Endoscopic ultrasound-guided anterograde cholangiopancreatography
|
|
|
- Elizabeth Skinner
- 5 years ago
- Views:
Transcription
1 J Hepatobiliary Pancreat Sci (2011) 18: DOI /s TOPICS Advances in therapeutic ultrasound and endoscopy in hepato-biliary-pancreatic diseases Endoscopic ultrasound-guided anterograde cholangiopancreatography Kenneth F. Binmoeller Thai Nguyen-Tang Published online: 29 December 2010 Ó Japanese Society of Hepato-Biliary-Pancreatic Surgery and Springer 2010 Abstract Endoscopic retrograde cholangiopancreatography (ERCP) may fail in 10 15% of cases. A growing percentage of such cases are due to the inaccessible papilla after gastric bypass surgery for the treatment of obesity. Endoscopic ultrasonography (EUS) offers an alternative route of access to the bile and pancreatic ducts. Using the curved linear array echoendoscope, access to the bile and pancreatic ducts is possible under real-time EUS guidance. The route of access is anterograde, in contrast to the retrograde approach of ERCP. We have coined the term EUS-guided anterograde cholangiopancreatography (EACP) to cover the spectrum of EUS-guided techniques for accessing and draining the bile and pancreatic ducts. These techniques are reviewed in this paper. The literature has validated the feasibility of EACP but complication rates have been high; the safety profile of EACP must improve. This will require tools, designed for EUS-guided applications, that enable safer transenteric access and drainage. Keywords EUS-guided biliopancreatic therapy Endosonography-guided biliary and pancreatic drainage Anterograde biliary and pancreatic drainage Introduction Endoscopic retrograde cholangiopancreatography (ERCP) is the preferred way to drain an obstructed bile or K. F. Binmoeller (&) T. Nguyen-Tang Interventional Endoscopy Services, California Pacific Medical Center, San Francisco, CA, USA BinmoeK@sutterhealth.org pancreatic duct [1]. However, in 10 15% of cases, transpapillary drainage may not be feasible or may fail (Table 1). A growing percentage of these cases is due to the inaccessibility of the papilla after gastric bypass surgery to treatm obesity. When transpapillary drainage is not an option or fails, patients are usually referred for percutaneous drainage (for biliary obstruction) or surgical bypass (for biliary and pancreatic obstruction). These approaches carry significantly higher morbidity and mortality rates compared with ERCP and transpapillary drainage [2, 3]. Endoscopic ultrasonography (EUS) offers an alternative route of access to the bile and pancreatic ducts. Using the curved linear array (CLA) echoendoscope, access to the bile and pancreatic ducts is possible under real-time EUS guidance [4]. The route of access is anterograde, in contrast to the retrograde approach of ERCP. We have coined the term EUS-guided anterograde cholangiopancreatography (EACP) to cover the spectrum of EUSguided techniques for accessing and draining the bile and pancreatic ducts (Table 2). These techniques will be reviewed, including their indications, available data on efficacy and outcomes, and limitations. Procedure preparation and equipment Consent In our department, patients referred for therapeutic ERCP give consent for both ERCP and EACP, as it is impossible to predict when ERCP might fail and EACP will be required. Patients with known difficult anatomy (altered anatomy, gastric outlet obstruction) or prior failed ductal access are more likely to require EACP. EACP is performed in the same procedural session as ERCP by the
2 320 J Hepatobiliary Pancreat Sci (2011) 18: Table 1 Causes of failed retrograde access to the bile and pancreatic ducts Failed ductal cannulation Unidentifiable papilla Tumor infiltration of the papilla Juxtapapillary diverticulum High-grade stricture Difficult anatomy Inability to reach the papilla (or ductal anastomosis) Gastric outlet obstruction High-grade duodenal stenosis Post-peptic changes Post-surgical anatomy Gastrectomy Gastric bypass Whipple Hepaticojejunostomy Billroth II Table 2 Classification of EUS-guided pancreatobiliary interventions 1. Anterograde-retrograde access and downstream drainage (EUS-guided rendezvous procedure) 2. Anterograde access and upstream drainage EUS-guided hepaticogastrostomy EUS-guided choledochoduodenostomy EUS-guided pancreaticogastrostomy EUS-guided pancreaticoduodenostomy 3. Anterograde access and downstream drainage EUS-guided anterograde transpapillary stent placement EUS-guided anterograde transanastomotic stent placement same operator, thus avoiding the delay and expense of a second procedure (and sedation) session. Antibiotic coverage We routinely give antibiotics (ciprofloxacin or a third generation cephalosporin) prior to EACP. The rationale is to minimize the risk of peritonitis from leakage of ductal or enteric contents at the transmural puncture site. Oral antibiotics are continued for a minimum of 3 days after the procedure. Echoendoscope CLA echoendoscopes are commercially available with two channel sizes: small (standard) and large (therapeutic). The channel size determines the upper limit of the stent size that can be placed. The therapeutic CLA echoendoscope with a channel of 3.7 or 3.8 mm enables passage of a 10 Fr stent. A standard CLA echoendoscope with channel size of 2.8 mm allows passage of a 7 Fr stent. In our unit we use the therapeutic CLA echoendoscope for all EACP interventions to keep all options open. Although a therapeutic CLA echoendoscope is not required for a rendezvous procedure (the echoendoscope is exchanged for a duodenoscope for stent placement), the guidewire may fail to cross the stricture and/or ampulla, in which case rescue upstream transenteric stent drainage, performed through the echoendoscope, will be required. Ductal access A conventional FNA needle can be used to access the bile or pancreatic duct. The choice of FNA needle size depends on the clinical context, the goal of the procedure, and the ductal anatomy. Our default needle size is 19 gauge, through which a inch, 400-cm long wire can be inserted. The drawback of the 19 gauge needle is its relative stiffness, which results in a very tangential angle of puncture. The elevator, when activated, has virtually no effect on the puncture angle. It is also difficult to penetrate indurated tissue with the 19 gauge needle. We rarely use the 22 gauge needle, as it only accepts a inch guidewire. This wire is inadequate for EUS-guided intervention because it: (1) is hard to see on fluoroscopy; (2) is hard to steer; and (3) lacks the stability and trackability required for over-the-wire intervention. The only instance where a 22 gauge needle may be required is when targeting of a nondilated duct (e.g., intrahepatic or pancreatic) with the 19 gauge fails. The inch wire will need to be exchanged for a inch wire through a catheter. A 25 gauge needle does not accept a wire but it might be considered when the goal is a diagnostic cholangiogram or pancreatogram in a patient with a coagulation disorder or low platelet count. An alternative to using the FNA needle to achieve ductal access is the diathermic needle knife with removable inner needle (Zimmon needle knife, Cook Medical). Pure cutting current is applied during puncture to penetrate tissue. The advantage of using the needle knife is the ability to immediately exchange the inner needle for a guidewire. The outer catheter can then be easily steered in the duct, off-axis from the angle that the duct was punctured. A drawback of the needle knife is the limited visibility of the needle at the catheter tip, both on ultrasound and fluoroscopy. Another drawback is the risk of diathermy trauma to tissue, which is a particular concern should the needle veer off course during puncture. Whereas a continuous stainless steel needle will maintain the predicted trajectory path as it is advanced, the more flexible needle knife catheter may veer off-axis into a neighboring structure, which may be a major vessel.
