Workup for Perinatal Stroke Does Not Predict Recurrence
|
|
|
- Piers McDowell
- 5 years ago
- Views:
Transcription
1 Workup for Perinatal Stroke Does Not Predict Recurrence Laura L. Lehman, MD; Jeanette Beaute, BA; Kush Kapur, PhD; Amy R. Danehy, MD; Miya E. Bernson-Leung, MD; Hayley Malkin, BA; Michael J. Rivkin, MD; Cameron C. Trenor, III, MD, MMSc Background and Purpose Perinatal stroke, including neonatal and presumed perinatal presentation, represents the age in childhood in which stroke occurs most frequently. The roles of thrombophilia, arteriopathy, and cardiac anomalies in perinatal ischemic stroke are currently unclear. We took a uniform approach to perinatal ischemic stroke evaluation to study these risk factors and their association with recurrent stroke. Methods We reviewed records of perinatal stroke patients evaluated from August 2008 to February 2016 at a single referral center. Demographics, echocardiography, arterial imaging, and thrombophilia testing were collected. Statistical analysis was performed using Fisher exact test. Results Across 215 cases, the median follow-up was 3.17 years (1.49, 6.46). Females comprised 42.8% of cases. Age of presentation was neonatal (110, 51.2%) or presumed perinatal (105, 48.8%). The median age at diagnosis was 2.9 days (interquartile range, ) for neonatal stroke and 12.9 months (interquartile range, ) for presumed perinatal stroke. Strokes were classified as arterial (149, 69.3%), venous (60, 27.9%), both (4, 1.9%), or uncertain (2, 0.9%) by consensus imaging review. Of the 215 cases, there were 6 (2.8%) recurrent ischemic cerebrovascular events. Abnormal thrombophilia testing was not associated with recurrent stroke, except for a single patient with combined antithrombin deficiency and protein C deficiency. After excluding venous events, 155 patients were evaluated for arteriopathy and cardioembolic risk factors; neither was associated with recurrent stroke. Positive family history of thrombosis was not predictive of abnormal thrombophilia testing. Conclusions Thrombophilia, arteriopathy, or cardioembolic risk factors were not predictive of recurrent events after perinatal stroke. Thrombophilia evaluation in perinatal stroke should only rarely be considered. (Stroke. 2017;48: DOI: /STROKEAHA ) Key Words: echocardiography pregnancy perinatal stroke thrombophilia Perinatal ischemic stroke is the most common presentation of pediatric stroke. 1 Perinatal ischemic stroke is defined as a focal disruption of cerebral blood flow secondary to arterial or cerebral venous thrombosis or embolization, between 20 weeks of fetal life through 28th postnatal day, confirmed by neuroimaging. 2 Thus, perinatal ischemic stroke occurs in the prenatal, birth, or postnatal time periods. Clinical presentation from birth to 28 days of life is termed neonatal stroke, while presentation later in life is called presumed perinatal stroke. Risk factors that have been associated with cases of ischemic perinatal stroke can be divided into maternal, placental, and fetal. Maternal risk factors include thrombophilia, infertility, prolonged rupture of membranes, preeclampsia, smoking, intrauterine growth restriction, and infection. 1,3 6 The placental risk factors include chorioamnionitis, placental infarcts, and placental weight less than the 10th percentile. 7 Fetal risk factors include thrombophilia, congenital heart disease, and arteriopathy. 6,8 10 The roles of fetal risk factors, including thrombophilia, arteriopathy, and cardioembolic risk factors, in the pathogenesis of perinatal ischemic stroke or recurrence risk are unclear. Thrombophilia has been associated with perinatal ischemic stroke, including deficiencies in antithrombin, protein C, protein S, factor V Leiden, and prothrombin gene mutation G20210A, as well as with elevations in homocysteine and lipoprotein (a) and positive antiphospholipid antibodies Limited by their retrospective, multicenter approach, these studies compile data from varied laboratory panels with inconsistent definitions of abnormal thrombophilia testing. Recent evaluation of 135 patients and 77 controls found no increase in thrombophilia in children after perinatal stroke. 15 However, this study did not assess risk factors for recurrent stroke after perinatal stroke. Arteriopathy is rarely reported in perinatal arterial ischemic stroke, except for 1 case report of an arterial dissection. 8 Congenital heart disease is associated with perinatal arterial Received March 15, 2017; final revision received June 9, 2017; accepted June 14, From the Stroke and Cerebrovascular Center (L.L.L., J.B., A.R.D., M.E.B.-L., H.M., M.J.R., C.C.T.), Departments of Neurology (L.L.L., J.B., K.K., M.E.B.-L., M.J.R.), Psychiatry (M.J.R.), and Radiology (A.R.D., M.J.R.), and Division of Hematology/Oncology (H.M., C.C.T.), Boston Children s Hospital, Harvard Medical School, MA. Presented in part at the International Stroke Conference, Los Angeles, CA, February 17 19, Correspondence to Laura Lehman, MD, Boston Children s Hospital, 300 Longwood Ave, Fegan 11, Boston, MA laura.lehman@childrens. harvard.edu 2017 American Heart Association, Inc. Stroke is available at DOI: /STROKEAHA
2 Lehman et al Workup for Perinatal Stroke 2079 ischemic stroke, including recurrent stroke. 16,17 The utility of echocardiogram for the use of prediction of recurrent stroke after neonatal stroke in the absence of known concern for congenital heart disease is unknown. We took a uniform approach to perinatal ischemic stroke evaluation to better understand thrombophilic risk factors. Since 2008, our evaluation of children with perinatal ischemic stroke has consistently included a standard thrombophilia evaluation and a magnetic resonance angiography (MRA) or computed tomography angiography of head and neck and echocardiogram in children with perinatal arterial ischemic stroke. We have reviewed these data to determine the frequency of abnormal findings and whether these predict stroke recurrence after perinatal stroke in this retrospective study. Materials and Methods Following Boston Children s Hospital Institutional Review Board approval, we reviewed records of all patients evaluated in our Cerebrovascular Disorders and Stroke Program from August 2008 to February Inclusion criteria for this study included any patient with a diagnosis of perinatal stroke, including arterial and venous infarcts, as well as neonatal and presumed perinatal presentation. We retrospectively collected demographics, thrombophilia, arterial imaging, and echocardiography data into a Research Electronic Data Capture database. 18 All data were extracted by a study team member and verified by a stroke physician. Demographic data included sex, race, ethnicity, birth date, age at stroke diagnosis, and age at last follow-up. Data reviewed included family history of thrombosis, specific thrombophilia testing, MRA and computed tomography angiography and echocardiogram findings. If a child did not have thrombophilia laboratory testing done, the patient was not included, which was <5% of our cohort. Details around recurrent cerebrovascular events were also collected, and all recurrent events underwent multidisciplinary review for confirmation. Infarcts were defined as arterial, venous, or indeterminate through consensus discussion in an unblinded multidisciplinary conference review including neuroradiologist, neurologists, and a hematologist. Thrombophilia was assessed as a risk factor for recurrence for all types of perinatal strokes with acute laboratory assessment in neonatal stroke patients and deferred to older than 6 months in presumed perinatal stroke patients. Because arteriopathy and cardioembolic sources do not explain venous infarcts, assessment of these risk factors was restricted to the subset of arterial ischemic or indeterminate strokes. Factor V Leiden was diagnosed by activated protein C resistance and confirmed with genetic testing. Prothrombin gene mutation (FII G20210A) was diagnosed with genetic testing. Thresholds for protein C, protein S, and antithrombin deficiencies used published agenormalized reference ranges on modern instruments. 