Heart-Lung Transplantation for Irreversible Pulimonary Hypertension
|
|
|
- Nancy Small
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLES Heart-Lung Transplantation for Irreversible Pulimonary Hypertension S. W. Jamieson, M.B., F.R.C.S., E. B. Stinson, M.D., P. E. Oyer, M.D., Ph.D., B. A. Reitz, M.D., J. Baldwin, M.D., D. Modry, M.D., K. Dawkins, M.B., J. Theodore, M.D., S. Hunt, M.D., and N. E. Shumway, M.D., Ph.D. ABSTRACT Combined heart and lung transplantation was carried out in 17 patients at Stanford University between March, 1981, and December, The recipients were between 22 and 45 years old. All patients had endstage pulmonary hypertension; ;LO had Eisenmenger s syndrome and the remaining 7, primary pulmonary hypertension. Five patients died within the first few postoperative weeks. The remainder are well between four weeks and 33 months from operation. The immunosuppressive protocol has consisted of cyclosporine with an initial coursc of rabbit antithymocyte globulin. Azathioprine also was given for the first two weeks and then was replaced with prednisone. Rejection, as diagnosed by cardiac biopsy, was treated with high doses of methylprednisolone. Modifications of technique that have developed include the removal of the recipient heart and lungs separately, and l~reservation of the lungs with a modified Collins solution instead of a cardioplegic solution. Rejection occurred in 6 of the 12 survivors. Infections developed in 9 patients, but only one resulted in a fatal outcome (Legionella). Thus, the results of clinical heartlung transplantation have been considerably superior to clinical efforts in lung transplantation. It is suggested that the combined operation is preferable for the following reasons: (1) all diseased tissue is removed, thus eliminating recurrent infection and ventilatioidperfusion disparity; (2) transplantation of the entire heart-lung block preserves coronary-bronchial vascular anastomoses and makes airway dehiscence less likely; and (3) to date, diagnosis of rejection by cardiac biopsy has appeared to be a satisfactory method of diagnosing and taeating pulmonary rejection. Cardiopulmonary transplantation represents a viable therapeutic approach for patients with end-stage pulmonary hypertension with or without associated congenital heart disease. Demikhov [l] was among the first to perform successful experimental heart-lung transplantation operations. In the 1940s, he transplanted the heart and lungs in dogs From the Department of Cardiovascular Surgery, Stanford University Medical Center, Stanford, CA. The annual J. Maxwell Chamberlain Memcrial Paper, presented at the Twentieth Annual Meeting of The Society of Thoracic Surgeons, San Antonio, TX, Jan 23-25, Address reprint requests to Dr. Jamieson, Department of Cardiovascular Surgery, Stanford University Medical Center, Stanford, CA without the use of either hypothermia or cardiopulmonary bypass by making the appropriate vascular connections with the recipient s heart and lungs in place and later excluding them from the circulation. He constructed separate anastomoses for the right and left bronchi. Respiratory difficulties, notably related to the respiratory pattern, were responsible for death in the majority of dogs, and only 2 out of a total of 67 animals survived for 5 days. The heart and lungs are denervated after transplantation, and it became apparent that the dog was greatly dependent on pulmonary afferent nerves for respiratory control. In 1953, Neptune and colleagues [2] used central cooling with circulatory arrest to perform heart-lung transplantation in dogs, with survival for up to 6 hours. In 1957, Webb and Howard [3] reported six cardiopulmonary transplants using cardiopulmonary bypass in dogs, with survival ranging from 75 minutes to 22 hours. Again, a failure to resume spontaneous respiration was noted, and they suggested the possibility of cardiac and unilateral lung transplantation for clinical application t4, 51. In 1961, Lower and associates [6] achieved 6-day survival in dogs but noted that denervation led to increased tidal volumes and a slowed respiratory rate with long periods of apnea. Nine years later, Grinnan and coworkers [7] accomplished transplantation in 1 dog (out of 25) that lived for 10 days. These early experiments demonstrated that combined heart and lung transplantation was technically feasible and that a few animals would maintain enough spontaneous respiratory effort to survive for short periods. However, cardiopulmonary transplantation in dogs has never resulted in long-term survival. Haglin and co-workers [8] showed that denervation of both lungs was not compatible with long-term survival in dogs but that this was not the case in primates. Nakae and co-workers [9] also demonstrated a species difference in regard to pulmonary innervation, and reported that disruption of pulmonary afferent nerves in cats and dogs was not compatible with survival but that monkeys maintained a normal respiratory pattern. One of the first clinical heart-lung transplant operations was carried out in 1968, in a 2-month old infant with a complete atrioventricular canal defect [lo]. The child died 14 hours after operation, but it was noted that spontaneous respiration recurred. Another clinical transplant was performed in 1970 on a 43-year-old man with emphysema [ll]. He died of progressive respiratory failure after 8 days. A patient with chronic obstructive lung disease underwent combined heart and lung 554
2 555 Jamieson et al: Heart-Lung Transplantation for Irreversible Pulmonary Hypertension transplantation in 1971 [12]. The 49-year-old patient survived for 23 days after operation. In 1972, long-term survivors of cardiopulmonary transplantation were reported by Castaneda and colleagues [13], who studied autotransplants in baboons. Five of 25 animals lived as long as two years [14]. The advent of cyclosporine [15] as an immunosuppressant heralded the present era of successful cardiopulmonary allotransplantation. This drug provides superior immunosuppression to azathioprine and steroids combined [ 161 and allows adequate tissue healing. Thus, airway dehiscence, historically a major obstacle to long-term pulmonary allotransplant survival, is less likely. Long-term survivors after cardiopulmonary allografting in primates were reported by Reitz and associates [17] in Twenty-seven monkeys underwent cardiopulmonary transplantation using cyclosporine immunosuppression, and most survived for several months. Two of the monkeys remain alive today, almost five years after replacement of the heart and both lungs. Cyclosporine was first used in the ongoing program in clinical cardiac transplantation at Stanford in The clinical results [ 181, together with the laboratory experience with heart-lung transplantation in primates treated with cyclosporine, suggested that a clinical trial of combined heart and lung transplantation would at last be appropriate. Material and Methods Recipients There are many patients who might benefit from combined heart and lung transplantation. The first category consists of those who have damage to both heart and lungs. This includes patients with advanced pulmonary vascular disease, either Eisenmenger s syndrome or primary pulmonary hypertension. Pulmonary vascular disease is a chronic debilitating illness that is unresponsive to medical therapy in its terminal stages. The patients are usually young, in the third and fourth decades of life, and have marked functional disability. The occurrence of repeated syncopal episodes, hemoptysis, or both indicates a poor prognosis for 6- to 12-month survival. Many patients with Eisenmenger s syndrome have had one or more palliative operations, and most of those with primary pulmonary hypertension have had openlung biopsies. The adhesions caused by previous operations increase the risk of operation, since all patients have hepatic dysfunction and coagulation abnormalities, more marked in those with primary pulmonary hypertension because of tricuspid regurgitation. Also in patients with Eisenmenger s syndrome, large collateral vessels develop in the posterior mediastinum, which become less easily identifiable among the adhesions resulting from previous operations. The second category of potential recipients for combined heart and lung transplantation consists of those with irreversible disease of both lungs without major cardiac involvement. The operation could reasonably be applied to this group since the results of heart-lung transplantation are superior to those for lung transplantation alone. Included in this group are such patients as those with severe chronic obstructive airway disease, pulmonary fibrosis, cystic fibrosis, and other enzyme deficiencies. The combined operation in these patients would also avoid the problems that result from leaving one damaged lung in place, such as ventilation/ perfusion defects and a reservoir of infection within the chest. General requirements for prospective recipients are similar to those for patients having a cardiac transplant. Younger patients without other systemic illness and without severe secondary organ dysfunction have a better chance for survival and rehabilitation. Contraindications in our program include any active infection, diabetes mellitus, or extensive previous cardiac procedures. It is important that patients be psychologically stable and able to reliably follow a complex medical program. Apart from these broad indications of suitability, other more specific requirements