Aortic Dissection Associated with Acute Myocardial Infarction and Stroke Found at Autopsy
|
|
|
- Bruce Gallagher
- 5 years ago
- Views:
Transcription
1 CASE REPORT Aortic Dissection Associated with Acute Myocardial Infarction and Stroke Found at Autopsy Hiroaki Kawano, Yoichi Tomichi, Satoki Fukae, Yuji Koide, Genji Toda and Katsusuke Yano Abstract It is sometimes very difficult to diagnose dissecting aortic aneurysms in the early stage. We report an autopsy case in which an acute myocardial infarction and cerebral infarction simultaneously occurred and the symptoms were transiently ameliorated in a patient with an acute aortic dissection. Key words: aortic dissection, myocardial infarction, cerebral infarction, reperfusion injury, sudden cardiac death (DOI: /internalmedicine ) Introduction The extension of aortic dissection into the brachiocephalic and common carotid arteries and the coronary arteries may lead to ischemic stroke and acute myocardial infarction. In some cases with aortic dissection, the false lumen is closed by thrombus just after the aortic dissection. However, there has so far been no report about acute myocardial infarction and cerebral infarction simultaneously occurring and transient amelioration of the symptoms in a patient with acute aortic dissection. We herein present an autopsy case report of a patient with acute myocardial infarction and stroke and transient amelioration of the symptoms caused by aortic dissection. Case Report A 49-year-old man presented with an acute onset of chest pain and left hemiparesis at 5 am in December He was transported to a local hospital. A chest X-ray showed only mild cardiomegaly, and an electrocardiogram (ECG) showed first degree atrioventricular (AV) block, wide QRS complex, and ST-segment elevation in the I, avl, and V1 to V6 leads (Fig. 1). Chest computed tomography (CT) showed normal findings, and brain CT showed no abnormal findings such as hemorrhage, hematoma, and mass. Thus, the patient was diagnosed as acute myocardial infarction and cerebral infarction, and he was transferred to our hospital for further evaluation and treatment at 8 am. His past medical history included diabetes mellitus. His father had died of aortic aneurysm. On admission, the physical examination revealed height of 172 cm, weight of 91 kg, a consciousness level of Glasgow coma scale (GCS) 10 [Japan coma scale (JCS) 20], blood pressure of 70/44 mmhg without difference between right and left upper extremities, regular pulse rate of 88 beats/min, and mild left hemiparesis. No significant murmur was heard, and lung was clear. There was only mild cardiomegaly of chest X-ray on admission, which was same in the previous hospital. His ECG on admission showed left axis deviation, right bundle branch block, and poor R wave progression in V3-6, and STsegment depression in the II, III, and avf leads. The AV block and ST-segment elevation in the I, avl, and V1 to V6 leads had disappeared (Fig. 2). An echocardiogram (UCG) demonstrated left ventricular ejection fraction (LVEF) of 62% with mild hypokinesis of the anteroseptal wall of the left ventricle (LV) and relative hyperkinesis of the posterior wall of LV. Neither valvular diseased nor pericardial effusion was seen. The white blood cell count (WBC) was /mm 3.The blood urea nitrogen was 18 mg/dl, creatinine 1.6 mg/dl, aspartate aminotransferase ( AST) 354 IU/ l, alanine Department of Cardiovascular Medicine, Course of Medical and Dental Science, Graduate School of Biomedical Science, Nagasaki University, Nagasaki Received for publication September 30, 2005; Accepted for publication May 25, 2006 Correspondence to Dr. Hiroaki Kawano, Department of Cardiovascular Medicine, Course of Medical and Dental Science, Graduate School of Biomedical Science, Nagasaki University, Sakamoto, Nagasaki, Nagasaki
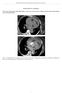
2 Figure1. AchestX-rayshowedonlymildcardiomegaly,andanelectrocardiogram showedstsegmentelevationini,avl,andv1tov6leadsinthelocalhospital. aminotransferase (ALT) 111 IU/l, lactate dehydrogenase (LDH) 748 IU/l, creatine kinase (CK) 3705 IU/l, CK-MB 306 IU/l, and C-reactive protein 0.03 mg/dl (Table 1). An emergency coronary angiogram (CAG) was performed, and it showed no significant stenosis of the coronary arteries (Fig. 2C, D). Although the diameter of left main trunk was smaller than that of the left anterior descending or circumflex coronary artery, there was no finding that indicates aortic or coronary dissection, i.e., compression of coronary artery lumen at the systolic phase or false lumen of ascending aorta detected by contrast medium during CAG. Thus, we thought that the left coronary artery spontaneously recanalized after it was occluded by either spasm or thrombus. These cardiac examinations were quickly followed by brain magnetic resonance imaging (MRI) and brain angiography to identify the cause of left hemiparesis because an abnormal consciousness level and left hemiparesis were his main symptoms at that time. Brain MRI showed several scattered small infarct lesions in the left frontal and parietal lobes. Brain angiography demonstrated an occlusion of the small branches of the right middle cerebral artery although this lesion did not account for his symptoms. In addition, the carotid arteries had no stenotic lesions. We therefore thought that the right middle cerebral artery spontaneously recanalized after occlusion by the thrombus from hypokinetic LV due to a myocardial infarction. He was admitted to the neurosurgery ward, and edaravone, a free radical scavenger, was used for the treatment of cerebral infarction, while the intravenous infusion of heparin and nitroglycerin was done to prevent myocardial infarction. His vital sings including blood pressure and pulse rate were stable, and he gradually recovered and he was able to talk and the GCS improved to 15 (JCS 1). However, the patient suddenly developed dyspnea at 5 pm. An ECG showed Q waves in V1 to V5. An UCG demonstrated 17% of LVEF with akinesis in the anteroseptal wall and apex of LV without valvular disease nor pericardial effusion. A laboratory analysis was performed and showed elevations in WBC (17600 /mm 3 ), serum AST (1820 IU/l), LDH (4015 IU/l), CK (17915 IU/l), and CK-MB(1405 IU/l) (Table 1). The patient blood pressure had gradually decreased, and his cardiac index was 1.8 l/min, and the mean pulmonary artery pressure