The endovascular management of visceral artery aneurysms and pseudoaneurysms
|
|
|
- Joan Carson
- 6 years ago
- Views:
Transcription
1 The endovascular management of visceral artery aneurysms and pseudoaneurysms Nirman Tulsyan, MD, a Vikram S. Kashyap, MD, a Roy K. Greenberg, MD, a Timur P. Sarac, MD, a Daniel G. Clair, MD, a Gregory Pierce, MD, b and Kenneth Ouriel, MD, a Cleveland, Ohio Objective: Visceral artery aneurysms may be treated by aneurysm exclusion, excision, revascularization, and endovascular techniques. The purpose of this study was to review the outcomes of the management of visceral artery aneurysms with catheter-based techniques. Methods: Between 1997 and 2005, 90 patients were identified with a diagnosis of visceral artery aneurysm. This was inclusive of aneurysmal disease of the celiac axis, superior mesenteric artery (SMA), inferior mesenteric artery, and their branches. Surveillance without intervention occurred in 23 patients, and 19 patients underwent open aneurysm repair (4 ruptures). The endovascular treatment of 48 consecutive patients (mean age 58, 60% men) with 20 visceral artery aneurysms (VAA) and 28 visceral artery pseudoaneurysms (VAPA) was the basis for this study. Electronic and hardcopy medical records were reviewed for demographic data and clinical variables. Original computed tomography (CT) scans and fluoroscopic imaging were evaluated. Results: The endovascular treatment of visceral artery aneurysms was technically successful in 98% of 48 procedures, consisting of 3 celiac axis repairs, 2 left gastric arteries, 1 SMA, 12 hepatic arteries, 20 splenic arteries, 7 gastroduodenal arteries, 1 middle colic artery, and 2 pancreaticoduodenal arteries. Of these, 29 (60%) were performed for symptomatic disease (5 ruptured aneurysms). Procedures were performed in the endovascular suite under local anesthesia with conscious sedation (94%). The femoral artery was used as the preferential access site (90%). Coil embolization was used for aneurysm exclusion in 96%. N-butyl-2-cyanoacrylate (glue) was used selectively (19%) using a triaxial system with a 3F microcatheter for persistent flow or multiple branches. The 30-day mortality was 8.3% (n 4). One patient died from recurrent gastrointestinal bleeding after gastroduodenal embolization, and the remaining died of unrelated causes. All perioperative deaths occurred in patients requiring urgent or emergent intervention in the setting of hemodynamic instability. No patients undergoing elective intervention died in the periprocedural period. Postprocedural imaging was performed after 77% of interventions at a mean of 16 months. Complete exclusion of flow within the aneurysm sac occurred in 97% interventions with follow-up imaging, but coil and glue artifact complicated CT evaluation. Postembolization syndrome developed in three patients (6%) after splenic artery embolization. There was no evidence of hepatic insufficiency or bowel ischemia after either hepatic or mesenteric artery aneurysm treatment. Three patients required secondary interventions for persistent flow (n 1) and recurrent bleeding from previously embolized aneurysms (n 2). Conclusion: Visceral artery aneurysms and pseudoaneurysms can be successfully treated with endovascular means with low periprocedural morbidity; however, the urgent repair of these lesions is still associated with elevated mortality rates. Aneurysm exclusion can be accomplished with coil embolization and the selective use of N-butyl-2-cyanoacrylate. Current catheter-based techniques extend our ability to exclude visceral artery aneurysms, but imaging artifact hampers postoperative CT surveillance. (J Vasc Surg 2007;45: ) Aneurysmal degeneration of the visceral branches of the abdominal aorta is a rare and potential life-threatening disease entity 1,2 with a documented prevalence of 0.1% to 2%. 3,4 The augmented use of ultrasonography and crosssectional body imaging for intra-abdominal pathology, coupled with increased instrumentation of the biliary tract, has raised the prevalence and incidental identification of visceral artery aneurysms (VAA) and pseudoaneurysms (VAPA). From the Departments of Vascular Surgery a and Interventional Radiology, b The Cleveland Clinic Foundation. Competition of interest: none. Presented at the 2006 Vascular Annual Meeting, Philadelphia, Pa, Jun 1 to 3, Reprint requests: Vikram S. Kashyap, MD, The Cleveland Clinic Foundation, Department of Vascular Surgery, S40, 9500 Euclid Ave, Cleveland, OH ( kashyav@ccf.org) /$32.00 Copyright 2007 by The Society for Vascular Surgery. doi: /j.jvs Although small VAA generally remain asymptomatic, they follow an insidious course and the risk for aneurysm 5 rupture and death remains real. Shanley et reviewed al cases of VAA from 1985 to 1995 in the English literature, reporting a mortality rate of 21% for ruptured hepatic artery aneurysms and 100% for ruptured celiac artery aneurysms. VAA have been historically managed with either close surveillance or open surgical intervention. Current open surgical therapeutic options for VAA and VAPA include aneurysm resection with revascularization, aneurysm ligation, or end-organ resection (ie, splenectomy). Endovascular approaches to managing VAA and VAPA (Figs 1, 2, and 3) offer an alternative to conventional open surgery with the benefit of low procedural morbidity and mortality. Endoluminal ablation of VAA and VAPA have been shown to be highly technically successful, 6 but concern of aneurysm 7 reperfusion during follow-up persists. Furthermore, because ablative endoluminal therapy of VAA and VAPA often requires highly radiodense materials, such as glue and
2 JOURNAL OF VASCULAR SURGERY Volume 45, Number 2 Tulsyan et al 277 coils, postoperative surveillance for aneurysm reperfusion and parent vessel patency may be suboptimal. The purpose of this study was to describe our singlecenter experience with the endovascular ablative management of VAA and VAPA. Specific focus was given to procedural techniques, rates of technical success, perioperative morbidity and mortality, durability of repair, and adequacy of postoperative imaging modalities. Fig 1. A, Preoperative computed tomography (CT) image demonstrates a 3.0 cm distal splenic artery aneurysm in a young woman. The splenic artery aneurysm was incidentally discovered during an evaluation for an unrelated cause of abdominal pain. B, Aortography with selective celiac axis imaging confirmed the presence of a splenic artery aneurysm. A shaped 6F sheath was placed into the ostium of the celiac axis.a 5 F hydrophilic catheter was then used with a hydrophilic inch wire to selectively gain access into the splenic artery. A 3F microcatheter was advanced thru the 5F catheter over a inch wire. N-butyl-2-cyanoacrylate (N-BCA), diluted 1:3 with ethiodized oil, was used to occlude the outflow vessel. Coils were deployed in the aneurysm sac and in the inflow vessel to completely exclude the aneurysm. Angiography after deployment of coils and N-BCA confirms successful exclusion of the aneurysm sac and absence of flow within outflow vessels. C, Postoperative CT demonstrates coil and glue artifact with no gross evidence of aneurysm sac flow. PATIENTS AND METHODS A retrospective review was performed of patients who underwent endovascular treatment of VAA or VAPA at The Cleveland Clinic Foundation from January 1, 1997, to July 31, During the study interval, 90 patients were identified with VAA. Endoluminal ablation of a VAA or VAPA was performed in 48 patients (51 procedures), representing 53.5% of all patients diagnosed with aneurysms of the visceral vessels. Three patients required an additional endoluminal procedure. Demographic and clinical data were obtained through review of physician and hospital records. Preoperative and postoperative imaging consisted of computed tomography (CT), magnetic resonance imaging (MRI) and angiography (MRA), duplex scanning, or a combination of these. Preoperative imaging was reviewed from captured and stored electronic images (MagicView program, Siemens, Erlangen, Germany) to confirm the diagnosis of VAA/VAPA. Patients with symptomatic or asymptomatic aneurysms of the celiac axis, superior mesenteric artery (SMA), and inferior mesenteric artery, and their respective branches, were included in the analysis. Patients with VAA in the setting of aortic dissection or concomitant aortic aneurysm were excluded. Pseudoaneurysms were distinguished from true aneurysms by clinical and imaging criteria. Clinically, patients with VAPA typically presented with an antecedent history of arterial trauma, intra-abdominal or retroperitoneal inflammation or malignancy, or biliary tract manipulation. Imaging of VAPA demonstrated evidence of focal arterial disruption in the setting of an otherwise normal artery. Evidence of surrounding inflammation in the setting of an irregular aneurysmal wall was also present. Patients who underwent diagnostic angiography without the intention of endovascular treatment were excluded. Preoperative demographic data included age, sex, and cardiovascular risk factors (Table I). Specifically, risk factors assessed included hypertension, hyperlipidemia, coronary artery disease, renal insufficiency, diabetes mellitus, and history of tobacco use. Patients were also assessed for whether their VAA/VAPA was symptomatic, ruptured, or hemodynamically stable at presentation. Operative technique. Percutaneous interventions were performed by the faculty of The Cleveland Clinic Department of Vascular Surgery and Department of Interventional Radiology in dedicated endovascular suites with fixed imaging. The most common technique (81.3%) for endoluminal VAA/VAPA therapy was ablation with coils. In all cases, ablative therapy of the outflow tract, the
