Important role of mechanical circulatory support in acute myocardial infarction complicated by cardiogenic shock
|
|
|
- Melvin Blankenship
- 5 years ago
- Views:
Transcription
1 European Journal of Cardio-Thoracic Surgery 48 (2015) doi: /ejcts/ezu478 Advance Access publication 4 December 2014 ORIGINAL ARTICLE Cite this article as: Truby L, Naka Y, Kalesan B, Ota T, Kirtane AJ, Kodali S et al. Important role of mechanical circulatory support in acute myocardial infarction complicated by cardiogenic shock. Eur J Cardiothorac Surg 2015;48: Important role of mechanical circulatory support in acute myocardial infarction complicated by cardiogenic shock Lauren Truby a, Yoshifumi Naka a, Bindu Kalesan a, Takeyoshi Ota a, Ajay J. Kirtane b, Susheel Kodali b, Natasha Nikic a, Lily Mundy a, Paolo Colombo b, Ulrich P. Jorde b and Hiroo Takayama a, * a Department of Surgery, Columbia University Medical Center, New York, NY, USA b Department of Medicine, Columbia University Medical Center, New York, NY, USA * Corresponding author. 177 Fort Washington Ave, New York, NY 10032, USA. Tel: ; fax: ; hirofu2@hotmail.com (H. Takayama). Received 29 July 2014; received in revised form 21 October 2014; accepted 31 October 2014 Abstract OBJECTIVES: Acute myocardial infarction (AMI) complicated by cardiogenic shock (CS) remains associated with significant mortality despite the widespread application of early revascularization strategies. Recent evidence suggests that the use of intra-aortic balloon pump (IABP) counterpulsation does not improve mortality in this cohort of patients. We summarize our experience with mechanical circulatory support (MCS) therapy for AMI/CS. METHODS: This is a retrospective review of 61 patients who received MCS therapy for AMI/CS at our institution between March 2007 and March RESULTS: Mean age was 60.2 ± 10.3 years; mean ejection fraction was 24 ± 15% and 29% of patients were receiving active cardiopulmonary resuscitation at the time of support initiation. Prior to the initiation of MCS, 70.5% of patients had an IABP. Mean arterial pressure improved significantly with MCS (63 mmhg prior to MCS, 82 mmhg after MCS, P 0.01). Mean length of support was 9.5 ± 11.0 days, and overall survival to 30 days was 59.0%. Among 30-day survivors, 44.4% required device exchange to a durable MCS device. Ultimately, only 31% (52.8% of patients who survived to 30 days) achieved myocardial recovery. CONCLUSIONS: Short-term MCS therapy with subsequent aggressive use of durable MCS device may improve the unacceptably high mortality rate in AMI/CS. Rigorous prospective studies of MCS therapy in AMI/CS are warranted. Keywords: Acute myocardial infarction Mechanical circulatory support INTRODUCTION Despite decades of progress in risk factor modification and pharmacological therapy, Americans are hospitalized for new acute myocardial infarction (AMI) every year and will have a recurrent attack. Although the rates of death related to cardiovascular disease are declining, the burden of disease remains high, with coronary heart disease alone accounting for one in every six deaths in the USA [1]. Among these patients, cardiogenic shock (CS) is not uncommon, estimated to complicate 7 10% of AMIs [2]. Despite trends towards aggressive and early revascularization, mortality of AMI/CS continues to be 50 60%, approaching 80 90% in those with severe haemodynamic compromise [3]. Recently, the results of the Intra-Aortic Balloon Pump in Cardiogenic Shock II (IABP-SHOCK II) trial failed to demonstrate a mortality benefit with the use of intra-aortic balloon pump (IABP) counterpulsation a widely used adjuvant therapy in AMI/CS [4]. In light of the high mortality of AMI/CS and the failure of IABP to improve outcomes, the study of novel and innovative devices and therapies for AMI/CS is warranted [5]. Prior reported series of mechanical circulatory support (MCS) therapy for AMI/CS have been small and anecdotal [6 9]. Herein, we report our 6-year experience with MCS therapy for patients with AMI/CS. METHODS This is a retrospective, institutional review board-approved review of 61 patients who received MCS therapy for CS following AMI between March 2007 and March Due to the retrospective nature of the study, informed consent was waived. CS was defined as a state of organ hypoperfusion characterized by the following: (i) a systolic blood pressure of less than 90 mmhg for more than 30 min in the absence of hypovolaemia or pharmacological agents (e.g. vasopressors) required to achieve a systolic pressure of 90 mmhg, (ii) a decline in cardiac index The Author Published by Oxford University Press on behalf of the European Association for Cardio-Thoracic Surgery. All rights reserved.
2 L. Truby et al. / European Journal of Cardio-Thoracic Surgery 323 (<1.8 l/min/m 2 without support or <2.2 l/min/m 2 with support) or (iii) elevated left ventricular (LV) filling pressures ( pulmonary capillary wedge pressure >18 mmhg) [10]. Our strategy for treating CS has been previously reported [11]. Patients presenting with ST-elevation AMI to our institution proceed directly to the catheterization laboratory for emergent revascularization whenever feasible. For patients with cardiopulmonary arrest or severe haemodynamic instability at any point during their hospital course, the interdisciplinary MCSD team is called to evaluate the patient. Prior to initiation of MCS, patients at our institution generally receive pharmacologic haemodynamic support and, in many cases, an IABP or other percutaneous ventricular assist device (VAD). Our devices of choice for acute circulatory support include percutaneous VADs [Impella 2.5, 5.0, CP (Abiomed, Inc., Danvers, MA, USA) and TandemHeart (CardiacAssist, Inc., Pittsburgh, PA, USA)], venoarterial extracorporeal membranous oxygenation (VA-ECMO) and a surgically placed short-term VAD [CentriMag VAD (Thoratec, Corp., Pleasanton, CA, USA)]. Only VA-ECMO and CentriMag VAD were considered to be a mechanical circulatory support device (MCSD) in the present study. We do not consider IABP and Impella 2.5 as devices of choice for severe CS due to insufficient circulatory support. In addition, our use of other percutaneous VADs is limited. Generally, biventricular support with the shortterm VAD is preferred for CS [12]. Generally, the inflow and outflow cannulation sites of the left ventricular assist device (LVAD) are the LV apex and ascending aorta, whereas those of the right ventricular assist device are the right atrium and the main pulmonary artery. The detailed insertion technique of the short-term VAD is described elsewhere [12]. In those patients with unknown mental status, severe coagulopathy, or who are too unstable to go to the operating room, VA-ECMO is utilized (Fig. 1). Whenever feasible, VA-ECMO is inserted percutaneously; the arterial cannula of Fr through the femoral artery and the venous cannula of Fr through the femoral vein. When ipsilateral pedal pulse signal is absent with Doppler examination, a 6- to 10-Fr cannula was inserted under surgical cut down into the superficial femoral artery to perfuse the limb. VA-ECMO is exchanged to a short-term VAD when prolonged support (>7 days) is expected. We do not use durable MCSDs as bridge-to-decision devices. While supported with the short-term device, patients are managed by the multidisciplinary MCSD team, and undergo evaluation for heart transplantation or implantable LVAD for destination therapy. Once a patient s general condition improves, the patient s myocardial function is evaluated by weaning the device under echocardiographic and haemodynamic monitoring. Depending on the result of these weaning studies and eligibility for heart replacement therapy, the short-term device can be explanted as a transition to one of the following destinations: durable MCSD, myocardial recovery or heart transplantation. For patients undergoing device exchange to durable MCSD, HeartMate XVE, or more recently HeartMate II and HVAD, LVADs are used for patients who need only left ventricular support. Thoratec Paracorporeal VAD, Implantable VAD or a total artificial heart are considered for those who need biventricular support. Basic demographics, past medical history and information regarding patient s hospital stay were collected. Laboratory values, haemodynamic parameters and use of inotropes and vasopressors were recorded immediately prior to and 24 h after initiation of the mechanical support. Data from the catheterization laboratory at the time of revascularization were also included. If the patient underwent right heart catheterization within 24 h prior to MCS, cardiac power output (CPO) was calculated as mean arterial pressure (MAP) CO/451. In patients who were undergoing active cardiopulmonary resuscitation (CPR), the following values were assigned: a systolic blood pressure of 60 mmhg, a diastolic blood pressure of 20 mmhg and a cardiac index of 0 l/min/m 2 [13]. These values were chosen to represent the haemodynamic effect of adequate chest compressions in accordance with the prior studies. Outcomes The primary outcome of interest was 30-day mortality. Other outcomes of interest included survival to discharge and myocardial recovery (defined as survival to 30 days or discharge from the hospital and recovery of native heart function as evidenced by ability TX & MCS Figure 1: Acute MCS decision algorithm. AMI: acute myocardial infarction; OR: operating room; VA-ECMO: venoarterial extracorporeal membranous oxygenation; LVAD: left ventricular assist device; OHT: orthotopic heart transplant.