3 J Hepatobiliary Pancreat Sci (2011) 18: Guidewires The guidewires used in EACP are the same as those used in ERCP. We routinely start with the inch hydrophilic Glidewire inserted through a 19 gauge needle. As in ERCP, the hydrophilic Glidewire has excellent steerability to negotiate tortuous ducts and high-grade strictures. The low coefficient of friction, however, is a drawback for over-thewire exchange of accessories. During the rendezvous procedure, extreme care must be taken that the Glidewire does not slip back during the withdrawal of the echoendoscope and insertion of the duodenoscope. One can exchange the Glidewire through a standard ERCP catheter for a stiffer instrumentation wire, but this requires advancement of the catheter across the bowel lumen and obstruction. A 22 gauge needle will only accept a inch guidewire. As mentioned above, the inch guidewires lack the stability and trackability required for over-the-wire intervention. In the United States, the hydrophilic Glidewire is only available in a inch size, which creates too much friction between the wire and needle. Even if the inch size were available, the Glidewire is barely visible on fluoroscopy at this size and therefore not likely to be useful. Tract dilation Dilation is required prior to stenting. As in ERCP, graduated bougies and non-compliant balloon catheters can be used. Each has pros and cons. Bougies have the advantage of excellent operator control of the dilation force, as the operator can gauge the amount of resistance encountered during advancement of the bougie, However, the dilation force is axial, which can lead to a separation of tissue planes during bougie advancement. Balloons have the advantage that they can be inserted in a compressed state, thereby minimizing the delivery catheter size to around 5 Fr. Upon balloon inflation, the dilation force is radial. However, balloons dilate to a fixed diameter in an all-or-nothing fashion which increases the risks of perforation and bleeding. It is noted that the size of the bougie or balloon should not substantially exceed the size of the stent to be inserted in order to minimize the risk of transmural leakage of ductal and enteric contents. This is a consideration when deciding whether to dilate with a bougie or balloon, as the smallest dilation balloon size is 4 mm (12 Fr). Occasionally, passage of a balloon or bougie across the bowel wall after guidewire access may fail. If this happens, a smaller profile catheter, such as a finely tapered ERCP catheter, can be used to prime the tract for dilation. If this fails, penetration can be facilitated with diathermy using a double lumen needle knife catheter. Alternatively, a catheter with a diathermic ring at the tip can be used. Endoscopists in Europe have used a 6.5 Fr diathermic ring device (Endoflex, Voerde, Germany) with good results. Currently, only a 10 Fr diathermic ring device (Cystotome CST10; Cook Medical) is approved for use in the United States. The Cystotome was designed for endoscopic transmural puncture of large pseudocysts and has been successfully used for this indication, but there is no reported experience for puncture of the bile or pancreatic ducts. The Cystotome is a rigid device that is difficult to advance across the oblique exit of the working channel of the therapeutic CLA echoendoscope. Stents The choice of stent type, size and length depends on the ductal anatomy. Again, as in ERCP, straight and pigtail plastic stents and self-expandable metal stents (SEMS) can be used. Pigtail stents are a logical choice to minimize the risk of stent migration (especially into the duct), but the pigtail end makes stent insertion more difficult owing to a weakened coaxial transfer of force. We therefore prefer to use straight stents for transenteric drainage. We have not found migration to be a problem when the flaps are deployed properly. A further advantage of a straight stent is the ability to retrieve or exchange the stent over the wire without loss of ductal access. Covered SEMS have been used for transenteric drainage, but may migrate, particularly with shortening [5]. The covering may block drainage of a secondary duct (e.g., cystic duct or intrahepatic branch). Uncovered SEMS are generally unsuited for transenteric drainage due to leakage between the struts. Uncovered SEMS can be placed in exchange for a temporary plastic stent after the fistula tract has matured (Fig. 2f). We always use SEMS when a malignant stricture can be traversed and drained downstream. This is justified since plastic stent clogging is likely to require a repeat EACP procedure. EUS-guided puncture It is helpful to fluoroscopically assess the position of the echoendoscope before puncturing the duct. The exit path of the needle should be oriented towards the downstream portion of the duct. To access the left hepatic bile duct, the scope is positioned in the proximal stomach along the lesser curve. To access the proximal and distal extrahepatic bile ducts, the scope is positioned in the mid-stomach and duodenal bulb, respectively. In the duodenal bulb, it may be necessary to shift from a long to a short position; in the long position the needle tends to orient towards the upstream bifurcation, whereas in the short position the needle orients towards the downstream ampulla. A trade-off of the short position is that it can be unstable, with a tendency for the echoendoscope to fall back into the stomach. Transhepatic access is generally preferrable to extrahepatic access due to the protection afforded by the liver
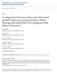
4 322 J Hepatobiliary Pancreat Sci (2011) 18: Fig. 1 EUS-guided rendezvous. Presentation with jaundice. Upper endoscopy showed a large fungating ampullary tumor. Biopsies confirmed adenocarcinoma. ERCP was attempted, but failed to access the bile duct. a Under EUS-guidance a dilated left intrahepatic duct is punctured with a 19 gauge FNA needle (arrow). b After aspiration of bile, contrast is injected under fluoroscopy. A distal bile duct stricture is seen (arrow). c A inch hydrophilic guidewire is advanced across the stricture and looped in the duodenal lumen. d After exchange of the echoendoscope for a duodenoscope, the guidewire is seen exiting the ampullary tumor. e The guidewire is grasped with a snare and pulled through the channel of the duodenoscope. f A 10-Fr biliary plastic stent is successfully placed over the wire parenchyma against complications of a bile leak (as is well known from percutaneous transhepatic access). The extrahepatic route has the advantage of easier, more direct access. It is usually easier to access the extrahepatic bile duct from the duodenal bulb. The bile duct runs along the duodenal wall as it emerges from the pancreatic head (this is also the location used by surgeons to create a choledochoduodenostomy). The portal vein is usually deep to the bile duct and therefore not in the needle path. The pancreatic duct can be punctured at virtually any point along its length from the stomach to the duodenal bulb. It is easiest to access the junction of the neck to body region from the stomach. The initial puncture point should not be too close to the stricture in order to have some distance to steer the guidewire through the stricture. Analogous to transhepatic drainage, the pancreatic parenchyma surrounding the pancreatic duct is thought to protect against complications of a possible leak from the pancreatic duct.
