Embolotherapy for Pulmonary Arteriovenous Malformations in Patients without Hereditary Hemorrhagic Telangiectasia
|
|
|
- Rolf Carr
- 5 years ago
- Views:
Transcription
1 Embolotherapy for Pulmonary Arteriovenous Malformations in Patients without Hereditary Hemorrhagic Telangiectasia Ji Hoon Shin, MD Soo Jin Park, MD Gi-Young Ko, MD Hyun-Ki Yoon, MD Dong-Il Gwon, MD Jin-Hyoung Kim, MD Kyu-Bo Sung, MD Index terms: Pulmonary arteriovenous malformation Hereditary hemorrhagic telangiectasia Embolotherapy Amplatz vascular plug DOI: /kjr Korean J Radiol 2010;11: Received May 26, 2009; accepted after revision December 30, All authors: Department of Radiology and Research Institute of Radiology, University of Ulsan College of Medicine, Asan Medical Center, Seoul , Korea Address reprint requests to: Ji Hoon Shin, MD, Department of Radiology and Research Institute of Radiology, University of Ulsan College of Medicine, Asan Medical Center, 86 Asanbyeongwon-gil, Songpa-gu, Seoul , Korea. Tel. (822) Fax. (822) jhshin@amc.seoul.kr Objective: To evaluate the clinical and radiological outcomes of transcatheter embolotherapy for treating sporadic pulmonary arteriovenous malformations (PAVMs) that were not associated with hereditary hemorrhagic telangiectasia. Materials and Methods: Between January 2001 and June 2008, thirty-five sporadic PAVMs were detected in 23 patients. The clinical follow up consisted of assessing the changes of the signs and symptoms of the PAVMs, and radiological evaluation with chest radiographs or chest CT scans. Results: The lower lung regions (63%) and peripheral locations (86%) were the common locations of the PAVMs. Thirty-four PAVMs (97%) had simple architecture (one arterial feeder within a single pulmonary segment). Technical success was achieved in 33 PAVMs (94%); two cases of technical failure were due to catheterization failure (n = 1) and too large a feeding artery (17 mm) that disabled embolotherapy (n = 1). Coils and Amplatz vascular plugs were used in 30 and three PAVMs, respectively. Inadvertent placement of one coil (n = 1) and pulmonary infarction (n = 1) occurred, but no relevant symptoms developed. For the 13 patients with available data, the mean arterial O 2 saturation changed significantly from 92% to 98%. Complete or near-complete involution of the sac was observed in 30 of the 33 embolized PAVMs (91%). In these 33 embolized PAVMs, the mean sac diameter significantly decreased from mm to 0.68 mm. Conclusion: Sporadic PAVMs are mostly the simple type with predominance in the lower lobe and peripheral locations. Transcatheter embolotherapy with coils or Amplatz vascular plugs is a safe and effective treatment for sporadic PAVMs and this provides excellent functional and radiological improvement. P ulmonary arteriovenous malformations (PAVMs) are abnormal communications between the pulmonary arteries and veins without any intervening capillary beds. Severe complications from PAVMs may occur, including massive hemoptysis and hemothorax, as well as neurologic complications, including transient ischemic attack, cerebral stroke and cerebral abscess due to the right-to-left shunting that facilitates the passage of septic emboli into the cerebral circulation (1). Thus treating PAVMs is justified when this is technically feasible, and even for PAVMs that are asymptomatic. About 70-95% of all PAVMs are associated with hereditary hemorrhagic telangiectasia (HHT or Rendu-Osler-Weber syndrome) (2-7), which is an autosomal dominant genetic disorder that is characterized by recurrent epistaxis, mucocutaneous telangiectasia and visceral vascular involvement, including arteriovenous communications that may develop in virtually any organ and especially in the lungs (2, 3). 312 Korean J Radiol 11(3), May/Jun 2010
2 Embolotherapy for Pulmonary AVM The incidence of HHT is particularly high in the American, European and Afro-Caribbean populations (1) and there have been many reports on PAVMs associated with HHT (1, 4-7). The sporadic types of PAVMs, which are not associated with HHT, are rare, and there are only limited reports on their clinical features, radiological characteristics and treatment outcomes. The purpose of this study was to evaluate the clinical and radiological outcomes of performing transcatheter embolotherapy for sporadic PAVMs. MATERIALS AND METHODS The charts of the subjects of this study were reviewed with the approval of our Institutional Review Board. Informed consent for the chart review was waived. Informed consent was obtained from all the patients at the time of the procedures. Patients Of a cohort of 25 consecutive patients with PAVMs and who were referred for transcatheter embolotherapy between January 2001 and June 2008, 23 (92%) had sporadic PAVMs and these patients were included in this report; the two excluded patients had PAVMs associated with HHTs. HHT was diagnosed when at least two criteria were met: 1) the patients had cutaneous telangiectasia, epistaxis and/or visceral involvement such as pulmonary, hepatic or central nervous system AVMs, and 2) there was a first degree family history of HHT (8). The 23 included patients consisted of 21 females and two males, and their average age was 48.1 years (range: years). Embolization Procedure All the patients underwent complete diagnostic pulmonary angiography before their embolotherapy. A 5- Fr Cobra or Headhunter catheter (Cook, Bloomington, IN) was used to access the pulmonary arteries in both lungs. After selective catheterization, the feeding arteries of the PAVMs were embolized, as close to the sac as possible, with using coils or Amplatz vascular plugs (since 2007) of an appropriate size. The embolic coils we used were platinum coils with synthetic fibers (Tornado coils or Nester coils, Cook). The coils were deployed until repeated injections of contrast medium demonstrated the cessation of flow through the PAVMs. The choice of whether to use coils or Amplatz vascular plugs was made at the discretion of the operator. The diameter of the feeding artery was measured on the diagnostic angiograms to select a coil of suitable size. The coil diameter was overestimated to avoid accidental coil migration. The true diameter of the artery at the site of coil placement was determined from the diameter of the selected catheter as a reference for magnification corrections. After positioning the first coil, the second coil of the same diameter or a smaller diameter was then positioned. The patients with multiple PAVMs in both lungs were sometimes treated in two sessions, depending on the patient s tolerance and the total amount of contrast medium used. Follow Up and Data Analysis The clinical follow up consisted of assessing the changes of the signs and symptoms of the PAVMs, and radiological evaluation with chest radiographs and/or chest CT scans. The characteristics of the assessed PAVMs included their number, a lobar location, a central or peripheral location, the angioarchitecture, the diameters of the feeding artery and the aneurysmal sac, the technical success, the complications during embolotherapy or follow up, the change of the arterial oxygen saturation level and the clinical outcome. Pulmonary arteriovenous malformations that were located in the right upper, right middle and left upper lung lobes were considered to be located in the upper lung zones, and the PAVMs that were located in the right and left lower lobes were considered to be located in the lower lung zones. A peripheral location was defined as the lung parenchyma within 4 cm of the pleural surface and a central location was defined as the more centrally located portion of the lung parenchyma (9). The simple type angioarchitecture consisted of one or more arterial feeders within a single pulmonary segment, whereas the complex type had two or more arterial feeders from more than one pulmonary segment (2, 6). The diffuse type was defined as diffuse involvement of multiple segments or lobes with numerous, variably sized lesions (10). The technical success was defined as the successful embolization for all visible PAVMs with observing no residual PAVM filling on the final angiogram. The arterial oxygen saturation level (SaO 2 ), which is a parameter of the right-to-left shunt fraction, was calculated by conducting arterial blood gas analysis before and after embolization. The patient outcome was tracked to the most recent radiological follow up. A PAVM was considered to have been successfully treated if complete or near complete involution (i.e., linear scar only) of the aneurismal sac was noted on the follow-up chest CT scans (6). Disappearance of a sac on the chest radiograph was considered acceptable in those patients who had no follow-up CT scan if the sac had been seen on the chest radiograph taken before embolization (6). Korean J Radiol 11(3), May/Jun