3 278 Tulsyan et al JOURNAL OF VASCULAR SURGERY February 2007 Fig 2. An elderly man presented with signs of hypovolemic shock and abdominal pain. After initial stabilization, a computed tomography (CT) scan demonstrated the presence of a large mesenteric hematoma with a contrast blush arising from a mesenteric branch. A, Selective visceral angiography identified a fusiform aneurysm of the left branch of the middle colic artery. B, A 6F sheath was placed into the ostium of the superior mesenteric artery. A 5F hydrophilic catheter was advanced to the origin of the middle colic artery. A 3F microcatheter with inch wire was used to selectively cannulate the middle colic artery and its left branch. The microcatheter was advanced through the aneurysm into its outflow vessel. N-butyl-2-cyanoacrylate (N-BCA) and inch coils were deployed within the aneurysm sac and N-BCA was instilled within the inflow vessel. C, Postoperative imaging demonstrated a patent superior mesenteric artery and middle colic artery. The left branch was not visualized because it was completely ablated. Coils and glue are evident, however. VAA/VAPA itself, and the inflow artery was attempted. N-butylcyanoacrylate (N-BCA) glue (Cordis Neurovascular, Miami, Fla) or a combination of coils and N-BCA was used for ablation in 4.2% and 15% of cases, respectively. The United States Food and Drug Administration has approved N-BCA for the preoperative ablation of intracranial arteriovenous malformations, and we have found a benefit in extending its use to the treatment of VAA and endoleaks after endoluminal stent grafting. Depending on the desired rate of polymerization, N-BCA is diluted with ethiodized oil, a polymerization-retardant. Specifically, when embolizing a vessel with high rates of blood flow, we desired quick in vivo polymerization and a ratio of 1:1 oil to N-BCA was used. In situations where the microcatheter tip was positioned distant from the desired site of polymerization, a greater volume of ethiodized oil (ie, 2:1, 3:1 dilutions) was added to delay glue polymerization. Although the decision to use coils or N-BCA, or both, was physician-dependent, the glue was routinely used when access into the aneurysm s outflow vessel was unattainable. Conscious sedation with local anesthetic was used in 45 of 48 interventions. Three patients required general anesthesia in the setting of hemodynamic instability secondary to blood loss from symptomatic disease. Endovascular access for all procedures was through the femoral artery (89.6%) or brachial artery (10.4%). A 5F (56.3%) or 6F sheath (29.2%) was used in most cases, and a 7F sheath was used in the rest. A shaped guiding catheter was used selectively in the ostia of the visceral vessel in instances in which a sheath could not successfully be engaged. Intravascular ultrasound was required in one patient to assist in identification of a celiac axis pseudoaneurysm that was not clearly demonstrated on selective angiography. A triaxial endovascular system with a 3F microcatheter was used in 64.6% of interventions and was specifically required for the deployment of N-BCA or inch intravascular coils. We have also found a microcatheter system useful for interventions upon the distal aspect of an arterial bed and for the selective embolization of an aneurysm/pseudoaneurysm cavity with preservation of the proximal parent artery. An uncovered self-expanding nitinol stent was selectively placed to preserve flow within a visceral vessel and to exclude coils placed within aneurysmal artery from encroaching and compromising a nondiseased parent artery (n 2) and to treat hemodynamically significant dissection resulting from visceral vessel cannulation (n 1). Percutaneous mechanical thrombectomy of the celiac axis and femoral artery was required during two separate procedures to recanalize an acute procedure-related occlusion during hepatic artery embolization. Owing to the rich collateral network between the celiac axis and SMA, postembolization imaging through both arterial trees was routinely performed to confirm exclusion of the aneurysmal segment. All patients with elective repair underwent systemic anticoagulation with heparin to achieve an activated clotting time of 250 seconds. Patients with rupture received small doses (2 to 3000 units) of heparin after selective visceral cannulation. Three patients with hemodynamic instability received no anticoagulation. Technical success was defined as the successful deployment of coils or glue (or both) within the intended artery, exclusion of the aneurysmal arterial segment without evidence of contrast extravasation, and cessation of hemorrhage, if originally present. In instances of aneurysmal disease of second-order or third-order branches, technical
4 JOURNAL OF VASCULAR SURGERY Volume 45, Number 2 Tulsyan et al 279 Table I. Demographic and clinical factors for 48 patients undergoing endovascular management of visceral artery aneurysms and pseudoaneurysms Variable* No. patients (%) Male sex 29 (60) Hypertension 21 (44) Hyperlipidemia 10 (21) Coronary artery disease 12 (25) Diabetes mellitus 6 (13) Tobacco use 5 (10) Renal dysfunction 3 (6) *Mean patient age, 58.1 years. Includes only current smokers. Serum creatinine 1.5 mg/dl or dialysis-dependent. successful aneurysm ablation included resolution of gastrointestinal bleeding/hemobilia in such symptomatic cases and absence of flow on follow-up CT or MRI/MRA. Postoperative imaging was assessed for sac flow, aneurysm size change, adequacy of end-organ perfusion, and severity of coil or N-BCA artifact. Postprocedural imaging artifact was graded by severity: grade 1, minor with no radiopaque scatter; grade 2, moderate with mild radiopaque scatter beyond the region treated; and grade 3, severe with significant radiopaque scatter. The interval of follow-up at The Cleveland Clinic Foundation was recorded and averaged 15.6 months (range, 1 to 75 months). Fig 3. A middle-aged man, who had previously undergone aortohepatic bypass grafting for an occluded celiac axis, presented with an incidentally discovered large pancreaticoduodenal aneurysm. A, His computed tomography (CT) scan demonstrated a large aneurysm arising from a branch of the superior mesenteric artery (SMA). B, CT shows the aneurysm collaterilizing with the superior pancreaticoduodenal arcade of the gastroduodenal artery (GDA). He underwent selective angiography of the aortohepatic bypass and SMA, demonstrating filling of the aneurysm via both mesenteric vessels. A 6F sheath was first placed into the ostium of the aortohepatic bypass, with subsequent passage of a hydrophilic 5F catheter into the distal aspect of the bypass. Selective cannulation of the GDA was then performed with a microcatheter and inch wire. Glue ablation of the aneurysm sac, as well as its inflow via the GDA and inferior pancreaticoduodenal vessels, was achieved. C, Postoperative imaging confirmed successful ablation of the aneurysm with a patent SMA. success was further defined as exclusion of the aneurysm with preservation of flow within the intended parent artery. In three cases, VAA or VAPA with very sluggish flow in the fully anticoagulated state were considered successfully excluded. Data analysis and statistical methods. Periprocedural data, associated morbidity, and mortality 30 days of the procedure were determined. Follow-up documentation of RESULTS During the study period, 48 patients (mean age, 58 years) underwent endovascular management of VAA or VAPA. The anatomic distribution of aneurysms treated included 12 hepatic artery aneurysms (20%), 3 celiac axis aneurysms (6.3%), 2 left gastric aneurysms (4.2%), 2 SMA branch aneurysms (4.2%), 20 splenic artery aneurysms (41.7%), and 9 gastroduodenal/pancreaticoduodenal artery aneurysms (18.8%). Overall, 28 (58%) of the interventions were for pseudoaneurysmal pathology. In 65% of patients, treatment was required for symptomatic disease, including rupture, pain, gastrointestinal bleeding, and/or hemobilia. The symptoms at presentation and the distribution of lesions amongst the various arterial beds (Fig 4) were significantly different between VAA and VAPA. Of the 48 patients, 22 (46%) underwent urgent or emergent procedures. Treatment was for VAA in 42% of patients, and splenic artery aneurysms comprised 75% of true aneurysms in our study. The mean size of all VAA was 2.4 cm. At presentation, 30% of patients with VAA were symptomatic, and one third of these warranted urgent intervention. Only one case of hemodynamic instability secondary to a VAA was noted, however. Asymptomatic VAA (30%) were incidentally identified and treated on the basis of dimensional criteria. Two true aneurysms presented with rupture: one was a 2.5-cm hepatic artery aneurysm, and the other was a middle colic artery aneurysm of unknown size.
