Outcomes of Biventricular Repair for Congenitally Corrected Transposition of the Great Arteries
|
|
|
- Sherilyn Walters
- 6 years ago
- Views:
Transcription
1 Outcomes of Biventricular Repair for Congenitally Corrected Transposition of the Great Arteries Hong-Gook Lim, MD, PhD, Jeong Ryul Lee, MD, PhD, Yong Jin Kim, MD, PhD, Young-Hwan Park, MD, PhD, Tae-Gook Jun, MD, PhD, Woong-Han Kim, MD, PhD, Chang-Ha Lee, MD, PhD, Han Ki Park, MD, PhD, Ji-Hyuk Yang, MD, Chun-Soo Park, MD, and Jae Gun Kwak, MD Department of Thoracic and Cardiovascular Surgery, Seoul National University College of Medicine, Seoul National University Children s Hospital, Xenotransplantation Research Center, Seoul National University Hospital, Transplantation Research Institute, Medical Research Center, Seoul National University, Department of Thoracic and Cardiovascular Surgery, Yonsei University College of Medicine, and Department of Thoracic and Cardiovascular Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, and Department of Thoracic and Cardiovascular Surgery, Sejong General Hospital, Sejong Heart Institute, Bucheon, Korea Background. This study was undertaken to evaluate long-term results of biventricular repairs for congenitally corrected transposition of the great arteries, and to analyze the risk factors that affect mortality and morbidity. Methods. Between 1983 and 2009, 167 patients with congenitally corrected transposition of the great arteries underwent biventricular repairs. The physiologic repairs were performed in 123 patients, and anatomic repairs in 44. Average follow-up was years. Results. Kaplan-Meier estimated survival was 83.3% 0.5% at 25 years in biventricular repair. In anatomic repair, left ventricular training and right ventricular dysfunction had negative impact on survival, but bidirectional cavopulmonary shunt had positive impact on survival. The reoperation-free ratio was 10.1% 7.8% at 22 years after physiologic repair, and 46.2% 12.4% at 15 years after anatomic repair (p 0.885). Freedom from any arrhythmia was 49.6% 7.5% at 22 years after physiologic repair, and 60.8% 14.8% at 18 years after anatomic repair (p 0.458). Freedom from systemic atrioventricular valve and ventricular dysfunction as well as tricuspid valve and right ventricular dysfunction was significantly higher in anatomic repair than in physiologic repair. Conclusions. Long-term results of biventricular repair were satisfactory. Patients presenting with right ventricular dysfunction or need for left ventricular training represent a high-risk group of anatomic repair for which selection criteria are particularly important. Late functional outcomes of anatomic repair were excellent compared with physiologic repair. Anatomic repair is the procedure of choice for those patients if both ventricles are adequate or if surgical technique is modified with the help of additional a bidirectional cavopulmonary shunt. (Ann Thorac Surg 2010;89:159 67) 2010 by The Society of Thoracic Surgeons Congenitally corrected transposition of the great arteries (CCTGA) is characterized by atrioventricular (AV) and ventriculoarterial discordance [1]. The optimal surgical management of patients with CCTGA is still to be determined. The early results after physiologic repair are on the whole quite good; however, the results in the medium to long term are disappointing. A particular problem with physiologic repair seems to be a high incidence of late death caused by cardiac failure [2 5]. Concerns about the long-term function of the morphologic right ventricle (RV) and the systemic AV valve (tricuspid) have led to the concept of anatomic repair that incorporates the morphologically left ventricle (LV) and morphologically left AV valve (mitral) in the systemic circulation [6]. Accepted for publication Aug 25, Address correspondence to Dr Lee, Department of Thoracic and Cardiovascular Surgery, Seoul National University College of Medicine, 28 Yongon-dong, Jongro-gu, Seoul, , Korea; jrl@plaza.snu. ac.kr. In 1990, Dr Ilbawi [6] reported success with anatomic repair for AV discordance as an alternative to physiologic repair. Ilbawi s contribution of using the LV in the systemic circulation expanded the options for these patients [7 9]. Advantages in terms of RV and tricuspid valve (TV) function combined with low operative morbidity and mortality, and the fact that the LV becomes the systemic ventricle, have resulted in the application of this procedure to almost all patients with CCTGA, despite its complexity [10 13]. So far, no study has analyzed the long-term results of biventricular repair including one-and-a-half ventricular repair for CCTGA. Because of the relative rarity of suitable candidates, we included data from four institutions. So, the present multicenter study seeks to evaluate the outcome of biventricular repair for CCTGA, and to analyze the factors that predict outcomes after biventricular repair. In particular, we wish to compare longterm outcomes after physiologic versus anatomic repair for CCTGA, and evaluate the impact of additional bidirectional cavopulmonary shunt on survival by The Society of Thoracic Surgeons /10/$36.00 Published by Elsevier Inc doi: /j.athoracsur
2 160 LIM ET AL Ann Thorac Surg CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 2010;89: Abbreviations and Acronyms AV atrioventricular CCTGA congenitally corrected transposition of the great arteries LV left ventricle PA pulmonary artery PSVT paroxysmal supraventricular tachycardia PV pulmonary ventricle RV right ventricle TV tricuspid valve VSD ventricular septal defect Material and Methods Institutional Review Board approval was obtained for the conduct of this retrospective study, and as individual patients were not identified, individual patient consent for the study was waived. Data collection was performed following strict guidelines to protect patient information. Between 1983 and 2009, a total of 167 patients (median age 4.1 years; range, 1 months to 61.9 years old) with CCTGA underwent biventricular repairs for CCTGA in four institutions. Medical records, preoperative and postoperative echocardiograph data, and cardiac catheterization data and operative notes were reviewed. Of the 167 patients, 141 were situs solitus and 26 were situs inversus; 135 patients had ventricular septal defect (VSD). Regarding pulmonary outflow tract, 41 patients had no pulmonary stenosis, 74 had pulmonary stenosis, and 52 pulmonary atresia. Fifty-four patients underwent preoperative Blalock-Taussig shunt. The severity of AV valve regurgitation was graded as I (jet area/atrial area 10%); II (jet area/atrial area 10% to 20%); III (jet area/atrial area 20% to 33%); and IV (jet area/atrial area 33%), and valvar dysfunction was defined as regurgitation of grade II and more. Ventricular function was judged as good, mild, moderate, and severe dysfunction; and ventricular dysfunction was defined as mild to moderate dysfunction and worse. In physiologic repair, the mean grade of tricuspid regurgitation (TR) was The grade of TR was 0 in 56 patients, I in 22, I to II in 1, II in 18, II to III in 2, III in 9, and IV in 15. In anatomic repair, the mean grade of TR was The grade of TR was 0 in 19 patients, I in 7, I to II in 5, II in 6, II to III in 4, III in 2, and IV in 1. For physiologic repair, RV function was good in 94 patients, with mild dysfunction in 13, mild to moderate dysfunction in 9, and severe dysfunction in 7. For anatomic repair, RV function was good in 27 patients, with mild dysfunction in 7, mild to moderate dysfunction in 6, moderate dysfunction in 2, and severe dysfunction in 2. For physiologic repair, preoperative rhythm was sinus in 113 patients, and for anatomic repair, it was sinus in 41. For physiologic repair, preoperative arrhythmia occurred in 10 patients. Complete AV block occurred in 4 patients (3 required intraoperative permanent pacemaker), second-degree AV block in 1, atrial fibrillation in 3, and intermittent paroxysmal supraventricular tachycardia (PSVT) in 2. For anatomic repair, preoperative arrhythmia occurred in 3 patients. Complete AV block occurred in 2 patients (requiring preoperative permanent pacemaker), and intermittent PSVT in 1. The physiologic repairs consisted of atrial septal defect or VSD closure in 14 patients, TV surgery in 21, pulmonary ventricle (PV) to pulmonary artery (PA) conduit interposition in 54, relief of PV outflow tract obstruction in 26, and réparation à l étage ventriculaire in 8. The anatomic repairs were double-switch operation (atrial switch plus arterial switch) in 10 patients, and atrial switch plus intraventricular rerouting (with or without extracardiac conduits) in 34 (see the Appendix). Five patients underwent physiologic one-and-a-half ventricular repair, and 14 underwent anatomic one-and-a-half ventricular repair. Statistical analyses were performed using SPSS version 17.0 software (SPSS, Chicago, IL). Data are presented as mean SD or median with ranges, as appropriate. The 2 test was used to compare categorical variables, and the t tests for continuous variables. Estimated survival and freedom from events including