decisions during surgery, such as patch and shunt use, could not be determined. However, detailed information on follow-up data was available, and the long-term clinical effect of this rare surgery could be carefully analyzed. CONCLUSIONS For patients with nonacute symptomatic ICA occlusion and symptoms referable to a low-flow state or embolic events due to ECA stenosis, selective ECA endarterectomy seems a feasible and durable treatment with low operative risk and offering freedom from major neurologic symptoms during follow-up. AUTHOR CONTRIBUTIONS Conception and design: MF, BR, AH, FM, GD Analysis and interpretation: MF, BR, AH, GD Data collection: MF, BR, AH Writing the article: MF, BR, AH, GD Critical revision of the article: MF, BR, AH, CK, MS, FM, GD Final approval of the article: MF, BR, AH, CK, MS, FM, GD Statistical analysis: MF, BR Obtained funding: Not applicable Overall responsibility: GD REFERENCES 1. van Laar PJ, van der Grond J, Bremmer JP, Klijn CJ, Hendrikse J. Assessment of the contribution of the external carotid artery to brain perfusion in patients with internal carotid artery occlusion. Stroke 2008;39: Klijn CJ, Kappelle LJ. Haemodynamic stroke: clinical features, prognosis, and management. Lancet Neurol 2010;9: Barnett HJ, Peerless SJ, Kaufmann JC. Stump on internal carotid arteryda source for further cerebral embolic ischemia. Stroke 1978;9: Powers WJ, Clarke WR, Grubb RL, Videen TO, Adams HP, Derdeyn CP. Extracranial-intracranial bypass surgery for stroke prevention in hemodynamic cerebral ischemia. JAMA 2011;306: Paty PS, Adeniyi JA, Mehta M, Darling RC 3rd, Chang BB, Kreienberg PB, et al. Surgical treatment of internal carotid artery occlusion. J Vasc Surg 2003;37: Karkos CD, Fearn SJ, McCollum CN. External carotid surgery. Vasc Endovasc Surg 2000;34:303-8.
7 Volume 58, Number 1 Fokkema et al AbuRahma AF, Copeland SE. Bilateral internal carotid artery occlusion: natural history and surgical alternatives. Cardiovasc Surg 1998;6: Harris LM, Pillai L, Ricotta JJ. External carotid endarterectomy with internal carotid artery transposition flap angioplasty for symptomatic internal carotid artery occlusion. Cardiovasc Surg 1995;3: Rush DS, Holloway WO, Fogartie JE Jr, Fine JG, Haynes JL. The safety, efficacy, and durability of external carotid endarterectomy. J Vasc Surg 1992;16:407-11; discussion: Boontje AH. External carotid artery revascularization: indications, operative techniques and results. J Cardiovasc Surg (Torino) 1992;33: Floriani M, Giulini SM, Bonardelli S, Portolani N, Cangiotti L, Tambussi U, et al. Surgical treatment of lesions obstructing the external carotid artery. J Cardiovasc Surg (Torino) 1989;30: Sterpetti AV, Schultz RD, Feldhaus RJ. External carotid endarterectomy: indications, technique, and late results. J Vasc Surg 1988;7: Friedman SG, Lamparello PJ, Riles TS, Imparato AM. Revascularization of the external carotid artery. Arch Surg 1988;123: Nicolosi A, Klinger D, Bandyk D, Towne J. External carotid endarterectomy in the treatment of symptomatic patients with internal carotid artery occlusion. Ann Vasc Surg 1988;2: Belkin M, Bucknam CA, Lowe R. Benefit of external carotid endarterectomy in patients with advanced cerebrovascular disease. Am Surg 1988;54: Satiani B, Das BM, Vasko JS. Reconstruction of the external carotid artery. Surg Gynecol Obstet 1987;164: Gertler JP, Cambria RP. The role of external carotid endarterectomy in the treatment of ipsilateral internal carotid occlusion: collective review. J