5 280 Tulsyan et al JOURNAL OF VASCULAR SURGERY February 2007 Unlike true VAA, 89% of the pseudoaneurysms were symptomatic at presentation. Most of the visceral false aneurysms presented with gastrointestinal bleeding or hemobilia, such that 92% of these patients required urgent intervention. The mean size for all false aneurysms treated was 3.0 cm. Three pseudoaneurysms (1 SMA, 1 celiac, 1 splenic) presented with rupture. Technical success was achieved in 47 (98%) of 48 of procedures. One technical failure occurred during treatment of a celiac artery aneurysm distal to an ostial occlusion. Retrograde perfusion of a 2.8-cm aneurysm through the gastroduodenal arcade and splenic artery warranted intervention. Upon completion of the procedure, persistent flow through the aneurysm was identified. Follow-up imaging 3 weeks later demonstrated a slight decrease in aneurysm size. A secondary intervention was attempted to ablate the aneurysm sac, but was unsuccessful and aborted due to diminishing sac size. Interventions on the hepatic arterial tree, gastroduodenal/ pancreaticoduodenal arteries, and left gastric artery were performed primarily for pseudoaneurysms related to percutaneous biliary catheters, intravascular chemoembolization catheters, local infectious and inflammatory processes, or iatrogenic operative injury. The 30-day operative mortality was 8.3%. Two unstable patients with extensive hepatobiliary surgery died after embolization: one died from recurrent bleeding in the setting of unresectable carcinoma. A third patient, treated for a ruptured hepatic artery aneurysm, died after a subarachnoid hemorrhage caused from a ruptured anterior cerebral artery aneurysm. A fourth patient died from complications from an underlying intra-abdominal malignancy after a technically successful endovascular treatment of an acutely ruptured 2-cm jejunal artery pseudoaneurysm. The four patients who died in the perioperative period were among the 22 patients who required urgent or emergent intervention because of hemodynamic instability attributable to a symptomatic VAA or VAPA (18% mortality rate). There were no deaths amongst patients electively treated for VAA/VAPA (Table II). Access-related complications developed in two patients. One sustained a documented groin hematoma not requiring transfusion. In the other patient, access-related femoral artery thrombosis occurred and was treated with percutaneous mechanical thrombectomy. This patient also developed a retroperitoneal hematoma ipsilateral to the access site. Both instances of access-related complications occurred during urgent therapy for symptomatic VAPA. There were no instances of femoral or brachial artery pseudoaneurysms. Excluding the four patients who died in the perioperative period, the mean length of stay for patients undergoing endovascular VAA or VAPA ablation was 5.3 days (range, 1 to 51 days). The mean lengths of stay were 1.8 days after intervention for VAA and 7.8 days after VAPA treatment. The length of stay for patients with VAPA was extended owing to complications attributable to recent surgeries or significant comorbidities warranting admission. Fig 4. Distribution of visceral artery aneurysms (VAA) and visceral artery pseudoaneurysms (VAPA) amongst the various visceral arterial beds. (SMA, Superior mesenteric artery.) Three patients (6.3%) required secondary interventions. One unsuccessful secondary intervention was attempted in the case of a celiac axis aneurysm, as previously described. A second patient, with Caroli disease and percutaneous biliary catheters, required coil embolization for hemobilia emanating from a third-order hepatic artery pseudoaneurysm. He presented 2 weeks later with recurrent gastrointestinal bleeding and hemobilia. Repeat angiography demonstrated migration of the recently placed coils into the pseudoaneurysm sac associated with sac growth. Successful recoiling proximal to the diseased segment was performed. Another secondary intervention was needed in a patient with a history of orthotopic hepatic transplantation who underwent coil embolization of a bleeding hepatic artery pseudoaneurysm. She presented 2 years later with rebleeding through the previously coiled segment that necessitated repeat endovascular ablation. No access site complications resulted from these reinterventions. Postprocedural imaging was available in 37 (77%) of the 48 patients. This consisted of angiography (n 1), MRI/MRA (n 3), and CT (n 33). Two patients also underwent adjunctive duplex imaging. The mean length of radiologic follow-up was 15.6 months (range, 1 day to 75 months). Flow through the previously treated aneurysm sac was identified in only one patient 3 weeks after embolization; thus, aneurysm exclusion was confirmed in 36 (97.3%) of 37 postoperative studies. No patient demonstrated gross evidence of aneurysm sac growth or endoleak. In addition, no significant decrease in aneurysm sac size post-intervention was noted on follow-up. Six end-organ infarcts, all within the splenic bed, were identified. Volumetric analysis determined the mean infarct size was 19%. Two additional patients displayed evidence of splenic atrophy after embolization without evidence of splenic infarcts. Splenic size was preserved in all cases of splenic artery embolization with postintervention splenic infarct. Of note, all splenic changes were identified during the review of images for this retrospective study. None of these patients exhibited any hematologic or infectious complication or other evidence of clinical sequelae from the changes in spleen volume. No instances of hepatic infarc-
6 JOURNAL OF VASCULAR SURGERY Volume 45, Number 2 Tulsyan et al 281 Table II. Distribution of elective and urgent interventions for visceral artery aneurysms and pseudoaneurysms with associated perioperative results Arterial bed Urgent vs elective No. Mean size (mm) Technical success (%) 30-day mortalityn (%) End-organ ischemia Splenic Urgent Elective (29) Celiac axis branches* Urgent (22) 0 Elective (20) SMA Urgent (100) 0 Elective Hepatic Urgent (11) 0 Elective *Except splenic/hepatic. tion or bowel ischemia were identified during follow-up. No patients were identified with visceral artery aneurysms of other arterial beds. None of the 37 patients with postoperative follow-up had hepatic insufficiency or intestinal ischemia attributable to aneurysm ablation. Postembolization syndrome developed after endovascular ablation of a splenic artery aneurysm in three patients. In one case, there was evidence of distal embolization of N-BCA into the splenic hilum with the presence of multisegmental splenic infarction. Another patient had evidence of splenic atrophy without infarcts. The third patient demonstrated evidence of multiple underperfused segments of spleen. These patients had left-sided abdominal discomfort and diaphragmatic irritation that resolved over time. Despite evidence of splenic ischemia and postembolization syndrome in nearly 40% of patients with treated splenic VAA/VAPA, no patient demonstrated hematologic changes related to splenic insufficiency. Five of 33 CT scans were deemed to have grade 1 artifact, 11 had grade 2 artifact, and 17 had grade 3 artifact. Grade 1 artifact was noted in one MRI/MRA, and grade 3 artifacts were noted in two. No association could be identified between coils and N-BCA and the degree of artifact. DISCUSSION Visceral artery aneurysms and pseudoaneurysms are rare but potentially lethal disease entities. The clinical significance of identifying and appropriately treating these pathologies stems from an effort to prevent aneurysm rupture into the peritoneal cavity or hepatobiliary and gastrointestinal tract. The increased application of high-resolution imaging techniques has resulted in increased identification of VAAs. In addition, increased manipulation of the biliary tree through percutaneous and endoscopic techniques, as well as placement of intravascular chemoembolization catheters, has resulted in a greater incidence of pseudoaneurysmal degeneration of the visceral vessels. Arterial trauma related to laparoscopic treatment of intra-abdominal and retroperitoneal pathologies has also contributed to the increasing incidence of VAPA. Although open surgical repair of these aneurysms remains the gold standard, endoluminal techniques may offer a viable alternative for therapy. Pseudoaneurysms of the splenic artery from pancreatic inflammation, mesenteric artery owing to abdominal sepsis or operative injury, and intrahepatic arterial tree from catheter or stent trauma pose a unique challenge to management: 1. Open surgical repair in these hostile environments is often fraught with technical difficulty and potentially elevates the associated morbidity of the repair. 