reoperation, arrhythmia, AV valve regurgitation, and ventricular dysfunction were determined by the Kaplan-Meier method. Variables were evaluated using by the likelihood ratio test in the Cox proportional hazards regression model. Hazard ratios with 95% confidence intervals were constructed for the significant multivariable predictors. A p value of less than 0.05 was set as the level of statistical significance. Results Early mortality was 7.2%. Patients were followed for years (range, 0 to 24.9). Late mortality was 4.5%. The Kaplan-Meier survival rate was 92.8% 0.2% at 1 year, 87.6% 2.8% at 10 years, and 83.3% 0.5 % at 25 years in biventricular repair (Fig 1). The cause of mortality included low cardiac output syndrome in 6 patients, arrhythmia in 4, heart failure in 3, respiratory arrest in 1, disseminated intravascular coagulopathy in 1, ventricular dysfunction in 1, thromboembolism in 1, fungal endocarditis in 1, and mediastinitis in 1 (Table 1). Postoperative complications occurred in 53 patients (31.7%). After physiologic repair, complications occurred in 38 patients (30.9%), including arrhythmia in 23, TR in 1, acute respiratory distress syndrome in 1, and transient seizure in 1. After anatomic repair, complications occurred in 15 patients (34.1%), including arrhythmia in 5, low cardiac output syndrome in 2, neurologic complication in 2, atrial baffle stenosis in 2, and acute renal failure in 1 (p 0.70). Reoperations were required in 71 patients (45.8%). After physiologic repair, reoperations were required in 60 patients (50.9%), and after anatomic repair, in 11 (29.7%) (Fig 1). With physiologic repair, reoperations included conduit change in 33 patients, TV replacement in 22, permanent pacemaker implantation in 11, pulmonic valve replacement in 7, PA angioplasty in 7, TV repair in 5, relief of PV outflow tract obstruction in 4, mitral valve repair in 3, aortic valve repair in 2, mitral valve repair in 1, left ventricular outflow tract widening in 1, bidirectional cavopulmonary shunt in 1,
3 Ann Thorac Surg LIM ET AL 2010;89: CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 161 Fig 1. Kaplan-Meier curves for survival, reoperation, and arrhythmia. (A) The probability of survival, in years, for the whole group (n 167). (B) Survival excluding hospital operative mortality. (C) Freedom from reoperation. (D) Freedom from arrhythmia. (a) Anatomic repair. (b) Physiologic repair. Maze in 1, and implantable cardioverter defibrillator in 1. With anatomic repair, reoperations included conduit change in 10 patients, venous pathway widening in 5, subaortic membrane resection in 2, PA angioplasty in 2, left ventricular outflow tract widening in 2, pulmonic valve replacement in 1, TV replacement in 1, and permanent pacemaker implantation in 1 (Table 2). Arrhythmias occurred in 49 patients (29.3%). Arrhythmias after physiologic repair occurred in 40 (32.5%), and after anatomic repair, in 9 (20.5%) (Fig 1). After physiologic repair, complete AV block occurred in 27 patients (including permanent pacemaker implantation in 23), atrial fibrillation in 9, PSVT in 7, atrial flutter in 3, sinus node dysfunction in 2, ventricular tachycardia in 1, and ventricular fibrillation in 1 (requiring implantable cardioverter defibrillator). After anatomic repair, complete AV block requiring permanent pacemaker implantation occurred in 3, atrial flutter in 5, PSVT in 2, ventricular tachycardia in 1, and first-degree AV block in 1. The freedom from tachyarrhythmia was 72.8% 7.9% at 23 years after physiologic repair, and 68.2% 16.1% at 18 years after anatomic repair (p 0.296). The freedom from bradyarrhythmia was 69.3% 5.2% at 25 years after physiologic repair, and 83.8% 6.4% at 18 years after anatomic repair (p 0.301). The incidence of complete AV block during follow-up after operation was significantly lower for anatomic repair group (6.8%) than for physiologic repair (22.0%; p 0.03), and also tended to be lower for Rastelli-type anatomic repair (3.2%) than for double-switch repair (15.4%; p 0.14) (Table 3). Last follow-up echocardiography results after physiologic repair were available for 123 patients at a follow-up duration of years (range, 0 to 24). The grade of TR was 0 in 12 patients, I in 27, I to II in 15, II in 18, II to III in 6, III in 6, III to IV in 1, and IV in 17 (excluding TV replacement in 21). The mean grade of TR was ; the TR was significantly deteriorated as compared with the preoperative TR of (p 0.001). The RV function was good in 52 patients, with mild dysfunction in 21, mild to moderate dysfunction in 27, moderate dysfunction in 7, and severe dysfunction in 16; the RV function was significantly deteriorated as compared with preoperative RV function (p 0.001). Last follow-up echocardiography results after anatomic repair were
4 162 LIM ET AL Ann Thorac Surg CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 2010;89: Table 1. Risk Factors for Mortality in Biventricular Repair Univariable Multivariable Variable HR 95% CI p Value HR 95% CI p Value Biventricular repair Arrhythmia Pulmonary stenosis Pulmonary atresia Ventricular septal defect Preoperative PAB Preoperative shunt BCPS Tricuspid regurgitation RV dysfunction Physiologic repair CPB time Aortic cross-clamp time Age Physiologic repair Arrhythmia Pulmonary stenosis Pulmonary atresia Ventricular septal defect Preoperative shunt BCPS Tricuspid regurgitation RV dysfunction CPB time Aortic cross-clamp time Age Anatomic repair Arrhythmia Pulmonary stenosis Pulmonary atresia Ventricular septal defect Preoperative shunt Preoperative PAB LV training Tricuspid regurgitation RV dysfunction Age CPB time Aortic cross-clamp time Mustard/Senning ASO/Rastelli BCPS Complete AV block ASO arterial switch operation; AV atrioventricular; BCPS bidirectional cavopulmonary shunt; CI confidence interval; CPB cardiopulmonary bypass; HR hazard ratio; LV left ventricle; PAB pulmonary artery banding; RV right ventricle. available for 44 patients at a follow-up duration of years (range, 0 to 18.5). The grade of TR was 0 in 19 patients, I in 11, I to II in 6, II in 2, II to III in 3, and III in 3. The mean grade of TR was As compared with preoperative TR of , no change was observed (p 0.367). The RV function was good in 34 patients, with mild dysfunction in 5, and mild to moderate dysfunction in 5; the RV function was significantly improved as compared with preoperative RV function (p 0.002). The grade of mitral regurgitation was 0 in 19 patients, I in 7, I to II in 8, II in 3, and III in 1. The mean grade of mitral regurgitation was The LV
5 Ann Thorac Surg LIM ET AL 2010;89: CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 163 Table 2. Risk Factors for Reoperation Univariable Multivariable Variable HR 95% CI p Value HR 95% CI p Value Pulmonary stenosis Pulmonary atresia Ventricular septal defect Preoperative PAB Preoperative shunt Tricuspid regurgitation RV dysfunction Age Physiologic repair BCPS CPB time Aortic cross-clamp time Arrhythmia BCPS bidirectional cavopulmonary shunt; CI confidence interval; CPB cardiopulmonary bypass; HR hazard ratio; PAB pulmonary artery banding; RV right ventricle. function was good in 35 patients, with mild dysfunction in 6, mild to moderate dysfunction in 1, moderate dysfunction in 1, and severe dysfunction in 1. Freedom from systemic AV valve and ventricular dysfunction as well as from TV and RV dysfunction were significantly higher after anatomic repair than after physiologic repair (Fig 2). Follow-up data after physiologic repair were available for 111 patients at the follow-up duration of years (range, 0 to 24.9). The last follow-up rhythm was sinus in 81 patients (including intermittent PSVT in 3), pacing in 25 (including atrial fibrillation in 1), and atrial fibrillation in 5. Follow-up data after anatomic repair were available for 37 patients at the follow-up duration of years (range, 0.4 to 18.5). The last follow-up rhythm was sinus in 34 patients, and pacing in 3 (p 0.017). After physiologic repair, 97 patients met the criteria for New York Heart Association functional class I, 11 met criteria for class II, and 3 met criteria for class III. After anatomic repair, 34 patients met the criteria for the New York Heart Association functional class I, and 2 who had moderate aortic regurgitation and LV dysfunction after the anatomic repair with arterial switch, met criteria for class II; 1 had neurologic complication (p 0.46). Comment This study not only is one of the largest cohorts of biventricular repair in patients with CCTGA, but also analyzes long-term results of physiologic and anatomic repair, including one-and-a-half ventricular repair. For physiologic repair, our recent long-term survivals of 84.7% 5.4% at 25 years were good compared with the data previously reported [2 5]. The only previously identified risk factor for decreased long-term survival after physiologic repair was reported to be the presence of preoperative TR [14]. The poorest outcome was also reported among patients who required TV replacement either at the initial operation or later during follow-up [5]. Therefore, the surgical management should include consideration