Association between reperfusion and shrinkage percentage of aneurysmal sac after
|
|
|
- Patricia Copeland
- 5 years ago
- Views:
Transcription
1 Original article Association between reperfusion and shrinkage percentage of aneurysmal sac after embolization of pulmonary arteriovenous malformation: Evaluation based on contrast-enhanced thin-section CT images Satoko Makimoto 1, Takao Hiraki 1, Hideo Gobara 1, Hiroyasu Fujiwara 1, Toshihiro Iguchi 1, Yusuke Matsui 1, Hidefumi Mimura 2, Susumu Kanazawa 1 1 Department of Radiology, Okayama University Medical School, Okayama, Japan 2 Department of Diagnostic Radiology 2, Kawasaki Hospital, Kawasaki Medical School, Okayama, Japan Corresponding author: Satoko Makimoto Department of Radiology, Okayama University Medical School Kitaku Shikatacho, Okayama , Japan Phone: ; Fax: ; s_cogacoga@yahoo.co.jp The authors declare no conflicts of interest or funding sources to disclose.
2 Abstract Purpose: To investigate an association between reperfusion and percentage of shrinkage of the aneurysmal sac after embolization of pulmonary arteriovenous malformation (PAVM) and to determine the cut-off value of shrinkage percentage for indicating reperfusion. Materials and Methods: Twenty-two PAVMs with completely embolized feeding arteries with coils were examined. The percentage of sac shrinkage and the presence of reperfusion were evaluated on computed tomography (CT) before and 1, 3, and 12 months after embolization. The percentages of sac shrinkage were compared between occlusion group and reperfusion group. The receiver operating characteristic (ROC) curve was generated to determine the diagnostic efficiency of reperfusion of PAVM by using shrinkage percentages. Results: Reperfusion was seen in 14, 13, and 11 lesions at 1, 3, and 12 months, respectively. The mean percentage of sac shrinkage was significantly different between the 2 groups at 3 and 12 months. The area under ROC curve was at 3 months and at 12 months. All of 9 lesions with <60% sac shrinkage at 12 months showed reperfusion. Conclusion: The percentage of sac shrinkage was closely associated with reperfusion after embolization of PAVMs at 3 and 12 months. A shrinkage percentage of <60% at 12 months indicated reperfusion. Key words: pulmonary arteriovenous malformation, reperfusion, contrast-enhanced CT 2
3
4 Introduction Pulmonary arteriovenous malformation (PAVM) is an abnormal connection between the pulmonary arterial circulation and the pulmonary venous circulation with no intervening capillary bed. PAVM may cause life-threatening complications, including stroke, cerebral abscess, and hemoptysis [1 3]. Since the first report of successful transcatheter embolization of a PAVM in 1977 [4], it has been accepted as standard treatment. However, embolization occasionally results in incomplete occlusion of the shunt (i.e., reperfusion). Criteria for determining embolization success (i.e., absence of reperfusion) on radiological images have varied with different studies. One study determined success by visual assessment, which was indicated by complete or near-complete (linear scar only) resolution of the lesion on computed tomography (CT) or chest radiograph [5 8]; another indicated success by >30% reduction of lesion size [9]; and others indicated success by >70% reduction [5, 6]. Visual assessment is often subjective and depends on the modality (CT versus chest radiograph) and slice thickness of CT images. Measurement of size reduction is objective, but which cut-off level accurately indicates the absence of reperfusion has not been fully investigated. Thus, we sought to retrospectively investigate an association between reperfusion and the shrinkage percentage of the aneurysmal sac after embolization using dynamic contrast-enhanced thin-section CT images. Subsequently, the cut-off value of shrinkage percentage for indicating reperfusion was determined. Materials and methods Study Population Our Institutional Review Board (IRB) approved this retrospective study with a waiver 1
5 of obtaining informed consent. Between August 1999 and July 2011, we had treated 89 PAVMs in 42 patients with transcatheter coil embolization. Inclusion criteria were as follows: (a) the feeding artery of the lesion was completely embolized with coils; and (b) follow-up dynamic enhanced CT with thin-section reconstructions of the lesion of interest was performed at 1, 3, and 12 months. Exclusion criteria were as follows: (a) the sac or the draining vein of the lesion was embolized; (b) any of the follow-up CT examinations at 1, 3, and 12 months was unavailable; (c) follow-up CT was performed without contrast; and (d) thin-section reconstructed CT images were unavailable for the lesion of interest. Consequently, twenty-two lesions in 16 patients were included in this study. Characteristics of the study population are summarized in Table 1. Briefly, there were 5 men and 11 women; mean age was 52.6 ± 19.1 years. Seven patients were diagnosed with hereditary hemorrhagic telangiectasia. The mean diameter of the feeding arteries was 3.7 ± 1.1 mm. The type of PAVM was simple in 17 and complex in 5 lesions, according to the classification by White et al [10]. Embolization Technique Criteria for embolization of PAVMs in our institution were lesions with a feeding artery larger than 3 mm in diameter [11 13] and/or those that caused clinical signs and symptoms. The endpoint of the embolization was complete occlusion of all feeding arteries. Through a femoral vein sheath, pulmonary arteriography was performed to assess the lesion using a 4- or 5-F catheter. Then, the catheter or a microcatheter through the catheter was advanced into the feeding artery of the lesion until its tip was immediately in front of the sac. Immediately before embolization, 3000 IU of heparin was administered intravenously for prophylactic anticoagulation, followed by additional administration of 1000 IU per hour. Any other anti-platelet or anti-coagulant drugs were 2
6 not administrated before, during, or after the procedure. First, one or a few detachable bare microcoils were placed to prevent coil migration. Then, the feeding artery was embolized using pushable fibered microcoils alone or a combination of pushable fibered microcoils and inch coils. After embolization, pulmonary arteriography was performed to confirm complete occlusion of the feeding artery. Follow-up Examination Embolization outcomes were evaluated with non-contrast followed by dynamic contrast-enhanced CT scanning using a single-detector or a multi-detector row scanner (Aquilion multi, Aquilion16, and Aquilion64; Toshiba Medical Systems Corporation, Tokyo, Japan, Discovery CT750 HD; GE Healthcare, Milwaukee, WI, USA, SOMATOM Definition Flash; Siemens Medical Systems, Erlangen, Germany) 1, 3, and 12 months after embolization. The scanner settings were 120 kv with the tube current set at 300 ma or automatically set by the exposure control system, depending on type of CT scanner. The region scanned extended from the cervicothoracic junction to the upper part of the abdomen. Images were acquired during deep inspiration. After non-contrast CT scanning, a total of ml of contrast medium was administered intravenously at a rate of 3 5 ml/s and CT images were acquired 33 s and 90 s after initiation of contrast administration. From each dataset, in addition to contiguous 5-mm transverse CT images of the whole thorax, contiguous thin-section (2 3-mm thick) transverse CT images of the area of interest were reconstructed with both mediastinal and lung windows. Evaluation of Follow-up CT Reperfusion of the aneurysmal sac was evaluated on the thin-section transverse CT images with the mediastinal window. Reperfusion was deemed present when the 3
7 aneurysmal sac was enhanced. The sac was considered to show enhancement when the CT number of the sac on contrast images increased by more than 100 Hounsfield units, comparing with that on non-contrast images. The maximum short-axis diameter of the sac was measured on the thin-section transverse CT images with the lung window. Aneurysmal sac shrinkage was measured using a reduction percentage of the diameter of the sac, comparing with that before embolization. The lesions were divided into 2 groups according to the presence or absence of reperfusion at each follow-up time point (1, 3, and 12 months). Sac shrinkage percentage was compared between the 2 groups (reperfusion group versus occlusion group) with Student s t-test. Receiver operating characteristic (ROC) curves were generated to determine the diagnostic efficiency by using percentages of sac shrinkage to predict reperfusion. A P value < 0.05 was considered statistically significant. The statistical analyses were performed using commercially available software (SPSS software, IBM, Chicago IL, USA). Results Embolization The feeding artery was embolized with microcoils alone for 15 lesions and a combination of microcoils and inch coils for 7 lesions. The mean volume of coils deposited was 143 ± 125 mm 3 (Table 1). Pulmonary arteriography immediately after embolization showed complete occlusion of the feeding artery in all lesions. Nevertheless, aneurysmal sac of 8 lesions was slowly opacified during the venous phase. This opacification was suggested to result from venous inflow into the sac from adjacent lung perfused by normal pulmonary arterial branches [14]. No complication 4
