Influence of Radiologically Evident Residual Intimal Tear on Expansion of Descending Aorta Following Surgery for Acute Type I Aortic Dissection
|
|
|
- Joy Irene Barrett
- 5 years ago
- Views:
Transcription
1 Korean J Thorac Cardiovasc Surg 2014;47:6-12 ISSN: X (Print) ISSN: (Online) Clinical Research Influence of Radiologically Evident Residual Intimal Tear on Expansion of Descending Aorta Following Surgery for Acute Type I Aortic Dissection Yun Seok Kim, M.D. 1, Jeong Heon Kim 2, Joon Bum Kim, M.D. 1, Dong Hyun Yang, M.D. 3, Joon-Won Kang, M.D. 3, Su Kyung Hwang, M.D. 1, Suk Jung Choo, M.D. 1, Cheol Hyun Chung, M.D. 1 Background: Although a residual intimal tear may contribute to the dilatation of the descending aorta following surgical repair of acute type I aortic dissection (AD), its causal relationship has not been elucidated by clinical data due to the limited resolution of imaging modalities. Methods: This study enrolled 41 patients (age, 55.2±11.9 years) who were evaluated with dual-source computed tomography (CT) imaging of the whole aorta in the setting of the surgical repair of acute type I AD. Logistic regression models were used to determine the predictors of a composite of the aortic aneurysm formation (diameter >55 mm) and rapid aortic expansion (>5 mm/yr). Results: On initial CT, a distal re-entry tear was identified in 9 patients. Two patients failed to achieve proximal tear exclusion by the surgery. Serial follow-up CT evaluations (median, 24.6 months; range, 6.0 to 67.2 months) revealed that 14 patients showed rapid expansion of the descending aorta or aortic aneurysm formation. A multivariate analysis revealed that the residual intimal tear (odds ratio [OR], 4.31; 95% confidence interval [CI], 1.02 to 19.31) and the patent false lumen in the early postoperative setting (OR, 4.64; 95% CI, 0.99 to 43.61) were predictive of the composite endpoint. Conclusion: The presence of a residual intimal tear following surgery for acute type I AD adversely influenced the expansion of the descending aorta. Key words: 1. Aortic dissection 2. Aneurysm 3. Surgery 4. Risk analysis INTRODUCTION Acute DeBakey type I aortic dissection is a life threatening medical emergency having a very high mortality rate if not treated surgically [1]. The surgical principles for the management of acute type I aortic dissection include the replacement of the affected proximal aorta and the exclusion of the primary intimal tear, consequently leaving the descending aorta untreated surgically [2]. Therefore, residual chronic dissection in the downstream aorta is a frequent condition following the urgent surgery for acute type I aortic dissection, and it is well known that this lesion predisposes the aorta to aneurysmal formation [3,4]. Several studies have been conducted to identify the risk factors of aneurysmal changes in the de- 1 Department of Thoracic and Cardiovascular Surgery, Asan Medical Center, University of Ulsan College of Medicine, 2 Department of Thoracic and Cardiovascular Surgery, University of Ulsan College of Medicine, 3 Department of Radiology, Asan Medical Center, University of Ulsan College of Medicine Received: September 2, 2013, Revised: October 8, 2013, Accepted: October 10, 2013 Corresponding author: Joon Bum Kim, Department of Thoracic and Cardiovascular Surgery, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul , Korea (Tel) (Fax) ( ) jbkim1975@amc.seoul.kr C The Korean Society for Thoracic and Cardiovascular Surgery All right reserved. CC This is an open access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 6
2 Residual Intimal Tear in Acute Type I Dissection scending aorta and have shown that the presence of connective tissue disorders, the size and the false lumen status of the descending aorta, and a failure to exclude the primary intimal tear were correlated with aneurysm formation [2-6]. Further, the potential risk factors of the aneurysmal changes in the descending aorta may include the presence of a distal reentry tear that cannot be excluded during the urgent proximal operation. As with the failure to exclude the primary intimal tear, the distal reentry tears may be predisposed to the persistent patency of the false lumen in the descending aorta, which is also a well-known risk factor of aneurysm formation [7-10]. Nevertheless, this hypothesis has not been tested in real clinical settings because of the limited resolution of imaging modalities to identify such distal reentrant tears, which are typically small (<1 cm), through comprehensive evaluations on the whole aorta. Now, in the era of evolving imaging modalities in clinical medicine, we have many modern tools that may allow us to identify such reentry tears with excellent resolution [11,12]. When gated by electrocardiography (ECG), current multi-detector computed tomography (CT) can obtain images of the cardiovascular system with a resolution of <1 mm and minimum motion artifact. In this study, we hypothesized that a distal reentry tear identified by the current multi-detector CT in the setting of acute type I aortic dissection may correlate with aneurysm formation of the descending aorta following proximal aorta replacement. Therefore, we performed risk factor analyses to determine the independent predictors of the descending aorta aneurysmal changes following surgery for acute DeBakey type I aortic dissection, considering the distal reentry tear identifiable by the current multi-detector CT to be one of the important covariates in the multivariable model. METHODS 1) Patients Between November 2006 and December 2011, 71 patients underwent an emergency operation for acute type I aortic dissection at Asan Medical Center. In these 71 patients, 23 patients were excluded because of poor quality CT images that were obtained from the referring hospitals. Of the remaining 48 patients, 7 patients who were not followed up with a CT evaluation beyond 6 months (including 2 patients who died within 6 months of surgery) were further excluded, resulting in the consideration of a total of 41 subjects in this study. Asan Medical Center ethics committee/review board waived the requirement for informed patient consent because this is a retrospective study. 2) Computed tomography techniques and follow-up All CT scans were obtained in less than 48 hours after the symptom onset. Aortic CT angiography was conducted using either a first-generation dual-source CT (Somatom Definition; Siemens, Erlangen, Germany) or a second-generation dual-source CT (Somatom Definition Flash; Siemens). A contrast agent was administered using a power injector (Stellant D; Medrad, Indianola, PA, USA) at the rate of 3.5 to 4.0 ml/sec, with a total volume of 100 ml of iomeprol (Iomeron 370, Bracco Imaging, Italy), followed by 40 ml of a saline chaser. A region of interest was placed in the descending thoracic aorta, and image acquisition was automatically initiated once a selected threshold (100 HU) was reached using bolus tracking. An ECG-gated scan was conducted for the thoracic aorta followed by a non-ecg-gated scan for the abdominal aorta. To reduce the radiation dose, tube current modulation was implemented with a body-size adaptive tube voltage (range, 100 to 120 kvp) and a tube-current-time product (range, 270 to 440 mas for the thoracic aorta; 200 mas for the abdominal aorta). In addition, the ECG-based tube current modulation was implemented (relative risk interval, 65% to 85%). Image parameters were as follows: beam collimation: mm (first generation) and mm (second generation); gantry rotation time: 330 ms (first generation) and 280 ms (second generation); and pitch: (for the thoracic aorta; adapted to the heart rate) and 1 (for the abdominal aorta). Axial images were obtained in contiguous 1.0- to 2.5-mm-thick sections from the aortic arch branching vessels to below the iliac bifurcation. The true and false lumen diameters were measured at the proximal descending (just distal to the aortic arch), mid descending (at the level of the pulmonary artery bifurcation), and lower descending (at the center of the left atrium) thoracic aorta and at the abdominal aorta (the level of origin of the renal ar- 7
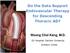