of earlier timing of TV replacement or a cardiac repair, which relieves the RV and TV of a systemic workload [15]. In our series, preoperative PA banding and cardiopulmonary bypass time were risk factors for overall mortality, but TR and RV dysfunction were not risk factors. The patients who required TV replacement had also good results, 4.8% overall mortality, because TV replacement was performed at the earliest sign of increasing symptoms or progressive systemic ventricular deterioration to preserve RV function [3]. However, for anatomic repair, our series showed that the patients with RV dysfunction showed a worse survival rate than did the other patients. The reasons might include severe TR, especially associated with Ebstein anomaly, RV hypoplasia, high pulmonary vascular resistance, and heart failure. Our data also demonstrated that patients (n 6; age range, 2.19 to years) who complete LV training had deterioration in LV dysfunction at an earlier stage, resulting in more mortality compared with patients who did not require training. Actually, selecting the best procedure is difficult in these patients with an intact ventricle septum, severe TR, and RV dysfunction in old age, but in our early experience, LV training followed by anatomic repair was not decided under strict selection criteria. The durability of LV function after LV training has been reported to be low due to a high incidence of the trained LV failure after the anatomic repair [12, 16]. The LV conditioning time to which the ventricle was subjected to systemic pressures before the anatomic repair was also short [16] because the LV was subjected only to pulmonic pressures all through from birth to LV training. Longer follow-up will be needed for evaluation of deterioration of LV function late after LV training. In this series, 5 patients with physiologic one-and-ahalf ventricular repair had good results without mortal-
6 164 LIM ET AL Ann Thorac Surg CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 2010;89: Table 3. Risk Factors for Arrhythmia Univariable Multivariable Variable HR 95% CI p Value HR 95% CI p Value Overall arrhythmia Pulmonary stenosis Pulmonary atresia Ventricular septal defect Preoperative PAB Preoperative shunt Tricuspid regurgitation RV dysfunction Age Physiologic repair BCPS Cardiopulmonary bypass time Aortic cross-clamp time Tachyarrhythmia Pulmonary stenosis Pulmonary atresia Ventricular septal defect Preoperative PAB Preoperative shunt Tricuspid regurgitation RV dysfunction Age Physiologic repair BCPS Cardiopulmonary bypass time Aortic cross-clamp time Bradyarrhythmia Pulmonary stenosis Pulmonary atresia VSD Preoperative PAB Preoperative shunt Tricuspid regurgitation RV dysfunction Age Physiologic repair BCPS Cardiopulmonary bypass time Aortic cross-clamp time BCPS bidirectional cavopulmonary shunt; CI confidence interval; CPB cardiopulmonary bypass; HR hazard ratio; PAB pulmonary artery banding; RV right ventricle; VSD ventricular septal defect. ity. It was particularly applicable in situations where the atrial switch with the Rastelli procedure is not possible in CCTGA with pulmonary stenosis because of the position of the VSD. It was also beneficial in the patients with hypoplasia or malfunction of the LV because of unloading the LV by reducing flow through the LV to PA connection. The anatomic one-and-a-half type of ventricular repair is very useful particularly in hypoplasia or malfunction of the RV because of unloading the RV. It carries also no risk of superior vena cava obstruction, with less risk of obstruction to the pulmonary venous return from increasing the intra-atrial space, less risk of arrhythmias from reducing the intra-atrial suture lines, and reduced ischemic time. The widest and most reliable application of partial biventricular repair is likely to be for patients with hypoplasia or functional compromise of the right-side heart complex, or both [17, 18]. The presence of a straddling AV valve or an inlet VSD with no outlet extension would make it difficult to tunnel the VSD to the aorta without compromising the volume of the RV because of the size of the baffle as well as TV function. In these circumstances, the anatomic one-and-a-half type of
7 Ann Thorac Surg LIM ET AL 2010;89: CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 165 Fig 2. Freedom from atrioventricular valve and ventricular dysfunction. (A) Freedom from tricuspid valve (TV) dysfunction. (B) Freedom from right ventricle (RV) dysfunction. (C) Freedom from systemic atrioventricular (AV) valve dysfunction. (D) Freedom from systemic ventricular dysfunction. Atrioventricular valve dysfunction was defined as regurgitation grade of 2 and more; ventricular dysfunction was defined as mild to moderate dysfunction and worse. (a) Anatomic repair. (b) Physiologic repair. ventricular repair was applied, resulting in a positive impact on survival, as demonstrated by this study. Risks for reoperation were pulmonary atresia, as indicated by multivariate analysis, which was caused by the need for conduit change or pulmonary valve replacement. After physiologic repair, the prevalence of systemic AV valve failure is likely to result in a considerably higher incidence of reoperation in the longer term among patients who have undergone a physiologic approach [2, 4, 19]. The most frequent early complication after surgical correction of CCTGA is complete heart block [2, 4, 20]. The incidence of complete heart block tends to be lower after anatomic repair than after physiologic repair [2, 4, 20 22]. In this study, the incidence of postoperative complete AV block was also lower after anatomic repair than after physiologic repair (6.8% versus 22.0%, p 0.03). In the Rastelli-type anatomic repair, the closure of VSD through the right ventriculotomy allows a more ready accessibility to the RV aspect of the septum than the other approaches, and that is important in avoiding the conduction system [6, 23]. In our patients, the Rastelli-type anatomic repair (3.2%) was associated with the lowest incidence of postoperative heart block compared with the anatomic repair with arterial switch (15.4%) and the physiologic repair (22.0%) [22]. The pulmonary atresia, VSD, and preoperative shunt had protective effect on the bradyarrhythmia, which was related to the fact that in CCTGA with pulmonary atresia and VSD, the physiologic repair with PV-PA conduit interposition had less complete AV block than relief of PV outflow tract obstruction without conduit; and the Rastelli-type anatomic repair also had the lowest incidence of complete AV block, but old age was a risk factor for the bradyarrhythmia. Although a long-term complication after anatomic repair is the development of surgically induced arrhythmias by suture line and suture load, our anatomic repair group tended to have similar tachyarrhythmic events even though atrial switch was added, but they had fewer bradyarrhythmic events such as complete AV block. In our series, the long-term follow-up data demon-
8 166 LIM ET AL Ann Thorac Surg CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 2010;89: strate that funtional status was good in both biventricular repairs, but freedom from systemic AV valve and ventricular dysfunction as well as from TV and RV dysfunction were significantly higher after anatomic repair than after physiologic repair. Late mortality was 5.9% after physiologic repair, but 0% after anatomic repair. Our data showed that with the restoration of the LV to the systemic circulation by the anatomic repair, the incidence of systemic AV valve regurgitation and ventricular failure was reduced, and good functional status was achieved without long-term mortality. The study is limited by its retrospective design, which might include bias as to the selection of surgical methods. The 25-year period of surgical experience might have been associated with changes in selection and management of patients undergoing the biventricular repair that could influence long-term results. The earliest candidates for anatomic repair were often the worst. They were often selected by virtue of being unsuitable for the physiologic repairs owing to the presence of various risk factors and contraindications. A well-designed, large, multicenter cohort study will be the only practical solution in resolving the optimal choice of surgical procedures for these patients. In conclusion, long-term results of biventricular repair were satisfactory. Patients presenting with RV dysfunction or need for LV training represent a high-risk group of anatomic repair patients for whom selection criteria are particularly important. Our study demonstrates the superiority of anatomic repair compared with physiologic repair in systemic AV valve and ventricular function, although the incidence of reoperation or arrhythmia was not different. Anatomic repair is the procedure of choice for those patients if both ventricles are adequate or if surgical technique is modified with the help of an additional bidirectional cavopulmonary shunt. References 1. Van Praagh R. What is congenitally corrected transposition? N Engl J Med 1970;282: Termignon