8 occurred in any of the embolization procedures. Reperfusion and Sac Shrinkage Cases of occlusion and reperfusion are shown in Fig. 1 and 2, respectively. Reperfusion and shrinkage percentage of the aneurysmal sac at each follow-up point in all cases are summarized in Table 1. Reperfusion was seen in 14, 13, and 11 lesions at 1, 3, and 12 months, respectively. In all cases of reperfusion, the sac was enhanced on CT images in both of the two phases. Of the 14 lesions with reperfusion at 1 month, 3 lesions were spontaneously occluded at 3 months, while 2 of the 8 lesions with occlusion at 1 month showed reperfusion at 3 months. Of the 13 lesions with reperfusion at 3 months, 2 lesions were spontaneously occluded at 12 months. Mean (± SD) shrinkage percentage of the aneurysmal sac for all 22 lesions was 39.7 ± 16.5% (range, %), 52.8 ± 17.9% (range, %), and 56.1 ± 21.7% (range, %) at 1, 3, and 12 months, respectively. There were no lesions that showed partial or mural thrombosis in the venous sac on any follow-up CT images. Among the 8 lesions that showed retrograde opacification of aneurysmal sac on pulmonary arteriography immediately after embolization, 3 lesions were unenhanced on CT at 1 month. Of the other 5 lesions, 1 became unenhanced at 3 month and another did at 12 months. The ROC curve using sac shrinkage percentages and a dot plot of shrinkage percentages in the reperfusion group and the occlusion group at 1 month are shown in Fig. 3. At 1 month, the mean shrinkage of the aneurysmal sac was 45.6 ± 18.0% in the occlusion group (n = 8) and 36.3 ± 15.1% in the reperfusion group (n = 14); the difference was not significant (P = 0.21). The area under the ROC curve was (95% CI, ). 5
9 The ROC curve using sac shrinkage percentages and a dot plot of shrinkage percentages in the reperfusion group and the occlusion group at 3 months are shown in Fig. 4. At 3 months, the mean shrinkage was 41.4 ± 12.1% in the reperfusion group (n = 13) and 66.3 ± 10.4% in the occlusion group (n = 9); the difference was significant (P < 0.001). The area under the ROC curve was (95% CI, ). The sensitivity for reperfusion was 100% (13/13) and the specificity was 89% (8/9) when the cut-off value of the shrinkage was set at 60%; the sensitivity was 62% (8/13) and the specificity was 100% (9/9) when the cut-off value of shrinkage was set at 50% (Table 2). ROC curve using sac shrinkage percentages and a dot plot of shrinkage percentages in the reperfusion group and the occlusion group at 12 months are shown in Fig. 5. At 12 months, the mean shrinkage of the aneurysmal sac was 39.7 ± 16.3% in the reperfusion group (n = 11) and 72.5 ± 11.3% in the occlusion group (n = 11); the difference was significant (P < 0.001). The area under the ROC curve was (95% CI, ). Sensitivity was 100% (11/11) and specificity was 55% (6/11) when the cut-off value of the shrinkage was set at 70%; sensitivity was 82% (9/11) and specificity was 100% (11/11) when the cut-off value of the shrinkage was set at 60% (Table 3). Patient Outcome The mean follow-up period of the patients was 28 ± 12 months (range, months). All patients were alive and none developed symptoms (e.g., hemoptysis or dyspnea) or events (e.g., brain ischemia, abscess) related to the pulmonary AVMs. Discussion 6
10 The literature includes different modalities using various criteria for post-embolization PAVM evaluation. The modalities include arterial blood partial pressure [6, 15], oxygen shunt testing [8], contrast echocardiography [8], chest radiography [6, 8, 15], unenhanced CT [5-8, 15], enhanced CT [9, 16], and pulmonary angiography [5-8, 15, 16]. The criteria for embolization success include complete or near-complete resolution (only linear scar visible) of the lesion on chest radiograph or CT [5-8], >30% reduction of the sac size [9], >70% reduction of the sac size [5, 6], <3% shunt fraction by lung perfusion scintigraphy [15], stable arterial blood gas levels (variance within 10% of value after embolization) [6, 15], and no perfusion of the lesion on enhanced CT [9] or pulmonary angiogram [5-8, 15, 16]. We believe that chest radiography, arterial blood partial pressure, contrast echocardiography, and lung perfusion scintigraphy are not sensitive enough to document minor reperfusion. Although pulmonary angiography is the most reliable modality for evaluation of reperfusion, its invasiveness makes it difficult to perform routinely for follow-up of the lesions. Thus, we used enhanced CT scanning for evaluation. Because the ability to detect reperfusion may depend on reconstructed image thickness, especially for small lesions, this study included only the cases in which thin-slice reconstructed images were available. The proportions of reperfusion in our study were higher, compared with those in previous large series: 3% (11/393 lesions) by Pollak et al. [7], 7% (22/306 lesions) by Prasad et al. [8], and 8% (25/296 lesions) by Mager et al. [15]. In those studies, however, the presence of reperfusion was surveyed mainly by unenhanced CT or chest radiography [7], by oxygen shunt testing, contrast echocardiography, and unenhanced CT [8], or by chest radiography and/or arterial blood gas [16]. Only when reperfusion 7
11 was suspected by screening, pulmonary angiography was performed for confirmation. Sagara et al. [16] followed up patients with enhanced CT or pulmonary angiography. They showed 57% (8/14) reperfusion, which is similar to our result. We suggest that percentage of reperfusion depends highly on how intensively it was surveyed by using an examination with a contrast. The degree of shrinkage of the sac was not significantly different between the reperfusion group and the occlusion group at 1 month, which suggests that 1 month is too soon to make a significant difference in degree of sac shrinkage by the presence of reperfusion. ROC analyses showed a close relationship between reperfusion and sac shrinkage at 3 and 12 months. At 3 months, >60% shrinkage of the sac always indicated occlusion and <50% shrinkage always indicated reperfusion; at 12 months, >70% shrinkage percentage always indicated occlusion, while <60% shrinkage percentage always indicated reperfusion. These results are similar to the findings reported by Milic et al. [5]: all PAVMs with documented reperfusion at angiography exhibited residual sac and/or draining vein on CT and all PAVMs without documented reperfusion at angiography demonstrated at least 70% reduction of the sac size. Thus, we suggest that the cut-off value of sac shrinkage indicating occlusion at 12 months should be 70%. In contrast, the cut-off value of sac shrinkage indicating reperfusion should be 50% at 3 months and 60% at 12 months. Notably, 3 of the 14 reperfused lesions at 1 month were spontaneously occluded at 3 months, while 2 of the 8 occluded lesions at 1 month showed reperfusion at 3 months. These results indicate that the embolized PAVMs are hemodynamically unstable and thus efficacy of the embolization cannot be determined at 1 month. There are 4 mechanisms of reperfusion [5, 7]: (i) recanalization [6], (ii) accessory vessel 8
