JAPM CONTENTS. Journal of Anesthesia and Perioperative Medicine. Original Articles. Review Articles. Opinions
|
|
|
- Roy Rice
- 5 years ago
- Views:
Transcription
1 JAPM EDITORS-IN-CHIEF Tian-Long Wang, Xuan Wu Hospital of Capital Medical University, Jin Liu, West Hospital of Sichuan University, ASSOCIATE EDITORS-IN-CHIEF Fu-Shan Xue, Plastic Surgery Hospital, Chinese Academy of Medical Sciences and Peking Union Medical College, Li- Ze Xiong, Xijing Hospital, the Fourth Military Medical University, Qu-Lian Guo, Xiangya Hosptial, Central South University, Wei- Feng Yu, Eastern Hepatobiliary Surgery Hospital, the Second Military Medical University, Zhi-Yi Zuo, University of Virginia, USA MANAGING EDITOR An-Huai Yu, JAPM Editorial Office, EDITORIAL BOARD Adrian W Gelb, University of California San Francisco, USA Carl Lynch III, University of Virginia Health System, USA Chingmuh Lee, University of California, USA Christer H Svensen, Karolinska Institutet, Sweden Donald S. Prough, University of Texas Medical Branch, USA Dong-Xin Wang, Peking University First Hospital, Guo-Lin Wang, Tianjin Medical University General Hospital, Hai-Chen Chu, the Affiliated Hospital of Medical College, Qingdao University, Hai-Long Dong, Xijing Hospital, the Fourth Military Medical University, Hong Ma, the First Hospital of Medical University, Huang-Ping Yu, Chang Gung Memorial Hospital, Taiwan, Jeffrey Huang, Anesthesiologists of Greater Orlando, Sheridan Healthcare, USA Jian-Jun Yang, Jinling Hospital, Jian-Zhong Sun, Thomas Jefferson University, USA Jing Zhao, Peking Union Medical College Hospital, John H. Zhang, Loma Linda University, USA Jun Ma, Beijing Anzhen Hospital, Capital Medical University, Jun-Li Cao, Xuzhou Medical College, Jun-Ming Zhang, University of Cincinnati College of Medicine, USA Keith Candiotti, University of Miami, USA Ke-Xuan Liu, the First Affiliated Hospital, Sun Yat-Sen University, Ki Hyuk Hong, Department of Anesthesiology and Pain Medicine, Inje University College of Medicine, Korea Ling Wei, Emory University School of Medicine, USA Michael G. Irwin, the University of Hong Kong, Hongkong, Min Yan, the Second Affiliated Hospital, Medicine School of Zhejiang University, Muksudul Alam ABM, Shaheed Suhrawardy Medical College & Hospital, Bangladesh Niccolò Terrando, Karolinska Institutet, Sweden Robert Whittington, Columbia University, USA Roewer Norbert, University Hospital of Wuerzburg, Germany Ru-Rong Wang, West Hospital of Sichuan University, Su Min, the First Affiliated Hospital of Chongqing Medical University, Ting-Hua Wang, Sichuan University,, Massachusetts General Hospital, Harvard Medical School, USA Wei Xiao, Xuan Wu Hospital of Capital Medical University, Wei-Dong Mi, Chinese PLA General Hospital, Wen-Jinn Liaw, Tungs Taichung MetroHarbor Hospital, Taiwan, Wen-Zhi Li, the Second Affiliated Hospital of Harbin Medical University, Xavier Paqueron, Clinical Centre in Angoulême, France Xiang-Ming Fang, Zhejiang University, Xiao- Ming Deng, Changhai Hospital, the Second Military Medical University, Xue-Yin Shi, Changzheng Hospital, the Second Military Medical University, Ying-Wei Wang, Xinhua Hospital, Shanghai Jiaotong University School of Medicine, Yu-Guang Huang, Peking Union Medical College Hospital, Yuan-Xiang Tao, Rutgers, the State University of New Jersey, New Jersey Medical School, USA Yun Yue, Beijing Chaoyang Hospital, Capital Medical University, Zhang-Sheng Yu, Indiana University School of Medicine, USA Zheng Guo, Shanxi Medical University, Zheng-Liang Ma, Drum Tower Hospital, Medical School of Nanjing University, Zhongcong Xie, Massachusetts General Hospital and Harvard Medical School, USA Zhong-Yuan Xia, Renmin Hospital of Wuhan University, Zi-Qing Hei, the Third Affiliated Hospital of Sun Yat-sen University, November, 2014 Volume 1 Issue 2 CONTENTS Original Articles 63 Diagnostic and Therapeutic Strategies for Hypercarbia in Elderly Patients Undergoing Prolonged Retroperitoneoscopic Surgery The Role of TcPCO 2 and PEEP Cui-Cui Kong, Wei Xiao, Guo-Xun Xu, Ting Yang, and Tian-Long Wang 72 Prevalence and Risk Factors of Postoperative Residual Curarization in Patients Arriving at Postanesthesia Care Unit after General Anesthesia: A Prospective Cohort Study Min Xie, Dong-Xin Wang, and Zhi-Yu Geng 79 Activation of Spinal EphrinBs/EphBs Contributes to Morphine Dependence and Tolerance He Liu, Di-Yang Ling, Yan Yuan, Xue-Hai Guan, Jia-Ping Ruan, Hong-Xing Zhang, Hai-Lei Ding, and Jun-Li Cao 90 Melanocortin 4 Receptor Is Involved in the Development of Morphine Tolerance Hong-Mei Xu, Ze-Jun Niu, Hai-Chen Chu, and Xue-Feng Zhang Review Articles 97 The Role of Inflammation in Postoperative Cognitive Dysfunction Guo-Xun Xu, Ting Yang, and Niccolò Terrando 104 Inflammation and Heart Diseases: Role of Toll-Like Receptor Signaling Opinions 118 Anesthesia, Surgery and Neuroinflammation Krzysztof Laudanski, and Roderic G. Eckenhoff 122 Surgery, Neuroinflammation and Long-Term Outcome Monty Lyman, and Da-Qing Ma PUBLISHER Evidence Based Communications (EBC), Hong Kong,
2 Review Article Inflammation and Heart Diseases: Role of Toll-Like Receptor Signaling ABSTRACT From the Department of Anesthesia, Critical Care and Pain Medicine, Massachusetts General Hospital, Harvard Medical School, Boston, USA. Correspondence to Dr. at Citation:. Inflammation and heart diseases: role of toll- like receptor signaling. J Anesth Perioper Med 2014; 1: Aim of review: Heart diseases such as septic cardiomyopathy, ischemic myocardial injury and acute myocarditis pose significant perioperative risk to surgical patients and present challenges to anesthesiologists. Myocardial inflammation is a common theme of these diseases and plays an important role in their pathogeneses. Toll- like receptors (TLRs) are an important part of the innate immune system. The aim of this article is to provide a brief review on the major landmark studies of TLRs and their signaling, the complex and critical role of TLRs in severe sepsis, ischemic myocardial injury, and myocarditis. The article intends to cover animal studies defining the molecular mechanisms by which TLR signaling contributes to the pathogenesis of these heart diseases as well as the recent clinical trials targeting TLR for sepsis intervention. Method: Literatures were searched via PubMed with the key words TLRs, sepsis, myocardial ischemia, and myocarditis. A few previously published review articles in the relevant fields were referenced. Recent findings: TLRs detect invading pathogens through the pathogen- associated molecular pattern (PAMP) recognition and play an essential role in the host defense. TLRs can also sense endogenous molecules with the danger-associated molecular pattern (DAMP), such as heat shock proteins (HSPs), high mobility group 1 (HMGB- 1) and extracellular RNA, which are produced under various injurious conditions. Studies in the past decade have clearly established the critical role of TLR signaling in mediating cardiac inflammation in the context of severe sepsis, myocardial ischemia- reperfusion injury and acute myocarditis. A variety of microbial and non- microbial TLR ligands have been identified under these critical conditions. These ligands act through TLRs and elicit potent biochemical and inflammatory responses. By mediating the complex cardiac as well as systemic inflammation, either beneficial or deleterious in nature, TLRs play a pivotal role in the development of these cardiac diseases. Recent TLR4 antagonist (eritoran) Phase I-III clinical trials represent the latest effort targeting TLR signaling for sepsis therapeutics. Summary: Studies of the past decade have firmly established the role of TLR signaling in cardiac inflammation and dysfunction during severe sepsis, ischemic myocardial injury, and acute myocarditis. Understanding the complex cellular and molecular pathways by which TLR signaling controls myocardial inflammation and injury provides insight into the mechanisms of these cardiac diseases and will impact on how we diagnose and treat these critical conditions in the future. 104 This is an open-access article, published by Evidence Based Communications (EBC). This work is licensed under the Creative Commons Attribution 4.0 International License, which permits unrestricted use, distribution, and reproduction in any medium or format for any lawful purpose.to view a copy of this license, visit
3 Heart Inflammation and TLR Signaling M yocardial inflammation is featured in several clinical conditions including septic cardiomyopathy, myocardial ischemia- reperfusion (I/R) injury, and myocarditis. Under these critical conditions, foreign pathogens (e.g., bacteria or virus) or endogenous danger molecules (e.g., heat shock proteins [HSPs] or RNA) released from injured tissues induce local and systemic innate immune responses that lead to myocardial inflammation. Such innate im - mune responses could be both detrimental and beneficial in nature. Toll- like receptors (TLRs) are a critical part of human innate immune system. TLRs recognize pathogens via pathogen- associated molecular pattern (PAMP) (1) and endogenous danger molecules via danger- associated molecular pattern (DAMP) (2). This article reviews animal and human studies that demonstrate the role of TLR signaling in myocardial inflammation involved in the aforementioned cardiac conditions. TLRs also contribute to the development of inflammation in atherosclerosis that leads to myocardial ischemic injury and acute coronary syndromes. These studies have been reviewed elsewhere (3). Toll-Like Receptors Discovery of Toll and TLR Toll, meaning "amazing" and "wonderful" in German, was first described by Christian Nusslein- Volhard and colleagues in 1985 when they found that Toll gene was critical for the embryonic development of the fruit flies Drosophila. Together with Edward Lewis and Eric Wieschaus, she received Nobel Prize in Physiology or Medicine in 1995 for their discoveries concerning "genetic control of early embryonic development". A decade later, Hoffmann and colleagues (4) found that Toll was also essential to the host innate im - munity against fungal infection. In 1997, a group of investigators led by Medzhitov and Janeway at Yale University (5) discovered that a human homolog of the Drosophila Toll protein was a transmembrane protein with an extracellular domain consisting of a leucine- rich repeat and cytoplasmic domain homologous to the cytoplasmic domain of human IL- 1 receptor. Expression of a constitutively active form of human Toll or Tolllike protein activated nuclear factor kappa B (NFκB) pathway. Subsequently, several groups identified that mice with mutated Tlr4 gene, either a missense point mutation (Pro His, C3H/HeJ strain) or null mutation (C57 BL/10 ScCr strain), conferred a natural hyporesponsiveness to endotoxin (6, 7). Targeted gene disruption led to TLR4- deficient mice (TLR4 -/- ) resistant to lipopolysaccharide (LPS) (8). These early investigations established TLR4 as the receptor for LPS or endotoxin. Signal Transduction Pathways TLRs are single- spanning membrane glycoproteins with a leucine- rich repeat of extracellular domains and an intracellular toll/interleukin-1 receptor (TIR) domain. As summarized in table 1, TLRs consist of a family of receptors that specifically bind to a wide range of pathogens including bacteria, fungi, parasites, and viruses through "PAMP" recognition (1, 9). Accumulating evidence has indicated that TLRs can also act as a stress sensor in response to non- infectious tissue injury and recognize a variety of endogenous danger molecules through "DAMP" recognition (2). TLR1, TLR2, TLR4, TLR5, and TLR6 are located primarily on the plasma membrane and recognize mainly microbial components such as lipids, lipoproteins, and proteins, whereas TLR3, TLR7/ 8, and TLR9 reside on the membranes of intracellular compartments, such as endosomes, and are responsible for the recognition of microbial nucleic acids such as double-stranded RNA (TLR3), single- stranded RNA (TLR7/8), and DNA (TLR9) (9, 48) (Figure 1). The mrna expression of the 10 TLRs has been detected in human heart (49), but not yet at the protein level. Upon activation, TLRs form dimers and initiate the downstream signaling (Figure 1). Heterodimerization occurs between TLR2 and TLR1 or TLR6, and between TLR4 and myeloid differentiation factor 2 (MD- 2), whereas the other TLRs form homodimers. The resulting TIR- TIR com - plexes trigger the downstream signaling through a set of 5 specific adaptors (50), i.e., myeloid differentiation factor 88 (MyD88), TIR domain- containing adaptor protein (TIRAP), TIR domaincontaining adaptor inducing IFN-β-mediated transcription factor (Trif), Trif- related adaptor molecule (TRAM), and sterile α- and heat- armadillomotif- containing protein (SARM). Depending on 105
