doi: /j.athoracsur
|
|
|
- Harvey Blankenship
- 5 years ago
- Views:
Transcription
1 doi: /j.athoracsur
2 1 Appropriate Route Selection for Extracardiac Total Cavopulmonary Connection in Apicocaval Juxtaposition Sei Morizumi, MD, Hideyuki Kato, MD, Shinya Kanemoto, MD, PhD, Mio Noma, MD, PhD, Masakazu Abe, MD, PhD, Yuzuru Sakakibara, MD, PhD, and Yuji Hiramatsu, MD, PhD Department of Cardiovascular Surgery, Faculty of Medicine, University of Tsukuba, Tsukuba, Japan Running Head; Keywords; CHD-Fontan, CHD-univentricular heart, Outcomes Word Count; 3486 words Address for correspondence: Yuji Hiramatsu, MD, PhD Department of Cardiovascular Surgery, Faculty of Medicine, University of Tsukuba Tennodai, Tsukuba , Japan Tel; Fax;
3 2 [Abstract] Background. A malpositioned heart with apicocaval juxtaposition may complicate the management of patients with functional single ventricles when total cavopulmonary connection is performed. We reviewed our experience with extracardiac total cavopulmonary connection in patients with apicocaval juxtaposition with a special focus on route selection and outcomes. Methods. Out of 68 patients who underwent extracardiac total cavopulmonary connection at our hospitals, 10 patients with apicocaval juxtaposition were included in this study. The mean follow-up was 40 ± 28 months. Patient demographics were compared with data on patients without apicocaval juxtaposition. Results. The age at operation was 8 ± 7 years. We carefully chose conduit routes to create satisfactory fluid dynamics. The conduit was placed between the inferior vena cava and the ipsilateral pulmonary artery in 2 patients, and the conduit crossed midline in 8. The mean postoperative pulmonary artery pressure was 13 ± 2 mmhg. The surgical and postoperative data were not significantly different when compared with the patients without apicocaval juxtaposition. There were no conduit-related early or late complications except for one patient who had poor ventricular function. Conclusions. Extracardiac total cavopulmonary connection in apicocaval juxtaposition can be carried out with favorable mid-term outcomes. The route between the inferior vena cava and the contralateral pulmonary artery should be the primary choice when the relevant pulmonary artery is in good shape. Care must be taken in regard to critical conduit oppression by the ventricle in cases with large ventricular volume and/or poor ventricular function. (243 words)
4 3 Since extracardiac total cavopulmonary connection (EC-TCPC) was first introduced as a definitive procedure for patients with functionally univentricular heart in 1990 [1], many surgeons have adopted this approach as their procedure of choice for the Fontan completion. It has been well established that EC-TCPC has potential advantages over lateral tunnel-type connection. It makes it possible to avoid aortic cross-clamping and atriotomy, therefore allowing for a shorter duration of cardiopulmonary bypass (CPB). Near-optimal laminar flow in the systemic venous pathway means no atrial stretch or arrhythmia in the long-term, although the prosthetic conduit lacks growth potential and patients may be obliged to have lifelong prophylactic anticoagulant therapy [2-4]. In a malpositioned univentricular heart with apicocaval juxtaposition (ACJ), however, the completion of EC-TCPC may be compromised by difficulty in securing an appropriate conduit pathway. When the conduit is positioned behind the apex toward the ipsilateral pulmonary artery (PA), obstruction of the conduit or oppression either on the pulmonary veins, atrium or ventricle is of concern because of the narrow space. On the other hand, when the conduit crosses the midline toward the contralateral PA, a long curved conduit route may cause a kink or serious energy loss. Little is known about the outcome of the EC-TCPC for ACJ because of the rare morphological features of this alignment. Only one recent clinical investigation has focused on this issue [5] and several others are case or technical reports [6-9]. We therefore set out to examine our experience with EC-TCPC in ACJ and shed some light on the factors which influence the decision on route choice. Patients and Methods Patients Between 2001 and 2011, 68 patients underwent EC-TCPC at our two pediatric centers (University of Tsukuba Hospital and Ibaraki Children s Hospital) following the same management policy. Among them, we retrospectively reviewed the medical records of 10 patients with functional single ventricle and ACJ. Charts were examined for patient demographics including age, weight, diagnosis, conduit route, conduit size, pre-
5 4 and postoperative hemodynamic data, additional cardiac operations, and operative details. Endpoints included take down, thromboembolic events and death. These data were compared with the data of 58 patients without ACJ. The study was approved by the Institutional Review Board at University of Tsukuba Hospital and Ibaraki Children s Hospital, and individual consent for the study was waived owing to its retrospective medical record review design. Operative Technique Based on a careful preoperative evaluation, we chose a conduit route to create the most appropriate cephalad (conduit to the PA) anastomosis which would provide satisfactory fluid dynamics for Fontan circulation. After re-do median sternotomy, dissection around the heart was carefully performed. CPB was established with direct bicaval cannulation. The heart was arrested by aortic cross clamping with cold crystalloid cardioplegia infusion through the aortic root when intracardiac manipulation such as the creation of an atrial septal defect, valve repair or main PA division was required. Otherwise an extracardiac conduit (Gore-Tex, Stretch Vascular Graft) was anastomosed with the caudal surface of either the right or left PA on the beating heart. In 2 patients the extracardiac conduit was placed between the inferior vena cava (IVC) and the ipsilateral PA behind the ventricle to create the shortest route. In the 8 other patients the conduit was placed between the IVC and the contralateral PA taking a slightly roundabout route. After extensive dissection and mobilization of the IVC at the diaphragmatic level, the caudal end of the conduit was sutured to the transected IVC in an end-to-end fashion. A fenestration was created only in patient No.8 who had a dilated ventricle with poor function. Postoperative Evaluation A routine postoperative evaluation was made by echocardiography, cineangiography and cardiac catheterization about 1 month after surgery and postoperative PA pressure was measured. Some patients underwent cardiac catheterization about 1 year after surgery, but this is not routine. Computed tomography
6 5 (CT) was performed only when follow-up physicians requested it for evaluation. Anticoagulation Anticoagulation therapy with intravenous heparin infusion (200 U/kg/day) was initiated within 12 hours after surgery when hemostasis was secured. Subsequently heparin was replaced by warfarin sodium as soon as the patients resumed oral intake. Thereafter the international normalized ratio of prothrombin time was maintained at Statistical Analysis All of the patients data were reviewed retrospectively from the database of the University of Tsukuba Hospital and Ibaraki Children s Hospital. Quantitative data are presented as mean ± standard deviation. Comparisons between the two groups were performed with an unpaired two-tailed t-test for normally distributed variables. Statistical significance was considered at p values less than Results Patient Characteristics The characteristics of the patients with ACJ are listed in Table 1. The diagnoses of these patients included the heterotaxy syndrome (n = 4, right isomerism in 3 cases, left isomerism in 1), right ventricular type univentricular heart (n = 1), double outlet right ventricle (n = 2), double inlet left ventricle (n = 1), and univentricular heart with indefinite ventricular type (n = 2). The mean age at operation was 8 ± 7 years (range, 3-24), and the mean body weight was 22.1 ± 14.8 kg (range, ). Preoperative cardiac catheterization showed adequate hemodynamic data for Fontan-type repair, with Nakata-index of 272 ± 160 mm 2 /m 2 (range, ) and a mean PA pressure of 11 ± 4 mmhg (range, 6 18). All 10 patients underwent bidirectional cavopulmonary connection before EC-TCPC based on a staged Fontan strategy. There was no significant difference in the preoperative patient characteristics when compared with the 58
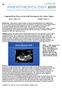
7 6 patients without ACJ (Table 2). Surgical Outcomes In the patients with ACJ, the mean CPB time was 196 ± 67 minutes (range, minutes). The heart was arrested only when intracardiac manipulation was required. The diameter of the extracardiac conduit was 16 mm in 1 patient, 18 mm in 8 patients, and 20 mm in 1 patient. The mean postoperative PA pressure was 13 ± 2 mmhg (range, mmhg, including the last data on patient No. 8). The median duration of intensive care unit stay was 6 days. The mean follow-up was 40 ± 28 months (range, 2-71 months). These surgical and postoperative data were not significantly different when compared with the patients without ACJ (Table 2). There was no conduit-related reoperation in any patient expect for 1 in whom acute conduit occlusion developed. Postoperative cineangiogram (Fig 1) and CT (Fig 2) showed a curved but unobstructed venous pathway when the conduit was placed between the IVC and the contralateral PA. On the other hand, in a case in which the conduit was positioned behind the apex, CT showed no conduit obstruction or oppression either on the pulmonary veins or ventricle, although slight compression on the atrium was seen (Fig 3). One young adult patient with double outlet of right ventricle (No.8) developed acute thrombotic occlusion of the conduit on the 8th postoperative day. Despite efforts with surgical thrombectomy and thrombolysis, the patient died due to bleeding and multiple organ dysfunctions within 48 hours. Since the patient had a large and poorly functioning single right ventricle (ejection fraction 41%, diastolic diameter 65mm), an extracardiac TCPC was selected instead of an intracardiac tunnel to avoid cardiac arrest, and a fenestrated conduit was placed between the IVC and the contralateral PA so as to avoid compression behind the enlarged ventricle. Still, the conduit was constricted between the bottom of the enlarged ventricle and the diaphragm. Among the 67 other TCPC cases, none of the patients experienced early or late death, conduit stenosis or pulmonary venous obstruction.