12 development [6, 17], (iii) bronchial arterial supply [16], and (iv) pulmonary-artery-to-pulmonary-artery collateral development [18]. Previous studies showed that the most common (33 100%) mechanism of reperfusion is recanalization of the embolized artery [5-8, 15-17, 19]. Treatment strategies for reperfusion are controversial. Some hold that any reperfusion should be treated because some patients with reperfused PAVMs developed neurologic events [5, 6]; others suggest that reperfusion with a feeding artery <3 mm is too small to be occluded [9]. We agreed with the latter suggestion and performed no repeat embolization for reperfusion, because the feeding arteries of all reperfused lesions were <3 mm in diameter. In our study, none of the patients with reperfused AVMs developed symptoms or signs related to reperfusion during follow-up. Our study has several limitations. This study was retrospective. The relatively strict inclusion criteria resulted in a small sample size. Reperfusion was not angiographically confirmed. Thus, the rate of reperfusion in our study might have been underestimated, and without angiography, the mechanism of reperfusion could not be determined. In 8 lesions showing retrograde opacification of aneurysmal sac on arteriography immediately after embolization, enhancement of the sac on CT at any follow-up time point might have resulted from residual retrograde opacification rather than reperfusion. The relatively short follow-up period (up to 1 year after embolization) is another limitation. However, we suggest that presence of reperfusion is unlikely to change after 1 year. Conclusions The percentage of shrinkage of the aneurysmal sac was closely associated with reperfusion at 3 and 12 months. Sac shrinkage of <50% at 3 months and of <60% at 12 9
13 months indicated reperfusion. 10
14 References 1.Gossage JR, Kanj G. Pulmonary arteriovenous malformations. A state of the art review. Am J Respir Crit Care Med. 1998;158: Swanson KL, Prakash UB, Stanson AW. Pulmonary arteriovenous fistulas: Mayo Clinic experience, Mayo Clin Proc. 1999;74: Shovlin CL, Letarte M. Hereditary haemorrhagic telangiectasia and pulmonary arteriovenous malformations: issues in clinical management and review of pathogenic mechanisms. Thorax. 1999;54: Porstmann W. Therapeutic embolization of arteriovenous pulmonary fistula by catheter technique. In: Kelop O, ed. Current concepts in pediatric radiology. Berlin: Springer, 1977; Milic A, Chan RP, Cohen JH, Faughnan ME. Reperfusion of pulmonary arteriovenous malformations after embolotherapy. J Vasc Interv Radiol. 2005;16: Lee DW, White RI Jr, Egglin TK, Pollak JS, Fayad PB, Wirth JA, et al. Embolotherapy of large pulmonary arteriovenous malformations: long-term results. Ann Thorac Surg. 1997;64: Pollak JS, Saluja S, Thabet A, Henderson KJ, Denbow N, White RI Jr. Clinical and anatomic outcomes after embolotherapy of pulmonary arteriovenous malformations. J Vasc Interv Radiol. 2006;17: Prasad V, Chan RP, Faughnan ME. Embolotherapy of pulmonary arteriovenous malformations: efficacy of platinum versus stainless steel coils. J Vasc Interv Radiol. 2004;15: Remy-Jardin M, Dumont P, Brillet PY, Dupuis P, Duhamel A, Remy J. Pulmonary 11
15 arteriovenous malformations treated with embolotherapy: helical CT evaluation of long-term effectiveness after 2-21-year follow-up. Radiology. 2006;239: White RI Jr, Pollak JS, Wirth JA. Pulmonary arteriovenous malformations: diagnosis and transcatheter embolotherapy. J Vasc Interv Radiol. 1996;7: Hewes RC, Auster M, White RI Jr. Cerebral embolism--first manifestation of pulmonary arteriovenous malformation in patients with hereditary hemorrhagic telangiectasia. Cardiovasc Intervent Radiol. 1985;8: White RI Jr, Lynch-Nyhan A, Terry P, Buescher PC, Farmlett EJ, Charnas L, et al. Pulmonary arteriovenous malformations: techniques and long-term outcome of embolotherapy. Radiology. 1988;169: Moussouttas M, Fayad P, Rosenblatt M, Hashimoto M, Pollak J, Henderson K, et al. Pulmonary arteriovenous malformations: cerebral ischemia and neurologic manifestations. Neurology. 2000;55: Pugash RA. Pulmonary arteriovenous malformations: overview and transcatheter embolotherapy. Can Assoc Radiol J. 2001;52: Mager JJ, Overtoom TT, Blauw H, Lammers JW, Westermann CJ. Embolotherapy of pulmonary arteriovenous malformations: long-term results in 112 patients. J Vasc Interv Radiol. 2004;15: Sagara K, Miyazono N, Inoue H, Ueno K, Nishida H, Nakajo M. Recanalization after coil embolotherapy of pulmonary arteriovenous malformations: study of long-term outcome and mechanism for recanalization. AJR Am J Roentgenol. 1998;170: Saluja S, Sitko I, Lee DW, Pollak J, White RI Jr. Embolotherapy of pulmonary arteriovenous malformations with detachable balloons: long-term durability and efficacy. J Vasc Interv Radiol. 1999;10:
16 18. Faughnan ME, Thabet A, Mei-Zahav M, Colombo M, Maclusky I, Hyland RH, et al. Pulmonary arteriovenous malformations in children: outcomes of transcatheter embolotherapy. J Pediatr. 2004;145: Andersen PE, Kjeldsen AD. Clinical and Radiological Long-Term Follow-up After Embolization of Pulmonary Arteriovenous Malformations. Cardiovasc Intervent Radiol. 2006;29:
17 Figure legends Fig. 1 A case of successfully occluded pulmonary arteriovenous malformation after embolization. a. CT image before embolization shows an aneurysmal sac (arrow) with maximum short-axis diameter of 24.7 mm. b. CT image 1 month after embolization shows an aneurysmal sac (arrow) with maximum short-axis diameter of 18.2 mm (26.3% shrinkage) without perfusion. Enhancement demonstrated at the periphery of the sac indicates an adjacent pulmonary vessel (arrowhead). c. CT image 3 months after embolization shows an aneurysmal sac (arrow) with maximum short-axis diameter of 7.3 mm (70.4% shrinkage) without perfusion. Arrowhead indicates the deposited coils. d. CT image 12 months after embolization shows an aneurysmal sac (arrow) with maximum short-axis diameter of 6.7 mm (72.9% shrinkage) without perfusion. Arrowhead indicates the deposited coils. Fig. 2 A case of reperfused pulmonary arteriovenous malformation after embolization. a. CT image before embolization shows an aneurysmal sac (arrow) with maximum short-axis diameter of 9.5 mm. b. CT image 1 month after embolization shows a perfused aneurysmal sac (arrow) with maximum short-axis diameter of 4.7 mm (50.5% shrinkage). c. CT image 3 months after embolization shows a perfused aneurysmal sac (arrow) with maximum short-axis diameter of 4.7 mm (50.5% shrinkage). d. CT image 12 months after embolization shows a perfused aneurysmal sac (arrow) 14
18 with maximum short-axis diameter of 5.1 mm (46.4% shrinkage). Fig. 3 Receiver-operating characteristic (ROC) curves using sac shrinkage percentages (a) and a dot plot (b) at 1 month. a. The area under the ROC curve was (95% CI, ) at 1 month. b. Mean shrinkage of the aneurysmal sac was 36.3 ± 15.1% in the reperfusion group (n = 14) whereas it was 45.6 ± 18.0% in the occlusion group (n = 8); the difference was not significant (P = 0.21). Fig. 4 Receiver-operating characteristic (ROC) curves using sac shrinkage percentages (a) and a dot plot (b) at 3 months. a. The area under the ROC curve was (95% CI, ) at 3 months. b. Mean shrinkage was 41.4 ± 12.1% in the reperfusion group (n = 13) whereas it was 66.3 ± 10.4% in the occlusion group (n = 9); the difference was significant (P < 0.001). Fig. 5 Receiver-operating characteristic (ROC) curves using sac shrinkage percentages (a) and a dot plot (b) at 12 months. a. The area under the ROC curve was (95% CI, ) at 12 months. b. Mean shrinkage of the aneurysmal sac was 39.7 ± 16.3% in the reperfusion group (n = 11) whereas it was 72.5 ± 11.3% in the occlusion group (n = 11); the difference was significant (P < 0.001). 15
19 Table 1. Summary of 22 lesions in 16 patients Follow up results 1 mo 3 mo 12 mo Lesion no. Patient no. Sex Age (yrs) Diameter of Volume of coils Retrograde Dimameter of Presence of Lesion Sac shrinkage Sac shrinakge Sac shrinkage feeding artery deposited opacification Reperfusion Reperfusion Reperfusion feeding artery HHT Type (mm)* (mm 3 (%) (%) (%) )** via draining (mm) 1 1 F 58 yes simple yes no 32.5 yes 54.5 no F 58 yes complex no yes 44.7 yes 41.3 yes F 59 no simple yes yes 38.9 no 63.9 no F 33 yes simple no no 32.3 no 54.6 no F 64 no simple no yes 50.5 yes 50.5 yes F 60 no complex no no 38.0 no 62.0 no M 16 yes simple yes no 47.5 yes 44.3 yes M 16 yes complex yes no 26.3 no 70.4 no M 14 yes simple yes yes 42.0 yes 43.2 yes M 14 yes simple no yes 36.7 yes 36.7 yes M 14 yes simple no yes 22.4 yes 24.5 yes M 14 yes simple no yes 48.4 yes 52.4 yes M 14 yes simple no yes 35.1 yes 25.6 yes F 74 no simple yes yes 64.5 no 73.8 no M 60 no complex no no 63.2 no 77.8 no F 82 no simple no yes 36.7 yes 50.3 yes F 51 no simple no yes 13.2 no 63.2 no F 71 no simple yes yes 45.2 yes 59.6 yes M 50 yes complex no no 80.1 no 90.0 no F 62 no simple no yes 11.4 yes 24.3 yes M 40 no simple yes yes 19.0 yes 31.0 no F 48 no simple no no 45.1 no 67.6 no HHT hereditary hemorrhagic telangiectasia, M male, F female *The largest diameter of the feeding arteries is shown in case of complex lesions. ** Volume of coils deposited is calculated using diameter and length of the coils.