19 Patients were diagnosed with antithrombin, protein C, or protein S deficiency when functional testing was low for age after 6 months of age for protein S and antithrombin and after 1 year of age for protein C. If the child only had testing at diagnosis but not repeat testing, these patients were not diagnosed with thrombophilia, and testing was considered unconfirmed. Unconfirmed testing in the analysis was considered not done. Elevated lipoprotein(a) and homocysteine levels were defined as a single test greater than reference range. For lipoprotein(a), age-appropriate reference ranges are not available, and we used a conservative normal range of 0 to 29 mg/dl. Antiphospholipid antibodies, including lupus anticoagulant, anti-cardiolipin IgG and IgM, and anti-β2 glycoprotein-1 IgG and IgM, were tested and considered positive if >40 U/mL tested at least twice >12 weeks apart. Lupus anticoagulant was considered positive if a screening lupus anticoagulant-sensitive activated partial thromboplastin time (Stago; Parsippany, NJ) is prolonged and then neutralized with addition of hexagonal phospholipids. Positive family history was defined as first degree family member with myocardial infarction or stroke before age 50 years, deep vein thrombosis, pulmonary embolus, or recurrent miscarriages. We defined arteriopathy as abnormal arteries found on initial computed tomography angiography or MRA interpreted as likely causing the perinatal arterial ischemic stroke. Embryonic variants and diminished flow to large infarcts were not considered arteriopathies. All cases of possible arteriopathy underwent multidisciplinary review for consensus. Cardioembolic risk factors included patent foramen ovale (PFO), congenital heart disease, extracorporeal membrane oxygenation, cardiac surgery, cardiac catheterization, and intracardiac thrombus. Statistical Analysis We used Fisher exact test to examine whether family history of thrombosis predicted abnormal thrombophilia testing and whether thrombophilia, arteriopathy, or cardioembolic risk factors predicted recurrent event. Statistical significance was defined as a P value <0.05. Results We evaluated 215 cases of perinatal ischemic stroke with a median follow-up of 3.17 years (interquartile range [IQR], ) counted since birth. The median age at diagnosis was 2.9 days (IQR, ) for neonatal stroke and 12.9 months (IQR, ) for presumed perinatal stroke. Out of the 215 children, 14 (6.5%) were preterm infants. Characteristics of this patient cohort are described in Table 1. Of the 215 cases, 6 (2.8%) had recurrent ischemic Table 1. Demographics of Children With Perinatal Stroke Characteristic N=215 (%) Sex Females 92 (42.8%) Race White 148 (68.8%) Black 16 (7.4%) Asian 4 (1.9%) Other 18 (8.4%) Unknown 29 (13.5%) Type of stroke Arterial 149 (69.3%) Venous 60 (27.9%) Both 4 (1.9%) Indeterminate 2 (0.9%) Presentation Neonatal 110 (51.2%) Arterial 68 (61.2%) Venous 39 (35.5%) Both 3 (2.7%) Indeterminate 0 (0%) Presumed perinatal 105 (48.8%) Arterial 81 (77.1%) Venous 21 (20.0%) Both 1 (0.9%) Indeterminate 2 (1.9%)
3 2080 Stroke August 2017 cerebrovascular events: 3 venous, 2 arterial, and 1 arterial and venous. Of the recurrences, there was 1% recurrence rate in the presumed perinatal stroke group (1/105) compared with 4.5% rate in the neonatal stroke group (5/110). The anatomic distribution and associated risk factors in all 6 cases of recurrent stroke are reviewed in Table 2. Brief case vignettes are provided below for each case of recurrent stroke. Patient 1 is a male born at 32 weeks gestation. Both his brother and mother had known antithrombin deficiency. Initial head ultrasound was concerning for left hemispheric hemorrhage. Subsequent magnetic resonance imaging (MRI) at 6 days of life identified a left middle cerebral artery stroke with hemorrhagic transformation and a normal MRA of the head. Repeat MRI at 15 days of life identified new cerebral sinovenous thrombosis involving the sagittal sinus, right transverse sinus, straight sinus, and vein of Galen with bilateral ischemic and hemorrhagic venous infarct. Patient 2 is a male born at 30 weeks gestation who presented with apneic episode. Head ultrasound found hemorrhage, confirmed by MRI at 2 days old, showing left temporal lobe hemorrhage with medullary venous thrombosis and right middle cerebral artery stroke with normal MRA of the head. Subsequent MRI at 2 weeks old was found to have a new large superior sagittal sinus thrombosis. Case 3 is a male born at 41 weeks, diagnosed postnatally with Pierre Robin Sequence who presented soon after birth with seizures. MRI at 7 days old identified hemorrhagic venous infarction and a superior sagittal venous thrombosis. He later developed a right middle cerebral artery territory stroke at 11 years of age after spinal fusion surgery. Patient 4 was born full term. He had an MRI when he was 11 weeks old because of concern of bilateral extremity weakness. His MRI was significant for bilateral encephalomalacia in the bilateral middle cerebral artery territories and left anterior cerebral artery territory. He presented again at 6 months of age with seizure and had bilateral watershed injury with again a normal MRA. At 8 months of age, MRI for recurrent seizure showed watershed ischemia again, and his MRA was read as normal but retrospectively showed evidence of early moyamoya. At 3 years of age, he was diagnosed with bilateral moyamoya when he presented with an acute right middle cerebral artery stroke. Patient 5 is a female born at 39 weeks with abnormal placental pathology consistent with fetal thrombotic vasculopathy. She had an MRI at 10 days old because of multiple congenital anomalies, revealing an acute left posterior cerebral artery stroke. Genetic testing demonstrated trisomy 12p. She had a follow-up MRI and MRA at 4 years of age for transient ischemia attack when she presented with left-sided weakness that resolved completely; this MRI showed no acute injury, and MRA was normal. She presented at 9 years of age with a right hemiparesis and had a left hemispheric stroke involving anterior cerebral artery, posterior cerebral artery, and middle cerebral artery and was diagnosed with bilateral large vessel vasculitis. She was treated with steroids, and her vasculature improved. Patient 6 is a male born at 39 weeks gestation with significant perinatal distress and was treated with therapeutic hypothermia. His postcooling MRI at 5 days Table 2. Recurrent Ischemic Cerebrovascular Events Patient No. Presenting Event Timing of Presentation Recurrent Event Age at Recurrence Risk Factors Identified 1 Arterial: left MCA AIS with hemorrhagic transformation 2 Arterial and venous: right MCA multifocal AIS and temporal lobe hemorrhage with medullary vein thrombosis and infarction 3 Venous: venous infarction with hemorrhage and superior sagittal venous thrombosis 4 Arterial: multifocal encephalomalacia bilateral MCA and left ACA Neonatal; 6 days old Neonatal; 2 days old Venous: dural venous sinus and medullary vein thrombosis Venous: superior sagittal sinus thrombosis 16 days old Deficiencies of antithrombin (36%) and protein C (63%)* 17 days old None Neonatal; 7 days old Arterial: right MCA AIS 11 y old Perioperative (spinal fusion); elevated lipoprotein(a) Presumed perinatal; 11 weeks old Arterial: multiple AIS 5 Arterial: left PCA AIS Neonatal; 10 days old Arterial: left hemispheric AIS involving ACA, MCA, and PCA 6 Venous: left periventricular venous infarction Neonatal; 5 days old New hemorrhagic venous infarct and new right PCA AIS 6 mo old (seizure with watershed white matter infarction); 8 mo (watershed acute injury in setting of seizure); 3 y (seizure, R MCA stroke and Moyamoya) Moyamoya identified at 3 y of age 7 y old CNS vasculitis identified at recurrence, elevated lipoprotein(a) 12 days old None ACA indicates anterior cerebral artery; AIS, arterial ischemic stroke; CNS, central nervous system; DOL, day of life; GA, gestational age; MCA, middle cerebral artery; MRA, magnetic resonance angiography; and PCA, posterior cerebral artery. *In parentheses are the functional levels.