8 7 Comments Our experience shows favorable clinical EC-TCPC outcomes in patients with functional single ventricle and ACJ. Nine of 10 patients tolerated EC-TCPC without early mortality, re-exploration, take down or significant morbidity. Either conduit route could be conducted without external compression, pulmonary venous obstruction or thromboembolic event. Based on our experience, the route between the IVC and the contralateral PA should take precedence over the route behind the ventricle since a space for the conduit placement can be easily secured without flipping over the ventricle or extensive dissection. The biggest concern in this design is a relatively longer and curved conduit which crosses the midline toward the contralateral PA and may therefore lead to a certain amount of energy loss. However, no excessive venous resistance, kinks or thromboembolic events were encountered in this roundabout route in the standard risk cases. We do not think that conduit oppression by the spine is a serious matter because the IVC usually locates anterior to the spine in normal anatomy and even in heterotaxy (Fig 2). Probably the most important factor in choosing the conduit route is the facility in making a satisfactory cephalad anastomosis which provides better fluid dynamics in Fontan circulation. If one of the PAs is good in size without severe adhesion, calcification or previous stenting, and can be exposed widely against the aorta, it is preferable as a site for cephalad anastomosis. The need for pulmonary augmentation can be another inevitable reason in selecting the anastomotic site. A conduit can then be conducted towards the IVC in either way. When both PAs are in equal condition, although route choice depends on space availability and severity of adhesion, it is quite rational to choose the route between the IVC and the contralateral PA with minimal dissection. In this setting, a fenestration can be easily created even after cessation of CPB since the conduit and the atrium are adjacent to each other. The reasons we chose the route behind the ventricle as exceptions in two of our cases are as follows. In case No.5, there was tight adhesion and calcification at the right PA (contralateral to the IVC) after repeated surgical manipulations in previous PA plasty procedures. In case No.6, the right PA (contralateral to the IVC) was a little smaller than the opposite PA and angled off toward the posterior. In addition, since the enlarged
9 8 ascending aorta was overlying the right PA, it was better to secure a cephalad anastomosis onto the left PA. In both cases, conduit space behind the atrium and ventricle was relaxed by opening the pleural cavity. Maximum efforts were made to avoid pulmonary venous obstruction by aggressive dissection around the pulmonary veins. In adult patients with dilated ventricles with poor function as in our case No. 8, a conduit route should be created very carefully [10, 11]. Our choice was not successful since the space between the bottom of the enlarged ventricle and the diaphragm was probably too narrow and therefore the long conduit was compressed and inevitably had a nearly right-angled curve around the IVC anastomotic site. With such conditions, an intraatrial tunnel could be an alternative but such a complex procedure requires aortic cross clamping and cardiac arrest, and therefore may deteriorate ventricular function [12]. Kawahira and colleagues described a modified Fontan technique with a handmade shoetree extracardiac graft which gently bridged the vertebra in a patient with ACJ [8]. The technique may be effective in anastomosing the IVC orifice with the conduit without creating an obstructive venous pathway. In the literature, there are only a few reports which have addressed the issue of EC-TCPC in patients with ACJ. Surprisingly, these reports and several other case presentations have all come from Japan or South Korea [5-9]. It is well known that there is a higher incidence of heterotaxy in eastern Asia, but there may be a higher incidence of ACJ as well. Previous reports have not clearly mentioned how to decide upon an appropriate conduit route, although Sakurai and colleagues showed that there was no obvious superiority of the pathway behind the ventricle as compared with the pathway crossing the spine. They pointed out that the condition of the anastomotic site, dimension of the apex and need for pulmonary augmentation are important factors in selecting the pathway [5]. In the present report, we clearly state that the route between the IVC and the contralateral PA should be the primary choice as far as there is no concern about PA size and condition since the route is less invasive and technically beneficial.
10 9 Study Limitations This is a retrospective, observational study. Although all patients had clear documentation of pre- and postoperative variables, other interesting variables such as pulmonary vascular resistance and dimension of the atrium or ventricle were less well documented and could not be examined in relation to the outcome. As the study covered more than 25 years of experience since first palliation, older patients could be treated on the palliation policy in the early surgical era. Moreover, since the number of ACJ patients for each conduit pathway was small, comparative analyses with regard to outcome for each group could not been performed. In conclusion, EC-TCPC for patients with functional single ventricle and ACJ can be carried out with favorable mid-term outcomes. The route between the IVC and the contralateral PA should be the primary choice if the PA is in good shape. Care must be taken regarding critical conduit oppression by the ventricle in cases with large ventricular volume and/or poor ventricular function. Acknowledgment The authors wish to thank Joseph H. Gorman, III, MD, University of Pennsylvania for the language review.