4 Review Article Table 1. TLR Ligands: PAMP versus DAMP*. TLRs TLR2 TLR3 TLR4 TLR5 TLR7 TLR8 TLR9 TLR11 PAMP Lipopeptides Peptidoglycan Lipoteichoic acid LPS Lipoarabinomannan Zymosan Glycosyl phosphatidyl inositol anchors Hemaglutinin protein Double-stranded RNA Poly (I:C) Small interfering RNAs LPS Flagellin Single-stranded RNA Imidazoquinoline compounds Guanine analogs Single-stranded RNA Unmethylated CpG DNA motif Profilin-like molecule Pathogens Bacteria Gram+bacteria Gram+bacteria Leptospira interrogans Mycobacteria Fungi Trypanosoma Measles virus Virus Gram- bacteria Bacteria Flagella Virus Virus Bacteria, virus Toxoplasma gondii Uropathogenic bacteria *Used with permission from Feng and Chao (47). References , , DAMP HSP60 HSP70 Gp96 HMGB1 Bioglycan Versican Hyaluronan fragments mrna HSP60, HSP70, HSP72, HSP22 HMGB1 Fibronectin, Biglycan, Tenascin-C, Versican Hyaluronan, Lower molecular weight HA, Heparin sulfate ssrna ssrna Chromatin-IgG complex References 11 13, , 16, the adaptors recruited, TLR signaling can be divided into two distinct pathways: MyD88-dependent and Trif-dependent pathways. MyD88- dependent pathway is activated by all TLRs with exception of TLR3. MyD88 signaling leads to inflammatory cytokine production by activating the transcription factor NF-κB and mitogen-activated protein kinases (MAPKs) such as c- Jun N- terminal kinase (JNK) and p38. MyD88 recruits IL- 1 receptor- associated kinase (IRAKs). The IRAK1- TNF receptor- associated factor 6 (TRAF6) complex then activates transforming growth factor- a activated kinase 1 (TAK1) through a process involving cytosol translocation of TAK1 and two regulatory components TAK binding protein 2 (TAB2) and TAB3 and the ubiquitination of TRAF6. Activated TAK1 then phosphorylates I- κb kinase beta (IKKβ), leading to phosphorylation and degradation of I- κb, which releases the NF- κb p50/p65 subunits and results in the nuclear translocation and DNA binding of NF-κB (9). Trif- dependent pathway is utilized by TLR3 and TLR4. It induces type I interferon (IFN) and inflammatory cytokines through activation of the transcription factor interferon regulatory factor 3 (IRF3) and NF-κB. Trif associates with TRAF3 and TRAF6. TRAF3 links a signaling complex involving the noncanonical IKKs, TRAF family member-associated NF-κB activator (TANK) binding kinase- 1 (TBK1) and IKKi, which catalyzes phosphorylation of IRF3/7 and induces its nuclear translocation and IFN- β expression. Moreover, Trif also recruits TRAF6 and receptor-interacting protein 1, with the help of TAK1, leading to the activation of NF- κb and MAPKs through ubiquitination- dependent mechanism similar to MyD88-dependent pathway (9, 48). TLRs in Septic Cardiomyopathy Sepsis is defined as the systemic inflammatory re- 106
5 Heart Inflammation and TLR Signaling Figure 1. Toll-Like Receptors: Ligands and Signaling Pathways. All TLRs are transmembrane proteins. Some TLRs such as TLR1, TLR2, 4, TLR5 and TLR6 are expressed on the cell surface whereas others such as TLR3, TLR7/8, and TLR9 are located almost exclusively in intra-cellular com partments such as endosomes. Different TLRs recognize different microbial components (Table 1). For example, TLR2 recognizes the PAMPs lipopeptides or peptidoglycan, a wall component of Gram-positive (G+) bacteria, e.g., Staphylococcus aureus or Streptococcus pneumoniate. It also recognizes DAMPs such as HSPs and high mobility group 1 (HMGB- 1) protein. TLR2 heterodimerizes either with TLR1 to recognize triacylated lipopeptide or with TLR6 to recognize diacylated lipopeptides. TLR4 senses LPS or endotoxin, a wall component of Gram- negative (G-) bacteria such as Escherichia coli. TLR5 senses bacterial flagellin, a protein component of flagella. TLR3 recognizes viral double- stranded RNA (dsrna), whereas TLR7 and 8 are the sensors for single stranded RNA (ssrna). Finally, TLR9 senses bacterial CpG- rich hypomethylated DNA (CpG DNA) motifs. Upon respective ligands binding, TLRs form homo- or heterodimers and recruit one or more adaptor proteins, namely, MyD88, MAL/TIRAP, TRIF, or TRAM, to the cytoplasmic domains of the receptors through interactions between Toll/IL- 1 receptor (TIR) domains present in each receptor and each adaptor. All TLRs with exception of TLR3 use the common MyD88-dependent pathway. Mal acts as a bridge to recruit MyD88 to TLR2 and TLR4 signaling, whereas TRIF is used in TLR3 signaling and, in association with TRAM, in TLR4 signaling. In MyD88- dependent pathway, MyD88 associates with IRAK4 and IRAK1. IRAK4 in turn phosphorylates IRAK1 and promotes their association with TRAF6, which serves as a platform to recruit and activate the kinase TAK1. Activated TAK1 activates the IKK complex, com posed of IKKα, IKKβ, and NEMO (IKKγ), which in turn catalyze phosphorylation and subsequent degradation of IκB. I-κB degradation lets NF-κB (i.e., p50/p65) free to translocate from the cytoplasm to the nucleus where it activates multiple inflammatory cytokine gene expression. The transcription factor IRF7 is activated as the downstream signaling molecule of TLR 7/8 and TLR9. It is directly phosphorylated by IRAK1 and then translocates into the nucleus to induce the expression of type I IFN-α and IFN-inducible genes. In the Trif-dependent pathway, Trif interacts with TRAF3 to activate TBK1 and IKK-i, resulting in the activation of IRF3/7 which then translocate into the nucleus to activate the transcription of IFN-β and IFN-inducible genes. sponse syndrome that occurs during infection. It has an estimated prevalence of 751,000 cases JAPM each year in the United States (51). Sepsis is the 10th leading cause of death in the U.S. (52) with November, 2014 Volume 1 Issue 2 107
6 Review Article a mortality of 28.6%. The hospital mortality of severe sepsis in the U.S. was 27% in 2007, down from 39% in 2000 (53), whereas in, the mortality rate of severe sepsis in 10 teaching hospitals was 49% in 2007 (54). Cardiovascular collapse induced by cardiac dysfunction and profound vasodilatation represents a main feature of septic shock and contributes to its high mortality (55). TLRs play a pivotal role in the host innate immune defense and facilitate the adaptive immunity against foreign pathogens. However, as detailed below, inappropriate innate immune response via multiple TLRs may also contribute to the pathogenesis of sepsis. Several TLRs including TLR2, TLR3, TLR4, TLR5, and TLR9 are reportedly involved in the development of septic cardiomyopathy and mortality in animal models (Table 2). Animal models such as cecum ligation and puncture (CLP) closely resemble the clinical scenario of sepsis such as bowel perforation and have been widely used in sepsis research (56). TLR2 Several lines of evidence support the notion that TLR2 signaling contributes to bacteria- induced cardiac inflammation and dysfunction. In isolated hearts, S. aureus activates cardiac TLR2 signaling and induces marked cardiac inflammation and contractile dysfunction (57). In isolated adult cardiomyocytes, we have demonstrated that peptidoglycan- associated lipoprotein, a naturally occurring TLR2 ligand and a ubiquitous Gram- negative bacterial outer- membrane protein (76), induces cytokine production and inhibits cardiomyocyte function (58). In an animal model of bacterial sepsis, we have found that TLR2 -/- mice have better survival, markedly im - proved cardiac function, and depressed systemic and myocardial cytokine production (59) and markedly reduced intracellular reactive oxygen species (ROS) production (77) when compared to WT mice following CLP procedure. Finally, mitochondrial dysfunction is a key molecular event associated with organ injury in severe sepsis. Recent evidence has demonstrated that among several TLR ligands tested, TLR2/1 activation by Pam3cys is sufficient to induce both intracellular H 2O 2 and mitochondrial O 2 produc- - tion. The effect is specific for TLR2/1 as TLR3 or 9 ligands do not induce ROS production (78). Polymicrobial sepsis in mice induces mitochondrial dysfunction in leukocytes, as demonstrated by increased H 2O 2 and mitochondrial O 2 - production, attenuated complex III activity, loss of mitochondrial membrane potential (ΔΨm), and depletion of intracellular ATP. There is significant improvement in mitochondrial function in septic TLR2 -/- mice as evidenced by attenuated mitochondrial ROS production, better- maintained mitochondrial ΔΨm and higher cellular ATP production. The studies demonstrate that TLR2 signaling plays an important role in mediating mitochondrial dysfunction during polymicrobial sepsis (78). It remains unclear whether TLR2 mediates mitochondrial dysfunction in cardiomyocytes and whether mitochondrial dysfunction may contribute to myocardial dysfunction during sepsis. TLR3 TLR3 was originally identified as the receptor for double- stranded RNA of viral origin (27). Stimulation of TLR3-Trif signaling activates the transcriptional factors, NF- κb and IRF3/7, and subsequently results in the production of various cytokines such as type I IFN, which represents the major host anti-viral mechanism. In a nonviral bacterial sepsis model, however, systemic deletion of TLR3 confers a survival benefit, im - proved cardiac function, and reduced inflammatory cell infiltration (61). These data suggest that TLR3 plays a role in cardiac inflammation and dysfunction in bacterial sepsis. It is unclear what the ligands are responsible for TLR3 activation in the setting of bacterial sepsis. Both bacterial and host RNA are present in the circulation of septic mice and could potentially function as the agonists of TLR3 in sepsis. Interestingly, in a double hit model, treatment with the TLR3 ligand poly (I:C) of animals before CLP surgery enhances host immunity and improves the survival of septic animals (62). These results suggest a dynamic role for TLR3 in the pathogenesis of polymicrobial sepsis. TLR4 TLR4 has long been linked to endotoxin- induced cardiac dysfunction and inflammation. LPS administration in animals induces NF-κB ac- 108