3 Yun Seok Kim, et al tery). The endpoint of this study was the development of aortic aneurysm in any segment, defined as a maximal aortic luminal diameter >55 mm, or aortic expansion rate >5 mm/yr on follow-up CT [13]. 3) Surgical technique During median sternotomy, the right axillary or the right femoral arteries were cannulated. Venous cannulation was established by the single right atrial or bicaval method. Distal anastomosis was accomplished during moderate or deep hypothermic circulatory arrest. In general, antegrade selective cerebral perfusion was used in moderate hypothermia and retrograde cerebral perfusion was used in deep hypothermia. Based on the site of the proximal intimal tear and the presence of connective tissue disorders, we determined the extent of replacement: ascending aorta, hemiarch, or total arch replacement. If there is no proximal intimal tear in the ascending aorta or the aortic arch, the extent of replacement is limited in the hemiarch in non-marfan patients. Resuspension of the aortic valve, replacement of the aortic valve, or modified Bentall s procedure was performed as required. 4) Statistics Categorical variables are presented as numbers and percentages and were compared with the chi-square test and Fisher s exact test. Continuous variables are expressed as mean±standard deviation or median with range, and were compared with Student unpaired t-test or the Mann-Whitney U-test. For the multivariate analyses, the logistic regression models were used to determine the risk factors of the composite of the development of aortic aneurysm or rapid aortic expansion. Preoperative and operative variables were evaluated in the models, and those with a p-value of 0.20 or less in the univariate analyses were candidates for the multivariate logistic regression models. Multivariate analyses involved a backward elimination technique, and only variables with a p-value of less than 0.10 were used in the final model. The final models were validated using 1,000 bootstrap samples. All reported p-values were two-sided, and the p-values of less than 0.05 were considered statistically significant. SPSS ver (SPSS Inc., Chicago, IL, USA) was used for the statistical analyses. Table 1. Baseline patient profiles and CT findings Variable Value Demographic & baseline risks Age (yr) 55.2±11.9 Female gender 20 (48.8) Diabetes mellitus 0 Hypertension 17 (41.4) Marfan syndrome 4 (9.8) Preoperative condition Shock 4 (9.8) Malperfusion Cerebrovascular attack 4 (9.8) Visceral malperfusion 0 Peripheral malperfusion 4 (9.8) Intramural hematoma 6 (14.6) Retro-A dissection 6 (14.6) CT findings Distal extent Descending thoracic 2 (4.9) Abdominal, suprarenal 3 (7.3) Abdominal, infrarenal 7 (17.0) Iliac or beyond iliac 28 (68.3) Proximal intimal tear 34 (82.9) Ascending aorta 17 (41.5) Aortic arch 15 (36.6) Beyond aortic arch 2 (4.9) Distal reentry intimal tear 9 (22.0) Abdominal, suprarenal 4 (9.8) Abdominal, infrarenal 2 (4.9) Iliac or beyond iliac 3 (7.3) No intimal tear 6 (14.6) Values are presented as mean±standard deviation or number (%). CT, computed tomography. RESULTS 1) Baseline patient characteristics The baseline patients demographics and clinical profiles, and the details of initial CT findings are presented in Table 1. Proximal intimal tears were identified in 34 patients (82.9%). Among them, 32 patients (78.0%) had the proximal intimal tears in the ascending aorta or the aortic arch, whereas 2 patients (4.9%) had the proximal tears beyond the aortic arch. Distal intimal tears were identified in 9 patients (22.0%) (Fig. 1). Multiple intimal tears were identified in 2 patients (4.9%): one had a proximal intimal tear at the proximal aortic 8
4 Residual Intimal Tear in Acute Type I Dissection Fig. 1. (A, B) The intimal tear (arrow) connecting the true and the false lumen in the dissected descending aorta. arch and three distal intimal tears at the suprarenal and infra-renal abdominal aorta and the left common iliac artery, and the other had a proximal intimal tear at the ascending aorta and two distal intimal tears at the suprarenal and infra-renal abdominal aorta. Six patients (14.6%) were diagnosed with type I intramural hematoma without a definite intimal tear through the whole aorta. There was one patient who had a distal intimal tear without a proximal intimal tear. 2) Operative procedures Ascending aorta replacement was performed in 3 patients (7.3%). Among them, 1 patient underwent concomitant resuspension of the aortic valve, and another underwent concomitant replacement of the aortic valve. Hemiarch replacement with or without ascending aorta replacement was performed in 27 patients (65.9%). Among them, 19 patients underwent concomitant resuspension of the aortic valve, 3 patients underwent concomitant coronary artery bypass surgery, and 2 patients underwent concomitant modified Bentall s procedure. Total arch replacement with or without ascending aorta replacement was performed in 11 patients (26.8%). Among them, 8 patients underwent concomitant resuspension of the aortic valve and 1 patient underwent concomitant modified Bentall s procedure. Among 34 patients (82.9%) who had an identified proximal intimal tear, complete exclusion of the proximal intimal tear was achieved in 32 patients (78.0%). The remaining 2 patients (4.9%) failed to achieve proximal tear exclusion; hemiarch replacement and total arch replacement were each performed in one of the 2. Of the 2 patients, one patient was one of the 9 patients who were identified as having a distal reentry tear on the initial CT evaluation. Consequently, 10 patients (24.4%) were revealed to have a residual intimal tear postoperatively. 3) Effects of residual intimal tear on the fate of the descending aorta The median CT follow-up duration was 24.6 months (range, 6.0 to 67.2 months). There were no significant differences in the baseline diameters of the descending aorta according to the presence of the postoperative residual intimal tears (Table 2). However, in the early postoperative period, complete thrombosis of the false lumen was more frequently found in patients without the residual intimal tears compared with those without tears. The follow-up revealed that the diameters and growth rates of the whole descending aorta were larger and faster, respectively, in the patients with the residual tears, with statistical significance in most aortic segments (Table 2). According to the patency of the false lumens, diameters of the descending thoracic aorta, particularly in the mid and distal segments, showed a decreasing tendency in patients with complete thrombosis of the false lumen. The last follow-up revealed that the diameters of the whole segments of the de- 9
5 Yun Seok Kim, et al Table 2. False lumen status, diameter and expansion rate of the descending aorta Variable Residual tear (+) Residual tear (-) p-value Baseline aorta diameter (mm) Early postoperative false lumen status Complete obliteration Partial thrombosis Patent Last follow-up aorta diameter (mm) Aortic expansion rate (mm/yr) 37.6± ± ± ±3.1 1 (10.0) 3 (30.0) 6 (60.0) 43.1± ± ± ± ± ± ± ±4.7 Values are presented as mean±standard deviation or number (%). 37.1± ± ± ± (45.2) 11 (35.5) 6 (19.4) 36.4± ± ± ± ± ± ± ± Table 3. Aortic expansion rate according to false lumen status in early postoperative period Variable Complete thrombosis Patent false lumen p-value Baseline aorta diameter (mm) Aortic expansion rate (mm/yr) Last follow-up aorta diameter (mm) 35.4± ± ± ± (-4.9 to 2.2) (-5.5 to 1.4) (-7.0 to 2.1) 1.83 (-0.4 to 9.4) 32.9± ± ± ± ± ± ± ± (-9.4 to 16.7) 2.82 (-5.7 to 15.7) 2.14 (-7.6 to 15.4) 2.24 (-0.3 to 13.5) 39.5± ± ± ± < scending thoracic aorta were significantly smaller in patients with complete false lumen thrombosis than in those with patent false lumen (Table 3). During follow-up, 14 patients (34.1%) eventually showed rapid expansion of the descending aorta, and of them, two patients developed aortic aneurysm. The multivariate analysis revealed that the postoperative residual intimal tear was the only risk factor for the composite outcome of aortic enlargement or rapid expansion while the postoperative patency of false lumen showed borderline statistical significance (p=0.054) (Table 4). 10