11 10 References 1) Marcelletti C, Corno A, Giannico S, et al. Inferior vena cava-pulmonary artery extracardiac conduit. A new form of right heart bypass. J Thorac Cardiovasc Surg 1995;110: ) Marcelletti CF, Iorio FS, Abella RF, et al. Late results of extracardiac Fontan repair. Semin Thorac Cardiovasc Surg Pediatr Card Surg Annu 1999;2: ) Tokunaga S, Kado H, Imoto Y, et al. Total cavopulmonary connection with an extracardiac conduit: Experience with 100 patients. Ann Thorac Surg 2002;73: ) Schreiber C, Horer J, Vogt M, et al. Nonfenestrated extracardiac total cavopulmonary connection in 132 consecutive patients. Ann Thorac Surg 2007;84: ) Sakurai T, Kado H, Nakano T, et al. The impact of extracardiac conduit-total cavopulmonary connection on apicocaval juxtaposition. Eur J Cardiothorac Surg 2010;38: ) Hisaoka T, Hiramatsu T, Okamura Y. Total cavopulmonary connection with straight conduit for apicocaval juxtaposition. Gen Thorac Cardiovasc Surg 2009;57: ) Kitayama H, Oku H, Matsumoto T, Onoe M. Total cavopulmonary connection using a pedicled pericardial conduit for a patient with apicocaval juxtaposition. Ann Thorac Surg 2001;72: ) Kawahira Y, Nishigaki K, Ueno T. Extracardiac Fontan procedure bridging the vertebra for apicocaval juxtaposition. Ann Thorac Surg 2006;82: ) Lim HG, Kim WH, Oh SS, et al. Alternative Fontan connection for apicocaval juxtaposition. Ann Thorac Surg 2005;79: ) Fujii Y, Sano S, Kotani Y, et al. Midterm to long-term outcome of total cavopulmonary connection in high-risk adult candidates. Ann Thorac Surg 2009;87: ) Burkhalt HM, Dearani JA, Mair DD, et al. The modified Fontan procedure: early and late results in 132 adult patients. J Thorac Cardiovasc Surg 2003;125: ) Yoshikawa Y, Ishibashi H, Uemura H, Kawahira Y, Yagihara T. Pathologic findings in atrial musculature seven years after the intraatrial tunnel Fontan. Ann Thorac Surg 2002;73:663-4
12 11 Table 1. Patients' Characteristics, and Pre-, Intra and Postoperative Data in Apicocaval Juxtaposition No. Diagnosis Age Weight PAI Preop mpap Conduit Route CPB AXC Fenestration Postop mpap Follow Up Adverse Event Prognosis (year) (kg) (mm 2 /m 2 ) (mmhg) (mm) (min) (min) (mmhg) (month) 1 SV, PA, Dextrocardia Contra Alive 2 SV, PA, Situs Inversus Contra Alive 3 DORV, PS, Situs Inversus Contra Alive 4 SV, PS, Asplenia Contra Alive 5 RV type SV, PA, Situs Inversus Ipsi Alive 6 Hypoplastic LV, AVSD, TOF Ipsi Alive Polysplenia 7 SV, PS, Asplenia, Dextrocardia Contra Alive TAPVC Ia 8 DORV, TA, PS, Dextrocardia Contra (20) - Conduit Occlusion Dead 9 DILV, PS Contra Alive 10 SV, PS, Asplenia, Dextrocardia Contra Alive TAPVC III AVSD = atrioventricular septal defect; AXC = aortic cross clamp; Contra = IVC-contralateral PA route; DILV = double inlet left ventricle; DORV = double outlet right ventricle; Ipsi = IVC-ipsilateral PA route; mpap = mean pulmonary artery pressure; PA = pulmonary atresia; PAI = pulmonary artery index (Nakata index); PS = pulmonary stenosis; SV = single ventricle; TA = tricuspid atresia; TAPVC = total anomalous of pulmonary venous connection; TOF = tetralogy of Fallot
13 12 Table 2. Comparison of Two Groups Regarding Pre-, Intra- and Postoperative Data Patients with ACJ Patients without ACJ p Value (n = 10) (n = 58) Age (year) 8 ± 7 5 ± Body Weight (kg) 22.1 ± ± PAI (mm 2 /m 2 ) 272 ± ± Preoperative mpap (mmhg) 11 ± 4 11 ± CPB time (minute) 196 ± ± Diameter of Conduit 16mm mm mm 1 1 Fenestration 1 (No. 8) 4 Postoperative mpap (mmhg) 13 ± 2 14 ± ICU Stay (day) 6 ± 2 5 ± Follow Up (month) 40 ± ± Adverse Event Thrombosis 1 (No. 8) 0 Death 1 (No. 8) 0 ACJ = apicocaval juxtaposition; CPB = cardiopulmonary bypass; ICU = intensive care unit; mpap = mean pulmonary artery pressure; PAI = pulmonary artery index (Nakata index)
14 13 Figure Legends Fig 1. Cineangiogram of the extracardiac conduit shows a curved and unobstructed venous pathway in the inferior vena cava to the contralateral pulmonary artery route in a patient with apicocaval juxtaposition. Fig 2. Computed tomography image of the extracardiac conduit placed between the inferior vena cava (IVC) and the contralateral pulmonary artery in an asplenia patient with apicocaval juxtaposition (patient No. 10, Two months after surgery). (A to D) Four levels from the cephalad anastomosis to the IVC. The conduit crosses midline but is not oppressed by the spine since the IVC locates anterior to the spine. (A = atrium; C = conduit; PA = pulmonary artery; PV = pulmonary vein; V = ventricle) Fig 3. Computed tomography image of the extracardiac conduit placed between the inferior vena cava (IVC) and the ipsilateral pulmonary artery in a patient with apicocaval juxtaposition (patient No. 5, Seven years after surgery). (A, B) Cephalad portion of the conduit locates between the atrium and the pulmonary veins. The conduit slightly presses the atrium but not the pulmonary veins. (C, D) Caudal portion of the conduit near the IVC. The conduit has no contact with the ventricle throughout the route. (A = atrium; C = conduit; PV = pulmonary vein; V = ventricle)
15 Figure 1 14
16 Figure 2 15
17 Figure 3 16
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions
 Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
Appendix A.1: Tier 1 Surgical Procedure Terms and Definitions Tier 1 surgeries AV Canal Atrioventricular Septal Repair, Complete Repair of complete AV canal (AVSD) using one- or two-patch or other technique,
The evolution of the Fontan procedure for single ventricle
 Hemi-Fontan Procedure Thomas L. Spray, MD The evolution of the Fontan procedure for single ventricle cardiac malformations has included the development of several surgical modifications that appear to
Hemi-Fontan Procedure Thomas L. Spray, MD The evolution of the Fontan procedure for single ventricle cardiac malformations has included the development of several surgical modifications that appear to
The pericardial sac is composed of the outer fibrous pericardium
 Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Pericardiectomy for Constrictive or Recurrent Inflammatory Pericarditis Mauricio A. Villavicencio, MD, Joseph A. Dearani, MD, and Thoralf M. Sundt, III, MD Anatomy and Preoperative Considerations The pericardial
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Staged palliation culminating in a successful Fontan
 Extracardiac Conduit Fontan Procedure Scott M. Bradley, MD Staged palliation culminating in a successful Fontan procedure is the current surgical goal for most patients with a functional single ventricle.
Extracardiac Conduit Fontan Procedure Scott M. Bradley, MD Staged palliation culminating in a successful Fontan procedure is the current surgical goal for most patients with a functional single ventricle.