Vasc Surg 1987;6: Street DL, Ricotta JJ, Green RM, DeWeese JA. The role of external carotid revascularization in the treatment of ocular ischemia. J Vasc Surg 1987;6: Fisher DF Jr, Valentine RJ, Patterson CB, Clagett GP, Fry RE, Myers SI, et al. Is external carotid endarterectomy a durable procedure? Am J Surg 1986;152: Rogers LA. Carotid angioplasty in the management of external carotid artery stenosis associated with an occluded internal carotid artery. Neurosurgery 1982;11: Nicholls SC, Bergelin R, Strandness DE. Neurologic sequelae of unilateral carotid artery occlusion: immediate and late. J Vasc Surg 1989;10:542-7; discussion: Klijn CJ, Kappelle LJ, van Schooneveld MJ, Hoppenreijs VP, Algra A, Tulleken CA, et al. Venous stasis retinopathy in symptomatic carotid artery occlusion. Stroke 2002;33: Grant EG, Benson CB, Moneta GL, Alexandrov AV, Baker JD, Bluth EI, et al. Carotid artery stenosis: grayscale and Doppler ultrasound diagnosisdsociety of Radiologists in Ultrasound consensus conference. Ultrasound Q 2003;19: Flaherty ML, Flemming KD, McClelland R, Jorgensen NW, Brown RD. Population-based study of symptomatic internal carotid artery occlusion. Stroke 2004;35:e Klijn CJ, Kappelle LJ, Algra A, van Gijn J. Outcome in patients with symptomatic occlusion of the internal carotid artery or intracranial arterial lesions: a meta-analysis of the role of baseline characteristics and type of antithrombotic treatment. Cerebrovasc Dis 2001;12: Persoon S, Luitse MJ, de Borst GJ, van der Zwan A, Algra A, Kappelle LJ, et al. Symptomatic internal carotid artery occlusion: a long-term follow-up study. J Neurol Neurosurg Psychiatry 2011;82: Bryan DS, Carson J, Hall H, He Q, Qato K, Lozanski L, et al. Natural history of carotid artery occlusion. Ann Vasc Surg 2013;27: Quinones-Baldrich WJ. Management of the occluded and nearly occluded extracranial internal carotid arteries. In: Ernst C, Stanley J, editors. Current therapy in vascular surgery. 3rd ed. Philadelphia, PA: Mosby-Year Book, Inc; p Klijn CJ, Kappelle LJ, Tulleken CA, van Gijn J. Symptomatic carotid artery occlusion: a reappraisal of hemodynamic factors. Stroke 1997;28: O Hara PJ, Hertzer NR, Beven EG. External carotid revascularization: review of a ten-year experience. J Vasc Surg 1985;2: Hendrikse J, van der Grond J, Lu H, van Zijl PC, Golay X. Flow territory mapping of the cerebral arteries with regional perfusion MRI. Stroke 2004;35: Persoon S, Klijn CJ, Algra A, Kappelle LJ. Bilateral carotid artery occlusion with transient or moderately disabling ischaemic stroke: clinical features and long-term outcome. J Neurol 2009;256: Submitted Sep 13, 2012; accepted Dec 18, Additional material for this article may be found online at
8 151.e1 Fokkema et al July 2013 Supplementary Table (online only). Patients with a single event after or during an ipsilateral internal carotid artery occlusion as their indication for surgery No. Single event Time from ICA occlusion to surgery Reasons for surgery 1 Stroke 1 month String sign contralateral ICA, ECA stenosis (>80%) 2 Amaurosis fugax 2 months Severe four-vessel disease 3 Stroke 3 weeks High-grade contralateral ICA stenosis (80%-99%) and severe bilateral ECA stenosis (>70%) 4 Stroke 6 months Bilateral ICA occlusion and severe bilateral ECA stenosis (>70%) 5 Stroke 5 months Severe four-vessel disease 6 Ocular ischemic syndrome with blindness 9 months Bilateral ICA occlusion and young age; ECA stenosis (>80%) ECA, External carotid artery; ICA, internal carotid artery.