5 J Hepatobiliary Pancreat Sci (2011) 18: Anterograde-retrograde access and downstream drainage (rendez-vous procedure) The rendezvous procedure is derived from the percutaneous technique whereby a guidewire is passed anterogradely across the stricture and papilla (or surgical anastomosis) for subsequent rendezvous retrograde drainage by ERCP [6]. Percutaneous access under fluoroscopic guidance is substituted for transgastric or transduodenal access under EUS-guidance. This procedure minimizes the role of interventional EUS and should be considered an advanced cannulation technique for ERCP (Fig. 1). Procedure 1. At the time of initial endoscopy, a clip is placed adjacent to the papilla to mark its location. 2. For bile duct access, we first attempt a transhepatic approach from the stomach with a 19 gauge FNA needle. The stomach provides an excellent window to image and access the left hepatic ducts. The surrounding hepatic parenchyma acts as a sponge to absorb and minimize bile leakage. If transhepatic access fails, we puncture the extrahepatic bile duct from the duodenum or stomach using a 22 gauge FNA needle. 3. Bile or pancreatic juice is aspirated to confirm access. 4. Contrast medium is injected to obtain a ductogram, delineate the ductal anatomy, and show relevant pathology. 5. Fluoroscopic guidance is used for anterograde passage of a guidewire through the FNA needle across the stricture and across the papilla, identified by the previously placed clip. The guidewire is advanced to form 2 3 loops in the duodenal lumen. 6. The FNA needle is removed while leaving the wire in place. The elevator is closed to help anchor the position of the wire. 7. The echoendoscope is removed over the wire under fluoroscopic monitoring taking care that the wire remains looped in the duodenum. 8. The esophagus is intubated with the duodenoscope alongside the wire. The duodenoscope is advanced to the papilla where the wire exiting the papillary orifice is grasped with a snare and pulled through the accessory channel. 9. The wire is retracted until it clears the site of transmural puncture and lies completely within the duct. Standard ERCP intervention and stenting is performed over the wire. The duct should be adequately decompressed to minimize the risk of bile leakage at the transmural puncture site. 10. In patients with post-surgical anatomy (Billroth II or Roux-en-Y) a colonoscope or enteroscope may be used to complete the ERCP procedure. Available data About a hundred cases of successful EUS-guided rendezvous procedures performed for pancreatobiliary obstructions have been reported in the literature (Table 3). Success rates vary between 35 and 78% in the largest cases series. EUS-guided puncture of the duct and ductography are accomplished in most cases. Failure is mainly due to inability to steer a guidewire across the stricture. A rescue upstream transenteric drainage is then performed to drain the obstructed duct. When combining attempted EUS-guided rendezvous and upstream drainage in cases of failure, the overall drainage success rate is 87%. The reported complication rates are 12 17% and include bile leaks, self-resolving pneumoperitoneum, subcapsular hematoma and post-procedure pancreatitis. Limitations and challenges The rendezvous procedure is limited by two requirements: (1) an endoscopically accessible papilla (or bilio-enteric anastomosis); and (2) successful passage of the guidewire across the stricture into the downstream small bowel. Accessing the bile duct with a wire is easy, but manipulating the wire within the duct and across the stricture can be difficult when the axis of the needle and the downstream bile duct lumen are not aligned. The wire tends to catch at the needle tip during to-and-fro manipulation, and may even shear off with forceful wire retraction. Bile, which is viscous and sticky, contributes to friction between the wire and needle. As the rendezvous procedure requires an exchange of the echoendoscope for a duodenoscope, it is easy to lose wire access during the exchange. Keeping the wire looped several times in the duodenal or jejunal lumen will help anchor the wire s position. The process of pulling the wire through the working channel of the duodenoscope requires patience; if the snare catheter is pulled too forcefully, the wire will slip through the closed snare. The wire can also exert traumatic shearing forces along the bile duct and liver. Anterograde access and upstream transenteric drainage Ductal access is similar to that of EUS-guided rendezvous, upstream transenteric drainage is performed when the stricture cannot be traversed with a wire or when the papilla or surgical anastomosis cannot not be reached with an
6 324 J Hepatobiliary Pancreat Sci (2011) 18: Table 3 Studies evaluating EUS-guided rendezvous and anterograde drainage No. of cases Biliary/pancreatic drainage Successful rendezvous biliary/pancreatic Successful drainage biliary/pancreatic Complications related to the procedure Bataille et al. [12] 1 0/1 0/1 (100%) 0/1 (100%) None Mallery et al. [13] 6 2/4 2/1 (50%) 2/1 (50%) Transient fever (1) Kahaleh et al. [14] 5 5/0 3/0 (60%) 4/0 (80%) None Will et al. [15] 1 0/1 0/1 (100%) 0/1 (100%) None Kahaleh et al. [16] 6 6/0 4/0 (67%) 5/0 (83%) None Kahaleh et al. [17] 23 23/0 18/0 (78%) 21/23 (91%) Bleeding (1) Bile leak (1) Pneumoperitoneum (2) Tarantino et al. [18] 9 9/0 4/0 (44%) 9/0 (100%) None Brauer et al. [19] 20 12/8 4/3 (35%) 11/7 (90%) None Maranki et al. [20] 49 49/0 32/0 (65%) 41/0 (84%) Bleeding (1) Bile leak (1) Pneumoperitoneum (4) Our data [21, 22] 54 43/11 24/4 (71%) 31/9 (74%) Pancreatitis (4) Subcapsular hematoma (1) Bile leak (1) endoscope. For biliary drainage, the transhepatic route (hepaticogastrostomy, Fig. 2) is preferred due to a lower risk of bile leak complications. There are theoretical advantages to creating a fistula that is upstream from the obstructing stricture: the stent is not subject to tumor ingrowth or overgrowth, and there should be a lower propensity to clogging (Figs. 2, 4). Procedure technique 1. The obstructed duct is punctured under EUS-guidance with a 19 gauge needle. 2. Bile or pancreatic juice is aspirated to confirm access. 3. Contrast is injected to obtain a ductogram and delineate the ductal anatomy. 4. Fluoroscopic guidance is used for anterograde advancement of a stiff inch guidewire. 5. The needle is removed with the wire left in place. 6. The tract is dilated with bougies up to the size of the stent to be inserted. If transmural advancement of the bougie fails, a double lumen needle knife is used to apply diathermy during advancement of the catheter. 7. A straight plastic stent is placed over the wire. The plastic stent can be exchanged for an SEMS at a later session after the tract matures. Available data The available data on EUS-guided hepatico-gastrostomy is summarized in Table 4. Only 22 cases have been reported in the literature with a high rate of technical success exceeding 90%. The overall complication rate is 22% and includes cholangitis, bilioma, ileus and stent occlusion. Both plastic and metal stents have been used for transenteric drainage. Bories et al. [5] reported two cases of peritoneal leak caused by shortening of the metal stent after deployment. The available data on EUS-guided choledochoduodenostomy is summarized in Table 5. Thirty-four cases have been reported and the overall success rate of the procedure is high (89%) but a high complication rate (21%) is also noted. The reported complications include 5 pneumoperitoneums (15%) and 2 bile leaks (6%). In the majority of cases plastic stents were used to drain the common bile duct into duodenum. The available data on EUS-guided pancreaticoenterostomy is addressed below. Limitations and challenges The main limitation of transhepatic drainage is the lack of adherence between the stomach and the liver. A shift in the liver s position relative to the stomach wall may cause the stent to dislocate, resulting in a bile leak into the peritoneal space. The lack of adherence also increases the risk of bleeding from the liver surface. Similarly, the main drawback of a choledocho-enterostomy is the absence of adherence between the bile duct and the bowel wall. As seen from the literature, there is a very high risk of bile leak