In 1980, Bex and associates 1 first introduced the initial
 Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Technique of Aortic Translocation for the Management of Transposition of the Great Arteries with a Ventricular Septal Defect and Pulmonary Stenosis Victor O. Morell, MD, and Peter D. Wearden, MD, PhD In
Segmental approach to normal and abnormal situs arrangement - Echocardiography -
 Segmental approach to normal and abnormal situs arrangement - Echocardiography - Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London No disclosures
Segmental approach to normal and abnormal situs arrangement - Echocardiography - Jan Marek Great Ormond Street Hospital & Institute of Cardiovascular Sciences, University College London No disclosures
Heart Transplantation in Patients with Superior Vena Cava to Pulmonary Artery Anastomosis: A Single-Institution Experience
 Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
Korean J Thorac Cardiovasc Surg 2018;51:167-171 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.3.167 Heart Transplantation in Patients with Superior
CMR for Congenital Heart Disease
 CMR for Congenital Heart Disease * Second-line tool after TTE * Strengths of CMR : tissue characterisation, comprehensive access and coverage, relatively accurate measurements of biventricular function/
CMR for Congenital Heart Disease * Second-line tool after TTE * Strengths of CMR : tissue characterisation, comprehensive access and coverage, relatively accurate measurements of biventricular function/
Cardiac Catheterization Cases Primary Cardiac Diagnoses Facility 12 month period from to PRIMARY DIAGNOSES (one per patient)
 PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
PRIMARY DIAGNOSES (one per patient) Septal Defects ASD (Atrial Septal Defect) PFO (Patent Foramen Ovale) ASD, Secundum ASD, Sinus venosus ASD, Coronary sinus ASD, Common atrium (single atrium) VSD (Ventricular
Conversion of Atriopulmonary to Cavopulmonary Anastomosis in Management of Late Arrhythmias and Atrial Thrombosis
 Conversion of Atriopulmonary to Cavopulmonary Anastomosis in Management of Late Arrhythmias and Atrial Thrombosis Jane M. Kao, MD, Juan c. Alejos, MD, Peter W. Grant, MD, Roberta G. Williams, MD, Kevin
Conversion of Atriopulmonary to Cavopulmonary Anastomosis in Management of Late Arrhythmias and Atrial Thrombosis Jane M. Kao, MD, Juan c. Alejos, MD, Peter W. Grant, MD, Roberta G. Williams, MD, Kevin
Children with Single Ventricle Physiology: The Possibilities
 Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
Children with Single Ventricle Physiology: The Possibilities William I. Douglas, M.D. Pediatric Cardiovascular Surgery Children s Memorial Hermann Hospital The University of Texas Health Science Center
The Double Switch Using Bidirectional Glenn and Hemi-Mustard. Frank Hanley
 The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
The Double Switch Using Bidirectional Glenn and Hemi-Mustard Frank Hanley No relationships to disclose CCTGA Interesting Points for Discussion What to do when. associated defects must be addressed surgically:
Surgical Treatment for Double Outlet Right Ventricle. Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery
 for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
for Double Outlet Right Ventricle Masakazu Nakao Consultant, Paediatric Cardiothoracic Surgery 1 History Intraventricular tunnel (Kawashima) First repair of Taussig-Bing anomaly (Kirklin) Taussig-Bing
The Rastelli procedure has been traditionally used for repair
 En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
En-bloc Rotation of the Truncus Arteriosus A Technique for Complete Anatomic Repair of Transposition of the Great Arteries/Ventricular Septal Defect/Left Ventricular Outflow Tract Obstruction or Double
Perioperative Management of DORV Case
 Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Perioperative Management of DORV Case James P. Spaeth, MD Department of Anesthesia Cincinnati Children s Hospital Medical Center University of Cincinnati Objectives: 1. Discuss considerations regarding
Techniques for repair of complete atrioventricular septal
 No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
No Ventricular Septal Defect Patch Atrioventricular Septal Defect Repair Carl L. Backer, MD *, Osama Eltayeb, MD *, Michael C. Mongé, MD *, and John M. Costello, MD For the past 10 years, our center has
Common Defects With Expected Adult Survival:
 Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
Common Defects With Expected Adult Survival: Bicuspid aortic valve :Acyanotic Mitral valve prolapse Coarctation of aorta Pulmonary valve stenosis Atrial septal defect Patent ductus arteriosus (V.S.D.)
An anterior aortoventriculoplasty, known as the Konno-
 The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
The Konno-Rastan Procedure for Anterior Aortic Annular Enlargement Mark E. Roeser, MD An anterior aortoventriculoplasty, known as the Konno-Rastan procedure, is a useful tool for the cardiac surgeon. Originally,
Obstructed total anomalous pulmonary venous connection
 Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
Total Anomalous Pulmonary Venous Connection Richard A. Jonas, MD Children s National Medical Center, Department of Cardiovascular Surgery, Washington, DC. Address reprint requests to Richard A. Jonas,
The vast majority of patients, especially children, who
 Technique of Mechanical Pulmonary Valve Replacement John M. Stulak, MD, and Joseph A. Dearani, MD The vast majority of patients, especially children, who require pulmonary valve replacement (PVR), obtain
Technique of Mechanical Pulmonary Valve Replacement John M. Stulak, MD, and Joseph A. Dearani, MD The vast majority of patients, especially children, who require pulmonary valve replacement (PVR), obtain
9/8/2009 < 1 1,2 3,4 5,6 7,8 9,10 11,12 13,14 15,16 17,18 > 18. Tetralogy of Fallot. Complex Congenital Heart Disease.
 Current Indications for Pediatric CTA S Bruce Greenberg Professor of Radiology Arkansas Children s Hospital University of Arkansas for Medical Sciences greenbergsbruce@uams.edu 45 40 35 30 25 20 15 10
Current Indications for Pediatric CTA S Bruce Greenberg Professor of Radiology Arkansas Children s Hospital University of Arkansas for Medical Sciences greenbergsbruce@uams.edu 45 40 35 30 25 20 15 10
Intra- or extracardiac Fontan operation? A simple strategy when to do what
 Clinical research Intra- or extracardiac Fontan operation? A simple strategy when to do what Wlodzimierz Kuroczynski 1, David Senft 1, Amelie Elsaesser 2, Christoph Kampmann 1 1 Department of Pediatric
Clinical research Intra- or extracardiac Fontan operation? A simple strategy when to do what Wlodzimierz Kuroczynski 1, David Senft 1, Amelie Elsaesser 2, Christoph Kampmann 1 1 Department of Pediatric
Introduction. Study Design. Background. Operative Procedure-I
 Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
Risk Factors for Mortality After the Norwood Procedure Using Right Ventricle to Pulmonary Artery Shunt Ann Thorac Surg 2009;87:178 86 86 Addressor: R1 胡祐寧 2009/3/4 AM7:30 SICU 討論室 Introduction Hypoplastic
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE
 SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
SURGICAL TREATMENT AND OUTCOME OF CONGENITAL HEART DISEASE Mr. W. Brawn Birmingham Children s Hospital. Aims of surgery The aim of surgery in congenital heart disease is to correct or palliate the heart
CMS Limitations Guide - Radiology Services
 CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
CMS Limitations Guide - Radiology Services Starting October 1, 2015, CMS will update their existing medical necessity limitations on tests and procedures to correspond to ICD-10 codes. This limitations
Surgical Results in Patients With Pulmonary Atresia-Major Aortopulmonary Collaterals in Association With Total Anomalous Pulmonary Venous Connection
 Surgical Results in Patients With Pulmonary Atresia-Major Aortopulmonary Collaterals in Association With Total Anomalous Pulmonary Venous Connection Richard D. Mainwaring, MD, V. Mohan Reddy, MD, Olaf
Surgical Results in Patients With Pulmonary Atresia-Major Aortopulmonary Collaterals in Association With Total Anomalous Pulmonary Venous Connection Richard D. Mainwaring, MD, V. Mohan Reddy, MD, Olaf
Heart and Soul Evaluation of the Fetal Heart
 Heart and Soul Evaluation of the Fetal Heart Ivana M. Vettraino, M.D., M.B.A. Clinical Associate Professor, Michigan State University College of Human Medicine Objectives Review the embryology of the formation
Heart and Soul Evaluation of the Fetal Heart Ivana M. Vettraino, M.D., M.B.A. Clinical Associate Professor, Michigan State University College of Human Medicine Objectives Review the embryology of the formation
5.8 Congenital Heart Disease
 5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
5.8 Congenital Heart Disease Congenital heart diseases (CHD) refer to structural or functional heart diseases, which are present at birth. Some of these lesions may be discovered later. prevalence of Chd
Fontan Deterioration in Pediatric Cardiologist s s View. Pusan National University Hospital Hyoung Doo Lee M.D.
 Fontan Deterioration in Pediatric Cardiologist s s View Pusan National University Hospital Hyoung Doo Lee M.D. Outcomes of Fontan operation JTCS 2006:131;172-80 Mitchell ME et al Jan. 1992~Dec. 1999, 332
Fontan Deterioration in Pediatric Cardiologist s s View Pusan National University Hospital Hyoung Doo Lee M.D. Outcomes of Fontan operation JTCS 2006:131;172-80 Mitchell ME et al Jan. 1992~Dec. 1999, 332
Over the last 27 years, since Fontan and Baudet [1] Univentricular Repair: Is Routine Fenestration Justified?