was 30 mmhg (Forrester IV). Although the intravenous infusion of catecholamine was started, his blood pressure did not increase. Therefore, percutaneous cardiopulmonary support (PCPS) was initiated to correct the systemic hypoperfusion. His hemodynamic state stabilized after PCPS was used. However, at 11 am on the next day, he suddenly suffered cardiac arrest. A temporary pacemaker did not enable the patient to recover from cardiac arrest. As a result, the patient died two days after the admission. An autopsy was performed, and it revealed a Stanford type A aortic dissection. The point of entry was seen at the ascending aorta about 5 cm above the aortic valve (Fig. 3A) and the dissection extended from the aortic root to the abdominal aorta where the superior mesenteric artery branched. The bilateral carotid arteries were also involved by the arterial dissection. Both the right and left coronary arteries were also involved by the dissection, and their lumens were compressed by the hematoma formed in the false lumen (Fig. 3B). The dissection of the left coronary artery reached the bifurcation of the left anterior descending branch and circumflex branch (Fig. 3C). The dissection of the right coronary artery reached 2 cm from the ostium (Fig. 3D). A microscopic analysis showed: 1) a hemorrhagic infarc- 958
3 Figure2. Anelectrocardiographyshowedaleftaxisdeviation,arightbundlebranchblock,poor RwaveprogresioninV3-6,andanST-segmentdepresioninthe I,II,andaVFleads(A).An echocardiogram demonstratedaleftventricularejectionfractionof62% withmildhypokinesisof theanteroseptalwaloftheleftventricleandrelativehyperkinesisoftheposteriorwaloftheleft ventricle(b).anemergencycoronaryangiogram wasperformed,butthepatient scoronaryarterieswerenormal,andtherewasnoostialstenosisoftheleft(c)orright(d)coronaryarteries. Table1. LaboratoryData tion and contraction band necrosis were seen in the myocardium of the anterolateral wall of LV which indicated the occurrence of reperfusion injury (Fig. 4A); 2) cystic medial necrosis was seen in the media of aortic wall with mild atherosclerotic change (Fig. 4B). [This may suggest that he had Marfan s syndrome] and 3) in the false lumen of the aortic dissection, a thrombus had partially organized (Fig. 4C). However, only a fresh thrombus was seen in the false lumen of the coronary artery (Fig. 4D) and aortic root. Discussion This is the first autopsied case report in which an acute myocardial infarction and cerebral infarction simultaneously occurred and the symptoms were transiently ameliorated in a patient with an acute aortic dissection. Hagan et al (1) reported the incidences of myocardial infarction and cerebrovascular accident to be 3.2% and 4.7% in acute aortic dissection, respectively. Therefore, the occurrence of aortic dissection simultaneously associated with both myocardial 959
4 Figure3. Photographsofautopsy.(A)AutopsyrevealedStanfordtypeAaorticdissection.The entrywasseenatascendingaortaabout5cm aboveaorticvalve(arrow).thethrombuswasseen inthefalselumen(asterisk).(b)aorticdisectionreachedtheaorticroot,andthethrombusand hematomawereseeninthefalselumenofaorticroot(asterisk).(c)thedisectionofleftcoronary arteryreachedthebifurcationofleftanteriordescendingbranchandcircumflexbranch,andtheir lumenswerecompresedbythehematomainthepseudolumen(arrows).(lmt;leftmaintrunk, LAD;leftanteriordescendingbranch,LCX;leftcircumflexbranch).(D)Thedisectionofright coronaryarteryreached2cm from theostium. infarction and stroke seems rare. Less common symptoms at the initial evaluation for aortic dissection, occurring with or without associated chest pain include congestive heart failure, syncope, cerebrovascular accident, cardiac arrest, sudden death, and so on (1). As a result, it is sometimes very difficult to diagnose dissecting aortic aneurysms (DAA), particularly in the early stages, due to the manifold signs and symptoms (2). The present case presented with chest pain and left hemiparesis, and we were not able to clinically diagnose the aortic dissection even after the examinations including coronary and brain angiographies. In the present case, a transient ST-segment elevation and a spontaneous amelioration of these symptoms, including chest pain and neurological abnormalities, also made it difficult to make an accurate diagnosis. We thought that the myocardial infarction had resulted from a nonatherosclerotic coronary disease such as a coronary embolism and spasm and that the coronary artery had then spontaneously recanalized because coronary angiography showed normal coronary arteries on admission. We also speculated that the cerebral infarction had been due to an occlusion of the cerebral artery by a thrombus from the akinetic LV wall, and that the cerebral artery had then spontaneously recanalized. Although in most patients, neurological deficits from an aortic dissection are permanent (3-6), only transient symptoms of an aortic dissection have also been reported (7-9). In addition, only one case report of aortic dissection with a transient ST-segment elevation due to a left main coronary artery obstruction has been previously published (10). The mechanisms of aortic branch obstruction have been discussed as follows: 1) a bulging of the dissected false lumen, which produces an occlusion at the branch orifice, 2) subsequent distal thrombosis, 3) eventual intimal detachment at the branch orifice with perfusion largely via the false channel, and 4) a dissection extending into the branch orifice (11). However, the precise mechanism of such transient ischemia has yet not been fully elucidated. Syed and Fiad (8) speculated that rather than thrombosis or shearing of the artery, a transient occlusive valve phenomenon attributable to the progression of the dissection may lead to transient ischemia. Ashida et al (10) mentioned that a decreased blood pressure and the presence of aortic regurgitation accelerated the collapse of the true lumen during diastole in the ascending aorta by the intimal flap, thus resulting in a functional obstruction of the left main coronary artery, which may have been related to transient ST-segment 960