3 Shin et al. Paired Student s t-tests were used to evaluate the statistical significance of the changes of the SaO 2 and the aneurismal sac diameter. The SPSS version 14.0 statistical package (SPSS, Chicago, IL) was used for all the statistical analyses, with p values 0.05 indicating statistical significance. RESULTS The PAVMs in all 23 patients were diagnosed as a result of incidental imaging findings (n = 6, 26%), respiratory symptoms (n = 15, 65%) or neurologic events (n = 2, 9%) (Table 1). Embolotherapy improved the respiratory symptoms in all 15 patients who had respiratory symptoms. The neurologic manifestations such as brain abscess and thalamic infarction with associated symptoms were improved by surgical drainage and conservative management, respectively, before embolotherapy. A total of 35 PAVMs were detected on CT scans in 23 patients, with five patients (22%) having two or more PAVMs each. Twenty-two (63%) PAVMs were located in the lower lung zones (11 each in the right and left lower lobes), and 13 (37%) in the upper lung zones (2 each in the right and left upper lobes, respectively, and 9 in the right middle lobe). Thirty (86%) PAVMs had a peripheral location, and five (14%) had a central location. Thirty-four (97%) PAVMs had simple angioarchitecture, and one (3%) had diffuse angioarchitecture. The mean diameter of the feeding arteries in the 34 simple PAVMs was 5.15 (median, 2.89 mm; range, mm), with two arteries having of a diameter < 3 mm, 18 arteries had a diameter in the range 3-5 mm, and 14 arteries had a diameter > 5 mm. In these 34 simple PAVMs, the mean diameter of the aneurismal sac was Table 1. Characteristics and Outcomes of Pulmonary Arteriovenous Malformations No. Age/ Gender Circumstances No. SaO Lobar Embolic Technical Sac 2 of of Change Location Materials Success Involution* Diagnosis PAVMs (pre post) F.U. Months Remarks / F Chest discomfort 1 RLL Coil Yes Yes / F Dyspnea 1 RML Coil Yes No / F Asymptomatic 1 LLL Coil Yes Yes / F Hemoptysis 1 RLL Coil Yes Yes NA / F Dyspnea 9 RML, RLL, Coil No in one PAVM **Yes** Inadvertent LLL (cath. failure) coil placement / F Dyspnea 2 LLL,RLL Coil No in RLL **Yes** Right lower PAVM lobectomy for (too large feeder) RLL PAVM / F Dyspnea 2 LLL, LLL Coil Yes Yes / F Hemoptysis 1 RML Coil Yes Yes / F Hemoptysis 1 LUL Coil Yes Yes NA / F Hemoptysis 1 RML Coil Yes No NA / M Hemoptysis 2 RLL, LLL Coil Yes No in one NA 01 Pulmonary PVAM infarction / F Dyspnea 1 RUL Coil Yes Yes / F Asymptomatic 1 LLL AVP Yes Yes NA / F Chest discomfort 1 RUL Coil Yes Yes NA / F Asymptomatic 1 RML Coil Yes Yes NA / F Thalamic infarction 1 RLL Coil Yes Yes NA / F Dyspnea 1 RLL Coil Yes Yes / F Hemoptysis 1 RLL Coil Yes Yes / F Hemoptysis 1 LLL AVP Yes Yes NA / F Asymptomatic 1 LUL Coil Yes Yes / F Asymptomatic 2 RML, RLL Coil Yes Yes NA 75 Diffuse type for RLL PAVM / M Brain abscess 1 LLL Coil Yes Yes / F Asymptomatic 1 RML AVP Yes Yes Note. PAVMs = pulmonary arteriovenous malformations, RUL = right upper lobe, RML = right middle lobe, RLL = right lower lobe, LUL = left upper lobe, LLL = left lower lobe, AVP = Amplatz vascular plug, cath. failure = catheterization failure, Sac involution* means complete or near complete involution (i.e. linear scar only) of aneurismal sac, Yes** for treated PAVM(s), NA = not applicable 314 Korean J Radiol 11(3), May/Jun 2010
4 Embolotherapy for Pulmonary AVM (median, mm; range, 4-54 mm). The one diffuse PAVM had an aneurismal sac diameter of 40 mm. Of the 35 PAVMs, 33 (32 simple and one diffuse) were successfully embolized with no residual filling, making the technical success rate 94% (Figs. 1, 2). Twenty-two patients had one session of embolotherapy, while one patient received two sessions of embolotherapy because there were nine PAVMs in both lungs. One to twenty three coils were used for 29 simple PAVMs (average, 5.4 per PAVM), whereas 54 coils were used for the one diffuse type PAVM. Amplatz vascular plugs (6 or 12 mm in diameter) were used for three simple PAVMs, which had feeding artery diameters of 3, 8 and 10 mm (Fig. 2). Each PAVM required only one vascular plug, with complete or near-complete obliteration of the sac observed during follow up. The vascular plug was oversized 30-50% greater than the feeding artery diameter. The cases of technical failure were caused by failure of catheterization (n = 1) or too large a feeding artery (17 mm) that disabled the embolotherapy (n = 1). The former case showed no change in the sac size on the follow-up CT scans; this patient did not undergo further treatment. The latter case was not embolized due to the high risk of coil migration into the right atrium; this patient A B C Fig year-old female with large pulmonary arteriovenous malformation in left lower lobe (Patient No. 6). Simple radiograph (A), left selective pulmonary arteriogram (B), and CT angiogram (C) show large 32-mm-diameter pulmonary arteriovenous malformation (arrows) with single arterial feeder (arrowheads in C) and single draining vein. Left pulmonary arteriogram (D) after embolotherapy with placing four Nester coils shows no evidence of pulmonary arteriovenous malformation. Simple radiograph (E) 19 months after embolotherapy shows complete disappearance of pulmonary arteriovenous malformation shadow. D E Korean J Radiol 11(3), May/Jun
5 Shin et al. underwent right lower lobectomy to remove the PAVM five days later. During embolotherapy, one coil was inadvertently placed into the right upper pulmonary artery without any symptomatic change in one patient (No. 5 in Table 1). In another patient (No. 11 in Table 1), a follow-up CT scan three weeks after embolotherapy showed a pulmonary infarction distal to the embolized pulmonary artery (Fig. 3). His vague right chest pain subsided within several days, and pleurisy did not develop. The SaO 2 follow-up data recorded 2-24 months after embolotherapy was available for 13 patients. Their mean arterial oxygen saturation changed significantly, from 92% (range: 74.0 to 99.8%) before embolization to 98% (range: 91.7 to 100%) after embolization (p = 0.027). Radiological examinations, which consisted of chest CT scans and radiography in 11 patients and chest radiography only in 12 patients, during an average follow-up period of months (range: 1-75 months) showed complete or near-complete involution in 30 of 33 embolized PAVMs (91%). In these 33 embolized PAVMs, the mean diameter of the sac significantly decreased, from mm Fig year-old female with incidentally found pulmonary arteriovenous malformation in left lower lobe (Patient No. 13). Left selective pulmonary arteriogram (A) shows 25-mm-diameter pulmonary arteriovenous malformation (arrows) with single arterial feeder (8 mm in diameter) and single draining vein. Spot radiograph (B) shows deployment of 12 mm-diameter Amplatz vascular plug (arrows). Left pulmonary arteriogram (C) after embolotherapy shows no evidence of pulmonary arteriovenous malformation. Follow-up chest radiograph (D) three months later shows near-complete obliteration of previous pulmonary arteriovenous malformation shadow (arrows). A B C D 316 Korean J Radiol 11(3), May/Jun 2010
6 Embolotherapy for Pulmonary AVM A B C Fig year-old male with small pulmonary arteriovenous malformation in right lower lobe (Patient No. 11). Right pulmonary arteriogram (A) shows small pulmonary arteriovenous malformation (arrows) with single arterial feeder and single draining vein. Right pulmonary arteriogram (B) after embolotherapy with placing two Nester coils shows no evidence of pulmonary arteriovenous malformation. Follow-up CT scan (C) after three weeks shows pulmonary infarction (arrows) distal to embolized pulmonary artery. (range: 4-40 mm) before embolotherapy to mm (range: 0-10 mm) after embolotherapy (p < 0.001). In the remaining three PAVMs, the aneurismal sac diameter decreased, from 36 to 10 mm, from 8 to 6 mm and from 14 to 7 mm, respectively. There was no case of recanalization or sac enlargement during follow up. DISCUSSION Twenty-three of the 25 consecutive patients with PAVMs and who were referred for transcatheter embolotherapy had sporadic PAVMs. In Western countries, PAVMs are highly associated with HHT, which is a common genetic disorder. The reports on HHT and associated PAVMs have been limited in Asian countries. A greater understanding of the characteristics of sporadic PAVMs can help in their management. For example, we found that respiratory symptoms were most common in the patients with sporadic PAVMs, as was the incidental detection of this condition. In contrast, the PAVMs associated with HHT were most commonly detected during systemic screening for HHT (3). In the symptomatic patients with PAVMs associated with HHT, respiratory symptoms are more common than neurologic events, and this is similar to our findings for patients