Guidelines for Ultrasound Surveillance
 Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion
 Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
The contribution of the external carotid artery to cerebral perfusion in carotid disease
 The contribution of the external carotid artery to cerebral perfusion in carotid disease Shirley J. Fearn, PhD, FRCS, Andrew J. Picton, BSc, Andrew J. Mortimer, MD, FRCA, Andrew D. Parry, MBChB, FRCS,
The contribution of the external carotid artery to cerebral perfusion in carotid disease Shirley J. Fearn, PhD, FRCS, Andrew J. Picton, BSc, Andrew J. Mortimer, MD, FRCA, Andrew D. Parry, MBChB, FRCS,
Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary
 SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
SOCIETY FOR VASCULAR SURGERY DOCUMENT Updated Society for Vascular Surgery guidelines for management of extracranial carotid disease: Executive summary John J. Ricotta, MD, a Ali AbuRahma, MD, FACS, b
Natural history of carotid artery occlusion contralateral to carotid endarterectomy
 From the Southern Association for Vascular Surgery Natural history of carotid artery occlusion contralateral to carotid endarterectomy Ali F. AbuRahma, MD, Patrick A. Stone, MD, Shadi Abu-Halimah, MD,
From the Southern Association for Vascular Surgery Natural history of carotid artery occlusion contralateral to carotid endarterectomy Ali F. AbuRahma, MD, Patrick A. Stone, MD, Shadi Abu-Halimah, MD,
TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS
 TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS Assistant Professor of Surgery Director of Carotid Interventions Division of Vascular & Endovascular Surgery Stony Brook University
TCAR: TransCarotid Artery Revascularization Angela A. Kokkosis, MD, RPVI, FACS Assistant Professor of Surgery Director of Carotid Interventions Division of Vascular & Endovascular Surgery Stony Brook University
Endovascular Should Be Considered First Line Therapy
 Revascularization of Patients with Critical Limb Ischemia Endovascular Should Be Considered First Line Therapy Michael Conte David Dawson David L. Dawson, MD Revised Presentation Title A Selective Approach
Revascularization of Patients with Critical Limb Ischemia Endovascular Should Be Considered First Line Therapy Michael Conte David Dawson David L. Dawson, MD Revised Presentation Title A Selective Approach
Surgical Procedures for. Symptomatic Post-CAS Carotid. Restenosis: Experiences and. Mid-Term Outcomes. Lefeng Qu M.D., Ph.D. Professor of Surgery
 Surgical Procedures for Symptomatic Post-CAS Carotid Restenosis: Experiences and Mid-Term Outcomes Lefeng Qu M.D., Ph.D. Professor of Surgery Department of Vascular and Endovascular Surgery, Changzheng
Surgical Procedures for Symptomatic Post-CAS Carotid Restenosis: Experiences and Mid-Term Outcomes Lefeng Qu M.D., Ph.D. Professor of Surgery Department of Vascular and Endovascular Surgery, Changzheng
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
New Trials in Progress: ACT 1. Jon Matsumura, MD Cannes, France June 28, 2008
 New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
New Trials in Progress: ACT 1 Jon Matsumura, MD Cannes, France June 28, 2008 Faculty Disclosure I disclose the following financial relationships: Consultant, CAS training director, and/or research grants
TIA SINGOLO E IN CRESCENDO: due diversi scenari della rivascolarizzazione urgente carotidea
 TIA SINGOLO E IN CRESCENDO: due diversi scenari della rivascolarizzazione urgente carotidea R. Pini, G.L. Faggioli, M. Gargiulo, E. Pisano, A. Pilato, E. Gallitto, C. Mascoli, L.M. Cacioppa, A. Vacirca,
TIA SINGOLO E IN CRESCENDO: due diversi scenari della rivascolarizzazione urgente carotidea R. Pini, G.L. Faggioli, M. Gargiulo, E. Pisano, A. Pilato, E. Gallitto, C. Mascoli, L.M. Cacioppa, A. Vacirca,
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE?
 UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
UPMC HAMOT CAROTID ARTERY DISEASE WHERE DO WE GO FROM HERE? Richard W. Petrella M.D. FACP,FACC,FASCI DEPARTMENT CHAIRMAN CVM&S UPMC HAMOT MEDICAL CENTER 1 LEARNING OBJECTIVES REVIEW THE RISK FACTORS FOR
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO
 Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
Carotid Artery Disease and What s Pertinent JOSEPH A PAULISIN DO Goal of treatment of carotid disease Identify those at risk of developing symptoms Prevent patients at risk from developing symptoms Prevent
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
03/30/2016 DISCLOSURES TO OPERATE OR NOT THAT IS THE QUESTION CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE
 CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