5 Figure4. Microphotographsofdisectingaorta.(A)Ahemorrhagicinfarctionandcontraction bandnecrosiswereseeninthemyocardium oftheanterolateralwalofleftventricle(he stain. Scalebarindicates50μm).(B)Mildcysticmedialnecrosiswasseenintheaorticwal(ElasticaVan Giesonstain.Scalebarindicates125μm).(C)Inthefalselumenoftheaorticdisection,thrombus waspartialyorganized(azanstain.scalebarindicates250μm).(d)onlyfreshthrombuswas seeninthefalselumenofthecoronaryarterydisection(azanstain.scalebarindicates250μm). changes. The mechanism of acute myocardial infarction in patients with acute aortic dissection is probably due to a compression of the extramural portion of the coronary artery by the false channel of the dissecting hematoma (12). An autopsy demonstrated a total obstruction of the bilateral coronary arteries due to compression by the false channel of the dissecting hematoma, which had caused the final sudden cardiac arrest in the present case. However, coronary angiography did not demonstrate coronary ostial stenosis either during systole or diastole when the ST-segment elevation had disappeared at the precordial leads in the ECG on admission. The autopsy also demonstrated that an organized thrombus had been seen in the false lumen of the ascending aorta although only fresh hematoma was seen in the false lumen of the coronary arteries and aortic root near the entry of aortic dissection. These findings suggested that, at first, the aortic dissection extending into the branch orifice had caused the left coronary artery obstruction, and then the thrombosed closing of the false lumen had released the obstruction of the left coronary artery, which may be related to the transient ECG change. And redissection of the ascending aorta near the coronary arteries caused the final sudden cardiac arrest in the present case. The false lumen aortic arch and the brachiocephalic arteries also demonstrated an organized thrombus. Furthermore, brain angiography demonstrated the occlusion of the small branches of the right middle cerebral artery. Thus, cerebral infarction seems to be caused by both the occlusion of the brachiocephalic artery due to aortic dissection and distal thrombosis. As a result, the transient ischemia of the brain also seems to be related to the occlusion of the false lumen after the dissection. An acute Stanford type A aortic dissection with coronary involvement is associated with a high mortality rate. Therefore aggressive coronary revascularization and early aortic repair are necessary to salvage these critically ill patients (13). When coronary angiography shows stenosis of the coronary arteries compressed by the false lumen of an acute aortic dissection, either stenting or surgery is performed to save the patient s life (14, 15). However, the left ventricular function of patients tends to remain depressed postoperatively, which limits their quality of life even when successful surgical treatments were performed in patients with a type A acute aortic dissection combined with myocardial infarction caused by a retrograde dissection into the left main trunk of the coronary artery (16, 17). The present case demonstrated the severe myocardal damage after the recanalization. Therefore, reperfusion injury, as well as ostial stenosis may be one of the most important factors to explain why 961
6 the left ventricular function of patients with acute myocardial infarction associated with aortic dissection remains depressed after successful coronary revascularization. If aortic dissection is not considered in the differential diagnosis of patients with myocardial infarction and stroke, aortography, enhanced CT, or transesophageal echocardiography may not be performed, and angiography alone is unable to detect an aortic dissection. We therefore strongly recommended that an aortic dissection be included in the differential diagnosis in patients presenting with acute myocardial infarction and stroke even when the ECG changes and symptoms are transient. References 1. Hagan PG, Wienaber CA, Isselbacher EM. The International Registry of Acute Aortic Dissection (IRAD): new insight into an old disease. JAMA 283: , Hashimoto S, Kumada T, Kubo S, Noda M, Osakada G, Yamazato A, Kawai C. The pitfalls in the clinical diagnosis of dissecting aortic aneurysm. J Cardiol 22: , 1992 (in Japanese). 3. Weisman AD, Adams RD. The neurological complications of dissecting anuerysm. Brain 67: 6-91, Moersch FP, Sayre GP. Neurologic manifestations associated with dissecting anuerysm of aorta. JAMA 144: , Goever O, Heyer EJ, Vieux U. Painless dissections of aorta presenting as acute neurologic syndromes. Stroke 17: , Prendes JL. Neurovascular syndromes of aortic dissection. Am Fam Physician 23: , Gaul C, Dietrich W, Tomandl B, Neundorfer B, Erbguth FJ. Aortic dissection presenting with transient global amnesia-like symptoms. Neurology 63: , Syed MA, Fiad TM. Transient paraplegia as a presenting feature of aortic dissection in a young man. Emerg Med 19: , J Inzelberg R, Nisipeanu P, Blumen SC, Kovach I, Groisman GM, Carasso RL. Transient unilateral mydriasis as the presenting sign of aortic and carotid dissection. Neurology 55: , Ashida K, Arakawa K, Yamagishi T, et al. A case of aortic dissection with transient ST-segment elevation due to functional left main coronary artery obstruction. Jpn Circ J 64: , Cambria RP, Brewater DC, Gertler J, et al. Vascular complications associated with spontaneous aortic dissection. J Vasc Surg 7: , Khan R, Amaram S, Gomes JA, Kelen GJ, Lynfield J, El-Sherif N. Myocardial infarction following acute aortic dissection. Cathet Cardiovasc Diagn 6: , Kawahito K, Adachi H, Murata S, Yamaguchi A, Ino T. Coronary malperfusion due to type A aortic dissection: mechanism and surgical management. Ann Thorac Surg 76: , Ohara Y, Hiasa Y, Hosokawa S. Successful treatment in a case of acute aortic dissection complicated with acute myocardial infarction due to occlusion of the left main coronary artery. J Invasive Cardiol 15: , Cardozo C, Riadh R, Mazen M. Acute myocardial infarction due to left main compression aortic dissection treated by direct stenting. J Invasive Cardiol 16: 89-91, Tominaga R, Tomita Y, Toshima Y, et al. Acute type A aortic dissection involving the left main trunk of the coronary artery-a report of two successful cases. Jpn Circ J 63: , Ohtani N, Kiyokawa K, Asada H, Kawakami T. Stanford type A acute dissection developing acute myocardial infarction. Cardiovasc Surg 48: 69-72, The Japanese Society of Internal Medicine 962
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
WHI Form Report of Cardiovascular Outcome Ver (For items 1-11, each question specifies mark one or mark all that apply.
 WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
WHI Form - Report of Cardiovascular Outcome Ver. 6. COMMENTS To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: OMB# 095-044 Exp: 4/06 -Affix label here- Clinical Center/ID:
A Case of Acute Type B Aortic Dissection: Limited Role of Laboratory Testing for the Diagnosis of Mesenteric Ischemia
 Case Report A Case of Acute Type B Aortic Dissection: Limited Role of Laboratory Testing for the Diagnosis of Mesenteric Ischemia Koichi Akutsu, MD, 1 Hitoshi Matsuda, MD, 2 Hiroaki Sasaki, MD, 2 Kenji
Case Report A Case of Acute Type B Aortic Dissection: Limited Role of Laboratory Testing for the Diagnosis of Mesenteric Ischemia Koichi Akutsu, MD, 1 Hitoshi Matsuda, MD, 2 Hiroaki Sasaki, MD, 2 Kenji
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Supplementary material 1. Definitions of study endpoints (extracted from the Endpoint Validation Committee Charter) 1.
 Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Rationale, design, and baseline characteristics of the SIGNIFY trial: a randomized, double-blind, placebo-controlled trial of ivabradine in patients with stable coronary artery disease without clinical
Acute myocardial infarction (MI) due to extension of
 Coronary Malperfusion Due to Type A Aortic Dissection: Mechanism and Surgical Management Koji Kawahito, MD, Hideo Adachi, MD, Sei-ichiro Murata, MD, Atsushi Yamaguchi, MD, and Takashi Ino, MD Department
Coronary Malperfusion Due to Type A Aortic Dissection: Mechanism and Surgical Management Koji Kawahito, MD, Hideo Adachi, MD, Sei-ichiro Murata, MD, Atsushi Yamaguchi, MD, and Takashi Ino, MD Department
B myonephropathic metabolic syndrome MNMS 33 CT DeBakey IIIb MNMS
 13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
13 603 607 2004 B B myonephropathic metabolic syndrome MNMS33 CT DeBakey IIIb MNMS 20 A MNMSMNMS 13 603 607 2004 MNMS B malperfusion myonephropathic metabolic syndrome MNMS MNMS Haimovici 1 3 MNMS B MNMS
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME. DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18
 UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
UPDATE ON THE MANAGEMENTACUTE CORONARY SYNDROME DR JULES KABAHIZI, Psc (Rwa) Lt Col CHIEF CONSULTANT RMH/KFH 28 JUNE18 INTRODUCTION The clinical entities that comprise acute coronary syndromes (ACS)-ST-segment
(For items 1-12, each question specifies mark one or mark all that apply.)
 Form 121 - Report of Cardiovascular Outcome Ver. 9.2 COMMENTS -Affix label here- Member ID: - - To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: - Central Case No.:
Form 121 - Report of Cardiovascular Outcome Ver. 9.2 COMMENTS -Affix label here- Member ID: - - To be completed by Physician Adjudicator Date Completed: - - (M/D/Y) Adjudicator Code: - Central Case No.:
Case 47 Clinical Presentation
 93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
93 Case 47 C Clinical Presentation 45-year-old man presents with chest pain and new onset of a murmur. Echocardiography shows severe aortic insufficiency. 94 RadCases Cardiac Imaging Imaging Findings C
Ischemic heart disease
 Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Ischemic heart disease Introduction In > 90% of cases: the cause is: reduced coronary blood flow secondary to: obstructive atherosclerotic vascular disease so most of the time it is called: coronary artery
Echocardiographic Evaluation of the Aorta
 Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Echocardiographic Evaluation of the Aorta William F. Armstrong M.D. Director Echocardiography Laboratory Professor of Medicine University of Michigan The Aorta: What to Evaluate Dimensions / shape Atherosclerotic
Conus artery occlusion causing isolated right ventricular outflow tract infarction: novel application of cardiac magnetic resonance in anterior STEMI
 Case Report Conus artery occlusion causing isolated right ventricular outflow tract infarction: novel application of cardiac magnetic resonance in anterior STEMI Melissa Lyle 1, Ryan C. Van Woerkom 2,
Case Report Conus artery occlusion causing isolated right ventricular outflow tract infarction: novel application of cardiac magnetic resonance in anterior STEMI Melissa Lyle 1, Ryan C. Van Woerkom 2,
A case of ascending aortic dissection mimicking acute myocardial infarction and complicated with pericardial tamponade
 Case Report A case of ascending aortic dissection mimicking acute myocardial infarction and complicated with pericardial tamponade Amer Hawatmeh, Ahmad Abu Arqoub, Ahmad Isbitan, Fayez Shamoon Department
Case Report A case of ascending aortic dissection mimicking acute myocardial infarction and complicated with pericardial tamponade Amer Hawatmeh, Ahmad Abu Arqoub, Ahmad Isbitan, Fayez Shamoon Department
Abnormalities Caused by Left Bundle Branch Block
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Physician Assistant Studies, Department 12-17-2010 Abnormalities Caused by Left Bundle Branch
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Physician Assistant Studies, Department 12-17-2010 Abnormalities Caused by Left Bundle Branch
Learning from errors. A Arrivi, 1 G Tanzilli, 1 L Tritapepe, 2 G Mazzesi, 3 E Mangieri 1
 Learning from errors Undetected acute aortic dissection in a patient referred for primary coronary angioplasty: a successful treatment of perioperative bleeding after abciximab administration A Arrivi,
Learning from errors Undetected acute aortic dissection in a patient referred for primary coronary angioplasty: a successful treatment of perioperative bleeding after abciximab administration A Arrivi,
