Endoscopic Ultrasound-Guided Biliary Drainage
|
|
|
- Marylou McCoy
- 5 years ago
- Views:
Transcription
1 Review Article pissn eissn Korean J Radiol 2012;13(S1):S74-S82 Endoscopic Ultrasound-Guided Biliary Drainage Everson L.A. Artifon, MD, PhD, Flávio C. Ferreira, MD, Paulo Sakai, MD, PhD All authors: University of São Paulo, São Paulo, SP-Brazil Objective: To demonstrate a comprehensive review of published articles regarding endoscopic ultrasound (EUS)-guided biliary drainage. Materials and Methods: Review of studies regarding EUS-guided biliary drainage including case reports, case series and previous reviews. Results: EUS-guided hepaticogastrostomy, coledochoduodenostomy and choledoantrostomy are advanced biliary and pancreatic endoscopy procedures, and together make up the echo-guided biliary drainage. Hepaticogastrostomy is indicated in cases of hilar obstruction, while the procedure of choice is the coledochoduodenostomy or choledochoantrostomy in distal lesions. Both procedures must be performed only after unsuccessful ERCPs. The indication of these procedures must be made under a multidisciplinary view while sharing information with the patient or legal guardian. Conclusion: Hepaticogastrostomy and coledochoduodenostomy or choledochoantrostomy are feasible when performed by endoscopists with expertise in biliopancreatic endoscopy. Advanced echo-endoscopy should currently be performed under a rigorous protocol in educational institutions. Index terms: Biliary tract; Drainage; Endosonography; Gastrointestinal endoscopy; Obstructive jaundice INTRODUCTION Endoscopic biliary stenting at ERCP is a well-established therapy for both benign and malignant biliary obstructions (1-3). Biliary cannulation fails in 10-15% of cases due to several reasons including ampullary pathology (tumor, stenosis, stones), periampullary diverticulum, anatomic variations or in patients where the papilla cannot be reached by the duodenoscope as in gastric outlet Received October 25, 2011; accepted after revision December 14, Corresponding author: Everson L.A. Artifon, MD, PhD, University of São Paulo Medical School, Av. Dr. Enéas de Carvalho Aguiar, 255-Cerqueira César , São Paulo, SP-Brazil. Tel: (5511) Fax: (5511) eartifon@hotmail.com This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. obstruction and surgically altered anatomy (gastric bypass, Roux-en-Y reconstruction). To overcome ERCP failures and improve outcomes over those afforded by more invasive alternatives - percutaneous transhepatic biliary drainage (PTBD) and surgery, as well as endoscopic ultrasound (EUS)- guided ductal access techniques paired with standard ERCP drainage techniques, have been developed in recent years. This hybrid procedure is given a variety of names, but the more encompassing one is endosonographic cholangiopancreatography (ESCP)(4). Based on the combination of the three possible access routes (intrahepatic bile duct, extrahepatic bile duct, and pancreatic duct) with the three possible drainage routes (transmural, transpapillary antegrade, and transpapillary retrograde), ESCP admits several variant approaches for both pancreatic and biliary drainage; the last also referred to collectively as EUS-guided biliary drainage (EUSBD). The rationale for all variant EUSBD approaches, as a second-line option in select difficult cases where ERCP is S74
2 Endoscopic US-Guided Biliary Drainage not feasible, is threshold. EUSBD may be potentially more convenient because it is performed in the same session, more physiological given that it allows immediate internal biliary drainage, and less invasive given that it affords a more accurate control as well as more access sites to the bile duct than the classical alternatives of PTBD or surgery. EUS-BD is an invasive and complex procedure. Knowledge about the full array of needle devices, guidewires, dilators and stents, as well as the subtle variations in scope position (gastric or duodenal), scope orientation (upward and downward), and stent anchoring techniques, is highly recommended for increasing procedure success rates and minimize complications. EUS-Guided Hepatico-Gastrostomy EUS-guided hepatico-gastrostomy (HG) was first reported in 2003 by Burmester et al. with the performance of EUS-HG in a Billroth II patient with unresectable pancreatic cancer and failed ERCP due to tumor infiltration of the papilla. EUS-HG is closely related to EUS-guided drainage of pancreatic pseudocysts (5). The procedure consists of identification of the bile duct by EUS, followed by a puncture with a needle. The puncture tract is then dilated using cautery, mechanical devices, or both, and a stent is placed across the puncture tract to drain the duct into the GI tract lumen. Technique of EUS-Guided Hepatico-Gastrostomy (EUS- HG) The procedural steps of EUS-HG are as follows: Using an interventional echoendoscope, the dilated left hepatic duct (usually segment III) is well visualized. EUS-HG is then performed under combined fluoroscopic and ultrasound guidance, with the tip of the echoendoscope positioned such that the ultrasound transducer is either in the middle part of the small curvature of the stomach or slightly upwards, closer to the cardia. A 19G FNA needle is inserted transgastrically into a peripheral branch of the left hepatic duct, and contrast medium is injected. Before injecting the contrast fluid, bile can be aspirated through the needle in order to confirm the intraductal position of the needle tip. Opacification delineates fluoroscopically the dilated biliary tree above the point of obstruction. The needle is exchanged over a guidewire for a 6.0-Fr diathermic sheath, which is then used to enlarge the channel between the stomach (or jejunum in patients with total gastrectomy), and the left hepatic duct. The diathermic sheath is advanced across the intervening liver parenchyma by using a cutting current. After removing the guidewire, the diathermic sheath, which is an 8.5-Fr, 8-cm - long hepatico-gastric stent) or an 8 cm long covered self-expandable metal stent (SEMS), partially covered or fully covered, is placed transmurally. Fluoroscopy confirms adequate stent placement and function by showing contrast drainage through the stent into the stomach (Fig. 1). Bile leakage into the peritoneum is the major risk factor for