20 Table 2. Number of lesions with reperfusion according to sac shrinkage at 3 months Sac shrinkage (%) Reperfusion <50% 50 60% >60% Yes No 0 1 8
21 Table 3. Number of lesions with reperfusion according to sac shrinkage at 12 months Sac shrinkage (%) Reperfusion <60% 60 70% >70% Yes No 0 5 6
22 Fig1a Fig1b
23 Fig1c Fig1d
24 Fig2a Fig2b
25 Fig2c Fig2d
26 Fig3a Fig3b
27 Fig4a Fig4b
28 Fig5a Fig5b
Where is the Origin of the Last Normal Branch from Feeding Artery of Pulmonary Arteriovenous Malformations?
 Cardiovasc Intervent Radiol (2018) 41:1849 1856 https://doi.org/10.1007/s00270-018-2063-4 CLINICAL INVESTIGATION ARTERIAL INTERVENTIONS Where is the Origin of the Last Normal Branch from Feeding Artery
Cardiovasc Intervent Radiol (2018) 41:1849 1856 https://doi.org/10.1007/s00270-018-2063-4 CLINICAL INVESTIGATION ARTERIAL INTERVENTIONS Where is the Origin of the Last Normal Branch from Feeding Artery
Embolotherapy for Pulmonary Arteriovenous Malformations in Patients without Hereditary Hemorrhagic Telangiectasia
 Embolotherapy for Pulmonary Arteriovenous Malformations in Patients without Hereditary Hemorrhagic Telangiectasia Ji Hoon Shin, MD Soo Jin Park, MD Gi-Young Ko, MD Hyun-Ki Yoon, MD Dong-Il Gwon, MD Jin-Hyoung
Embolotherapy for Pulmonary Arteriovenous Malformations in Patients without Hereditary Hemorrhagic Telangiectasia Ji Hoon Shin, MD Soo Jin Park, MD Gi-Young Ko, MD Hyun-Ki Yoon, MD Dong-Il Gwon, MD Jin-Hyoung
Pulmonary arteriovenous malformations (PAVMs)
 Endovascular Repair of PAVM by Embolotherapy In a patient with a transient ischemic attack or stroke, a positive contrast echocardiogram does not always mean a patent foramen ovale. BY ROBERT I. WHITE,
Endovascular Repair of PAVM by Embolotherapy In a patient with a transient ischemic attack or stroke, a positive contrast echocardiogram does not always mean a patent foramen ovale. BY ROBERT I. WHITE,
(received 8 March 2013, accepted 15 April 2013)
 Akita J Med 40 : 13-21, 2013 (13) Kazuhiro Sato 1), Takanobu Shioya 2), Mariko Asano 1), Yuji Okuda 1), Hajime Miura 1), Masaaki Sano 1), Kenji Iino 1), Toshimitsu Kosaka 1), Hiroyuki Watanabe 1), Manabu
Akita J Med 40 : 13-21, 2013 (13) Kazuhiro Sato 1), Takanobu Shioya 2), Mariko Asano 1), Yuji Okuda 1), Hajime Miura 1), Masaaki Sano 1), Kenji Iino 1), Toshimitsu Kosaka 1), Hiroyuki Watanabe 1), Manabu
New Definition and Natural History of Patients With Diffuse Pulmonary Arteriovenous Malformations*
 Original Research PULMONARY VASCULAR DISEASE New Definition and Natural History of Patients With Diffuse Pulmonary Arteriovenous Malformations* Twenty-Seven Year Experience Paola Pierucci, MD; Joshua Murphy,
Original Research PULMONARY VASCULAR DISEASE New Definition and Natural History of Patients With Diffuse Pulmonary Arteriovenous Malformations* Twenty-Seven Year Experience Paola Pierucci, MD; Joshua Murphy,
Endovascular Management of Pulmonary Arteriovenous Malformation
 Bahrain Medical Bulletin, Vol. 36, No. 3, September 2014 ABSTRACT Endovascular Management of Pulmonary Arteriovenous Malformation Omar Mohammed Omar, MSc* Wael Hamed Ibrahim, MD, PhD** Noora Abdulaziz
Bahrain Medical Bulletin, Vol. 36, No. 3, September 2014 ABSTRACT Endovascular Management of Pulmonary Arteriovenous Malformation Omar Mohammed Omar, MSc* Wael Hamed Ibrahim, MD, PhD** Noora Abdulaziz
Treating Pulmonary Arteriovenous Malformations: What to Do and What Not to Do
 Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 2016 Treating Pulmonary Arteriovenous Malformations: What to Do and What Not to Do Ripal Gandhi Baptist Hospital
Baptist Health South Florida Scholarly Commons @ Baptist Health South Florida All Publications 2016 Treating Pulmonary Arteriovenous Malformations: What to Do and What Not to Do Ripal Gandhi Baptist Hospital
Preliminary experience with the micro vascular plug for the treatment of pulmonary arteriovenous malformation: case series of four patients
 Duvnjak et al. CVIR Endovascular (2018) 1:19 https://doi.org/10.1186/s42155-018-0027-z CVIR Endovascular CASE REPORT Preliminary experience with the micro vascular plug for the treatment of pulmonary arteriovenous
Duvnjak et al. CVIR Endovascular (2018) 1:19 https://doi.org/10.1186/s42155-018-0027-z CVIR Endovascular CASE REPORT Preliminary experience with the micro vascular plug for the treatment of pulmonary arteriovenous
Stephen Binsse, Jacques Sellier, Jérome Lucas, Mostafa El Hajjam, Pascal Lacombe
 SPONTANEOUS RUPTURE OF PULMONARY ARTERIOVENOUS MALFORMATIONS IN HEREDITARY HAEMORRHAGIC TELANGIECTASIA (HHT) REVIEW OF 12 CASES Stephen Binsse, Jacques Sellier, Jérome Lucas, Mostafa El Hajjam, Pascal
SPONTANEOUS RUPTURE OF PULMONARY ARTERIOVENOUS MALFORMATIONS IN HEREDITARY HAEMORRHAGIC TELANGIECTASIA (HHT) REVIEW OF 12 CASES Stephen Binsse, Jacques Sellier, Jérome Lucas, Mostafa El Hajjam, Pascal
Pulmonary Arteriovenous Malformations And Osler Weber Rendu Syndrome: An Unusual Cause Of Dyspnea
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 5 Number 2 Pulmonary Arteriovenous Malformations And Osler Weber Rendu Syndrome: An Unusual Cause Of H Amin, A Friere, C Lal, M Pugazhenthi Citation
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 5 Number 2 Pulmonary Arteriovenous Malformations And Osler Weber Rendu Syndrome: An Unusual Cause Of H Amin, A Friere, C Lal, M Pugazhenthi Citation
Pulmonary arteriovenous malformations: endovascular therapy
 Review rticle Pulmonary arteriovenous malformations: endovascular therapy Murthy R. Chamarthy, Harold Park, Patrick Sutphin, Girish Kumar, Daniel Lamus, Sachin Saboo, Matthew nderson, Sanjeeva P. Kalva
Review rticle Pulmonary arteriovenous malformations: endovascular therapy Murthy R. Chamarthy, Harold Park, Patrick Sutphin, Girish Kumar, Daniel Lamus, Sachin Saboo, Matthew nderson, Sanjeeva P. Kalva
Pulmonary arteriovenous malformations (PAVMs)
 Pulmonary Arteriovenous Malformations and Coronary Artery Fistulas Diagnosis, evaluation, and indications for closure. BY MARK D. OSTEN, MD, AND ERIC M. HORLICK, MDCM Pulmonary arteriovenous malformations
Pulmonary Arteriovenous Malformations and Coronary Artery Fistulas Diagnosis, evaluation, and indications for closure. BY MARK D. OSTEN, MD, AND ERIC M. HORLICK, MDCM Pulmonary arteriovenous malformations
Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550032 Volume 2, Issue 4 Case Report Pulmonary Arteriovenous Malformations Complicated with Paradoxical Embolic Stroke Cheah Wai Hun
Neurologic Manifestation as Initial Presentation in a Case of Hereditary Haemorrhagic Telangiectasia
 Clinical Medicine Insights: Case Reports Case report Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Neurologic Manifestation as Initial Presentation in a
Clinical Medicine Insights: Case Reports Case report Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Neurologic Manifestation as Initial Presentation in a