4 Lehman et al Workup for Perinatal Stroke 2081 old showed small left acute ischemic periventricular venous infarction. He had his follow-up MRI and MRA at 12 days of life showing acute right posterior cerebral artery stroke and a large temporal lobe hemorrhagic venous infarct. All of the recurrent events were documented as a separate event not an extension of the initial event. Analysis of laboratory testing for thrombophilia and association with recurrent stroke was performed (Table 3). Approximately one third of patients had at least 1 abnormal test, most commonly elevation of lipoprotein(a). The only single test associated with stroke recurrence was antithrombin deficiency, found in 1 patient with recurrent stroke who also had protein C deficiency. However, when we used the Bonferroni correction for multiple comparisons, the P value was not significant (P=0.255). Family history of thrombosis was analyzed as a predictor of abnormal thrombophilia testing. Of 18 patients with a positive family history, 10 patients had no thrombophilia abnormalities (P=0.2970). Analysis of arteriopathy and cardioembolic risk factors was restricted to the 155 cases of perinatal arterial ischemic stroke because arteriopathy and cardioembolic risk factors are irrelevant to venous strokes. Arterial imaging (MRA or computed tomography angiography) was performed in 114 patients, and echocardiogram was performed in 97 patients. Of 155 perinatal arterial ischemic stroke cases, there were no cases of arteriopathy on initial imaging. There were 4 recurrences, and none had arteriopathy on initial imaging (P=1.000). Subsequently, 3 children had arteriopathy at time of recurrence. Of 97 patients with echocardiogram data, 50 (51.5%) patients had PFOs. Out of the 85 children with presumed perinatal strokes, 10 (11.8%) had PFOs compared with 40 (54.8%) of the 85 infants with neonatal stroke. Out of the 4 (4.1%) with recurrent strokes, 2 (50.0%) of these had PFOs. Of the 93 patients without recurrent stroke, 48 (51.6%) had PFOs. In our current sample, PFO was not predictive of recurrent stroke (P=1.000). None of the recurrent cases had other (non- PFO) cardioembolic risk factors compared with 13 (14.0%) of the cases without recurrence. Other cardioembolic risk factors identified included 1 with valve vegetations, 3 with atrial septal defect, 3 with ventricular septal defect, 1 with cardiomyopathy, and 5 with complex congenital heart disease; none of these were associated with stroke recurrence (P=1.000). Discussion We evaluated 215 cases of perinatal ischemic stroke at a single hospital referral center. Similar to other studies of children with perinatal ischemic stroke, 49% were presumed perinatal stroke and 51% were neonatal in presentation. 20,21 We found a rate of recurrent cerebrovascular events of 2.8% similar to the previously reported rate of 3%. 16 Using a strict definition of thrombophilia and Fisher exact test, only antithrombin deficiency was associated with recurrent stroke, based on a single patient who also had a protein C deficiency. We hesitate to conclude that antithrombin deficiency is specifically associated with stroke recurrence after perinatal stroke based on 1 case. Factor V Leiden, prothrombin gene mutation, protein C deficiency, protein S deficiency, elevated homocysteine, elevated lipoprotein (a), and persistent antiphospholipid antibodies were not associated with recurrent Table 3. Thrombophilia Thrombophilia in Children With Perinatal Stroke Recurrence (N=6) No Recurrence (N=209) Total=215 P Value Any abnormal None 3 (50.0%) 139 (66.5%) 142 (66.0%) One or more 3 (50.0%) 70 (33.5%) 73 (34.0%) Factor V Leiden Heterozygote 0 (0.0%) 15 (7.6%) 15 (7.4%) Wild-type 6 (100.0%) 183 (92.4%) 189 (92.6%) Prothrombin Heterozygote 0 (0.0%) 8 (4.2%) 8 (4.0%) Wild-type 6 (100.0%) 184 (95.8%) 190 (96.0%) Antithrombin Deficient 1 (20.0%) 0 (0.0%) 1 (0.5%) * Normal 4 (80.0%) 191 (100.0%) 195 (99.5%) * Protein C Deficient 1 (16.7%) 11 (5.7%) 12 (6.0%) Normal 5 (83.3%) 183 (94.3%) 188 (94.0%) Protein S Deficient 0 (0.0%) 13 (6.8%) 13 (6.6%) Normal 5 (100.0%) 178 (93.2%) 183 (93.4%) Lipoprotein (a) Elevated 2 (50. %) 33 (17.6%) 35 (18.2%) Normal 2 (50.0%) 155 (82.4%) 157 (81.8%) Homocysteine Normal 6 (100%) 197 (100%) 203 (100%) Anticardiolipin IgG Normal 5 (100%) 102 (100%) 107 (100%) Anticardiolipin IgM Normal 5 (100%) 102 (100%) 107 (100%) β2-glycoprotein IgG Normal 3 (100%) 84 (100%) 87 (100%) β2-glycoprotein IgM Normal 3 (100%) 83 (100%) 86 (100%) Lupus anticoagulant Positive 0(0%) 0 (0%) 0 (0%) Negative 4 (100%) 102 (100%) 106 (100%) *Using Bonferroni correction P value is not significant (P=0.255). stroke. Existing literature is limited to case reports, case series, or meta-analyses associating variable thrombophilia evaluations to stroke in limited numbers of patients. 14 A small number
5 2082 Stroke August 2017 of studies exist that examine cohorts of children after perinatal stroke, with only a few of these studies reporting recurrent events and none having enough recurrent events to answer the question of whether thrombophilia is associated with recurrence. 16 Our rate of abnormal thrombophilia testing (33.5%) may be lower than other series because of our strict definition of thrombophilia and the use of elevated homocysteine rather than methylenetetrahydrofolate reductase polymorphisms as a thrombotic risk factor. Even though antiphospholipid antibody syndrome is associated with recurrent stroke in older children, we did not have a single case of persistently elevated antiphospholipid antibodies after perinatal stroke. 22 Our data raise questions about the role of thrombophilia testing in perinatal stroke. In this study, positive family history of thrombosis was not predictive of abnormal thrombophilia testing. This finding may be limited by sample size because larger studies of pediatric venous thrombosis suggest that positive family history is predictive of thrombophilia and recurrence. 23 Unlike stroke in older patients, the workup for arteriopathy and cardioembolic risk factors does not predict recurrent stroke. 24,25 Compared with a 5-year recurrence rate of 66% in pediatric stroke patients with arteriopathy, our study identified no patients with arteriopathy at diagnosis and recurrence after perinatal arterial ischemic stroke. 24 Arterial occlusion in neonatal arterial ischemic stroke is isolated and may result from thromboembolism rather than primary arterial pathology. 26,27 The presence of arteriopathy in perinatal arterial ischemic stroke is rare. When identified, especially if arteriopathy exists in the same vascular territory as the infarct, this may warrant additional investigation and follow-up. The role of arterial imaging to evaluate causation of perinatal stroke is unclear, and arteriopathy is not predictive of recurrent stroke in our study. In older children, complex congenital heart disease is an established risk factor for recurrent stroke. 17,25 In our cohort of perinatal arterial ischemic stroke, none of the cases of recurrent stroke had congenital heart disease. In our cohort, the percentage of infants with PFOs at time of neonatal stroke (54.8%) and in older children with presumed perinatal stroke (11.8%) is similar to previously reported rates in the general population of infants, with 58% having a PFO on day of life one and 27% having a PFO at 6 weeks of life. 28,29 The presence of PFO and other cardiac anomalies on echocardiogram were also not predictive of recurrent stroke. As few of our patients had symptomatic congenital heart disease, our data provide contrast to literature on patients with symptomatic congenital heart disease in whom 14% had recurrent stroke after initial neonatal stroke. 17 In our cohort, only 5 patients had complex congenital heart disease, and all of these had known cardiac conditions prior to echocardiography. The role of echocardiography to detect occult cardioembolic causes of perinatal stroke is unclear. Our study is limited by the sample size available to us at a single institution but strengthened by a uniform approach to risk factor assessment after perinatal stroke. We were also limited by having only a median of 3.17 years of follow-up. The low recurrence rate after perinatal stroke is encouraging but limits our power to detect associations between various risk factors and recurrence. Although the majority of patients were seen in our multidisciplinary clinic, there was still some variation in practice, as well as clinician preference, leading to some patients not having MRA of head, echocardiogram, or complete thrombophilia evaluation. Further, our study does not include a control group of infants to determine whether rates of thrombophilia are greater in the perinatal stroke population; recent case control study from a Canadian registry found no association with thrombophilia and perinatal stroke. 15 Our study included mostly white patients, which may limit applicability to other ethnic groups. Because thrombophilia, arteriopathy, and cardioembolic risk factors are not predictive of recurrence, our data support other hypotheses about the pathogenesis of perinatal stroke, including those that address placental and maternal risk factors. Abnormal placental pathology has been associated with perinatal ischemic stroke. 7,30 The low recurrence rate after perinatal stroke supports placental or maternal risk factors as causative rather than thrombophilia, cardiac, or arterial risk factors because these risk factors persist in the patient and would be expected, theoretically, to carry increased risk of recurrent stroke if causative. Our data also suggest that the mechanisms of recurrent strokes are distinct from the mechanisms of perinatal events as, in this cohort, rare recurrent strokes occurred either acutely or years later because of acquired arteriopathy or periprocedural events. Conclusions Thrombophilia testing may not be indicated in the assessment of perinatal stroke in the absence of positive family history or additional thrombotic complications. Cervicocephalic arterial imaging and echocardiogram do not predict recurrent stroke, and their role in identifying causative arteriopathy or occult cardiac disease is unclear. In the absence of other clinical concerns, use of arterial or cardiac imaging after perinatal arterial ischemic stroke should be carefully considered. Clinicians should consider the cost and, for older children, the risk of sedation for these imaging studies. Future research should focus on placental and other risk factors as the pathogenesis of perinatal stroke. None. Disclosure References 1. Wu YW, March WM, Croen LA, Grether JK, Escobar GJ, Newman TB. Perinatal stroke in children with motor impairment: a population-based study. Pediatrics. 2004;114: doi: /peds Raju TN, Nelson KB, Ferriero D, Lynch JK; NICHD-NINDS Perinatal Stroke Workshop Participants. Ischemic perinatal stroke: summary of a workshop sponsored by the National Institute of Child Health and Human Development and the National Institute of Neurological Disorders and Stroke. Pediatrics. 2007;120: doi: /peds Lee J, Croen LA, Backstrand KH, Yoshida CK, Henning LH, Lindan C, et al. Maternal and infant characteristics associated with perinatal arterial stroke in the infant. JAMA. 2005;293: doi: / jama Harteman JC, Groenendaal F, Kwee A, Welsing PM, Benders MJ, de Vries LS. Risk factors for perinatal arterial ischaemic stroke in fullterm infants: a case-control study. Arch Dis Child Fetal Neonatal Ed 2012;97:F411 F416. doi: /archdischild Darmency-Stamboul V, Chantegret C, Ferdynus C, Mejean N, Durand C, Sagot P, et al. Antenatal factors associated with
6 Lehman et al Workup for Perinatal Stroke 2083 perinatal arterial ischemic stroke. Stroke. 2012;43: doi: /STROKEAHA Simchen MJ, Goldstein G, Lubetsky A, Strauss T, Schiff E, Kenet G. Factor v Leiden and antiphospholipid antibodies in either mothers or infants increase the risk for perinatal arterial ischemic stroke. Stroke. 2009;40: doi: /STROKEAHA Elbers J, Viero S, MacGregor D, DeVeber G, Moore AM. Placental pathology in neonatal stroke. Pediatrics. 2011;127:e722 e729. doi: /peds Lequin MH, Peeters EA, Holscher HC, de Krijger R, Govaert P. Arterial infarction caused by carotid artery dissection in the neonate. Eur J Paediatr Neurol. 2004;8: doi: /j.ejpn deveber G, Monagle P, Chan A, MacGregor D, Curtis R, Lee S, et al. Prothrombotic disorders in infants and children with cerebral thromboembolism. Arch Neurol. 1998;55: McQuillen PS, Barkovich AJ, Hamrick SE, Perez M, Ward P, Glidden DV, et al. Temporal and anatomic risk profile of brain injury with neonatal repair of congenital heart defects. Stroke. 2007;38(2 suppl): doi: /01.STR Günther G, Junker R, Sträter R, Schobess R, Kurnik K, Heller C, et al; Childhood Stroke Study Group. Symptomatic ischemic stroke in fullterm neonates: role of acquired and genetic prothrombotic risk factors. Stroke. 2000;31: Nowak-Göttl U, Debus O, Findeisen M, Kassenböhmer R, Koch HG, Pollmann H, et al. Lipoprotein (a): its role in childhood thromboembolism. Pediatrics. 1997;99:E Suppiej A, Franzoi M, Gentilomo C, Battistella PA, Drigo P, Gavasso S, et al. High prevalence of inherited thrombophilia in presumed peri-neonatal ischemic stroke. Eur J Haematol. 2008;80: doi: /j x. 14. Kenet G, Lütkhoff LK, Albisetti M, Bernard T, Bonduel M, Brandao L, et al. Impact of thrombophilia on risk of arterial ischemic stroke or cerebral sinovenous thrombosis in neonates and children: a systematic review and meta-analysis of observational studies. Circulation. 2010;121: doi: /CIRCULATIONAHA Curtis C, Mineyko A, Massicotte P, Leaker M, Jiang XY, Floer A, et al. Thrombophilia risk is not increased in children after perinatal stroke. Blood. 2017;129: doi: /blood Kurnik K, Kosch A, Sträter R, Schobess R, Heller C, Nowak-Göttl U; Childhood Stroke Study Group. Recurrent thromboembolism in infants and children suffering from symptomatic neonatal arterial stroke: a prospective follow-up study. Stroke. 2003;34: doi: /01. STR Rodan L, McCrindle BW, Manlhiot C, MacGregor DL, Askalan R, Moharir M, et al. Stroke recurrence in children with congenital heart disease. Ann Neurol. 2012;72: doi: /ana Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap) a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42: doi: /j. jbi Monagle P, Barnes C, Ignjatovic V, Furmedge J, Newall F, Chan A, et al. Developmental haemostasis. Impact for clinical haemostasis laboratories. Thromb Haemost. 2006;95: doi: /TH Lee J, Croen LA, Lindan C, Nash KB, Yoshida CK, Ferriero DM, et al. Predictors of outcome in perinatal arterial stroke: a population-based study. Ann Neurol. 2005;58: doi: /ana Curry CJ, Bhullar S, Holmes J, Delozier CD, Roeder ER, Hutchison HT. Risk factors for perinatal arterial stroke: a study of 60 motherchild pairs. Pediatr Neurol. 2007;37: doi: /j. pediatrneurol Berkun Y, Padeh S, Barash J, Uziel Y, Harel L, Mukamel M, et al. Antiphospholipid syndrome and recurrent thrombosis in children. Arthritis Rheum. 2006;55: doi: /art Sundquist K, Sundquist J, Svensson PJ, Zöller B, Memon AA. Role of family history of venous thromboembolism and thrombophilia as predictors of recurrence: a prospective follow-up study. J Thromb Haemost. 2015;13: doi: /jth Fullerton HJ, Wu YW, Sidney S, Johnston SC. Risk of recurrent childhood arterial ischemic stroke in a population-based cohort: the importance of cerebrovascular imaging. Pediatrics. 2007;119: doi: /peds Ziesmann MT, Nash M, Booth FA, Rafay MF. Cardioembolic stroke in children: a clinical presentation and outcome study. Pediatr Neurol. 2014;51: doi: /j.pediatrneurol Fluss J, Garcia-Tarodo S, Granier M, Villega F, Ferey S, Husson B, et al. Perinatal arterial ischemic stroke related to carotid artery occlusion. Eur J Paediatr Neurol. 2016;20: doi: /j. ejpn Husson B, Hertz-Pannier L, Adamsbaum C, Renaud C, Presles E, Dinomais M, et al. MR angiography findings in infants with neonatal arterial ischemic stroke in the middle cerebral artery territory: A prospective study using circle of Willis MR angiography. Eur J Radiol. 2016;85: doi: /j.ejrad Wang NK, Shen CT, Lin MS. Results of echocardiographic screening in 10,000 newborns. Acta Paediatr Taiwan. 2007;48: Arlettaz R, Arcjer N, Wilinson AR. Natural history of innocent heart mumurs in newborn babies: Controlled Echocardigraphic Study. Arch Dis Child Fetal Neonatal Ed 1998;78:F166 F Bernson-Leung M, Boyd T, Danehy A, Meserve E, Rivkin M. Placental pathology in neonatal stroke: a retrospective case control study. Neurology 2016;86.I
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants?
 Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
Should infants with perinatal thrombosis be screened for thrombophilia and treated by anticoagulants? Shoshana Revel-Vilk, MD MSc Pediatric Hematology Center, Pediatric Hematology/Oncology Department,
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
Perinatal thrombosis: implications for mothers and neonates
 CHALLENGING SCENARIOS IN THROMBOSIS Perinatal thrombosis: implications for mothers and neonates Sarah H. O Brien 1,2 1 Division of Pediatric Hematology/Oncology, Nationwide Children s Hospital/Ohio State
CHALLENGING SCENARIOS IN THROMBOSIS Perinatal thrombosis: implications for mothers and neonates Sarah H. O Brien 1,2 1 Division of Pediatric Hematology/Oncology, Nationwide Children s Hospital/Ohio State
Transient ischemic attack (TIA) in children has received
 Predictors of Stroke After Transient Ischemic Attack in Children Laura L. Lehman, MD; Christopher G. Watson, BS; Kush Kapur, PhD; Amy R. Danehy, MD; Michael J. Rivkin, MD Background and Purpose Transient
Predictors of Stroke After Transient Ischemic Attack in Children Laura L. Lehman, MD; Christopher G. Watson, BS; Kush Kapur, PhD; Amy R. Danehy, MD; Michael J. Rivkin, MD Background and Purpose Transient
SWISS SOCIETY OF NEONATOLOGY. Neonatal sinovenous thrombosis
 SWISS SOCIETY OF NEONATOLOGY Neonatal sinovenous thrombosis August 2006 2 Hauri-Hohl A, Zeilinger G, Pasquier S, Children s Hospital of Aarau, Switzerland Swiss Society of Neonatology, Thomas M Berger,
SWISS SOCIETY OF NEONATOLOGY Neonatal sinovenous thrombosis August 2006 2 Hauri-Hohl A, Zeilinger G, Pasquier S, Children s Hospital of Aarau, Switzerland Swiss Society of Neonatology, Thomas M Berger,
Guidelines for management of stroke in childhood
 Guidelines for management of stroke in childhood A clinical syndrome typified by rapidly developing signs of focal or global disturbance of cerebral functions, lasting more than 24 hrs or leading to death,
Guidelines for management of stroke in childhood A clinical syndrome typified by rapidly developing signs of focal or global disturbance of cerebral functions, lasting more than 24 hrs or leading to death,
Are there still any valid indications for thrombophilia screening in DVT?
 Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
Carotid artery stenosis and risk of stroke Are there still any valid indications for thrombophilia screening in DVT? Armando Mansilha MD, PhD, FEBVS Faculty of Medicine of University of Porto Munich, 2016
VTE in Children: Practical Issues
 VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
VTE in Children: Practical Issues Wasil Jastaniah MBBS,FAAP,FRCPC Consultant Pediatric Hem/Onc/BMT May 2012 Top 10 Reasons Why Pediatric VTE is Different 1. Social, ethical, and legal implications. 2.
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Thrombophilia. Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC. GASCO Atlanta Sept 8 th, Disclosures. Conflicts of interest: NONE
 LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
LA APLA 1 3 ACA Anti-ß2-GP I 2 45 Thrombophilia Stephan Moll, MD Medicine, Heme-Coag UNC Chapel Hill, NC GASCO Atlanta Sept 8 th, 2017 Disclosures Conflicts of interest: NONE Off-label product use discussion:
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO
 THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
THROMBOPHILIA TESTING: PROS AND CONS SHANNON CARPENTER, MD MS CHILDREN S MERCY HOSPITAL KANSAS CITY, MO DISCLAIMER I m a pediatrician I will be discussing this issue primarily from a pediatric perspective
Thrombophilia: To test or not to test
 Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Kenneth Bauer, MD Harvard Medical School, Boston, MA Professor of Medicine VA Boston Healthcare System Chief, Hematology Section Beth Israel Deaconess Medical Center, Boston, MA Director, Thrombosis Clinical
Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy
 Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
Original article: Study of role of MRI brain in evaluation of hypoxic ischemic encephalopathy *Dr Harshad Bhagat, ** Dr Ravindra Kawade, ***Dr Y.P.Sachdev *Junior Resident, Department Of Radiodiagnosis,
APPENDIX A NORTH AMERICAN SYMPTOMATIC CAROTID ENDARTERECTOMY TRIAL
 APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
APPENDIX A Primary Findings From Selected Recent National Institute of Neurological Disorders and Stroke-Sponsored Clinical Trials That Have shaped Modern Stroke Prevention Philip B. Gorelick 178 NORTH
Cryptogenic Stroke/PFO with Thrombophilia and VTE: Do We Know What To Do?
 Cryptogenic Stroke/PFO with Thrombophilia and VTE: Do We Know What To Do? Robert J. Sommer, MD Columbia University Medical Center New York, NY Disclosure Statement of Financial Interest Within the past
Cryptogenic Stroke/PFO with Thrombophilia and VTE: Do We Know What To Do? Robert J. Sommer, MD Columbia University Medical Center New York, NY Disclosure Statement of Financial Interest Within the past
Arterial Ischemic Stroke with Protein S Deficiency in Pakistan
 Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
Case Reports Arterial Ischemic Stroke with Protein S Deficiency in Pakistan Faika Usman, Ali Hassan, Arsalan Ahmad From Section of Neurology, Department of Medicine, Shifa International Hospitals and College
CEREBRO VASCULAR ACCIDENTS
 CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
Ayman Mahmoud Alboudi MD, MSc Rashid Hospital, Dubai, UAE
 Systemic Varicella Zoster Infection Causing Cerebral Venous Thrombosis and Revealing Prothrombotic State Ayman Mahmoud Alboudi MD, MSc Rashid Hospital, Dubai, UAE CVT is a rare disorder with incidence
Systemic Varicella Zoster Infection Causing Cerebral Venous Thrombosis and Revealing Prothrombotic State Ayman Mahmoud Alboudi MD, MSc Rashid Hospital, Dubai, UAE CVT is a rare disorder with incidence
Pediatric Stroke. David Griesemer, MD Levine Children s Hospital / Carolinas Healthcare Charlotte, NC
 Pediatric Stroke David Griesemer, MD Levine Children s Hospital / Carolinas Healthcare Charlotte, NC A whole different problem Atherosclerosis and modifiable factors are not relevant issues Populations
Pediatric Stroke David Griesemer, MD Levine Children s Hospital / Carolinas Healthcare Charlotte, NC A whole different problem Atherosclerosis and modifiable factors are not relevant issues Populations
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute ischemic stroke TOAST classification of, 270 Acute myocardial infarction (AMI) cardioembolic stroke following, 207 208 noncardioembolic
Index Note: Page numbers of article titles are in boldface type. A Acute ischemic stroke TOAST classification of, 270 Acute myocardial infarction (AMI) cardioembolic stroke following, 207 208 noncardioembolic
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Thrombophilia. Diagnosis and Management. Kevin P. Hubbard, DO, FACOI
 Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
Thrombophilia Diagnosis and Management Kevin P. Hubbard, DO, FACOI Clinical Professor of Medicine Kansas City University of Medicine and Biosciences-College of Osteopathic Medicine Kansas City, Missouri
DISCLOSURE. Presented by: Merav Sendowski, MD Oregon Health and Science University
 Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
Thrombophilia! DISCLOSURE Presented by: Merav Sendowski, MD Oregon Health and Science University Created by: Thomas Deloughery, MD Oregon Health and Science University Current Relevant Financial Relationship(s)
CLINICAL CASE PRESENTATION
 European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
European Winter School of Internal Medicine 2015 Riga, Latvia, 26-30 January CLINICAL CASE PRESENTATION Vasiliy Chulkov South Ural State Medical University (Chelyabinsk, Russia) CHELYABINSK CLINICAL HISTORY
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
GERIATRICS CASE PRESENTATION