6 Residual Intimal Tear in Acute Type I Dissection Table 4. Risk factors for enlargement or rapid expansion of the descending aorta Variable Age Gender Hypertension Marfan syndrome Distal extent of aortic dissection Initial diameter of aortic segments Total arch versus hemiarch repair Presence of distal reentry intimal tear Exclusion of proximal intimal tear Postoperative residual intimal tear Postoperative patency of false lumen RR, relative risk; CI, confidence interval. Univariate Multivariate p-value RR 95% CI p-value DISCUSSION After surgical repair of acute type I aortic dissection, the distal dissected aorta is usually left untreated leaving the downstream aorta in danger of developing aortic aneurysm. Park et al. [7] identified several risk factors for the development of descending aortic aneurysm after the surgical repair of acute type I aortic dissection including patent or wide false lumens, larger aortic diameter, Marfan syndrome, younger age, and male sex. In agreement with the cited study, many studies have also indicated the patent false lumen as a strong risk factor for distal aortic dilatation, late death, and requirements for distal aorta reintervention [3,5,6,8,14]. As non-exclusion of the primary intimal tear has also been revealed as a risk factor for aortic dilatation [9], various surgical procedures to exclude an intimal tear and thereby to obliterate the false lumen have been suggested in previous studies. For instance, a group advocated the routine performance of the total arch replacement in type I aortic dissection in order to exclude an invisible intimal tear, and revealed an acceptable operative risk and improved long-term outcomes [15]. Recently, several groups reported on the use of arch replacement combined with stent-graft implantation in the proximal descending aorta in the setting of acute type I aortic dissection [16,17]. The most important purpose of these efforts is to prevent descending aortic aneurysm by inducing false lumen thrombosis. On the other hand, another study reported that total arch replacement was associated with greater morbidity and mortality than hemiarch replacement in acute type I aortic dissection [18]. Of note, Sakaguchi et al. [10] reported that although the patency of the false lumen was associated with poor prognosis, but it was not influenced by the extent of the aortic replacement. With respect to this, an accurate identification of the intimal tears preoperatively is very important to avoid an unnecessarily extensive arch replacement, which may increase morbidity or mortality. In this study, we evaluated the effects of the intimal tear as well as the patency of the false lumen on the development of descending aortic aneurysm. We attempted to resect proximal intimal tears as much as possible in all individuals, but it was not achieved in two patients (4.9%), in whom the intimal tear was invisible in the operating field. In the present study, we supposed that the intimal tear was indispensible to the patency of the false lumen and demonstrated that patients with a residual intimal tear had a greater propensity to have false lumen patency. Nevertheless, only 14 patients among 31 patients who had no residual intimal tear showed complete obliteration of the false lumen. This finding indicates that the sensitivity of dual-source CT may still be limited in the detection of very small intimal tears that have hemodynamic significance. This retrospective non-randomized study has several limitations. First, the follow-up CT scans were not taken at 11
7 Yun Seok Kim, et al the same interval, and the cumulative rate of the aortic dilatation might have been affected. Second, we included patients who survived more than 6 months and followed them by dual-source CT. This might have caused a selection bias. Third, the number of samples was relatively small (n=41), and we could not collect more samples because we introduced dual-source CT only in November In conclusion, the presence of a residual intimal tear following surgery for acute type I aortic dissection adversely influenced the descending aorta in the late period. These results indicate that efforts should be directed to the obliteration of the distal re-entry tear in the development of forthcoming surgical techniques for acute type I aortic dissection. CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Booher AM, Isselbacher EM, Nienaber CA, et al. The IRAD classification system for characterizing survival after aortic dissection. Am J Med 2013;126:730.e Kim JB, Lee CH, Lee TY, et al. Descending aortic aneurysmal changes following surgery for acute DeBakey type I aortic dissection. Eur J Cardiothorac Surg 2012;42: Zierer A, Voeller RK, Hill KE, Kouchoukos NT, Damiano RJ Jr, Moon MR. Aortic enlargement and late reoperation after repair of acute type A aortic dissection. Ann Thorac Surg 2007;84: Halstead JC, Meier M, Etz C, et al. The fate of the distal aorta after repair of acute type A aortic dissection. J Thorac Cardiovasc Surg 2007;133: Immer FF, Hagen U, Berdat PA, Eckstein FS, Carrel TP. Risk factors for secondary dilatation of the aorta after acute type A aortic dissection. Eur J Cardiothorac Surg 2005;27: Yeh CH, Chen MC, Wu YC, Wang YC, Chu JJ, Lin PJ. Risk factors for descending aortic aneurysm formation in medium-term follow-up of patients with type A aortic dissection. Chest 2003;124: Park KH, Lim C, Choi JH, et al. Midterm change of descending aortic false lumen after repair of acute type I dissection. Ann Thorac Surg 2009;87: Kimura N, Tanaka M, Kawahito K, Yamaguchi A, Ino T, Adachi H. Influence of patent false lumen on long-term outcome after surgery for acute type A aortic dissection. J Thorac Cardiovasc Surg 2008;136:1160-6, 1166.e Unosawa S, Hata M, Niino T, Shimura K, Shiono M. Prognosis of patients undergoing emergency surgery for type A acute aortic dissection without exclusion of the intimal tear. J Thorac Cardiovasc Surg 2013;146: Sakaguchi G, Komiya T, Tamura N, et al. Patency of distal false lumen in acute dissection: extent of resection and prognosis. Interact Cardiovasc Thorac Surg 2007;6: Maldjian PD, Partyka L. Intimal tears in thoracic aortic dissection: appearance on MDCT with virtual angioscopy. AJR Am J Roentgenol 2012;198: Quint LE, Platt JF, Sonnad SS, Deeb GM, Williams DM. Aortic intimal tears: detection with spiral computed tomography. J Endovasc Ther 2003;10: Hiratzka LF, Bakris GL, Beckman JA, et al ACCF/AHA/AATS/ACR/ASA/SCA/SCAI/SIR/STS/SVM guidelines for the diagnosis and management of patients with Thoracic Aortic Disease: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines, American Association for Thoracic Surgery, American College of Radiology, American Stroke Association, Society of Cardiovascular Anesthesiologists, Society for Cardiovascular Angiography and Interventions, Society of Interventional Radiology, Society of Thoracic Surgeons, and Society for Vascular Medicine. Circulation 2010;121:e Fattouch K, Sampognaro R, Navarra E, et al. Long-term results after repair of type a acute aortic dissection according to false lumen patency. Ann Thorac Surg 2009;88: Hirotani T, Nakamichi T, Munakata M, Takeuchi S. Routine extended graft replacement for an acute type A aortic dissection and the patency of the residual false channel. Ann Thorac Surg 2003;76: Kato M, Kuratani T, Kaneko M, Kyo S, Ohnishi K. The results of total arch graft implantation with open stent-graft placement for type A aortic dissection. J Thorac Cardiovasc Surg 2002;124: Pochettino A, Brinkman WT, Moeller P, et al. Antegrade thoracic stent grafting during repair of acute DeBakey I dissection prevents development of thoracoabdominal aortic aneurysms. Ann Thorac Surg 2009;88: Kim JB, Chung CH, Moon DH, et al. Total arch repair versus hemiarch repair in the management of acute DeBakey type I aortic dissection. Eur J Cardiothorac Surg 2011;40:
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery
 Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Is close radiographic and clinical control after repair of acute type A aortic dissection really necessary for improved long-term survival?
