Cell-based description of ventricular contraction in a model of the human cardiovascular system
|
|
|
- Aileen Reeves
- 6 years ago
- Views:
Transcription
1 Cell-based description of ventricular contraction in a model of the human cardiovascular system S. Kosta J. Negroni E. Lascano P. C. Dauby University of Liege, GIGA - Cardiovascular Sciences, Belgium ( sarah.kosta@ulg.ac.be). Department of Comparative Cellular and Molecular Biology, Favaloro University, Buenos Aires, Argentina Abstract: A multiscale model of the cardiovascular system (CVS) is presented. Hemodynamics is described by a lumped parameter model, while heart contraction is described at the cellular scale. An electrophysiological model and a mechanical model were coupled and adjusted so that the pressure and volume of both ventricles are linked to the force and length of a half-sarcomere. Particular attention was paid to the extremal values of the sarcomere length, which must keep physiological values. This model is able to reproduce healthy behavior, preload variations experiments, and ventricular failure. Keywords: Mathematical models - Physiological models - Multiscale models - Cardiovascular system - Sarcomere contraction 1. INTRODUCTION Mathematical models of biological systems have become a powerful tool for cardiovascular sciences. These models allow for a variety of studies that are generally difficult to implement experimentally. A model of the whole cardiovascular system (CVS) basically needs a mathematical description of the following two components: The hemodynamics of the systemic and pulmonary circulation The active contraction of the heart The hemodynamics, i.e. the blood flow evolution inside the blood vessels, is described here with a lumpedparameter model. The heart contraction is often decribed with ad hoc models, like the varying elastance model. Such macroscopic models are not based on the cardiac tissue properties and can not reproduce behaviors that arise from the microscopic scale. In this work we use a cardiac cell contraction model that we connect to the organ scale in order to get a multiscale model of the human CVS. The purpose of this model is to link macroscopic properties to the microscopic behaviors they originate from, a correlation impossible to establish with phenomenological models. R sys P vc V vc Vena cava P ao V ao Aorta R av R tc P rv V rv RV P lv V lv LV Active contraction R mt P pa V pa PA P pu V pu PU Fig. 1. Diagram of the 6-chamber hemodynamic model: left ventricle (LV), right ventricle (RV), pulmonary artery (PA), pulmonary vein (PU), aorta (AO), vena cava (VC). 2.1 Flow in the CVS The flow inside the systemic and pulmonary circulation can be written as: R pv R pul 2. METHODS Q(t) = P i(t) P o(t) R (1) Our lumped-parameters model of the CVS consists of a 6-chamber model, two of which being able of active contraction (Burkhoff and Tyberg (1993)). A schematic representation of this model is depicted on Fig. 1. P.C.D. acknowledges travel financial support from F.R.S.-FNRS. where P i is the pressure at the entrance of the chamber, P o the pressure at the exit, and R is the hydraulic resistance of the blood vessels. The four cardiac valves (mitral, aortic, tricuspid, and pulmonary) act as diodes and allow for the unidirectionnality of the flow.
2 2.2 Passive chambers The aorta (AO), vena cava (VC), pulmonary artery (PA), and pulmonary vein (PU) are considered as passive chamber (unable of active contraction). The pressure-volume relationship in these chambers is written as: P (t) = E V (t) (2) where E is the elastance of the corresponding chamber. Finally, the chamber volume changes are described by the following differential equation: dv dt = Q in Q out (3) where Q in and Q out are the flows that respectively enters and leaves the chamber. stroke (TSCa 3). Finally the three calcium ions can detach (TS ) and the crossbridges eventually detach to end the cycle. The active force is also proportionnal to the concentrations of the three states with attached crossbridges (TSCa 3, TSCa 3, and TS ). Troponin currents were added in the equation governing calcium concentration from the Ten Tusscher and Panfilov model, thus linking the electrophysiology and the mechanical contraction of the cell. We then had to reduce the total cytosolic calcium buffer concentration to 100 µm provided that the buffering due to troponin was taken into account in the calcium kinetics described previously. Ventricle model To connect the force F m and total length L m of the half-sarcomere to the pressure and volume of the active chamber, both ventricles are simply considered as spheres, as shown on Fig Active chambers Cell model The left and right ventricles are capable of active contractions, which are described at the cellular scale. Cardiac cells are excitable and contractile. We use the electrophysiological model of ten Tusscher and Panfilov (2006) to describe the ionic currents across the cell membrane and the mechanical model of Negroni and Lascano (2008) to describe the contraction. The cellular force is derived from the contraction of a half-sarcomere (basic unit of cell contraction), as shown on Fig. 2. Thick filament Parallel element Thin filament Fig. 3. Spherical ventricle model. Left: Top view of the ventricle. N sarcomeres are aligned along a circle of radius R (dotted black). Right: Both ventricles are assimilated to thin spheres. The wall stress σ is related to the force produced by the sarcomeres and allows for the calculus of the pressure inside the ventricle. As already done by Shim et al. (2007), we assume that N half-sarcomeres of total rest length L m0 are aligned along a circle of radius R 0 : Fig. 2. Sarcomere contraction model (adapted from Negroni and Lascano (2008)). Left: Representation of a half-sarcomere of length L. L m is the total length and allows to account for the compliant (elastic) ends of the muscle. Right: Calcium kinetics. Myosin heads (also called crossbridges) of the thick filament attach to the thin filament and initiate the muscular contraction. This model describes the behavior of an equivalent crossbridge that represents all the crossbridges of the half-thick filament. It is assimilated to a linear spring of horizontal elongation h. The active force is proportionnal to this elongation. A parallel