7 J Hepatobiliary Pancreat Sci (2011) 18: Fig. 2 EUS-guided hepaticogastrostomy. Presentation with painless jaundice. Abdominal CT showed a hypodense mass in the head of the pancreas. EUS fine needle aspiration confirmed a locally advanced adenocarcinoma. ERCP was attempted but failed to access the duct because of a duodenal stricture with severe periampullary inflammation. a Transhepatic puncture of a dilated left hepatic duct with a 19G FNA needle (arrow). b Cholangiogram shows complete obstruction at the distal bile duct stricture (arrow). Despite numerous manipulations, the inch hydrophilic guidewire could not be passed across the stricture (arrow). A previously placed clip marking the location of the ampulla is seen (arrow). c The tract is dilated with a bougie (arrow). d A 8.5-Fr hepaticogastric stent is successfully placed. e The position of the stent (arrow) is confirmed on fluoroscopy and shows that the retained contrast has drained. f Six weeks later the plastic stent is exchanged for an 8 mm x 6 cm uncoated selfexpandable metal stent (Wallflex, Boston Scientific) and pneumoperitoneum. Compounding this, intraductal pressures are higher in the extrahepatic bile duct than in the intrahepatic duct. Post-surgery anatomy can pose obvious limitations for transenteric drainage. Left hepatectomy eliminates transhepatic access, prior gastrojejunostomy or biliary bypass surgery (hepaticojejunostomy) eliminates extrahepatic access. There is limited experience regarding the management of an occluded stent. If a mature tract has formed, stent replacement may not be required. However, it is unknown how long it takes for a mature tract to form, or whether an unstented tract will close over time. For long-term stenting, our preference is to exchange a straight plastic stent over the wire for an SEMS. Larger series with longer follow-up are needed to determine the optimal drainage strategy using plastic and metal stents. Anterograde access and downstream drainage EUS-guided anterograde biliary SEMS placement This procedure is derived from percutaneous internal stent drainage performed by interventional radiologists [8, 9]. The prerequisite for EUS-guided anterograde
8 326 J Hepatobiliary Pancreat Sci (2011) 18: Table 4 Studies evaluating EUS-guided hepaticogastric drainage No. of cases Puncture and dilation devices Stent placed Technical success (%) Clinical success (%) Complications related to the procedure Burmester et al. [23] 1 Fistulotome Plastic None Giovaninni et al. [24] 1 19 gauge needle Plastic None Needle knife Kahaleh et al. [17] 1 19 or 22 gauge needle Plastic None Artifon et al. [25] 1 19 gauge needle SEMS None Will et al. [26] 4 19 gauge needle SEMS Cholangitis (1) 6 Fr bougie and 4- or 6-mm balloon Bories et al. [5] or 22 gauge needle 6 or 8.5 Fr cystotome Plastic (7) SEMS (3) Ileus (1) Stent occlusion (1) Bilioma (1) Cholangitis (1) Maranki et al. [20] 3 19 or 22 gauge needle Plastic Not available Table 5 Studies evaluating EUS-guided choledochoduodenal drainage No. of cases Puncture and dilation devices Stent placed Technical success (%) Clinical success (%) Complications related to the procedure Giovannini et al. [27] 1 Needle knife Plastic None Dilating catheter Burmester et al. [23] 2 Fistulotome Plastic Bile peritonitis (1) Puspok et al. [11] 5 Needle knife Plastic None Kahaleh et al. [17] 1 19 gauge needle SEMS Pneumoperitoneum (1) Fujita et al. [28] 1 19 gauge needle Plastic None Dilating catheter Ang et al. [29] 2 Needle knife Plastic Pneumoperitoneum (1) Dilating catheter Yamao et al. [30] 5 Needle knife Plastic Pneumoperitoneum (1) Dilating catheter Tarantino et al. [18] 4 19 gauge or 22 gauge needle Plastic None Balloon dilation Itoi et al. [31] 4 19 gauge needle or Needle knife Plastic Bile peritonitis (1) Dilating catheter or Balloon dilation Maranki et al. [20] 4 19 gauge needle NA NA NA NA Dilating catheter or Balloon dilation Brauer et al. [19] 3 19 gauge or 22 gauge needle Plastic Pneumoperitoneum (1) Our data [21] 2 Needle knife SEMS Pneumoperitoneum (1) NA Not available biliary SEMS placement is the successful traversement of the stricture with a guidewire. Cases have been reported in patients with malignant strictures and an endoscopically inaccessible papilla or bilioenteric anastomosis (Fig. 3). Procedure technique 1. EUS-guidance is used to puncture the obstructed duct with a 19 gauge needle. 2. Bile is aspirated to confirm biliary access.
9 J Hepatobiliary Pancreat Sci (2011) 18: Fig. 3 EUS-guided anterograde SEMS placement. Presentation with jaundice, post right hepatectomy and Roux-en-Y hepaticojejunostomy for cholangiocarcinoma. The hepaticojejunostomy could not be reached with the double balloon enteroscope. a CT showing liver metastases and dilated ducts in the residual left lobe. b Cholangiogram after EUS-guided puncture of the left intrahepatic ducts. A inch hydrophilic guidewire is advanced across the strictured hepaticojejunostomy into the jejunal loop (arrow). c The tract is dilated with a bougie catheter (arrow). d A10mm9 6cm metal stent is deployed anterograde across the stricture (arrow) 3. Contrast is injected to obtain a ductogram and delineate the ductal anatomy. 4. Fluoroscopic guidance is used for anterograde advancement of a inch hydrophilic guidewire across the stricture. 5. The 19 gauge needle is removed with the wire left in place. 6. The tract is dilated with a 7 Fr bougie catheter. 7. The hydrophilic guidewire is exchanged for a inch instrumentation wire through the bougie catheter. 8. A biliary SEMS is advanced over the guidewire with deployment across the stricture and downstream papilla or anastomosis. Available data We recently reported a series of 5 patients who underwent anterograde biliary SEMS placement because of a nontraversable high-grade duodenal stricture (n = 4) and an endoscopically unreachable biliary anastomosis in a patient with a hepaticojejunostomy (n = 1) [10]. The SEMS was successfully deployed with a decrease in bilirubin levels in all cases. No post-procedural complications were noted after a median follow-up of 9.2 months. Puspok et al. [11] previously described a successful EUS-guided transhepatic SEMS in a single patient with a malignant biliary obstruction following gastrectomy and Roux-en-Y anastomosis. Bories et al. [5] successfully placed an SEMS transhepatically and under EUS guidance in 2 patients. However, these procedures were performed in a two-stage fashion with initial creation of a hepaticogastrostomy tract followed by anterograde placement of an SEMS in a second procedure. Limitations and challenges The right biliary system is not accessible to this method of drainage and the presence of dilated ducts is necessary. Due to the limited available data, further studies are warranted to confirm the efficacy and safety of this technique. EUS-guided pancreatic duct drainage The main indications for EUS-guided drainage of the pancreatic duct are symptomatic obstruction due to chronic pancreatitis, post-surgical stricture of the pancreaticojejunal anastomosis, or a ductal disruption. The puncture site varies depending on the site of the stenosis. In most cases the main pancreatic duct is targeted from the stomach (transgastric route). The easiest transmural access to the pancreatic duct is at the junction of the genu and body. Puncturing a non- or minimally dilated pancreatic duct can be difficult with a 19 gauge needle and may require a 22 gauge needle. The penetration of fibrosed pancreatic parenchyma is also facilitated by a 22 gauge needle. However, the 22 gauge needle takes only a inch wire, which is difficult to see and to guide. There is also a tendency for the guidewire to enter side branches. Drainage