3 324 L. Truby et al. / European Journal of Cardio-Thoracic Surgery Table 1: Patient demographics and preoperative characteristics by device Overall VA-ECMO CM P-value n =61 n =38 n =23 Age in years, mean ± SD 60.2 ± ± ± Male gender, % (n) 69 (42) 66 (25) 74 (17) 0.51 BMI (kg/m 2 ), mean ± SD 28.6 ± ± ± Hypertension, % (n) 56 (34) 53 (20) 61 (14) 0.53 Hyperlipidaemia, % (n) 46 (28) 42 (16) 52 (12) 0.44 Diabetes mellitus, % (n) 46 (28) 47 (18) 44 (10) 0.76 IABP, % (n) 71 (43) 55 (21) 96 (22) SBP (mmhg), mean ± SD 92.1 ± ± ± DBP (mmhg), mean ± SD 49.0 ± ± ± MAP (mmhg), mean ± SD 63.0 ± ± ± CVP (mmhg), mean ± SD 12.0 ± ± ± Lactate (mg/dl), median (IQR) 3.3 ( ) 3.0 ( ) 3.4 ( ) 0.55 ph, mean ± SD 7.3 ± ± ± Creatinine (mg/dl), mean ± SD 1.8 ± ± ± Active CPR, % (n) 29 (17) 37 (14) 14 (3) 0.07 VA-ECMO: venoarterial extracorporeal membranous oxygenation; CM: CentriMag; BMI: body mass index; IABP: intra-aortic balloon pump; SBP: systolic blood pressure; DBP: diastolic blood pressure; MAP: mean arterial pressure; CVP: central venous pressure; CPR: cardiopulmonary resuscitation; SD: standard deviation. to wean from mechanical support). Other outcomes included device exchange to a durable MCSD and orthotopic heart transplantation. Adverse events including infection, cerebrovascular accident and bleeding were defined according to the INTERMACS criteria. Statistical analysis Data are presented using mean values and standard deviations (SDs) for continuous variables and percentages for categorical variables. Those variables that are non-normally distributed are presented as medians and IQRs. Fisher s exact t-tests were used for comparison of means and Pearson s χ 2 test was used to compare categorical variables. Kruskal Wallis tests were used for non-parametric variables. Continuous variables were dichotomized using clinically appropriate thresholds. Because of the small number of patients reviewed and lack of sufficient power, univariate and multivariate analysis was not performed. Probit regression was used to generate predicted in-hospital mortality for varying levels of CPO. All Kaplan Meier survival estimates were created using survival days to last established contact with the patient. Stata/SE version 13 (STATA Corporation, College Station, TX, USA) was used for statistical analysis. RESULTS Patient characteristics Among over 400 patients who presented to our institution with ST-elevation AMI during the study period, a total of 61 patients received MCS therapy for AMI/CS. Initial MCSD was VA-ECMO in 38 patients and a short-term VAD in 23 patients. The average age of the patient was 60.2 ± 10.3 years and 69% were male (Table 1). Forty-eight percent of patients had triple-vessel coronary artery disease, when compared with 28% with two-vessel and 25% with Table 2: Distribution of coronary lesions and correlates of myocardial dysfunction Culprit vessel n =61 % LAD Left main Left circumflex 2 3 OM1, OM2 3 5 RCA 3 5 Coronary artery disease n =61 % Single vessel Double vessel Triple Revascularized Peak troponin ± Preop ejection fraction 24.3 ± 14.5 LAD: left anterior descending artery; OM: obtuse marginal artery; RCA: right coronary artery. single-vessel disease (Table 2). The culprit vessel was the LAD in 69% with the left main coronary artery being the second most common (16%). Seventy-five percent of patients were revascularized on the day of presentation with almost 90% undergoing primary PCI, with a median time to MCS of 1 day and mean of 4.0 ± 7.3 days. Overall, 71% of patients had an IABP placed prior to initiation of MCS therapy and 14.8% had a percutaneous VAD [Impella 2.5 LP (Abiomed, Inc.)]. Twenty-nine percent of patients were undergoing active chest compressions at the time of support initiation (37% of VA-ECMO patients). Mean peak troponin was ± µg/l with a median of 76.6 µg/l, and the mean preoperative ejection fraction of the overall cohort was 24 ± 15%. Mean length of support was 9.5 ± 11.0 days (3.8 ± 2.5 days for VA-ECMO and 18.8 ± 13.3 days for short-term VAD). Nine patients initially supported with VA-ECMO underwent device exchange to a short-term VAD for prolonged support.
4 L. Truby et al. / European Journal of Cardio-Thoracic Surgery 325 Table 3: Pre- and postoperative haemodynamics and laboratory values Table 4: Outcomes Outcomes Survival Overall VAECMO CM n Survival to discharge (%) day survival (%) Destination Myocardial recovery (%) Durable MCSD (%) MCSD: mechanical circulatory support device. Initiation of MCS resulted in significant improvements in haemodynamics (Table 3). MAP prior to MCS was 63 ± 25 mmhg, which improved to 82 ± 12 mmhg after initiation of the circulatory support (P < 0.01). BUN, creatinine and lactate tended to improve after the addition of MCS. Overall survival to 30 days was 59% (Table 4, Fig. 2). When the baseline characteristics of survivors and non-survivors to 30 days were compared, only a history of hyperlipidaemia was more likely to be found among survivors (58.3 vs 28.0%, P = 0.019) (Table 5). Among patients who survived to 30 days, 44% (n = 14) of patients were transitioned to a durable MCSD (11 to Heartmate II, 2 to Heartmate XVE and 1 to TAH). Common causes of in-hospital death included multisystem organ failure (n = 13), neurological non-recovery (n = 7) and asystole (n = 4). Eighteen patients had initial MCSD explanted for myocardial recovery during the index hospital stay with an additional 1 patient who had subsequent explant of a durable MCSD. Ultimately, 31% of the entire cohort (53% of those who survived to 30 days) achieved myocardial recovery. CPO was available in 36 of the 61 patients. Those patients who were undergoing active CPR were assigned a cardiac output of 0 l/min, and thus a CPO of 0 W as previously described [13]. Mean CPO prior to mechanical support was 0.43 ± 0.48 W. Based upon Before MCS After MCS a P-value 95% CI SBP (mmhg), mean ± SD 92.1 ± ± DBP (mmhg), mean ± SD 49.0 ± ± 2.9 < MAP (mmhg), mean ± SD 63.0 ± ± 1.9 < CVP (mmhg), mean ± SD 12.0 ± ± Mean PAP (mmhg), mean ± SD 33.6 ± ± Lactate (mg/dl), median (IQR) 4.3 ± ± ph, mean ± SD 7.3 ± ± 0.01 < Cr (mg/dl), mean ± SD 1.8 ± ± BUN (mg/dl), mean ± SD 33.1 ± ± Haemoglobin (g/dl), mean ± SD 12.0 ± ± 0.2 < AST (U/l), mean ± SD ± ± ALT (U/l), mean ± SD ± ± SBP: systolic blood pressure; DBP: diastolic blood pressure; MAP: mean arterial pressure; CVP: central venous pressure; PAP: pulmonary artery pressure; Cr: creatinine; BUN: blood urea nitrogen; AST: aspartate aminotransferase; ALT: alanine aminotransferase; SD: standard deviation. a 24 h after MCS initiation. Figure 2: Overall 30-day survival. findings from the SHOCK trial registry, a threshold of 0.53 W was utilized for bivariate analysis [14]. Lower levels of CPO were not significantly associated with an increased probability of 30-day mortality. When the probability of in-hospital mortality was generated based upon pre-mcs CPO values, the probability of in-hospital mortality was 50% for those with a CPO of 0 W decreasing to 30% at 0.69 W, which was the median of our cohort (Fig. 3). Among 30-day survivors, 17 were unable to recover native heart function. The number of vasopressors and inotropes used prior to MCS was associated with myocardial recovery without statistical significance (OR: 0.45, 95% CI: , P = 0.07). Peak troponin level was not a predictor of myocardial recovery. Adverse events INTERMACS-defined major bleeding occurred in 31%. Cerebrovascular accident occurred in 17% of the patients (3.3% haemorrhagic and 13.1% ischaemic). Among VA-ECMO patients, limb ischaemia requiring placement of a distal perfusion cannula TX & MCS
5 326 L. Truby et al. / European Journal of Cardio-Thoracic Surgery Table 5: Thirty-day survivors versus non-survivors Survivors Non-survivors P-value Age >65, n (%) 11 (44.0) 10 (27.8) 0.19 Male gender, n (%) 17 (68.0) 25 (69.4) 0.91 BMI >30, n (%) 13 (36.1) 9 (36.0) 0.99 History of hyperlipidaemia, n (%) 21 (58.3) 7 (28.0) History of diabetes mellitus, n (%) 17 (47.2) 11 (44.0) 0.80 History of hypertension, n (%) 21 (58.3) 13 (52.0) 0.62 History of COPD, n (%) 2 (5.6) 2 (8.0) 0.70 Pre-MCS IABP 27 (75.0) 16 (64.0) 0.35 Baseline mean arterial pressure <60 mmhg, n (%) 11 (39.3) 10 (47.6) 0.56 Baseline lactate >2.5 mg/dl, n (%) 9 (56.3) 5 (71.4) 0.50 Baseline ph <7.35, n (%) 13 (48.2) 7 (53.9) 0.74 Baseline creatinine >2 mg/dl, n (%) 8 (27.6) 5 (21.7) 0.63 Number of vasopressors and inotropes, mean ± SD 2.18 ± ± Revascularization prior to MCS, n (%) 30 (83.3) 18 (72.0) 0.29 Cardiac power output <0.53 W, n (%) 13 (54.2) 8 (66.7) 0.47 Pre-MCS ejection fraction 10%, n (%) 6 (28.7) 4 (23.5) 0.73 Peak troponin >227 ng/ml, n (%) 9 (32.1) 6 (28.6) 0.79 Same-day initiation of MCS, n (%) 12 (33.3) 11 (45.8) 0.33 Active CPR at MCS initiation, n (%) 9 (25.0) 8 (32.0) 0.55 BMI: body mass index; COPD: chronic obstructive pulmonary disease; IABP: intra-aortic balloon pump; MCS: mechanical circulatory support; CPR: cardiopulmonary resuscitation; SD: standard deviation. Bold values indicate significant of P values. Figure 3: Probability of in-hospital mortality based upon