elastic element is added to account for the passive force of the muscle. Calcium kinetics is described with a 5-state model represented on Fig. 2 (two states from the original paper were merged into one, see Negroni et al. (2015)). A troponin system (TS) is composed of three adjacent troponintropomyosin units and can fix three calcium ions in one step (TSCa 3 ). Then three crossbridges can attach to the actin molecules in a weak pre-power stroke state (TSCa 3 ), then in a state where they are able to develop a power L m0 = 2πR 0 N. (4) This radius was chosen so that the total half-sarcomere length L m during a heartbeat varies between physiologically relevant extremes, i.e. between 0.98 and µm (Rodriguez et al. (1992)). There is indeed an important (yet not fully elucidated) relationship between the force and the length of the cardiac muscle. This leads to important properties at the organ scale, especially the Franck-Starling mechanism. Thus it was essential to get the correct interval of variation for L m in our multiscale model. The blood volume inside the ventricle is given by: V int = 4 3 πr in 3. (5) During a heartbeat, this volume varies according equation (3). Thus L m is given by: where R is calculated using: L m = 2πR N (6)
3 V int + V wr = 4 3 πr3. (7) In this relation, V wr is the constant volume of the incompressible wall included between r int (at the beginning of diastole) and R. Now we have to connect the pressure P inside the ventricular cavity to the force F produced by the half-sarcomeres. We assume that many contractile units are distributed homogeneously in all directions on the ventricular wall (Shim et al. (2007)), so that the wall stress σ can be considered uniform. With a constant wall stress σ, the equilibrium of the two hemispheres of the ventricles gives the following expression of the pressure inside the active chambers: where σ is given by: P = σ( r out 2 r in 2 σ = F A 1) (8) with F the force and A the cross-sectional area. The mechanical contraction model actually provides F m, the force normalized with respect to the muscle crosssectional area measured at a defined reference state, A r : (9) F m = F A r. (10) Assuming that muscle units have constant volume, we also have: L r A r = L m A (11) where L r is the total sarcomere length at the reference aera A r. From (9) - (11), we can obtain the pressure-force relation of our multiscale model : L m P = 7.5 F m ( r 2 out L r r 2 1) + γ(v in V 0 ) 3. (12) in The 7.5 factor stands for the units change (pressure is expressed in mmhg) and the last term is a passive pressure that accounts globally for the elastic properties of the tissue surrounding the ventricle (γ is the stiffness and V 0 is the unstressed volume). The multiscale model presented above depends on many parameters, which can be split into microscopic (or cellular) parameters and macroscopic (or hemodynamic) parameters. The hemodynamic parameters (resistances and elastances of passive chambers, wall thickness of the ventricles) were optimized so that the following quantities range around human physiological values: systolic pressure (for both ventricles), amplitude of the aortic pressure, amplitude of the pulmonary artery pressure, systolic volume (for both ventricles), and stroke volume. The values of the cellular parameters can be obtained in the original papers in which the electrophysiological model and the contractile model were developed (ten Tusscher and Panfilov (2006); Negroni and Lascano (2008)). However, when these values of the cellular parameters are used in the complete multiscale model of the CVS, the ventricular pressure calculated at the end of diastole (filling phase of the ventricle) was found too high, while the systolic pressure (ejecting phase of the ventricle) was too low compared to physiological values. This difficulty originates from the too simple geometrical description of the ventricles, which are here considered as spheres. In a real heart, bundles of cardiac fibers are actually wrapped around the ventricular cavity so that the ventricle is also twisted in a very complex way during contraction. Of course the spherical model of ventricles presented above cannot take into account this aspect of contraction and an adaptation of the values of some parameters was necessary to compensate for the simplicity of the model. From (8), it is easy to understand that the systolic pressure, which is related to the maximum active force generated in the sarcomeres, can be increased by increasing the ventricle wall thickness. However, since the diastolic pressure, which is related to the passive force in the myocytes, also increases with the wall thickness, we had to drastically reduce the intensity of the sarcomere passive force in order to recover physiological diastolic pressures. In summary, the price to pay for the spherical model of the ventricles is a value of the wall thickness which is higher than standard physiological values and an important reduction factor to apply to the cellular parameter measuring the passive force of the sarcomere. All other cellular parameters keep however their original values, except for the total cytosolic calcium buffer concentration, as explained previously. The adjusted parameters are summarized in Table 1. Table 1. Adjusted parameters Parameter K e (In passive force) L e (In passive force) SBV (Stressed Blood Volume) R sys (Systemic resistance) R pul (Pulmonary resistance) R mt (Mitral valve resistance) R tc (Tricuspid valve resistance) R vaor (Aortic valve resistance) R pv (Pulmonary valve resistance) E ao (Aorta elastance) E vc (Vena cava elastance) E pa (Pulmonary artery elastance) E pv (Pulmonary vein elastance) V lvw (Left ventricular wall volume) V rvw (Right ventricular wall volume) 3. RESULTS Value mnmm 2 µm 5 3 mnmm 2 µm ml mmhg ms ml mmhg ms ml mmhg ms ml mmhg ms ml mmhg ms ml mmhg ms ml mmhg ml mmhg ml mmhg ml mmhg ml ml ml We first simulated a baseline situation corresponding to a healthy individual. Some important microscopic variables are presented on Fig. 4 with their corresponding macroscopic variables. The action potential, the intracellular calcium, and the force time evolutions are correctly reproduced. It is important to stress that the sarcomere length lies between physiological values (Rodriguez et al. (1992)).