EUS-HG. Several strategies are used by different authors to minimize this risk. A 6 or 7-Fr naso-biliary drain with mild aspiration or gravity drainage can be left in place through the metal stent over 48 hours, even if this is somewhat inconvenient to the patient. More recently, this method has been developed into a more patientfriendly approach to minimize the risk of leakage, by combining an uncovered metal stent with a covered metal stent inside. The uncovered stent is initially deployed to provide anchorage and prevent migration. The covered stent is inserted coaxially and deployed within the first stent. Finally, in cases where the guidewire crosses the downstream stricture antegradely, hepaticogastrostomy can be combined with antegrade placement of an additional metal stent bridging in the distal stricture, which further decreases the pressure gradient across the transmural stent by providing additional downstream decompression of the bile duct (6). Alternative strategies used by other authors to prevent migration include the placement of fully covered SEMS with both ends flared (7), or forceful balloon expansion upon stent deployment (as opposed to gradual spontaneous self-expansion over several hours) to monitor foreshortening and the insertion of a double pig-tail stent through the expanded SEMS in order to provide additional anchorage (8). EUS-HG in Comparison with Other EUSBD Approaches The specific anatomic features of patients that may make EUS-HG preferable to other EUSBD are based on the intrahepatic access route and the transmural drainage route. Intrahepatic access is the only choice in patients with proximal (hilar) biliary obstruction, and is usually more convenient in patients with distal gastrectomy since imaging the common bile duct (CBD) under EUS is not always possible in postoperative altered anatomy setting (9). One advantage of transmural drainage after intrahepatic bile duct access over transpapillary drainage is that the S75
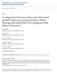
3 Artifon et al. Fig. 1. Endoscopic ultrasound (EUS)-guided hepatico gastrostomy is demonstrated using step-by-step technique in which we can see EUS images with dilated IHD, puncture, cholangiography, guidewire placement, fistulization using needle-knife catheter, and deployment of partially covered self-expandable metal stent. challenging step of antegrade guidewire passage (required for both rendezvous and antegrade stenting) is avoided. In addition to guidewire passage, rendezvous requires an accessible papilla, which is usually not the case in patients with a surgically altered anatomy or tight duodenal stenosis. Antegrade stent insertion does not require an accessible papilla, but involves dilation of the puncture tract, just as EUS-HG. In patients with postoperative anatomy, antegrade transpapillary stenting without combined hepaticogastrostomy is less convenient for stent revisions, since HG provides easy repeat access to the bile duct without the need for a repeat puncture. Stent revisions are not uncommonly required during follow-up. The advantages of EUS-HG over rendezvous or antegrade stent insertion are particularly relevant in patients with prior duodenal or biliary SEMS who experience recurrent biliary obstruction (10). However, these variant EUSBD approaches should be viewed as complementary rather than mutually exclusive. For example, as mentioned when discussing strategies to minimize the risk of bile leakage in EUS-HG, antegrade transpapillary stents can be combined with transmural stenting (6). Püspök et al. (11) performed an antegrade transpapillary SEMS insertion in a patient with recurrent gastric cancer after a Roux-en-Y gastrectomy. The authors then left a transmural plastic stent across the puncture tract to both minimize the risk of leakage and to preserve access. Dual drainage (antegrade and transmural) has also been used serially. Fujita et al. (12) performed transesophageal EUSBD by inserting a 7-Fr plastic stent into a peripheral left bile duct branch in a patient with advanced gastric cancer. Ten days later, the plastic stent was cannulated with a guidewire and removed with a snare (13). Then, using flexible devices through the mature fistula, the guidewire was manipulated under fluoroscopy across the malignant distal bile duct stricture, and a SEMS passed antegradely over the wire was subsequently deployed across the stricture above the papilla. Patients with distal bile duct obstruction without prior gastrectomy who have both intra and extrahepatic bile duct dilations (and no gross ascites), are the only cases in which an intrahepatic or extrahepatic access site for EUSBD might be preferable if the selection criteria for EUSBD versus PTBD are broad, [i.e., EUSBD is favoured as the initial second-line approach after failed ERCP, and this type of patient may represent just 20% of the candidate population (14)]. Operator preference plays a part in this small patient subset. CBD offers a more obvious target for an EUS puncture, the echoendoscope is in a more anchored position, and access to the CBD probably makes rendezvous easier than for intrahepatic access. On the other hand, intrahepatic EUSBD is performed with an echoendoscope in a more straight position, which favors the transmission of the pushing force during stent insertion. It is also probably S76
4 Endoscopic US-Guided Biliary Drainage easier to penetrate a small intrahepatic bile duct surrounded by liver parenchyma than the fibrotic, hard wall of the CBD. Literature Findings Based on the Perspective of Evidence-Based Medicine To date, transmural intrahepatic EUSBD has been reported in 51 patients, EUS-HG in 42, and other closely related variant approaches through a transjejunal or a transesophageal route in 9. In five patients with total gastrectomy, the left bile duct was similarly accessed under EUS from below the cardia and transmural stents were placed across the jejunal wall. In the remaining four patients, a cephalad peripheral left bile duct branch was selected for puncture, so that eventually the stent pierced the wall of the intra-abdominal esophagus slightly above the cardia. Approximately half of these patients come from three small series, which specifically deal with transmural intrahepatic EUSBD (6, 10, 15), whereas the other