Two-tube method for treatment of spontaneous esophageal rupture and concomitant mediastinal infection
|
|
|
- Alannah Gray
- 5 years ago
- Views:
Transcription
1 Clinical Report Two-tube method for treatment of spontaneous esophageal rupture and concomitant mediastinal infection Journal of International Medical Research 2018, Vol. 46(4) ! The Author(s) 2018 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: / journals.sagepub.com/home/imr Liang-liang Yu 1, Zheng-fu He 2, Qi-fang Liu 3, Ning Dai 1, Jian-min Si 1, Bei Ye 4 and Jian-cang Zhou 5 Abstract Objective: Spontaneous esophageal rupture (SER) is a rare but life-threatening condition with high mortality. The prognosis of patients with SER treated with surgical intervention or the traditional three-tube method is controversial. Thus, the aim of this study was to evaluate the clinical efficacy, feasibility, and safety of a new two-tube method involving a trans-fistula drainage tube and a three-lumen jejunal feeding tube for the treatment of SER without concomitant pleural rupture. Methods: From January 2007 to June 2016, patients with SER and managed with the two-tube method or other methods were retrospectively analyzed. Data collected included initial presentation, procedure time, duration of treatment, numbers of patients with eventual healing of leaks, and complications. Results: The average procedure time for the two-tube method was minutes. In comparison with the control method, the two-tube method had a similar diagnosis time ( vs days) but a significantly higher successful closure rate (94.4% vs. 63.6%) and shorter treatment time ( vs days). No complications associated with performance of the two-tube method occurred. 1 Department of Gastroenterology, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, China 2 Department of Thoracic Surgery, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, China 3 Department of Endoscopy Center, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, China 4 Taizhou Vocational College of Science and Technology, Taizhou, Zhejiang, China 5 Department of Critical Care Medicine, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou, China Corresponding author: Jian-cang Zhou, Department of Critical Care Medicine, Sir Run Run Shaw Hospital, Zhejiang University School of Medicine, Hangzhou , China. jiancangzhou@zju.edu.cn Creative Commons Non Commercial CC BY-NC: This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 License ( which permits non-commercial use, reproduction and distribution of the work without further permission provided the original work is attributed as specified on the SAGE and Open Access pages (
2 Yu et al Conclusion: The two-tube method is an effective and safe approach for patients with SER. Keywords Two-tube method, spontaneous esophageal rupture, endoscopic therapy, jejunal feeding tube, minimally invasive treatment, closure rate Date received: 30 July 2017; revised 27 November 2017; accepted: 19 December 2017 Introduction Spontaneous esophageal rupture (SER) is a rare but catastrophic condition with high mortality. 1 3 Current treatment options include conservative treatment, surgical intervention, endoscopic stent placement, thoracic closed drainage, and the traditional three-tube method (jejunal feeding tube, gastrointestinal decompression tube, and thoracic closed drainage tube). However, the most effective and feasible treatment option for SER remains controversial, and no standardized treatment algorithm has been established. The present study was performed to introduce and evaluate the clinical efficacy, feasibility, and safety of a new two-tube method (transfistula drainage tube and three-lumen jejunal feeding tube) for the treatment of SER. Materials and methods Study patients From January 2007 to June 2016, the clinical data of patients who were admitted to our hospital and with a diagnosis of SER were retrospectively analyzed. The diagnosis of SER was made according to one or more of the following criteria: clinical judgment, iodine contrast upper gastrointestinal radiography findings, chest computed tomography (CT) findings, or endoscopy findings. 2,4 Patients with an esophageal fistula due to postoperative anastomotic leakage or necrosis and those with SER with concurrent pleural rupture were excluded. The ethics committee of Sir Run Run Shaw Hospital approved the study ( ) and waived the need for consent because of the retrospective observational nature of the study. Equipment A GIF-Q260J endoscopy system and FG- 32L-1 endoscopic foreign body forceps (Olympus, Tokyo Japan), a Freka threelumen jejunal feeding tube and Freka nasogastric tube (Fresenius Kabi AG, Bad Homburg vor der H ohe, Germany), and a 1000-mA digital subtraction angiography system (Siemens AG, Berlin/Munich, Germany) were used in this study. Two-tube method Upon confirmation of the diagnosis of SER, the location, size, and number of leaks were further evaluated by CT or iodine contrast upper gastrointestinal radiography. All patients were admitted to the intensive care unit and underwent basic treatments including optimization of perfusion and respiratory function, broadspectrum intravenous antibiotic therapy, nutritional support, or chest tube drainage. 5 This was usually defined as the traditional three-tube method (jejunal feeding tube,
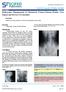
3 1530 Journal of International Medical Research 46(4) gastrointestinal decompression tube, and thoracic closed drainage tube). The two-tube procedure was accomplished under endoscopy. After the patients had been sedated with intravenous injection of midazolam or propofol, the following procedures were performed. (1) The endoscope was inserted to confirm the location of the leakage and estimate the number and size of the leaks. (2) If the endoscope could enter the leakage cavity, the necrosis within the cavity was directly removed from the cavity. A trans-fistula nasogastric tube was then placed to drain the leakage cavity using an endoscopic foreign body forceps and endoscopic visualization (Figure 1). Otherwise, for patients with a small leak orifice, the drainage tube was placed under X-ray fluoroscopic guidance. The guide wire was first placed in the leakage cavity under X-ray fluoroscopic and endoscopic visualization, and the nasogastric tube was then guided into the leakage cavity. The transfistula nasogastric tube was used as a drainage tube for the necrosis in the leakage cavity and was connected to an intermittent continuous vacuum pump at a negative pressure of 40 to 60 cm H 2 O. The leak cavity was flushed with normal saline at least twice a day. (3) The three-lumen jejunal feeding tube is a commercially available three-lumen tube. The lumen connected to Figure 1. Placement of drainage tube into the leakage cavity. (a) Endoscopic view of the leak orifice. (b) Inside view of the cavity under endoscopy (c) Placement of the drainage tube into the leakage cavity using endoscopic foreign body forceps and endoscopic visualization. (d) Simultaneous placement of the threelumen jejunal feeding tube.