7 Heart Inflammation and TLR Signaling Table 2. Role of TLRs in Endotoxin Shock and Septic Cardiac Dysfunction. TLRs Sepsis TLR2 S. aureus activates TLR2 signaling and induces cardiomyocyte dysfunction (57). Peptidoglycan-associated lipoprotein induces cytokine production and inhibits cardiomyocyte function via TLR2-MyD88 signaling in vitro (58). TLR2 -/- mice have reduced myocardial inflammation and leukocyte ROS production, improved cardiac function/leukocyte mitochondrial function, and better survival compared to WT mice in polymicrobial sepsis (59, 60). TLR3 TLR3 -/- mice have reduced inflammatory cell infiltration, improved cardiac function, and better survival (61). Pretreatment of animals with poly (I:C) enhances host immunity and improves survival of septic animals (62). TLR4 Endotoxin (LPS) induces cardiac dysfunction in vivo most likely through a hematopoietic TLR4- mediated mechanism (63-65). MyD88 and Trif, two adaptors of TLR4, play an important role in mediating endotoxin-induced cardiac dysfunction (66). Studies in tissue-specific MyD88 -/- suggest that both cardiac and myeloid MyD88 play a role in cardiac dysfunction in endotoxin shock (67). TLR4 deletion offers protection against lethal Gram- negative bacteria- induced inflammation and mortality (68), but offers no protection or even deleterious effect in a CLP model of polymicrobial sepsis (69, 70). TLR4 antagonist (eritoran) blocks inflammatory effects of LPS in animals (71) and in healthy volunteers (72). But in a Phase III clinical trial, eritoran fails to offer any survival benefit compared with placebo in patients with severe sepsis (73). TLR5 Bacterial flagellin induces myocardial inflammation and cardiac dysfunction (74). TLR9 Bacterial DNA and RNA inhibit cardiomyocyte function (75). tivation (79) that leads to robust myocardial cytokines expression, such as TNFα, IL-1β, and myocardial dysfunction (80, 81). This process is dependent of TLR4, CD14, IRAK- 1, MyD88, and Trif. The endotoxin- induced cardiac dysfunction may be an indirect effect secondary to immune cell activation. Cardiomyocytes isolated from LPS- treated mice exhibit reduced function, but in vitro treatment of cardiomyocytes with LPS fails to inhibit its function (63). Further studies in chimeric mice suggest that TLR4 in bone marrow- derived hematopoietic cells is responsible for cardiac dysfunction during endotoxic shock (63-65). However, others made an opposite observation (82). Of note, deletion of MyD88 or Trif, the two adaptors downstream of LPS- TLR4 signaling, appears to offer equal protection against myocardial inflammation, cardiac depression, and high mortality in endotoxemia (66). Most recently, using a Cre- flox system, we have generated tissue- specific MyD88 deletion models (67). In these studies, Cre recombinase transgenic mice with α- myosin heavy chain (α- MHC) or lysozyme M (Lyz) promoters were cross- bred with MyD88-loxP (MyD88 fl/fl ) mice, respectively, to generate cardiomyocyte- (α- MHC- MyD88 -/- ) or myeloid-specific (Lyz-MyD88 -/- ) MyD88 deletion models and their respective MyD88 fl/fl littermates. Using these models, we demonstrate that both cardiomyocyte- and myeloid- MyD88 play a role in mediating cardiac dysfunction and mortality induced by endotoxin shock. However, myeloid MyD88 signaling appears playing a predominant role in systemic and cardiac inflammation following endotoxin challenge (67). In animal models of polymicrobial sepsis, the role of TLR4 is more complex and may well depend on the types as well as the severity of bacterial infection. For example, while TLR4 deletion clearly confers a survival benefit in endotoxin shock (6) or lethal Gram- negative bacterial sepsis (68), it offers no survival benefit (69) or even deleterious effect (70) in CLP models of polymicrobial sepsis. These data suggest that host mobilizes different innate immune mechanisms in endotoxemia and polymicrobial septic peritonitis. Moreover, our previous studies indicate that MyD88, but not Trif, plays a predominant role in mediating cardiac dysfunction, marked systemic inflammation, and mortality in a lethal model of bacterial sepsis, whereas MyD88 and Trif are both critical for systemic inflammation, cardiac depression and mortality during endotoxin shock (66). Finally, different from severe and lethal sepsis, in a low-grade model of polymicrobial sepsis with low mortality (10-20% ) (70) or in a non-lethal model of Gram-negative bacterial sepsis (68), the lack of TLR4 is proven to be detrimental, demonstrating the essential role of TLR4 in preserving cardiac function and surviv- 109
8 Review Article al in bacterial sepsis. There are several possible mechanisms that may explain the deleterious im - pact of TLR4 deficiency on cardiac function in low- grade bacterial sepsis (70). First, TLR4 is critically involved in the effective host immune defense against bacterial invasion. WT mice exhibit more robust neutrophil migratory and phagocytic functions and markedly reduced bacterial loading compared with TLR4 def mice. It is speculated that as results of uncontrolled bacterial dissemination in the absence of TLR4, animals lacking TLR4 have more systemic cytokine production including IL- 6, a major cardiodepressant. Second, TLR4 signaling may play a cardiac "preconditioning-like" role during low-grade bacterial infection. Very small doses of LPS pretreatment confer a cardioprotective effect against hypoxic injury (83). It seems possible that a small amount of endotoxin released from bacterial peritonitis to the circulatory system in the early stage of the low-grade polymicrobial sepsis could activate TLR4 signaling and initiate a "preconditioning- like" cardiac protection against subsequent myocardial depression during sepsis. Supporting this hypothesis are the reports that administration of low dose of endotoxin offers protection against both subsequent endotoxin challenges and polymicrobial infection (84). TLR5 Bacterial flagellin, a TLR5 ligand, induces marked myocardial inflammation and contractile dysfunction (74). The flagellin-induced NF-κB activation is TLR5- dependent. In vivo administration of flagellin leads to myocardial NF-κB activation and expression of cytokines, increased myocardial neutrophil infiltration, and reversible cardiac dysfunction (74). TLR9 Bacterial DNA and RNA derived from S. aureus and E. coli induce a concentration-dependent depression of rat cardiomyocyte function (75). Pretreatment with DNase or RNase abrogates this effect. Similarly, in vivo administration of synthetic DNA (CpG- ODN) causes myocardial NF-κB activation and inflammatory cytokine production (TNFα, IL- 1β and IL- 6). In vitro, CpG- ODN inhibits sarcomere shortening of isolated mouse cardiomyocytes. Both the in vivo and in vitro effects of CpG are abolished in TLR9- deficient mice (85). It is unclear, however, whether or not host nucleotides released play a role in polymicrobial sepsis. Complements Like TLRs, the complements are a critical part of the innate immunity. While both systems have been well studied as separate components in the host defense, the interplay between the two components under the pathological conditions such as severe sepsis and their possibly intertwined role in sepsis- induced tissue injury and organ failure is poorly understood. There are three separate but convergent pathways of complement activation, i.e., 1) classic, 2) lectin, and 3) alternative pathway (AP). Complement factor B (cfb) is a necessary component of the AP. Targeted deletion of cfb leads to abrogation of the AP (86). Three groups of investigators including us have demonstrated an up- regulation of cfb expression in macrophages (87, 88) and cardiomyocytes (88, 89) by TLR activation. Moreover, the work from our lab suggests that cfb acts downstream of TLRs during sepsis and plays an important role in septic cardiomyopathy (88). Polymicrobial sepsis augments cfb levels in the serum and the heart. Sepsis also leads to the AP activation, C3 fragment deposition in the kidney and heart. Importantly, during sepsis, absence of cfb confers a protective effect with improved survival and cardiac function. However, the underlying mechanisms by which cfb contributes to septic cardiomyopathy is unknown and remains to be investigated (88). Targeting TLRs As a Potential Therapeutic There is a growing interest in the targeting of TLRs for the prevention and treatment of diseases such as cancer, rheumatoid arthritis, inflam - matory bowl disease and sepsis. Both TLR agonists (TLR7, TLR8, TLR9) and antagonists (TLR2, TLR4, TLR9) have been developed for different diseases and through different stages of clinical trials (90). One of the most notable clinical trials for sepsis is eritoran (E5564). Eritoran is a synthetic lipid A antagonist that blocks LPS from binding to MD2-TLR4 receptor, which reduces the inflammatory effects of LPS in human monocytes (91), in animals (71), and in healthy 110
9 Heart Inflammation and TLR Signaling volunteers (72). In a Phase II clinical trial, eritoran is well tolerated and decreases 28- day allcause mortality of severe sepsis by only 6.7%, a modest and statistically insignificant benefit (92). The subsequent Phase III clinical trial (NCT ) in 1,961 patients with severe sepsis reveals that use of eritoran offers no survival benefit compared with placebo (73). TLRs in Ischemic Myocardial Injury Innate immune response is by far the most com - mon cause of myocardial inflammation after I/R injury and is characterized by cytokine release, endothelial cell activation, complement deposition, inflammatory cell infiltration, and increased vascular permeability. Many of these inflammatory responses are mediated by specific signaling mechanisms (93). One of such signaling mechanisms is that mediated by TLRs. A large body of evidence indicates that TLR signaling plays dual role-- both beneficial and deleterious role in the event of I/R injury (94). For example, it is well documented that pretreatment with low dose LPS provides potent cardioprotection against I/R injury, a phenomenon called LPS preconditioning. In the absence of systemic TLR4 activation (by LPS), however, mice deficient for TLR4 or MyD88 exhibit reduced myocardial inflammation and smaller myocardial infarction (MI) compared to WT following I/R injury, indicating that TLR4 mediates myocardial inflammation and infarction following I/R (95-97). As summarized by Eckle and Eltzschig (98) and illustrated in figure 2 and table 3, activation of TLR4- MyD88 signaling confers potent dual effect-- promoting myocardial inflammation via NF- κb- dependent mechanisms and protecting