 doi:10.1510/icvts.2010.239764 Interactive CardioVascular and Thoracic Surgery 11 (2010) 620 625 www.icvts.org Best evidence topic - Aortic and aneurysmal Is close radiographic and clinical control after
doi:10.1510/icvts.2010.239764 Interactive CardioVascular and Thoracic Surgery 11 (2010) 620 625 www.icvts.org Best evidence topic - Aortic and aneurysmal Is close radiographic and clinical control after
Long-Term Predictors of Descending Aorta Aneurysmal Change in Patients With Aortic Dissection
 Journal of the American College of Cardiology Vol. 50, No. 8, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.03.064
Journal of the American College of Cardiology Vol. 50, No. 8, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.03.064
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Effect of false lumen partial thrombosis on repaired acute type A aortic dissection
 Acquired Cardiovascular Disease Tsai et al Effect of false lumen partial thrombosis on repaired acute type A aortic dissection Meng-Ta Tsai, MD, a Hsuan-Yin Wu, MD, a,b Jun-Neng Roan, MD, a,c Yi-Shan Tsai,
Acquired Cardiovascular Disease Tsai et al Effect of false lumen partial thrombosis on repaired acute type A aortic dissection Meng-Ta Tsai, MD, a Hsuan-Yin Wu, MD, a,b Jun-Neng Roan, MD, a,c Yi-Shan Tsai,
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Update on Acute Aortic Syndrome
 SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
SUNDAY Update on Acute Aortic Syndrome Diana Litmanovich, MD Learning objectives To be familiar with the definition, natural history, and imaging findings of acute aortic syndrome, including: I. Aortic
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation
 Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias. UCSF Vascular Symposium April 7-9, Acute Aortic Dissection
 Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Aortic Dissection: Natural History What is the Natural History of Aortic Dissection? UCSF Vascular Symposium April 7-9, 2011 Asymptomatic Radiology / Clinical data Report / Cohort bias Referral bias Stephen
Effects of Early Anticoagulation on the Degree of Thrombosis After Repair of Acute DeBakey Type I Aortic Dissection
 Effects of Early Anticoagulation on the Degree of Thrombosis After Repair of Acute DeBakey Type I Aortic Dissection Suk-Won Song, MD, PhD, Kyung-Jong Yoo, MD, PhD, Do-Kyun Kim, MD, Bum-Koo Cho, MD, PhD,
Effects of Early Anticoagulation on the Degree of Thrombosis After Repair of Acute DeBakey Type I Aortic Dissection Suk-Won Song, MD, PhD, Kyung-Jong Yoo, MD, PhD, Do-Kyun Kim, MD, Bum-Koo Cho, MD, PhD,
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD
 Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Early outcomes of acute retrograde dissection in the aortic arch and the ascending aorta data from IRAD Foeke JH Nauta, MD, PhD Resident Cardiothoracic Surgery, Academic Medical Center, Amsterdam Disclosure
Long-Term Results After Repair of Type A Acute Aortic Dissection According to False Lumen Patency
 Long-Term Results After Repair of Type A Acute Aortic Dissection According to False Lumen Patency Khalil Fattouch, MD, PhD, Roberta Sampognaro, MD, Emiliano Navarra, MD, Marco Caruso, MD, PhD, Calogera
Long-Term Results After Repair of Type A Acute Aortic Dissection According to False Lumen Patency Khalil Fattouch, MD, PhD, Roberta Sampognaro, MD, Emiliano Navarra, MD, Marco Caruso, MD, PhD, Calogera
Acute Aortic Dissection: Decision and Outcome
 Acute Aortic Dissection: Decision and Outcome Marc R. Moon, M.D. John M. Shoenberg Chair in CV Disease Chief, Cardiac Surgery Director, Center for Diseases of the Thoracic Aorta Washington University School
Acute Aortic Dissection: Decision and Outcome Marc R. Moon, M.D. John M. Shoenberg Chair in CV Disease Chief, Cardiac Surgery Director, Center for Diseases of the Thoracic Aorta Washington University School
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Midterm Results of Aortic Arch Replacement in a Stanford Type A Aortic Dissection With an Intimal Tear in the Aortic Arch
 ORIGINAL ARTICLE DOI 10.4070 / kcj.2009.39.7.270 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Midterm Results of Aortic Arch Replacement in a Stanford
ORIGINAL ARTICLE DOI 10.4070 / kcj.2009.39.7.270 Print ISSN 1738-5520 / On-line ISSN 1738-5555 Copyright c 2009 The Korean Society of Cardiology Midterm Results of Aortic Arch Replacement in a Stanford
Department of Cardiovascular Surgery, Beijing Anzhen Hospital of Capital Medical University, Beijing Aortic Disease Center, Beijing, China;
 Featured Article Sun s procedure of total arch replacement using a tetrafurcated graft with stented elephant trunk implantation: analysis of early outcome in 398 patients with acute type A aortic dissection
Featured Article Sun s procedure of total arch replacement using a tetrafurcated graft with stented elephant trunk implantation: analysis of early outcome in 398 patients with acute type A aortic dissection
What Determines Aortic False Lumen Growth Post Dissection?
 Aortic Dissections What Determines Aortic False Lumen Growth Post Dissection? UCSF Vascular Symposium April 26, 2012 Most common aortic emergency Incidence of aortic dissections are 2/100,000 person-years
Aortic Dissections What Determines Aortic False Lumen Growth Post Dissection? UCSF Vascular Symposium April 26, 2012 Most common aortic emergency Incidence of aortic dissections are 2/100,000 person-years
Strategies in the surgical treatment of type A aortic arch dissection
 Perspective Strategies in the surgical treatment of type A aortic arch dissection Jehangir J. Appoo 1*, Zlatko Pozeg 2* 1 Libin Cardiovascular Institute of Alberta, Division of Cardiac Surgery, Department
Perspective Strategies in the surgical treatment of type A aortic arch dissection Jehangir J. Appoo 1*, Zlatko Pozeg 2* 1 Libin Cardiovascular Institute of Alberta, Division of Cardiac Surgery, Department
Therapeutic Pathway In Acute Aortic Dissection. Speaker: Cesare Quarto Consultant Cardiac Surgeon Royal Brompton Hospital, London UK
 Therapeutic Pathway In Acute Aortic Dissection Speaker: Cesare Quarto Consultant Cardiac Surgeon Royal Brompton Hospital, London UK Disclosure of Interest Speaker name: Cesare Quarto I do not have any
Therapeutic Pathway In Acute Aortic Dissection Speaker: Cesare Quarto Consultant Cardiac Surgeon Royal Brompton Hospital, London UK Disclosure of Interest Speaker name: Cesare Quarto I do not have any
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D.
 Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Do the Data Support Endovascular Therapy for Descending Thoracic AD? Woong Chol Kang, M.D. Gil Hospital, Gachon University Incheon, Korea Classification of AD Acute vs. Chronic (2weeks) (IIIa, b) type
Descending endograft for DeBakey type 1 aortic dissection: pro
 Perspective Descending endograft for DeBakey type 1 aortic dissection: pro Paolo Berretta, Marco Di Eusanio Division of Cardiac Surgery, G. Mazzini Hospital, Teramo, Italy Correspondence to: Marco Di Eusanio.
Perspective Descending endograft for DeBakey type 1 aortic dissection: pro Paolo Berretta, Marco Di Eusanio Division of Cardiac Surgery, G. Mazzini Hospital, Teramo, Italy Correspondence to: Marco Di Eusanio.
Accepted Manuscript. Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi
 Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Animesh Rathore, MD 4/22/17. The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management
 Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Frozen Elephant Trunk in Acute Aortic Dissection
 Frozen Elephant Trunk in Acute Aortic Dissection Derek R. Brinster, M.D. Professor of Cardiovascular and Thoracic Surgery Hofstra North Shore-LIJ School of Medicine Director of Aortic Surgery for the North
Frozen Elephant Trunk in Acute Aortic Dissection Derek R. Brinster, M.D. Professor of Cardiovascular and Thoracic Surgery Hofstra North Shore-LIJ School of Medicine Director of Aortic Surgery for the North
No Disclosure. Aortic Dissection in Japan. This. The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair
 No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
No Disclosure The Challenge of Acute and Chronic Type B Aortic Dissections with Endovascular Aortic Repair Toru Kuratani Department of Cardiovascular Surgery Osaka University Graduate School of Medicine,
Understanding the Predictors of Aneurysmal Degeneration in Type B Dissection
 Understanding the Predictors of Aneurysmal Degeneration in Type B Dissection A case example illustrating when early endovascular intervention may provide the best outcome. BY DITTMAR BÖCKLER, MD, PhD;
Understanding the Predictors of Aneurysmal Degeneration in Type B Dissection A case example illustrating when early endovascular intervention may provide the best outcome. BY DITTMAR BÖCKLER, MD, PhD;
Endovascular surgery in Marfan syndrome: CON
 Perspective Endovascular surgery in Marfan syndrome: CON Nicholas T. Kouchoukos Division of Cardiovascular and Thoracic Surgery, Missouri Baptist Medical Center, BJC Healthcare, St. Louis, Missouri, USA
Perspective Endovascular surgery in Marfan syndrome: CON Nicholas T. Kouchoukos Division of Cardiovascular and Thoracic Surgery, Missouri Baptist Medical Center, BJC Healthcare, St. Louis, Missouri, USA
Emerging Roles for Distal Aortic Interventions in Type A Dissection Surgery
 Emerging Roles for Distal Aortic Interventions in Type A Dissection Surgery Type A Dissection Workshop 2014 CCC Vancouver Oct 26 th, 2014 Jehangir Appoo Libin Cardiovascular Institute University of Calgary
Emerging Roles for Distal Aortic Interventions in Type A Dissection Surgery Type A Dissection Workshop 2014 CCC Vancouver Oct 26 th, 2014 Jehangir Appoo Libin Cardiovascular Institute University of Calgary
Effects of partial thrombosis on distal aorta after repair of acute DeBakey type I aortic dissection
 Song et al Acquired Cardiovascular Disease Effects of partial on distal aorta after repair of acute DeBakey type I aortic dissection Suk-Won Song, MD, PhD, a Byung-Chul Chang, MD, PhD, b Bum-Koo Cho, MD,
Song et al Acquired Cardiovascular Disease Effects of partial on distal aorta after repair of acute DeBakey type I aortic dissection Suk-Won Song, MD, PhD, a Byung-Chul Chang, MD, PhD, b Bum-Koo Cho, MD,
Importance of false lumen thrombosis in type B aortic dissection prognosis
 Importance of false lumen thrombosis in type B aortic dissection prognosis Santi Trimarchi, MD, PhD, a Jip L. Tolenaar, MD, a Frederik H. W. Jonker, MD, PhD, b Brian Murray, MD, c Thomas T. Tsai, MD, d
Importance of false lumen thrombosis in type B aortic dissection prognosis Santi Trimarchi, MD, PhD, a Jip L. Tolenaar, MD, a Frederik H. W. Jonker, MD, PhD, b Brian Murray, MD, c Thomas T. Tsai, MD, d
Is there a way to predict the risk in uncomplicated Type B aortic dissections? FRANS MOLL University Medical Centre Utrecht - Netherlands
 Is there a way to predict the risk in uncomplicated Type B aortic dissections? FRANS MOLL University Medical Centre Utrecht - Netherlands Disclosures: - Consultant Philips Health Care - Best Doctors Overview
Is there a way to predict the risk in uncomplicated Type B aortic dissections? FRANS MOLL University Medical Centre Utrecht - Netherlands Disclosures: - Consultant Philips Health Care - Best Doctors Overview
Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider
 Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider Matthias Thielmann, MD, PhD, FAHA Thoracic and Cardiovascular Surgery, West-German Heart and Vascular Center
Optimised management of type A aortic dissection with visceral malperfusion concept to reconsider Matthias Thielmann, MD, PhD, FAHA Thoracic and Cardiovascular Surgery, West-German Heart and Vascular Center
Early- and medium-term results after aortic arch replacement with frozen elephant trunk techniques a single center study
 Featured Article Early- and medium-term results after aortic arch replacement with frozen elephant trunk techniques a single center study Sergey Leontyev*, Martin Misfeld*, Piroze Daviewala, Michael A.
Featured Article Early- and medium-term results after aortic arch replacement with frozen elephant trunk techniques a single center study Sergey Leontyev*, Martin Misfeld*, Piroze Daviewala, Michael A.
Frozen Elephant Trunk procedure in patients with aortic dissection type B and concomitant aortic arch or ascending aortic pathology
 Frozen Elephant Trunk procedure in patients with aortic dissection type B and concomitant aortic arch or ascending aortic pathology Eduard Charchyan MD, PhD, Yurii Belov MD, PhD, Denis Breshenkov, Alexey
Frozen Elephant Trunk procedure in patients with aortic dissection type B and concomitant aortic arch or ascending aortic pathology Eduard Charchyan MD, PhD, Yurii Belov MD, PhD, Denis Breshenkov, Alexey
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Scientific Exhibit. Authors: D. Takenaka, Y. Ohno, Y. Onishi, K. Matsumoto, T.
 The feasibility of biphasic contrast-media-injection-protocol for chest imaging on 320-slice volume MDCT: Direct comparison of biphasic and bolus contrast-media injection protocols on 320-slice volume
The feasibility of biphasic contrast-media-injection-protocol for chest imaging on 320-slice volume MDCT: Direct comparison of biphasic and bolus contrast-media injection protocols on 320-slice volume
Treatment of acute type B aortic dissection: Current status
 MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
MEET Cannes, 18. - 21.06.2009 Treatment of acute type B aortic dissection: Current status Christoph A. Nienaber, MD, FACC University of Rostock Department of Internal Medicine, Cardiology christoph.nienaber@med.uni-rostock.de
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when?
 Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
Acute Type B dissection. Closure of the infra diaphragmatic tear: how and when? Prof. Olgierd Rowiński II Department of Clinical Radiology Medical University of Warsaw Disclosure Speaker name: Olgierd
IMAGING the AORTA. Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011
 IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
IMAGING the AORTA Mirvat Alasnag FACP, FSCAI, FSCCT, FASE June 1 st, 2011 September 11, 2003 Family is asking $67 million in damages from two doctors Is it an aneurysm? Is it a dissection? What type of
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Extended Arch Techniques for Acute Aortic Dissection: a systematic review and classification
 Extended Arch Techniques for Acute Aortic Dissection: a systematic review and classification Holly Smith PGY2 Thoracic Aortic Rounds, Foothills Hospital September 25, 2015 Libin Cardiovascular Institute
Extended Arch Techniques for Acute Aortic Dissection: a systematic review and classification Holly Smith PGY2 Thoracic Aortic Rounds, Foothills Hospital September 25, 2015 Libin Cardiovascular Institute
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection: Con
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection: Con Thomas G. Gleason, M.D. Ronald V. Pellegrini Professor and Chief Division of Cardiac Surgery University of Pittsburgh Presenter
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection: Con Thomas G. Gleason, M.D. Ronald V. Pellegrini Professor and Chief Division of Cardiac Surgery University of Pittsburgh Presenter
STS/EACTS LatAm CV Conference 2017
 STS/EACTS LatAm CV Conference 2017 Joseph E. Bavaria, MD Director, Thoracic Aortic Surgery Program Roberts-Measey Professor and Vice Chair of CV Surgery University of Pennsylvania Immediate-Past President
STS/EACTS LatAm CV Conference 2017 Joseph E. Bavaria, MD Director, Thoracic Aortic Surgery Program Roberts-Measey Professor and Vice Chair of CV Surgery University of Pennsylvania Immediate-Past President
Total Endovascular Repair Type A Dissection. Eric Herget Interventional Radiology
 Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Total Endovascular Repair Type A Dissection Eric Herget Interventional Radiology 65 year old male Acute Type A Dissection Severe Aortic Regurgitation No co-morbidities Management? Part II Evolving Global
Acute Aortic Syndromes
 Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Acute Aortic Syndromes Carole J. Dennie, MD Acute Thoracic Aortic Syndromes Background Non-Traumatic Acute Thoracic Aortic Syndromes Carole Dennie MD FRCPC Associate Professor of Radiology and Cardiology
Influence of patent false lumen on long-term outcome after surgery for acute type A aortic dissection
 Surgery for Acquired Cardiovascular Disease Kimura et al Influence of patent false lumen on long-term outcome after surgery for acute type A aortic dissection Naoyuki Kimura, MD, a Masashi Tanaka, MD,
Surgery for Acquired Cardiovascular Disease Kimura et al Influence of patent false lumen on long-term outcome after surgery for acute type A aortic dissection Naoyuki Kimura, MD, a Masashi Tanaka, MD,
Type A acute aortic dissection (A-AAD) remains to
 30 YASUDA S et al. Circ J 2017; 81: 30 35 ORIGINAL ARTICLE doi: 10.1253/circj.CJ-16-0462 Aortic Disease Evaluation and Influence of Brachiocephalic Branch Re-entry in Patients With Type A Acute Aortic
30 YASUDA S et al. Circ J 2017; 81: 30 35 ORIGINAL ARTICLE doi: 10.1253/circj.CJ-16-0462 Aortic Disease Evaluation and Influence of Brachiocephalic Branch Re-entry in Patients With Type A Acute Aortic
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Endovascular Treatment of Malperfusion Syndrome
 Endovascular Treatment of Malperfusion Syndrome in Type B Aortic Dissection Department of Cardiology, Pusan National luniveristy i Hospital, Han Cheol Lee Endovascular Treatment Indication of Type B Aortic
Endovascular Treatment of Malperfusion Syndrome in Type B Aortic Dissection Department of Cardiology, Pusan National luniveristy i Hospital, Han Cheol Lee Endovascular Treatment Indication of Type B Aortic
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine
 Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
The morbidity and mortality rates associated with the. Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection
 Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection Tomoki Shimokawa, MD, Kazutaka Horiuchi, MD, Naomi Ozawa, MD, Kenu Fumimoto, MD, Susumu Manabe, MD, Tetsuya Tobaru, MD, and
Outcome of Surgical Treatment in Patients With Acute Type B Aortic Dissection Tomoki Shimokawa, MD, Kazutaka Horiuchi, MD, Naomi Ozawa, MD, Kenu Fumimoto, MD, Susumu Manabe, MD, Tetsuya Tobaru, MD, and
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Chronic type A dissection: when to operate? Francois Dagenais, MD PII: S0022-5223(18)33131-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.032 Reference: YMTC 13781 To appear in: The
Accepted Manuscript Chronic type A dissection: when to operate? Francois Dagenais, MD PII: S0022-5223(18)33131-3 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.032 Reference: YMTC 13781 To appear in: The
Type II arch hybrid debranching procedure
 Safeguards and Pitfalls Type II arch hybrid debranching procedure Prashanth Vallabhajosyula, Wilson Y. Szeto, Nimesh Desai, Caroline Komlo, Joseph E. Bavaria Division of Cardiovascular Surgery, University
Safeguards and Pitfalls Type II arch hybrid debranching procedure Prashanth Vallabhajosyula, Wilson Y. Szeto, Nimesh Desai, Caroline Komlo, Joseph E. Bavaria Division of Cardiovascular Surgery, University
Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist. M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria
 Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Evidence Surgical aortic arch replacement with a Dacron
Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Evidence Surgical aortic arch replacement with a Dacron
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns
 CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
CT angiography in type I acute aortic dissection complicated with malperfusion - a visual review of obstruciton patterns Eneva M. St. Ekaterna University Hospital Report objectives 1. Review malperfusion
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations
 The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
The Petticoat Technique Managing Type B Dissection with both Early and Long Term Considerations Joseph V. Lombardi, MD Professor & Chief, Division of Vascular & Endovascular Surgery Department of Surgery,
CLINICAL RESEARCH. Zhihuang Qiu Liangwan Chen Hua Cao Guican Zhang Fan Xu Qiang Chen
 e-issn 1643-3750 DOI: 10.12659/MSM.892492 Received: 2014.09.15 Accepted: 2014.10.28 Published: 2015.03.04 Analysis of Risk Factors for Acute Kidney Injury after Ascending Aortic Replacement Combined with
e-issn 1643-3750 DOI: 10.12659/MSM.892492 Received: 2014.09.15 Accepted: 2014.10.28 Published: 2015.03.04 Analysis of Risk Factors for Acute Kidney Injury after Ascending Aortic Replacement Combined with
Dissection de type B: l étude Instead et corollaire stratégique
