By Bertram Pitt, M.D., Eric C. Elliot, M.D., and Donald E. Gregg, Ph.D., M.D.
|
|
|
- Melina Hutchinson
- 6 years ago
- Views:
Transcription
1 Adrenergic Receptor Activity in the Coronary Arteries of the Unanesthetized Dog By Bertram Pitt, M.D., Eric C. Elliot, M.D., and Donald E. Gregg, Ph.D., M.D. ABSTRACT Both a- (vasoconstrictor) and (- (vasodilator) receptor activity was demonstrated in the coronary arteries of the unanesthetized dog independent of adrenergic receptors in the myocardium. In the y-receptor blocked animal, a-adrenergic receptor activity was demonstrated after intravenous and intracoronary injections of epinephrine and norepinephrine by the occurrence of coronary vasoconstriction which could be eliminated by blocking a-adrenergic receptors as well. Coronary vasoconstriction was also seen prior to /-receptor blockade after intravenous phenylephrine and, on occasion, after intracoronary injections of norepinephrine. /-adrenergic receptor activity was demonstrated in several instances after intravenous or intracoronary injections of catecholamines by an initial vasodilatation which could be eliminated by /-adrenergic receptor blockade and which occurred before there was any change in myocardial or systemic hemodynamics. The role of this independent adrenergic receptor activity in the control of the coronary circulation remains to be determined. ADDITIONAL KEY WORDS vasodilator myocardium catecholamines block of a- and y-receptors intracoronary injections systemic hemodynamics norepinephrine vasoconstrictor phenylephrine epinephrine Considerable controversy has existed concerning the effects of catecholamines on the coronary circulation. In part, this is due to indirect methods for the measurement of coronary blood flow and the use of open chest anesthetized animals in which varying degrees of hypoxia and myocardial failure often coexist. Although there is general agreement that catecholamines can cause an increase in coronary blood flow (), this has been attributed by some to myocardial stimulation and subsequent metabolic vasodilatation rather than to a direct effect on the coronary arteries (, ). The recent demonstration of /-adrenergic receptor activity as manifested by coronary relaxation in isolated coronary artery strips (), and in the non- From the Department of Cardiorespiratory Diseases, Walter Reed Army Institute of Research, Walter Reed Army Medical Center, Washington, D. C.. Accepted for publication June, 967. beating heart (, 6), as well as a-receptor activity as manifested by coronary contraction in isolated coronary artery strips (), and vasoconstriction in the open chest animal with j8-receptors blocked (7-9) has renewed interest in the primary action of the catecholamines on the coronary vasculature. The present study was undertaken in an attempt to determine whether a- and /- adrenergic receptor activity could be demonstrated in the coronary arteries of the unanesthetized dog, using chronically implanted electromagnetic flow transducers and adrenergic blocking agents. Methods The standard animal preparation and methods used for analysis of data in our laboratory have been described previously () and will be briefly reviewed below. Electromagnetic flow x The principles of laboratory animal care as promulgated by the National Society for Medical Research were observed. Circulation Research, Vol. XXI, July 967 7
2 Intravenous Injections at Experiment Isoproterenol Epinephrine Norepinephrinc? I"» n?* J Isoproterenol? - S Time (sec) Fixed Ventricular Heart rate (beat/min) Rate before Cor. flow (ml/min) TABLE ^-Receptor Blockade Stroke syst. flow (ml) After Stroke diast. flow (ml) Mean aortic press. (mm Hg) ^-Receptor Blockade Mean cor. resist Late diast. cor. resist Cardiac output (ml/min) Stroke vol. (ml) O\ TJ in r- r~ O r» a in bl en
3 ADRENERGIC ACTIVITY IN CORONARY ARTERIES 77 CO O H CO CO o o O CM O O -^ to co ci co w oj t - ( o o o o o o O o o o o o oo co o oo in i H H M H O O <C O IO lfl O o ri ci «'ri * O O t l O O O O O ^ t-oi>oocooco transducers were placed around the left circumflex coronary artery and central aorta to measure phasic and mean coronary blood flow and cardiac output. Zero coronary blood flow was obtained by a polyethylene snare located distal to the coronary flow transducer. Central aortic pressure was obtained through a chronically implanted polyvinyl catheter. Intravenous injections were made through a chronically implanted jugular venous catheter. Coronary flow and cardiac output were determined by planimetric integration of the phasic flow tracings. In one group of dogs weighing 6 to kg, surgical heart block was produced to weeks prior to the implantation of flow transducers, either by a modification of the Starzl technique () or by electrocoagulation of the atrioventricular node, and the heart was paced thereafter with a variable rate pacemaker. One of these animals did not have an aortic flow transducer. In another group of dogs of similar weight with intact conducting system, a coronary arterial catheter was implanted into the left circumflex coronary artery distal to the coronary flow transducer and snare by the Herd-Barger technique (). Two of these animals did not have an aortic flow transducer. All animals were trained to lie quietly and were studied to weeks postimplantation in the resting state..! oooq-^qq o o CO CO o o CM qpppi-j o o CM I Circulation Research, Vol. XXI, July 967 Results INTRAVENOUS INJECTIONS AT FIXED VENTRICULAR RATES (TABLE ) In the animals with fixed ventricular rates, isoproterenol (. /".g/kg iv) led to a 6% increase in mean coronary blood flow to sec after injection. This was accompanied by a marked fall in mean aortic pressure (% below control) resulting in a decrease in mean and late diastolic coronary vascular resistance of 8 and %, respectively. Cardiac output rose % above control and was associated with a decrease in systolic ejection period. The increase in coronary blood flow was accomplished by increasing stroke systolic coronary flow while stroke diastolic coronary flow remained unchanged or fell slightly in animals. After /-adrenergic receptor blockade with intravenous propranolol ( to mg/kg), isoproterenol had no effect on mean or late diastohc coronary vascular resistance in animals, while in the fourth there was a slight increase in resistance.