cardiomyocytes against apoptosis (99). Of note, a similar dual effect has been previously reported for NF-κB (100). Myocardial lschemia Attenuated Apoptosis Apoptosis LPS TLR4 Myd88 NFκB Enhanced Inflammation Inflammation Figure 2. Dual Role of TLR Signaling in Myocardial I/R Injury. Pretreatment with LPS provides potent protection against subsequent myocardial ischemia, involving signal transduction through MyD88, and convergence on inos and guanylate cyclase (not shown) (101). As such, TLR4- dependent activation of NFκB could provide cardioprotection from ischemia by dampening programmed myocardial cell death (apoptosis) (99, 102). However, previous studies in knockout mice for TLR4 or MyD88 (95, 97, 103) demonstrate attenuated susceptibility to myocardial I/R injury. These later findings could reflect increases in myocardial inflammation during ischemia reperfusion injury (98, Used with permission). LPS Preconditioning against I/R Injury Evidence from several lines of investigation suggest that activation of systemic TLR4 by LPS protects myocardium against I/R injury (94). In animal models of I/R injury, both in vivo and in exvivo, prior systemic administration of sub- lethal dose of LPS reduces subsequent MI and im - proves cardiac functions. The cardioprotective effect of LPS usually occurs between hours a- fter administration of LPS and is abolished by cycloheximide, suggesting a mechanism involving de novo synthesis of cardioprotective proteins. LPS administration induces a robust induction of inos in the heart, a process mediated via TLR4. Employing genetic and pharmacological approaches, we demonstrate that TLR4- MyD88, but not TLR2 or Trif, mediates the LPS- induced preconditioning effect. Importantly, inos -/- mice or WT mice treated with the inos inhibitor 1400W fail to respond to TLR4- mediated NO production and are not protected by the LPS preconditioning. While sgcα 1 mice have normal -/- NO production in response to LPS, they are not 111
10 Review Article Table 3. Role of TLR Signaling in Myocardial I/R Injury. TLRs and adaptor Myocardial I/R injury TLR2 In an ex-vivo model, TLR2 -/- mice exhibit improved LV function compared with WT mice following I/R (104). In vivo, TLR2 -/- mice have reduced cardiac inflammation and smaller MI sizes compared to WT mice after I/R (105). TLR3 TLR3 -/- mice exhibit reduced myocardial infarct and improved function compared to WT mice after I/R (106, 107). TLR4 TLR4 may play a dual role in I/R injury: beneficial preconditioning effect and deleterious effect by mediating I/R injury (94). LPS preconditioning: a small dose of LPS administration offers a cardiac protection against I/R injury. The effect is mediated via TLR4, MyD88, inos, and sgcα1 (101). Myocardial I/R activates cardiac innate immune signaling via TLR4-MyD88 (108). TLR4 def (C57/BL10 ScCr) or mutated (C3H/HeJ) mice have significantly smaller MI sizes and attenuated myocardial inflammation (95, 96). Blocking TLR4 by eritoran leads to decreased MI sizes and attenuated myocardial inflammation (109). MyD88 MyD88 -/- mice have reduced MI sizes and improved LV function when compared to WT controls after I/R (110). MyD88 -/- mice also exhibit significantly reduced myocardial cytokines and neutrophil infiltration (103, 110). Studies employing chimeric MyD88 deletion models suggest that MyD88 signaling in circulating neutrophils plays a critical role in myocardial neutrophil infiltration and development of MI during I/R (103, 111). Trif Trif deletion leads to reduced MI sizes, but it has no impact on myocardial neutrophil recruitment and cytokine production following I/R (106). protected by TLR4- elicited cardiac protection (101). Together, these data suggest that inos and sgcα 1 are essential for the TLR4- induced cardiac protection. The in vivo preconditioning cardioprotection is in consistent with the in vitro anti- apoptotic effect of TLR4 signaling in isolated cardiomyocytes (99, 102). TLR Signaling Contributes to I/R Injury During I/R, injured myocardium releases a group of endogenous danger molecules that are capable of activating various TLRs. These include HSPs, fibrinogen, soluble heparan sulfate, HMGB- 1, and RNA, among others. These danger molecules induce marked myocardial inflam - mation and may contribute to myocardial injury and cardiac dysfunction. Several studies have indicated that TLR2 signaling plays a role in myocardial I/R injury (104, 105, 112, 113). In an ex vivo model of I/ R, TLR2 -/- mice exhibited improved LV function compared to WT mice (104). In vivo, TLR2 -/- mice had reduced cardiac inflammatory responses and smaller MI sizes compared to WT after I/ R. Using chimeric TLR2 deletion models, Arslan and colleagues have identified that leukocyte TLR2 plays a prominent role in mediating myocardial injury during I/R. Importantly, these cardiac benefits in TLR2 -/- mice are associated with persistent attenuation of myocardial inflammation, such as reduced leukocyte infiltration and attenuated cytokine production (105). TLR2 is also involved in coronary artery endothelial dysfunction with impaired vessel relaxation induced by transient ischemia (112). The role of TLR4 in I/R injury has been extensively studied. We have demonstrated that transient myocardial ischemia rapidly activates IRAK- 1 kinase via TLR4- MyD88 signaling (108). Activated TLR4 mediates both inflammation and apoptosis in the heart. In lost-of-function studies, TLR4- deficient (C57/B10 ScCr) or mutated (C3H/HeJ) mice have significantly smaller infarct sizes compared to their respective control mice. The decreased infarction is associated with attenuated cardiac inflammation as evidenced by fewer neutrophil infiltration, reduced NF-κB/AP- 1 activity, less cytokine production, and lower lipid peroxides production and complement 3 deposition in the heart (95, 96). Blocking TLR4 signaling by eritoran also results in decreased infarct sizes and attenuated myocardial inflammation (109). Finally, TLR4 signaling may also mediate inflammatory response and contribute to myocardial injury during heart transplantation (114). Given its critical position in multiple TLR signaling, it is not surprising that the innate im - mune adaptor MyD88 plays an important role in myocardial inflammation and injury after I/R (110, 115). Compared to WT mice, MyD88 KO mice have markedly reduced MI and significantly improved LV function after transient ischemia 112
11 Heart Inflammation and TLR Signaling (110). MyD88 -/- mice also exhibit significantly reduced myocardial cytokines and neutrophil infiltration (103, 110). This is associated with markedly attenuated neutrophil migratory function and decreased neutrophil CXCR2 expression (103). In contrast, deletion of Trif, another innate immune adaptor, while leads to reduced MI sizes (106), has no impact on myocardial neutrophil recruitment following I/R or on neutrophil CXCR2 modulation (103). Interestingly, MyD88- deficiency had no significant impact on infarct sizes and cardiac function in isolated hearts subjected to global I/R (110). Finally, chimeric MyD88 deletion models demonstrate that compared to WT mice transplanted with MyD88 +/+ bone marrow, WT mice transplanted with MyD88 -/- donor bone marrow have significantly decreased MI sizes. Taken together, these findings suggest that MyD88 signaling is essential for maintaining neutrophil migratory function and chemokine receptor expression during myocardial I/R. MyD88 signaling in circulating neutrophils plays a critical role in myocardial neutrophil infiltration and development of MI during I/R (111). TLR3 is the receptor for double-stranded RNA (27). Stimulation of TLR3-Trif signaling activates the transcriptional factors, NF- κb and IRF3/7, and subsequently results in the production of various cytokines such as type I IFN (116). Recent studies have suggested that TLR3 signaling may also recognize endogenous RNA released from necrotic cells (117, 118). In the heart, TLR3-Trif signaling is well known for its critical role in the host innate immune response against virus- induced myocarditis. However, the role of TLR3- Trif signaling in the pathogenesis of myocardial I/ R injury is much less clear. Two recent studies demonstrate the possible role of TLR3 signaling in myocardial I/R injury. Mice lacking TLR3 exhibit reduced myocardial infarct and improved function (106, 107). We have tested the release and the potential role of cellular RNA in myocardial I/R injury (106). Hypoxia in vitro and I/R in vivo lead to release of cellular RNA including microrna. Necrotic cardiomyocytes induce a robust and dose- dependent, cytokine response in cultured cardiomyocytes, which is markedly reduced by RNase but not DNase, and partially blocked in TLR3- deficient cardiomyocytes. In vivo, RNase administration reduced serum RNA level, attenuated myocardial cytokine production, leukocyte infiltration and apoptosis, and conferred cardiac protection against I/R injury. These results suggest that extracellular RNA released during I/R may contribute to myocardial inflammation and infarction (106). However, the nature of extracellular RNAs involved in I/R injury and the underlying signaling mechanisms are unclear. TLRs in Myocarditis Myocarditis is defined clinically as inflammation of the heart muscle. It is a major cause of sudden, unexpected death in adults less than 40 years of age and young athletes. The estimated incidence of myocarditis in the general population ranges from 1.06 to 5.0% (119, 120). The causes of acute myocarditis include infection, autoimmune disorders, systemic diseases, drugs and toxins. Table 4 summarizes the major findings related to the role of TLRs in viral and autoimmune myocarditis. Viral Myocarditis Trypanosoma cruz and Chagas' disease are the major contributors to the high incidence of myocarditis in South America, whereas viruses are the predominant cause of myocarditis in North America and Europe. While the exact role of various TLRs in viral myocarditis and cardiomyopathy is yet to be defined, both protective and detrimental effects have been reported. TLR3 is considered as a major host anti- viral defense mechanism. Mice deficient of TLR3 are more susceptible to encephalomyocarditis virus (EMCV) infection with higher mortality, increased myocardial viral load, and more severe myocardial injury (121). However, myocardial inflammatory cell infiltration and cytokine mrna expression are attenuated and delayed in TLR3 -/- mice. These studies suggest that EMCV invasion induces a TLR3-dependent myocardial inflammatory response, which is an important protective mechanism against the virus- induced myocardial injury and mortality. A similar study has been reported in coxsackievirus- induced myocarditis (122). Local myocardial production of IFN- γ is significantly reduced in TLR3 -/- hearts, suggesting that type II IFN may play a critical role in the anti- 113