half comes from either mixed series in which EUS-HG is reported along extrahepatic EUSBD (7, 11, 16-19) or individual case reports (12, 20-24) (Table 1). EUS-HG (or its variants) was technically successful in 49 out of these 51 patients, with clinical resolution of biliary obstruction in 46 cases. Therefore EUS-HG had a 94% per-protocol success rate and a 90.2% success rate on an intention-to-treat basis. These success rates are very high, considering the difficult patient population in which EUS-HG was attempted. However, it is important to remember that success was achieved at the expense of an overall 20% complication rate, twice as high as that of ERCP. Most complications were accounted for by inadequate biliary drainage, resulting in either peritoneal bile leakage or cholangitis (Table 1). Plastic stents caused cholangitis due to early migration (19) or early clogging (6). Foreshortening of transmural SEMS led to bile perotinitis or biloma, requiring percutaneous drainage and repeat EUSBD (6), and caused the only reported death to date (24). Half of the complications were nonetheless mild, manifesting as transient abdominal pain with or without pneumoperitoneum that settled on conservative measures. There is great consistency across all reports on EUS-HG regarding technical details except for the use of cautery, be it kneedle-knives or fistulotomes and the choice of the stent. Overall, any diathermy use was reported in just 39.5% of cases, with some authors using it routinely (6), and others resorting to it selectively (7) (only after failure Table 1. Summary of Published Literature on EUS-HG and Related Transmural Intrahepatic EUSBD Techniques Author/Ref/Year n Total n IH-Transmural Success Complications Initial Stent EUSBD EUSHG non-hg Technical Clinical n Type Plastic SEMS Burmester Püspök Artifon Bories cholangitis, 1 ileus, 1 biloma 7 3 Will cholangitis, 1 pain 2 5 Chopin-Laly Iglesias-Garcia NS NS Horaguchi Cholangitis 7 0 Maranki Park Pneumo 0 9 Park Martins Peritonitis & death 0 1 Eum Total mild / 5 severe Note. Case reports from Giovannini et al. (20) and Fujita et al. (12) are not tallied because they are already included in case series by Bories et al. (6) and Horaguchi et al. (19), respectively. EUSBD = endoscopic ultrasound-guided biliary drainage, HG = hepatico-gastrostomy, Pneumo = pneumoperitoneum, SEMS = self-expandable metal stent S77
5 Artifon et al. to advance a mechanical dilator over the guidewire), or do not use it at all (15). As detailed in Table 1, 7 to 8.5-Fr plastic stents were placed in 46% of cases, whereas uncovered, partially covered or fully covered SEMS were placed initially in 54% of cases. It is difficult to draw significant conclusions from published reports, since no formal comparisons have been made between the two types of stents. SEMS are appealing for three reasons. First, upon full expansion, SEMS effectively seals the puncture/dilation tract, which would in theory prevent leakage more effectively. Secondly, their larger diameter provides better long-term patency, which would decrease the need for stent revisions. Finally, if dysfunction by ingrowth or clogging occurs, management is somewhat less challenging than with plastic stents, since a new stent (plastic or SEMS) can easily be inserted through the occluded SEMS in place. In contrast, exchanging a clogged plastic transmural stent usually requires overthe-wire replacement, because free-hand removal involves the risk of track disruption with subsequent guidewire passage into the peritoneum, hence requiring repeat EUSBD (or PTBD) to re-establish drainage (13). These presumed advantages of SEMS must be balanced against the fact that transmural SEMS insertion and deployment are somewhat more demanding than they are for ERCP. In particular, the serious risk of foreshortening and bile peritonitis should be prevented with careful attention to detail (24). EUS-Guided Choledocho-Duodenostomy Rationale EUS-guided extrahepatic bile duct drainage is performed in a procedure where the CBD is punctured from a transduodenal or transgastric approach (usually from the distal antrum). The CBD is more easily imaged under EUS than the intrahepatic bile ducts, providing a faster, cleaner access without repeated puncture attempts, thereby minimizing risks. The retroperitoneal location of the CBD makes it also an attractive access site for patients with ascites, in whom fluid around the liver makes transhepatic access (whether percutaneous or transgastric under EUS) more difficult and hazardous. Besides the advantages of extrahepatic access over intrahepatic access, the specific rationale for EUS- Choledochoduodenostomy (CDS) is also derived from the transmural drainage route, as opposed to transpapillary EUSBD (antegrade or rendezvous) (11, 25). The real choice between transmural and transpapillary drainage after extrahepatic bile duct access under EUS, therefore lies between EUS-CDS and rendezvous. Proponents of rendezvous argue that it may be less invasive than EUS- CDS, since transmural interventions are usually limited to puncture and guidewire passage. Hence, drainage is accomplished retrogradely via ERCP without the need for puncture tract dilation (26). However, EUSBD rendezvous carries a 20% failure rate; even in expert centers, because guidewire passage across the stricture and the papilla is often unsuccessful. The needle allows virtually no interplay with the guidewire, which cannot be manipulated across the stricture through a needle in the same way as it can be done at ERCP using flexible catheters. Therefore, advantages of EUS-CDS over transpapillary rendezvous are its higher success rate and relative simplicity, which appear to make it a more reproducible approach, despite being perhaps more invasive. Nonetheless, both EUSBD variant approaches can be considered complementary inasmuch as these procedures are used in a heterogeneous patient population. As we will discuss below, some indications are better suited for EUS-CDS, whereas in other cases EUSBD rendezvous is clearly advantageous. Similarly, even if rendezvous is the intended drainage technique, EUS-CDS can be used as a second line approach to salvage the significant proportion of failed rendezvous cases (17, 27). This open-ended approach to EUSBD (i.e., including both