cardiac power output (CPO). or vascular surgery intervention occurred in 7 patients (11.5%). LV distension, requiring placement of surgical vent or decompression with a percutaneous VAD [Impella 2.5 LP (Abiomed, Inc.)], also occurred in 7 patients [15]. DISCUSSION Our analysis, one of the largest cohorts of MCS therapy in AMI/CS, demonstrated a 59% survival to 30 days among a particularly ill patient cohort. Among survivors, 53% were weaned to myocardial recovery and 44% were transitioned to a durable MCSD. Our survival is consistent with the previous studies reporting a 30-day survival ranging from 23 to 76% [7]. In 2001, Willms et al. published a series of 25 patients who received VA-ECMO for AMI/CS, demonstrating an overall survival of 23% [7]. A more recent series of 33 patients placed on VA-ECMO for AMI/CS published by Bermudez et al. demonstrated an improved 30-day survival of 64% [8]. Tang et al. reported an even better 30-day survival of 76% in 21 patients who had VA-ECMO for similar aetiology [9]. We have also summarized our experience of 27 patients who underwent CentriMag VAD insertion for various aetiologies of CS with an overall survival to discharge rate of 74% [16]. Thirteen of these patients developed CS secondary to AMI. By including all patients who received MCS therapy for AMI/CS, this study is unique in its focus on treatment strategy rather than a particular device. Comparing the outcomes of existing studies is not straightforward. Although the threshold for recognizing CS is well defined, as an entity it encompasses a broad spectrum of clinical and haemodynamic instability. As a result, variability in outcome is greatly influenced by the severity of the patients condition across studies. For instance Kagawa et al. reported their experience of combined therapy with VA-ECMO and PCI for AMI complicated by cardiac arrest, which is the most severe form of CS [17]. The 30-day survival was only 29%. Additionally, Sakamoto et al. recently published a series of 98 patients with AMI/CS complicated by CS (n = 34) or cardiac arrest (n = 64), with 32.7% surviving to discharge [18]. Based on the severity of haemodynamic instability in these cohorts, it is difficult to compare these outcomes to the aforementioned studies. The 30-day survival of 59% in our study compares favourably with the 53.3% in the SHOCK trial and the IABP-SHOCK II trial. In order to account for potential inter-study variability when comparing the present study with similar historical populations, we chose to focus on CPO: a metric found to be a significant predictor of in-hospital mortality in the SHOCK trial registry cohort [14]. Among the 406 patients with right heart catheterization data available from their registry, mean CPO was 0.62 W. In comparison, mean CPO in our cohort was 0.43 W. When the probability of in-hospital mortality was generated based on CPO, as it
6 L. Truby et al. / European Journal of Cardio-Thoracic Surgery 327 was in the SHOCK trial registry, predicted in-hospital mortality in our cohort appears satisfactory, particularly at lower levels of CPO. Interestingly, CPO was no longer a significant predictor of in-hospital mortality or 30-day mortality in our cohort. Even when patients undergoing CPR were excluded from the analysis, survival of those with the most severe degree of haemodynamic compromise approached 60% and CPO remained a nonsignificant predictor of in-hospital mortality (data not shown). Findings in the IABP-SHOCK II trial further support the need for more powerful device therapy in this patient population. While our study provides more evidence suggesting improved survival with MCS therapy in AMI/CS, no well-designed study has been conducted to definitively elucidate its role. In order to improve the unacceptably high mortality rate in AMI/CS, further investigation is warranted. It is possible that findings of such a study might lead to a paradigm shift in the current regime of AMI/CS therapy, from early revascularization to early revascularization and systemic flow restoration. Another important outcome of interest in this study was device explant to myocardial recovery. Previously published evidence suggests that the ability of MCS to unload the left ventricle may help promote myocardial recovery [19]. This is likely secondary to molecular remodelling following reduction of myocardial wall stress [20]. However, the physiology of VA-ECMO, one of the most widely used MCSDs in this cohort, exposes the damaged left ventricle to increased afterload with resultant increased wall stress [21]. The propensity for myocardial recovery has not been extensively studied in this patient cohort. Fifty-nine percent of survivors achieved this end-point in our cohort. Interestingly, variables such as culprit vessels, revascularization, peak troponin and CPO, which are associated with extent of myocardial damage and are often used clinically to predict myocardial recovery, were not found to be significant predictors of myocardial recovery in the present study. It is interesting to note, also, that despite VA-ECMO patients being more acutely ill at the time of device use, the rates of myocardial recovery are similar between VA-ECMO and Centrimag patients. While this could reflect the successful utility of the device in this acutely ill patient population, it could reflect the fact that Centrimag patients often have a longer time course of illness. Thus, while they appear more stable, they may have less ability to recover native heart function than those patients with a more acute insult. Only a history of hyperlipidaemia (OR: 2.79, 95% CI: , P = 0.07) and the number of vasopressors and inotropes used prior to MCS (OR: 0.45, 95% CI: , P = 0.07) were somewhat associated with myocardial recovery. Exchange to durable MCSD was performed in 44%, which is remarkably higher than 3.6% in the revascularization arm of the SHOCK trial. Aggressive use of heart replacement therapy might be one of the important reasons for better survival in our study. Percutaneous LVADs were not considered MCS therapy in the present study. To date, there have been three randomized trials evaluating the efficacy of percutaneous LVADs when compared with IABPs for patients with AMI/CS [22 24]. A meta-analysis of these trials included 100 patients, most with AMI/CS. Pooled survival data revealed the 45% 30-day mortality rate in LVAD patients to be non-significantly different from the 43% 30-day mortality among those treated with IABP (P = 0.80) [25]. In comparison to percutaneous VADs, VA-ECMO and surgical VADs are able to generate greater flows and can often be used for longer durations of support. However, newer generations of percutaneous LVADs that allow higher rates of flow are also likely to improve outcomes. Limitations Although these data represent one of the largest reported series of patients with AMI/CS treated with MCS, the overall power to detect independent correlates of clinical outcomes is limited. Additionally, this retrospectively conducted study does not capture the entire population (or denominator) of patients who presented to our institution with AMI/CS; as such, there is selection bias in the sample of patients who ultimately went on to require MCS. Inter-study comparisons (between our study with others previously published) are similarly difficult. CONCLUSIONS In our experience, the use of MCS was not only feasible for patients with AMI/CS, but was suggestive of improved survival compared with conventional management. Future studies to further elucidate the appropriate criteria and timing for device initiation could help to further improve outcomes. A prospective multicentre large-scale trial would aid in better evaluating the efficacy of MCS therapy in AMI/CS patients. Conflict of interest: Ulrich P. Jorde and Yoshifumi Naka receive consultant fee from Thoratec, Corp. REFERENCES [1] Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Borden WB et al. Heart disease and stroke statistics 2013 update: a report from the American Heart Association. Circulation 2013;127:e6 e245. [2] Hochman JS, Sleeper LA, Webb JG, Sanborn TA, White HD, Talley JD et al. Early revascularization in acute myocardial infarction complicated by cardiogenic shock. SHOCK Investigators. Should we emergently revascularize occluded coronaries for cardiogenic shock. N Engl J Med 1999;341: [3] Goldberg RJ, Spencer FA, Gore JM, Lessard D, Yarzebski J. Thirty-year trends (1975 to 2005) in the magnitude of, management of, and hospital death rates associated with cardiogenic shock in patients with acute myocardial infarction: a population-based perspective. Circulation 2009;119: [4] Thiele H, Zeymer U, Neumann FJ, Ferenc M, Olbrich HG, Hausleiter J et al. Intraaortic balloon support for myocardial infarction with cardiogenic shock. N Engl J Med 2012;367: [5] O Connor CM, Rogers JG. Evidence for overturning the guidelines in cardiogenic shock. N Engl J Med 2012;367: [6] Hendry PJ, Masters RG, Mussivand TV, Smith S, Davies RA, Finlay S et al. Circulatory support for cardiogenic shock due to acute myocardial infarction: a Canadian experience. Can J Cardiol 1999;15: [7] Willms DC, Atkins PJ, Dembitsky WP, Jaski BE, Gocka I. Analysis of clinical trends in a program of emergent ECLS for cardiovascular collapse. ASAIO J 1997;43:65 8. [8] Bermudez CA, Rocha RV, Toyoda Y, Zaldonis D, Sappington PL, Mulukutla S et al. Extracorporeal membrane oxygenation for advanced refractory shock in acute and chronic cardiomyopathy. Ann Thorac Surg 2011;92: [9] Tang GH, Malekan R, Kai M, Lansman SL, Spielvogel D. Peripheral venoarterial extracorporeal membrane oxygenation improves survival in myocardial infarction with cardiogenic shock. J Thorac Cardiovasc Surg 2013;145: e32 3. [10] Thiele H, Allam B, Chatellier G, Schuler G, Lafont A. Shock in acute myocardial infarction: the Cape Horn for trials? Eur Heart J 2010;31: [11] Takayama H, Truby L, Koekort M, Uriel N, Colombo P, Mancini DM et al. Clinical outcome of mechanical circulatory support for refractory cardiogenic shock in the current era. J Heart Lung Transplant 2013;32: TX & MCS