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns
 CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
Myocardial contusion injury (MCI) may occur as a rare
 Cardiovascular Images Myocardial Contusion in an 8-Year-Old Boy A Kick to the Heart Danielle M. Moyé, MD; Adrian K. Dyer, MD; Poonam P. Thankavel, MD Myocardial contusion injury (MCI) may occur as a rare
Cardiovascular Images Myocardial Contusion in an 8-Year-Old Boy A Kick to the Heart Danielle M. Moyé, MD; Adrian K. Dyer, MD; Poonam P. Thankavel, MD Myocardial contusion injury (MCI) may occur as a rare
HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM
 REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
REVIEW DATE REVIEWER'S ID HEART AND SOUL STUDY OUTCOME EVENT - MORBIDITY REVIEW FORM : DISCHARGE DATE: RECORDS FROM: Hospitalization ER Please check all that may apply: Myocardial Infarction Pages 2, 3,
Blunt trauma, Chest contusion, Acute myocardial infarction
 Case Reports A Case of Blunt Chest Trauma Induced Acute Myocardial Infarction Involving Two Vessels Chao-Hung LAI, 1 MD, Tsochiang MA, 2 PhD, Ting-Chuan CHANG, 1 MD, Mu-Hsin CHANG, 1 MD, Pesus CHOU, 3
Case Reports A Case of Blunt Chest Trauma Induced Acute Myocardial Infarction Involving Two Vessels Chao-Hung LAI, 1 MD, Tsochiang MA, 2 PhD, Ting-Chuan CHANG, 1 MD, Mu-Hsin CHANG, 1 MD, Pesus CHOU, 3
CORONARY arteriovenous fistulas are uncommon, but their detection has. Rupture of a Giant Saccular Aneurysm of Coronary Arteriovenous Fistulas
 Rupture of a Giant Saccular Aneurysm of Coronary Arteriovenous Fistulas Masahiro ITO, MD, Makoto KODAMA, MD, Makihiko SAEKI, 1 MD, Hiroshi FUKUNAGA, MD, Tomoji GOTO, 2 MD, Hidenori INOUE, 2 MD, Shigetaka
Rupture of a Giant Saccular Aneurysm of Coronary Arteriovenous Fistulas Masahiro ITO, MD, Makoto KODAMA, MD, Makihiko SAEKI, 1 MD, Hiroshi FUKUNAGA, MD, Tomoji GOTO, 2 MD, Hidenori INOUE, 2 MD, Shigetaka
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM. General Instructions: ID NUMBER: FORM NAME: H F A DATE: 10/13/2017 VERSION: CONTACT YEAR NUMBER:
 ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
ARIC HEART FAILURE HOSPITAL RECORD ABSTRACTION FORM General Instructions: The Heart Failure Hospital Record Abstraction Form is completed for all heart failure-eligible cohort hospitalizations. Refer to
Topic. Updates on Definition of Myocardial Infarction
 Topic Updates on Definition of Myocardial Infarction In the past, general consensus for MI? Definition of MI by WHO - Combination of 2 of 3 characteristics - 1. Typical Symptoms 2. Enzyme Rise 3. Typical
Topic Updates on Definition of Myocardial Infarction In the past, general consensus for MI? Definition of MI by WHO - Combination of 2 of 3 characteristics - 1. Typical Symptoms 2. Enzyme Rise 3. Typical
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
2019 Qualified Clinical Data Registry (QCDR) Performance Measures
 2019 Qualified Clinical Data Registry (QCDR) Performance Measures Description: This document contains the 18 performance measures approved by CMS for inclusion in the 2019 Qualified Clinical Data Registry
2019 Qualified Clinical Data Registry (QCDR) Performance Measures Description: This document contains the 18 performance measures approved by CMS for inclusion in the 2019 Qualified Clinical Data Registry
Disclosures: Acute Aortic Syndrome. A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO
 Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
CORONARY ARTERY DISEASES
 CORONARY ARTERY DISEASES It has been estimated that over one third of the population eventually will die of CAD, and 20% will develop symptoms when younger than age 60 years. ANATOMY OF THE CORONARY ARTERIES
CORONARY ARTERY DISEASES It has been estimated that over one third of the population eventually will die of CAD, and 20% will develop symptoms when younger than age 60 years. ANATOMY OF THE CORONARY ARTERIES
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
THE PATIENT WAS a 66-year-old man who experienced
 Acute Medicine & Surgery 2018; 5: 189 193 doi: 10.1002/ams2.324 Case Report Treatment of a patient with acute aortic dissection using extracorporeal cardiopulmonary resuscitation after an out-of-hospital
Acute Medicine & Surgery 2018; 5: 189 193 doi: 10.1002/ams2.324 Case Report Treatment of a patient with acute aortic dissection using extracorporeal cardiopulmonary resuscitation after an out-of-hospital
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor. Cardiothoracic Radiology
 New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
Images in Cardiovascular Medicine
 Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
Images in Cardiovascular Medicine Numerous Small Vegetations Revealing Libman-Sacks Endocarditis in Catastrophic Antiphospholipid Syndrome Hideo Yamamoto, MD; Tamaki Iwade, MD; Ryuji Nakano, MD; Masahiro
ISPUB.COM. A pulled muscle," - Aortic Dissection. A Bhagra, N Anand, M Fernanda Bellolio INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Radiology Volume 9 Number 1 A pulled muscle," - Aortic Dissection A Bhagra, N Anand, M Fernanda Bellolio Citation A Bhagra, N Anand, M Fernanda Bellolio. A pulled muscle,"
ISPUB.COM The Internet Journal of Radiology Volume 9 Number 1 A pulled muscle," - Aortic Dissection A Bhagra, N Anand, M Fernanda Bellolio Citation A Bhagra, N Anand, M Fernanda Bellolio. A pulled muscle,"