4 The pressure-volume loops are also correctly reproduced. Some hemodynamic variables are also shown on Fig. 5. Fig. 5. Hemodynamic variables. The top two curves represent the flow through the aortic valve (normal) and through the pulmonary valve (dotted) during one heartbeat. Left ventricular pressure (bold), aortic pressure (dashed), right ventricular pressure (normal) and pulmonary pressure (dash-dotted) are also represented. Fig. 4. Top panel: Action potential (bold), normalized force (normal), and intracellular calcium (dashed) time evolution during one heartbeat in the left ventricle. Middle panel: Sarcomere length (normal) and left ventricular volume (dash-dotted) time evolution during the same heartbeat. Bottom panel: Pressurevolume loop in the left (bold) and right (normal) ventricle during the same heartbeat. We also simulated a preload variation experiment. To mimic the inflation of a Fogarty balloon, which is a current way of reducing preload, we have increased tricuspid valve resistance, thus allowing less blood to enter the right ventricle. The consequences on the pressure-volume loops on both ventricles are presented on Fig. 6. It is worth emphasizing that the upper left corners of the PV-loops are not exactly located on a straight line, as often postulated when varying elastance models of contraction are used. Fig. 6. Pressure-volume loops in the left and right ventricle during a decrease in preload in the right ventricle. Eventually, we simulated a case of ventricular failure. It has been shown that heart failure symptoms originate at the cellular scale (Beuckelmann et al. (1992, 1993); Wang and Hill (2010)). Alterations in ionic currents and calcium handling lead to a prolonged action potential, a lower peak of intracellular calcium, and a lower force. Reduction in current densities of the inward rectifier K + current and the transient outward K + current, increased activity of the Na + /Ca 2+ exchanger and a reduced Ca 2+ sequestration by the sarcoplasmic reticulum were implemented in our model. Our multiscale model is then able to connect these cellular altered properties to the hemodynamics variables, as shown on Fig DISCUSSION We have developed a multiscale model of the human CVS based on the ten Tusscher and Panfilov model of electrophysiology, the Negroni and Lascano model of sarcomere contraction, and a lumped parameter model of hemodynamics. The ventricle model is quite simple compared to other works (Arts et al. (1991), Bovendeerd et al. (1992)), but this approach was chosen for its low computational cost. The aim of our work is to connect two scales of cardiac
5 contraction and study the correlation of microscopic and macroscopic variables inside a complete CVS model. This implies the computation of many heart beats in a row, which is the reason we choose a simple spherical ventricle model. Our results, on the other hand, correlate well with experimental data. Our multiscale model can account for a healthy behavior as shown in Fig. 4 and 5. More importantly, it is also able to reproduce pathological behaviors that originate at the cellular scale, like heart failure, and the consequences on the whole CVS. It is also able to reproduce basic hemodynamic experiments like preload variations. Our approach in building this multiscale model was similar to Shim et al. (2007) but with four major differences: we carefully choose the volume V wr from Fig. 3 so that the sarcomere length ranges between extremal physiological values. The pressure-force relationship derived in (8) was also different from the one used by Shim et al. (2007). We also used the last version from the mechanical model of Negroni and Lascano (2008). Eventually, we used our model to reproduce heart failure symptoms. ACKNOWLEDGEMENTS Th. Desaive and A. Pironet are cordially acknowledged for comments and advice, especially in the identification of the hemodynamic parameters. Fig. 7. Ventricular failure (dashed) versus normal ventricle. From top to bottom: action potential, intracellular calcium, normalized force, pressure-volume loops. REFERENCES Beuckelmann, D. J., Nabauer, M., and Erdmann, E. (1992). Intracellular calcium handling in isolated ventricular myocytes from patients with terminal heart failure. Circulation, 85, Beuckelmann, D. J., Nabauer, M., and Erdmann, E. (1993). Alterations of K+ currents in isolated human ventricular myocytes from patients with terminal heart failure. Circ. Res., 73, Burkhoff, D., and Tyberg, J. V. (1993). Why does pulmonary venous pressure rise after onset of LV dysfunction: a theoretical analysis. Am J Physiol Heart Circ Physiol, 265, H1819-H1828. Negroni, J. A., and Lascano, E. C. (2008). Simulation of steady state and transient cardiac muscle response experiments with a Huxley-based contraction model. J Mol Cell Cardiol, 45, Negroni, J. A., Morotti, S., Lascano, E. C., Gomes, A. V, Grandi, E., Puglisi, J. L., and Bers, D. M. (2015). β- adrenergic effects on cardiac myofilaments and contraction in an integrated rabbit ventricular myocyte model. J. Mol. Cell. Cardiol. 81, 162?75. J Mol Cell Cardiol, 81, Rodriguez, E. K. et al. (1992). A method to reconstruct myocardial sarcomere lengths and orientations at transmural sites in beating canine hearts. Am J Physiol Heart Circ Physiol, 263, H293-H306. Shim, E. B., Amano, A., Takahata, T., Shimayoshi, T., and Noma, A. (2007). The cross-bridge dynamics during ventricular contraction predicted by coupling the cardiac cell model with a circulation model. J Physiol Sci, 57, Ten Tusscher, K. H. W. J., and Panfilov, A. V. (2006). Alternans and spiral breakup in a human ventricular
6 tissue model. Am J Physiol Heart Circ Physiol, 291, H1088-H1100. Wang, Y., and Hill, J. A. (2010). Electrophysiological remodeling in heart failure. J. Mol. Cell. Cardiol, 48,
GIGA - In Silico Medicine, University of Liege, Belgium, 2
 S. Kosta 1,*, A. Pironet 1, J.A. Negroni 2, E.C. Lascano 2, P.C. Dauby 1 1 GIGA - In Silico Medicine, University of Liege, Belgium, 2 Department of Comparative Cellular and Molecular Biology, Favaloro
S. Kosta 1,*, A. Pironet 1, J.A. Negroni 2, E.C. Lascano 2, P.C. Dauby 1 1 GIGA - In Silico Medicine, University of Liege, Belgium, 2 Department of Comparative Cellular and Molecular Biology, Favaloro
Multiscale model of the human cardiovascular system: description of heart failure and comparison of contractility indices
 Multiscale model of the human cardiovascular system: description of heart failure and comparison of contractility indices S. Kosta, a, J. Negroni, b, E. Lascano, b, and P. C. Dauby a a GIGA - In Silico
Multiscale model of the human cardiovascular system: description of heart failure and comparison of contractility indices S. Kosta, a, J. Negroni, b, E. Lascano, b, and P. C. Dauby a a GIGA - In Silico
BioMedical Engineering OnLine 2013, 12:8
 BioMedical Engineering OnLine This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. A multi-scale
BioMedical Engineering OnLine This Provisional PDF corresponds to the article as it appeared upon acceptance. Fully formatted PDF and full text (HTML) versions will be made available soon. A multi-scale
Eindhoven University of Technology. Exam Modeling Cardiac Function (8W160)
 Eindhoven University of Technology department of Biomedical Engineering group Cardiovascular Biomechanics Exam Modeling Cardiac Function (8W160) January 21, 2011, 14.00 17.00 h This exam consists of 6
Eindhoven University of Technology department of Biomedical Engineering group Cardiovascular Biomechanics Exam Modeling Cardiac Function (8W160) January 21, 2011, 14.00 17.00 h This exam consists of 6