7 328 L. Truby et al. / European Journal of Cardio-Thoracic Surgery [12] Takayama H, Chen JM, Jorde UP, Naka Y. Implantation technique of the CentriMag biventricular assist device allowing ambulatory rehabilitation. Interact CardioVasc Thorac Surg 2011;12: [13] Kar B, Gregoric ID, Basra SS, Idelchik GM, Loyalka P. The percutaneous ventricular assist device in severe refractory cardiogenic shock. J Am Coll Cardiol 2011;57: [14] Fincke R, Hochman JS, Lowe AM, Menon V, Slater JN, Webb JG et al. Cardiac power is the strongest hemodynamic correlate of mortality in cardiogenic shock: a report from the SHOCK trial registry. J Am Coll Cardiol 2004;44: [15] Koeckert MS, Jorde UP, Naka Y, Moses JW, Takayama H. Impella LP 2.5 for left ventricular unloading during venoarterial extracorporeal membrane oxygenation support. J Card Surg 2011;26: [16] Worku B, Pak SW, van Patten D, Housman B, Uriel N, Colombo P et al. The CentriMag ventricular assist device in acute heart failure refractory to medical management. J Heart Lung Transplant 2012;31: [17] Kagawa E, Dote K, Kato M, Sasaki S, Nakano Y, Kajikawa M et al. Should we emergently revascularize occluded coronaries for cardiac arrest? Rapid-response extracorporeal membrane oxygenation and intra-arrest percutaneous coronary intervention. Circulation 2012;126: [18] Sakamoto S, Taniguchi N, Nakajima S, Takahashi A. Extracorporeal life support for cardiogenic shock or cardiac arrest due to acute coronary syndrome. Ann Thorac Surg 2012;94:1 7. [19] Simon MA, Primack BA, Teuteberg J, Kormos RL, Bermudez C, Toyoda Y et al. Left ventricular remodeling and myocardial recovery on mechanical circulatory support. J Card Fail 2010;16: [20] Young JB. Healing the heart with ventricular assist device therapy: mechanisms of cardiac recovery. Ann Thorac Surg 2001;71:S [21] Burkhoff D, Naidu SS. The science behind percutaneous hemodynamic support: a review and comparison of support strategies. Catheter Cardiovasc Interv 2012;80: [22] Thiele H, Sick P, Boudriot E, Diederich KW, Hambrecht R, Niebauer J et al. Randomized comparison of intra-aortic balloon support with a percutaneous left ventricular assist device in patients with revascularized acute myocardial infarction complicated by cardiogenic shock. Eur Heart J 2005; 26: [23] Burkhoff D, Cohen H, Brunckhorst C, O Neill WW, TandemHeart Investigators G. A randomized multicenter clinical study to evaluate the safety and efficacy of the TandemHeart percutaneous ventricular assist device versus conventional therapy with intra-aortic balloon pumping for treatment of cardiogenic shock. Am Heart J 2006;152: 469e1 8. [24] Seyfarth M, Sibbing D, Bauer I, Frohlich G, Bott-Flugel L, Byrne R et al. A randomized clinical trial to evaluate the safety and efficacy of a percutaneous left ventricular assist device versus intra-aortic balloon pumping for treatment of cardiogenic shock caused by myocardial infarction. J Am Coll Cardiol 2008;52: [25] Cheng JM, den Uil CA, Hoeks SE, van der Ent M, Jewbali LS, van Domburg RT et al. Percutaneous left ventricular assist devices vs. intra-aortic balloon pump counterpulsation for treatment of cardiogenic shock: a meta-analysis of controlled trials. Eur Heart J 2009;30:
Management of Cardiogenic Shock. Dr Stephen Pettit, Consultant Cardiologist
 Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Dr Stephen Pettit, Consultant Cardiologist Cardiogenic shock Management of Cardiogenic Shock Outline Definition, INTERMACS classification Medical management of cardiogenic shock PA catheters and haemodynamic
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend )
 Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Intraaortic Balloon Counterpulsation- Supportive Data for a Role in Cardiogenic Shock ( Be Still My Friend ) Stephen G. Ellis, MD Section Head, Interventional Cardiology Professor of Medicine Cleveland
Mechanical Cardiac Support in Acute Heart Failure. Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research
 Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Mechanical Cardiac Support in Acute Heart Failure Michael Felker, MD, MHS Associate Professor of Medicine Director of Heart Failure Research Disclosures Research Support and/or Consulting NHLBI Amgen Cytokinetics
Bridging With Percutaneous Devices: Tandem Heart and Impella
 Bridging With Percutaneous Devices: Tandem Heart and Impella DAVID A. BARAN, MD, FACC, FSCAI SYSTEM DIRECTOR, ADVANCED HEART FAILURE, TX AND MCS SENTARA HEART HOSPITAL NORFOLK, VA PROFESSOR OF MEDICINE
Bridging With Percutaneous Devices: Tandem Heart and Impella DAVID A. BARAN, MD, FACC, FSCAI SYSTEM DIRECTOR, ADVANCED HEART FAILURE, TX AND MCS SENTARA HEART HOSPITAL NORFOLK, VA PROFESSOR OF MEDICINE
Short-Term Ventricular Assist Devices (Implantable and Percutaneous)
 Curr Surg Rep (2014) 2:58 DOI 10.1007/s40137-014-0058-x ARTIFICIAL ORGAN CT SURGERY (S AKHTER, SECTION EDITOR) Short-Term Ventricular Assist Devices (Implantable and Percutaneous) Hiroo Takayama Lauren
Curr Surg Rep (2014) 2:58 DOI 10.1007/s40137-014-0058-x ARTIFICIAL ORGAN CT SURGERY (S AKHTER, SECTION EDITOR) Short-Term Ventricular Assist Devices (Implantable and Percutaneous) Hiroo Takayama Lauren
AllinaHealthSystem 1
 : Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
: Definition End-organ hypoperfusion secondary to cardiac failure Venoarterial ECMO: Patient Selection Michael A. Samara, MD FACC Advanced Heart Failure, Cardiac Transplant & Mechanical Circulatory Support
Andrew Civitello MD, FACC
 Timing the Transition from Short Term to Long Term Mechanical Circulatory Support Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's
Timing the Transition from Short Term to Long Term Mechanical Circulatory Support Andrew Civitello MD, FACC Medical Director, Heart Transplant Program Director, Fellowship Co-Director, Baylor St. Luke's
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
DECLARATION OF CONFLICT OF INTEREST Cardiogenic Shock Mechanical Support Eulàlia Roig FESC Heart Failure and HT Unit Hospital Sant Pau - UAB Barcelona. Spain No conflics of interest Mechanical Circulatory
ORIGINAL ARTICLE. Abstract INTRODUCTION
 European Journal of Cardio-Thoracic Surgery 52 (2017) 1055 1061 doi:10.1093/ejcts/ezx189 Advance Access publication 22 June 2017 ORIGINAL ARTICLE Cite this article as: Takeda K, Garan AR, Ando M, Han J,
European Journal of Cardio-Thoracic Surgery 52 (2017) 1055 1061 doi:10.1093/ejcts/ezx189 Advance Access publication 22 June 2017 ORIGINAL ARTICLE Cite this article as: Takeda K, Garan AR, Ando M, Han J,
Counterpulsation. John N. Nanas, MD, PhD. Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece
 John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
John N. Nanas, MD, PhD Professor and Head, 3 rd Cardiology Dept, University of Athens, Athens, Greece History of counterpulsation 1952 Augmentation of CBF Adrian and Arthur Kantrowitz, Surgery 1952;14:678-87
Extra Corporeal Life Support for Acute Heart failure
 Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Extra Corporeal Life Support for Acute Heart failure Benjamin Medalion, MD Director Heart and Lung Transplantation Department of Cardiothoracic Surgery Rabin Medical Center, Beilinson Campus, Israel Mechanical
Update on Mechanical Circulatory Support. AATS May 5, 2010 Toronto, ON Canada
 Update on Mechanical Circulatory Support AATS May 5, 2010 Toronto, ON Canada Disclosures NONE Emergency Circulatory Support ECMO Tandem Heart Impella Assessment Cardiac Function Pulmonary function Valvular
Update on Mechanical Circulatory Support AATS May 5, 2010 Toronto, ON Canada Disclosures NONE Emergency Circulatory Support ECMO Tandem Heart Impella Assessment Cardiac Function Pulmonary function Valvular
Rhondalyn C. McLean. 2 ND YEAR RESEARCH ELECTIVE RESIDENT S JOURNAL Volume VII, A. Study Purpose and Rationale
 A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
A Randomized Clinical Study To Compare The Intra-Aortic Balloon Pump To A Percutaneous Left Atrial-To-Femoral Arterial Bypass Device For Treatment Of Cardiogenic Shock Following Acute Myocardial Infarction.
Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017
 Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017 Pascal Vranckx MD, PhD. Medical director Cardiac Critical Care Services Hartcentrum Hasselt Belgium Disclosure
Mechanical circulatory support in cardiogenic shock The Cardiologist s view ACCA Masterclass 2017 Pascal Vranckx MD, PhD. Medical director Cardiac Critical Care Services Hartcentrum Hasselt Belgium Disclosure
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO)
 Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Cath Lab Essentials : LV Assist Devices for Hemodynamic Support (IABP, Impella, Tandem Heart, ECMO) Michael A. Gibson, MD Assistant Professor of Medicine University of California, Irvine Division of Cardiology
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012
 Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Acute heart failure: ECMO Cardiology & Vascular Medicine 2012 Lucia Jewbali cardiologist-intensivist 14 beds/8 ICU beds Acute coronary syndromes Heart failure/ Cardiogenic shock Post cardiotomy Heart
Assist Devices in STEMI- Intra-aortic Balloon Pump
 Assist Devices in STEMI- Intra-aortic Balloon Pump Ioannis Iakovou, MD, PhD Onassis Cardiac Surgery Center Athens, Greece Cardiogenic shock 5-10% of pts after a heart attack 60000-70000 pts in Europe/year
Assist Devices in STEMI- Intra-aortic Balloon Pump Ioannis Iakovou, MD, PhD Onassis Cardiac Surgery Center Athens, Greece Cardiogenic shock 5-10% of pts after a heart attack 60000-70000 pts in Europe/year
Predictors of Survival for Patients with Acute Decompensated Heart Failure Requiring Extra-Corporeal Membrane Oxygenation Therapy
 ASAIO Journal 2018 Adult Circulatory Support Predictors of Survival for Patients with Acute Decompensated Heart Failure Requiring Extra-Corporeal Membrane Oxygenation Therapy A. RESHAD GARAN,* WAQAS A.
ASAIO Journal 2018 Adult Circulatory Support Predictors of Survival for Patients with Acute Decompensated Heart Failure Requiring Extra-Corporeal Membrane Oxygenation Therapy A. RESHAD GARAN,* WAQAS A.
Implantable Ventricular Assist Devices and Total Artificial Hearts. Policy Specific Section: June 13, 1997 March 29, 2013
 Medical Policy Implantable Ventricular Assist Devices and Total Artificial Hearts Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective
Medical Policy Implantable Ventricular Assist Devices and Total Artificial Hearts Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective
Management of Acute Shock and Right Ventricular Failure
 Management of Acute Shock and Right Ventricular Failure Nader Moazami, MD Department of Thoracic and Cardiovascular Surgery and Biomedical Engineering, Cleveland Clinic NONE Disclosures CARDIOGENIC SHOCK
Management of Acute Shock and Right Ventricular Failure Nader Moazami, MD Department of Thoracic and Cardiovascular Surgery and Biomedical Engineering, Cleveland Clinic NONE Disclosures CARDIOGENIC SHOCK
ECMO as a bridge to durable LVAD therapy. Jonathan Haft, MD Department of Cardiac Surgery University of Michigan
 ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
ECMO as a bridge to durable LVAD therapy Jonathan Haft, MD Department of Cardiac Surgery University of Michigan Systolic Heart Failure Prevalence 4.8 million U.S. 287,000 deaths per year $39 billion spent
Surgical Options for Temporary MCS
 Surgical Options for Temporary MCS Michael A. Acker, MD Julian Johnson Professor of Surgery Chief of Cardiovascular Surgery Director of Heart and Vascular Center University of Pennsylvania Health System
Surgical Options for Temporary MCS Michael A. Acker, MD Julian Johnson Professor of Surgery Chief of Cardiovascular Surgery Director of Heart and Vascular Center University of Pennsylvania Health System
Cardiogenic Shock. Dr. JPS Henriques. Academic Medical Center University of Amsterdam The Netherlands
 Cardiogenic Shock Dr. JPS Henriques Academic Medical Center University of Amsterdam The Netherlands Conflict of interest disclosure Research grant Abbott Vascular Research grant Abiomed Inc. Global Impella
Cardiogenic Shock Dr. JPS Henriques Academic Medical Center University of Amsterdam The Netherlands Conflict of interest disclosure Research grant Abbott Vascular Research grant Abiomed Inc. Global Impella
Introduction to Acute Mechanical Circulatory Support
 Introduction to Acute Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive
Introduction to Acute Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive
Circulatory Support: From IABP to LVAD
 Circulatory Support: From IABP to LVAD Howard A Cohen, MD, FACC, FSCAI Director Division of Cardiovascular Intervention Co Director Cardiovascular Interventional ti Laboratories Lenox Hill Heart & Vascular
Circulatory Support: From IABP to LVAD Howard A Cohen, MD, FACC, FSCAI Director Division of Cardiovascular Intervention Co Director Cardiovascular Interventional ti Laboratories Lenox Hill Heart & Vascular
ECMO as a Bridge to Heart Transplant in the Era of LVAD s.
 Christian Bermudez MD. Associate Professor Director Thoracic Transplantation Division Cardiac Surgery Department of Surgery University of Pennsylvania ECMO as a Bridge to Heart Transplant in the Era of
Christian Bermudez MD. Associate Professor Director Thoracic Transplantation Division Cardiac Surgery Department of Surgery University of Pennsylvania ECMO as a Bridge to Heart Transplant in the Era of
เอกราช อร ยะช ยพาณ ชย
 30 July 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Disclosure Speaker, CME service: Merck, Otsuka, Servier Consultant, non-cme service: Novartis, Menarini
30 July 2016 เอกราช อร ยะช ยพาณ ชย Heart Failure and Transplant Cardiology aekarach.a@chula.ac.th Disclosure Speaker, CME service: Merck, Otsuka, Servier Consultant, non-cme service: Novartis, Menarini
ORIGINAL ARTICLE. Alexander M. Bernhardt a, *, Theo M.M.H. De By b, Hermann Reichenspurner a and Tobias Deuse a. Abstract INTRODUCTION
 European Journal of Cardio-Thoracic Surgery 48 (2015) 158 162 doi:10.1093/ejcts/ezu406 Advance Access publication 29 October 2014 ORIGINAL ARTICLE Cite this article as: Bernhardt AM, De By TMMH, Reichenspurner
European Journal of Cardio-Thoracic Surgery 48 (2015) 158 162 doi:10.1093/ejcts/ezu406 Advance Access publication 29 October 2014 ORIGINAL ARTICLE Cite this article as: Bernhardt AM, De By TMMH, Reichenspurner
Case - Advanced HF and Shock (INTERMACS 1)
 Case - Advanced HF and Shock (INTERMACS 1) Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive Director,
Case - Advanced HF and Shock (INTERMACS 1) Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure Programs Executive Director,
8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference Dubai: October Acute Coronary Syndromes
 8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference 2017 OSPEDALE Dubai: 19-21 October 2017 Acute Coronary Syndromes Antonio Colombo Centro Cuore Columbus and S. Raffaele
8th Emirates Cardiac Society Congress in collaboration with ACC Middle East Conference 2017 OSPEDALE Dubai: 19-21 October 2017 Acute Coronary Syndromes Antonio Colombo Centro Cuore Columbus and S. Raffaele
The majority of patients with cardiomyopathy
 Selection of Hemodynamic Support: An Approach for Coronary Interventions in Shock and High-Risk PCI The role of hemodynamic support devices in emergent cardiogenic shock and elective high-risk percutaneous
Selection of Hemodynamic Support: An Approach for Coronary Interventions in Shock and High-Risk PCI The role of hemodynamic support devices in emergent cardiogenic shock and elective high-risk percutaneous
A Validated Practical Risk Score to Predict the Need for RVAD after Continuous-flow LVAD
 A Validated Practical Risk Score to Predict the Need for RVAD after Continuous-flow LVAD SK Singh MD MSc, DK Pujara MBBS, J Anand MD, WE Cohn MD, OH Frazier MD, HR Mallidi MD Division of Transplant & Assist
A Validated Practical Risk Score to Predict the Need for RVAD after Continuous-flow LVAD SK Singh MD MSc, DK Pujara MBBS, J Anand MD, WE Cohn MD, OH Frazier MD, HR Mallidi MD Division of Transplant & Assist
Percutaneous Mechanical Circulatory Support Devices
 Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Percutaneous Mechanical Circulatory Support Devices Daniel Vazquez RN, RCIS Miami Cardiac & Vascular Institute FINANCIAL DISCLOSURES none CASE STUDY CASE STUDY 52 year old gentlemen Complaining of dyspnea
Right Ventricular Failure: Prediction, Prevention and Treatment
 Right Ventricular Failure: Prediction, Prevention and Treatment 3 rd European Training Symposium for Heart Failure Cardiologists and Cardiac Surgeons University Hospital Bern June 24-25, 2016 Disclosures:
Right Ventricular Failure: Prediction, Prevention and Treatment 3 rd European Training Symposium for Heart Failure Cardiologists and Cardiac Surgeons University Hospital Bern June 24-25, 2016 Disclosures:
Rationale for Prophylactic Support During Percutaneous Coronary Intervention
 Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Rationale for Prophylactic Support During Percutaneous Coronary Intervention Navin K. Kapur, MD, FACC, FSCAI Assistant Director, Interventional Cardiology Director, Interventional Research Laboratories