Complete Proximal Occlusion of All Three Main Coronary Arteries Complicated With a Left Main Coronary Aneurysm: A Case Report
 J Cardiol 2004 Nov; 44 5 : 201 205 Complete Proximal Occlusion of All Three Main Coronary Arteries Complicated With a Left Main Coronary Aneurysm: A Case Report Takatoshi Hiroshi Akira Takahiro Masayasu
J Cardiol 2004 Nov; 44 5 : 201 205 Complete Proximal Occlusion of All Three Main Coronary Arteries Complicated With a Left Main Coronary Aneurysm: A Case Report Takatoshi Hiroshi Akira Takahiro Masayasu
Update on Acute Aortic Syndrome
 SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
Multimodality Imaging of the Thoracic Aorta
 Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm
 CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
CASE REPORT Left ventricle pseudoaneurysm as late postoperative complication of a large apical aneurysm Mariana M. Floria 1, 4, Carmen Elena Pleșoianu 2, 4, Michel Buche 3, Baudouin Marchandise 4, Erwin
Case 9799 Stanford type A aortic dissection: US and CT findings
 Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report
 Concurrent subarachnoid hemorrhage and AMI 155 Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report Chen-Chuan Cheng 1, Wen-Shiann Wu 1, Chun-Yen Chiang 1, Tsuei-Yuang Huang
Concurrent subarachnoid hemorrhage and AMI 155 Concurrent Subarachnoid Hemorrhage and Acute Myocardial Infarction: A Case Report Chen-Chuan Cheng 1, Wen-Shiann Wu 1, Chun-Yen Chiang 1, Tsuei-Yuang Huang
Diseases of the Aorta
 Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
Diseases of the Aorta ASE Review 2018 Susan E Wiegers, MD, FASE, FACC Professor of Medicine My great friend Dr. Roberto Lang Disclosure None related to this presentation 1 Objectives Aneurysm Dissection
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Form 4: Coronary Evaluation
 Form : Coronary Evaluation Print this Form t Started Date of Coronary Evaluation Coronary Evaluation Indication for Coronary Evaluation Check only one. Angio NOT DONE: n invasive test performed Followup
Form : Coronary Evaluation Print this Form t Started Date of Coronary Evaluation Coronary Evaluation Indication for Coronary Evaluation Check only one. Angio NOT DONE: n invasive test performed Followup
Form 4: Coronary Evaluation
 Patient Details Hidden Show Show/Hide Annotations Form : Coronary Evaluation Print this Form t Started Date of Coronary Evaluation Coronary Evaluation Indication for Coronary Evaluation Check only one.
Patient Details Hidden Show Show/Hide Annotations Form : Coronary Evaluation Print this Form t Started Date of Coronary Evaluation Coronary Evaluation Indication for Coronary Evaluation Check only one.
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD
 Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Myocardial infarction
 CHAPTER-I CARDIOVASCULAR SYSTEM Myocardial infarction SUB: PHARMACOTHERAPEUTICS-I CODE:T0820006 Dr. Venugopal Pharm.D Assistant Professor Department of Pharm.D Kriahna Teja Pharmacy College,Tirupati. Definition
CHAPTER-I CARDIOVASCULAR SYSTEM Myocardial infarction SUB: PHARMACOTHERAPEUTICS-I CODE:T0820006 Dr. Venugopal Pharm.D Assistant Professor Department of Pharm.D Kriahna Teja Pharmacy College,Tirupati. Definition
cardiac imaging planes planning basic cardiac & aortic views for MR
 cardiac imaging planes planning basic cardiac & aortic views for MR Dianna M. E. Bardo, M. D. Assistant Professor of Radiology & Cardiovascular Medicine Director of Cardiac Imaging cardiac imaging planes
cardiac imaging planes planning basic cardiac & aortic views for MR Dianna M. E. Bardo, M. D. Assistant Professor of Radiology & Cardiovascular Medicine Director of Cardiac Imaging cardiac imaging planes
Neurological outcomes and mortality in patients with type A aortic dissection. Impact of intra-operative management
 Neurological outcomes and mortality in patients with type A aortic dissection. Impact of intra-operative management P Santé, M. Buonocore L Majello, A Caiazzo, G Petrone, G Nappi Dept. of Cardiothoracic
Neurological outcomes and mortality in patients with type A aortic dissection. Impact of intra-operative management P Santé, M. Buonocore L Majello, A Caiazzo, G Petrone, G Nappi Dept. of Cardiothoracic
Results of Ischemic Heart Disease
 Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Ischemic Heart Disease: Angina and Myocardial Infarction Ischemic heart disease; syndromes causing an imbalance between myocardial oxygen demand and supply (inadequate myocardial blood flow) related to
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases
 Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
Cardiovascular Disorders Lecture 3 Coronar Artery Diseases By Prof. El Sayed Abdel Fattah Eid Lecturer of Internal Medicine Delta University Coronary Heart Diseases It is the leading cause of death in
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Anomalous Origin of Left Coronary Artery from Main Pulmonary Artery (ALCAPA) Who Underwent Two Coronary System Repair with a Novel Technique
 Open Journal of Clinical Diagnostics, 2014, 4, 182-191 Published Online September 2014 in SciRes. http://www.scirp.org/journal/ojcd http://dx.doi.org/10.4236/ojcd.2014.43027 Anomalous Origin of Left Coronary
Open Journal of Clinical Diagnostics, 2014, 4, 182-191 Published Online September 2014 in SciRes. http://www.scirp.org/journal/ojcd http://dx.doi.org/10.4236/ojcd.2014.43027 Anomalous Origin of Left Coronary
12 Lead ECG Interpretation
 12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI).