 Dissection de type B: l étude Instead et corollaire stratégique Christoph A. Nienaber, MD, FACC University Rostock Heartcenter Med. Clinic I Cardiology christoph.nienaber@med.uni-rostock.de Type B aortic
Dissection de type B: l étude Instead et corollaire stratégique Christoph A. Nienaber, MD, FACC University Rostock Heartcenter Med. Clinic I Cardiology christoph.nienaber@med.uni-rostock.de Type B aortic
Femoral Versus Aortic Cannulation for Surgery of Chronic Ascending Aortic Aneurysm
 Femoral Versus Aortic Cannulation for Surgery of Chronic Ascending Aortic Aneurysm Fitsum Lakew, MD, Piotr Pasek, MD, Michael Zacher, MD, Anno Diegeler, MD, and Paul P. Urbanski, MD Department of Cardiovascular
Femoral Versus Aortic Cannulation for Surgery of Chronic Ascending Aortic Aneurysm Fitsum Lakew, MD, Piotr Pasek, MD, Michael Zacher, MD, Anno Diegeler, MD, and Paul P. Urbanski, MD Department of Cardiovascular
When and how to replace the aortic arch for type A dissection
 Perspective When and how to replace the aortic arch for type A dissection Roberto Di Bartolomeo, Alessandro Leone, Luca Di Marco, Davide Pacini Cardiac Surgery Department, S. Orsola-Malpighi Hospital,
Perspective When and how to replace the aortic arch for type A dissection Roberto Di Bartolomeo, Alessandro Leone, Luca Di Marco, Davide Pacini Cardiac Surgery Department, S. Orsola-Malpighi Hospital,
Joseph E. Bavaria, MD
 EACTS Master Class on Aortic Valve Repair Joseph E. Bavaria, MD Director, Thoracic Aortic Surgery Program Roberts Measey Professor and Vice Chair of CV Surgery University of Pennsylvania Immediate-Past
EACTS Master Class on Aortic Valve Repair Joseph E. Bavaria, MD Director, Thoracic Aortic Surgery Program Roberts Measey Professor and Vice Chair of CV Surgery University of Pennsylvania Immediate-Past
Multimodality Imaging of the Thoracic Aorta
 Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Multimodality Imaging of the Thoracic Aorta Steven Goldstein MD, FACC Director Noninvasive Cardiology MedStar Heart and Vascular Institute Washington Hospital Center Saturday, October 8, 2016 DISCLOSURE
Total arch replacement with separated graft technique and selective antegrade cerebral perfusion
 Masters of Cardiothoracic Surgery Total arch replacement with separated graft technique and selective antegrade cerebral perfusion Teruhisa Kazui 1,2 1 Hamamatsu University School of Medicine, Hamamatsu,
Masters of Cardiothoracic Surgery Total arch replacement with separated graft technique and selective antegrade cerebral perfusion Teruhisa Kazui 1,2 1 Hamamatsu University School of Medicine, Hamamatsu,
Prediction of Intimal Tear Site by Computed Tomography in Acute Aortic Dissection Type A
 Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Prediction of Intimal Tear Site by Computed Tomography in Acute Aortic Dissection Type A Jun Sung Kim, MD 1, Kay-Hyun Park, MD 1, Cheong Lim,
Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Prediction of Intimal Tear Site by Computed Tomography in Acute Aortic Dissection Type A Jun Sung Kim, MD 1, Kay-Hyun Park, MD 1, Cheong Lim,
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
OPEN AND ENDOVASCULAR TECHNIQUES IN THE CARDIOTHORACIC SURGEON S HANDS
 4 th Aortic Live Symposium OPEN AND ENDOVASCULAR TECHNIQUES IN THE CARDIOTHORACIC SURGEON S HANDS A/Prof George Matalanis Director Cardiac Surgery Austin Hospital Disclosure I do not have any potential
4 th Aortic Live Symposium OPEN AND ENDOVASCULAR TECHNIQUES IN THE CARDIOTHORACIC SURGEON S HANDS A/Prof George Matalanis Director Cardiac Surgery Austin Hospital Disclosure I do not have any potential
Acute non-complicated TBD Do need TEVAR treatment
 Acute non-complicated TBD Do need TEVAR treatment Prof. Dr. med. Christoph A. Nienaber Universität Rostock Universitäres Herzzentrum christoph.nienaber@med.uni-rostock.de Survival in type B dissection
Acute non-complicated TBD Do need TEVAR treatment Prof. Dr. med. Christoph A. Nienaber Universität Rostock Universitäres Herzzentrum christoph.nienaber@med.uni-rostock.de Survival in type B dissection
Clinical Trials of Acute and Chronic Dissections. Gregory Landry MD
 Clinical Trials of Acute and Chronic Dissections Gregory Landry MD No disclosures Acute vs chronic dissection: Definitions 1950s: Acute < 2 weeks, Chronic > 2 weeks 2013: European Interdisciplinary Consensus
Clinical Trials of Acute and Chronic Dissections Gregory Landry MD No disclosures Acute vs chronic dissection: Definitions 1950s: Acute < 2 weeks, Chronic > 2 weeks 2013: European Interdisciplinary Consensus
Neurological outcomes and mortality in patients with type A aortic dissection. Impact of intra-operative management
 Neurological outcomes and mortality in patients with type A aortic dissection. Impact of intra-operative management P Santé, M. Buonocore L Majello, A Caiazzo, G Petrone, G Nappi Dept. of Cardiothoracic
Neurological outcomes and mortality in patients with type A aortic dissection. Impact of intra-operative management P Santé, M. Buonocore L Majello, A Caiazzo, G Petrone, G Nappi Dept. of Cardiothoracic
128-slice dual-source CT coronary angiography using highpitch scan protocols in 102 patients
 128-slice dual-source CT coronary angiography using highpitch scan protocols in 102 patients Poster No.: C-0634 Congress: ECR 2010 Type: Scientific Exhibit Topic: Cardiac Authors: Y. H. Choe, J. W. Lee,
128-slice dual-source CT coronary angiography using highpitch scan protocols in 102 patients Poster No.: C-0634 Congress: ECR 2010 Type: Scientific Exhibit Topic: Cardiac Authors: Y. H. Choe, J. W. Lee,
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D.
 CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
Morphological analysis of the thoracic aorta in case of TBAD without treatment.
 Master project: Hemodynamic pattern of type B aortic dissection progression and remodelling of the false lumen after endovascular treatment: imaging informed numerical simulations Aortic dissection is
Master project: Hemodynamic pattern of type B aortic dissection progression and remodelling of the false lumen after endovascular treatment: imaging informed numerical simulations Aortic dissection is
Lulu Liu, Chaoyi Qin, Jianglong Hou, Da Zhu, Bengui Zhang, Hao Ma, Yingqiang Guo
 Case Report One-stage hybrid surgery for acute Stanford type A aortic dissection with David operation, aortic arch debranching, and endovascular graft: a case report Lulu Liu, Chaoyi Qin, Jianglong Hou,
Case Report One-stage hybrid surgery for acute Stanford type A aortic dissection with David operation, aortic arch debranching, and endovascular graft: a case report Lulu Liu, Chaoyi Qin, Jianglong Hou,
debris + 3 debris debris debris Tel: ,3
 13 467 471 2004 debris + 3 13.2 15.47.0 6.5 7.7 0 3 25.012.5 7.0 0 13 467 471 2004 Tel: 075-251-5752 602-8566 463-1 2004 3 7 2004 5 18 30 1 2,3 4 2000 7 debris debris debris 7 13 4 Table 1 Patients profiles
13 467 471 2004 debris + 3 13.2 15.47.0 6.5 7.7 0 3 25.012.5 7.0 0 13 467 471 2004 Tel: 075-251-5752 602-8566 463-1 2004 3 7 2004 5 18 30 1 2,3 4 2000 7 debris debris debris 7 13 4 Table 1 Patients profiles
Another pregnancy after a previous aortic dissection in pregnancy?