with sporadic PAVMs. Little is known regarding the radiological characteristics of sporadic PAVMs. We found that multiplicity (22%) was less common, while PAVMs located in the lower lung zone (63%) and peripheral locations (86%) were common. These findings are similar to those of previous reports, which also found that lower lobar (65-91%) and peripheral (73%) locations were common in patients with HHTassociated PAVMs (5, 9, 11), although the incidence of multiplicity in the peripheral locations was much higher (35-65%) (3, 7, 11-13). We also found that the simple type of angioarchitecture was more common in the sporadic PAVMs (97%) than that in the HHT-associated (80-92%) PAVMs (5, 9, 11). Yet the patients with HHT are more likely to have multiple, variably sized lesions, including microscopic lesions (3, 4, 6, 11). We found that 94% of all the visible PAVMs were successfully embolized with no residual PAVM filling. It is difficult to compare our technical success rate with that of the previous reports because the parameters of technical success in the previous reports was not described in detail and 16-32% of the patients in the previous reports required several sessions of embolotherapy (6, 9). We observed failure of catheterization in one patient who had nine PAVMs, and one of these in the right middle lobe could not be catheterized. The unembolized PAVM did not change in size. Catheterization failure has been reported to be the most common cause of failure during the first embolotherapy attempt, and so these cases required Korean J Radiol 11(3), May/Jun
7 Shin et al. multiple sessions of embolotherapy, and especially in the cases where the feeding arteries were small (11). Another patient had a feeding artery that was too large for embolotherapy (17 mm). In this patient, the large draining vein was too close to the right atrium, so embolotherapy was not attempted. Even with using an occlusion balloon, it would be difficult to occlude a feeding artery with such a large diameter. Surgery is a good alternative in such cases. An Amplatz vascular plug was successfully used in three patients, and each of these three patients had a relatively large feeding artery. This plug can be used for PAVMs with larger arteries (up to 10 mm) and that have high flow, where the alternative may be multiple coils (14, 15). Complete or near-complete involution was observed in 30 of 33 embolized PAVMs (91%), with a significant decrease of the sac size. This result is comparable to those previously reported results, with complete or near complete involution observed in 75-93% of the PAVMs in patients, of whom most (84-96%) had PAVMs associated with HHT (5, 6, 9). In contrast to these previous studies, in which the rate of recanalization was reported to be 2-19%, we observed no case of recanalization of embolized PAVMs (5, 6, 9). The rate of recanalization tends to be higher in complex PAVMs and lower in patients with simple PAVMs (5). The persistence or reperfusion of successfully embolized PAVMs has been reported to occur during recanalization of the embolized vessels, during growth of a missed or previously small accessory artery and when there is collateral flow into the pulmonary artery (6). No case of recanalization or sac enlargement was noted in this study and this could be due to the fact that the majority of the PAVMs were the simple type of PAVMs where single arterial feeders were present, and there were fewer cases of residual PAVMs. We found that the arterial oxygen saturation level significantly increased after embolotherapy. This improvement was related to the improvement of respiratory symptoms in all 15 patients who displayed respiratory symptoms. Among the observed complications, one patient experienced inadvertent coil embolization (4%), but subsequent pulmonary infarction was not observed. Reflux or migration of the coils within the pulmonary circulation has been reported in 3-6% of patients (5, 16). These coils can migrate to the aneurismal sac or they can reflux into the normal branches of the pulmonary arteries without sequelae. Dislocated coils can be retrieved (5). Three cases of systemic embolization of coils to the mitral valve leaflet or left ventricle have been reported (16, 17). Pulmonary infarction has been reported to occur in 5% of embolotherapy procedures (16). Hemoptysis or chest pain can also occur. Pulmonary infarction may be associated with pleurisy and a high frequency of abnormally enlarged systemic arteries, which can place patients at risk for future hemoptysis (5, 18). Although our patient with pulmonary infarction showed neither pleurisy nor hemoptysis during follow up, these sequelae should be kept in mind when performing further follow-up imaging. The major limitation of this study was the small number of PAVMs, although the study s patients were collected in a large tertiary referral hospital over an eight year period. No comparisons were made with the PAVMs accompanying HHT because these were much less common during the study period. Another limitation was the retrospective design of the study. In addition, the arterial oxygen saturation measurements and CT scans before and after embolotherapy were not available for all the patients. In conclusion, our results indicate that sporadic PAVMs are mostly the simple type with predominance in the lower lobe and the periphery of the lung. Transcatheter embolotherapy is a safe and effective treatment for patients with sporadic PAVMs, and this procedure provides excellent functional and radiological improvement. References 1. Cottin V, Plauchu H, Bayle JY, Barthelet M, Revel D, Cordier JF. Pulmonary arteriovenous malformations in patients with hereditary hemorrhagic telangiectasia. Am J Respir Crit Care Med 2004;169: White RI Jr, Pollak JS, Wirth JA. Pulmonary arteriovenous malformations: diagnosis and transcatheter embolotherapy. J Vasc Interv Radiol 1996;7: Cottin V, Chinet T, Lavole A, Corre R, Marchand E, Reynaud- Gaubert M, et al. Pulmonary arteriovenous malformations in hereditary hemorrhagic telangiectasia: a series of 126 patients. Medicine (Baltimore) 2007;86: Gupta P, Mordin C, Curtis J, Hughes JM, Shovlin CL, Jackson JE. Pulmonary arteriovenous malformations: effect of embolization on right-to-left shunt, hypoxemia, and exercise tolerance in 66 patients. AJR Am J Roentgenol 2002;179: Mager JJ, Overtoom TT, Blauw H, Lammers JW, Westermann CJ. Embolotherapy of pulmonary arteriovenous malformations: long-term results in 112 patients. J Vasc Interv Radiol 2004;15: Pollak JS, Saluja S, Thabet A, Henderson KJ, Denbow N, White RI Jr. Clinical and anatomic outcomes after embolotherapy of pulmonary arteriovenous malformations. J Vasc Interv Radiol 2006;17: Swanson KL, Prakash UB, Stanson AW. Pulmonary arteriovenous fistulas: Mayo Clinic experience, Mayo Clinic Proc 1999;74: Shovlin CL, Guttmacher AE, Buscarini E, Faughnan ME, Hyland RH, Westermann CJ, et al. Diagnostic criteria for hereditary hemorrhagic telangiectasia (Rendu-Osler-Weber syndrome). Am J Med Genet 2000;91: Remy-Jardin M, Dumont P, Brillet PY, Dupuis P, Duhamel A, Remy J. Pulmonary arteriovenous malformations treated with 318 Korean J Radiol 11(3), May/Jun 2010
8 Embolotherapy for Pulmonary AVM embolotherapy: helical CT evaluation of long-term effectiveness after 2-21-year follow-up. Radiology 2006;239: Pierucci P, Murphy J, Henderson KJ, Chyun DA, White RI Jr. New definition and natural history of patients with diffuse pulmonary arteriovenous malformations: twenty-seven-year experience. Chest 2008;133: White RI Jr, Lynch-Nyhan A, Terry P, Buescher PC, Farmlett EJ, Charnas L, et al. Pulmonary arteriovenous malformations: techniques and long-term outcome of embolotherapy. Radiology 1988;169: Dines DE, Arms RA, Bernatz PE, Gomes MR. Pulmonary arteriovenous fistulas. Mayo Clinic Proc 1974;49: Moussouttas M, Fayad P, Rosenblatt M, Hashimoto M, Pollak J, Henderson K, et al. Pulmonary arteriovenous malformations: cerebral ischemia and neurologic manifestations. Neurology 2000;55: Andersen PE, Kjeldsen AD. Occlusion of pulmonary arteriovenous malformations by use of vascular plug. Acta Radiol 2007;48: Ferro C, Rossi UG, Bovio G, Seitun S, Rossi GA. Percutaneous transcatheter embolization of a large pulmonary arteriovenous fistula with an amplatzer vascular plug. Cardiovasc Intervent Radiol 2007;30: Prasad V, Chan RP, Faughnan ME. Embolotherapy of pulmonary arteriovenous malformations: efficacy of platinum versus stainless steel coils. J Vasc Interv Radiol 2004;15: Haitjema T, ten Berg JM, Overtoom TT, Ernst JM, Westermann CJ. Unusual complications after embolization of a pulmonary arteriovenous malformation. Chest 1996;109: Brillet PY, Dumont P, Bouaziz N, Duhamel A, Laurent F, Remy J, et al. Pulmonary arteriovenous malformation treated with embolotherapy: systemic collateral supply at multidetector CT angiography after 2-20-year follow-up. Radiology 2007;242: Korean J Radiol 11(3), May/Jun