![Over the last 27 years, since Fontan and Baudet [1] Univentricular Repair: Is Routine Fenestration Justified? Over the last 27 years, since Fontan and Baudet [1] Univentricular Repair: Is Routine Fenestration Justified?](/thumbs/80/82006124.jpg) Univentricular Repair: Is Routine Fenestration Justified? Balram Airan, MCh, Rajesh Sharma, MCh, Shiv Kumar Choudhary, MCh, Smruti R. Mohanty, MCh, Anil Bhan, MCh, Ujjwal Kumar Chowdhari, MCh, Rajnish
Univentricular Repair: Is Routine Fenestration Justified? Balram Airan, MCh, Rajesh Sharma, MCh, Shiv Kumar Choudhary, MCh, Smruti R. Mohanty, MCh, Anil Bhan, MCh, Ujjwal Kumar Chowdhari, MCh, Rajnish
The Fontan circulation. Folkert Meijboom
 The Fontan circulation Folkert Meijboom What to expect? Why a Fontan-circulation Indications How does it work Types of Fontan circulation Historical overview Role of echocardiography What to expect? Why
The Fontan circulation Folkert Meijboom What to expect? Why a Fontan-circulation Indications How does it work Types of Fontan circulation Historical overview Role of echocardiography What to expect? Why
Glenn Shunts Revisited
 Glenn Shunts Revisited What is a Super Glenn Patricia O Brien, MSN, CPNP-AC Nurse Practitioner, Pediatric Cardiology No Disclosures Single Ventricle Anatomy Glenn Shunt Cavopulmonary Anastomosis Anastomosis
Glenn Shunts Revisited What is a Super Glenn Patricia O Brien, MSN, CPNP-AC Nurse Practitioner, Pediatric Cardiology No Disclosures Single Ventricle Anatomy Glenn Shunt Cavopulmonary Anastomosis Anastomosis
3/14/2011 MANAGEMENT OF NEWBORNS CARDIAC INTENSIVE CARE CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 WITH HEART DEFECTS
 CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
CONFERENCE FOR HEALTH PROFESSIONALS IRVINE, CA. MARCH 7, 2011 MANAGEMENT OF NEWBORNS WITH HEART DEFECTS A NTHONY C. CHANG, MD, MBA, MPH M E D I C AL D I RE C T OR, HEART I N S T I T U T E C H I LDRE N
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
The modified Konno procedure, or subaortic ventriculoplasty,
 Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
Modified Konno Procedure for Left Ventricular Outflow Tract Obstruction David P. Bichell, MD The modified Konno procedure, or subaortic ventriculoplasty, first described by Cooley and Garrett in1986, 1
Chapter 2 Cardiac Interpretation of Pediatric Chest X-Ray
 Chapter 2 Cardiac Interpretation of Pediatric Chest X-Ray Ra-id Abdulla and Douglas M. Luxenberg Key Facts The cardiac silhouette occupies 50 55% of the chest width on an anterior posterior chest X-ray
Chapter 2 Cardiac Interpretation of Pediatric Chest X-Ray Ra-id Abdulla and Douglas M. Luxenberg Key Facts The cardiac silhouette occupies 50 55% of the chest width on an anterior posterior chest X-ray
S. Bruce Greenberg, MD FNASCI and President, NASCI Professor of Radiology and Pediatrics University of Arkansas for Medical Sciences
 S. Bruce Greenberg, MD FNASCI and President, NASCI Professor of Radiology and Pediatrics University of Arkansas for Medical Sciences No financial disclosures Aorta Congenital aortic stenosis/insufficiency
S. Bruce Greenberg, MD FNASCI and President, NASCI Professor of Radiology and Pediatrics University of Arkansas for Medical Sciences No financial disclosures Aorta Congenital aortic stenosis/insufficiency
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum
 Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Mid-term Result of One and One Half Ventricular Repair in a Patient with Pulmonary Atresia and Intact Ventricular Septum Kagami MIYAJI, MD, Akira FURUSE, MD, Toshiya OHTSUKA, MD, and Motoaki KAWAUCHI,
Tricuspid Valve Repair for Ebstein's Anomaly
 Tricuspid Valve Repair for Ebstein's Anomaly Joseph A. Dearani, MD, and Gordon K. Danielson, MD E bstein's anomaly is a malformation of the tricuspid valve and right ventricle that is characterized by
Tricuspid Valve Repair for Ebstein's Anomaly Joseph A. Dearani, MD, and Gordon K. Danielson, MD E bstein's anomaly is a malformation of the tricuspid valve and right ventricle that is characterized by
I worldwide [ 11. The overall number of transplantations
 Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
Expanding Applicability of Transplantation After Multiple Prior Palliative Procedures Alan H. Menkis, MD, F. Neil McKenzie, MD, Richard J. Novick, MD, William J. Kostuk, MD, Peter W. Pflugfelder, MD, Martin
Lateral Tunnel Versus Extracardiac Conduit Fontan Procedure: A Concurrent Comparison
 Lateral Tunnel Versus Extracardiac Conduit Fontan Procedure: A Concurrent Comparison S. Prathap Kumar, FRCS, Catherine S. Rubinstein, FNP, Janet M. Simsic, MD, Ashby B. Taylor, MD, J. Philip Saul, MD,
Lateral Tunnel Versus Extracardiac Conduit Fontan Procedure: A Concurrent Comparison S. Prathap Kumar, FRCS, Catherine S. Rubinstein, FNP, Janet M. Simsic, MD, Ashby B. Taylor, MD, J. Philip Saul, MD,
Surgical Management of TOF in Adults. Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital
 Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Surgical Management of TOF in Adults Dr Flora Tsang Associate Consultant Department of Cardiothoracic Surgery Queen Mary Hospital Tetralogy of Fallot (TOF) in Adults Most common cyanotic congenital heart
Management of complex CHD in adults
 Management of complex CHD in adults Victor Tsang Society of Thoracic Surgeons of Thailand 2016 The impact of infant cardiac surgery Over 90 % of infants born with CHD will reach adulthood By 2010, adults
Management of complex CHD in adults Victor Tsang Society of Thoracic Surgeons of Thailand 2016 The impact of infant cardiac surgery Over 90 % of infants born with CHD will reach adulthood By 2010, adults
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients
 The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
The Turkish Journal of Pediatrics 2008; 50: 549-553 Original The incidence and risk factors of arrhythmias in the early period after cardiac surgery in pediatric patients Selman Vefa Yıldırım 1, Kürşad
Atrial fibrillation (AF) is associated with increased morbidity
 Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
Ablation of Atrial Fibrillation with Concomitant Surgery Edward G. Soltesz, MD, MPH, and A. Marc Gillinov, MD Atrial fibrillation (AF) is associated with increased morbidity and mortality in coronary artery
42yr Old Male with Severe AR Mild LV dysfunction s/p TOF -AV Replacement(tissue valve) or AoV plasty- Kyung-Hwan Kim
 42yr Old Male with Severe AR Mild LV dysfunction s/p TOF -AV Replacement(tissue valve) or AoV plasty- Kyung-Hwan Kim Current Guideline for AR s/p TOF Surgery is reasonable in adults with prior repair of
42yr Old Male with Severe AR Mild LV dysfunction s/p TOF -AV Replacement(tissue valve) or AoV plasty- Kyung-Hwan Kim Current Guideline for AR s/p TOF Surgery is reasonable in adults with prior repair of
What is the Definition of Small Systemic Ventricle. Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University
 What is the Definition of Small Systemic Ventricle Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University Contents Introduction Aortic valve stenosis Aortic coarctation
What is the Definition of Small Systemic Ventricle Hong Ryang Kil, MD Department of Pediatrics, College of Medicine, Chungnam National University Contents Introduction Aortic valve stenosis Aortic coarctation