12 Review Article Table 4. Role of TLR Signaling in Viral and Autoimmune Myocarditis. TLRs and adaptor Myocarditis TLR3 TLR3 -/- mice are more susceptible to encephalomyocarditis virus infection with higher mortality, increased viral load, reduced myocardial inflammation, and more severe myocardial injury (121). A similar finding is reported in coxsackievirus-induced myocarditis (122). These studies demonstrate that TLR3 signaling represents a major anti-viral defense mechanism. TLR3 -/- mice show similar myocardial inflammation in autoimmune myocarditis as WT mice (123). TLR4 TLR4 contributes to viral myocarditis-induced myocardial inflammation and exacerbates coxsackievirus replication and myocarditis (124). TLR7 TLR7 -/- mice are protected from experimental autoimmune myocarditis (125). MyD88 MyD88 -/- mice have less myocardial inflammation and injury, reduced CVB3 viral titers, and improved survival, demonstrating MyD88 signaling as a major contributor to CVB-induced myocardial inflammation and as a critical regulator in cardiac viral replication possibly via type I IFN-dependent mechanism (126). MyD88 -/- mice are protected from myocarditis after immunization with α- MHC- derived peptide (MyHC- α) and complete Freund's adjuvant (125). Trif Trif plays a protective role against viral myocarditis. Similar to TLR3 -/- mice, Trif -/- mice have higher viral load, lower cytokine gene expression than WT mice (122, 127) and marked increase in mortality after CVB3 infection (127). viral responses of TLR3 signaling (122). Different from TLR3, TLR4 signaling seems contributing to myocardial injury during viral myocarditis. TLR4 mrna is reportedly increased in endomyocardial biopsy samples from patients with clinically suspected myocarditis and from those with idiopathic dilated cardiomyopathy. This is associated with enteroviral replication and cardiac dysfunction in human myocarditis (128). In an animal model of myocarditis, TLR4 and IL- 12 receptor β1 exacerbated coxsackievirus replication and myocarditis, whereas IFN- γ protected against viral replication (124). TLR4 signaling is also associated with increased pro- inflammatory cytokines (IL- 1β and IL- 18) expression in the infected hearts (124). MyD88 and Trif are two adaptors critical for TLR signaling, but their roles in viral myocarditis are very much different. Compared to WT mice, mice deficient in MyD88 have less myocardial inflammation and injury, reduced coxsackievirus B 3 (CVB3) viral titers, and improved survival (126). The myocardial cytokines including IFN-γ are significantly decreased, but IFN-α and IFN- β are increased in MyD88 -/- mice. This study establishes MyD88 signaling as a major contributor to CVB- induced myocardial inflam - mation and a critical regulator in viral replication in the heart possibly via type I IFN- dependent mechanism (126). In contrast, Trif plays a protective role against viral myocarditis. Similar to TLR3 -/- mice, Trif -/- mice have higher viral load, attenuated cytokine gene expression than WT mice (122, 127), and marked increase in mortality after CVB3 infection (127). The antiviral protection of Trif signaling is likely mediated by type I IFN- β since myocardial IFN- β expression is markedly suppressed in Trif -/- mice and administration of IFN- β effectively reduced myocardial viral load and local inflammation and markedly improved the long term survival rate in Trif-deficient animals (127). Autoimmune Myocarditis In a significant subset of patients with myocarditis, host autoimmunity plays an important role in the development of myocarditis and subsequent dilated cardiomyopathy (129). TLR signaling can activate the adaptive immune system by inducing cytokine production and up- regulating co- stimulatory molecules of antigen presenting cells, and play a role in the development in autoimmune myocarditis. In a mouse model of autoimmune myocarditis, investigators have demonstrated that TLR4- induced Th1 immune response is required for the development of myocarditis induced by myosin and BCG (130). Similarly, in comparison to WT, MyD88 -/- mice are protected from myocarditis after immunization with α- MHC- derived peptide (MyHC-α) and complete Freund's adjuvant (125). This protection against autoimmune myocarditis is due to impaired expansion of heart- specific CD4 + T cells. The serine/threonine kinase PKC- 114
13 Heart Inflammation and TLR Signaling theta is required for T cell- driven myocarditis. However, TLR9 activation could overcome the PKC- theta deficiency and restored autoimmune myocarditis (131). To determine the role of the intracellular TLRs in autoimmune myocarditis, Pagni and colleagues induced experimental autoim - mune myocarditis (EAM) in mice deficient in TLR3, TLR7, and TLR9. They found that myocardial cellular infiltration and in vitro proliferation of MyHC-α- restimulated splenocytes were markedly reduced in TLR7 -/- and MyD88 -/- mice, while TLR3 -/- and TLR9 -/- mice showed similar myocardial inflammatory cell infiltration as WT mice. These data suggest that TLR7 and MyD88 signaling mediates myocardial inflammation and injury during the EAM (123). Summary and Future Directions Myocardial inflammation is a common theme of a group of diseases that include severe sepsis, ischemic myocardial injury and acute myocarditis, and contributes to their pathogenesis. These cardiac diseases often pose significant perioperative risk to surgical patients and present challenges to anesthesiologists. Understanding the molecular mechanisms controlling myocardial inflammation under these critical conditions is important for the development of future therapeutic strategy and potentially improves the perioperative care. During the past decade, the role of TLR signaling in cardiac inflammation has been extensively studied. A variety of microbial and non-microbial TLR ligands have been identified under these critical conditions. These ligands act through TLRs and elicit potent biochemical and pro- inflammatory responses. By mediating the complex cardiac inflammatory signaling, either beneficial or deleterious in nature, TLRs play a pivotal role in the development of these cardiac diseases. Several important future directions should be considered. While numerous studies have indicated the contributory role of TLRs in the development of septic cardiomyopathy, ischemic myocardial injury and myocarditis, there are many unanswered questions that are critical for our ultimate understanding of the role of TLR signaling. For example, multiple TLRs are involved in polymicrobial sepsis. Given the recent disappointing eritoran phase III trial and the complex role of TLR4 and TLR2 in polymicrobial sepsis, how to modulate multiple TLR signaling pathways to achieve therapeutic goal may be critical. Would blocking MyD88 signaling be more efficacious compared to individual TLR antagonist (i.e., eritoran) in the setting of polymicrobial sepsis? How could we keep the delicate balance between blocking hyperinflammatory response and maintaining essential host innate immune function during bacterial infection? The identification of novel TLR ligands in septic tissue injury will be the focus of intense laboratory investigation. MicroRNA, either from pathogens or host, and its novel role as gene regulator and extracellular TLR ligand will be defined. In myocardial ischemic injury, how do myocardial TLRs become activated? How do the endogenous danger molecules such as extracellular RNA interact with myocardial TLRs and contribute to I/R injury? How would the dual role of TLR4 signaling, i.e., pro- inflammatory vs. antiapoptotic effect, determine the final outcome of myocardial injury? Importantly, how can we promote the protective preconditioning effect by TLR ligands and at the same time prohibits the injurious pro- inflammatory of TLR signaling during myocardial ischemia? Dissecting the com - plex molecular and cellular pathways by which TLR signaling controls myocardial inflammation and cardiomyocyte injury will shed light on the mechanisms of these diseases and have significant clinical implications. The work in our laboratory during the past decade has been supported in part by National Institutes of Health (R01- GM and R01- GM097259), American Heart Association (Grant-in-Aid T), Foundation for Anesthesia Education and Research (FAER), William F. Milton Fund of Harvard University, and International Anesthesia Research Society (IARS). No other potential conflict of interest relevant to this review was reported. I would like to thank all current and former trainees in my laboratory at Massachusetts General Hospital, Harvard Medical School for their dedication and contributions. The following individuals have made the major contributions to our work discussed in this article: Yan Feng, Lin Zou, Yan Shen, Rui Si, Yan Li, E Wang, Ming Zhang, Yu Gong, Chan Chen, Dan Li. 115
Innate Immunity. Chapter 3. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples. Antimicrobial peptide psoriasin
 Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Innate Immunity. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples Chapter 3. Antimicrobial peptide psoriasin
 Know Differences and Provide Examples Chapter * Innate Immunity * kin and Epithelial Barriers * Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive
Know Differences and Provide Examples Chapter * Innate Immunity * kin and Epithelial Barriers * Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive
2. Innate immunity 2013
 1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
1 Innate Immune Responses 3 Innate immunity Abul K. Abbas University of California San Francisco The initial responses to: 1. Microbes: essential early mechanisms to prevent, control, or eliminate infection;
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics
 Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
Toll-like Receptors (TLRs): Biology, Pathology and Therapeutics Dr Sarah Sasson SydPATH Registrar 23 rd June 2014 TLRs: Introduction Discovered in 1990s Recognise conserved structures in pathogens Rely
Innate immunity. Abul K. Abbas University of California San Francisco. FOCiS
 1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
1 Innate immunity Abul K. Abbas University of California San Francisco FOCiS 2 Lecture outline Components of innate immunity Recognition of microbes and dead cells Toll Like Receptors NOD Like Receptors/Inflammasome
Toll-like Receptor Signaling
 Toll-like Receptor Signaling 1 Professor of Medicine University of Massachusetts Medical School, Worcester, MA, USA Why do we need innate immunity? Pathogens multiply very fast We literally swim in viruses
Toll-like Receptor Signaling 1 Professor of Medicine University of Massachusetts Medical School, Worcester, MA, USA Why do we need innate immunity? Pathogens multiply very fast We literally swim in viruses
Innate Immunity & Inflammation
 Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
Innate Immunity & Inflammation The innate immune system is an evolutionally conserved mechanism that provides an early and effective response against invading microbial pathogens. It relies on a limited
TOLL-LIKE RECEPTORS AND CYTOKINES IN SEPSIS
 TOLL-LIKE RECEPTORS AND CYTOKINES IN SEPSIS A/PROF WILLIAM SEWELL ST VINCENT S CLINICAL SCHOOL, UNSW SYDPATH, ST VINCENT S HOSPITAL SYDNEY GARVAN INSTITUTE INNATE VERSUS ADAPTIVE IMMUNE RESPONSES INNATE