4 Yu et al the most distal tip was used for jejunal feeding, while the other two were used as gastrointestinal decompression tubes (Figure 2). The gastrointestinal decompression tube lumen of the three-lumen jejunal feeding tube was also connected to an intermittent continuous vacuum pump at a negative pressure of 40 to 60 cm H 2 Otoeliminate gastric fluid, saliva, and phlegm. All patients were given enteral nutrition through the jejunal feeding tube. (4) If necessary, contrast radiography or endoscopy was performed to evaluate the location of the drainage tube and the size of the leakage cavity (Figure 3). The drainage tube was gradually withdrawn according to the amount of drained necrotic tissue, drainage tube location, and the size of the leakage cavity on serial endoscopic or CT check-ups. Figure 2. Structure of the three-lumen jejunal feeding tube. Arrow 1: the opening of the jejunal nutritional tube lumen. Arrow 2: the opening of the gastrointestinal decompression tube lumen. Arrow 3: the gastrointestinal decompression tube segment of the three-lumen jejunal feeding tube. Arrow 4: the jejunal nutritional tube segment of the threelumen jejunal feeding tube. The third opening allows for air filling to facilitate gastrointestinal decompression. Usually, 2 to 3 cm of the tube was withdrawn per week. Eventually, when the leakage cavity had closed as shown by contrast radiography or endoscopic examination, the drainage tube was removed from the leakage cavity. Approximately 4 to 6 weeks later, the leakage was usually cured and the leak orifice was closed. A further chest CT scan was performed in necessary to confirm the leakage cavity closure. Finally, the three-lumen jejunal feeding tube was removed when the patient successfully restarted oral feeding. The two indications for surgical management were the presence of sepsis with failure of at least one organ and inefficient drainage through a radiological or endoscopic approach. 6 Statistical analysis Descriptive data are reported as either mean standard deviation, median (interquartile range), or number and percentage. With respect to the differences in outcomes between the two-tube method and other management techniques, categorical variables were compared using chi-square analysis. Continuous variables were compared using an independent-sample t test for normally distributed data. 7 Statistical analysis was performed using SPSS 16.0 (Chicago, IL, USA). Significance was defined as a P value of <0.05. Results The two-tube method was performed for 18 patients, while 11 patients with SER were managed with control methods. The patients treated with the two-tube method comprised 16 men and 2 women. Their mean age was 46.2 years (range, years). There were no significant differences in the initial symptoms or underlying comorbidities between the two groups (Table 1). Although the two-tube method had a diagnosis time similar to
5 1532 Journal of International Medical Research 46(4) Figure 3. Evolution of esophageal leakage. (a) Endoscopic view of the two-tube placement method. Endoscopic view of the leakage (b) after 14 days and (c) 21 days later. (d) The leak orifice closed (arrow) after 42 days of the two-tube treatment. that of the control method ( vs days), it rendered a significantly higher successful closure rate (94.4% vs. 63.6%, P ¼ 0.033) and shorter treatment time ( vs days, P ¼ 0.014) (Table 1). Two tubes were successfully placed in all cases. The procedure time varied from 15 to 30 minutes (mean, minutes). The treatment cost included the three-lumen jejunal feeding tube, a nasogastric tube, endoscopic examination, and some sedation (total of approximately 250 US dollars). One patient died of severe sepsis and respiratory failure. No complications such as massive hemorrhage or secondary esophageal stricture occurred. Discussion SER is a rare condition associated with high mortality. The incidence is approximately 0.02%, but the mortality rate ranges from 10% to as high as 60%. 3 5,8 It is a life-threatening condition characterized by disruption of the distal esophagus due to barotrauma, resulting in contamination of the mediastinum and pleural cavity with gastric contents. Therefore, early recognition and prompt drainage of
6 Yu et al Table 1. Baseline characteristics of patients who underwent the two-tube method and other interventions Variables Two-tube method group (n ¼ 18) Control group (n ¼ 11) P value Age (y) Male sex 16 (88.9) 9 (81.8) Initial symptoms Vomiting Fever 17 9 Chest pain Subcutaneous emphysema 10 7 Symptom onset to diagnosis (days) Duration of treatment (days) Successful closure 17 (94.4) 7 (63.6) Comorbidity Coronary heart disease Chronic obstructive pulmonary disease 3 3 Diabetes mellitus 4 3 Hypertension 6 4 Data are presented as mean standard deviation, n (%), or n. the leakage is of paramount importance. In this study, the two-tube method had a significantly higher successful closure rate (94.4% vs. 63.6%, P ¼ 0.033) and shorter treatment time ( vs days, P ¼ 0.014) than the control method. SER was first described by Herman Boerhaave in 1724; thus, is known as Boerhaave syndrome. 4 Because the expected triad of vomiting, chest pain, and subcutaneous emphysema is encountered in only some patients, early diagnosis of SER remains a clinical challenge even now. Patients with SER usually present with atypical symptoms such as respiratory distress, and the physical examination findings are often nonspecific. 9,10 Consequently, this entity is often misdiagnosed as a perforated peptic ulcer, acute pancreatitis, acute cholecystitis, myocardial infraction, pulmonary embolism, or spontaneous pneumothorax, which can lead to a delay in the administration of appropriate treatment. 8,11 Thus, an accurate diagnosis of SER requires a high index of suspicion, especially in patients with one or two symptoms of the triad. The treatment of SER depends on the location, size, and duration of the perforation; underlying esophageal disease; and underlying health status of the patient. Adequate drainage and nutritional support are two essential principles in the management of SER. 12 Treatment options are categorized into conservative, endoscopic, and surgical. Nevertheless, no consensus regarding the best therapy has been reached. Simple conservative treatments, 13 including fasting, intravenous broad-spectrum antibiotics, gastrointestinal decompression, and nutritional support, are generally associated with poor therapeutic effects because digestive fluid may continue to leak into the cavity and the necrotic tissue is not drained. Hence, a thoracic closed drainage tube is placed by most physicians to drain the necrotic tissue and relieve the inflammation. However, given that the leakage and secondary inflammation are mainly located in the mediastinum in most patients, 14