JL, Leca F, Vouhe PR, et al. Classic repair of congenitally corrected transposition and ventricular septal defect. Ann Thorac Surg 1996;62: van Son JA, Danielson GK, Huhta JC, et al. Late results of systemic atrioventricular valve replacement in corrected transposition. J Thorac Cardiovasc Surg 1995;109: Yeh T, Connelly MS, Coles JG, et al. Atrioventricular discordance: results of repair in 127 patients. J Thorac Cardiovasc Surg 1999;117: Hraska V, Duncan BW, Mayer JE, Freed M, del Nido PJ, Jonas RA. Long-term outcome of surgically treated patients with corrected transposition of the great arteries. J Thorac Cardiovasc Surg 2005;129: Ilbawi MN, DeLeon SY, Backer CL, et al. An alternative approach to the surgical management of physiologically corrected transposition witch ventricular septal defect and pulmonary stenosis or atresia. J Thorac Cardiovasc Surg 1990;100: Di Donato RM, Troconis CJ, Marino B, et al. Combined Mustard and Rastelli operations. An alternative approach for repair of associated anomalies in congenitally corrected transposition in situs inversus (I,D,D). J Thorac Cardiovasc Surg 1992;104: Imai Y, Sawatari K, Hoshino S, Ishihara K, Nakazawa M, Momma K. Ventricular function after anatomic repair in patients with atrioventricular discordance. J Thorac Cardiovasc Surg 1994;107: Mee RB. The double switch operation with accent on the Senning component. Semin Thorac Cardiovasc Surg Pediatr Card Surg Ann 2005;17: Karl TR, Weintraub RG, Brizard CP, Cochrane AD, Mee RR. Senning plus arterial switch for discordant (congenitally corrected) transposition. Ann Thorac Surg 1997;64: Langley SM, Winlaw DS, Stumper O, et al. Midterm results after restoration of the morphologically left ventricle to the systemic circulation in patients with congenitally corrected transposition of the great arteries. J Thorac Cardovasc Surg 2003;125: Bautista-Hernandez V, Marx GR, Gauvreau K, Mayer JE, Cecchin F, del Nido PJ. Determinants of left ventricular dysfunction after anatomic repair of congenitally corrected transposition of the great arteries. Ann Thorac Surg 2006;82: Shin oka T, Kurosawa H, Imai Y, et al. Outcomes of definitive surgical repair for congenitally corrected transposition of the great arteries or double outlet right ventricle with discordant atrioventricular connections: risk analyses in 189 patients. J Thorac Cardiovasc Surg 2007;133: Huhta JC, Danielson GK, Ritter DG, Ilstrup DM. Survival in atrioventricular discordance. Pediatr Cardiol 1985;6: Mee RB. Severe right ventricular failure after Mustard or Senning operation. Two-stage repair: pulmonary artery banding and switch. J Thorac Cardiovasc Surg 1986;92: Quinn DW, McGuirk SP, Metha C, et al. The morphologic left ventricle that requires training by means of pulmonary artery banding before the double-switch procedure for congenitally corrected transposition of the great arteries is at risk of late dysfunction. J Thorac Cardiovasc Surg 2008;135: Van Arsdell GS, Williams WG, Maser CM, et al. Superior vena cava to pulmonary artery anastomosis: an adjunct to biventricular repair. J Thorac Cardiovasc Surg 1996;112: Reddy VM, McElhinney DB, Silverman NH, Marianeschi SM, Hanley FL. Partial biventricular repair for complex congenital heart defects: an intermediate option for complicated anatomy or functionally borderline right complex heart. J Thorac Cardiovasc Surg 1998;116: Biliciler-Denktas G, Feldt RH, Connolly HM, Weaver AL, Puga FJ, Danielson GK. Early and late results of operations for defects associated with corrected transposition and other anomalies with atrioventricular discordance in a pediatric population. J Thorac Cardiovasc Surg 2001;122: McGrath LB, Kirklin JW, Blackstone EH, Pacifico AD, Kirklin JK, Bargeron LM. Death and other events after cardiac repair in discordant atrioventricular connection. J Thorac Cardiovasc Surg 1985;90: Imamura M, Drummond-Webb JJ, Murphy DJ, et al. Results of the double switch operation in the current era. Ann Thorac Surg 2000;70: Alghamdi AA, McCrindle BW, Van Arsdell GS. Physiologic versus anatomic repair of congenitally corrected transposition of the great arteries: meta-analysis of individual patient data. Ann Thorac Surg 2006;81: de Leval MR, Bastos P, Stark J, Taylor JF, Macartney FJ, Anderson RH. Surgical technique to reduce the risks of heart block following closure of ventricular septal defect in atrioventricular discordance. J Thorac Cardiovasc Surg 1979;78:
9 Ann Thorac Surg LIM ET AL 2010;89: CONGENITAL REPAIR OF TRANSPOSITION OF GREAT ARTERIES 167 Appendix Type of Operation Physiologic Repair Anatomic Repair Diagnosis Type of Operation No. Type of Operation No. No pulmonary stenosis VSD or ASD VSD or ASD closure 14 Senning and ASO 6 Mustard and ASO 4 Tricuspid regurgitation Tricuspid valve replacement 21 Pulmonary stenosis or atresia VSD or ASD PV-PA conduit interposition 54 Senning and Rastelli 15 Relief of PVOT obstruction 26 Mustard and Rastelli 14 REV 8 Senning and ASO 2 Mustard and ASO 1 Senning and REV 1 Mustard and REV 1 Total ASD atrial septal defect; ASO arterial switch operation; PA pulmonary artery; PV pulmonary ventricle; PVOT pulmonary ventricular outflow tract; REV réparation à l étage ventriculaire; VSD ventricular septal defect.
The Double Switch Using Bidirectional Glenn and Hemi-Mustard. Frank Hanley
 The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
M/3, cc-tga, PS, BCPC(+) Double Switch Operation
 2005 < Pros & Cons > M/3, cc-tga, PS, BCPC(+) Double Switch Operation Congenitally corrected TGA Atrio-Ventricular & Ventriculo-Arterial discordance Physiologically corrected circulation with the morphologic
2005 < Pros & Cons > M/3, cc-tga, PS, BCPC(+) Double Switch Operation Congenitally corrected TGA Atrio-Ventricular & Ventriculo-Arterial discordance Physiologically corrected circulation with the morphologic
Congenitally corrected transposition (cctga) is defined
 Results of the Double Switch Operation in the Current Era Michiaki Imamura, MD, PhD, Jonathan J. Drummond-Webb, MD, Daniel J. Murphy, Jr, MD, Lourdes R. Prieto, MD, Larry A. Latson, MD, Scott D. Flamm,
Results of the Double Switch Operation in the Current Era Michiaki Imamura, MD, PhD, Jonathan J. Drummond-Webb, MD, Daniel J. Murphy, Jr, MD, Lourdes R. Prieto, MD, Larry A. Latson, MD, Scott D. Flamm,
Since first successfully performed by Jatene et al, the
 Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Long-Term Predictors of Aortic Root Dilation and Aortic Regurgitation After Arterial Switch Operation Marcy L. Schwartz, MD; Kimberlee Gauvreau, ScD; Pedro del Nido, MD; John E. Mayer, MD; Steven D. Colan,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum
 Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Common Defects With Expected Adult Survival:
 Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Index Note: Page numbers of article titles are in boldface type. A ACHD. See Adult congenital heart disease (ACHD) Adult congenital heart disease (ACHD), 503 512 across life span prevalence of, 504 506
Surgical Treatment for Double Outlet Right Ventricle. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy
 Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
Double outlet right ventricle: navigation of surgeon to chose best treatment strategy Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London Double outlet
Patients with congenitally corrected transposition of the great arteries
 Surgery for Congenital Heart Disease Midterm results after restoration of the morphologically left ventricle to the systemic circulation in patients with congenitally corrected transposition of the great
Surgery for Congenital Heart Disease Midterm results after restoration of the morphologically left ventricle to the systemic circulation in patients with congenitally corrected transposition of the great
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
In conventional repair of the associated malformations
 Intermediate Results of the Double-Switch Operations for Atrioventricular Discordance Masahiro Koh, MD, Toshikatsu Yagihara, MD, Hideki Uemura, MD, Koji Kagisaki, MD, Ikuo Hagino, MD, Toru Ishizaka, MD,
Intermediate Results of the Double-Switch Operations for Atrioventricular Discordance Masahiro Koh, MD, Toshikatsu Yagihara, MD, Hideki Uemura, MD, Koji Kagisaki, MD, Ikuo Hagino, MD, Toru Ishizaka, MD,
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Tricuspid valve surgery in patients with a systemic right ventricle
 Tricuspid valve surgery in patients with a systemic right ventricle Roderick Scherptong, Hubert Vliegen, Michiel Winter, Barbara Mulder, Ernst van der Wall, Dave Koolbergen, Mark Hazekamp Eduard Holman,
Tricuspid valve surgery in patients with a systemic right ventricle Roderick Scherptong, Hubert Vliegen, Michiel Winter, Barbara Mulder, Ernst van der Wall, Dave Koolbergen, Mark Hazekamp Eduard Holman,
cctga patients need lifelong follow-up in an age-appropriate facility with expertise in
 ONLINE SUPPLEMENT ONLY: ISSUES IN THE ADULT WITH CCTGA General cctga patients need lifelong follow-up in an age-appropriate facility with expertise in congenital heart disease care at annual intervals.