Ramani GV et al. Mayo Clin Proc 2010;85:180-95
 THERAPIES FOR ADVANCED HEART FAILURE: WHEN TO REFER Navin Rajagopalan, MD Assistant Professor of Medicine University of Kentucky Director, Congestive Heart Failure Medical Director of Cardiac Transplantation
THERAPIES FOR ADVANCED HEART FAILURE: WHEN TO REFER Navin Rajagopalan, MD Assistant Professor of Medicine University of Kentucky Director, Congestive Heart Failure Medical Director of Cardiac Transplantation
The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities
 The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
The Pathophysiology of Cardiogenic Shock Knowledge Gaps & Opportunities Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management
 Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
Planned, Short-Term RVAD During Durable LVAD Implant: Indications and Management Yoshifumi Naka, MD, PhD Columbia University Medical Center New York, NY Disclosure Abbott/St. Jude Med./Thoratec Consultant
LV Distension and ECLS Lungs
 LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
LV Distension and ECLS Lungs Kevin W. Hatton, MD, FCCM Interim Vice-Chair for Anesthesiology Research Division Chief, Anesthesiology Critical Care Medicine Program Director, Anesthesiology Critical Care
Ventricular Assisting Devices in the Cathlab. Unrestricted
 Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Ventricular Assisting Devices in the Cathlab Unrestricted What is a VAD? A single system device that is surgically attached to the left ventricle of the heart and to the aorta for left ventricular support
Percutaneous Cardiopulmonary Support after Acute Myocardial Infarction at the Left Main Trunk
 Original Article Percutaneous Cardiopulmonary Support after Acute Myocardial Infarction at the Left Main Trunk Takashi Yamauchi, MD, PhD, 1 Takafumi Masai, MD, PhD, 1 Koji Takeda, MD, 1 Satoshi Kainuma,
Original Article Percutaneous Cardiopulmonary Support after Acute Myocardial Infarction at the Left Main Trunk Takashi Yamauchi, MD, PhD, 1 Takafumi Masai, MD, PhD, 1 Koji Takeda, MD, 1 Satoshi Kainuma,
Echo assessment of patients with an ECMO device
 Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
Echo assessment of patients with an ECMO device Evangelos Leontiadis Cardiologist 1st Cardiology Dept. Onassis Cardiac Surgery Center Athens, Greece Gibbon HLM 1953 Goldstein DJ et al, NEJM 1998; 339:1522
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Chief Medical Officer First Coast Cardiovascular Institute, Jacksonville, FL Professor of Medicine, UCF, Orlando, FL None DISCLOSURE Percutaneous
Mechanics of Cath Lab Support Devices
 Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Mechanics of Cath Lab Support Devices Issam D. Moussa, MD Professor of Medicine Mayo Clinic College of Medicine Chair, Division of Cardiovascular Diseases Mayo Clinic Jacksonville, Florida DISCLOSURE Presenter:
Cardiogenic Shock Protocol
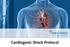 Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Cardiogenic Shock Protocol Impella Devices Best Practices in AMI Cardiogenic Shock Identify 1-3 SBP < 90 mmhg or on inotropes /pressors Cold, clammy, tachycardia Lactate elevated > 2 mmoi /L Stabilize
Short-Term Ventricular Assist Devices as a Bridge to Decision/ Recovery
 Chapter 67 Short-Term Ventricular Assist Devices as a Bridge to Decision/ Recovery ALLA GOPALA KRISHNA GOKHALE CH. RAVIRAJU V.V.K. BHARADWAJA KODURU VENKATA RAMANA INTRODUCTION Heart diseases and heart
Chapter 67 Short-Term Ventricular Assist Devices as a Bridge to Decision/ Recovery ALLA GOPALA KRISHNA GOKHALE CH. RAVIRAJU V.V.K. BHARADWAJA KODURU VENKATA RAMANA INTRODUCTION Heart diseases and heart
MEDICAL POLICY SUBJECT: VENTRICULAR ASSIST DEVICES
 MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
MEDICAL POLICY PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical policy criteria are not applied.
Matching Patient and Pump in the New Era of Percutaneous Mechanical Circulatory Support
 Matching Patient and Pump in the New Era of Percutaneous Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced
Matching Patient and Pump in the New Era of Percutaneous Mechanical Circulatory Support Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced
Which mechanical assistance for cardiogenic shock?
 Which mechanical assistance for cardiogenic shock? Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre et Marie Curie Sorbonne
Which mechanical assistance for cardiogenic shock? Alain Combes, MD, PhD, Hôpital Pitié-Salpêtrière, AP-HP Inserm UMRS 1166, ican, Institute of Cardiometabolism and Nutrition Pierre et Marie Curie Sorbonne
PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR
 PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR Dr Susanna Price MD PhD MRCP ESICM FFICM FESC Consultant Cardiologist & Intensivist Royal Brompton & Harefield NHS Foundation Trust DECLARATIONS Educational
PUMP FAILURE COMPLICATING AMI: ISCHAEMIC VSR Dr Susanna Price MD PhD MRCP ESICM FFICM FESC Consultant Cardiologist & Intensivist Royal Brompton & Harefield NHS Foundation Trust DECLARATIONS Educational
How to do Primary Angioplasty. - Patients with Cardiogenic Shock
 How to do Primary Angioplasty - Patients with Cardiogenic Shock Advanced Cardiovascular Intervention 2011 Dan Blackman Leeds General Infirmary MY CONFLICTS OF INTEREST ARE: Research Grants Medicines Company
How to do Primary Angioplasty - Patients with Cardiogenic Shock Advanced Cardiovascular Intervention 2011 Dan Blackman Leeds General Infirmary MY CONFLICTS OF INTEREST ARE: Research Grants Medicines Company
Implantable Ventricular Assist Devices and Total Artificial Hearts
 Implantable Ventricular Assist Devices and Total Artificial Hearts Policy Number: Original Effective Date: MM.06.017 05/21/1999 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Implantable Ventricular Assist Devices and Total Artificial Hearts Policy Number: Original Effective Date: MM.06.017 05/21/1999 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Accepted Manuscript. Improving Survival in Cardiogenic shock: Is Impella the Answer?,, James J Glazier MD, Amir Kaki MD S (18)
 Accepted Manuscript Improving Survival in Cardiogenic shock: Is Impella the Answer?,, James J Glazier MD, Amir Kaki MD PII: S0002-9343(18)30496-0 DOI: 10.1016/j.amjmed.2018.04.045 Reference: AJM 14684
Accepted Manuscript Improving Survival in Cardiogenic shock: Is Impella the Answer?,, James J Glazier MD, Amir Kaki MD PII: S0002-9343(18)30496-0 DOI: 10.1016/j.amjmed.2018.04.045 Reference: AJM 14684
Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California
 High Risk PCI Making Possible the Impossible Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California Disclosures Abiomed Research Support Consulting Agreement
High Risk PCI Making Possible the Impossible Ray Matthews MD Professor of Clinical Medicine Chief of Cardiology University of Southern California Disclosures Abiomed Research Support Consulting Agreement
Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ
 Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ Low cardiac output/cardiogenic Shock State of end-organ hypoperfusion due to cardiac failure.
Low cardiac output & Mechanical Support นายแพทย อรรถภ ม ส ศ ภอรรถ ศ ลยศาสตร ห วใจและทรวงอก โรงพยาบาล ราชว ถ Low cardiac output/cardiogenic Shock State of end-organ hypoperfusion due to cardiac failure.
EACTS Adult Cardiac Database
 EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
EACTS Adult Cardiac Database Quality Improvement Programme List of changes to Version 2.0, 13 th Dec 2018, compared to version 1.0, 1 st May 2014. INTRODUCTORY NOTES This document s purpose is to list
CABG for ischemic cardiomyopathy, post myocardial infarction and cardiogenic shock
 CABG for ischemic cardiomyopathy, post myocardial infarction and cardiogenic shock Yoshiya Toyoda, MD, PhD William Maul Measey Professor of Surgery Chief, Cardiovascular Surgery Surgical Director, Mechanical
CABG for ischemic cardiomyopathy, post myocardial infarction and cardiogenic shock Yoshiya Toyoda, MD, PhD William Maul Measey Professor of Surgery Chief, Cardiovascular Surgery Surgical Director, Mechanical
Improving Outcomes in Patients With Ventricular Assist Devices Transferred From Outlying to Tertiary Care Hospitals
 The Journal of The American Society of Extra-Corporeal Technology Improving Outcomes in Patients With Ventricular Assist Devices Transferred From Outlying to Tertiary Care Hospitals Mark B. Anderson, MD;*
The Journal of The American Society of Extra-Corporeal Technology Improving Outcomes in Patients With Ventricular Assist Devices Transferred From Outlying to Tertiary Care Hospitals Mark B. Anderson, MD;*
Acute Mechanical Circulatory Support Right Ventricular Support Devices
 Acute Mechanical Circulatory Support Right Ventricular Support Devices Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
Acute Mechanical Circulatory Support Right Ventricular Support Devices Navin K. Kapur, MD, FACC, FSCAI, FAHA Associate Professor, Department of Medicine Interventional Cardiology & Advanced Heart Failure
ST-Elevation Myocardial Infarction & Cardiogenic Shock. - What Should We Do?
 ST-Elevation Myocardial Infarction & Cardiogenic Shock - What Should We Do? Advanced Angioplasty 2008 Dan Blackman Leeds General Infirmary Conflicts of interest Advisory Boards Cordis Boston Scientific
ST-Elevation Myocardial Infarction & Cardiogenic Shock - What Should We Do? Advanced Angioplasty 2008 Dan Blackman Leeds General Infirmary Conflicts of interest Advisory Boards Cordis Boston Scientific
Heart rescue: the role of mechanical circulatory support in the management of severe refractory cardiogenic shock
 REVIEW C URRENT OPINION Heart rescue: the role of mechanical circulatory support in the management of severe refractory cardiogenic shock Gabriel T. Sayer a, Joshua N. Baker b, and Kimberly A. Parks a
REVIEW C URRENT OPINION Heart rescue: the role of mechanical circulatory support in the management of severe refractory cardiogenic shock Gabriel T. Sayer a, Joshua N. Baker b, and Kimberly A. Parks a
Innovative ECMO Configurations in Adults
 Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Innovative ECMO Configurations in Adults Practice at a Single Center with Platinum Level ELSO Award for Excellence in Life Support Monika Tukacs, BSN, RN, CCRN Columbia University Irving Medical Center,
Final published version:
 Clinical Characteristics and Outcomes of Patients With Myocardial Infarction and Cardiogenic Shock Undergoing Coronary Artery Bypass Surgery: Data From The Society of Thoracic Surgeons National Database
Clinical Characteristics and Outcomes of Patients With Myocardial Infarction and Cardiogenic Shock Undergoing Coronary Artery Bypass Surgery: Data From The Society of Thoracic Surgeons National Database
To ECMO Or Not To ECMO Challenges of venous arterial ECMO. Dr Emily Granger St Vincent s Hospital Darlinghurst NSW
 To ECMO Or Not To ECMO Challenges of venous arterial ECMO Dr Emily Granger St Vincent s Hospital Darlinghurst NSW The Start: 1972 St Vincent s Hospital The Turning Point ECMO program restarted in 2004
To ECMO Or Not To ECMO Challenges of venous arterial ECMO Dr Emily Granger St Vincent s Hospital Darlinghurst NSW The Start: 1972 St Vincent s Hospital The Turning Point ECMO program restarted in 2004
CARDIOGENIC SHOCK. Antonio Pesenti. Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI)
 CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
CARDIOGENIC SHOCK Antonio Pesenti Università degli Studi di Milano Bicocca Azienda Ospedaliera San Gerardo Monza (MI) Primary myocardial dysfunction resulting in the inability of the heart to mantain an
Implantable Ventricular Assist Devices and Total Artificial Hearts
 Implantable Ventricular Assist Devices and Total Artificial Hearts Policy Number: Original Effective Date: MM.06.017 05/21/1999 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Implantable Ventricular Assist Devices and Total Artificial Hearts Policy Number: Original Effective Date: MM.06.017 05/21/1999 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
ECMO AND SHORT-TERM SUPPORT:
 ECMO AND SHORT-TERM SUPPORT: UTILIZATION GUIDELINES AND IMPACT OF THE NEW HEART ALLOCATION SYSTEM Jeffrey Teuteberg Section Chief of Heart Failure, Cardiac Transplant and Mechanical Circulatory Support
ECMO AND SHORT-TERM SUPPORT: UTILIZATION GUIDELINES AND IMPACT OF THE NEW HEART ALLOCATION SYSTEM Jeffrey Teuteberg Section Chief of Heart Failure, Cardiac Transplant and Mechanical Circulatory Support
Ischemic Ventricular Septal Rupture
 Ischemic Ventricular Septal Rupture Optimal Management Strategies Juan P. Umaña, M.D. Chief Medical Officer FCI Institute of Cardiology Disclosures Abbott Mitraclip Royalties Johnson & Johnson Proctor
Ischemic Ventricular Septal Rupture Optimal Management Strategies Juan P. Umaña, M.D. Chief Medical Officer FCI Institute of Cardiology Disclosures Abbott Mitraclip Royalties Johnson & Johnson Proctor
3/1/2017. Heart Failure is a major driver of morbidity and mortality in the US 1-7
 Approaches to Cardiogenic Shock Margarita Camacho MD, FACS Surgical Director Cardiac Transplant and Mechanical Assist Device Program RWJ/Barnabas Health Heart Centers at Newark Beth Israel Medical Center
Approaches to Cardiogenic Shock Margarita Camacho MD, FACS Surgical Director Cardiac Transplant and Mechanical Assist Device Program RWJ/Barnabas Health Heart Centers at Newark Beth Israel Medical Center
The Role of Mechanical Circulatory Support in Cardiogenic Shock: When to Utilize
 The Role of Mechanical Circulatory Support in Cardiogenic Shock: Presented by Nancy Scroggins ACNP, CNS-CC CV Surgery ACNP Bayshore Medical Center The Role of Mechanical Circulatory Support in Cardiogenic
The Role of Mechanical Circulatory Support in Cardiogenic Shock: Presented by Nancy Scroggins ACNP, CNS-CC CV Surgery ACNP Bayshore Medical Center The Role of Mechanical Circulatory Support in Cardiogenic
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know!
 Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Mechanical Circulatory Support (MCS): What Every Pharmacist Needs to Know! Matthew A. Wanat, PharmD, BCPS, BCCCP, FCCM Clinical Assistant Professor University of Houston College of Pharmacy Clinical Pharmacy
Mechanical Support in the Failing Fontan-Kreutzer
 Mechanical Support in the Failing Fontan-Kreutzer Stephanie Fuller MD, MS Thomas L. Spray Endowed Chair in Congenital Heart Surgery Associate Professor, The Perelman School of Medicine at the University
Mechanical Support in the Failing Fontan-Kreutzer Stephanie Fuller MD, MS Thomas L. Spray Endowed Chair in Congenital Heart Surgery Associate Professor, The Perelman School of Medicine at the University
Please cite this article as: Ellie J Coromilas MD, Koji Takeda MD, PhD, Masahiko Ando MD,
 Accepted Manuscript Comparison of Percutaneous and Surgical Right Ventricular Assist Device Support Following Durable Left Ventricular Assist Device Insertion Ellie J Coromilas MD, Koji Takeda MD, PhD,
Accepted Manuscript Comparison of Percutaneous and Surgical Right Ventricular Assist Device Support Following Durable Left Ventricular Assist Device Insertion Ellie J Coromilas MD, Koji Takeda MD, PhD,
Modern Left Ventricular Assist Devices (LVAD) : An Intro, Complications, and Emergencies
 Modern Left Ventricular Assist Devices (LVAD) : An Intro, Complications, and Emergencies ERIC T. ROME D.O. HEART FAILURE, MECHANICAL ASSISTANCE AND TRANSPLANTATION CVI Left Ventricular Assist Device An
Modern Left Ventricular Assist Devices (LVAD) : An Intro, Complications, and Emergencies ERIC T. ROME D.O. HEART FAILURE, MECHANICAL ASSISTANCE AND TRANSPLANTATION CVI Left Ventricular Assist Device An
Percutaneous mechanical circulatory support for treatment and prevention of hemodynamic instability Engström, A.E.
 UvA-DARE (Digital Academic Repository) Percutaneous mechanical circulatory support for treatment and prevention of hemodynamic instability Engström, A.E. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Percutaneous mechanical circulatory support for treatment and prevention of hemodynamic instability Engström, A.E. Link to publication Citation for published version
Description. Section: Surgery Effective Date: April 15, Subsection: Transplant Original Policy Date: September 13, 2012 Subject:
 Last Review Status/Date: March 2016 Page: 1 of 30 Description Mechanical devices to assist or replace a failing heart have been developed over many decades of research. A ventricular assist device (VAD)
Last Review Status/Date: March 2016 Page: 1 of 30 Description Mechanical devices to assist or replace a failing heart have been developed over many decades of research. A ventricular assist device (VAD)
Total Artificial Hearts and Implantable Ventricular Assist Devices
 Total Artificial Hearts and Implantable Ventricular Assist Devices Policy Number: 7.03.11 Last Review: 12/2017 Origination: 12/2001 Next Review: 12/2018 Policy Blue Cross and Blue Shield of Kansas City
Total Artificial Hearts and Implantable Ventricular Assist Devices Policy Number: 7.03.11 Last Review: 12/2017 Origination: 12/2001 Next Review: 12/2018 Policy Blue Cross and Blue Shield of Kansas City
Ted Feldman, M.D., MSCAI FACC FESC
 Support Technologies and High Risk Intervention Patient Selection: When Not to Use Them Ted Feldman, M.D., MSCAI FACC FESC Evanston Hospital SCAI Fall Fellows Course Las Vegas December 7-10 th, 2014 Ted
Support Technologies and High Risk Intervention Patient Selection: When Not to Use Them Ted Feldman, M.D., MSCAI FACC FESC Evanston Hospital SCAI Fall Fellows Course Las Vegas December 7-10 th, 2014 Ted
Adult Circulatory Support. Copyright American Society of Artificial Internal Organs. Unauthorized reproduction of this article is prohibited.
 ASAIO Journal 2016 Adult Circulatory Support Percutaneous Venoarterial Extracorporeal Membrane Oxygenation for Refractory Cardiogenic Shock Is Associated with Improved Short- and Long-Term Survival Katarzyna
ASAIO Journal 2016 Adult Circulatory Support Percutaneous Venoarterial Extracorporeal Membrane Oxygenation for Refractory Cardiogenic Shock Is Associated with Improved Short- and Long-Term Survival Katarzyna
Cardiogenic Shock. Carlos Cafri,, MD
 Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Cardiogenic Shock Carlos Cafri,, MD SHOCK= Inadequate Tissue Mechanisms: Perfusion Inadequate oxygen delivery Release of inflammatory mediators Further microvascular changes, compromised blood flow and
Useful? Definition of High-risk? Pre-OP/Intra-OP/Post-OP? Complication vs Benefit? Mortality? Morbidity?