7 1534 Journal of International Medical Research 46(4) placement of a simple closed thoracic drainage tube is not enough to drain the abscessed cavities that are wrapped within the mediastinum. 15,16 Until 10 years ago, the most commonly used treatment method was a surgical operation, which was thought to thoroughly drain the leakage, pleural cavity, and mediastinal infection. However, such treatment is invasive and associated with high costs and a longer length of hospital stay. Endoscopic clipping is a promising technique for early and small esophageal ruptures. 17,18 One limitation is that these clips do not allow for treatment of large defects and are not resistant enough to bring together distant, inflamed anastomotic edges. Thus, the efficacy of these techniques is limited by the defect size (generally <2 cm for endoscopic clips). 6 The advent of the endoscopic stent technique revolutionized the management of SER, especially for patients with a small leakage and those unsuitable for open surgery. 19,20 The mediastinal inflammation may persist, causing the temporary closed leakage to open. Other adverse events associated with stent placement and removal include insufficient closure of the leaks, stent migration and development of strictures after stent removal, uncontrollable hematemesis, and difficult stent removal. Currently, the main therapy for SER is the three-tube method, which includes a nasogastric decompression tube, a nasojejunal enteral nutrition tube, and a chest drainage tube. However, the inflammation associated with SER persists for a long time because this management technique does not ensure effective drainage of the mediastinal inflammation and therefore renders a longer length of hospital stay. We introduced a less invasive but effective two-tube method for the treatment of SER. This technique involves the use of a trans-fistula drainage tube and a threelumen jejunal feeding tube. In our pilot study of 18 patients, 17 patients recovered smoothly and the leakages closed much more quickly than in traditional therapy. The two-tube method may have the following four advantages. (1) First, irrigation and drainage can be performed simultaneously. The irrigation frequency and the amount and composition of the irrigation solution can be adjusted according to the characteristics and quantity of the daily drainage fluid. (2) The continuous negative drainage of the tube placed within the leakage cavity may precipitate adherence of the bilateral walls to each other, accelerating closure of the leak cavity. (3) The jejunal nutrition tube enables enteral nutritional support, which not only provides ample nutrition to facilitate closure of the leakage but also decreases the incidence of late inflammation due to bacterial translocation associated with a long fasting period. (4) Finally, thoracic closed drainage is not needed for the vast majority of patients who undergo treatment with our new approach, greatly reducing pain and facilitating earlier mobilization and rehabilitation. Considering the one patient who died of severe sepsis and respiratory failure in the two-tube method group, it may be beneficial to continuously lavage and simultaneously drain the abscess cavity with negative pressure. Moreover, for patients with new-onset sepsis or uncontrolled inflammation, an earlier switch to a surgical operation may be an alternative therapy. In conclusion, the two-tube method is an effective, minimally invasive approach to the treatment of SER. The method could be utilized as an alternative therapeutic option for SER. Author contributions Liang-liang Yu: Study design, data acquisition, chart abstraction, data analysis/interpretation, manuscript drafting Zheng-fu He: Chart abstraction, data analysis/interpretation, manuscript revision
8 Yu et al Qi-fang Liu: Data analysis/interpretation, manuscript revision Ning Dai: Data acquisition, manuscript revision Jian-min Si: Data acquisition, manuscript revision Bei Ye: Data acquisition, manuscript revision Jian-cang Zhou: Study concept and design, data analysis/interpretation, manuscript revision Declaration of conflicting interest The authors declare the there is no conflict of interest. Funding This study was supported by the Medical Science and Technology Foundation of Zhejiang Province, China (Grant No. 2016KYB142) and the Zhejiang Province Key Science and Technology Innovation Team Foundation, China (Grant No. 2013TD13). References 1. Rustagi T and Majumder S. Dysphagia and spontaneous esophageal perforation in sarcoidosis. Dig Dis Sci 2013; 58: Lindenmann J, Matzi V, Neuboeck N, et al. Management of esophageal perforation in 120 consecutive patients: clinical impact of a structured treatment algorithm. J Gastrointest Surg 2013; 17: Ieta K, Oki A, Teshigahara K, et al. Recurrent spontaneous esophageal rupture. Clin J Gastroenterol 2013; 6: Walker WS, Cameron EWJ and Walbaum PR. Diagnosis and management of spontaneous transmural rupture of the oesophagus (Boerhaaves syndrome). Br J Surg 1985; 72: Van der Weg G, Wikkeling M, van Leeuwen M, et al. A rare case of oesophageal rupture: Boerhaave s syndrome. Int J Emerg Med 2014; 7: Messager M, Warlaumont M, Renaund F, et al. Recent improvements in the management of esophageal anastomotic leak after surgery for cancer. Eur J Surg Oncol 2017; 43: Zhang ZH. Univariate description and bivariate statistical inference: the first step delving into data. Ann Transl Med 2016; 4: Connelly CL, Lamb PJ and Paterson-Brown S. Outcomes following Boerhaave s syndrome. Ann R Coll Surg Engl 2013; 95: Inci S, Gundogdu F, Gungor H, et al. Misdiagnosed chest pain: spontaneous esophageal rupture. Acta Cardiol Sin 2013; 29: Korczynski P, Krenke R, Fangrat A, et al. Acute respiratory failure in a patient with spontaneous esophageal rupture (Boerhaave syndrome). Respir Care 2011; 56: Garas G, Zarogoulidis P, Efthymiou A, et al. Spontaneous esophageal rupture as the underlying cause of pneumothorax: early recognition is crucial. J Thorac Dis 2014; 6: Girard E, Messager M, Sauvanet A, et al. Anastomotic leakage after gastrointestinal surgery: diagnosis and management. J Visc Surg 2014; 151: Sulpice L, Dileon S, Rayar M, et al. Conservative surgical management of Boerhaave s syndrome: experience of two tertiary referral centers. Int J Surg 2013; 11: Crestanello JA, Deschamps C, Cassivi SD, et al. Selective management of intrathoracic anastomotic leak after esophagectomy. J Thorac Cardiovasc Surg 2005; 129: Djarv T, Derogar M and Lagergren P. Influence of co-morbidity on longterm quality of life after oesophagectomy for cancer. Br J Surg 2014; 101: Markar SR, Arya S, Karthikesalingam A, et al. Technical factors that affect anastomotic integrity following esophagectomy: systematic review and meta-analysis. Ann Surg Oncol 2013; 20: Otsuka K, Murakami M, Ariyoshi T, et al. Endoscopic clipping of spontaneous esophageal rupture: case reports of three patients. Int J Surg Case Rep 2017; 38:
9 1536 Journal of International Medical Research 46(4) 18. Rokszin R, Simonka Z, Paszt A, et al. Successful endoscopic clipping in the early treatment of spontaneous esophageal perforation. Surg Laparosc Endosc Percutan Tech 2011; 21:e311 e Ota K, Takeuchi T and Higuchi K. Temporary insertion of a covered selfexpandable metal stent for spontaneous esophagealrupture. Dig Endosc 2014; 26: Koivukangas V, Bianc ari F, Meril ainen S, et al. Esophageal stenting for spontaneous esophageal perforation. J Trauma Acute Care Surg 2012; 73:
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic management of sleeve leaks
 Endoscopic management of sleeve leaks Mr Damien Loh Oesophagogastric and Bariatric Surgeon The Alfred The clinical problem Incidence 0.1-7% Inpatient mortality 2-5% High morbidity Prolonged ICU and in-hospital
Endoscopic management of sleeve leaks Mr Damien Loh Oesophagogastric and Bariatric Surgeon The Alfred The clinical problem Incidence 0.1-7% Inpatient mortality 2-5% High morbidity Prolonged ICU and in-hospital
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
IATROGENIC OESOPHAGEAL PERFORATION
 IATROGENIC OESOPHAGEAL PERFORATION TAOLE MOKOENA DPhil FRCS PROFESSOR OF SURGERY UNIVERSITY OF PRETORIA 17 TH Controversies and Problems in Surgery Symposium 4-5 October 2013 Introduction Perforation of
IATROGENIC OESOPHAGEAL PERFORATION TAOLE MOKOENA DPhil FRCS PROFESSOR OF SURGERY UNIVERSITY OF PRETORIA 17 TH Controversies and Problems in Surgery Symposium 4-5 October 2013 Introduction Perforation of
JMSCR Volume 03 Issue 04 Page April 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x A Rare Case of Boerhaaves Syndrome Managed Conservatively Authors Dr. Vinaya Ambore 1, Dr. Vikram Wagh 2, Dr. Prashant Turkar 3, Dr. Kapil
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x A Rare Case of Boerhaaves Syndrome Managed Conservatively Authors Dr. Vinaya Ambore 1, Dr. Vikram Wagh 2, Dr. Prashant Turkar 3, Dr. Kapil
Endoscopic Management of Perforations
 Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
Original Article Treatment of postoperative intrathoracic reconstruction after digestive tract fistula in esophageal and cardiac carcinoma
 Int J Clin Exp Med 2017;10(1):802-807 www.ijcem.com /ISSN:1940-5901/IJCEM0019893 Original Article Treatment of postoperative intrathoracic reconstruction after digestive tract fistula in esophageal and
Int J Clin Exp Med 2017;10(1):802-807 www.ijcem.com /ISSN:1940-5901/IJCEM0019893 Original Article Treatment of postoperative intrathoracic reconstruction after digestive tract fistula in esophageal and
Case Presentation Surgery Grand Round. Amid Keshavarzi, MD UCHSC 4/9/2006
 Case Presentation Surgery Grand Round Amid Keshavarzi, MD UCHSC 4/9/2006 Case Presentation 12 y/o female Presented to OSH after accidental swallowing of plastic fork in the bus, CXR/AXR form OSH did not
Case Presentation Surgery Grand Round Amid Keshavarzi, MD UCHSC 4/9/2006 Case Presentation 12 y/o female Presented to OSH after accidental swallowing of plastic fork in the bus, CXR/AXR form OSH did not
FTS Oesophagectomy: minimal research to date 3,4
 Fast Track Programme in patients undergoing Oesophagectomy: A Single Centre 5 year experience Sullivan J, McHugh S, Myers E, Broe P Department of Upper Gastrointestinal Surgery Beaumont Hospital Dublin,
Fast Track Programme in patients undergoing Oesophagectomy: A Single Centre 5 year experience Sullivan J, McHugh S, Myers E, Broe P Department of Upper Gastrointestinal Surgery Beaumont Hospital Dublin,
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions
 Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Selective Nonoperative Management of Contained Intrathoracic Esophageal Disruptions John L. Cameron, M.D., Richard F. Kieffer, M.D., Thomas R. Hendrix, M.D., Denis G. Mehigan, M.., and R. Robinson aker,
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Author's response to reviews
 Author's response to reviews Title: Fully covered self-expandable metal stents (SEMS), partially covered SEMS and self-expandable plastic stents for the treatment of benign esophageal ruptures and anastomotic
Author's response to reviews Title: Fully covered self-expandable metal stents (SEMS), partially covered SEMS and self-expandable plastic stents for the treatment of benign esophageal ruptures and anastomotic
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Bin Qiu, Feiyue Feng, Shugeng Gao. Introduction
 Original Article Partial esophagogastrostomy with esophagogastric anastomosis below the aortic arch in cardiac carcinoma: characteristics and treatment of postoperative anastomotic leakage Bin Qiu, Feiyue
Original Article Partial esophagogastrostomy with esophagogastric anastomosis below the aortic arch in cardiac carcinoma: characteristics and treatment of postoperative anastomotic leakage Bin Qiu, Feiyue
A unique case of esophageal perforation caused by prickly pears
 A unique case of esophageal perforation caused by prickly pears Abstract This is a report of a previously healthy 20-yearold male presenting with the sensation of a foreign object being stuck in the throat
A unique case of esophageal perforation caused by prickly pears Abstract This is a report of a previously healthy 20-yearold male presenting with the sensation of a foreign object being stuck in the throat
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Early View Article: Online published version of an accepted article before publication in the final form.
 : Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title: What is the treatment
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Left Sided Chest Pain: A Case Report of Boerhaave Syndrome Mimicking Acute Coronary Syndrome
 664 Left Sided Chest Pain: A Case Report of Boerhaave Syndrome Mimicking Acute Coronary Syndrome Hoo F.K. 1 *, Lee S.H. 2, Shariful Hasan 1, Wan Aliaa WS 1, Mohd Sazlly Lim S 1, Hamidon Basri 1 1 Department
664 Left Sided Chest Pain: A Case Report of Boerhaave Syndrome Mimicking Acute Coronary Syndrome Hoo F.K. 1 *, Lee S.H. 2, Shariful Hasan 1, Wan Aliaa WS 1, Mohd Sazlly Lim S 1, Hamidon Basri 1 1 Department
Esophageal injuries. Pre-test /11/10. 新光急診張志華醫師 Facebook.com/jack119. O What is the most common cause of esophageal injuries?
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Is Endoluminal Vacuum Therapy Sponge Worthy? Benny Weksler, MD PII: S0022-5223(18)32263-3 DOI: 10.1016/j.jtcvs.2018.08.021 Reference: YMTC 13343 To appear in: The Journal of Thoracic
Accepted Manuscript Is Endoluminal Vacuum Therapy Sponge Worthy? Benny Weksler, MD PII: S0022-5223(18)32263-3 DOI: 10.1016/j.jtcvs.2018.08.021 Reference: YMTC 13343 To appear in: The Journal of Thoracic
ESOPHAGEAL PERFORATION. Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013
 ESOPHAGEAL PERFORATION Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013 OUTLINE Risk factors Diagnosis Management GOALS Make sure you don t miss it If
ESOPHAGEAL PERFORATION Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013 OUTLINE Risk factors Diagnosis Management GOALS Make sure you don t miss it If
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Reliable management of post-esophagectomy anastomotic fistula with endoscopic trans-fistula negative pressure drainage
 Liu et al. World Journal of Surgical Oncology 2014, 12:240 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Reliable management of post-esophagectomy anastomotic fistula with endoscopic trans-fistula
Liu et al. World Journal of Surgical Oncology 2014, 12:240 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Reliable management of post-esophagectomy anastomotic fistula with endoscopic trans-fistula
A video demonstration of the Li s anastomosis the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma
 Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Surgical Technique A video demonstration of the the key part of the non-tube no fasting fast track program for resectable esophageal carcinoma Yan Zheng*, Yin Li*, Zongfei Wang, Haibo Sun, Ruixiang Zhang
Adult Trauma Feeding Access Guideline
 Adult Trauma Feeding Access Guideline Background: Enteral feeding access mode (NGT, NDT, PEG, PEG-J, Jejunostomy tube) dependent upon patient characteristics. Enteral feeding management guidelines aim
Adult Trauma Feeding Access Guideline Background: Enteral feeding access mode (NGT, NDT, PEG, PEG-J, Jejunostomy tube) dependent upon patient characteristics. Enteral feeding management guidelines aim
How I Do It? Per-oral Endoscopic Myotomy (POEM) Ping-hong ZHOU, MD. Endoscopy Center, Zhongshan Hospital Fudan University, Shanghai, China
 How I Do It? Per-oral Endoscopic Myotomy (POEM) Ping-hong ZHOU, MD Endoscopy Center, Zhongshan Hospital Fudan University, Shanghai, China The 2 nd World Congress on CONTROVERSIES IN GASTROENTEROLOGY Prof.
How I Do It? Per-oral Endoscopic Myotomy (POEM) Ping-hong ZHOU, MD Endoscopy Center, Zhongshan Hospital Fudan University, Shanghai, China The 2 nd World Congress on CONTROVERSIES IN GASTROENTEROLOGY Prof.