are that the major disease process be isolated to the heart and lungs and that there not be serious hepatic or renal impairment. We have avoided recipients with a serum bilirubin level higher than 3.5 mg/dl or a creatinine clearance of less than 50 ml per minute. Postoperative treatment with cyclosporine requires these limitations, since this drug is metabolized almost exclusively by the liver and is toxic to both liver and kidneys. Because of the shortage of suitable donors, we have chosen, for the moment, to restrict potential recipients to those with pulmonary hypertension. Several factors make these patients favored candidates. There is always substantial cardiac involvement even in the primary form of this disease, and the patients are relatively young. The tracheobronchial tree is generally sterile, involvement of other organs is usually only the result of cardiac failure, and there is little likelihood of recurrence of the original disease. All 17 patients in the present series had end-stage pulmonary vascular disease with incapacitating symptoms. All exhibited a rapidly deteriorating clinical course resistant to conventional medical or surgical therapy. Ten of the patients had congenital heart disease and Eisenmenger s syndrome; 7 had primary pulmonary hypertension. There were 4 women and 13 men, rangmg from 22 to 45 years old. Cardiac catheterization revealed fixed high pulmonary vascular resistance. In the group with Eisenmenger s syndrome, 1 recipient had undergone multiple palliative surgical procedures, 1 had undergone pulmonary artery banding, and 1 had undergone ligation of a persistent ductus arteriosus. Four patients with primary pulmonary hypertension had undergone openlung biopsy. Donors Donors suitable for heart-lung transplantation are found less frequently than for renal or cardiac transplantation. Brain death may be accompanied by neurogenic pulmo-
3 556 The Annals of Thoracic :Surgery Vol 38 No 6 December 1984 nary edema or thoracic trauma, and prolonged ventilatory support may result in tracheobronchial infection. Probably only about 10% of potential cadaver donors have lungs suitable for combined heart and lung transplantation. Potential donors should be less than 35 years old. Compatibility with the ABO blood group and a negative cross-match between recipient serum and donor lymphocytes are required. Then! should be an absence of preexisting heart or lung disease, a close size match, and completely clear chest roentgenograms. The electrocardiogram should show no acute injury pattern. Satisfactory myocardial function with an adequate blood pressure without high-dose inotropic support should be present. Additional requiremlents include a satisfactory gas exchange, with an arterial oxygen tension of higher than 100 mm Hg on forced inspiratory oxygen of 40%, peak inspiratory pressures of less than 30 mm Hg with normal tidal volumes, and an absence of infected pulmonary secretions. The length of time that the patients have been ventilated is not as critical as the care that they have received during this time, and we have used donors who have been ventilated for as long as 5 days, whereas others have been unsuitable, as a result of pneumonic changes, on the day of death. The importance of size disparity between the transplanted lungs and the recipient s thoracic cage remains to be determined by further experience, but it seems clear that donor lungs that must be compressed to fit within the recipient thoracic case would develop severe atelectasis and pulmonary shunting. Whether a major mismatch in the opposite direction (the transplantation of small donor lungs into a 1arg;e thoracic cavity) would be as detrimental is unlikely, though we have noted the development of substantial pleural effusions when the lungs have been smaller than the recipient s chest cavity. The development of techniques for distant procurement will increase the number of available donors. Although satisfactory methods for heart preservation are available for a period of up to about 4 hours [19], techniques that reliably provide complete protection for lung tissue for this same period are not. A good deal of experimental work with single lung transplants has been reported [20, 211, but in initial experimental trials in our laboratory, application to the combined heart and lung graft has so far yielded unreliable preservation of lung function. We believe that distant lung procurement is not yet ready for clinical use, and at present, heart-lung donors are moved to the transplant center. Opera tion A most important aspect of the operative approach is to remove the recipient s heart and lungs without injury to the vagus or phrenic nerves or to the left recurrent laryngeal nerve. In addition, meticulous hemostasis with respect to the recipient s bronchial arterial circulation is essential, particularly in patients with Eisenmenger s syndrome in whom these vessels are especially large and delicate. i Fig 1. After removal of the heart, an incision is made through the oblique sinus to separate the right and left pulmonary veins. The vagus nerves lie immediately behind the pulmonary hilum on each side and anterior to the esophagus. The phrenic nerves are anterior to the hilum on each side, generally closer to the right hilum than the left. The left recurrent laryngeal nerve passes around the ligamentum arteriosum posterior to the pulmonary arterial bifurcation. The anatomy of the bronchial arteries is somewhat variable, but usually there are several large branches arising from the aorta and passing on either side posterior to the trachea and both bronchi. The size, friability, and relative inaccessibility of these vessels after implantation of the graft make their control critical. In the first 5 patients, the recipient s heart and lungs were removed together [22], but subsequent experience has shown that separate excision affords better visualization of the nerves and posterior mediastinal vessels [23]. The current practice is to remove the heart first, leaving a posterior cuff of both left and right atria. An incision along the posterior wall of the left atrium up the oblique sinus (Fig 1) allows separation of the lungs, and the left lung is then excised. The left side of the pericardium is removed except for a small ribbon containing the phrenic nerve. The right lung is removed in similar fashion, again preserving the right phrenic nerve. Then the remnants of the pulmonary artery are removed, leaving only a small segment in the area of the ductus ligament to avoid injury to the left recurrent laryngeal nerve. Finally, the trachea is exposed in the midline and divided just above the carina, and the bronchial remnants are excised. At present, our knowledge of lung preservation requires that the donor heart and lungs be removed in the adjoining room. Cardiopulmonary bypass is not required for this operation, and coordination is made with other transplant teams so that other organs can be removed. Prior dissection within the abdomen is carried out if required, and then the donor heart and lungs are exposed. After full-body heparinization, the superior
4 557 Jamieson et al: Heart-Lung Transplantation for Irreversible Pulmonary Hypertension quently. A certain amount of atelectasis is seen in all patients, and pleural effusions have been common, presumably contributed to by interruption of lymphatics on the posterior wall of the thorax. Fig 2. The tracheal anastomosis has been completed. A curvilinear incision is made in the right atrium, and the atria are anastomosed as shown. vena cava is ligated and divided, and the inferior vena cava is cut. After the heart has emptied, the aorta is cross-clamped and 500 ml of cold cardioplegic solution is infused into the aortic root. Simultaneously, 1.5 liters of modified Collins solution (high osmolality and high potassium) is infused into the pulmonary artery, and the tip of the left atrial appendage is amputated to allow egress of this fluid. Care is taken that the left ventricle does not become distended, and ventilation is continued using unwarmed room air. Implantation of the donor organs commences with the tracheal anastomosis, followed by the aortic and atrial anastomoses. The incision in the donor atrium is made in curvilinear fashion to avoid injury to the sinus node during implantation (Fig 2). All anastomoses are performed with continuous polypropylene sutures. After removal of air from the heart, ventilation is begun and the aortic cross-clamp is removed. Cardiopulmonary bypass is discontinued after a suitable period of resuscitation. Immediate postoperative care is similar to that of all patients who have undergone routine cardiopulmonary bypass except for the use of isoproterenol to provide chronotropic support (the cardiac output of the denervated heart is rate dependent) and the strict avoidance of high inspired oxygen concentrations. Immunosuppression is begun, and the patient is nursed in reversed barrier isolation. Extubation is accomplished early, and thereafter the patient is encouraged to cough and breathe deeply. Postural physiotherapy is used fre- Immunosuppression The regimen of immunosuppression that we have chosen for combined heart and lung transplantation begins with a preoperative dose of cyclosporine (18 mg per kilogram of body weight) and continues with oral administrations of cyclosporine twice daily for an indefinite period, as regulated by serum cyclosporine levels. We no longer use intravenous preparations of this agent. Immediately