ONLINE SUPPLEMENT ONLY: ISSUES IN THE ADULT WITH CCTGA General cctga patients need lifelong follow-up in an age-appropriate facility with expertise in congenital heart disease care at annual intervals.
"Giancarlo Rastelli Lecture"
 "Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
"Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions
 Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Corrective Repair of Complete Atrioventricular
 Corrective Repair of Complete Atrioventricular Canal Defects and Major Associated Cardiac Anomalies A. D. Pacifico, M.D., A. Ricchi, M.D., L. M. Bargeron, Jr., M.D., E. C. Colvin, M.D., J. W. Kirklin,
Corrective Repair of Complete Atrioventricular Canal Defects and Major Associated Cardiac Anomalies A. D. Pacifico, M.D., A. Ricchi, M.D., L. M. Bargeron, Jr., M.D., E. C. Colvin, M.D., J. W. Kirklin,
When to implant an ICD in systemic right ventricle?
 When to implant an ICD in systemic right ventricle? Département de rythmologie et de stimulation cardiaque Nicolas Combes n.combes@clinique-pasteur.com Pôle de cardiologie pédiatrique et congénitale Risk
When to implant an ICD in systemic right ventricle? Département de rythmologie et de stimulation cardiaque Nicolas Combes n.combes@clinique-pasteur.com Pôle de cardiologie pédiatrique et congénitale Risk
Children with Single Ventricle Physiology: The Possibilities
 Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
TGA, VSD, and LVOTO. Cheul Lee, MD. Department of Thoracic and Cardiovascular Surgery Sejong General Hospital
 Surgical Management of TGA, VSD, and LVOTO Cheul Lee, MD Department of Thoracic and Cardiovascular Surgery Sejong General Hospital TGA, VSD, and LVOTO Incidence : 0.7% of all CHD 20% of TGA with VSD 4%
Surgical Management of TGA, VSD, and LVOTO Cheul Lee, MD Department of Thoracic and Cardiovascular Surgery Sejong General Hospital TGA, VSD, and LVOTO Incidence : 0.7% of all CHD 20% of TGA with VSD 4%
Surgical Results in Patients With Double Outlet Right Ventricle: A 20-Year Experience
 Surgical Results in Patients With Double Outlet Right Ventricle: A 20-Year Experience John W. Brown, MD, Mark Ruzmetov, MD, Yuji Okada, MD, Palaniswamy Vijay, PhD, MPH, and Mark W. Turrentine, MD Section
Surgical Results in Patients With Double Outlet Right Ventricle: A 20-Year Experience John W. Brown, MD, Mark Ruzmetov, MD, Yuji Okada, MD, Palaniswamy Vijay, PhD, MPH, and Mark W. Turrentine, MD Section
Anatomic repair of corrected transposition or atrio-ventricular discordance 1 Report of 8 cases
 European Journal of Cardio-thoracic Surgery 13 (1998) 117 123 Anatomic repair of corrected transposition or atrio-ventricular discordance 1 Report of 8 cases D. Metras a, *, B. Kreitmann a, A. Fraisse
European Journal of Cardio-thoracic Surgery 13 (1998) 117 123 Anatomic repair of corrected transposition or atrio-ventricular discordance 1 Report of 8 cases D. Metras a, *, B. Kreitmann a, A. Fraisse
Cardiovascular Surgery
 Cardiovascular Surgery Intention-to-Treat Analysis of Pulmonary Artery Banding in Conditions With a Morphological Right Ventricle in the Systemic Circulation With a View to Anatomic Biventricular Repair
Cardiovascular Surgery Intention-to-Treat Analysis of Pulmonary Artery Banding in Conditions With a Morphological Right Ventricle in the Systemic Circulation With a View to Anatomic Biventricular Repair
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
Heart Transplantation in Patients with Superior Vena Cava to Pulmonary Artery Anastomosis: A Single-Institution Experience
 Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Congenitally Corrected Transposition of the Great Arteries (cctga or l-loop TGA)
 Congenitally Corrected Transposition of the Great Arteries (cctga or l-loop TGA) Mary Rummell, MN, RN, CPNP, CNS Clinical Nurse Specialist, Pediatric Cardiology/Cardiac Surgery Doernbecher Children s Hospital,
Congenitally Corrected Transposition of the Great Arteries (cctga or l-loop TGA) Mary Rummell, MN, RN, CPNP, CNS Clinical Nurse Specialist, Pediatric Cardiology/Cardiac Surgery Doernbecher Children s Hospital,
T ciated with atrioventricular (AV) discordance have
 Tricuspid Valve Abnormalities in Patients With Atrioventricular Discordance: Surgical Implications Pave1 Horvath, MD, Marek Szufladowicz, MD, Marc R. de Leval, MD, Martin J. Elliott, MD, and Jaroslav Stark,
Tricuspid Valve Abnormalities in Patients With Atrioventricular Discordance: Surgical Implications Pave1 Horvath, MD, Marek Szufladowicz, MD, Marc R. de Leval, MD, Martin J. Elliott, MD, and Jaroslav Stark,
Are There Indications for Atrial Switch (or Atrial Inversion Surgery) in the 21st Century? Marcelo B. Jatene
 Are There Indications for Atrial Switch (or Atrial Inversion Surgery) in the 21st Century? Marcelo B. Jatene marcelo.jatene@incor.usp.br No disclosures Transposition of Great Arteries in the 21st century
Are There Indications for Atrial Switch (or Atrial Inversion Surgery) in the 21st Century? Marcelo B. Jatene marcelo.jatene@incor.usp.br No disclosures Transposition of Great Arteries in the 21st century
Intermediate Results From the Period of the Congenital Heart Surgeons Transposition Study: 1985 to 1989
 Intermediate Results From the Period of the Congenital Heart Surgeons Transposition Study: 1985 to 1989 Kevin Turley, MD, Edward D. Verrier, MD, and Congenital Heart Surgeons Society Database California
Intermediate Results From the Period of the Congenital Heart Surgeons Transposition Study: 1985 to 1989 Kevin Turley, MD, Edward D. Verrier, MD, and Congenital Heart Surgeons Society Database California
The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients
 The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
TGA Surgical techniques: tips & tricks (Arterial switch operation)
 TGA Surgical techniques: tips & tricks (Arterial switch operation) Seoul National University Children s Hospital Woong-Han Kim Surgical History 1951 Blalock and Hanlon, atrial septectomy 1954 Mustard et
TGA Surgical techniques: tips & tricks (Arterial switch operation) Seoul National University Children s Hospital Woong-Han Kim Surgical History 1951 Blalock and Hanlon, atrial septectomy 1954 Mustard et
What Can the Database Tell Us About Reoperation?