2. This patient cohort often presents with significant comorbid conditions (pancreatitis, hepatobiliary disease) that elevate the risk of major operative vascular reconstruction. 3. Because many of these patients present acutely with bleeding or rupture, risk-stratification, and medical optimization may not be feasible. As such, minimally invasive endoluminal techniques may offer a distinct advantage to conventional repair. Most of the literature on open repair of visceral artery aneurysms is limited to small series and case reviews. Owing to the relative paucity of visceral artery aneurysms, outcomes for open repair are typically not distinguished by arterial bed. Furthermore, most of the existing studies have not made a distinction between true aneurysms and false aneurysms. This bears significance in assessing operative morbidity and mortality, because the risk of aneurysm rupture is a function of the visceral vessel involved as well as aneurysmal vs pseudoaneurysmal pathology. Mortality rates after the elective treatment of visceral artery aneurysms has been documented as approximately 5%. 8 Conventional treatment of ruptured visceral artery aneurysms is associated with significant mortality. In the setting of splenic artery aneurysm rupture, open reconstruction is associated with operative mortality rates of 10% to 25%. 9 Perioperative death rates may be even greater during conventional treatment of ruptured hepatic, SMA, 3,10 and celiac axis aneurysms. The use of minimally invasive techniques may provide a survival benefit not only for elective interventions but also for urgent procedures in patients presenting with visceral aneurysm rupture. Splenic artery aneurysms comprised 42% of aneurysms treated in this study. The preponderance of aneurysmal disease of the splenic bed is not unexpected. In fact, true splenic artery aneurysms account for 60% of all splanchnic aneurysms. 11 Because variations in hormonal milieu are
7 282 Tulsyan et al JOURNAL OF VASCULAR SURGERY February 2007 believed to contribute to extracellular matrix degeneration, it is not surprising that splenic artery aneurysms are more common in women than in men. Our study did not demonstrate the generally reported fourfold greater incidence of splenic artery aneurysms in women, but women did account for 60% of our cohort. A concern exists for splenic insufficiency after main splenic artery embolization. It was of interest that evidence of splenic ischemia, such as infarcts or significant atrophy, was noted in 40% of cases after splenic artery ablation, but it seemed to have minimal clinical sequelae. This was primarily noted after embolization of distal splenic artery or hilar/intrasplenic aneurysms. Conventional repair of these lesions, with its attendant morbidity, would typically require distal splenic artery ligation or splenectomy. Recently, stent graft repair of splenic artery 12,13 aneurysms has received increasing attention. It offers the potential benefit of maintaining splenic perfusion while excluding the aneurysm, thereby eliminating the risk of rupture. Our review of postoperative imaging suggested that the natural history of true splenic artery aneurysms may also involve elongation and increasing tortuosity of the vessel. In such instances, delivery of a covered stent to a mid-splenic or distal-splenic artery aneurysm may be technically unattainable because of existing device limitations. As such, endovascular stent grafting of these lesions may be confined to the proximal splenic artery. Further assessment of this mode of therapy is warranted for the treatment of splenic artery aneurysms and aneurysmal degeneration of other visceral beds. Technical success was achieved in 98% of our interventions. This is in concordance with other recent reports documenting the high rates of technical success attainable 6 with the endovascular management of VAA. Our study is unique owing to the significant percentage of patients treated for distal extrahepatic, intrahepatic, gastroduodenal/ pancreaticoduodenal, and intrasplenic/hilar lesions. To achieve such rates of technical success, aneurysmal exclusion requires intraoperative high-resolution imaging, technical expertise in visceral vessel cannulation, comfort with use of a triaxial system, and knowledge in the proper preparation and deployment of N-BCA. Although N-BCA is currently approved for the presurgical endoluminal ablation of cerebral arteriovenous malformations, we have found invaluable the extension of its use to treat endoleaks after endovascular aortic aneurysm repair and in the treatment of visceral artery aneurysms. Unlike coils, which are solid, N-BCA is deployed in liquid form before polymerization. This feature is beneficial in ablating aneurysms with multiple outflow vessels or in the setting of persistent aneurysm flow despite coiling. The use of N-BCA requires meticulous detail in preparation. Because it polymerizes on contact with tissue and blood, care must be exercised to reduce the risk of polymerization ex vivo or within the catheter system before deployment. Realizing the potential for microcatheter polymerization, we routinely use a triaxial system with a 3F microcatheter. In such a system, a sheath or guiding catheter is placed into the visceral vessel of interest. A 4F or 5F catheter is telescoped through the sheath or guiding catheter, through which a microcatheter is used for glue deployment. If the glue polymerizes within the microcatheter, rapid exchange of microcatheters is possible without losing visceral vessel access. A 3F microcatheter has also been useful in the exclusion of aneurysms of the intrahepatic circulation and distal arterial beds, where access with a 5F catheter may be unsafe or technically unattainable. We noted a perioperative mortality rate of 8.3%, which is higher than previously reported for the endoluminal 14 ablation of visceral artery aneurysms. All patients who died in the perioperative period had required emergent intervention because of hemorrhage. No mortalities occurred after elective aneurysm ablation. This underscores a critical finding that the endovascular management of VAA/ VAPA in the elective setting has a low rate of perioperative morbidity and mortality. However, the emergent treatment of these lesions, similar to open reconstruction, is associated with elevated rates of procedural morbidity. This study represents, to our knowledge, the largest review of endoluminally excluded visceral artery aneurysms. Radiologic surveillance after ablation highlights the mid-term durability of endovascular aneurysm ablation. No patient with VAA sustained a delayed aneurysm rupture during follow-up. In addition, no patient demonstrated evidence of aneurysm sac growth on postoperative surveillance. Conversely, aneurysm sac shrinkage was also not observed. The use of embolization materials to fill the aneurysm sac likely causes the aneurysm to mold itself to its internal contents. A dilemma is posed with current ablative techniques, however. Although a fluoroscopically identifiable agent is required for accurate deployment, current radiopaque agents create a significant amount of radiologic artifact on postoperative imaging. Assessment of aneurysm sac growth is thereby hampered. The development of fluoroscopically identifiable ablative agents that are not highly radiodense on noninvasive radiologic imaging is needed. In addition, investigation should be performed of alternative means of surveillance, such as color-flow duplex. Our study has various limitations. Inherent to its retrospective design, we are unable to draw conclusions about treatment paradigms for VAA or optimal modes of ablation. Guidelines for size criteria for intervention also cannot be extrapolated from our study. We generally treat all symptomatic aneurysms, visceral aneurysms in women of gestational age, and aneurysms sized 2 cm, but these guidelines have been extrapolated from literature specific to true splenic artery aneurysms. Just as the mortality after rupture of aneurysms of different arterial trees is different, the risk of rupture may also vary between visceral vessels. Pseudoaneurysms must also be evaluated separately 15 from true aneurysms. Tessier et alreviewed their experi - ence with splenic artery pseudoaneurysms during an 18- year period. They did not identify pseudoaneurysm size as being a predictor of risk for rupture because both small (0.3 cm) and large (17 cm) pseudoaneurysms had ruptured in their series. It has been our protocol to treat all visceral artery pseudoaneurysms irrespective of size.