Specific Issues After Extracardiac Fontan Operation: Ventricular Function, Growth Potential, Arrhythmia, and Thromboembolism
 Specific Issues After Extracardiac Fontan Operation: Ventricular Function, Growth Potential, Arrhythmia, and Thromboembolism Ujjwal K. Chowdhury, MCh, Diplomate NB, Balram Airan, MCh, Shyam Sundar Kothari,
Specific Issues After Extracardiac Fontan Operation: Ventricular Function, Growth Potential, Arrhythmia, and Thromboembolism Ujjwal K. Chowdhury, MCh, Diplomate NB, Balram Airan, MCh, Shyam Sundar Kothari,
Tetralogy of Fallot (TOF) with absent pulmonary valve
 Repair of Tetralogy of Fallot with Absent Pulmonary Valve Syndrome Karl F. Welke, MD, and Ross M. Ungerleider, MD, MBA Tetralogy of Fallot (TOF) with absent pulmonary valve syndrome (APVS) occurs in 5%
Repair of Tetralogy of Fallot with Absent Pulmonary Valve Syndrome Karl F. Welke, MD, and Ross M. Ungerleider, MD, MBA Tetralogy of Fallot (TOF) with absent pulmonary valve syndrome (APVS) occurs in 5%
Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy
 Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy Tom R. Karl, MS, MD he most commonly reported coronary artery malformation leading to sudden death in children and young
Coronary Artery from the Wrong Sinus of Valsalva: A Physiologic Repair Strategy Tom R. Karl, MS, MD he most commonly reported coronary artery malformation leading to sudden death in children and young
Ebstein s anomaly is characterized by malformation of
 Fenestrated Right Ventricular Exclusion (Starnes Procedure) for Severe Neonatal Ebstein s Anomaly Brian L. Reemtsen, MD,* and Vaughn A. Starnes, MD*, Ebstein s anomaly is characterized by malformation
Fenestrated Right Ventricular Exclusion (Starnes Procedure) for Severe Neonatal Ebstein s Anomaly Brian L. Reemtsen, MD,* and Vaughn A. Starnes, MD*, Ebstein s anomaly is characterized by malformation
Segmental Analysis. Gautam K. Singh, M.D. Washington University School of Medicine St. Louis
 Segmental Analysis Gautam K. Singh, M.D. Washington University School of Medicine St. Louis Segmental Analysis Segmental Analysis: From Veins to Ventricles Segmental Approach to Evaluation of Congenital
Segmental Analysis Gautam K. Singh, M.D. Washington University School of Medicine St. Louis Segmental Analysis Segmental Analysis: From Veins to Ventricles Segmental Approach to Evaluation of Congenital
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease
 Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Outcomes of Mitral Valve Repair for Mitral Regurgitation Due to Degenerative Disease TIRONE E. DAVID, MD ; SEMIN THORAC CARDIOVASC SURG 19:116-120c 2007 ELSEVIER INC. PRESENTED BY INTERN 許士盟 Mitral valve
Assessing Cardiac Anatomy With Digital Subtraction Angiography
 485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
485 JACC Vol. 5, No. I Assessing Cardiac Anatomy With Digital Subtraction Angiography DOUGLAS S., MD, FACC Cleveland, Ohio The use of intravenous digital subtraction angiography in the assessment of patients
Corrective Repair of Complete Atrioventricular
 Corrective Repair of Complete Atrioventricular Canal Defects and Major Associated Cardiac Anomalies A. D. Pacifico, M.D., A. Ricchi, M.D., L. M. Bargeron, Jr., M.D., E. C. Colvin, M.D., J. W. Kirklin,
Corrective Repair of Complete Atrioventricular Canal Defects and Major Associated Cardiac Anomalies A. D. Pacifico, M.D., A. Ricchi, M.D., L. M. Bargeron, Jr., M.D., E. C. Colvin, M.D., J. W. Kirklin,
All You Need to Know About Situs and Looping Disorders: Embryology, Anatomy, and Echocardiography
 All You Need to Know About Situs and Looping Disorders: Embryology, Anatomy, and Echocardiography Helena Gardiner Co-Director of Fetal Cardiology, The Fetal Center, University of Texas at Houston Situs
All You Need to Know About Situs and Looping Disorders: Embryology, Anatomy, and Echocardiography Helena Gardiner Co-Director of Fetal Cardiology, The Fetal Center, University of Texas at Houston Situs
Data Collected: June 17, Reported: June 30, Survey Dates 05/24/ /07/2010
 Job Task Analysis for ARDMS Pediatric Echocardiography Data Collected: June 17, 2010 Reported: Analysis Summary For: Pediatric Echocardiography Exam Survey Dates 05/24/2010-06/07/2010 Invited Respondents
Job Task Analysis for ARDMS Pediatric Echocardiography Data Collected: June 17, 2010 Reported: Analysis Summary For: Pediatric Echocardiography Exam Survey Dates 05/24/2010-06/07/2010 Invited Respondents
Repair of Complete Atrioventricular Septal Defects Single Patch Technique
 Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
Repair of Complete Atrioventricular Septal Defects Single Patch Technique Fred A. Crawford, Jr., MD The first repair of a complete atrioventricular septal defect was performed in 1954 by Lillehei using
The radial procedure was developed as an outgrowth
 The Radial Procedure for Atrial Fibrillation Takashi Nitta, MD The radial procedure was developed as an outgrowth of an alternative to the maze procedure. The atrial incisions are designed to radiate from
The Radial Procedure for Atrial Fibrillation Takashi Nitta, MD The radial procedure was developed as an outgrowth of an alternative to the maze procedure. The atrial incisions are designed to radiate from
The goal of the hybrid approach for hypoplastic left heart
 The Hybrid Approach to Hypoplastic Left Heart Syndrome Mark Galantowicz, MD The goal of the hybrid approach for hypoplastic left heart syndrome (HLHS) is to lessen the cumulative impact of staged interventions,
The Hybrid Approach to Hypoplastic Left Heart Syndrome Mark Galantowicz, MD The goal of the hybrid approach for hypoplastic left heart syndrome (HLHS) is to lessen the cumulative impact of staged interventions,
"Giancarlo Rastelli Lecture"
 "Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
"Giancarlo Rastelli Lecture" Surgical treatment of Malpositions of the Great Arteries Pascal Vouhé Giancarlo Rastelli (1933 1970) Cliquez pour modifier les styles du texte du masque Deuxième niveau Troisième
T who has survived first-stage palliative surgical management
 Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
Intermediate Procedures After First-Stage Norwood Operation Facilitate Subsequent Repair Richard A. Jonas, MD Department of Cardiac Surgery, Children s Hospital, Boston, Massachusetts Actuarial analysis
Congenital Heart Disease in the Adult Presenting for Non-Cardiac Surgery
 Page 1 Congenital Heart Disease in the Adult Presenting for Non-Cardiac Surgery Susan S. Eagle, M.D. Nashville, Tennessee Introduction: Advancement of surgical techniques and medical management patients
Page 1 Congenital Heart Disease in the Adult Presenting for Non-Cardiac Surgery Susan S. Eagle, M.D. Nashville, Tennessee Introduction: Advancement of surgical techniques and medical management patients
Hybrid Stage I Palliation / Bilateral PAB
 Hybrid Stage I Palliation / Bilateral PAB Jeong-Jun Park Dept. of Thoracic & Cardiovascular Surgery Asan Medical Center, University of Ulsan CASE 1 week old neonate with HLHS GA 38 weeks Birth weight 3.0Kg
Hybrid Stage I Palliation / Bilateral PAB Jeong-Jun Park Dept. of Thoracic & Cardiovascular Surgery Asan Medical Center, University of Ulsan CASE 1 week old neonate with HLHS GA 38 weeks Birth weight 3.0Kg