Association between reperfusion and shrinkage percentage of aneurysmal sac after
 Original article Association between reperfusion and shrinkage percentage of aneurysmal sac after embolization of pulmonary arteriovenous malformation: Evaluation based on contrast-enhanced thin-section
Original article Association between reperfusion and shrinkage percentage of aneurysmal sac after embolization of pulmonary arteriovenous malformation: Evaluation based on contrast-enhanced thin-section
(received 8 March 2013, accepted 15 April 2013)
 Akita J Med 40 : 13-21, 2013 (13) Kazuhiro Sato 1), Takanobu Shioya 2), Mariko Asano 1), Yuji Okuda 1), Hajime Miura 1), Masaaki Sano 1), Kenji Iino 1), Toshimitsu Kosaka 1), Hiroyuki Watanabe 1), Manabu
Akita J Med 40 : 13-21, 2013 (13) Kazuhiro Sato 1), Takanobu Shioya 2), Mariko Asano 1), Yuji Okuda 1), Hajime Miura 1), Masaaki Sano 1), Kenji Iino 1), Toshimitsu Kosaka 1), Hiroyuki Watanabe 1), Manabu
Pulmonary arteriovenous malformations (PAVMs)
 Endovascular Repair of PAVM by Embolotherapy In a patient with a transient ischemic attack or stroke, a positive contrast echocardiogram does not always mean a patent foramen ovale. BY ROBERT I. WHITE,
Endovascular Repair of PAVM by Embolotherapy In a patient with a transient ischemic attack or stroke, a positive contrast echocardiogram does not always mean a patent foramen ovale. BY ROBERT I. WHITE,
New Definition and Natural History of Patients With Diffuse Pulmonary Arteriovenous Malformations*
 Original Research PULMONARY VASCULAR DISEASE New Definition and Natural History of Patients With Diffuse Pulmonary Arteriovenous Malformations* Twenty-Seven Year Experience Paola Pierucci, MD; Joshua Murphy,
Original Research PULMONARY VASCULAR DISEASE New Definition and Natural History of Patients With Diffuse Pulmonary Arteriovenous Malformations* Twenty-Seven Year Experience Paola Pierucci, MD; Joshua Murphy,
Where is the Origin of the Last Normal Branch from Feeding Artery of Pulmonary Arteriovenous Malformations?
 Cardiovasc Intervent Radiol (2018) 41:1849 1856 https://doi.org/10.1007/s00270-018-2063-4 CLINICAL INVESTIGATION ARTERIAL INTERVENTIONS Where is the Origin of the Last Normal Branch from Feeding Artery
Cardiovasc Intervent Radiol (2018) 41:1849 1856 https://doi.org/10.1007/s00270-018-2063-4 CLINICAL INVESTIGATION ARTERIAL INTERVENTIONS Where is the Origin of the Last Normal Branch from Feeding Artery
Endovascular Management of Pulmonary Arteriovenous Malformation
 Bahrain Medical Bulletin, Vol. 36, No. 3, September 2014 ABSTRACT Endovascular Management of Pulmonary Arteriovenous Malformation Omar Mohammed Omar, MSc* Wael Hamed Ibrahim, MD, PhD** Noora Abdulaziz
Bahrain Medical Bulletin, Vol. 36, No. 3, September 2014 ABSTRACT Endovascular Management of Pulmonary Arteriovenous Malformation Omar Mohammed Omar, MSc* Wael Hamed Ibrahim, MD, PhD** Noora Abdulaziz
Pulmonary Arteriovenous Malformations And Osler Weber Rendu Syndrome: An Unusual Cause Of Dyspnea
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 5 Number 2 Pulmonary Arteriovenous Malformations And Osler Weber Rendu Syndrome: An Unusual Cause Of H Amin, A Friere, C Lal, M Pugazhenthi Citation
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 5 Number 2 Pulmonary Arteriovenous Malformations And Osler Weber Rendu Syndrome: An Unusual Cause Of H Amin, A Friere, C Lal, M Pugazhenthi Citation
Neurologic Manifestation as Initial Presentation in a Case of Hereditary Haemorrhagic Telangiectasia
 Clinical Medicine Insights: Case Reports Case report Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Neurologic Manifestation as Initial Presentation in a
Clinical Medicine Insights: Case Reports Case report Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Neurologic Manifestation as Initial Presentation in a
Stephen Binsse, Jacques Sellier, Jérome Lucas, Mostafa El Hajjam, Pascal Lacombe
 SPONTANEOUS RUPTURE OF PULMONARY ARTERIOVENOUS MALFORMATIONS IN HEREDITARY HAEMORRHAGIC TELANGIECTASIA (HHT) REVIEW OF 12 CASES Stephen Binsse, Jacques Sellier, Jérome Lucas, Mostafa El Hajjam, Pascal
SPONTANEOUS RUPTURE OF PULMONARY ARTERIOVENOUS MALFORMATIONS IN HEREDITARY HAEMORRHAGIC TELANGIECTASIA (HHT) REVIEW OF 12 CASES Stephen Binsse, Jacques Sellier, Jérome Lucas, Mostafa El Hajjam, Pascal
International Journal of Diagnostic Imaging, 2014, Vol. 1, No. 2
 CASE REPORT Transthoracic contrast echocardiography for detection of pulmonary arteriovenous malformations in hereditary hemorrhagic telangiectasia: How can the process be improved for patient safety?
CASE REPORT Transthoracic contrast echocardiography for detection of pulmonary arteriovenous malformations in hereditary hemorrhagic telangiectasia: How can the process be improved for patient safety?
Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
.. CHEST Original Research
 .. CHEST Original Research Diffuse Pulmonary Arteriovenous Malformations in Hereditary Hemorrhagic Telangiectasia* PULMONARY ARTERIOVENOUS MALFORMATIONS Long-term Results of Embolization According to the
.. CHEST Original Research Diffuse Pulmonary Arteriovenous Malformations in Hereditary Hemorrhagic Telangiectasia* PULMONARY ARTERIOVENOUS MALFORMATIONS Long-term Results of Embolization According to the
Pulmonary arteriovenous malformations (PAVMs)
 Pulmonary Arteriovenous Malformations and Coronary Artery Fistulas Diagnosis, evaluation, and indications for closure. BY MARK D. OSTEN, MD, AND ERIC M. HORLICK, MDCM Pulmonary arteriovenous malformations
Pulmonary Arteriovenous Malformations and Coronary Artery Fistulas Diagnosis, evaluation, and indications for closure. BY MARK D. OSTEN, MD, AND ERIC M. HORLICK, MDCM Pulmonary arteriovenous malformations
Treating Pulmonary Arteriovenous Malformations: What to Do and What Not to Do
 Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 2016 Treating Pulmonary Arteriovenous Malformations: What to Do and What Not to Do Ripal Gandhi Baptist Hospital
Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 2016 Treating Pulmonary Arteriovenous Malformations: What to Do and What Not to Do Ripal Gandhi Baptist Hospital
Preliminary experience with the micro vascular plug for the treatment of pulmonary arteriovenous malformation: case series of four patients
 Duvnjak et al. CVIR Endovascular (2018) 1:19 https://doi.org/10.1186/s42155-018-0027-z CVIR Endovascular CASE REPORT Preliminary experience with the micro vascular plug for the treatment of pulmonary arteriovenous
Duvnjak et al. CVIR Endovascular (2018) 1:19 https://doi.org/10.1186/s42155-018-0027-z CVIR Endovascular CASE REPORT Preliminary experience with the micro vascular plug for the treatment of pulmonary arteriovenous
Pulmonary arteriovenous malformations: endovascular therapy
 Review rticle Pulmonary arteriovenous malformations: endovascular therapy Murthy R. Chamarthy, Harold Park, Patrick Sutphin, Girish Kumar, Daniel Lamus, Sachin Saboo, Matthew nderson, Sanjeeva P. Kalva
Review rticle Pulmonary arteriovenous malformations: endovascular therapy Murthy R. Chamarthy, Harold Park, Patrick Sutphin, Girish Kumar, Daniel Lamus, Sachin Saboo, Matthew nderson, Sanjeeva P. Kalva
Endovascular treatment of pulmonary arteriovenous malformations in hereditary haemorrhagic telangiectasia
 Published 28 July 2015, doi:10.4414/smw.2015.14151 Cite this as: Endovascular treatment of pulmonary arteriovenous malformations in hereditary haemorrhagic telangiectasia Malik Babaker a, Stepane Breault
Published 28 July 2015, doi:10.4414/smw.2015.14151 Cite this as: Endovascular treatment of pulmonary arteriovenous malformations in hereditary haemorrhagic telangiectasia Malik Babaker a, Stepane Breault
Individual Pulmonary Vein Atresia in Adults: Report of Two Cases
 Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia
 Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia Vincent Cottin, Henri Plauchu, Jean-Yves Bayle, Martine Barthelet, Didier Revel, and Jean-François Cordier Service
Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia Vincent Cottin, Henri Plauchu, Jean-Yves Bayle, Martine Barthelet, Didier Revel, and Jean-François Cordier Service
Pulmonary arteriovenous malformations presenting as difficult-to-control asthma: a case report
 Navratil et al. Journal of Medical Case Reports 2013, 7:32 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Pulmonary arteriovenous malformations presenting as difficult-to-control asthma: a case
Navratil et al. Journal of Medical Case Reports 2013, 7:32 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Pulmonary arteriovenous malformations presenting as difficult-to-control asthma: a case
Hereditary Hemorrhagic Telangiectasia or Osler-Weber -Rendu Syndrome: Management of Epistaxis in 4 Cases.
 Hereditary Hemorrhagic Telangiectasia or Osler-Weber -Rendu Syndrome: Management of Epistaxis in 4 Cases. Salina H a, Lim PS a, Gendeh BS a a Department of Otorhinolaringology-Head and Neck Surgery, Faculty
Hereditary Hemorrhagic Telangiectasia or Osler-Weber -Rendu Syndrome: Management of Epistaxis in 4 Cases. Salina H a, Lim PS a, Gendeh BS a a Department of Otorhinolaringology-Head and Neck Surgery, Faculty
Endovascular Treatment of Pulmonary and Cerebral Arteriovenous
 Endovascular Treatment of Pulmonary and Cerebral Arteriovenous Current Pharmaceutical Design, 2005, 11, 000-000 1 1381-6128/05 $50.00+.00 Â 2005 Bentham Science Publishers Ltd. Teleangiectasia E. De Cillis1,
Endovascular Treatment of Pulmonary and Cerebral Arteriovenous Current Pharmaceutical Design, 2005, 11, 000-000 1 1381-6128/05 $50.00+.00 Â 2005 Bentham Science Publishers Ltd. Teleangiectasia E. De Cillis1,
L angiografia ha ancora un ruolo?
 Aggiornamenti di Radiologia Interventistica L angiografia ha ancora un ruolo? Roberto Iezzi Dipartimento di Bioimmagini e Scienze Radiologiche Istituto di Radiologia, Policlinico A. Gemelli Università
Aggiornamenti di Radiologia Interventistica L angiografia ha ancora un ruolo? Roberto Iezzi Dipartimento di Bioimmagini e Scienze Radiologiche Istituto di Radiologia, Policlinico A. Gemelli Università
Pulmonary arteriovenous fistula
 International Journal of Medical Imaging 2014; 2(2): 34-38 Published online April 10, 2014 (http://www.sciencepublishinggroup.com/j/ijmi) doi: 10.11648/j.ijmi.20140202.16 Pulmonary arteriovenous fistula
International Journal of Medical Imaging 2014; 2(2): 34-38 Published online April 10, 2014 (http://www.sciencepublishinggroup.com/j/ijmi) doi: 10.11648/j.ijmi.20140202.16 Pulmonary arteriovenous fistula
Pulmonary Arteriovenous Malformations: Current Technique of Transcatheter Embolization and Subsequent Management
 Educational Paper from SIRAP Pulmonary Arteriovenous Malformations: Current Technique of Transcatheter Embolization and Subsequent Management 1) Department of Radiology, Nagoya City University Graduate
Educational Paper from SIRAP Pulmonary Arteriovenous Malformations: Current Technique of Transcatheter Embolization and Subsequent Management 1) Department of Radiology, Nagoya City University Graduate
Cerebral abscesses among Danish patients with hereditary haemorrhagic telangiectasia
 Acta Neurol Scand 2014: 129: 192 197 DOI: 10.1111/ane.12167 2013 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd ACTA NEUROLOGICA SCANDINAVICA Cerebral abscesses among Danish patients with hereditary
Acta Neurol Scand 2014: 129: 192 197 DOI: 10.1111/ane.12167 2013 John Wiley & Sons A/S. Published by John Wiley & Sons Ltd ACTA NEUROLOGICA SCANDINAVICA Cerebral abscesses among Danish patients with hereditary
Imaging of Hereditary Hemorrhagic Telangiectasia
 Cardiovasc Intervent Radiol DOI 10.1007/s00270-008-9344-2 PICTORIAL ESSAY Imaging of Hereditary Hemorrhagic Telangiectasia Marie-France Carette Æ Cosmina Nedelcu Æ Marc Tassart Æ Jean-Didier Grange Æ Marie
Cardiovasc Intervent Radiol DOI 10.1007/s00270-008-9344-2 PICTORIAL ESSAY Imaging of Hereditary Hemorrhagic Telangiectasia Marie-France Carette Æ Cosmina Nedelcu Æ Marc Tassart Æ Jean-Didier Grange Æ Marie
Coils and plugs have emerged as the most commonly
 The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
Hereditary hemorrhagic telangiectasia (HHT): Whole body imaging findings with emphasis in central nervous system involvement
 Hereditary hemorrhagic telangiectasia (HHT): Whole body imaging findings with emphasis in central nervous system involvement Poster No.: C-824 Congress: ECR 2009 Type: Topic: Authors: Keywords: DOI: Educational
Hereditary hemorrhagic telangiectasia (HHT): Whole body imaging findings with emphasis in central nervous system involvement Poster No.: C-824 Congress: ECR 2009 Type: Topic: Authors: Keywords: DOI: Educational
Transcatheter closure of right coronary artery fistula to the right ventricle
 Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Case Report Transcatheter closure of right coronary artery fistula to the right ventricle Abstract Coronary artery fistula (CAF) is an uncommon anomaly usually congenital but can be acquired. Although,
Graded contrast echocardiography in pulmonary arteriovenous malformations
 Eur Respir J 2010; 35: 1279 1285 DOI: 10.1183/09031936.00104309 CopyrightßERS 2010 Graded contrast echocardiography in pulmonary arteriovenous malformations J.A. Parra*, J. Bueno #, J. Zarauza ", C. Fariñas-Alvarez
Eur Respir J 2010; 35: 1279 1285 DOI: 10.1183/09031936.00104309 CopyrightßERS 2010 Graded contrast echocardiography in pulmonary arteriovenous malformations J.A. Parra*, J. Bueno #, J. Zarauza ", C. Fariñas-Alvarez
Reproducibility Of Exercise Testing In Patients With Pulmonary Arteriovenous Malformations
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2012 Reproducibility Of Exercise Testing In Patients With
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2012 Reproducibility Of Exercise Testing In Patients With
Anatomy, Physiology and Management of Patients with Diffuse Pulmonary Arteriovenous Malformations
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 4-12-2009 Anatomy, Physiology and Management of Patients with Diffuse
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 4-12-2009 Anatomy, Physiology and Management of Patients with Diffuse
Delayed Intracranial Air Embolism After Interventional Therapy of Congenital Pulmonary Arteriovenous Fistula
 Delayed Intracranial Air Embolism After Interventional Therapy of Congenital Pulmonary Arteriovenous Fistula WA N G W E I D E PA R T M E N T O F C A R D I O LO GY C H I L DREN S H O S P I TA L, Z H E J
Delayed Intracranial Air Embolism After Interventional Therapy of Congenital Pulmonary Arteriovenous Fistula WA N G W E I D E PA R T M E N T O F C A R D I O LO GY C H I L DREN S H O S P I TA L, Z H E J
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by
 24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
24. An infant with recurrent pneumonia underwent a frontal chest radiograph (Fig 24-A) followed by diagnosis? ndings, what is the most likely A. Pulmonary sequestration B. Congenital pulmonary airway malformation
Role of Transthoracic Contrast Echocardiography in the Clinical Diagnosis of Hereditary Hemorrhagic Telangiectasia
 CHEST Original Research PULMONARY PROCEDURES Role of Transthoracic Contrast Echocardiography in the Clinical Diagnosis of Hereditary Hemorrhagic Telangiectasia Sebastiaan Velthuis, MD ; Veronique M. M.