8 JOURNAL OF VASCULAR SURGERY Volume 45, Number 2 Tulsyan et al 283 Ideally, randomized controlled trials comparing endovascular ablation with open reconstruction are required to make firm recommendations for protocols of therapy. Given the paucity of visceral artery aneurysms, however, the distinct behavior between aneurysms of different visceral vessels and the malignant natural history of pseudoaneurysms, such studies would likely be not be realistic or fulfilling. Longer-term follow-up with larger patient cohorts are necessary to elucidate the ultimate role of endoluminal therapy in the treatment of visceral artery aneurysms and pseudoaneurysms. AUTHOR CONTRIBUTIONS Conception and design: VSK, NT, RKG Analysis and interpretation: VSK, NT, RKG, TPS, DGC, GP, KO Data collection: VSK, NT Writing the article: VSK, NT Critical revision of the article: RKG, TPS, DGC, GP, KO Final approval of the article: VSK, NT, RKG, TPS, DGC, GP, KO Statistical analysis: VSK, NT Obtained funding: Not applicable Overall responsibility: VSK REFERENCES 1. Venturini M, Angeli E, Salvioni M, De Cobelli F, Trentin C, Carlucci M, et al. Hemorrhage from a right hepatic artery pseudoaneurysm: endovascular treatment with a coronary stent-graft. J Endovasc Ther 2002;9: Arneson MA, Smith RS. Ruptured hepatic artery aneurysm: case report and review of literature. Ann Vasc Surg 2005;19: Hossain A, Reis ED, Dave SP, Kerstein MD, Hollier LH. Visceral artery aneurysms: experience in a tertiary-care center. Am Surg 2001;67: Zelenock G, Stanley J. Splanchnic artery aneurysms. In: Rutherford R, editor. Vascular surgery. 5th ed. Philadelphia: WB Saunders; p Shanley CJ, Shah NL, Messina LM. Common splanchnic artery aneurysms: splenic, hepatic, and celiac. Ann Vasc Surg 1996;10: Kasirajan K, Greenberg RK, Clair D, Ouriel K. Endovascular management of visceral artery aneurysm. J Endovasc Ther 2001;8: Melissano G, Chiesa R. Successful surgical treatment of visceral artery aneurysms. After failure of percutaneous treatment. Tex Heart Inst J 1998;25: Messina LM, Shanley CJ. Visceral artery aneurysms. Surg Clin North Am 1997;77: Mattar SG, Lumsden AB. The management of splenic artery aneurysms: experience with 23 cases. Am J Surg 1995;169: Wagner WH, Allins AD, Treiman RL, Cohen JL, Foran RF, Levin PM, et al. Ruptured visceral artery aneurysms. Ann Vasc Surg 1997;11: Berceli SA. Hepatic and splenic artery aneurysms. Semin Vasc Surg 2005;18: Larson RA, Solomon J, Carpenter JP. Stent graft repair of visceral artery aneurysms. J Vasc Surg 2002;36: Moyer HR, Hiramoto JS, Wilson MW, Reddy P, Messina LM, Schneider DB. Stent-graft repair of a splenic artery aneurysm. J Vasc Surg 2005;41: Chiesa R, Astore D, Guzzo G, Frigerio S, Tshomba Y, Castellano R, et al. Visceral artery aneurysms. Ann Vasc Surg 2005;19: Tessier DJ, Stone WM, Fowl RJ, Abbas MA, Andrews JC, Bower TC, et al. Clinical features and management of splenic artery pseudoaneurysm: case series and cumulative review of literature. J Vasc Surg 2003;38: Submitted Jun 26, 2006; accepted Oct 30, DISCUSSION Dr Paul Van Bemmelen (Philadelphia, Pa). Did you rule out mycotic aneurysms in this population? Were there any comparable open treatments done during this time period, or is everybody treated endovascularly? Dr Nirman Tulsyan. During the study period, we identified 90 patients with visceral artery aneurysms. Nineteen patients underwent open treatment. The choice of therapeutic modality was primarily operator-dependent given the retrospective nature of this paper. Of the patients who presented with true aneurysms, none clinically manifested prodromal symptoms or signs to suggest presence of a mycotic aneurysm or microbial arteritis with aneurysmal degeneration. With respect to the pseudoaneurysms, the majority of patients presented with signs of systemic inflammation, whether that be intra-abdominal sepsis or retroperitoneal inflammation. While it is possible that these lesions were mycotic, we did not make the distinction nor did it change our management. Dr Grayson Wheatley (Phoenix, Ariz). How do you approach visceral artery aneurysms with respect to embolization versus excluding with an endoluminal graft? I would think that some of these visceral aneurysms would be amenable to exclusion rather than embolization. Dr Tulsyan. Subsequent to the end of the study period, we ve actually treated multiple patients with stent grafts in an effort to maintain parent artery patency. With regard to true aneurysms, we have noted that use of stent grafts is a function of the location of the aneurysm. In the setting of a splenic artery aneurysm, for example, distal, hilar, or intrasplenic lesions would be technically difficult to treat with currently available stent grafts. Additionally, we have noted a significant amount of elongation and tortuosity of parent arteries that occurs in the setting of visceral artery aneurysms. In attempting to treat a distal vessel it may be difficult to deliver your device. It may be feasible, however, in the setting of more proximal lesions. Dr. Robert Cambria (Bangor, Me). Several small series have indicated association of stenosis of major visceral vessels with pseudoaneurysms or, rather, true aneurysms of the visceral segments. Did you notice this association and did it impact in any way on your approach? And finally, were there any aneurysms that you attempted to treat but could not? Dr Tulsyan. In reviewing all of the imaging, we actually did not find a high incidence of aortoiliac occlusive disease. As such, this did not alter our treatment. There was one technical failure in our series. This occurred in a patient who underwent successful treatment of a celiac axis aneurysm but had persistent flow within the celiac trunk after embolization. On follow-up imaging, there was a decrease in aneurysm size. However, since there was significant flow on completion angiography, a secondary intervention was performed via the SMA. Dr Kenneth Cherry (Charlottesville, Va). When you have an aneurysm that involves either the SMA or one of its major branches, are you at all hesitant about providing an occlusive solution as opposed to one that insures continued patency? Dr Tulsyan. All the patients in our study with mesenteric aneurysms were treated for lesions of branch vessels. We would be very hesitant to ablate a main trunk aneurysm of the SMA, for example, since the risk and sequelae of end-organ ischemia is significant in this situation. We would elect for alternative therapy in this instance.
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral Artery Aneurysms Endovascular vs. Open?
 Disclosures Visceral Artery Aneurysms Endovascular vs. Open? John S. Lane III, MD Professor and Acting Chief of Vascular Surgery UC San Diego, Department of Surgery None relevant UCSF Vascular Symposium,
Disclosures Visceral Artery Aneurysms Endovascular vs. Open? John S. Lane III, MD Professor and Acting Chief of Vascular Surgery UC San Diego, Department of Surgery None relevant UCSF Vascular Symposium,
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE
 MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
MODERN METHODS FOR TREATING ABDOMINAL ANEURYSMS AND THORACIC AORTIC DISEASE AAA FACTS 200,000 New Cases Each Year Ruptured AAA = 15,000 Deaths per Year in U.S. 13th Leading Cause of Death 80% Chance of
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Endovascular treatment of a hepatic artery pseudoaneurysm associated with gastrointestinal tract bleeding
 Endovascular treatment of a hepatic artery pseudoaneurysm associated with gastrointestinal tract bleeding Tryfon Vainas, MD, PhD, a Elisabeth Klompenhouwer, MD, b Lucien Duijm, MD, PhD, b Xander Tielbeek,
Endovascular treatment of a hepatic artery pseudoaneurysm associated with gastrointestinal tract bleeding Tryfon Vainas, MD, PhD, a Elisabeth Klompenhouwer, MD, b Lucien Duijm, MD, PhD, b Xander Tielbeek,
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University Hospital Sangmin Kim
 Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Endovascular Procedures for Isolated Common Iliac and Internal Iliac Aneurysm Chungbuk Regional Cardiovascular Center, Division of Cardiology, Departments of Internal Medicine, Chungbuk National University
Visceral Artery Aneurysms: Review of Current Management Options Ulka Sachdev-Ost, MD
 MOUNT SINAI JOURNAL OF MEDICINE 77:296 303, 2010 296 Visceral Artery Aneurysms: Review of Current Management Options Ulka Sachdev-Ost, MD University of Pittsburgh Medical Center, Pittsburgh, PA OUTLINE
MOUNT SINAI JOURNAL OF MEDICINE 77:296 303, 2010 296 Visceral Artery Aneurysms: Review of Current Management Options Ulka Sachdev-Ost, MD University of Pittsburgh Medical Center, Pittsburgh, PA OUTLINE
VISCERAL ANEURYSM MANAGEMENT WHICH ENDOVASCULAR OPTION? PATRICE MWIPATAYI
 VISCERAL ANEURYSM MANAGEMENT WHICH ENDOVASCULAR OPTION? PATRICE MWIPATAYI FCS (SA), MMed, FRACS Professor of Vascular surgery Royal Perth Hospital, University of Western Australia, Perth, WA Conflict of
VISCERAL ANEURYSM MANAGEMENT WHICH ENDOVASCULAR OPTION? PATRICE MWIPATAYI FCS (SA), MMed, FRACS Professor of Vascular surgery Royal Perth Hospital, University of Western Australia, Perth, WA Conflict of
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA)
 The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 29, 2018 Mesenteric Arteriogram & Thrombectomy/Thrombolysis
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of October 29, 2018 Mesenteric Arteriogram & Thrombectomy/Thrombolysis
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
The contemporary management of splenic artery aneurysms
 From the Society for Vascular Surgery The contemporary management of splenic artery aneurysms Ryan O. Lakin, MD, a James F. Bena, MS, b Timur P. Sarac, MD, a Samir Shah, MD, a Leonard P. Krajewski, MD,
From the Society for Vascular Surgery The contemporary management of splenic artery aneurysms Ryan O. Lakin, MD, a James F. Bena, MS, b Timur P. Sarac, MD, a Samir Shah, MD, a Leonard P. Krajewski, MD,
FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX
 FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX 2018 A BIT OF HISTORY First use of F-EVAR : 1990s Park et al. J Vasc Interv Radiol. 1996;7:819-823. Faruqi et al. J Endovasc Surg.
FEVAR FIFTEEN YEARS OF EFFICIENCY E.DUCASSE MD PHD FEBVS CHU DE BORDEAUX 2018 A BIT OF HISTORY First use of F-EVAR : 1990s Park et al. J Vasc Interv Radiol. 1996;7:819-823. Faruqi et al. J Endovasc Surg.