after discontinuation of bypass, 500 mg of methylprednisolone are administered intravenously, followed by 125 mg every 8 hours for a total of three doses. No further steroids are given for two weeks in an effort to avoid impaired tracheal healing. Cyclosporine immunosuppression is augmented for the first two weeks with azathioprine, given orally at a dose of 1.5 mg/kg/day, and an initial 3-day course of rabbit antithymocyte globulin (ATG) given intramuscularly. The dose of ATG is adjusted to reduce the circulating T- lymphocyte population to less than 5%. After two weeks, azathioprine is replaced with prednisone, 0.2 mg/kg/day administered orally. Patients with the original diagnosis of primary pulmonary hypertension require very small doses of cyclosporine, and the hepatic impairment of these patients is greatly exacerbated by cyclosporine administration. All patients experience a degree of renal dysfunction with cyclosporine therapy, and dialysis with plasma ultrafiltration has been required in 5 recipients as a temporary measure. Endomyocardial biopsy [24] is initially camed out on a weekly basis; after discharge from the hospital, it is done on a less frequent schedule depending on the clinical course. Rejection episodes within the first month, as diagnosed by cardiac biopsy, are treated with intravenous boluses of methylprednisolone (1 gm) daily for 3 days. Episodes of rejection resistant to this regimen are treated with additional rabbit ATG. After a month, rejection seems to be adequately treated by augmented oral steroids. We have not used additional techniques to diagnose pulmonary rejection, since our initial laboratory experience indicated that cardiac and pulmonary rejection proceed hand in hand (251. Recent studies indicate that this may not be an absolute rule and that it may be possible to encounter pulmonary rejection in primates without substantial cardiac rejection. Therefore, the concept of the cardiac biopsy providing an absolute prediction of the state of rejection of the lung might have to be tempered by the knowledge that pulmonary rejection can occur at a different tempo from that of the heart. The frequency and severity of rejection episodes as diagnosed by cardiac biopsy have been somewhat less following heart-lung transplantation than those observed with cardiac transplantation alone. A systematic review and comparison of cardiac biopsy specimens
5 ~ ~ ~~ ~~ ~ 558 The Annals of Thoracic Surgery Vol 38 No 6 December 1984 Data on 17 Patients Undergoing Heart-Lung Transplantation Patient No., Day of Sex, Age (yr) Diagnosis Rejection Infection Dischargeb 1. F, 45 PPH 2 Herpes (cutaneous) M, 30 ES 0 Cytomegalovirus (systemic) F, 29 ES X Not at risk for rejection or infection (4) 4. M, 40 ES 0 None F, 37 PPH 2 None F, 29 PPH X Not at risk for rejection or infection (23) 7. M, 22 ES X Not at risk for rejection or infection (0) 8. M, 40 ES 0 Bacteroides (blood and lung), M, 22 ES 2 cytomegalovirus (systemic) Enterococcus (lung) M, 28 ES 2 None M, 38 ES 0 None M, 33 ES 0 Cytomegalovirus (systemic) M, 33 PPH 1 Serrutiu (pulmonary), cytomegalo- 60 virus (systemic reactivation) 14. F, 28 PPH X Candida (systemic) (16) 15. M, 42 ES 0 Legionella, Serratia (33) 16. M, 22 PPH 1 Serru t ia M, 37 PPH 0 Enterococcus 64 Number of acute rejechon episodes occurrmg in the hospital and requinng intravenous administrahon of methylprednisolone bnumbers in parentheses represent day of death of the patient PPH = pnmary pulmonary hypertension, 1 3 = Eisenmenger s syndrome were made between 88 patients with cardiac transplants (treated with cyclosporine and prednisone, with the first 27 also receiving rabbit ATG) and 16 patients receiving heart-lung transplants (treated with cyclosporine and azathioprine and with a change to prednisone at two weeks). Evidence of myocyte necrosis (acute rejection requiring treatment) was seen in 299 (24.6%) of the 1,214 biopsy specimens from cardiac transplant recipients compared with 22 (13.8%) of the 160 specimens from heart-lung recipients (p < 0.001). Whether this is due to the different regimen of immunosuppression or to an inherent difference stemming from the transplantation of pulmonary tissue remains to be determined. The frequency of rejection episodes, as with cardiac rejection, is highest within the first 60 days after transplantation. Rejection episodes requiring one or more courses of augmented immunosuppression have occurred in 6 of the 12 long-term su::vivors, and resolution of rejection occurred in each with treatment. Nine patients have sustained serious :Infections (Table), although infection was responsible for the patient s death in only one instance. Additional details regarding the inhospital course of each patient are given in the Table. Loss of Pulmonary Innervation Transplantation of both lungs results in the loss of pulmonary innervation. It is unlikely that these nerves will regenerate, since reinnervation of allografted organs is rare [26], and in the fifteen years experience of the car- diac transplantation program at Stanford, no regeneration of cardiac autonomic nerves has been documented. The patients discussed in this report have provided the first opportunity to study the regulation of breathing in human beings in whom both lungs have been totally denervated. The recipient is immediately and probably permanently subject to other methods of regulation of breathing, but breathing patterns have been normal in most instances. Most, but not all, patients have maintained a carbon dioxide tension ranging from 45 to 49 mm Hg, especially immediately after operation. Regulation of breathing apparently occurs satisfactorily by way of chest wall afferent nerves, carotid body receptors, and inherent rhythmic control of breathing. During exercise, appropriate increases in minute volume, tidal volume, and respiratory rate occur, as found when the patients were studied 4 months postoperatively. Blood gases remain normal. Bronchial Arteries The healing of the airway anastomosis has been of major concern in lung transplantation. Unilateral lung transplantation has been plagued by bronchial dehiscence [27], and factors such as the length of the bronchial segment of the graft have been demonstrated to be important [28]. In single lung transplants there is no arterial vascular contribution from the donor side. In this respect, combined heart and lung transplants stand at a distinct advantage, since coronary-bronchial collaterals
6 559 Jamieson et al: Heart-Lung Transplantation for Irreversible Pulmonary Hypertension A Fig 3. Typical appearance of coronary angiograms from a patient 6 months after operation showing the collateral circulation from (A) the left coronary artery (arrow) and (B) the right coronary artery. can open up to restore vascularity to the vessels previously supplied by the bronchial arteries. Shortly after the operation has been completed, arterial bleeding can be seen from the cut surfaces of the donor pleural reflections and elsewhere. Necrosis, rupture, or late stenosis at the tracheal anastomosis has not yet been seen in the patients receiving a transplant to date or in the primate survivors of heartlung transplantation in our laboratory. In patients, coronary arteriograms made after operation have invariably shown the development of collaterals to the area of the suture line from the donor coronary circulation through atrial branches of the coronary arteries (Fig 3). Therefore, in human beings, the bronchial arterial supply directly from the aorta is relatively unimportant. The "Implantation Response" The postoperative management of patients with lung transplants is complicated by the development of impaired pulmonary gas exchange and the radiological appearance of interstitial edema about a week after operation. This syndrome, which is not present within the first few days after operation, has been termed the reimplantation response [27, 291, though we suggest the term implantation response for this phenomenon. The response is defined as a transient, reversible defect in pulmonary gas exchange, compliance, and vascular resistance and coincides with roentgenographic pulmonary edema early after operation. The cause is unknown, but it is likely that surgical trauma, ischemia, denervation, lymphatic interruption, and other pro- B cesses, exclusive of rejection, all contribute [27]. The entity is worrisome, although it resolves after a period of several days without specific therapy. It is absolutely vital, however, to differentiate this response from pulmonary rejection or infection. The finding has been described in animals and patients undergoing lung transplantation [27, 301 and in primates undergoing combined heart and lung transplantation [ 171, both allografts and autografts. The typical appearance of the implantation response in 1 of our patients is seen in Figure 4A; spontaneous resolution is shown in Figure 4B. A systematic review of the postoperative chest radiographs of the first 10 heart-lung recipients demonstrated the radiographic appearance of interstitial edema in all by the second postoperative week. It was not seen in 10 consecutive patients undergoing cardiac transplantation or 10 consecutive patients having coronary artery bypass. On the average, the radiological abnormality peaked on the eleventh postoperative day (range, 4 to 20 days). The pattern persisted for an average of 7 days (range, 2 to 12 days) and then resolved. Because of this tendency for pulmonary edema to develop during the first three weeks after transplantation, an aggressive diuresis is maintained, with the aim of achieving a negative weight balance early after operation. The 10 patients just mentioned had lost an average of 2.4 kg by the end of the third week. Severe oliguria (possibly a result of cyclosporine toxicity) necessitated hemodialysis with ultrafiltration in 5 patients. The implantation response is likely to be a reflection of increased capillary permeability or lymphatic interruption or both. Lymphatics probably regenerate after lung transplantation by the third week [20], thereby coinciding with the resolution of this process. The puzzling aspect of this phenomenon, however, is the lag period observed before its onset, since lymphatic interruption is present immediately. This delay might incriminate isch-