rendezvous and EUS-CDS), results in comparatively higher success rates than that of an EUSBD series, hence limiting their approach to just rendezvous (26). It is important to know that choledochoantrostomy, described by Artifon et al. (28), is a new technique that is useful for those patients with duodenal bulb infiltration, and may be a new and feasible tool as a variant of choledochoduodenostomy. EUS-Guided Choledochoduodenostomy Technique Indications In common with other EUSBD techniques, EUS-CDS should only be considered in patients with confirmed (not just suspected) biliary obstruction after a failed ERCP and despite maximal attempts by experienced operators. EUS-CDS has specific anatomic requirements differing from other EUSBD alternatives. The first anatomic requirement is distal biliary obstruction. In other words, EUS-CDS is not suitable for proximal (hilar) biliary obstruction where intrahepatic EUSBD approaches are clearly required. The S78
6 Endoscopic US-Guided Biliary Drainage second anatomic requirement is the ability to image the CBD under EUS. Since the CBD is typically imaged from the distal stomach or the duodenal bulb, this is difficult or impossible in patients with prior gastrectomy and gastrojejunostomy (e,g, Roux-en-Y) (9). Finally, as with most other EUSBD approaches, EUS- CDS is predominantly used in patients with malignant biliary obstruction. Where alternative approaches such as rendezvous may rightly be considered after failed cannulation in patients with documented benign causes of biliary obstruction (eg, CBD stones or papillary stenosis), EUS-CDS is less adequate in these distinct settings, where biliary drainage is usually accomplished by means of a sphincterotomy (with or without stone removal) as opposed to stenting. Technical Data Puncture of the CBD from the duodenum (EUS-CDS) is the most common approach for biliary drainage. A similar approach from the stomach (EUS-choledochogastrostomy or EUS-choledochoantrostomy) may also be used in selected instances depending on the patient s anatomy. The orientation of the needle should be checked with fluoroscopy before the puncture is actually carried out. EUSguided puncture can be made with different sized needles, mostly 19G and 22G, which are inserted transduodenally into the bile duct under EUS visualization. To confirm needle ductal access, the stylet is removed and bile is aspirated. If there is a bile return, contrast medium is injected into the bile duct for cholangiography, and then, a 450 cm long guidewire is inserted through the outer sheath and its position is confirmed fluoroscopically (Fig. 2). After guidewire access into the bile duct, some dilation of the puncture track is usually necessary, using either a dilating biliary catheter, a papillary balloon dilator or two types of needles commonly used at ERCP such as needle-knife or cystotome. This is aimed at dilating the choledochoduodenal fistula to facilitate stent insertion. Finally, a 5-Fr to 10-Fr plastic stent (straight or pigtail) or a fully covered SEMS is inserted through the choledochoduodenostomy site into the CBD. Care should be taken to monitor, by fluoroscopy, the intraductal placement of the proximal end of the stent and to monitor by endoscopy the intraduodenal (or intragastric) position of the distal (closer to the scope) end of the stent. This latter aspect is of particular relevance when using SEMS. To prevent SEMS dislodgment, an adequate length of SEMS (15-20 mm) should be left inside the GI lumen. Additional anchorage techniques to prevent dislodgment are forceful balloon dilation of the SEMS up to 8-10 mm after initial deployment, or the use of a coaxial double pig-tail through the SEMS, as reported for pseudocyst drainage using transmural SEMS (29). Operator confidence with specific devices also plays a role in the success of the method. Some authors feel that access without cautery is less prone to complications and for performing mechanical dilation, which requires a stiffer inch guidewire for support, subsequently use of a 19-gauge EUS-FNA needle. These authors use access with cautery, only selectively after failed mechanical dilation (7, 8). Other authors find the stiffer 19-gauge EUS-FNA needles to be cumbersome to use in the relatively long position of the echoendoscope in the duodenum, and resort to either Fig. 2. Endoscopic ultrasound (EUS)-guided choledochoduodenostomy. It is demonstrated step-by-step technique in which we can see EUS images with dilated common bile duct, puncture, cholangiography, guidewire placement, fistulization using needle-knife catheter, deployment of partially covered self-expandable metal stent. S79
7 Artifon et al. initial direct needle-knife access under EUS (30), or needleknife access under a thinner inch guidewire passed into the CBD after puncture with a 22-gauge EUS-FNA needle (31). Literature Findings Based on the Perspective of Evidence- Based Medicine EUS-guided choledochoduodenostomy was first reported by Giovannini et al. (32). As detailed earlier, the puncture needles available consist of conducting and nonconducting needles. About half of each kind of needle has been used in published reports. This is in contrary to what is reported for intrahepatic EUSBD, where nonconducting needle access is clearly preferred. In most reported cases, a plastic stent has been placed. However, the use of SEMS has increasingly been reported (7). The success rate for the 61 cases reported to date is as high as 95%, with excellent results in all successfully drained patients (100% per-protocol clinical response rate). There were some cases where stent insertion was too difficult and a nasobiliary drainage tube was placed instead (19, 33). Another interesting variation on EUS-CDS is illustrated by a few cases where the extrahepatic bile duct was punctured from the stomach rather than the standard transduodenal approach (7, 34). Although only 6 cases were reported, all were successful. Expected Complications and Treatment Options Complications can be divided into procedure-related complications and stent-related complications. Definitions of procedural complications are not well standardized. Most are related to bile or just air leakeage into the retroperitoneum by transduodenal access or the peritoneum by transgastric access to