 1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
1) Severe, crushing substernal chest pain 2) radiate to the neck, jaw, epigastrium, or left arm. 3- rapid and weak pulse 4- nausea (posterior MI). 5- cardiogenic shock (massive MIs >40% of the left ventricle)
Case Report Subacute Staphylococcusepidermidis Bacterial Endocarditis Complicated by Mitral-Aortic Intervalvular Fibrosa Pseudoaneurysm
 Case Reports in Cardiology Volume 2012, Article ID 467210, 4 pages doi:10.1155/2012/467210 Case Report Subacute Staphylococcusepidermidis Bacterial Endocarditis Complicated by Mitral-Aortic Intervalvular
Case Reports in Cardiology Volume 2012, Article ID 467210, 4 pages doi:10.1155/2012/467210 Case Report Subacute Staphylococcusepidermidis Bacterial Endocarditis Complicated by Mitral-Aortic Intervalvular
Case Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer
 Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
Case 12305 Acute ascending thoracic aortic rupture due to penetrating atherosclerotic ulcer Lopes Dias J, Costa NV, Leal C, Alves P, Bilhim T Section: Chest Imaging Published: 2014, Dec. 19 Patient: 68
THORACIC AORTIC DISSECTION
 The Essence of Aortic Dissection THORACIC AORTIC DISSECTION Aortic dissection can be classified as acute if it s onset has been less than 14 days or chronic if its onset has been more than 14 days. Mortality
The Essence of Aortic Dissection THORACIC AORTIC DISSECTION Aortic dissection can be classified as acute if it s onset has been less than 14 days or chronic if its onset has been more than 14 days. Mortality
Acute Myocardial Infarction
 Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Acute Myocardial Infarction Hafeza Shaikh, DO, FACC, RPVI Lourdes Cardiology Services Asst.Program Director, Cardiology Fellowship Associate Professor, ROWAN-SOM Acute Myocardial Infarction Definition:
Myocardial Infarction
 Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Myocardial Infarction MI = heart attack Defined as necrosis of heart muscle resulting from ischemia. A very significant cause of death worldwide. of these deaths, 33% -50% die before they can reach the
Syncope Due to Intracavitary Left Ventricular Obstruction Secondary to Giant Esophageal Hiatus Hernia
 American Journal of Medical Case Reports, 2017, Vol. 5, No. 4, 89-93 Available online at http://pubs.sciepub.com/ajmcr/5/4/4 Science and Education Publishing DOI:10.12691/ajmcr-5-4-4 Syncope Due to Intracavitary
American Journal of Medical Case Reports, 2017, Vol. 5, No. 4, 89-93 Available online at http://pubs.sciepub.com/ajmcr/5/4/4 Science and Education Publishing DOI:10.12691/ajmcr-5-4-4 Syncope Due to Intracavitary
ADVANCED CARDIOVASCULAR IMAGING. Medical Knowledge. Goals and Objectives PF EF MF LF Aspirational
 Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Medical Knowledge Goals and Objectives PF EF MF LF Aspirational Know the basic principles of magnetic resonance imaging (MRI) including the role of the magnetic fields and gradient coil systems, generation
Acute Aortic Syndromes
 Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
The Cardiovascular System. Chapter 15. Cardiovascular System FYI. Cardiology Closed systemof the heart & blood vessels. Functions
 Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
Chapter 15 Cardiovascular System FYI The heart pumps 7,000 liters (4000 gallons) of blood through the body each day The heart contracts 2.5 billion times in an avg. lifetime The heart & all blood vessels
A Case of Left Main Coronary Stenting for Acute Myocardial Infarction Complicated by Ascending Aortic Dissection
 증례 Korean Circulation J 2004;34(12):1210-1215 Case of Left Main Coronary Stenting for cute Myocardial Infarction Complicated by scending ortic Dissection Yong Seop Kwon, MD, Hyun Sang Lee, MD, Jae Kook
증례 Korean Circulation J 2004;34(12):1210-1215 Case of Left Main Coronary Stenting for cute Myocardial Infarction Complicated by scending ortic Dissection Yong Seop Kwon, MD, Hyun Sang Lee, MD, Jae Kook
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction. Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING
 Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Cardiac Pathology & Rehabilitation
 Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
Cardiac Pathology & Rehabilitation Which of the following best describes the physical activity performed in my leisure time? A. I perform vigorous physical activity 3X/week for 20 minutes each time B.
New ASE Guidelines: What you must know
 New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
New ASE Guidelines: What you must know Federico M Asch MD, FASE, FACC Chair, ASE Guidelines and Standards Committee Medstar Washington Hospital Center Medstar Health Research Institute Georgetown University
An Approach to the Patient with Syncope. Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva
 An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
An Approach to the Patient with Syncope Guy Amit MD, MPH Soroka University Medical Center Beer-Sheva Case presentation A 23 y.o. man presented with 2 episodes of syncope One during exercise,one at rest
BEDSIDE ASSESSMENT OF PATIENTS WITH STEMI
 BEDSIDE ASSESSMENT OF PATIENTS WITH STEMI Prof. Maria Dorobantu, PhD, FESC, FACC Emergency Hospital of Bucharest, Romania Presenter Disclosures There are no conflicts/ grants/ disclosures for this presentation.
BEDSIDE ASSESSMENT OF PATIENTS WITH STEMI Prof. Maria Dorobantu, PhD, FESC, FACC Emergency Hospital of Bucharest, Romania Presenter Disclosures There are no conflicts/ grants/ disclosures for this presentation.