 Another pregnancy after a previous aortic dissection in pregnancy? Dr Leisa Freeman GUCH & Maternal Cardiology Unit Norfolk & Norwich University Hospital UK Arterial wall changes & haemodynamic effects
Another pregnancy after a previous aortic dissection in pregnancy? Dr Leisa Freeman GUCH & Maternal Cardiology Unit Norfolk & Norwich University Hospital UK Arterial wall changes & haemodynamic effects
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR
 Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept
 The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
The role of false lumen intervention to promote remodelling via induced thrombosis the FLIRT concept Professor Christoph A. Nienaber The Royal Brompton and Harefield NHS Trust Cardiology and Aortic Centre
Aortic CT: Intramural Hematoma. Leslie E. Quint, M.D.
 Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Aortic CT: Intramural Hematoma Leslie E. Quint, M.D. 43 M Mid back pain X several months What type of aortic disease? A. Aneurysm with intraluminal thrombus B. Chronic dissection with thrombosed false
Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta
 02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
TEVAR for Chronic dissections: indications for TEVAR, long term results
 TEVAR for Chronic dissections: indications for TEVAR, long term results J Sobocinski, R Azzaoui, B Maurel, R Spear, T Martin-Gonzalez, A Hertault, S Haulon Centre de l Aorte, Chirurgie vasculaire, Hôpital
TEVAR for Chronic dissections: indications for TEVAR, long term results J Sobocinski, R Azzaoui, B Maurel, R Spear, T Martin-Gonzalez, A Hertault, S Haulon Centre de l Aorte, Chirurgie vasculaire, Hôpital
Vascular Intervention
 10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
10 : 389-393, 2001 B Vascular Intervention 1 1 2 1 1 1 1 3 2 1 1997 7 2000 4 B 29 19 10 50 84 66.1 stent graft S/G primary entry stenting S/G 12 4 2 1 1 40 mm 8 1 MOF 1 endoleak + 11 91.6% 10 stenting
Are stent-grafts for acute type B dissection durable? Est-ce que les stents graft pour la dissection aigue de type B sont efficaces à moyen terme?
 Are stent-grafts for acute type B dissection durable? Est-ce que les stents graft pour la dissection aigue de type B sont efficaces à moyen terme? Martin Björck, Johnny Steuer, Anders Wanhainen Uppsala
Are stent-grafts for acute type B dissection durable? Est-ce que les stents graft pour la dissection aigue de type B sont efficaces à moyen terme? Martin Björck, Johnny Steuer, Anders Wanhainen Uppsala
Disclosures: Acute Aortic Syndrome. A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO
 Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Midterm Change of Descending Aortic False Lumen After Repair of Acute Type I Dissection
 Midterm Change of Descending Aortic False Lumen After Repair of Acute Type I Dissection Kay-Hyun Park, MD, PhD, Cheong Lim, MD, PhD, Jin Ho Choi, MD, Euisuk Chung, MD, Sang Il Choi, MD, PhD, Eun Ju Chun,
Midterm Change of Descending Aortic False Lumen After Repair of Acute Type I Dissection Kay-Hyun Park, MD, PhD, Cheong Lim, MD, PhD, Jin Ho Choi, MD, Euisuk Chung, MD, Sang Il Choi, MD, PhD, Eun Ju Chun,
Covered stent graft for distal stent graft-induced new entry after frozen elephant trunk operation for aortic dissection.
 Research Article http://www.alliedacademies.org/annals-of-cardiovascular-and-thoracic-surgery/ Covered stent graft for distal stent graft-induced new entry after frozen elephant trunk operation for aortic
Research Article http://www.alliedacademies.org/annals-of-cardiovascular-and-thoracic-surgery/ Covered stent graft for distal stent graft-induced new entry after frozen elephant trunk operation for aortic
Verbrede mediastinum: Treatment
 Verbrede mediastinum: Treatment Klinische les - Cardiale Heelkunde Gabriele Bislenghi ASO Heelkunde UZ Leuven Moderator: prof. B. Meuris Overview Aortic dissection Boerhaave Aortic Dissection Aortic dissection
Verbrede mediastinum: Treatment Klinische les - Cardiale Heelkunde Gabriele Bislenghi ASO Heelkunde UZ Leuven Moderator: prof. B. Meuris Overview Aortic dissection Boerhaave Aortic Dissection Aortic dissection
Aortic Dissection in BAV Patients: The IRAD Experience and Beyond
 Aortic Dissection in BAV Patients: The IRAD Experience and Beyond Eduardo Bossone, MD, Ph.D, FESC, FACC Cardiology Division - Heart Dept. University of Salerno, Italy I have no financial relationships
Aortic Dissection in BAV Patients: The IRAD Experience and Beyond Eduardo Bossone, MD, Ph.D, FESC, FACC Cardiology Division - Heart Dept. University of Salerno, Italy I have no financial relationships
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad).
 Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad). AS. Eleshra, MD 1, T. Kölbel, MD, PhD 1, F. Rohlffs, MD 1, N. Tsilimparis, MD, PhD 1,2 Ahmed Eleshra
Endovascular therapy for Ischemic versus Nonischemic complicated acute type B aortic dissection (catbad). AS. Eleshra, MD 1, T. Kölbel, MD, PhD 1, F. Rohlffs, MD 1, N. Tsilimparis, MD, PhD 1,2 Ahmed Eleshra
Is a Paradigm Shift towards Early Endovascular Treatment of Type B Dissection justified?
 Is a Paradigm Shift towards Early Endovascular Treatment of Type B Dissection justified? Dittmar Böckler Department of Vascular and Endovascular Surgery University of Heidelberg, Germany Disclosure Speaker
Is a Paradigm Shift towards Early Endovascular Treatment of Type B Dissection justified? Dittmar Böckler Department of Vascular and Endovascular Surgery University of Heidelberg, Germany Disclosure Speaker
Extra-Anatomic Ascending Aorta to Abdominal Aorta Bypass in Takayasu Arteritis Patients with Mid-Aortic Syndrome
 Korean J Thorac Cardiovasc Surg 2017;50:270-274 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2017.50.4.270 in Takayasu Arteritis Patients with Mid-Aortic
Korean J Thorac Cardiovasc Surg 2017;50:270-274 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2017.50.4.270 in Takayasu Arteritis Patients with Mid-Aortic
Case 9799 Stanford type A aortic dissection: US and CT findings
 Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
Case 9799 Stanford type A aortic dissection: US and CT findings Accogli S, Aringhieri G, Scalise P, Angelini G, Pancrazi F, Bemi P, Bartolozzi C Department of Diagnostic and Interventional Radiology, University
UC SF An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR. Disclosures.
 An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR Disclosures Royalties and research grant support from Cook Medical, Inc. Jade S. Hiramoto,
An Algorithm to Choose Which Uncomplicated (Asymptomatic) Acute Type B Dissection Patients Should Undergo TEVAR Disclosures Royalties and research grant support from Cook Medical, Inc. Jade S. Hiramoto,
The MAIN-COMPARE Study
 Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
Long-Term Outcomes of Coronary Stent Implantation versus Bypass Surgery for the Treatment of Unprotected Left Main Coronary Artery Disease Revascularization for Unprotected Left MAIN Coronary Artery Stenosis:
