DOI: /CIRCEP
|
|
|
- Julie Houston
- 5 years ago
- Views:
Transcription
1 Initial Experience of Assessing Esophageal Tissue Injury and Recovery Using Delayed-Enhancement MRI Following Atrial Fibrillation Ablation Troy J. Badger, Yaw A. Adjei Poku, Nathan S. Burgon, Saul Kalvaitis, Akram Shaaban, Daniel N Sommers, Joshua J.E. Blauer, Eric N. Fish, Nazem Akoum, Thomas S. Haslem, Eugene G. Kholmovski, Rob S. MacLeod, Douglas G. Adler and Nassir F. Marrouche Circ Arrhythmia Electrophysiol published online Sep 17, 2009; DOI: /CIRCEP Circulation: Arrhythmia and Electrophysiology is published by the American Heart Association Greenville Avenue, Dallas, TX Copyright 2009 American Heart Association. All rights reserved. Print ISSN: Online ISSN: The online version of this article, along with updated information and services, is located on the World Wide Web at: Subscriptions: Information about subscribing to Circulation: Arrhythmia and Electrophysiology is online at Permissions: Permissions & Rights Desk, Lippincott Williams & Wilkins, a division of Wolters Kluwer Health, 351 West Camden Street, Baltimore, MD Phone: Fax: journalpermissions@lww.com Reprints: Information about reprints can be found online at
2 Initial Experience of Assessing Esophageal Tissue Injury and Recovery Using Delayed-Enhancement MRI Following Atrial Fibrillation Ablation Troy J. Badger MD 1, Yaw A. Adjei-Poku MD 1, Nathan S. Burgon BS 1, Saul Kalvaitis MD 1, Akram Shaaban MBBCh 2, Daniel N. Sommers MD 2, Joshua J.E. Blauer BS 1, Eric N. Fish 1, Nazem Akoum MD 1, Thomas S. Haslem BS 1, Eugene G. Kholmovski PhD 1, Rob S. MacLeod PhD 1, Douglas G. Adler MD 3 and Nassir F. Marrouche MD 1 1 Comprehensive Arrhythmia and Research Management, University of Utah School of Medicine. Salt Lake City, Utah. 2 Department of Radiology, University of Utah. Salt Lake City, Utah. 3 Department of Gastroenterology, University of Utah. Salt Lake City, Utah Corresponding Author Nassir F. Marrouche, MD Director, Cardiac Electrophysiology Laboratories Director, Atrial Fibrillation Program Division of Cardiology University of Utah Health Sciences Center 30 North 1900 East Room 4A100 Salt Lake City, Utah Nassir.Marrouche@hsc.utah.edu Phone: Fax: Journal Subject Codes: atrial fibrillation, pulmonary vein antrum isolation, delayedenhancement MRI, esophageal injury
3 Abstract: Background: Esophageal wall thermal injury following atrial fibrillation (AF) ablaiton is a potentially serious complication. However, no noninvasive modality has been used to describe and screen patients to examine whether esophageal wall injury has occurred. We describe a noninvasive method of using delayed-enhancement MRI (DE-MRI) to detect esophageal wall injury and subsequent recovery following AF ablation. Methods and Results: We analyzed the DE-MRI scans of 41 patients prior to ablation, and at 24 hours and 3 months post-ablation to determine whether there was evidence of contrast enhancement in the esophagus following AF ablation. In patients with contrast enhancement, three-dimensional segmentation of the esophagus was performed using a novel image processing method. Upper gastrointestinal endoscopy (UGE) was then performed. Repeat DE-MRI and UGE was performed one week later to track changes in lesions. The wall thickness of the anterior and posterior r wall of the esophagus was measured at three e time points; prior to ablation, 24 hours post, and 3 months post. Evaluation of pre-ablation MRI scans demonstrated no cases of esophageal enhancement. At twenty-four hours, 5 patients showed contrast enhancement. Three of these patients underwent UGE, which demonstrated esophageal lesions. Repeat UGE and MRI one week later demonstrated resolution of the lesions. All five patients had confirmed resolution of enhancement at 3 months. All patients with esophageal tissue enhancement demonstrated LA wall enhancement directly adjacent to the regions of anterior wall esophageal enhancement. Conclusion: Our preliminary results indicate DE-MRI can assess the extent and follow progression of esophageal wall injury following catheter ablation of AF. It appears acute esophageal injury recovers within one week of the procedure. Key Words: atrial fibrillation, ablation, magnetic resonance imaging, upper gastrointestinal endoscopy, esophageal injury 2
4 Introduction Atrio-esophageal (AE) fistula is a serious and oftentimes fatal complication of intraoperative and endocardial catheter ablation of atrial fibrillation (AF). 1-5 Fistula formation results from the collateral thermal effect of radiofrequency (RF) energy on the esophagus during ablation of the left atrium (LA). 6 This injury is thought to occur due to a close anatomical relationship between the posterior structures of the left atrium, a target during circumferential ablation, and the anterior wall of the esophagus. 6-9 Recent reports have also demonstrated subclinical thermal damage to the esophagus immediately medi postablation. 10 Endoscopic evaluation in these patients demonstrated erythematous and necrotic lesions in the anterior wall of the esophagus in regions of close proximity to the LA; lesions which often self-resolve by later follow-up. 10 Given the serious nature of ablation-related complications, use of a noninvasive modality to assess the post-ablation esophageal response could contribute significantly to monitoring early complications, tracking lesion progression and initiating early intervention to avoid serious procedural consequences. In this report, we describe the use of DE-MRI to visualize and follow esophageal tissue injury following radiofrequency catheter ablation of AF. Methods Study Population Between April 2008 and August 2008, fifty-seven consecutive patients who presented to the University of Utah for AF ablation had MRI scans at three time points; prior to 3
5 ablation, within twenty-four hours post-ablation, and at three months post-ablation. Of these patients, sixteen had an uninterpretable scan due to patient motion and blurring, significant navigator artifact, and/or incorrect choice of inversion time. Forty-one patients were thus included in the final analysis. Written and informed consent was obtained in all patients and the study was approved by the IRB at the University of Utah. Patients with esophageal enhancement were given the option to undergo upper gastrointestinal endoscopy (UGE) at the time of the scan. Three patients underwent UGE. The clinical demographics of the study patients are shown in Table 1. Delayed Enhancement MRI Patients underwent a DE-MRI sequence as previously described. d 11 Briefly, all patients underwent MRI studies on a 1.5 Tesla Avanto clinical scanner (Siemens Medical Solutions, Erlangen, Germany) using a body surface phased array coil. A delayed enhancement sequence was used to identify injured or nonviable tissue. DE-MRI was acquired about 15 minutes following contrast agent injection (0.1 mmol/kg, Multihance (Bracco Diagnostic Inc., Princeton, NJ)) using a 3D inversion recovery, respiration navigated, ECG-gated, gradient echo pulse sequence. The full dose of contrast was given in all patients with an estimated glomerular filtration rate (egfr) > 60. Patient s with egfr between were given half the contrast dose. Typical acquisition parameters were: free-breathing using navigator gating, a transverse imaging volume with voxel size = 1.25 x 1.25 x 2.5 mm (reconstructed to x x 1.25 mm), TR/TE = 5.4/2.3 ms, inversion time (TI) = ms, GRAPPA with R=2 and 46 reference lines. ECG gating was used to acquire a small subset of phase encoding views during the diastolic 4
6 phase of the LA cardiac cycle. The time interval between the R- peak of the ECG and the start of data acquisition was defined using the cine images of the LA. Fat saturation was used to suppress fat signal. The TE of the scan (2.3 ms) was chosen such that fat and water are out of phase and the signal intensity of partial volume fat-tissue voxels was reduced allowing improved delineation of the LA wall boundary. The TI value for the DE-MRI scan was identified using a scout scan. Typical scan time for the DE-MRI study was 5-10 minutes depending on subject respiration and heart rate. Radiofrequency Catheter Ablation All patients underwent pulmonary vein antrum isolation with posterior wall and septal debulking. The technique is briefly summarized below. After venous access, cess a 14-pole coronary sinus catheter was placed into the coronary sinus via the right internal n jugular access (TZ Medical Inc., Portland, OR or BARD, NJ) for use as a mapping reference. A phased-array ultrasound catheter was positioned in the mid-right atrium (Siemens AG Inc., Malvern, PA, USA) and used to guide a double transseptal puncture, through which was placed a 10-pole Lasso catheter and an F-curve, Thermocool 3.5-mm irrigated tip ablation catheter (Biosense-Webster Inc). Using fluoroscopy and electroanatomic mapping (CARTOMERGE, Biosense-Webster Inc.) for catheter navigation, intracardiac potentials in the PV antra and on the posterior wall were mapped during sinus rhythm, and were targeted for ablation if fractionation was seen distinct from far-field atrial potentials. Lasso-guided RF delivery was performed, using Lasso electrogram artifacts to confirm ablation catheter tip location relative to the substrate of interest. Lesions were delivered using 50 W with a 50 C temperature limit, for a duration of 10 seconds (maximum 15 seconds), with the endpoint being elimination of all local electrograms. 5
7 When all antral and posterior wall targets had been ablated, this entire region was resurveyed for any return of electrical activity, and any such regions demonstrating electrical recovery were retreated. In addition, entry block in all four pulmonary veins was confirmed with the ablation catheter after debulking was accomplished. DE-MRI Based Esophageal Monitoring Protocol Within twenty-four hours following the AF ablation procedure, all patients underwent DE-MRI in order to assess for acute esophageal injury. Patients with no contrast enhancement or changes in wall thickness were then assessed for esophageal injury on their MRI at their routine three-month follow-up visit. Patients exhibiting acute injury at 24 hours underwent upper GI endoscopy for lesion confirmation and repeat MRI within one week to assess for lesion progression or change. DE-MRI Image Analysis and Processing Follow acquisition of the scan, each 2D slice was evaluated in a random, blinded fashion for the presence of contrast enhancement in the esophageal wall by two independent experts in cardiac MRI. A positive finding required agreement between both reviewers. A kappa statistic of.796 (p = <0.001) was calculated for inter-rater agreement. The esophageal images displaying contrast enhancement were then segmented into 3D models along with 3D generation of the LA and analyzed to see if regions of esophageal enhancement overlapped regions of LA enhancement. Three-dimensional segmentation was accomplished by manually segmenting the contours of the LA and esophageal walls and then stacking the 2D slices into 3D models. Following volume rendering of the images, a smooth table opacity and color-look-up-table were applied to better illuminate the contrast enhancement. 6