7 560 The Annals of Thoracic Surgery Vol 38 No 6 December 1984 A B Fig 4. Typical chest roentgenograms from a single patient. (A) Roentgenogram made 10 days after operution illustrates the implantation response. (B) One month later, th? condition has resolved without specific treatment. emic changes of the lung as the primary cause, with resolution aided by lymphatic regeneration. Results Twelve of the 17 patients are alive at intervals ranging from 1 to 30 months. Four patients died within 1 month of transplantation. One of them died on the fourth day as a result of severe hemorrhage B t the time of operation. She had transposition of the great vessels and pulmonary hypertension, and had undergone multiple palliative surgical procedures. Another had progressive renal and neurological impairment, and required dialysis and respiratory support until her dee th on the twenty-third postoperative day. One patient died during operation of a massive capillary leak phenomenon of the donor lungs, with failure of gas exchange and profound hypoxemia associated with pulmonary hypertension. Another patient died of progressive renal and hepatic failure and pulmonary sepsis on the sixtee nth postoperative day. This patient had severe prerenal azotemia and passive hepatic congestion preoperative ly, and these problems were greatly exacerbated in the early postoperative period. One patient died late. After an initially favorable course, he died of progressive pulmonary infection on the thirty-third postoperative day. Legionella was grown from the pleural fluid on the tenth postoperative day. Because of this rapid infection arid because the Legionella species was of a different strain from others encountered in our transplant population, it is possible that this infection was present in the donor lungs at the time of transplantation. The remaining patients have done well. Total cumulative survival following heart-lung transplantation now exceeds fifteen patient-years. All survivors have a normal exercise tolerance (New York Heart Association Functional Class I), and 9 patients who underwent repeat cardiac catheterization at one year had normal hemodynamics and normal pulmonary artery pressures. Two patients had repeat cardiac catheterization two years after transplantation, and the findings were again normal. The patients have maintained a normal functional capacity, and exercise freely and without limitation. The results of coronary arteriography have been normal, with the exception of the collateral arteries already described. Nine patients have survived more than 12 months after operation, and the first patient is alive and well nearly three years after operation. The long-term outlook for these patients remains uncertain. However, 2 monkeys in the laboratory studies apparently are well some four and a half years after heart-lung transplantation, without evidence of pulmonary hypertension or impaired gas exchange. Coronary artery disease is a complication often seen after cardiac transplantation, and it is likely that this will also be a potential complication after combined transplantation. The pulmonary vascular equivalent of coronary artery disease has not yet been seen, but probably can be expected to occur. Measures currently used to minimize this complication in recipients of a cardiac transplant may also be important in the combined transplant; they include antiplatelet drugs, low lipid diets, and regular physical activity. Five patients show evidence of early bronchiectatic changes, presumably a result of pulmonary denervation. Whether the main factor is large airway sensory loss giving rise to an impaired cough reflex or ciliary dysfunction is still being investigated. Continuing studies are focusing on improved control of the immune response, noninvasive methods of diagnosing rejection, mechanisms for changes in pulmonary
8 561 Jamieson et al: Heart-Lung Transplantation for Irreversible Pulmonary Hypertension vascular resistance and pulmonary epithelial permeability after transplantation, and the applicability of the technique to other clinical syndromes associated with advanced pulmonary disease. Comment Patients with end-stage pulmonary vascular disease pose a formidable therapeutic challenge. Those with Eisenmenger s syndrome are difficult to treat medically and cannot be treated with surgical procedures, including cardiac transplantation. Cardiopulmonary transplantation represents the only therapeutic avenue for these patients. Primary pulmonary hypertension is similarly difficult to treat medically, and is a progressive and fatal illness. Patients with primary pulmonary hypertension could theoretically be treated by unilateral lung transplantation, though this would leave them with only one functional lung. We believe that combined heart and bilateral lung transplantation is likely to prove a more successful approach. Advantages of the combined operation are that all diseased pulmonary tissue is removed, thus preventing both recurrent infection and ventilation/ perfusion imbalance caused by the remaining lung. A tracheal anastomosis, since it receives a better blood supply, is more likely to heal than a bronchial anastomosis; this is further aided in the combined operation since coronary-bronchial anastomoses in the en bloc graft are preserved. An additional advantage is provided by the ability to obtain sequential biopsies of the heart, since there appears to be a close correlation between cardiac and pulmonary rejection. Clinical experience with heart-lung transplantation has been encouraging to date and is considerably superior to that for unilateral lung transplantation. Currently the greatest problem confronting the program, the lack of suitable donors, for the moment precludes the application of combined heart and lung transplantation to many other conditions that involve terminal lung disease. References 1. Demikhov VP: Some essential points of the techniques of transplantation of the heart, lungs and other organs. In Experimental Transplantation of Vital Organs. Moscow, Medgiz State Press for Medical Literature in Moscow, 1960, chap 2, pp 29-48; translated from Russian by Basil Haigh, Consultants Bureau, New York, Neptune WB, Cookson BA, Bailey CP, et al: Complete homologous heart transplantation. Arch Sur 66:174, Webb WR, Howard HS: Cardiopulmonary transplantation. Surg Forum 8:313, Webb WR, Howard HS, Neely WA: Practical methods of homologous cardiac transplantation. J Thorac Surg 37361, Webb WR, de Guzman V, Hoopes JE: Cardiopulmonary transplantation: experimental study of current problems. Am Surg 27236, Lower RR, Stofer RC, Hurley EJ, Shumway NE: Complete homograft replacement of the heart and both lungs. Surgery 50:842, Grinnan GLB, Graham WH, Childs JW, Lower RR: Cardiopulmonary transplantation. J Thorac Cardiovasc Surg 60:609, Haglin J, Telander RL, Muzzall RE, et al: Comparison of lung autotransplantation in the primate and dog. Surg Forum 14196, Nakae S, Webb WR, Theodorides T, Gregg WL: Respiratory function following cardiopulmonary denervation in dog, cat and monkey. Surg Gynecol Obstet 125:1285, Cooley DA, Bloodwell RD, Hallman GL, et al: Organ transplantation for advanced cardiopulmonary disease. Ann Thorac Surg 8:30, Lillehei CW: Discussion of Wildevuur CRH, Benfield JR A review of 23 human lung transplantations by 20 surgeons. Ann Thorac Surg 9:489, Barnard CN, Cooper DKC: Clinical transplantation of the heart: a review of 13 years personal experience. J R SOC Med 74:670, Castaneda AR, Arnar D, Schmidt-Habelman P, et al: Cardiopulmonary autotransplantation in primates. J Cardiovasc Surg (Torino) 13:523, Castaneda AR, Zamora R, Schmidt-Habelman P, et al: Cardiopulmonary autotransplantation in primates (baboons): late functional results. Surgery 72:1064, Borel JF, Feurer C, Gubler HU, Stahelin H: Biological effects of cyclosporin A: a new antilymphocytic agent. Agents Actions 6:648, Borel JF: Cyclosporin-A: a present experimental status. Transplant Proc 13:344, Reitz BA, Burton NA, Jamieson SW, et al: Heart and lung transplantation: auto- and allotransplantation in primates with extended survival. J Thorac Cardiovasc Surg 80:360, Oyer PE, Stinson EB, Jamieson SW, et al: Cyclosporin A in cardiac allografting: a preliminary experience. Transplant Proc 15:1247, Watson DC, Reitz BA, Baumgartner WA, et al: Distant heart procurement for transplantation. Surgery 86:56, Veith FJ, Montefusco C, Kamholz SL, Mollenkopf FP: Lung transplantation. Heart Transplant 2:155, Modry DL, Walpoth B, Cohen R, et al: Heart-lung preservation in the dog followed by lung transplantation: a new model for assessment of lung preservation. Heart Transplant 2287, Reitz BA, Wallwork J, Hunt SA, et al: Heart-lung transplantation: successful therapy for patients with pulmonary vascular disease. N Engl J Med 306:557, Jamieson SW, Baldwin J, Reitz BA, et al: Combined heart and lung transplantation. Lancet 1:1130, Caves PK, Stinson EB, Billingham ME, Shumway NE: Percutaneous transvenous endomyocardial biopsy in human heart recipients. Ann Thorac Surg 16:325, Reitz BA, Gaudiani VA, Hunt SA, et al: Diagnosis and treatment of allograft rejection in heart-lung transplant recipients. J Thorac Cardiovasc Surg 85:354, Kondo Y, Matheny JL, Hardy JD: Autonomic reinnervation of cardiac transplants: further observations in dogs and rhesus monkeys. Ann Surg 176:42, Veith FJ: Lung transplantation. Surg Clin North Am 58:357, Pinsker KL, Koerner SK, Kamholz SL, et al: Effect of donor bronchial length on healing: a canine model to evaluate bronchial anastomotic problems in lung transplantation. J Thorac Cardiovasc Surg 77:669, Siegelman SS, Sinha SB, Veith FJ: Pulmonary reimplantation response. Ann Surg 17730, 1973
9 562 The Annals of Thoracic Surgery Vol 38 No 6 December Baranski EJ, Scicchitano LP, Camishon RC: Pulmonary hypertension following cardiopulmonary transplantation. Surg Forum 14:200, 1963 Discussion DR. BARTLEY GRIFFITH (Pittsburgh, PA): Aware of the early good results initiated by Reitz and co-workers and now confirmed by Jamieson and associates, my colleagues and I embarked on a similar program in heart-lung transplantation. During the last 18 months, we have evolved some different practices from those discussed by Dr. Jamieson. The differences include the selection of candidates, the maintenance of donors, a fear that the endomyocardial biopsy might not mirror lung rejection, and some concern about overimmunosuppression with respect to the development of lymphoproliferative disease. Candidates have included 3 patierits with pulmonary vascular disease, 1 patient with cystic fikrosis, 2 patients with obstructive lung disease, and 1 patient with eosinophilic granuloma of the lung. These patients have been accepted as a result of referral practice rather than a strong interest in pushing the limits of the operation. Although the patients with obstructive lung disease have not survived, all others have demonstrated early survival. The results certainly reemphasize the outstanding success and therapeutic nature of the operation for selected patients. We have found it easier to place donors on bypass. The bypass enables us to accomplish a relaxed removal of multiple organs including heart, lungs, liver, and kidneys, absolute hemostasis of the posterior heart-lung tiloc, and hypothermic lung preservation without flushing the pulmonary artery. Early in the series we used such a flush for procurement of lungs, thus relying on the flush of the pulmonaiy artery to cool and exsanguinate the lung. Subsequently, experimental canine and clinical human use of hypothermic (4 C) bypass has suggested that the flush is unnecessary and perhaps harmful for local procurement. Radiographs of recipients 4 months after transplantation demonstrate the hemostatic clips in the posterior aspect of the heart-lung bloc. We believe that much of the heralded postoperative hemorrhage occurs from the donor organ bloc rather than from uncontrolled vessels in the recipient. We have reservations about the endomyocardial biopsy always mirroring the rejection phenomena. We believe clinical rejection of the lung may occur with only minimal myocardial interstitial infiltrate. In one instance, simultaneous lung and heart biopsy specimens revealed scanty myocardial infiltration, yet there were desquamative macrophages in some of the air spaces and mild interstitial infiltration with round cells and fibroblasts. The lung tissue failed to grow infectious pathogens, but the recipient progressed to a fulminating lung failure. The differential diagnosis between rejection and viral infection can be difficult. Last, we are concerned about the potential for overimmunosuppression with multiple immunosuppressive agents including azathioprine, cyclosporine, and rabbit ATG. Among our 4 survivors, a lymphoproliferative disease developed in 2. We believe it is related to Epstein-Barr viral infection. In a lymph node removed from a patient 4 months after transplantation, the nuclear material was stained by immunofluorescence for the presence of Epstein-Barr nuclear antigen. The patient is free from clinical disease with reduction in immune suppression. It may be that we are overimmunosuppressing this group of patients, and I believe that in the future we will eliminate the early use of rabbit ATG and possibly even azathioprine. DR. JAMIESON: Thank you. I believe that the present era of successful transplantation, both of the heart and of the heart-lung bloc, is the result of the work of many, many pioneers. We are fortunate to be at the end of a long chain of such conscientious and industrious workers.
MODERATOR Felix Rapaport, other members of this
 The First Lung Transplant in Man (1963) and the First Heart Transplant in Man (1964) J.D. Hardy MODERATOR Felix Rapaport, other members of this distinguished panel, and members of the audience, I will
The First Lung Transplant in Man (1963) and the First Heart Transplant in Man (1964) J.D. Hardy MODERATOR Felix Rapaport, other members of this distinguished panel, and members of the audience, I will
Acute Isolated Pulmonaw Reiection Following Transplantatich of the Heart and Both Lungs: Experimental and Clinical Observations
 Acute Isolated Pulmonaw Reiection Following Transplantatich of the Heart and Both Lungs: Experimental and Clinical Observations D. Novitzky, M.D., D. K. C. Cooper, Ph.D., F.R.C.S., A. G. Rose, Ch.B., M.Med.(Path),
Acute Isolated Pulmonaw Reiection Following Transplantatich of the Heart and Both Lungs: Experimental and Clinical Observations D. Novitzky, M.D., D. K. C. Cooper, Ph.D., F.R.C.S., A. G. Rose, Ch.B., M.Med.(Path),
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure
 Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Extracorporeal Life Support Organization (ELSO) Guidelines for Pediatric Respiratory Failure Introduction This pediatric respiratory failure guideline is a supplement to ELSO s General Guidelines for all
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure. Heart Failure at the Shoe XI October 5, 2012
 Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure Heart Failure at the Shoe XI October 5, 2012 Robert S.D. Higgins, MD, MSHA Executive Director, Comprehensive Transplant Center Evolution
Evolution of Surgical Therapies for End-Stage Cardiopulmonary Failure Heart Failure at the Shoe XI October 5, 2012 Robert S.D. Higgins, MD, MSHA Executive Director, Comprehensive Transplant Center Evolution
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Surgical Technique of Experimental Lung Transplantation in Rabbits
 Original Article Surgical Technique of Experimental Lung Transplantation in Rabbits Shigetoshi Yoshida, MD, Yasuo Sekine, MD, Yukio Saitoh, MD, Kazuhiro Yasufuku, MD, Takekazu Iwata, MD, and Takehiko Fujisawa,
Original Article Surgical Technique of Experimental Lung Transplantation in Rabbits Shigetoshi Yoshida, MD, Yasuo Sekine, MD, Yukio Saitoh, MD, Kazuhiro Yasufuku, MD, Takekazu Iwata, MD, and Takehiko Fujisawa,
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
Clinical Policy: Heart-Lung Transplant Reference Number: CP.MP.132
 Clinical Policy: Reference Number: CP.MP.132 Effective Date: 01/18 Last Review Date: 05/18 Coding Implications Revision Log Description Heart-lung transplantation is treatment of choice for patients with
Clinical Policy: Reference Number: CP.MP.132 Effective Date: 01/18 Last Review Date: 05/18 Coding Implications Revision Log Description Heart-lung transplantation is treatment of choice for patients with
Vasculature and innervation of the heart. A. Bendelic Human Anatomy Department
 Vasculature and innervation of the heart A. Bendelic Human Anatomy Department Plan: 1. Arterial blood supply of the heart. Coronary arteries 2. Venous drainage of the heart. Cardiac veins 3. Innervation
Vasculature and innervation of the heart A. Bendelic Human Anatomy Department Plan: 1. Arterial blood supply of the heart. Coronary arteries 2. Venous drainage of the heart. Cardiac veins 3. Innervation
The arterial switch operation has been the accepted procedure
 The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
The Arterial Switch Procedure: Closed Coronary Artery Transfer Edward L. Bove, MD The arterial switch operation has been the accepted procedure for the repair of transposition of the great arteries (TGA)
Management of a Patient after the Bidirectional Glenn
 Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Management of a Patient after the Bidirectional Glenn Melissa B. Jones MSN, APRN, CPNP-AC CICU Nurse Practitioner Children s National Health System Washington, DC No Disclosures Objectives qbriefly describe
Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents
 Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents March, 2013 Sponsored by: Commission on Education Committee on Residency Training in Diagnostic Radiology 2013 by American
Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents March, 2013 Sponsored by: Commission on Education Committee on Residency Training in Diagnostic Radiology 2013 by American
Chapter 4 Section 24.1
 Surgery Chapter 4 Section 24.1 Issue Date: October 27, 1995 Authority: 32 CFR 199.4(e)(5) 1.0 CPT 1 PROCEDURE CODES 32850-32854, 33930-33935 2.0 DIAGNOSTIC RELATED GROUPS (DRGs) 495 for lung transplant.
Surgery Chapter 4 Section 24.1 Issue Date: October 27, 1995 Authority: 32 CFR 199.4(e)(5) 1.0 CPT 1 PROCEDURE CODES 32850-32854, 33930-33935 2.0 DIAGNOSTIC RELATED GROUPS (DRGs) 495 for lung transplant.
I worldwide [ 11. The overall number of transplantations
 Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
SINCE the introduction of Imuran and
 Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
Cadaveric Renal Transplantation With Cyclosporin-A and Steroids T. R. Hakala, T. E. Starzl, J. T. Rosenthal, B. Shaw, and S. watsuki SNCE the introduction of muran and prednisone in 1961, and despite the
The 1-year survival rate approaches 80% for patients
 Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
Obstructed total anomalous pulmonary venous connection
 Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Index. Note: Page numbers of article titles are in boldface type
 Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
Index Note: Page numbers of article titles are in boldface type A Acute coronary syndrome, perioperative oxygen in, 599 600 Acute lung injury (ALI). See Lung injury and Acute respiratory distress syndrome.
CHAPTER 3 SECTION 1.6B HEART-LUNG AND LUNG TRANSPLANTATION TRICARE POLICY MANUAL M, MARCH 15, 2002 SURGERY AND RELATED SERVICES
 TRICARE POLICY MANUAL 6010.47-M, MARCH 15, 2002 SURGERY AND RELATED SERVICES CHAPTER 3 SECTION 1.6B ISSUE DATE: October 27, 1995 AUTHORITY: 32 CFR 199.4(e)(5) I. CODES A. CPT 1 Procedure Codes 33930, 33935,
TRICARE POLICY MANUAL 6010.47-M, MARCH 15, 2002 SURGERY AND RELATED SERVICES CHAPTER 3 SECTION 1.6B ISSUE DATE: October 27, 1995 AUTHORITY: 32 CFR 199.4(e)(5) I. CODES A. CPT 1 Procedure Codes 33930, 33935,
CARDIOVASCULAR SURGERY
 Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
Volume 107, Number 4 April 1994 The Journal of THORACIC AND CARDIOVASCULAR SURGERY Cardiac and Pulmonary Transplantation Risk factors for graft failure associated with pulmonary hypertension after pediatric
The technique of unilateral double lobar lung transplantation in a canine model
 The technique of unilateral double lobar lung transplantation in a canine model Daisuke Okutani, MD Hiroshi Date, MD Makio Hayama, MD Hidetoshi Inokawa, MD Mikio Okazaki, MD Itaru Nagahiro, MD Yoshifumi
The technique of unilateral double lobar lung transplantation in a canine model Daisuke Okutani, MD Hiroshi Date, MD Makio Hayama, MD Hidetoshi Inokawa, MD Mikio Okazaki, MD Itaru Nagahiro, MD Yoshifumi
Chapter 5: Other mediastinal structures. The Large Arteries. The Aorta. Ascending aorta
 Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Chapter 5: Other mediastinal structures The Large Arteries The Aorta The aorta is the main arterial trunk of the systemic circulation and in the healthy state its wall contain a large amount of yellow
Implantable Ventricular Assist Devices and Total Artificial Hearts. Policy Specific Section: June 13, 1997 March 29, 2013
 Medical Policy Implantable Ventricular Assist Devices and Total Artificial Hearts Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective
Medical Policy Implantable Ventricular Assist Devices and Total Artificial Hearts Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective
Technique of Successful Clinical Double-Lung Transplantation
 Technique of Successful Clinical Double-Lung Transplantation G. A. Patterson, M.D., F.R.C.S. (C), J. D. Cooper, M.D., F.R.C.S. (C), B. Goldman, M.D., F.R.C.S. (C), R. D. Weisel, M.D., F.R.C.S. (C), F.
Technique of Successful Clinical Double-Lung Transplantation G. A. Patterson, M.D., F.R.C.S. (C), J. D. Cooper, M.D., F.R.C.S. (C), B. Goldman, M.D., F.R.C.S. (C), R. D. Weisel, M.D., F.R.C.S. (C), F.
Deliberate Renal Ischemia
 Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Pulmonary Valve Replacement
 Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Pulmonary Valve Replacement with Fascia Lata J. C. R. Lincoln, F.R.C.S., M. Geens, M.D., M. Schottenfeld, M.D., and D. N. Ross, F.R.C.S. ABSTRACT The purpose of this paper is to describe a technique of
Cardiovascular Anatomy Dr. Gary Mumaugh
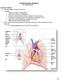 Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
Cardiovascular Anatomy Dr. Gary Mumaugh Location of Heart Approximately the size of your fist Location o Superior surface of diaphragm o Left of the midline in mediastinum o Anterior to the vertebral column,
Cardiovascular system Physiology Sheet (1)
 Cardiovascular system Physiology Sheet (1) In any patient the most important thing is the cardiorespiratory system, if any patient comes to you with a car accident for example the first thing that you
Cardiovascular system Physiology Sheet (1) In any patient the most important thing is the cardiorespiratory system, if any patient comes to you with a car accident for example the first thing that you
Radiological Anatomy of Thorax. Dr. Jamila Elmedany & Prof. Saeed Abuel Makarem
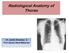 Radiological Anatomy of Thorax Dr. Jamila Elmedany & Prof. Saeed Abuel Makarem Indications for Chest x - A chest x-ray may be used to diagnose and plan treatment for various conditions, including: Diseases/Fractures
Radiological Anatomy of Thorax Dr. Jamila Elmedany & Prof. Saeed Abuel Makarem Indications for Chest x - A chest x-ray may be used to diagnose and plan treatment for various conditions, including: Diseases/Fractures
Unit 6: Circulatory System. 6.2 Heart
 Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Unit 6: Circulatory System 6.2 Heart Functions of Circulatory System 1. The heart is the pump necessary to circulate blood to all parts of the body 2. Arteries, veins and capillaries are the structures
Prepared Pulmonary venous Orifice
 HOW TO DO IT The Surgical Technique of Heterotopic Heart Transplantation D. Novitzky, M.D., F.C.S.(S.A.), D. K. C. Cooper, M.A., M.B., B.S., Ph.D., F.R.C.S., and C. N. Barnard, M.D., M.Med., M.S., Ph.D.,
HOW TO DO IT The Surgical Technique of Heterotopic Heart Transplantation D. Novitzky, M.D., F.C.S.(S.A.), D. K. C. Cooper, M.A., M.B., B.S., Ph.D., F.R.C.S., and C. N. Barnard, M.D., M.Med., M.S., Ph.D.,
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ
 Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Post Operative Management in Heart Transplant นพ พ ชร อ องจร ต ศ ลยศาสตร ห วใจและทรวงอก จ ฬาลงกรณ Art of Good Cooking Good Ingredient Good donor + OK recipient Good technique Good team Good timing Good
Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line
 L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
L 14 A B O R A T O R Y Thorax THORACIC WALL Identify the lines used in anatomical surface descriptions of the thorax. median line mid-axillary line mid-clavicular line Identify the surface landmarks of
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Heart Transplant ation Technique
 Heart Transplant ation Technique R. Morton Bolman I11 Since its clinical inception in 1967, heart transplantation has benefited thousands of patients with heart failure. The surgical technique has remained
Heart Transplant ation Technique R. Morton Bolman I11 Since its clinical inception in 1967, heart transplantation has benefited thousands of patients with heart failure. The surgical technique has remained
PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.*
 Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
Published Online: 1 July, 1914 Supp Info: http://doi.org/10.1084/jem.20.1.3 Downloaded from jem.rupress.org on December 24, 2018 PATCHING AND SECTION OF THE PULMONARY ORIFICE OF THE HEART.* BY THEODORE
11.1 The Aortic Arch General Anatomy of the Ascending Aorta and the Aortic Arch Surgical Anatomy of the Aorta