The Clinical Outcomes of Damus-Kaye-Stansel Procedure According to Surgical Technique
 Korean J Thorac Cardiovasc Surg 24;4:344-349 ISSN: 2233-6X (Print) ISSN: 293-656 (Online) Clinical Research http://dx.doi.org/.59/kjtcs.24.4.4.344 The Clinical Outcomes of Damus-Kaye-Stansel Procedure
Korean J Thorac Cardiovasc Surg 24;4:344-349 ISSN: 2233-6X (Print) ISSN: 293-656 (Online) Clinical Research http://dx.doi.org/.59/kjtcs.24.4.4.344 The Clinical Outcomes of Damus-Kaye-Stansel Procedure
Outline. Congenital Heart Disease. Special Considerations for Special Populations: Congenital Heart Disease
 Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
Special Considerations for Special Populations: Congenital Heart Disease Valerie Bosco, FNP, EdD Alison Knauth Meadows, MD, PhD University of California San Francisco Adult Congenital Heart Program Outline
M/3, cc-tga, PS, BCPC(+) Double Switch Operation
 2005 < Pros & Cons > M/3, cc-tga, PS, BCPC(+) Double Switch Operation Congenitally corrected TGA Atrio-Ventricular & Ventriculo-Arterial discordance Physiologically corrected circulation with the morphologic
2005 < Pros & Cons > M/3, cc-tga, PS, BCPC(+) Double Switch Operation Congenitally corrected TGA Atrio-Ventricular & Ventriculo-Arterial discordance Physiologically corrected circulation with the morphologic
Ebstein s anomaly is a congenital malformation of the right
 Cone Reconstruction of the Tricuspid Valve for Ebstein s Anomaly: Anatomic Repair Joseph A. Dearani, MD, Emile Bacha, MD, and José Pedro da Silva, MD Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Cone Reconstruction of the Tricuspid Valve for Ebstein s Anomaly: Anatomic Repair Joseph A. Dearani, MD, Emile Bacha, MD, and José Pedro da Silva, MD Division of Cardiovascular Surgery, Mayo Clinic, Rochester,
Congenital Heart Defects
 Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Normal Heart Congenital Heart Defects 1. Patent Ductus Arteriosus The ductus arteriosus connects the main pulmonary artery to the aorta. In utero, it allows the blood leaving the right ventricle to bypass
Total Cavopulmonary Connections in Children With a Previous Norwood Procedure
 Total Cavopulmonary Connections in Children With a Previous Norwood Procedure Anthony Azakie, MD, Brian W. McCrindle, MD, FRCP(C), Lee N. Benson, MD, FRCP(C), Glen S. Van Arsdell, MD, Jennifer L. Russell,
Total Cavopulmonary Connections in Children With a Previous Norwood Procedure Anthony Azakie, MD, Brian W. McCrindle, MD, FRCP(C), Lee N. Benson, MD, FRCP(C), Glen S. Van Arsdell, MD, Jennifer L. Russell,
Surgical Management Of TAPVR. Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital
 Surgical Management Of TAPVR Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital No Disclosures Goals Review the embryology and anatomy Review Surgical Strategies for repair Discuss
Surgical Management Of TAPVR Daniel A. Velez, M.D. Congenital Cardiac Surgeon Phoenix Children s Hospital No Disclosures Goals Review the embryology and anatomy Review Surgical Strategies for repair Discuss
LONG TERM OUTCOMES OF PALLIATIVE CONGENITAL HEART DISEASE
 LONG TERM OUTCOMES OF PALLIATIVE CONGENITAL HEART DISEASE S Bruce Greenberg, MD, FACR, FNASCI Professor of Radiology and Pediatrics Arkansas Children's Hospital University of Arkansas for Medical Sciences
LONG TERM OUTCOMES OF PALLIATIVE CONGENITAL HEART DISEASE S Bruce Greenberg, MD, FACR, FNASCI Professor of Radiology and Pediatrics Arkansas Children's Hospital University of Arkansas for Medical Sciences
Absent Pulmonary Valve Syndrome
 Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Absent Pulmonary Valve Syndrome Fact sheet on Absent Pulmonary Valve Syndrome In this condition, which has some similarities to Fallot's Tetralogy, there is a VSD with narrowing at the pulmonary valve.
Surgical options for tetralogy of Fallot
 Surgical options for tetralogy of Fallot Serban Stoica FRCS(CTh) MD ACHD study day, 19 September 2017 Anatomy Physiology Children Adults Complications Follow up Anatomy Etienne Fallot (1850-1911) VSD Overriding
Surgical options for tetralogy of Fallot Serban Stoica FRCS(CTh) MD ACHD study day, 19 September 2017 Anatomy Physiology Children Adults Complications Follow up Anatomy Etienne Fallot (1850-1911) VSD Overriding
What Can the Database Tell Us About Reoperation?
 AATS/STS Congenital Heart Disease Postgraduate Symposium May 5, 2013 What Can the Database Tell Us About Reoperation? Jeffrey P. Jacobs, M.D. All Children s Hospital Johns Hopkins Medicine The Congenital
AATS/STS Congenital Heart Disease Postgraduate Symposium May 5, 2013 What Can the Database Tell Us About Reoperation? Jeffrey P. Jacobs, M.D. All Children s Hospital Johns Hopkins Medicine The Congenital
Unifocalization of Major Aortopulmonary Collaterals in Single-Ventricle Patients
 CARDIOVASCULAR Unifocalization of Major Aortopulmonary Collaterals in Single-Ventricle Patients Olaf Reinhartz, MD, V. Mohan Reddy, MD, Edwin Petrossian, MD, Sam Suleman, BS, Richard D. Mainwaring, MD,
CARDIOVASCULAR Unifocalization of Major Aortopulmonary Collaterals in Single-Ventricle Patients Olaf Reinhartz, MD, V. Mohan Reddy, MD, Edwin Petrossian, MD, Sam Suleman, BS, Richard D. Mainwaring, MD,
Surgical Experience with Unroofed Coronary Sinus
 Surgical Experience with Unroofed Coronary Sinus Jan Quaegebeur, M.D., John W. Kirklin, M.D., Albert D. Pacifico, M.D., and Lionel M. Bargeron, Jr., M.D. ABSTRACT Between January, 1967, and October, 1977,
Surgical Experience with Unroofed Coronary Sinus Jan Quaegebeur, M.D., John W. Kirklin, M.D., Albert D. Pacifico, M.D., and Lionel M. Bargeron, Jr., M.D. ABSTRACT Between January, 1967, and October, 1977,
FUNCTIONALLY SINGLE VENTRICLE
 MORPHOLOGICAL DETERMINANTS VI TRAN EuroEcho, Budapest, 7 th December 2011 DECLARATION OF CONFLICT OF INTEREST: I have nothing to declare What is the functionally single ventricle? The heart that is incapable
MORPHOLOGICAL DETERMINANTS VI TRAN EuroEcho, Budapest, 7 th December 2011 DECLARATION OF CONFLICT OF INTEREST: I have nothing to declare What is the functionally single ventricle? The heart that is incapable
Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016
 1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
1 Adult Congenital Heart Disease: What All Echocardiographers Should Know Sharon L. Roble, MD, FACC Echo Hawaii 2016 DISCLOSURES I have no disclosures relevant to today s talk 2 Why should all echocardiographers
Syed Aqeel Hussain, Iftikhar Ahmed, Rana Intesar Ul Haq, Kamal Saleem
 Original Article Pak Armed Forces Med J 2015; 65(Suppl): S43-47 A COMPARISON OF THREE DIFFERENT TECHNIQUES TO PERFORM BI-DIRECTIONAL GLENN SHUNT Syed Aqeel Hussain, Iftikhar Ahmed, Rana Intesar Ul Haq,
Original Article Pak Armed Forces Med J 2015; 65(Suppl): S43-47 A COMPARISON OF THREE DIFFERENT TECHNIQUES TO PERFORM BI-DIRECTIONAL GLENN SHUNT Syed Aqeel Hussain, Iftikhar Ahmed, Rana Intesar Ul Haq,
Preoperative Echocardiographic Assessment of Uni-ventricular Repair
 Preoperative Echocardiographic Assessment of Uni-ventricular Repair Salem Deraz, MD Pediatric Cardiologist, Aswan Heart Centre Magdi Yacoub Heart Foundation Uni-ventricular repair A single or series of
Preoperative Echocardiographic Assessment of Uni-ventricular Repair Salem Deraz, MD Pediatric Cardiologist, Aswan Heart Centre Magdi Yacoub Heart Foundation Uni-ventricular repair A single or series of
Ebstein s anomaly is defined by a downward displacement
 Repair of Ebstein s Anomaly Sylvain Chauvaud, MD Ebstein s anomaly is a tricuspid valve anomaly associated with poor right ventricular contractility in severe cases. Surgery is indicated in all symptomatic
Repair of Ebstein s Anomaly Sylvain Chauvaud, MD Ebstein s anomaly is a tricuspid valve anomaly associated with poor right ventricular contractility in severe cases. Surgery is indicated in all symptomatic
The Chest X-ray for Cardiologists
 Mayo Clinic & British Cardiovascular Society at the Royal College of Physicians, London : 21-23-October 2013 Cases-Controversies-Updates 2013 The Chest X-ray for Cardiologists Michael Rubens Royal Brompton
Mayo Clinic & British Cardiovascular Society at the Royal College of Physicians, London : 21-23-October 2013 Cases-Controversies-Updates 2013 The Chest X-ray for Cardiologists Michael Rubens Royal Brompton
Extracardiac vs Intra-atrial Lateral Tunnel Fontan: Extracardiac is Better. No it s not: (They both have problems)
 Extracardiac vs Intra-atrial Lateral Tunnel Fontan: Extracardiac is Better No it s not: (They both have problems) Why is it difficult to analyze outcomes after the Fontan procedure? Wide range of patient
Extracardiac vs Intra-atrial Lateral Tunnel Fontan: Extracardiac is Better No it s not: (They both have problems) Why is it difficult to analyze outcomes after the Fontan procedure? Wide range of patient
Anatomy of Atrioventricular Septal Defect (AVSD)
 Surgical challenges in atrio-ventricular septal defect in grown-up congenital heart disease Anatomy of Atrioventricular Septal Defect (AVSD) S. Yen Ho Professor of Cardiac Morphology Royal Brompton and
Surgical challenges in atrio-ventricular septal defect in grown-up congenital heart disease Anatomy of Atrioventricular Septal Defect (AVSD) S. Yen Ho Professor of Cardiac Morphology Royal Brompton and
Anomalous Systemic Venous Connection Systemic venous anomaly
 World Database for Pediatric and Congenital Heart Surgery Appendix B: Diagnosis (International Paediatric and Congenital Cardiac Codes (IPCCC) and definitions) Anomalous Systemic Venous Connection Systemic
World Database for Pediatric and Congenital Heart Surgery Appendix B: Diagnosis (International Paediatric and Congenital Cardiac Codes (IPCCC) and definitions) Anomalous Systemic Venous Connection Systemic
Intracardiac Lateral Tunnel Fontan by using Right Atrial Wall
 Intracardiac Lateral Tunnel Fontan by using Right Atrial Wall Md Zahidul Islam¹, AM Asif Rahim², Kazi Abul Hasan¹, Syed Imtiaz Ahsan¹ 1 Department of Paediatric Cardiac Surgery, National Institute of Cardiovascular
Intracardiac Lateral Tunnel Fontan by using Right Atrial Wall Md Zahidul Islam¹, AM Asif Rahim², Kazi Abul Hasan¹, Syed Imtiaz Ahsan¹ 1 Department of Paediatric Cardiac Surgery, National Institute of Cardiovascular
The need for right ventricular outflow tract reconstruction
 Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Polytetrafluoroethylene Bicuspid Pulmonary Valve Implantation James A. Quintessenza, MD The need for right ventricular outflow tract reconstruction and pulmonary valve replacement is increasing for many
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
REVISION OF PREVIOUS FONTAN CONNECTIONS TO TOTAL EXTRACARDIAC CAVOPULMONARY ANASTOMOSIS: A MULTICENTER EXPERIENCE
 REVISION OF PREVIOUS FONTAN CONNECTIONS TO TOTAL EXTRACARDIAC CAVOPULMONARY ANASTOMOSIS: A MULTICENTER EXPERIENCE Carlo F. Marcelletti, MD a Frank L. Hanley, MD b Constantine Mavroudis, MD c Doff B. McElhinney,
REVISION OF PREVIOUS FONTAN CONNECTIONS TO TOTAL EXTRACARDIAC CAVOPULMONARY ANASTOMOSIS: A MULTICENTER EXPERIENCE Carlo F. Marcelletti, MD a Frank L. Hanley, MD b Constantine Mavroudis, MD c Doff B. McElhinney,
The application of autologous pulmonary artery in surgical correction of complicated aortic arch anomaly
 Original Article The application of autologous pulmonary artery in surgical correction of complicated aortic arch anomaly Shusheng Wen, Jianzheng Cen, Jimei Chen, Gang Xu, Biaochuan He, Yun Teng, Jian
Original Article The application of autologous pulmonary artery in surgical correction of complicated aortic arch anomaly Shusheng Wen, Jianzheng Cen, Jimei Chen, Gang Xu, Biaochuan He, Yun Teng, Jian
Pulmonary Valve Replacement
 Pulmonary Valve Replacement Christian Kreutzer MD Hospital Nacional Alejandro Posadas Hospital Universitario Austral (No disclosures) Scope of the problem. CHD with PS or PA require a RVOT procedure. Tetralogy
Pulmonary Valve Replacement Christian Kreutzer MD Hospital Nacional Alejandro Posadas Hospital Universitario Austral (No disclosures) Scope of the problem. CHD with PS or PA require a RVOT procedure. Tetralogy
Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents
 Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents March, 2013 Sponsored by: Commission on Education Committee on Residency Training in Diagnostic Radiology 2013 by American
Cardiac Radiology In-Training Test Questions for Diagnostic Radiology Residents March, 2013 Sponsored by: Commission on Education Committee on Residency Training in Diagnostic Radiology 2013 by American
doi: /j.athoracsur
 doi: 0.0/j.athoracsur.0.0.0 Effects of Landiolol Hydrochloride on Intractable Tachyarrhythmia After Pediatric Cardiac Surgery Chiho Tokunaga, MD, PhD, Yuji Hiramatsu, MD, PhD, Shinya Kanemoto, MD, PhD,
doi: 0.0/j.athoracsur.0.0.0 Effects of Landiolol Hydrochloride on Intractable Tachyarrhythmia After Pediatric Cardiac Surgery Chiho Tokunaga, MD, PhD, Yuji Hiramatsu, MD, PhD, Shinya Kanemoto, MD, PhD,
A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution
 Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Original Article A Unique Milieu for Perioperative Care of Adult Congenital Heart Disease Patients at a Single Institution Ghassan Baslaim, MD, and Jill Bashore, RN Purpose: Adult patients with congenital
Mid-term result of atrioventricular valve replacement in patients with a single ventricle
 Interactive CardioVascular and Thoracic Surgery (2018) 1 6 doi:10.1093/icvts/ivy155 ORIGINAL ARTICLE Cite this article as: Sughimoto K, Hirata Y, Hirahara N, Miyata H, Suzuki T, Murakami A et al. Mid-term
Interactive CardioVascular and Thoracic Surgery (2018) 1 6 doi:10.1093/icvts/ivy155 ORIGINAL ARTICLE Cite this article as: Sughimoto K, Hirata Y, Hirahara N, Miyata H, Suzuki T, Murakami A et al. Mid-term
Although most patients with Ebstein s anomaly live
 Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
Management of Neonatal Ebstein s Anomaly Christopher J. Knott-Craig, MD, FACS Although most patients with Ebstein s anomaly live through infancy, those who present clinically as neonates are a distinct
DGPK guideline: PAPVC
 DGPK guideline: PAPVC Partial anomalous pulmonary venous connection (PAPVC) Harald Bertram, Hannover Oliver Dewald, Bonn Angelika Lindinger, Kaiserslautern & Trier DGPK guideline committee No disclosures
DGPK guideline: PAPVC Partial anomalous pulmonary venous connection (PAPVC) Harald Bertram, Hannover Oliver Dewald, Bonn Angelika Lindinger, Kaiserslautern & Trier DGPK guideline committee No disclosures