4 78 PITT, ELLIOT, GREGG Epinephrine (. fig/kg iv) led to a 9% increase in coronary blood flow to sec after injection. This was done by increasing both stroke systolic and diastolic coronary flow. Mean aortic pressure rose 7% CONTROL EPINEPHRINE jig I V Seconds FIGURE Hemodynamic effects of epinephrine, fig/kg iv before and after p-adrenergic receptor blockade with propranolol ( mg/kg). Conducting system previously blocked and heart paced at beat/min. H.R. = heart rate. ECG electrocardiogram lead II. ABP phasic aortic blood pressure curve (numbers indicate mean pressure, mm Hg, but mean pressure line should be ignored). LCF = phasic left circumflex flow curve; numbers indicate mean flow (ml/min). LDCR late diastolic coronary resistance; numbers just above zero coronary flow line (dotted) represent aortic blood pressure (mm Hg) divided by coronary flow (ml/min) just before isometric contraction. CO = cardiac output (ml/min). Paper speed, 7 mm/sec. Vertical time lines,. sec. CONTROL Phenylephrine (ig V- Seconds H R ABP /\ /V ^ 'V LCF LDCR C above control while mean and late diastolic coronary vascular resistance fell and 6% respectively. The effects on cardiac output were small. After /-adrenergic receptor blockade with intravenous propranolol, epineph- /V- ' 7 \ r l\ I". L._ FIGURE i \ 99 Hemodynamic effects of phenylephrine, ng/kg iv. Conducting system previously blocked and heart paced at beat/min. Order of curves and abbreviations same as in Figure. Mean pressure lines on phasic pressure curves should be ignored. Paper speed, 7 mm/sec. Vertical time lines,. sec. f Circulation Research, Vol. XXI, Juh 967
5 ADRENERGIC ACTIVITY IN CORONARY ARTERIES 79 TABLEi IntracoTonary Injections before fl-receptor Blockade Experiment Isoproterenol Time fsec) Heart rate (beat/min) Cor. flow (ml/min) Mean aortic press. (mm Hg) 98 8 Mean cor. resist Late diast. cor. resist Cardiac output (ml/min) Systolic ejection period (sec) Epinephrine ,.' Norepinephrine Isoproterenol After p-receptor Blockade Epinephrine Norepinephrine rine had a variable effect on coronary blood flow but consistently increased both mean and late diastolic coronary vascular resistance ( and %). In some experiments with intravenous cate- cholamines, coronary vascular resistance fell before any change occurred in systemic or myocardial hemodynamics. In a representative animal with a fixed ventricular rate, epinephrine (. /^g/kg iv) led to a 69% rise Circulation Research, Vol. XXI, July 967
6 8 PITT, ELLIOT, GREGG in mean coronary blood flow and a fall in mean and late diastolic coronary vascular resistance before there was any change in aortic pressure, cardiac output, systolic ejection period, mean or peak ventricular ejection rates (Fig. ). After /-adrenergic receptor blockade with intravenous propranolol, epinephrine led to a % fall in coronary blood flow despite a rise in mean aortic pressure of mm Hg. The results with norepinephrine (. /u-g/ kg) were qualitatively similar to those with epinephrine. However, the increase in coronary blood flow (%) and fall in mean and late diastolic coronary vascular resistance (% each) after norepinephrine were less than with epinephrine. After /-adrenergic receptor blockade with intravenous propranolol, the increase in mean coronary resistance (%) and late diastolic coronary vascular resistance (6%) was greater with norepinephrine than with epinephrine. Coronary vasoconstriction could also be demonstrated prior to /-adrenergic receptor blockade. Phenylephrine (. ju-g/kg) was given intravenously with ventricular rate again held constant; it led to a fall in coronary blood flow 6% below control despite an increase in mean aortic pressure of mm Hg(Fig.). Following a-adrenergic receptor blockade with intravenous dibenzylene ( mg/kg) in animals, epinephrine and norepinephrine caused a fall in coronary vascular resistance. In dog with a-receptors blocked, intravenous epinephrine ( /xg/kg) led to an increase in coronary blood flow from a control of to 6 ml/min (8% above control) while mean aortic pressure fell from 8 to 6 mm Hg (9% below control). This resulted in a fall in mean and late diastolic coronary vascular resistance of 8 and 9%. Cardiac output increased from 8 to ml/min (% above control) while the heart rate was held constant at 7 beat/min. After a-adrenergic receptor blockade with intravenous dibenzylene, and ^-adrenergic receptor blockade with intravenous propranolol ( to mg/ kg), epinephrine and norepinephrine either had no effect on coronary vascular resistance or led to a small fall in resistance. In the other animal cited above, epinephrine ( fig /kg) increased coronary blood flow from to ml/min (% above control) while mean aortic pressure increased from 8 to mm Hg (% above control). Mean coronary resistance remained unchanged while late diastolic coronary vascular resistance fell 6%. Cardiac output fell from to ml/ min (% below control) while the heart rate was held constant at 7 beat/min. These results are in contrast to the coronary vasoconstriction seen with epinephrine after /- adrenergic receptor blockade alone (Table ). INTRACORONARY INJECTIONS (TABLE II) The direct effects of the catecholamines on the coronary circulation were evaluated in dogs with intact conducting systems. Repeated intracoronary injections of isotonic CONTROL SEC 7 SEC t7z V.,. :. ml IC FIGURE Continuous record showing hemodynamic effects of intravenous isotonic sodium chloride. Conducting system intact and heart not paced. Order of curves and abbreviations same as in Figure. Mean pressure and flow lines on phasic curves of blood pressure, coronary flow and cardiac output should he ignored. Paper speed, mm/sec. Vertical time lines,. sec. Circulation Research, Vol. XXI, July 967
7 ADRENERGIC ACTIVITY IN CORONARY ARTERIES 8 saline (. ml) led to a maximum % increase in coronary blood flow and % fall in coronary resistance. In a representative animal (Fig. ), control recordings were obtained with the dog in the resting state. Isotonic saline was then given through the chronically implanted coronary artery catheter, and led to a fall in late diastolic coronary vascular resistance from. to. units (9% below control), sec after injection. Intracoronary isoproterenol injections (.6 /j.g in. ml isotonic saline) led to a 7% increase in mean coronary blood flow to sec after injection. Mean and late diastolic coronary vascular resistance fell and % respectively. Heart rate, aortic pressure, systolic ejection period, and cardiac output changed less than % at this time. After /8- adrenergic receptor blockade with intravenous propranolol ( mg/kg), isoproterenol in a dose equal to that used previously, failed to elicit a significant rise in coronary blood flow or fall in coronary vascular resistance. In the same animal as shown in Figure, SEC 7 SEC SEC 6 T ISOPROTERENOL I.6 ug in No Cl. ml IC FIGURE Continuous record showing hemodynamic effects of intracoronary isoproterenol. Conducting system intact and heart not paced. Order of curves and abbreviations same as in Figure. Mean pressure and flow lines on phasic curves of blood pressure, coronary flow and cardiac output should be ignored. Paper speed, mm/sec. Vertical time lines,. sec. Epinephrine (6^g IC) - Seconds 6 I& FIGURE S Hemodynamic effects of intracoronary epinephrine before and after p-adrenergic receptor blockade with propranolol ( mg/kg). Conducting system intact and heart not paced. Order of curves and abbreviations as in Figure. Mean pressure and flow lines on phasic curves of blood pressure, coronary flow and cardiac output should be ignored. Paper speed, 7 mm/see. Vertical time lines,. sec. Circulation Research, Vol. XXI, Jub 967