CAROTID INTERVENTION IS INDICATED FOR ASYMPTOMATIC CAROTID OCCLUSIVE DISEASE Elizabeth L. Detschelt, M.D. Allegheny Health Network Vascular and Endovascular Symposium April 2, 2016 DISCLOSURES I have no
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk
 Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Preoperative risk factors for carotid endarterectomy: Defining the patient at high risk Amy B. Reed, MD, a Peter Gaccione, MA, b Michael Belkin, MD, b Magruder C. Donaldson, MD, b John A. Mannick, MD,
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Disclosures. State of the Art Management of Carotid Stenosis. NIH funding for clinical trials Consultant for Scientia Vascular and Medtronic
 State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
State of the Art Management of Carotid Stenosis Mark R. Harrigan, MD UAB Stroke Center Professor of Neurosurgery, Neurology, and Radiology University of Alabama, Birmingham Disclosures NIH funding for
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Carotid Stenosis 1/24/2019. Review of Primary Studies. NASCET- Moderate stenosis. ACAS (Asymptomatic Carotid Atherosclerosis Study) NASCET
 Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Hemodynamic effect of carotid stenting and carotid endarterectomy
 Hemodynamic effect of carotid stenting and carotid endarterectomy Peter Jan van Laar, MD, a Jeroen van der Grond, PhD, b Frans L. Moll, MD, PhD, c Willem P. Th. M. Mali, MD, PhD, a and Jeroen Hendrikse,
Hemodynamic effect of carotid stenting and carotid endarterectomy Peter Jan van Laar, MD, a Jeroen van der Grond, PhD, b Frans L. Moll, MD, PhD, c Willem P. Th. M. Mali, MD, PhD, a and Jeroen Hendrikse,
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Fast-track CEA: a 3-year experience
 Fast-track CEA: a 3-year experience Giorgio L. Poletto, MD Milano, Italy 6th ACST-2 Collaborators Meeting, Palau de Congresos, Valencia. 24th and 25th September 2018. Stroke prevention Primary prevention:
Fast-track CEA: a 3-year experience Giorgio L. Poletto, MD Milano, Italy 6th ACST-2 Collaborators Meeting, Palau de Congresos, Valencia. 24th and 25th September 2018. Stroke prevention Primary prevention:
Amaurosis fugax: some aspects of management
 Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY
 GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
GUIDELINE FOR RECOVERY ROOM MANAGEMENT OF PATIENTS AFTER CAROTID ENDARTERECTOMY Full Title of Guideline: Author (include email and role): Guideline for Recovery Room Management of Patients after Carotid
Axillary-to-carotid artery bypass grafting for symptomatic severe common carotid artery occlusive disease
 Axillary-to-carotid artery bypass grafting for symptomatic severe common carotid artery occlusive disease Joseph P. Archie, Jr, PhD, MD, Raleigh, NC Purpose: Revascularization of the internal or external
Axillary-to-carotid artery bypass grafting for symptomatic severe common carotid artery occlusive disease Joseph P. Archie, Jr, PhD, MD, Raleigh, NC Purpose: Revascularization of the internal or external
Daniel S. Rush, MD, William O. Holloway, MD, James E. Fogartie, Jr., MD, Joseph G. Fine, MD, and James L. Haynes, MD, Columbia and Greenwood, S.C.
 The safety, efficacy, and carotid endarterectomy durability of external Daniel S. Rush, MD, William. Holloway, MD, James E. Fogartie, Jr., MD, Joseph G. Fine, MD, and James L. Haynes, MD, Columbia and
The safety, efficacy, and carotid endarterectomy durability of external Daniel S. Rush, MD, William. Holloway, MD, James E. Fogartie, Jr., MD, Joseph G. Fine, MD, and James L. Haynes, MD, Columbia and
The outcome of external carotid endarterectomy during routine carotid endarterectomy
 The outcome of external carotid endarterectomy during routine carotid endarterectomy Joseph P. Archie, Jr, PhD, MD, Raleigh, NC Purpose: This study is an analysis of the outcome of a common method of management
The outcome of external carotid endarterectomy during routine carotid endarterectomy Joseph P. Archie, Jr, PhD, MD, Raleigh, NC Purpose: This study is an analysis of the outcome of a common method of management
Internal Carotid Artery Occlusion: Clinical and Therapeutic Implications
 94 Internal Carotid Artery Occlusion: Clinical and Therapeutic Implications VIVIAN U. FRITZ, M.D., CHRIS L. VOLL, M.D., AND LEWIS J. LEVIEN, M.D., PH.D. Downloaded from http://ahajournals.org by on November
94 Internal Carotid Artery Occlusion: Clinical and Therapeutic Implications VIVIAN U. FRITZ, M.D., CHRIS L. VOLL, M.D., AND LEWIS J. LEVIEN, M.D., PH.D. Downloaded from http://ahajournals.org by on November
Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA
 Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA SUNY DOWNSTATE MEDICAL CENTER Case 61 year old male referred to Vascular Surgery for left internal carotid stenosis Presented with transient