Pulmonary Arteriovenous Malformations: Current Technique of Transcatheter Embolization and Subsequent Management
 Educational Paper from SIRAP Pulmonary Arteriovenous Malformations: Current Technique of Transcatheter Embolization and Subsequent Management 1) Department of Radiology, Nagoya City University Graduate
Educational Paper from SIRAP Pulmonary Arteriovenous Malformations: Current Technique of Transcatheter Embolization and Subsequent Management 1) Department of Radiology, Nagoya City University Graduate
Endovascular treatment of pulmonary arteriovenous malformations in hereditary haemorrhagic telangiectasia
 Published 28 July 2015, doi:10.4414/smw.2015.14151 Cite this as: Endovascular treatment of pulmonary arteriovenous malformations in hereditary haemorrhagic telangiectasia Malik Babaker a, Stepane Breault
Published 28 July 2015, doi:10.4414/smw.2015.14151 Cite this as: Endovascular treatment of pulmonary arteriovenous malformations in hereditary haemorrhagic telangiectasia Malik Babaker a, Stepane Breault
Radiation Exposure in Pregnancy. John R. Mayo UNIVERSITY OF BRITISH COLUMBIA
 Radiation Exposure in Pregnancy John R. Mayo UNIVERSITY OF BRITISH COLUMBIA Illustrative Clinical Scenario 32 year old female 34 weeks pregnant with recent onset shortness of breath and central chest pain
Radiation Exposure in Pregnancy John R. Mayo UNIVERSITY OF BRITISH COLUMBIA Illustrative Clinical Scenario 32 year old female 34 weeks pregnant with recent onset shortness of breath and central chest pain
.. CHEST Original Research
 .. CHEST Original Research Diffuse Pulmonary Arteriovenous Malformations in Hereditary Hemorrhagic Telangiectasia* PULMONARY ARTERIOVENOUS MALFORMATIONS Long-term Results of Embolization According to the
.. CHEST Original Research Diffuse Pulmonary Arteriovenous Malformations in Hereditary Hemorrhagic Telangiectasia* PULMONARY ARTERIOVENOUS MALFORMATIONS Long-term Results of Embolization According to the
Reproducibility Of Exercise Testing In Patients With Pulmonary Arteriovenous Malformations
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2012 Reproducibility Of Exercise Testing In Patients With
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine January 2012 Reproducibility Of Exercise Testing In Patients With
EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS
 Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
Arteriovenous fistula after radiosurgery for multiple CAVM EMBOLIZATION OF ARTERIOVENOUS FISTULA AFTER RADIOSURGERY FOR MULTIPLE CEREBRAL ARTERIOVENOUS MALFORMATIONS Chao-Bao Luo, Wan-Yuo Guo, Michael
International Journal of Diagnostic Imaging, 2014, Vol. 1, No. 2
 CASE REPORT Transthoracic contrast echocardiography for detection of pulmonary arteriovenous malformations in hereditary hemorrhagic telangiectasia: How can the process be improved for patient safety?
CASE REPORT Transthoracic contrast echocardiography for detection of pulmonary arteriovenous malformations in hereditary hemorrhagic telangiectasia: How can the process be improved for patient safety?
PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT OF VASCULAR OCCLUSION EXTENT AND LOCALIZATION OF EMBOLI 1. BACKGROUND
 JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
Pulmonary arteriovenous fistula
 International Journal of Medical Imaging 2014; 2(2): 34-38 Published online April 10, 2014 (http://www.sciencepublishinggroup.com/j/ijmi) doi: 10.11648/j.ijmi.20140202.16 Pulmonary arteriovenous fistula
International Journal of Medical Imaging 2014; 2(2): 34-38 Published online April 10, 2014 (http://www.sciencepublishinggroup.com/j/ijmi) doi: 10.11648/j.ijmi.20140202.16 Pulmonary arteriovenous fistula
Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the Uterus with Fibroids
 Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the
Acta Radiologica ISSN: 0284-1851 (Print) 1600-0455 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Embolization of Spontaneous Rupture of an Aneurysm of the Ovarian Artery Supplying the
Endovascular Treatment of Pulmonary and Cerebral Arteriovenous
 Endovascular Treatment of Pulmonary and Cerebral Arteriovenous Current Pharmaceutical Design, 2005, 11, 000-000 1 1381-6128/05 $50.00+.00 Â 2005 Bentham Science Publishers Ltd. Teleangiectasia E. De Cillis1,
Endovascular Treatment of Pulmonary and Cerebral Arteriovenous Current Pharmaceutical Design, 2005, 11, 000-000 1 1381-6128/05 $50.00+.00 Â 2005 Bentham Science Publishers Ltd. Teleangiectasia E. De Cillis1,
Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases
 Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
L angiografia ha ancora un ruolo?
 Aggiornamenti di Radiologia Interventistica L angiografia ha ancora un ruolo? Roberto Iezzi Dipartimento di Bioimmagini e Scienze Radiologiche Istituto di Radiologia, Policlinico A. Gemelli Università
Aggiornamenti di Radiologia Interventistica L angiografia ha ancora un ruolo? Roberto Iezzi Dipartimento di Bioimmagini e Scienze Radiologiche Istituto di Radiologia, Policlinico A. Gemelli Università
Role of the Radiologist
 Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Renal Artery Embolization in Post Traumatic Vascular Lesions
 Med. J. Cairo Univ., VoL 81, No. 2, March: 69-73, 2013 www.medicaljournalofcairouniversity.com Renal Artery Embolization in Post Traumatic Vascular Lesions IHAB I. ALI, M.D.*; HESHAM BADAWY, M.D.**; AMR
Med. J. Cairo Univ., VoL 81, No. 2, March: 69-73, 2013 www.medicaljournalofcairouniversity.com Renal Artery Embolization in Post Traumatic Vascular Lesions IHAB I. ALI, M.D.*; HESHAM BADAWY, M.D.**; AMR
Epidermiology Early pulmonary embolism
 Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Epidermiology Early pulmonary embolism Sitang Nirattisaikul Faculty of Medicine, Prince of Songkla University 3 rd most common cause of cardiovascular death in the United States, following ischemic heart
Type II Endoleak Embolization Choice of Materials: EVOH, Glue, Thrombin & Coils. Michael S. Rosenberg, MD Assistant Professor of Radiology
 Type II Endoleak Embolization Choice of Materials: EVOH, Glue, Thrombin & Coils Michael S. Rosenberg, MD Assistant Professor of Radiology Michael Rosenberg, M. D. No relevant financial relationship reported
Type II Endoleak Embolization Choice of Materials: EVOH, Glue, Thrombin & Coils Michael S. Rosenberg, MD Assistant Professor of Radiology Michael Rosenberg, M. D. No relevant financial relationship reported
Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia
 Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia Vincent Cottin, Henri Plauchu, Jean-Yves Bayle, Martine Barthelet, Didier Revel, and Jean-François Cordier Service
Pulmonary Arteriovenous Malformations in Patients with Hereditary Hemorrhagic Telangiectasia Vincent Cottin, Henri Plauchu, Jean-Yves Bayle, Martine Barthelet, Didier Revel, and Jean-François Cordier Service
Detectability of subsegmental pulmonary vessels in 64 MDCT-pulmonary angiography.