8 8 PITT, ELLIOT, GREGG isoproterenol led to a rise in coronary blood flow and fall in late diastolic coronary vascular resistance from. to.7 units at sec, and to. units at 7 sec after injection (% below control) while mean aortic pressure, heart rate, cardiac output, mean ventricular and peak ventricular ejection rates, and tension-time index calculated according to method of Sarnoff et al. () were not increased from control values (Fig. ). Ten seconds after injection, myocardial effects first became noticeable, and at sec, were manifested by a decrease in systolic ejection period from. to. sec (% below control), along with an increase in peak ventricular ejection rate (8% abpve control) and mean ventricular ejection rate (% above control). Intracoronary injections of epinephrine (.6 fig in. ml isotonic saline) increased mean coronary blood flow %, and decreased mean and late diastolic coronary vascular resistance and % respectively, to sec after beginning injection without any increase in heart rate, aortic pressure or change in systolic ejection period. After /- adrenergic receptor blockade, epinephrine led to an increase in. mean and late diastolic coronary vascular resistance of 9 and % respectively. In the experiment shown in Figure, epinephrine caused an initial coronary vasodilatation before any significant change in myocardial or systemic hemodynamics. Twelve seconds after injection, there was a further decrease in late diastolic coronary vascular resistance. The coronary vasodilatation seen at this time was accompanied by myocardial effects as manifested by a decrease in systolic ejection period. After /- adrenergic receptor blockade, epinephrine (.6 fig) led to a small increase in mean and late diastolic coronary vascular resistance. After a-adrenergic receptor blockade with intravenous dibenzylene ( mg/kg), intracoronary epinephrine and norepinephrine caused an initial coronary vasodilatation. In animal, epinephrine (.6 fig) led to an initial increase in coronary blood flow from to ml/min (% above control) while mean aortic pressure increased slightly from to mm Hg, to sec after injection. This resulted in a fall in mean and late diastolic coronary vascular resistance of and 8% respectively. Cardiac output and heart rate remained unchanged. After the administration of propranolol ( mg/kg) to the a-receptor blocked animal, epinephrine and norepinephrine had no effect on coronary vascular resistance. In the animal cited above, epinephrine (.6 fig) led to a slight fall in mean aortic pressure from to 98 mm Hg, while coronary blood flow remained unchanged at ml/min. Mean coronary resistance fell % while late diastolic resistance was unchanged. Discussion The results of the present investigation are consistent with the presence of both a- and /-adrenergic receptors in the coronary arteries of the unanesthetized dog, independent of adrenergic receptors in the myocardium. The finding of coronary vasoconstriction after intravenous and intracoronary injections of epinephrine and norepinephrine in the /-receptor blocked animal, and its elimination by a-adrenergic receptor blockade, suggests the presence of a- (vasoconstrictor) adrenergic receptors in the coronary arteries. These results are consistent with the findings of Zuberbuhler and Bohr () that epinephrine and norepinephrine cause contraction of isolated coronary artery strips after /-receptor blockade. Similarly Doutheil et al. (7), Gaal et al. (9), and Parratt (8) have demonstrated a-receptor activity after /-receptor blockade in the anesthetized open chest dog. Our finding of coronary vasoconstriction after intravenous phenylephrine and, in some instances, after intracoronary norepinephrine in the unanesthetized animal, is further evidence for the presence of a-receptors in the coronary arteries and suggests that these receptors can influence coronary flow in the absence of /-receptor blockade. The increase in coronary flow after intravenous catecholamine injection was accompanied by changes in aortic pressure and Circulation Research, Vol. XXI, July 967
9 ADRENERGIC ACTIVITY IN CORONARY ARTERIES 8 cardiac output, and could be attributed, at least in part, to myocardial stimulation and subsequent metabolic vasodilatation. There were, however, several instances in the unanesthetized dog with fixed ventricular rate, in which intravenous catecholamines caused an increase in coronary blood flow before any change in aortic pressure, systolic ejection period or cardiac output. Similarly, initial coronary vasodilatation after intracoronary isoproterenol, epinephrine and, in some instances, after norepinephrine, which can be eliminated by /-adrenergic receptor blockade, suggests the presence of /-adrenergic receptors in the coronary arteries. The initial coronary vasodilatation occurred to sec after beginning intracoronary injection of catecholamines before any significant increase in systemic or myocardial hemodynamic effects. Control intracoronary injection with isotonic saline led to a maximum? increase in coronary blood flow as compared to a greater than % increase in some experiments with isoproterenol and epinephrine. The increase in coronary blood flow seen to sec after intracoronary injection of catecholamines can be attributed both to a direct effect on the coronary vessels and to secondary metabolic vasodilatation. Myocardial effects were manifested on the coronary flow pattern by a shortening of the systolic flow period and, on occasion, by backflow during late systole. The positive chronotropic effect usually seen after catecholamines was minimized in our preparation by injection distally into the left circumflex coronary artery thereby bypassing the sinus node artery which usually originates from the right coronary artery (). Klocke et al. () found that catecholamines in physiologic concentrations failed to increase significantly the myocardial oxygen consumption in the arrested heart and Sonnenblick et al. (6) found that myocardial oxygen consumption is directly related to the speed of ventricular contraction. Therefore, it is unlikely that the initial coronary vasodilatation seen in our experiments before any increase in myocardial or systemic hemody- Circilaiiofi Research, Vol. XXI, Jub 967 namics was due to an increase in myocardial oxygen consumption and subsequent metabolic vasodilatation. Catecholamines in physiologic concentrations in nonbeating hearts can cause coronary vasodilatation (, 6); this adds further evidence that catecholamineinduced vasodilatation is, at least in part, due to a direct effect upon the vessels themselves. The conflicting reports on the direct effects of epinephrine and norepinephrine on the coronary vasculature, reviewed by Berne (), can be explained by the presence of both (X- and /-adrenergic receptors in the coronary circulation. Although we have not seen any initial coronary vasoconstriction after epinephrine prior to /-receptor blockade, it is possible that this may occur under certain conditions. Zuberbuhler and Bohr () have reported that in isolated coronary artery strips there are relatively more /-adrenergic receptors present in the small coronary vessels, and more a-receptors in the larger coronary vessels. The effects of the administration of an agent with both a- and /- adrenergic receptor activity such as epinephrine or norepinephrine may, therefore, depend on the relative proportion and distribution of a- and /-adrenergic receptors in the coronary vessels of a given animal, the route of administration, and on the experimental conditions affecting sympathetic tone such as anesthesia, hypoxia, and myocardial failure during open chest experiments. Studies in the completely denervated heart have shown that sympathetic nervous impulses are unnecessary for the performance of the heart under certain physiologic conditions (7). These studies make it unlikely that adrenergic receptors in the coronary arteries are essential to life. They may, however, play an important role in modifying the physiologic and pathophysiologic adaptation of the coronary circulation. References. BEHN'E, R. M.: Regulation of coronary blood flow. Physiol. Rev. :, 96.. BEBN'E, R. M.: Effect of epinephrine and norepinephrine on coronary circulation. Circulation Res. 6: 6, 98.