Model-based computation of total stressed blood volume from a preload reduction manoeuvre
 Model-based computation of total stressed blood volume from a preload reduction manoeuvre Antoine Pironet a, 1, Thomas Desaive a, J. Geoffrey Chase b, Philippe Morimont a, Pierre C. Dauby a a University
Model-based computation of total stressed blood volume from a preload reduction manoeuvre Antoine Pironet a, 1, Thomas Desaive a, J. Geoffrey Chase b, Philippe Morimont a, Pierre C. Dauby a a University
The Heart. Happy Friday! #takeoutyournotes #testnotgradedyet
 The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
The Heart Happy Friday! #takeoutyournotes #testnotgradedyet Introduction Cardiovascular system distributes blood Pump (heart) Distribution areas (capillaries) Heart has 4 compartments 2 receive blood (atria)
Chapter 13 The Cardiovascular System: Cardiac Function
 Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Chapter 13 The Cardiovascular System: Cardiac Function Overview of the Cardiovascular System The Path of Blood Flow through the Heart and Vasculature Anatomy of the Heart Electrical Activity of the Heart
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Pressure-calcium relationships in perfused mouse hearts
 Pressure-calcium relationships in perfused mouse hearts Guy A. MacGowan, Jonathan A. Kirk, Caroline Evans and Sanjeev G. Shroff AJP - Heart 290:2614-2624, 2006. First published Jan 13, 2006; doi:10.1152/ajpheart.00979.2005
Pressure-calcium relationships in perfused mouse hearts Guy A. MacGowan, Jonathan A. Kirk, Caroline Evans and Sanjeev G. Shroff AJP - Heart 290:2614-2624, 2006. First published Jan 13, 2006; doi:10.1152/ajpheart.00979.2005
Cardiovascular system
 BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
BIO 301 Human Physiology Cardiovascular system The Cardiovascular System: consists of the heart plus all the blood vessels transports blood to all parts of the body in two 'circulations': pulmonary (lungs)
Heart Pump and Cardiac Cycle. Faisal I. Mohammed, MD, PhD
 Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
BME 5742 Bio-Systems Modeling and Control. Lecture 41 Heart & Blood Circulation Heart Function Basics
 BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
BME 5742 Bio-Systems Modeling and Control Lecture 41 Heart & Blood Circulation Heart Function Basics Dr. Zvi Roth (FAU) 1 Pumps A pump is a device that accepts fluid at a low pressure P 1 and outputs the
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
EXAM II Animal Physiology ZOO 428 Fall 2006
 V Eq EXAM II Animal Physiology ZOO 428 Fall 2006 = RT X o. ln( [ zf [ X ) RT p K[K o pna[na o pcl[cl i V = m ln i F pk[k i pna[na i pcl[cl o I = g(v m V eq. ) Q = C m V m Q Driving Force = V m V eq. 10
V Eq EXAM II Animal Physiology ZOO 428 Fall 2006 = RT X o. ln( [ zf [ X ) RT p K[K o pna[na o pcl[cl i V = m ln i F pk[k i pna[na i pcl[cl o I = g(v m V eq. ) Q = C m V m Q Driving Force = V m V eq. 10
MECHANICAL PROPERTIES OF THE HEART I & II
 MECHANICAL PROPERTIES OF THE HEART I & II Recommended Reading: Guyton, A. Textbook of Medical Physiology, 1 th Edition. Chapters 9, 14, 2. Berne & Levy. Principles of Physiology. 4 th Edition. Chapter
MECHANICAL PROPERTIES OF THE HEART I & II Recommended Reading: Guyton, A. Textbook of Medical Physiology, 1 th Edition. Chapters 9, 14, 2. Berne & Levy. Principles of Physiology. 4 th Edition. Chapter
Modeling of Anatomy, Electrophysiology and Tension Development in the Human Heart
 European Functional Cardiac Modeling Meeting Modeling of Anatomy, Electrophysiology and Tension Development in the Human Heart Dr.-Ing. Gunnar Seemann Overview Electrophysiology Tension development Anatomy
European Functional Cardiac Modeling Meeting Modeling of Anatomy, Electrophysiology and Tension Development in the Human Heart Dr.-Ing. Gunnar Seemann Overview Electrophysiology Tension development Anatomy
Muscle Tissue- 3 Types
 AN INTRODUCTION TO MUSCLE TISSUE Muscle Tissue- 3 Types Skeletal muscle (focus on these) Cardiac muscle Smooth muscle FUNCTIONS OF SKELETAL MUSCLES Produce movement of the skeleton Maintain posture and
AN INTRODUCTION TO MUSCLE TISSUE Muscle Tissue- 3 Types Skeletal muscle (focus on these) Cardiac muscle Smooth muscle FUNCTIONS OF SKELETAL MUSCLES Produce movement of the skeleton Maintain posture and
Cardiovascular System Notes: Physiology of the Heart
 Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiac Physiology an Overview
 Cardiac Physiology an Overview Dr L J Solomon Department of Paediatrics and Child Health School of Medicine Faculty of Health Sciences University of the Free State and PICU Universitas Academic Hospital
Cardiac Physiology an Overview Dr L J Solomon Department of Paediatrics and Child Health School of Medicine Faculty of Health Sciences University of the Free State and PICU Universitas Academic Hospital
THESIS NEW FRANK-STARLING BASED CONTRACTILITY AND VENTRICULAR STIFFNESS INDICES: CLINICALLY APPLICABLE ALTERNATIVE TO EMAX. Submitted by.
 THESIS NEW FRANK-STARLING BASED CONTRACTILITY AND VENTRICULAR STIFFNESS INDICES: CLINICALLY APPLICABLE ALTERNATIVE TO EMAX Submitted by Haiming Tan Graduate Degree Program in Bioengineering In partial
THESIS NEW FRANK-STARLING BASED CONTRACTILITY AND VENTRICULAR STIFFNESS INDICES: CLINICALLY APPLICABLE ALTERNATIVE TO EMAX Submitted by Haiming Tan Graduate Degree Program in Bioengineering In partial
Physiology sheet #2. The heart composed of 3 layers that line its lumen and cover it from out side, these layers are :
 Physiology sheet #2 * We will talk in this lecture about cardiac muscle physiology, the mechanism and the energy sources of their contraction and intracellular calcium homeostasis. # Slide 4 : The heart
Physiology sheet #2 * We will talk in this lecture about cardiac muscle physiology, the mechanism and the energy sources of their contraction and intracellular calcium homeostasis. # Slide 4 : The heart
PROBLEM SET 2. Assigned: February 10, 2004 Due: February 19, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Cardiovascular Physiology
 Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
Cardiovascular Physiology Lecture 1 objectives Explain the basic anatomy of the heart and its arrangement into 4 chambers. Appreciate that blood flows in series through the systemic and pulmonary circulations.
SIKLUS JANTUNG. Rahmatina B. Herman
 SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
SIKLUS JANTUNG Rahmatina B. Herman The Cardiac Cycle Definition: The cardiac events that occur from the beginning of one heartbeat to the beginning of the next The cardiac cycle consists of: - Diastole
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Supplemental methods Pericardium In several studies, it has been shown that the pericardium significantly modulates ventricular interaction. 1-4 Since ventricular interaction has
SUPPLEMENTAL MATERIAL Supplemental methods Pericardium In several studies, it has been shown that the pericardium significantly modulates ventricular interaction. 1-4 Since ventricular interaction has
MUSCLE TISSUE (MUSCLE PHYSIOLOGY) PART I: MUSCLE STRUCTURE
 PART I: MUSCLE STRUCTURE Muscle Tissue A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle Functions of Skeletal Muscles Produce skeletal movement Maintain body position Support
PART I: MUSCLE STRUCTURE Muscle Tissue A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle Functions of Skeletal Muscles Produce skeletal movement Maintain body position Support
Circulatory Systems. All cells need to take in nutrients and expel metabolic wastes.