the CBD, with or without the added infection. The severity ranges from a selflimiting condition that resolves within hours with conservative measures, to full-blown peritonitis requiring emergency surgery; however, most reported complications are mild and the need for emergency surgery is exceedingly rare. Other interventional measures that may be required in the event of complications, such as percutaneous drainage, are however not all that uncommon. Peri-procedural leakage of bile into the abdominal cavity is most likely due to poor drainage. Poor drainage can be caused by factors such as too large a fistula, early stent clogging, and inappropriate positioning of the stent including foreshortening of SEMS. Late stent-related complications, since a mature fistula is formed, are similar to those seen with transpapillary stents placed at ERCP, namely, migration and stent occlusion. Stent migration or occlusion is managed as well the same way as in stents placed at ERCP, by inserting a new stent. The technique for repeat stent placement differs from what is commonly done at ERCP. If a clogged plastic stent is in place across the fistula, a guidewire is advanced through the stent and the stent is grasped with a snare passed overthe-wire and removed over it. This somewhat more complex maneuver is aimed at keeping guidewire access to the duct after stent removal. After plastic stent removal, a SEMS may be placed using a duodenoscope. If clogging of a SEMS occurs, the debris occluding its lumen may be cleaned up. However, just cleaning is probably not long-lasting in this setting. A new coaxial stent needs to be placed inside the clogged one, either a plastic stent, or a SEMS, the so-called stent-in-stent approach. Distal stent migration into the GI tract lumen with a mature fistula only involves repeat biliary drainage, since migrated stents usually pass out spontaneously. Repeat biliary drainage may be attempted in several ways, the simplest being placing a new stent through the same fistula, if it is still visible. If the fistula cannot be identified endoscopically, either repeat EUS-CDS through a new puncture site or PTBD are required. If proximal stent migration to the retroperitoneum or the peritoneum occurs, recovery of the stent as well as emergency surgery should be considered. This serious complication, however, has not yet been reported for EUS-CDS. Finally, even if the less serious distal migration occurs but the fistula is still immature (a fibrous track not yet formed), this may cause bile leakage into the abdomen. In the event of stent migration and leakage with an immature fistula, repeat EUS-guided biliary drainage (perhaps using a SEMS), or PTBD need to be considered. Surgery should also be considered depending on the patient s condition. COMMENTS Interventional EUS techniques for biliary drainage complement ERCP to achieve biliary access and drainage, but are invasive procedures that require careful patient selection and experienced operators backed by a multidisciplinary team. Further technical improvements are likely to reduce the number of adverse events and will probably contribute to S80
8 Endoscopic US-Guided Biliary Drainage the more widespread adoption of these procedures as a second-line approach to biliary drainage after failed ERCP. The readers also could appreciate a new EUS technology in which a forward view of ultrasound image is possible, and may facilitate the acquirement of an appropriate window to the therapeutic EUS (35). A short double face metal stent may be used to create a fistulisation between the dilated biliary tree and duodenum; this kind of stent is named an AXIOS Stent (X Lumena), and is also useful for treatment of pancreatic pseudocysts. Although multicenter trials aimed at standardizing the technique for performing EUS-guided biliary drainage would be desirable, the relatively few patient candidates for it and the wide spectrum of technical variations reported to date make this endeavor difficult to accomplish in the near future. Detailed prospective studies with homogeneous inclusion criteria and careful follow-up and dedicated hands-on training models will probably be more effective in advancing this burgeoning field of interventional endoscopy. REFERENCES 1. Fogel EL, Sherman S, Devereaux BM, Lehman GA. Therapeutic biliary endoscopy. Endoscopy 2001;33: Smith AC, Dowsett JF, Russell RC, Hatfield AR, Cotton PB. Randomised trial of endoscopic stenting versus surgical bypass in malignant low bileduct obstruction. Lancet 1994;344: Lai EC, Mok FP, Tan ES, Lo CM, Fan ST, You KT, et al. Endoscopic biliary drainage for severe acute cholangitis. N Engl J Med 1992;326: Wiersema MJ, Sandusky D, Carr R, Wiersema LM, Erdel WC, Frederick PK. Endosonography-guided cholangiopancreatography. Gastrointest Endosc 1996;43: Giovannini M. EUS-guided pancreatic pseudocyst drainage. Tech Gastrointest Endosc 2007;9: Bories E, Pesenti C, Caillol F, Lopes C, Giovannini M. Transgastric endoscopic ultrasonography-guided biliary drainage: results of a pilot study. Endoscopy 2007;39: Park do H, Koo JE, Oh J, Lee YH, Moon SH, Lee SS, et al. EUS-guided biliary drainage with one-step placement of a fully covered metal stent for malignant biliary obstruction: a prospective feasibility study. Am J Gastroenterol 2009;104: Perez-Miranda M, de la Serna C, Diez-Redondo P, Vila JJ. Endosonography-guided cholangiopancreatography as a salvage drainage procedure for obstructed biliary and pancreatic ducts. World J Gastrointest Endosc 2010;2: Wilson JA, Hoffman B, Hawes RH, Romagnuolo J. EUS in patients with surgically altered upper GI anatomy. Gastrointest Endosc 2010;72: Park do H, Song TJ, Eum J, Moon SH, Lee SS, Seo DW, et al. EUS-guided hepaticogastrostomy with a fully covered metal stent as the biliary diversion technique for an occluded biliary metal stent after a failed ERCP (with videos). Gastrointest Endosc 2010;71: Püspök A, Lomoschitz F, Dejaco C, Hejna M, Sautner T, Gangl A. Endoscopic ultrasound guided therapy of benign and malignant biliary obstruction: a case series. Am J Gastroenterol 2005;100: Fujita N, Noda Y, Kobayashi G, Ito K, Obana T, Horaguchi J, et al. Temporary endosonography-guided biliary drainage for transgastrointestinal deployment of a self-expandable metallic stent. J Gastroenterol 2008;43: Fujita N, Sugawara T, Noda Y, Kobayashi G, Ito K, Obana T, et al. Snare-over-the-wire technique for safe exchange of a stent following endosonography-guided biliary drainage. Dig Endosc 2009;21: Perez-Miranda M, De la Serna C, Diez-Redondo MP, Gomez de la Cuesta S, Gil-Simon P, Alcaide N, et al. Endosonographyguided cholangiopancreatography (ESCP) as the primary approach for ductal drainage after failed ERCP. Gastrointest Endosc 2010;71:AB Will U, Thieme A, Fueldner F, Gerlach R, Wanzar I, Meyer F. Treatment of biliary obstruction in selected patients by endoscopic ultrasonography (EUS)-guided transluminal biliary drainage. Endoscopy 2007;39: Burmester E, Niehaus J, Leineweber T, Huetteroth T. EUScholangio-drainage of the bile duct: report of 4 cases. Gastrointest Endosc 2003;57: Maranki J, Hernandez AJ, Arslan B, Jaffan AA, Angle JF, Shami VM, et al. Interventional endoscopic ultrasoundguided cholangiography: long-term experience of an emerging alternative to percutaneous transhepatic cholangiography. Endoscopy 2009;41: Eum J, Park do H, Ryu CH, Kim HJ, Lee SS, Seo DW, et al. EUS-guided biliary drainage with a fully covered metal stent as a novel route for natural orifice transluminal endoscopic biliary interventions: a pilot study (with videos). Gastrointest Endosc 2010;72: Horaguchi J, Fujita N, Noda Y, Kobayashi G, Ito K, Obana T, et al. Endosonography-guided biliary drainage in cases with difficult transpapillary endoscopic biliary drainage. Dig Endosc 2009;21: Giovannini M, Dotti M, Bories E, Moutardier V, Pesenti C, Danisi C, et al. Hepaticogastrostomy by echo-endoscopy as a palliative treatment in a patient with metastatic biliary obstruction. Endoscopy 2003;35: Artifon EL, Chaves DM, Ishioka S, Souza TF, Matuguma SE, Sakai P. Echoguided hepatico-gastrostomy: a case report. Clinics (Sao Paulo) 2007;62: Chopin-Laly X, Ponchon T, Guibal A, Adham M. Endoscopic biliogastric stenting: a salvage procedure. Surgery 2009;145:123 S81
9 Artifon et al. 23. Iglesias-García J, Lariño-Noia J, Seijo-Ríos S, Domínguez- Muñoz JE. Endoscopic ultrasound for cholangiocarcinoma reevaluation after Wallstent placement. Rev Esp Enferm Dig 2008;100: Martins FP, Rossini LG, Ferrari AP. Migration of a covered metallic stent following endoscopic ultrasound-guided hepaticogastrostomy: fatal complication. Endoscopy 2010;42 Suppl 2:E126-E Nguyen-Tang T, Binmoeller KF, Sanchez-Yague A, Shah JN. Endoscopic ultrasound (EUS)-guided transhepatic anterograde self-expandable metal stent (SEMS) placement across malignant biliary obstruction. Endoscopy 2010;42: Kim YS, Gupta K, Mallery S, Li R, Kinney T, Freeman ML. Endoscopic ultrasound rendezvous for bile duct access using a transduodenal approach: cumulative experience at a single center. A case series. Endoscopy 2010;42: Brauer BC, Chen YK, Fukami N, Shah RJ. Single-operator EUS-guided cholangiopancreatography for difficult pancreaticobiliary access (with video). Gastrointest Endosc 2009;70: Artifon EL, Okawa L, Takada J, Gupta K, Moura EG, Sakai P. EUS-guided choledochoantrostomy: an alternative for biliary drainage in unresectable pancreatic cancer with duodenal invasion. Gastrointest Endosc 2011;73: Talreja JP, Shami VM, Ku J, Morris TD, Ellen K, Kahaleh M. Transenteric drainage of pancreatic-fluid collections with fully covered self-expanding metallic stents (with video). Gastrointest Endosc 2008;68: Yamao K, Sawaki A, Takahashi K, Imaoka H, Ashida R, Mizuno N. EUS-guided choledochoduodenostomy for palliative biliary drainage in case of papillary obstruction: report of 2 cases. Gastrointest Endosc 2006;64: Tarantino I, Barresi L, Repici A, Traina M. EUS-guided biliary drainage: a case series. Endoscopy 2008;40: Giovannini M, Moutardier V, Pesenti C, Bories E, Lelong B, Delpero JR. Endoscopic ultrasound-guided bilioduodenal anastomosis: a new technique for biliary drainage. Endoscopy 2001;33: Itoi T, Itokawa F, Sofuni A, Kurihara T, Tsuchiya T, Ishii K, et al. Endoscopic ultrasound-guided choledochoduodenostomy in patients with failed endoscopic retrograde cholangiopancreatography. World J Gastroenterol 2008;14: Kahaleh M, Hernandez AJ, Tokar J, Adams RB, Shami VM, Yeaton P. Interventional EUS-guided cholangiography: evaluation of a technique in evolution. Gastrointest Endosc 2006;64: Kida M, Araki M, Miyazawa S, Ikeda H, Kikuchi H, Watanabe M, et al. Fine needle aspiration using forward-viewing endoscopic ultrasonography. Endoscopy 2011;43: S82
Review Article EUS-Guided Biliary Drainage
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Jintao Guo, Siyu Sun, Xiang Liu, Sheng Wang, Nan Ge, and Guoxin Wang. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
BILIARY CANNULATION FOR the treatment of biliary
 Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Gastrointestinal Intervention
 Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
Endoscopic ultrasound-guided anterograde cholangiopancreatography
 J Hepatobiliary Pancreat Sci (2011) 18:319 331 DOI 10.1007/s00534-010-0358-1 TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde
J Hepatobiliary Pancreat Sci (2011) 18:319 331 DOI 10.1007/s00534-010-0358-1 TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde
Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction
 CASE SERIES Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction Fauze Maluf-Filho, Felipe Alves Retes, Carla
CASE SERIES Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction Fauze Maluf-Filho, Felipe Alves Retes, Carla
Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable Metal Stent for Malignant Biliary Obstruction
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 6284094, 10 pages https://doi.org/10.1155/2017/6284094 Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 6284094, 10 pages https://doi.org/10.1155/2017/6284094 Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable
Endoscopic ultrasound guided biliary drainage: a comprehensive review
 Review Article Endoscopic ultrasound guided biliary drainage: a comprehensive review Avantika Mishra, Amy Tyberg Department of Gastroenterology, Rutgers Robert Wood Johnson University Hospital, New Brunswick,
Review Article Endoscopic ultrasound guided biliary drainage: a comprehensive review Avantika Mishra, Amy Tyberg Department of Gastroenterology, Rutgers Robert Wood Johnson University Hospital, New Brunswick,
Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A Literature Review
 Gastroenterology Research and Practice Volume 2013, Article ID 869214, 9 pages http://dx.doi.org/10.1155/2013/869214 Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A
Gastroenterology Research and Practice Volume 2013, Article ID 869214, 9 pages http://dx.doi.org/10.1155/2013/869214 Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A
International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches
 E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
CASO CLÍNICO. Los autores reportan el caso de una paciente derivada. Summary. Resumen
 CASO CLÍNICO Extrahepatic anterograde covered self-expandable metallic stent placement across malignant biliary obstruction passed by endoscopic ultrasound guidance access: a challenging technique Everson
CASO CLÍNICO Extrahepatic anterograde covered self-expandable metallic stent placement across malignant biliary obstruction passed by endoscopic ultrasound guidance access: a challenging technique Everson
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis
 Original article Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis Authors Theodore W. James, Todd H. Baron Institution
Original article Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis Authors Theodore W. James, Todd H. Baron Institution
ORIGINAL PAPERS. Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP
 ORIGINAL PAPERS Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Ana María Mora-Soler, Alberto Álvarez-Delgado, María Concepción Piñero-Pérez, Antonio Velasco-Guardado,
ORIGINAL PAPERS Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Ana María Mora-Soler, Alberto Álvarez-Delgado, María Concepción Piñero-Pérez, Antonio Velasco-Guardado,
Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or
 Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Authors: Ana María Mora Soler, Alberto Álvarez Delgado, María Concepción Piñero Pérez, Antonio Velasco-Guardado,
Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Authors: Ana María Mora Soler, Alberto Álvarez Delgado, María Concepción Piñero Pérez, Antonio Velasco-Guardado,
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Endoscopic ultrasound guided gastrojejunostomy
 Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study
 609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Endoscopic Ultrasound-Guided Pancreatobiliary Endoscopy in Surgically Altered Anatomy
 FOCUSED REVIEW SERIES: Pancreatobiliary endoscopy in altered gastointestinal anatomy Clin Endosc 2016;49:515-529 https://doi.org/10.5946/ce.2016.144 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access
FOCUSED REVIEW SERIES: Pancreatobiliary endoscopy in altered gastointestinal anatomy Clin Endosc 2016;49:515-529 https://doi.org/10.5946/ce.2016.144 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access
efficacy. Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience
 E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction
 Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
EUS Guided Pancreatic Duct Drainage: When? How?
 PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Biliary Metal Stents MAKING A DIFFERENCE TO HEALTH
 Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy
 Review Article A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy Rucha Mehta Shah, Paul Tarnasky, Prashant Kedia
Review Article A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy Rucha Mehta Shah, Paul Tarnasky, Prashant Kedia
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
6/17/2016. ERCP in June 26, Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates
 ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm
 Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Advanced Cannulation Techniques
 Advanced Cannulation Techniques Priya A. Jamidar, M.D., FASGE Professor of Medicine, Director of Endoscopy Yale School Disclosures Consultant to Boston Scientific and Olympus America Cannulation at ERCP
Advanced Cannulation Techniques Priya A. Jamidar, M.D., FASGE Professor of Medicine, Director of Endoscopy Yale School Disclosures Consultant to Boston Scientific and Olympus America Cannulation at ERCP
Original Policy Date 12:2013
 MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
MP 6.01.30 Magnetic Resonance Cholangiopancreatography Medical Policy Section Radiology Is12:2013sue 3:2005 Original Policy Date 12:2013 Last Review Status/Date 12:2013 Return to Medical Policy Index Disclaimer
Urgent endoscopic ultrasound-guided choledochoduodenostomy for acute obstructive suppurative cholangitis-induced sepsis
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v22.i16.4264 World J Gastroenterol 2016 April 28; 22(16): 4264-4269 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v22.i16.4264 World J Gastroenterol 2016 April 28; 22(16): 4264-4269 ISSN 1007-9327
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Gastrointestinal Intervention
 Gastrointest Interv 2016;5:203 211 Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided biliary drainage Majid A. Almadi, 1 Nonthalee Pausawasdi,
Gastrointest Interv 2016;5:203 211 Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided biliary drainage Majid A. Almadi, 1 Nonthalee Pausawasdi,
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures
 E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Approach to the Biliary Stricture
 Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Index. Springer Nature Singapore Pte Ltd K.-H. Lai et al. (eds.), Biliopancreatic Endoscopy,
 A Acute cholangitis biliary endoprosthesis, 70 intraductal ultrasonography, 243 Acute cholecystitis, 33, 143, 226 Acute intracystic hemorrhage, EUS-FNA, 241 Acute pancreatitis EUS-FNA, 240 intraductal
A Acute cholangitis biliary endoprosthesis, 70 intraductal ultrasonography, 243 Acute cholecystitis, 33, 143, 226 Acute intracystic hemorrhage, EUS-FNA, 241 Acute pancreatitis EUS-FNA, 240 intraductal
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Gastric / EUS Metal Stents
 Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
ERCP in altered anatomy. Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway
 ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents
 REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Maximize Control. Minimize Migration.
 Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Endoscopic ultrasound guided biliary and pancreatic duct interventions
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v6.i11.513 World J Gastrointest Endosc 2014 November 16; 6(11): 513524 ISSN 19485190
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v6.i11.513 World J Gastrointest Endosc 2014 November 16; 6(11): 513524 ISSN 19485190
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
7/11/2017. We re gonna help a lot of people today. Biliary/Pancreatic Endoscopy. AGS July 1-2, Kenneth M. Sigman, MD
 Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Interventional EUS for the Diagnosis and Treatment of Locally Advanced Pancreatic Cancer
 REVIEW Interventional EUS for the Diagnosis and Treatment of Locally Advanced Pancreatic Cancer Mohammad Al-Haddad 1,2, Mohamad A Eloubeidi 3 1 Division of Gastroenterology and Hepatology, Department of
REVIEW Interventional EUS for the Diagnosis and Treatment of Locally Advanced Pancreatic Cancer Mohammad Al-Haddad 1,2, Mohamad A Eloubeidi 3 1 Division of Gastroenterology and Hepatology, Department of
Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal Stent for Acute Cholecystitis: A Systematic Review
 REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage?
 EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Afferent Loop Syndrome: Treatment by Means of the Placement of Dual Stents
 Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
CURRICULUM VITAE
 CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
and Transmural Drainage
 HPB Surgery, 2000, Vol. 11, pp. 333-338 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
HPB Surgery, 2000, Vol. 11, pp. 333-338 Reprints available directly from the publisher Photocopying permitted by license only (C) 2000 OPA (Overseas Publishers Association) N.V. Published by license under
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
ORIGINAL PAPERS. R. Insertion of fully covered self-expanding metal stents in benign biliary diseases. ABSTRACT MATERIALS AND METHODS INTRODUCTION
 ORIGINAL PAPERS Insertion of fully covered self-expanding metal stents in benign biliary diseases Mariana Omodeo, Ignacio Málaga, Dante Manazzoni, Cecilia Curvale, Julio de María, Martín Guidi and Raúl
ORIGINAL PAPERS Insertion of fully covered self-expanding metal stents in benign biliary diseases Mariana Omodeo, Ignacio Málaga, Dante Manazzoni, Cecilia Curvale, Julio de María, Martín Guidi and Raúl
MAKING CONNECTIONS. Los Angeles Medical Center
 MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
CPT 2014 Overview of GI Changes
 CPT 2014 Overview of GI Changes The following table is a listing of the new,, and deleted codes in the Esophagus/Endoscopy section effective January 1, 2014. The table lists the CPT code, a brief description
CPT 2014 Overview of GI Changes The following table is a listing of the new,, and deleted codes in the Esophagus/Endoscopy section effective January 1, 2014. The table lists the CPT code, a brief description
Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance for Extraluminal Complicated Cysts
 Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Title: Insertion of fully covered self-expanding. metal stents in benign biliary diseases. Rev
 Title: Insertion of fully covered self-expanding metal stents in benign biliary diseases Authors: Mariana Omodeo, Ignacio Malaga, Dante Manazzoni, Cecilia Curvale, Julio de Maria, Martín Alejandro Guidi,
Title: Insertion of fully covered self-expanding metal stents in benign biliary diseases Authors: Mariana Omodeo, Ignacio Malaga, Dante Manazzoni, Cecilia Curvale, Julio de Maria, Martín Alejandro Guidi,
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Usefulness of Forward-Viewing Endoscope for Endoscopic Retrograde Cholangiopancreatography in Patients with Billroth II Gastrectomy
 ORIGINAL ARTICLE Clin Endosc 2012;45:397-403 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2012.45.4.397 Open Access Usefulness of Forward-Viewing Endoscope for Endoscopic
ORIGINAL ARTICLE Clin Endosc 2012;45:397-403 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2012.45.4.397 Open Access Usefulness of Forward-Viewing Endoscope for Endoscopic
AXIOS Stent and Delivery System
 PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the Elderly and Unwell
 Cardiovasc Intervent Radiol (2015) 38:964 970 DOI 10.1007/s00270-014-1014-y CLINICAL INVESTIGATION NON-VASCULAR INTERVENTIONS Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the
Cardiovasc Intervent Radiol (2015) 38:964 970 DOI 10.1007/s00270-014-1014-y CLINICAL INVESTIGATION NON-VASCULAR INTERVENTIONS Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
ORIGINAL ARTICLE: Clinical Endoscopy
 ORIGINAL ARTICLE: Clinical Endoscopy Anchoring flap versus flared end, fully covered self-expandable metal stents to prevent migration in patients with benign biliary strictures: a multicenter, prospective,
ORIGINAL ARTICLE: Clinical Endoscopy Anchoring flap versus flared end, fully covered self-expandable metal stents to prevent migration in patients with benign biliary strictures: a multicenter, prospective,
Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline
 Guideline 277 Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline Authors J.-M. Dumonceau 1, A. Tringali 2, D. Blero 3,
Guideline 277 Biliary stenting: Indications, choice of stents and results: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline Authors J.-M. Dumonceau 1, A. Tringali 2, D. Blero 3,
Evaluation and Management of Refractory Biliary Stricture. J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc.
 Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
Evaluation and Management of Refractory Biliary Stricture J. David Horwhat, MD, FACG Director of Endoscopy Lancaster Gastroenterology, Inc Outline What defines a refractory biliary stricture Endoscopic
AXIOS Stent and Electrocautery Enhanced Delivery System. Quick Reference Guide
 AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