10 8 PITT, ELLIOT, GREGG. HARDIN, R. A., SCOTT, J. B., AND HADDY, F. J.: Effect of epinephrine and norepinephrine on coronary vascular resistance in dogs. Am. J. Physiol. : 76, 96.. ZuBERBUHLER, R. C, AND BOHE, D. F.: Responses of coronary smooth muscle to catecholamines. Circulation Res. 6:, 96.. DOUTHELL, U.: Wirkung von Brenzcatechinaminen auf die Coronardurchblutung an asystolischen Hundeherzen. Pflugers Arch. 87:, KLOCKE, F. J., KAISEH, G. A., Ross, J., JR., AND BRAUNWALD, E.: An intrinsic adrenergic vasodilator mechanism in the coronary vascular bed of the dog. Circulation Res. 6: 76, DOUTHEIL, U., TEN BRUCCENCATE, H. G., AND KRAMER, K.: Coronarvasomotorik under - Noradrenalin und Isopropylnoradrenalin nach Blockierung der adrenergischen /-Receptoren durch Nethalide. Pflugers Arch. 8: 8, PARRATT, J. R.: Blockade of sympathetic beta receptors in the myocardial circulation. Brit. J. Pharmacol. : 6, GAAL, P. G., KATTUS, A. A., KOLIN, A., AND Ross, C: Effects of adrenalin and noradrenalin on coronary blood flow before and after beta adrenergic blockade. Brit. J. Pharmacol. 6: 7, 9.. GRECG, D. E. KHOURI, E. M., AND RAYFORD, C. R.: Systemic and coronary energetics in the resting unanesthetized dog. Circulation Res. 6:, 96.. STARZL, T. E., AND GAERTNER, R. A.: Chronic heart block in dogs: A method for producing experimental heart failure. Circulation : 9, 9.. HERD, J. A., AND BARGER, A. C: Simplified technique for chronic catheterization of blood vessels. J. Appl. Physiol. 9: 7, 96.. SARNOFF, S. J., BRAUNWALD, E., WELCH, G. H., JR., CASE, R. B., AND STAINSBY, W. N.: Hemodynamic determinants of oxygen consumption of the heart with special reference to the tension-time index. Am. J. Physiol. 9: 8, 98.. JAMES, T. N.: Anatomy of the sinus node of the dog. Anat. Rec. :, 96.. KLOCKE, F. J., KAISER, G. A., Ross, J., JR., AND BRAUNWALD, E.: Mechanism of increase of myocardial oxygen uptake produced by catecholamines. Am. J. Physiol. 9:, SONNENBLICK, E. H., Ross, J., JR., COVELL, J. W., KAISER, G. A., AND BRAUNWALD, E.: Velocity of contraction as a determinant of myocardial oxygen consumption. Am. J. Physiol. 9: 9, DONALD, D. E., AND SHEPHERD, J. T.: Response to exercise in dogs with cardiac denervation. Am. J. Physiol. : 9, 98. Circulation Research, Vol. XXI, July 967
Coronary Hemodynamic Effects of Increasing Ventricular Rate in the Unanesthetized Dog
 Coronary Hemodynamic Effects of Increasing Ventricular Rate in the Unanesthetized Dog By Bertram Pitt, M.D., and Donald E. Gregg, Ph.D., M.D. ABSTRACT In five unanesthetized dogs with surgical heart block,
Coronary Hemodynamic Effects of Increasing Ventricular Rate in the Unanesthetized Dog By Bertram Pitt, M.D., and Donald E. Gregg, Ph.D., M.D. ABSTRACT In five unanesthetized dogs with surgical heart block,
is Prevented by Atropine
 Brit. Heart J., 1969, 31, 67. Action of Propranolol on Left Ventricular Contraction in Aortic Stenosis When a Fall in Heart Rate is Prevented by Atropine JOHN HAMER AND JAMES FLEMING From the Department
Brit. Heart J., 1969, 31, 67. Action of Propranolol on Left Ventricular Contraction in Aortic Stenosis When a Fall in Heart Rate is Prevented by Atropine JOHN HAMER AND JAMES FLEMING From the Department
Effects of Beta-Receptor Blockade on the Systemic and Coronary Hemodynamic Response to an Increasing Ventricular Rate in the Unanesthetized Dog
 Effects of Beta-Receptor Blockade on the Systemic and Coronary Hemodynamic Response to an Increasing Ventricular Rate in the Unanesthetized Dog By Fred R. Cobb, M.D., Robert J. Bache, M.D., aul A. Eberr,
Effects of Beta-Receptor Blockade on the Systemic and Coronary Hemodynamic Response to an Increasing Ventricular Rate in the Unanesthetized Dog By Fred R. Cobb, M.D., Robert J. Bache, M.D., aul A. Eberr,
Determination of Stroke Volume from Left Ventricular Isovolumetric Contraction and Ejection Times
 Determination of Stroke Volume from Left Ventricular Isovolumetric Contraction and Ejection Times Clarence M. AGRESS, M.D. and Stanley WEGNER SUMMARY Examination was made of the relationship of left ventricular
Determination of Stroke Volume from Left Ventricular Isovolumetric Contraction and Ejection Times Clarence M. AGRESS, M.D. and Stanley WEGNER SUMMARY Examination was made of the relationship of left ventricular
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006
 SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Citation Acta medica Nagasakiensia. 1984, 29
 NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
NAOSITE: Nagasaki University's Ac Title Author(s) Efficacy of Coenzyme Q10 Administra Aortic Stenosis and Pacemaker Induc Igarashi, Katsuro Citation Acta medica Nagasakiensia. 1984, 29 Issue Date 1984-10-25
Electrical Conduction
 Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Sinoatrial (SA) node Electrical Conduction Sets the pace of the heartbeat at 70 bpm AV node (50 bpm) and Purkinje fibers (25 40 bpm) can act as pacemakers under some conditions Internodal pathway from
Effect of Atrial and Ventricular Tachycardia on Cardiac Oxygen Consumption