8 Esophageal Wall Measurements The thickness of the anterior wall and posterior wall of the esophagus was measured at the same anatomical location of the DE-MRI obtained pre-ablation, as well as twentyfour hours and three months post-ablation. Slices of interest were based on images with contrast enhancement in the posterior wall or pulmonary vein antra of the LA. Anterior wall and posterior wall measurements of the esophagus were taken on at least three separate slices with each patient averaging 4 slices. The same measurements were then obtained at the same anatomical locations on the two other scans. Upper Gastrointestinal Endoscopy After obtaining informed consent, the endoscope was passed under direct vision with monitoring of heart rate, respiratory rate, blood pressure, and oxygen saturations continuously throughout the procedure. The endoscope was introduced through the mouth and advanced to the second portion of the duodenum. Radial endosonography n was performed at 7.5 MHz and 10.0 MHz with Doppler. Endoscopic ultrasound was used when appropriate. The images were then interpreted by the gastroenterologist who performed the procedure. Three patients underwent UGE on the same days as the acquisition of the DE-MRI scan following the ablation procedure due to detection of esophageal wall enhancement on DE-MRI. Two patients with esophageal contrast enhancement seen on DE-MRI were offered and refused UGE. Follow up Following the procedure, all patients underwent 24-hour observation on a telemetry unit. Patients continued anti-coagulation therapy with warfarin (international normalized ratio of ) for a minimum of three months. Patients were assessed for esophageal 7
9 symptoms during the 24-hour post-ablation monitoring period as well at a three-month clinic visit. All patients were discharged on an eight-week course of an oral proton-pump inhibitor. Statistical Analysis Continuous variables are presented as the mean plus or minus one standard deviation. Tests for significance were performed using a repeated measures One-Way ANOVA test. Turkey s multiple comparision was used to test for significance between time points. The results of these reviewers were compared using Cohens Kappa statistic to assess for inter-rater agreement. Differences were considered significant nt at p < Statistical analysis was performed using the SPSS 15.0 Statistical Package age (SPSS S Inc.; Chicago, IL). Results Esophageal Contrast Enhancement Of the pre-ablation scans, 0/41 demonstrated esophageal enhancement. At twenty-four hours post-ablation, 5/41 (12.2%) showed contrast enhancement in the anterior wall of the esophagus. Figure 1 demonstrates the MRI findings at all time points of five patients who had enhancement at 24 hours post-ablation. All five patients did not have enhancement prior to ablation and all patients had resolution of enhancement on their 3 months post-ablation scan. Three of the patients with contrast enhancement had repeat DE-MRI within one week with all patients demonstrating resolution of esophageal enhancement. All areas of esophageal enhancement were adjacent to regions of LA wall enhancement targeted during the ablation. Of the five patients with esophageal enhancement, the closest contact point of the esophagus to the LA was the left superior 8
10 pulmonary vein antra in three patients (Figure 1), and the posterior wall in two patients. Two out of the five patients exhibited esophageal symptoms after the procedure, including one patient with a burning epigastric pain and the other patient with pain and irritation with swallowing. Esophageal Wall Measurements Esophagus Anterior wall Mean esophageal anterior wall thickness was 1.81 ± 0.36 mm on pre ablation, 2.16 ± 0.39 mm on 24 hr, and 1.88 ± 0.26 mm on three month scans. A statistical significance was observed when comparing these means (p <0.001) using analysis of variance. Post Hoc testing showed significance between pre and 24 hr post ablation scans (p <0.001). and also 24 hr and three month scans (p <0.001). There was no statistical significance between pre and three month scans (p = 0.66). The average age change in thickness of the anterior wall from pre ablation to 24 hrs post ablation was 0.36 ± 0.51, ± 0.44 from 24 hrs to three months post ablation, and 0.23 ± 0.56 from pre to three months post ablation. Analysis of variance showed a statistical significance between these three means (p <0.001). Using post hoc analysis, a statistical significance between the change in thickness between pre to 24 hrs post ablation and 24 hrs to three months post ablation (p <0.001) was found. Statistical significance was also found when comparing 24 hrs to three months post ablation and pre to three months post ablation (p < 0.001). However, there was no significance between change in thickness from pre to three months post ablation (p = 0.27) Esophagus Posterior wall 9
11 Mean esophageal posterior wall thickness was 1.85 ± 0.32 mm on pre ablation, 1.96 ± 0.28 mm on 24 hr, and 1.92 ± 0.31 mm on three month scans. A statistical significance was not observed when comparing these means (p = 0.07) using an analysis of variance. Post Hoc testing also did not show significance between pre and 24 hr post ablation scans (p = 0.06), 24 hr and three month scans (p = 0.78), or pre and three month scans (p = 0.48). The average change in thickness of the posterior wall from pre ablation to 24 hrs post ablation was 0.14 ± 0.33, ± 0.27 from 24 hrs to three months post ablation, and 0.21 ± 0.56 from pre to three months post ablation. Analysis of variance showed a statistical significance between these mean values (p = 0.001). Further r analysis alys using post hoc statistics revealed a statistical significance between the change in thickness between pre to 24 hrs post ablation and 24 hrs to three months post ablation (p = 0.02). Statistical significance was also found when comparing 24 hrs to three months post ablation and pre to three months post ablation (p = 0.001). However, there was no significance between change in thickness from pre to three months post ablation (p = 0.54) Upper Gastrointestinal Endoscopy Out of the five patients who displayed esophageal enhancement on DE-MRI at 24 hours post-ablation, three patients elected to undergo upper gastrointestinal endoscopy. Two patients refused the procedure. One patient experienced a superficial large erosions (1-2 cm) with nodular base in the lower third of the esophagus. The second patient had localized mucosal abnormality characterized by pale erythema found at 32cm from the incisors. This was an area of approximately 1cm in diameter, with diffuse borders. There 10
12 was no ulceration or signs of bleeding. Endoscopic ultrasound demonstrated preservation of esophageal wall architecture despite the mucosal injury with no mediastinal or periesophageal adenopathy detected. The third patient revealed an irregular and erythematous lesion in the lower third of the anterior wall. All three patients had lesion size and location that correlated with the anatomical location of enhancement identified on DE-MRI based on the 3D recreations of the esophagus. Two patients had repeat endoscopy one week later, which showed healing of the esophageal lesion. A patient example is demonstrated in Figure 2. Discussion In this study we describe the feasibility and initial experience e of using DE-MRI to detect acute esophageal wall injury following catheter ablation of AF. Although h DE-MRI has been shown to visualize post-ablation LA changes resulting from the RF energy 11, there have not been any reports describing esophageal wall changes using this modality. In our study, 12.2% of patients showed esophageal anterior wall injury on DE-MRI immediately post ablation in regions targeted during the procedure with all patients showing complete lesion resolution within one week post-ablation. Endoscopic evaluation correlated the size and location of MRI enhancement patterns with intraluminal lesions detected with endoscopy. Our findings of post-ablative esophageal changes are consistent with other reports detailing this phenomenon. A recent analysis by Schmidt et al demonstrated frequent erythematous (29%) and necrotic changes (18%) in the anterior wall of the esophagus twenty-four hours post-af ablation. 10 These authors used repeat endoscopy to show complete recovery of the erythematous esophageal changes by two-weeks post-ablation 11
13 and recovery of the necrotic changes by one-month post ablation. Another recent study by Singh et al demonstrated that 11% of asymptomatic patients experienced post-ablation esophageal ulcerations from RF energy. 12 Recovery of lesions as measured by resolution of contrast enhancement might be explained by a partial inflammatory reaction occurring in the esophagus immediately following ablation. This could be similar to the inflammatory state that has been described in the LA immediately following RF ablation. 13, 14 It has recently been reported that gadolinium enhancement in the LA in the immediate post-ablative state might represent edema/hemorrhage rather than true myocyte necrosis, as the enhancement often recedes by later follow up. 15 A similar transient inflammatory process from the radiofrequency energy with subsequent healing and recovery may also occur in the immediate post-ablative esophagus.. The gadolinium uptake and wall thickening seen in the posterior wall of the esophagus might also represent edema rather than necrosis as this tissue is not in near contact with the ablation energy, yet appears to undergo transient post-ablative changes as well. Figure 3 demonstrates both LA and esophageal enhancement resolution following ablation. In this patient example, extensive enhancement is seen in the anterior wall of the esophagus and throughout a significant portion of the LA at 24 hours post-ablation. Repeat imaging at three months demonstrates complete resolution of esophageal lesions with decrease in LA enhancement to regions solely confined to the the pulmonary vein antra. The resolution of contrast enhancement and return of wall thickness to preprocedure baseline levels suggesting acute esophageal injury is often a transient phenomenon. 12