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
SUPPLEMENTAL MATERIAL
 SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
SUPPLEMENTL MTERIL Marie erna, Martin Kocher, Rohit Philip Thomas. cute aorta, overview of acute T findings and endovascular treatment options (doi: 10.5507/bp.2016.060) Fig. 1. : Non-enhanced T, hemopericardium
Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome
 Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
Diagnosis and Management of Acute Myocardial Infarction
 Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
Diagnosis and Management of Acute Myocardial Infarction Acute Myocardial Infarction (AMI) occurs as a result of prolonged myocardial ischemia Atherosclerosis leads to endothelial rupture or erosion that
TSDA Boot Camp September 13-16, Introduction to Aortic Valve Surgery. George L. Hicks, Jr., MD
 TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
TGA atrial vs arterial switch what do we need to look for and how to react
 TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
TGA atrial vs arterial switch what do we need to look for and how to react Folkert Meijboom, MD, PhD, FES Dept ardiology University Medical entre Utrecht The Netherlands TGA + atrial switch: Follow-up
TAVR : Caring for your patients before and after TAVR
 TAVR : Caring for your patients before and after TAVR Zubair Ahmed MD FSCAI Interventional Cardiologist Washington Regional Medical Center / Walker Heart Institute What is Aortic Valve Stenosis? AVA ~4
TAVR : Caring for your patients before and after TAVR Zubair Ahmed MD FSCAI Interventional Cardiologist Washington Regional Medical Center / Walker Heart Institute What is Aortic Valve Stenosis? AVA ~4
Optimal repair of acute aortic dissection
 Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Optimal repair of acute aortic dissection Dept. of Vascular Surgery, The 2nd Xiang-Yale Hospital, Central-South University, China Hunan Major Vessels Diseases Clinical Center Chang Shu Email:changshu01@yahoo.com
Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter
 Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter Nirat Beohar, MD Associate Professor of Medicine Director Cardiac Catheterization Laboratory, Medical Director Structural
Options for my no option Patients Treating Heart Conditions Via a Tiny Catheter Nirat Beohar, MD Associate Professor of Medicine Director Cardiac Catheterization Laboratory, Medical Director Structural
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Distal Coronary Artery Dissection Following Percutaneous Transluminal Coronary Angioplasty
 Distal Coronary rtery Dissection Following Percutaneous Transluminal Coronary ngioplasty Douglas. Murphy, M.D., Joseph M. Craver, M.D., and Spencer. King 111, M.D. STRCT The most common cause of acute
Distal Coronary rtery Dissection Following Percutaneous Transluminal Coronary ngioplasty Douglas. Murphy, M.D., Joseph M. Craver, M.D., and Spencer. King 111, M.D. STRCT The most common cause of acute
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial
 An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
An aneurysm is a localized abnormal dilation of a blood vessel or the heart Types: 1-"true" aneurysm it involves all three layers of the arterial wall (intima, media, and adventitia) or the attenuated
Case 1. Case 2. Case 3
 Case 1 The correct answer is D. Occasionally, the Brugada syndrome can present similar morphologies to A and also change depending on the lead position but in the Brugada pattern the r is wider and ST
Case 1 The correct answer is D. Occasionally, the Brugada syndrome can present similar morphologies to A and also change depending on the lead position but in the Brugada pattern the r is wider and ST
Ischemic Heart Disease
 Ischemic Heart Disease Dr Rodney Itaki Lecturer Division of Pathology University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology General Consideration Results from partial
Ischemic Heart Disease Dr Rodney Itaki Lecturer Division of Pathology University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology General Consideration Results from partial
Simultaneous Acute ST Elevation Myocardial Infarction And Acute Left Subclavian Artery Thrombosis
 Simultaneous Acute ST Elevation Myocardial Infarction And Acute Left Subclavian Artery Thrombosis Chee Yang CHIN, MBChB, MRCP(UK) C.W.L. Chin, P.T.L. Chiam, R.S. Tan National Heart Centre Singapore 26
Simultaneous Acute ST Elevation Myocardial Infarction And Acute Left Subclavian Artery Thrombosis Chee Yang CHIN, MBChB, MRCP(UK) C.W.L. Chin, P.T.L. Chiam, R.S. Tan National Heart Centre Singapore 26
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow
 The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
CMS Limitations Guide - Cardiovascular Services
 CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
, David Stultz, MD. Aortic Dissection. David Stultz, MD October 7, 2003
 Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
Aortic Dissection David Stultz, MD October 7, 2003 Background Incidence of 1 in 2000 in US Early mortality of 1%/hour for proximal dissection Two theories of formation Breach of intimal layer of aorta
Total Endovascular Repair Type A Dissection. Eric Herget Interventional Radiology
 Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Aortic arch pathology. Cerebral ischemia following carotid artery stenosis.
 Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
Important: -Subclavian Steal Syndrome -Cerebral ischemia Aortic arch pathology. Cerebral ischemia following carotid artery stenosis. Mina Aubeed & Alba Hernández Pinilla Aortic arch pathology Common arch
CMS Limitations Guide - Cardiovascular Services
 CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Cardiovascular Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
EAE Teaching Course. Magnetic Resonance Imaging. Competitive or Complementary? Sofia, Bulgaria, 5-7 April F.E. Rademakers
 EAE Teaching Course Magnetic Resonance Imaging Competitive or Complementary? Sofia, Bulgaria, 5-7 April 2012 F.E. Rademakers Complementary? Of Course N Engl J Med 2012;366:54-63 Clinical relevance Treatment
EAE Teaching Course Magnetic Resonance Imaging Competitive or Complementary? Sofia, Bulgaria, 5-7 April 2012 F.E. Rademakers Complementary? Of Course N Engl J Med 2012;366:54-63 Clinical relevance Treatment
J. Schwitter, MD, FESC Section of Cardiology
 J. Schwitter, MD, FESC Section of Cardiology CMR Center of the CHUV University Hospital Lausanne - CHUV Switzerland Centre de RM Cardiaque J. Schwitter, MD, FESC Section of Cardiology CMR Center of the
J. Schwitter, MD, FESC Section of Cardiology CMR Center of the CHUV University Hospital Lausanne - CHUV Switzerland Centre de RM Cardiaque J. Schwitter, MD, FESC Section of Cardiology CMR Center of the
Paraplegia in endovascular repair of TAA and in TEVAR: Incidence, prevention and therapy. Johannes Lammer Medical University Vienna, Austria
 Paraplegia in endovascular repair of TAA and in TEVAR: Incidence, prevention and therapy Johannes Lammer Medical University Vienna, Austria Conflict of interests: none 68y, male, PAU in coral reef aorta,
Paraplegia in endovascular repair of TAA and in TEVAR: Incidence, prevention and therapy Johannes Lammer Medical University Vienna, Austria Conflict of interests: none 68y, male, PAU in coral reef aorta,