 Effect of Atrial and Ventricular Tachycardia on Cardiac Oxygen Consumption fly Henry S. Badeer, M.D., and Kholil A. Feisol, M.D. Clinical experience has shown that ventricular is a more serious arrhythmia
Effect of Atrial and Ventricular Tachycardia on Cardiac Oxygen Consumption fly Henry S. Badeer, M.D., and Kholil A. Feisol, M.D. Clinical experience has shown that ventricular is a more serious arrhythmia
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Work as a Correlate of Canine Left Ventricular Oxygen Consumption, and the Problem of Catecholamine Oxygen Wasting
 273 Work as a Correlate of Canine Left Ventricular Oxygen Consumption, and the Problem of Catecholamine Oxygen Wasting G. ALEC ROOKE AND ERIC 0. FEIGL SUMMARY Neither stroke volume nor external cardiac
273 Work as a Correlate of Canine Left Ventricular Oxygen Consumption, and the Problem of Catecholamine Oxygen Wasting G. ALEC ROOKE AND ERIC 0. FEIGL SUMMARY Neither stroke volume nor external cardiac
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 11 The Cardiovascular System Slides 11.1 11.19 Lecture Slides in PowerPoint by Jerry L. Cook The Cardiovascular System
ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A
 THE EFFECTS OF ACUTELY INCREASED SYSTEMIC RESIST- ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A METHOD FOR THE CLINICAL DETECTION OF MITRAL INSUFFICIENCY By EUGENE BRAUNWALD, G. H. WELCH, JR., AND ANDREW G.
THE EFFECTS OF ACUTELY INCREASED SYSTEMIC RESIST- ANCE ON THE LEFT ATRIAL PRESSURE PULSE: A METHOD FOR THE CLINICAL DETECTION OF MITRAL INSUFFICIENCY By EUGENE BRAUNWALD, G. H. WELCH, JR., AND ANDREW G.
Effects of Propranolol on Patients with Complete Heart Block and Implanted Pacemakers
 Effects of Propranolol on Patients with Complete Heart Block and Implanted Pacemakers By EPHRAIM DONOSO, M.D., LAWRENCE J. COHN, M.D., BERTRAM J. NEWMAN, M.D., HENRY S. BLOOM, M.D., WILLIAm C. STFIN, M.D.,
Effects of Propranolol on Patients with Complete Heart Block and Implanted Pacemakers By EPHRAIM DONOSO, M.D., LAWRENCE J. COHN, M.D., BERTRAM J. NEWMAN, M.D., HENRY S. BLOOM, M.D., WILLIAm C. STFIN, M.D.,
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
The Cardiovascular System
 11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
11 PART A The Cardiovascular System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Cardiovascular
THE increase in cardiac output during
 Effects of Cateeholamines and Atropine on Cardiovascular Response to Exercise in the Dog By ERNST W. 0. KECK, M.D., MICHAEL J. ALLWOOD, M.B., PH.D., ROBERT J. MARSHALL, M.D., M.R.C.P., AND JOHN T. SHEPHERD,
Effects of Cateeholamines and Atropine on Cardiovascular Response to Exercise in the Dog By ERNST W. 0. KECK, M.D., MICHAEL J. ALLWOOD, M.B., PH.D., ROBERT J. MARSHALL, M.D., M.R.C.P., AND JOHN T. SHEPHERD,
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition
 TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
Reduction of the Cardiac Response to Postganglionic Sympathetic Nerve Stimulation in Experimental Heart Failure
 Reduction of the Cardiac Response to Postganglionic Sympathetic Nerve Stimulation in Experimental Heart Failure By James W. Covell, M.D., Charles A. Chidsey, M.D., and Eugene Braunwald, M.D. ABSTRACT The
Reduction of the Cardiac Response to Postganglionic Sympathetic Nerve Stimulation in Experimental Heart Failure By James W. Covell, M.D., Charles A. Chidsey, M.D., and Eugene Braunwald, M.D. ABSTRACT The
Central haemodynamics during spontaneous angina pectoris
 British Heart Journal, I974, 36, I0-I09I Central haemodynamics during spontaneous angina pectoris From the Department of Clinical Physiology, Malmo General Hospital, S-214 OI Malmo, Sweden. Central pressures
British Heart Journal, I974, 36, I0-I09I Central haemodynamics during spontaneous angina pectoris From the Department of Clinical Physiology, Malmo General Hospital, S-214 OI Malmo, Sweden. Central pressures
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Cholinergic mechanisms on the heart and coronary circulaidon
 Br. J. Pharmac. (1970), 38, 93-105. Cholinergic mechanisms on the heart and coronary circulaidon MARTA I. BLESA AND G. ROSS Department of Physiology, U.C.L.A. School of Medicine, Los Angeles, California
Br. J. Pharmac. (1970), 38, 93-105. Cholinergic mechanisms on the heart and coronary circulaidon MARTA I. BLESA AND G. ROSS Department of Physiology, U.C.L.A. School of Medicine, Los Angeles, California
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Collin County Community College
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 5 The Heart 1 The Heart Beat and the EKG 2 1 The Heart Beat and the EKG P-wave = Atrial depolarization QRS-wave = Ventricular depolarization
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 5 The Heart 1 The Heart Beat and the EKG 2 1 The Heart Beat and the EKG P-wave = Atrial depolarization QRS-wave = Ventricular depolarization
-12. -Ensherah Mokheemer - ABDULLAH ZREQAT. -Faisal Mohammad. 1 P a g e
 -12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
-12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Special circulations, Coronary, Pulmonary. Faisal I. Mohammed, MD,PhD
 Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Warm Up- Monday -AND- Setup Cornell Notes.