14 Evidence shows that lesions placed in the LA increase the luminal temperature of the esophagus, supporting the notion that RF energy delivery effects mediastinal structures outside the LA. 6 Although our study used an ablative technique targeting the LA posterior wall, we do not feel this caused an increase in the incidence of esophageal injury. Based on the significant anatomical overlap of the esophagus, many standard pulmonary vein antra techniques have the potential to damage the esophagus. 9 This has been shown to be especially pertinent to techniques targeting the left pulmonary vein antra; as prior studies have shown this is the most common location of LA-esophageal contact. 6 The close anatomical overlap of the esophagus to the pulmonary vein antra, primarily the left pulmonary vein antrum, is demonstrated in Figure 1.. Additional d i studies are required red to correlate the frequency and extent of esophageal tissue damage following AF ablation among the different techniques and ablation parameters utilized. Esophageal fistula occurs during the acute post-af ablation state, usually u within 2 weeks of the procedure. 2, 16 Although DE-MRI findings of patients who develop LAesophageal fistulas are not known, the implementation of DE-MRI as a noninvasive screening tool in the acute post-procedure stages has the potential to identify those patients at increased risk of developing this serious complication. Identification of these patients could potentially lead to early interventions to minimize the consequences of the complication. Deciphering which patients who experience acute esophageal injury who are at risk of these complications should be a topic of interest for future research. Study Limitations Given the prospective nature of this analysis, expert MRI reviewers were not blinded to 13
15 the time point of scan acquisition, since MRI findings dictated further clinical management. In our study, only patients with positive MRI findings underwent endoscopy for correlation, thus we do not have immediate 24 hour endoscopy data on patients with a normal appearing DE-MRI. Although all patients underwent DE-MRI prior to the ablation and did not demonstrate any contrast enhancement in the esophagus, patients with pre-existing esophageal pathology were not excluded from the study. Conclusions Our preliminary results indicate that DE-MRI has the ability to detect and monitor progression of esophageal lesions following catheter ablation of AF. Acute esophageal injury appears common in the immediate post-ablation state with resolution of the findings by later follow up. This appears to indicate that some patients experience a transient inflammatory matory response in the post-ablative esophagus that recovers without the development of serious procedure-related complications. Conflict of Interest Disclosures: None References 1. Sonmez B, Demirsoy E, Yagan N, Unal M, Arbatli H, Sener D, Baran T, Ilkova F. A fatal complication due to radiofrequency ablation for atrial fibrillation: atrioesophageal fistula. The Annals of thoracic surgery. 2003; 76: Paponne C, Oral H, Santinelli V, Vicedeomini G, Lang C, Manguso F, Torracca L, Benussi S, Alfieri O, Hong R, Lau W, Hirata K, Shikuma N, Hall B, Morady F. 14
16 Atrio-esophageal fistula as a complication of percutaneous transcatheter ablation of atrial fibrulation. Circulation. 2004; 109: Scanavacca MI, D'Avila A, Parga J, Sosa E. Left atrial-esophageal fistula following radiofrequency catheter ablation of atrial fibrillation. J Cardiovasc Electrophysiol. 2004; 15: Doll N, Borger MA, Fabricius A, Stephan S, Gummert J, Mohr FW, Hauss J, Kottkamp H, Hindricks G. Esophageal perforation during left atrial radiofrequency ablation: Is the risk too high? J Thorac Cardiovasc Surg. 2003; 125: Gillinov AM, Pettersson G, Rice TW. Esophageal injury during radiofrequency ablation for atrial fibrillation. J Thorac Cardiovasc Surg. 2001; 122: Cummings JE, Schweikert RA, Saliba WI, Burkhardt JD, Brachmannn J, Gunther J, Schibgilla V, Verma A, Dery M, Drago JL, Kilicaslan F, Natale A. Assessment of temperature, proximity, and course of the esophagus during radiofrequency ablation within the left atrium. Circulation. 2005; 112: Sanchez-Quintana D, Cabrera JA, Climent V, Farre J, Mendonca MC, Ho SY. Anatomic relations between the esophagus and left atrium and relevance for ablation of atrial fibrillation. Circulation. 2005; 112: Wazni OM, Tsao HM, Chen SA, Chuang HH, Saliba W, Natale A, Klein AL. Cardiovascular imaging in the management of atrial fibrillation. Journal of the American College of Cardiology. 2006; 48: Lemola K, Sneider M, Desjardins B, Case I, Han J, Good E, Tamirisa K, Tsemo A, Chugh A, Bogun F, Pelosi F, Jr., Kazerooni E, Morady F, Oral H. Computed 15
17 tomographic analysis of the anatomy of the left atrium and the esophagus: implications for left atrial catheter ablation. Circulation. 2004; 110: Schmidt M, Nolker G, Marschang H, Gutleben KJ, Schibgilla V, Rittger H, Sinha AM, Ritscher G, Mayer D, Brachmann J, Marrouche NF. Incidence of oesophageal wall injury post-pulmonary vein antrum isolation for treatment of patients with atrial fibrillation. Europace. 2008; 10: Peters DC, Wylie JV, Hauser TH, Kissinger KV, Botnar RM, Essebag V, Josephson ME, Manning WJ. Detection of pulmonary vein and left atrial scar after catheter ablation with three-dimensional navigator-gated gated delayed enhancement MR imaging: initial experience. Radiology. ogy. 2007; 07; 243: Singh SM, d'avila A, Doshi SK, Brugge WR, Bedford RA, Mela T, Ruskin JN, Reddy VY. Esophageal Injury and Temperature Monitoring During Atrial Fibrillation Ablation. Circulation: Arrhythmia and Electrophysioly. 2008; 1: Okada T, Yamada T, Murakami Y, Yoshida N, Ninomiya Y, Shimizu T, Toyama J, Yoshida Y, Ito T, Tsuboi N, Kondo T, Inden Y, Hirai M, Murohara T. Prevalence and severity of left atrial edema detected by electron beam tomography early after pulmonary vein ablation. Journal of American College of Cardiology. 2007; 49: Steel KE, Roman-Gonzalez J, O'Bryan CLt. Images in cardiovascular medicine. Severe left atrial edema and heart failure after atrial fibrillation ablation. Circulation. 2006; 113:e
18 15. Badger TJ, Oakes RS, Daccarett M, Burgon NS, Akoum N, Fish EN, Blauer JJE, Rao SN, Adjei-Poku Y, Kholmovski EG, Vijayakumar S, Di Bella EVR, MacLeod RS, Marrouche NF. Temporal left atrial lesion formation after ablation of atrial fibrillation Heart Rhythm. 2009; 6: Cummings JE, Schweikert RA, Saliba WI, Burkhardt JD, Kilikaslan F, Saad E, Natale A. Brief communication: atrial-esophageal fistulas after radiofrequency ablation. Ann Intern Med. 2006; 144:
19 Table 1: Patient Demographics Total Patients 41 Male 22 Female 19 Age ± AF Type Paroxysmal 23 Persistent 18 Underlying Disease CAD 4 Diabetes 4 CHF 4 Hypertension 22 18
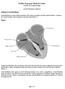
20 Figure 1. Acute Post-Ablation Esophageal Changes and Recovery. This figure depicts five patient examples of esophageal changes post-af ablation. Pre-procedure MRI (left) in all patients did not demonstrate any esophageal contrast enhancement. However, at 24 hours post-ablation (middle) all five patients had anterior wall thickening with significant contrast enhancement primarily located in the anterior wall. This enhancement and wall thickening showed complete resolution by three months postprocedure (right) even though chronic left atrial scar remained. Regions of esophageal enhancement were in close relation to radiofrequency-induced scarring in the left atrium from the ablation procedure. Figure 2. Evaluation of Esophageal Lesions with Endoscopy. Three patients with enhancement seen on DE-MRI at twenty-four hours underwent nt endoscopy. The patient example below is a 62 year-old male with paroxysmal AF who experienced ence increased gadolinium uptake (yellow arrow) in the anterior wall of the esophagus on MRI at 24 hours post-ablation. Endoscopic findings at that time point confirmed the presence of a superficial erosion on in the anterior wall. Repeat imaging and endoscopy one week later showed full recovery of the esophageal lesion on MRI and UGE. Figure 3. Recovery of Contrast Enhancement in the Anterior wall of the Esophagus. This patient example is of a 57 year-old female presenting for catheter ablation of paroxysmal AF. Three-dimensional segmentation of the LA and esophagus at 24-hours post-ablation (left) demonstrates significant contrast enhancement (orange). However, by three months post-ablation (right) there is resolution of all enhancement in the esophagus. Contrast enhancement in the LA decreases significantly to involve only portions surrounding the left pulmonary veins. Our findings indicate a possible inflammatory process that occurs in both the LA and esophagus shortly after the ablation procedure, which partially or fully resolves by later follow up. This example also demonstrates the close anatomical relationship between the LA and esophagus, primarily at the antra regions targeted during the ablation procedures. 19
21
22
23
Initial Experience of Assessing Esophageal Tissue Injury and Recovery Using Delayed-Enhancement MRI After Atrial Fibrillation Ablation
 Initial Experience of Assessing Esophageal Tissue Injury and Recovery Using Delayed-Enhancement MRI After Atrial Fibrillation Ablation Troy J. Badger, MD; Yaw A. Adjei-Poku, MD; Nathan S. Burgon, BS; Saul
Initial Experience of Assessing Esophageal Tissue Injury and Recovery Using Delayed-Enhancement MRI After Atrial Fibrillation Ablation Troy J. Badger, MD; Yaw A. Adjei-Poku, MD; Nathan S. Burgon, BS; Saul
Tailored Management of Atrial Fibrillation Using a LGE-MRI Based Model: From the Clinic to the Electrophysiology Laboratory
 1 Techniques and Technology Editor: Hugh Calkins, M.D. Tailored Management of Atrial Fibrillation Using a LGE-MRI Based Model: From the Clinic to the Electrophysiology Laboratory GASTON R. VERGARA, M.D.
1 Techniques and Technology Editor: Hugh Calkins, M.D. Tailored Management of Atrial Fibrillation Using a LGE-MRI Based Model: From the Clinic to the Electrophysiology Laboratory GASTON R. VERGARA, M.D.