10 328 J Hepatobiliary Pancreat Sci (2011) 18: Fig. 4 EUS-guided pancreaticogastrostomy. Presentation with painful chronic pancreatitis. ERCP was attempted but a wire failed to cross a tight pancreatic duct stricture in the head. a EUSguided puncture of a dilated pancreatic duct in the genu region with a 19G needle (arrow). b A inch hydrophilic guidewire failed to traverse the stricture. Fluroscopic (c) and endoscopic (d) views of a 7 Fr 9 7cm straight pancreatic stent (arrow), inserted after tract dilation with bougie catheters can be accomplished using a rendezvous approach if the stricture can be negotiated with a wire and the papilla or pancreaticojejunostomy can be reached with the endoscope. Failing this, transenteric drainage is performed. The procedure steps are similar to those of hepaticogastrostomy outlined above. Our preference is to use a straight 7 Fr stent for transgastric drainage. We replace the single stent with two 7 Fr stents if there is recurrence of symptoms (Fig. 4). Available data The reported data are summarized in Table 6. A total of 72 patients underwent EUS-guided pancreatic drainage. The pancreatic duct was accessed and drained in the majority of patients via the transgastric route. The technical success rate was 91% with a complication rate of 15%. Complications included post-procedural pain (n = 4), bleeding (n = 3), perforations (n = 3) and pancreatitis (n = 1). Tessier et al. [7] reported stent dysfunction requiring repeat endoscopies during the a median follow-up of 14.5 months 55%. Limitations and challenges The technical challenges relate to the fibrotic changes of chronic pancreatitis, which make needle penetration of the pancreas and tract dilation difficult. As mentioned, a 22 gauge needle can be used to achieve penetration and duct access, but leads to a second hurdle of tract dilation for stent drainage. The smallest bougies and balloons advanced over a wire usually fail to penetrate the pancreas and will buckle. One solution is to use cautery with a double lumen needle knife or diathermic ring device. The risks, including pancreatitis, leakage, and perforation, remain to be defined in larger studies. EACP versus PTCD EACP has a number of theoretical advantages over percutaneous transhepatic cholangiodrainage (PTCD). Drainage is internal, and thereby eliminates problems with external percutaneous drainage, including local skin pain, infection, drain care, and bile loss. EACP is not limited by obesity, and less limited by ascites than PTCD. Ultrasound guidance and the use of color Doppler improves the safety profile of EACP by avoiding vessels. Practical advantages are the ability to perform EACP in the same session as a failed ERCP. In our department ERCP and EACP are performed by the same operator. EACP provides excellent access to the left lobe, which can be limited by PTCD. However, access to the right
11 J Hepatobiliary Pancreat Sci (2011) 18: Table 6 Studies evaluating EUS-guided pancreatic drainage No. of cases Puncture and dilation devices Drainage route Technical success (%) Complications related to the procedure François et al. [32] 4 19 gauge needle Transgastric 100 None Cystotome Kahaleh et al. [33] 2 19 gauge needle Transgastric 100 None Balloon dilation Kahaleh et al. [34] gauge or 22 gauge needle Balloon dilation Transgastric 83 Bleeding (1) Perforation (1) Tessier et al. [7] 36 19, 22 gauge needle or cystotome Transgastric (29) Transduodenal (7) 92 Pancreatitis (1) Hematoma (1) Will et al. [35] gauge needle Dilating catheter and stent retriever Transgastric 69 Pain (4) Bleeding (1) Perforation (1) Our data [21] 5 19 gauge needle Dilating catheter Transgastric 100 Perforation (1) Ampulla or bilioenteric anastomosis accessible? YES EUS-Guided Rendezvous NO Anterograde access Stricture traversable? YES Downstream drainage NO Upstream drainage Fig. 6 Algorithm for EUS-guided interventions when ERCP access fails Fig. 5 Lumen-apposing stent (AXIOS, Xlumena Inc) lobe with EACP is limited. EACP uniquely provides access to the pancreatic duct. EACP versus ERCP There are theoretical advantages of EACP over ERCP. By avoiding the ampulla and accidental cannulation or injection of the pancreatic duct, EACP eliminates any risk of pancreatitis. The problem of difficult cannulation is also eliminated. Anterograde transenteric drainage eliminates all instrumentation (wire passage, dilation and stenting) of the downstream stricture. Creating a natural fistula at a distance from the obstructing tumor solves the problem of tumor ingrowth and overgrowth which can cause stent obstruction, and it may solve the problem of stent clogging. Future developments Tubular stents that are currently used to accomplish endoscopic translumenal drainage do not impart lumento-lumen anchorage. What is needed is a lumen-apposing stent that enables the creation of a leak-proof conduit between nonadherent lumens such as the bile duct and the duodenum (choledochoduodenostomy). In the porcine model, a fully covered expandable lumen-apposing stent (AXIOS, Xlumena Inc, Mountainview, CA) was tested and found to create a safe, durable, leak-free conduit (Fig. 5). The stent was easily removable at 4 weeks [36]. Future developments should enable the integration of the multiple steps required to achieve translumenal ductal drainage into a single catheter-based device. After lumen access, tract dilation and stent deployment should occur seamlessly in a co-axial fashion without instrument exchanges.
12 330 J Hepatobiliary Pancreat Sci (2011) 18: Conclusion Over recent years, we have seen the emergence of EACP as a viable strategy to achieve drainage of the bile and pancreatic ducts when ERCP is not feasible or fails. The algorithm in Fig. 6 outlines the use of EACP in our department. For biliary drainage, EACP has numerous theoretical advantages over PTCD. For pancreatic duct drainage, EACP offers a less invasive alternative to pancreatic bypass surgery. The literature has validated the feasibility of EACP but complication rates have been high and the safety profile of EACP must be improved. This will require improvements in device development and training. It must be emphasized that the tools used to perform EACP have been borrowed from ERCP and other sectors of interventional endoscopy. Tools designed for EUS-guided applications that enable safer transenteric access and drainage are needed. The input from innovative device manufacturers is critical at this stage. Training is a second issue that will need to be addressed. The complexity of EACP requires the highest levels of training in both EUS and ERCP. Training programs in pancreaticobiliary endoscopy must integrate the two procedures if EACP is to be disseminated into the broad community. References 1. Carr-Locke DL. Overview of the role of ERCP in the management of diseases of the biliary tract and the pancreas. Gastrointest Endosc. 2002;56:S Winick AB, Waybill PN, Venbrux AC. Complications of percutaneous transhepatic biliary interventions. Tech Vasc Interv Radiol. 2001;4: Smith AC, Dowsett JF, Russell RC, Hatfield AR, Cotton PB. Randomised trial of endoscopic stenting versus surgical bypass in malignant low bile duct obstruction. Lancet. 1994;344: Wiersema MJ, Sandusky D, Carr R, et al. Endosonography-guided cholangiopancreatography. Gastrointest Endosc. 1996;43: Bories E, Pesenti C, Caillol F, Lopes C, Giovannini M. Transgastric endoscopic ultrasonography-guided biliary drainage: results of a pilot study. Endoscopy. 2007;39: Dowsett JF, Vaira D, Hatfield AR, et al. Endoscopic biliary therapy using the combined percutaneous and endoscopic technique. Gastroenterology. 1989;96: Tessier G, Bories E, Arvanitakis M, et al. EUS-guided pancreatogastrostomy and pancreatobulbostomy for the treatment of pain in patients with pancreatic ductal dilatation inaccessible for transpapillary endoscopic therapy. Gastrointest Endosc. 2007;65: Stoker J, Lameris JS, van Blankenstein M. Percutaneous metallic self-expandable endoprostheses in malignant hilar biliary obstruction. Gastrointest Endosc. 