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1
 Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Treatment options for endoleaks: stents, embolizations and conversions
 Treatment options for endoleaks: stents, embolizations and conversions Poster No.: C-0861 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit G. Lombardi; napoli/it Arteries / Aorta, Abdomen,
Treatment options for endoleaks: stents, embolizations and conversions Poster No.: C-0861 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit G. Lombardi; napoli/it Arteries / Aorta, Abdomen,
Talent Abdominal Stent Graft
 Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Talent Abdominal with THE Xcelerant Hydro Delivery System Expanding the Indications for EVAR Treat More Patients Short Necks The Talent Abdominal is the only FDA-approved device for proximal aortic neck
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Management of Endoleaks
 Management of Endoleaks Sarah Ikponmwosa, MD Brooklyn VA 6/20/08 Questions Advantages of endovascular repair Definition of an endoleak Types of endoleaks Management of type lll endoleak Diagnosis of type
Management of Endoleaks Sarah Ikponmwosa, MD Brooklyn VA 6/20/08 Questions Advantages of endovascular repair Definition of an endoleak Types of endoleaks Management of type lll endoleak Diagnosis of type
Endovascular Techniques for Visceral Artery Aneurysm Treatment
 Wednesday, January 31, 2017 17:21-17:27 Endovascular Techniques for Visceral Artery Aneurysm Treatment S.Müller-Hülsbeck, MD, EBIR, FCIRSE, FICA, FSIR ACADEMIC HOSPITALS Flensburg of Kiel University Faculty
Wednesday, January 31, 2017 17:21-17:27 Endovascular Techniques for Visceral Artery Aneurysm Treatment S.Müller-Hülsbeck, MD, EBIR, FCIRSE, FICA, FSIR ACADEMIC HOSPITALS Flensburg of Kiel University Faculty
Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair
 583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
583 Increased Flexibility of AneuRx Stent-Graft Reduces Need for Secondary Intervention Following Endovascular Aneurysm Repair Frank R. Arko, MD; W. Anthony Lee, MD; Bradley B. Hill, MD; Paul Cipriano,
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
An endoleak is radiographic or ultrasonic evidence
 Complex Coil Embolization of Multiple Type II Endoleaks Liquid embolics, detachable coils, and plugs to repair an enlarging abdominal aortic aneurysm sac 5 years after EVAR. BY FRANK R. ARKO, MD; ABRAHAM
Complex Coil Embolization of Multiple Type II Endoleaks Liquid embolics, detachable coils, and plugs to repair an enlarging abdominal aortic aneurysm sac 5 years after EVAR. BY FRANK R. ARKO, MD; ABRAHAM
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Retrograde Embolization of a Symptomatic Hypogastric Artery Aneurysm
 Retrograde Embolization of a Symptomatic Hypogastric Artery Aneurysm Andrew Unzeitig MD Piedmont Atlanta Hospital Georgia Vascular Society 2017 Annual Meeting Lake Oconee, Georgia Disclosures None Case
Retrograde Embolization of a Symptomatic Hypogastric Artery Aneurysm Andrew Unzeitig MD Piedmont Atlanta Hospital Georgia Vascular Society 2017 Annual Meeting Lake Oconee, Georgia Disclosures None Case
Endovascular Repair o Abdominal. Aortic Aneurysms. Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida
 Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Endovascular Repair o Abdominal Aortic Aneurysms Cesar E. Mendoza, M.D. Jackson Memorial Hospital Miami, Florida Disclosure Nothing to disclose. 2 Mr. X AAA Mr. X. Is a 70 year old male who presented to
Abdominal & retroperitoneal endovascular intervention, Bo Kalin, Karolinska Hospital
 Abdominal & retroperitoneal endovascular intervention, Bo Kalin, Karolinska Hospital What is endovascular therapy. Diagnosing Traumatic Arterial Injury Clinical signs CT / CT-angiography To diminish a
Abdominal & retroperitoneal endovascular intervention, Bo Kalin, Karolinska Hospital What is endovascular therapy. Diagnosing Traumatic Arterial Injury Clinical signs CT / CT-angiography To diminish a
Case Report A Case of Successful Coil Embolization for a Late-Onset Type Ia Endoleak after Endovascular Aneurysm Repair with the Chimney Technique
 Case Reports in Vascular Medicine Volume 2016, Article ID 5307416, 4 pages http://dx.doi.org/10.1155/2016/5307416 Case Report A Case of Successful Coil Embolization for a Late-Onset Type Ia Endoleak after
Case Reports in Vascular Medicine Volume 2016, Article ID 5307416, 4 pages http://dx.doi.org/10.1155/2016/5307416 Case Report A Case of Successful Coil Embolization for a Late-Onset Type Ia Endoleak after
Endovascular management of visceral artery aneurysms and pseudoaneurysms
 Endovascular management of visceral artery aneurysms and pseudoaneurysms Poster No.: C-2321 Congress: ECR 2016 Type: Authors: Keywords: DOI: Scientific Exhibit I. Paladini, C. Marcato, S. Bruni, E. Epifani,
Endovascular management of visceral artery aneurysms and pseudoaneurysms Poster No.: C-2321 Congress: ECR 2016 Type: Authors: Keywords: DOI: Scientific Exhibit I. Paladini, C. Marcato, S. Bruni, E. Epifani,
Treatment of Thoracoabdominal Aneurysms Is there a need for custom-made devices?
 : FETURED TECHNOLOGY: JOTEC E-XTR DESIGN ENGINEERING Treatment of Thoracoabdominal neurysms Is there a need for custom-made devices? INTERVIEW ND CSE PRESENTTIONS WITH DNIEL RNZN, MD, ND NDREJ SCHMIDT,
: FETURED TECHNOLOGY: JOTEC E-XTR DESIGN ENGINEERING Treatment of Thoracoabdominal neurysms Is there a need for custom-made devices? INTERVIEW ND CSE PRESENTTIONS WITH DNIEL RNZN, MD, ND NDREJ SCHMIDT,
Endovascular Abdominal Repair: Technical Tips to Achieve Best Results and Avoid Disaster
 Endovascular Abdominal Repair: Technical Tips to Achieve Best Results and Avoid Disaster RICHARD R. HEUSER, MD, FACC, FACP, FESC, FASCI Director Of Cardiology, St. Luke s Medical Center, Phoenix, Arizona
Endovascular Abdominal Repair: Technical Tips to Achieve Best Results and Avoid Disaster RICHARD R. HEUSER, MD, FACC, FACP, FESC, FASCI Director Of Cardiology, St. Luke s Medical Center, Phoenix, Arizona
CUSTOM-MADE SCALLOPED THORACIC ENDOGRAFTS IN DIFFERENT HOSTILE AORTIC ANATOMIES
 CUSTOM-MADE SCALLOPED THORACIC ENDOGRAFTS IN DIFFERENT HOSTILE AORTIC ANATOMIES A SERIES OF THREE CASE REPORTS Joel Sousa Department of Department of Angiology and Vascular Surgery Hospital S. João, Porto,
CUSTOM-MADE SCALLOPED THORACIC ENDOGRAFTS IN DIFFERENT HOSTILE AORTIC ANATOMIES A SERIES OF THREE CASE REPORTS Joel Sousa Department of Department of Angiology and Vascular Surgery Hospital S. João, Porto,
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique
 Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
Repair of Intracranial Vessel Perforation with Onyx-18 Using an Exovascular Retreating Catheter Technique Michael Horowitz M.D. Pittsburgh, Pennsylvania Background Iatrogenic intraprocedural rupture rates
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft
 MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
MEDICAL Reimbursement Guide Zenith Fenestrated AAA Endovascular Graft Disclaimer: The information provided herein reflects Cook s understanding of the procedure(s) and/or device(s) from sources that may
Francesco Giurazza, 1 Mattia Silvestre, 2 Amedeo Cervo, 2 and Franco Maglione Introduction. 2. Case Presentation
 Case Reports in Vascular Medicine Volume 2015, Article ID 291953, 5 pages http://dx.doi.org/10.1155/2015/291953 Case Report Endovascular Treatment of a Dissected Celiac Trunk Aneurysm Complicated with
Case Reports in Vascular Medicine Volume 2015, Article ID 291953, 5 pages http://dx.doi.org/10.1155/2015/291953 Case Report Endovascular Treatment of a Dissected Celiac Trunk Aneurysm Complicated with
Daniela Branzan MD, Department of Vascular Surgery and Department of Interventional Angiology University Hospital Leipzig
 Ischemic Preconditioning with Minimally Invasive Segmental Artery Coil Embolization (MISACE) prior to Endovascular TAAA Repair: Clinical Experience in 50+ Patients Daniela Branzan MD, Department of Vascular
Ischemic Preconditioning with Minimally Invasive Segmental Artery Coil Embolization (MISACE) prior to Endovascular TAAA Repair: Clinical Experience in 50+ Patients Daniela Branzan MD, Department of Vascular
ADDITIONS. The following codes have been added.