Management of Carotid Disease CHRISTOPHER LAU PGY-3 BROOKLYN VA SUNY DOWNSTATE MEDICAL CENTER Case 61 year old male referred to Vascular Surgery for left internal carotid stenosis Presented with transient
CEA and cerebral protection Volodymyr labinskyy, MD
 CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease
 Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease Jan M. Sloves RVT, RCS, FASE Technical Director New York Cardiovascular Associates Disclosures
Beyond Stenosis Severity: Top 5 Important Duplex Characteristics to Identify in a Patient with Carotid Disease Jan M. Sloves RVT, RCS, FASE Technical Director New York Cardiovascular Associates Disclosures
Reduction of flow velocities in patients with ischemic events in the middle cerebral artery long-term follow-up with ultrasound
 Acta Neurol. Belg., 20,, -5 Original articles Reduction of flow velocities in patients with ischemic events in the middle cerebral artery long-term follow-up with ultrasound Christine Kremer and Kasim
Acta Neurol. Belg., 20,, -5 Original articles Reduction of flow velocities in patients with ischemic events in the middle cerebral artery long-term follow-up with ultrasound Christine Kremer and Kasim
DESCRIPTION: Percent of asymptomatic patients undergoing CEA who are discharged to home no later than post-operative day #2
 Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Treatment Considerations for Carotid Artery Stenosis. Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery
 Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
Treatment Considerations for Carotid Artery Stenosis Danielle Zielinski, RN, MSN, ACNP Rush University Neurosurgery 4.29.2016 There is no actual or potential conflict of interest in regards to this presentation
a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers
 The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
The study a physician-initiated study investigating the RoadSaver stent in carotid lesions Dr. Michel Bosiers Conflict of interest have the following potential conflicts of interest to report: Consulting
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Measure #260: Rate of Carotid Endarterectomy (CEA) for Asymptomatic Patients, without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Patient Safety
Predictors of restenosis and cardiovascular events in patients undergoing percutaneous angioplasty for subclavian/innominate artery stenosis
 Predictors of restenosis and cardiovascular events in patients undergoing percutaneous angioplasty for subclavian/innominate artery stenosis Tadeusz Przewlocki, Anna Kablak Ziembicka, Piotr Pieniazek,
Predictors of restenosis and cardiovascular events in patients undergoing percutaneous angioplasty for subclavian/innominate artery stenosis Tadeusz Przewlocki, Anna Kablak Ziembicka, Piotr Pieniazek,
The superiority of synthetic arterial grafts over autologous veins in carotid-subclavian bypass
 The superiority of synthetic arterial grafts over autologous veins in carotid-subclavian bypass Stanley Ziomek, M.D., William J. Quifiones-Baldrich, M.D., Ronald W. Busuttil, M.D., Ph.D., J. Dennis Baker,
The superiority of synthetic arterial grafts over autologous veins in carotid-subclavian bypass Stanley Ziomek, M.D., William J. Quifiones-Baldrich, M.D., Ronald W. Busuttil, M.D., Ph.D., J. Dennis Baker,
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for
 Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease
 The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease GJ de Borst Department of Vascular Surgery RECOMMENDATION GRADING CRITERIA What is new
The most important recommendations from the 2017 ESVS/ESC guideline on the management of carotid artery disease GJ de Borst Department of Vascular Surgery RECOMMENDATION GRADING CRITERIA What is new
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase <48h)
 Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Symptomatic Internal Carotid Artery Occlusion: A long-term follow-up study
 Symptomatic Internal Carotid Artery Occlusion: A long-term follow-up study Suzanne Persoon, Merel Luitse, Gert Jan De Borst, Albert Van Der Zwan, Ale Algra, L. Jaap Kappelle, Catharina J.M. Klijn To cite
Symptomatic Internal Carotid Artery Occlusion: A long-term follow-up study Suzanne Persoon, Merel Luitse, Gert Jan De Borst, Albert Van Der Zwan, Ale Algra, L. Jaap Kappelle, Catharina J.M. Klijn To cite
Cerebrovascular Disease. RTC Conference Resident Presenter: Dr. Christina Bailey Faculty: Dr. Jeff Dattilo October 2, 2009
 Cerebrovascular Disease RTC Conference Resident Presenter: Dr. Christina Bailey Faculty: Dr. Jeff Dattilo October 2, 2009 Cerebrovascular Disease Stroke is the 3 rd leading cause of death and the leading