From the Division of Cardiology and Department of Radiology, Virginia Commonwealth University Medical Center, Richmond, Virginia, USA
 Accuracy of Intracardiac Echocardiography for Assessing the Esophageal Course Along the Posterior Left Atrium: A Comparison to Magnetic Resonance Imaging DAVID N. KENIGSBERG, M.D., BENJAMIN P. LEE, M.D.,
Accuracy of Intracardiac Echocardiography for Assessing the Esophageal Course Along the Posterior Left Atrium: A Comparison to Magnetic Resonance Imaging DAVID N. KENIGSBERG, M.D., BENJAMIN P. LEE, M.D.,
Esophageal Injury Following Radiofrequency Ablation for Atrial Fibrillation
 Esophageal Injury Following Radiofrequency Ablation for Atrial Fibrillation Jonathan Keshishian Division of Digestive Diseases and Nutrition University of South Florida Morsani College of Medicine, Tampa,
Esophageal Injury Following Radiofrequency Ablation for Atrial Fibrillation Jonathan Keshishian Division of Digestive Diseases and Nutrition University of South Florida Morsani College of Medicine, Tampa,
Magnetic Resonance Imaging: Description of Technology and Protocols
 Magnetic Resonance Imaging: Description of Technology and Protocols 2 Gaston R. Vergara and Nassir F. Marrouche Abstract Since its introduction in the late 1970s, catheter-based radiofrequency ablation
Magnetic Resonance Imaging: Description of Technology and Protocols 2 Gaston R. Vergara and Nassir F. Marrouche Abstract Since its introduction in the late 1970s, catheter-based radiofrequency ablation
Prevalence of Fever in Patients Undergoing Left Atrial Ablation of Atrial Fibrillation Guided by Barium Esophagraphy
 Prevalence of Fever in Patients Undergoing Left Atrial Ablation of Atrial Fibrillation Guided by Barium Esophagraphy RUBINDER S. RUBY, M.D., DARRYL WELLS, M.D., SUNDAR SANKARAN, M.D., ERIC GOOD, D.O.,
Prevalence of Fever in Patients Undergoing Left Atrial Ablation of Atrial Fibrillation Guided by Barium Esophagraphy RUBINDER S. RUBY, M.D., DARRYL WELLS, M.D., SUNDAR SANKARAN, M.D., ERIC GOOD, D.O.,
Arrhythmia/Electrophysiology
 Arrhythmia/Electrophysiology Computed Tomographic Analysis of the Anatomy of the Left Atrium and the Esophagus Implications for Left Atrial Catheter Ablation Kristina Lemola, MD; Michael Sneider, MD; Benoit
Arrhythmia/Electrophysiology Computed Tomographic Analysis of the Anatomy of the Left Atrium and the Esophagus Implications for Left Atrial Catheter Ablation Kristina Lemola, MD; Michael Sneider, MD; Benoit
Radiofrequency (RF) catheter ablation of atrial fibrillation
 Esophageal Injury and Temperature Monitoring During Atrial Fibrillation Ablation Sheldon M. Singh, MD; Andre d Avila, MD; Shephal K. Doshi, MD; William R. Brugge, MD; Rudolph A. Bedford, MD; Theofanie
Esophageal Injury and Temperature Monitoring During Atrial Fibrillation Ablation Sheldon M. Singh, MD; Andre d Avila, MD; Shephal K. Doshi, MD; William R. Brugge, MD; Rudolph A. Bedford, MD; Theofanie
Author Proof Delayed-enhancement MRI & the visualization of ablation scar Future Cardiol.
 MRI in cardiac electrophysiology: the emerging role of delayed enhancement MRI in atrial fibrillation ablation Troy J Badger, Yaw A Adjei-Poku & Nassir F Marrouche Author for correspondence: Atrial Fibrillation
MRI in cardiac electrophysiology: the emerging role of delayed enhancement MRI in atrial fibrillation ablation Troy J Badger, Yaw A Adjei-Poku & Nassir F Marrouche Author for correspondence: Atrial Fibrillation
NIH Public Access Author Manuscript J Am Coll Cardiol. Author manuscript; available in PMC 2013 August 18.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Cardiol. 2011 July 5; 58(2): 177 185. doi:10.1016/j.jacc.2011.04.008. Dark Regions of No-Reflow on Late Gadolinium Enhancement
NIH Public Access Author Manuscript Published in final edited form as: J Am Coll Cardiol. 2011 July 5; 58(2): 177 185. doi:10.1016/j.jacc.2011.04.008. Dark Regions of No-Reflow on Late Gadolinium Enhancement
Dark Regions of No-Reflow on Late Gadolinium Enhancement Magnetic Resonance Imaging Result in Scar Formation After Atrial Fibrillation Ablation
 Journal of the American College of Cardiology Vol. 58, No. 2, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2011.04.008
Journal of the American College of Cardiology Vol. 58, No. 2, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2011.04.008
Introduction Atrial fibrillation (AF) can be effectively treated by catheter ablation. Typically, ablation targets the ostia of the pulmonary
 Initial experience with magnetic resonance imaging of atrial scar and co-registration with electroanatomic voltage mapping during atrial fibrillation: Success and limitations David D. Spragg, MD, FHRS,
Initial experience with magnetic resonance imaging of atrial scar and co-registration with electroanatomic voltage mapping during atrial fibrillation: Success and limitations David D. Spragg, MD, FHRS,
Oesophageal temperature monitoring and incidence of oesophageal lesions after pulmonary vein isolation using a remote robotic navigation system
 Europace (2010) 12, 655 661 doi:10.1093/europace/euq061 CLINICAL RESEARCH Ablation for Atrial Fibrillation Oesophageal temperature monitoring and incidence of oesophageal lesions after pulmonary vein isolation
Europace (2010) 12, 655 661 doi:10.1093/europace/euq061 CLINICAL RESEARCH Ablation for Atrial Fibrillation Oesophageal temperature monitoring and incidence of oesophageal lesions after pulmonary vein isolation
Επιπλοκές κατάλυσης πνευµονικών φλεβών
 Επιπλοκές κατάλυσης πνευµονικών φλεβών Παναγιώτης Ιωαννίδης Διευθυντής Τµήµατος Αρρυθµιών & Επεµβατικής Ηλεκτροφυσιολογίας Βιοκλινικής Αθηνών ΣΕΜΙΝΑΡΙΑ ΟΜΑΔΩΝ ΕΡΓΑΣΙΑΣ Ιωάννινα, 27-2-2015 Solving an equation
Επιπλοκές κατάλυσης πνευµονικών φλεβών Παναγιώτης Ιωαννίδης Διευθυντής Τµήµατος Αρρυθµιών & Επεµβατικής Ηλεκτροφυσιολογίας Βιοκλινικής Αθηνών ΣΕΜΙΝΑΡΙΑ ΟΜΑΔΩΝ ΕΡΓΑΣΙΑΣ Ιωάννινα, 27-2-2015 Solving an equation
Integration of CT and fluoroscopy images in the ablative treatment of atrial fibrillation
 Clinical applications Integration of CT and fluoroscopy images in the ablative treatment of atrial fibrillation C. Kriatselis M. Tang M. Roser J-H. erds-li E. leck Department of Internal Medicine/Cardiology,
Clinical applications Integration of CT and fluoroscopy images in the ablative treatment of atrial fibrillation C. Kriatselis M. Tang M. Roser J-H. erds-li E. leck Department of Internal Medicine/Cardiology,
480 April 2004 PACE, Vol. 27
 Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
Accepted Manuscript. Real Time MRI Guided Radiofrequency Atrial Ablation and Visualization of Lesion Formation at 3-Tesla
 Accepted Manuscript Real Time MRI Guided Radiofrequency Atrial Ablation and Visualization of Lesion Formation at 3-Tesla Gaston R. Vergara, Sathya Vijayakumar, Eugene G. Kholmovski, Joshua J.E. Blauer,
Accepted Manuscript Real Time MRI Guided Radiofrequency Atrial Ablation and Visualization of Lesion Formation at 3-Tesla Gaston R. Vergara, Sathya Vijayakumar, Eugene G. Kholmovski, Joshua J.E. Blauer,
Original Article Pulmonary vein isolation without left atrial mapping
 www.ipej.org 142 Original Article Pulmonary vein isolation without left atrial mapping Attila Kardos MD 1, Csaba Foldesi MD 1, Karoly Ladunga MSc, PhD 1, Attila Toth MD 2, Tamas Szili-Torok MD, PhD 1 1
www.ipej.org 142 Original Article Pulmonary vein isolation without left atrial mapping Attila Kardos MD 1, Csaba Foldesi MD 1, Karoly Ladunga MSc, PhD 1, Attila Toth MD 2, Tamas Szili-Torok MD, PhD 1 1
Catheter ablation of the pulmonary veins (PVs) is. Anatomic Relationship of the Esophagus and Left Atrium*
 Anatomic Relationship of the Esophagus and Left Atrium* Implication for Catheter Ablation of Atrial Fibrillation Hsuan-Ming Tsao, MD; Mei-Han Wu, MD; Satoshi Higa, MD; Kun-Tai Lee, MD; Ching-Tai Tai, MD;
Anatomic Relationship of the Esophagus and Left Atrium* Implication for Catheter Ablation of Atrial Fibrillation Hsuan-Ming Tsao, MD; Mei-Han Wu, MD; Satoshi Higa, MD; Kun-Tai Lee, MD; Ching-Tai Tai, MD;
New Magnetic Resonance Imaging-Based Method for Defining the Extent of Left Atrial Wall Injury After the Ablation of Atrial Fibrillation
 Journal of the American College of Cardiology Vol. 52, No. 15, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.05.062
Journal of the American College of Cardiology Vol. 52, No. 15, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.05.062
University of Groningen. Ablation of atrial fibrillation de Maat, Gijs Eduard