 ISPUB.COM The Internet Journal of Radiology Volume 11 Number 2 Detectability of subsegmental pulmonary vessels in 64 MDCT-pulmonary angiography. T Niemann, G Bongartz Citation T Niemann, G Bongartz. Detectability
ISPUB.COM The Internet Journal of Radiology Volume 11 Number 2 Detectability of subsegmental pulmonary vessels in 64 MDCT-pulmonary angiography. T Niemann, G Bongartz Citation T Niemann, G Bongartz. Detectability
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Lung Perfusion Analysis New Pathways in Lung Imaging. Case Study Brochure PLA 309 Hospital
 Lung Perfusion Analysis New Pathways in Lung Imaging Case Study Brochure PLA 309 Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2012 all rights reserved. Design and specifications
Lung Perfusion Analysis New Pathways in Lung Imaging Case Study Brochure PLA 309 Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2012 all rights reserved. Design and specifications
Individual Pulmonary Vein Atresia in Adults: Report of Two Cases
 Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Case Report DOI: 10.3348/kjr.2011.12.3.395 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(3):395-399 Individual Pulmonary Vein Atresia in Adults: Report of Two Cases Hyoung Nam Lee, MD, Young
Chronic Thromboembolic Pulmonary Hypertension (CTEPH): A Primer
 Chronic Thromboembolic Pulmonary Hypertension (CTEPH): A Primer H. Page McAdams, MD Duke University Medical Center Durham, NC 27710 page.mcadams@duke.edu Question Which of the following imaging tests is
Chronic Thromboembolic Pulmonary Hypertension (CTEPH): A Primer H. Page McAdams, MD Duke University Medical Center Durham, NC 27710 page.mcadams@duke.edu Question Which of the following imaging tests is
Hereditary hemorrhagic telangiectasia (HHT): Whole body imaging findings with emphasis in central nervous system involvement
 Hereditary hemorrhagic telangiectasia (HHT): Whole body imaging findings with emphasis in central nervous system involvement Poster No.: C-824 Congress: ECR 2009 Type: Topic: Authors: Keywords: DOI: Educational
Hereditary hemorrhagic telangiectasia (HHT): Whole body imaging findings with emphasis in central nervous system involvement Poster No.: C-824 Congress: ECR 2009 Type: Topic: Authors: Keywords: DOI: Educational
Graded contrast echocardiography in pulmonary arteriovenous malformations
 Eur Respir J 2010; 35: 1279 1285 DOI: 10.1183/09031936.00104309 CopyrightßERS 2010 Graded contrast echocardiography in pulmonary arteriovenous malformations J.A. Parra*, J. Bueno #, J. Zarauza ", C. Fariñas-Alvarez
Eur Respir J 2010; 35: 1279 1285 DOI: 10.1183/09031936.00104309 CopyrightßERS 2010 Graded contrast echocardiography in pulmonary arteriovenous malformations J.A. Parra*, J. Bueno #, J. Zarauza ", C. Fariñas-Alvarez
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Management of Endoleaks. Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09
 Management of Endoleaks Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09 Endoleak Failure to totally exclude the abdominal aortic aneurysm (AAA) from continued perfusion and pressurization
Management of Endoleaks Michael Meuse, M.D Vascular and Interventional Radiology 12/14/09 Endoleak Failure to totally exclude the abdominal aortic aneurysm (AAA) from continued perfusion and pressurization
As data on coil embolization
 A Complete Embolization System The Ruby coil and POD devices. As data on coil embolization become more A robust, so must the tools and technology we use. Penumbra, Inc. has advanced this technology with
A Complete Embolization System The Ruby coil and POD devices. As data on coil embolization become more A robust, so must the tools and technology we use. Penumbra, Inc. has advanced this technology with
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Coils and plugs have emerged as the most commonly
 The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
A Rare Case of Cerebral Air Embolism Caused by Pulmonary Arteriovenous Malformation After Removal of a Central Venous Catheter
 Case Report This is Advance Publication Article Kurume Medical Journal, 65, 00-00, 2018 A Rare Case of Cerebral Air Embolism Caused by Pulmonary Arteriovenous Malformation After Removal of a Central Venous
Case Report This is Advance Publication Article Kurume Medical Journal, 65, 00-00, 2018 A Rare Case of Cerebral Air Embolism Caused by Pulmonary Arteriovenous Malformation After Removal of a Central Venous
Supraselective bronchial artery embolization in patients with massive hemoptysis.
 Supraselective bronchial artery embolization in patients with massive hemoptysis. Poster No.: C-2259 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit A. Svare, S. Rud#icka, E. Kadakovska,
Supraselective bronchial artery embolization in patients with massive hemoptysis. Poster No.: C-2259 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit A. Svare, S. Rud#icka, E. Kadakovska,
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction. Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING
 Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Pulmonary Embolism. Thoracic radiologist Helena Lauri
 Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Pulmonary Embolism Thoracic radiologist Helena Lauri 8.5.2017 Statistics 1-2 out of 1000 adults annually are diagnosed with deep vein thrombosis (DVT) and/or pulmonary embolism (PE) About half of patients
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Cover Page The handle http://hdl.handle.net/1887/19768 holds various files of this Leiden University dissertation. Author: Langevelde, Kirsten van Title: Are pulmonary embolism and deep-vein thrombosis
Terumo Scholarship Case Study Dr B Maher, University Hospital Southampton NHS Foundation Trust
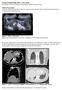 Terumo Scholarship 2015 - Case Study Dr B Maher, University Hospital Southampton NHS Foundation Trust Clinical Presentation A 41year old female presented with pelvic pain and menorrhagia. Pelvic ultrasound
Terumo Scholarship 2015 - Case Study Dr B Maher, University Hospital Southampton NHS Foundation Trust Clinical Presentation A 41year old female presented with pelvic pain and menorrhagia. Pelvic ultrasound
Delayed Intracranial Air Embolism After Interventional Therapy of Congenital Pulmonary Arteriovenous Fistula
 Delayed Intracranial Air Embolism After Interventional Therapy of Congenital Pulmonary Arteriovenous Fistula WA N G W E I D E PA R T M E N T O F C A R D I O LO GY C H I L DREN S H O S P I TA L, Z H E J
Delayed Intracranial Air Embolism After Interventional Therapy of Congenital Pulmonary Arteriovenous Fistula WA N G W E I D E PA R T M E N T O F C A R D I O LO GY C H I L DREN S H O S P I TA L, Z H E J
A 33-year-old male with a chest lesion on a routine chest radiograph
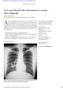 WHAT S YOUR DIAGNOSIS? A 33-year-old male with a chest lesion on a routine chest radiograph Editor: Husn Frayha Authors: Mohammed Khalid,*Neelam Malik, Suzanne Abbas, A 33-year-old Bahraini male presented
WHAT S YOUR DIAGNOSIS? A 33-year-old male with a chest lesion on a routine chest radiograph Editor: Husn Frayha Authors: Mohammed Khalid,*Neelam Malik, Suzanne Abbas, A 33-year-old Bahraini male presented
HEMOPTYSIS. Prof. G. Zuliani
 HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
HEMOPTYSIS Prof. G. Zuliani HEMOPTYSIS Hemoptysis is the expectoration of blood, that can range from blood-streaking of sputum (Hemoptoe) to the presence of gross blood in the absence of any accompanying
Vascular Malformations
 Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Percutaneous Transarterial Embolization of Pseudoaneurysm Secondary to Pancreatitis: a case report
 Chin J Radiol 2003; 28: 347-351 347 Percutaneous Transarterial Embolization of Pseudoaneurysm Secondary to Pancreatitis: a case report HSIN-YI LAI YUNG-FANG CHEN HSEIN-JAR CHIANG WU-CHUNG SHEN Department
Chin J Radiol 2003; 28: 347-351 347 Percutaneous Transarterial Embolization of Pseudoaneurysm Secondary to Pancreatitis: a case report HSIN-YI LAI YUNG-FANG CHEN HSEIN-JAR CHIANG WU-CHUNG SHEN Department
Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving the Laterocavernous Sinus
 Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Quality Metrics. Stroke Related Procedure Outcomes
 Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
Quality Metrics Stroke Related Procedure Outcomes Below is a description of some of the stroke-related procedures performed at St. Dominic Hospital in Jackson, with quality information on the complication
7/5/2016. Neonatal high-output cardiac failure. Case 1 POSTNATAL STRATEGIES FOR CEREBRAL ATERIOVENOUS MALFORMATIONS
 John Deveikis, M.D. POSTNATAL STRATEGIES FOR CEREBRAL ATERIOVENOUS MALFORMATIONS JULY, 2016 Neonatal high-output cardiac failure Tachypnea, tachycardia, hypotension, failure to thrive When congenital heart
John Deveikis, M.D. POSTNATAL STRATEGIES FOR CEREBRAL ATERIOVENOUS MALFORMATIONS JULY, 2016 Neonatal high-output cardiac failure Tachypnea, tachycardia, hypotension, failure to thrive When congenital heart
University Journal of Medicine and Medical Specialities
 ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
ISSN 2455-2852 2018, Vol. 4(5) Imaging Assessment of Vascular Thoracic Outlet Syndrome BALAJI A AYYAMPERUMAL Department of Radio Diagnosis,MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL Abstract
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils
 High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
High-Flow, Small-Hole Arteriovenous Fistulas: Treatment with Electrodetachable Coils Guido Guglielmi, Fernando Viñuela, Gary Duckwiler, Jacques Dion, and Alfredo Stocker Summary: We present one case of
Post-catheterization pseudoaneurysms treatment with ultrasound-guided thrombin injection
 Post-catheterization pseudoaneurysms treatment with ultrasound-guided thrombin injection Poster No.: C-2107 Congress: ECR 2010 Type: Topic: Scientific Exhibit Interventional Radiology Authors: A. Ladas,
Post-catheterization pseudoaneurysms treatment with ultrasound-guided thrombin injection Poster No.: C-2107 Congress: ECR 2010 Type: Topic: Scientific Exhibit Interventional Radiology Authors: A. Ladas,
Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations
 J Neurosurg 78: 167-175, 1993 Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations NAYEF R. F. AL-RODHAN, M.D., PH.D., THORALF
J Neurosurg 78: 167-175, 1993 Occlusive hyperemia: a theory for the hemodynamic complications following resection of intracerebral arteriovenous malformations NAYEF R. F. AL-RODHAN, M.D., PH.D., THORALF
Endoleak Sealing after AAA Endovascular Repair. When and How?
 Endoleak Sealing after AAA Endovascular Repair. When and How? Poster No.: C-1086 Congress: ECR 2013 Type: Educational Exhibit Authors: D. Quintana Blanco, B. González Humara, E. Torres Diez, C. Jimenez
Endoleak Sealing after AAA Endovascular Repair. When and How? Poster No.: C-1086 Congress: ECR 2013 Type: Educational Exhibit Authors: D. Quintana Blanco, B. González Humara, E. Torres Diez, C. Jimenez
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Risk of Pulmonary Embolism After Negative MDCT Pulmonary Angiography Findings
 E. C. Kavanagh 1 A. O Hare G. Hargaden J. G. Murray Received March 20, 2003; accepted after revision August 25, 2003. 1 All authors: Department of Radiology, Mater Misericordiae Hospital, Eccles St., Dublin
E. C. Kavanagh 1 A. O Hare G. Hargaden J. G. Murray Received March 20, 2003; accepted after revision August 25, 2003. 1 All authors: Department of Radiology, Mater Misericordiae Hospital, Eccles St., Dublin
Pulmonary arteriovenous malformations presenting as difficult-to-control asthma: a case report
 Navratil et al. Journal of Medical Case Reports 2013, 7:32 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Pulmonary arteriovenous malformations presenting as difficult-to-control asthma: a case
Navratil et al. Journal of Medical Case Reports 2013, 7:32 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Pulmonary arteriovenous malformations presenting as difficult-to-control asthma: a case
Endovascular Treatment of Type II Endoleak Following TEVAR for Thoracic Aortic Aneurysm: Squeeze Technique to Reach the Aneurysmal Sac
 Endovascular Treatment of Type II Endoleak Following TEVAR for Thoracic Aortic Aneurysm: Squeeze Technique to Reach the Aneurysmal Sac Chang Won Kim Department of Radiology Pusan National University Hospital
Endovascular Treatment of Type II Endoleak Following TEVAR for Thoracic Aortic Aneurysm: Squeeze Technique to Reach the Aneurysmal Sac Chang Won Kim Department of Radiology Pusan National University Hospital
System.
 System www.penumbrainc.com POD System Case Examples 45 cm of POD Packing Coil in 1.5 to 3 mm diameter dilating vessel Bronchial Artery Embolization Dr. Amit Kakkar and Dr. Aksim Rivera, Bronx, NY Inflow:
System www.penumbrainc.com POD System Case Examples 45 cm of POD Packing Coil in 1.5 to 3 mm diameter dilating vessel Bronchial Artery Embolization Dr. Amit Kakkar and Dr. Aksim Rivera, Bronx, NY Inflow:
Contaminated Wound: Report of a Cas
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
Time-resolved Magnetic Resonance Angiography for assessment of recanalization after coil embolization of visceral artery aneurysms
 Signature: Pol J Radiol, 2013; 78(1): 64-68 DOI: 10.12659/PJR.883769 CASE REPORT Received: 2012.09.29 Accepted: 2013.01.15 Time-resolved Magnetic Resonance Angiography for assessment of recanalization
Signature: Pol J Radiol, 2013; 78(1): 64-68 DOI: 10.12659/PJR.883769 CASE REPORT Received: 2012.09.29 Accepted: 2013.01.15 Time-resolved Magnetic Resonance Angiography for assessment of recanalization
Case Endovascular management of non maturing dyalisis vascular access
 Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Paediatric cerebrovascular CT angiography towards better image quality
 Original Article Paediatric cerebrovascular CT angiography towards better image quality Stefanie C. Thust, Wui Khean Kling Chong, Roxana Gunny, Asif Mazumder, Marius Poitelea, Anna Welsh, Ash Ederies,
Original Article Paediatric cerebrovascular CT angiography towards better image quality Stefanie C. Thust, Wui Khean Kling Chong, Roxana Gunny, Asif Mazumder, Marius Poitelea, Anna Welsh, Ash Ederies,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Cover Page The handle http://hdl.handle.net/1887/21764 holds various files of this Leiden University dissertation. Author: Mos, Inge Christina Maria Title: A more granular view on pulmonary embolism Issue
Imaging of Hereditary Hemorrhagic Telangiectasia
 Cardiovasc Intervent Radiol DOI 10.1007/s00270-008-9344-2 PICTORIAL ESSAY Imaging of Hereditary Hemorrhagic Telangiectasia Marie-France Carette Æ Cosmina Nedelcu Æ Marc Tassart Æ Jean-Didier Grange Æ Marie
Cardiovasc Intervent Radiol DOI 10.1007/s00270-008-9344-2 PICTORIAL ESSAY Imaging of Hereditary Hemorrhagic Telangiectasia Marie-France Carette Æ Cosmina Nedelcu Æ Marc Tassart Æ Jean-Didier Grange Æ Marie
Anterior Spinal Artery and Artery of Adamkiewicz Detected by Using Multi-Detector Row CT
 AJNR Am J Neuroradiol 24:13 17, January 2003 Anterior Spinal Artery and Artery of Adamkiewicz Detected by Using Multi-Detector Row CT Kohsuke Kudo, Satoshi Terae, Takeshi Asano, Masaki Oka, Kenshi Kaneko,