 GERIATRICS CASE PRESENTATION CASE 79 year old Patient X was admitted to hospital with SOB. He had a hx of sarcoidosis and asbestosis. Home oxygen requirement is 3-3.5litre. He was admitted, given ceftriaxone
GERIATRICS CASE PRESENTATION CASE 79 year old Patient X was admitted to hospital with SOB. He had a hx of sarcoidosis and asbestosis. Home oxygen requirement is 3-3.5litre. He was admitted, given ceftriaxone
SWISS SOCIETY OF NEONATOLOGY. Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions
 SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
SWISS SOCIETY OF NEONATOLOGY Diagnostic evaluation of a symptomatic cerebrovascular accident in a neonate with focal convulsions July 2013 2 Anderson S, Rimensberger P, Service de Néonatologie et des Soins
Mimi Lu, MD Clinical Assistant Professor Department of Emergency Medicine University of Maryland School of Medicine
 Mimi Lu, MD Clinical Assistant Professor Department of Emergency Medicine University of Maryland School of Medicine Disclosures I have no relevant financial relationships with the manufacturer(s) of any
Mimi Lu, MD Clinical Assistant Professor Department of Emergency Medicine University of Maryland School of Medicine Disclosures I have no relevant financial relationships with the manufacturer(s) of any
Patent Foramen Ovale and Cryptogenic Stroke: Do We Finally Have Closure? Christopher Streib, MD, MS
 Patent Foramen Ovale and Cryptogenic Stroke: Do We Finally Have Closure? Christopher Streib, MD, MS 11-8-18 Outline 1. Background 2. Anatomy of patent foramen ovale (PFO) 3. Relationship between PFO and
Patent Foramen Ovale and Cryptogenic Stroke: Do We Finally Have Closure? Christopher Streib, MD, MS 11-8-18 Outline 1. Background 2. Anatomy of patent foramen ovale (PFO) 3. Relationship between PFO and
I t is increasingly recognised that arterial cerebral infarction
 F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
F252 ORIGINAL ARTICLE Does cranial ultrasound imaging identify arterial cerebral infarction in term neonates? F Cowan, E Mercuri, F Groenendaal, L Bassi, D Ricci, M Rutherford, L de Vries... See end of
Recent Advances in Neurology Difficult Cases
 Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Patient X: History Part 1 Recent Advances in Neurology Difficult Cases Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Brain Center Previously healthy 14-year old
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase <48h)
 Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Antithrombotic therapy in patients with transient ischemic attack / stroke (acute phase
Neuropathology lecture series. III. Neuropathology of Cerebrovascular Disease. Physiology of cerebral blood flow
 Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
Chapter. Absolute risk of venous and arterial thrombosis in HIV-infected patients and effects of combination antiretroviral therapy
 Chapter Absolute risk of venous and arterial thrombosis in HIV-infected patients and effects of combination antiretroviral therapy Willem M. Lijfering Min Ki ten Kate Herman G. Sprenger Jan van der Meer
Chapter Absolute risk of venous and arterial thrombosis in HIV-infected patients and effects of combination antiretroviral therapy Willem M. Lijfering Min Ki ten Kate Herman G. Sprenger Jan van der Meer
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
Advances in the clinical recognition and radiographic
 Urgent Clinical Challenges in Children With Ischemic Stroke Analysis of 1065 Patients From the 1-800-NOCLOTS Pediatric Stroke Telephone Consultation Service Stefan Kuhle, MD; Lesley Mitchell, MSc; Maureen
Urgent Clinical Challenges in Children With Ischemic Stroke Analysis of 1065 Patients From the 1-800-NOCLOTS Pediatric Stroke Telephone Consultation Service Stefan Kuhle, MD; Lesley Mitchell, MSc; Maureen
Pediatric Neurointervention: Vein of Galen Malformations
 Pediatric Neurointervention: Vein of Galen Malformations Johanna T. Fifi, M.D. Assistant Professor of Neurology, Neurosurgery, and Radiology Icahn School of Medicine at Mount Sinai November 9 th, 2014
Pediatric Neurointervention: Vein of Galen Malformations Johanna T. Fifi, M.D. Assistant Professor of Neurology, Neurosurgery, and Radiology Icahn School of Medicine at Mount Sinai November 9 th, 2014
Talking About The Facts: Stroke In Children
 Talking About The Facts: Stroke In Children AWARENESS LEADS TO A QUICKER RESPONSE AND LIFESAVING OUTCOMES FOR CHILDREN. Pediatric Stroke Warriors continues to strengthen communities by providing support
Talking About The Facts: Stroke In Children AWARENESS LEADS TO A QUICKER RESPONSE AND LIFESAVING OUTCOMES FOR CHILDREN. Pediatric Stroke Warriors continues to strengthen communities by providing support
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
NIH Public Access Author Manuscript Pediatr Neurol. Author manuscript; available in PMC 2009 October 30.
 NIH Public Access Author Manuscript Published in final edited form as: Pediatr Neurol. 2008 May ; 38(5): 329 334. doi:10.1016/j.pediatrneurol.2007.12.012. Very Early Arterial Ischemic Stroke in Premature
NIH Public Access Author Manuscript Published in final edited form as: Pediatr Neurol. 2008 May ; 38(5): 329 334. doi:10.1016/j.pediatrneurol.2007.12.012. Very Early Arterial Ischemic Stroke in Premature
Outline. Calgary Pediatric Stroke Program. Parent Information and Networking Session
 Calgary Pediatric Stroke Program Parent Information and Networking Session Perinatal Stroke Adam Kirton MD MSc FRCPC Pediatric Neurologist Alberta Children s Hospital Sonia Rothenmund RN, BN, CNN(C) Pediatric
Calgary Pediatric Stroke Program Parent Information and Networking Session Perinatal Stroke Adam Kirton MD MSc FRCPC Pediatric Neurologist Alberta Children s Hospital Sonia Rothenmund RN, BN, CNN(C) Pediatric
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Emergently? Michigan Institute for Neurological Disorders. Garden City Hospital, Garden City, Michigan
 Why Should TIA be Treated Emergently? Anne M. Pawlak, D.O. F.A.C.N. Michigan Institute for Neurological Disorders Director Neurology Residency Program, Garden City Hospital, Garden City, Michigan According
Why Should TIA be Treated Emergently? Anne M. Pawlak, D.O. F.A.C.N. Michigan Institute for Neurological Disorders Director Neurology Residency Program, Garden City Hospital, Garden City, Michigan According
Cryptogenic Strokes: Evaluation and Management
 Cryptogenic Strokes: Evaluation and Management 77 yo man with hypertension and hyperlipidemia developed onset of left hemiparesis and right gaze preference, last seen normal at 10:00 AM Brought to ZSFG
Cryptogenic Strokes: Evaluation and Management 77 yo man with hypertension and hyperlipidemia developed onset of left hemiparesis and right gaze preference, last seen normal at 10:00 AM Brought to ZSFG
Anaesthesiologic management of a parturient with a known antiphospholipid syndrome
 Anaesthesiologic management of a parturient with a known antiphospholipid syndrome Pascal Vuilleumier Universitätsklinik für Anästhesie und Schmerztherapie Case presentation: Mrs A. B. 1975 Early monday
Anaesthesiologic management of a parturient with a known antiphospholipid syndrome Pascal Vuilleumier Universitätsklinik für Anästhesie und Schmerztherapie Case presentation: Mrs A. B. 1975 Early monday
Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease
 Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Cronicon OPEN ACCESS EC NEUROLOGY Research Article Clinical Features and Subtypes of Ischemic Stroke Associated with Peripheral Arterial Disease Jin Ok Kim, Hyung-IL Kim, Jae Guk Kim, Hanna Choi, Sung-Yeon
Cerebrovascular Disease
 Neuropathology lecture series Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O 2 consumption (resting):
Neuropathology lecture series Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O 2 consumption (resting):
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
AVC chez les jeunes causes et devenir