 University of Groningen Ablation of atrial fibrillation de Maat, Gijs Eduard IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Ablation of atrial fibrillation de Maat, Gijs Eduard IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Cardiac Imaging in abnormal rhythm Role of MDCT
 Cardiac Imaging in abnormal rhythm Role of MDCT Cardiac Imaging in abnormal rhythm Role of MDCT Scope of the problem CT in Atrial Fibrillation CT and pacing Ventricular arrhythmia Other applications 1
Cardiac Imaging in abnormal rhythm Role of MDCT Cardiac Imaging in abnormal rhythm Role of MDCT Scope of the problem CT in Atrial Fibrillation CT and pacing Ventricular arrhythmia Other applications 1
Ablation Lesion Assessment
 HRC 2016 Ablation Lesion Assessment The creation of effective and permanent lesions Ian Wright Imperial College Healthcare Wed 09:00-09:30 Hall 11 Objective Examine the role of existing strategies and
HRC 2016 Ablation Lesion Assessment The creation of effective and permanent lesions Ian Wright Imperial College Healthcare Wed 09:00-09:30 Hall 11 Objective Examine the role of existing strategies and
Raphael Rosso MD, Yuval Levi Med. Eng., Sami Viskin MD Tel Aviv Sourasky Medical Center
 Radiofrequency Ablation of Atrial Fibrillation: Comparison of Success Rate of Circular Ablation vs Point-by-Point Ablation with Contact Force Assessment in Paroxysmal and Persistent Atrial Fibrillation
Radiofrequency Ablation of Atrial Fibrillation: Comparison of Success Rate of Circular Ablation vs Point-by-Point Ablation with Contact Force Assessment in Paroxysmal and Persistent Atrial Fibrillation
Ο ΡOΛΟΣ ΤΗΣ ΑΠΕΙΚOΝΙΣΗΣ ΣΤΗΝ ΗΛΕΚΤΡΟΦΥΣΙΟΛΟΓIΑ - ΥΠΟΣΤΡΩΜΑ ΚΟΛΠΟΙ ΩΤΙΑ ΑΞΙΟΛΟΓΗΣΗ ΟΥΛΗΣ
 Ο ΡOΛΟΣ ΤΗΣ ΑΠΕΙΚOΝΙΣΗΣ ΣΤΗΝ ΗΛΕΚΤΡΟΦΥΣΙΟΛΟΓIΑ - ΥΠΟΣΤΡΩΜΑ ΚΟΛΠΟΙ ΩΤΙΑ ΑΞΙΟΛΟΓΗΣΗ ΟΥΛΗΣ Κώστας Παπαδόπουλος, Επιμ. Α Καρδιολογίας, Νοσοκομείο Ερυθρός Σταυρός ATRIA ANATOMY Complex anatomy Best knowledge
Ο ΡOΛΟΣ ΤΗΣ ΑΠΕΙΚOΝΙΣΗΣ ΣΤΗΝ ΗΛΕΚΤΡΟΦΥΣΙΟΛΟΓIΑ - ΥΠΟΣΤΡΩΜΑ ΚΟΛΠΟΙ ΩΤΙΑ ΑΞΙΟΛΟΓΗΣΗ ΟΥΛΗΣ Κώστας Παπαδόπουλος, Επιμ. Α Καρδιολογίας, Νοσοκομείο Ερυθρός Σταυρός ATRIA ANATOMY Complex anatomy Best knowledge
New magnetic resonance imaging based method to define. extent of left atrial wall injury after the ablation of atrial
 New magnetic resonance imaging based method to define extent of left atrial wall injury after the ablation of atrial fibrillation Christopher J. McGann MD 3, Eugene G. Kholmovski PhD 3, Robert S. Oakes
New magnetic resonance imaging based method to define extent of left atrial wall injury after the ablation of atrial fibrillation Christopher J. McGann MD 3, Eugene G. Kholmovski PhD 3, Robert S. Oakes
Case Report Asymptomatic Pulmonary Vein Stenosis: Hemodynamic Adaptation and Successful Ablation
 Case Reports in Cardiology Volume 2016, Article ID 4979182, 4 pages http://dx.doi.org/10.1155/2016/4979182 Case Report Asymptomatic Pulmonary Vein Stenosis: Hemodynamic Adaptation and Successful Ablation
Case Reports in Cardiology Volume 2016, Article ID 4979182, 4 pages http://dx.doi.org/10.1155/2016/4979182 Case Report Asymptomatic Pulmonary Vein Stenosis: Hemodynamic Adaptation and Successful Ablation
Atrial fibrillation (AF) is the most common sustained arrhythmia in adults and
 12 Chapter Atrial Fibrillation Ablation Atrial Fibrillation Ablation George Thomas, MD Amin Al-Ahmad, MD Executive Summary Atrial fibrillation (AF) is the most common sustained arrhythmia in adults and
12 Chapter Atrial Fibrillation Ablation Atrial Fibrillation Ablation George Thomas, MD Amin Al-Ahmad, MD Executive Summary Atrial fibrillation (AF) is the most common sustained arrhythmia in adults and
MRI of the left atrium: predicting clinical outcomes in patients with atrial fibrillation
 MRI of the left atrium: predicting clinical outcomes in patients with atrial fibrillation Expert Rev. Cardiovasc. Ther. 9(1), xxx xxx (2010) Marcos Daccarett 1, Chris J McGann 1, Nazem W Akoum 1, Rob S
MRI of the left atrium: predicting clinical outcomes in patients with atrial fibrillation Expert Rev. Cardiovasc. Ther. 9(1), xxx xxx (2010) Marcos Daccarett 1, Chris J McGann 1, Nazem W Akoum 1, Rob S
Velocity Vector Imaging as a new approach for cardiac magnetic resonance: Comparison with echocardiography
 Velocity Vector Imaging as a new approach for cardiac magnetic resonance: Comparison with echocardiography Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman 1,
Velocity Vector Imaging as a new approach for cardiac magnetic resonance: Comparison with echocardiography Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman 1,
Radiofrequency catheter ablation of atrial fibrillation (AF)
 Esophageal Capsule Endoscopy After Radiofrequency Catheter Ablation for Atrial Fibrillation Documented Higher Risk of Luminal Esophageal Damage With General Anesthesia as Compared With Conscious Sedation
Esophageal Capsule Endoscopy After Radiofrequency Catheter Ablation for Atrial Fibrillation Documented Higher Risk of Luminal Esophageal Damage With General Anesthesia as Compared With Conscious Sedation
Non Contrast MRA. Mayil Krishnam. Director, Cardiovascular and Thoracic Imaging University of California, Irvine
 Non Contrast MRA Mayil Krishnam Director, Cardiovascular and Thoracic Imaging University of California, Irvine No disclosures Non contrast MRA-Why? Limitations of CTA Radiation exposure Iodinated contrast
Non Contrast MRA Mayil Krishnam Director, Cardiovascular and Thoracic Imaging University of California, Irvine No disclosures Non contrast MRA-Why? Limitations of CTA Radiation exposure Iodinated contrast
5Real-time integration of
 5Real-time integration of intracardiac echocardiography and multi-slice computed tomography to guide radiofrequency catheter ablation for atrial fibrillation Dennis W. den Uijl 1 Laurens F. Tops 1 José
5Real-time integration of intracardiac echocardiography and multi-slice computed tomography to guide radiofrequency catheter ablation for atrial fibrillation Dennis W. den Uijl 1 Laurens F. Tops 1 José
Electrical disconnection of pulmonary vein (PV) myocardium
 Left Atrial Appendage Activity Masquerading as Pulmonary Vein Potentials Dipen Shah, MD; Michel Haissaguerre, MD; Pierre Jais, MD; Meleze Hocini, MD; Teiichi Yamane, MD; Laurent Macle, MD; Kee Joon Choi,
Left Atrial Appendage Activity Masquerading as Pulmonary Vein Potentials Dipen Shah, MD; Michel Haissaguerre, MD; Pierre Jais, MD; Meleze Hocini, MD; Teiichi Yamane, MD; Laurent Macle, MD; Kee Joon Choi,
Global left ventricular circumferential strain is a marker for both systolic and diastolic myocardial function
 Global left ventricular circumferential strain is a marker for both systolic and diastolic myocardial function Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman
Global left ventricular circumferential strain is a marker for both systolic and diastolic myocardial function Toshinari Onishi 1, Samir K. Saha 2, Daniel Ludwig 1, Erik B. Schelbert 1, David Schwartzman
Progression of atrial fibrillation: can we prevent it? Early catheter ablation will stop progression of atrial fibrillation pro
 Progression of atrial fibrillation: can we prevent it? Early catheter ablation will stop progression of atrial fibrillation pro Jerónimo Farré MD, Madrid, ES AF: the kingdom of wishful thinking In AF we
Progression of atrial fibrillation: can we prevent it? Early catheter ablation will stop progression of atrial fibrillation pro Jerónimo Farré MD, Madrid, ES AF: the kingdom of wishful thinking In AF we
Circumferential Pulmonary-Vein Ablation for Chronic Atrial Fibrillation
 The new england journal of medicine original article Circumferential Pulmonary-Vein Ablation for Chronic Atrial Fibrillation Hakan Oral, M.D., Carlo Pappone, M.D., Aman Chugh, M.D., Eric Good, D.O., Frank
The new england journal of medicine original article Circumferential Pulmonary-Vein Ablation for Chronic Atrial Fibrillation Hakan Oral, M.D., Carlo Pappone, M.D., Aman Chugh, M.D., Eric Good, D.O., Frank
The Who, What, Why, and How-To Guide for Circumferential Pulmonary Vein Ablation
 1226 TECHNIQUES AND TECHNOLOGY Editor: Hugh Calkins, M.D. The Who, What, Why, and How-To Guide for Circumferential Pulmonary Vein Ablation CARLO PAPPONE, M.D., PH.D., and VINCENZO SANTINELLI, M.D. From
1226 TECHNIQUES AND TECHNOLOGY Editor: Hugh Calkins, M.D. The Who, What, Why, and How-To Guide for Circumferential Pulmonary Vein Ablation CARLO PAPPONE, M.D., PH.D., and VINCENZO SANTINELLI, M.D. From
From the Comprehensive Arrhythmia and Research Management (CARMA) Center, University of Utah School of Medicine, Salt Lake City, Utah.