CHEST Original Research PULMONARY PROCEDURES Role of Transthoracic Contrast Echocardiography in the Clinical Diagnosis of Hereditary Hemorrhagic Telangiectasia Sebastiaan Velthuis, MD ; Veronique M. M.
Pulmonary vascular anatomy & anatomical variants
 Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
BRTO: Updates to Techniques
 Session XIV: BRTO, PARTO and Portal Hypertension GEST2016 BRTO: Updates to Techniques Hiro Kiyosue Oita University Hospital, Japan Hiro Kiyosue, MD Royalty: Cook, Medkit Consulting Fee: Stryker Japan,
Session XIV: BRTO, PARTO and Portal Hypertension GEST2016 BRTO: Updates to Techniques Hiro Kiyosue Oita University Hospital, Japan Hiro Kiyosue, MD Royalty: Cook, Medkit Consulting Fee: Stryker Japan,
Genotype phenotype relationship in Hereditary Hemorrhagic Telangiectasia
 JMG Online First, published on September 9, 2005 as 10.1136/jmg.2005.035451 Genotype phenotype relationship in Hereditary Hemorrhagic Telangiectasia T.G.W. Letteboer 1, J.J. Mager 2, R.J. Snijder 2, B.P.C.
JMG Online First, published on September 9, 2005 as 10.1136/jmg.2005.035451 Genotype phenotype relationship in Hereditary Hemorrhagic Telangiectasia T.G.W. Letteboer 1, J.J. Mager 2, R.J. Snijder 2, B.P.C.
Supraselective bronchial artery embolization in patients with massive hemoptysis.
 Supraselective bronchial artery embolization in patients with massive hemoptysis. Poster No.: C-2259 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit A. Svare, S. Rud#icka, E. Kadakovska,
Supraselective bronchial artery embolization in patients with massive hemoptysis. Poster No.: C-2259 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit A. Svare, S. Rud#icka, E. Kadakovska,
EGIS BILIARY STENT. 1. Features & Benefits 2. Ordering information 3. References
 EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
Coronary to Bronchial Artery Fistula Causing Massive Hemoptysis in Patients with Longstanding Pulmonary Tuberculosis
 Case Report DOI: 10.3348/kjr.2012.13.1.102 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(1):102-106 Coronary to Bronchial Artery Fistula Causing Massive Hemoptysis in Patients with Longstanding
Case Report DOI: 10.3348/kjr.2012.13.1.102 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(1):102-106 Coronary to Bronchial Artery Fistula Causing Massive Hemoptysis in Patients with Longstanding
Endovascular Treatment of Type II Endoleak Following TEVAR for Thoracic Aortic Aneurysm: Squeeze Technique to Reach the Aneurysmal Sac
 Endovascular Treatment of Type II Endoleak Following TEVAR for Thoracic Aortic Aneurysm: Squeeze Technique to Reach the Aneurysmal Sac Chang Won Kim Department of Radiology Pusan National University Hospital
Endovascular Treatment of Type II Endoleak Following TEVAR for Thoracic Aortic Aneurysm: Squeeze Technique to Reach the Aneurysmal Sac Chang Won Kim Department of Radiology Pusan National University Hospital
Complications of Portal Vein Embolization: Evaluation on Cross-Sectional Imaging
 Pictorial Essay Intervention http://dx.doi.org/10.3348/kjr.2015.16.5.1079 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2015;16(5):1079-1085 Complications of Portal Vein Embolization: Evaluation on Cross-Sectional
Pictorial Essay Intervention http://dx.doi.org/10.3348/kjr.2015.16.5.1079 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2015;16(5):1079-1085 Complications of Portal Vein Embolization: Evaluation on Cross-Sectional
Epidermiology Early pulmonary embolism
 Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
TCTAP C-217 Bilateral Pulmonary Arterio Venus Fistula Managed by Vascular Plugs and Coil Manotosh Panja 1 1 BelleVue Clinic, India
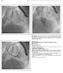 S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
S450 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY, VOL. 65, NO. 17, SUPPL S, 2015 Case Summary. Aneurysm at LVOT is a rare complication after Bentall operation and the aneurysm may increase in size. In
Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!!
 The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
The lateral chest radiograph: Challenging area around the thoracic aorta!!! Do you want to be an excellent Radiologist? - Focus on the thoracic aorta on lateral chest image!!! Dong Yoon Han 1, So Youn
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
A 33-year-old male with a chest lesion on a routine chest radiograph
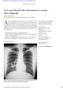 WHAT S YOUR DIAGNOSIS? A 33-year-old male with a chest lesion on a routine chest radiograph Editor: Husn Frayha Authors: Mohammed Khalid,*Neelam Malik, Suzanne Abbas, A 33-year-old Bahraini male presented
WHAT S YOUR DIAGNOSIS? A 33-year-old male with a chest lesion on a routine chest radiograph Editor: Husn Frayha Authors: Mohammed Khalid,*Neelam Malik, Suzanne Abbas, A 33-year-old Bahraini male presented
Asymptomatic Primary Isolated Pulmonary Vein Stenosis in an Adult: A Case Report 1
 Asymptomatic Primary Isolated Pulmonary Vein Stenosis in an Adult: A Case Report 1 Ji Hyun Kim, M.D., Ho Sung Lee, M.D., Jae Sung Choi, M.D., Ju Ock Na, M.D., Yong Hoon Kim, M.D., Sung Shick Jou, M.D.
Asymptomatic Primary Isolated Pulmonary Vein Stenosis in an Adult: A Case Report 1 Ji Hyun Kim, M.D., Ho Sung Lee, M.D., Jae Sung Choi, M.D., Ju Ock Na, M.D., Yong Hoon Kim, M.D., Sung Shick Jou, M.D.