 Warm Up- Monday Brainstorm in your notebook: If the heart sends blood to all organs, how and where does the heart get blood to provide oxygen for its muscles? -AND- Setup Cornell Notes. Announcements Unit
Warm Up- Monday Brainstorm in your notebook: If the heart sends blood to all organs, how and where does the heart get blood to provide oxygen for its muscles? -AND- Setup Cornell Notes. Announcements Unit
Sympathetic Control of Coronary Circulation
 Sympathetic of Coronary Circulation By Eric. Feigl, M.D. ABSTRACT The sympathetic control of left circumflex coronary blood flow was studied by stellate ganglion and hypothalamic stimulation. Flow was
Sympathetic of Coronary Circulation By Eric. Feigl, M.D. ABSTRACT The sympathetic control of left circumflex coronary blood flow was studied by stellate ganglion and hypothalamic stimulation. Flow was
Effect of Exercise on Cardiac Output, Left Coronary Flow and Myocardial Metabolism in the Unanesthetized Dog
 Effect of Exercise on Cardiac Output, Left Coronary Flow and Myocardial Metabolism in the Unanesthetized Dog By Edward M. Khouri, Donald E. Gregg, Ph.D., M.D., and Claudia R. Rayford, Ph.D. Studies of
Effect of Exercise on Cardiac Output, Left Coronary Flow and Myocardial Metabolism in the Unanesthetized Dog By Edward M. Khouri, Donald E. Gregg, Ph.D., M.D., and Claudia R. Rayford, Ph.D. Studies of
The Cardiovascular System (Heart)
 The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
The Cardiovascular System The Cardiovascular System (Heart) A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function
BUSINESS. Articles? Grades Midterm Review session
 BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
BUSINESS Articles? Grades Midterm Review session REVIEW Cardiac cells Myogenic cells Properties of contractile cells CONDUCTION SYSTEM OF THE HEART Conduction pathway SA node (pacemaker) atrial depolarization
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Chronotropic and Inotropic Effects of 3 Kinds of Alpha-Adrenergic Blockers on the Isolated Dog Atria
 Chronotropic and Inotropic Effects of 3 Kinds of Alpha-Adrenergic Blockers on the Isolated Dog Atria Shigetoshi CHIBA, M.D., Yasuyuki FURUKAWA, M.D., and Hidehiko WATANABE, M.D. SUMMARY Using the isolated
Chronotropic and Inotropic Effects of 3 Kinds of Alpha-Adrenergic Blockers on the Isolated Dog Atria Shigetoshi CHIBA, M.D., Yasuyuki FURUKAWA, M.D., and Hidehiko WATANABE, M.D. SUMMARY Using the isolated
Arterial CO 2, Myocardial O 2 Consumption, and Coronary Blood Flow in the Dog
 Arterial CO 2, Myocardial O 2 Consumption, and Coronary Blood Flow in the Dog 217 THOM ROOKE AND HARVEY V. SPARKS SUMMARY We determined the effect of changes in arterial Pco 2 on the relationship between
Arterial CO 2, Myocardial O 2 Consumption, and Coronary Blood Flow in the Dog 217 THOM ROOKE AND HARVEY V. SPARKS SUMMARY We determined the effect of changes in arterial Pco 2 on the relationship between
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Structure and organization of blood vessels
 The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
The cardiovascular system Structure of the heart The cardiac cycle Structure and organization of blood vessels What is the cardiovascular system? The heart is a double pump heart arteries arterioles veins
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
WHILE it is generally agreed that elevation
 The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
The Derivation of Coronary Sinus Flow During Elevation of Right Ventricular Pressure By HERMAN M. GELLER, B.S., M.D., MARTIN BRANDFONBRENEU, M.D., AND CARL J. WIGGERS, M.D., The derivation of coronary
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
Approximately the size of your fist Location. Pericardial physiology
 Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
Heart Anatomy Approximately the size of your fist Location Superior surface of diaphragm Left of the midline Anterior to the vertebral column, posterior to the sternum Wednesday, March 28, 2012 Muscle
The Mammalian Circulatory System
 The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
The Mammalian Heart The Mammalian Circulatory System Recall: What are the 3 cycles of the mammalian circulatory system? What are their functions? What are the three main vessel types in the mammalian circulatory
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Physiology and Pharmacology
 Pharmacokinetics Physiology and Pharmacology Pharmacokinetics of Local Anesthetics Uptake Oral Route Topical Route Injection Distribution Metabolism (Biotransformation) Excretion Uptake Vasoactivity Local
Pharmacokinetics Physiology and Pharmacology Pharmacokinetics of Local Anesthetics Uptake Oral Route Topical Route Injection Distribution Metabolism (Biotransformation) Excretion Uptake Vasoactivity Local
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
THE low blood pressure, the prolonged
 The Effect of Immersion Hypothermia on Coronary Blood Flow By ROBERT M. BERNE, M.D. In severe hypothermia resistance in the coronary vascular bed is reduced and flow continues despite very low aortic pressure.
The Effect of Immersion Hypothermia on Coronary Blood Flow By ROBERT M. BERNE, M.D. In severe hypothermia resistance in the coronary vascular bed is reduced and flow continues despite very low aortic pressure.