1993;39: Becker CD, Glattli A, Maibach R, Baer HU. Percutaneous palliation of malignant obstructive jaundice with the wallstent endoprosthesis: Follow-up and reintervention in patients with hilar and non-hilar obstruction. J Vasc Interv Radiol. 1993;4: Nguyen-Tang T, Binmoeller KF, Sanchez-Yague A, Shah NJ. Endoscopic ultrasound (EUS)-guided anterograde self-expandable metal stent (SEMS) placement across malignant biliary obstruction. Endoscopy. 2010;42: Puspok A, Lomoschitz F, Dejaco C, et al. Endoscopic ultrasound guided therapy of benign and malignant biliary obstruction: a case series. Am J Gastroenterol. 2005;100: Bataille L, Deprez P. A new application for therapeutic EUS: main pancreatic duct drainage with a pancreatic rendezvous technique. Gastrointest Endosc. 2002;55: Mallery S, Matlock J, Freeman ML. EUS-guided rendezvous drainage of obstructed biliary and pancreatic ducts: report of 6 cases. Gastrointest Endosc. 2004;59: Kahaleh M, Yoshida C, Kane L, Yeaton P. Interventional EUS cholangiography: a report of five cases. Gastrointest Endosc. 2004;60: Will U, Meyer F, Manger T, Wanzar I. Endoscopic ultrasoundassisted rendezvous maneuver to achieve pancreatic duct drainage in obstructive chronic pancreatitis. Endoscopy. 2005;37: Kahaleh M, Wang P, Shami VM, Tokar J, Yeaton P. EUS-guided transhepatic cholangiography: report of 6 cases. Gastrointest Endosc. 2005;61: Kahaleh M, Hernandez AJ, Tokar J, et al. Interventional EUSguided cholangiography: evaluation of a technique in evolution. Gastrointest Endosc. 2006;64: Tarantino I, Barresi L, Repici A, Traina M. EUS-guided biliary drainage: a case series. Endoscopy. 2008;40: Brauer BC, Chen YK, Fukami N, Shah RJ. Single-operator EUSguided cholangiopancreatography for difficult pancreaticobiliary access (with video). Gastrointest Endosc. 2009;70: Maranki J, Hernandez AJ, Arslan B, et al. Interventional endoscopic ultrasound-guided cholangiography: long-term experience of an emerging alternative to percutaneous transhepatic cholangiography. Endoscopy. 2009;41: Nguyen-Tang T, Binmoeller KF, Sanchez-Yague A, Shah NJ. Endoscopic ultrasound (EUS)-guided endoscopic anterograde cholangiopancreatography (EACP) with anterograde interventions. Gastrointest Endosc. 2009;69:AB Nguyen-Tang T, Binmoeller KF, Sanchez-Yague A, Shah NJ. Single-operator, single-session endoscopic ultrasound guided rendezvous in failed ERCP. Gastrointest Endosc. 2009;69: AB Burmester E, Niehaus J, Leineweber T, Huetteroth T. EUS-cholangio-drainage of the bile duct: report of 4 cases. Gastrointest Endosc. 2003;57: Giovannini M, Dotti M, Bories E, et al. Hepaticogastrostomy by echo-endoscopy as a palliative treatment in a patient with metastatic biliary obstruction. Endoscopy. 2003;35: Artifon EL, Chaves DM, Ishioka S, et al. Echoguided hepaticogastrostomy: a case report. Clinics (Sao Paulo). 2007;62: Will U, Thieme A, Fueldner F, et al. Treatment of biliary obstruction in selected patients by endoscopic ultrasonography (EUS)-guided transluminal biliary drainage. Endoscopy. 2007;39: Giovannini M, Moutardier V, Pesenti C, et al. Endoscopic ultrasound-guided bilioduodenal anastomosis: a new technique for biliary drainage. Endoscopy. 2001;33: Fujita N, Noda Y, Kobayashi G, et al. Histological changes at an endosonography-guided biliary drainage site: a case report. World J Gastroenterol. 2007;13: Ang TL, Teo EK, Fock KM. EUS-guided transduodenal biliary drainage in unresectable pancreatic cancer with obstructive jaundice. JOP. 2007;8: Yamao K, Bhatia V, Mizuno N, et al. EUS-guided choledochoduodenostomy for palliative biliary drainage in patients with
13 J Hepatobiliary Pancreat Sci (2011) 18: malignant biliary obstruction: results of long-term follow-up. Endoscopy. 2008;40: Itoi T, Itokawa F, Sofuni A, et al. Endoscopic ultrasound-guided choledochoduodenostomy in patients with failed endoscopic retrograde cholangiopancreatography. World J Gastroenterol. 2008;14: Francois E, Kahaleh M, Giovannini M, Matos C, Deviere J. EUSguided pancreaticogastrostomy. Gastrointest Endosc. 2002;56: Kahaleh M, Yoshida C, Yeaton P. EUS anterograde pancreatography with gastropancreatic duct stent placement: review of two cases. Gastrointest Endosc. 2003;58: Kahaleh M, Hernandez AJ, Tokar J, et al. EUS-guided pancreaticogastrostomy: analysis of its efficacy to drain inaccessible pancreatic ducts. Gastrointest Endosc. 2007;65: Will U, Fueldner F, Thieme AK, et al. Transgastric pancreatography and EUS-guided drainage of the pancreatic duct. J Hepatobiliary Pancreat Surg. 2007;14: Binmoeller KF, Shah J. A novel lumen-apposing stent for translumenal fluid collections. Endoscopy (in press).
Gastrointestinal Intervention
 Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
Gastrointest Interv 2012; 1:11 18 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review
 Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
Gut and Liver, Vol. 7, No. 2, March 2013, pp. 129-136 Review Advances in Endoscopic Ultrasound-Guided Biliary Drainage: A Comprehensive Review Savreet Sarkaria, Ho-Su Lee, Monica Gaidhane, and Michel Kahaleh
BILIARY CANNULATION FOR the treatment of biliary
 Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A Literature Review
 Gastroenterology Research and Practice Volume 2013, Article ID 869214, 9 pages http://dx.doi.org/10.1155/2013/869214 Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A
Gastroenterology Research and Practice Volume 2013, Article ID 869214, 9 pages http://dx.doi.org/10.1155/2013/869214 Review Article Outcomes of Endoscopic-Ultrasound-Guided Cholangiopancreatography: A
Jintao Guo, Siyu Sun, Xiang Liu, Sheng Wang, Nan Ge, and Guoxin Wang. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Gastroenterology Research and Practice Volume 2016, Article ID 9469472, 6 pages http://dx.doi.org/10.1155/2016/9469472 Clinical Study Endoscopic Ultrasound-Guided Biliary Drainage Using a Fully Covered
Endoscopic Ultrasound-Guided Biliary Drainage
 Review Article http://dx.doi.org/10.3348/kjr.2012.13.s1.s74 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(S1):S74-S82 Endoscopic Ultrasound-Guided Biliary Drainage Everson L.A. Artifon, MD, PhD,
Review Article http://dx.doi.org/10.3348/kjr.2012.13.s1.s74 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2012;13(S1):S74-S82 Endoscopic Ultrasound-Guided Biliary Drainage Everson L.A. Artifon, MD, PhD,
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Review Article EUS-Guided Biliary Drainage
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches
 E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
E175 International multicenter comparative trial of transluminal EUS-guided biliary drainage via hepatogastrostomy vs. choledochoduodenostomy approaches Authors Mouen A. Khashab 1, Ahmed A. Messallam 1,
Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction
 CASE SERIES Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction Fauze Maluf-Filho, Felipe Alves Retes, Carla
CASE SERIES Transduodenal Endosonography-Guided Biliary Drainage and Duodenal Stenting for Palliation of Malignant Obstructive Jaundice and Duodenal Obstruction Fauze Maluf-Filho, Felipe Alves Retes, Carla
ORIGINAL PAPERS. Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP
 ORIGINAL PAPERS Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Ana María Mora-Soler, Alberto Álvarez-Delgado, María Concepción Piñero-Pérez, Antonio Velasco-Guardado,
ORIGINAL PAPERS Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Ana María Mora-Soler, Alberto Álvarez-Delgado, María Concepción Piñero-Pérez, Antonio Velasco-Guardado,
Principles of ERCP: papilla cannulation, indications/contraindications and risks. Dr. med. Henrik Csaba Horváth PhD
 Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
Principles of ERCP: papilla cannulation, indications/contraindications and risks Dr. med. Henrik Csaba Horváth PhD Evolution of ERCP 1968. 1970s ECPG Endoscopic CholangioPancreatoGraphy Japan 1974 Biliary
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
EUS Guided Pancreatic Duct Drainage: When? How?
 PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or
 Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Authors: Ana María Mora Soler, Alberto Álvarez Delgado, María Concepción Piñero Pérez, Antonio Velasco-Guardado,
Title: Endoscopic ultrasound-guided choledochoduodenostomy after a failed or impossible ERCP Authors: Ana María Mora Soler, Alberto Álvarez Delgado, María Concepción Piñero Pérez, Antonio Velasco-Guardado,
Endoscopic ultrasound guided gastrojejunostomy
 Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable Metal Stent for Malignant Biliary Obstruction
 Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 6284094, 10 pages https://doi.org/10.1155/2017/6284094 Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable
Hindawi Gastroenterology Research and Practice Volume 2017, Article ID 6284094, 10 pages https://doi.org/10.1155/2017/6284094 Research Article Endoscopic Ultrasound-Guided Biliary Drainage Using Self-Expandable
Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis
 Original article Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis Authors Theodore W. James, Todd H. Baron Institution
Original article Practical applications and learning curve for EUS-guided hepaticoenterostomy: results of a large single-center US retrospective analysis Authors Theodore W. James, Todd H. Baron Institution
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction
 Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Endoscopic ultrasound guided biliary drainage: a comprehensive review
 Review Article Endoscopic ultrasound guided biliary drainage: a comprehensive review Avantika Mishra, Amy Tyberg Department of Gastroenterology, Rutgers Robert Wood Johnson University Hospital, New Brunswick,
Review Article Endoscopic ultrasound guided biliary drainage: a comprehensive review Avantika Mishra, Amy Tyberg Department of Gastroenterology, Rutgers Robert Wood Johnson University Hospital, New Brunswick,
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Endoscopic Ultrasound-Guided Pancreatobiliary Endoscopy in Surgically Altered Anatomy
 FOCUSED REVIEW SERIES: Pancreatobiliary endoscopy in altered gastointestinal anatomy Clin Endosc 2016;49:515-529 https://doi.org/10.5946/ce.2016.144 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access
FOCUSED REVIEW SERIES: Pancreatobiliary endoscopy in altered gastointestinal anatomy Clin Endosc 2016;49:515-529 https://doi.org/10.5946/ce.2016.144 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access
CASO CLÍNICO. Los autores reportan el caso de una paciente derivada. Summary. Resumen
 CASO CLÍNICO Extrahepatic anterograde covered self-expandable metallic stent placement across malignant biliary obstruction passed by endoscopic ultrasound guidance access: a challenging technique Everson
CASO CLÍNICO Extrahepatic anterograde covered self-expandable metallic stent placement across malignant biliary obstruction passed by endoscopic ultrasound guidance access: a challenging technique Everson
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
efficacy. Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience
 E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
E76 THIEME Endoscopic ultrasound-guided gastrojejunostomy with a lumen-apposing metal stent: a multicenter, international experience Authors Institutions Amy Tyberg, Manuel Perez-Miranda, Ramon Sanchez-Ocaña,
A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy
 Review Article A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy Rucha Mehta Shah, Paul Tarnasky, Prashant Kedia
Review Article A review of endoscopic ultrasound guided endoscopic retrograde cholangiopancreatography techniques in patients with surgically altered anatomy Rucha Mehta Shah, Paul Tarnasky, Prashant Kedia
Approach to the Biliary Stricture
 Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Approach to the Biliary Stricture ACG Eastern Postgraduate Course Washington DC June 8, 2014 Steven A. Edmundowicz MD FASGE Chief of Endoscopy Division of Gastroenterology Professor of Medicine Disclosures
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
6/17/2016. ERCP in June 26, Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates
 ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in 2016 June 26, 2016 Kenneth M. Sigman, M.D. Birmingham Gastroenterology Associates 1 2 3 Diagnostic/Therapeutic ERCP Biliary Obstruction Benign stricture Malignant Stones Ductal injuries Cholangitis
ERCP in altered anatomy. Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway
 ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
ERCP in altered anatomy Lars Aabakken Oslo University Hospital - Rikshospitalet Oslo, Norway CO2 as insufflation gas Reduces post-procedure pain Reduces in-procedure bowel distension Improves the intubation
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
AXIOS Stent and Electrocautery Enhanced Delivery System *
 Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Advancing Pancreaticobiliary Disease Management AXIOS Stent and Electrocautery Enhanced Delivery System * Select a Menu Option Below Features & Benefits Expanding Innovation Ordering Information & Resources
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Evaluation of a new stent for EUS-guided pancreatic duct drainage: long-term follow-up outcome
 Evaluation of a new stent for EUS-guided pancreatic duct drainage: long-term follow-up outcome Authors Yukitoshi Matsunami 1,TakaoItoi 1, Atsushi Sofuni 1, Takayoshi Tsuchiya 1,KentaroKamada 1, Reina Tanaka
Evaluation of a new stent for EUS-guided pancreatic duct drainage: long-term follow-up outcome Authors Yukitoshi Matsunami 1,TakaoItoi 1, Atsushi Sofuni 1, Takayoshi Tsuchiya 1,KentaroKamada 1, Reina Tanaka
Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures
 E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
E96 THIEME Lumen-apposing covered self-expanding metal stent for management of benign gastrointestinal strictures Authors Institution Shounak Majumder, Navtej S. Buttar, Christopher Gostout, Michael J.
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Index. Springer Nature Singapore Pte Ltd K.-H. Lai et al. (eds.), Biliopancreatic Endoscopy,
 A Acute cholangitis biliary endoprosthesis, 70 intraductal ultrasonography, 243 Acute cholecystitis, 33, 143, 226 Acute intracystic hemorrhage, EUS-FNA, 241 Acute pancreatitis EUS-FNA, 240 intraductal
A Acute cholangitis biliary endoprosthesis, 70 intraductal ultrasonography, 243 Acute cholecystitis, 33, 143, 226 Acute intracystic hemorrhage, EUS-FNA, 241 Acute pancreatitis EUS-FNA, 240 intraductal
Biliary Metal Stents MAKING A DIFFERENCE TO HEALTH
 Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
The first stents designed for use in the biliary tree and
 Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Imaging and Advanced Technology Michael B. Wallace, Section Editor Expandable Gastrointestinal Stents TODD H. BARON Department of Medicine, Division of Gastroenterology & Hepatology, Mayo Clinic, Rochester,
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm
 Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Gastric / EUS Metal Stents
 Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
7/11/2017. We re gonna help a lot of people today. Biliary/Pancreatic Endoscopy. AGS July 1-2, Kenneth M. Sigman, MD
 Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
Biliary/Pancreatic Endoscopy AGS July 1-2, 2017 Kenneth M. Sigman, MD We re gonna help a lot of people today 1 2 3 4 Cannulation It all starts with cannulation Double Wire Cannulation Difficult cannulations
EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study
 609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage?
 EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
AXIOS Stent and Electrocautery Enhanced Delivery System. Quick Reference Guide
 AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
Maximize Control. Minimize Migration.
 Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas
 ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
The role of ERCP in chronic pancreatitis
 The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
The role of ERCP in chronic pancreatitis Marianna Arvanitakis Erasme University Hospital, ULB, Brussels, Belgium 10 th Nottingham Endoscopy Masterclass SPEAKER DECLARATIONS This presenter has the following
Endoclips, hemostasis Endoscopic balloon sphincteroplasty, see Ampullary balloon dilation. 540 Subject Index
 Subject Index ABD, see Ampullary balloon dilation Acute suppurative cholangitis, antibiotic therapy 13 Adrenal gland, endoscopic ultrasound fine needle aspiration 505 Ampulla of Vater tumor, see Papillectomy,
Subject Index ABD, see Ampullary balloon dilation Acute suppurative cholangitis, antibiotic therapy 13 Adrenal gland, endoscopic ultrasound fine needle aspiration 505 Ampulla of Vater tumor, see Papillectomy,
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the Elderly and Unwell
 Cardiovasc Intervent Radiol (2015) 38:964 970 DOI 10.1007/s00270-014-1014-y CLINICAL INVESTIGATION NON-VASCULAR INTERVENTIONS Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the
Cardiovasc Intervent Radiol (2015) 38:964 970 DOI 10.1007/s00270-014-1014-y CLINICAL INVESTIGATION NON-VASCULAR INTERVENTIONS Stenting of the Cystic Duct in Benign Disease: A Definitive Treatment for the
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
Endoscopic Retrograde Cholangiopancreatography (ERCP)
 Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
Endoscopic Retrograde Cholangiopancreatography (ERCP) Medical Imaging and Treatment of the Bile and Pancreatic Ducts CIE-02718 Understanding ERCP Brochure Update_F.indd 1 7/11/18 9:51 A Minimally Invasive
MAKING CONNECTIONS. Los Angeles Medical Center
 MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
MAKING CONNECTIONS Los Angeles Medical Center Resident: Chris Molloy, MD Fellow: Christian Coroian, MD, MBA Attending: Tina Hardley, MD Program/Dept(s): Los Angeles Medical Center CHIEF COMPLAINT & HPI
Afferent Loop Syndrome: Treatment by Means of the Placement of Dual Stents
 Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Vascular complications in percutaneous biliary interventions: A series of 111 procedures
 Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Vascular complications in percutaneous biliary interventions: A series of 111 procedures Poster No.: C-0744 Congress: ECR 2013 Type: Educational Exhibit Authors: A. BHARADWAZ; AARHUS, Re/DK Keywords: Obstruction
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Interventional Radiology Rounds:
 1295 Interventional Radiology Rounds: University of California, San Francisco Percutaneous Biliary Drainage in the Management of Cholangiocarcinoma Robert K. Kerlan, Jr., Moderator1 Anton C. Pogany2 Henry
1295 Interventional Radiology Rounds: University of California, San Francisco Percutaneous Biliary Drainage in the Management of Cholangiocarcinoma Robert K. Kerlan, Jr., Moderator1 Anton C. Pogany2 Henry
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Gastrointestinal Intervention
 Gastrointest Interv 2016;5:203 211 Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided biliary drainage Majid A. Almadi, 1 Nonthalee Pausawasdi,
Gastrointest Interv 2016;5:203 211 Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Endoscopic ultrasound-guided biliary drainage Majid A. Almadi, 1 Nonthalee Pausawasdi,
Advanced Cannulation Techniques
 Advanced Cannulation Techniques Priya A. Jamidar, M.D., FASGE Professor of Medicine, Director of Endoscopy Yale School Disclosures Consultant to Boston Scientific and Olympus America Cannulation at ERCP
Advanced Cannulation Techniques Priya A. Jamidar, M.D., FASGE Professor of Medicine, Director of Endoscopy Yale School Disclosures Consultant to Boston Scientific and Olympus America Cannulation at ERCP
Endoscopic ultrasound guided biliary and pancreatic duct interventions
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v6.i11.513 World J Gastrointest Endosc 2014 November 16; 6(11): 513524 ISSN 19485190
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v6.i11.513 World J Gastrointest Endosc 2014 November 16; 6(11): 513524 ISSN 19485190
A patient with an unusual congenital anomaly of the pancreaticobiliary tree
 A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
A patient with an unusual congenital anomaly of the pancreaticobiliary tree Thomas Hocker, HMS IV BIDMC Core Radiology Case Presentation September 17, 2007 Review of Normal Pancreaticobiliary Tract Anatomy
North Medical Endoscopic Biliary Stent (BilS)
 North Medical Endoscopic Biliary Stent (BilS) Instructions for Use Manufactured by North Medical DEVICE NAME North Medical Endoscopic Biliary Stent (BilS) DEVICE DESCRIPTION North Medical's BilS stent
North Medical Endoscopic Biliary Stent (BilS) Instructions for Use Manufactured by North Medical DEVICE NAME North Medical Endoscopic Biliary Stent (BilS) DEVICE DESCRIPTION North Medical's BilS stent
Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal Stent for Acute Cholecystitis: A Systematic Review
 REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
REVIEW Clin Endosc 2018;51:450-462 https://doi.org/10.5946/ce.2018.024 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided Gallbladder Drainage Using a Lumen-Apposing Metal
RX Biliary System. Start
 Start We re in! When you control the wire, efficiency comes along for the ride. The of Physician-Controlled Wireguided Cannulation Physician-controlled wireguided cannulation (WGC) facilitates deep biliary
Start We re in! When you control the wire, efficiency comes along for the ride. The of Physician-Controlled Wireguided Cannulation Physician-controlled wireguided cannulation (WGC) facilitates deep biliary
Allium Trans-hepatic Biliary Stent (BIS)
 Allium Trans-hepatic Biliary (BIS) Instructions for Use Manufactured by Allium Ltd. DEVICE NAME Allium Trans-hepatic Biliary (BIS) DEVICE DESCRIPTION The Trans-hepatic BIS is a flexible, self-expanding
Allium Trans-hepatic Biliary (BIS) Instructions for Use Manufactured by Allium Ltd. DEVICE NAME Allium Trans-hepatic Biliary (BIS) DEVICE DESCRIPTION The Trans-hepatic BIS is a flexible, self-expanding
AXIOS Stent and Delivery System
 PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
PRESCRIPTIVE INFORMATION AXIOS Stent and Delivery System Warning REFER TO THE DEVICE DIRECTIONS FOR USE FOR COMPLETE INSTRUCTIONS ON DEVICE USE. RX ONLY. CAUTION: FEDERAL LAW (USA) RESTRICTS THIS DEVICE
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
WallFlex Biliary RX Fully Covered Stent System Prescriptive Information
 Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
WallFlex Biliary Metal Stents
 WallFlex Biliary Metal Stents Please Note: These steps are intended to be for general guidance only. For complete instructions for use, indications, contraindications and warnings, please refer to the
WallFlex Biliary Metal Stents Please Note: These steps are intended to be for general guidance only. For complete instructions for use, indications, contraindications and warnings, please refer to the
Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser
 16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
Biliary Strictures: the Long and the Short of It. Willis Parsons, M.D. Medical Director of GI Lab Northwest Community Hospital Arlington Heights, IL
 Biliary Strictures: the Long and the Short of It Willis Parsons, M.D. Medical Director of GI Lab Northwest Community Hospital Arlington Heights, IL Consultant to Cook Medical Disclosure Objectives 1) Understand
Biliary Strictures: the Long and the Short of It Willis Parsons, M.D. Medical Director of GI Lab Northwest Community Hospital Arlington Heights, IL Consultant to Cook Medical Disclosure Objectives 1) Understand
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents
 REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
REVIEW ARTICLE Annals of Gastroenterology (2018) 31, 1-6 Through the LAMS towards the future: current uses and outcomes of lumen-apposing metal stents Alessandro Mussetto a, Alessandro Fugazza b, Lorenzo
Slide 1. Slide 2. Slide 3 Pancreatic Cancer- Case #1. Endoscopic management of GI malignancy. Endoscopic approaches in GI malignancy- Agenda
 Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