TOLL-LIKE RECEPTORS AND CYTOKINES IN SEPSIS A/PROF WILLIAM SEWELL ST VINCENT S CLINICAL SCHOOL, UNSW SYDPATH, ST VINCENT S HOSPITAL SYDNEY GARVAN INSTITUTE INNATE VERSUS ADAPTIVE IMMUNE RESPONSES INNATE
Review Article Toll-Like Receptors and Myocardial Inflammation
 SAGE-Hindawi Access to Research International Journal of Inflammation Volume 211, Article ID 17352, 21 pages doi:1.461/211/17352 Review Article Toll-Like Receptors and Myocardial Inflammation Yan Feng
SAGE-Hindawi Access to Research International Journal of Inflammation Volume 211, Article ID 17352, 21 pages doi:1.461/211/17352 Review Article Toll-Like Receptors and Myocardial Inflammation Yan Feng
Structure and Function of Antigen Recognition Molecules
 MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
MICR2209 Structure and Function of Antigen Recognition Molecules Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will examine the major receptors used by cells of the innate and
Identification of Microbes
 Identification of Microbes Recognition by PRR (pattern recognition receptors) Recognize conserved molecular patterns on microbes called pathogen associated molecular patterns (PAMPs) which are not present
Identification of Microbes Recognition by PRR (pattern recognition receptors) Recognize conserved molecular patterns on microbes called pathogen associated molecular patterns (PAMPs) which are not present
1. TLR. TLR Toll-like receptors. Toll Toll-like receptor, TLR TLR TLR TLR. type I TLR TLR. Toll
 54pp.145 152 2004 1. TLR T B TLR Toll-like receptors TLR TLR I IFN TLR T B B T Toll NF- B 1996 565-0871 3-1 TEL 06-6879-8303 FAX 06-6879-8305 E-mail uemattsu@biken.osaka-u.ac.jp Toll Toll-like receptor,
54pp.145 152 2004 1. TLR T B TLR Toll-like receptors TLR TLR I IFN TLR T B B T Toll NF- B 1996 565-0871 3-1 TEL 06-6879-8303 FAX 06-6879-8305 E-mail uemattsu@biken.osaka-u.ac.jp Toll Toll-like receptor,
Newly Recognized Components of the Innate Immune System
 Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Chapter 3 The Induced Responses of Innate Immunity
 Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
Chapter 3 The Induced Responses of Innate Immunity Pattern recognition by cells of the innate immune system Pattern recognition by cells of the innate immune system 4 main pattern recognition receptors
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine
 Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Intracellular MHC class II molecules promote TLR-triggered innate. immune responses by maintaining Btk activation
 Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Intrinsic cellular defenses against virus infection
 Intrinsic cellular defenses against virus infection Detection of virus infection Host cell response to virus infection Interferons: structure and synthesis Induction of antiviral activity Viral defenses
Intrinsic cellular defenses against virus infection Detection of virus infection Host cell response to virus infection Interferons: structure and synthesis Induction of antiviral activity Viral defenses
Genome-wide association study of esophageal squamous cell carcinoma in Chinese subjects identifies susceptibility loci at PLCE1 and C20orf54
 CORRECTION NOTICE Nat. Genet. 42, 759 763 (2010); published online 22 August 2010; corrected online 27 August 2014 Genome-wide association study of esophageal squamous cell carcinoma in Chinese subjects
CORRECTION NOTICE Nat. Genet. 42, 759 763 (2010); published online 22 August 2010; corrected online 27 August 2014 Genome-wide association study of esophageal squamous cell carcinoma in Chinese subjects
MICR2209. Innate Immunity. Dr Allison Imrie
 MICR2209 Innate Immunity Dr Allison Imrie allison.imrie@uwa.edu.au Synopsis: In this lecture we will review the different mechanisms which consbtute the innate immune response, and examine the major cells
MICR2209 Innate Immunity Dr Allison Imrie allison.imrie@uwa.edu.au Synopsis: In this lecture we will review the different mechanisms which consbtute the innate immune response, and examine the major cells
Lecture on Innate Immunity and Inflammation. Innate Immunity: An Evolutionary View
 Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
TD-BF01: Innate immunity to microorganisms
 TD-BF01: Innate immunity to microorganisms I. Toll receptors (adapted from Takeuchi, O. et al. (1999) Immunity 11:443; Kawai, T. et al. (1999) Immunity 11:115; Hemmi, H. et al. (2000) Nature 408:740; Muzio,
TD-BF01: Innate immunity to microorganisms I. Toll receptors (adapted from Takeuchi, O. et al. (1999) Immunity 11:443; Kawai, T. et al. (1999) Immunity 11:115; Hemmi, H. et al. (2000) Nature 408:740; Muzio,
Innate Immunity. Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016
 Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016 Objectives: Explain how innate immune system recognizes foreign substances
Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 2 August 2016 Objectives: Explain how innate immune system recognizes foreign substances
Lecture on Innate Immunity and Inflammation
 Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Lecture on Innate Immunity and Inflammation Evolutionary View Epithelial barriers to infection Four main types of innate recognition molecules:tlrs, CLRs, NLRs, RLRs NF-κB, the master transcriptional regulator
Role of Innate Immunity in Control of Adaptive Immunity
 Role of Innate Immunity in Control of Adaptive Immunity Innate Immunity The burden of pathogen sensing is placed on the innate immune system Danger hypothesis Missing Self Based on the detection of molecular
Role of Innate Immunity in Control of Adaptive Immunity Innate Immunity The burden of pathogen sensing is placed on the innate immune system Danger hypothesis Missing Self Based on the detection of molecular
The Innate Immune Response is Conserved Throughout Evolution and is Triggered by Pattern Recognition. Lipopolysaccharide = Lipid + Polysaccharide
 The Innate Immune Response is Conserved Throughout Evolution and is Triggered by Pattern Recognition Lipopolysaccharide = Lipid + Polysaccharide E.coli Cell wall organization Lipopolysaccharide Outer membrane
The Innate Immune Response is Conserved Throughout Evolution and is Triggered by Pattern Recognition Lipopolysaccharide = Lipid + Polysaccharide E.coli Cell wall organization Lipopolysaccharide Outer membrane
Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD.
 Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD. Chapter 13: Mechanisms of Immunity to Viral Disease Prepared by
Allergy and Immunology Review Corner: Chapter 13 of Immunology IV: Clinical Applications in Health and Disease, by Joseph A. Bellanti, MD. Chapter 13: Mechanisms of Immunity to Viral Disease Prepared by
3/10/14. Ultrastructural organization. Gram Stain. Infection leads to production of inducers of inflammation. Gram negative.
 Infection leads to production of inducers of inflammation or dendritic cell Inflammatory mediators: Complex and many, but include: Lipids and Proteins (cytokines/chemokines) TNF Others Ultrastructural
Infection leads to production of inducers of inflammation or dendritic cell Inflammatory mediators: Complex and many, but include: Lipids and Proteins (cytokines/chemokines) TNF Others Ultrastructural
Immunology Part II. Innate Immunity. 18. April 2018, Ruhr-Universität Bochum Marcus Peters,
 Immunology Part II Innate Immunity 18. April 2018, Ruhr-Universität Bochum Marcus Peters, marcus.peters@rub.de Conserved structures of pathogens PAMPs are detected by Pattern Recognition Receptors PRRs
Immunology Part II Innate Immunity 18. April 2018, Ruhr-Universität Bochum Marcus Peters, marcus.peters@rub.de Conserved structures of pathogens PAMPs are detected by Pattern Recognition Receptors PRRs
The Innate Immune Response
 The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
The Innate Immune Response FUNCTIONS OF THE IMMUNE SYSTEM: Recognize, destroy and clear a diversity of pathogens. Initiate tissue and wound healing processes. Recognize and clear damaged self components.
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Bruce A. Beutler and Jules A. Hoffmann. Ralph M. Steinman
 PRESS RELEASE 20-0-03 The Nobel Assembly at Karolinska Institutet has today decided that The 20 Nobel Prize in Physiology or Medicine shall be divided, with one half jointly to Bruce A. Beutler and Jules
PRESS RELEASE 20-0-03 The Nobel Assembly at Karolinska Institutet has today decided that The 20 Nobel Prize in Physiology or Medicine shall be divided, with one half jointly to Bruce A. Beutler and Jules
1. The scavenger receptor, CD36, functions as a coreceptor for which TLR? a. TLR ½ b. TLR 3 c. TLR 4 d. TLR 2/6
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Novel function of NADPH oxidase in atherosclerosis. Yun Soo Bae Department of Life Science Ewha Womans University
 Novel function of NADPH oxidase in atherosclerosis Yun Soo Bae Department of Life Science Ewha Womans University Recent understanding of ROS: act as second messengers e e Catalase/peroxidase O 2 H 2 O
Novel function of NADPH oxidase in atherosclerosis Yun Soo Bae Department of Life Science Ewha Womans University Recent understanding of ROS: act as second messengers e e Catalase/peroxidase O 2 H 2 O
Pathogen Recognition and Inflammatory Signaling in Innate Immune Defenses
 CLINICAL MICROBIOLOGY REVIEWS, Apr. 2009, p. 240 273 Vol. 22, No. 2 0893-8512/09/$08.00 0 doi:10.1128/cmr.00046-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Pathogen Recognition
CLINICAL MICROBIOLOGY REVIEWS, Apr. 2009, p. 240 273 Vol. 22, No. 2 0893-8512/09/$08.00 0 doi:10.1128/cmr.00046-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Pathogen Recognition
Innate Immunity: (I) Molecules & (II) Cells
 Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Autoimmunity. Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens
 Autoimmunity Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens Autoimmune disease can be caused to primary defects in B cells, T cells and possibly
Autoimmunity Autoimmunity arises because of defects in central or peripheral tolerance of lymphocytes to selfantigens Autoimmune disease can be caused to primary defects in B cells, T cells and possibly
Relative sizes of infectious agents
 Relative sizes of infectious agents Bacteria Protozoa Viruses RBC 0.005 0.01 0.03 01 03 05 1 3 5 10 30 50 100 300 Size in microns ( µm ) - log scale Immunity to Infection Principle 1 Every clinical infection
Relative sizes of infectious agents Bacteria Protozoa Viruses RBC 0.005 0.01 0.03 01 03 05 1 3 5 10 30 50 100 300 Size in microns ( µm ) - log scale Immunity to Infection Principle 1 Every clinical infection
EMPEROR'S COLLEGE MTOM COURSE SYLLABUS HERB FORMULAE II
 COURSE DESCRIPTION The second of three courses in the Herb Formulae series. Categories covered in Formulae II include the Tonify Qi and Blood, Regulate Qi, Invigorate the Blood, Stop Bleeding, Stabilize
COURSE DESCRIPTION The second of three courses in the Herb Formulae series. Categories covered in Formulae II include the Tonify Qi and Blood, Regulate Qi, Invigorate the Blood, Stop Bleeding, Stabilize
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
NFκB What is it and What s the deal with radicals?