 Circulatory Systems All cells need to take in nutrients and expel metabolic wastes. Single celled organisms: nutrients from the environment can diffuse (or be actively transported) directly in to the cell
Circulatory Systems All cells need to take in nutrients and expel metabolic wastes. Single celled organisms: nutrients from the environment can diffuse (or be actively transported) directly in to the cell
Health Science 20 Circulatory System Notes
 Health Science 20 Circulatory System Notes Functions of the Circulatory System The circulatory system functions mainly as the body s transport system. It transports: o Oxygen o Nutrients o Cell waste o
Health Science 20 Circulatory System Notes Functions of the Circulatory System The circulatory system functions mainly as the body s transport system. It transports: o Oxygen o Nutrients o Cell waste o
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
All About the Heart. Structures of the heart. Layers. Chambers
 All About the Heart Your heart is a muscle. It is slightly larger than your fist and weighs less than a pound. It is located to the left of the middle of your chest. Your heart pumps blood to the lungs
All About the Heart Your heart is a muscle. It is slightly larger than your fist and weighs less than a pound. It is located to the left of the middle of your chest. Your heart pumps blood to the lungs
Chapter 7 The Muscular System. Mosby items and derived items 2012 by Mosby, Inc., an affiliate of Elsevier Inc. 1
 Chapter 7 The Muscular System Mosby items and derived items 2012 by Mosby, Inc., an affiliate of Elsevier Inc. 1 INTRODUCTION A. Muscular tissue enables the body and its parts to move 1. Three types of
Chapter 7 The Muscular System Mosby items and derived items 2012 by Mosby, Inc., an affiliate of Elsevier Inc. 1 INTRODUCTION A. Muscular tissue enables the body and its parts to move 1. Three types of
Heart Dissection. 5. Locate the tip of the heart or the apex. Only the left ventricle extends all the way to the apex.
 Heart Dissection Page 1 of 6 Background: The heart is a four-chambered, hollow organ composed primarily of cardiac muscle tissue. It is located in the center of the chest in between the lungs. It is the
Heart Dissection Page 1 of 6 Background: The heart is a four-chambered, hollow organ composed primarily of cardiac muscle tissue. It is located in the center of the chest in between the lungs. It is the
Cardiac Cycle. Each heartbeat is called a cardiac cycle. First the two atria contract at the same time.
 The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
The Heartbeat Cardiac Cycle Each heartbeat is called a cardiac cycle. First the two atria contract at the same time. Next the two ventricles contract at the same time. Then all the chambers relax. http://www.youtube.com/watch?v=frd3k6lkhws
Muscle Cells & Muscle Fiber Contractions. Packet #8
 Muscle Cells & Muscle Fiber Contractions Packet #8 Skeletal muscle is attached to bones and is responsible for movement. Introduction Introduction II Skeletal muscle is composed of bundles of muscle fibers
Muscle Cells & Muscle Fiber Contractions Packet #8 Skeletal muscle is attached to bones and is responsible for movement. Introduction Introduction II Skeletal muscle is composed of bundles of muscle fibers
CIRCULATORY PHYSIOLOGY SECTION 3: CARDIAC MECHANICS *
 CIRCULATORY PHYSIOLOGY SECTION 3: CARDIAC MECHANICS * Summary: In this we will look at the mechanical action of the heart as a pump and how it is able to adjust its stroke volume as a result of the Frank-
CIRCULATORY PHYSIOLOGY SECTION 3: CARDIAC MECHANICS * Summary: In this we will look at the mechanical action of the heart as a pump and how it is able to adjust its stroke volume as a result of the Frank-
d) Cardiovascular System Higher Human Biology
 d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
d) Cardiovascular System Higher Human Biology What can your remember about the heart and blood vessels? What is the Cardiovascular System? The cardiovascular system, also known as the circulatory system,
Model-Based Stressed Blood Volume is an Index of Fluid Responsiveness
 Preprints of the 9th IFAC Symposium on Biological and Medical Systems The International Federation of Automatic Control Model-Based Stressed Blood Volume is an Index of Fluid Responsiveness Antoine Pironet
Preprints of the 9th IFAC Symposium on Biological and Medical Systems The International Federation of Automatic Control Model-Based Stressed Blood Volume is an Index of Fluid Responsiveness Antoine Pironet
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition
 TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
TEACH Lesson Plan Manual for Herlihy s The Human Body in Health and Illness 5 th edition Chapter 17 Function of the Heart Lesson 17.1 Function of the Heart 1. Define cardiac cycle with respect to systole
Mathematical Model of the Electromechanical Heart Contractile System Regulatory Subsystem Physiological Considerations
 Physiol. Res. 50: 425-432, 2001 Mathematical Model of the Electromechanical Heart Contractile System Regulatory Subsystem Physiological Considerations M. MLČEK, J. NEUMANN, O. KITTNAR, V. NOVÁK Institute
Physiol. Res. 50: 425-432, 2001 Mathematical Model of the Electromechanical Heart Contractile System Regulatory Subsystem Physiological Considerations M. MLČEK, J. NEUMANN, O. KITTNAR, V. NOVÁK Institute
Chapter 18 - Heart. I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity)
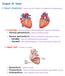 Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Chapter 18 - Heart I. Heart Anatomy: size of your fist; located in mediastinum (medial cavity) A. Coverings: heart enclosed in double walled sac called the pericardium 1. Fibrous pericardium: dense connective
Cardiovascular Physiology
 chapter 3 Cardiovascular Physiology I. CIRCUITRY OF THE CARDIOVASCULAR SYSTEM (FIGURE 3-1) A. Cardiac output of the left heart equals cardiac output of the right heart. Cardiac output from the left side
chapter 3 Cardiovascular Physiology I. CIRCUITRY OF THE CARDIOVASCULAR SYSTEM (FIGURE 3-1) A. Cardiac output of the left heart equals cardiac output of the right heart. Cardiac output from the left side
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
The Arterial and Venous Systems Roland Pittman, Ph.D.