 AATS/STS Congenital Heart Disease Postgraduate Symposium May 5, 2013 What Can the Database Tell Us About Reoperation? Jeffrey P. Jacobs, M.D. All Children s Hospital Johns Hopkins Medicine The Congenital
AATS/STS Congenital Heart Disease Postgraduate Symposium May 5, 2013 What Can the Database Tell Us About Reoperation? Jeffrey P. Jacobs, M.D. All Children s Hospital Johns Hopkins Medicine The Congenital
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Masahiro Koh*, Toshikatsu Yagihara, Hideki Uemura, Koji Kagisaki, Soichiro Kitamura
 European Journal of Cardio-thoracic Surgery 26 (2004) 767 772 www.elsevier.com/locate/ejcts Functional biventricular repair using left ventricle pulmonary artery conduit in patients with discordant atrioventricular
European Journal of Cardio-thoracic Surgery 26 (2004) 767 772 www.elsevier.com/locate/ejcts Functional biventricular repair using left ventricle pulmonary artery conduit in patients with discordant atrioventricular
Long-Term Results After the Rastelli Repair for Transposition of the Great Arteries
 PEDIATRIC CARDIAC SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS member
PEDIATRIC CARDIAC SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS member
Complex Congenital Heart Disease in Adults
 Complex Congenital Heart Disease in Adults Linda B. Haramati, MD Disclosures Complex Congenital Heart Disease in Adults Linda B. Haramati MD, MS Jeffrey M. Levsky MD, PhD Meir Scheinfeld MD, PhD Department
Complex Congenital Heart Disease in Adults Linda B. Haramati, MD Disclosures Complex Congenital Heart Disease in Adults Linda B. Haramati MD, MS Jeffrey M. Levsky MD, PhD Meir Scheinfeld MD, PhD Department
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT
 LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
LEFT VENTRICULAR OUTFLOW OBSTRUCTION WITH A VSD: OPTIONS FOR SURGICAL MANAGEMENT 10-13 March 2017 Ritz Carlton, Riyadh, Saudi Arabia Zohair AlHalees, MD Consultant, Cardiac Surgery Heart Centre LEFT VENTRICULAR
Adult Congenital Heart Disease T S U N ` A M I!
 Adult Congenital Heart Disease T S U N ` A M I! Erwin Oechslin, MD, FRCPC, FESC Director, Congenital Cardiac Centre for Adults University Health Network Peter Munk Cardiac Centre / Toronto General Hospital
Adult Congenital Heart Disease T S U N ` A M I! Erwin Oechslin, MD, FRCPC, FESC Director, Congenital Cardiac Centre for Adults University Health Network Peter Munk Cardiac Centre / Toronto General Hospital
Commissural Malalignment of Aortic-Pulmonary Sinus in Complete Transposition of Great Arteries
 Commissural Malalignment of Aortic-Pulmonary Sinus in Complete Transposition of Great Arteries Soo-Jin Kim, MD, Woong-Han Kim, MD, Cheong Lim, MD, Sam Se Oh, MD, and Yang-Min Kim, MD Departments of Pediatric
Commissural Malalignment of Aortic-Pulmonary Sinus in Complete Transposition of Great Arteries Soo-Jin Kim, MD, Woong-Han Kim, MD, Cheong Lim, MD, Sam Se Oh, MD, and Yang-Min Kim, MD Departments of Pediatric
Congenital Heart Disease II: The Repaired Adult
 Congenital Heart Disease II: The Repaired Adult Doreen DeFaria Yeh, MD FACC Assistant Professor, Harvard Medical School MGH Adult Congenital Heart Disease Program Echocardiography Section, no disclosures
Congenital Heart Disease II: The Repaired Adult Doreen DeFaria Yeh, MD FACC Assistant Professor, Harvard Medical School MGH Adult Congenital Heart Disease Program Echocardiography Section, no disclosures
Cardiac Catheterization Cases Primary Cardiac Diagnoses Facility 12 month period from to PRIMARY DIAGNOSES (one per patient)
 PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
Double switch operation in cardiac anomalies with atrioventricular and ventriculoarterial discordance
 Double switch operation in cardiac anomalies with atrioventricular and ventriculoarterial discordance Since June 1987, 10 of 19 consecutive patients with atrioventricular and ventriculoarterial discordance
Double switch operation in cardiac anomalies with atrioventricular and ventriculoarterial discordance Since June 1987, 10 of 19 consecutive patients with atrioventricular and ventriculoarterial discordance
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20556 holds various files of this Leiden University dissertation. Author: Scherptong, Roderick Wiebe Conrad Title: Characterization of the right ventricle
Cover Page The handle http://hdl.handle.net/1887/20556 holds various files of this Leiden University dissertation. Author: Scherptong, Roderick Wiebe Conrad Title: Characterization of the right ventricle
Indications and Outcomes of the Double Switch in cctga. David Barron Birmingham, UK
 Indications and Outcomes of the Double Switch in cctga David Barron Birmingham, UK No Disclosures cctga: The Problem cctga does not fit into neat, clincially discrete sub-groups Atrial Situs Wide range
Indications and Outcomes of the Double Switch in cctga David Barron Birmingham, UK No Disclosures cctga: The Problem cctga does not fit into neat, clincially discrete sub-groups Atrial Situs Wide range
Risk Analysis of the Long-Term Outcomes of the Surgical Closure of Secundum Atrial Septal Defects
 Korean J Thorac Cardiovasc Surg 2017;50:78-85 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2017.50.2.78 Risk Analysis of the Long-Term Outcomes of the
Korean J Thorac Cardiovasc Surg 2017;50:78-85 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2017.50.2.78 Risk Analysis of the Long-Term Outcomes of the
The first report of the Society of Thoracic Surgeons
 REPORT The Society of Thoracic Surgeons National Congenital Heart Surgery Database Report: Analysis of the First Harvest (1994 1997) Constantine Mavroudis, MD, Melanie Gevitz, BA, W. Steves Ring, MD, Charles
REPORT The Society of Thoracic Surgeons National Congenital Heart Surgery Database Report: Analysis of the First Harvest (1994 1997) Constantine Mavroudis, MD, Melanie Gevitz, BA, W. Steves Ring, MD, Charles
Ventricular function after anatomic repair in patients with atrioventricular discordance
 Ventricular function after anatomic repair in patients with atrioventricular discordance Since June 1989, 18 patients with atrioventricular discordant anomalies under 15 years of age underwent anatomic
Ventricular function after anatomic repair in patients with atrioventricular discordance Since June 1989, 18 patients with atrioventricular discordant anomalies under 15 years of age underwent anatomic
Adult Congenital Heart Disease Certification Examination Blueprint
 Adult Congenital Heart Disease Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
Adult Congenital Heart Disease Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the
CMR for Congenital Heart Disease
 CMR for Congenital Heart Disease * Second-line tool after TTE * Strengths of CMR : tissue characterisation, comprehensive access and coverage, relatively accurate measurements of biventricular function/
CMR for Congenital Heart Disease * Second-line tool after TTE * Strengths of CMR : tissue characterisation, comprehensive access and coverage, relatively accurate measurements of biventricular function/
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
Successful radiofrequency catheter ablation in refractory atrial flutter developed 15years after Mustard's operation -a case report-