 The Virtual Free Radical School NFκB What is it and What s the deal with radicals? Emily Ho, Ph.D Linus Pauling Institute Scientist Department of Nutrition and Food Management Oregon State University 117
The Virtual Free Radical School NFκB What is it and What s the deal with radicals? Emily Ho, Ph.D Linus Pauling Institute Scientist Department of Nutrition and Food Management Oregon State University 117
Lung Reperfusion Injury
 Lung Reperfusion Injury Michael S. Mulligan, M.D. Professor of Surgery Chief, Section of Thoracic Surgery Director, Lung Transplant Program University of Washington Medical Center Guiding Principles in
Lung Reperfusion Injury Michael S. Mulligan, M.D. Professor of Surgery Chief, Section of Thoracic Surgery Director, Lung Transplant Program University of Washington Medical Center Guiding Principles in
PKR is required for macrophage apoptosis after activation of TLR-4. By Christina, Ania and Xiaofu
 PKR is required for macrophage apoptosis after activation of TLR-4 By Christina, Ania and Xiaofu Introduction Macrophage PAMP Bacteria LPS Gram -ve LTA Gram +ve activation Clearance Macrophage PAMP Bacteria
PKR is required for macrophage apoptosis after activation of TLR-4 By Christina, Ania and Xiaofu Introduction Macrophage PAMP Bacteria LPS Gram -ve LTA Gram +ve activation Clearance Macrophage PAMP Bacteria
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION
 CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
Under the Radar Screen: How Bugs Trick Our Immune Defenses
 Under the Radar Screen: How Bugs Trick Our Immune Defenses Session 3: Toll-like receptors (TLRs) Marie-Eve Paquet and Gijsbert Grotenbreg Whitehead Institute for Biomedical Research Introduction to Toll-like
Under the Radar Screen: How Bugs Trick Our Immune Defenses Session 3: Toll-like receptors (TLRs) Marie-Eve Paquet and Gijsbert Grotenbreg Whitehead Institute for Biomedical Research Introduction to Toll-like
Inflammatory Pathways in Sepsis: TLRs and Innate Immunity. Keith R. Walley, MD St. Paul s Hospital University of British Columbia Vancouver, Canada
 Inflammatory Pathways in Sepsis: TLRs and Innate Immunity Keith R. Walley, MD St. Paul s Hospital University of British Columbia Vancouver, Canada Early Goal-Directed Therapy Rivers E et al. NEJM 345:1368-77,
Inflammatory Pathways in Sepsis: TLRs and Innate Immunity Keith R. Walley, MD St. Paul s Hospital University of British Columbia Vancouver, Canada Early Goal-Directed Therapy Rivers E et al. NEJM 345:1368-77,
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel:
 Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 11 T-Cell Activation, Differentiation, and Memory Copyright 2013 by W. H. Freeman and
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 11 T-Cell Activation, Differentiation, and Memory Copyright 2013 by W. H. Freeman and
Innate Immunity II. Integration. Lindsay Nicholson Advanced Immunology L2
 Innate Immunity II Integration Lindsay Nicholson Advanced Immunology L2 l.nicholson@bristol.ac.uk Lecture 1 Defining Innate Immunity Recognition and effector mechanisms (I) Lecture 2 Recognition and effector
Innate Immunity II Integration Lindsay Nicholson Advanced Immunology L2 l.nicholson@bristol.ac.uk Lecture 1 Defining Innate Immunity Recognition and effector mechanisms (I) Lecture 2 Recognition and effector
Overview of the Immune System
 Overview of the Immune System Immune System Innate (Nonspecific) Adaptive (Specific) Cellular Components Humoral Components Cell-Mediated Humoral (Ab) Antigens Definitions Immunogen Antigen (Ag) Hapten
Overview of the Immune System Immune System Innate (Nonspecific) Adaptive (Specific) Cellular Components Humoral Components Cell-Mediated Humoral (Ab) Antigens Definitions Immunogen Antigen (Ag) Hapten
Role of TLR- / NLR-signaling and the associated cytokines involved in recruitment of neutrophils in murine models of Staphylococcus aureus infection
 Virulence ISSN: 2150-5594 (Print) 2150-5608 (Online) Journal homepage: http://www.tandfonline.com/loi/kvir20 Role of TLR- / NLR-signaling and the associated cytokines involved in recruitment of neutrophils
Virulence ISSN: 2150-5594 (Print) 2150-5608 (Online) Journal homepage: http://www.tandfonline.com/loi/kvir20 Role of TLR- / NLR-signaling and the associated cytokines involved in recruitment of neutrophils
Innate Immunity. By Dr. Gouse Mohiddin Shaik
 Innate Immunity By Dr. Gouse Mohiddin Shaik Types of immunity Immunity Innate / inborn Non-specific Acquired / adaptive Specific 3rd line of defense Physical barriers Skin, Saliva, Mucous, Stomach acid,
Innate Immunity By Dr. Gouse Mohiddin Shaik Types of immunity Immunity Innate / inborn Non-specific Acquired / adaptive Specific 3rd line of defense Physical barriers Skin, Saliva, Mucous, Stomach acid,
Commensal Bacteria, Toll-like Receptors and Intestinal Injury. Journal Club December 16, 2004
 Commensal Bacteria, Toll-like Receptors and Intestinal Injury Journal Club December 16, 2004 Gut-Commensal Interactions Nutrient metabolism Tissue development Resistance to colonization with pathogens
Commensal Bacteria, Toll-like Receptors and Intestinal Injury Journal Club December 16, 2004 Gut-Commensal Interactions Nutrient metabolism Tissue development Resistance to colonization with pathogens
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Animal Models to Understand Immunity
 Animal Models to Understand Immunity Hussein El Saghire hesaghir@sckcen.be Innate Adaptive immunity Immunity MAPK and NF-kB TLR pathways receptors Fast Slow Non-specific Specific NOD-like receptors T-cell
Animal Models to Understand Immunity Hussein El Saghire hesaghir@sckcen.be Innate Adaptive immunity Immunity MAPK and NF-kB TLR pathways receptors Fast Slow Non-specific Specific NOD-like receptors T-cell
Innate Immunity. Jan 8 th Prof. dr. sc. Ivana Novak Nakir 1
 Innate Immunity Jan 8 th 2018. Prof. dr. sc. Ivana Novak Nakir 1 Adaptive Innate 2 Immune system overview 1 st line of defense skin (2m 2 ) and mucosal membranes (~400m 2 ): physical barrier, lymphoid
Innate Immunity Jan 8 th 2018. Prof. dr. sc. Ivana Novak Nakir 1 Adaptive Innate 2 Immune system overview 1 st line of defense skin (2m 2 ) and mucosal membranes (~400m 2 ): physical barrier, lymphoid
Toll-like receptors in health and disease in the brain: mechanisms and therapeutic potential
 Clinical Science (2011) 121, 367 387 (Printed in Great Britain) doi:10.1042/cs20110164 367 R E V I E W Toll-like receptors in health and disease in the brain: mechanisms and therapeutic potential Mark
Clinical Science (2011) 121, 367 387 (Printed in Great Britain) doi:10.1042/cs20110164 367 R E V I E W Toll-like receptors in health and disease in the brain: mechanisms and therapeutic potential Mark
F12 Sorbent Based and Hybrid Therapies for Extracorporeal Support Continuous Hemodiafiltration with Cytokine-Adsorbing Hemofilters (CAH-CHDF)
 F12 Sorbent Based and Hybrid Therapies for Extracorporeal Support Continuous Hemodiafiltration with Cytokine-Adsorbing Hemofilters (CAH-CHDF) Hiroyuki Hirasawa, MD, PhD Professor Emeritus, Department of
F12 Sorbent Based and Hybrid Therapies for Extracorporeal Support Continuous Hemodiafiltration with Cytokine-Adsorbing Hemofilters (CAH-CHDF) Hiroyuki Hirasawa, MD, PhD Professor Emeritus, Department of
The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors
 The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors Taro Kawai 1,2 & Shizuo Akira 1,2 The discovery of Toll-like receptors (TLRs) as components that recognize conserved
The role of pattern-recognition receptors in innate immunity: update on Toll-like receptors Taro Kawai 1,2 & Shizuo Akira 1,2 The discovery of Toll-like receptors (TLRs) as components that recognize conserved
All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity
 1 2 3 4 5 6 7 8 9 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 In innate immunity, recognition and
1 2 3 4 5 6 7 8 9 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 In innate immunity, recognition and
محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases
 محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases Immunity to infection depends on a combination of innate mechanisms (phagocytosis, complement, etc.) and antigen
محاضرة مناعت مدرس المادة :ا.م. هدى عبدالهادي علي النصراوي Immunity to Infectious Diseases Immunity to infection depends on a combination of innate mechanisms (phagocytosis, complement, etc.) and antigen
Innate Immunity and the Paradoxes of Viral Pathogens and Tissue Injury in Gene Therapy
 Innate Immunity and the Paradoxes of Viral Pathogens and Tissue Injury in Gene Therapy Daniel R. Salomon, M.D. Department of Molecular and Experimental Medicine The Scripps Research Institute Tissue and
Innate Immunity and the Paradoxes of Viral Pathogens and Tissue Injury in Gene Therapy Daniel R. Salomon, M.D. Department of Molecular and Experimental Medicine The Scripps Research Institute Tissue and
Innate Immunity. Natural or native immunity
 Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
Innate Immunity 1 Innate Immunity Natural or native immunity 2 When microbes enter in the body 3 Secondly, it also stimulates the adaptive immune system 4 Immunologic memory 5 Components of Innate Immunity
11/25/2017. THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS BARRIER DEFENSES INNATE IMMUNITY OF VERTEBRATES
 THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
THE IMMUNE SYSTEM Chapter 43 IMMUNITY INNATE IMMUNITY EXAMPLE IN INSECTS Exoskeleton made of chitin forms the first barrier to pathogens Digestive system is protected by a chitin-based barrier and lysozyme,
Innate Immunity. Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 July 2017
 Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 July 2017 Objectives: Explain how innate immune system recognizes foreign substances
Innate Immunity Hathairat Thananchai, DPhil Department of Microbiology Faculty of Medicine Chiang Mai University 25 July 2017 Objectives: Explain how innate immune system recognizes foreign substances
General Overview of Immunology. Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center
 General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
JAPM CONTENTS. Journal of Anesthesia and Perioperative Medicine. Original Articles. Systematic Review and Meta-Analysis. Review Articles.