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
The circulatory system
 Introduction to Physiology (Course # 72336) 1 הלב עקרונות בסיסיים (הכנה למעבדת לב) Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Introduction to Physiology (Course # 72336) 1 הלב עקרונות בסיסיים (הכנה למעבדת לב) Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Effect of Left Ventricular Hypertension, Ischemia and Vasoactive Drugs on the Myocardial Distribution of Coronary Flow
 Effect of Left Ventricular Hypertension, Ischemia and Vasoactive Drugs on the Myocardial Distribution of Coronary Flow By Thomas W. Moir, M.D., and Don W. DeBra, M.D. ABSTRACT Distribution of coronary
Effect of Left Ventricular Hypertension, Ischemia and Vasoactive Drugs on the Myocardial Distribution of Coronary Flow By Thomas W. Moir, M.D., and Don W. DeBra, M.D. ABSTRACT Distribution of coronary
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Principles of Anatomy and Physiology 14 th Edition CHAPTER 20 The Cardiovascular System: The Heart Introduction The purpose of the chapter is to: 1. Learn about the components of the cardiovascular system
Introduction to Physiology (Course # 72336) 1. Adi Mizrahi Textbook Chapter 12
 Introduction to Physiology (Course # 72336) 1 עקרונות בסיסיים (הכנה למעבדת לב) הלב Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
Introduction to Physiology (Course # 72336) 1 עקרונות בסיסיים (הכנה למעבדת לב) הלב Adi Mizrahi mizrahia@cc.huji.ac.il Textbook Chapter 12 2 The circulatory system To the heart Away from the heart 3 L 2.5
OXYGEN CONSUMPTION' JREISSATY, AND JIRO NAKANO 4. cannula was introduced via the left external jugular vein
 EFFECT OF AORTIC INSUFFICIENCY ON ARTERIAL BLOOD PRESSURE, CORONARY BLOOD FLOW AND CARDIAC OXYGEN CONSUMPTION' By RENE WEGRIA, GERHARD MUELHEIMS,2 JAMES GOLUB,3 ROBERT JREISSATY, AND JIRO NAKANO 4 (From
EFFECT OF AORTIC INSUFFICIENCY ON ARTERIAL BLOOD PRESSURE, CORONARY BLOOD FLOW AND CARDIAC OXYGEN CONSUMPTION' By RENE WEGRIA, GERHARD MUELHEIMS,2 JAMES GOLUB,3 ROBERT JREISSATY, AND JIRO NAKANO 4 (From
Cardiac Output in Conscious One-clip, Two-kidney Renovascular Hypertensive Rats*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 1, March, 1983 HIJM 32-9 59 Cardiac Output in Conscious One-clip, Two-kidney Renovascular Hypertensive Rats*) Yasuhiro TERANISHI and Juro IRIUCHIJIMA
Hiroshima Journal of Medical Sciences Vol. 32, No. 1, March, 1983 HIJM 32-9 59 Cardiac Output in Conscious One-clip, Two-kidney Renovascular Hypertensive Rats*) Yasuhiro TERANISHI and Juro IRIUCHIJIMA
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Enhancement of Coronary Vasodilator Action of Adenosine Triphosphate by Dipyridamole
 Enhancement of Coronary Vasodilator Action of Adenosine Triphosphate by Dipyridamole By Skoda Afomo, M.D., Ph.D., and George S. O'Brien, M.D., Ph.D. ABSTRACT It has been reported that previously administered
Enhancement of Coronary Vasodilator Action of Adenosine Triphosphate by Dipyridamole By Skoda Afomo, M.D., Ph.D., and George S. O'Brien, M.D., Ph.D. ABSTRACT It has been reported that previously administered
The Circulatory System (p )
 The Circulatory System (p. 268-281) How Does Gravity Affect Blood Circulation? As with all land animals, the giraffe and the corn snake are constantly subject to the force of gravity The circulatory system
The Circulatory System (p. 268-281) How Does Gravity Affect Blood Circulation? As with all land animals, the giraffe and the corn snake are constantly subject to the force of gravity The circulatory system
Hemodynamic effects of isoproterenol and norepinephrine in acute cardiac tamponade
 Hemodynamic effects of isoproterenol and norepinephrine in acute cardiac tamponade Noble O. Fowler, John C. Holmes J Clin Invest. 1969;48(3):502-507. https://doi.org/10.1172/jci106007. Research Article
Hemodynamic effects of isoproterenol and norepinephrine in acute cardiac tamponade Noble O. Fowler, John C. Holmes J Clin Invest. 1969;48(3):502-507. https://doi.org/10.1172/jci106007. Research Article
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
An Official Journal of the American Heart Association
 Circulation Research SEPTEMBER VOL. XXV 1969 NO. 3 An Official Journal of the American Heart Association Myocardial Contractile Response to Norepinephnne, Isoproterenol, and Calcium Chloride in Hyperthyroid
Circulation Research SEPTEMBER VOL. XXV 1969 NO. 3 An Official Journal of the American Heart Association Myocardial Contractile Response to Norepinephnne, Isoproterenol, and Calcium Chloride in Hyperthyroid
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Cardiovascular System Notes: Physiology of the Heart
 Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Lab 16. The Cardiovascular System Heart and Blood Vessels. Laboratory Objectives
 Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
Lab 16 The Cardiovascular System Heart and Blood Vessels Laboratory Objectives Describe the anatomical structures of the heart to include the pericardium, chambers, valves, and major vessels. Describe
Cardiovascular System. Heart
 Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
Cardiovascular System Heart Electrocardiogram A device that records the electrical activity of the heart. Measuring the relative electrical activity of one heart cycle. A complete contraction and relaxation.
In the name of GOD. Animal models of cardiovascular diseases: myocardial infarction & hypertension
 In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
In the name of GOD Animal models of cardiovascular diseases: myocardial infarction & hypertension 44 Presentation outline: Cardiovascular diseases Acute myocardial infarction Animal models for myocardial
Evidence for the Direct Effect of Adrenergic Drugs on the Cerebral Vascular Bed of the Unanesthetized Goat
 Evidence for the Direct Effect of Adrenergic Drugs on the Cerebral Vascular Bed of the Unanesthetized Goat BY SALVADOR LLUCH, M.D., CHARLES REIMANN, M.D., AND GERALD GLICK, M.D. Abstract: Evidence for
Evidence for the Direct Effect of Adrenergic Drugs on the Cerebral Vascular Bed of the Unanesthetized Goat BY SALVADOR LLUCH, M.D., CHARLES REIMANN, M.D., AND GERALD GLICK, M.D. Abstract: Evidence for
Pressure-Flow Relationships in the Coronary Circulation
 Pressure-Flow Relationships in the Coronary Circulation By Wadie M. Fam, M.D., Ph.D., and Maurice McGregor, M.D. ABSTRACT This study was designed to define more accurately the respective influences of
Pressure-Flow Relationships in the Coronary Circulation By Wadie M. Fam, M.D., Ph.D., and Maurice McGregor, M.D. ABSTRACT This study was designed to define more accurately the respective influences of
The Cardiovascular System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Essentials of Human Anatomy & Physiology Elaine N. Marieb Slides 11.1 11.19 Seventh Edition Chapter 11 The Cardiovascular System Functions of the Cardiovascular system Function of the heart: to pump blood
Duration of the Phases of Left Ventricular Systole
 Duration of the Phases of Left Ventricular Systole By Andrew G. Wallace, M.D., Jere H. Mitchell, M.D., N. Sheldon Skinner, M.D., and Stanley J. Sarnoff, M.D. The influence of heniodynamic variables on
Duration of the Phases of Left Ventricular Systole By Andrew G. Wallace, M.D., Jere H. Mitchell, M.D., N. Sheldon Skinner, M.D., and Stanley J. Sarnoff, M.D. The influence of heniodynamic variables on
Forward Looking Statement
 Forward Looking Statement This presentation contains forward-looking statements. All forward looking statements are management s (Dave Rosa) present expectations of future events and are subject to a number
Forward Looking Statement This presentation contains forward-looking statements. All forward looking statements are management s (Dave Rosa) present expectations of future events and are subject to a number
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co.
 Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Anatomy Review: The Heart Graphics are used with permission of A.D.A.M. Software, Inc. and Benjamin/Cummings Publishing Co. Anatomy Views Label the diagrams of the heart below: Interactive Physiology Study
Actions of prostaglandin F20 on the splenic vascular and capsular smooth muscle in the dog
 Br. J. Pharmac. (1971), 41, 1-7 Actions of prostaglandin F20 on the splenic vascular and capsular smooth muscle in the dog B. N. DAVIES ADi P. G. WITHRINGTON Department of Physiology, Medical College of
Br. J. Pharmac. (1971), 41, 1-7 Actions of prostaglandin F20 on the splenic vascular and capsular smooth muscle in the dog B. N. DAVIES ADi P. G. WITHRINGTON Department of Physiology, Medical College of
Figure ) The specific chamber of the heart that is indicated by letter A is called the. Diff: 1 Page Ref: 364
 Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Essentials of Anatomy and Physiology, 9e (Marieb) Chapter 11 The Cardiovascular System Short Answer Figure 11.1 Using Figure 11.1, identify the following: 1) The Purkinje fibers are indicated by label.
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Circulation. Sinoatrial (SA) Node. Atrioventricular (AV) Node. Cardiac Conduction System. Cardiac Conduction System. Linked to the nervous system
 Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Circulation Cardiac Conduction System AHS A H S Your body resembles a large roadmap. There are routes or arteries that take you downtown to the heart of the city and veins that take you to the outskirts
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Circulatory System Review
 Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
Circulatory System Review 1. Know the diagrams of the heart, internal and external. a) What is the pericardium? What is myocardium? What is the septum? b) Explain the 4 valves of the heart. What is their
The Cardiovascular System
 Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
Chapter 18 Part A The Cardiovascular System 1/19/16 1 Annie Leibovitz/Contact Press Images Similarities of Cardiac and Skeletal Muscle RMP Ion concentration Deploarization Action Potential Repolarization
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
THE EFFECT OF PROPRANOLOL ON THE CARDIO- VASCULAR RESPONSES TO ISOPRENALINE, ADRENALINE AND NORADRENALINE IN THE ANAESTHETIZED DOG
 Brit. J. Pharmacol. (1966), 26, 322-333. THE EFFECT OF PROPRANOLOL ON THE CARDIO- VASCULAR RESPONSES TO ISOPRENALINE, ADRENALINE AND NORADRENALINE IN THE ANAESTHETIZED DOG BY R. G. SHANKS From Imperial
Brit. J. Pharmacol. (1966), 26, 322-333. THE EFFECT OF PROPRANOLOL ON THE CARDIO- VASCULAR RESPONSES TO ISOPRENALINE, ADRENALINE AND NORADRENALINE IN THE ANAESTHETIZED DOG BY R. G. SHANKS From Imperial
Prevention of Acetylcholine-Induced Atrial Fibrillation. Shigetoshi CHIBA, M.D. and Koroku HASHIMOTO, M.D.
 Prevention of Acetylcholine-Induced Atrial Fibrillation by Electric Pacing Shigetoshi CHIBA, M.D. and Koroku HASHIMOTO, M.D. SUMMARY The sinus node artery of 10 dog hearts was auto-perfused with blood
Prevention of Acetylcholine-Induced Atrial Fibrillation by Electric Pacing Shigetoshi CHIBA, M.D. and Koroku HASHIMOTO, M.D. SUMMARY The sinus node artery of 10 dog hearts was auto-perfused with blood
RESEARCH IN BASIC SCIENCE
 RESEARCH IN BASIC SCIENCE Effect of High-Dose Sodium Bicarbonate on the Vasopressor Effects of Epinephrine During Cardiopulmonary Resuscitation Barry E. Bleske, Pharm.D., Eric W Warren, Pharm.D., Ted L.
RESEARCH IN BASIC SCIENCE Effect of High-Dose Sodium Bicarbonate on the Vasopressor Effects of Epinephrine During Cardiopulmonary Resuscitation Barry E. Bleske, Pharm.D., Eric W Warren, Pharm.D., Ted L.
Cardiovascular System: The Heart
 Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
Cardiovascular System: The Heart I. Anatomy of the Heart (See lab handout for terms list) A. Describe the size, shape and location of the heart B. Describe the structure and function of the pericardium
QUIZ 2. Tuesday, April 6, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Mechanism of Constriction of Large Coronary Arteries by #-Adrenergic Receptor Blockade
 389 Mechanism of Constriction of Large Coronary Arteries by #-Adrenergic Receptor Blockade Stephen F. Vatner and Thomas H. Hintze From the Departments of Medicine, Harvard Medical School and Brigham and
389 Mechanism of Constriction of Large Coronary Arteries by #-Adrenergic Receptor Blockade Stephen F. Vatner and Thomas H. Hintze From the Departments of Medicine, Harvard Medical School and Brigham and
Effects of Hypoxia and Metabolic Inhibitors on the Intrinsic Heart Rate and Myocardial Contractility in Dogs
 Effects of Hypoxia and Metabolic Inhibitors on the Intrinsic Heart Rate and Myocardial Contractility in Dogs By Anthony D. Jose, M.A., and Frank Sritt, M.B. ABSTRACT Previous studies have shown that after
Effects of Hypoxia and Metabolic Inhibitors on the Intrinsic Heart Rate and Myocardial Contractility in Dogs By Anthony D. Jose, M.A., and Frank Sritt, M.B. ABSTRACT Previous studies have shown that after
Myocardial lactate metabolism during isometric hand grip test
 British HeartJournal, I975, 37, 79-84. Myocardial lactate metabolism during isometric hand grip test Comparison with pacing tachycardia F. Khan Nakhjavan, Gangaiah Natarajan, Allan M. Smith, Michael Dratch,
British HeartJournal, I975, 37, 79-84. Myocardial lactate metabolism during isometric hand grip test Comparison with pacing tachycardia F. Khan Nakhjavan, Gangaiah Natarajan, Allan M. Smith, Michael Dratch,
My task is to provide some general information
 AJH 1998;11:41S 45S Aging, Changes in the Cardiovascular System, and Responses to Stress Myron Weisfeldt My task is to provide some general information about the cardiovascular changes associated with
AJH 1998;11:41S 45S Aging, Changes in the Cardiovascular System, and Responses to Stress Myron Weisfeldt My task is to provide some general information about the cardiovascular changes associated with
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
Large Arteries of Heart
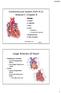 Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
Cardiovascular System (Part A-2) Module 5 -Chapter 8 Overview Arteries Capillaries Veins Heart Anatomy Conduction System Blood pressure Fetal circulation Susie Turner, M.D. 1/5/13 Large Arteries of Heart