 Preoperative intraaortic balloon counterpulsation in high-risk CABG Stefan Klotz, M.D. Preoperative IABP in high-risk CABG Questions?? Useful? Definition of High-risk? Pre-OP/Intra-OP/Post-OP? Complication
Preoperative intraaortic balloon counterpulsation in high-risk CABG Stefan Klotz, M.D. Preoperative IABP in high-risk CABG Questions?? Useful? Definition of High-risk? Pre-OP/Intra-OP/Post-OP? Complication
Evolving strategies in the treatment of acute myocardial infarction-induced cardiogenic shock
 Perspective Evolving strategies in the treatment of acute myocardial infarction-induced cardiogenic shock Vakhtang Tchantchaleishvili, Heidi Schubmehl, Michael F. Swartz, William Hallinan, H. Todd Massey
Perspective Evolving strategies in the treatment of acute myocardial infarction-induced cardiogenic shock Vakhtang Tchantchaleishvili, Heidi Schubmehl, Michael F. Swartz, William Hallinan, H. Todd Massey
The development of cardiogenic shock portends an extremely poor prognosis. Cardiogenic Shock: A Lethal Complication of Acute Myocardial Infarction
 TREATMENT UPDATE Cardiogenic Shock: A Lethal Complication of Acute Myocardial Infarction David R. Holmes, Jr, MD Mayo Graduate School of Medicine, Mayo Clinic, Rochester, MN Cardiogenic shock is a serious
TREATMENT UPDATE Cardiogenic Shock: A Lethal Complication of Acute Myocardial Infarction David R. Holmes, Jr, MD Mayo Graduate School of Medicine, Mayo Clinic, Rochester, MN Cardiogenic shock is a serious
MANAGEMENT OF CARDIOGENIC SHOCK
 MANAGEMENT OF CARDIOGENIC SHOCK CASE PRESENTATION 37 year old Dutch female No known coronary artery disease risk factors 1 week post partum at time of presentation (G3P3) after an uncomplicated normal
MANAGEMENT OF CARDIOGENIC SHOCK CASE PRESENTATION 37 year old Dutch female No known coronary artery disease risk factors 1 week post partum at time of presentation (G3P3) after an uncomplicated normal
Acute Myocardial Infarction Complicated by Cardiogenic Shock
 Acute Myocardial Infarction Complicated by Cardiogenic Shock Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional
Acute Myocardial Infarction Complicated by Cardiogenic Shock Navin K. Kapur, MD, FACC, FSCAI Assistant Professor, Division of Cardiology Director, Acute Circulatory Support Program Director, Interventional
Name of Policy: Ventricular Assist Devices and Total Artificial Hearts
 Name of Policy: Ventricular Assist Devices and Total Artificial Hearts Policy #: 033 Latest Review Date: February 2014 Category: Surgery Policy Grade: A Background/Definitions: As a general rule, benefits
Name of Policy: Ventricular Assist Devices and Total Artificial Hearts Policy #: 033 Latest Review Date: February 2014 Category: Surgery Policy Grade: A Background/Definitions: As a general rule, benefits
Ventricular Assist Device in Acute Myocardial Infarction
 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY VOL. 67, NO. 16, 2016 ª 2016 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 0735-1097/$36.00 PUBLISHED BY ELSEVIER http://dx.doi.org/1016/j.jacc.2016.02.025
JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY VOL. 67, NO. 16, 2016 ª 2016 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN 0735-1097/$36.00 PUBLISHED BY ELSEVIER http://dx.doi.org/1016/j.jacc.2016.02.025
Total Artificial Hearts and Implantable Ventricular Assist Devices
 Total Artificial Hearts and Implantable Ventricular Assist Devices Policy Number: 7.03.11 Last Review: 12/2018 Origination: 12/2001 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City
Total Artificial Hearts and Implantable Ventricular Assist Devices Policy Number: 7.03.11 Last Review: 12/2018 Origination: 12/2001 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City
Ventricular Assist Devices for Permanent Therapy: Current Status and Future
 Ventricular Assist Devices for Permanent Therapy: Current Status and Future Prospects Francis D. Pagani MD PhD Professor of Cardiac Surgery University of Michigan April 28 th, 2012 Disclosures NHLBI and
Ventricular Assist Devices for Permanent Therapy: Current Status and Future Prospects Francis D. Pagani MD PhD Professor of Cardiac Surgery University of Michigan April 28 th, 2012 Disclosures NHLBI and
Howard Todd Massey, Jae Hwan Choi, Elizabeth J. Maynes, Vakhtang Tchantchaleishvili
 Keynote Lecture Series Temporary support strategies for cardiogenic shock: extracorporeal membrane oxygenation, percutaneous ventricular assist devices and surgically placed extracorporeal ventricular
Keynote Lecture Series Temporary support strategies for cardiogenic shock: extracorporeal membrane oxygenation, percutaneous ventricular assist devices and surgically placed extracorporeal ventricular
Initial experience with Imacor htee-guided management of patients following transplant and mechanical circulatory support.
 Thomas Jefferson University Jefferson Digital Commons Department of Cancer Biology Faculty Papers Department of Cancer Biology Fall 11-1-2012 Initial experience with Imacor htee-guided management of patients
Thomas Jefferson University Jefferson Digital Commons Department of Cancer Biology Faculty Papers Department of Cancer Biology Fall 11-1-2012 Initial experience with Imacor htee-guided management of patients
Left Ventricular Assist Devices (LVADs): Overview and Future Directions
 Left Ventricular Assist Devices (LVADs): Overview and Future Directions FATIMA KARAKI, M.D. PGY-3, DEPARTMENT OF MEDICINE WASHINGTON UNIVERSITY IN ST. LOUIS ST. LOUIS, MISSOURI, USA St. Louis, Missouri,
Left Ventricular Assist Devices (LVADs): Overview and Future Directions FATIMA KARAKI, M.D. PGY-3, DEPARTMENT OF MEDICINE WASHINGTON UNIVERSITY IN ST. LOUIS ST. LOUIS, MISSOURI, USA St. Louis, Missouri,
Cite this article as:
 doi: 10.21037/acs.2018.08.06 Cite this article as: Loforte A, Baiocchi M, Gliozzi G, Coppola G, Di Bartolomeo R, Lorusso R. Percutaneous pulmonary artery venting via jugular vein while on peripheral extracorporeal
doi: 10.21037/acs.2018.08.06 Cite this article as: Loforte A, Baiocchi M, Gliozzi G, Coppola G, Di Bartolomeo R, Lorusso R. Percutaneous pulmonary artery venting via jugular vein while on peripheral extracorporeal
Total Artificial Hearts and Implantable Ventricular Assist Devices
 Total Artificial Hearts and Implantable Ventricular Assist Devices Policy Number: 7.03.11 Last Review: 12/2013 Origination: 12/2001 Next Review: 12/2014 Policy Blue Cross and Blue Shield of Kansas City
Total Artificial Hearts and Implantable Ventricular Assist Devices Policy Number: 7.03.11 Last Review: 12/2013 Origination: 12/2001 Next Review: 12/2014 Policy Blue Cross and Blue Shield of Kansas City
Concomitant Aortic Valve Procedures in Patients Undergoing Implantation of Continuous-Flow LVADs: An INTERMACS Database Analysis
 Concomitant Aortic Valve Procedures in Patients Undergoing Implantation of Continuous-Flow LVADs: An INTERMACS Database Analysis April 11, 2014 Jason O. Robertson, M.D., M.S.; David C. Naftel, Ph.D., Sunil
Concomitant Aortic Valve Procedures in Patients Undergoing Implantation of Continuous-Flow LVADs: An INTERMACS Database Analysis April 11, 2014 Jason O. Robertson, M.D., M.S.; David C. Naftel, Ph.D., Sunil
Multicenter Study of MagLev Technology in Patients Undergoing Mechanical Circulatory Support Therapy with HeartMate 3 (MOMENTUM 3) Long Term Outcomes
 Multicenter Study of MagLev Technology in Patients Undergoing Mechanical Circulatory Support Therapy with (MOMENTUM 3) Long Term Outcomes Mandeep R. Mehra, MD, Daniel J. Goldstein, MD, Nir Uriel, MD, Joseph
Multicenter Study of MagLev Technology in Patients Undergoing Mechanical Circulatory Support Therapy with (MOMENTUM 3) Long Term Outcomes Mandeep R. Mehra, MD, Daniel J. Goldstein, MD, Nir Uriel, MD, Joseph
ECMO and VAD implantation
 1 Udine ECMO Workshop ECMO and VAD implantation Prof. Tomaso Bottio Division of Cardiac Surgery (Director Prof. Gino gerosa) ECMO Extracorporeal membrane oxygena1on (ECMO) is a rescue therapy to support
1 Udine ECMO Workshop ECMO and VAD implantation Prof. Tomaso Bottio Division of Cardiac Surgery (Director Prof. Gino gerosa) ECMO Extracorporeal membrane oxygena1on (ECMO) is a rescue therapy to support
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock. 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI
 Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
Percutaneous Mechanical Circulatory Support for Cardiogenic Shock 24 th Annual San Diego Heart Failure Symposium Ryan R Reeves, MD FSCAI The Need for Circulatory Support Basic Pathophysiologic Problems:
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Total Artificial Hearts and Ventricular Assist Devices Page 1 of 39 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Total Artificial Hearts and Ventricular Assist
Total Artificial Hearts and Ventricular Assist Devices Page 1 of 39 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Total Artificial Hearts and Ventricular Assist
Cardiogenic shock (CS) remains
 The Impella 2.5 and 5.0 devices for ST-elevation myocardial infarction patients presenting with severe and profound cardiogenic shock: The Academic Medical Center intensive care unit experience* Annemarie
The Impella 2.5 and 5.0 devices for ST-elevation myocardial infarction patients presenting with severe and profound cardiogenic shock: The Academic Medical Center intensive care unit experience* Annemarie