Cerebrovascular Disease RTC Conference Resident Presenter: Dr. Christina Bailey Faculty: Dr. Jeff Dattilo October 2, 2009 Cerebrovascular Disease Stroke is the 3 rd leading cause of death and the leading
Protokollanhang zur SPACE-2-Studie Neurology Quality Standards
 Protokollanhang zur SPACE-2-Studie Neurology Quality Standards 1. General remarks In contrast to SPACE-1, the neurological center participating in the SPACE-2 trial will also be involved in the treatment
Protokollanhang zur SPACE-2-Studie Neurology Quality Standards 1. General remarks In contrast to SPACE-1, the neurological center participating in the SPACE-2 trial will also be involved in the treatment
Lecture Outline: 1/5/14
 John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
Feasibility of Endovascular Recanalization for Symptomatic Cervical Internal Carotid Artery Occlusion
 Journal of the American College of Cardiology Vol. 49, No. 7, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.11.029
Journal of the American College of Cardiology Vol. 49, No. 7, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.11.029
Limitations of Other Embolic Protection Devices - Filters. Carotid Stenting with Flow Reversal. Limitations of Distal Occlusion
 Carotid Stenting with Flow Reversal Marc Schermerhorn, MD Division of Vascular and Endovascular Surgery Beth Israel Deaconess Center Boston, MA Limitations of Other Embolic Protection Devices - Filters
Carotid Stenting with Flow Reversal Marc Schermerhorn, MD Division of Vascular and Endovascular Surgery Beth Israel Deaconess Center Boston, MA Limitations of Other Embolic Protection Devices - Filters
Carotid Artery Stenosis
 Evidence-Based Approach to Carotid Artery Stenosis Seong-Wook Park, MD Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea Carotid Artery Stenosis Carotid
Evidence-Based Approach to Carotid Artery Stenosis Seong-Wook Park, MD Division of Cardiology, Asan Medical Center University of Ulsan College of Medicine, Seoul, Korea Carotid Artery Stenosis Carotid
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Carotid Artery Stenting Today: A Few Updating Remarks
 Carotid Artery Stenting Today: A Few Updating Remarks Camilo R. Gomez, MD, MBA Director, Alabama Neurological Institute Birmingham, Alabama Disclaimer & Warning Company Pharmaceutical BMS-Sanofi-Aventis
Carotid Artery Stenting Today: A Few Updating Remarks Camilo R. Gomez, MD, MBA Director, Alabama Neurological Institute Birmingham, Alabama Disclaimer & Warning Company Pharmaceutical BMS-Sanofi-Aventis
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH
 ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
ESC Congress 2011 SIMULTANEOUS HYBRID REVASCULARIZATION OF CAROTID AND CORONARY DISEASE IN PATIENTS WITH ACUTE CORONARY SYNDROME: INITIAL RESULTS OF A NEW THERAPEUTIC APPROACH AUTHORS: Marta Ponte 1, RICARDO
Advances in the treatment of posterior cerebral circulation symptomatic disease
 Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Extracranial Carotid Artery Stenting With or Without Distal Protection Device
 Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
Extracranial Carotid Artery Stenting With or Without Distal Protection Device Eak-Kyun Shin MD. Professor of Medicine Division of Cardiology, Heart Center, Gil Medical Center Gacheon Medical School Incheon,
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Quality ID #345 (NQF 1543): Rate of Asymptomatic Patients Undergoing Carotid Artery Stenting (CAS) Who Are Stroke Free or Discharged Alive National Quality Strategy Domain: Effective Clinical Care 2018
Quality ID #345 (NQF 1543): Rate of Asymptomatic Patients Undergoing Carotid Artery Stenting (CAS) Who Are Stroke Free or Discharged Alive National Quality Strategy Domain: Effective Clinical Care 2018
ORIGINAL CONTRIBUTION. Long-term Risk of Stroke and Other Vascular Events in Patients With Asymptomatic Carotid Artery Stenosis
 ORIGINAL CONTRIBUTION Long-term Risk of Stroke and Other Vascular Events in Patients With Asymptomatic Carotid Artery Stenosis Zurab G. Nadareishvili, MD, PhD; Peter M. Rothwell, MD, PhD; Vadim Beletsky,
ORIGINAL CONTRIBUTION Long-term Risk of Stroke and Other Vascular Events in Patients With Asymptomatic Carotid Artery Stenosis Zurab G. Nadareishvili, MD, PhD; Peter M. Rothwell, MD, PhD; Vadim Beletsky,
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Outcome
 Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
Measure #344: Rate of Carotid Artery Stenting (CAS) for Asymptomatic Patients, Without Major Complications (Discharged to Home by Post-Operative Day #2) National Quality Strategy Domain: Effective Clinical
Carotid endarterectomy to correct asymptomatic carotid stenosis: Ten years