 Opening Remarks Free abstract sessions Successful radiofrequency catheter ablation in refractory atrial flutter developed 15years after Mustard's operation -a case report- An adult case of catheter ablation
Opening Remarks Free abstract sessions Successful radiofrequency catheter ablation in refractory atrial flutter developed 15years after Mustard's operation -a case report- An adult case of catheter ablation
Damus-Kaye-Stansel Procedure: Midterm Follow-up and Technical Considerations
 Damus-Kaye-Stansel Procedure: Midterm Follow-up and Technical Considerations Thomas L. Carter, MD, Richard D. Mainwaring, MD, and John J. Lamberti, MD Division of Cardiac Surgery, Children's Hospital and
Damus-Kaye-Stansel Procedure: Midterm Follow-up and Technical Considerations Thomas L. Carter, MD, Richard D. Mainwaring, MD, and John J. Lamberti, MD Division of Cardiac Surgery, Children's Hospital and
3/14/2011 MANAGEMENT OF NEWBORNS CARDIAC INTENSIVE CARE CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 WITH HEART DEFECTS
 CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
The Rastelli procedure has been traditionally used for repair
 En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
Double Outlet Right Ventricle with Anterior and Left-Sided Aorta and Subpulmonary Ventricular Septal Defect
 Case Report Double Outlet Right Ventricle with Anterior and Left-Sided rta and Subpulmonary Ventricular Septal Defect Luciana Braz Peixoto, Samira Morhy Borges Leal, Carlos Eduardo Suaide Silva, Sandra
Case Report Double Outlet Right Ventricle with Anterior and Left-Sided rta and Subpulmonary Ventricular Septal Defect Luciana Braz Peixoto, Samira Morhy Borges Leal, Carlos Eduardo Suaide Silva, Sandra
Right ventricular dysfunction after atrial repair for
 CURRENT REVIEW Arterial Switch Operation After Left Ventricular Retraining in the Adult Massimo A. Padalino, MD, Giovanni Stellin, MD, William J. Brawn, FRCS, Giuseppe Fasoli, MD, Luciano Daliento, MD,
CURRENT REVIEW Arterial Switch Operation After Left Ventricular Retraining in the Adult Massimo A. Padalino, MD, Giovanni Stellin, MD, William J. Brawn, FRCS, Giuseppe Fasoli, MD, Luciano Daliento, MD,
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Atrioventricular valve repair: The limits of operability
 Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
Atrioventricular valve repair: The limits of operability Francis Fynn-Thompson, MD Co-Director, Center for Airway Disorders Surgical Director, Pediatric Mechanical Support Program Surgical Director, Heart
The pulmonary valve is the most common heart valve
 Biologic versus Mechanical Valve Replacement of the Pulmonary Valve After Multiple Reconstructions of the RVOT Tract S. Adil Husain, MD, and John Brown, MD Indiana University School of Medicine, Department
Biologic versus Mechanical Valve Replacement of the Pulmonary Valve After Multiple Reconstructions of the RVOT Tract S. Adil Husain, MD, and John Brown, MD Indiana University School of Medicine, Department
A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution
 Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT
 ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
ECHOCARDIOGRAPHIC APPROACH TO CONGENITAL HEART DISEASE: THE UNOPERATED ADULT Karen Stout, MD, FACC Divisions of Cardiology University of Washington Medical Center Seattle Children s Hospital NO DISCLOSURES
Tetralogy of Fallot (TOF) with atrioventricular (AV)
 Tetralogy of Fallot with Atrioventricular Canal Defect: Two Patch Repair Sitaram M. Emani, MD, and Pedro J. del Nido, MD Tetralogy of Fallot (TOF) with atrioventricular (AV) canal defect is classified
Tetralogy of Fallot with Atrioventricular Canal Defect: Two Patch Repair Sitaram M. Emani, MD, and Pedro J. del Nido, MD Tetralogy of Fallot (TOF) with atrioventricular (AV) canal defect is classified
Surgical Treatment for Atrioventricular Septal Defect. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Surgical Treatment for Atrioventricular Septal Defect Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Rastelli classification (Rastelli) Pulmonary artery banding (Muller & Dammann)
Extracardiac vs Intra-atrial Lateral Tunnel Fontan: Extracardiac is Better. No it s not: (They both have problems)
 Extracardiac vs Intra-atrial Lateral Tunnel Fontan: Extracardiac is Better No it s not: (They both have problems) Why is it difficult to analyze outcomes after the Fontan procedure? Wide range of patient
Extracardiac vs Intra-atrial Lateral Tunnel Fontan: Extracardiac is Better No it s not: (They both have problems) Why is it difficult to analyze outcomes after the Fontan procedure? Wide range of patient
Anatomic repair for congenitally corrected transposition of the great arteries: A single-institution 19-year experience
 Anatomic repair for congenitally corrected transposition of the great arteries: A single-institution 19-year experience Bari Murtuza, MD, PhD, a David J. Barron, FRCS, a Oliver Stumper, MD, PhD, b John
Anatomic repair for congenitally corrected transposition of the great arteries: A single-institution 19-year experience Bari Murtuza, MD, PhD, a David J. Barron, FRCS, a Oliver Stumper, MD, PhD, b John
Mitral Valve Disease, When to Intervene
 Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Mitral Valve Disease, When to Intervene Swedish Heart and Vascular Institute Ming Zhang MD PhD Interventional Cardiology Structure Heart Disease Conflict of Interest None Current ACC/AHA guideline Stages
Hemodynamic Assessment After Complete Repair of Pulmonary Atresia With Major Aortopulmonary Collaterals
 Hemodynamic Assessment After Complete Repair of Pulmonary Atresia With Major Aortopulmonary Collaterals Richard D. Mainwaring, MD, V. Mohan Reddy, MD, Lynn Peng, MD, Calvin Kuan, MD, Michal Palmon, BS,
Hemodynamic Assessment After Complete Repair of Pulmonary Atresia With Major Aortopulmonary Collaterals Richard D. Mainwaring, MD, V. Mohan Reddy, MD, Lynn Peng, MD, Calvin Kuan, MD, Michal Palmon, BS,
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
FUNCTIONALLY SINGLE VENTRICLE
 MORPHOLOGICAL DETERMINANTS VI TRAN EuroEcho, Budapest, 7 th December 2011 DECLARATION OF CONFLICT OF INTEREST: I have nothing to declare What is the functionally single ventricle? The heart that is incapable
MORPHOLOGICAL DETERMINANTS VI TRAN EuroEcho, Budapest, 7 th December 2011 DECLARATION OF CONFLICT OF INTEREST: I have nothing to declare What is the functionally single ventricle? The heart that is incapable
Right ventricular failure, tricuspid valve insufficiency,
 Comparable Systemic Ventricular Function in Healthy Adults and Patients With Unoperated Congenitally Corrected Transposition Using MRI Dobutamine Stress Testing Ali Dodge-Khatami, MD, Igor I. Tulevski,
Comparable Systemic Ventricular Function in Healthy Adults and Patients With Unoperated Congenitally Corrected Transposition Using MRI Dobutamine Stress Testing Ali Dodge-Khatami, MD, Igor I. Tulevski,
T who has survived first-stage palliative surgical management
 Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
TGA atrial vs arterial switch what do we need to look for and how to react
 TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Congenital heart disease: When to act and what to do?
 Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Leading Article Congenital heart disease: When to act and what to do? Duminda Samarasinghe 1 Sri Lanka Journal of Child Health, 2010; 39: 39-43 (Key words: Congenital heart disease) Congenital heart disease
Echocardiographic assessment in Adult Patients with Congenital Heart Diseases
 Echocardiographic assessment in Adult Patients with Congenital Heart Diseases Athanasios Koutsakis Cardiologist, Cl. Research Fellow George Giannakoulas Ass. Professor in Cardiology 1st Cardiology Department,
Echocardiographic assessment in Adult Patients with Congenital Heart Diseases Athanasios Koutsakis Cardiologist, Cl. Research Fellow George Giannakoulas Ass. Professor in Cardiology 1st Cardiology Department,
Complete Transposition of the Great Arteries
 1 Complete Transposition of the Great Arteries Contents Introduction 2 Anatomy 3 Complete Transposition of the Great Arteries, with or without Ventricular Septal Defect 5 Indication for Surgery 5 Approach
1 Complete Transposition of the Great Arteries Contents Introduction 2 Anatomy 3 Complete Transposition of the Great Arteries, with or without Ventricular Septal Defect 5 Indication for Surgery 5 Approach
Clinical material and methods. Fukui Cardiovascular Center, Fukui, Japan
 Mitral Valve Regurgitation after Atrial Septal Defect Repair in Adults Shohei Yoshida, Satoshi Numata, Yasushi Tsutsumi, Osamu Monta, Sachiko Yamazaki, Hiroyuki Seo, Takaaki Samura, Hirokazu Ohashi Fukui
Mitral Valve Regurgitation after Atrial Septal Defect Repair in Adults Shohei Yoshida, Satoshi Numata, Yasushi Tsutsumi, Osamu Monta, Sachiko Yamazaki, Hiroyuki Seo, Takaaki Samura, Hirokazu Ohashi Fukui
Adults With Congenital Heart. Disease. An Expanding Population. In this article:
 Adults With Congenital Heart Disease An Expanding Population Continued progress in diagnosing and managing infants and children with congenital heart disease will likely result in a better prognosis and
Adults With Congenital Heart Disease An Expanding Population Continued progress in diagnosing and managing infants and children with congenital heart disease will likely result in a better prognosis and
Management of complex CHD in adults
 Management of complex CHD in adults Victor Tsang Society of Thoracic Surgeons of Thailand 2016 The impact of infant cardiac surgery Over 90 % of infants born with CHD will reach adulthood By 2010, adults
Management of complex CHD in adults Victor Tsang Society of Thoracic Surgeons of Thailand 2016 The impact of infant cardiac surgery Over 90 % of infants born with CHD will reach adulthood By 2010, adults
Avariety of conditions can prevent a successful biventricular
 Which Two Ventricles Cannot Be Used for a Biventricular Repair? Echocardiographic Assessment Norman H. Silverman, MD, and Doff B. McElhinney, MD Division of Pediatric Cardiology, Department of Pediatrics,
Which Two Ventricles Cannot Be Used for a Biventricular Repair? Echocardiographic Assessment Norman H. Silverman, MD, and Doff B. McElhinney, MD Division of Pediatric Cardiology, Department of Pediatrics,
Conversion of Atriopulmonary to Cavopulmonary Anastomosis in Management of Late Arrhythmias and Atrial Thrombosis
 Conversion of Atriopulmonary to Cavopulmonary Anastomosis in Management of Late Arrhythmias and Atrial Thrombosis Jane M. Kao, MD, Juan c. Alejos, MD, Peter W. Grant, MD, Roberta G. Williams, MD, Kevin
Conversion of Atriopulmonary to Cavopulmonary Anastomosis in Management of Late Arrhythmias and Atrial Thrombosis Jane M. Kao, MD, Juan c. Alejos, MD, Peter W. Grant, MD, Roberta G. Williams, MD, Kevin
Hybrid Stage I Palliation / Bilateral PAB
 Hybrid Stage I Palliation / Bilateral PAB Jeong-Jun Park Dept. of Thoracic & Cardiovascular Surgery Asan Medical Center, University of Ulsan CASE 1 week old neonate with HLHS GA 38 weeks Birth weight 3.0Kg
Hybrid Stage I Palliation / Bilateral PAB Jeong-Jun Park Dept. of Thoracic & Cardiovascular Surgery Asan Medical Center, University of Ulsan CASE 1 week old neonate with HLHS GA 38 weeks Birth weight 3.0Kg
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin. Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong
 Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Perimembranous VSD: When Do We Ask For A Surgical Closure? LI Xin Department of Cardiothoracic Surgery Queen Mary Hospital Hong Kong Classification (by Kirklin) I. Subarterial (10%) Outlet, conal, supracristal,
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
What is the Definition of Small Systemic Ventricle. Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University
 What is the Definition of Small Systemic Ventricle Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University Contents Introduction Aortic valve stenosis Aortic coarctation
What is the Definition of Small Systemic Ventricle Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University Contents Introduction Aortic valve stenosis Aortic coarctation
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/19123 holds various files of this Leiden University dissertation. Author: Hoohenkerk, Gerard Joannes Franciscus Title: Surgical correction of atrioventricular
Cover Page The handle http://hdl.handle.net/1887/19123 holds various files of this Leiden University dissertation. Author: Hoohenkerk, Gerard Joannes Franciscus Title: Surgical correction of atrioventricular
Failure of epicardial pacing leads in congenital heart disease: not uncommon and difficult to predict
 DOI 10.1007/s12471-011-0158-5 ORIGINAL ARTICLE Failure of epicardial pacing leads in congenital heart disease: not uncommon and difficult to predict M. C. Post & W. Budts & A. Van de Bruaene & R. Willems
DOI 10.1007/s12471-011-0158-5 ORIGINAL ARTICLE Failure of epicardial pacing leads in congenital heart disease: not uncommon and difficult to predict M. C. Post & W. Budts & A. Van de Bruaene & R. Willems
Appendix A.2: Tier 2 Surgical Procedure Terms and Definitions
 Appendix A.2: Tier 2 Surgical Procedure Terms and Definitions Tier 2 surgeries Anomalous Systemic Venous Connection Anomalous Systemic Venous Connection Repair Repair includes a range of surgical approaches,
Appendix A.2: Tier 2 Surgical Procedure Terms and Definitions Tier 2 surgeries Anomalous Systemic Venous Connection Anomalous Systemic Venous Connection Repair Repair includes a range of surgical approaches,
Transvenous Pacemaker Implantation 22 years after the Mustard Procedure
 Case Report Transvenous Pacemaker Implantation 22 years after the Mustard Procedure Masato Sakamoto MD, Yoshie Ochiai MD, Yutaka Imoto MD, Akira Sese MD, Mamie Watanabe MD, Kunitaka Joo MD Department of
Case Report Transvenous Pacemaker Implantation 22 years after the Mustard Procedure Masato Sakamoto MD, Yoshie Ochiai MD, Yutaka Imoto MD, Akira Sese MD, Mamie Watanabe MD, Kunitaka Joo MD Department of
The Clinical Outcomes of Damus-Kaye-Stansel Procedure According to Surgical Technique
 Korean J Thorac Cardiovasc Surg 24;4:344-349 ISSN: 2233-6X (Print) ISSN: 293-656 (Online) Clinical Research http://dx.doi.org/.59/kjtcs.24.4.4.344 The Clinical Outcomes of Damus-Kaye-Stansel Procedure
Korean J Thorac Cardiovasc Surg 24;4:344-349 ISSN: 2233-6X (Print) ISSN: 293-656 (Online) Clinical Research http://dx.doi.org/.59/kjtcs.24.4.4.344 The Clinical Outcomes of Damus-Kaye-Stansel Procedure
Congenital Heart Disease in the Adult Presenting for Non-Cardiac Surgery
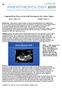 Page 1 Congenital Heart Disease in the Adult Presenting for Non-Cardiac Surgery Susan S. Eagle, M.D. Nashville, Tennessee Introduction: Advancement of surgical techniques and medical management patients
Page 1 Congenital Heart Disease in the Adult Presenting for Non-Cardiac Surgery Susan S. Eagle, M.D. Nashville, Tennessee Introduction: Advancement of surgical techniques and medical management patients
Accessory and Anomalous Atrioventricular Valvar Tissue Causing Outflow Tract Obstruction
 JACC Vol. 32, No. 6 November 15, 1998:1741 8 1741 PEDIATRIC CARDIOLOGY Accessory and Anomalous Atrioventricular Valvar Tissue Causing Outflow Tract Obstruction Surgical Implications of a Heterogeneous
JACC Vol. 32, No. 6 November 15, 1998:1741 8 1741 PEDIATRIC CARDIOLOGY Accessory and Anomalous Atrioventricular Valvar Tissue Causing Outflow Tract Obstruction Surgical Implications of a Heterogeneous
DIAGNOSIS, MANAGEMENT AND OUTCOME OF HEART DISEASE IN SUDANESE PATIENTS
 434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
434 E AST AFRICAN MEDICAL JOURNAL September 2007 East African Medical Journal Vol. 84 No. 9 September 2007 DIAGNOSIS, MANAGEMENT AND OUTCOME OF CONGENITAL HEART DISEASE IN SUDANESE PATIENTS K.M.A. Sulafa,
Intracardiac Lateral Tunnel Fontan by using Right Atrial Wall
 Intracardiac Lateral Tunnel Fontan by using Right Atrial Wall Md Zahidul Islam¹, AM Asif Rahim², Kazi Abul Hasan¹, Syed Imtiaz Ahsan¹ 1 Department of Paediatric Cardiac Surgery, National Institute of Cardiovascular
Intracardiac Lateral Tunnel Fontan by using Right Atrial Wall Md Zahidul Islam¹, AM Asif Rahim², Kazi Abul Hasan¹, Syed Imtiaz Ahsan¹ 1 Department of Paediatric Cardiac Surgery, National Institute of Cardiovascular
ADULT CONGENITAL HEART DISEASE AN UPDATE FOR CARDIOLOGISTS AND PRIMARY CARE PHYSICIANS
 ADULT CONGENITAL HEART DISEASE AN UPDATE FOR CARDIOLOGISTS AND PRIMARY CARE PHYSICIANS V.S. Mahadevan, MD, F.R.C.P. Director, Structural and Adult congenital Interventional Cardiology Program William W
ADULT CONGENITAL HEART DISEASE AN UPDATE FOR CARDIOLOGISTS AND PRIMARY CARE PHYSICIANS V.S. Mahadevan, MD, F.R.C.P. Director, Structural and Adult congenital Interventional Cardiology Program William W
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