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Congenital Lung Malformations: Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 51-60, Abr.-Jun., 2006 Congenital Lung Malformations: Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
A Rare Case of Cerebral Air Embolism Caused by Pulmonary Arteriovenous Malformation After Removal of a Central Venous Catheter
 Case Report This is Advance Publication Article Kurume Medical Journal, 65, 00-00, 2018 A Rare Case of Cerebral Air Embolism Caused by Pulmonary Arteriovenous Malformation After Removal of a Central Venous
Case Report This is Advance Publication Article Kurume Medical Journal, 65, 00-00, 2018 A Rare Case of Cerebral Air Embolism Caused by Pulmonary Arteriovenous Malformation After Removal of a Central Venous
Fatal rupture of pulmonary arteriovenous malformation in hereditary haemorrhagic telangiectasis and severe PAH
 Eur Respir Rev 2009; 18: 111, 42 46 DOI: 10.1183/09059180.00011113 CopyrightßERSJ Ltd 2009 CASE REPORT Fatal rupture of pulmonary arteriovenous malformation in hereditary haemorrhagic telangiectasis and
Eur Respir Rev 2009; 18: 111, 42 46 DOI: 10.1183/09059180.00011113 CopyrightßERSJ Ltd 2009 CASE REPORT Fatal rupture of pulmonary arteriovenous malformation in hereditary haemorrhagic telangiectasis and
As data on coil embolization
 A Complete Embolization System The Ruby coil and POD devices. As data on coil embolization become more A robust, so must the tools and technology we use. Penumbra, Inc. has advanced this technology with
A Complete Embolization System The Ruby coil and POD devices. As data on coil embolization become more A robust, so must the tools and technology we use. Penumbra, Inc. has advanced this technology with
You Won t Believe What I Saw on. Disclosures. Goals. Dimensions 2013 October 18 th Michael Pfeiffer, MD. No Financial Disclosures
 You Won t Believe What I Saw on that ECHO! Dimensions 2013 October 18 th Michael Pfeiffer, MD Disclosures No Financial Disclosures Goals Review unusual and unique echocardiographic images. Briefly present
You Won t Believe What I Saw on that ECHO! Dimensions 2013 October 18 th Michael Pfeiffer, MD Disclosures No Financial Disclosures Goals Review unusual and unique echocardiographic images. Briefly present
1. Introduction. Central European Journal of Medicine. Sadık Kadri Açikgöz 1, Gülten Taçoy 1*, Baran Önal 2, Beytullah Yıldırım 3, Atiye Çengel 1
 Cent. Eur. J. Med. 4(3) 2009 369-373 DOI: 10.2478/s11536-009-0028-3 Central European Journal of Medicine Arterial embolisation and coiling for high-output heart failure and pulmonary hypertension ınduced
Cent. Eur. J. Med. 4(3) 2009 369-373 DOI: 10.2478/s11536-009-0028-3 Central European Journal of Medicine Arterial embolisation and coiling for high-output heart failure and pulmonary hypertension ınduced
Embolization Therapy: Pulmonary AVMs; Veno-Venous Collaterals. Matthew J. Gillespie MD, FSCAI The Children s Hospital of Philadelphia
 Embolization Therapy: Pulmonary AVMs; Veno-Venous Collaterals Matthew J. Gillespie MD, FSCAI The Children s Hospital of Philadelphia SCAI Fellows Course 2014 December 8, 2014 Presenter Disclosure Information
Embolization Therapy: Pulmonary AVMs; Veno-Venous Collaterals Matthew J. Gillespie MD, FSCAI The Children s Hospital of Philadelphia SCAI Fellows Course 2014 December 8, 2014 Presenter Disclosure Information
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Intrahepatic Portosystemic Venous Shunt: Successful Embolization Using the Amplatzer Vascular Plug II
 Case Report http://dx.doi.org/10.3348/kjr.2012.13.6.827 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(6):827-831 Intrahepatic Portosystemic Venous Shunt: Successful Embolization Using the Amplatzer
Case Report http://dx.doi.org/10.3348/kjr.2012.13.6.827 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(6):827-831 Intrahepatic Portosystemic Venous Shunt: Successful Embolization Using the Amplatzer
An Arteriovenous Malformation in the Suprapatellar Fat Pad of the Knee associated with Klippel-Trenaunay- Weber Syndrome: A Case Report 1
 n rteriovenous Malformation in the Suprapatellar Fat Pad of the Knee associated with Klippel-Trenaunay- Weber Syndrome: Case Report 1 Mi Hyun Park, M.D., Soon Tae Kwon, M.D., yung Seok Shin, M.D., Young
n rteriovenous Malformation in the Suprapatellar Fat Pad of the Knee associated with Klippel-Trenaunay- Weber Syndrome: Case Report 1 Mi Hyun Park, M.D., Soon Tae Kwon, M.D., yung Seok Shin, M.D., Young
Vascular Malformations of the Brain. William A. Cox, M.D. Forensic Pathologist/Neuropathologist. September 8, 2014
 Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Peripheral Arteriovenous Malformations with a Dominant Outflow Vein: Results of Ethanol Embolization
 Peripheral Arteriovenous Malformations with a Dominant Outflow Vein: Results of Ethanol Embolization Sung Ki Cho, MD 1 Young Soo Do, MD 1 Dong Ik Kim, MD 2 Young Wook Kim, MD 2 Sung Wook Shin, MD 1 Kwang
Peripheral Arteriovenous Malformations with a Dominant Outflow Vein: Results of Ethanol Embolization Sung Ki Cho, MD 1 Young Soo Do, MD 1 Dong Ik Kim, MD 2 Young Wook Kim, MD 2 Sung Wook Shin, MD 1 Kwang
Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University Hospital Sangmin Kim
 Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Beyond Pulmonary Emboli: Acquired Abnormalities of the Pulmonary Arteries on CTA
 Beyond Pulmonary Emboli: Acquired Abnormalities of the Pulmonary Arteries on CTA Sean Cleary, MD and Katherine Kaproth-Joslin, MD/PhD University of Rochester Medical Center Rochester, NY Financial Disclosures
Beyond Pulmonary Emboli: Acquired Abnormalities of the Pulmonary Arteries on CTA Sean Cleary, MD and Katherine Kaproth-Joslin, MD/PhD University of Rochester Medical Center Rochester, NY Financial Disclosures
Palliative Treatment of Malignant Esophagopulmonary Fistulas With Covered Expandable Metallic Stents
 Vascular and Interventional Radiology Original Research Vascular and Interventional Radiology Original Research FOCUS ON: Kyung Rae Kim 1,2 Ji Hoon Shin 2 Ho-Young Song 2 Gi-Young Ko 2 Jin Hyoung Kim 2
Vascular and Interventional Radiology Original Research Vascular and Interventional Radiology Original Research FOCUS ON: Kyung Rae Kim 1,2 Ji Hoon Shin 2 Ho-Young Song 2 Gi-Young Ko 2 Jin Hyoung Kim 2
Transcatheter Embolization in the Treatment of Coronary Artery Fistulas
 JACC Vol. 18, No. I 187 REPORTS ON THERAPY Transcatheter Embolization in the Treatment of Coronary Artery Fistulas JOHN F. REIDY, FRCP, FRCR, RUI T. ANJOS, MD, SHAKEEL A. QURESHI, MRCP, EDWARD J. BAKER,
JACC Vol. 18, No. I 187 REPORTS ON THERAPY Transcatheter Embolization in the Treatment of Coronary Artery Fistulas JOHN F. REIDY, FRCP, FRCR, RUI T. ANJOS, MD, SHAKEEL A. QURESHI, MRCP, EDWARD J. BAKER,
MINIMALLY INVASIVE MANAGEMENT OF RENOVASCULAR COMPLICATIONS AFTER RENAL GRAFT TRANSPLANTATION
 MINIMALLY INVASIVE MANAGEMENT OF RENOVASCULAR COMPLICATIONS AFTER RENAL GRAFT TRANSPLANTATION Gortes, Francisco Javier B.S; Salsamendi, Jason Thomas M.D LEARNING OBJECTIVES Educate physicians on the prompt
MINIMALLY INVASIVE MANAGEMENT OF RENOVASCULAR COMPLICATIONS AFTER RENAL GRAFT TRANSPLANTATION Gortes, Francisco Javier B.S; Salsamendi, Jason Thomas M.D LEARNING OBJECTIVES Educate physicians on the prompt
HEMOPTYSIS. Prof. G. Zuliani
 HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Pulmonary arteriovenous malformations and other pulmonary. aspects of hereditary haemorrhagic telangiectasia
 Eur Respir Mon 2011; 54: 218 245. DOI: 10.1183/1025448x.10008410 Pulmonary arteriovenous malformations and other pulmonary aspects of hereditary haemorrhagic telangiectasia Claire L Shovlin, 1 2 Peter
Eur Respir Mon 2011; 54: 218 245. DOI: 10.1183/1025448x.10008410 Pulmonary arteriovenous malformations and other pulmonary aspects of hereditary haemorrhagic telangiectasia Claire L Shovlin, 1 2 Peter
Rendu Osler Weber disease or Hereditary Hemorrhagic Telangiectasia (HHT): liver vascular involvement
 Rendu Osler Weber disease or Hereditary Hemorrhagic Telangiectasia (HHT): liver vascular involvement Elisabetta Buscarini Gastroenterology Dept European Reference Center for HHT ASST Ospedale Maggiore
Rendu Osler Weber disease or Hereditary Hemorrhagic Telangiectasia (HHT): liver vascular involvement Elisabetta Buscarini Gastroenterology Dept European Reference Center for HHT ASST Ospedale Maggiore
CY2015 Hospital Outpatient: Endovascular Procedure APCs and Complexity Adjustments
 CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
CY2015 Hospital Outpatient: Endovascular Procedure APCs Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) CMS finalized the implementation of 25 Comprehensive APC to further
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils
 High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