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 9 ISSUE 1 Perforation Of The Caecum Owing To Benign Rectal Obstruction: A Paradigm Of Damage Control In Emergency Colorectal Surgery DIMITRIOS
World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 9 ISSUE 1 Perforation Of The Caecum Owing To Benign Rectal Obstruction: A Paradigm Of Damage Control In Emergency Colorectal Surgery DIMITRIOS
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
REPEATED INTRANODAL LYMPHANGIOGRAPHY FOR THE TREATMENT OF LYMPHATIC LEAKAGE
 59 Lymphology 48 (2015) 59-63 REPEATED INTRANODAL LYMPHANGIOGRAPHY FOR THE TREATMENT OF LYMPHATIC LEAKAGE S. Kariya, M. Nakatani, R. Yoshida, Y. Ueno, A. Komemushi, N. Tanigawa Department of Radiology,
59 Lymphology 48 (2015) 59-63 REPEATED INTRANODAL LYMPHANGIOGRAPHY FOR THE TREATMENT OF LYMPHATIC LEAKAGE S. Kariya, M. Nakatani, R. Yoshida, Y. Ueno, A. Komemushi, N. Tanigawa Department of Radiology,
Managing esophageal fistulae by endoscopic transluminal drainage in esophageal cancer patients with superior mediastinal sepsis after esophagectomy
 Chinese Journal of Cancer Case Research Managing esophageal fistulae by endoscopic transluminal drainage in esophageal cancer patients with superior mediastinal sepsis after esophagectomy Yu-Zhen Zheng
Chinese Journal of Cancer Case Research Managing esophageal fistulae by endoscopic transluminal drainage in esophageal cancer patients with superior mediastinal sepsis after esophagectomy Yu-Zhen Zheng
Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article
 Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article Authors: Dr Vaibhav Pandey 1*, Dr. Pranay Panigrahi 2 Srivastav 4 & Dr Rakesh Kumar
Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article Authors: Dr Vaibhav Pandey 1*, Dr. Pranay Panigrahi 2 Srivastav 4 & Dr Rakesh Kumar
Long Term Follow-up. 6 Month 1 Year Annual enter year #: What is the assessment date: / / Unknown. Is the patient alive? Yes No
 Long Term Follow-up 6 Month 1 Year Annual enter year #: What is the assessment date: / / Unknown Is the patient alive? Yes No Was an exam performed by a bariatric physician or PA/NP? Yes No Was the patient
Long Term Follow-up 6 Month 1 Year Annual enter year #: What is the assessment date: / / Unknown Is the patient alive? Yes No Was an exam performed by a bariatric physician or PA/NP? Yes No Was the patient
Departement of Surgery Faculty of Medicine University Sumatera Utara
 SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
Fluoroscopy-Guided Endoscopic Removal of Foreign Bodies
 CASE REPORT Clin Endosc 2017;50:197-201 https://doi.org/10.5946/ce.2016.085 Print ISSN 2234-2400 / On-line ISSN 2234-2443 Open Access Fluoroscopy-Guided Endoscopic Removal of Foreign odies Junhwan Kim
CASE REPORT Clin Endosc 2017;50:197-201 https://doi.org/10.5946/ce.2016.085 Print ISSN 2234-2400 / On-line ISSN 2234-2443 Open Access Fluoroscopy-Guided Endoscopic Removal of Foreign odies Junhwan Kim
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN)
 An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula
 European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
European Radiology Springer-Verlag 2003 DOI 10.1007/s00330-002-1818-z Tips and Tricks in Radiology Covered stenting in patients with lifting of gastric and high esophago-tracheal fistula T. Lehnert J.
Current Management of Postpneumonectomy Bronchopleural Fistula
 Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
Conference Report United European Gastroenterology Week (UEGW) 2016
 Conference Report United European Gastroenterology Week (UEGW) 2016 HemoPill acute trial - non-invasive detection of upper GI bleeding feasible and safe Swiss FTRD trial - 94% R0-resection of colonic non-lifting
Conference Report United European Gastroenterology Week (UEGW) 2016 HemoPill acute trial - non-invasive detection of upper GI bleeding feasible and safe Swiss FTRD trial - 94% R0-resection of colonic non-lifting
Mortality Secondary to Esophageal Anastomotic Leak
 Original Article Mortality Secondary to Esophageal Anastomotic Leak Khaled Alanezi, MD, and John D. Urschel, MD Background: Esophageal anastomotic leak is a potentially life threatening complication of
Original Article Mortality Secondary to Esophageal Anastomotic Leak Khaled Alanezi, MD, and John D. Urschel, MD Background: Esophageal anastomotic leak is a potentially life threatening complication of
Treatment of esophageal anastomotic leakage with self-expanding metal stents: analysis of risk factors for treatment failure
 E420 Treatment of esophageal anastomotic leakage with self-expanding metal stents: analysis of risk factors for treatment failure Authors Saga Persson 1, Ioannis Rouvelas 1, Koshi Kumagai 1, Huan Song
E420 Treatment of esophageal anastomotic leakage with self-expanding metal stents: analysis of risk factors for treatment failure Authors Saga Persson 1, Ioannis Rouvelas 1, Koshi Kumagai 1, Huan Song
Key words: gastric cancer, postoperative complication, total gastrectomy
 Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Diaphragmatic Hernia Presenting With Intrathoracic Perforation
 ISPUB.COM The Internet Journal of Surgery Volume 2 Number 1 Diaphragmatic Hernia Presenting With Intrathoracic Perforation A ERDOGAN Citation A ERDOGAN.. The Internet Journal of Surgery. 2000 Volume 2
ISPUB.COM The Internet Journal of Surgery Volume 2 Number 1 Diaphragmatic Hernia Presenting With Intrathoracic Perforation A ERDOGAN Citation A ERDOGAN.. The Internet Journal of Surgery. 2000 Volume 2
Esophageal Bypass Using a Gastric Tube for a Malignant Tracheoesophageal/ Bronchoesophageal Fistula: A Report of 4 Cases
 Int Surg 2011;96:189 193 Case Report Esophageal Bypass Using a Gastric Tube for a Malignant Tracheoesophageal/ Bronchoesophageal Fistula: A Report of 4 Cases Takeshi Hanagiri, Masaru Morita, Yoshiki Shigematsu,
Int Surg 2011;96:189 193 Case Report Esophageal Bypass Using a Gastric Tube for a Malignant Tracheoesophageal/ Bronchoesophageal Fistula: A Report of 4 Cases Takeshi Hanagiri, Masaru Morita, Yoshiki Shigematsu,
Science & Technologies
 A GIANT LIVER HYDATIDE CYST SIMULTANEOUSLY PERFORATED TO PERITONEAL AND PLEURAL CAVITIES A RARE CASE REPORT. Ivan P. Novakov Department of Special Surgery; Medical University - Plovdiv Abstract. Background.