 456 11 Surgical Anatomy of the Aorta 11.1 The Aortic Arch 11.1.1 General Anatomy of the Ascending Aorta and the Aortic Arch Surgery of the is one of the most challenging areas of cardiac and vascular surgery,
456 11 Surgical Anatomy of the Aorta 11.1 The Aortic Arch 11.1.1 General Anatomy of the Ascending Aorta and the Aortic Arch Surgery of the is one of the most challenging areas of cardiac and vascular surgery,
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow
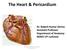 The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
The Heart & Pericardium Dr. Rakesh Kumar Verma Assistant Professor Department of Anatomy KGMU UP Lucknow Fibrous skeleton Dense fibrous connective tissue forms a structural foundation around AV & arterial
The evolution of the Fontan procedure for single ventricle
 Hemi-Fontan Procedure Thomas L. Spray, MD The evolution of the Fontan procedure for single ventricle cardiac malformations has included the development of several surgical modifications that appear to
Hemi-Fontan Procedure Thomas L. Spray, MD The evolution of the Fontan procedure for single ventricle cardiac malformations has included the development of several surgical modifications that appear to
Mediastinum and pericardium
 Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum and pericardium Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com The mediastinum: is the central compartment of the thoracic cavity surrounded by
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Original Policy Date
 MP 7.03.07 Heart/Lung Transplant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
MP 7.03.07 Heart/Lung Transplant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy Index
University of Wisconsin - Madison Cardiovascular Medicine Fellowship Program UW CICU Rotation Goals and Objectives
 Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
Background: The field of critical care cardiology has evolved considerably over the past 2 decades. Contemporary critical care cardiology is increasingly focused on the management of patients with advanced
This is not a required assignment but it is recommended.
 SU 12 Name: This is not a required assignment but it is recommended. BIO 116 - Anatomy & Physiology II Practice Assignment 2 - The Respiratory and Cardiovascular Systems 1. The exchange of oxygen and carbon
SU 12 Name: This is not a required assignment but it is recommended. BIO 116 - Anatomy & Physiology II Practice Assignment 2 - The Respiratory and Cardiovascular Systems 1. The exchange of oxygen and carbon
This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors
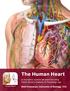 1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
1 This lab activity is aligned with Visible Body s A&P app. Learn more at visiblebody.com/professors 2 PRE-LAB EXERCISES: A. Watch the video 29.1 Heart Overview and make the following observations: 1.
AN ATOMY OF THE CARDIOVASCULAR SYSTEM
 Student Name CHAPTER 18 AN ATOMY OF THE CARDIOVASCULAR SYSTEM T he heart is actually two pumps one moves blood to the lungs, the other pushes it out into the body. These two functions seem rather elementary
Student Name CHAPTER 18 AN ATOMY OF THE CARDIOVASCULAR SYSTEM T he heart is actually two pumps one moves blood to the lungs, the other pushes it out into the body. These two functions seem rather elementary
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension
 Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
Tohoku J. Exp. Med., 1994, 174, 41-48 Late Results after Correction of Ventricular Septal Defect with Severe Pulmonary Hypertension KIYOSHI HANEDA, NAOSHI SATO, TAKAO TOGO, MAKOTO MIURA, MASAKI RATA and
BOGOMOLETS NATIONAL MEDICAL UNIVERSITY DEPARTMENT OF HUMAN ANATOMY. Guidelines. Module 2 Topic of the lesson Aorta. Thoracic aorta.
 BOGOMOLETS NATIONAL MEDICAL UNIVERSITY DEPARTMENT OF HUMAN ANATOMY Guidelines Academic discipline HUMAN ANATOMY Module 2 Topic of the lesson Aorta. Thoracic aorta. Course 1 The number of hours 3 1. The
BOGOMOLETS NATIONAL MEDICAL UNIVERSITY DEPARTMENT OF HUMAN ANATOMY Guidelines Academic discipline HUMAN ANATOMY Module 2 Topic of the lesson Aorta. Thoracic aorta. Course 1 The number of hours 3 1. The
Chapter 13 Worksheet Code It
 Class: Date: Chapter 13 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. A cardiac catheterization diverts blood from the heart to the aorta. 2. Selective vascular
Class: Date: Chapter 13 Worksheet 3 2 1 Code It True/False Indicate whether the statement is true or false. 1. A cardiac catheterization diverts blood from the heart to the aorta. 2. Selective vascular
Aberrant Right Subclavian Artery Aneurysm
 Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Επεμβατικές στρατηγικές στην πνευμονική υπέρταση
 Επεμβατικές στρατηγικές στην πνευμονική υπέρταση Παναγιώτης Καρυοφύλλης Καρδιολόγος Ωνάσειο Καρδιοχειρουργικό Κέντρο Mortality in PAH 2015 ESC/ERS Guidelines. Treatment algorithm Since BAS is performed
Επεμβατικές στρατηγικές στην πνευμονική υπέρταση Παναγιώτης Καρυοφύλλης Καρδιολόγος Ωνάσειο Καρδιοχειρουργικό Κέντρο Mortality in PAH 2015 ESC/ERS Guidelines. Treatment algorithm Since BAS is performed
Coding Companion for Cardiology/Cardiothoracic/ Vascular Surgery. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Cardiology/Cardiothoracic/ Vascular Surgery A comprehensive illustrated guide to coding and reimbursement 2014 Contents Getting Started with Coding Companion...i Chest Wall...1 General
Coding Companion for Cardiology/Cardiothoracic/ Vascular Surgery A comprehensive illustrated guide to coding and reimbursement 2014 Contents Getting Started with Coding Companion...i Chest Wall...1 General
Ann Vasc Dis Vol. 6, No. 3; 2013; pp Online August 12, Annals of Vascular Diseases doi: /avd.oa Original Article
 Ann Vasc Dis Vol. 6, No. 3; 2013; pp 578 582 Online August 12, 2013 2013 Annals of Vascular Diseases doi:10.3400/avd.oa.13-00056 Original Article Respiratory and Hemodynamic Changes in Patients with Chronic
Ann Vasc Dis Vol. 6, No. 3; 2013; pp 578 582 Online August 12, 2013 2013 Annals of Vascular Diseases doi:10.3400/avd.oa.13-00056 Original Article Respiratory and Hemodynamic Changes in Patients with Chronic
Anatomy and Physiology, Spring 2015 Exam II: Form A April 9, Name Student Number
 Anatomy and Physiology, Spring 2015 Exam II: Form A April 9, 2015 Name Student Number For Questions 1 2 refer to the following table. 1 Ventricular pressure is greater than aortic 6 AV valve is open 2
Anatomy and Physiology, Spring 2015 Exam II: Form A April 9, 2015 Name Student Number For Questions 1 2 refer to the following table. 1 Ventricular pressure is greater than aortic 6 AV valve is open 2
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation
 Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
Extracorporeal Life Support (ECLS) as a Bridge to Decision in Lung Transplantation Gabriel Loor, MD Baylor St. Lukes Medical Center Surgical Director Lung Transplantation Co-chief Section of Adult Cardiac
06/04/2013 ISHLT. 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013
 LUNG TRANSPLANTS The Journal of Heart and Lung Transplantation, 2012 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013 LUNG TRANSPLANTATION:STATE OF THE ART L. Santambrogio
LUNG TRANSPLANTS The Journal of Heart and Lung Transplantation, 2012 2 International Conference on Respiratory Physiotherapy ARIR Genova, March 21 23, 2013 LUNG TRANSPLANTATION:STATE OF THE ART L. Santambrogio
AORTIC COARCTATION. Synonyms: - Coarctation of the aorta
 AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
AORTIC COARCTATION Synonyms: - Coarctation of the aorta Definition: Aortic coarctation is a congenital narrowing of the aorta, usually located after the left subclavian artery, near the ductus or the ligamentum