 JAPM EDITORS-IN-CHIEF Jin Liu, West Hospital of Sichuan University, Tian-Long Wang, Xuan Wu Hospital of Capital Medical University, ASSOCIATE EDITORS-IN-CHIEF Qu-Lian Guo, Xiangya Hosptial, Central South
JAPM EDITORS-IN-CHIEF Jin Liu, West Hospital of Sichuan University, Tian-Long Wang, Xuan Wu Hospital of Capital Medical University, ASSOCIATE EDITORS-IN-CHIEF Qu-Lian Guo, Xiangya Hosptial, Central South
Test Bank for The Immune System 4th Edition by Parham
 Test Bank for The Immune System 4th Edition by Parham CHAPTER 3: INNATE IMMUNITY: THE INDUCED RESPONSE TO INFECTION 3 1 C-type lectins are so called because of the role of in facilitating receptor:ligand
Test Bank for The Immune System 4th Edition by Parham CHAPTER 3: INNATE IMMUNITY: THE INDUCED RESPONSE TO INFECTION 3 1 C-type lectins are so called because of the role of in facilitating receptor:ligand
How the Innate Immune System Profiles Pathogens
 How the Innate Immune System Profiles Pathogens Receptors on macrophages, neutrophils, dendritic cells for bacteria and viruses Broad specificity - Two main groups of bacteria: gram positive, gram-negative
How the Innate Immune System Profiles Pathogens Receptors on macrophages, neutrophils, dendritic cells for bacteria and viruses Broad specificity - Two main groups of bacteria: gram positive, gram-negative
Alcoholic hepatitis is a drug-induced disorder
 Alcoholic hepatitis is a drug-induced disorder Gyongyi Szabo, MD, PhD Professor of Medicine University of Massachusetts Medical School Source: 2 Sobernation.com Clinical Progression of ALD Mortality Acute
Alcoholic hepatitis is a drug-induced disorder Gyongyi Szabo, MD, PhD Professor of Medicine University of Massachusetts Medical School Source: 2 Sobernation.com Clinical Progression of ALD Mortality Acute
Immunology. T-Lymphocytes. 16. Oktober 2014, Ruhr-Universität Bochum Karin Peters,
 Immunology T-Lymphocytes 16. Oktober 2014, Ruhr-Universität Bochum Karin Peters, karin.peters@rub.de The role of T-effector cells in the immune response against microbes cellular immunity humoral immunity
Immunology T-Lymphocytes 16. Oktober 2014, Ruhr-Universität Bochum Karin Peters, karin.peters@rub.de The role of T-effector cells in the immune response against microbes cellular immunity humoral immunity
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 13: Cytokines
 Chapter 13: Cytokines Definition: secreted, low-molecular-weight proteins that regulate the nature, intensity and duration of the immune response by exerting a variety of effects on lymphocytes and/or
Chapter 13: Cytokines Definition: secreted, low-molecular-weight proteins that regulate the nature, intensity and duration of the immune response by exerting a variety of effects on lymphocytes and/or
Integrin CD11b negatively regulates TLR-triggered inflammatory responses by. activating Syk and promoting MyD88 and TRIF degradation via cbl-b
 Integrin CD11b negatively regulates TLR-triggered inflammatory responses by activating Syk and promoting MyD88 and TRIF degradation via cbl-b Chaofeng Han, Jing Jin, Sheng Xu, Haibo Liu, Nan Li, and Xuetao
Integrin CD11b negatively regulates TLR-triggered inflammatory responses by activating Syk and promoting MyD88 and TRIF degradation via cbl-b Chaofeng Han, Jing Jin, Sheng Xu, Haibo Liu, Nan Li, and Xuetao
D2 inhibits TLR2- initiated 12p40 transcription (-) TLR2 PGN MDP. MyD88 IRAK ECSIT TRAF6 NIK. Smallest unit of PGN muramyl dipeptide IKK.
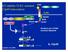 D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
Root & Branch Bulk Formula List
 An asterisk * indicates the inclusion of 1 or more granule versions of an herb because of limited availability on the American herbal market. These products are usually animal in nature like E Jiao, Shui
An asterisk * indicates the inclusion of 1 or more granule versions of an herb because of limited availability on the American herbal market. These products are usually animal in nature like E Jiao, Shui
EGFR kinase activity is required for TLR4 signaling and the septic shock response
 Manuscript EMBOR-2015-40337 EGFR kinase activity is required for TLR4 signaling and the septic shock response Saurabh Chattopadhyay, Manoj Veleeparambil, Darshana Poddar, Samar Abdulkhalek, Sudip K. Bandyopadhyay,
Manuscript EMBOR-2015-40337 EGFR kinase activity is required for TLR4 signaling and the septic shock response Saurabh Chattopadhyay, Manoj Veleeparambil, Darshana Poddar, Samar Abdulkhalek, Sudip K. Bandyopadhyay,
Preconditioning reprograms TLR signaling following cerebral ischemia the emergence of a neuroprotective program
 Oregon Health & Science University OHSU Digital Commons Scholar Archive September 2008 Preconditioning reprograms TLR signaling following cerebral ischemia the emergence of a neuroprotective program Brenda
Oregon Health & Science University OHSU Digital Commons Scholar Archive September 2008 Preconditioning reprograms TLR signaling following cerebral ischemia the emergence of a neuroprotective program Brenda
Overview of the immune system
 Overview of the immune system Immune system Innate (nonspecific) 1 st line of defense Adaptive (specific) 2 nd line of defense Cellular components Humoral components Cellular components Humoral components
Overview of the immune system Immune system Innate (nonspecific) 1 st line of defense Adaptive (specific) 2 nd line of defense Cellular components Humoral components Cellular components Humoral components
TOLL-LIKE RECEPTOR- INDUCED CYTOKINE SECRETION BY HUMAN MONOCYTES IN HEALTHY DONORS AND SEPTIC PATIENTS ASSESSED AT THE SINGLE CELL LEVEL
 DEPARTMENT OF MEDICINE, HUDDINGE DIVISION OF INFECTIOUS DISEASES Karolinska Institutet, Stockholm, Sweden TOLL-LIKE RECEPTOR- INDUCED CYTOKINE SECRETION BY HUMAN MONOCYTES IN HEALTHY DONORS AND SEPTIC
DEPARTMENT OF MEDICINE, HUDDINGE DIVISION OF INFECTIOUS DISEASES Karolinska Institutet, Stockholm, Sweden TOLL-LIKE RECEPTOR- INDUCED CYTOKINE SECRETION BY HUMAN MONOCYTES IN HEALTHY DONORS AND SEPTIC
Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells
 Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells Andrew H. Lichtman, M.D. Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard
Immunology Basics Relevant to Cancer Immunotherapy: T Cell Activation, Costimulation, and Effector T Cells Andrew H. Lichtman, M.D. Ph.D. Department of Pathology Brigham and Women s Hospital and Harvard
Interleukin-6; pathogenesis and treatment of autoimmune inflammatory diseases
 54 Review Article Interleukin-6; pathogenesis and treatment of autoimmune inflammatory diseases Toshio Tanaka 1, 2), Masashi Narazaki 3), Kazuya Masuda 4) and Tadamitsu Kishimoto 4, ) 1) Department of
54 Review Article Interleukin-6; pathogenesis and treatment of autoimmune inflammatory diseases Toshio Tanaka 1, 2), Masashi Narazaki 3), Kazuya Masuda 4) and Tadamitsu Kishimoto 4, ) 1) Department of
Cellular stress response and innate immune signaling: integrating pathways in host defense and inflammation
 Review Cellular stress response and innate immune signaling: integrating pathways in host defense and inflammation Sujatha Muralidharan and Pranoti Mandrekar 1 Department of Medicine, University of Massachusetts
Review Cellular stress response and innate immune signaling: integrating pathways in host defense and inflammation Sujatha Muralidharan and Pranoti Mandrekar 1 Department of Medicine, University of Massachusetts
Macrophage Activation & Cytokine Release. Dendritic Cells & Antigen Presentation. Neutrophils & Innate Defense
 Macrophage Activation & Cytokine Release Dendritic Cells & Antigen Presentation Neutrophils & Innate Defense Neutrophils Polymorphonuclear cells (PMNs) are recruited to the site of infection where they
Macrophage Activation & Cytokine Release Dendritic Cells & Antigen Presentation Neutrophils & Innate Defense Neutrophils Polymorphonuclear cells (PMNs) are recruited to the site of infection where they
Basis of Immunology and
 Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Innate Immunity: (I) Molecules & (II) Cells. Part II: Cells (aka the Sentinels)
 Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Innate Immunity: (I) Molecules & (II) Cells Stephanie Eisenbarth, M.D., Ph.D. FOCIS Advanced Course 2/19/18 Department of Laboratory Medicine Yale School of Medicine Department of Immunobiology Yale School
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
TRPM8 in the negative regulation of TNFα expression during cold stress
 in the negative regulation of TNFα expression during cold stress Xin-Pei Wang 1, Xuan Yu 1, Xiao-Jin Yan 1, Fan Lei 2, Yu-Shuang Chai 1, Jing-Fei Jiang 1, Zhi- Yi Yuan 1, Dong-Ming Xing 1, Li-Jun Du 1*
in the negative regulation of TNFα expression during cold stress Xin-Pei Wang 1, Xuan Yu 1, Xiao-Jin Yan 1, Fan Lei 2, Yu-Shuang Chai 1, Jing-Fei Jiang 1, Zhi- Yi Yuan 1, Dong-Ming Xing 1, Li-Jun Du 1*
Liu Jing and Liu Jing Diagnosis System in Classical TCM Discussions of Six Divisions or Six Confirmations Diagnosis System in Classical TCM Texts
 Liu Jing and Liu Jing Diagnosis System in Classical TCM Discussions of Six Divisions or Six Confirmations Diagnosis System in Classical TCM Texts Liu Jing Bian Zheng system had developed about 1800 years
Liu Jing and Liu Jing Diagnosis System in Classical TCM Discussions of Six Divisions or Six Confirmations Diagnosis System in Classical TCM Texts Liu Jing Bian Zheng system had developed about 1800 years
CELL BIOLOGY - CLUTCH CH THE IMMUNE SYSTEM.
 !! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
!! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
Nature Immunology doi: /ni.3268
 Supplementary Figure 1 Loss of Mst1 and Mst2 increases susceptibility to bacterial sepsis. (a) H&E staining of colon and kidney sections from wild type and Mst1 -/- Mst2 fl/fl Vav-Cre mice. Scale bar,
Supplementary Figure 1 Loss of Mst1 and Mst2 increases susceptibility to bacterial sepsis. (a) H&E staining of colon and kidney sections from wild type and Mst1 -/- Mst2 fl/fl Vav-Cre mice. Scale bar,
Cutaneous Immunology: Innate Immune Responses. Skin Biology Lecture Series
 Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections
 ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections Jean-Claude Sirard Christophe Carnoy Fiordiligie Casilag Delphine Cayet The partners
ABIMMUNE Repurposing disused antibiotics with immune modulators as antimicrobial strategy for respiratory tract infections Jean-Claude Sirard Christophe Carnoy Fiordiligie Casilag Delphine Cayet The partners
Innate Immunity. Bởi: OpenStaxCollege
 Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
The Immune System All animals have innate immunity, a defense active immediately
 The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 INNATE IMMUNITY (all animals) Recognition of traits shared
The Immune System All animals have innate immunity, a defense active immediately upon infection Vertebrates also have adaptive immunity Figure 43.2 INNATE IMMUNITY (all animals) Recognition of traits shared
生命科学基础 (21)- 动物的免疫器官. The Immune System. KE, Yuehai 柯越海. Zhejiang University, School of Basic Medical Sciences (BMS-ZJU) 浙江大学基础医学院
 生命科学基础 (21)- 动物的免疫器官 The Immune System KE, Yuehai 柯越海 Zhejiang University, School of Basic Medical Sciences (BMS-ZJU) 浙江大学基础医学院 Outlines The Immune System 1. Innate immunity 2. Adaptive immunity 3. Immune
生命科学基础 (21)- 动物的免疫器官 The Immune System KE, Yuehai 柯越海 Zhejiang University, School of Basic Medical Sciences (BMS-ZJU) 浙江大学基础医学院 Outlines The Immune System 1. Innate immunity 2. Adaptive immunity 3. Immune
Innate immunity. Monika Raulf. Lecture Tasks of the immune system. Body protection against damaging influences
 Innate immunity Monika Raulf Lecture 20.04.2016 Tasks of the immune system Body protection against damaging influences Deployment of a strong defense 2 The line of defence Skin Mucosa Sweat Digestive fluids
Innate immunity Monika Raulf Lecture 20.04.2016 Tasks of the immune system Body protection against damaging influences Deployment of a strong defense 2 The line of defence Skin Mucosa Sweat Digestive fluids