 The Arterial and Venous Systems Roland Pittman, Ph.D. OBJECTIVES: 1. State the primary characteristics of the arterial and venous systems. 2. Describe the elastic properties of arteries in terms of pressure,
The Arterial and Venous Systems Roland Pittman, Ph.D. OBJECTIVES: 1. State the primary characteristics of the arterial and venous systems. 2. Describe the elastic properties of arteries in terms of pressure,
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]
![QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY]](/thumbs/96/126998162.jpg) QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
QUIZ/TEST REVIEW NOTES SECTION 1 CARDIAC MYOCYTE PHYSIOLOGY [CARDIOLOGY] Learning Objectives: Describe the ionic basis of action potentials in cardiac contractile and autorhythmic cells Explain the relationship
CIRCULATORY SYSTEM BLOOD VESSELS
 Name: Block: CIRCULATORY SYSTEM Multicellular organisms (above the level of roundworms) rely on a circulatory system to bring nutrients to, and take wastes away from, cells. In higher organisms such as
Name: Block: CIRCULATORY SYSTEM Multicellular organisms (above the level of roundworms) rely on a circulatory system to bring nutrients to, and take wastes away from, cells. In higher organisms such as
The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits:
 1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
The effect of electrical conductivity of myocardium on cardiac pumping efficacy: a computational study
 DOI 10.1186/s12938-016-0295-6 BioMedical Engineering OnLine RESEARCH Open Access The effect of electrical conductivity of myocardium on cardiac pumping efficacy: a computational study Ana Rahma Yuniarti
DOI 10.1186/s12938-016-0295-6 BioMedical Engineering OnLine RESEARCH Open Access The effect of electrical conductivity of myocardium on cardiac pumping efficacy: a computational study Ana Rahma Yuniarti
QUIZ 1. Tuesday, March 2, 2004
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
How does the heart pump? From sarcomere to ejection volume
 How does the heart pump? From sarcomere to ejection volume Piet Claus Cardiovascular Imaging and Dynamics Department of Cardiovascular Diseases University Leuven, Leuven, Belgium Course on deformation
How does the heart pump? From sarcomere to ejection volume Piet Claus Cardiovascular Imaging and Dynamics Department of Cardiovascular Diseases University Leuven, Leuven, Belgium Course on deformation
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CLINICAL CARDIOVASCULAR IDENTIFICATION WITH LIMITED DATA AND FAST FORWARD SIMULATION
 CLINICAL CARDIOVASCULAR IDENTIFICATION WITH LIMITED DATA AND FAST FORWARD SIMULATION Christopher E. Hann, J. Geoffrey Chase, Geoffrey M. Shaw, Steen Andreassen, Bram W. Smith Centre for Bioengineering,
CLINICAL CARDIOVASCULAR IDENTIFICATION WITH LIMITED DATA AND FAST FORWARD SIMULATION Christopher E. Hann, J. Geoffrey Chase, Geoffrey M. Shaw, Steen Andreassen, Bram W. Smith Centre for Bioengineering,
Mechanics of Cardiac Tissue
 Bioengineering 6000: System Physiology I Mechanics of Cardiac Tissue PD Dr.-Ing. Frank B. Sachse Overview Recapitulation Excitation Propagation II Force Development Experimental Studies Anatomy Cross Bridge
Bioengineering 6000: System Physiology I Mechanics of Cardiac Tissue PD Dr.-Ing. Frank B. Sachse Overview Recapitulation Excitation Propagation II Force Development Experimental Studies Anatomy Cross Bridge
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Muscle Dr. Ted Milner (KIN 416)
 Muscle Dr. Ted Milner (KIN 416) Muscles are biological motors which actively generate force and produce movement through the process of contraction. The molecular mechanism responsible for muscle contraction
Muscle Dr. Ted Milner (KIN 416) Muscles are biological motors which actively generate force and produce movement through the process of contraction. The molecular mechanism responsible for muscle contraction
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006
 SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
SymBioSys Exercise 2 Cardiac Function Revised and reformatted by C. S. Tritt, Ph.D. Last updated March 20, 2006 The goal of this exercise to explore the behavior of the heart as a mechanical pump. For
MECHANICAL PROPERTIES OF THE HEART
 MECHANICAL PROPERTIES OF THE HEART I. INTRODUCTION The heart is a muscular pump connected to the systemic and pulmonary vascular systems. Working together, the principle job of the heart and vasculature
MECHANICAL PROPERTIES OF THE HEART I. INTRODUCTION The heart is a muscular pump connected to the systemic and pulmonary vascular systems. Working together, the principle job of the heart and vasculature
Patient-specific modeling of heart and circulation
 Patient-specific modeling of heart and circulation Theo Arts t.arts@bf.unimaas.nl Maastricht University, *Maastricht University Hospital **University of Tecnology, Eindhoven The Netherlands *Tammo Delhaas,
Patient-specific modeling of heart and circulation Theo Arts t.arts@bf.unimaas.nl Maastricht University, *Maastricht University Hospital **University of Tecnology, Eindhoven The Netherlands *Tammo Delhaas,
Flow in the Iliac Artery
 Flow in the Iliac Artery Flow in an iliac artery Modeling the electromechanical activity of the heart (with R. Ruiz-Baier, D.Ambrosi, F.Nobile, L.Pavarino and S.Rossi) Al Cuore del problema..! Left ventricle
Flow in the Iliac Artery Flow in an iliac artery Modeling the electromechanical activity of the heart (with R. Ruiz-Baier, D.Ambrosi, F.Nobile, L.Pavarino and S.Rossi) Al Cuore del problema..! Left ventricle
Estimating afterload, systemic vascular resistance and pulmonary vascular resistance in an intensive care setting
 Estimating afterload, systemic vascular resistance and pulmonary vascular resistance in an intensive care setting David J. Stevenson James Revie Geoffrey J. Chase Geoffrey M. Shaw Bernard Lambermont Alexandre
Estimating afterload, systemic vascular resistance and pulmonary vascular resistance in an intensive care setting David J. Stevenson James Revie Geoffrey J. Chase Geoffrey M. Shaw Bernard Lambermont Alexandre
Bio 449 Fall Exam points total
 Name: Exam 2 100 points total Multiple choice. As with any test, choose the best answer in each case. Each question is 3 points. Comments are provided in italic for questions that too many people missed!
Name: Exam 2 100 points total Multiple choice. As with any test, choose the best answer in each case. Each question is 3 points. Comments are provided in italic for questions that too many people missed!
The Heart. Made up of 3 different tissue: cardiac muscle tissue, nerve tissue, and connective tissue.