AJNR Am J Neuroradiol 24:13 17, January 2003 Anterior Spinal Artery and Artery of Adamkiewicz Detected by Using Multi-Detector Row CT Kohsuke Kudo, Satoshi Terae, Takeshi Asano, Masaki Oka, Kenshi Kaneko,
Role of MDCT in Identification of the Bleeding Site and the Vessels Causing Hemoptysis
 MDCT Detection of leeding Site and Vessels Causing Hemoptysis Chest Imaging Pictorial Essay ntoine Khalil 1 Muriel Fartoukh 2 Marc Tassart 1 ntoine Parrot 2 Claude Marsault 1 Marie-France Carette 1 Khalil,
MDCT Detection of leeding Site and Vessels Causing Hemoptysis Chest Imaging Pictorial Essay ntoine Khalil 1 Muriel Fartoukh 2 Marc Tassart 1 ntoine Parrot 2 Claude Marsault 1 Marie-France Carette 1 Khalil,
GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE
 2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
Treatment options for endoleaks: stents, embolizations and conversions
 Treatment options for endoleaks: stents, embolizations and conversions Poster No.: C-0861 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit G. Lombardi; napoli/it Arteries / Aorta, Abdomen,
Treatment options for endoleaks: stents, embolizations and conversions Poster No.: C-0861 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit G. Lombardi; napoli/it Arteries / Aorta, Abdomen,
Comparison of CT findings between MDR-TB and XDR-TB
 Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
The Location and Size of Pulmonary Embolism in Antineoplastic Chemotherapy Patients 1
 The Location and Size of Pulmonary Embolism in Antineoplastic Chemotherapy Patients 1 Yun Joo Park, M.D., Woocheol Kwon, M.D., Won-Yeon Lee, M.D. 2, Sang Baek Koh, M.D. 3, Seong Ah Kim, M.D., Myung Soon
The Location and Size of Pulmonary Embolism in Antineoplastic Chemotherapy Patients 1 Yun Joo Park, M.D., Woocheol Kwon, M.D., Won-Yeon Lee, M.D. 2, Sang Baek Koh, M.D. 3, Seong Ah Kim, M.D., Myung Soon
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
The Continuing Role of Pushable Coils: Advances and Fiscal Responsibilities JAMES F BENENATI MD
 The Continuing Role of Pushable Coils: Advances and Fiscal Responsibilities JAMES F BENENATI MD James Benenati, MD Royalty: Penumbra Stock: Covidien Consultant/Advisory Board: Penumbra, Endoshape, Scientia
The Continuing Role of Pushable Coils: Advances and Fiscal Responsibilities JAMES F BENENATI MD James Benenati, MD Royalty: Penumbra Stock: Covidien Consultant/Advisory Board: Penumbra, Endoshape, Scientia
Vascular Malformations of the Brain. William A. Cox, M.D. Forensic Pathologist/Neuropathologist. September 8, 2014
 Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Vascular Malformations of the Brain William A. Cox, M.D. Forensic Pathologist/Neuropathologist September 8, 2014 Vascular malformations of the brain are classified into four principal groups: arteriovenous
Popliteal vein aneurysm presenting as recurrent pulmonary embolism
 vein aneurysm presenting as recurrent pulmonary embolism Joel Lim 1*, Martin Marshall 2 1. Department of Clinical Services, Royal Perth Hospital, Perth, Australia 2. Department of Diagnostic and Radiology,
vein aneurysm presenting as recurrent pulmonary embolism Joel Lim 1*, Martin Marshall 2 1. Department of Clinical Services, Royal Perth Hospital, Perth, Australia 2. Department of Diagnostic and Radiology,
Pulmonary vascular anatomy & anatomical variants
 Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
B-Flow, Power Doppler and Color Doppler Ultrasound in the Assessment of Carotid Stenosis: Comparison with 64-MD-CT Angiography
 Med. J. Cairo Univ., Vol. 85, No. 2, March: 805-809, 2017 www.medicaljournalofcairouniversity.net B-Flow, Power Doppler and Color Doppler Ultrasound in the Assessment of Carotid Stenosis: Comparison with
Med. J. Cairo Univ., Vol. 85, No. 2, March: 805-809, 2017 www.medicaljournalofcairouniversity.net B-Flow, Power Doppler and Color Doppler Ultrasound in the Assessment of Carotid Stenosis: Comparison with
Role of Three-Dimensional Rotational Angiography in the Treatment of Spinal Dural Arteriovenous Fistulas
 Open Access Case Report DOI: 10.7759/cureus.1932 Role of Three-Dimensional Rotational Angiography in the Treatment of Spinal Dural Arteriovenous Fistulas Yigit Ozpeynirci 1, Bernd Schmitz 2, Melanie Schick
Open Access Case Report DOI: 10.7759/cureus.1932 Role of Three-Dimensional Rotational Angiography in the Treatment of Spinal Dural Arteriovenous Fistulas Yigit Ozpeynirci 1, Bernd Schmitz 2, Melanie Schick
Utilization patterns and yield of Computed Tomography Pulmonary Angiogram (CTPA) at a tertiary teaching hospital - Liverpool Hospital
 Utilization patterns and yield of Computed Tomography Pulmonary Angiogram (CTPA) at a tertiary teaching hospital - Liverpool Hospital Poster No.: R-0017 Congress: Type: Authors: Keywords: DOI: 2014 CSM
Utilization patterns and yield of Computed Tomography Pulmonary Angiogram (CTPA) at a tertiary teaching hospital - Liverpool Hospital Poster No.: R-0017 Congress: Type: Authors: Keywords: DOI: 2014 CSM
Penumbra, Inc. has been successful in bringing a
 Ruby Coil and POD System: A Coil Platform for Fast and Easy Embolization BY PARAG J. PATEL, MD, AND FRANK R. ARKO III, MD Penumbra, Inc. has been successful in bringing a complete embolization system to
Ruby Coil and POD System: A Coil Platform for Fast and Easy Embolization BY PARAG J. PATEL, MD, AND FRANK R. ARKO III, MD Penumbra, Inc. has been successful in bringing a complete embolization system to
Coronary to Bronchial Artery Fistula Causing Massive Hemoptysis in Patients with Longstanding Pulmonary Tuberculosis
 Case Report DOI: 10.3348/kjr.2012.13.1.102 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(1):102-106 Coronary to Bronchial Artery Fistula Causing Massive Hemoptysis in Patients with Longstanding
Case Report DOI: 10.3348/kjr.2012.13.1.102 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(1):102-106 Coronary to Bronchial Artery Fistula Causing Massive Hemoptysis in Patients with Longstanding
P ulmonary embolism (PE) is a common disease estimated to
 53 PULMONARY EMBOLISM Prospective evaluation of unsuspected pulmonary embolism on contrast enhanced multidetector CT (MDCT) scanning Gillian Ritchie, Simon McGurk, Catriona McCreath, Catriona Graham, John
53 PULMONARY EMBOLISM Prospective evaluation of unsuspected pulmonary embolism on contrast enhanced multidetector CT (MDCT) scanning Gillian Ritchie, Simon McGurk, Catriona McCreath, Catriona Graham, John
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment
 Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
Imaging of acute pulmonary thromboembolism*
 Silva, Isabela et al. Imaging of acute pulmonary thromboembolism Imaging of acute pulmonary thromboembolism* C. ISABELA S. SILVA, NESTOR L. MÜLLER The diagnosis of acute pulmonary thromboembolism is based
Silva, Isabela et al. Imaging of acute pulmonary thromboembolism Imaging of acute pulmonary thromboembolism* C. ISABELA S. SILVA, NESTOR L. MÜLLER The diagnosis of acute pulmonary thromboembolism is based
You Won t Believe What I Saw on. Disclosures. Goals. Dimensions 2013 October 18 th Michael Pfeiffer, MD. No Financial Disclosures
 You Won t Believe What I Saw on that ECHO! Dimensions 2013 October 18 th Michael Pfeiffer, MD Disclosures No Financial Disclosures Goals Review unusual and unique echocardiographic images. Briefly present
You Won t Believe What I Saw on that ECHO! Dimensions 2013 October 18 th Michael Pfeiffer, MD Disclosures No Financial Disclosures Goals Review unusual and unique echocardiographic images. Briefly present