 Carotid endarterectomy to correct asymptomatic carotid stenosis: Ten years later David Rosenthal, M.D., Randal Rudderman, M.D., Edgar Borrero, M.D., David H. Hafner, M.D., Garland D. Perdue, M.D., Pano
Carotid endarterectomy to correct asymptomatic carotid stenosis: Ten years later David Rosenthal, M.D., Randal Rudderman, M.D., Edgar Borrero, M.D., David H. Hafner, M.D., Garland D. Perdue, M.D., Pano
Contemporary management of brachiocephalic occlusive disease. TM Sullivan Minneapolis, MN
 Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Management of cervicocephalic arterial dissection. Ciro G. Randazzo, MD, MPH Thomas Jefferson University Hospital, Department of Neurosurgery
 Management of cervicocephalic arterial dissection Ciro G. Randazzo, MD, MPH Thomas Jefferson University Hospital, Department of Neurosurgery Definition Disruption of arterial wall, either at level of intima-media
Management of cervicocephalic arterial dissection Ciro G. Randazzo, MD, MPH Thomas Jefferson University Hospital, Department of Neurosurgery Definition Disruption of arterial wall, either at level of intima-media
Distal vertebral artery reconstruction: Long-term outcome
 Distal vertebral artery reconstruction: Long-term outcome Edouard Kieffer, MD, Barbara Praquin, MD, Laurent Chiche, MD, Fabien Koskas, MD, and Amine Bahnini, MD, Paris, France Purpose: The purpose of this
Distal vertebral artery reconstruction: Long-term outcome Edouard Kieffer, MD, Barbara Praquin, MD, Laurent Chiche, MD, Fabien Koskas, MD, and Amine Bahnini, MD, Paris, France Purpose: The purpose of this
Carotid Revascularization
 Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Intervention versus standard medical treatment in patients with symptomatic occlusion of the internal carotid artery: a randomised oxygen-15 PET study
 Persoon et al. EJNMMI Research 2013, 3:79 ORIGINAL RESEARCH Open Access Intervention versus standard medical treatment in patients with symptomatic occlusion of the internal carotid artery: a randomised
Persoon et al. EJNMMI Research 2013, 3:79 ORIGINAL RESEARCH Open Access Intervention versus standard medical treatment in patients with symptomatic occlusion of the internal carotid artery: a randomised
Carotid Artery Stenting (CAS) Pathophysiology. Technical Considerations. Plaque characteristics: relevant concepts. CAS and CEA
 Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Carotid Artery Stenting (CAS) Carotid Artery Stenting for Stroke Risk Reduction Matthew A. Corriere MD, MS, RPVI Assistant Professor of Surgery Department of Vascular and Endovascular Surgery Rationale:
Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
 Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
Journal of Neuroendovascular Therapy 2017; 11: 371 375 Online March 3, 2017 DOI: 10.5797/jnet.cr.2016-0114 Posterior Cerebral Artery Aneurysms with Common Carotid Artery Occlusion: A Report of Two Cases
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
CHAPTER 5. Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms
 CHAPTER 5 Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms Christine A.C. Wijman, Joao A. Gomes, Michael R. Winter, Behrooz Koleini, Ippolit C.A. Matjucha, Val E. Pochay, Viken L.
CHAPTER 5 Symptomatic and Asymptomatic Retinal Embolism Have Different Mechanisms Christine A.C. Wijman, Joao A. Gomes, Michael R. Winter, Behrooz Koleini, Ippolit C.A. Matjucha, Val E. Pochay, Viken L.
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION
 FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 93875 Non-invasive physiologic studies of extracranial arteries, complete bilateral study (eg, periorbital
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 93875 Non-invasive physiologic studies of extracranial arteries, complete bilateral study (eg, periorbital
Extracranial to intracranial bypass for intracranial atherosclerosis
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
Assessment of the procedural etiology of stroke resulting from carotid artery stenting
 Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Assessment of the procedural etiology of stroke resulting from carotid artery stenting 1. Study Purpose and Rationale: A. Background Stroke is the 3 rd leading cause of death in the United States and carries
Special Topic Section
 Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
Special Topic Section Cerebrovasc Dis 2004;18:69 74 DOI: 10.1159/000078753 Received: March 8, 2004 Accepted: March 8, 2004 Published online: June 1, 2004 International Carotid Stenting Study: Protocol
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
Internal carotid artery near-total occlusions: Is it justified to operate on them?