Unilateral Lung Transplantation Using Right and Left Upper Lobes: An Experimental
 Unilateral Lung Transplantation Using Right and Left Upper Lobes: An Experimental Study Hitoshi Nishikawa, M.D., Takahiro Oto, M.D., Ph.D., Shinji Otani, M.D., Ph.D., Masaaki Harada, M.D., Norichika Iga,
Unilateral Lung Transplantation Using Right and Left Upper Lobes: An Experimental Study Hitoshi Nishikawa, M.D., Takahiro Oto, M.D., Ph.D., Shinji Otani, M.D., Ph.D., Masaaki Harada, M.D., Norichika Iga,
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine
 Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Heart transplantation is the gold standard treatment for
 Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Organ Care System for Heart Procurement and Strategies to Reduce Primary Graft Failure After Heart Transplant Masaki Tsukashita, MD, PhD, and Yoshifumi Naka, MD, PhD Primary graft failure is a rare, but
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments
 Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Done By : Rahmeh Alsukkar Date : 26 /10/2017 slide 23 The lobes in the right and left lungs are divided into segments,which called bronchopulmonary segments Each segmental bronchus passes to a structurally
Heart Transplantation for Patients with a Fontan Procedure
 Heart Transplantation for Patients with a Fontan Procedure Kirk R. Kanter MD Professor of Surgery Pediatric Cardiac Surgery Emory University School of Medicine Children s Healthcare of Atlanta Atlanta,
Heart Transplantation for Patients with a Fontan Procedure Kirk R. Kanter MD Professor of Surgery Pediatric Cardiac Surgery Emory University School of Medicine Children s Healthcare of Atlanta Atlanta,
Pulmonary thromboendarterectomy (PTE) is indicated for
 Pulmonary Thromboendarterectomy Steven R. Meyer, MD, PhD, and Christopher G.A. McGregor, MB, FRCS, MD (Hons) Division of Cardiovascular Surgery, Department of Surgery, Mayo Clinic, Rochester, Minnesota.
Pulmonary Thromboendarterectomy Steven R. Meyer, MD, PhD, and Christopher G.A. McGregor, MB, FRCS, MD (Hons) Division of Cardiovascular Surgery, Department of Surgery, Mayo Clinic, Rochester, Minnesota.
10/23/2017. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
The External Anatomy of the Lungs. Prof Oluwadiya KS
 The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
Heart-lung transplantation: adult indications and outcomes
 Brief Report Heart-lung transplantation: adult indications and outcomes Yoshiya Toyoda, Yasuhiro Toyoda 2 Temple University, USA; 2 University of Pittsburgh, USA Correspondence to: Yoshiya Toyoda, MD,
Brief Report Heart-lung transplantation: adult indications and outcomes Yoshiya Toyoda, Yasuhiro Toyoda 2 Temple University, USA; 2 University of Pittsburgh, USA Correspondence to: Yoshiya Toyoda, MD,
Anatomy of the Heart
 Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
Biology 212: Anatomy and Physiology II Anatomy of the Heart References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapter
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th & 12 th Eds.)
 PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
PLEURAL CAVITY AND LUNGS Dr. Milton M. Sholley SELF STUDY RESOURCES Essential Clinical Anatomy 3 rd ed. (ECA): pp. 70 81 Syllabus: 6 pages (Page 6 lists corresponding figures for Grant's Atlas 11 th &
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Policy Specific Section: May 16, 1984 April 9, 2014
 Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Medical Policy Heart Transplant Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Transplant Original Policy Date: Effective Date: May 16, 1984 April 9, 2014 Definitions
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Corticosteroids and Prevention of Pulmonary Damage Following Cardiopulmonary Bypass in Puppies
 Corticosteroids and Prevention of Pulmonary Damage Following Cardiopulmonary Bypass in Puppies David G. Hill, M.D., Mary Jane Aguilar, Jon C. Kosek, M.D., and J. Donald Hill, M.D., M.D. ABSTRACT A technique
Corticosteroids and Prevention of Pulmonary Damage Following Cardiopulmonary Bypass in Puppies David G. Hill, M.D., Mary Jane Aguilar, Jon C. Kosek, M.D., and J. Donald Hill, M.D., M.D. ABSTRACT A technique
Pulmonary vascular anatomy & anatomical variants
 Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Review Article Pulmonary vascular anatomy & anatomical variants Asha Kandathil, Murthy Chamarthy Department of Radiology, University of Texas Southwestern Medical Center, Dallas, TX, USA Contributions:
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Human Heart Transplantation: Current Status
 Human Heart Transplantation: Current Status Randall B. Griepp, M.D., Edward B. Stinson, M.D.," Charles P. Bieber, M.D., Bruce A. Reitz, M.D., Jack G. Copeland, M.D., Philip E. Oyer, M.D., and Norman E.
Human Heart Transplantation: Current Status Randall B. Griepp, M.D., Edward B. Stinson, M.D.," Charles P. Bieber, M.D., Bruce A. Reitz, M.D., Jack G. Copeland, M.D., Philip E. Oyer, M.D., and Norman E.
Anatomy of the Lungs. Dr. Gondo Gozali Department of anatomy
 Anatomy of the Lungs Dr. Gondo Gozali Department of anatomy 1 Pulmonary Function Ventilation and Respiration Ventilation is the movement of air in and out of the lungs Respiration is the process of gas
Anatomy of the Lungs Dr. Gondo Gozali Department of anatomy 1 Pulmonary Function Ventilation and Respiration Ventilation is the movement of air in and out of the lungs Respiration is the process of gas
The Heart. The Heart A muscular double pump. The Pulmonary and Systemic Circuits
 C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
C H A P T E R 19 The Heart The Heart A muscular double pump circuit takes blood to and from the lungs Systemic circuit vessels transport blood to and from body tissues Atria receive blood from the pulmonary
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D.
 Combined Valvular and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D. ABSTRACT Between July, 97, and March, 975,45 patients underwent combined valvular
Combined Valvular and Coronary Artery Surgery George M. Callard, M.D., John B. Flege, Jr., M.D., and Joseph C. Todd, M.D. ABSTRACT Between July, 97, and March, 975,45 patients underwent combined valvular
Use of the Total Artificial Heart in the Failing Fontan Circulation J William Gaynor, M.D.
 Use of the Total Artificial Heart in the Failing Fontan Circulation J William Gaynor, M.D. Daniel M. Tabas Endowed Chair in Pediatric Cardiothoracic Surgery at The Children s Hospital of Philadelphia The
Use of the Total Artificial Heart in the Failing Fontan Circulation J William Gaynor, M.D. Daniel M. Tabas Endowed Chair in Pediatric Cardiothoracic Surgery at The Children s Hospital of Philadelphia The
Listing Form: Heart or Cardiovascular Impairments. Medical Provider:
 Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Listing Form: Heart or Cardiovascular Impairments Medical Provider: Printed Name Signature Patient Name: Patient DOB: Patient SS#: Date: Dear Provider: Please indicate whether your patient s condition
Anatomy & Physiology
 1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
1 Anatomy & Physiology Heart is divided into four chambers, two atrias & two ventricles. Atrioventricular valves (tricuspid & mitral) separate the atria from ventricles. they open & close to control flow
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column,
 Dr. Gary Mumaugh Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column, posterior to the sternum Posteriorly the
Dr. Gary Mumaugh Approximately the size of your fist Location Superior surface of diaphragm Left of the midline in mediastinum Anterior to the vertebral column, posterior to the sternum Posteriorly the