 Evaluation of the left atrial substrate in patients with lone atrial fibrillation using delayed-enhanced MRI: Implications for disease progression and response to catheter ablation Christian Mahnkopf,
Evaluation of the left atrial substrate in patients with lone atrial fibrillation using delayed-enhanced MRI: Implications for disease progression and response to catheter ablation Christian Mahnkopf,
LA Debulking for Atrial Fibrillation. Introduction: Though pulmonary vein (PV) isolation has
 1 Magnetic Resonance Imaging-Confirmed Ablative Debulking of the Left Atrial Posterior Wall and Septum for Treatment of Persistent Atrial Fibrillation: Rationale and Initial Experience NATHAN M. SEGERSON,
1 Magnetic Resonance Imaging-Confirmed Ablative Debulking of the Left Atrial Posterior Wall and Septum for Treatment of Persistent Atrial Fibrillation: Rationale and Initial Experience NATHAN M. SEGERSON,
LA Debulking for Atrial Fibrillation. Introduction: Though pulmonary vein (PV) isolation has
 126 Magnetic Resonance Imaging-Confirmed Ablative Debulking of the Left Atrial Posterior Wall and Septum for Treatment of Persistent Atrial Fibrillation: Rationale and Initial Experience NATHAN M. SEGERSON,
126 Magnetic Resonance Imaging-Confirmed Ablative Debulking of the Left Atrial Posterior Wall and Septum for Treatment of Persistent Atrial Fibrillation: Rationale and Initial Experience NATHAN M. SEGERSON,
Does the left atrial appendage morphology correlates with the risk of stroke in patients with atrial fibrillation? Result from a multicenter study.
 Does the left atrial appendage morphology correlates with the risk of stroke in patients with atrial fibrillation? Result from a multicenter study. Luigi Di Biase, MD, PhD, Fiorenzo Gaita, MD, Ilaria Salvetti,
Does the left atrial appendage morphology correlates with the risk of stroke in patients with atrial fibrillation? Result from a multicenter study. Luigi Di Biase, MD, PhD, Fiorenzo Gaita, MD, Ilaria Salvetti,
Characteristics of Rapid Rhythms Recorded Within Pulmonary Veins During Atrial Fibrillation
 Characteristics of Rapid Rhythms Recorded Within Pulmonary Veins During Atrial Fibrillation HIROSHI TADA, MEHMET ÖZAYDIN, HAKAN ORAL, BRADLEY P. KNIGHT, AMAN CHUGH, CHRISTOPH SCHARF, FRANK PELOSI, Jr.,
Characteristics of Rapid Rhythms Recorded Within Pulmonary Veins During Atrial Fibrillation HIROSHI TADA, MEHMET ÖZAYDIN, HAKAN ORAL, BRADLEY P. KNIGHT, AMAN CHUGH, CHRISTOPH SCHARF, FRANK PELOSI, Jr.,
Impaired Regional Myocardial Function Detection Using the Standard Inter-Segmental Integration SINE Wave Curve On Magnetic Resonance Imaging
 Original Article Impaired Regional Myocardial Function Detection Using the Standard Inter-Segmental Integration Ngam-Maung B, RT email : chaothawee@yahoo.com Busakol Ngam-Maung, RT 1 Lertlak Chaothawee,
Original Article Impaired Regional Myocardial Function Detection Using the Standard Inter-Segmental Integration Ngam-Maung B, RT email : chaothawee@yahoo.com Busakol Ngam-Maung, RT 1 Lertlak Chaothawee,
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
New technology to minimize radiation
 Room 103-104 15/April/2016 New technology to minimize radiation Jun Kim University of Ulsan College of Medicine Asan Medical Center Heart Institute Disclosure NONE I have no experience using Carto Univu
Room 103-104 15/April/2016 New technology to minimize radiation Jun Kim University of Ulsan College of Medicine Asan Medical Center Heart Institute Disclosure NONE I have no experience using Carto Univu
Faletti et al. Journal of Cardiovascular Magnetic Resonance 2014, 16:41
 Faletti et al. Journal of Cardiovascular Magnetic Resonance 2014, 16:41 TECHNICAL NOTES Open Access Use of oral gadobenate dimeglumine to visualise the oesophagus during magnetic resonance angiography
Faletti et al. Journal of Cardiovascular Magnetic Resonance 2014, 16:41 TECHNICAL NOTES Open Access Use of oral gadobenate dimeglumine to visualise the oesophagus during magnetic resonance angiography
Journal of the American College of Cardiology Vol. 57, No. 7, by the American College of Cardiology Foundation ISSN /$36.
 Journal of the American College of Cardiology Vol. 57, No. 7, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2010.09.049
Journal of the American College of Cardiology Vol. 57, No. 7, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2010.09.049
Balloon and Mesh Catheter Ablation of Pulmonary Veins
 Balloon and Mesh Catheter Ablation of Pulmonary Veins ISHNE 2009 Atul Verma, MD FRCPC Cardiology/Electrophysiology Heart Rhythm Program, Division of Cardiology Southlake Regional Health Centre Newmarket,
Balloon and Mesh Catheter Ablation of Pulmonary Veins ISHNE 2009 Atul Verma, MD FRCPC Cardiology/Electrophysiology Heart Rhythm Program, Division of Cardiology Southlake Regional Health Centre Newmarket,
Since pulmonary veins (PVs) have
 Case Report Hellenic J Cardiol 2011; 52: 371-376 Left Atrial-Pulmonary Vein Reentrant Tachycardia Following Pulmonary Vein Isolation Dionyssios Leftheriotis, Feifan Ouyang, Karl-Heinz Kuck II. Med. Abteilung,
Case Report Hellenic J Cardiol 2011; 52: 371-376 Left Atrial-Pulmonary Vein Reentrant Tachycardia Following Pulmonary Vein Isolation Dionyssios Leftheriotis, Feifan Ouyang, Karl-Heinz Kuck II. Med. Abteilung,
Imaging and Diagnostic Testing
 Imaging and Diagnostic Testing Echocardiographic left atrial reverse remodeling after catheter ablation of atrial fibrillation is predicted by preablation delayed enhancement of left atrium by magnetic
Imaging and Diagnostic Testing Echocardiographic left atrial reverse remodeling after catheter ablation of atrial fibrillation is predicted by preablation delayed enhancement of left atrium by magnetic
Clinical Value of Noninducibility by High-Dose Isoproterenol Versus Rapid Atrial Pacing After Catheter Ablation of Paroxysmal Atrial Fibrillation
 13 Clinical Value of Noninducibility by High-Dose Isoproterenol Versus Rapid Atrial Pacing After Catheter Ablation of Paroxysmal Atrial Fibrillation THOMAS CRAWFORD, M.D., AMAN CHUGH, M.D., ERIC GOOD,
13 Clinical Value of Noninducibility by High-Dose Isoproterenol Versus Rapid Atrial Pacing After Catheter Ablation of Paroxysmal Atrial Fibrillation THOMAS CRAWFORD, M.D., AMAN CHUGH, M.D., ERIC GOOD,
Correspondence should be addressed to Sang Jin Lee;
 Hindawi Publishing Corporation Case Reports in Gastrointestinal Medicine Volume 2014, Article ID 923637, 6 pages http://dx.doi.org/10.1155/2014/923637 Case Report Severe Gastroparesis following Radiofrequency
Hindawi Publishing Corporation Case Reports in Gastrointestinal Medicine Volume 2014, Article ID 923637, 6 pages http://dx.doi.org/10.1155/2014/923637 Case Report Severe Gastroparesis following Radiofrequency
Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm
 Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm AMAN CHUGH, MEHMET OZAYDIN, CHRISTOPH SCHARF, STEVE W.K. LAI, BURR HALL, PETER CHEUNG, FRANK PELOSI, JR, BRADLEY
Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm AMAN CHUGH, MEHMET OZAYDIN, CHRISTOPH SCHARF, STEVE W.K. LAI, BURR HALL, PETER CHEUNG, FRANK PELOSI, JR, BRADLEY
MR coronary artery imaging with 3D motion adapted gating (MAG) in comparison to a standard prospective navigator technique
 Journal of Cardiovascular Magnetic Resonance (2005) 7, 793 797 Copyright D 2005 Taylor & Francis Inc. ISSN: 1097-6647 print / 1532-429X online DOI: 10.1080/10976640500287547 ANGIOGRAPHY MR coronary artery
Journal of Cardiovascular Magnetic Resonance (2005) 7, 793 797 Copyright D 2005 Taylor & Francis Inc. ISSN: 1097-6647 print / 1532-429X online DOI: 10.1080/10976640500287547 ANGIOGRAPHY MR coronary artery
The pulmonary veins have been demonstrated to often
 Pulmonary Vein Isolation for Paroxysmal and Persistent Atrial Fibrillation Hakan Oral, MD; Bradley P. Knight, MD; Hiroshi Tada, MD; Mehmet Özaydın, MD; Aman Chugh, MD; Sohail Hassan, MD; Christoph Scharf,
Pulmonary Vein Isolation for Paroxysmal and Persistent Atrial Fibrillation Hakan Oral, MD; Bradley P. Knight, MD; Hiroshi Tada, MD; Mehmet Özaydın, MD; Aman Chugh, MD; Sohail Hassan, MD; Christoph Scharf,
MR Advance Techniques. Vascular Imaging. Class II
 MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
MR Advance Techniques Vascular Imaging Class II 1 Vascular Imaging There are several methods that can be used to evaluate the cardiovascular systems with the use of MRI. MRI will aloud to evaluate morphology
Noninducibility of Atrial Fibrillation as an End Point of Left Atrial Circumferential Ablation for Paroxysmal Atrial Fibrillation A Randomized Study
 Noninducibility of Atrial Fibrillation as an End Point of Left Atrial Circumferential Ablation for Paroxysmal Atrial Fibrillation A Randomized Study Hakan Oral, MD; Aman Chugh, MD; Kristina Lemola, MD;
Noninducibility of Atrial Fibrillation as an End Point of Left Atrial Circumferential Ablation for Paroxysmal Atrial Fibrillation A Randomized Study Hakan Oral, MD; Aman Chugh, MD; Kristina Lemola, MD;
Image integration in catheter ablation of atrial fibrillation
 Europace (2008) 10, iii48 iii56 doi:10.1093/europace/eun235 Image integration in catheter ablation of atrial fibrillation Laurens F. Tops 1,2 *, Martin J. Schalij 2, Dennis W. den Uijl 2, Theodore P. Abraham
Europace (2008) 10, iii48 iii56 doi:10.1093/europace/eun235 Image integration in catheter ablation of atrial fibrillation Laurens F. Tops 1,2 *, Martin J. Schalij 2, Dennis W. den Uijl 2, Theodore P. Abraham
CLINICAL COMPENDIUM. The HeartLight Endoscopic Ablation System Putting a New Level of PVI Precision Close at Hand. CardioFocus.com
 CLINICAL COMPENDIUM The HeartLight Endoscopic Ablation System Putting a New Level of PVI Precision Close at Hand CardioFocus.com Published results summarized in this compendium may include references to
CLINICAL COMPENDIUM The HeartLight Endoscopic Ablation System Putting a New Level of PVI Precision Close at Hand CardioFocus.com Published results summarized in this compendium may include references to
Cardiovascular Magnetic Resonance Imaging of Scar Development Following Pulmonary Vein Isolation: A Prospective Study
 Cardiovascular Magnetic Resonance Imaging of Scar Development Following Pulmonary Vein Isolation: A Prospective Study The Harvard community has made this article openly available. Please share how this
Cardiovascular Magnetic Resonance Imaging of Scar Development Following Pulmonary Vein Isolation: A Prospective Study The Harvard community has made this article openly available. Please share how this
Echo assessment of the failing heart
 Echo assessment of the failing heart Mark K. Friedberg, MD The Labatt Family Heart Center The Hospital for Sick Children Toronto, Ontario, Canada Cardiac function- definitions Cardiovascular function:
Echo assessment of the failing heart Mark K. Friedberg, MD The Labatt Family Heart Center The Hospital for Sick Children Toronto, Ontario, Canada Cardiac function- definitions Cardiovascular function:
Should hybrid ablation be the standard of care instead of transcatheter ablation techniques?