 Internal carotid artery near-total occlusions: Is it justified to operate on them? Christos D. Liapis Professor (Em) of Vascular Surgery Athens University Medical School Director Vascular & Endovascular
Internal carotid artery near-total occlusions: Is it justified to operate on them? Christos D. Liapis Professor (Em) of Vascular Surgery Athens University Medical School Director Vascular & Endovascular
Randomized trial of vein versus Dacron patching during carotid endarterectomy: Long-term results
 Randomized trial of vein versus Dacron patching during carotid endarterectomy: Long-term results Ross Naylor, MD, FRCS, a Paul D. Hayes, FRCS, a David A. Payne, FRCS, a Holger Allroggen, MD, MRCP, b Sarah
Randomized trial of vein versus Dacron patching during carotid endarterectomy: Long-term results Ross Naylor, MD, FRCS, a Paul D. Hayes, FRCS, a David A. Payne, FRCS, a Holger Allroggen, MD, MRCP, b Sarah
CAROTID DEBATE High-Grade Asymptomatic Disease Should Be Repaired Selectively; Medical Management is NOT Enough
 Todd W GenslerMD April 28, 2018 CAROTID DEBATE High-Grade Asymptomatic Disease Should Be Repaired Selectively; Medical Management is NOT Enough DISCLOSURES I have no financial disclosures Presenter name
Todd W GenslerMD April 28, 2018 CAROTID DEBATE High-Grade Asymptomatic Disease Should Be Repaired Selectively; Medical Management is NOT Enough DISCLOSURES I have no financial disclosures Presenter name
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Field Strength. Regional Perfusion Imaging (RPI) matches cerebral arteries to flow territories
 Field Strength Changing how the world looks at MR. Regional Perfusion Imaging (RPI) matches cerebral arteries to flow territories Research groups in Utrecht, Baltimore and Singapore collaborate on this
Field Strength Changing how the world looks at MR. Regional Perfusion Imaging (RPI) matches cerebral arteries to flow territories Research groups in Utrecht, Baltimore and Singapore collaborate on this
Carotid Stenosis (carotid artery disease)
 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
Carotid Artery Stenting
 Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Carotid Artery Stenting Woong Chol Kang M.D. Gil Medical Center, Gachon University of Medicine and Science, Incheon, Korea Carotid Stenosis and Stroke ~25% of stroke is due to carotid disease, the reminder
Edinburgh Research Explorer
 Edinburgh Research Explorer No evidence that severity of stroke in internal carotid occlusion is related to collateral arteries Citation for published version: Mead, GE, Wardlaw, JM, Lewis, SC, Dennis,
Edinburgh Research Explorer No evidence that severity of stroke in internal carotid occlusion is related to collateral arteries Citation for published version: Mead, GE, Wardlaw, JM, Lewis, SC, Dennis,
Clinical Decision Making: Hyperacute Management of Symptomatic Carotid Artery Disease
 Clinical Decision Making: Hyperacute Management of Symptomatic Carotid Artery Disease Tarvinder Singh, MS, MD Neurohospitalist Swedish Neuroscience Institute 1 Objectives Definition Why the urgency? Evidence/Guidelines
Clinical Decision Making: Hyperacute Management of Symptomatic Carotid Artery Disease Tarvinder Singh, MS, MD Neurohospitalist Swedish Neuroscience Institute 1 Objectives Definition Why the urgency? Evidence/Guidelines
EVAR replaced standard repair in most cases. Why?
 EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
Stroke prevention by carotid endarterectomy. Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p
 Title Stroke prevention by carotid endarterectomy Author(s) Lau, H; Cheng, SWK Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p. 484-490 Issued Date 1998 URL http://hdl.handle.net/10722/45393 Rights
Title Stroke prevention by carotid endarterectomy Author(s) Lau, H; Cheng, SWK Citation Hong Kong Practitioner, 1998, v. 20 n. 9, p. 484-490 Issued Date 1998 URL http://hdl.handle.net/10722/45393 Rights
Carotid Artery Revascularization: Current Strategies. Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014
 Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Carotid Artery Revascularization: Current Strategies Shonda Banegas, D.O. Vascular Surgery Carondelet Heart and Vascular Institute September 6, 2014 Disclosures None 1 Stroke in 2014 Stroke kills almost
Alma Mater Studiorum Università di Bologna
 Alma Mater Studiorum Università di Bologna S.Orsola-Malpighi, Bologna, Italia Chirurgia Vascolare The volume of cerebral ischaemic lesion predicts the outcome after symptomatic carotid revascularisation
Alma Mater Studiorum Università di Bologna S.Orsola-Malpighi, Bologna, Italia Chirurgia Vascolare The volume of cerebral ischaemic lesion predicts the outcome after symptomatic carotid revascularisation
GUNDERSEN/LUTHERAN ULTRASOUND DEPARTMENT POLICY AND PROCEDURE MANUAL
 GUNDERSEN/LUTHERAN ULTRASOUND DEPARTMENT POLICY AND PROCEDURE MANUAL SUBJECT: Carotid Duplex Ultrasound SECTION: Vascular Ultrasound ORIGINATOR: Deborah L. Richert, BSVT, RDMS, RVT DATE: October 15, 2015
GUNDERSEN/LUTHERAN ULTRASOUND DEPARTMENT POLICY AND PROCEDURE MANUAL SUBJECT: Carotid Duplex Ultrasound SECTION: Vascular Ultrasound ORIGINATOR: Deborah L. Richert, BSVT, RDMS, RVT DATE: October 15, 2015