A GIANT LIVER HYDATIDE CYST SIMULTANEOUSLY PERFORATED TO PERITONEAL AND PLEURAL CAVITIES A RARE CASE REPORT. Ivan P. Novakov Department of Special Surgery; Medical University - Plovdiv Abstract. Background.
Delayed Perforation Occurring after Endoscopic Submucosal Dissection for Early Gastric Cancer
 CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
Comparative Study for the Efficacy of Small Bore Catheter in the Patients with Iatrogenic Pneumothorax
 Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Original Article. Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome
 Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
Tropical Gastroenterology 2015;36(1):31 35 Original Article Gastrointestinal bleeding in acute pancreatitis: etiology, clinical features, risk factors and outcome Surinder S Rana 1, Vishal Sharma 1, Deepak
Review Article The Use of Self-Expanding Plastic Stents in the Management of Oesophageal Leaks and Spontaneous Oesophageal Perforations
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2011, Article ID 418103, 6 pages doi:10.1155/2011/418103 Review Article The Use of Self-Expanding Plastic Stents in the Management
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2011, Article ID 418103, 6 pages doi:10.1155/2011/418103 Review Article The Use of Self-Expanding Plastic Stents in the Management
Jejunostomy after oesophagectomy, how and why I do it
 Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
Jejunostomy after oesophagectomy, how and why I do it Graeme Couper. Consultant Oesophago-gastric Surgeon, The Royal Infirmary of Edinburgh BAPEN Conference 2010 2nd & 3rd November Harrogate International
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study
 Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Original article: Comparison Between Primary Closure of Common Bile Duct and T- Tube Drainage After Open Choledocholithiasis: A Hospital Based Study Kali CharanBansal Principal Specialist (General surgery)
Anastomotic Complications after Esophagectomy. Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine
 Anastomotic Complications after Esophagectomy Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine Use of Stomach as Conduit Simplest choice after esophagectomy Single anastomosis
Anastomotic Complications after Esophagectomy Bryan Meyers, MD MPH Thoracic Surgery Washington University School of Medicine Use of Stomach as Conduit Simplest choice after esophagectomy Single anastomosis
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
MATERIALS AND METHODS Patients
 Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Recurrent Retropharyngeal Abscess with Esophageal Perforation due to Chopstick Injury
 Recurrent Retropharyngeal Abscess with Esophageal Perforation due to Chopstick Injury Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Recurrent Retropharyngeal Abscess with Esophageal Perforation due to Chopstick Injury Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Intramural esophageal hematoma: Dissection of the perforation
 Case report Intramural esophageal hematoma: Dissection of the perforation Martin Gómez Zuleta, MD, 1 Álvaro Rodríguez Gómez, MD, 2 Amaranto Siado, MD. 3 1 Assistant Professor in the Gastroenterology Unit
Case report Intramural esophageal hematoma: Dissection of the perforation Martin Gómez Zuleta, MD, 1 Álvaro Rodríguez Gómez, MD, 2 Amaranto Siado, MD. 3 1 Assistant Professor in the Gastroenterology Unit
Gallstone ileus:diagnostic and therapeutic dilemma
 Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Saurabh et al. 1 CASE SERIES OPEN ACCESS Gallstone ileus:diagnostic and therapeutic dilemma Shireesh Saurabh, Andrew Camerota, Jeffrey Zavotsky ABSTRACT Introduction: Gallstone ileus is a rare complication
Esophageal perforations are challenging to manage and are
 Endoscopic Techniques for the Management of Esophageal Perforation Karen Joanna Dickinson, MBBS, BSc, MD, FRCS, and Shanda H. Blackmon, MD, MPH Esophageal perforations or leaks can be spontaneous, iatrogenic,
Endoscopic Techniques for the Management of Esophageal Perforation Karen Joanna Dickinson, MBBS, BSc, MD, FRCS, and Shanda H. Blackmon, MD, MPH Esophageal perforations or leaks can be spontaneous, iatrogenic,
Is surgical Apgar score an effective assessment tool for the prediction of postoperative complications in patients undergoing oesophagectomy?
 Interactive CardioVascular and Thoracic Surgery 27 (2018) 686 691 doi:10.1093/icvts/ivy148 Advance Access publication 9 May 2018 BEST EVIDENCE TOPIC Cite this article as: Li S, Zhou K, Li P, Che G. Is
Interactive CardioVascular and Thoracic Surgery 27 (2018) 686 691 doi:10.1093/icvts/ivy148 Advance Access publication 9 May 2018 BEST EVIDENCE TOPIC Cite this article as: Li S, Zhou K, Li P, Che G. Is
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
Penetrating Wounds of the Esophagus
 Panagiotis N. Symbas, M.D., Denis H. Tyras, M.D., Charles R. Hatcher, Jr., M.D., and Byron Perry, M.D. ABSTRACT The histories of 22 patients with perforation of the esophagus from bullet or stab wounds
Panagiotis N. Symbas, M.D., Denis H. Tyras, M.D., Charles R. Hatcher, Jr., M.D., and Byron Perry, M.D. ABSTRACT The histories of 22 patients with perforation of the esophagus from bullet or stab wounds
Spotlight on Esophageal Perforation A multinational study using the Pittsburgh Esophageal Perforation Severity Scoring System
 Spotlight on Esophageal Perforation A multinational study using the Pittsburgh Esophageal Perforation Severity Scoring System Michael Schweigert Department of Thoracic Surgery Objective Esophageal perforation
Spotlight on Esophageal Perforation A multinational study using the Pittsburgh Esophageal Perforation Severity Scoring System Michael Schweigert Department of Thoracic Surgery Objective Esophageal perforation
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
VIDEO ASSISTED RETROPERITONEAL DEBRIDEMENT IN HUGE INFECTED PANCREATIC PSEUDOCYST
 Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Esophageal Stent Placement for the Treatment of Acute Intrathoracic Anastomotic Leak After Esophagectomy
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse
 The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
The Percutaneous Endoscopic Gastrostomy Geoffrey Axiak M.Sc. Nursing (Manch.), B.Sc. Nursing, P.G. Dip. Nutrition & Dietetics Clinical Nutrition Practice Nurse What is a P.E.G.? Percutaneous Endoscopic
Michele Bettinelli RN CCRN Lahey Health and Medical Center
 Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Michele Bettinelli RN CCRN Lahey Health and Medical Center Differentiate the types of varices Identify glue preparations utilized when treating gastric varices Review the process of glue administration
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
BURIED BUMPER SYNDROME: A RARE COMPLICATION OF PERCUTANEOUS ENDOSCOPIC GASTROSTOMY
 BURIED BUMPER SYNDROME: A RARE COMPLICATION OF PERCUTANEOUS ENDOSCOPIC GASTROSTOMY Farhan Khan, Tan Xiao Ping* and Umesh Guragain Department of Gastroenterology, The Affiliated Hospital of Yangtze Medical
BURIED BUMPER SYNDROME: A RARE COMPLICATION OF PERCUTANEOUS ENDOSCOPIC GASTROSTOMY Farhan Khan, Tan Xiao Ping* and Umesh Guragain Department of Gastroenterology, The Affiliated Hospital of Yangtze Medical
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Case discussion. Anastomotic leakage. intern superviser
 Case discussion Anastomotic leakage intern superviser Basic data Name : XX ID: M101881671 Age:51 Y Gender: male Past history: Hospitalized for acute diverticulitis on 2004/7/17, 2005/5/28 controlled by
Case discussion Anastomotic leakage intern superviser Basic data Name : XX ID: M101881671 Age:51 Y Gender: male Past history: Hospitalized for acute diverticulitis on 2004/7/17, 2005/5/28 controlled by
Extreme Endo Toolbox. Slide 1. Slide 2. Slide 3. Outline. Endo Toolbox - Requisites
 Slide 1 Extreme Endo Toolbox Pramod Malik, MD, FACG, FASGE, AGAF, CPI Gastroenterology Associates of Tidewater Slide 2 Outline New Tools - Confocal endomicroscopy (Cellvizio) - HD/ NBI/ FICE - Ovesco clip
Slide 1 Extreme Endo Toolbox Pramod Malik, MD, FACG, FASGE, AGAF, CPI Gastroenterology Associates of Tidewater Slide 2 Outline New Tools - Confocal endomicroscopy (Cellvizio) - HD/ NBI/ FICE - Ovesco clip
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil
 Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Nutritional Management in Enterocutaneous fistula Dr Deepak Govil MS, PhD (GI Surgery) Senior Consultant Surgical Gastroenterology Indraprastha Apollo Hospital New Delhi What is enterocutaneous fistula
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment)
 Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Surgery for Complications of Peptic Ulcer Disease (Definitive Treatment) Amid Keshavarzi, MD UCHSC Grand Round 3/20/2006 Department of Surgery Introduction Epidemiology Pathophysiology Clinical manifestation
Since central airway stenosis is often a lifethreatening. Double Y-stenting for tracheobronchial stenosis. Masahide Oki and Hideo Saka
 Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL
 SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
SIGNIFICANCE OF EXTRALUMINAL ABDOMINAL GAS: LOOKING FOR AIR IN ALL THE WRONG PLACES Richard M. Gore, MD North Shore University Health System University of Chicago Evanston, IL SCBT/MR 2012 October 26,
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Classification and Management of Leaks after Gastric Bypass for Patients with Morbid Obesity: A Prospective Study of 60 Patients
 OBES SURG (2012) 22:855 862 DOI 10.1007/s11695-011-0519-6 CLINICAL REPORT Classification and Management of Leaks after Gastric Bypass for Patients with Morbid Obesity: A Prospective Study of 60 Patients
OBES SURG (2012) 22:855 862 DOI 10.1007/s11695-011-0519-6 CLINICAL REPORT Classification and Management of Leaks after Gastric Bypass for Patients with Morbid Obesity: A Prospective Study of 60 Patients
Abdominal Compartment Syndrome. Jeff Johnson, MD
 Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
SciFed Journal of Public Health. Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature
 SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
SciFed Journal of Public Health Case Report Open Access Endoscopic Management of Obstetrical Uretero-Uterine Fistula. Case Report and Review of Literature * Yasin Idweini * Chairperson of Urology Department
Not over when the surgery is done: surgical complications of obesity
 Not over when the surgery is done: surgical complications of obesity Gianluca Bonanomi, MD, FRCS Consultant Surgeon and Honorary Senior Lecturer Chelsea and Westminster Hospital London The Society for
Not over when the surgery is done: surgical complications of obesity Gianluca Bonanomi, MD, FRCS Consultant Surgeon and Honorary Senior Lecturer Chelsea and Westminster Hospital London The Society for
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
2018 International Conference on Medicine, Biology, Materials and Manufacturing (ICMBMM 2018)
 2018 International Conference on Medicine, Biology, Materials and Manufacturing (ICMBMM 2018) Clinical Study on the Treatment of Metastatic Malignant Bowel Obstruction with Transgastric Intestinal Obstruction
2018 International Conference on Medicine, Biology, Materials and Manufacturing (ICMBMM 2018) Clinical Study on the Treatment of Metastatic Malignant Bowel Obstruction with Transgastric Intestinal Obstruction
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Management of esophageal anastomotic leaks, perforations, and fistulae with self-expanding plastic stents
 Management of esophageal anastomotic leaks, perforations, and fistulae with self-expanding plastic stents Yiyang Dai, MD, a Sascha S. Chopra, MD, b S oren Kneif, PhD, a and Michael H unerbein, MD, PhD
Management of esophageal anastomotic leaks, perforations, and fistulae with self-expanding plastic stents Yiyang Dai, MD, a Sascha S. Chopra, MD, b S oren Kneif, PhD, a and Michael H unerbein, MD, PhD