 The Heart The Heart Made up of 3 different tissue: cardiac muscle tissue, nerve tissue, and connective tissue. Your heart pumps with a regular beat (Heart Rate) Your heart rate can change depending on
The Heart The Heart Made up of 3 different tissue: cardiac muscle tissue, nerve tissue, and connective tissue. Your heart pumps with a regular beat (Heart Rate) Your heart rate can change depending on
Muscles and Animal Movement
 Muscles and Animal Movement Evolution of Muscle and Movement Animals are the only multicellular organisms that actively move. Movement is due to muscle cells (motor proteins) Muscle proteins have homologues
Muscles and Animal Movement Evolution of Muscle and Movement Animals are the only multicellular organisms that actively move. Movement is due to muscle cells (motor proteins) Muscle proteins have homologues
The relation between stroke work and end-diastolic volume in the ventricles
 Modelling in Medicine and Biology VI 123 The relation between stroke work and end-diastolic volume in the ventricles R. M. Shoucri Department of Mathematics and Computer Science, Royal Military College
Modelling in Medicine and Biology VI 123 The relation between stroke work and end-diastolic volume in the ventricles R. M. Shoucri Department of Mathematics and Computer Science, Royal Military College
Lab Activity 23. Cardiac Anatomy. Portland Community College BI 232
 Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
Lab Activity 23 Cardiac Anatomy Portland Community College BI 232 Cardiac Muscle Histology Branching cells Intercalated disc: contains many gap junctions connecting the adjacent cell cytoplasm, creates
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies
 Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Pearson's Comprehensive Medical Assisting Administrative and Clinical Competencies THIRD EDITION CHAPTER 27 The Cardiovascular System Lesson 1: Overview of the Cardiovascular System Lesson Objectives Upon
Description of Cardiac Hemodynamics Using a Physical Model: Pressure-Volume Diagrams and the Effect of AV Delay
 42 March 2002 Description of Cardiac Hemodynamics Using a Physical Model: Pressure-Volume Diagrams and the Effect of AV Delay M. SCHIER, B. HENSEL Department of Biomedical Engineering, Friedrich-Alexander
42 March 2002 Description of Cardiac Hemodynamics Using a Physical Model: Pressure-Volume Diagrams and the Effect of AV Delay M. SCHIER, B. HENSEL Department of Biomedical Engineering, Friedrich-Alexander
From PV loop to Starling curve. S Magder Division of Critical Care, McGill University Health Centre
 From PV loop to Starling curve S Magder Division of Critical Care, McGill University Health Centre Otto Frank 1890 s Frank-Starling Relationship ( The Law of the Heart ) The greater the initial stretch
From PV loop to Starling curve S Magder Division of Critical Care, McGill University Health Centre Otto Frank 1890 s Frank-Starling Relationship ( The Law of the Heart ) The greater the initial stretch
AnS SI 214 Practice Exam 2 Nervous, Muscle, Cardiovascular
 AnS SI 214 Practice Exam 2 Nervous, Muscle, Cardiovascular Select the best answer choice in the questions below. 1) On the electrocardiogram, repolarization of the atria is represented by the: A) P wave
AnS SI 214 Practice Exam 2 Nervous, Muscle, Cardiovascular Select the best answer choice in the questions below. 1) On the electrocardiogram, repolarization of the atria is represented by the: A) P wave
Question No: 2 What is released from the sarcoplasmic reticulum into the myofibril, causing tension development in a muscle?
 Volume: 600 Questions Question No: 1 Each muscle fiber is surrounded by a connective tissue called? A. Fasiciculi B. Perimysium C. Endomysium D. Epimysium Question No: 2 What is released from the sarcoplasmic
Volume: 600 Questions Question No: 1 Each muscle fiber is surrounded by a connective tissue called? A. Fasiciculi B. Perimysium C. Endomysium D. Epimysium Question No: 2 What is released from the sarcoplasmic
Cardiac Conduction System
 Cardiac Conduction System What causes the Heart to Beat? Heart contracts by electrical signals! Cardiac muscle tissue contracts on its own an electrical signal is sent out by the heart so that all cells
Cardiac Conduction System What causes the Heart to Beat? Heart contracts by electrical signals! Cardiac muscle tissue contracts on its own an electrical signal is sent out by the heart so that all cells
Aulia Khamas Heikhmakhtiar and Ki Moo Lim. 1. Introduction
 Computational and Mathematical Methods in Medicine Volume 216, Article ID 693482, 8 pages http://dx.doi.org/1.1155/216/693482 Research Article Computational Analysis of Pumping Efficacy of a Left Ventricular
Computational and Mathematical Methods in Medicine Volume 216, Article ID 693482, 8 pages http://dx.doi.org/1.1155/216/693482 Research Article Computational Analysis of Pumping Efficacy of a Left Ventricular
The All-or-None Principle Motor units also comply to a rule known as the all-ornone principle (or law).
 The All-or-None Principle Motor units also comply to a rule known as the all-ornone principle (or law). This principle stipulates that, when a motor unit is stimulated to contract, it will do so to its
The All-or-None Principle Motor units also comply to a rule known as the all-ornone principle (or law). This principle stipulates that, when a motor unit is stimulated to contract, it will do so to its
Outline. Electrical Activity of the Human Heart. What is the Heart? The Heart as a Pump. Anatomy of the Heart. The Hard Work
 Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Electrical Activity of the Human Heart Oguz Poroy, PhD Assistant Professor Department of Biomedical Engineering The University of Iowa Outline Basic Facts about the Heart Heart Chambers and Heart s The
Circulatory System 10.1
 1 Circulatory System 10.1 2 ARTERIES Arteries-blood vessels that carry blood away from the heart Thick walls Inner & Outer layers: connective tissue Middle layers are muscle and elastic connective tissue
1 Circulatory System 10.1 2 ARTERIES Arteries-blood vessels that carry blood away from the heart Thick walls Inner & Outer layers: connective tissue Middle layers are muscle and elastic connective tissue
Biology Unit 3 The Human Heart P
 Biology 2201 Unit 3 The Human Heart P 314-321 Structure and Function of the Human Heart Structure of the Human Heart Has four Chambers (2 Atria and 2 Ventricles) Made of Cardiac Muscle Found in Chest Cavity
Biology 2201 Unit 3 The Human Heart P 314-321 Structure and Function of the Human Heart Structure of the Human Heart Has four Chambers (2 Atria and 2 Ventricles) Made of Cardiac Muscle Found in Chest Cavity
MASSACHUSETTS INSTITUTE OF TECHNOLOGY
 Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Harvard-MIT Division of Health Sciences and Technology HST.542J: Quantitative Physiology: Organ Transport Systems Instructors: Roger Mark and Jose Venegas MASSACHUSETTS INSTITUTE OF TECHNOLOGY Departments
Blood must move! 4/15/2014. Heart Basics
 What is the CARDIOVASCULAR system? The cardiovascular system carries blood and dissolved substances to and from different places in the body. The Heart has the job of pumping these things around the body.