 ADDITIONS The following codes have been added. 99446 Interprofessional telephone/internet assessment and management service provided by treating/requesting physician or other qualified health care professional;
ADDITIONS The following codes have been added. 99446 Interprofessional telephone/internet assessment and management service provided by treating/requesting physician or other qualified health care professional;
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease
 Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
How to manage TAVI related vascular complications. Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI
 How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
Hypogastric Preservation Using Retrograde Endovascular Bypass
 Hypogastric Preservation Using Retrograde Endovascular Bypass Mathew Wooster MD, Adam Tanious MD, Brad Johnson MD, Murray Shames MD, Paul Armstrong MD, Martin Back MD Florida Vascular Society 30 th Annual
Hypogastric Preservation Using Retrograde Endovascular Bypass Mathew Wooster MD, Adam Tanious MD, Brad Johnson MD, Murray Shames MD, Paul Armstrong MD, Martin Back MD Florida Vascular Society 30 th Annual
The Society for Vascular Surgery Clinical Practice Guidelines on the Management
 1 2 3 4 5 The Society for Vascular Surgery Clinical Practice Guidelines on the Management of Visceral Aneurysms Rabih A. Chaer, MD, 1 Christopher J. Abularrage, MD, 2 Dawn M. Coleman, MD, 3 Mohammad H.
1 2 3 4 5 The Society for Vascular Surgery Clinical Practice Guidelines on the Management of Visceral Aneurysms Rabih A. Chaer, MD, 1 Christopher J. Abularrage, MD, 2 Dawn M. Coleman, MD, 3 Mohammad H.
The Ventana Off-the-Shelf Graft for Pararenal AAA. Andrew Holden Associate Professor of Radiology Auckland Hospital
 The Ventana Off-the-Shelf Graft for Pararenal AAA Andrew Holden Associate Professor of Radiology Auckland Hospital Disclosures Andrew Holden, MBChB, FRANZCR Investigator in Nellix and Ventana Trials Clinical
The Ventana Off-the-Shelf Graft for Pararenal AAA Andrew Holden Associate Professor of Radiology Auckland Hospital Disclosures Andrew Holden, MBChB, FRANZCR Investigator in Nellix and Ventana Trials Clinical
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Imaging abdominal vascular emergencies. V.Stoynova
 Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely
 Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Is EVAS a proper choice in women?
 Is EVAS a proper choice in women? CACVS 2018 Jan MM Heyligers, PhD, FEBVS Consultant Vascular Surgeon Elisabeth TweeSteden Hospital Tilburg The Netherlands Disclosures Consultant for Endologix DEVASS =Dutch
Is EVAS a proper choice in women? CACVS 2018 Jan MM Heyligers, PhD, FEBVS Consultant Vascular Surgeon Elisabeth TweeSteden Hospital Tilburg The Netherlands Disclosures Consultant for Endologix DEVASS =Dutch
Description. Section: Surgery Effective Date: April 15, Subsection: Surgery Original Policy Date: December 6, 2012 Subject:
 Last Review Status/Date: March 2015 Page: 1 of 6 Description Wireless sensors implanted in an aortic aneurysm sac after endovascular repair are being investigated to measure post procedural pressure. It
Last Review Status/Date: March 2015 Page: 1 of 6 Description Wireless sensors implanted in an aortic aneurysm sac after endovascular repair are being investigated to measure post procedural pressure. It
PERPHERAL ARTERY ANEURYSM. By Pooja Sharma and Susanna Sebastianpillai
 PERPHERAL ARTERY ANEURYSM By Pooja Sharma and Susanna Sebastianpillai Defintions True Aneurysm Involves all three layers of the vessel. Have two basic shapes; Fusiform = symmetric widening of the vessels
PERPHERAL ARTERY ANEURYSM By Pooja Sharma and Susanna Sebastianpillai Defintions True Aneurysm Involves all three layers of the vessel. Have two basic shapes; Fusiform = symmetric widening of the vessels
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue
 Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Interventions in Visceral Artery Bleed
 Interventions in Visceral Artery Bleed Dr. Arun Gupta Consultant, Interventional Radiology Sir Ganga Ram Hospital, Delhi, India. INTRODUCTION Visceral artery aneurysms (VAAs) are rare, reported incidence
Interventions in Visceral Artery Bleed Dr. Arun Gupta Consultant, Interventional Radiology Sir Ganga Ram Hospital, Delhi, India. INTRODUCTION Visceral artery aneurysms (VAAs) are rare, reported incidence
How to Determine Tolerance for Branch Vessel Coverage
 How to Determine Tolerance for Branch Vessel Coverage Venita Chandra, MD Clinical Assistant Professor of Surgery Division of Stanford Medical School, Stanford, CA PNEC May 25 th, 2017 DISCLOSURES Venita
How to Determine Tolerance for Branch Vessel Coverage Venita Chandra, MD Clinical Assistant Professor of Surgery Division of Stanford Medical School, Stanford, CA PNEC May 25 th, 2017 DISCLOSURES Venita
The First 150 Endovascular AAA Repairs at a Single Institution: How Steep Is the Learning Curve?
 J ENDOVASC THER 69 CLINICAL INVESTIGATION The First 50 Endovascular AAA Repairs at a Single Institution: How Steep Is the Learning Curve? W. Anthony Lee, MD; Yehuda G. Wolf, MD; Bradley B. Hill, MD; Paul
J ENDOVASC THER 69 CLINICAL INVESTIGATION The First 50 Endovascular AAA Repairs at a Single Institution: How Steep Is the Learning Curve? W. Anthony Lee, MD; Yehuda G. Wolf, MD; Bradley B. Hill, MD; Paul
Ancillary Components with Z-Trak Introduction System
 Ancillary Components with Z-Trak Introduction System Zenith Flex AAA Endovascular Graft Ancillary Components Converter Converters can be used to convert a bifurcated graft into an aortouniiliac graft if
Ancillary Components with Z-Trak Introduction System Zenith Flex AAA Endovascular Graft Ancillary Components Converter Converters can be used to convert a bifurcated graft into an aortouniiliac graft if
Rupture Risk and Etiology of Visceral Artery Aneurysms and Pseudoaneurysms: A Single-Center Experience
 Original Manuscript Rupture Risk and Etiology of Visceral Artery Aneurysms and Pseudoaneurysms: A Single-Center Experience Vascular and Endovascular Surgery 2016, Vol. 50(1) 10-15 ª The Author(s) 2016
Original Manuscript Rupture Risk and Etiology of Visceral Artery Aneurysms and Pseudoaneurysms: A Single-Center Experience Vascular and Endovascular Surgery 2016, Vol. 50(1) 10-15 ª The Author(s) 2016
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
SANWICH TECHNIQUE TO REDUCE COMPLICATIONS WHEN TREATING BILATERAL INTERNAL ILIAC ARTERY
 SANWICH TECHNIQUE TO REDUCE COMPLICATIONS WHEN TREATING BILATERAL INTERNAL ILIAC ARTERY TRAN TRA GIANG.MD Interventional cardiovascular department Hanoi Heart Hospital, Hanoi, Viet Nam Nothing to Disclose
SANWICH TECHNIQUE TO REDUCE COMPLICATIONS WHEN TREATING BILATERAL INTERNAL ILIAC ARTERY TRAN TRA GIANG.MD Interventional cardiovascular department Hanoi Heart Hospital, Hanoi, Viet Nam Nothing to Disclose
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Possible graft-related complications in visceral debranching for hybrid B dissection repair
 Featured Article Possible graft-related complications in visceral debranching for hybrid B dissection repair Roberto Chiesa, Yamume Tshomba, Davide Logaldo, Andrea Kahlberg, Domenico Baccellieri, Luca
Featured Article Possible graft-related complications in visceral debranching for hybrid B dissection repair Roberto Chiesa, Yamume Tshomba, Davide Logaldo, Andrea Kahlberg, Domenico Baccellieri, Luca
EVAR replaced standard repair in most cases. Why?
 EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
The Role of US in Chronic Mesenteric Ischemia. Sagar S. Gandhi, MD Vascular Health Alliance Greenville Health System
 The Role of US in Chronic Mesenteric Ischemia Sagar S. Gandhi, MD Vascular Health Alliance Greenville Health System No Disclosures Mesenteric Ischemia Anatomy Presentation Diagnostic tools Treatment Celiac
The Role of US in Chronic Mesenteric Ischemia Sagar S. Gandhi, MD Vascular Health Alliance Greenville Health System No Disclosures Mesenteric Ischemia Anatomy Presentation Diagnostic tools Treatment Celiac
2019 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule
 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Chapter 18. Recommended clinical competencies for initiating a program in endovascular repair of the thoracic aorta
 Chapter 18 Recommended clinical competencies for initiating a program in endovascular repair of the thoracic aorta Ross Milner, MD, Karthik Kasirajan, MD, and Elliot L. Chaikof, MD, PhD, Atlanta, Ga The
Chapter 18 Recommended clinical competencies for initiating a program in endovascular repair of the thoracic aorta Ross Milner, MD, Karthik Kasirajan, MD, and Elliot L. Chaikof, MD, PhD, Atlanta, Ga The
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Robert F. Cuff, MD FACS SHMG Vascular Surgery
 Robert F. Cuff, MD FACS SHMG Vascular Surgery Objectives To become familiar with the commercially available fenestrated EVAR graft Discuss techniques to increase success Review available data to determine
Robert F. Cuff, MD FACS SHMG Vascular Surgery Objectives To become familiar with the commercially available fenestrated EVAR graft Discuss techniques to increase success Review available data to determine
Case Report Idiopathic Giant Hepatic Artery Pseudoaneurysm
 Hindawi Case Reports in Vascular Medicine Volume 2017, Article ID 4658065, 4 pages https://doi.org/10.1155/2017/4658065 Case Report Idiopathic Giant Hepatic Artery Pseudoaneurysm Ahmed Abdelbaki, 1 Neeraj
Hindawi Case Reports in Vascular Medicine Volume 2017, Article ID 4658065, 4 pages https://doi.org/10.1155/2017/4658065 Case Report Idiopathic Giant Hepatic Artery Pseudoaneurysm Ahmed Abdelbaki, 1 Neeraj
Access More Patients. Customize Each Seal.
 Access More. Customize Each Seal. The Least Invasive Path Towards Proven Patency ULTRA LOW PROFILE TO EASE ADVANCEMENT The flexible, ultra-low 12F ID Ovation ix delivery system enables you to navigate
Access More. Customize Each Seal. The Least Invasive Path Towards Proven Patency ULTRA LOW PROFILE TO EASE ADVANCEMENT The flexible, ultra-low 12F ID Ovation ix delivery system enables you to navigate
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment
 Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]
![General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ] General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]](/thumbs/76/74079340.jpg) General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
Case Report Spleen-Preserving Surgery in Splenic Artery Aneurysm
 Hindawi Case Reports in Surgery Volume 2017, Article ID 8716962, 4 pages https://doi.org/10.1155/2017/8716962 Case Report Spleen-Preserving Surgery in Splenic Artery Aneurysm Ulaş Aday,Emre Bozdağ,EbubekirGündeş,Selçuk
Hindawi Case Reports in Surgery Volume 2017, Article ID 8716962, 4 pages https://doi.org/10.1155/2017/8716962 Case Report Spleen-Preserving Surgery in Splenic Artery Aneurysm Ulaş Aday,Emre Bozdağ,EbubekirGündeş,Selçuk
An unusual source of right upper quadrant pain
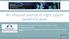 Originally Posted: Month, 00, 20xx An unusual source of right upper quadrant pain Resident(s): Ashish R. Vyas MD (PGY-V), Dominic T. Semaan M.D., J.D. (PGY-V) Attending(s): Dr. Denis Lincoln Program/Dept(s):
Originally Posted: Month, 00, 20xx An unusual source of right upper quadrant pain Resident(s): Ashish R. Vyas MD (PGY-V), Dominic T. Semaan M.D., J.D. (PGY-V) Attending(s): Dr. Denis Lincoln Program/Dept(s):
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Physician s Vascular Interpretation Examination Content Outline
 Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Percutaneous Approaches to Aortic Disease in 2018
 Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Percutaneous Approaches to Aortic Disease in 2018 Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network Case 78 year old F Lower CP and upper
Vascular Access: Management of Complications. Chris Burrell, South West Cardiothoracic Centre, Plymouth
 Vascular Access: Management of Complications Chris Burrell, South West Cardiothoracic Centre, Plymouth Alternative Vascular Access Sites Femoral Axillary Brachial Radial Ulnar Femoral v Radial Vascular
Vascular Access: Management of Complications Chris Burrell, South West Cardiothoracic Centre, Plymouth Alternative Vascular Access Sites Femoral Axillary Brachial Radial Ulnar Femoral v Radial Vascular
History of the Powerlink System Design and Clinical Results. Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ
 History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
History of the Powerlink System Design and Clinical Results Edward B. Diethrich Arizona Heart Hospital Phoenix, AZ Powerlink System: Unibody-Bifurcated Design Long Main Body Low-Porosity Proprietary eptfe
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Case Endovascular management of non maturing dyalisis vascular access
 Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Case 10238 Endovascular management of non maturing dyalisis vascular access Guedes Pinto 1, Erique; Madeira 2, Célia; Sousa 3, Marta; Penha 1, Diana; Rosa 1, Luís; Germano 1, Ana; Baptista 1, Manuela 1
Scanning Mesenteric and Hypogastric Artery Aneurysms
 Scanning Mesenteric and Hypogastric Artery Aneurysms Marsha M. Neumyer, BS, RVT, FSVU, FSDMS, FAIUM International Director Vascular Diagnostic Education Services Vascular Resource Associates Harrisburg,
Scanning Mesenteric and Hypogastric Artery Aneurysms Marsha M. Neumyer, BS, RVT, FSVU, FSDMS, FAIUM International Director Vascular Diagnostic Education Services Vascular Resource Associates Harrisburg,
6. Endovascular aneurysm repair
 Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques
 Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Infected Lower Extremity Aneurysms C. Stefan Kénel-Pierre, MD
 Infected Lower Extremity Aneurysms C. Stefan Kénel-Pierre, MD University Hospital of Brooklyn Department of Surgery History 52F c PMHx of HTN, asthma p/w fever, malaise s/p one week of ABx for presumed
Infected Lower Extremity Aneurysms C. Stefan Kénel-Pierre, MD University Hospital of Brooklyn Department of Surgery History 52F c PMHx of HTN, asthma p/w fever, malaise s/p one week of ABx for presumed
Nellix Endovascular System: Clinical Outcomes and Device Overview
 Nellix Endovascular System: Clinical Outcomes and Device Overview Jeffrey P. Carpenter, MD Professor and Chief, Department of Surgery CAUTION: Investigational device. This product is under clinical investigation
Nellix Endovascular System: Clinical Outcomes and Device Overview Jeffrey P. Carpenter, MD Professor and Chief, Department of Surgery CAUTION: Investigational device. This product is under clinical investigation
Outcomes of endovascular repair of isolated iliac artery aneurysms. A. Stella
 Alma Mater Studiorum Bologna University S.Orsola-Malpighi, Bologna, Italy Vascular Surgery Outcomes of endovascular repair of isolated iliac artery aneurysms A. Stella Isolated iliac artery aneurysms treated
Alma Mater Studiorum Bologna University S.Orsola-Malpighi, Bologna, Italy Vascular Surgery Outcomes of endovascular repair of isolated iliac artery aneurysms A. Stella Isolated iliac artery aneurysms treated
Approaches to type II Endoleaks: Transcaval, transarterial, translumbar. Saher Sabri,MD University of Virginia
 Approaches to type II Endoleaks: Transcaval, transarterial, translumbar Saher Sabri,MD University of Virginia Saher Sabri, M.D. Speakers Bureau: W.L.Gore & Associates, Abbott Type 2 Endoleaks after EVAR
Approaches to type II Endoleaks: Transcaval, transarterial, translumbar Saher Sabri,MD University of Virginia Saher Sabri, M.D. Speakers Bureau: W.L.Gore & Associates, Abbott Type 2 Endoleaks after EVAR
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Case Report Surgical Treatment for Profunda Femoris Artery Aneurysms: Five Case Reports
 Case Reports in Vascular Medicine Volume 2015, Article ID 375278, 5 pages http://dx.doi.org/10.1155/2015/375278 Case Report Surgical Treatment for Profunda Femoris Artery Aneurysms: Five Case Reports Kimihiro
Case Reports in Vascular Medicine Volume 2015, Article ID 375278, 5 pages http://dx.doi.org/10.1155/2015/375278 Case Report Surgical Treatment for Profunda Femoris Artery Aneurysms: Five Case Reports Kimihiro