 Should hybrid ablation be the standard of care instead of transcatheter ablation techniques? Christian Shults, MD Assistant Professor, Georgetown University School of Medicine Cardiac Surgeon, Medstar
Should hybrid ablation be the standard of care instead of transcatheter ablation techniques? Christian Shults, MD Assistant Professor, Georgetown University School of Medicine Cardiac Surgeon, Medstar
Advanced imaging of the left atrium - strain, CT, 3D, MRI -
 Advanced imaging of the left atrium - strain, CT, 3D, MRI - Monica Rosca, MD Carol Davila University of Medicine and Pharmacy, Bucharest, Romania Declaration of interest: I have nothing to declare Case
Advanced imaging of the left atrium - strain, CT, 3D, MRI - Monica Rosca, MD Carol Davila University of Medicine and Pharmacy, Bucharest, Romania Declaration of interest: I have nothing to declare Case
Evidence for Longitudinal and Transverse Fiber Conduction in Human Pulmonary Veins
 Evidence for Longitudinal and Transverse Fiber Conduction in Human Pulmonary Veins Relevance for Catheter Ablation Javier E. Sanchez, MD; Vance J. Plumb, MD; Andrew E. Epstein, MD; G. Neal Kay, MD Background
Evidence for Longitudinal and Transverse Fiber Conduction in Human Pulmonary Veins Relevance for Catheter Ablation Javier E. Sanchez, MD; Vance J. Plumb, MD; Andrew E. Epstein, MD; G. Neal Kay, MD Background
Case Report Epicardial Ablation: Prevention of Phrenic Nerve Damage by Pericardial Injection of Saline and the Use of a Steerable Sheath
 87 Case Report Epicardial Ablation: Prevention of Phrenic Nerve Damage by Pericardial Injection of Saline and the Use of a Steerable Sheath Kars Neven, MD 1, Juan Fernández-Armenta, MD 2, David Andreu,
87 Case Report Epicardial Ablation: Prevention of Phrenic Nerve Damage by Pericardial Injection of Saline and the Use of a Steerable Sheath Kars Neven, MD 1, Juan Fernández-Armenta, MD 2, David Andreu,
Radiofrequency Ablation vs Antiarrhythmic Drugs as First-line Treatment of Symptomatic Atrial Fibrillation JAMA. 2005;293:
 PRELIMINARY COMMUNICATION Radiofrequency Ablation vs Antiarrhythmic Drugs as First-line Treatment of Symptomatic Atrial Fibrillation A Randomized Trial Oussama M. Wazni, MD Nassir F. Marrouche, MD David
PRELIMINARY COMMUNICATION Radiofrequency Ablation vs Antiarrhythmic Drugs as First-line Treatment of Symptomatic Atrial Fibrillation A Randomized Trial Oussama M. Wazni, MD Nassir F. Marrouche, MD David
Atrial Fibrillation Ablation Using a Robotic Catheter Remote Control System
 Journal of the American College of Cardiology Vol. 51, No. 25, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.03.027
Journal of the American College of Cardiology Vol. 51, No. 25, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.03.027
Functional Chest MRI in Children Hyun Woo Goo
 Functional Chest MRI in Children Hyun Woo Goo Department of Radiology and Research Institute of Radiology Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea No ionizing radiation
Functional Chest MRI in Children Hyun Woo Goo Department of Radiology and Research Institute of Radiology Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea No ionizing radiation
Catheter Ablation of Atrial Fibrillation in Patients with Prosthetic Mitral Valve
 Catheter Ablation of Atrial Fibrillation in Patients with Prosthetic Mitral Valve Luigi Di Biase, MD, PhD, FHRS Senior Researcher Texas Cardiac Arrhythmia Institute at St. David s Medical Center, Austin,
Catheter Ablation of Atrial Fibrillation in Patients with Prosthetic Mitral Valve Luigi Di Biase, MD, PhD, FHRS Senior Researcher Texas Cardiac Arrhythmia Institute at St. David s Medical Center, Austin,
MR Advance Techniques. Cardiac Imaging. Class IV
 MR Advance Techniques Cardiac Imaging Class IV Heart The heart is a muscular organ responsible for pumping blood through the blood vessels by repeated, rhythmic contractions. Layers of the heart Endocardium
MR Advance Techniques Cardiac Imaging Class IV Heart The heart is a muscular organ responsible for pumping blood through the blood vessels by repeated, rhythmic contractions. Layers of the heart Endocardium
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Atrial ectopic beats within the pulmonary veins (PVs) are
 Phased-Array Intracardiac Echocardiography Monitoring During Pulmonary Vein Isolation in Patients With Atrial Fibrillation Impact on Outcome and Complications Nassir F. Marrouche, MD; David O. Martin,
Phased-Array Intracardiac Echocardiography Monitoring During Pulmonary Vein Isolation in Patients With Atrial Fibrillation Impact on Outcome and Complications Nassir F. Marrouche, MD; David O. Martin,
This overview was prepared in October 2011, and updated in March 2012.
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous balloon cryoablation for pulmonary vein isolation in atrial fibrillation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous balloon cryoablation for pulmonary vein isolation in atrial fibrillation
From the Division of Cardiology, Department of Internal Medicine, University of Michigan Medical Center, Ann Arbor, Michigan
 118 Reprinted with permission from JOURNAL OF CARDIOVASCULAR ELECTROPHYSIOLOGY, Volume 13, No. 2, February 2002 Copyright 2002 by Futura Publishing Company, Inc., Armonk, NY 10504-0418 Differentiation
118 Reprinted with permission from JOURNAL OF CARDIOVASCULAR ELECTROPHYSIOLOGY, Volume 13, No. 2, February 2002 Copyright 2002 by Futura Publishing Company, Inc., Armonk, NY 10504-0418 Differentiation
 2004 3 32 3 Chin J Cardiol, March 2004, Vol. 32 No. 3 211 4 ( ) 4 (HRA) (CS), 10 (Lasso ),, 4 (3 ) (1 ), 118,3,1, 417, ; ; The electrophysiological characteristics and ablation treatment of patients with
2004 3 32 3 Chin J Cardiol, March 2004, Vol. 32 No. 3 211 4 ( ) 4 (HRA) (CS), 10 (Lasso ),, 4 (3 ) (1 ), 118,3,1, 417, ; ; The electrophysiological characteristics and ablation treatment of patients with
Is cardioversion old hat? What is new in interventional treatment of AF symptoms?
 Is cardioversion old hat? What is new in interventional treatment of AF symptoms? Joseph de Bono Consultant Electrophysiologist University Hospitals Birmingham Atrial Fibrillation (AF) Affects 2% of the
Is cardioversion old hat? What is new in interventional treatment of AF symptoms? Joseph de Bono Consultant Electrophysiologist University Hospitals Birmingham Atrial Fibrillation (AF) Affects 2% of the
Atrial fibrillation is the most common cause of arrhythmia in humans. It contributes
 Cardiopulmonary Support and Physiology Ablation of atrial fibrillation and esophageal injury: Effects of energy source and ablation technique Heike Aupperle, DVM, a Nicolas Doll, MD, PhD, b Thomas Walther,
Cardiopulmonary Support and Physiology Ablation of atrial fibrillation and esophageal injury: Effects of energy source and ablation technique Heike Aupperle, DVM, a Nicolas Doll, MD, PhD, b Thomas Walther,
Atrial Fibrillation Ablation: in Whom and How
 Update on Consensus Statement on Management of Atrial Fibrillation: EHRA 2012 Atrial Fibrillation Ablation: in Whom and How Update of HRS/EHRA AF/ECAS Ablation Document 2012 Anne M Gillis MD FHRS Professor
Update on Consensus Statement on Management of Atrial Fibrillation: EHRA 2012 Atrial Fibrillation Ablation: in Whom and How Update of HRS/EHRA AF/ECAS Ablation Document 2012 Anne M Gillis MD FHRS Professor
Catheter Ablation of Atrial Fibrillation
 Cardiology Update 2011 Catheter Ablation of Atrial Fibrillation Laurent Haegeli University Hospital Zurich February 16, 2011 Willem Einthoven and Sir Thomas Lewis The first ECG in 1903 Willem Einthoven
Cardiology Update 2011 Catheter Ablation of Atrial Fibrillation Laurent Haegeli University Hospital Zurich February 16, 2011 Willem Einthoven and Sir Thomas Lewis The first ECG in 1903 Willem Einthoven
Pulmonary Vein Antral Isolation Using an Open Irrigation Ablation Catheter for the Treatment of Atrial Fibrillation
 Journal of the American College of Cardiology Vol. 49, No. 15, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.12.041
Journal of the American College of Cardiology Vol. 49, No. 15, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.12.041
Essentials of Clinical MR, 2 nd edition. 99. MRA Principles and Carotid MRA
 99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
99. MRA Principles and Carotid MRA As described in Chapter 12, time of flight (TOF) magnetic resonance angiography (MRA) is commonly utilized in the evaluation of the circle of Willis. TOF MRA allows depiction
Time to recurrence of atrial fibrillation influences outcome following catheter ablation
 Time to recurrence of atrial fibrillation influences outcome following catheter ablation Larraitz Gaztañaga, MD, David S. Frankel, MD, Maria Kohari, MD, Lavanya Kondapalli, MD, Erica S. Zado, PA-C, FHRS,
Time to recurrence of atrial fibrillation influences outcome following catheter ablation Larraitz Gaztañaga, MD, David S. Frankel, MD, Maria Kohari, MD, Lavanya Kondapalli, MD, Erica S. Zado, PA-C, FHRS,
Low Incidence of Esophageal Lesions After Pulmonary Vein Isolation Using Contact-Force Sensing Catheter Without Esophageal Temperature Probe
 CLINICAL STUDY Low Incidence of Esophageal Lesions After Pulmonary Vein Isolation Using Contact-Force Sensing Catheter Without Esophageal Temperature Probe Christian Blockhaus, 1 MD, Patrick Müller, 1
CLINICAL STUDY Low Incidence of Esophageal Lesions After Pulmonary Vein Isolation Using Contact-Force Sensing Catheter Without Esophageal Temperature Probe Christian Blockhaus, 1 MD, Patrick Müller, 1
Ankara, Turkey 2 Department of Cardiology, Division of Arrhythmia and Electrophysiology, Yuksek Ihtisas
 258 Case Report Electroanatomic Mapping-Guided Radiofrequency Ablation of Adenosine Sensitive Incessant Focal Atrial Tachycardia Originating from the Non-Coronary Aortic Cusp in a Child Serhat Koca, MD
258 Case Report Electroanatomic Mapping-Guided Radiofrequency Ablation of Adenosine Sensitive Incessant Focal Atrial Tachycardia Originating from the Non-Coronary Aortic Cusp in a Child Serhat Koca, MD
The Effect of Fat Pad Modification during Ablation of Atrial Fibrillation: Late Gadolinium Enhancement MRI Analysis
 The Effect of Fat Pad Modification during Ablation of Atrial Fibrillation: Late Gadolinium Enhancement MRI Analysis KOJI HIGUCHI, M.D., MEHMET AKKAYA, M.D., MATTHIAS KOOPMANN, M.D., JOSHUA J.E. BLAUER,
The Effect of Fat Pad Modification during Ablation of Atrial Fibrillation: Late Gadolinium Enhancement MRI Analysis KOJI HIGUCHI, M.D., MEHMET AKKAYA, M.D., MATTHIAS KOOPMANN, M.D., JOSHUA J.E. BLAUER,
Prevalence of Asymptomatic Recurrences of Atrial Fibrillation After Successful Radiofrequency Catheter Ablation
 920 Prevalence of Asymptomatic Recurrences of Atrial Fibrillation After Successful Radiofrequency Catheter Ablation HAKAN ORAL, M.D., SRIKAR VEERAREDDY, M.D., ERIC GOOD, D.O., BURR HALL, M.D., PETER CHEUNG,
920 Prevalence of Asymptomatic Recurrences of Atrial Fibrillation After Successful Radiofrequency Catheter Ablation HAKAN ORAL, M.D., SRIKAR VEERAREDDY, M.D., ERIC GOOD, D.O., BURR HALL, M.D., PETER CHEUNG,
A Magnetic Resonance Imaging Method for
 Journal of Cardiovascular Magnetic Resonance, 1(1), 59-64 (1999) INVITED PAPER Use of MRI in ASD Asessment A Magnetic Resonance Imaging Method for Evaluating Atrial Septa1 Defects Godtfred Holmvang Cardiac
Journal of Cardiovascular Magnetic Resonance, 1(1), 59-64 (1999) INVITED PAPER Use of MRI in ASD Asessment A Magnetic Resonance Imaging Method for Evaluating Atrial Septa1 Defects Godtfred Holmvang Cardiac
Atrial fibrillation ablation in patients with known sludge in the left atrial appendage
 J Interv Card Electrophysiol (2014) 40:147 151 DOI 10.1007/s10840-014-9892-0 Atrial fibrillation ablation in patients with known sludge in the left atrial appendage Mohammed Hajjiri & Scott Bernstein &
J Interv Card Electrophysiol (2014) 40:147 151 DOI 10.1007/s10840-014-9892-0 Atrial fibrillation ablation in patients with known sludge in the left atrial appendage Mohammed Hajjiri & Scott Bernstein &
Clinical Applications
 C H A P T E R 16 Clinical Applications In selecting pulse sequences and measurement parameters for a specific application, MRI allows the user tremendous flexibility to produce variations in contrast between
C H A P T E R 16 Clinical Applications In selecting pulse sequences and measurement parameters for a specific application, MRI allows the user tremendous flexibility to produce variations in contrast between
The influence of varying energy settings on efficacy and safety of endoscopic pulmonary vein isolation
 The influence of varying energy settings on efficacy and safety of endoscopic pulmonary vein isolation Andreas Metzner, MD,* Erik Wissner, MD, FHRS,* Bas Schoonderwoerd, MD,* Andre Burchard, MD, Roland
The influence of varying energy settings on efficacy and safety of endoscopic pulmonary vein isolation Andreas Metzner, MD,* Erik Wissner, MD, FHRS,* Bas Schoonderwoerd, MD,* Andre Burchard, MD, Roland
Paroxysmal atrial fibrillation (AF) is often triggered by
 Acute Pulmonary Vein Isolation Is Achieved by a Combination of Reversible and Irreversible Atrial Injury After Catheter Ablation Evidence From Magnetic Resonance Imaging Aruna Arujuna, MBChB, MRCP; Rashed
Acute Pulmonary Vein Isolation Is Achieved by a Combination of Reversible and Irreversible Atrial Injury After Catheter Ablation Evidence From Magnetic Resonance Imaging Aruna Arujuna, MBChB, MRCP; Rashed
Understanding Atrial Fibrillation
 Understanding Atrial Fibrillation Todd J. Florin, M.D. Table of Contents The Normal Heart...1 What is Atrial Fibrillation...3 Risks of Afib: Stroke...5 Treatment Options...7 Radiofrequency Ablation...9
Understanding Atrial Fibrillation Todd J. Florin, M.D. Table of Contents The Normal Heart...1 What is Atrial Fibrillation...3 Risks of Afib: Stroke...5 Treatment Options...7 Radiofrequency Ablation...9
Storia dell ablazione della fibrillazione atriale: da dove siamo partiti, dove siamo, dove andremo. Prof. Fiorenzo Gaita
 Storia dell ablazione della fibrillazione atriale: da dove siamo partiti, dove siamo, dove andremo Prof. Fiorenzo Gaita Knowledge Idea Serendipity Technology (right tools) Serendipity - discovery of a
Storia dell ablazione della fibrillazione atriale: da dove siamo partiti, dove siamo, dove andremo Prof. Fiorenzo Gaita Knowledge Idea Serendipity Technology (right tools) Serendipity - discovery of a
Catheter ablation of atrial fibrillation: Indications and tools for improvement of the success rate of the method. Konstantinos P.
 Ioannina 2015 Catheter ablation of atrial fibrillation: Indications and tools for improvement of the success rate of the method Konstantinos P. Letsas, MD, FESC SECOND DEPARTMENT OF CARDIOLOGY LABORATORY
Ioannina 2015 Catheter ablation of atrial fibrillation: Indications and tools for improvement of the success rate of the method Konstantinos P. Letsas, MD, FESC SECOND DEPARTMENT OF CARDIOLOGY LABORATORY
High-Resolution MR Angiography: Results in Diseased Arteries
 IAGS Proceedings NEW IMAGING FOR NEW AND OLD DISEASES High-Resolution MR Angiography: Results in Diseased Arteries Peter Gonschior, M D, Ingo Pragst, M D, Gregor Valassis, M D, Claudia Vo g e l - Wiens,
IAGS Proceedings NEW IMAGING FOR NEW AND OLD DISEASES High-Resolution MR Angiography: Results in Diseased Arteries Peter Gonschior, M D, Ingo Pragst, M D, Gregor Valassis, M D, Claudia Vo g e l - Wiens,
Intracardiac Echocardiography in Premature Ventricular Complex/Ventricular Tachycardia Ablation
 Intracardiac Echocardiography in Premature Ventricular Complex/Ventricular Tachycardia Ablation Tae-Seok Kim Sung-Hwan Kim ECG & EP CASES Tae-Seok Kim, MD, Sung-Hwan Kim, MD Department of Internal Medicine,
Intracardiac Echocardiography in Premature Ventricular Complex/Ventricular Tachycardia Ablation Tae-Seok Kim Sung-Hwan Kim ECG & EP CASES Tae-Seok Kim, MD, Sung-Hwan Kim, MD Department of Internal Medicine,
Planning study for minimally invasive cardiac arrhythmias ablation with intensity modulation proton therapy Vennarini Sabina
 Planning study for minimally invasive cardiac arrhythmias ablation with intensity modulation proton therapy Vennarini Sabina (sabina.vennarini@apss.tn.it) Introduction Atrial Fibrillation (AF): most common
Planning study for minimally invasive cardiac arrhythmias ablation with intensity modulation proton therapy Vennarini Sabina (sabina.vennarini@apss.tn.it) Introduction Atrial Fibrillation (AF): most common