What is the CARDIOVASCULAR system? The cardiovascular system carries blood and dissolved substances to and from different places in the body. The Heart has the job of pumping these things around the body.
By: Stephanie Bendtsen, Joseph Calderan, and Celeste Dupont Team 17 Client: Dr. Sun
 By: Stephanie Bendtsen, Joseph Calderan, and Celeste Dupont Team 17 Client: Dr. Sun Flow Loop Design Introduction Purpose: to build a pulsatile flow loop that allows for implementation and testing of mechanical
By: Stephanie Bendtsen, Joseph Calderan, and Celeste Dupont Team 17 Client: Dr. Sun Flow Loop Design Introduction Purpose: to build a pulsatile flow loop that allows for implementation and testing of mechanical
Age-related changes in cardiovascular system. Dr. Rehab Gwada
 Age-related changes in cardiovascular system Dr. Rehab Gwada Objectives explain the main structural and functional changes in cardiovascular system associated with normal aging Introduction aging results
Age-related changes in cardiovascular system Dr. Rehab Gwada Objectives explain the main structural and functional changes in cardiovascular system associated with normal aging Introduction aging results
The Circulatory System. The Heart, Blood Vessels, Blood Types
 The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
The Circulatory System The Heart, Blood Vessels, Blood Types The Closed Circulatory System Humans have a closed circulatory system, typical of all vertebrates, in which blood is confined to vessels and
Cardiac Properties MCQ
 Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Cardiac Properties MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Cardiac Valves: a- Prevent backflow of blood from the ventricles to the atria during
Skeletal muscle in the light of its structure
 Mechanism of contraction of Skeletal muscle in the light of its structure By Dr. Mudassar Ali Roomi (MBBS, M. Phil) Muscle Tissue Skeletal Muscle Cardiac Muscle Smooth Muscle Skeletal Muscle Long cylindrical
Mechanism of contraction of Skeletal muscle in the light of its structure By Dr. Mudassar Ali Roomi (MBBS, M. Phil) Muscle Tissue Skeletal Muscle Cardiac Muscle Smooth Muscle Skeletal Muscle Long cylindrical
CHAPTER 6 2/9/2016. Learning Objectives List the four traits that all muscle types have in common.
 Learning Objectives List the four traits that all muscle types have in common. CHAPTER 6 The Muscular System Demonstrate and explain the use of antagonistic muscle pairs. Describe the attachment of muscle
Learning Objectives List the four traits that all muscle types have in common. CHAPTER 6 The Muscular System Demonstrate and explain the use of antagonistic muscle pairs. Describe the attachment of muscle
Estimating afterload, systemic vascular resistance and pulmonary vascular resistance in an intensive care setting
 Estimating afterload, systemic vascular resistance and pulmonary vascular resistance in an intensive care setting David J. Stevenson James Revie Geoffrey J. Chase Geoffrey M. Shaw Bernard Lambermont Alexandre
Estimating afterload, systemic vascular resistance and pulmonary vascular resistance in an intensive care setting David J. Stevenson James Revie Geoffrey J. Chase Geoffrey M. Shaw Bernard Lambermont Alexandre
Computational Modeling of Cardiac Resynchronization Therapy. Britta Baynes UC San Diego- Cardiac Mechanics Research Group
 Computational Modeling of Cardiac Resynchronization Therapy Britta Baynes UC San Diego- Cardiac Mechanics Research Group Background Cardiac Resynchronization Therapy (CRT) is a widely used and proven treatment
Computational Modeling of Cardiac Resynchronization Therapy Britta Baynes UC San Diego- Cardiac Mechanics Research Group Background Cardiac Resynchronization Therapy (CRT) is a widely used and proven treatment
Lecture 13: The Cardiovascular System ref: Cardiovascular Physiology, D. Mohrman and L. Heller, 4th ed. McGraw-Hill (1997)
 Lecture 13: The Cardiovascular System ref: Cardiovascular Physiology, D. Mohrman and L. Heller, 4th ed. McGraw-Hill (1997) Blood Heart Blood Vessels Arteries - capillaries - Veins Ventilation-Perfusion
Lecture 13: The Cardiovascular System ref: Cardiovascular Physiology, D. Mohrman and L. Heller, 4th ed. McGraw-Hill (1997) Blood Heart Blood Vessels Arteries - capillaries - Veins Ventilation-Perfusion
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Chp. 5 The cardiovascular system. What are the function of the cardiovascular system? Arteries and arterioles:
 5.1 Overview of the cardiovascular system Chp. 5 The cardiovascular system Includes the heart and blood vessels Brings nutrients to cells and helps get rid of wastes Blood is refreshed in the lung, kidneys,
5.1 Overview of the cardiovascular system Chp. 5 The cardiovascular system Includes the heart and blood vessels Brings nutrients to cells and helps get rid of wastes Blood is refreshed in the lung, kidneys,
The Cardiac Cycle Clive M. Baumgarten, Ph.D.
 The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital
 LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
LV geometric and functional changes in VHD: How to assess? Mi-Seung Shin M.D., Ph.D. Gachon University Gil Hospital LV inflow across MV LV LV outflow across AV LV LV geometric changes Pressure overload
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary.
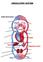 CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
CIRCULATORY SYSTEM 1. Which of the following blood vessels has a thin elastic layer? A. Aorta. B. Pulmonary artery. C. Posterior vena cava. D. Mesenteric capillary. 2. Capillary beds are equipped with
Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS
 Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS Program Director, Cardiovascular Technology Florida SouthWestern State College Fort Myers, FL Disclosures Speaker s Bureau: None Stockholder: None
Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS Program Director, Cardiovascular Technology Florida SouthWestern State College Fort Myers, FL Disclosures Speaker s Bureau: None Stockholder: None
Major Function of the Cardiovascular System. Transportation. Structures of the Cardiovascular System. Heart - muscular pump
 Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
Structures of the Cardiovascular System Heart - muscular pump Blood vessels - network of tubes Blood - liquid transport vehicle brachiocephalic trunk superior vena cava right pulmonary arteries right pulmonary