Bronchobiliary fistula treated with histoacryl embolization under bronchoscopic guidance: A case report
 Respiratory Medicine CME (2008) 1, 164 168 respiratory MEDICINE CME CASE REPORT Bronchobiliary fistula treated with histoacryl embolization under bronchoscopic guidance: A case report Jung Hyun Kim a,
Respiratory Medicine CME (2008) 1, 164 168 respiratory MEDICINE CME CASE REPORT Bronchobiliary fistula treated with histoacryl embolization under bronchoscopic guidance: A case report Jung Hyun Kim a,
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Pulmonary arterio-venous fistulas. Pulmonary arterio-venous fistulas. Pulmonary angiogram. Typical patient presentation
 Pulmonary arterio-venous fistulas Pulmonary arterio-venous fistulas No conflicts of interest to declare Julien I.E.Hoffman Department of Pediatrics UCSF Typical patient presentation KB was cyanotic at
Pulmonary arterio-venous fistulas Pulmonary arterio-venous fistulas No conflicts of interest to declare Julien I.E.Hoffman Department of Pediatrics UCSF Typical patient presentation KB was cyanotic at
PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT OF VASCULAR OCCLUSION EXTENT AND LOCALIZATION OF EMBOLI 1. BACKGROUND
 JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
Type II Endoleak Embolization Choice of Materials: EVOH, Glue, Thrombin & Coils. Michael S. Rosenberg, MD Assistant Professor of Radiology
 Type II Endoleak Embolization Choice of Materials: EVOH, Glue, Thrombin & Coils Michael S. Rosenberg, MD Assistant Professor of Radiology Michael Rosenberg, M. D. No relevant financial relationship reported
Type II Endoleak Embolization Choice of Materials: EVOH, Glue, Thrombin & Coils Michael S. Rosenberg, MD Assistant Professor of Radiology Michael Rosenberg, M. D. No relevant financial relationship reported
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute ischemic stroke TOAST classification of, 270 Acute myocardial infarction (AMI) cardioembolic stroke following, 207 208 noncardioembolic
Index Note: Page numbers of article titles are in boldface type. A Acute ischemic stroke TOAST classification of, 270 Acute myocardial infarction (AMI) cardioembolic stroke following, 207 208 noncardioembolic
Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome. Original Policy Date
 MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
MP 4.01.11 Ovarian and Internal Iliac Vein Embolization as a Treatment of Pelvic Congestion Syndrome Medical Policy Section OB/Gyn/Reproduction Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date
Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations
 J Neurosurg 78: 167-175, 1993 Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations NAYEF R. F. AL-RODHAN, M.D., PH.D., THORALF
J Neurosurg 78: 167-175, 1993 Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations NAYEF R. F. AL-RODHAN, M.D., PH.D., THORALF
EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS
 Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
Chronic Thromboembolic Pulmonary Hypertension (CTEPH): A Primer
 Chronic Thromboembolic Pulmonary Hypertension (CTEPH): A Primer H. Page McAdams, MD Duke University Medical Center Durham, NC 27710 page.mcadams@duke.edu Question Which of the following imaging tests is
Chronic Thromboembolic Pulmonary Hypertension (CTEPH): A Primer H. Page McAdams, MD Duke University Medical Center Durham, NC 27710 page.mcadams@duke.edu Question Which of the following imaging tests is
CHIEF COMPLAINT & HPI
 THE GREAT HOUDINI Resident: Marc Lim, MD Attending: Shekher Maddineni, MD Program/Department: Westchester Medical Center/New York Medical College/Department of Radiology CHIEF COMPLAINT & HPI Chief Complaint
THE GREAT HOUDINI Resident: Marc Lim, MD Attending: Shekher Maddineni, MD Program/Department: Westchester Medical Center/New York Medical College/Department of Radiology CHIEF COMPLAINT & HPI Chief Complaint
Renal Artery Embolization in Post Traumatic Vascular Lesions
 Med. J. Cairo Univ., VoL 81, No. 2, March: 69-73, 2013 www.medicaljournalofcairouniversity.com Renal Artery Embolization in Post Traumatic Vascular Lesions IHAB I. ALI, M.D.*; HESHAM BADAWY, M.D.**; AMR
Med. J. Cairo Univ., VoL 81, No. 2, March: 69-73, 2013 www.medicaljournalofcairouniversity.com Renal Artery Embolization in Post Traumatic Vascular Lesions IHAB I. ALI, M.D.*; HESHAM BADAWY, M.D.**; AMR
SDAVFs are rare acquired vascular lesions predominantly
 CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
CLINICAL REPORT W.J. van Rooij R.J. Nijenhuis J.P. Peluso M. Sluzewski G.N. Beute B. van der Pol Spinal Dural Fistulas without Swelling and Edema of the Cord as Incidental Findings SUMMARY: SDAVFs cause
Urinary tract embolization
 Beograd, 14.10.2012 Urinary tract embolization asist. Peter Popovič, MD, MSc Head of abdominal radiology department, Institute of Radiology, UMC Ljubljana Embolization Who and when procedure: local/general
Beograd, 14.10.2012 Urinary tract embolization asist. Peter Popovič, MD, MSc Head of abdominal radiology department, Institute of Radiology, UMC Ljubljana Embolization Who and when procedure: local/general
Coil Embolization for Coronary Artery Fistula with Giant
 Case Report Coil Embolization for Coronary Artery Fistula with Giant Acta Aneurysm Cardiol Sin 2012;28:259 263 Transcatheter Coil Embolization for Coronary Artery Fistula with Giant Aneurysm Originating
Case Report Coil Embolization for Coronary Artery Fistula with Giant Acta Aneurysm Cardiol Sin 2012;28:259 263 Transcatheter Coil Embolization for Coronary Artery Fistula with Giant Aneurysm Originating
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program
 Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Molla Teshome MD, Habtamu Belete MD Aurora Health Care Internal Medicine Residency Program History 32 year-old male who presented with a 4 days history of: Productive cough Right sided pleuritic chest
Angiographic and Clinical Characteristics of Patients with Cerebral Arteriovenous Malformations Associated with Hereditary Hemorrhagic Telangiectasia
 AJNR Am J Neuroradiol :6, June/July Angiographic and Clinical Characteristics of Patients with Cerebral Arteriovenous Malformations Associated with Hereditary Hemorrhagic Telangiectasia Shunji Matsubara,
AJNR Am J Neuroradiol :6, June/July Angiographic and Clinical Characteristics of Patients with Cerebral Arteriovenous Malformations Associated with Hereditary Hemorrhagic Telangiectasia Shunji Matsubara,
AN UNCOMMON CAUSE OF MASSIVE HEMATURIA
 Originally Posted: August, 01, 2014 AN UNCOMMON CAUSE OF MASSIVE HEMATURIA Resident(s): Monzer Chehab, MD, Alexander Copelan MD Attending(s): Purushottam Dixit, MD Program/Dept(s): Oakland University William
Originally Posted: August, 01, 2014 AN UNCOMMON CAUSE OF MASSIVE HEMATURIA Resident(s): Monzer Chehab, MD, Alexander Copelan MD Attending(s): Purushottam Dixit, MD Program/Dept(s): Oakland University William
Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases
 Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Vascular Malformations
 Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Devendra V. Kulkarni, Rahul G. Hegde, Ankit Balani, and Anagha R. Joshi. 2. Case Report. 1. Introduction
 Case Reports in Radiology, Article ID 614647, 4 pages http://dx.doi.org/10.1155/2014/614647 Case Report A Rare Case of Pulmonary Atresia with Ventricular Septal Defect with a Right Sided Aortic Arch and
Case Reports in Radiology, Article ID 614647, 4 pages http://dx.doi.org/10.1155/2014/614647 Case Report A Rare Case of Pulmonary Atresia with Ventricular Septal Defect with a Right Sided Aortic Arch and
Pictorial essay of unusual radiologic manifestations of pulmonary and airway metastasis at initial presentation of lung cancer
 Pictorial essay of unusual radiologic manifestations of pulmonary and airway metastasis at initial presentation of lung cancer Poster No.: C-2297 Congress: ECR 2012 Type: Educational Exhibit Authors: Y.
Pictorial essay of unusual radiologic manifestations of pulmonary and airway metastasis at initial presentation of lung cancer Poster No.: C-2297 Congress: ECR 2012 Type: Educational Exhibit Authors: Y.
The Pulmonary Embolism Severity Index in Predicting the Prognosis of Patients With Pulmonary Embolism
 ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.2.123 The Pulmonary Embolism Severity Index in Predicting the Prognosis of Patients With Pulmonary Embolism Won-Ho Choi 1, Sung Uk Kwon 1,2, Yoon Jung Jwa 1,
ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.2.123 The Pulmonary Embolism Severity Index in Predicting the Prognosis of Patients With Pulmonary Embolism Won-Ho Choi 1, Sung Uk Kwon 1,2, Yoon Jung Jwa 1,
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction. Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING
 Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