 AVC chez les jeunes causes et devenir Barbara Goeggel Simonetti Chef de clinique groupe de recherche neurovasculaire Neurologie Hôpital de l Ile et Université de Berne Médecin adjoint en neuropédiatrie,
AVC chez les jeunes causes et devenir Barbara Goeggel Simonetti Chef de clinique groupe de recherche neurovasculaire Neurologie Hôpital de l Ile et Université de Berne Médecin adjoint en neuropédiatrie,
ACUTE CENTRAL PERIFERALEMBOLISM
 EAE TEACHING COURSE 2010 Belgrade, Serbia October 22-23, 2010 ACUTE CENTRAL and PERIFERALEMBOLISM Maria João Andrade Lisbon, PT BACKGROUND Stroke is a leading cause of mortality and long-term disability
EAE TEACHING COURSE 2010 Belgrade, Serbia October 22-23, 2010 ACUTE CENTRAL and PERIFERALEMBOLISM Maria João Andrade Lisbon, PT BACKGROUND Stroke is a leading cause of mortality and long-term disability
TIA triage in Not all that glitters is gold
 TIA triage in 2016 Not all that glitters is gold Disclosures No industry related disclosures Expert witness work Overview Definition Implications Guidelines, secondary prevention Implementation of guidelines
TIA triage in 2016 Not all that glitters is gold Disclosures No industry related disclosures Expert witness work Overview Definition Implications Guidelines, secondary prevention Implementation of guidelines
RESPECT Safety Findings
 CO-1 SCAI Town Hall Meeting Monday, October 31, 2016 Washington, DC RESPECT Safety Findings John D. Carroll, M.D., MSCAI Professor of Medicine Cardiology University of Colorado School of Medicine University
CO-1 SCAI Town Hall Meeting Monday, October 31, 2016 Washington, DC RESPECT Safety Findings John D. Carroll, M.D., MSCAI Professor of Medicine Cardiology University of Colorado School of Medicine University
Ischemic Stroke in Critically Ill Patients with Malignancy
 Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Neonatal cerebral sinovenous thrombosis: Two cases, two different gene polymorphisms and risk factors
 The Turkish Journal of Pediatrics 2017; 59: 71-75 DOI: 10.24953/turkjped.2017.01.012 Case Report Neonatal cerebral sinovenous thrombosis: Two cases, two different gene polymorphisms and risk factors Özden
The Turkish Journal of Pediatrics 2017; 59: 71-75 DOI: 10.24953/turkjped.2017.01.012 Case Report Neonatal cerebral sinovenous thrombosis: Two cases, two different gene polymorphisms and risk factors Özden
Pediatric Arterial Ischemic Stroke Mahendra Moharir, MD, MSc, FRACP; Gabrielle deveber, MD
 Review Article Address correspondence to Dr Mahendra Moharir, Division of Neurology, The Hospital for Sick Children, 555 University Avenue, Toronto, Ontario M5G 1X8, Canada, mahendranath.moharir@ sickkids.ca.
Review Article Address correspondence to Dr Mahendra Moharir, Division of Neurology, The Hospital for Sick Children, 555 University Avenue, Toronto, Ontario M5G 1X8, Canada, mahendranath.moharir@ sickkids.ca.
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Slide 1. Slide 2 Conflict of Interest Disclosure. Slide 3 Stroke Facts. The Treatment of Intracranial Stenosis. Disclosure
 Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Slide 1 The Treatment of Intracranial Stenosis Helmi Lutsep, MD Vice Chair and Dixon Term Professor, Department of Neurology, Oregon Health & Science University Chief of Neurology, VA Portland Health Care
Is Stroke Frequency Declining?
 Is Stroke Frequency Declining? Etiologic Factors Clinical, Anatomic, Technique-related, and Device-specific Samir Kapadia, MD Professor of Medicine Section head, Interventional Cardiology Director, Cardiac
Is Stroke Frequency Declining? Etiologic Factors Clinical, Anatomic, Technique-related, and Device-specific Samir Kapadia, MD Professor of Medicine Section head, Interventional Cardiology Director, Cardiac
DIFFERENT STROKES FOR DIFFERENT FOLKS!!
 DIFFERENT STROKES FOR DIFFERENT FOLKS!! Identifying Stroke Subtypes SWAROOP PAWAR M.D., MPH. Vascular Neurologist UMG Neuroscience Associates Greenville Health System None Disclosures Outline Stroke, TIA
DIFFERENT STROKES FOR DIFFERENT FOLKS!! Identifying Stroke Subtypes SWAROOP PAWAR M.D., MPH. Vascular Neurologist UMG Neuroscience Associates Greenville Health System None Disclosures Outline Stroke, TIA
ORIGINAL CONTRIBUTION. Anticoagulation Therapy in Pediatric Patients With Sinovenous Thrombosis
 Anticoagulation Therapy in Pediatric Patients With Sinovenous Thrombosis A Cohort Study ORIGINAL CONTRIBUTION Gabrielle deveber, MD; Anthony Chan, MBBS; Paul Monagle, MBBS; Velma Marzinotto, BScN; Derek
Anticoagulation Therapy in Pediatric Patients With Sinovenous Thrombosis A Cohort Study ORIGINAL CONTRIBUTION Gabrielle deveber, MD; Anthony Chan, MBBS; Paul Monagle, MBBS; Velma Marzinotto, BScN; Derek
Stroke in children. Arterial ischaemic stroke. Perinatal stroke. THEME Stroke
 THEME Stroke Stroke in children BACKGROUND Stroke is a major cause of disability and death in children. It can have devastating consequences for families and enormous costs to society. Although considered
THEME Stroke Stroke in children BACKGROUND Stroke is a major cause of disability and death in children. It can have devastating consequences for families and enormous costs to society. Although considered
Cerebrovascular Disease
 Neuropathology lecture series Cerebrovascular Disease Kurenai Tanji, M.D., Ph.D. December 11, 2007 Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output:
Neuropathology lecture series Cerebrovascular Disease Kurenai Tanji, M.D., Ph.D. December 11, 2007 Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output:
Imaging of Perinatal Stroke
 Imaging of Perinatal Stroke Roxana S. Gunny, MBBS, MRCP, FRCR a,b, *, Doris Lin, MD, PhD c KEYWORDS Perinatal arterial ischemic stroke Presumed perinatal arterial ischemic stroke Cerebral sinovenous thrombosis
Imaging of Perinatal Stroke Roxana S. Gunny, MBBS, MRCP, FRCR a,b, *, Doris Lin, MD, PhD c KEYWORDS Perinatal arterial ischemic stroke Presumed perinatal arterial ischemic stroke Cerebral sinovenous thrombosis
AIDS with Acute Cerebral Infarct: A Case Report
 74 AIDS with Acute Cerebral Infarct: A Case Report Lin-Hui Wu 1, Wei-Hung Chen 1, Li-Ming Lien 1, Chien-Hsien Huang 2, and Hou-Chang Chiu 1 Abstract- A 38 year-old male presented with an acute onset of
74 AIDS with Acute Cerebral Infarct: A Case Report Lin-Hui Wu 1, Wei-Hung Chen 1, Li-Ming Lien 1, Chien-Hsien Huang 2, and Hou-Chang Chiu 1 Abstract- A 38 year-old male presented with an acute onset of
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
The Epidemiology of Stroke and Vascular Risk Factors in Cognitive Aging
 The Epidemiology of Stroke and Vascular Risk Factors in Cognitive Aging REBECCA F. GOTTESMAN, MD PHD ASSOCIATE PROFESSOR OF NEUROLOGY AND EPIDEMIOLOGY JOHNS HOPKINS UNIVERSITY OCTOBER 20, 2014 Outline
The Epidemiology of Stroke and Vascular Risk Factors in Cognitive Aging REBECCA F. GOTTESMAN, MD PHD ASSOCIATE PROFESSOR OF NEUROLOGY AND EPIDEMIOLOGY JOHNS HOPKINS UNIVERSITY OCTOBER 20, 2014 Outline
Sindrome da anticorpi antifosfolipidi: clinica e terapia. Vittorio Pengo Clinical Cardiology, Padova, Italy
 Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Sindrome da anticorpi antifosfolipidi: clinica e terapia Vittorio Pengo Clinical Cardiology, Padova, Italy Revised Classification Criteria for the Antiphospholipid Syndrome J Thromb Haemost 2006;4:295-306
Lecture Outline: 1/5/14
 John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
Hypoxic ischemic brain injury in neonates - early MR imaging findings
 Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
Hypoxic ischemic brain injury in neonates - early MR imaging findings Poster No.: C-1208 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit E.-M. Heursen, R. Reina Cubero, T. Guijo Hernandez,
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Clinical Study Circle of Willis Variants: Fetal PCA
 Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK?
 VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
VENOUS THROMBOEMBOLISM AND CORONARY ARTERY DISEASE: IS THERE A LINK? Ayman El-Menyar (1), MD, Hassan Al-Thani (2),MD (1)Clinical Research Consultant, (2) Head of Vascular Surgery, Hamad General Hospital
Perinatal arterial ischemic stroke (PAS) is defined as a
 Factor V Leiden and Antiphospholipid Antibodies in Either Mothers or Infants Increase the Risk for Perinatal Arterial Ischemic Stroke Michal J. Simchen, MD; Gal Goldstein, MD; Aaron Lubetsky, MD; Tzipi
Factor V Leiden and Antiphospholipid Antibodies in Either Mothers or Infants Increase the Risk for Perinatal Arterial Ischemic Stroke Michal J. Simchen, MD; Gal Goldstein, MD; Aaron Lubetsky, MD; Tzipi
Brain Attack. Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship. Case Medical Center
 Brain Attack Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship Stroke is a common and devastating disorder Third leading antecedent of death in American men, and second among
Brain Attack Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship Stroke is a common and devastating disorder Third leading antecedent of death in American men, and second among
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
DOWNLOAD OR READ : PERINATAL EVENTS AND BRAIN DAMAGE IN SURVIVING CHILDREN BASED ON PAPERS PRESENTED AT AN INTERNATIONA PDF EBOOK EPUB MOBI Page 1 Page 2 perinatal events and brain damage in surviving
TIA: Updates and Management 2008
 TIA: Updates and Management 2008 S. Andrew Josephson, MD Department of Neurology, Neurovascular Division University of California San Francisco Commonly Held TIA Misconceptions TIA is easy to diagnose
TIA: Updates and Management 2008 S. Andrew Josephson, MD Department of Neurology, Neurovascular Division University of California San Francisco Commonly Held TIA Misconceptions TIA is easy to diagnose
What is the appropriate evaluation of cryptogenic stroke, and when is a hypercoagulability work-up needed? David E. Thaler, MD, PhD, FAHA
 What is the appropriate evaluation of cryptogenic stroke, and when is a hypercoagulability work-up needed? David E. Thaler, MD, PhD, FAHA Neurologist in Chief, Tufts Medical Center Professor and Chair
What is the appropriate evaluation of cryptogenic stroke, and when is a hypercoagulability work-up needed? David E. Thaler, MD, PhD, FAHA Neurologist in Chief, Tufts Medical Center Professor and Chair
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
DWI assessment of ischemic changes in the fetal brain
 DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
DWI assessment of ischemic changes in the fetal brain Dafi Bergman, 4 th year Medical student in the 4-year program, Sackler school of medicine B.Sc Life and Medical Sciences, Tel Aviv University Supervised
Stroke in Children: How often does that happen?
 What s New in Pediatric Stroke? Advances in Pediatric Stroke Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Stroke & Cerebrovascular Disease Center Epidemiology:
What s New in Pediatric Stroke? Advances in Pediatric Stroke Heather J. Fullerton, MD, MAS Professor of Neurology & Pediatrics Director, Pediatric Stroke & Cerebrovascular Disease Center Epidemiology:
THROMBOPHILIA SCREENING
 THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
THROMBOPHILIA SCREENING Introduction The regulation of haemostasis Normally, when a clot occurs, it exactly occurs where it has to be and does not grow more than necessary due to the action of the haemostasis
Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset
 CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
CLINICAL ARTICLE Longitudinal anterior-to-posterior shift of collateral channels in patients with moyamoya disease: an implication for its hemorrhagic onset Shusuke Yamamoto, MD, Satoshi Hori, MD, PhD,
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
Advances in the treatment of posterior cerebral circulation symptomatic disease
 Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Advances in the treatment of posterior cerebral circulation symptomatic disease Athanasios D. Giannoukas MD, MSc(Lond.), PhD(Lond.), FEBVS Professor of Vascular Surgery Faculty of Medicine, School of Health
Canadian Best Practice Recommendations for Stroke Care. (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management
 Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Canadian Best Practice Recommendations for Stroke Care (Updated 2008) Section # 3 Section # 3 Hyperacute Stroke Management Reorganization of Recommendations 2008 2006 RECOMMENDATIONS: 2008 RECOMMENDATIONS:
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
How to Evaluate Patients with Cryptogenic Stroke
 How to Evaluate Patients with Cryptogenic Stroke Jeffrey Saver, MD Professor of Neurology Director, How to Evaluate Patients with Cryptogenic Stroke Disclosure Scientific Consultant, Unpaid Trialist: AGA
How to Evaluate Patients with Cryptogenic Stroke Jeffrey Saver, MD Professor of Neurology Director, How to Evaluate Patients with Cryptogenic Stroke Disclosure Scientific Consultant, Unpaid Trialist: AGA
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Laboratory Evaluation of Venous Thrombosis Risk
 Laboratory Evaluation of Venous Thrombosis Risk Dorothy M. Adcock, MD Volume 17, Number 12 December 2003 Objective: The reader will be able to discuss the concepts of risk factor, risk potential and thrombotic
Laboratory Evaluation of Venous Thrombosis Risk Dorothy M. Adcock, MD Volume 17, Number 12 December 2003 Objective: The reader will be able to discuss the concepts of risk factor, risk potential and thrombotic
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
PFO Management update
 PFO Management update May 12, 2017 Peter Casterella, MD Swedish Heart and Vascular 1 PFO Update 2017: Objectives Review recently released late outcomes of RESPECT trial and subsequent FDA approval of PFO
PFO Management update May 12, 2017 Peter Casterella, MD Swedish Heart and Vascular 1 PFO Update 2017: Objectives Review recently released late outcomes of RESPECT trial and subsequent FDA approval of PFO
Critical Review Form Therapy
 Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Critical Review Form Therapy A transient ischaemic attack clinic with round-the-clock access (SOS-TIA): feasibility and effects, Lancet-Neurology 2007; 6: 953-960 Objectives: To evaluate the effect of
Supplemental Figures and Legends
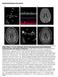 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Perlman J, Clinics Perinatol 2006; 33: Underlying causal pathways. Antenatal Intrapartum Postpartum. Acute near total asphyxia
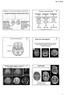 Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Perlman J, Clinics Perinatol 2006; 33:335-353 Underlying causal pathways Antenatal Intrapartum Postpartum Acute injury Subacute injury Associated problem Reduced fetal movements Placental insufficiency
Epidemiology and etiology of pediatric stroke
 Galley Proof 7/04/2010; 13:22 File: jpn402.tex; BOKCTP/llx p. 1 Journal of Pediatric Neurology 8 (2010) 1 5 1 DOI 10.3233/JPN-2010-0402 IOS Press Epidemiology and etiology of pediatric stroke Burkhard
Galley Proof 7/04/2010; 13:22 File: jpn402.tex; BOKCTP/llx p. 1 Journal of Pediatric Neurology 8 (2010) 1 5 1 DOI 10.3233/JPN-2010-0402 IOS Press Epidemiology and etiology of pediatric stroke Burkhard
Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO) Closure. April Reference: NHSCB/A09/PS/a
 Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO) Closure April 2013 Reference: NHSCB/A09/PS/a NHS Commissioning Board Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO)
Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO) Closure April 2013 Reference: NHSCB/A09/PS/a NHS Commissioning Board Clinical Commissioning Policy Statement: Patent Foramen Ovale (PFO)
